Disconnected health systems lose money every day. This is because when a hospital network runs different EHR systems in each department, its staff spend more time fixing data than using it. At the same time, clinicians have to track down records, billing teams type in the same information over and over, and compliance checks turn into last-minute scrambles. For large organizations, this kind of fragmentation brings big financial and regulatory risks.
An EHR integration solution can solve these problems by connecting clinical systems, billing, labs, pharmacies, and third-party apps through one reliable data pipeline. Instead of records being stuck in separate systems, everyone can see up-to-date patient information in real time, all in one place. The results are clear: less manual work, quicker care, easier compliance, and a setup that can grow with the organization.
Intellivon has helped many healthcare organizations build EHR integration solutions that turn scattered, costly systems into connected, high-performing infrastructure. This blog walks through the key steps to building an EHR integration platform, from planning the architecture to putting it into action in an enterprise-grade system.
Why EHR Integration Fails in Real Systems
Building an EHR integration solution often hits walls because real-world healthcare environments are messy. While the theory of data exchange is simple, the execution frequently fails due to debt and a lack of unified standards.
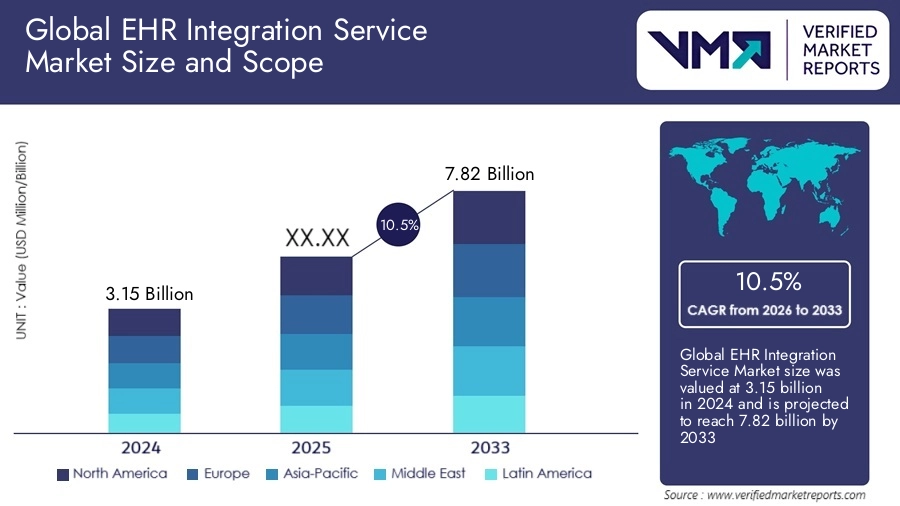
Understanding these specific friction points is the first step toward building a platform that truly scales. The EHR integration services market is valued at USD 3.15 billion in 2024. It is projected to reach USD 7.82 billion by 2033, growing at a CAGR of 10.5% from 2026 to 2033.
1. Fragmented Systems Break Care Workflows
Most healthcare environments operate on a patchwork of disconnected software. When an integration does not account for a clinician’s actual movement, it adds clicks instead of removing them.
Fragmented data forces users to jump between screens, causing fatigue and slowing patient throughput.
2. Inconsistent Data Creates Clinical Risks
Data quality is the silent killer of health tech projects. When information enters an EHR from multiple sources, it often lacks a common format.
This inconsistency leads to mapping errors that can compromise patient safety. Investors must prioritize data normalization to ensure the platform remains a reliable asset rather than a liability.
3. Legacy APIs Limit Interoperability
Many older EHRs rely on outdated protocols never meant for modern cloud connectivity. These interfaces lack the speed and security required for real-time exchange, creating bottlenecks.
Modern solutions must wrap these systems in agile layers like FHIR to ensure the platform can handle high traffic without performance drops.
4. Compliance gaps delay deployment
Healthcare is heavily regulated, and security oversights lead to massive fines. Many projects fail because they treat compliance as an afterthought.
If a platform cannot prove its security credentials immediately, enterprise partners will walk away, stalling the route to market and ROI.
In summary, these hurdles represent the gap between a generic tool and a high-value enterprise asset. Solving for legacy bottlenecks transforms a technical challenge into a competitive market advantage.
Types of EHR Systems and Integration Complexity
Selecting the right architecture for an EHR integration solution depends heavily on the existing infrastructure of your target provider networks.
Enterprise leaders must evaluate these systems not just as databases, but as the primary environment where their capital will operate. Understanding these technical landscapes is vital for any investor looking to build a scalable and profitable platform.
