Healthcare organizations are losing efficiency because there’s a gap nobody talks about, which is disconnected patient monitoring and clinical record systems. Imagine real-time vitals living on one platform while a patient’s history is tucked away in another, so care teams move more slowly, compliance risks pile up, and managing chronic conditions quietly becomes even more expensive. We’re well past the debate about whether integration matters. Now, everyone’s asking how to actually build it the right way.
When you bring remote patient monitoring together with EHR infrastructure, the whole game changes. Suddenly, the data flows seamlessly from bedside to back office. At the same time, clinicians get a single source of truth and can act on live patient information right inside the system that stores their medical history. For organizations handling big patient populations, that means better outcomes, fewer readmissions, and real dollars saved.
Intellivon is an expert in developing enterprise-level RPM+EHR platforms that connect these systems with precision, security, and the ability to scale. This blog draws from our expertise and talks about architecture, interoperability standards, and compliance surrounding these platforms.
Why RPM + EHR Is Now a Clinical Priority
Remote patient monitoring (RPM) integrated with electronic health record (EHR) systems has become a clinical and operational priority.
This shift comes from the need to move beyond episodic visits toward continuous, real-time patient care. At the same time, it aligns with modern healthcare demands, including reimbursement models, staffing constraints, and AI-driven clinical workflows.
The global remote patient monitoring (RPM) market is set to expand from approximately USD 39.97 billion in 2025 to over USD 103.95 billion by 2033, growing at a CAGR of around 12.7%. This growth is driven by rising chronic disease cases, aging populations, and stronger support from telehealth and RPM reimbursement policies.
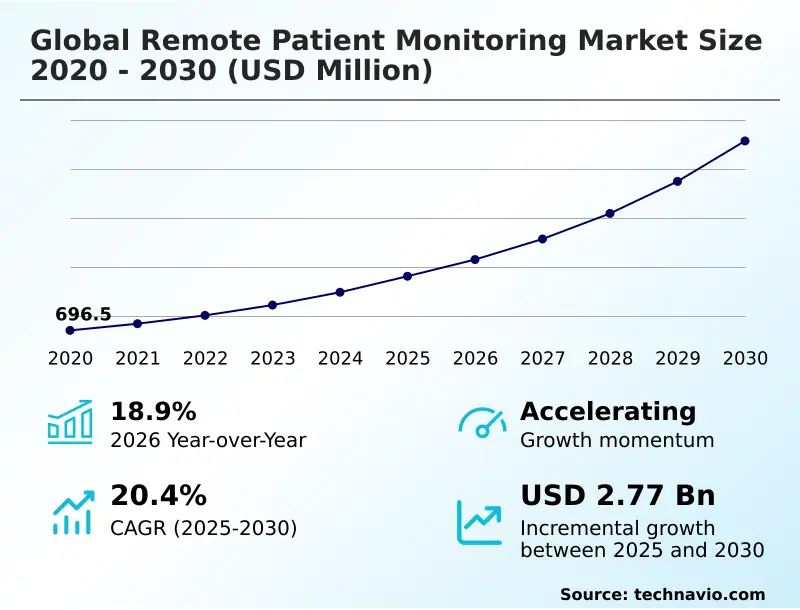
Integrating Remote Patient Monitoring with Electronic Health Records creates a unified ecosystem that transforms passive data into active clinical intelligence.
1. Bridging the Gap in Chronic Disease Management
Managing chronic conditions requires more than occasional check-ups. It demands a constant stream of physiological data to prevent acute episodes. When RPM tools feed directly into an EHR, clinicians receive a comprehensive view of a patient’s health trajectory.
This connectivity allows for early intervention before a condition escalates into a costly emergency room visit. Therefore, healthcare providers can shift from reactive treatments to proactive wellness strategies.
2. Maximizing Operational Efficiency and Revenue
Manual data transcription is a significant bottleneck in clinical workflows. It often leads to human error and administrative fatigue among nursing staff. By automating the flow of data from wearable devices to the patient chart, organizations reclaim valuable time.
Furthermore, this integration simplifies the documentation required for CPT reimbursement codes. Consequently, the enterprise sees a direct improvement in both operational throughput and the bottom line.
3. Enhancing Patient Engagement and Retention
Patients today expect the same digital convenience in healthcare that they experience in retail or banking. A seamless RPM experience makes patients feel continuously cared for without the friction of frequent travel.
When they see their data reflected accurately in their portal, their trust in the provider increases. This digital transparency fosters higher adherence to treatment plans. Ultimately, satisfied patients are more likely to remain within a specific health system, driving long-term enterprise growth.
The convergence of remote monitoring and core health records is no longer an optional innovation but a strategic necessity. Organizations that bridge this technical divide will lead the market in both clinical outcomes and operational resilience.
What RPM + EHR Integration Actually Means
Remote patient monitoring combined with EHR integration is the technical and clinical unification of two systems that have historically operated in silos. RPM captures real-time patient vitals through connected devices. EHR holds the complete longitudinal health record.
When both systems share a live data pipeline, clinicians stop toggling between platforms and start making decisions from a single, continuously updated patient profile.
RPM vs EHR vs Care Platforms Explained
Healthcare systems often use RPM, EHR, and care platforms together. However, each serves a very different purpose. Understanding this distinction is critical before building or integrating a solution.
Otherwise, teams end up layering tools instead of creating a unified system that actually improves care delivery.
