In many outpatient clinics, the real issue is not patient volume but the small delays between visits that slowly reduce efficiency. Notes may get written on paper and could be missed later, which affects clinical continuity. Follow-ups often rely on memory, and this can gradually reduce consistency in care delivery. Over time, these gaps may quietly impact both outcomes and provider confidence.
Many healthcare institutions have started relying on certified EHR systems for ambulatory care because they need faster documentation and more reliable patient data access. With stricter HIPAA rules and complex coordination, these systems can support compliance and improve care workflows. Certified platforms guided by ONC standards now provide a scalable and trusted foundation for modern outpatient care.
Over the years, we’ve developed numerous certified EHR systems powered by healthcare interoperability frameworks and clinical data intelligence systems. As we have this expertise, we’re sharing this blog to discuss the steps to build a certified EHR system for ambulatory care.
Why Ambulatory EHR Demand Is Rising in 2026?
According to Fortune Business Insights, the global ambulatory EHR market was valued at USD 9.47 billion in 2025 and is projected to reach USD 15.93 billion by 2034, with a CAGR of 6.07%. North America led the sector with a 47.26% market share in 2025. These metrics confirm that digital infrastructure is now the primary determinant of financial health for private practices.
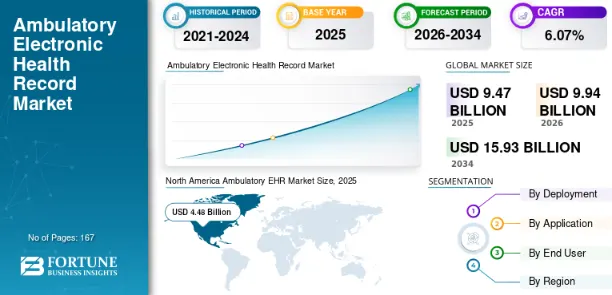
Source: Fortune Business Insights
The shift toward specialized ambulatory EHR stems from a rejection of bulky, hospital-centric legacy systems. In 2026, the market prioritizes agility and physician autonomy. Healthcare entrepreneurs recognize that inpatient software lacks the speed required for high-volume outpatient environments.
Dominant players like Epic have adapted with EpicCare Ambulatory, yet the market remains hungry for more agile, cloud-native alternatives.
Modern demand is fueled by the rapid decentralization of care. Investors are backing specialized clinics that require lean, purpose-built digital ecosystems. An ambulatory EHR is now a strategic engine designed to eliminate administrative friction and secure revenue in a competitive landscape.
Shift to Outpatient-First Models
Health systems are migrating high-volume procedures, including orthopedics and imaging, to Ambulatory Surgery Centers to maximize profitability. This transition is driven by payer cost-containment and patient demand for localized care.
For developers and investors, this creates a niche for systems that solve specific outpatient pain points:
- Throughput Optimization: Platforms must enable rapid charting to match the fast pace of clinic visits.
- Clinical Specialization: Success lies in “niching down” with pre-configured templates. For instance, ModMed has gained significant traction by building specialty-specific workflows for dermatology and orthopedics.
- Consumer Integration: Tools that offer mobile scheduling and transparent billing are winning by treating patients as consumers.
ONC Compliance Pressure
Regulatory focus has moved from simple data entry to radical data liquidity. The Office of the National Coordinator is strictly enforcing 21st Century Cures Act mandates regarding information blocking and standardized API usage.
New platforms must support FHIR® bulk data exports to remain viable. Non-compliance represents a significant commercial liability. Platforms like Athenahealth have thrived by managing these updates in the cloud, relieving the practice of manual compliance burdens. Practices are abandoning closed systems to avoid federal penalties and ensure participation in modern health exchanges.
Revenue Impact of MIPS
The EHR has become a critical financial tool under the Merit-based Incentive Payment System or MIPS. In 2026, Medicare reimbursement gaps between high and low performers are wide enough to dictate practice solvency.
Sophisticated EHRs automate MIPS data capture, turning compliance into a profit center. These systems allow owners to:
- Close Care Gaps: Automated flagging of missing screenings improves Quality scores.
- Automate Reporting: Workflows ensure “Promoting Interoperability” marks are met without manual audits.
- Enhance EBITDA: Securing maximum reimbursement multipliers is vital for private equity-backed groups looking to scale.