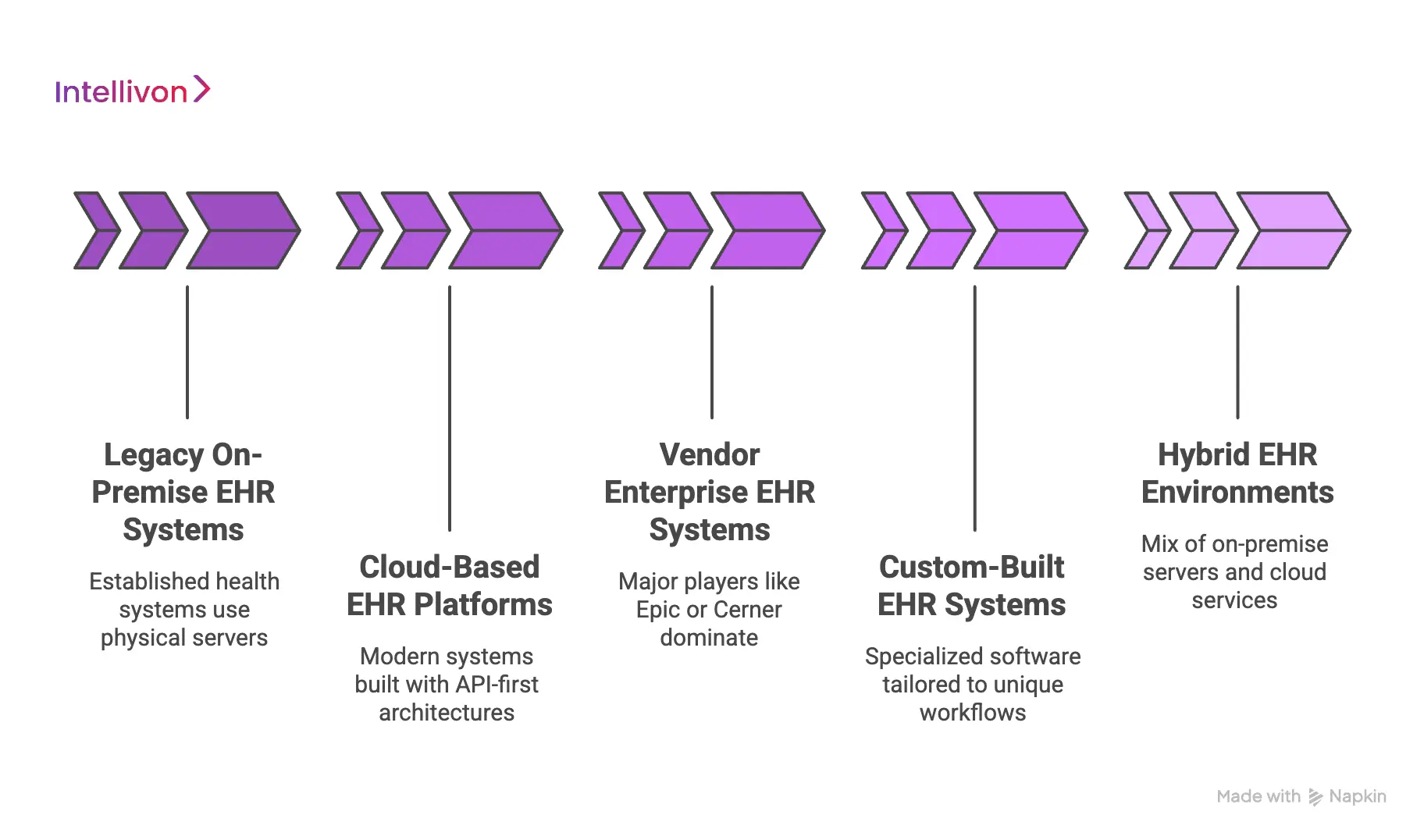
1. Legacy on-premise EHR systems
Many established health systems still house their data on physical servers located within their own facilities. A prime example of an on-premise system that still anchors large-scale healthcare is VistA (Veterans Health Information Systems and Technology Architecture).
Developed by the U.S. Department of Veterans Affairs (VA), VistA is one of the most widely deployed EHR systems in the world. These legacy environments are often the most difficult to integrate because they lack modern, web-ready connection points.
Consequently, they usually require custom VPN tunnels and specialized “bridge” software to function. While this complexity increases initial development costs, it also offers a high barrier to entry for competitors.
2. Cloud-based EHR platforms
Cloud-native systems represent the gold standard for modern healthcare interoperability. These platforms are built with API-first architectures, making it much easier to synchronize data in real-time.
Because they utilize standard web protocols, the deployment timeline for an EHR integration solution is significantly shorter. Investors typically see a faster ROI when targeting enterprises that have already migrated to the cloud.
3. Vendor enterprise EHR systems
Major market players like Epic or Cerner dominate the large-scale health system landscape. These vendors operate within proprietary ecosystems that have very strict “walled garden” access rules.
While they provide robust developer toolsets, gaining entry into their official marketplaces requires rigorous vetting and compliance audits. However, a successful integration here provides immediate access to thousands of high-value enterprise users.
4. Custom-built EHR systems
Some specialized clinics or academic research institutions use bespoke software tailored to unique clinical workflows. These systems rarely follow industry-standard data schemas, which makes automated data exchange quite challenging.
However, they offer a niche opportunity for high-margin strategic partnerships and specialized integration services. Building a bridge for these systems requires a highly flexible and intelligent data mapping engine.
5. Hybrid EHR environments
In many cases, a large medical group might use a mix of on-premise servers for imaging and cloud services for patient records. Managing this hybrid flow is where the most significant technical and strategic challenges lie.
A successful platform must be able to pull data from multiple disparate sources and present it as a single, coherent record. This specific versatility is exactly what enterprise decision-makers look for in a long-term technology partner.
In summary, the diversity of EHR hosting models dictates the complexity of your technical roadmap and total cost of ownership. Navigating these various architectures effectively is what separates a basic application from a resilient, enterprise-grade solution.
