The existing EHR platforms out there are just digital filing cabinets. They’re great at storing information, but cannot do much thinking. That difference matters because healthcare organizations sit on some of the richest data anywhere, but most of it’s locked away in clunky systems that can’t make sense of it, react, or share insights quickly enough to actually affect patient care when it counts. The tech to fix this is here. So, the real question is whether enterprises are choosing an EHR built to use that technology or just sticking with old habits.
Making an EHR “smart” with AI is a total rethink of the clinical backbone. With a truly AI-powered EHR, you don’t just document what happened. The system predicts what’s likely to happen next, flags risks before they get serious, cuts the paperwork headache for clinicians, and streamlines operations everywhere. The organizations that get this are building the platforms that’ll shape healthcare’s future. The ones treating AI like a dusty add-on are going to have to start over sooner than they think.
Intellivon has teamed up with healthcare companies to create large-scale AI-driven clinical systems that actually work. This blog dives into everything you need to build one, from its architecture to why every foundational choice matters down the road, and how we actually build these systems from the ground up.
Why Are Enterprises Moving to AI-Powered EHRs?
Healthcare providers are rapidly adopting AI-powered EHRs to reduce clinician burnout, improve efficiency, and deliver better patient outcomes.
At the same time, rising data volumes and the shift to value-based care are accelerating this transition. The AI-enhanced EHR market is growing rapidly. It is expected to increase from $9.54 billion in 2025 to $12.46 billion in 2026, at a CAGR of 30.7%.
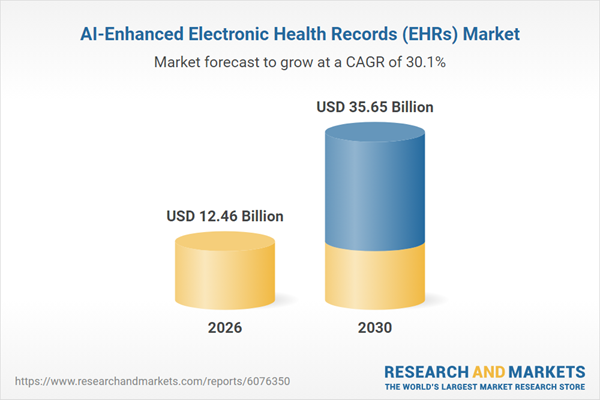
Traditional healthcare software often acts as a barrier between doctors and patients. Decision-makers are shifting toward AI-driven models to reclaim time and improve diagnostic accuracy. This transition represents a move from passive record-keeping to active clinical support.
1. Limits of Traditional EHR Systems Today
Most legacy systems function as static databases. They require manual data entry that leads to high burnout rates among clinical staff. Information is often trapped in silos, making it difficult to get a complete view of a patient’s history.
Consequently, these outdated platforms struggle to support the complex needs of modern, high-volume specialty clinics.
2. Shift Toward Data-Driven Clinical Decisions
Enterprises are moving away from reactive care. New systems analyze vast datasets to identify health trends before they become critical issues. By leveraging pattern recognition, providers can offer personalized treatment plans backed by concrete evidence.
Therefore, the EHR becomes a consultant rather than just a storage tool. This shift ensures that every medical decision is informed by the latest clinical research and historical patient performance.
3. Role of AI in Reducing Care Delays
Automation eliminates the bottlenecks found in traditional workflows. AI triages patient messages and flags urgent lab results for immediate review. In addition, intelligent scheduling tools predict cancellations and optimize room usage.
These efficiencies ensure that patients receive care faster, which directly impacts hospital throughput and overall revenue.
4. Demand for Intelligent Clinical Platforms
Market leaders now seek platforms that offer seamless interoperability. They want systems that “think” alongside the practitioner to prevent human error. Furthermore, investors recognize that scalable AI architecture is the only way to handle the growing influx of medical telemetry.
An intelligent platform is no longer a luxury but a fundamental requirement for competitive healthcare enterprises.
Smart EHR systems represent the future of profitable, high-impact healthcare. These platforms turn operational challenges into strategic advantages for growing medical enterprises.
What Defines a Smart EHR System with AI?
A smart EHR system is a clinical platform that uses artificial intelligence to move beyond passive data storage into active decision support. It reads patient data in real time, identifies patterns, flags risks, and automates routine workflows without waiting for manual input.
Therefore, instead of recording what happened, it helps clinical and operational teams respond to what is happening and anticipate what comes next.
The next evolution of healthcare software moves beyond static data storage. It focuses on turning raw information into actionable intelligence that drives both clinical excellence and business growth.
1. Real-Time Clinical Decision Support Systems
Clinical decision support tools act as a secondary safety net at the point of care. These systems analyze current patient data against established medical protocols in real time.
Therefore, providers receive immediate alerts regarding potential drug interactions or missed screenings. This technology significantly reduces medical errors while ensuring that all treatments align with the latest evidence-based guidelines. In addition, it helps standardize the quality of care across multiple clinic locations.
2. Predictive Analytics for Patient Outcomes
Predictive models allow leaders to anticipate patient needs before they become critical issues. By analyzing social determinants and historical health patterns, the software identifies individuals at high risk for readmission. Consequently, your team can intervene early with targeted wellness programs or follow-up calls.
This foresight not only improves patient longevity but also optimizes resource allocation within your facility. Better outcomes naturally lead to higher patient retention and a stronger reputation in the market.
3. Generative AI in Clinical Workflows
Generative AI is currently revolutionizing how clinicians handle documentation and administrative tasks. These tools can transcribe doctor-patient conversations and automatically draft highly accurate clinical notes.
