At first, a general EHR system may seem like a practical choice as it can cover multiple workflows and keep data in one place. Over time, specialists may start noticing delays during documentation and navigation as these systems were not designed for their exact clinical needs. They often need to adjust templates and workflows, which can gradually increase effort and reduce efficiency.
The popularity of specialty EHR software has started increasing because clinics now need faster documentation and more accurate coding while also reducing manual work. Specialty EHR systems can better align with specific clinical processes and support smoother daily operations. As a result, many practices now prefer systems that are built precisely for their field.
Over the years, we’ve built numerous specialty EHR software, powered by clinical NLP engines and medical imaging integration systems. As we have this expertise, we’re sharing this blog to discuss the steps to develop a specialty EHR software.
Market Demand for Specialty EHR Software
According to Grand View Research, the global electronic health records market is projected to reach USD 53.11 billion by 2033, signaling a massive transition from rigid, legacy systems toward specialized disruption. While major incumbents focus on massive hospital networks, they have created a significant void in the private practice sector. These specialized clinics are currently burdened by feature bloat and complex interfaces designed for general care, leaving them desperate for streamlined, niche-specific solutions.
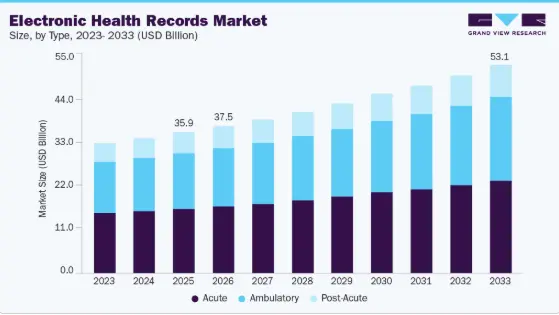
Source: Grand View Research
For the strategic investor, this represents a high-retention asset class where efficiency translates directly into ROI. In an era of shrinking reimbursements, specialty practices can no longer afford the productivity tax of generic software. Platforms that eliminate unnecessary clicks and automate specialty-specific billing do more than manage data; they actively improve a clinic’s bottom line, resulting in significantly lower churn rates than horizontal SaaS.
Rising Demand from Niche Specialty Clinics
Niche software addresses operational friction in areas like dermatology and oncology. An oncologist needs longitudinal tracking of tumor markers, while a behavioral health professional requires detailed therapy session documentation.
Success in this space is evidenced by platforms like Modernizing Medicine, which built a massive valuation by focusing on ophthalmology and dermatology. Similarly, WebPT dominated the rehabilitation market by aligning documentation with therapist-led recovery plans rather than acute care.
Investment Trends in Vertical HealthTech
Vertical HealthTech is currently outperforming horizontal SaaS in capital efficiency. Investors are prioritizing platforms that dominate a specific clinical vertical, as deep domain expertise creates a moat that is difficult for generalist competitors to cross.
Strategic capital is flowing into platforms that offer:
- Embedded Fintech: Specialized billing and payments integrated into the clinical workflow.
- Anonymized Data Insights: Aggregating niche data for pharmaceutical research.
- AI Automation: Predictive analytics that suggest treatment plans based on specialty history.
Shift Toward Personalized Clinical Workflows
Practitioners are demanding workflows that adapt to their specific practice style. For the entrepreneur, this requires a modular architecture where the user experience can be tailored without rewriting the core codebase.
This shift includes:
- Adaptive Documentation: Using NLP to categorize notes based on specialty terminology.
- Patient Portals: Shifting focus to mobile devices for specialty-specific monitoring.
- Decision Support: Logic engines that provide real-time, evidence-based guidance during patient encounters.
What Is Specialty EHR Software?
A specialty EHR is a highly calibrated digital environment engineered for the specific clinical requirements of a single medical branch. Unlike horizontal platforms that attempt to serve every department from pediatrics to pathology, specialty EHRs prioritize the unique data points, regulatory compliance, and patient journeys of a specific niche.
For the investor, this represents a move from “software as a utility” to “software as a clinical partner.” These systems are designed to mirror the physical workflow of a specialized exam room, ensuring that the technology stays out of the way of the provider-patient interaction.
