Hospitals today are overwhelmed with data. Vitals, diagnostics, lab results, medication records, and sensor outputs come in around the clock, across many departments, multiple shifts, and thousands of patients. The issue lies within the struggle to act on clinical data and information correctly and in a timely manner.
Clinical AI monitoring helps close that gap. When designed correctly for enterprises, these platforms detect patient deterioration early, reveal patterns that clinicians might miss, and provide insights that significantly change how hospitals respond to risks, thereby enhancing trust and, by default, sign-up rates.
Intellivon has spent years developing AI systems for complex and high-stakes environments. This experience influences our view of clinical platforms, not as mere software projects, but as essential infrastructure that must gain the trust of clinicians, administrators, and compliance teams all at once. This blog outlines what a serious investment in a clinical AI monitoring platform entails. It discusses architectural choices, regulatory issues, and how we build these platforms from the ground up.
Why Hospitals Need Real-Time Clinical AI Monitoring Systems
Hospitals are deploying real-time clinical AI monitoring systems as AI becomes more common in patient care. These platforms detect model drift, bias, and performance failures as they occur, helping ensure safer diagnostics.
They integrate directly with EHR systems to provide continuous oversight of clinical AI models. Adoption is also accelerating due to FDA regulatory expectations and growing liability risks in high-stakes healthcare environments.
According to Future Market Insights, the clinical AI governance market is expected to grow to USD 2.48 billion in 2026 and could reach USD 71.12 billion by 2036, reflecting a 39.9% CAGR during the forecast period.
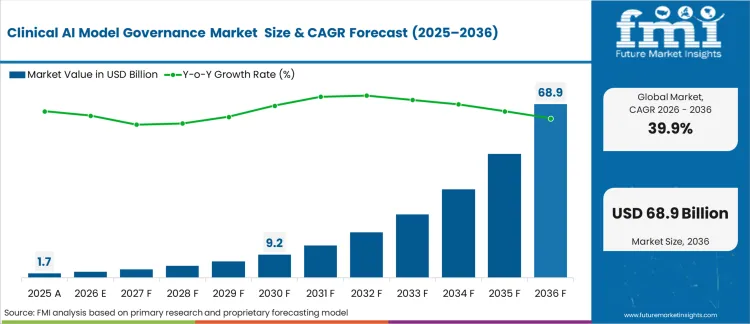
Healthcare systems face a critical transition from reactive care to proactive prevention. Investing in real-time clinical AI monitoring is no longer a luxury but a fundamental necessity for modern hospital operations.
Implementing clinical AI monitoring allows for the identification of subtle physiological shifts hours before a code blue occurs. This early window enables cheaper, less invasive treatments that protect the hospital’s bottom line.
What Is a Clinical AI Monitoring Platform?
A clinical AI monitoring platform is a sophisticated software layer that integrates real-time patient data with predictive analytics. Unlike traditional monitors that simply track current vitals, these platforms use machine learning to identify patterns of physiological decline.
They aggregate information from electronic health records, bedside devices, and laboratory results. By providing early warning scores, they empower clinical teams to intervene proactively before a medical crisis occurs.
Key Capabilities Hospitals Expect From These Platforms
Investing in clinical AI requires more than just raw predictive power. High-value platforms must seamlessly integrate into the high-stakes environment of a modern hospital while providing clear, actionable insights for diverse medical teams.
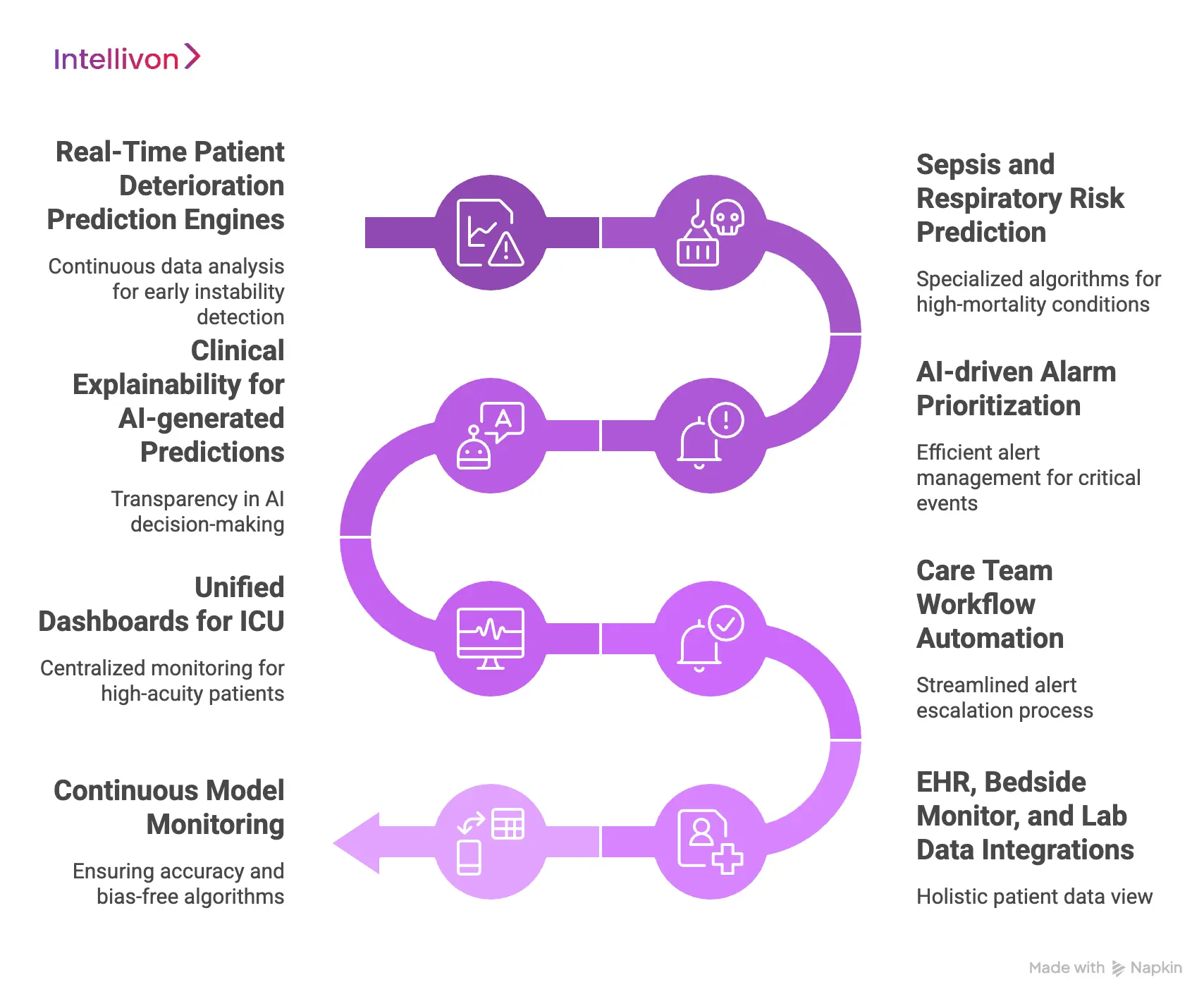
1. Real-Time Patient Deterioration Prediction Engines