This shift allows physicians to focus entirely on the patient rather than on a computer screen. Moreover, AI can summarize complex medical histories into concise briefs for specialists. Reducing the time spent on manual entry directly lowers burnout and increases the daily volume of patients you can treat.
Integrating intelligence into your digital foundation transforms your data into a strategic asset. This transition ensures your practice remains both clinically superior and operationally efficient.
What Is the Minimum AI Stack for Modern EHRs?
Building a competitive platform requires more than a simple database. Investors must look for a specific technical layer that allows the system to think and react. This “Minimum AI Stack” ensures the EHR remains relevant as medical technology evolves.
1. NLP for Clinical Data Structuring
Doctors spend hours typing notes that computers cannot easily read. Natural Language Processing solves this by converting “free text” into structured, searchable data. It extracts symptoms, medications, and dosages from physician narratives automatically.
Therefore, the system can cross-reference this data against pharmacy records or lab results without manual entry.
2. ML Models for Risk Prediction
Machine Learning models act as an early warning system. These algorithms scan patient histories to identify individuals at high risk for chronic conditions or readmission. By flagging these cases early, providers can intervene before a medical crisis occurs.
Consequently, this leads to better patient outcomes and significant cost savings for the healthcare facility.
3. Generative AI for Documentation
Documentation is often the largest drain on clinical productivity. Generative AI can now listen to patient-doctor conversations and draft accurate clinical summaries in real-time. This technology eliminates the need for after-hours “pajama time” spent on paperwork.
In addition, it ensures that every chart is comprehensive and ready for insurance billing immediately.
4. AI-Powered Clinical Decision Support
This layer provides real-time guidance during the point of care. It checks for drug-to-drug interactions and suggests evidence-based treatment paths based on the latest guidelines. Instead of replacing the doctor, it acts as a highly informed assistant.
This support reduces human error and ensures a high standard of care across the entire enterprise.
A robust AI stack is the backbone of any scalable medical platform. Investing in these core technologies ensures long-term operational viability and superior data integrity.
What AI Features Deliver the Most Clinical Impact?
For an enterprise to see a real return on investment, AI must solve specific operational pain points. Focusing on high-impact features ensures that the platform provides immediate value to both clinicians and administrators. These tools redefine the standard of care.
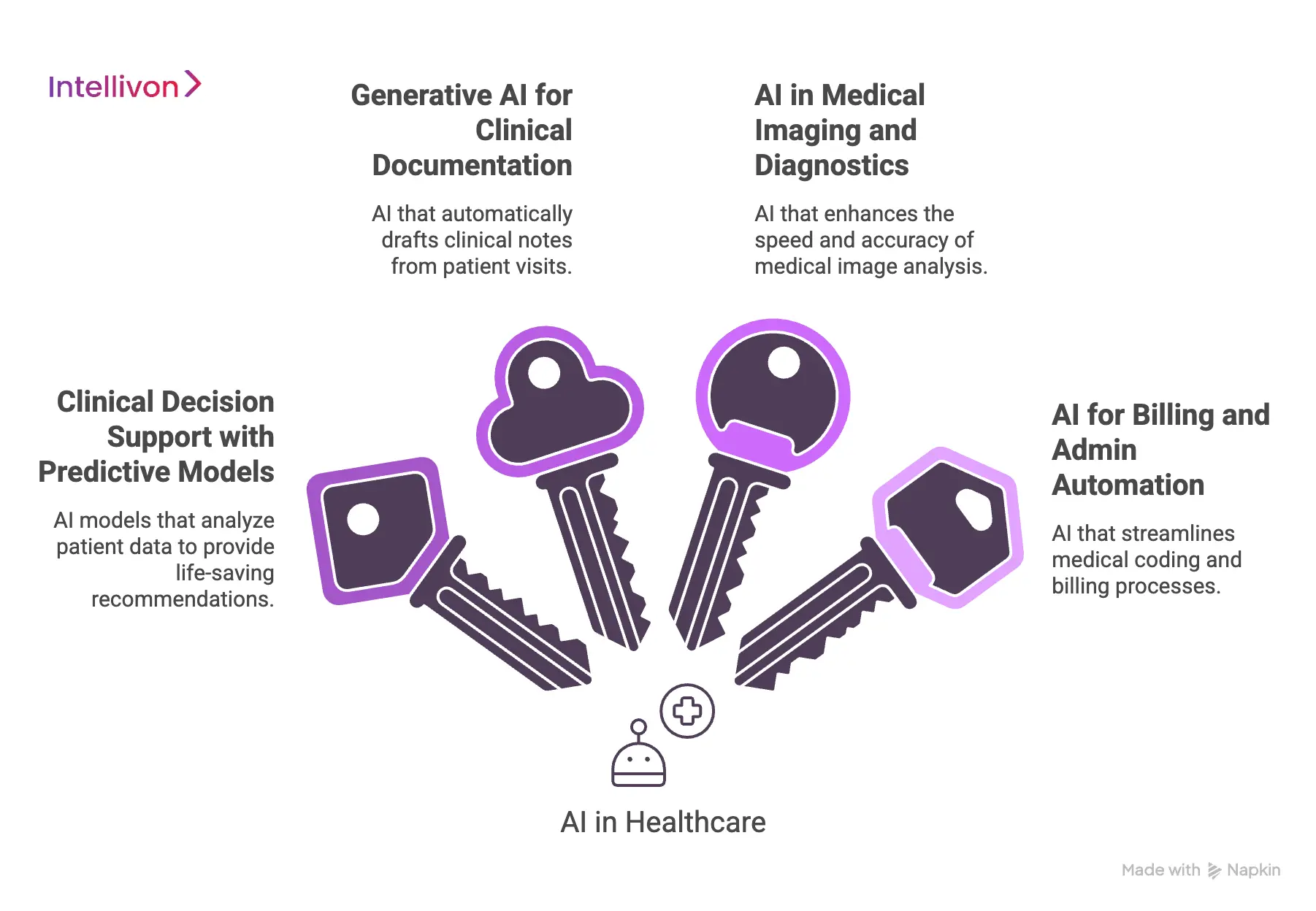
1. Clinical Decision Support with Predictive Models
Predictive models act as an invisible safety net during patient consultations. These systems analyze real-time vitals and historical data to alert doctors to silent risks, such as sepsis or sudden cardiac events.
