Anesthesia workflows demand constant awareness of patient condition, where even small changes in vitals or dosage can have immediate implications. This synchronized anesthesia EHR monitoring system ensures data from devices and infusion pumps is captured without latency, providing clinicians with a reliable, real-time picture for critical decision-making.
The synchronized exchange of data between monitoring devices, infusion pumps, and EHR platforms is critical within the operating room. This EHR-integrated anesthesia monitoring system ensures clinicians view a reliable patient profile by integrating data streams without introducing latency or information gaps.
In this blog, we explain how to develop anesthesia EHR integration and monitoring systems by examining core system components, architectural considerations, and practical steps involved in building reliable and real-time clinical monitoring solutions.
Why Hospitals Are Investing in Anesthesia EHR Systems?
Modern surgical suites generate massive data volumes, a reality that propelled the global anesthesia information management systems market to USD 534.07 billion in 2023, with projections indicating growth to USD 599.2 billion by 2025 and USD 774.66 billion by 2030, reflecting a steady 5.3% CAGR.
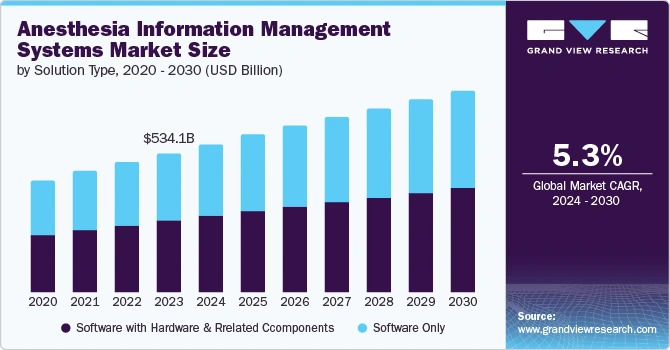
The implementation of a robust anesthesia EHR monitoring system allows facilities to capture this high-velocity data automatically. These digital platforms ensure that clinical precision and operational efficiency keep pace with an increasingly complex perioperative landscape.
Advanced neuroscience-based monitoring algorithms within these systems achieve an average accuracy of 98.0% for drug concentration and 97.09% for oxygen saturation, compared to 95.55% and 95.0% respectively for traditional methods.
Electronic records generally outperform handwritten ones in overall completeness. Studies have shown an 88.6% completeness rate for AIMS records compared to 81.5% for handwritten ones.
Hospitals with fully implemented EHRs saw a 291% decrease in death rates within low-mortality Diagnosis-Related Groups (DRGs) compared to those with no or partial systems.
A. Gaps in Traditional Anesthesia Documentation
Legacy systems often fail to capture the full physiological picture of a patient during surgery. Traditional methods rely on periodic sampling rather than continuous data streams, leading to several critical information gaps:
- Segmented Data Capture: Vital signs are often recorded at 5 or 15-minute intervals, which can miss transient but dangerous physiological events.
- Information Silos: Anesthesia data frequently remains trapped within the operating room, making it difficult for PACU or ICU teams to access immediate intraoperative trends.
- Lack of Contextual Metadata: Without integration, it is difficult to correlate a sudden change in blood pressure with the exact milligram of a drug administered at that same moment.
- Retrospective Logging: Clinicians often have to “chart backward” after a crisis has passed, which relies on memory and leads to significant inaccuracies.
B. Risks of Manual Data Entry in Operating Rooms
Manual transcription is a significant point of failure in high-acuity environments. The physical act of recording data during complex procedures introduces risks that can compromise both patient safety and institutional compliance.
| Risk Category | Impact of Manual Entry | Solution via Automation |
| Cognitive Load | Diverts the provider’s attention from the patient to the clipboard during critical moments. | Hands-free data streaming allows 100% focus on patient monitoring. |
| Transcription Error | Misplaced decimals or illegible handwriting can lead to medication or dosage mistakes. | Direct device-to-cloud synchronization ensures 100% data fidelity. |
| Legal Defensibility | Incomplete or inconsistent manual logs are difficult to defend in malpractice litigation. | Comprehensive, time-stamped digital audits provide an indisputable record of care. |
| Billing Accuracy | Human error in logging gas usage or drug waste leads to lost revenue or compliance flags. | Precise, automated consumption tracking ensures accurate financial reimbursement. |
C. Demand for Real-Time Perioperative Intelligence
The industry is shifting toward proactive care models that utilize live data to guide clinical behavior. Decision-makers are prioritizing systems that offer more than just storage; they require active intelligence.
- Smart Alarms and Notifications: Systems now use algorithms to filter out “noise” and only alert staff to clinically significant deviations in patient vitals.
- Predictive Analytics: By analyzing trends in real time, these platforms can suggest the likelihood of an adverse event before it occurs.
- Resource Optimization: Real-time visibility into OR progress allows management to predict exact closing times, improving staff scheduling and room turnover.
- Standardized Protocols: Integrated systems can prompt providers to follow evidence-based bundles, ensuring high-quality care across every surgical case.
D. How Digital Anesthesia Records Improve Outcomes
Transitioning to digital records directly influences the success rate of surgical interventions. By creating a unified data environment, healthcare facilities see measurable improvements in long-term patient recovery.
- Enhanced Decision Support: The system cross-references live intraoperative data against the patient’s longitudinal record, flagging potential drug-to-drug interactions or allergy risks instantly.
- Reduction in Post-Op Complications: High-fidelity monitoring helps in fine-tuning fluid management and anesthetic depth, which are directly linked to faster recovery times.
- Continuous Quality Improvement: Large datasets allow hospitals to identify which specific anesthetic protocols result in the lowest rates of post-operative nausea or respiratory distress.
- Streamlined Handoffs: Digital records provide the recovery team with a clear, visual history of the surgery, reducing the chance of communication errors during the transition of care.
What Is an Anesthesia EHR Monitoring System?
An anesthesia EHR monitoring system is a digital hub bridging medical hardware and hospital networks. By ingesting high-fidelity data, a robust anesthesia EHR system creates a continuous, automated record of the patient’s entire perioperative journey, replacing fragmented standalone monitors.