What Makes an EHR System “Certified” in Practice?
ONC certification is the primary gateway for market entry and reimbursement. Systems without this status are barred from federal marketplaces and private payer networks. It ensures a platform meets strict standards for clinical data management, privacy, and technical reliability.
Established solutions like Oracle Health have long set the benchmark for these requirements, ensuring that software remains stable under complex clinical loads.
Certification involves rigorous testing by an ONC-Authorized Testing Laboratory. Investing in a certified system mitigates risk by ensuring the product adheres to the highest industry benchmarks for safety and operational performance.
Criteria under ONC Certification
The ONC mandates “Conditions and Maintenance of Certification” to prevent information blocking and ensure accuracy:
- Clinical Quality Measures: Systems must accurately report quality data to CMS to qualify for practice incentive payments.
- Safety-Enhanced Design: Formal UX testing must prove the interface reduces clinician error during tasks like e-prescribing.
- Audit Transparency: Software must maintain detailed logs tracking all record access or edits to ensure total accountability.
Role of HIPAA in System Design
HIPAA dictates architecture through “Privacy by Design.” For high-stakes development, this goes beyond basic encryption. Systems like eClinicalWorks have navigated these requirements by integrating robust security protocols directly into their cloud-based ambulatory platforms.
Modern systems use multi-factor authentication and role-based access controls (RBAC) to protect data at rest and in transit. In the ambulatory sector, HIPAA compliance extends to mobile device interactions and patient portals.
Prioritizing platforms with automated “Business Associate Agreement” management and proactive breach detection limits long-term legal liability.
Interoperability and Data Exchange Standards
A siloed EHR is a failed asset. Modern certification requires the FHIR® standard, allowing disparate systems to communicate via standardized APIs.
True interoperability ensures patient records move seamlessly from clinics to specialists without manual intervention. Strategic systems integrate with national networks like CommonWell or Carequality. This connectivity is a competitive necessity for attracting large medical groups that coordinate care across multiple locations.
Who Should Invest in Ambulatory EHR Development?
Investing in ambulatory EHR development is a strategic move for those targeting the fastest-growing segment of healthcare. As care migrates away from hospitals, the infrastructure supporting outpatient clinics becomes a highly valuable asset. This investment is about owning the workflow of the modern medical practice.
The current market favors platforms that solve specific operational inefficiencies. Developing a proprietary or highly customized EHR allows for the capture of data and revenue that generic systems often overlook. For those with the capital to build, the focus should be on creating an ecosystem that acts as the central nervous system for high-growth medical groups.
1. Multi-Specialty Clinics Scaling Operations
Large-scale medical groups and multi-specialty clinics represent the most immediate use case for custom EHR investment. As these organizations expand, the limitations of off-the-shelf software, such as rigid workflows and per-user licensing fees, become significant barriers to profitability.
- Operational Control: Custom development allows these clinics to standardize care protocols across dozens of locations to ensure clinical consistency.
- Data Centralization: Multi-specialty groups require a single source of truth for patients seeing different specialists within one network. Systems like NextGen Healthcare have dominated this space by offering deep integration across varied clinical needs.
- Cost Efficiency: At scale, the cost of maintaining a proprietary system is often lower than the cumulative licensing fees of third-party vendors. This shift directly improves the group’s long-term EBITDA.
2. Startup Founders In Digital Health
The digital health sector is ripe for disruption by founders who can identify underserved niches. Entering the market with a specialized ambulatory EHR provides a clear value proposition in an industry tired of bloated software.
Success for startups lies in the Platform as a Service model. By building a lean, API first EHR, founders can offer seamless integrations with Telehealth and AI-driven diagnostics.
Modern entrants like Elation Health have challenged legacy giants by focusing on a clinical-first experience that prioritizes the physician’s time over data entry. Founders who prioritize user experience and interoperability from day one are best positioned to attract venture capital.
3. Providers Replacing Legacy Systems
A significant portion of the market still relies on outdated legacy software or manual paper records. These providers face mounting pressure to modernize due to declining reimbursements and increasing regulatory demands.
Replacing these systems is a high-priority investment for practices looking to:
- Recover Lost Revenue: Legacy systems often lack the sophisticated coding and billing triggers found in modern EHRs, which leads to frequent claim denials.