At the core of these platforms is the ability to process continuous data streams without latency. These engines analyze heart rate, blood pressure, and oxygen levels to find subtle markers of instability.
Unlike manual scoring systems, the AI operates in real-time, providing a dynamic risk profile for every bed in the facility. This capability ensures that clinical staff are always one step ahead of a potential crisis.
2. Sepsis and Respiratory Risk Prediction
Specific clinical pathways require specialized algorithms to be effective. A robust platform provides dedicated models for high-mortality conditions like sepsis, which often goes undetected in its early stages.
By identifying the inflammatory response or respiratory distress early, the system triggers life-saving protocols. These targeted predictions allow for precise medical interventions that significantly improve survival rates.
3. AI-driven Alarm Prioritization
Efficiency in a hospital is often hampered by “noise” from unnecessary alerts. Advanced platforms categorize alarms based on clinical urgency and the likelihood of a genuine event.
This prioritization ensures that a nurse’s attention is directed toward the most critical patient first. By reducing the cognitive load on staff, the hospital can maintain a calmer and more focused care environment.
4. Clinical Explainability for AI-generated Predictions
Trust is the most important currency in healthcare technology. Doctors will not act on a “black box” alert without knowing the underlying reason. Modern platforms provide “explainability” by highlighting exactly which vitals or lab trends triggered the warning.
This transparency allows the clinical team to validate the AI’s logic against their own professional observations.
5. Unified Dashboards for ICU
Centralized monitoring allows a single specialized team to oversee dozens of high-acuity patients simultaneously. These dashboards aggregate data into a “mission control” view, ranking patients by their current risk scores.
This high-level visibility is essential for resource planning and identifying which units require additional support. It transforms fragmented bedside data into a cohesive enterprise-wide strategy.
6. Care Team Workflow Automation
A prediction is only useful if it reaches the right person at the right time. Sophisticated platforms automate the escalation process by routing alerts directly to the rapid response team or the attending physician’s mobile device.
If an alert is not acknowledged within a set timeframe, the system automatically escalates it to the next level of seniority. This ensures that critical warnings never expire quietly at a nursing station.
7. EHR, Bedside Monitor, and Lab Data Integrations
For AI to be accurate, it must have a holistic view of the patient’s history and current status. The platform must pull data from the Electronic Health Record (EHR), real-time bedside monitors, and the laboratory information system.
This deep integration prevents data silos and allows the AI to consider comorbidities and medication history when calculating risk. A unified data layer is the prerequisite for any high-performing clinical AI.
8. Continuous Model Monitoring
Healthcare is dynamic, and AI models can “drift” over time as clinical practices or patient demographics change. Enterprise-grade platforms include built-in monitoring to ensure the algorithms remain accurate and unbiased.