A. Core Components of an Integrated OR Ecosystem
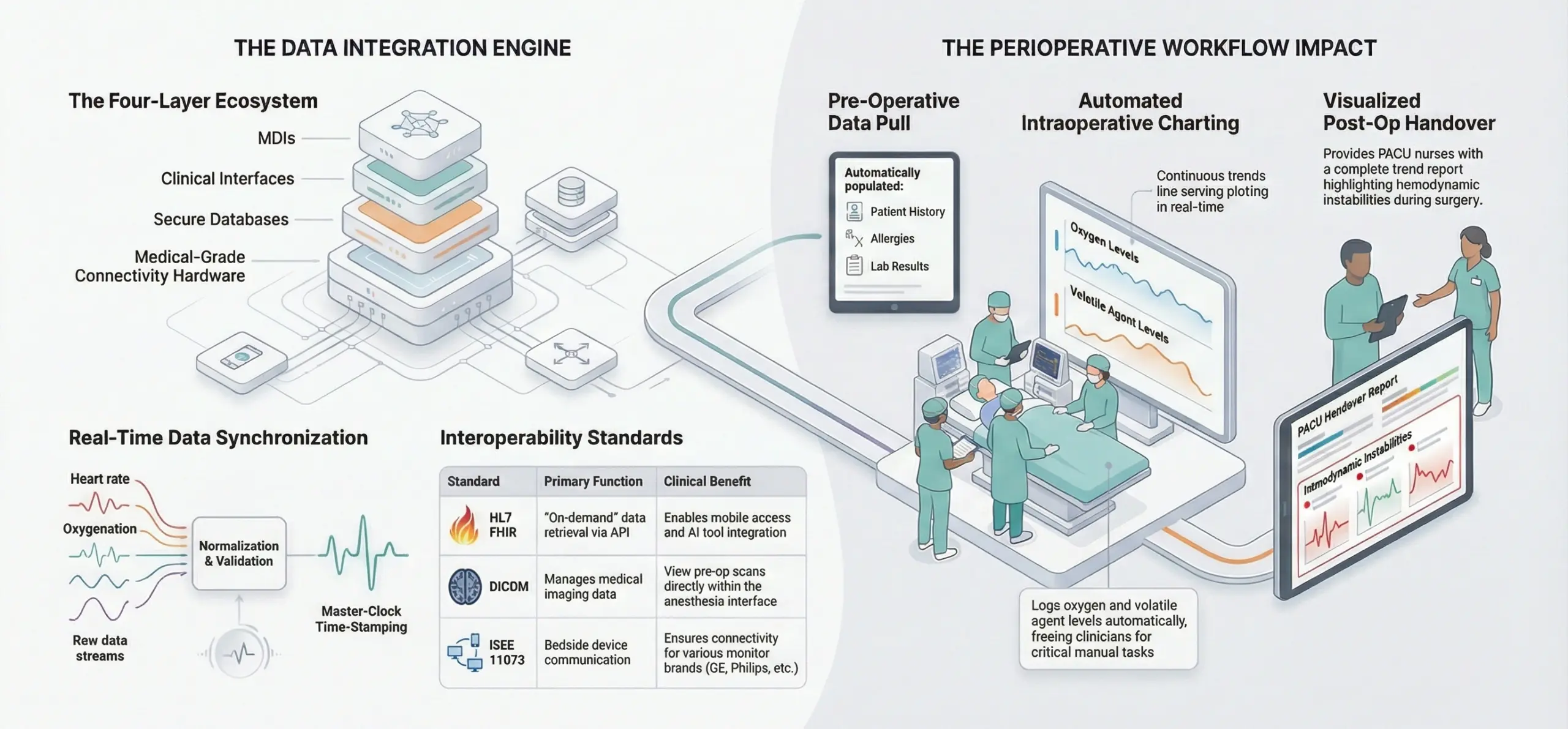
A functional anesthesia EHR monitoring system relies on the seamless interaction of several critical layers. Without the synchronization of these components, data remains fragmented and clinically underutilized.
- Medical Device Interfaces (MDIs): Hardware or software gateways that extract raw data from anesthesia machines, ventilators, and infusion pumps.
- Clinical Information System (CIS): The software interface where providers interact with data, adjust medication logs, and view real-time trends.
- Database and Storage Layer: A secure, high-speed repository designed to handle the massive volume of sub-second waveform data generated during surgery.
- Connectivity Hardware: The physical infrastructure, including medical-grade cabling or encrypted wireless networks, that ensures constant uptime within the shielded environment of an operating room.
B. How Monitoring Devices Sync With EHR Platforms
The synchronization process transforms raw electrical signals from a patient monitor into actionable clinical documentation. This multi-step process occurs in near real-time to ensure the digital record matches the patient’s current state.
- Data Acquisition: The monitor captures vitals like invasive blood pressure, SpO2, and end-tidal CO2.
- Normalization: Raw data from different manufacturers (e.g., GE, Philips, or Dräger) is converted into a standardized format that the central EHR can understand.
- Validation: The system filters out artifacts, such as false alarms caused by sensor movement, to ensure only high-quality data is committed to the permanent record.
- Time-Stamping: Every data point is synchronized with the hospital’s master clock, ensuring that medication administration aligns perfectly with physiological responses in the timeline.
C. Role of HL7 and FHIR in Data Interoperability
Interoperability is the backbone of any modern anesthesia EHR monitoring system. These standards ensure that different software platforms can “speak” the same language without custom, expensive translations for every new device.
| Standard | Primary Function | Clinical Benefit |
| HL7 v2 | The traditional “push” method for sending snapshots of patient data and billing info. | Reliable for basic ADT (Admission, Discharge, Transfer) and lab results. |
| HL7 FHIR | Uses modern API technology (similar to the web) to allow “on-demand” data retrieval. | Enables mobile access to live vitals and faster integration with third-party AI tools. |
| DICOM | Manages and communicates medical imaging data within the surgical workflow. | Allows anesthesiologists to view pre-op scans directly within the anesthesia interface. |
| IEEE 11073 | Specifically standardizes the communication between bedside medical devices. | Ensures “plug-and-play” connectivity for various monitor brands. |
D. Real-Time Data Flow Across Surgical Workflows
The value of an integrated system is most visible in how data moves alongside the patient. A well-designed system ensures that information is never static, following the patient from the holding area to the recovery suite.
- Pre-Operative Assessment: The system pulls the patient’s history, allergies, and lab results from the main EHR, pre-populating the anesthesia start-up screen.
- Intraoperative Transition: As soon as the patient is connected to the OR monitor, the anesthesia EHR monitoring system begins streaming vitals directly into the active surgical record.
- Automated Charting: Changes in oxygen concentration or volatile agent levels are logged automatically, allowing the clinician to focus on manual tasks like intubation or line placement.
- Post-Op Handover: Upon arrival in the PACU, the recovery nurse receives a complete, visualized trend report of the surgery, highlighting any hemodynamic instabilities that occurred under anesthesia.
Key Features Hospitals Expect Before Investing in an Anesthesia EHR System
The demand for automation drives hospital stakeholders to prioritize systems that reduce human error. A robust anesthesia EHR monitoring system provides the deep hardware integration necessary to streamline surgical workflows.
The following features represent the “gold standard” of what healthcare institutions prioritize during the procurement process.