Comparison: RPM vs EHR vs Care Platforms
| Component | Primary Role | Key Functions | Data Type | Users | Where It Fits |
| RPM (Remote Patient Monitoring) | Capture patient data outside clinical settings | Collect vitals, device data, alerts, and real-time monitoring | Continuous, high-frequency patient data | Clinicians, care teams | Extends care beyond hospitals into homes |
| EHR (Electronic Health Record) | Store and manage patient records | Clinical documentation, history, billing, and compliance | Structured clinical data | Doctors, nurses, and admin staff | System of record for healthcare operations |
| Care Platforms | Coordinate care workflows across systems | Care plans, task management, communication, analytics | Aggregated and contextual data | Care coordinators, providers, payers | Orchestrates care across multiple touchpoints |
How They Work Together
RPM systems continuously collect patient data. This data flows into the EHR, where it becomes part of the patient’s official medical record.
Care platforms then sit on top of both systems. They use this combined data to trigger workflows, assign tasks, and guide clinical decisions across teams.
Each system solves a different problem. RPM captures real-time data, EHR stores it, and care platforms act on it. Therefore, successful healthcare platforms do not treat these as separate tools. Instead, they integrate them into a single, connected ecosystem that supports continuous, coordinated care.
Core Capabilities of RPM + EHR Systems
Building an enterprise-grade ecosystem requires moving beyond simple data collection. The true value lies in how that data is synchronized, analyzed, and presented within the existing clinical environment.
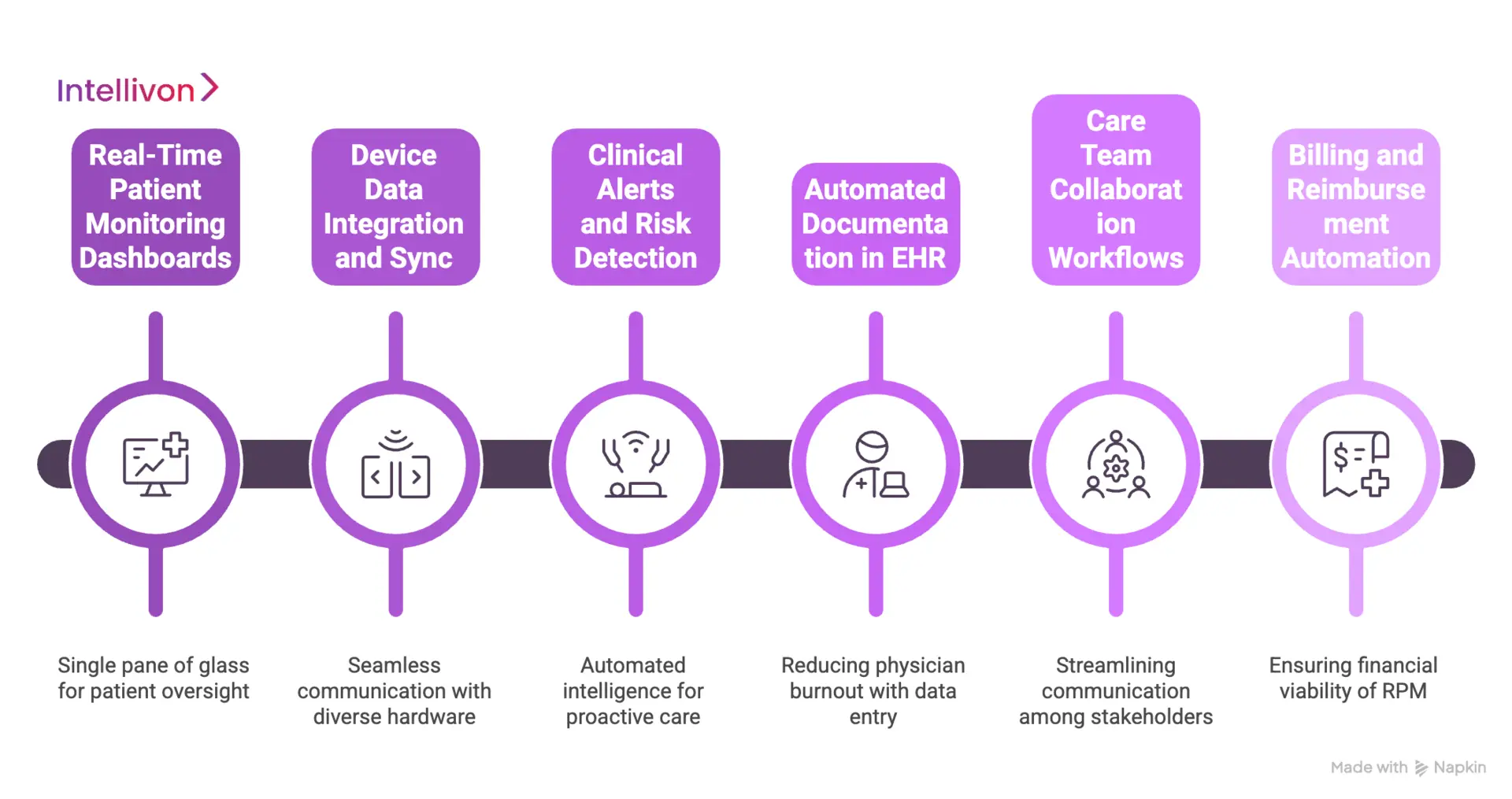
1. Real-Time Patient Monitoring Dashboards
Decision-makers need a single pane of glass to oversee vast patient populations effectively. These dashboards aggregate streaming data from multiple sources into a prioritized visual interface. Clinicians can quickly identify which patients are stable and which require immediate attention.
