Running several clinics in cities is a big challenge. This is because you need a plan for how you set up your systems. When you have clinics, patient information gets stuck in different places. At the same time, as you start scaling, it gets harder to manage with each new clinic. Additionally, the cost of using separate systems adds up and affects the budget profoundly. So using an EHR system that is based in the cloud is something you have to do if you want your healthcare network to keep growing.
However, not every EHR platform is built to handle patient information in multiple clinics at once. A system that performs well at three locations frequently fractures at fifteen because the architecture was never designed for that scale. The thing that really matters is how well the system can work with systems, how well it can adapt, and how well it can keep performing as your network gets bigger.
Intellivon makes quality systems that are based in the cloud and are made specifically for networks, with many clinics. In this blog, we will cover the architecture, compliance, AI workflows, and interoperability of these systems, with a focus on how our experts build them from the ground up.
Market Insights Of Cloud-Based EHR Systems
Cloud-based EHR systems now lead the market. They scale easily, reduce upfront costs, and integrate smoothly with AI and telehealth. As a result, they solve many operational issues seen in on-premise systems.
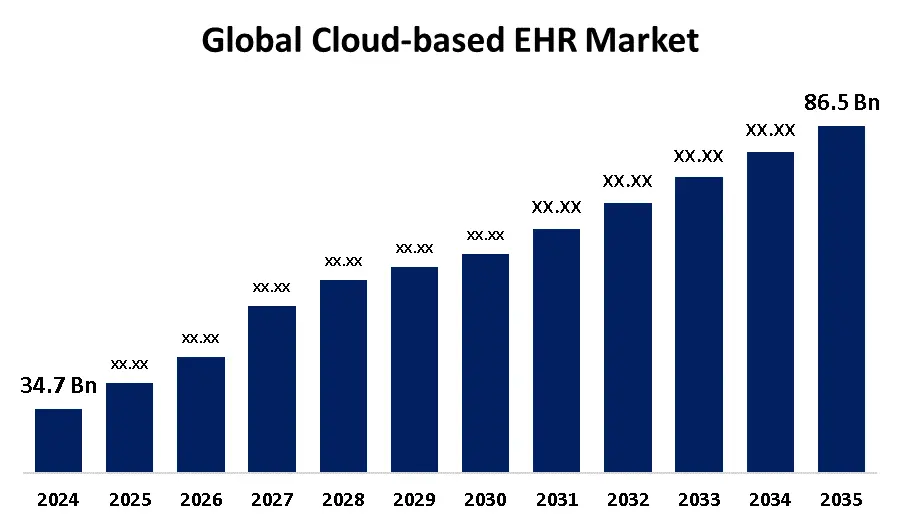
This growth is driven by the rising adoption of digital health solutions. Organizations are shifting to cloud systems because they are more cost-effective, accessible, and easier to scale across care networks.
What is a cloud-based EHR for clinic systems?
A cloud EHR for clinic systems is a centralized, web-based platform that manages patient health records, scheduling, and billing on remote servers. Unlike legacy on-premise software, these systems offer real-time data access across multiple locations via secure internet connections.
They eliminate the need for local hardware maintenance while providing automatic updates, high-level encryption, and seamless scalability to meet the evolving demands of modern enterprise healthcare environments.
How Cloud EHR Differs from Legacy Systems
Cloud-based EHR systems are built to support modern, distributed healthcare environments. In contrast, legacy systems were designed for single-location use and controlled infrastructure.
As healthcare organizations expand across multiple clinics, this difference becomes critical. Understanding how these systems operate helps decision-makers choose the right foundation for long-term scalability.
Cloud vs Legacy EHR: Key Differences
| Aspect | Cloud-Based EHR | Legacy (On-Premise) EHR |
| Deployment | Hosted on cloud infrastructure, accessed via the internet | Installed on local servers within the facility |
| Scalability | Easily scales across multiple clinics and users | Limited by physical infrastructure capacity |
| Access | Accessible anytime, anywhere across locations | Restricted to on-site or VPN-based access |
| Cost Structure | Lower upfront cost, subscription-based model | High upfront hardware and setup costs |
| Maintenance | Managed by a provider with automatic updates | Requires in-house IT for maintenance and upgrades |
| Integration | API-first, supports HL7, FHIR, third-party tools | Limited and often complex integrations |
| Data Synchronization | Real-time sync across all clinic locations | Delayed or manual data synchronization |
| Security & Compliance | Built-in cloud security and compliance frameworks | Dependent on internal infrastructure and controls |
| Performance at Scale | Designed for multi-location, high-volume usage | Performance degrades as the system expands |
Cloud-based EHR systems represent a shift in how healthcare infrastructure is designed. While legacy systems may still work for single clinics, they struggle to support growth, integration, and real-time coordination. As a result, multi-clinic systems increasingly move toward cloud-based EHR to enable scalability, efficiency, and connected care delivery.
Role of EHR In Multi-Clinic Operations
Managing a network of clinics requires more than just digitizing paper files; it requires a unified nervous system. A robust EHR ensures that a patient receiving care at one site has a consistent, up-to-date record available at any other location within the enterprise.
1. Standardizing Clinical Governance
In a multi-clinic environment, clinical protocols must remain consistent to ensure quality of care. A centralized EHR allows leaders to push standardized templates and workflows across the entire network.
Consequently, this reduces medical errors and ensures that every facility adheres to the same high standards of practice.
2. Centralized Financial and Operational Oversight
Managing multiple billing cycles and supply chains is impossible with fragmented data. An integrated EHR provides a “single pane of glass” for the CFO and operations team.
This visibility allows for real-time tracking of revenue cycles, patient volume, and resource allocation. Therefore, leadership can make data-driven decisions about where to expand or consolidate resources.
3. Seamless Patient Portability
Patients expect their medical history to follow them without manual faxing or phone calls. A unified system eliminates the need for duplicate intake forms and redundant testing.
By providing a “single source of truth,” the EHR improves the patient experience and builds long-term brand loyalty. Furthermore, it ensures that specialists have immediate access to primary care notes, closing the loop on patient safety.
Why do multi-clinic systems need cloud EHR?
Scaling a healthcare enterprise across multiple locations creates a “data fragmentation” crisis that on-premise systems cannot solve.