- Enhance Patient Retention: Modern patients expect digital touchpoints. Moving to a contemporary system enables patient portals, online scheduling, and automated reminders.
- Future-Proof Compliance: Transitioning to a modern, certified EHR ensures the practice stays ahead of evolving ONC and MIPS requirements to protect the business from future audits.
Key Features That Drive Daily Clinical Usage in EHR Systems
Clinical velocity determines an ambulatory EHR’s success. Software that introduces friction will fail, regardless of its technical sophistication. High-performance systems fade into the background, allowing clinicians to focus on patients while the platform manages data capture. The architecture must prioritize speed and financial accuracy within a unified interface.
1. Fast Charting
Time is the most constrained resource in outpatient settings. Fast charting requires specialty-specific templates and macro-driven data entry to reduce manual typing. Systems like ModMed incorporate voice-to-text and AI-assisted scribing to document encounters in real time. Minimizing clicks prevents the after-hours charting crisis that drives physician burnout.
2. E-Prescription Workflows
Seamless e-prescribing is a non-negotiable requirement for modern care. This feature must integrate real-time prescription drug monitoring programs (PDMP) and automated drug interaction checks. Platforms like Athenahealth reduce manual errors and pharmacy callbacks. For patients, it ensures medications are ready for pickup immediately, improving treatment adherence.
3. Real-Time Patient Portal
The patient portal bridges the clinic and the consumer. It must provide immediate access to lab results and visit summaries to meet transparency expectations. Beyond data viewing, a high-value portal like the one offered by eClinicalWorks facilitates secure messaging and digital intake. Allowing patients to update history before an appointment saves minutes of clinical time.
4. Billing And Coding Automation
Profitability depends on the Clean Claim Rate. Automated billing features should suggest ICD-10 and CPT codes based on clinical documentation. By performing real-time scrubbing for errors before submission, systems like NextGen Healthcare minimize denials and accelerate the revenue cycle. This ensures accurate reimbursement without requiring a massive back-office team.
5. Appointment And Workflow Management
Effective management synchronizes the front desk, nursing station, and physician. Real-time tracking boards show exactly where each patient is in the visit process. Systems like Greenway Health use automated reminders to reduce no-show rates, which is critical for a predictable revenue stream. Integrated scheduling allows the practice to optimize staff resources for higher volumes.
How to Build a Certified EHR System for Ambulatory Care?
Building a certified ambulatory EHR system starts with clearly defined clinical workflows and a secure architecture that must align with standards like HIPAA and ONC requirements. The platform can then be carefully developed with interoperable modules and rigorously tested so it can reliably handle high-volume outpatient care and meet certification criteria.
Over the years, we have built numerous certified EHR systems for ambulatory care, and this is how we approach it.
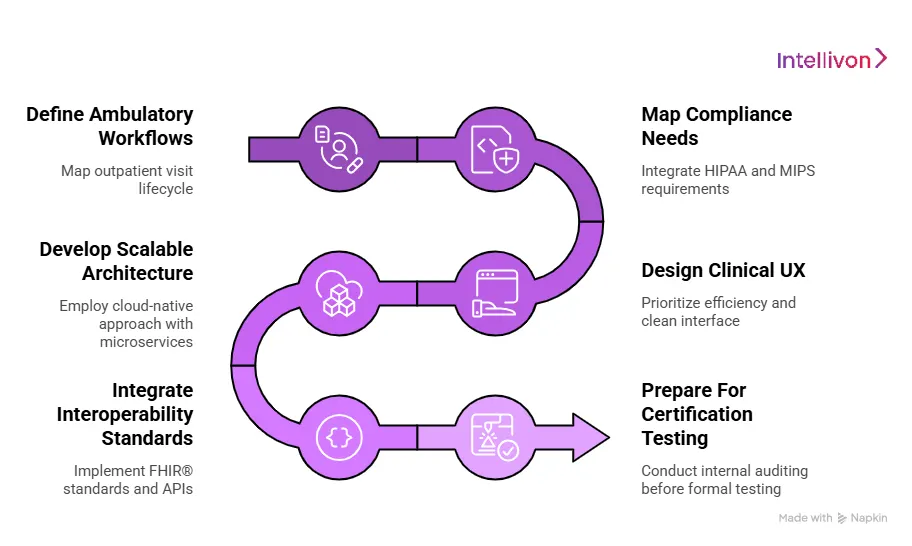
1. Define Ambulatory Workflows
We map the specific lifecycle of an outpatient visit, which differs significantly from inpatient stays. Our team analyzes every touchpoint, from the initial appointment request to post-visit follow-ups. By defining these journeys, we identify where automation can replace manual entry, such as pre-visit digital intake, reflecting the reality of a busy clinic.