Therefore, the system acts as a force multiplier for limited medical staff. This high-level visibility is essential for managing risk across a large enterprise.
2. Device Data Integration and Sync
The technical backbone of any RPM solution is its ability to communicate with diverse hardware. Whether using cellular blood pressure cuffs or Bluetooth glucose monitors, data must sync without manual user intervention.
A sophisticated integration layer handles the translation of various proprietary formats into a standardized health language. Consequently, the EHR remains the “source of truth” without being cluttered by raw, unorganized data packets.
3. Clinical Alerts and Risk Detection
Static data is informative, but automated intelligence is what saves lives and reduces liability. Advanced systems use clinical logic to trigger alerts when a patient’s vitals breach specific, pre-defined thresholds. These notifications are routed directly to the appropriate care coordinator within the EHR interface.
In addition, machine learning can identify subtle trends that suggest a brewing complication. Proactive risk detection minimizes the chance of readmissions and optimizes patient safety.
4. Automated Documentation in EHR
One of the primary drivers of physician burnout is the burden of manual data entry. Integrated systems automatically populate the patient’s longitudinal record with verified monitoring data.
This automation ensures that the medical history is always current and audit-ready. Furthermore, it eliminates the transcription errors that often plague manual reporting processes. Reliable documentation is the foundation of both clinical excellence and legal protection.
5. Care Team Collaboration Workflows
Remote monitoring involves nurses, specialists, and primary care providers. Integration allows these stakeholders to share notes and update care plans within the same digital environment.
Secure messaging and task assignment features ensure that no critical update falls through the cracks. This unified approach streamlines communication and reduces the “silo” effect common in large organizations. Improved coordination leads to more cohesive and efficient patient journeys.
6. Billing and Reimbursement Automation
For an RPM initiative to be sustainable, it must be financially viable and easy to bill. The system tracks the exact minutes spent on monitoring and the number of days during which data was transmitted. It then maps this activity to specific CPT codes, such as 99453 or 99457, for seamless claims submission.
This transparency ensures the organization captures all eligible revenue without increasing the administrative workload. Automated billing transforms a clinical program into a predictable and scalable revenue stream.
These core capabilities represent the engine room of a modern, integrated healthcare enterprise. By focusing on automation and workflow harmony, leaders can ensure their investment delivers both clinical impact and financial returns.
How RPM Data Flows into EHR Systems
Understanding the journey of a single heartbeat from a wearable device to a clinical chart is vital for any investor.
This movement of data must be fast, secure, and invisible to the end-user to be truly effective.
1. Device to Cloud to EHR Pipeline
The process begins at the patient’s home with a connected medical device. This hardware transmits raw data points to a secure cloud environment via cellular or Wi-Fi networks. Once in the cloud, the data undergoes a process called normalization to ensure it matches the hospital’s digital format.
Finally, the system pushes this refined information directly into the EHR through a secure bridge. This seamless flow allows doctors to see updates without ever leaving their primary software.
2. HL7 vs FHIR for Data Exchange
Choosing the right language for data transfer is a critical technical decision for your platform. Older systems often rely on HL7 v2, which acts like a rigid, one-way telegram. In contrast, FHIR (Fast Healthcare Interoperability Resources) is a modern, internet-based standard that works like a live website.
FHIR allows for “plug-and-play” connectivity and is the preferred choice for scaling large-scale digital health solutions. Therefore, investing in FHIR-native architecture ensures your platform remains compatible with future industry regulations.
3. Handling High-Frequency Patient Data
A common challenge in RPM is the sheer volume of incoming information. If every single data point hit the EHR instantly, the system would likely crash or overwhelm the doctors.
Strategic platforms use “edge processing” or cloud filters to manage this high-frequency traffic effectively. They aggregate thousands of data points and only send significant summaries or critical changes to the medical record. Consequently, the EHR stays lean while still providing a complete picture of the patient’s health.
4. Ensuring Data Accuracy and Consistency
Data is only useful if the clinical team can trust it completely. The system must verify that the information coming from a device actually belongs to the correct patient profile. Robust identity management protocols prevent data “ghosting” or cross-contamination between different users.
In addition, automated validation checks flag any readings that seem physically impossible or indicate a sensor malfunction. Maintaining this high level of consistency protects both the patient’s safety and the provider’s legal standing.
The technical plumbing of an RPM system dictates its long-term reliability and its ability to scale across an enterprise. By prioritizing modern data standards and smart filtering, organizations can build a foundation that supports better care and clearer insights.
Architecture Behind RPM + EHR Platforms
Investing in a healthcare platform requires a deep look at the underlying structural choices. A well-designed architecture ensures that the system can handle thousands of concurrent patients without compromising speed or data safety.
1. Monolith vs Microservices in Healthcare
A monolithic architecture bundles all functions into a single codebase, which is simpler to build initially. However, this approach often creates bottlenecks as the user base grows. In contrast, a microservices model breaks the platform into independent modules like billing, alerts, and data ingestion.
This separation allows you to scale specific services without affecting the entire system. Therefore, microservices offer the agility needed for an evolving healthcare enterprise.
2. API-First Design for Interoperability
An API-first strategy treats the connection points as the primary product rather than an afterthought. This means the system is built from the ground up to communicate with external lab systems and pharmacies.
By using standardized RESTful APIs, your platform becomes a “plug-and-play” solution for hospital networks. Consequently, integration times are slashed, and the cost of onboarding new partners decreases significantly. This modularity is a key selling point for high-value healthcare investors.