Cloud infrastructure acts as the glue, ensuring that administrative and clinical data move as fast as the patients themselves.
1. Managing patient data across locations
Fragmented data is a clinical risk. When a patient visits different clinics in your network, their history must be instantly available to every provider. A cloud EHR provides a single, synchronized database that updates in real-time.
This eliminates the need for manual record transfers and prevents dangerous gaps in medication history. Furthermore, it ensures that your data remains secure and accessible even if one physical location faces a hardware failure.
2. Standardizing workflows across clinics
Growth often leads to “process drift,” where every clinic begins practicing medicine differently. This lack of consistency makes it impossible to measure quality or efficiency accurately.
A cloud-based platform allows leadership to deploy unified clinical templates and administrative workflows globally. Consequently, whether a clinician is in New York or London, they follow the same optimized path.
This standardization is the only way to maintain a high “gold standard” of care across a massive enterprise.
3. Improving visibility and decision-making
Managing an enterprise without real-time data is like flying a plane blind. Legacy systems often require manual reports that are outdated by the time they reach the CFO’s desk. Cloud EHRs offer live dashboards that track everything from room utilization to billing cycles.
This level of visibility allows you to spot operational bottlenecks immediately. In addition, it provides the clean data sets required to feed AI models for predictive staffing and financial forecasting.
4. Scaling operations without system breakdown
Traditional software hits a wall when you add more locations, requiring expensive server upgrades and IT staff. Cloud-native systems are built for horizontal scaling, meaning they grow automatically with your volume. You can bring a new clinic online in days rather than months.
This elasticity ensures that system performance stays high, regardless of how many users are logged in simultaneously. Therefore, the technology becomes a growth enabler rather than a bottleneck for your expansion strategy.
At this stage, the decision is about building the right EHR infrastructure. This is where Intellivon works with healthcare enterprises to design and build scalable, API-first EHR platforms tailored to their operations.
What challenges do clinics face without EHR?
Operating a multi-clinic network without a centralized EHR creates invisible financial leaks and operational friction.
These systemic gaps limit your ability to scale and compromise the quality of clinical care across your enterprise.
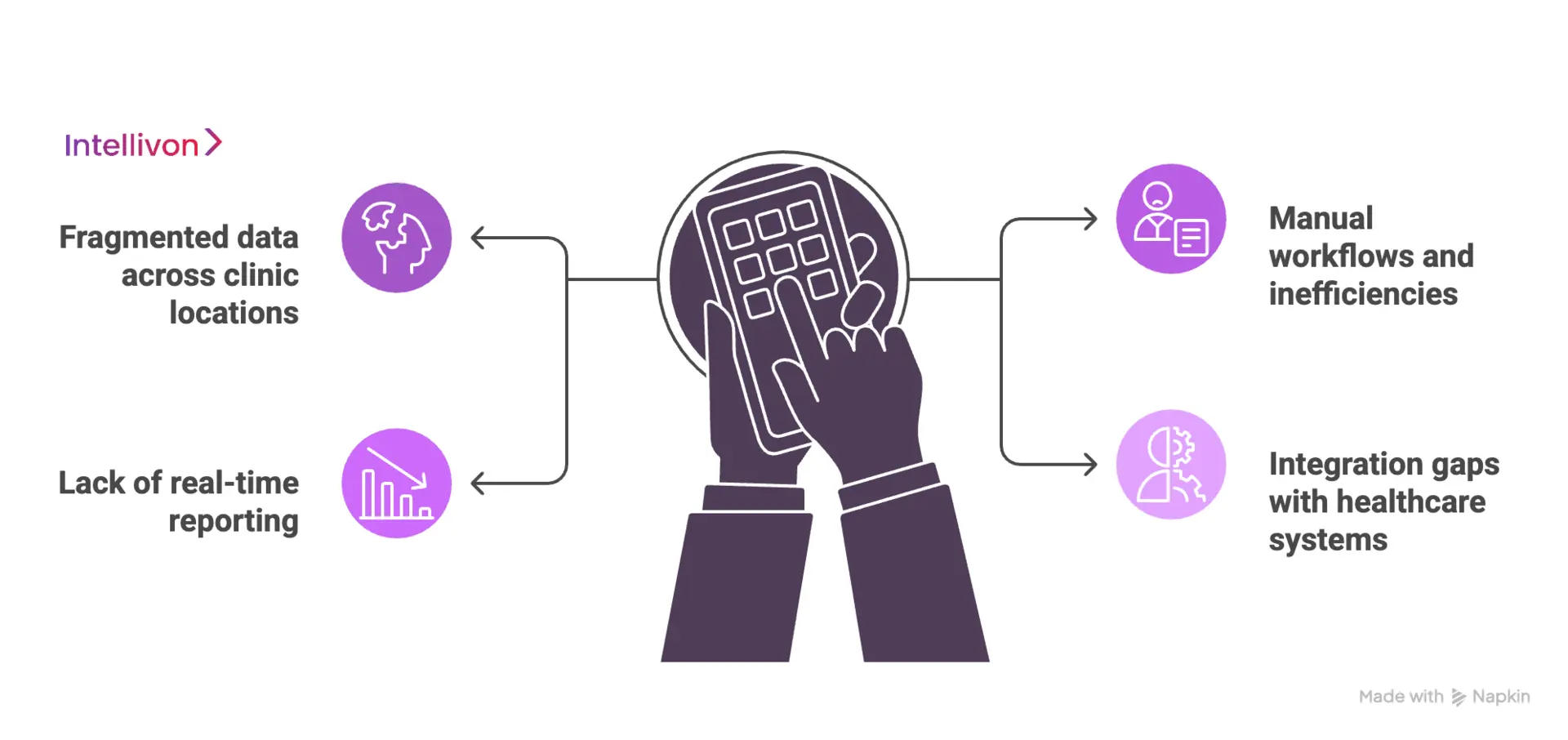
1. Fragmented data across clinic locations
Data silos are the biggest hurdle for growing healthcare brands. When patient records stay trapped at a single site, clinicians lose the “single source of truth” needed for safe, coordinated care.
This fragmentation leads to redundant testing and a disjointed experience that erodes patient trust.
2. Manual workflows and inefficiencies
Paper-based or basic digital processes act as a silent tax on your overhead. Staff spend hours on repetitive data entry, which triggers human error and increases administrative burnout.