For example, Penn Medicine developed a random-forest classifier that identifies septic shock 12 hours before clinical onset, significantly outperforming traditional bedside tools. Therefore, the system moves beyond simple alerts to provide life-saving, evidence-based recommendations at the point of care.
2. Generative AI for Clinical Documentation
Ambient sensing technology is revolutionizing the way doctors interact with patients. Using Generative AI, the system listens to a clinical visit and automatically drafts a structured note in the background.
A notable example is The Permanente Medical Group, which deployed ambient AI to over 10,000 physicians, resulting in a dramatic reduction in “pajama time” and improved patient engagement. Consequently, this feature directly combats clinician burnout while ensuring that medical records are more comprehensive and accurate than ever before.
3. AI in Medical Imaging and Diagnostics
Integrating AI directly into the imaging workflow allows for faster and more accurate screenings. Algorithms can now pre-scan X-rays, MRIs, and CT scans to flag abnormalities for immediate radiologist review.
At Mayo Clinic, AI models have been used to detect “silent” heart disease from standard EKG data that a human might miss. In addition, this triaging ensures that the most critical cases are prioritized in the queue, saving vital minutes in emergency situations.
4. AI for Billing and Admin Automation
Administrative overhead often consumes a massive portion of a healthcare facility’s revenue. AI-driven billing tools automate the complex process of medical coding by extracting relevant data from clinical notes.
For instance, many large health systems now use AI to identify “under-coding” or potential claim denials before they are even submitted to the payer. This automation streamlines the revenue cycle, ensuring that the enterprise is paid accurately and quickly for the services provided.
Selecting features with high clinical impact is the fastest way to achieve platform adoption. These tools transform the EHR into a strategic asset that drives both patient health and business growth.
Where Is AI Already Used in Smart EHR Systems?
AI is no longer a theoretical concept in healthcare; it is currently operational in leading medical centers worldwide. Strategic investors should look at these proven applications as the baseline for any modern platform.
These real-world use cases demonstrate how software can actively participate in the care delivery process.
1. Early Disease Detection Using AI Models
Smart systems now scan millions of data points to find subtle indicators of illness. For instance, Mount Sinai’s “Deep Patient” tool uses deep learning to predict the onset of diverse diseases, including Type 2 diabetes and certain cancers, long before symptoms appear.
Therefore, doctors can begin preventative treatments that are less invasive and more cost-effective. This capability transforms the EHR from a history book into a predictive radar.
2. AI for Personalized Treatment Planning
Every patient reacts differently to medication based on their genetic makeup and lifestyle. Modern EHRs use AI to analyze these variables and suggest the most effective drug dosages.
At Memorial Sloan Kettering, oncology platforms assist doctors by matching a patient’s specific tumor profile with the most successful clinical trial results. Consequently, patients receive “precision medicine” that is tailored specifically to their biological needs.
3. Hospital Resource Optimization with AI
Efficiency in a hospital is often a matter of logistics. AI algorithms predict when a surge of patients will arrive at the emergency room, allowing managers to staff accordingly.
Johns Hopkins Hospital utilizes a sophisticated “command center” that uses predictive analytics to manage bed availability and reduce patient wait times. In addition, these tools help prevent bottlenecking in operating rooms, ensuring the facility runs at peak financial and clinical performance.
4. AI-Driven Remote Patient Monitoring
Healthcare now extends far beyond the four walls of a clinic. Smart EHRs integrate with wearable devices to monitor chronic conditions like hypertension or heart disease in real-time.
For example, the Cleveland Clinic uses remote monitoring to track heart failure patients, automatically alerting the care team if a patient’s weight or blood pressure fluctuates dangerously. This proactive approach prevents emergency readmissions and keeps the patient safely at home.
The practical application of AI is already delivering measurable improvements in patient safety and hospital revenue. These established successes provide a clear roadmap for any entrepreneur looking to enter the digital health space.
How Do AI-Powered EHR Systems Improve ROI?
Investing in smart EHR technology is a strategic move to stabilize margins in an era of rising labor costs. For enterprise leaders, the return on investment (ROI) is a measurable reality across clinical and financial silos.
A 2024 IDC study sponsored by Microsoft found that healthcare organizations realize an average ROI of 3.2x within just 13 to 14 months. For high-maturity leaders, that return can jump to as high as 10.3x.
1. Reducing Admin Costs with Automation
Administrative tasks consume a staggering amount of healthcare resources, often totaling 25% of all U.S. healthcare spending. AI targets this inefficiency by automating labor-intensive workflows like insurance claim processing and clinical documentation.