3. Cloud Infrastructure for Scalability
Relying on physical on-site servers is no longer a viable strategy for modern RPM platforms. Cloud infrastructure allows the system to automatically adjust its resources based on real-time demand.
During a sudden spike in patient monitoring data, the cloud expands to prevent any lag or system crashes.
Furthermore, cloud providers offer built-in HIPAA-compliant security layers that protect sensitive patient information. Investing in a cloud-native approach ensures your platform is future-proof and ready for global expansion.
4. Middleware for Legacy EHR Systems
Many large hospital systems still operate on older, legacy EHR software that lacks modern connectivity. Middleware acts as a sophisticated translator that sits between your RPM platform and these aging systems.
It converts modern data formats into the specific languages that legacy software can understand. This avoids the need for a total and expensive system overhaul for the client. In addition, middleware provides a centralized hub for monitoring data integrity across multiple disparate systems.
The architectural framework of an RPM platform determines its long-term reliability and market competitiveness. By prioritizing modularity and cloud-native scaling, entrepreneurs can build a resilient solution that meets the rigorous demands of the modern medical landscape.
Integrating RPM with Epic, Cerner, and Others
Success in the remote monitoring market depends on the ability to live within the ecosystems of industry giants. For an investor, understanding these gatekeepers is the difference between a niche tool and a scalable enterprise solution.
1. Why EHR Vendor Differences Matter
Every EHR vendor has a unique “DNA” that dictates how it handles external data. Some systems prioritize rigid security silos, while others offer more flexible developer environments. If your platform cannot adapt to these internal logic variations, implementation costs will skyrocket.
Therefore, a one-size-fits-all approach to integration often leads to project delays. Strategic leaders must plan for these nuances to ensure a smooth rollout across diverse hospital networks.
2. Mastering Epic and Cerner Environments
Epic remains a dominant force, offering the “Open.epic” platform for third-party developers to access patient data. By utilizing these specific APIs, your RPM solution can push vitals directly into the clinician’s existing workflow.
In contrast, Cerner (Oracle Health) uses the “Millennium” architecture and Ignite APIs, which are built for massive datasets. Furthermore, mid-market vendors often lack this robust documentation, requiring specialized data bridges to translate information. Navigating these disparate systems effectively opens doors to the world’s largest healthcare contracts.
3. Key FHIR Resources for Scalability
The FHIR standard organizes health data into resources that act like standardized digital containers. For RPM, the most critical resource is the observation, which carries the actual physiological readings. Other resources, such as “Patient” and “Device,” ensure that every reading is correctly linked to the right person.
Using these standardized blocks allows your platform to talk to any modern EHR without custom coding. Consequently, this interoperability is the foundation of a future-proof healthcare business.
Navigating the complex landscape of EHR vendors is a primary hurdle for any remote monitoring initiative. By mastering both the major players and the underlying data standards, your organization can deliver a truly unified clinical experience.
Step-by-Step RPM + EHR Development Process
Building a high-performance healthcare platform requires a rigorous, phased approach that aligns technical execution with clinical necessity.
At Intellivon, we transform complex health data requirements into scalable, enterprise-grade solutions through a battle-tested development lifecycle.
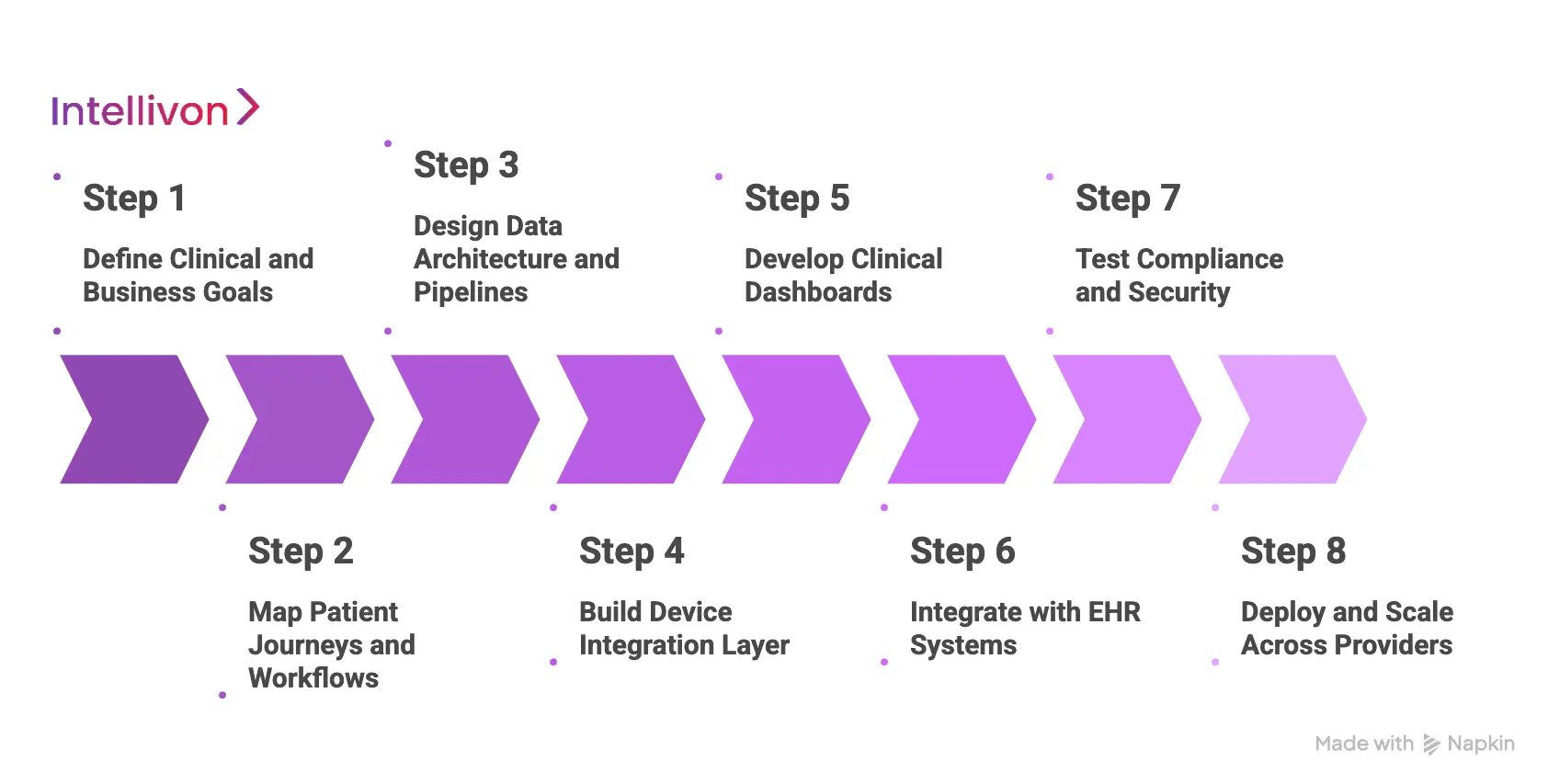
Step 1: Define Clinical and Business Goals
Every successful project begins with a clear understanding of the “why.” We collaborate with stakeholders to identify specific therapeutic areas, such as hypertension or diabetes management, that drive the highest ROI.
Furthermore, we define key performance indicators like reduced readmission rates or increased billing efficiency. Setting these benchmarks early ensures the technical roadmap remains focused on delivering measurable business value.
Step 2: Map Patient Journeys and Workflows