Consequently, these manual bottlenecks slow down patient throughput and lead to frequent billing discrepancies that hurt your bottom line.
3. Lack of real-time reporting
Leadership cannot steer an enterprise effectively without immediate access to performance data. Relying on manual spreadsheets means your financial and clinical insights are often weeks out of date.
Therefore, you miss critical opportunities to reallocate resources or address declining patient volume in specific locations.
4. Integration gaps with healthcare systems
Isolated systems struggle to communicate with external labs, pharmacies, and insurance providers. These gaps create delays in treatment cycles and complicate the referral process.
Failing to integrate with the broader healthcare ecosystem limits your market reach and can lead to non-compliance with evolving industry standards.
Solving these foundational pain points is the first step toward building a resilient, data-driven organization. Transitioning to a unified cloud architecture transforms these liabilities into scalable assets for long-term growth.
What makes an EHR suitable for clinic networks?
Selecting a platform for a distributed network requires a shift from local management to a global enterprise strategy.
The right system acts as a digital backbone that supports expansion while maintaining consistent care standards.
1. Scalability across multiple locations
A truly scalable EHR must handle the addition of new clinics without requiring a complete infrastructure overhaul. Cloud-native systems allow you to deploy standardized configurations to new sites in hours rather than weeks.
This elasticity ensures that as your patient volume grows, your software performance remains stable and responsive.
2. Interoperability with external systems
Modern healthcare enterprises thrive on their ability to exchange data with labs, imaging centers, and pharmacies. Therefore, your EHR must support HL7 and FHIR standards to ensure seamless communication across the medical ecosystem.
This connectivity reduces manual data entry and ensures that external diagnostic results are instantly available to your clinicians.
3. Custom workflows for different clinics
While standardization is important, individual clinics often have unique operational needs based on their specialty or local patient demographics. A flexible EHR allows for modular workflow adjustments without breaking the core system architecture.
This balance enables specialized departments to optimize their daily tasks while still feeding data into the central enterprise database.
4. Compliance and data security requirements
Managing a multi-clinic network multiplies the surface area for potential data breaches and regulatory slip-ups. Enterprise-grade systems provide centralized security controls, including multi-factor authentication and detailed audit logs to track every data interaction.
Maintaining HIPAA or GDPR compliance across all locations becomes a manageable, automated process rather than a manual nightmare.
Evaluating these core pillars ensures your technology investment supports long-term operational excellence. Prioritizing these features transforms your EHR from a simple record-keeping tool into a strategic growth engine.
What are the best EHRs for multi-clinic systems?
Navigating the EHR marketplace requires looking past feature lists to find architectural alignment with your business goals.
The “best” platform is the one that minimizes technical debt while maximizing clinical throughput across your entire network.
No Single Best EHR For All Clinics
In the enterprise healthcare space, a “one-size-fits-all” mentality often leads to expensive implementation failures. Your choice must be dictated by your specific clinical volume, specialty mix, and long-term exit or expansion strategy.
A platform that excels in a high-volume urgent care environment may lack the deep longitudinal tracking required for oncology or chronic disease management.
- Specialty-Specific vs. Generalist: Generalist systems offer broad utility but often require heavy customization to fit niche workflows. Conversely, specialty-native platforms provide immediate “out-of-the-box” efficiency for specific disciplines like dermatology or orthopedics.
- The Integration Trade-off: Choosing a massive, closed-loop ecosystem provides stability but may limit your ability to adopt cutting-edge third-party AI tools. Open, API-first platforms offer better long-term flexibility but require more internal technical oversight.
- User Adoption and Retention: If the interface is too complex, your clinicians will resist the transition. This friction hurts productivity and increases the risk of documentation errors that lead to billing denials.
Ultimately, the goal is to find a system that feels invisible to the clinician while providing robust data to the C-suite. Successful leaders prioritize platforms that offer a balance of rigid compliance and modular adaptability.
Best EHRs by clinic size and scale
The technological needs of a five-location boutique group differ wildly from a 50-location regional health system. Scaling clinical operations is as much about managing human workflows as it is about managing database capacity.
1. Small to Mid-Sized Growth Networks (5-15 Locations)
For rapidly expanding groups, platforms like Tebra (formerly Kareo) or DrChrono are often the logical starting point. These systems prioritize a lower total cost of ownership and fast deployment cycles.
They offer mobile-first interfaces that appeal to modern clinicians and integrated billing modules that simplify revenue cycle management for lean administrative teams.
These platforms allow smaller enterprises to punch above their weight class by automating patient intake and scheduling.
2. Mid-Market and Large Ambulatory Enterprises (20-50+ Locations)
As the organization matures, the need for advanced reporting and cross-site resource optimization becomes paramount. athenahealth stands out here due to its network-enabled model, which leverages data across its entire user base to proactively catch billing errors.
Similarly, NextGen Healthcare provides the deep clinical customization necessary for multi-specialty groups that need to standardize care without sacrificing specialty nuances. These systems are built to handle the complexities of diverse payer contracts and high-volume data processing.
3. Tier-1 Hospital-Affiliated Systems
For enterprises operating at a massive scale or those closely tied to academic centers, Epic and Oracle Health (Cerner) remain the dominant forces. These are complete operating systems for healthcare.
While they require significant capital investment and longer implementation timelines, they offer unparalleled ecosystem depth.
They provide a level of interoperability that is essential for complex, integrated delivery networks where patient data must flow between outpatient clinics and inpatient hospital wards seamlessly.
Leading Cloud EHR Platforms Overview
The modern EHR market is about which platform offers the most intelligent automation. For an enterprise, the choice often comes down to the balance between specialized clinical depth and broad operational scale.