Popular EHR Systems and Integration Approach
For an enterprise leader, the choice of an EHR integration solution often feels like navigating a series of high-walled gardens. Each major vendor has its own rules for data access, its own security protocols, and its own pricing model for third-party developers.
To build a truly scalable platform, your strategy must account for these vendor-specific nuances while maintaining a lean technical footprint.
Popular EHR Systems vs Integration Approach
| EHR System | API Framework | Integration Method | Complexity | Key Constraint | Best Strategy |
| Epic | FHIR + Interconnect | Connection Hub access + HL7/FHIR | High | Strict vendor approval | Use certified APIs + plan longer onboarding |
| Cerner | FHIR (Ignite APIs) | SMART on FHIR + REST APIs | Medium | Structured onboarding | Build FHIR-first, workflow-embedded apps |
| Allscripts | FHIR + Proprietary APIs | Developer program APIs | Medium | Data governance needs | Focus on billing + ambulatory workflows |
| MEDITECH | HL7 + FHIR (Expanse) | REST + middleware bridging | High | Legacy system limitations | Use middleware + hybrid integration |
| Athenahealth | REST APIs (MDP) | OAuth + cloud APIs | Low | Platform dependency | Fast API integration + rapid deployment |
1. Epic systems integration approach
Epic is the dominant force in the large-scale health system market, known for its “App Orchard” (now rebranded as Connection Hub).
Integrating with Epic usually requires a high degree of compliance and a significant upfront investment in vetting.
They primarily use a mix of FHIR APIs and their own proprietary Interconnect server. For an investor, an Epic integration is the “holy grail” because it unlocks access to the most prestigious medical centers in the world.
2. Cerner integration approach
Now part of the Oracle ecosystem, Cerner (Oracle Health) has traditionally been more open than some of its competitors.
They leverage the “Cerner Ignite” APIs, which are heavily focused on the HL7 FHIR standard. This makes Cerner a favorite for developers looking to build cross-platform tools quickly.
The integration approach here focuses on “pluggable” apps that can live directly inside the clinician’s existing workflow without forcing them to switch screens.
3. Allscripts integration approach
Allscripts (now Veradigm) has a long history of supporting open architecture through its Developer Program. They offer a robust set of proprietary APIs alongside standard FHIR resources.
Because Allscripts is often found in mid-market physician groups, the integration approach here is typically focused on ambulatory care and billing efficiency. This makes it a strategic target for platforms looking to optimize the financial side of a healthcare enterprise.
4. MEDITECH integration approach
MEDITECH is a staple in community hospitals and regional networks. Their Greenfield workspace provides the tools needed to build RESTful API connections. While older versions of MEDITECH can be difficult to navigate, their newer Expanse platform is built for modern web interoperability.
Integrating here requires a deep understanding of how community hospitals manage patient throughput with limited IT resources.
5. Athenahealth integration approach
Athenahealth is a cloud-native pioneer, making it one of the most developer-friendly systems on this list. Their “More Disruption Please” (MDP) program provides a clear, well-documented path for API integration.
Because Athenahealth manages the back-end hosting for all its clients, you don’t have to worry about individual hospital firewalls. This lower technical friction leads to a much faster “go-to-market” timeline for your EHR integration solution.
Why multi-EHR needs a unified layer
In a real-world enterprise environment, you will rarely deal with just one vendor. A large health system might use Epic for its hospitals and Athenahealth for its outpatient clinics. If you build separate “point-to-point” integrations for each, your code becomes a tangled mess that is impossible to maintain. This technical debt will eventually eat your margins and stall your ability to scale.
The solution is to build a unified middleware layer, which is a single engine that speaks every EHR language and translates it into one clean format for your app.
This “universal translator” approach allows you to add new EHR connections in weeks rather than months. For an entrepreneur, this is the ultimate competitive advantage, which is the ability to promise a client that your platform works with everything they already own.
Core Components of an EHR Integration System
Building an enterprise-grade EHR integration solution requires more than just a simple connection.
You must build a robust infrastructure that can handle the massive scale and high stakes of healthcare data. For investors, these components represent the “moat” that protects the platform from technical failure and security breaches.
1. API gateway for data exchange
The API gateway acts as the secure front door for all data moving in and out of the system. It manages traffic, enforces rate limits, and ensures that only authorized requests reach the core database.
This layer is essential for preventing system overloads and protecting against cyber threats. A well-designed gateway allows the platform to scale to millions of patient records without a drop in performance.
2. HL7 and FHIR interoperability layers
To talk to a diverse provider network, your system must speak multiple “languages.” Older systems still rely on HL7 v2, while modern platforms use the RESTful FHIR standard.
Having dedicated layers for both ensures that your solution is backward-compatible with legacy tech and future-proofed for the cloud. This versatility is a major selling point for enterprise leaders who manage hybrid environments.
3. Data mapping and normalization engine
Data rarely looks the same across different EHR vendors. A normalization engine acts as a universal translator, converting disparate data points into a single, clean format.
This process is critical for clinical accuracy and high-level analytics. Without it, the data remains a “digital landfill” that is impossible for decision-makers to use effectively.
4. Event-driven real-time sync system
Healthcare takes place in real-time. This is why an event-driven architecture ensures that when a doctor updates a chart, the integration reflects that change instantly.
