The healthcare technology landscape moves quickly. In 2026, EHR systems will not be built the same way they were just three years ago. The underlying structure has changed, compliance requirements have become stricter, and expectations from clinical and administrative teams have shifted significantly. Organizations that treat EHR development like a standard software project are already lagging behind.
Creating a modern EHR in 2026 means designing for interoperability from the start, integrating compliance into the infrastructure instead of adding it later, and considering AI-driven clinical workflows that leading health systems are already implementing at scale. The difference between a functional EHR and a strategic one is where many enterprises lose time, budget, and competitive edge.
Intellivon has spent years providing enterprise health technology for organizations in high-stakes clinical settings. This blog covers the full extent of our expertise in building these platforms from the ground up.
Why Most EHR Projects Fail Before Deployment
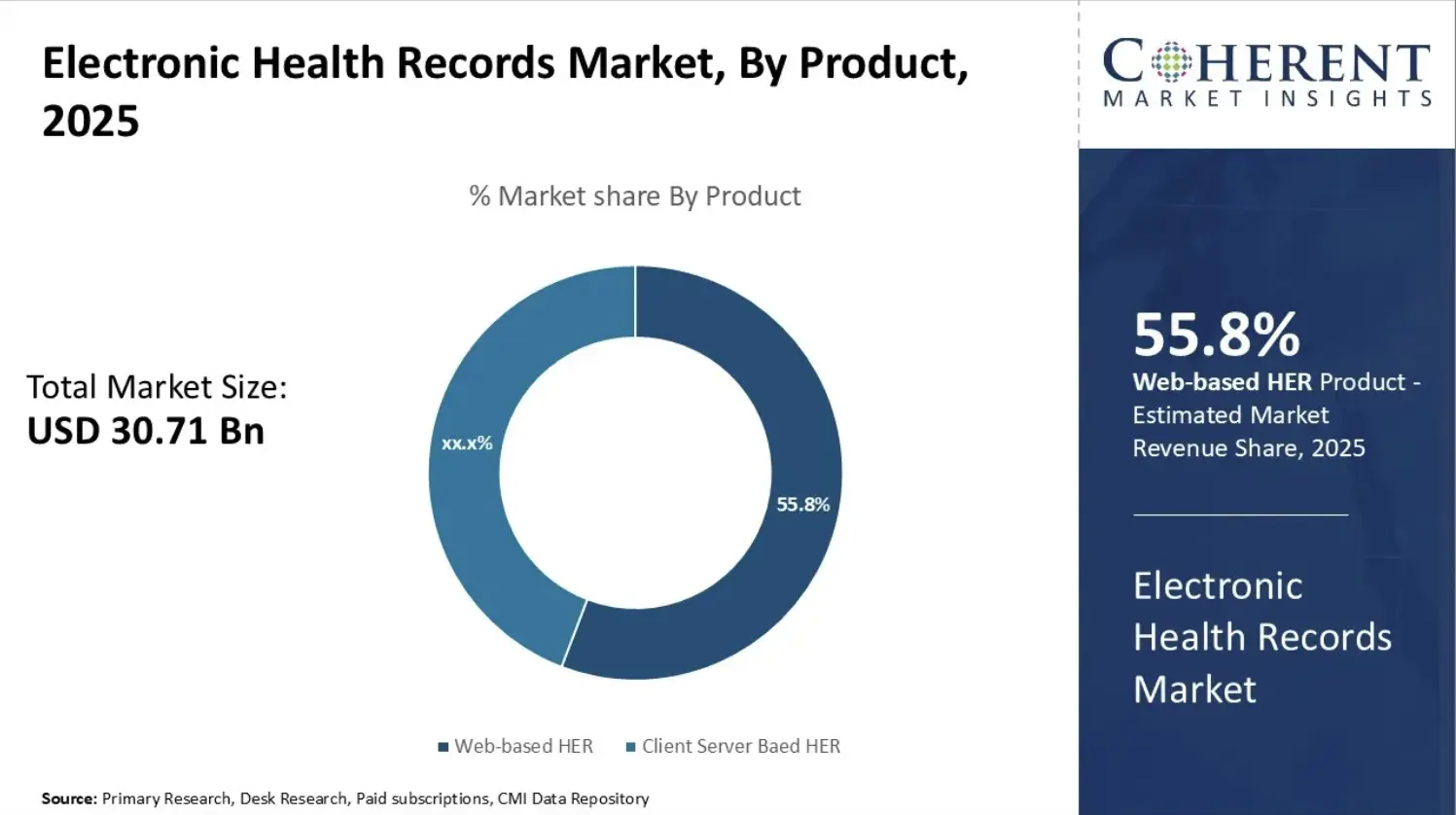
EHR projects fail before or around deployment because of weak governance, misaligned expectations, workflow conflicts, and poor change management. At the same time, the EHR market continues to grow rapidly. This growth is driven by digitization mandates, cloud adoption, and AI-powered analytics.