According to McKinsey, the U.S. healthcare system loses over $150 billion annually to appointment no-shows and administrative friction.
Furthermore, ambient AI tools have helped systems like Kaiser Permanente save nearly 16,000 hours of documentation time over a 15-month period. Therefore, facilities can reduce their reliance on manual data entry while simultaneously accelerating their revenue cycle.
2. Improving Outcomes with Predictive Care
Clinical outcomes directly impact the bottom line, especially in value-based care models. Predictive AI identifies high-risk patients before they require expensive emergency interventions.
At Penn Medicine, researchers used machine learning to detect sepsis 12 hours earlier than traditional methods, which can significantly lower ICU costs and mortality.
Consequently, better health outcomes lead to significant reductions in long-term operational expenditures. By preventing complications, enterprises avoid the high costs associated with extended hospital stays and readmissions.
3. Increasing Operational Efficiency
Efficiency is the ability to optimize hospital throughput without expanding physical infrastructure. AI-powered dashboards predict patient surges and optimize bed management in real-time.
For example, Tampa General Hospital utilized AI to boost appointment scheduling by 21% and decrease call abandonment rates by 56% within just two weeks of launch.
In addition, Mass General Brigham co-developed an algorithm that predicts “missed care opportunities” with up to 96% accuracy. These efficiencies ensure that existing resources generate maximum revenue while reducing staff burnout.
4. Minimizing Errors with AI Insights
Medical errors are a massive financial and legal liability for any healthcare enterprise. AI acts as a digital safety net, cross-referencing prescriptions and diagnoses against global medical databases to flag potential mistakes.
Research suggests that AI integration can reduce clinical errors by up to 86% in specific diagnostic settings. By catching these discrepancies early, organizations avoid the astronomical costs associated with malpractice and readmissions.
Furthermore, minimizing errors builds a culture of safety that enhances the institution’s brand and patient trust.
The financial case for AI-driven EHRs is built on the twin pillars of cost reduction and capacity expansion. These systems allow healthcare enterprises to scale their services while maintaining a lean, high-performance operational structure.
What Does an AI EHR System Architecture Look Like?
A scalable AI-powered EHR is a sophisticated, multi-layered ecosystem. For an enterprise, the goal is a modular “future-proof” system where AI models upgrade without rebuilding the platform.
This architectural separation ensures stability, security, and readiness for emerging medical technologies.
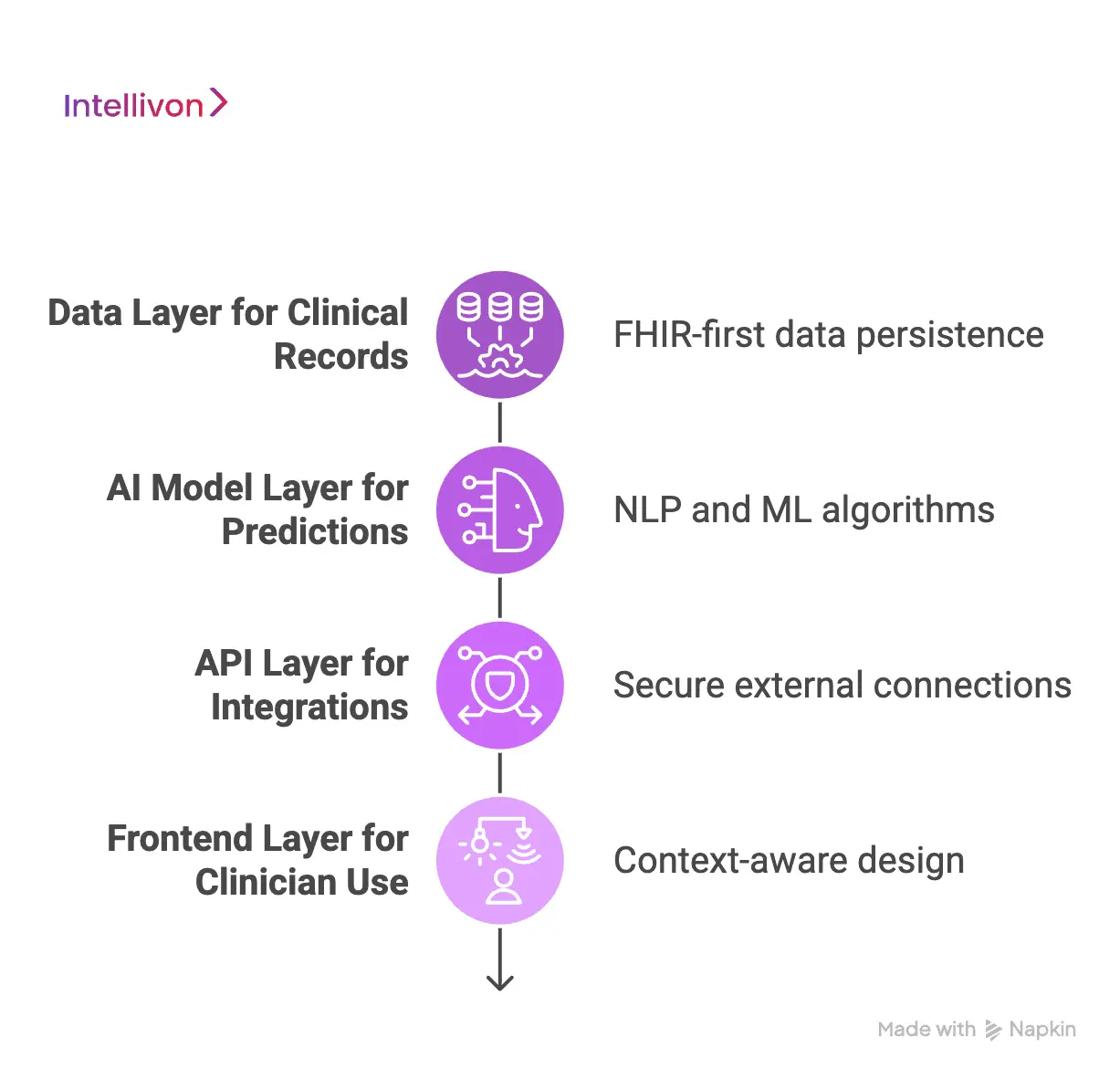
1. Data Layer for Clinical Records
The foundation is how the system organizes information. Modern architectures prioritize “FHIR-first” data persistence, using Fast Healthcare Interoperability Resources to make data machine-readable.