Leading Cloud EHR Platforms Comparison
| Platform | Best For | Core Strength | Key Capabilities | Limitations at Scale | Bottom Line |
| athenahealth | Mid-to-large ambulatory groups | Automated billing + network intelligence | Claim scrubbing, revenue cycle automation, and AthenaNet integrations | Limited deep customization for complex workflows | Strong for reducing admin workload through automation |
| eClinicalWorks | Large multi-specialty clinic networks | All-in-one patient engagement ecosystem | Healow portal, telehealth, AI (Sunoh.ai), end-to-end workflows | Can become complex and rigid at scale | Comprehensive platform covering the full patient journey |
| ModMed | Specialty clinics and surgical centers | Specialty-specific clinical workflows | Pre-built templates, touch-based UI, fast charting | Not ideal for diverse multi-clinic networks | Optimized for speed and efficiency in specialized care |
| NextGen Healthcare | Growing enterprise clinic systems | Advanced analytics + configurability | Population health, reporting, customizable workflows | Requires effort to configure for scale | Best for data-driven, value-based care organizations |
1. athenahealth: The Network-Enabled Leader
As a cloud-native pioneer, athenahealth operates on a single instance of software for its entire user base. This architecture allows the platform to act as a “collective brain,” where a billing rule update for one clinic instantly benefits every other site on the network.
- Best For: Mid-to-large ambulatory groups focused on high-performance revenue cycles.
- Core Strength: Automated claim scrubbing and a massive “AthenaNet” ecosystem of third-party integrations.
- The Bottom Line: It minimizes administrative overhead by handling much of the back-office heavy lifting as a service.
2. eClinicalWorks: The Market Giant
With one of the largest installed bases in the US, eClinicalWorks (eCW) provides an incredibly feature-rich environment. It has leaned heavily into AI with “Sunoh.ai,” an ambient listening tool that converts natural patient-provider conversations into structured clinical notes.
- Best For: Large multi-specialty groups that require deep, built-in patient engagement tools.
- Core Strength: The “Healow” patient portal and extensive telehealth capabilities are integrated directly into the workflow.
- The Bottom Line: It offers a comprehensive, all-in-one suite that covers every touchpoint of the patient journey.
3. ModMed: The Specialty Powerhouse
Modernizing Medicine (ModMed) disrupts the generalist model by building its EHR specifically for high-margin specialties like dermatology, orthopedics, and gastroenterology. Their touch-based interface is designed to mirror a specialist’s clinical logic rather than a generic data entry form.
- Best For: Specialized surgical centers or boutique multi-clinic networks where speed of charting is a priority.
- Core Strength: Pre-built, specialty-specific templates that eliminate the need for manual customization.
- The Bottom Line: By reducing the “clicks per visit,” ModMed significantly lowers physician burnout and increases daily patient throughput.
4. NextGen Healthcare: The Enterprise Architect
NextGen is a veteran in the space that has successfully transitioned its deep enterprise functionality to the cloud. It offers a robust population health management module, making it a favorite for organizations moving toward value-based care contracts.
- Best For: Growing clinical enterprises that need a balance of outpatient flexibility and hospital-grade reporting.
- Core Strength: Advanced analytics and a highly configurable interface that can be tailored to complex departmental needs.
- The Bottom Line: It provides the data-rich environment necessary for C-suite leaders to make long-term strategic pivots.
Selecting the right platform requires matching these technical “superpowers” to your specific business model. Whether you prioritize athena’s billing automation or ModMed’s clinical speed, your choice will define your enterprise’s scalability for the next decade.
How do top cloud EHRs compare today?
Comparing top EHRs in 2026 reveals that Athenahealth leads in RCM automation, while Epic dominates in deep clinical integration. Enterprises should prioritize FHIR-native platforms to ensure a 30% reduction in long-term technical debt and seamless multi-site data scaling.
Comparing enterprise-grade EHRs requires looking beyond basic charting to see how each architecture handles high-volume data and multi-site revenue cycles. The right choice depends on whether your strategy prioritizes deep clinical customization or standardized administrative automation.
1. Epic vs Athenahealth vs eClinicalWorks
These three giants represent different philosophies in healthcare IT. Epic offers a “complete ecosystem” but often requires heavy local infrastructure or certified hosting.
Athenahealth is a true cloud-native platform that functions as a business service. eClinicalWorks provides a middle ground with vast features and a massive global footprint.
| Feature | Epic (Community Connect) | Athenahealth | eClinicalWorks |
| Model | Enterprise / Hybrid | Cloud-Native (SaaS) | Cloud / On-Premise |
| Best For | Large Hospital-Affiliated Groups | Mid-to-Large Ambulatory | Multi-Specialty Clinics |
| Data Philosophy | Centralized Ecosystem | Network-Enabled Data | Feature-Rich Integration |
Epic excels in complex, high-acuity environments where patient longitudinal records are critical.
Athenahealth focuses on reducing “busy work” by managing billing rules at the network level. eClinicalWorks offers extensive patient engagement tools that are built directly into the core software.
2. NextGen vs Kareo vs AdvancedMD
This segment focuses on agility and specialized ambulatory workflows. NextGen is built for sophisticated multi-specialty enterprises that need deep reporting.
Kareo (now part of Tebra) and AdvancedMD target the “growth” phase, offering streamlined interfaces that prioritize ease of use and rapid deployment.
| Feature | NextGen Healthcare | Kareo (Tebra) | AdvancedMD |
| Market Focus | Mid-Market Enterprise | Small to Mid-Growth | Boutique & Mid-Size |
| Customization | High (Modular) | Moderate (Standardized) | High (Workflow-centric) |
| Implementation | 3–6 Months | 1–2 Months | 2–3 Months |
NextGen provides the analytical depth required for value-based care contracts. Kareo is often the preferred choice for lean operations looking to scale without heavy IT overhead.
AdvancedMD offers a highly flexible “workflow dashboard” that can be tailored to very specific front-office needs.
3. Feature and workflow comparison
Enterprise leaders must evaluate how a platform handles the “day in the life” of a clinician versus an administrator.
A platform might have great billing but a clunky clinical interface. Therefore, the balance between documentation speed and data accuracy is the primary metric for workflow success.
| Workflow Area | Top Performer | Key Advantage |
| Documentation | ModMed / eCW | Ambient AI and specialty-specific templates. |
| Patient Intake | AdvancedMD | Fully digital, self-service patient journeys. |
| Revenue Cycle | Athenahealth | Integrated “Billing as a Service” model. |
Documentation speed directly impacts patient volume. Systems that utilize AI to draft notes allow doctors to focus on the patient rather than the screen. Similarly, automated intake reduces front-desk friction, which is a common bottleneck in multi-clinic systems.
4. Integration capabilities across platforms
Interoperability is no longer optional for multi-site systems. Your EHR must talk to external labs, state registries, and imaging centers seamlessly.