2. Map Compliance Needs
We integrate compliance into the core codebase rather than treating it as an afterthought. We map technical requirements for HIPAA protection and the specific data capture points required for MIPS reporting. The system is architected to automatically track Quality measures without extra effort from the physician, preventing expensive mid-development pivots.
3. Design Clinical UX
Our UX philosophy centers on efficiency per click. In high-volume environments, every second saved during charting increases practice capacity. We prioritize a clean interface that surfaces relevant data, like allergies and medications, immediately. Taking inspiration from platforms like ModMed, we utilize touch-based interfaces that minimize cognitive load.
4. Develop Scalable Architecture
A robust architecture is essential as patient data grows. We employ a cloud-native approach with microservices, allowing the platform to scale horizontally across multiple locations. Security is multi-layered, featuring end-to-end encryption, multi-factor authentication, and automated audit logs. This allows for massive data volumes with near-constant uptime.
5. Integrate Interoperability Standards
Modern EHRs must be open ecosystems. We treat FHIR® standards and standardized APIs as mandatory for seamless exchange with labs, pharmacies, and hospitals. By building with an API-first mindset, we allow your clients to plug in third-party tools like Telehealth or AI diagnostics effortlessly. This is critical for ONC certification and market viability.
6. Prepare For Certification Testing
The final phase involves rigorous internal auditing before formal testing with an ONC-Authorized Testing Laboratory. We document the Safety-Enhanced Design and prove the system performs all required federal tasks. This preparation ensures the software meets the benchmarks for interoperability and clinical reliability required for a successful launch.
Cost Breakdown to Build an Ambulatory EHR System
Building an ambulatory EHR is a significant capital commitment, with costs scaling based on the complexity of your clinical workflows and the breadth of your interoperability requirements. As your development partner, we categorize these costs into distinct phases to ensure transparency and ROI.
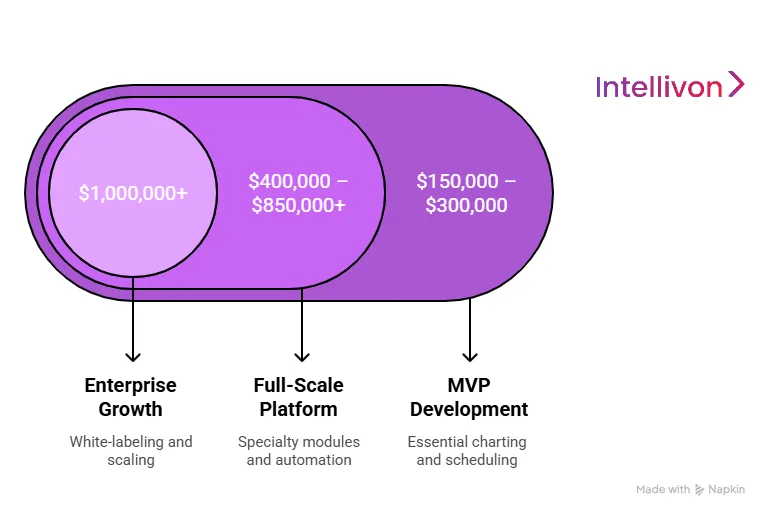
MVP Vs Full-Scale Costs
Launching a Minimum Viable Product allows you to enter the market quickly with essential charting and scheduling features. A Full-Scale Platform involves deeper specialty-specific modules and advanced automation.
| Phase | Estimated Cost Range | Focus Area |
| MVP Development | $150,000 – $300,000 | Core charting, HIPAA-compliant storage, and basic scheduling. |
| Full-Scale Platform | $400,000 – $850,000+ | Specialty templates, advanced analytics, and full billing suites. |
| Enterprise Growth | $1M+ | White-labeling capabilities, multi-site scaling, and AI integration. |
Starting with an MVP is the most efficient way to validate your user journey with real clinicians before committing to the high-cost features of a full-scale build.