A platform is only as good as its usability in a high-pressure clinical setting. We meticulously map the end-to-end journey for both the patient at home and the clinician in the hospital. This includes identifying touchpoints for data collection, alert triggers, and intervention protocols.
By visualizing these workflows, we eliminate friction points that typically lead to staff burnout. Consequently, the resulting system feels like a natural extension of the provider’s existing daily routine.
Step 3: Design Data Architecture and Pipelines
The technical foundation must be capable of handling massive, asynchronous data streams. We design a cloud-native architecture that prioritizes data integrity and low-latency processing. Our engineers build robust pipelines that ingest, normalize, and validate raw vitals before they reach the core database.
This structured approach prevents system congestion and ensures that clinicians always work with “clean” data. Therefore, the architecture scales effortlessly as your patient population grows.
Step 4: Build Device Integration Layer
Interacting with diverse hardware requires a sophisticated abstraction layer. We develop custom drivers and integration modules that allow the platform to communicate with any Bluetooth or cellular-enabled medical device.
This layer handles the complexities of different proprietary protocols and translates them into a unified format. In addition, we implement automated device provisioning to make the setup process “plug-and-play” for patients. This technical flexibility allows your enterprise to remain hardware-agnostic.
Step 5: Develop Clinical Dashboards
Data is useless if it cannot be interpreted quickly during a busy shift. We build intuitive, high-density dashboards that use color-coded triage systems to highlight at-risk patients. These interfaces provide longitudinal views of patient health, allowing doctors to spot trends that a single reading might miss.
Furthermore, we ensure the UI is responsive and optimized for both desktop and mobile environments. A clear visual hierarchy ensures that critical information is never more than a glance away.
Step 6: Integrate with EHR Systems
True clinical value is unlocked when the RPM data lives inside the primary medical record. We leverage FHIR and specialized APIs to create bi-directional sync between the monitoring platform and major EHRs like Epic or Cerner.
This ensures that vitals, notes, and alerts are automatically filed into the correct patient chart. By removing the need for manual data entry, we significantly increase the speed of clinical decision-making. Strategic integration turns a standalone tool into a core institutional asset.
Step 7: Test Compliance and Security
In healthcare, security is not an afterthought; it is a prerequisite for market entry. We conduct rigorous penetration testing and vulnerability assessments to ensure the platform meets HIPAA and SOC 2 standards.
Every data packet is encrypted using industry-leading protocols during transit and at rest. Additionally, we verify that role-based access controls are functioning perfectly to prevent unauthorized data exposure. This uncompromising focus on security protects your organization from catastrophic legal and financial risks.
Step 8: Deploy and Scale Across Providers
The final phase involves a controlled rollout followed by rapid horizontal scaling. We utilize containerized deployment strategies to ensure the platform remains stable across different hospital environments. Our team provides comprehensive training and technical support to ensure smooth onboarding for clinical staff.
As the user base expands, our automated scaling protocols adjust cloud resources in real-time to maintain peak performance. This ensures your investment continues to deliver value as you capture more of the market.
Developing a sophisticated RPM and EHR ecosystem is a complex journey that demands deep technical and clinical expertise. By following this structured eight-step process, Intellivon ensures your platform is built for reliability, security, and long-term enterprise growth.
Real Challenges in RPM + EHR Development
Building a bridge between remote devices and hospital records is rarely a straight path. For any investor, recognizing these technical and cultural hurdles early is the key to protecting your capital and ensuring a successful rollout.
1. Integrating with Legacy EHR Systems
Many established hospitals still use older software that was never built to talk to the modern cloud. These legacy systems often rely on rigid, one-way communication methods that make real-time updates difficult. To solve this, developers must build custom “translators” or middleware to move data without crashing the host system.