Platforms that use FHIR-native APIs allow you to plug in third-party AI tools or custom analytics dashboards without breaking the core system.
| Integration Type | Capability Level | Standard Used |
| Lab/Imaging | High (Bidirectional) | HL7 / FHIR |
| Patient Portals | High (Mobile-First) | API-Driven |
| External AI Tools | Variable | RESTful APIs |
Athenahealth and Epic lead in “data liquidity,” meaning they share information easily across different provider networks. However, smaller platforms are catching up by adopting open API standards. This allows even mid-sized clinics to participate in large-scale health information exchanges.
5. Multi-clinic scalability differences
Scaling to 50 locations is different than managing five. The core challenge is maintaining a “global” standard while allowing for “local” clinic nuances.
Some EHRs struggle with latency or data synchronization as the database grows, while others are built for unlimited horizontal scaling.
| Scalability Factor | Cloud-Native (Athena/eCW) | Hybrid/Hosted (Epic/NextGen) |
| New Site Launch | Days (Config-based) | Weeks (Instance-based) |
| Global Reporting | Real-time Centralized | Often requires Data Warehouse |
| System Updates | Instant / Universal | Scheduled / Manual |
Cloud-native systems generally offer a faster “time-to-value” for new locations. Because the infrastructure is shared, you don’t need to buy new servers for every branch. Conversely, enterprise systems like Epic provide deeper control over local site configurations at the cost of speed.
6. Pricing models and cost comparison
Understanding the “Total Cost of Ownership” (TCO) is vital for CFOs. Some platforms charge a flat monthly fee per provider, while others take a percentage of collections.
A “cheap” monthly fee can become expensive if the platform lacks automation, leading to higher staffing costs.
| Pricing Model | Average Cost Structure | Best For |
| Per Provider/Month | $300 – $700 | Predictable Budgeting |
| % of Collections | 4% – 8% | Performance-Based Growth |
| Enterprise Licensing | Custom Quote | Large, Stable Systems |
Percentage-based models (like Athenahealth) align the vendor’s success with your own. If you don’t get paid, they don’t get paid. Subscription models are easier for fixed-budget planning, but often hide “add-on” fees for things like patient reminders or lab integrations.
Evaluating these comparisons ensures your technology stack aligns with your operational reality. Choosing based on architectural fit rather than just brand name protects your investment and ensures clinical longevity.
Where do existing EHR systems fall short?
While legacy EHRs provided the first step toward digitization, many now act as a bottleneck for modern enterprise growth. Decision-makers often find that these systems lack the agility required to compete in a data-driven healthcare market.
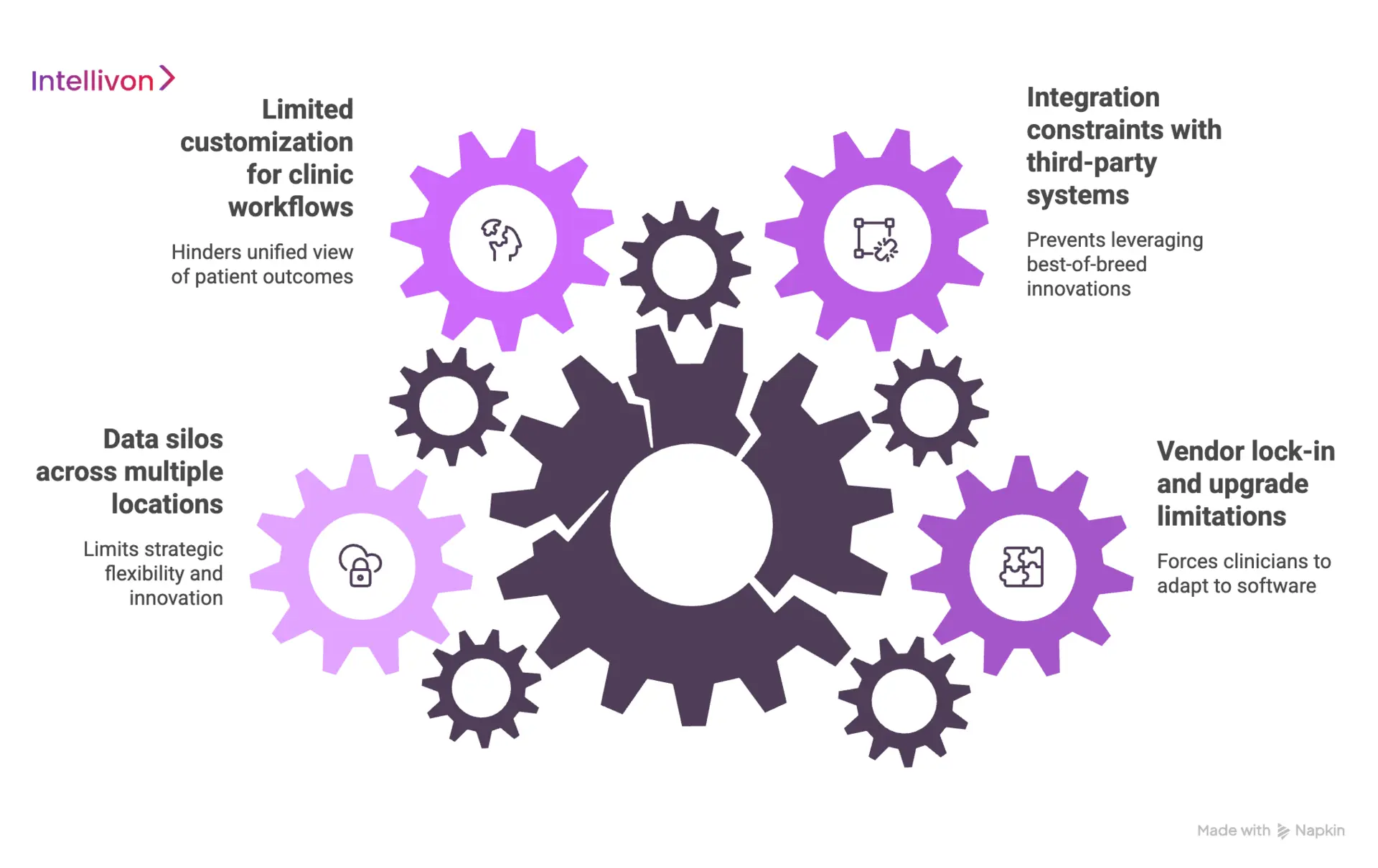
1. Limited customization for clinic workflows
Most established EHRs utilize a “one-size-fits-all” architecture that forces clinicians to adapt their practice to the software. This rigidity results in “death by a thousand clicks,” significantly contributing to physician burnout and reduced patient face-time.