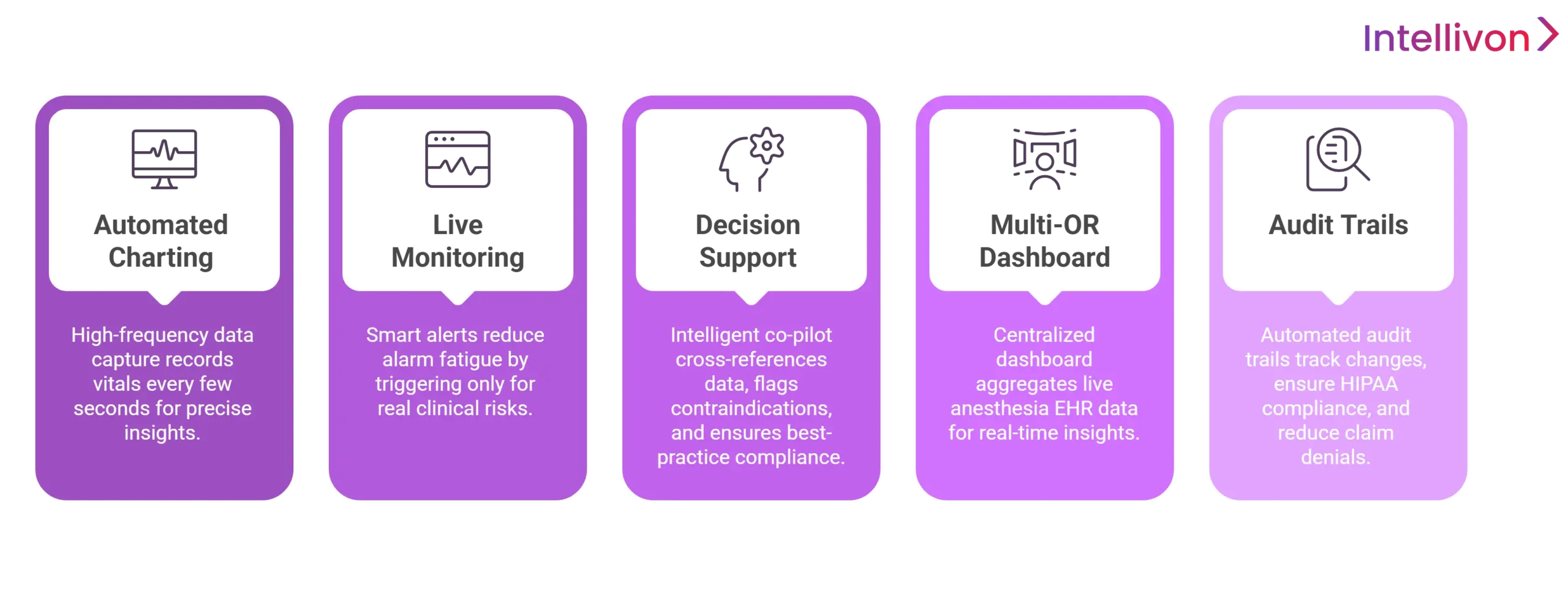
1. Automated Anesthesia Charting From Devices
The hallmark of a high-tier anesthesia EHR monitoring system is high-frequency data acquisition. This automation pulls vitals every few seconds, capturing precise hemodynamic shifts that manual recordings often miss.
The system tracks volatile anesthetic agents and ventilator settings directly from internal sensors. This creates an unalterable, high-fidelity record of gas flows and respiratory rates for improved clinical management.
2. Live Patient Monitoring With Smart Alerts
Modern integrated systems combat alarm fatigue by utilizing multi-parameter smart alerts. This anesthesia EHR monitoring system triggers notifications only when specific physiological factors suggest a genuine clinical crisis.
The system visually integrates these alerts into the digital record. This ensures a proactive safety net where every intervention is logically tied to the patient’s real-time physiological state.
3. Clinical Decision Support During Surgery
This intelligent co-pilot within the anesthesia EHR monitoring system cross-references live data with medical history. The platform flags medication contraindications based on real-time labs stored in the EHR.
The platform also ensures strict compliance with best-practice bundles. Visual reminders for prophylactic antibiotics significantly reduce the risk of surgical site infections and improve overall patient safety outcomes.
4. Multi-OR Dashboard With Central Visibility
A centralized dashboard aggregates live data from every active anesthesia EHR monitoring system. This “bird’s-eye view” allows a single supervisor to oversee multiple rooms and identify stable cases.
These dashboards also provide critical business intelligence for hospital management. Accurate predictions of room availability reduce gap time and minimize expensive staff overtime, creating a more profitable department.
5. Audit Trails and Compliance-Ready Records
The integrity of the medical record is maintained through an anesthesia EHR monitoring system featuring automated audit trails. These logs track every change, ensuring the facility remains HIPAA compliant.
The billing department utilizes these compliance-ready records to capture exact timestamps and drug dosages. This precision reduces claim denials and ensures full reimbursement for the complexity of care.
Must-Have Integrations for Anesthesia EHR Monitoring Systems
Effective scalability in a digital anesthesia environment depends on how seamlessly software communicates with diverse hardware. This anesthesia EHR monitoring system acts as a universal translator, pulling data from legacy monitors while pushing sub-second updates to cloud-based hospital records.
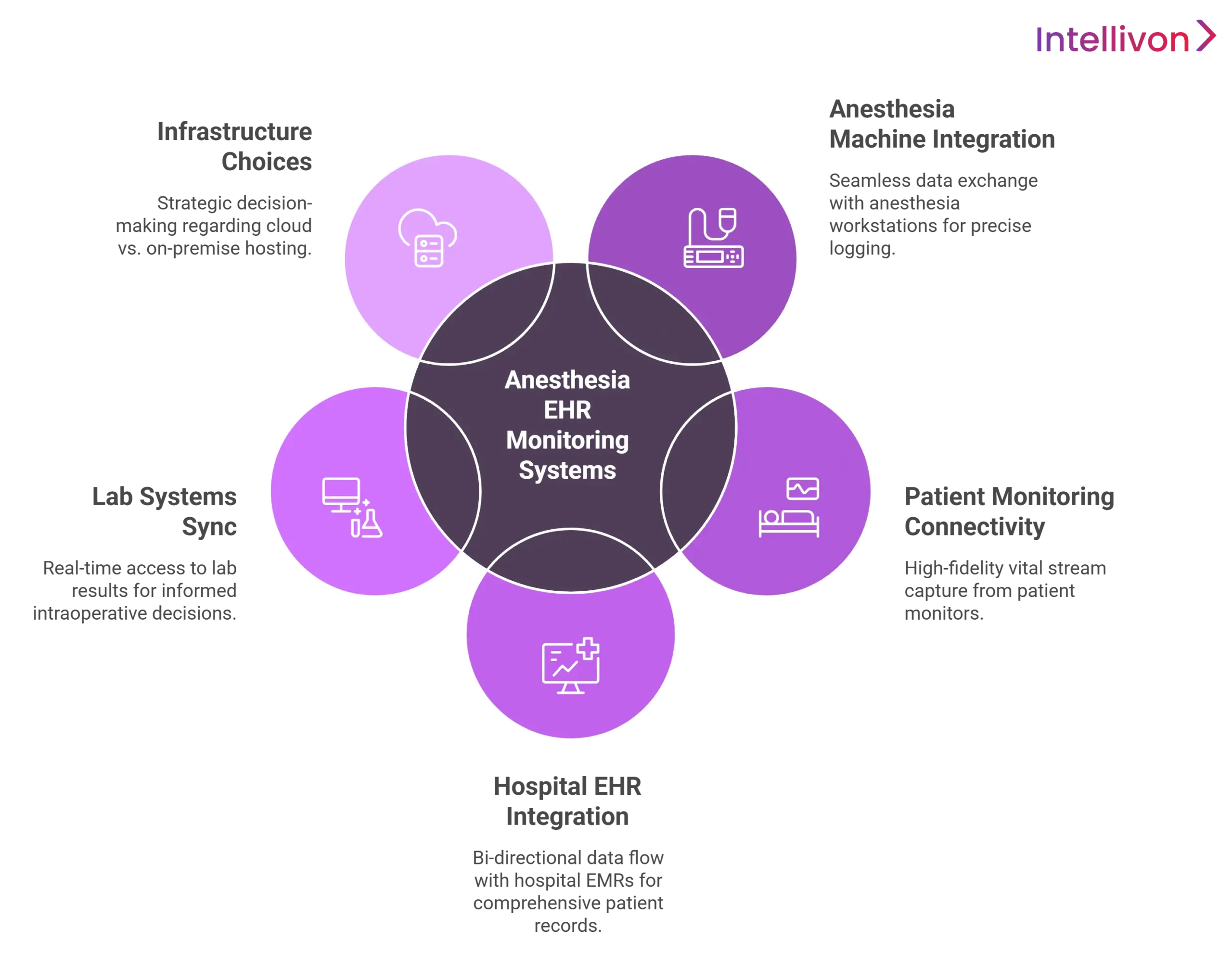
1. Integration With Anesthesia Machines
The anesthesia workstation is the primary data source for any perioperative record. Establishing a robust digital link with these machines ensures that every adjustment made by the clinician is captured with absolute precision.