This reflects a steady CAGR of around 8–10%. As a result, the market continues to expand at a consistent pace, driven by long-term healthcare digitization and system modernization efforts.
To build a resilient platform in 2026, you must move beyond basic software development and focus on high-stakes clinical infrastructure.
1. Building Software instead of Clinical Infrastructure
An EHR is not just a database. It is the central nervous system of a medical facility. Development fails when teams treat it like a standard SaaS product. Sustainable systems require a foundation that handles extreme data loads.
Therefore, your technical architecture must support life-critical reliability. It must ensure zero downtime during peak hours.
2. Ignoring Workflow Realities
Clinicians are already battling burnout from excessive documentation. New platforms often fail because they add clicks instead of removing them. If a tool disrupts a patient’s exam, the staff will eventually bypass it.
Success depends on shadowing real-world clinical paths. This ensures the technology acts as a silent assistant rather than a digital hurdle.
3. Underestimating Integration Complexity
Modern healthcare relies on a massive web of legacy software. Most projects stall when they realize how difficult it is to sync data. Specifically, labs and pharmacies often use incompatible formats.
Real-world expertise is necessary to navigate these communication gaps. Without a robust strategy for interoperability, your platform becomes an isolated island of data.
4. Treating Compliance as a Checklist
Data privacy is often handled as a late-stage hurdle. This reactive approach leads to massive security vulnerabilities.
In 2026, security must be baked into every layer of the system. True clinical integrity comes from building a “security-first” environment. This protects both patient trust and your capital investment simultaneously.
Building a platform that survives the pilot phase requires a shift in perspective. It is about creating a tool that doctors actually want to use every day.
The Shift From EHR Software to Clinical Infrastructure
Modern healthcare systems are moving beyond simple digital filing cabinets. In the past, leaders viewed Electronic Health Records (EHR) as isolated software applications. However, in 2026, the industry has pivoted toward seeing the EHR as foundational clinical infrastructure.
This shift is essential for organizations that want to maintain a competitive edge. Investors must recognize that building “just an app” is no longer a viable business strategy.
1. EHR as the system of record vs system of action
Historically, EHRs served primarily as a “system of record” to store patient history for billing. Today, the market demands a “system of action” that actively guides clinical decisions. A system of action uses live data to suggest the next best step for a patient’s care.
Consequently, clinicians no longer have to hunt for information across different tabs. Instead, the platform pushes relevant insights directly into their workflow. This transition transforms the EHR from a passive archive into an active participant in healthcare delivery.
2. Why disconnected tools break care delivery speed
Fragmented tools create digital friction that slows down every department in a hospital. When a nurse must log into three different systems to verify a lab result, patient safety is at risk.
Specifically, disconnected communication leads to treatment delays and increased staff burnout. Research shows that over 60% of healthcare organizations experience downtime due to these connectivity gaps.
Therefore, your investment must prioritize a unified ecosystem. A truly integrated platform eliminates the “context switching” that drains productivity and revenue.
3. Moving from data storage to real-time orchestration
Storing data is easy, but orchestrating it in real-time is the true technical challenge of 2026. Real-time orchestration involves synchronizing data, AI insights, and human actions across the entire enterprise.
For example, an orchestration engine can automatically update a surgeon’s schedule when a pre-op lab comes back abnormal. This moves the organization from reactive task-masking to proactive outcome coordination. By building an event-driven architecture, you ensure the system responds to clinical changes the moment they happen.