Therefore, without the ability to tailor interfaces to specific specialties or site-specific needs, your operational efficiency hits a hard ceiling.
2. Integration constraints with third-party systems
Legacy platforms were often built as closed loops, making it difficult and expensive to connect with modern health-tech tools. Whether you are trying to plug in a new AI-driven diagnostic tool or a specialized billing service, “walled garden” APIs create massive technical hurdles.
These constraints prevent your enterprise from leveraging the best-of-breed innovations that drive competitive advantages.
3. Data silos across multiple locations
In many multi-clinic systems, data remains “trapped” within individual site instances or departmental modules. This fragmentation prevents leadership from seeing a unified view of patient outcomes and financial health across the entire network.
Consequently, clinicians are often forced to manually reconcile records, which increases the risk of medical errors and administrative redundancy.
4. Vendor lock-in and upgrade limitations
Heavy reliance on a single vendor’s proprietary ecosystem creates a “hostage” situation where switching costs become prohibitively high. Upgrades are often slow, expensive, and disruptive, lagging behind the rapid pace of regulatory changes and technological shifts.
This lack of portability means your data is essentially owned by the vendor, limiting your strategic flexibility to pivot as the market evolves.
Understanding these shortcomings is essential for any leader looking to future-proof their clinical infrastructure. Recognizing where traditional systems fail allows you to identify the strategic gaps that a modern, AI-integrated solution must fill.
When should clinics consider a custom EHR?
Transitioning from a standard subscription to a custom-built architecture is a strategic pivot for high-growth healthcare enterprises. This move shifts your technology from a monthly overhead cost to a proprietary business asset.
1. When off-the-shelf systems stop scaling
Generic platforms often hit a performance ceiling when managing dozens of locations and hundreds of concurrent users. You may notice increasing latency, frequent sync errors, or ballooning per-provider licensing fees that erode your margins.
A custom solution eliminates these “growth taxes” by providing a high-performance infrastructure designed specifically for your projected volume.
2. When integrations become complex
If your team spends more time managing “middleware” than patient care, your current system is failing you. Off-the-shelf EHRs frequently struggle to maintain stable, bidirectional data flows with proprietary lab tools or specialized AI diagnostics.
Custom builds utilize FHIR-native APIs from the ground up, ensuring every part of your technical ecosystem communicates without friction.
3. When workflows differ across clinics
Multi-specialty networks often face the “clutter problem,” where a dermatologist is forced to navigate an interface designed for a general practitioner. Forcing diverse clinics into a single rigid template creates massive operational drag and clinician frustration.
Customization allows you to build modular “skins” for different departments, ensuring every clinician sees exactly what they need, and nothing else.
4. When data control becomes critical
For enterprises looking toward an exit or a major merger, owning your data is a non-negotiable requirement. Relying on a third-party vendor often means your patient insights are locked in a proprietary format that is difficult to migrate or analyze.
Custom EHRs provide absolute data sovereignty, allowing you to run advanced internal analytics and protect your most valuable intellectual property.
Recognizing these triggers early prevents your technology from becoming a liability during a critical expansion phase. Moving toward a bespoke system ensures your digital foundation is as unique and scalable as your business model.
How are modern cloud EHR platforms built?
Modern EHR engineering has moved away from monolithic codebases toward agile, distributed systems. This architectural shift allows for rapid updates and massive scalability without risking system-wide downtime.
1. Cloud-native microservices architecture
Modern platforms use a microservices approach for core functions. For instance, scheduling, billing, and charting run as independent services. This means an update to one module cannot crash the others.
Therefore, your enterprise benefits from the uptime during clinical hours. Consequently, the system evolves in real-time without requiring massive overnight version upgrades.
2. Centralized data with distributed access
A multi-clinic system requires a single source of clinical truth. However, this data must remain accessible from any authorized device globally. Modern builds use global cloud clusters to synchronize patient records instantly.
By centralizing the database, you eliminate data conflicts across different branches. Furthermore, this structure ensures clinical consistency for every patient at every location.
3. API-first design for integrations
In a connected healthcare world, the EHR acts as a hub. Modern platforms are built with an API-first mindset from the first day. They typically utilize FHIR standards to ensure seamless data exchange.
This allows your team to plug in third-party AI diagnostics with minimal effort. In addition, this openness protects your organization from future technical obsolescence.
4. Real-time analytics and reporting systems
Decision-making in a multi-site enterprise cannot wait for manual audits. Modern architectures integrate stream-processing engines to analyze data as it enters. This provides the C-suite with live dashboards for patient throughput.
Therefore, leadership can track revenue cycle health and resource allocation in real-time. This turns raw clinical data into actionable business intelligence immediately.
Understanding these technical foundations is key to evaluating a platform’s long-term viability. A robust architecture ensures that your technology remains a strategic asset for your clinic network.
What role does AI play in modern EHR?
AI is no longer a futuristic concept for healthcare enterprises. Today, it acts as a force multiplier that enhances clinical accuracy and operational speed across your entire network.
Therefore, integrating AI into your cloud EHR is a strategic necessity to maintain a competitive edge.