- Vaporizer Data: Automatically tracks the concentration of anesthetic gases (e.g., Sevoflurane, Isoflurane) to ensure accurate consumption logging.
- Ventilator Parameters: Real-time capture of tidal volume, peak airway pressure, and respiratory rate directly from the machine’s internal sensors.
- Gas Flow Metrics: Monitoring of fresh gas flow and oxygen percentages to provide a complete picture of the patient’s respiratory status.
- Manufacturer Agnostic Drivers: High-end systems utilize proprietary drivers to communicate with GE, Dräger, and Mindray machines simultaneously within the same facility.
2. Patient Monitoring Systems Connectivity
The patient monitor tracks the physiological response to surgery while the anesthesia machine handles ventilation. This anesthesia EHR monitoring system maintains high-fidelity vital streams, ensuring every heartbeat and breath is captured without manual intervention.
- Hemodynamic Data Streaming: Continuous capture of Heart Rate, Invasive Blood Pressure (IBP), and Non-Invasive Blood Pressure (NIBP) to detect sudden “crashes” or trends in cardiovascular stability instantly.
- Oxygenation and Respiratory Tracking: Real-time logging of SpO2 and Plethysmograph waveforms, providing a continuous record of peripheral oxygen saturation and respiratory effort.
- Neuromuscular Transmission (NMT): Automated recording of Train-of-Four (TOF) responses to ensure the patient is properly paralyzed during surgery and adequately reversed before waking.
- Brain Function Monitoring: Integration of BIS or Entropy values to track the depth of anesthesia, which is critical for preventing intraoperative awareness and tailoring drug delivery.
3. Hospital EHR and EMR Platform Integration
The anesthesia record cannot exist as an island; it must be a cohesive part of the patient’s longitudinal health history. Integration with major EMRs like Epic, Cerner, or MEDITECH is a non-negotiable requirement for modern hospital deployments.
- Bi-Directional Data Flow: The system pulls pre-existing conditions and allergies from the EMR and pushes the finalized anesthesia PDF back into the chart upon case closure.
- Single Sign-On (SSO): Clinicians use their standard hospital credentials to access the anesthesia EHR monitoring system, reducing “password fatigue” and improving security.
- Unified Billing: Procedures and supplies logged in the OR are automatically queued in the hospital’s central billing system to reduce revenue leakage.
- Consolidated Medication List: Real-time synchronization ensures that drugs administered in the OR appear in the patient’s “Active Medications” list for the floor nurses post-surgery.
4. Lab Systems and Preoperative Data Sync
Intraoperative decisions are often based on the most recent laboratory results. Integrating with the Laboratory Information System (LIS) ensures that the anesthesiologist has the most current data at their fingertips without leaving the patient’s side.
- Point-of-Care Testing (POCT): Results from “Stat” blood gas machines or thromboelastography (TEG) are sent directly to the anesthesia screen.
- Pre-Op Lab Sync: Hemoglobin, potassium and coagulation studies performed hours before surgery are automatically displayed as baseline references.
- Fluid Management Support: Access to real-time lab trends allows for more precise administration of blood products and IV fluids during major cases.
5. Cloud vs On-Premise Infrastructure Choices
Choosing the right hosting environment is a strategic decision that impacts the speed, security, and long-term cost of the anesthesia EHR monitoring system. Organizations must weigh the benefits of local control against the flexibility of modern distributed networks.
| Infrastructure Type | Core Characteristics | Primary Advantages | Key Considerations |
| On-Premise | Servers are physically located within the hospital data center. | Offers the lowest possible latency for high-speed waveform data and keeps information entirely within the facility’s physical firewall. | Requires significant internal IT resources for maintenance, hardware refreshes, and manual software updates. |
| Cloud (SaaS) | Data is hosted on secure, remote servers like AWS or Azure. | Enables rapid scaling across multiple hospital sites, provides automatic disaster recovery, and reduces upfront capital expenditure. | Depends on consistent internet connectivity and requires rigorous encryption protocols for HIPAA-compliant data in transit. |
| Hybrid / Edge | A mix of local “edge” processing with cloud-based long-term storage. | Combines the real-time speed of local processing with the advanced analytics and storage capacity of the cloud. | Involves a more complex initial architecture and requires sophisticated data synchronization logic. |
Anesthesia EHR Monitoring System Development Process
The construction of a professional anesthesia EHR monitoring system follows a rigorous engineering lifecycle. This process harmonizes high-speed data ingestion with clinical safety standards to ensure platform stability during critical surgical maneuvers.
This phased approach minimizes technical debt and maximizes hospital adoption through verified, interoperable workflows.