Compliance And Certification Factors
Certification is a specialized expense that covers both technical development and administrative fees. To achieve ONC Certification, you must budget for the rigorous testing required to prove your system’s safety and reliability.
- Testing Fees: ONC-Authorized Testing Laboratories (ONC-ATLs) typically charge between $20,000 and $45,000 per certification cycle.
- Compliance Engineering: Budget $50,000 – $100,000 for the specific engineering hours required to build “Conditions and Maintenance of Certification” features, such as bulk data export and safety-enhanced design (UX) documentation.
- Maintenance: Expect to allocate 15% – 20% of your annual budget to stay current with evolving federal mandates and security patches.
Integration And API Costs
A modern EHR is only as good as its connection to the broader healthcare grid. Integrating with third-party vendors for labs, imaging, and prescriptions carries both upfront and recurring costs.
Investor Note: “Data liquidity is the new gold standard. While APIs add to the initial cost, they are the primary drivers of long-term platform value.”
- E-Prescribing (eRx): Integrating services like Surescripts often involves a setup fee of $5,000 – $10,000 plus monthly transaction or per-provider fees.
- Lab/Imaging Interfaces: Each direct connection to a lab (like Quest or Labcorp) can cost $2,000 – $7,000 in setup time, though using a hub like Redox can streamline these costs through a unified API subscription.
- Standardized APIs: Developing and maintaining FHIR®-ready gateways typically requires an initial investment of $30,000 – $60,000 to ensure your system can communicate with hospital registries and national data exchanges.
How Certification Impacts Your Ambulatory EHR ROI?
Building an ONC-certified ambulatory EHR is a strategic investment that directly influences a practice’s financial health. Certification acts as a catalyst for market adoption and long-term asset valuation by aligning technical capabilities with federal reimbursement requirements.
The return on investment for a certified EHR is realized through the capture of federal incentives and the avoidance of “information blocking” penalties. A certified system transforms from a basic administrative tool into a primary driver of clinic revenue.
1. Incentive Eligibility Via MIPS
The Merit-based Incentive Payment System is the primary vehicle for Medicare reimbursement adjustments. Only clinicians using Certified Electronic Health Record Technology are eligible to earn positive payment multipliers.
- Reimbursement Boost: High-performing practices using certified workflows can see a significant percentage increase in Medicare Part B payments.
- Automated Tracking: Systems built with “Promoting Interoperability” dashboards track MIPS categories in real-time. This ensures clinicians hit targets without manual audits.
- Market Positioning: Clinics using certified platforms attract higher-value payer contracts by demonstrating superior data maturity.
2. Non-Compliance Risks
Operating a non-certified system introduces liabilities that can erase operational profit. Federal oversight has shifted from encouragement to strict financial enforcement.
Risk Alert: Information Blocking civil monetary penalties can reach up to $1 million per violation.
| Risk Factor | Financial Impact | Cause |
| MIPS Penalties | -9% Reimbursement | Failure to use certified technology for reporting. |
| Audit Failures | Recoupment of Funds | Lack of HIPAA-compliant audit trails and logs. |
| Payer Exclusion | Network Loss | Private payers increasingly require ONC-certified systems for contracts. |
3. Value Of ONC-Certified Platforms
A certified EHR is a liquid asset. For founders planning an exit or sale, valuation depends heavily on certification status and the ability to exchange data seamlessly.
The long-term value lies in Interoperability. By adhering to FHIR® and ONC standards, a platform becomes part of a national health data grid. This connectivity makes the software more attractive to large hospital systems and private equity groups looking for integrated data engines. Certification ensures the software is a future-proofed asset rather than a stranded data silo.
What Clinics Actually Need in Daily Workflows?
High-volume outpatient clinics prioritize functional speed over feature density. In these environments, EHR systems must serve as a frictionless tool that keeps pace with a rapid clinical cadence rather than acting as an administrative hurdle.
Successful ambulatory systems prioritize “Time-to-Chart.” When a provider moves through a packed schedule, the interface must surface the right data at the right moment without requiring deep menu navigation.
Reducing Encounter Clicks
Every extra click is a second lost. Across 40 encounters, redundant clicking can add 30 minutes of administrative labor to a physician’s day.
- Smart Defaults: Fields auto-populate based on previous visits or common protocols.
- One-Screen Views: Systems like ModMed use a “single-pane-of-glass” approach to view history, vitals, and notes simultaneously.