This “push” notification model is far more efficient than traditional polling methods. It reduces server load and ensures that clinicians always have the most current information at their fingertips.
5. Identity and access management layer
Security is the cornerstone of any EHR integration solution. A robust identity layer manages “who sees what” using industry standards like OAuth 2.0 and OpenID Connect.
This ensures that only the right people have access to sensitive patient data, which is a non-negotiable requirement for HIPAA compliance. For a business leader, this layer is the primary defense against catastrophic data leaks.
In summary, these core components are the building blocks of a resilient healthcare platform. By investing in this high-level architecture, you ensure your solution can handle the complexity of the modern medical landscape.
Let’s move on to the step-by-step process of building an EHR-integration solution for large healthcare enterprises.
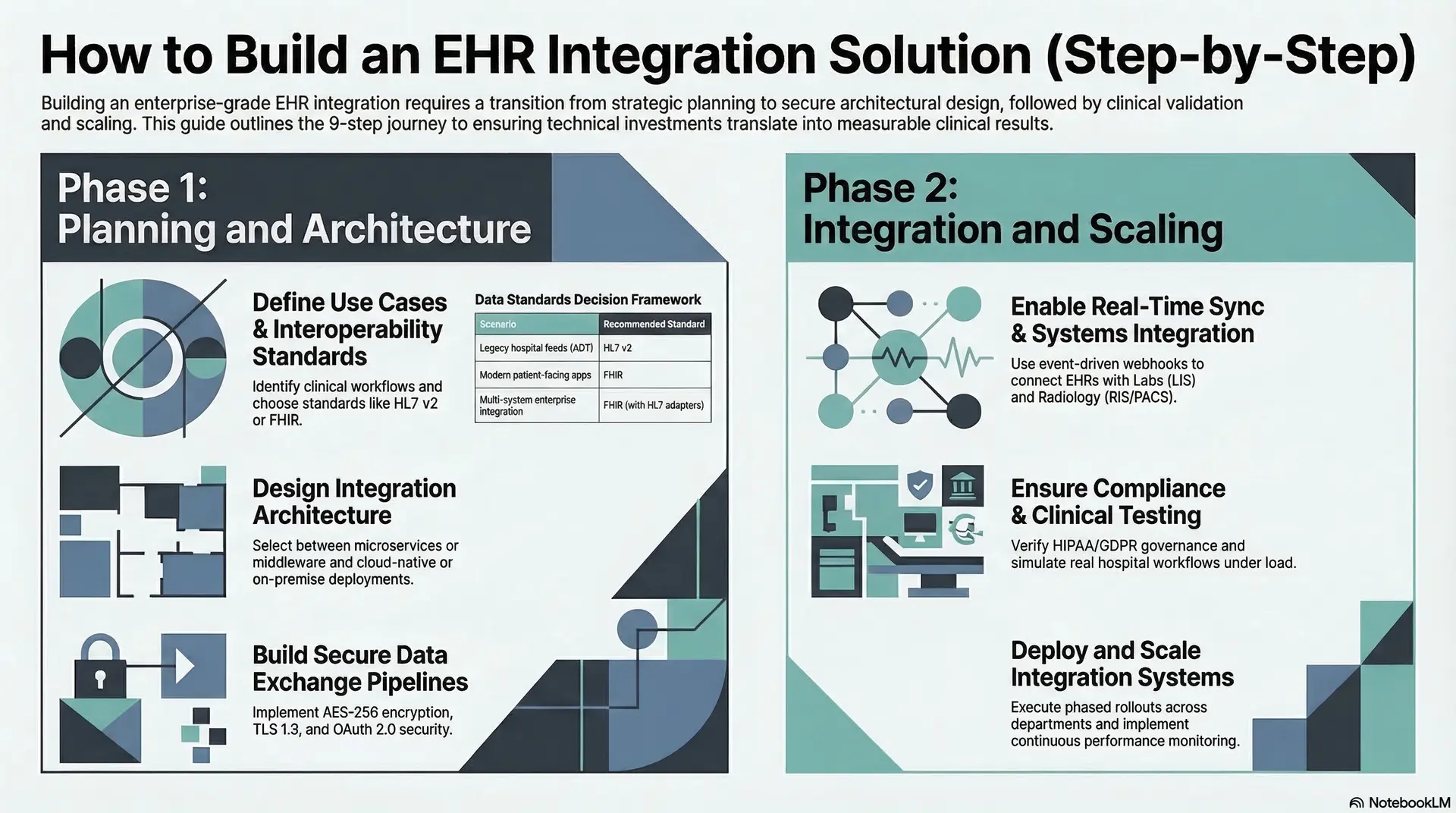
Step 1: Define Integration Use Cases First
Strategic planning begins with identifying exactly how your data will move to generate the highest ROI. For enterprise leaders, this stage is about ensuring technical investments translate into measurable clinical and financial results.
This is where Intellivon excels, helping you bridge the gap between high-level vision and technical execution.
1. Identify clinical workflows to prioritize
We begin by pinpointing high-friction areas like patient intake or automated pharmacy orders. Intellivon’s strategists focus on these specific tasks to deliver immediate, visible value to your provider network.
2. Map systems and data sources
Our team audits your existing landscape, from legacy on-premise servers to modern cloud platforms. By knowing exactly where your data lives, we prevent the costly architectural shifts that often plague less experienced developers.