Therefore, the integration process often requires more than just a simple API connection. Navigating these aging infrastructures is a primary technical cost in most healthcare projects.
2. Managing Continuous Data Streams
Remote devices can generate thousands of data points every hour for a single patient. If a platform tries to push every single heartbeat into a medical record, the database will quickly become overwhelmed.
Engineers must design smart filters that aggregate this data and only highlight significant changes or red flags. This ensures the system stays fast and the clinician is not buried under a mountain of irrelevant numbers. Consequently, managing data issues is vital for maintaining system performance at scale.
3. Ensuring Clinical-Grade Accuracy
In healthcare, a small error in data transmission can lead to a dangerous medical mistake. The system must guarantee that the blood pressure reading on the patient’s screen is exactly what appears in the doctor’s chart. This requires rigorous protocols between the device, the cloud, and the EHR to prevent data loss.
Furthermore, automated checks must flag any readings that seem physically impossible or indicate a sensor failure. Maintaining this level of precision is the only way to build long-term trust with medical professionals.
4. Meeting HIPAA and Compliance Needs
Protecting patient privacy is a legal mandate that carries heavy financial penalties for any slip-up. Every part of the data journey must be encrypted to meet strict HIPAA and SOC 2 security standards. This includes how data is stored on the device, how it travels over the internet, and who can see it in the hospital.
In addition, the system must maintain a permanent audit trail of every person who accessed a patient’s file. Keeping up with these evolving regulations is a continuous and necessary investment for any health platform.
5. Driving Adoption Among Care Teams
The most advanced technology in the world is useless if doctors and nurses refuse to use it. Many clinicians view new software as an extra burden that takes time away from their patients. To drive adoption, the RPM tool must feel like it simplifies their day rather than adding another task to their checklist.
This means keeping the interface clean and ensuring that alerts are truly meaningful and not just “crying wolf.” Therefore, focusing on the human experience is just as important as the underlying code.
While the obstacles in RPM development are significant, they are not insurmountable for an experienced team. By addressing these challenges with smart architecture and a focus on the end-user, organizations can build a solution that truly transforms patient care.
How Intellivon Solves RPM Integration Gaps
Moving from a pilot program to an enterprise-wide rollout requires more than a simple monitoring tool. At Intellivon, we bridge the gap between fragmented patient data and clinical action by building the foundational infrastructure that powers modern healthcare.
1. Building Clinical Infrastructure
Most vendors offer standalone applications that create new data silos rather than solving existing ones. We focus on building a deep clinical infrastructure that sits at the center of your existing digital ecosystem. This approach ensures that remote monitoring is not a “side project” but a core function of your medical delivery.
Therefore, our solutions are designed to grow and evolve alongside your institution’s strategic goals. Investing in infrastructure rather than isolated tools provides a much higher long-term return.
2. FHIR-First Integration Architecture
Interoperability is often the biggest failure point in digital health, which is why we utilize a FHIR-first design. By using the latest FHIR standards, we ensure your platform speaks the same language as any modern EHR.
This eliminates the need for expensive, custom-coded connectors every time you add a new hospital partner. Consequently, our architecture allows for rapid deployment across diverse networks without compromising data quality. A standardized language is the key to global scalability in healthcare.
3. Scalable Data Pipelines for RPM
Handling millions of data points from thousands of home devices requires a high-performance engine. Our engineers build scalable data pipelines that process, validate, and store patient vitals in real-time. We use intelligent “edge filtering” to ensure that only clinically relevant information reaches the physician’s dashboard.
This prevents system lag and ensures that your technical costs remain predictable as your patient count increases. Reliable pipelines turn raw noise into the actionable insights that save lives.
4. Workflow Automation for Care Teams
The true cost of RPM is often the human time required to monitor the incoming data. We solve this by implementing advanced workflow automation that handles the “heavy lifting” for your nursing staff.
From automated billing triggers to threshold-based emergency alerts, our system ensures that clinicians only step in when their expertise is truly needed. In addition, we integrate these tasks directly into the EHR interface to prevent app-switching. Automation transforms a labor-intensive process into a lean, high-efficiency operation.
5. Secure and Compliant System Design
In the enterprise world, security is the foundation of every partnership and every contract. Our designs incorporate end-to-end encryption and multi-factor authentication to exceed HIPAA and SOC 2 requirements.
We treat data privacy as a non-negotiable feature, ensuring that every byte of information is protected at rest and in motion. Furthermore, our detailed audit logs provide full transparency for regulatory reviews or internal quality checks. A secure system design protects your brand reputation as much as it protects your patients.
Our experts deliver a strategic advantage by solving the most difficult technical challenges in healthcare today. By focusing on standards, scalability, and security, we empower you to build a platform that truly leads the market.
Key Integrations Required in RPM Platforms
To work well in a hospital, a remote monitoring tool cannot stay in its own bubble. It must connect with the other software and devices that doctors already use every single day.
1. EHR Systems Like Epic and Cerner
The Electronic Health Record (EHR) is the digital brain of any modern hospital. If your monitoring data does not show up inside Epic or Cerner, doctors will likely ignore it. We build secure bridges that push heart rates and blood pressure levels directly into the patient’s main chart.
Therefore, medical staff do not have to waste time logging into a second website to see how a patient is doing. This smooth connection is the most important step for any enterprise-grade platform.