- Macro-Driven Entry: Shorthand “dot phrases” allow for the instant insertion of complex clinical descriptions.
Handling 50+ Daily Patients
Efficiency at scale is the hallmark of a high-performing ambulatory center. When volume exceeds 50 patients per day, workflow bottlenecks become financial liabilities.
- Digital Intake: Patients complete their history via a mobile portal, cutting check-in time by 50%.
- Real-Time Tracking: A digital board shows the status of every exam room, identifying which patients are ready.
- Instant Discharge: Handouts and prescriptions trigger automatically upon note signing, clearing the room immediately.
Eliminating Documentation Errors
Manual errors are clinical risks and the primary cause of insurance denials. Documentation must be both rapid and precise to ensure audit safety.
Clinical Gold Standard: “The best documentation is generated as a byproduct of the care process, not as a separate data entry task.”
- Guardrails: Built-in logic prevents signing a note if mandatory MIPS data or coding requirements are missing.
- Specialty Templates: Orthopedic or cardiology-specific prompts ensure only relevant clinical data is captured.
- AI Scribing: Ambient listening tools capture the conversation and draft the note automatically, ensuring accuracy without manual typing.
How ONC Certification Shapes Product Architecture?
Certification is not a cosmetic layer added to finished software; it is the structural blueprint. Building EHR systems for the ambulatory market requires a “compliance-first” engineering mindset where every database schema and API call aligns with federal mandates.
The architectural integrity of an ambulatory platform determines its ability to pass federal audits and exchange data securely. Without these core structural elements, a system remains a localized database rather than a certified health IT module.
1. ONC Standards
The Office of the National Coordinator (ONC) sets the technical benchmarks for interoperability and patient safety. These standards dictate how data must be formatted and transmitted.
- USCDI Adoption: Systems must support the United States Core Data for Interoperability (USCDI) to ensure a standardized “data vocabulary.”
- FHIR® APIs: Modern architecture must prioritize HL7® FHIR® for real-time data exchange with external apps and researchers.
- Standardized Transitions: Architecture must support the seamless generation of Consolidated Clinical Document Architecture (C-CDA) files for patient referrals.
2. Audit And Reporting
A certified system must act as its own “black box” recorder. Transparency is a mandatory architectural requirement to prevent fraud and ensure data accountability.
Compliance Requirement: “Every access point, modification, and data export must be captured in a tamper-proof audit log.”
| Capability | Technical Implementation | Purpose |
| Audit Logs | Immutable database entries for every action. | Forensic tracking of breaches or record tampering. |
| CQM Calculation | Automated logic for Clinical Quality Measures. | Accurate reporting for federal reimbursement. |
| Data Export | Bulk EHI (Electronic Health Information) tools. | Ensuring patients move data without “blocking.” |
Export to Sheets
3. Design From Day One
Attempting to “bolt on” certification features to a legacy codebase is a recipe for technical debt. High-performing systems are engineered with certification in the initial sprint.
The Development Workflow:
- Identity Management: Implement Multi-Factor Authentication and Role-Based Access Control at the kernel level.
- Safety-Enhanced Design: Conduct formal “User Centered Design” testing during wireframing to identify clinical error risks early.
- Encapsulated Logic: Keep certification-specific code modular so it can be updated as federal requirements evolve without breaking core features.
How to Design for High-Volume Patient Flow in EHR Systems?
Designing for high-volume patient flow requires EHR systems to move at the speed of thought. In a busy ambulatory environment, the software must act as a clinical accelerator rather than a data entry bottleneck.
The primary goal of an ambulatory interface is to reduce the cognitive load on the clinician. When a doctor is seeing a new patient every 15 minutes, the system must present the most critical data, such as allergies, active meds, and the chief complaint, without requiring a single scroll.
Rapid Input UI Patterns
Standard web forms are too slow for clinical use. High-volume systems like ModMed utilize specialized UI patterns designed for “heads-up” charting, where the doctor stays engaged with the patient while documenting.
- Dynamic Checklists: Instead of typing, clinicians use specialty-specific “Pick Lists” that adapt based on the diagnosis.
- Touch-Optimized Flowcharts: Visual body maps allow a provider to tap an area to instantly pull up relevant exam templates.
- Persistent Patient Headers: Critical safety data remains “sticky” at the top of the screen across all modules to prevent errors during rapid context switching.