What enterprises actually expect from EHR in 2026
Decision-makers now look for platforms that offer “clinical autonomy” through agentic AI. They expect a system that doesn’t just show data but also automates multi-step administrative tasks. Specifically, the EHR must handle prior authorizations and complex scheduling without manual intervention.
In addition, the infrastructure must be cloud-native to support massive, unpredictable data loads. Security is a fundamental expectation of the architecture. Ultimately, leaders want a platform that scales with their growth without requiring a total rebuild.
Investing in clinical infrastructure is a long-term strategy for operational excellence. It ensures that your technology remains a growth enabler rather than a technical debt burden.
Critical Decisions That Define ROI Of EHR Systems
Investing in an EHR system requires more than a technical roadmap; it demands a clear financial strategy. Many organizations fail because they do not define their return on investment early enough. Consequently, the project becomes a cost center instead of a revenue driver.
Strategic decision-makers must evaluate data ownership and architecture before the first line of code is written. These choices ultimately determine the platform’s long-term market value.
1. Patient data owners across your ecosystem
Data sovereignty is the most significant financial hurdle in modern healthcare. You must decide if the platform, the provider, or the patient holds the ultimate rights to the information. In 2026, shifting regulations favor patient-centric data control.
Therefore, your system must support granular consent management to remain compliant. Clear data governance ensures that information remains a liquid asset rather than a liability.
2. Centralized vs distributed clinical data models
Choosing between centralized and distributed models changes everything about your system’s speed. Centralized models offer high performance but create a single point of failure. In contrast, distributed models enhance security across multiple locations.
Specifically, a hybrid approach often works best for large-scale enterprises. This allows for fast local access while maintaining a secure, global record.
3. Build vs extend vs replace existing systems
The “rip and replace” method is often the most expensive path an enterprise can take. Sometimes, it is more efficient to extend a legacy system using modern API layers.
However, if the tech stack is too old, extending it may only delay a collapse. You must conduct a rigorous audit before making this choice. Often, building a new system is cheaper in the long run than patching outdated code.
4. Defining success metrics beyond “go-live”
Launching the software is only the beginning of the journey. Many leaders mistakenly view “go-live” as the finish line. Instead, you should measure success through clinician adoption and patient outcome improvements.
For instance, a successful EHR should reduce administrative charting by at least 30%. In addition, look for a measurable decrease in billing cycle times to justify the capital expenditure.
Ultimately, ROI in 2026 stems from strategic clarity rather than just code. Prioritizing modular architecture ensures your clinical infrastructure appreciates in value over time.
Architecture Decisions That Make or Break EHR Systems
Technical architecture is the silent engine of financial performance in modern healthcare. Strategic leaders must prioritize structural flexibility to avoid the massive technical debt common in legacy healthcare ecosystems.
1. Why API-first EHR platforms outperform
Legacy systems often fail because they lack the ability to communicate with external medical tools. In contrast, an API-first approach treats every data point as a bridge rather than an island. This architecture allows your platform to integrate instantly with third-party labs, wearables, and pharmacies.
Consequently, your system becomes a central hub that grows in value as the digital health market expands. Therefore, prioritizing open connectivity ensures your infrastructure remains relevant and highly scalable.
2. Microservices vs modular monoliths
Choosing between microservices and a modular monolith is a high-stakes decision for any healthcare enterprise. Microservices offer unparalleled scalability but increase the complexity of data synchronization. However, a modular monolith can provide a more stable environment for smaller clinical deployments.
Specifically, large-scale systems often benefit from microservices to handle high-traffic surges during peak clinical hours. You must balance the need for rapid updates against the maintenance costs of a highly distributed system.
3. Designing for interoperability from day one
Interoperability is no longer an optional feature; it is a regulatory and operational mandate. Most developers treat data sharing as an afterthought, which leads to fragmented patient records. In 2026, building on FHIR (Fast Healthcare Interoperability Resources) standards is the only way to ensure future-proofing.
Therefore, your architecture must support seamless data exchange across different hospital networks. This proactive design prevents the “data silos” that typically frustrate clinicians and delay patient care delivery.