Regular audits and performance checks are mandatory to maintain regulatory compliance and patient safety. This commitment to ongoing validation protects the hospital from the risks of outdated or inaccurate technology.
The integration of these capabilities creates a proactive safety net. By focusing on both technical depth and clinical utility, these platforms become indispensable assets for any forward-thinking healthcare enterprise.
Hospital Data Sources Powering Clinical AI Monitoring
High-performance clinical AI is only as reliable as the data it consumes. For an enterprise-grade platform, the strategy involves aggregating fragmented data points into a high-fidelity digital twin of the patient’s physiological state.
1. Bedside Monitors and ICU Telemetry Streams
The primary engine for real-time monitoring is the continuous flow of high-frequency waveform data. Bedside monitors capture heart rates, arterial blood pressure, and oxygen saturation levels every second.
Traditional systems often discard this granular information after it flashes on the screen. However, clinical AI platforms ingest these streams to identify micro-trends that precede a visible crash. This “invisible” data layer is the most critical asset for early warning systems.
2. Electronic Health Record Patient Histories
Context is what transforms a simple alert into a sophisticated clinical insight. By pulling longitudinal data from the Electronic Health Record (EHR), the AI understands a patient’s baseline. It factors in chronic conditions, past surgeries, and current medication lists to weight its predictions.
For example, a slight uptick in heart rate is interpreted differently for a marathon runner than for a patient with heart failure. This historical depth prevents the “one-size-fits-all” flaw of legacy monitoring.
3. Laboratory and Diagnostic Imaging Data
Biochemical markers often provide the first objective signs of internal distress, such as rising lactate levels in sepsis. The platform must integrate directly with laboratory information systems to incorporate these intermittent data points.
When combined with automated imaging reports, the AI can correlate physical vitals with internal biological changes. This multi-modal approach ensures that the system monitors the patient from both the inside and the outside.
4. Ventilator and Respiratory Device Telemetry
Respiratory failure is a leading cause of ICU mortality, making ventilator data indispensable. These devices provide technical metrics like tidal volume, peak inspiratory pressure, and oxygen concentration.
AI models analyze these variables to predict “ventilator dyssynchrony” or the readiness of a patient for weaning. By monitoring how a patient breathes against the machine, the platform helps clinicians optimize respiratory support and reduce time on mechanical ventilation.
5. Wearable and Remote Patient Monitoring Devices
As care shifts toward “hospital-at-home” models, the data perimeter is expanding beyond the four walls of the facility. Medical-grade wearables provide continuous telemetry for patients in lower-acuity wards or even their own homes.
These devices feed data into the central monitoring hub via secure cloud gateways. This ensures that the safety net remains intact even when a patient is no longer physically tethered to a bedside monitor.
6. Clinical Notes and Physician Observations
Some of the most valuable data is “unstructured,” hidden within the free-text notes of nurses and doctors. Natural Language Processing (NLP) allows the platform to scan these notes for qualitative observations, such as “patient appears confused” or “increased work of breathing.”
These human observations often catch symptoms that machines cannot yet sense. Integrating these notes ensures that the AI respects and utilizes the collective intuition of the frontline clinical staff.
Building a robust data pipeline is the most significant hurdle for any hospital’s AI strategy. Once these sources are unified, the platform transforms from a simple tool into a comprehensive enterprise intelligence asset.
Clinical AI Monitoring Platform Architecture
Designing an enterprise-grade monitoring platform requires a shift from monolithic software toward a distributed, resilient architecture. To maintain patient safety, the system must process massive data volumes with sub-second latency while ensuring complete clinical transparency.