2. Wearable and IoT Health Devices
Patients at home use many different tools like smart watches, digital scales, and blood pressure cuffs. A great platform must be able to “talk” to all these different brands without any glitches. At Intellivon, our experts create a central hub that collects this data and turns it into a simple format that a computer can read.
In addition, we make sure the devices are easy for patients to set up, often just requiring them to turn the power on. Consequently, better data from the home leads to better decisions in the clinic.
3. Labs, Pharmacies, and Billing Systems
Monitoring a patient often leads to new steps, like ordering a blood test or changing a prescription. Your platform should connect directly to lab systems and pharmacies to handle these tasks automatically.
Furthermore, the system must track every minute of care so it can send the correct bill to the insurance company. This automation ensures the hospital gets paid for its work without extra paperwork. A fully connected system handles the medical side and the business side at the same time.
4. Telehealth and Communication Tools
Sometimes, a doctor needs to see a patient face-to-face over a video call if their vitals look concerning. Integrated telehealth tools allow a nurse to start a video chat or send a secure text message directly from the monitoring screen.
This immediate connection can prevent a small health issue from becoming a major emergency. In addition, it keeps all the conversation notes in one safe place for future review. Better communication leads to a more personal and effective experience for everyone involved.
Connecting these different pieces of technology is what turns a simple gadget into a powerful medical system. By focusing on these key integrations, your organization can provide a complete and reliable service that scales with ease.
Security and Compliance in RPM Systems
Protecting patient data is the most critical hurdle for any healthcare enterprise. A single data breach can result in massive fines and a permanent loss of provider trust.
1. HIPAA and Data Privacy Requirements
Operating in the United States requires strict adherence to HIPAA regulations for handling Protected Health Information (PHI). Beyond basic compliance, achieving SOC 2 Type II certification demonstrates a long-term commitment to operational security.
These frameworks ensure that data is encrypted both at rest and during transit. Therefore, investors should prioritize platforms that treat security as a foundational feature rather than a checkbox. This level of rigor reduces legal liability for the entire enterprise.
2. Encryption and Access Control
Every piece of vital data moving from a home device must be shielded from unauthorized access. Advanced platforms use AES-256 encryption for storage and TLS 1.3 for secure data transmission.
Furthermore, multi-factor authentication ensures that only verified staff can view sensitive records. This ensures that individual identities remain protected even during large-scale data syncs. Consequently, robust encryption builds a “moat” around the patient’s digital life.
3. Audit Trails and Monitoring Systems
A secure system must keep a detailed record of every person who views or changes a medical file. These audit trails allow administrators to track exactly when and where data was accessed.
If a security issue occurs, these logs help teams identify the source and fix it immediately. In addition, real-time monitoring tools can flag suspicious login attempts from unknown locations. Constant oversight is the best defense against internal and external threats.
4. Secure APIs and Data Exchange Layers
When your RPM tool talks to an EHR, the connection point must be hardened against attacks. We use secure API gateways that act as digital bouncers, only letting authorized requests through.
These layers also use “rate limiting” to prevent the system from being overwhelmed by too many data requests at once. Furthermore, we regularly test these connections for vulnerabilities to stay ahead of new risks. A strong exchange layer ensures that data flows freely but safely between different health systems.
Security is the bedrock upon which successful RPM and EHR integrations are built. By investing in high-level compliance and encryption, organizations can scale their digital health initiatives with total confidence.
Cost to Build RPM + EHR Platforms in 2026
At Intellivon, RPM + EHR platforms are built as an enterprise healthcare infrastructure, and not as monitoring tools layered onto disconnected systems. The objective is to create a unified platform that captures patient data, integrates with clinical systems, and enables continuous care delivery across settings.
However, building a reliable RPM + EHR solution requires more than connecting devices to dashboards. It involves designing scalable data pipelines, ensuring interoperability with EHR systems, and meeting strict compliance requirements. As a result, healthcare organizations gain real-time visibility, reduce care gaps, and improve patient outcomes at scale.
Estimated Phase-Wise Cost Breakdown
| Phase | Description | Estimated Cost Range (USD) |
| Discovery & Clinical Planning | Define use cases, patient workflows, RPM scope, and EHR integration requirements | $8,000 – $15,000 |
| System Architecture & Data Design | Design RPM data pipelines, FHIR/HL7 integration, and infrastructure architecture | $10,000 – $20,000 |
| Device Integration Layer | Connect wearables, IoT devices, and remote monitoring systems | $8,000 – $18,000 |
| EHR Integration Development | Integrate with Epic, Cerner, or other EHRs using FHIR/HL7 APIs | $10,000 – $25,000 |
| Clinical Dashboard & UX Development | Build monitoring dashboards, alerts, and care workflows for providers | $7,000 – $18,000 |
| Compliance, Security & Testing | Implement HIPAA compliance, encryption, testing, and validation | $5,000 – $12,000 |
| Deployment & Scaling Setup | Cloud deployment, performance optimization, and scalability setup | $5,000 – $12,000 |
Estimated Total Cost
For most healthcare organizations, the cost to build an RPM + EHR platform typically ranges between:
$50,000 – $150,000
Key Factors That Influence Cost
- Number and type of devices integrated
- Complexity of EHR systems (Epic, Cerner, etc.)
- Real-time data processing requirements
- Level of automation in clinical workflows
- Compliance and security requirements
- Scalability across multiple providers or locations
Get a Precise Cost Breakdown
Every RPM + EHR platform is different. The final cost depends on your clinical workflows, integration complexity, and scale. Talk to Intellivon’s experts to get a tailored cost estimate for your platform.