4. Real-time vs batch clinical data flows
Healthcare decisions often depend on seconds, making the speed of data flow a critical ROI factor. Batch processing is efficient for billing, but it is dangerous for real-time clinical monitoring.
Specifically, an EHR in 2026 must utilize event-driven architecture to update patient vitals instantly. In addition, real-time flows allow for immediate AI-driven alerts that can save lives in intensive care units.
Choosing a hybrid model ensures your system handles both massive administrative loads and urgent clinical needs.
Superior architecture creates a platform that is both robust and adaptable. By making these structural choices early, you ensure your clinical infrastructure can pivot as the market evolves.
Designing Architecture Around Clinical Workflows
Software succeeds or fails based on its adoption by frontline medical staff. Strategic leaders must ensure the architecture mirrors the high-pressure reality of a hospital floor to avoid expensive deployment pushback.
1. Mapping real doctor and nurse workflows
Generic software design often collapses when it meets the chaotic pace of an emergency department. Consequently, your development team must shadow clinicians to understand the nuances of a shift.
Specifically, a nurse’s workflow differs significantly from a surgeon’s, requiring distinct data views. Therefore, mapping these unique journeys ensures the platform supports, rather than hinders, care delivery.
2. Reducing clicks and cognitive load in UI
Excessive clicks are the primary driver of physician burnout and data entry errors. In 2026, a high-performance EHR must prioritize a “minimalist” interface that surfaces only the most relevant data.
Specifically, using predictive search and smart defaults can cut documentation time by half. Reducing cognitive load allows clinicians to focus on the patient instead of the screen.
3. Handling exceptions, not just ideal workflows
Most EHR projects fail because they only design for the “perfect” patient encounter. However, clinical medicine is defined by interruptions, emergencies, and missing data. Your architecture must allow for rapid context switching without losing progress on a digital chart.
Therefore, building a robust “autosave” and “draft” logic is essential for maintaining data integrity during a crisis.
4. Aligning EHR flows with care delivery timelines
Timing is everything in healthcare, yet many systems suffer from latent data updates. An effective EHR must synchronize with the actual speed of a clinical consultation.
For example, lab results should trigger immediate notifications rather than waiting for a manual refresh. In addition, aligning digital inputs with the physical exam prevents the system from becoming a distraction.
Workflow-centric design transforms a cold database into a vital clinical tool. Prioritizing the human element ensures your infrastructure investment delivers both clinical and financial returns.
Ensuring Integration In EHR Systems
A siloed EHR is a liability that limits both clinical outcomes and financial growth. Successful deployment in 2026 requires a cohesive integration strategy that bridges the gap between disconnected medical touchpoints.
1. Unifying diagnostic and pharmacy networks
Fragmented data from external labs and pharmacies often creates dangerous delays in patient care. An integrated EHR must utilize bidirectional interfaces to sync prescriptions and test results in real-time.
Specifically, using FHIR-based APIs ensures that diagnostic data is immediately actionable for the physician. Consequently, this connectivity eliminates manual data entry and reduces the risk of medication errors across the provider network.
2. Syncing insurance and financial workflows
Revenue cycle management fails when clinical data does not communicate with billing systems. You must ensure that every clinical action triggers a corresponding administrative update for insurance claims.
Specifically, automated eligibility verification at the point of care prevents costly claim denials later in the cycle.
Therefore, a synchronized financial pipeline accelerates the “time-to-payment” and stabilizes the organization’s cash flow.
3. Streaming wearable and remote data
Remote patient monitoring (RPM) is no longer a niche feature; it is a standard expectation for modern chronic care. Your architecture must handle high-velocity data streams from consumer and medical-grade wearables.
In contrast to static records, these pipelines provide a continuous view of patient health between office visits. Therefore, building scalable ingestion layers allows your system to alert clinicians to red flags before they become emergencies.
4. Connecting legacy systems with zero downtime
Replacing a legacy hospital system is a high-stakes operation that cannot afford service interruptions. A “wrapper” strategy allows you to build modern layers over old databases while gradually migrating data.
Specifically, using a robust integration engine helps translate old message formats into modern digital standards without crashing the core system. This phased approach ensures continuous care delivery while you modernize the underlying clinical infrastructure.