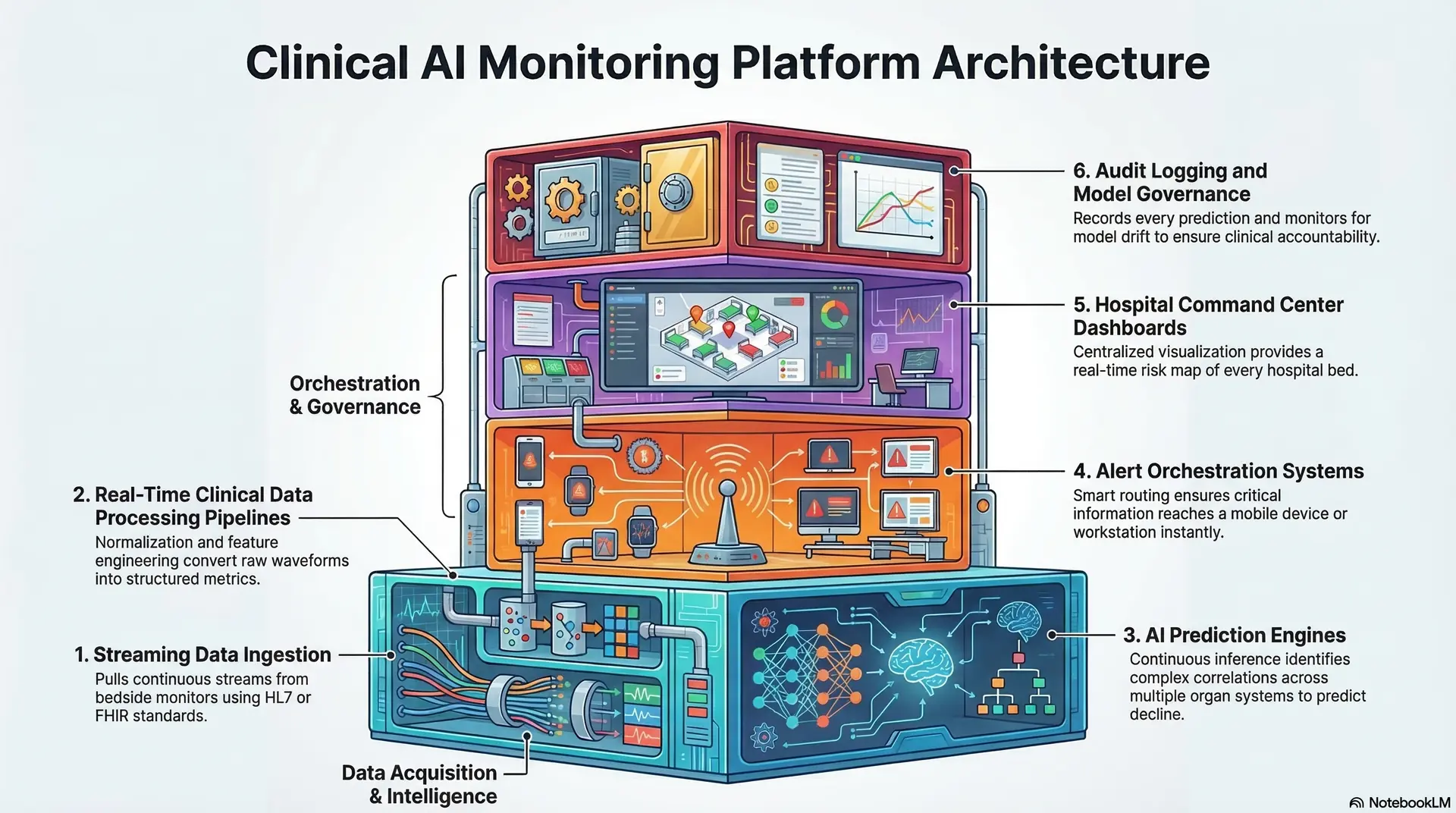
1. Streaming Data Ingestion
The architectural foundation begins with high-capacity ingestion gateways designed for medical data protocols. These gateways pull continuous streams from bedside monitors using HL7 or FHIR standards.
Because clinical data is often noisy or fragmented, the ingestion layer must handle packet loss without compromising the integrity of the patient record.
This stage ensures that every heartbeat and breath is captured as a clean, digital data point. Reliable ingestion is the prerequisite for any real-time clinical intervention strategy.
2. Real-Time Clinical Data Processing Pipelines
Once data enters the system, it passes through specialized processing pipelines for normalization and feature engineering. Raw waveforms are converted into structured metrics that the AI models can interpret.
This layer also handles “data fusion,” where asynchronous laboratory results are synchronized with synchronous heart rate trends. By cleaning and labeling data in flight, the platform prevents the “garbage in, garbage out” problem that plagues lower-tier solutions. These pipelines must be highly scalable to manage surges in data during peak hospital hours.
3. AI Prediction Engines
The intelligence layer consists of specialized machine learning models trained on millions of hours of physiological data. These engines run continuous inference, comparing a patient’s current state against known patterns of clinical decline. Rather than relying on simple thresholds, the AI identifies complex correlations across multiple organ systems.
For example, a stable blood pressure combined with a rising respiratory rate might trigger an early sepsis warning. This predictive power allows the platform to move beyond simple monitoring into active diagnostic support.
4. Alert Orchestration Systems
A high-performance architecture must include a sophisticated orchestration engine to manage alert distribution. This system applies logic-based rules to determine which clinician receives a specific notification based on their role and current shift.
It manages the “state” of an alert, tracking whether it has been seen, acknowledged, or escalated. By using “smart routing,” the platform ensures that critical information reaches a mobile device or workstation instantly. This reduces the time-to-treatment, which is the most vital metric in acute care.
5. Hospital Command Center Dashboards
Centralized visualization serves as the “cockpit” for the entire facility or health system. The architecture supports high-concurrency dashboards that provide a real-time risk map of every hospital bed.
These views allow senior clinicians to spot trends across different units and reallocate staffing resources as needed.
Because these dashboards are often the primary interface for decision-makers, they must be intuitive and lag-free. A unified view eliminates the silos that often lead to missed clinical events.
6. Audit Logging and Model Governance
For any platform operating in a regulated healthcare environment, a robust governance layer is mandatory. This infrastructure records every prediction made by the AI, along with the specific data points that influenced that decision. It allows for retrospective “root cause analysis” if a clinical event occurs or if a model requires retraining.