By using standardized resources for patients and medications, the AI performs consistent analysis across datasets. Therefore, the data layer acts as the “single source of truth,” ensuring predictions are grounded in real-time clinical context.
2. AI Model Layer for Predictions
This layer serves as the “brain,” housing algorithms that drive intelligence. It includes specialized modules like Natural Language Processing (NLP) for transcribing conversations and Machine Learning (ML) for risk stratification.
These models are isolated from core code, allowing developers to retrain them as medical research emerges. Consequently, the enterprise keeps its predictive tools at the cutting edge without risking system stability.
3. API Layer for Integrations
Healthcare requires constant communication between hospitals, labs, and payers. The API layer acts as a secure “gatekeeper” managing external connections via HL7 and RESTful protocols.
This simplifies pulling data from wearables or sending prescriptions to pharmacies. In addition, it enforces strict authentication, ensuring sensitive data is only shared with verified third-party systems.
4. Frontend Layer for Clinician Use
The frontend is where complex logic meets clinical practice. Rather than overwhelming doctors, a smart frontend uses “context-aware” design to surface relevant information. For example, it highlights worsening lab trends or suggests treatment pathways.
By focusing on intuitive dashboards and voice-enabled charting, this layer reduces cognitive load. This design-first approach is critical for high user adoption.
A modular architecture is the most important safeguard for your investment. It provides the flexibility to adapt to changing regulations and the scalability to support a growing healthcare network.
What Tech Stack Powers AI-Driven EHR Systems?
Selecting the right technology stack is the most critical decision for long-term scalability and security. Investors must ensure the underlying infrastructure can handle the massive computational demands of real-time AI.
A modern stack provides the high-performance environment necessary for continuous learning and instant clinical insights.
1. Cloud-Native Infrastructure for AI Workloads
Modern EHRs have moved away from on-premise servers toward flexible cloud environments like AWS HealthLake or Microsoft Cloud for Healthcare. These platforms offer “auto-scaling,” meaning they can handle thousands of simultaneous users without slowing down.
Therefore, the enterprise only pays for the computing power it uses, significantly reducing overhead costs. In addition, these providers offer built-in HIPAA compliance tools that simplify the regulatory burden for new platforms.
2. Machine Learning Frameworks in Healthcare
Developers use powerful frameworks such as PyTorch or TensorFlow to build and train the “brains” of the EHR. These tools allow engineers to create complex neural networks that recognize patterns in patient records.
For instance, Google’s Vertex AI is frequently used to manage the entire lifecycle of these models, from initial training to deployment. Consequently, this ensures that the AI remains accurate and can be updated easily as new medical data becomes available.
3. NLP Engines for Medical Data Processing
Generic NLP isn’t enough for the complex vocabulary of medicine. Specialized engines like Amazon Comprehend Medical or Google Healthcare Natural Language API are used to extract “medical entities” like dosages and symptoms from messy doctor notes.
These engines understand the nuances of clinical terminology and can link them to standardized codes like ICD-10. This automation turns unstructured narratives into valuable, searchable data for the entire clinical team.
4. Data Pipelines for Real-Time Processing
For AI to be useful at the bedside, it must process data instantly. Engineering teams use tools like Apache Kafka or AWS Kinesis to build real-time data pipelines.
These pipelines act as high-speed “conveyor belts” that move information from bedside monitors and lab results directly into the AI models. In addition, these systems ensure that critical alerts, such as a drop in oxygen levels, reach the physician’s mobile device in milliseconds.
5. Database Design for AI and Clinical Data
A smart EHR requires a hybrid database approach to manage both clinical records and AI insights. Developers often use PostgreSQL for structured patient data and “Vector Databases” like Pinecone or Milvus for AI-related tasks like similarity searches.
This design allows the system to quickly find “patients with similar symptoms” across millions of records. Furthermore, maintaining a FHIR-compliant database ensures that the platform can easily exchange data with any other hospital system globally.
A robust, cloud-first tech stack is the only way to ensure your platform can scale from a single clinic to a global health system. These choices determine your speed to market and your long-term operational costs.
What Integrations Are Required in Smart EHR Systems?
A smart EHR is only as powerful as the data it can access. For an enterprise, the value lies in a platform that communicates fluently with the entire healthcare ecosystem.
Seamless integration reduces manual data entry and ensures that the AI has a complete, real-time picture of every patient.
1. Integrating with HL7 and FHIR Standards
Standardization is the “language” of modern healthcare data. Using HL7 and FHIR (Fast Healthcare Interoperability Resources) ensures that your platform can exchange information with any other hospital system. These protocols allow for the secure transfer of patient demographics, clinical observations, and diagnostic reports.