Strategic integration transforms a standalone tool into a comprehensive healthcare ecosystem. By prioritizing connectivity, you ensure your platform remains the central hub for all clinical and financial activity.
Data Layer Strategy: The Hidden Backbone of EHR
A system’s long-term viability depends entirely on how it handles the massive influx of clinical information. Strategic leaders must prioritize a data architecture that remains flexible enough to evolve with shifting medical regulations.
1. Structuring patient data for long-term scalability
Scaling a healthcare platform requires a database that grows without sacrificing retrieval speed or accuracy. Consequently, you should avoid rigid table structures that break when new clinical fields are added. Specifically, a document-oriented approach often allows for more fluid updates to patient histories.
Therefore, building a “schema-light” foundation ensures your system handles thousands of concurrent users without performance degradation.
2. FHIR vs custom schemas
Custom schemas offer total control, but they often lead to expensive “integration debt” later. In contrast, adopting Fast Healthcare Interoperability Resources (FHIR) provides a universal language for medical data.
Using standardized resources ensures your platform communicates effortlessly with external hospital networks. Therefore, while custom builds might seem faster initially, FHIR-first strategies offer a much higher long-term ROI for the enterprise.
3. Real-time data pipelines vs delayed sync systems
Delayed synchronization creates a “data lag” that can lead to outdated clinical decisions and administrative errors. Real-time pipelines ensure that a lab result or a vitals update is visible across the entire organization instantly.
Specifically, utilizing message brokers like Kafka allows for the seamless streaming of high-velocity medical data. In addition, this real-time visibility is essential for triggering automated AI alerts that improve patient safety.
4. Building a single source of truth
Fragmented records are a major source of clinician frustration and redundant medical testing. You must implement a Master Patient Index (MPI) to resolve identity conflicts across different departments.
Specifically, a single source of truth ensures that a patient’s medication list is identical in the ER and the pharmacy. Consequently, this unified view protects the organization from liability while providing a superior experience for both staff and patients.
A robust data layer is the difference between a legacy burden and a scalable clinical asset. By prioritizing structural integrity now, you ensure your infrastructure remains a reliable foundation for decades.
Compliance, Security, and Risk Is Built Into the Core
Security is not a final layer to be added; it is a fundamental property of high-value clinical infrastructure. Investors must prioritize a “secure-by-design” philosophy to protect both patient trust and their financial capital.
1. Designing HIPAA-ready systems
Compliance fails when it is treated as a manual checklist after development is complete. Consequently, your architecture should utilize “encryption-at-rest” and “encryption-in-transit” as default settings for all medical data. Specifically, isolating Protected Health Information (PHI) in a secure, hardened vault reduces the overall attack surface.
Therefore, building compliance into the data layer ensures that your platform meets federal standards without constant manual auditing.
2. Role-based access and audit trails in EHR
Unauthorized access is a major liability that can lead to massive regulatory fines and reputational damage. You must implement a strict Role-Based Access Control (RBAC) model to ensure clinicians only see the data they need.
Specifically, every interaction with a patient record must be logged in an immutable, timestamped audit trail. In addition, this transparency allows your organization to quickly identify and mitigate potential internal security threats.
3. Managing cross-border healthcare data regulations
Expanding a healthcare platform globally requires navigating a complex web of regional privacy laws. For example, GDPR in Europe has much stricter data residency requirements than standard US regulations. Specifically, your infrastructure must support “data localization” to store patient records within specific geographic boundaries.
Therefore, building a flexible regulatory engine allows your enterprise to scale into new markets without a total system redesign.
4. Preventing breaches in distributed care environments
Modern healthcare often takes place outside the traditional hospital walls, increasing the risk of data leaks. You must secure every endpoint, from a doctor’s tablet to a patient’s home monitoring device.
Specifically, utilizing a “Zero Trust” architecture ensures that every connection is verified before any data is exchanged. Consequently, this multi-layered defense protects the integrity of the clinical record even in highly decentralized treatment environments.
Building a secure core is the ultimate insurance policy for your healthcare technology investment. Prioritizing risk management ensures your clinical infrastructure remains a trusted asset in an increasingly hostile digital landscape.