3. Define high-impact integration points
We identify the specific nodes where data exchange creates the most efficiency. Our experts prioritize points that reduce manual entry and minimize clinical errors, directly protecting your bottom line.
4. Align with patient journey flows
The integration must mirror the actual patient experience. We ensure data moves seamlessly from the initial appointment booking through to final billing, creating a frictionless journey for both the patient and the provider.
Step 2: Choose Interoperability Standards
Selecting a data standard is a decision about long-term technical debt and market reach. Choosing the wrong framework can lock an enterprise into a rigid infrastructure that becomes increasingly expensive to maintain.
1. HL7 vs FHIR: when to use each
Leverage HL7 v2 for high-volume, legacy hospital feeds such as ADT (Admission, Discharge, Transfer) messages. Conversely, utilize FHIR for modern patient-facing apps and cloud-based analytics where granular data access is a priority.
When to Use HL7 vs FHIR in Practice
| Scenario | Recommended Standard |
| Integrating legacy hospital systems | HL7 |
| Building new healthcare platforms | FHIR |
| Real-time patient data exchange | FHIR |
| Batch data processing workflows | HL7 |
| Multi-system enterprise integration | FHIR (with HL7 adapters) |
| Vendor systems with HL7 dependency | HL7 + middleware |
2. Designing FHIR-first APIs for scale
A FHIR-first architecture ensures your platform remains modular. This approach allows Intellivon to build systems that integrate easily with third-party AI tools and emerging digital health ecosystems without requiring a full backend rewrite.
3. Handling legacy system compatibility
Many large-scale health networks still operate on-premise servers that do not support modern APIs. We deploy secure translation layers to wrap these legacy systems, ensuring they can communicate with your modern cloud environment without compromising security.
4. Data transformation strategies
Data integrity is paramount during the translation between HL7 and FHIR. Intellivon implements strict mapping protocols to ensure that clinical data remains accurate and actionable, regardless of the source system’s age or complexity.
In summary, your choice of standards dictates the speed of your deployment and the agility of your platform. By aligning these choices with your specific business goals, you ensure the integration serves as a scalable asset rather than a technical bottleneck.
Step 3: Design Integration Architecture
The architecture of an EHR integration solution serves as the definitive blueprint for long-term reliability. A poorly designed foundation creates a cycle of frequent downtime and mounting maintenance costs.
Therefore, selecting a structure that aligns with high-level scaling requirements is a prerequisite for any viable enterprise deployment.
1. Microservices vs middleware architecture
A microservices approach allows for independent modules, ensuring that updates to one service do not jeopardize the entire system’s stability. While middleware offers initial simplicity, it often becomes a single point of failure as the provider network expands.
| Factor | Microservices Architecture | Middleware Architecture |
| Core Model | Independent services for each function | Central integration layer connects systems |
| Best For | Large-scale, evolving enterprise platforms | Faster integration across mixed systems |
| Scalability | High, each service scales independently | Moderate, scaling depends on middleware capacity |
| Flexibility | High, easier to add or update services | Lower changes can affect shared workflows |
| Maintenance | Easier in modular environments | Simpler early on, harder over time |
| Failure Risk | Isolated service failures | Middleware can become a bottleneck |
| Development Speed | Slower initial setup | Faster initial rollout |
| Integration Complexity | Higher upfront architecture effort | Easier for early-stage interoperability |
| Long-Term Fit | Better for complex, growing ecosystems | Better for limited or mid-scale integrations |
| Best Choice When | You need resilience and future scale | You need faster deployment across many systems |
2. Cloud-native vs on-prem deployment
Modern strategies favor cloud-native elasticity, yet some networks require on-premise components for data sovereignty. Intellivon specializes in hybrid deployments that balance cloud agility with physical security mandates.
| Factor | Cloud-Native Deployment | On-Prem Deployment |
| Core Model | Hosted in cloud infrastructure | Hosted within the hospital data center |
| Best For | Scalable, multi-site healthcare platforms | Highly regulated environments with strict control |
| Scalability | High, supports rapid expansion | Limited by local infrastructure capacity |
| Deployment Speed | Faster | Slower |
| Upfront Cost | Lower infrastructure investment | Higher hardware and setup cost |
| Maintenance | Managed through cloud operations | Managed internally by IT teams |
| Security Control | Strong, but shared responsibility | Highest direct infrastructure control |
| Compliance Fit | Good for most modern frameworks | Better for strict data residency needs |
| Disaster Recovery | Easier to automate | More complex and expensive |
| Best Choice When | You need agility and a faster rollout | You need local control and fixed infrastructure |
3. Real-time vs batch processing models
Real-time processing is non-negotiable for clinical alerts where seconds define outcomes. Conversely, batch processing remains more efficient for administrative overhead like insurance eligibility checks or end-of-day financial reporting.
| Factor | Real-Time Processing | Batch Processing |
| Core Model | Data moves instantly as events happen | Data moves in scheduled intervals |
| Best For | Clinical alerts, patient monitoring, care coordination | Billing, reporting, eligibility checks |
| Speed | Immediate | Delayed |
| Clinical Relevance | High | Low for urgent workflows |
| Operational Efficiency | Best for live decisions | Best for repetitive back-office tasks |
| Infrastructure Demand | Higher | Lower |
| Complexity | Higher event orchestration needed | Easier to manage |
| Error Handling | Needs instant recovery logic | Easier to review in bulk |
| Cost Impact | Higher due to always-on systems | Lower for non-urgent workflows |
| Best Choice When | Timing directly affects outcomes | Timing is less critical than efficiency |
4. High availability and fault tolerance
System downtime is a clinical risk, not just a technical inconvenience. The architecture must include redundant clusters and automated failover to guarantee 99.99% uptime. Intellivon ensures critical information remains accessible even during unexpected outages.