Therefore, a “FHIR-native” architecture is a non-negotiable requirement for any scalable EHR. This standardization drastically reduces the time and cost associated with building custom connectors for every new facility.
2. Connecting Labs, Pharmacies, and Devices
An effective EHR must act as a central hub for all clinical orders. Automated integrations with national laboratory chains and e-prescription networks like Surescripts allow for instant data flow. When a lab result is ready, it should automatically populate the patient’s chart and trigger an AI alert if the values are critical.
In addition, connecting directly to pharmacy benefits managers ensures that doctors know a patient’s insurance coverage before they even write a script. Consequently, this connectivity speeds up treatment cycles and improves the patient experience.
3. Interoperability with Legacy Systems
Most large healthcare enterprises still rely on older, “legacy” software for billing or scheduling. A smart EHR must be able to “wrap” around these existing systems rather than forcing a total replacement. Using middleware or specialized APIs, developers can extract data from outdated databases and feed it into the AI engine.
This approach allows organizations to modernize their clinical workflows without disrupting their established financial operations. Furthermore, it protects your initial investment by ensuring the new platform can play well with the old.
4. Wearables and Remote Monitoring Integration
The future of care is moving from the clinic to the home. Integrating with consumer wearables and medical-grade remote monitoring devices provides a continuous stream of health data. Whether it is a continuous glucose monitor or a smart heart rate sensor, this data allows the AI to detect trends between doctor visits.
For example, Mayo Clinic has successfully integrated remote monitoring to reduce hospital readmissions for chronic heart failure by nearly 40%. This integration transforms the EHR into a proactive tool for long-term health management.
Robust integration is the secret to platform “stickiness” and long-term user adoption. By connecting the dots between disparate data sources, you create a platform that is indispensable to the modern healthcare provider.
How Do You Ensure Security and AI Compliance?
For high-net-worth investors, security is not just a feature; it is the ultimate risk mitigation strategy. A single data breach can cost a healthcare enterprise an average of $10.93 million, according to IBM’s 2024 Cost of a Data Breach Report.
Building a smart EHR requires a “security-first” architecture that anticipates both cyber threats and the unique regulatory challenges posed by artificial intelligence.
1. HIPAA and GDPR Compliance Requirements
Operating in healthcare requires absolute adherence to HIPAA in the U.S. and GDPR in Europe. These regulations dictate how Protected Health Information is stored and shared. Modern platforms use automated compliance mapping to monitor every data interaction.
This proactive stance protects the enterprise from massive fines and reputational damage. Consequently, the system acts as its own regulator by flagging potential violations before they occur.
2. Data Encryption and Access Controls
Data must be protected both at rest and in transit using industry-standard encryption. However, encryption is only part of a robust defense strategy. The platform must also enforce Role-Based Access Control to limit data exposure.
This ensures a billing clerk cannot see sensitive psychiatric notes while a surgeon has immediate access to vitals. In addition, you create an environment where every user and device must be continuously verified.
3. AI Model Monitoring and Explainability
AI in healthcare cannot function as a “black box” that offers no reasoning. Explainable AI ensures that when a model flags a patient, it also surfaces the specific data points used. For example, the system might highlight heart rate variability or recent lab shifts as the primary triggers.
Furthermore, engineers must monitor these models for “data drift” as medical trends shift over time. Regular audits ensure the system remains a reliable partner for clinicians and patients alike.
4. Audit Trails for AI Decision Transparency
Transparency is the key to building trust with doctors and legal regulators. A smart EHR maintains an immutable log of every action taken by the AI. If a doctor chooses to override a suggested treatment path, the system records that specific reasoning.
These audit trails are vital for forensic analysis during legal or insurance reviews. This level of documentation proves the AI is augmenting professional medical judgment rather than replacing it.
A secure platform is a resilient asset that grows in value as regulatory scrutiny increases. By prioritizing transparency and encryption, you build a foundation that clinicians can trust with sensitive information.
How Do You Ensure Accuracy in AI EHR Outputs?
Accuracy in AI EHRs is maintained through Human-in-the-Loop (HITL) validation, stress-testing against diverse clinical datasets, and continuous model retraining. These systems utilize specialized feedback loops where clinician overrides are analyzed to improve future predictive performance and reduce false positives.
1. Human-in-the-Loop Validation Workflows
No AI model should make a final clinical decision without human oversight. Human-in-the-Loop (HITL) workflows ensure that every AI-generated suggestion is reviewed and confirmed by a licensed professional. Therefore, the technology acts as a first-pass filter that flags potential issues for a doctor’s final approval.
This collaborative approach significantly reduces the risk of automated errors while keeping the clinician in full control of the treatment plan. Consequently, the enterprise benefits from the speed of AI without sacrificing the nuance of human judgment.
2. Model Testing with Real Clinical Scenarios
Before deployment, models must be stress-tested against thousands of historical, anonymized patient records. This testing phase simulates complex medical cases to see how the AI handles conflicting data points or rare conditions. For instance, developers often use “adversarial testing” to try to trick the system into making incorrect predictions.
In addition, these simulations ensure the software remains stable across different patient demographics and hospital settings. This rigorous validation phase is essential for building a platform that investors can confidently scale across multiple regions.
3. Continuous Learning and Model Updates
Medical knowledge evolves rapidly, and an AI model must keep pace with the latest clinical research. A smart EHR uses a continuous learning pipeline to update its algorithms as new data becomes available.