How It Differs from General EHR Systems
The distinction between general and specialty EHRs is often the difference between a mass-market sedan and a precision-engineered racing vehicle. While both provide transportation, their internal configurations are built for entirely different performance metrics.
| Feature | General EHR (Horizontal) | Specialty EHR (Vertical) |
| Data Entry | Template-heavy and rigid | Intelligent, specialty-specific macros |
| Interface | Cluttered with irrelevant tabs | Streamlined to relevant clinical data |
| Implementation | Long, expensive, and disruptive | Faster deployment with built-in protocols |
| Reporting | Broad population health metrics | Deep-dive outcomes for specific pathologies |
General systems often require “workarounds” that lead to data fragmentation. A specialty system, conversely, utilizes a data architecture that recognizes the specific nomenclature and diagnostic patterns of its users from day one.
Key Specialties Using Custom EHR Platforms
While nearly every medical field benefits from customization, certain high-complexity specialties have become the primary drivers of this market expansion:
- Behavioral Health: Focuses on longitudinal tracking of mental health assessments, group therapy session notes, and complex state-specific reporting requirements.
- Ophthalmology: Requires heavy integration with specialized imaging equipment and quick-entry tools for high-volume patient days.
- Orthopedics: Centers on surgical scheduling, post-operative rehabilitation tracking, and integration with physical therapy protocols.
- Dermatology: Prioritizes visual documentation, anatomical mapping, and rapid “spot-to-billing” workflows.
Why Generic EHRs Fail Specialty Practices?
Generic EHRs prioritize horizontal scalability over clinical depth. Built primarily as administrative tools for regulatory compliance, they lack the architectural nuance required for specialized medicine. For an investor, this represents a massive market gap: these “one-size-fits-all” systems increase the cognitive and operational burden on the very providers they are meant to support.
The failure is rooted in a lack of specialized logic. When a platform forces a cardiologist and a pediatrician to use the same interface, it compels the clinician to fight the software rather than use it as a diagnostic aid. This misalignment leads to systemic inefficiencies that degrade both patient care and practice profitability.
Workflow Mismatch
Specialty practices operate on linear, highly specific clinical pathways. Generic EHRs disrupt this flow by forcing clinicians to navigate a rigid UI that does not mirror their actual physical movements or diagnostic thought processes during an exam.
- Data Fragmentation: Specialized data (e.g., orthopedic measurements) is often buried in generic “free-text” boxes, making it impossible to track outcomes or run longitudinal analytics.
- Procedural Friction: Generic systems lack native integration with specialty-specific hardware. This forces manual data entry, increasing the risk of human error and slowing patient throughput.
- Logical Gaps: A true specialty platform should act as a “clinical co-pilot.” Generic systems remain static, requiring the doctor to perform the heavy lifting of data retrieval manually.
Poor UX and Click Fatigue
In high-volume clinics, every click is a tax on time. “Click fatigue” is a primary driver of physician burnout and a barrier to scaling a healthcare business. When a system requires dozens of clicks for a routine note, it becomes a direct drain on the practice’s ROI.
Strategic investment in specialized UX focuses on contextual intelligence. A specialized platform anticipates the next move in the clinical journey, presenting only the tools relevant to that specific moment. Reducing this friction allows providers to see more patients without sacrificing documentation quality or mental well-being.
Revenue Loss
From a financial perspective, generic EHRs are “leaky buckets.” Because they lack specialty-specific coding logic, they frequently fail to capture the full billable complexity of specialized procedures, leading to significant revenue leakage.
- Under-Documentation: Without specialty-specific prompts, doctors often omit the nuanced details required to justify higher-reimbursement CPT codes.
- Denied Claims: Generic platforms lack the “scrubbing” sophistication needed for niche payer rules. High denial rates choke cash flow and increase administrative overhead costs.
- Audit Risks: Repetitive, “canned” templates in generic systems are red flags for auditors. A specialized EHR builds medical necessity directly into the workflow, ensuring every dollar billed is defensible.
Must-Have Features in Specialty EHR Software
The value of a specialty EHR lies in its ability to automate the unique complexities of a niche medical field. A high-performance platform must move beyond basic data entry, offering a sophisticated suite of tools that prioritize clinical speed, financial accuracy, and seamless data flow. These features are the non-negotiable pillars of a market-leading specialty solution.
1. Custom Templates & Smart Phrases
A competitive EHR must offer “day-one” utility through pre-configured templates that mirror a specialist’s diagnostic logic. Smart phrases and “macro” triggers allow clinicians to document complex findings in seconds.