Step 4: Build Secure Data Exchange Pipelines
Establishing a secure pipeline is a non-negotiable prerequisite for any enterprise-grade EHR integration. Beyond simple encryption, these pipelines must be engineered to withstand rigorous security audits and protect against evolving cyber threats that target high-value clinical data.
1. Encryption for healthcare data transfer
Data must remain unreadable to unauthorized entities at every stage of its journey. This requires a dual-layered approach to protection:
- Data at Rest: All clinical assets stored within your databases must utilize AES-256 encryption.
- Data in Transit: Every data exchange between the EHR and your platform must be secured via TLS 1.3.
2. Role-based access and identity control
Identity management ensures that data access is restricted to the absolute minimum required for a specific task. Intellivon implements granular permissions that align with actual clinical roles:
- Clinician Access: Full view of patient charts and medication history.
- Administrative Access: Restricted to billing and scheduling data without exposing sensitive health records.
3. API security and authentication
The API is the most vulnerable point of any integration and requires a “zero-trust” security architecture. We leverage industry-standard protocols to validate every single request:
- OAuth 2.0: For secure, token-based authorization that never exposes user credentials.
- OpenID Connect: To provide a robust identity layer on top of authorization protocols.
4. Logging and monitoring for compliance
Automated audit trails are the backbone of regulatory transparency. To satisfy HIPAA and GDPR mandates, every interaction with the data must be recorded and monitored in real-time:
- Detailed Audit Logs: Capturing who accessed the data, what was viewed, and when.
- Anomaly Detection: Intellivon integrates monitoring tools that alert your team to suspicious access patterns before they become breaches.
In summary, these secure pipelines act as the defensive perimeter for your clinical ecosystem. By prioritizing these security layers, you ensure your platform is as resilient as it is compliant.
Step 5: Enable Real-Time Clinical Data Sync
Reliable data synchronization is the heartbeat of clinical operations. Without it, practitioners risk making decisions based on outdated information. Therefore, ensuring your EHR integration solution handles data velocity with precision is a primary technical mandate.
1. Event-driven architecture for updates
Rather than inefficient polling, an event-driven model uses webhooks to trigger instant updates. This ensures that a patient’s vital signs or lab results are mirrored across the enterprise the moment they are recorded.
2. Handling data conflicts across systems
When multiple sources update a single record simultaneously, conflicts occur. Intellivon implements “source of truth” hierarchies and timestamping to resolve these overlaps automatically, preventing data corruption.
3. Ensuring data accuracy and consistency
Maintaining a single, coherent patient record requires strict validation rules. We utilize automated checksums and schema validation to ensure that data remains identical across every connected node in the provider network.
4. Reducing latency in clinical systems
Latency can stall critical workflows. By optimizing API calls and utilizing edge caching, Intellivon minimizes the delay between data entry and visibility, ensuring a high-performance experience for frontline clinicians.
In summary, real-time synchronization transforms a static database into a dynamic clinical asset. By prioritizing low latency and conflict resolution, you ensure your platform remains a trusted tool in high-stakes environments.
Step 6: Integrate Hospital Systems and Apps
An EHR does not exist in a vacuum; it is the central nervous system of a much larger technical body. To create a truly indispensable platform, you must ensure it communicates fluently with every ancillary system in the provider network.
This level of deep integration is what transforms a simple record-keeper into a comprehensive operational engine.
1. Integrating EHR with lab systems (LIS)
Laboratory data is the primary driver of clinical decision-making. Fast, bi-directional communication ensures that orders and results move without manual intervention:
- Order Automation: Electronic orders are sent directly from the EHR to the lab, reducing transcription errors.
- Real-Time Result Ingestion: As soon as a lab technician verifies a result, it populates the patient’s chart and triggers a notification for the clinician.
2. Connecting radiology systems (RIS/PACS)
Imaging files are massive and require specialized handling to remain accessible within a standard clinical workflow. Intellivon focuses on high-bandwidth connectivity for seamless viewing:
- PACS Bridging: Linking the Picture Archiving and Communication System (PACS) allows doctors to view high-resolution X-rays or MRIs directly within the patient’s record.
- Diagnostic Metadata: Beyond just the image, we sync the radiologist’s notes and findings to ensure the full clinical context is preserved.
3. Linking billing and claims systems
The financial health of an enterprise depends on the accuracy of its coding and billing cycles. Integration here ensures that clinical actions are immediately translated into revenue:
- Automated Charge Capture: Every procedure or consultation recorded in the EHR automatically generates a corresponding billing charge.
- Claims Scrubbing: By validating data against insurance rules before submission, Intellivon helps reduce claim denials and accelerates the reimbursement cycle.
4. Syncing patient portals and apps
Modern healthcare is increasingly patient-centric. Providing individuals with direct access to their own data improves engagement and health outcomes:
- Secure Data Mirroring: Patients can view their latest lab results, medication lists, and appointment schedules via mobile apps in real-time.