Furthermore, it monitors for “model drift” to ensure that the AI’s accuracy does not degrade over time. This layer provides the legal and clinical accountability necessary for enterprise-wide adoption.
A well-architected platform balances technical performance with clinical utility. When these components work in harmony, they create a resilient digital infrastructure that protects patients and optimizes hospital operations.
AI Models Used In Clinical Monitoring Platforms
Selecting the right algorithmic framework is a strategic decision that determines a platform’s clinical utility and predictive accuracy. For high-acuity environments, engineers deploy a hierarchy of models designed to process temporal data and extract hidden physiological markers.
1. Time-Series Deep Learning
Recurrent Neural Networks (RNNs) and Long Short-Term Memory (LSTM) networks are the workhorses of vitals analysis. These models are specifically engineered to process sequential data, such as continuous heart rate or arterial pressure.
By “remembering” previous data points, they can identify the trajectory of a patient’s health rather than just a snapshot in time. This longitudinal perspective is critical for distinguishing a temporary spike from a systemic decline.
Consequently, deep learning provides the foundation for identifying subtle trends that escape the human eye.
2. Transformer Models
Originally developed for natural language, Transformer architectures are now revolutionizing clinical monitoring through “Attention” mechanisms. These models can weigh the importance of different data inputs simultaneously, such as correlating a drop in oxygen with a specific lab result from six hours prior.
Transformers excel at handling “multi-modal” data, where diverse signals like waveforms and EHR notes must be synthesized. This high-dimensional analysis allows the platform to understand the broader clinical context of every patient.
It essentially provides a more sophisticated, “wide-lens” view of the intensive care unit.
3. Early Warning Score Prediction Models
While deep learning handles complexity, traditional machine learning models like Random Forests or Gradient Boosting are often used for standardized early warning scores. These models are highly efficient at binary classification, such as predicting whether a patient will require intubation within the next twelve hours.
They provide a high degree of “feature importance” transparency, showing exactly which vitals are driving the risk score. This balance of speed and interpretability makes them ideal for broad-scale screening across entire hospital wards. They serve as the first line of defense in automated patient surveillance.
4. Clinical Anomaly Detection Algorithms
Not every dangerous clinical event follows a known pattern, which is where unsupervised anomaly detection becomes vital. These algorithms establish a “baseline of normalcy” for each individual patient and trigger an alert when physiological behavior deviates from that norm.
This is particularly useful for identifying rare complications or equipment malfunctions that standard models might miss. By focusing on “outliers,” these systems provide an additional layer of safety that doesn’t rely on pre-defined disease labels. It ensures that the “unknown unknowns” of clinical care are still monitored.
5. Reinforcement learning for care workflow optimization
Beyond predicting illness, Reinforcement Learning (RL) is used to optimize the “action” side of the clinical equation. These models learn the best sequence of interventions to stabilize a patient or move them toward discharge.
RL agents can simulate thousands of patient trajectories to determine how staffing adjustments or bed assignments impact overall hospital throughput. This moves the AI from a passive observer to a strategic partner in operational efficiency. Ultimately, it helps leadership align clinical excellence with resource optimization.
The orchestration of these diverse model types creates a comprehensive intelligence layer. By matching the specific clinical challenge to the right mathematical approach, hospitals can achieve unprecedented levels of predictive precision and operational control.
Compliance Requirements For Clinical AI Platforms
Navigating the regulatory landscape is a strategic mandate for any enterprise-grade healthcare solution. For investors and developers, compliance ensures structural integrity, protecting the organization from significant legal and operational liabilities.
1. HIPAA Compliance
Foundational security starts with the Health Insurance Portability and Accountability Act (HIPAA). This requires robust administrative and technical safeguards to protect sensitive patient information (PHI).
Data must remain encrypted at rest and in transit using industry-standard protocols. Strict access controls ensure that only authorized personnel interact with live telemetry streams.
2. FDA SaMD Requirements
Algorithms that provide medical diagnoses are classified as Software as a Medical Device (SaMD). This classification triggers rigorous pre-market reviews and Quality Management System (QMS) mandates.
The FDA focuses on analytical and clinical validation to ensure performance remains reliable in high-stakes environments. Navigating these pathways is essential for legal clinical adoption.
3. EU AI Act Implications
The EU AI Act categorizes medical AI as “High-Risk,” requiring strict transparency and human oversight. This legislation mandates that AI systems remain traceable and perform consistently throughout their lifecycle.
Adhering to these global standards early ensures a platform is future-proofed for international expansion and ethical scaling.
4. Clinical Audit Trails and Explainable Predictions
Regulatory bodies demand a clear digital paper trail for every automated output. An audit trail captures the specific input data and the model version used for every risk score.
This transparency allows for “root cause analysis” if an adverse event occurs. It mitigates legal risks by proving the AI’s logic was grounded in verifiable clinical markers.