Minimizing Encounter Time
Efficiency is found in the seconds saved between the waiting room and the final signature. By optimizing the “digital path” of a patient, a clinic can increase its daily capacity without hiring additional staff.
| Workflow Stage | Efficiency Optimization | Time Saved (Avg) |
| Pre-Visit | Patient-driven digital intake via mobile. | 5 to 8 Minutes |
| Exam | Voice-to-text ambient AI scribing. | 4 to 6 Minutes |
| Post-Visit | Auto-calculated E/M coding suggestions. | 2 to 3 Minutes |
Workflow Automation
Repetitive tasks are the primary cause of physician burnout and clinical delays. Automation should target the “invisible” administrative work that happens behind the scenes of every visit.
Efficiency Rule: “If a clinician has to perform the same sequence of three clicks more than five times a day, those clicks should be replaced by a single automated trigger.”
- Smart Orders: Entering a diagnosis like “Strep Throat” should automatically queue the lab order, the antibiotic prescription, and the patient education handout.
- Result Routing: Normal lab results should be automatically pushed to the patient portal with a pre-written physician note, requiring only a one-tap approval.
- Task Escalation: If a critical lab result is not reviewed within a set timeframe, the system should automatically alert the nursing station or the on-call provider.
Why Choose Intellivon for Certified EHR Systems?
Partnering with Intellivon ensures that your vision for a high-performance medical platform is built on elite engineering and deep domain expertise. We transform complex clinical requirements into seamless EHR systems that clinicians actually prefer to use.
Intellivon provides the technical bridge between healthcare concepts and market-ready clinical assets. With over 500,000 hours of coding experience, our team of ex-MAANG/FAANG developers applies the same rigorous standards found at the world’s leading tech giants to the healthcare space.
Built For ONC Compliance
Compliance is hard-coded into the initial sprint. Every platform is designed to meet the Office of the National Coordinator standards from day one. This proactive engineering ensures your system is ready for certification without the need for expensive, late-stage refactoring.
Secure And Scalable Platforms
Our development team leverages its background at top-tier tech firms to build inherently secure and scalable architectures. We utilize cloud-native microservices and multi-layered encryption to protect data as your user base grows. This structural integrity allows for massive data volumes with 99.9% uptime.
Faster Time-To-Market
Intellivon accelerates your launch by utilizing a library of healthcare-ready modules. Instead of building every basic component from scratch, we focus our 500,000 hours of expertise on your unique value propositions. This modular approach significantly reduces development timelines while maintaining the highest quality standards.
Conclusion
Building a certified EHR system for ambulatory care requires a precise blend of clinical insight and high-tier engineering. By prioritizing ONC standards and high-velocity workflows from the very first sprint, a platform transitions from a simple data repository to a high-value clinical asset. This “compliance-by-design” approach not only secures federal incentive eligibility but also creates a scalable, interoperable foundation that drives long-term practice profitability and market valuation.
FAQs
Q1: What are the 4 types of EMR?
A1: Electronic Medical Record systems are generally categorized by their deployment and functional focus. These include Cloud-Based EMRs for remote access, On-Premise EMRs hosted on local servers, Specialty-Specific EMRs tailored for niche fields like pediatrics, and Mental Health EMRs designed with unique privacy features.
Q2: How to develop an EHR system?
A2: Developing EHR systems begins with mapping clinical workflows and regulatory requirements. The process involves designing a high-speed UI, building a secure cloud-native architecture, and integrating interoperability standards like FHIR®. Finally, the system undergoes rigorous testing and an official audit by an ONC-Authorized Testing Laboratory to meet federal mandates.
Q3: What is a certified EHR system?
A3: A certified EHR is a platform officially validated by the Office of the National Coordinator to meet specific technological and security standards. This certification ensures the system securely exchanges data, protects patient privacy, and accurately reports clinical quality measures. Use of certified technology is mandatory for healthcare providers to qualify for federal incentive programs.
Q4: What are the 4 types of records?
A4: In a clinical setting, data is organized into four core types: Administrative Records for demographics and insurance, Clinical Records containing physician notes and vitals, Legal Records including informed consent and HIPAA authorizations, and Financial Records for billing and claims. Integrating these into a unified digital interface is essential for any high-functioning ambulatory practice.