Step-by-Step: How Intellivon Builds EHR Platforms
Executing a high-stakes clinical migration requires a partner that balances technical precision with operational reality. At Intellivon, we utilize a battle-tested framework to transform your vision into a scalable, revenue-generating asset.
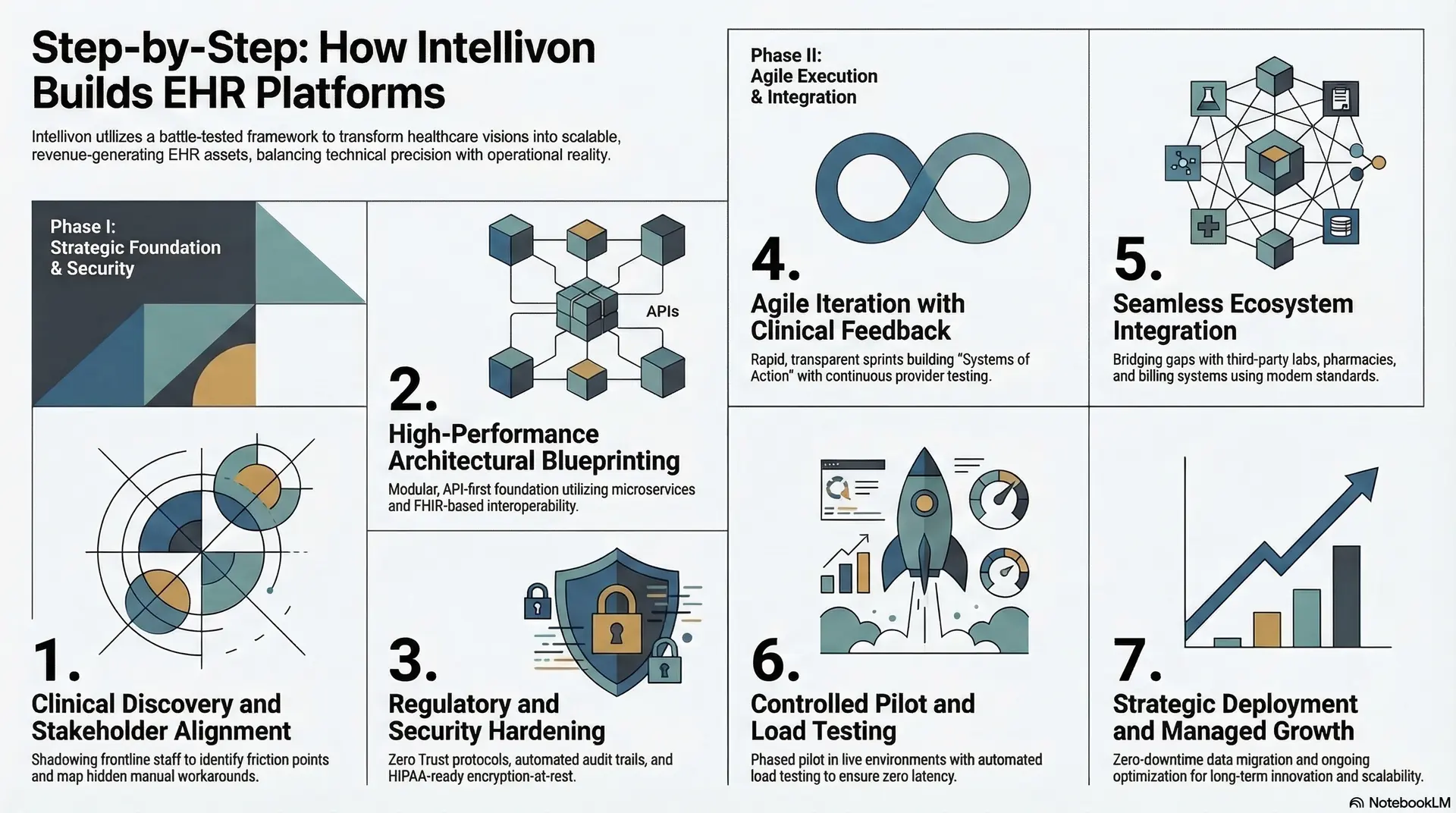
1. Clinical Discovery and Stakeholder Alignment
We begin by shadowing your frontline medical staff to identify the specific friction points in their daily routines. Specifically, we map the “hidden” manual workarounds that often bypass traditional software.