5. Risk Classification and Validation Processes
Every implementation must undergo formal risk classification to evaluate its impact on patient safety. This involves continuous performance monitoring to detect “model drift” as patient demographics change.
Validation is a continuous cycle of testing against gold-standard clinical data. A rigorous validation framework builds deep trust with hospital boards and financial stakeholders.
Compliance serves as a powerful competitive moat in the healthcare sector. By mastering these requirements, a platform transforms from a simple tool into a highly defensible, enterprise-ready asset.
Step-by-Step Process On How We Build A Clinical AI Monitoring Platform
Building an enterprise-grade clinical AI platform requires a disciplined engineering approach that balances technical innovation with medical safety.
At Intellivon, we follow a rigorous six-step methodology to ensure every deployment delivers measurable clinical impact and operational ROI.
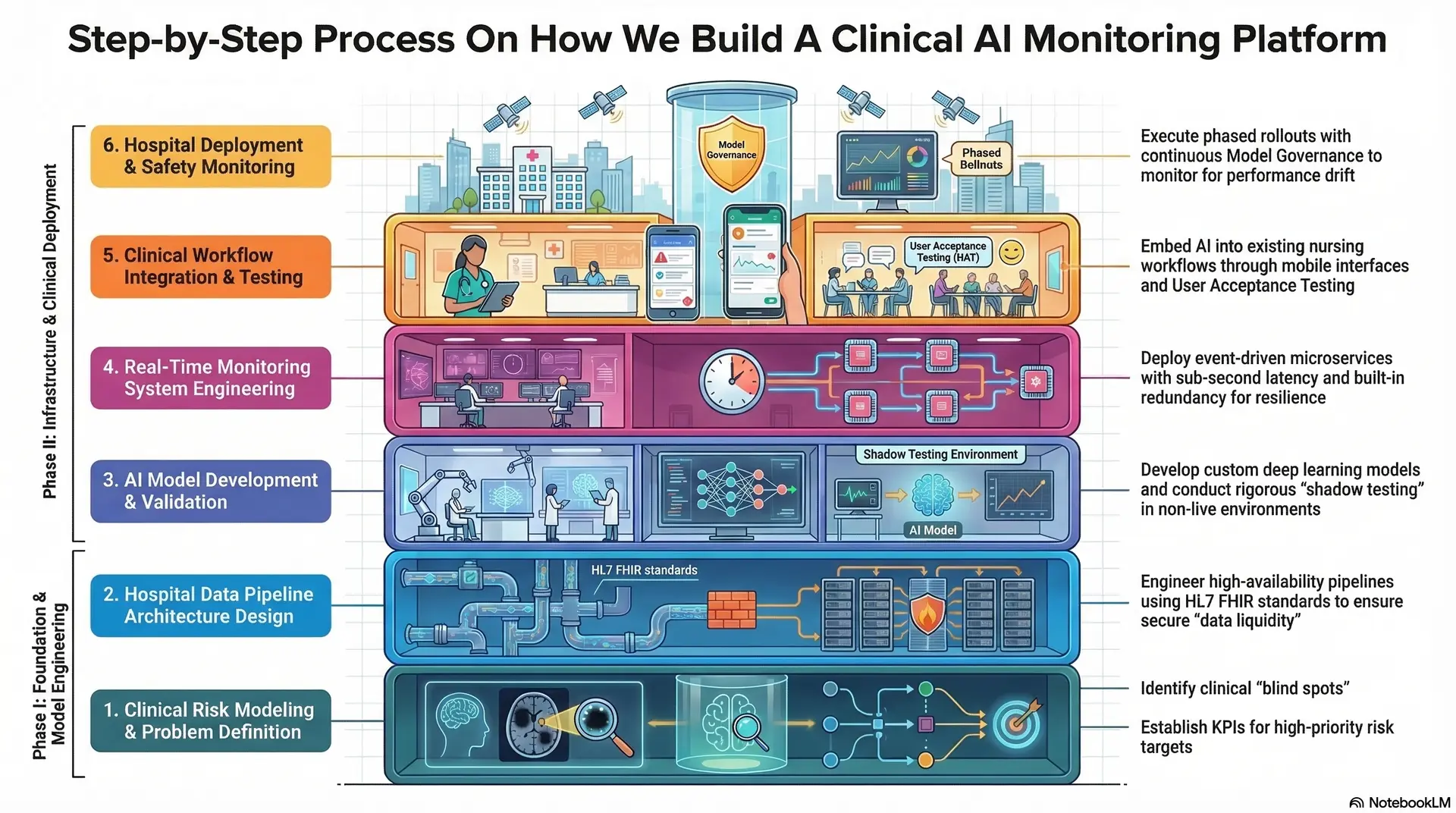
Step 1: Clinical Risk Modeling and Problem Definition
Success begins with identifying the specific clinical “blind spots” within a hospital’s current workflow. We collaborate with Chief Medical Officers to define high-priority risk targets, such as sepsis onset or post-surgical respiratory failure.