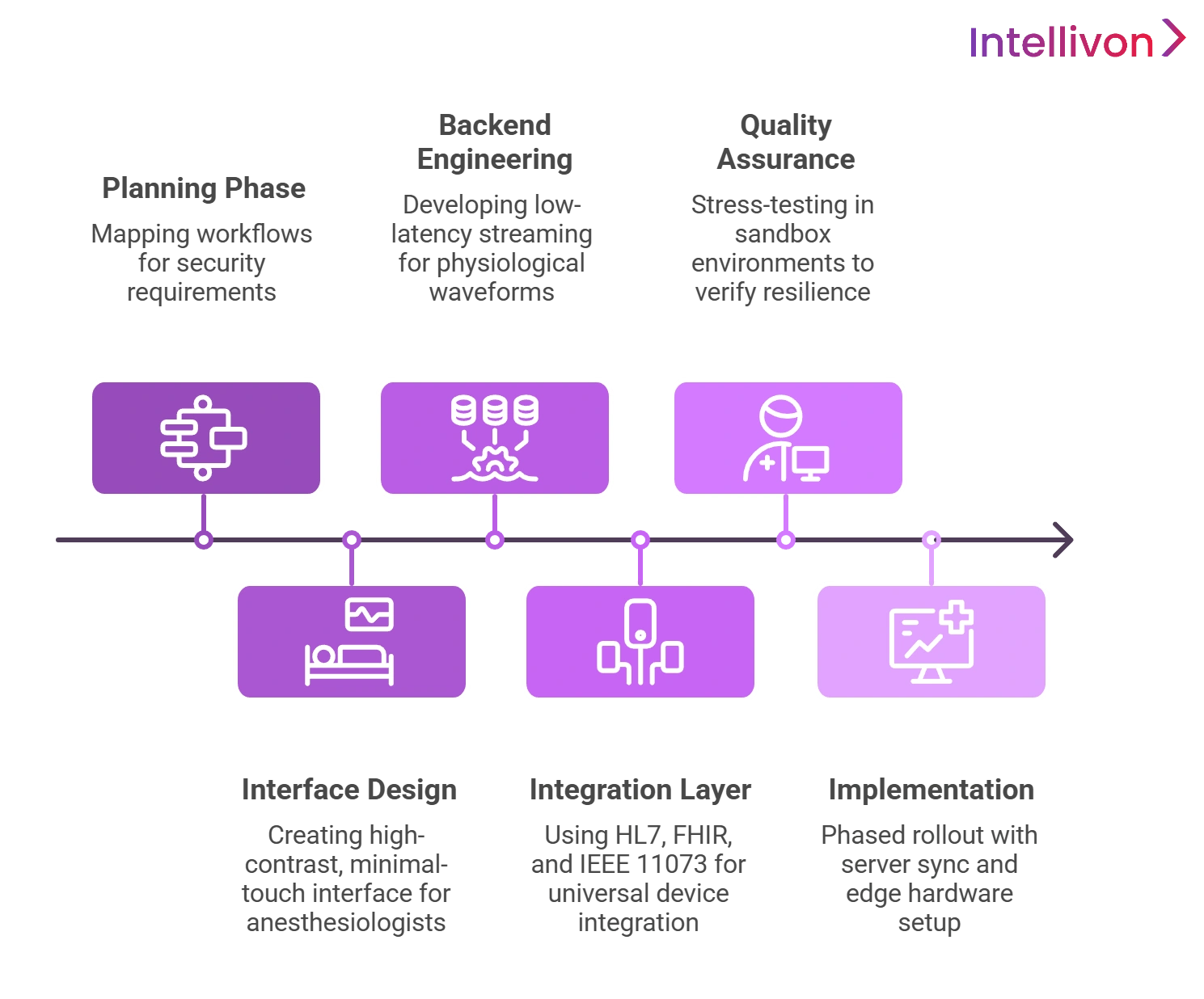
1. Defining Clinical and Technical Requirements
Foundational planning centers on mapping perioperative workflows to technical specifications. This stage involves identifying mandatory data points for anesthesia records, establishing hardware compatibility lists, and ensuring strict adherence to HIPAA and SOC2 security frameworks. Clear requirements prevent scope creep during complex integration phases.
2. Designing OR-Centric UX for Anesthesiologists
Interface architecture prioritizes high-contrast visibility and minimal touch-points. A successful design reduces cognitive load by displaying critical vitals and medication timers on a single, uncluttered screen. This user-centric focus ensures clinicians remain focused on the patient rather than navigating software.
3. Building Real-Time Data Capture Pipelines
Backend engineering focuses on low-latency streaming architectures capable of processing sub-second physiological waveforms. These pipelines utilize message brokers to handle high-volume data bursts from multiple ORs. Robust data ingestion is essential for maintaining a synchronized, “no-drop” digital anesthesia record.
4. Implementing Device Connectivity Protocols
Communication layers leverage industry standards like HL7, FHIR, and IEEE 11073 for universal hardware interaction. This protocol-heavy development allows the software to translate raw signals from ventilators and monitors into structured clinical data. These connectors form the backbone of interoperable systems.
5. Testing With Simulated Surgical Environments
Quality assurance involves stress-testing the platform within sandboxed environments that mimic high-acuity crises. Engineers simulate massive data influxes and network outages to verify system resilience. This “stress-test” methodology ensures the anesthesia EHR monitoring system performs reliably under real-world surgical pressure.
6. Deployment Across Multi-Operating Room Setups
Final implementation requires a phased rollout that includes server-side synchronization and localized “edge” hardware configuration. Technical teams focus on ensuring zero downtime during the transition from legacy systems. Scalable deployment strategies allow for centralized management across expansive, multi-site hospital networks.
Anesthesia EHR Monitoring System Development Cost
The costs below reflect optimized estimates for specialized medical software development, balancing high-security engineering with lean development practices for an anesthesia EHR monitoring system.
| Development Phase | MVP Level | Enterprise Level | Key Deliverables |
| Discovery & Compliance | $18,000 – $30,000 | $45,000 – $75,000 | Technical architecture, HIPAA roadmap, and clinical workflow mapping. |
| UX/UI & Prototyping | $10,000 – $18,000 | $30,000 – $55,000 | High-fidelity OR dashboards and accessible touch interfaces. |
| Core Engine & Connectivity | $40,000 – $65,000 | $120,000 – $190,000 | Real-time data pipelines and device driver development. |
| Security & Interoperability | $22,000 – $38,000 | $65,000 – $110,000 | End-to-end encryption and EMR (Epic/Cerner) bridging. |
| Testing & QA (V&V) | $15,000 – $28,000 | $40,000 – $80,000 | Clinical simulation testing and stress-load verification. |
| Total Estimated Cost | $85,000 – $159,000 | $240,000 – $410,000 | A validated, scalable anesthesia monitoring solution. |
Cost-Affecting Factors During Development
The final price of an anesthesia EHR system is influenced by technical and regulatory variables that can shift the budget by 15% to 25% during the build. Precise planning around these drivers is essential for maintaining the initial investment target.
- Device Integration Count: Standardizing for 1-2 brands is cost-effective, but supporting a mixed-fleet of 8+ different anesthesia machines and ventilators significantly increases integration hours.
- EMR Interoperability Level: Simple one-way exports are cheap; however, bi-directional API integration with platforms like Epic or Cerner adds $35,000 to $60,000 in specialized engineering.
- Data and Storage Needs: Capturing vitals at 1-second intervals requires 4x more investment in high-performance cloud storage and high-uptime SLAs compared to 1-minute intervals.
- Regulatory Audits: Achieving FDA Class II clearance or CE marking involves rigorous testing, potentially adding $40,000 to $120,000 to the total project lifecycle.
- Cybersecurity Protocols: Mandatory penetration testing and HIPAA audits for hospital-grade systems typically cost between $12,000 and $25,000 per round of verification.