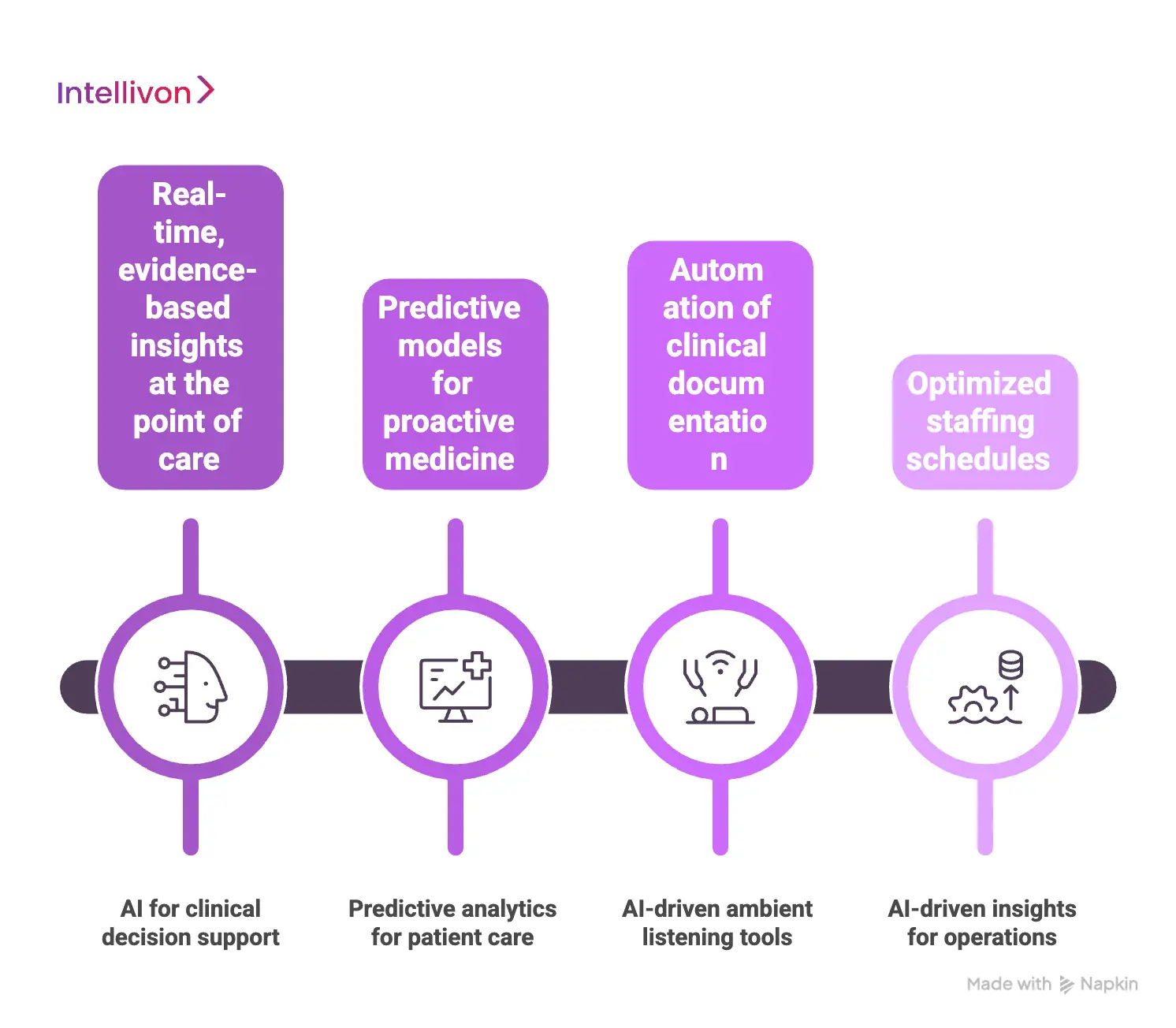
1. AI for clinical decision support
AI provides clinicians with real-time, evidence-based insights at the point of care. These systems analyze vast patient datasets to flag potential drug interactions or diagnostic gaps.
Consequently, your medical staff can make more informed decisions across multiple locations. In addition, this standardized intelligence ensures a high baseline of care quality throughout your enterprise.
2. Predictive analytics for patient care
Predictive models allow your organization to shift from reactive to proactive medicine. By analyzing historical data, the EHR can identify patients at high risk for chronic conditions or hospital readmissions.
This capability is particularly vital for multi-clinic systems managing diverse patient populations. Furthermore, these insights enable targeted interventions that improve long-term outcomes and reduce the total cost of care.
3. Automation of administrative workflows
Administrative friction is a primary driver of operational costs in large-scale healthcare. AI-driven ambient listening tools now automate clinical documentation by transcribing patient-provider conversations.
Therefore, your staff spends less time on manual data entry and more time on high-value patient interactions. This automation also reduces human error in coding and billing, ensuring faster revenue cycles.
4. AI-driven insights for operations
Managing a distributed network requires deep visibility into resource allocation and patient flow. AI algorithms can predict peak hours for specific clinics, allowing for optimized staffing schedules.
Consequently, leadership can minimize labor waste while maximizing patient throughput. These strategic insights turn raw operational data into a roadmap for sustainable enterprise growth.
The integration of AI transforms the EHR from a passive database into an active clinical partner. Investing in these intelligent capabilities ensures your network remains agile, accurate, and scalable for the next decade.
What integrations must clinic EHR support?
In a distributed healthcare network, your EHR cannot exist in isolation. It must serve as a central data exchange that communicates with every external partner in your ecosystem.
Therefore, prioritizing high-liquidity integrations is a technical mandate for any scalable clinical enterprise.
1. HL7 and FHIR interoperability
Interoperability standards like HL7 and FHIR are the universal languages of modern healthcare. These protocols allow patient data to move securely between disparate systems without manual intervention.
Consequently, your clinicians can access external records in real-time within their existing workflow. This connectivity is essential for maintaining a high standard of care across multiple clinic locations.
2. Labs, pharmacies, imaging systems
Bidirectional integration with diagnostic partners eliminates the need for manual faxes or phone calls. When a lab result is ready, it should automatically populate the patient’s chart and trigger a notification.
Furthermore, electronic prescribing reduces errors and improves patient medication adherence. This automation speeds up the treatment cycle and increases daily patient throughput for the entire organization.
3. Insurance and billing platforms
Revenue cycle management relies on seamless communication with insurance clearinghouses and payers. An integrated EHR can perform real-time eligibility checks before the patient even enters the exam room.
Therefore, your administrative team can resolve potential claim denials before they occur. This structural efficiency ensures a predictable cash flow and reduces the overhead costs of manual billing corrections.
4. Remote monitoring and wearables
The rise of telehealth and home-based care requires an EHR that can ingest data from external devices. Modern platforms must support integrations with glucose monitors, heart rate trackers, and other wearable technology.
Consequently, your providers can monitor high-risk patients between office visits. This proactive data stream allows for early interventions and supports your transition toward value-based care models.