By establishing clear KPIs, we ensure the AI solution aligns with the hospital’s strategic safety goals. This phase grounds the technology in real-world medical necessity rather than abstract data science.
Step 2: Hospital Data Pipeline Architecture Design
We engineer high-availability data pipelines capable of ingesting massive telemetry streams from diverse bedside monitors and EHR systems.
Our architects prioritize “data liquidity,” ensuring that information flows securely across the hospital’s internal network without latency. We implement HL7 FHIR standards to maintain interoperability and ensure the system can scale as more wards are added. This robust data foundation is the prerequisite for reliable real-time inference.
Step 3: AI Model Development and Validation
The Intellivon engineering team develops custom deep learning models tailored to the hospital’s specific patient demographics. We utilize historical datasets to train these models, focusing on high precision to minimize the “noise” of false alarms.
Each model undergoes “shadow testing,” where its predictions are compared against actual clinical outcomes in a non-live environment. This rigorous validation ensures the AI is medically sound before it ever touches a live patient record.
Step 4: Real-Time Monitoring System Engineering
We build the high-concurrency infrastructure needed to process live vitals and trigger instant alerts. This involves deploying event-driven microservices that can handle thousands of concurrent data points with sub-second latency.
The engineering focus here is on “resilience”, ensuring the platform remains operational even during local network fluctuations. We integrate redundancy at every level to guarantee that a critical alert is never lost in the digital ether.
Step 5: Clinical Workflow Integration and Testing
Technology is only effective if clinicians actually use it, so we embed the AI directly into existing nursing and physician workflows. We design intuitive mobile interfaces and centralized command center dashboards that prioritize the most urgent cases.
During this phase, we conduct extensive “User Acceptance Testing” (UAT) with frontline staff to refine alert thresholds and escalation protocols. This ensures the platform acts as a supportive partner rather than a source of “technology fatigue.”
Step 6: Hospital Deployment and Safety Monitoring
The final step is a phased rollout, starting with high-acuity units like the ICU before expanding ward-wide. Post-deployment, Intellivon provides continuous “Model Governance,” monitoring for any signs of performance drift or algorithmic bias.
We establish a feedback loop where clinical teams can report “near misses,” allowing us to fine-tune the system in real-time. This commitment to ongoing safety monitoring ensures the platform remains a trusted asset for years to come.
This structured approach transforms a complex AI concept into a functional, life-saving reality. By focusing on both engineering excellence and clinical empathy, we provide a blueprint for the future of proactive hospital care.
Cost to Build a Clinical AI Monitoring Platform
At Intellivon, clinical AI monitoring platforms are built as a real-time clinical intelligence infrastructure, not as alert systems layered onto hospital software. The objective is to create a platform that continuously analyzes patient data streams and helps clinicians detect critical events earlier.
However, building an enterprise clinical AI monitoring platform requires more than connecting bedside monitors or EHR systems. The platform must ingest real-time medical data, run predictive models, filter false alarms, and deliver accurate alerts to the right clinical teams.
When implemented correctly, clinical AI monitoring platforms allow hospitals to detect deteriorating patients sooner, reduce alarm fatigue in intensive care units, and improve clinical decision-making under high-pressure conditions.
Estimated Phase-Wise Development Cost
| Phase | Description | Estimated Cost Range (USD) |
| Clinical Workflow Discovery & Platform Design | Define clinical monitoring objectives, patient risk models, ICU workflows, and hospital integration requirements | $6,000 – $12,000 |
| Real-Time Data Infrastructure | Build data pipelines that ingest streaming data from bedside monitors, EHR systems, and laboratory systems | $10,000 – $22,000 |
| Predictive AI Model Development | Develop and train machine learning models that predict acute clinical events such as sepsis, cardiac arrest, or respiratory failure | $10,000 – $25,000 |
| Signal Processing & Noise Reduction Systems | Implement algorithms that filter non-critical alerts and reduce alarm fatigue in clinical environments | $7,000 – $16,000 |
| Clinical Alerting & Decision Systems | Develop alert orchestration engines that notify clinicians based on patient risk levels and hospital workflows | $7,000 – $15,000 |
| Hospital System Integrations | Integrate the platform with EHR systems, bedside monitoring devices, and hospital data infrastructure | $10,000 – $24,000 |
| Security & Healthcare Data Protection | Implement encryption, secure patient data handling, and healthcare-grade security frameworks | $6,000 – $12,000 |
| Testing & Clinical Validation | Conduct system validation, clinical workflow testing, and predictive model performance optimization | $4,000 – $9,000 |
| Deployment & Infrastructure Setup | Configure cloud infrastructure, monitoring dashboards, and operational deployment systems | $4,000 – $8,000 |
Total Initial Investment
$65,000 – $170,000
Ongoing maintenance and monitoring typically require 15–20% of the initial development cost annually.
This supports continuous model retraining, monitoring updates, and infrastructure scaling as hospitals deploy additional AI monitoring systems.