This discovery phase ensures that our technical roadmap is grounded in real-world clinical needs. Therefore, we align every feature with your organization’s broader operational goals from day one.
2. High-Performance Architectural Blueprinting
Our engineers design a modular, API-first foundation that prioritizes long-term data liquidity over short-term shortcuts. In contrast to rigid legacy builds, we utilize microservices to ensure your platform scales horizontally during peak traffic.
We bake FHIR-based interoperability into the core to prevent future integration debt. This blueprint serves as the structural “source of truth” for the entire development lifecycle.
3. Regulatory and Security Hardening
Security is treated as a foundational element rather than a late-stage compliance checklist. Consequently, we implement “Zero Trust” protocols and automated audit trails at the database level.
Our team configures HIPAA-ready encryption-at-rest to protect your most sensitive patient assets. Therefore, your platform remains resilient against both external cyber threats and internal data mismanagement.
4. Agile Iteration with Clinical Feedback
Development occurs in rapid, transparent sprints that allow for continuous testing by actual healthcare providers. We prioritize building “Systems of Action” that reduce the number of clicks required for routine documentation.
Specifically, this iterative loop identifies potential usability hurdles before they become expensive deployment blockers. Consequently, the final product feels like a silent assistant rather than a digital burden.
5. Seamless Ecosystem Integration
We bridge the gap between your new EHR and existing third-party labs, pharmacies, and billing systems. Our integration engines translate legacy HL7 messages into modern digital standards without disrupting ongoing care delivery.
We also ensure that financial workflows are synchronized to prevent revenue leakage during the transition. Therefore, your system becomes a unified hub for all clinical and administrative data.
6. Controlled Pilot and Load Testing
Before full-scale deployment, we execute a phased pilot in a live environment to monitor system performance under stress. We utilize automated load testing to ensure zero latency during high-volume data ingestion.
Specifically, our team monitors the “Time-to-Task” metrics to verify that the UI actually improves staff productivity. This final validation ensures the infrastructure is ready for the rigors of a 24/7 medical facility.
7. Strategic Deployment and Managed Growth
We oversee the “go-live” process with a focus on zero-downtime data migration and comprehensive staff training. Instead of viewing deployment as the end, we provide ongoing optimization to ensure the platform evolves with your needs.
We also monitor clinical outcome data to prove the ROI of your technology investment. Ultimately, we remain your long-term strategic partner for healthcare innovation and scalability.
Following a structured, expert-led process is the only way to ensure a successful EHR rollout in 2026. This disciplined approach guarantees that your investment remains both clinically effective and financially sound.
Cost to Develop an EHR System in 2026
At Intellivon, EHR systems are built as clinical infrastructure platforms, not feature-based applications. Therefore, even within a $50,000–$150,000 range, the focus remains on workflow alignment, integration readiness, and scalable architecture.
As a result, costs depend on how well the system is designed to support real clinical operations, not just how many features are included.
Estimated Phase-Wise Cost Breakdown
| Phase | Description | Estimated Cost Range (USD) |
| Discovery & Workflow Mapping | Define clinical workflows, user roles, and system scope | $5,000 – $10,000 |
| Architecture & Data Design | Design scalable structure, APIs, and patient data models | $8,000 – $20,000 |
| UI/UX for Clinical Use | Build intuitive interfaces aligned with care workflows | $5,000 – $15,000 |
| Core EHR Development | Develop patient records, scheduling, and clinical modules | $15,000 – $40,000 |
| Basic Integrations | Connect essential systems like labs or billing platforms | $8,000 – $25,000 |
| Security & Compliance Setup | Implement encryption, access control, and audit logs | $4,000 – $10,000 |
| Testing & QA | Ensure system reliability, performance, and usability | $3,000 – $10,000 |
| Deployment & Setup | Cloud deployment and initial infrastructure configuration | $2,000 – $8,000 |
Total Estimated Cost Range
- Lean EHR MVP: $50,000 – $80,000
- Operational Clinical System: $80,000 – $120,000
- Advanced Scalable EHR: $120,000 – $150,000
What You Get in This Budget Range (Real Clarity)
- Core patient record management
- Workflow-based scheduling and documentation
- Limited but critical integrations (labs, billing)
- Secure and compliant data handling
- Scalable architecture foundation for future expansion
What Is Typically Out of Scope at This Budget
- Deep multi-system integrations across large hospital networks
- Advanced AI diagnostics or predictive analytics
- Multi-location enterprise orchestration layers
- Complex real-time data pipelines at scale
Planning an EHR within a $50K–$150K budget? Talk to Intellivon’s experts to design a system that scales without costly rebuilds.