However, these updates are not applied blindly; they go through a “shadow deployment” phase where the new model is tested against the old one in a live environment.
Furthermore, this ensures that any “data drift” is identified and corrected before the update affects actual patient care. This persistent optimization cycle maintains the platform’s high accuracy over time.
4. Customization for Clinical Specialties
A generic AI model is often less effective than one tailored to a specific medical field. A customized EHR designed for oncology requires different logic than one built for pediatrics or orthopedics. Specialized modules allow the AI to understand the unique terminology and diagnostic patterns of each branch of medicine.
In addition, these custom layers ensure that the alerts and suggestions are highly relevant to the specific practitioner using the system. This level of specialization increases clinician adoption rates and ensures the platform delivers deep value within its niche.
Accuracy is the foundation of clinical trust and long-term financial viability. By investing in these verification and customization layers, you create a platform that consistently delivers high-quality outcomes in any medical environment.
How Does Intellivon Build AI-Powered EHR Systems?
Developing an enterprise-grade medical platform requires a blend of clinical insight and engineering precision. Intellivon utilizes a specialized, five-stage framework to transform fragmented healthcare data into a cohesive, intelligence-driven ecosystem.
This structured approach ensures every deployment is scalable, secure, and ready for high-stakes clinical environments. Therefore, investors can rely on a predictable development lifecycle that prioritizes speed to market without compromising safety.
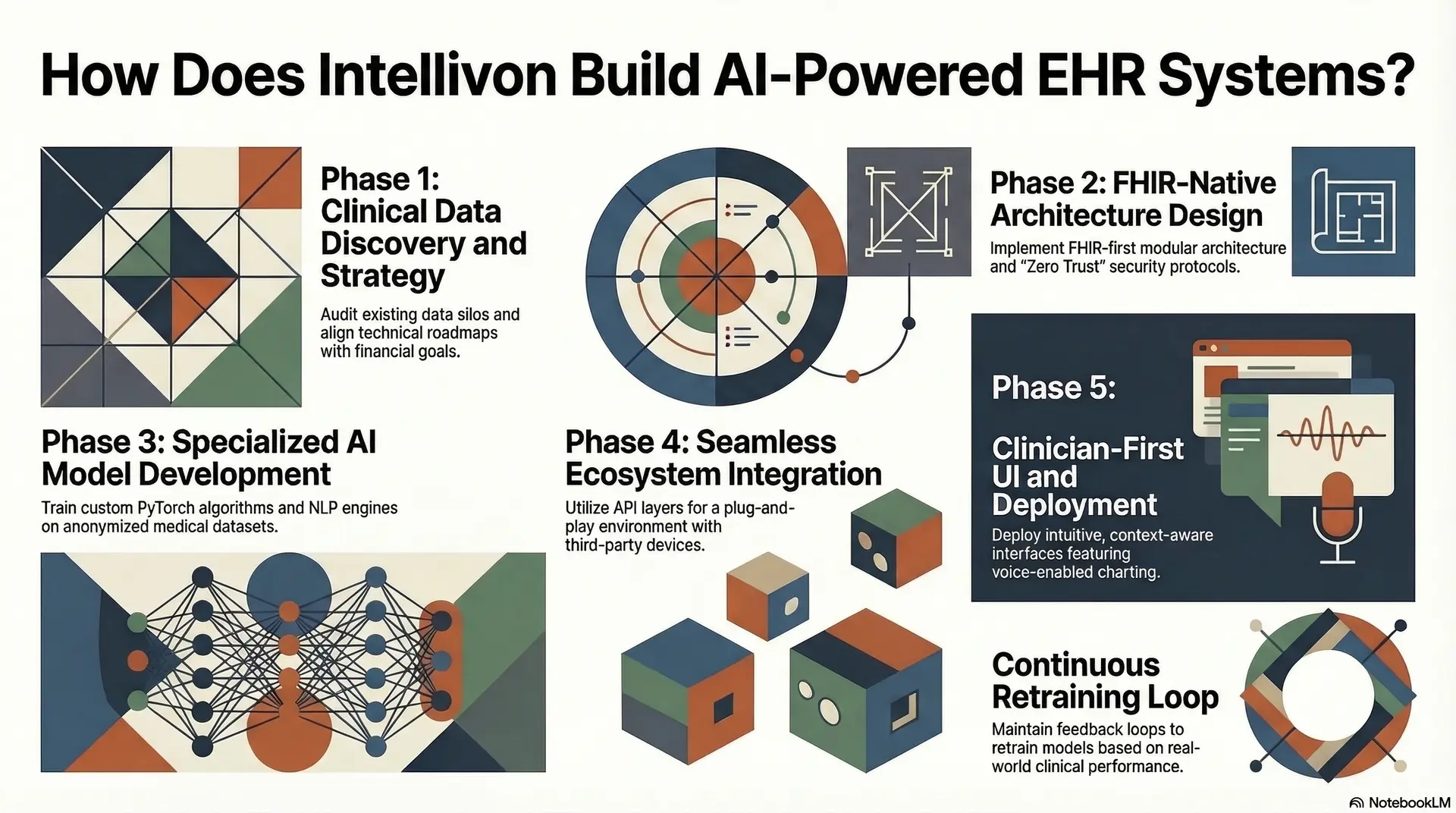
Phase 1: Clinical Data Discovery and Strategy
The process begins with a deep audit of existing data silos and clinical workflows.