Architecture Behind Anesthesia EHR Monitoring Systems
The technical foundation of an anesthesia EHR monitoring system must prioritize low-latency data handling and uncompromising security. Building a platform that operates within a surgical environment requires an architecture that can ingest high-velocity data from multiple sources while ensuring that the clinical record remains accurate and synchronized.
| Component | Technical Functionality | Strategic Value |
| Data Ingestion From Medical Devices | Utilizes specialized drivers and hardware gateways to pull raw signals from anesthesia machines and ventilators. | Ensures 100% data fidelity by eliminating manual transcription and capturing every physiological shift. |
| Stream Processing for Live Vital Tracking | Employs high-speed message brokers to process sub-second waveforms (ECG, SpO2) into readable clinical trends. | Provides clinicians with an instantaneous view of patient status, allowing for immediate intervention during crises. |
| Secure APIs for EHR Synchronization | Leverages HL7 FHIR-based RESTful APIs to push and pull data between the anesthesia module and the central hospital record. | Creates a unified patient history and automates the transfer of intraoperative logs to the permanent medical chart. |
| Alert Engines for Risk Detection | Runs complex algorithmic logic to identify abnormal patterns across multiple vitals simultaneously. | Reduces alarm fatigue by only triggering notifications for clinically significant events, enhancing overall patient safety. |
| Scalable Cloud Infrastructure | Uses containerized microservices and edge computing to manage data loads across multiple operating rooms. | Allows for rapid deployment across large hospital networks while maintaining the high uptime required for surgical care. |
Security & Compliance Framework of Anesthesia EHR Monitoring System
Rigorous legal and ethical standards are essential for hospital adoption of an EHR monitoring system. By prioritizing “security by design,” these platforms protect sensitive physiological waveforms and controlled substance logs, ensuring data integrity remains uncompromised during high-stakes surgical procedures.
1. Ensuring HIPAA Compliance in Anesthesia Systems
Compliance begins with the implementation of the Physical, Administrative, and Technical Safeguards mandated by HIPAA to protect sensitive patient information. Developing an anesthesia EHR monitoring system requires a security-first architecture that ensures Protected Health Information (PHI) is only accessible to authorized clinical personnel.
- Business Associate Agreements (BAAs): Establishing formal legal contracts with all cloud hosting providers and third-party vendors to ensure they meet federal data handling standards.
- Data Portability and Privacy: Implementing secure protocols that allow for the seamless export of anesthesia records into the hospital’s primary EMR without risking unauthorized exposure or data leakage.
- Workstation Security: Configuring automatic session timeouts and encrypted “tap-and-go” badge access to prevent unauthorized viewing of active anesthesia screens in busy operating rooms.
- Patient Rights Management: Ensuring the system can generate patient-readable summaries and maintain the integrity of the medical record for the duration of the required retention period.
2. Data Encryption and Secure Device Communication
To protect data in transit and at rest, the system employs Advanced Encryption Standard (AES-256) for storage and Transport Layer Security (TLS 1.3) for all communications between medical devices and the central server.
- End-to-End Encryption: Data captured from the anesthesia machine is encrypted at the source before being transmitted over the hospital network.
- Device Authentication: Each monitor or ventilator must pass a digital handshake protocol to ensure that only “white-listed” hospital hardware can stream data into the patient record.
- VPN-less Secure Tunnels: Modern architectures use specialized secure gateways to allow remote monitoring without the vulnerabilities associated with traditional VPNs.
3. Role-Based Access for Clinical Teams
Not every individual in the operating room requires the same level of data access. Role-Based Access Control (RBAC) ensures that permissions are granular and tied to specific clinical duties.
- Anesthesiologists: Have full read/write access to clinical vitals, medication logs, and the final attestation of the record.
- Surgical Nurses: May have “view-only” access to vitals for coordination but restricted access to anesthesia-specific drug dosing.
- IT/Administrative Staff: Can access system health metrics and audit logs but are strictly barred from viewing identifiable patient clinical data.
4. Handling Audit Logs and Legal Requirements
A defensible medical record requires an unalterable trail of every interaction that occurred within the software to meet both clinical and legal standards. These logs are essential for hospital quality reviews, proving the sequence of care, and providing a robust defense in the event of malpractice litigation.
- Immutable Write-Once Storage: Utilizing WORM (Write-Once-Read-Many) technology for all clinical entries, ensuring that once a data point is committed, it cannot be retroactively altered or deleted.
- Synchronized Network Time-Stamping: Linking all device data to a central Network Time Protocol (NTP) server to prove the exact chronological sequence of drug administrations relative to physiological changes.
- Comprehensive Version History: Tracking every manual modification or annotation made to the automated data stream, providing full transparency into who made a change and why.
- Forensic Audit Capability: Building search and reporting tools that allow administrators to reconstruct the entire clinical narrative of a surgical case during a regulatory audit or legal discovery process.
5. Cybersecurity Challenges in Connected ORs
The transition to “Connected ORs” increases the attack surface for potential cyber threats, including ransomware that could target life-critical systems.
- Legacy Vulnerabilities: Many older anesthesia machines were not designed with modern security in mind, requiring “Edge” security devices to wrap them in a protective digital layer.
- Network Segmentation: Successful systems isolate the anesthesia EHR monitoring system on a dedicated VLAN, preventing a breach in the hospital’s public Wi-Fi from reaching the surgical suite.
- Real-Time Threat Detection: Incorporating AI-driven anomaly detection can identify unusual data patterns that may indicate a brute-force attack or unauthorized data exfiltration attempts.
Timeline to Build a Full-Scale Anesthesia EHR Monitoring System
The development lifecycle of a medical-grade anesthesia EHR monitoring system is governed by technical precision and regulatory milestones. This structured timeline ensures patient safety and data integrity while guiding stakeholders through the complex requirements of device integration and hospital-wide deployment.
A. MVP Development Timeline for Core Features
The development of a medical-grade anesthesia EHR monitoring system MVP typically spans 4 to 6 months. This initial phase establishes a stable data ingestion engine capable of communicating with major anesthesia hardware.
- Engineering Core: Focuses on building the database architecture and high-speed data pipelines for real-time vitals.
- Interoperability Setup: Establishes essential HL7/FHIR data structures to ensure seamless hospital information exchange.
- Clinical Interface: Prioritizes designing a specialized operating room UI for displaying and recording live patient data.
- Phase Goal: Concludes with a system capable of reliable data recording within a controlled clinical environment.
B. Integration and Testing Phase Duration
The subsequent 3 to 5 months focus on expanding the anesthesia EHR monitoring system to include diverse hardware. This stage ensures high-frequency data bursts function without latency across the facility.
- Mixed-Fleet Validation: Engineers standardize drivers for various monitor brands to ensure seamless data synchronization.
- Stress Testing: The platform undergoes rigorous simulation to verify stability during high-volume surgical flows.
- User Experience Refinement: Clinical consultants perform alpha and beta testing to eliminate any workflow friction for anesthesiologists.