How We Built an RPM + EHR Platform for Providers
A multi-location healthcare provider partnered with Intellivon to unify remote patient monitoring with their existing EHR systems. The objective was to enable continuous, real-time care while eliminating fragmented workflows across systems.
1. The Challenge: Fragmented Patient Monitoring
The provider relied on multiple RPM devices to track patient vitals. However, each device operated within its own ecosystem, creating disconnected data streams.
This led to several operational issues:
- RPM data remained siloed across vendor dashboards
- Clinicians had to switch between multiple systems daily
- No direct integration with the EHR system
- Manual data entry increases errors and compliance risks
- Delays in identifying high-risk patients
As patient volumes increased, these inefficiencies began to impact both care quality and team productivity.
2. The Solution: Unified RPM + EHR Platform
Intellivon designed a unified platform that connected device data, clinical workflows, and EHR systems into a single layer.
The solution focused on:
- A centralized RPM data ingestion layer
- Real-time processing and alert generation
- FHIR-based integration with the EHR
- Embedded clinical dashboards within workflows
- Automated documentation and data syncing
As a result, clinicians could access patient data directly within the EHR, without switching between systems.
3. The Architecture and System Components
The platform was built using a modular, scalable architecture designed for interoperability.
Key components included:
- Device Integration Layer: Standardize data from multiple RPM devices into a unified format
- Processing and Alert Engine: Analyzed incoming data and triggered alerts based on clinical thresholds
- EHR Integration Layer (FHIR): Mapped data to resources like Observation and Patient for seamless syncing
- Clinical Workflow Layer: Delivered dashboards and alerts within existing provider workflows
- Security and Compliance Layer: Ensured encrypted data transmission and role-based access control
This architecture allowed the system to scale across multiple care settings without disrupting existing infrastructure.
4. Results: Improved Outcomes and Efficiency
The unified platform delivered measurable improvements across clinical and operational metrics:
- Reduced manual documentation efforts by over 40%
- Improved response time for high-risk patient alerts
- Enabled real-time visibility of patient data within the EHR
- Streamlined workflows across care teams
- Supported scaling of RPM programs without added complexity
As a result, the provider improved care delivery while maintaining operational efficiency at scale.
Conclusion
RPM EHR integration is becoming essential for delivering continuous, connected care. It bridges data gaps, improves clinical visibility, and enables faster decision-making across healthcare systems.
As providers move toward scalable, value-based models, building integrated platforms is no longer optional. The right approach combines real-time monitoring, seamless EHR connectivity, and workflow automation to support better outcomes while maintaining efficiency across growing patient populations.
Build an RPM + EHR Platform With Intellivon
At Intellivon, RPM + EHR platforms are built as an enterprise healthcare infrastructure, not as monitoring tools layered onto disconnected clinical systems. The objective is to create a unified platform that connects real-time patient data with clinical workflows, enabling continuous, coordinated care across settings.
Each platform is designed to support the full remote care lifecycle. This includes device integration, real-time patient monitoring, clinical alerts, EHR synchronization, care coordination, and automated documentation. As a result, healthcare providers gain real-time visibility into patient health while reducing manual effort and improving response times.
Our engineering approach focuses on AI-first, API-driven architectures combined with interoperability standards like HL7 and FHIR. This ensures seamless integration with EHR systems, wearable devices, labs, and care platforms without disrupting existing clinical operations.
Why Intellivon for RPM + EHR Development
- Clinical infrastructure, not just monitoring tools: Platforms are built to support continuous care delivery, not isolated data tracking.
- Designed for interoperability from day one: Seamless integration with EHRs, devices, and healthcare systems ensures consistent data flow and reliability.
- Real-time data processing and alerting: Enable faster clinical decisions with continuous monitoring and automated risk detection.
- Built for scale and compliance: Architectures support multi-provider environments while meeting global healthcare regulations.
Whether you are launching a new RPM platform or integrating remote monitoring into existing systems, Intellivon helps you design, build, and scale with confidence.
Talk to Intellivon’s healthcare experts to get a tailored roadmap and cost estimate for your RPM + EHR platform.
FAQs
Q1. What is RPM with EHR integration?
A1. RPM with EHR integration connects remote patient monitoring devices with electronic health record systems. It allows patient data such as vitals, symptoms, and device readings to flow directly into clinical records. As a result, providers get real-time visibility within existing workflows, improving decision-making and reducing manual documentation.
Q2. How long does RPM development take?
A2. RPM development typically takes 3 to 6 months, depending on complexity. Timelines vary based on device integrations, EHR systems, compliance requirements, and workflow design. More advanced platforms with real-time analytics and multi-system integration may take longer to build and deploy.
Q3. What devices integrate with RPM systems?
A3. RPM systems integrate with a wide range of medical and wearable devices, including blood pressure monitors, glucose meters, pulse oximeters, ECG monitors, smartwatches, fitness trackers, weight scales, and temperature sensors. These devices continuously capture patient data and transmit it to the platform for monitoring and analysis.
Q4. How secure are RPM platforms?
A4. RPM platforms are designed with strong security and compliance standards. They typically include end-to-end data encryption, role-based access controls, secure APIs for data exchange, and audit logs for tracking access and changes. In addition, platforms follow healthcare regulations like HIPAA to ensure patient data remains protected at all times.
Q5. Can RPM systems scale across hospitals?
A5. Yes, RPM systems can scale across hospitals and multi-location providers. Modern platforms are built using cloud-based, modular architectures that support high patient volumes and distributed care teams. As organizations grow, these systems can expand to handle more devices, users, and integrations without impacting performance or clinical workflows.