Timeline to Launch a Clinical AI Monitoring Platform
The development timeline depends on the number of hospital systems integrated and the complexity of predictive models used.
| Phase | Estimated Timeline |
| Clinical workflow discovery & monitoring design | 2 – 3 weeks |
| Data pipeline and infrastructure setup | 3 – 4 weeks |
| AI model development & signal processing systems | 4 – 6 weeks |
| Clinical integrations & testing | 3 – 4 weeks |
| Deployment & operational preparation | 2 – 3 weeks |
Typical development timeline:
3 – 5 months for an enterprise clinical AI monitoring platform.
Hidden Costs Healthcare Organizations Should Plan For
Even well-designed monitoring platforms can face operational challenges when indirect costs are overlooked.
- Clinical data integration costs increase as hospitals connect multiple medical devices and data sources.
- Model retraining requirements grow as patient populations and clinical patterns change.
- Infrastructure costs rise as real-time monitoring systems process large volumes of patient data.
- Clinical workflow adjustments require training for doctors and nurses adopting AI-assisted monitoring systems.
- Regulatory validation becomes necessary when predictive AI tools influence medical decision-making.
Best Practices to Avoid Budget Overruns
Based on Intellivon’s experience building clinical AI platforms, several strategies help hospitals manage development costs effectively.
- Define clinical monitoring objectives and patient risk models early in the planning stage.
- Prioritize real-time data architecture capable of handling high-frequency medical data streams.
- Design AI monitoring systems that minimize false alarms to maintain clinician trust.
- Integrate the platform with existing hospital infrastructure rather than replacing core systems.
- Ensure that explainability features allow clinicians to understand AI predictions and alerts.
- Maintain observability across predictive models, data pipelines, and clinical alert systems.
Healthcare organizations planning to build a clinical AI monitoring platform can work with Intellivon’s healthcare AI engineers to design and deploy real-time monitoring infrastructure aligned with clinical workflows, patient safety goals, and long-term hospital AI strategies.
Conclusion
Building clinical AI monitoring is a strategic investment in hospital safety and operational growth. These platforms transform reactive care into a proactive, data-driven enterprise strategy. By reducing alarm fatigue and predicting deterioration, leadership can optimize resources while significantly improving patient outcomes.
Intellivon provides the cutting-edge, enterprise-grade AI solutions necessary to scale these complex systems. Partner with us to lead the next generation of high-reliability healthcare delivery today.
Build a Clinical AI Monitoring Platform With Intellivon
At Intellivon, clinical AI platforms are engineered as hospital intelligence infrastructure, not as analytics tools layered onto existing EHR systems.
We design real-time clinical monitoring platforms that integrate bedside telemetry, hospital systems, and predictive AI to identify patient deterioration early and support proactive clinical intervention.
Our systems are built to support high-acuity hospital environments, including intensive care units, emergency departments, and centralized monitoring centers.
Why Hospitals Partner With Intellivon
- Real-Time Clinical Intelligence Architecture: We build streaming platforms capable of processing thousands of patient signals simultaneously while generating predictive insights for hospital care teams.
- Predictive Deterioration Detection Models: Our AI models detect subtle physiological changes that signal sepsis, respiratory failure, or cardiac arrest before traditional monitoring thresholds trigger alerts.
- Alarm Fatigue Reduction Systems: We design intelligent alert prioritization engines that filter unnecessary alarms and notify the right clinician at the right time.
- Hospital System Integrations: Our platforms integrate with EHRs, bedside monitors, ventilators, and lab systems to unify patient monitoring across hospital departments.
- Compliance-Ready Clinical AI Systems: Every platform is built with explainability, audit logging, and governance frameworks aligned with HIPAA, FDA, and global medical AI regulations.
Organizations planning to build a clinical AI monitoring platform can partner with Intellivon’s healthcare AI experts to design and deploy real-time monitoring infrastructure aligned with clinical workflows, patient safety priorities, and hospital AI transformation strategies.
FAQs
Q1. What is a clinical AI monitoring platform?
A1. A clinical AI monitoring platform analyzes real-time patient data from bedside monitors, EHR systems, and labs. It predicts critical events early and alerts clinicians before conditions become life-threatening.
Q2. How do clinical AI monitoring systems work?
A2. These systems ingest continuous patient data streams and run predictive AI models. The platform identifies risk patterns and alerts medical teams when a patient shows signs of deterioration.
Q3. What conditions can clinical AI monitoring detect?
A3. Clinical AI monitoring platforms can detect risks such as sepsis, cardiac arrest, respiratory failure, and patient deterioration by analyzing real-time clinical data patterns.
Q4. How do AI monitoring platforms reduce alarm fatigue?
A4. AI monitoring platforms filter noisy signals from medical devices and prioritize clinically meaningful alerts. This ensures that clinicians only receive alerts when intervention is likely required.
Q5. How long does it take to build a clinical AI monitoring platform?
A5. Developing an enterprise clinical AI monitoring platform typically takes 3–5 months, depending on predictive model complexity and integrations with hospital systems.