- Interactive Scheduling: Integration allows patients to book or reschedule visits directly, with the changes reflecting instantly in the provider’s master calendar.
In summary, these auxiliary integrations are what provide the “last mile” of value for an enterprise. By connecting these disparate systems, Intellivon creates a unified ecosystem that optimizes both clinical care and administrative efficiency.
Step 7: Ensure Compliance and Governance
In the healthcare sector, compliance is the ultimate gatekeeper of market entry. For those looking to scale an EHR integration solution, governance is a core component of the brand’s value.
1. HIPAA and GDPR compliance requirements
Adhering to global standards ensures that your platform can operate across borders and within the strictest regulatory environments. Intellivon treats these requirements as architectural foundations rather than checklists:
- Administrative Safeguards: Establishing clear policies for who can manage and access PHI (Protected Health Information).
- Technical Protections: Implementing the robust encryption and secure transmission protocols we established in previous steps to satisfy both US and EU mandates.
2. Audit trails and governance frameworks
Transparency is the only defense during a regulatory review. You must be able to reconstruct the history of every data point within your system to prove integrity:
- Granular Logging: Every instance of data access, modification, or transmission is timestamped and attributed to a specific user or system ID.
- Immutable Records: We ensure that audit logs cannot be altered or deleted, providing a “gold standard” of truth for internal and external auditors.
3. Managing patient consent systems
As data flows more freely, the complexity of managing who has “opted in” increases significantly. A centralized consent engine is necessary to respect patient autonomy while maintaining data utility:
- Dynamic Consent: Allowing patients to grant or revoke access to specific parts of their record (e.g., sharing lab results but not mental health notes).
- Automated Enforcement: Intellivon integrates these preferences directly into the API layer, so unauthorized data is automatically filtered out before it leaves the source system.
4. Risk management in integrations
Every new connection point in a provider network introduces a potential vulnerability. Managing this risk requires a proactive, “security-first” mindset:
- Vulnerability Scanning: Regularly testing the integration pipelines for weaknesses or outdated dependencies.
- Incident Response: Having a pre-defined, automated plan to isolate affected systems and notify stakeholders the moment a potential threat is detected.
Step 8: Test in Real Clinical Environments
A solution that works in a controlled lab setting often falters when introduced to the high-pressure reality of a hospital floor. Testing is a rigorous validation of the platform’s clinical and operational resilience.
For an enterprise, the cost of a “live” failure far outweighs the investment in comprehensive, real-world simulation.
1. Simulating real hospital workflows
A static data test cannot replicate the chaos of a busy emergency department or a high-volume outpatient clinic. We must simulate the actual sequence of events a clinician follows:
- Workflow Continuity: Testing how data flows from an initial triage note to a pharmacy order without requiring the user to refresh their screen.
- Edge Case Scenarios: Intellivon stresses the system by simulating “noisy” environments with overlapping data entries and interrupted network connections.
2. Data validation and error handling
In healthcare, an “error” is more than a technical bug; it is a potential threat to patient safety. The integration must be intelligent enough to catch and flag data inconsistencies:
- Schema Enforcement: Ensuring that a heart rate value from an external monitor correctly maps to the EHR’s specific data field.
- Graceful Degradation: If a connection to a specific lab system drops, Intellivon ensures the rest of the platform remains functional while providing clear, actionable error alerts to the staff.
3. Performance testing under load
An EHR integration solution must maintain its speed even during peak hours when thousands of users are active. Latency during a critical procedure is unacceptable:
- Concurrency Testing: Simulating thousands of simultaneous API calls to identify potential bottlenecks in the data pipeline.
- Stress Resilience: Determining the exact “breaking point” of the infrastructure to ensure that auto-scaling mechanisms trigger before a performance lag occurs.
4. User testing with clinical teams
The ultimate judge of an integration’s success is the person using it at the point of care. If a tool is too complex, it will be ignored or bypassed:
- Usability Audits: Observing doctors and nurses as they interact with the integrated data to identify “click fatigue” or confusing UI elements.
- Feedback Loops: Intellivon incorporates direct clinical feedback to refine the interface, ensuring the technology serves the workflow rather than dictating it.
Step 9: Deploy and Scale Integration Systems
Scaling an EHR integration solution requires a transition from a validated pilot to an enterprise-wide infrastructure. A disciplined rollout ensures that connectivity expands without compromising the stability of existing clinical operations.
1. Phased rollout across departments
Launching in high-impact areas like Radiology allows for early stabilization. Intellivon uses these phases to refine data flows before expanding to the broader network.
2. Scaling across hospital networks
Horizontal scaling requires standardized templates to manage diverse legacy configurations. We ensure centralized oversight while distributing data across multiple facility nodes.
3. Monitoring system performance
Continuous observation is mandatory to maintain peak health. Intellivon implements real-time dashboards to track latency and resolve bottlenecks before they impact frontline clinicians.
4. Continuous optimization strategy
A static integration quickly becomes obsolete as regulations evolve. We provide iterative updates to ensure your platform remains a high-performance clinical asset.
Key EHR Integration Challenges and Our Solutions
Identifying the technical barriers to a seamless EHR integration solution is only half the battle. For enterprise leaders, the real value lies in how those obstacles are systematically dismantled. Intellivon approaches these challenges with a dual focus on engineering excellence and clinical operational stability.