Conclusion
Developing an EHR system in 2026 is a strategic investment in the future of healthcare delivery. Success requires moving beyond static data storage and embracing a dynamic “System of Action.” Consequently, by prioritizing FHIR-native architecture and clinical workflow integration, you ensure long-term scalability and significant ROI. Therefore, the goal is to build a platform that empowers clinicians rather than one that adds to their documentation burden.
Ultimately, navigating this complex landscape requires a partner with deep technical and clinical expertise. Intellivon provides cutting-edge, enterprise-grade AI solutions specifically designed to modernize healthcare infrastructure. We help you transform fragmented data into a unified, high-performance ecosystem that drives growth. Contact us today to build a resilient EHR platform that defines the next decade of care.
Build an Enterprise EHR Platform With Intellivon
At Intellivon, EHR platforms are engineered as an enterprise clinical infrastructure, not as systems layered onto fragmented healthcare environments. The goal is to create a unified platform that manages patient data, automates workflows, and enables seamless care delivery across providers, systems, and settings.
Each solution is designed to support the full patient lifecycle. This includes smart scheduling, clinical documentation, decision support, care coordination, and automated billing. As a result, healthcare organizations gain real-time visibility, reduce operational inefficiencies, and deliver faster, more accurate care.
Our approach focuses on AI-first, API-driven architectures combined with interoperability standards like HL7 and FHIR. This ensures seamless integration with EHR systems, labs, pharmacies, billing platforms, and existing healthcare infrastructure without disrupting ongoing operations.
Why Partner With Intellivon?
- Clinical Infrastructure, Not Just Software: Built to support long-term clinical operations across complex healthcare ecosystems.
- AI-Driven Workflow Automation: Automates documentation, scheduling, billing, and care coordination to reduce manual effort.
- Integration-Ready Architecture: Connects seamlessly with healthcare systems, devices, and third-party platforms.
- Compliance-First Engineering: Designed with HIPAA-compliant security, encryption, and governance frameworks.
- Scalable for Enterprise Healthcare Systems: Supports multi-location providers and high patient volumes without performance bottlenecks.
Custom EHR platforms are no longer optional for organizations aiming to scale care delivery and improve clinical outcomes. Therefore, building the right system early directly impacts efficiency, compliance, and long-term scalability.
Connect with Intellivon’s experts to build an EHR platform tailored to your workflows, integrations, and growth roadmap.
FAQs
Q1. What is an EHR system in healthcare?
A1. An EHR (Electronic Health Record) system is a digital platform that stores, manages, and shares patient health information across providers. It supports clinical workflows, documentation, and decision-making in real time.
Q2. How long does it take to build an EHR system?
A2. EHR development typically takes 4 to 9 months, depending on complexity, integrations, and compliance requirements. MVP systems can be built faster, while enterprise platforms require longer timelines.
Q3. What integrations are required in EHR platforms?
A3. EHR systems commonly integrate with labs, pharmacies, billing systems, insurance platforms, and medical devices. They also use standards like HL7 and FHIR for seamless data exchange.
Q4. How secure are custom EHR systems?
A4. Custom EHR systems are designed with HIPAA-compliant security, including encryption, role-based access, audit logs, and secure data storage. Security is built into the architecture, not added later.
Q5. How much does it cost to build an EHR system?
A5. The cost typically ranges from $50,000 to $150,000 for a scalable EHR platform. Pricing depends on features, integrations, compliance scope, and system complexity.