This phase ensures the technical roadmap aligns perfectly with the financial goals of the enterprise. Consequently, the resulting platform solves real-world problems rather than offering generic features.
Phase 2: FHIR-Native Architecture Design
We build the foundation using a FHIR-first approach to ensure total data liquidity. Our engineers design a decoupled architecture where the data layer remains separate from the AI logic.
This modularity allows for independent scaling of storage and computing power as the user base grows. Furthermore, we implement “Zero Trust” security protocols at this stage to protect sensitive patient records. This architectural integrity is the primary safeguard for your long-term investment.
Phase 3: Specialized AI Model Development
Intellivon develops custom models tailored to specific clinical specialties rather than using off-the-shelf tools. Using frameworks like PyTorch, we train algorithms on high-quality, anonymized medical datasets to ensure high predictive accuracy.
We integrate Natural Language Processing engines specifically tuned for complex medical terminology. Therefore, the system can automate documentation and risk stratification with minimal human intervention. This phase turns raw information into a proactive clinical consultant.
Phase 4: Seamless Ecosystem Integration
A smart EHR must communicate with labs, pharmacies, and imaging centers instantly. We utilize robust API layers to create a “plug-and-play” environment for third-party medical devices and legacy software.
This connectivity ensures the AI has access to a 360-degree view of the patient at all times. In addition, we build real-time data pipelines that deliver critical alerts to clinicians in milliseconds.
Phase 5: Clinician-First UI and Deployment
The final stage focuses on the human element of healthcare technology. We design intuitive, context-aware interfaces that reduce the cognitive load on doctors and nurses. By incorporating voice-enabled charting and simplified dashboards, we ensure high adoption rates across the organization.
Following deployment, we maintain a continuous feedback loop to retrain AI models based on real-world performance.
This rigorous process allows Intellivon to deliver solutions that are not just technically advanced but also commercially viable. We provide the expertise needed to navigate the complexities of AI development while ensuring your platform is a growth enabler.
Conclusion
Building a smart EHR system is a strategic investment in the future of healthcare. These platforms transform clinical data into a powerful engine for both patient safety and operational growth. Therefore, selecting the right technical framework ensures your technology remains secure, scalable, and human-centric.
High-performance AI solutions help you lead the market by delivering measurable clinical results. Consequently, modernizing your digital infrastructure is the definitive step toward sustainable enterprise success.
Why Choose Intellivon To Build Smart EHR Systems?
At Intellivon, AI-powered EHR platforms are engineered as an enterprise clinical infrastructure, not as intelligent features layered onto disconnected healthcare systems. The objective is to build unified platforms that combine clinical data, AI-driven insights, and automated workflows to enable real-time, high-quality care delivery across complex healthcare environments.
Each solution is designed to support the full patient lifecycle. This includes AI-assisted documentation, predictive risk modeling, clinical decision support, care coordination, and automated administrative workflows. As a result, healthcare organizations gain real-time visibility, reduce clinician workload, and deliver faster, more accurate, and data-driven care.
Our approach focuses on AI-first, API-driven architectures, combined with interoperability standards like HL7 and FHIR. This ensures seamless integration with EHR systems, labs, pharmacies, medical devices, and legacy infrastructure without disrupting ongoing operations.
Why Partner With Intellivon?
- Clinical Infrastructure, Not Just Software: Built to support long-term, AI-driven clinical operations across complex and distributed healthcare ecosystems.
- AI-Driven Workflow Automation: Automates documentation, risk analysis, decision support, and administrative workflows to reduce manual burden and improve efficiency.
- Integration-Ready Architecture: Connects seamlessly with healthcare systems, devices, and third-party platforms using FHIR-based and API-first integration models.
- Compliance-First Engineering: Designed with HIPAA-compliant security, encryption, governance frameworks, and AI model transparency built into the system architecture.
- Scalable for Enterprise Healthcare Systems: Supports multi-location providers, high patient volumes, and real-time AI processing without performance or reliability issues.
AI-powered EHR platforms are becoming essential for organizations aiming to scale care delivery, improve outcomes, and operationalize data-driven healthcare. Therefore, building the right AI-enabled system early directly impacts efficiency, compliance, and long-term scalability.
Connect with Intellivon’s experts to build an AI-powered EHR platform tailored to your workflows, integrations, and long-term growth strategy.
FAQs
Q1. What is a smart EHR system with AI?
A1. A smart EHR system uses AI to go beyond storing patient records. It analyzes clinical data, predicts risks, automates documentation, and supports real-time decision-making. As a result, providers can deliver faster, more accurate, and data-driven care.
Q2. How long does AI EHR development take?
A2. AI-powered EHR development typically takes 6 to 12 months, depending on complexity, integrations, and AI features. Basic systems take less time, while enterprise platforms with predictive models and integrations require longer development cycles.
Q3. What AI features are essential in EHR?
A3. Key AI features include clinical decision support, predictive risk models, NLP-based documentation, and workflow automation. In addition, many systems include generative AI for notes and patient communication to improve efficiency and accuracy.
Q4. How much does AI EHR development cost?
A4. The cost to build an AI-powered EHR system ranges from $50,000 to $300,000+. It depends on features, AI model complexity, integrations, and compliance requirements. Enterprise-grade systems with advanced AI capabilities typically fall on the higher end.
Q5. Are AI-powered EHR systems secure?
A5. Yes, AI-powered EHR systems are secure when built with a compliance-first architecture. They follow standards like HIPAA and GDPR, use encryption, access controls, and audit logs. In addition, AI models are monitored to ensure transparency and data safety.