C. Compliance and Certification Timelines
Navigating the regulatory landscape for an anesthesia EHR monitoring system typically requires 6 to 12 months. This timeline runs parallel to development but depends on a feature-complete architecture.
- Regulatory Submissions: Documentation is prepared for FDA Class II clearance or CE marking to prove clinical safety.
- Security Audits: The system undergoes independent SOC2 certification and HIPAA audits to verify robust data protection.
- Clinical Validation: Formal studies are conducted to provide evidence of the system’s efficacy and accuracy in live environments.
D. Scaling Across Hospitals and Locations
Transitioning from a single-site pilot to a multi-hospital rollout generally takes 4 to 8 months. A scalable anesthesia monitoring system must support concurrent users across different geographic locations.
- Cloud Infrastructure: Engineering teams configure centralized cloud management and site-specific “edge” servers for low-latency performance.
- EMR Synchronization: The system is integrated with different instances of hospital EMRs like Epic or Cerner.
- Staff Adoption: Training protocols are established to ensure wide-scale clinical buy-in and consistent data entry across the enterprise.
Key Milestone Summary Table
Strategic planning for an anesthesia EHR monitoring system requires a clear roadmap. This summary table outlines the critical development phases, estimated durations, and primary goals necessary for a successful rollout.
| Milestone | Estimated Duration | Primary Goal |
| Phase 1: Architecture & MVP | 4 – 6 Months | Functional data ingestion from 1-2 device types and core OR UI. |
| Phase 2: Device & EMR Integration | 3 – 5 Months | Full connectivity with “mixed-fleet” monitors and Epic/Cerner platforms. |
| Phase 3: Security & Compliance | 6 – 12 Months | Achieving HIPAA, SOC2, and required medical device certifications. |
| Phase 4: Pilot & QA | 2 – 3 Months | Live-environment testing in a controlled, single-facility surgical suite. |
| Phase 5: Enterprise Scaling | 4 – 8 Months | Multi-site deployment and centralized administrative dashboard rollout. |
Real-World Use Cases and Implementation Scenarios
Deploying an anesthesia EHR monitoring system transforms theoretical data into a practical clinical asset. Across various medical environments, these systems bridge the gap between high-volume data production and actionable medical insights, ensuring that patient safety remains consistent regardless of the facility’s size or surgical complexity.
1. Large Hospitals Managing Multi-OR Operations
Enterprise systems allow surgical directors to oversee dozens of simultaneous cases from a single command center. This visibility optimizes room turnover and identifies staffing needs before delays occur.
Example: The Cleveland Clinic implemented a centralized “Operations Command Center” using real-time data to manage over 100 operating rooms, significantly reducing patient wait times and improving OR utilization.
2. Specialty Surgical Centers Optimization
Boutique centers leverage integrated records to maintain high-efficiency throughput while meeting strict accreditation standards. Automated charting reduces the administrative time required for each patient, increasing daily case capacity.
Example: The Texas Heart Institute utilized automated anesthesia record-keeping to streamline data flow during complex cardiovascular procedures, allowing for more precise titration of potent anesthetic agents and faster recovery.
3. Remote Monitoring for Critical Surgeries
Secure data streaming enables senior consultants to provide real-time guidance to junior residents or CRNAs from off-site locations. This capability ensures expert oversight for high-risk procedures without geographic limitations.
Example: GE Healthcare’s Mural Virtual Care Continuum allows a single intensivist or senior anesthesiologist to monitor multiple high-risk patients across different hospital wings or even different cities during critical surgical phases.
4. Data-Driven Decision Making in ICU and OR
Seamless data flow between the operating room and the intensive care unit ensures that post-operative care is based on accurate intraoperative trends rather than fragmented verbal handoffs.
Example: Mount Sinai Health System integrated its anesthesia records with its “Clinical Control Center” to use predictive analytics, identifying patients at risk for post-operative respiratory failure before they left the OR.
Case Study: Building a Smart Anesthesia Platform
A prominent surgical network required a modernized digital infrastructure to replace fragmented, manual documentation processes. The goal was to develop a unified anesthesia EHR monitoring system capable of capturing high-fidelity data.
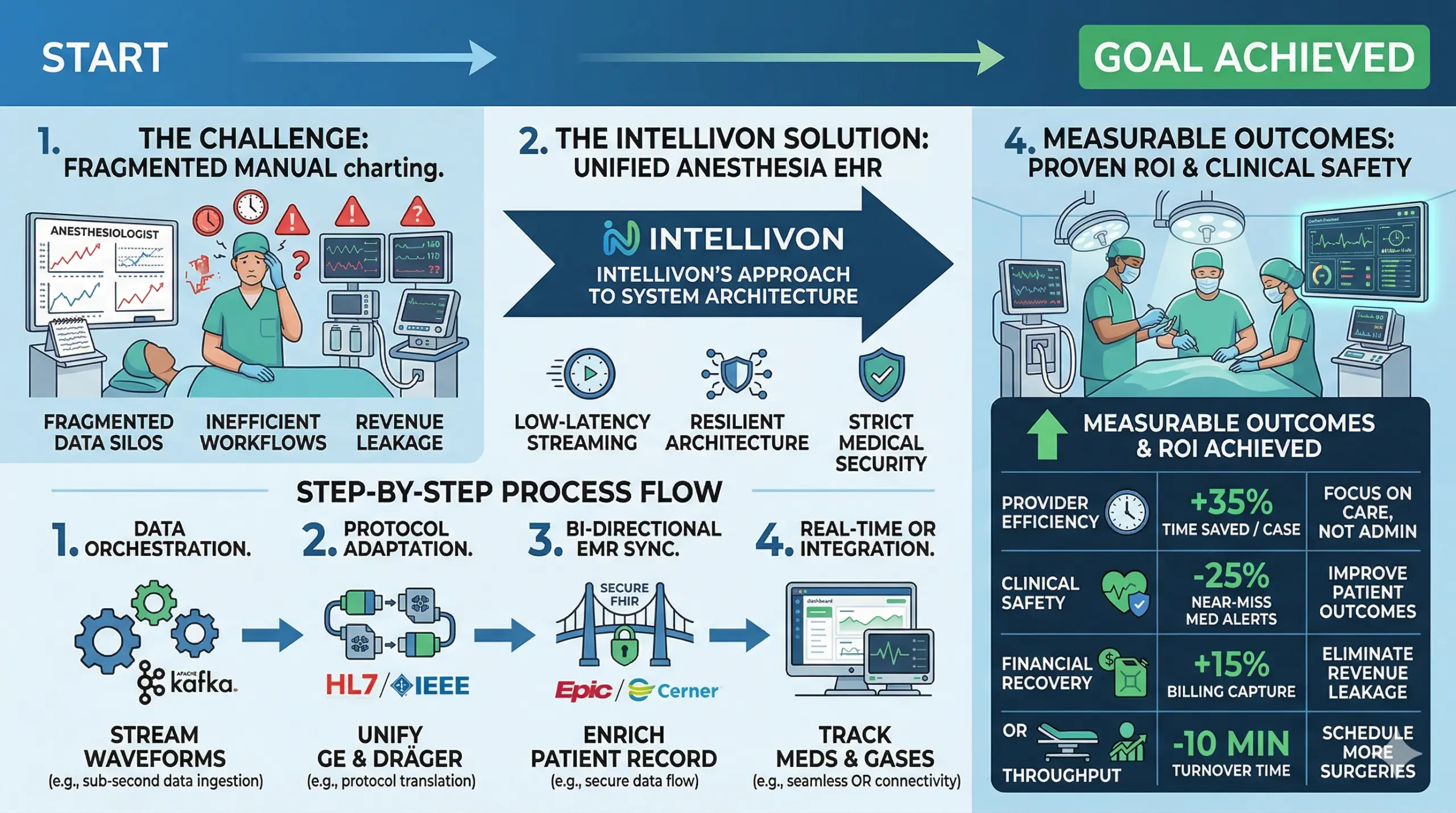
A. Problem Faced by the Healthcare Provider
The provider struggled with inconsistent data logging and significant information gaps during critical surgical transitions. These manual workflows created operational bottlenecks and increased the risk of preventable clinical errors.