1. Legacy systems lack modern APIs
Many established provider networks still operate on-premise systems that do not support RESTful APIs or modern web protocols. This creates a massive “data wall” that blocks real-time connectivity.
Our Solution: We deploy custom-built middleware “wrappers” that translate legacy HL7 v2 messages into modern FHIR resources. This allows your platform to communicate with decades-old infrastructure without requiring a full system overhaul.
2. Data inconsistency across systems
A “blood pressure” reading in one system might be coded differently in another, leading to fragmented patient records and dangerous clinical blind spots.
Our Solution: Intellivon utilizes an AI-driven normalization engine that maps disparate data points to a universal schema. This ensures that, regardless of the source, the data remains consistent and clinically actionable across the entire enterprise.
3. Real-time sync challenges
Traditional “polling” methods, where a system checks for updates every few minutes, create latency that can be life-threatening in emergency care settings.
Our Solution: We implement an event-driven architecture using high-performance webhooks. This ensures that as soon as a clinician saves a note, the integration triggers an instantaneous update across all connected platforms.
4. Security and compliance risks
Moving sensitive PHI across networks increases the surface area for cyberattacks and regulatory fines, especially when dealing with multiple third-party vendors.
Our Solution: Intellivon builds “zero-trust” pipelines featuring end-to-end AES-256 encryption and multi-factor authentication. We provide automated, immutable audit logs that make HIPAA and GDPR compliance a baseline standard rather than a constant worry.
5. Multi-system integration complexity
Enterprises often struggle to manage a “spaghetti” of point-to-point connections between EHRs, labs, and billing software, which becomes impossible to maintain as they scale.
Our Solution: We replace fragmented connections with a unified integration hub. This single-entry architecture allows you to add or remove systems without disrupting the core workflow, significantly reducing your long-term technical debt.
6. Performance issues at scale
As a provider network grows, the sheer volume of data can cause API timeouts and system lag, frustrating frontline clinicians and slowing down patient care.
Our Solution: Our infrastructure is built on cloud-native auto-scaling clusters. Intellivon optimizes query performance and utilizes edge caching to ensure that the system remains responsive, even when handling millions of concurrent patient records.
In summary, these solutions represent a shift from reactive troubleshooting to proactive infrastructure building. By addressing these core challenges at the architectural level, Intellivon ensures your integration remains a high-performance asset rather than a liability.
Conclusion
Building an enterprise-grade EHR integration solution is a high-stakes investment in your organization’s digital future. Success requires a transition from fragmented legacy tools to a unified, scalable data infrastructure. By prioritizing security, real-time synchronization, and clinical workflow alignment, you transform technical complexity into a definitive market advantage.
Intellivon provides the elite engineering expertise needed to navigate these healthcare landscapes. We help you build resilient systems that drive operational growth and superior patient outcomes.
Build an EHR Integration Solution with Intellivon
At Intellivon, EHR integration platforms are built as enterprise healthcare infrastructure, not as connectors layered onto fragmented systems. The goal is to create a unified integration layer that enables real-time data exchange, aligned clinical workflows, and scalable interoperability across healthcare ecosystems.
Our solutions integrate seamlessly with leading EHR systems like Epic, Cerner, MEDITECH, and Athenahealth, using HL7, FHIR, and API-driven architectures. This allows healthcare organizations to unify patient data, modernize integrations, and scale without disrupting existing systems or compliance requirements.
Why Partner With Intellivon?
- Governance-First Integration Architecture: Designed with audit trails, role-based access, and compliance controls to meet HIPAA, GDPR, and enterprise healthcare standards.
- Multi-EHR Integration Expertise: Proven capability to integrate across vendor ecosystems, including Epic, Cerner, and hybrid hospital environments.
- Scalable, Cloud-Native Infrastructure: Built to support multi-hospital networks, high patient volumes, and real-time clinical data exchange.
- End-to-End Development and Deployment: From architecture design to system integration, testing, and scaling, we manage the entire lifecycle.
Get a detailed cost breakdown and architecture roadmap tailored to your healthcare systems. Connect with Intellivon’s experts today.
FAQs
Q1. What is EHR integration in healthcare?
A1. EHR integration connects electronic health record systems with other hospital applications to enable seamless data exchange. It ensures clinicians have access to accurate, real-time patient data across systems, improving care coordination and operational efficiency.
Q2. How long does EHR integration take?
A2. EHR integration typically takes 3 to 9 months, depending on system complexity, number of integrations, and compliance requirements. Multi-hospital or legacy-heavy environments may take longer due to customization and testing needs.
Q3. What systems need integration?
A3. EHR systems often integrate with lab systems (LIS), radiology systems (RIS/PACS), billing and claims platforms, patient portals, wearable devices, and third-party healthcare applications to ensure unified workflows.
Q4. What technologies power integration?
A4. EHR integration is powered by HL7, FHIR, REST APIs, middleware platforms, cloud infrastructure, and event-driven architectures. These technologies enable secure, real-time, and scalable data exchange across healthcare systems.
Q5. How much does EHR integration cost?
A5. EHR integration typically costs between $40,000 and $150,000+, depending on system complexity, number of integrations, architecture design, and compliance requirements. Large enterprise deployments may exceed this range.