WRS Health exemplifies this by providing over 500 specialty-specific note formats, ensuring the interface matches the provider’s specific charting style immediately upon deployment.
2. AI Documentation Tools
Modern investment should prioritize Ambient Clinical Intelligence to eliminate the “screen barrier” between doctor and patient. AI-driven ambient listening can transcribe consultations into structured medical notes in real-time.
Platforms like Heidi AI or Sunoh.ai (integrated with eClinicalWorks) demonstrate this by converting natural bedside conversations into formatted clinical documentation, drastically reducing after-hours paperwork.
3. Integrated ICD-10 & CPT Support
To ensure maximum ROI, the platform must include intelligent coding assistance that bridges the gap between documentation and reimbursement. By suggesting accurate codes based on provider notes, the system prevents under-coding and reduces audit risk.
ModMed (Modernizing Medicine) leads here with its “adaptive learning” engine that suggests relevant ICD-10 and CPT codes based on the specific surgical or clinical documentation captured.
4. Device & System Integration
A specialty EHR must act as the central nervous system of the practice, integrating natively with diagnostic hardware like OCT scanners or EKGs. Direct data ingestion eliminates manual scanning, ensuring current diagnostic data is immediately available.
AdvancedMD excels in this area, offering hundreds of APIs to connect with vision care devices like keratometers and autorefractors, pulling data directly into the patient record.
5. Healthcare Interoperability
In a fragmented landscape, the ability to exchange data via HL7, FHIR, and API protocols is critical for market viability. Seamless interoperability ensures the platform can communicate with hospital systems, labs, and pharmacies.
Epic’s Care Everywhere is the gold standard for this, allowing disparate specialty systems to pull comprehensive patient histories from across the national healthcare network instantly.
6. Role-Based Dashboards
Efficiency is a team sport; the interface must adapt to the specific needs of surgeons, nurses, and administrative staff. Role-based dashboards surface the most relevant tasks and KPIs for each user, preventing information overload.
NextGen Healthcare provides highly tailorable dashboards that allow clinical staff to see patient flow while administrators track real-time revenue cycle metrics on the same platform.
Specialty-Wise EHR Feature Breakdown
Specialty EHR is not a singular product category but a collection of distinct vertical markets. Each medical discipline possesses a unique data architecture and clinical logic. Developing a platform that captures high market share requires more than a skin-deep rebrand; it necessitates deep functional integration of the specific tools that define that specialty’s daily operations.
1. Dermatology: Visual Mapping Tools
In dermatology, the skin is the primary data source. A standard text-based EHR is insufficient because it cannot track the progression of lesions over time. A market-leading dermatology platform must prioritize Visual Documentation over traditional typing.
- Anatomic Body Mapping: Interactive 3D models where clinicians can “pin” biopsy sites and lesions.
- Image Comparison Engines: Side-by-side historical photo viewing with integrated “digital ruler” tools for measuring growth.
- Example: EMA by ModMed utilizes a “virtual skin” interface that allows dermatologists to draw directly on clinical images, automatically generating the corresponding medical note and billing codes.
2. Cardiology: ECG & Imaging Integration
Cardiology is a high-volume, data-intensive field where clinicians rely on real-time diagnostic feeds. An EHR that requires manual entry of heart rates or blood pressure is a liability. The platform must serve as a high-speed data aggregator.
- Key Performance Indicator: The “Time-to-Data” metric. The system should pull EKG strips, stress test results, and echocardiogram loops directly into the patient record via DICOM imaging standards.
- Greenway Health specializes in this by offering deep integration with cardiac device manufacturers, ensuring that remote monitoring data flows into the clinical dashboard without manual intervention, enabling faster intervention for high-risk patients.
3. Orthopedics: ROM & Injury Tracking
Orthopedic surgery is fundamentally about mechanics and mobility. Documentation must reflect the functional status of the musculoskeletal system. A generic EHR fails to capture the granular progression of a patient’s recovery or the specific mechanics of a joint.
- ROM (Range of Motion) Tracking: Automated graphing of joint mobility over multiple visits.
- Surgical Planning Modules: Integration with PACS (Picture Archiving and Communication System) to allow surgeons to overlay templates on X-rays for pre-operative planning.
Example: Phoenix Ortho is designed specifically to mirror the orthopedic workflow, featuring a “one-click” injury-tracking system that correlates specific physical therapy outcomes with the initial surgical intervention.