- Documentation Latency: Anesthesiologists spent approximately 20% of their time on manual charting instead of active patient surveillance.
- Data Fragmentation: Physiological data from ventilators and monitors existed in silos, preventing a cohesive view of the patient’s intraoperative state.
- Billing Inaccuracy: Inconsistent logging of anesthetic agents led to a 12% revenue leakage due to uncaptured supply costs.
- Audit Risks: Hand-written records were often illegible or incomplete, posing significant compliance risks during regulatory inspections.
B. Intellivon’s Approach to System Architecture
Our development team focused on building a low-latency, resilient architecture designed to handle massive data bursts from multiple operating rooms simultaneously while maintaining strict medical-grade security and data integrity.
- Situation: The client needed a scalable, cloud-ready platform that could integrate with diverse, multi-vendor anesthesia machines without compromising real-time performance.
- Task: Our engineers were tasked with designing a streaming data pipeline that could ingest sub-second waveforms and synchronize them with the hospital’s central EMR.
- Action: We implemented a microservices architecture using Apache Kafka for data orchestration and built custom “adapter” modules for HL7 and IEEE 11073 protocol translation.
- Result: This approach achieved a 99.99% uptime during pilot testing and successfully consolidated data from GE and Dräger machines into a single unified dashboard.
C. Integration With Devices and EHR Systems
The integration strategy prioritized seamless connectivity between physical medical hardware and the digital record. This ensured that data flowed bi-directionally, enriching the patient’s longitudinal history with high-fidelity surgical insights.
| Integration Layer | Technical Solution |
| Medical Device Gateway | Developed proprietary drivers to extract real-time ventilator settings and volatile gas concentrations directly from the anesthesia workstation. |
| EMR Interoperability | Built a secure HL7 FHIR bridge to synchronize patient demographics, allergies, and lab results with the hospital’s Epic and Cerner environments. |
| Waveform Ingestion | Implemented a high-speed telemetry interface to capture and store continuous ECG and SpO2 waveforms for retrospective clinical analysis. |
| Pharmacy/LIS Link | Integrated with the hospital’s automated dispensing cabinets to track medication administration against physiological responses in real-time. |
D. Measurable Outcomes and ROI Achieved
Post-implementation data revealed significant improvements in both clinical safety and financial performance. The transition to an automated anesthesia EHR monitoring system provided a clear path to long-term operational sustainability.
| Metric Category | Outcome Achieved | Strategic Impact |
| Provider Efficiency | 35% reduction in time spent on documentation per surgical case. | Allows clinicians to focus more on patient care and less on administrative tasks. |
| Clinical Safety | 25% decrease in “near-miss” medication alerts due to real-time decision support. | Directly improves patient outcomes and reduces the risk of post-operative complications. |
| Financial Recovery | 15% increase in captured billing for anesthetic gases and controlled substances. | Eliminates revenue leakage and ensures full reimbursement for clinical resources used. |
| OR Throughput | 10-minute average reduction in room turnover time due to streamlined handoffs. | Enables the facility to schedule additional surgical cases, increasing overall profitability. |
Why Choose Intellivon for Your Anesthesia EHR Monitoring Platform?
Partnering with Intellivon ensures your surgical infrastructure is built on a foundation of clinical precision and technical excellence. We specialize in transforming complex perioperative data into high-performance, integrated healthcare solutions.
A. Domain Expertise in Healthcare IT Solutions
Our team brings years of specialized experience in navigating the intricate workflows of the operating room. We understand the critical nuances of anesthesia documentation, ensuring every digital feature aligns perfectly with real-world clinical demands.
B. Scalable and Future-Ready System Design
We engineer platforms that grow alongside your medical facility by utilizing modular microservices and cloud-native architectures, we ensure your anesthesia EHR monitoring system remains compatible with emerging medical technologies and increasing patient data volumes.
C. Strong Focus on Security and Compliance
Data integrity is our highest priority. We implement multi-layered encryption, rigorous HIPAA-compliant protocols, and SOC2-certified frameworks to protect sensitive patient information and ensure your facility meets every regulatory requirement with absolute confidence.
D. Dedicated Support and Post-Launch Optimization
Our commitment extends far beyond the initial deployment, providing continuous technical oversight, rapid troubleshooting, and iterative software updates based on clinician feedback to ensure your platform consistently delivers peak operational and financial performance.
Conclusion
Developing a professional anesthesia EHR monitoring system is a strategic move toward clinical excellence and operational efficiency. By automating data capture, ensuring high-fidelity monitoring, and maintaining rigorous compliance, hospitals can significantly reduce human error and improve patient safety. While the development and integration process requires technical precision and a structured timeline, the long-term benefits of real-time perioperative intelligence are invaluable. Ultimately, these advanced platforms empower care teams to focus on what matters most: delivering superior, data-driven patient care in high-stakes environments.
FAQs
Q.1. What is the cost to build an anesthesia EHR monitoring system?
A.1. Development costs typically range from $85,000 to over $300,000+. Total investment depends on the number of device integrations, bi-directional EMR connectivity, and the complexity of regulatory compliance and cybersecurity audits.
Q.2. How does the anesthesia EHR system handle data during patient transport?
A.2. Mobile connectivity features ensure the anesthesia EHR monitoring system maintains a continuous data stream. Wireless protocols prevent gaps in the medical record while moving patients between the ward and operating room.
Q.3. Which compliance standards apply to anesthesia EHR monitoring platforms?
A.3. Systems must strictly adhere to HIPAA for data privacy and SOC2 for security. Additionally, obtaining FDA Class II clearance is mandatory to ensure the software meets clinical safety requirements.
Q.4. How does an anesthesia EHR monitoring system reduce clinical errors?
A.4. The system automates high-frequency data collection to eliminate manual transcription gaps and legibility issues. By providing real-time alerts and cross-referencing patient history with live vitals, the platform helps clinicians catch potential complications before they escalate.