Building a connected technical foundation is the only way to future-proof your healthcare investment. These integrations transform your EHR into a dynamic hub that drives clinical excellence and financial sustainability.
How Intellivon Builds Cloud-Based EHR Platforms?
Building an enterprise-grade EHR requires a departure from rigid, legacy software development. At Intellivon, we prioritize a high-performance, modular architecture that transforms your clinical data into a scalable business asset.
Therefore, our engineering process ensures your platform is secure, compliant, and ready for rapid multi-site expansion.
Step 1: Strategic Discovery and Workflow Mapping
We begin by analyzing the specific operational friction within your multi-clinic network. Our team maps every touchpoint, from patient intake to final billing. Consequently, we identify exactly where manual bottlenecks occur.
This foundational step ensures the final platform aligns perfectly with your unique clinical goals.
Step 2: FHIR-Native Architectural Design
We build every platform using an API-first philosophy. By utilizing FHIR and HL7 standards from day one, we guarantee total data liquidity.
Therefore, your EHR can communicate seamlessly with any lab, pharmacy, or specialist. This open architecture prevents future vendor lock-in and protects your long-term technology investment.
Step 3: Cloud-Native Microservices Development
Our engineers deploy a distributed microservices model rather than a monolithic codebase. This means clinical documentation, scheduling, and billing operate as independent units.
Consequently, the system remains stable even during high-traffic periods. Furthermore, this modularity allows us to update specific features without taking your entire network offline.
Step 4: AI Integration and Ambient Automation
We embed advanced AI models directly into the clinical workflow. These tools automate medical charting by transcribing natural patient-provider conversations.
Therefore, your clinicians spend significantly less time on administrative data entry. In addition, our predictive models flag potential health risks and diagnostic gaps in real-time.
Step 5: Multi-Tenant Security and Compliance
Security is the bedrock of our development process. We implement end-to-end encryption and multi-factor authentication across all clinic locations. Consequently, your enterprise remains fully compliant with HIPAA, GDPR, and other global standards.
Furthermore, our centralized audit logs provide absolute visibility into every data interaction for total peace of mind.
Step 6: Seamless Migration and Integration
We handle the complex task of migrating legacy data into your new cloud environment. Our team ensures that historical records are mapped accurately to maintain clinical continuity.
Therefore, your transition to a modern platform happens without data loss or operational downtime. We also verify every bidirectional integration with your existing lab and pharmacy partners.
Step 7: Continuous Optimization and Scaling
Deployment is only the beginning of our strategic partnership. We provide real-time analytics dashboards that track patient throughput and revenue cycle health.
Consequently, leadership can make data-driven decisions to optimize resource allocation across all sites. As your network grows, our infrastructure scales horizontally to support unlimited new locations.
Our proven methodology turns complex technical challenges into a streamlined, high-growth engine. By choosing Intellivon, you gain a strategic partner dedicated to building the future of your healthcare enterprise.
Conclusion
Choosing the best cloud-based EHR for multi-clinic systems depends on scale, integrations, and long-term growth needs. While leading platforms offer strong capabilities, they often fall short in customization and flexibility. As clinic networks expand, the focus shifts from features to architecture.
Building a scalable, API-first EHR ensures seamless operations, real-time data flow, and future-ready infrastructure, positioning healthcare organizations to grow without system limitations.
Build a Cloud-Based EHR for Clinics with Intellivon
At Intellivon, cloud-based EHR platforms are engineered as enterprise healthcare infrastructure, not software layered onto disconnected systems. The goal is to create a unified platform that connects patient data, clinical workflows, and operational systems across every clinic location.
Each solution is designed to support multi-clinic scalability from day one. This includes centralized patient records, real-time data synchronization, cross-location scheduling, billing integration, and advanced reporting. As a result, healthcare organizations gain full visibility, reduce inefficiencies, and deliver consistent care across all sites.
Our approach focuses on AI-first, API-driven architectures combined with interoperability standards like HL7 and FHIR. This ensures seamless integration with labs, pharmacies, insurers, and existing healthcare systems without disrupting ongoing operations.
Why Intellivon for Cloud EHR Development?
- Built for Multi-Clinic Scale: Designed to handle distributed care networks with centralized control
- API-First Architecture: Enables seamless integrations and future system expansion
- Custom Workflow Design: Tailored to each clinic’s operational and clinical processes
- Compliance-Ready Systems: Aligned with healthcare regulations and data security standards
Ready to Build Your EHR Platform?
If your current system is limiting growth, it’s time to rethink your infrastructure. Intellivon helps you design and build a cloud-based EHR platform that scales with your clinics, integrates seamlessly, and supports long-term innovation.
Talk to Intellivon experts today to plan your EHR platform roadmap.
FAQs
Q1. What is a cloud-based EHR system?
A1. A cloud-based EHR system is a digital health platform hosted on remote servers and accessed via the internet. Unlike on-premise systems, it allows healthcare providers to store, manage, and access patient data from any location. As a result, clinics can ensure real-time data availability, improved collaboration, and easier system updates without managing physical infrastructure.
Q2. How does EHR work across clinics?
A2. An EHR system connects multiple clinic locations through a centralized database. This means patient records, appointments, billing data, and clinical notes are updated in real time and accessible across all sites. Consequently, providers can deliver consistent care, avoid duplicate records, and coordinate efficiently between clinics without delays.
Q3. How long does EHR development take?
A3. EHR development timelines depend on system complexity, integrations, and customization requirements. Typically, a basic MVP can take 3–4 months, while a fully scalable, multi-clinic EHR platform may take 6–12 months. However, timelines can extend further if advanced integrations, AI features, or compliance layers are required.
Q4. What integrations are required?
A4. A modern EHR system must integrate with multiple healthcare systems to function effectively. This includes labs, pharmacies, billing platforms, insurance providers, and imaging systems. In addition, interoperability standards like HL7 and FHIR are essential to ensure seamless data exchange across different healthcare environments.
Q5. How much does EHR cost?
A5. The cost of building a cloud-based EHR system depends on features, integrations, and scale. For multi-clinic systems, development typically ranges between $50,000 and $150,000. Additional costs may include cloud infrastructure, maintenance, and ongoing upgrades. Therefore, investing in a scalable architecture early helps reduce long-term operational costs.