4. Mental Health: Session-Based Notes
Mental health providers deal with unstructured, narrative-heavy data and strict privacy requirements (HIPAA/42 CFR Part 2). The architecture must support long-form narrative while maintaining the structure required for insurance reimbursement.
- Collaborative Care Models: Tools that allow psychiatrists and therapists to share relevant notes while maintaining “firewalled” privacy for sensitive therapy sessions.
- Outcome Measures: Automated delivery of PHQ-9 or GAD-7 assessments to patients, with results instantly visualized in the clinician’s view.
Example: TherapyNotes provides specialized “Counseling” and “Psychiatry” note types that auto-populate based on previous sessions, allowing for a narrative flow that still meets stringent medical necessity criteria.
5. Pediatrics: Growth Chart Automation
Pediatrics is defined by the tracking of development over time. A pediatric EHR must be “family-centric” rather than just “patient-centric,” managing complex immunization schedules and parental permissions.
Investor Insight: Pediatric platforms have a high “stickiness” factor because moving decades of immunization and developmental history to a new system is a massive friction point for clinics.
PCC (Pediatric Counseling & Controls) is a standout in this niche. It automates the plotting of CDC and WHO growth charts in real-time as vitals are entered and features a robust “Immunization Forecaster” that alerts staff to upcoming or missed doses based on specific state registries.
How to Develop a Specialty EHR Software?
To develop specialty EHR software, one should first define the target specialty and map real clinical workflows so the system fits how providers actually work. Then core modules can be built with a secure architecture, and compliance must be ensured while gradually integrating devices and carefully testing with real users.
We have built specialty EHR software for a wide range of clients, and this is how we approach it.
1. Target Specialty & Use Cases
We begin by identifying the most lucrative market entry points. Our team analyzes specific pain points of a chosen specialty, such as the high-resolution imaging needs of Ophthalmology or the longitudinal tracking required in Oncology.
By narrowing the scope to “North Star” use cases, we ensure your investment focuses on high-impact features. This strategy drives immediate user adoption and creates clear market differentiation from day one.
2. Map Clinical Workflows
Our architects map the digital journey to the physical movements of a clinic. We document every touchpoint from patient intake to final reimbursement, ensuring data flows seamlessly between different staff roles.
This rigorous mapping phase allows us to build a system that acts as a natural extension of the medical team. We eliminate the friction points that typically plague generic solutions that force doctors to change how they practice.
3. Design to Minimize Fatigue
We treat click fatigue as a form of technical debt. Our designers utilize progressive disclosure and contextual UI to ensure that doctors only see what they need, exactly when they need it.
By prioritizing a zero-friction interface, we build products that actively reduce physician burnout. This is a key selling point that makes your platform the preferred choice for practice managers and hospital boards looking for efficiency.
4. Core Modules & Integrations
We build with a modular, API-first philosophy. This ensures your platform acts as the central nervous system of the practice. Our engineers specialize in native integrations with diagnostic hardware and third-party labs for real-time data ingestion.
This modularity allows your EHR to grow and adapt over time. It makes it easy to add new features or enter adjacent specialties without requiring a total architectural overhaul or massive reinvestment.
5. Compliance & Data Security
Security is the bedrock of our development process. We implement Security by Design, ensuring every build is HIPAA-compliant and audit-ready. We handle the complexities of data encryption, multi-factor authentication, and HL7/FHIR interoperability standards.
For the investor, a robust compliance framework protects the valuation of the company. It ensures your product meets the most stringent institutional requirements during future due diligence or acquisition talks.
6. User Testing & Iteration
We believe in battle-testing every feature before a full-scale commercial launch. Our team facilitates Beta deployments in real clinical environments, using heatmaps and user feedback to identify and resolve bottlenecks instantly.
This rapid iteration cycle ensures the final product is polished and practical. By the time your product hits the wider market, it has already been validated by the healthcare professionals who will use it every day.
Cost to Develop Specialty EHR Software
Investing in a specialty EHR requires a strategic capital allocation that balances immediate market entry with long-term scalability. The total investment is rarely a flat fee. It is a dynamic budget influenced by the depth of clinical logic and the complexity of the regulatory environment.
For a serious stakeholder, understanding the breakdown of these costs is the difference between a high-growth asset and a stalled project.
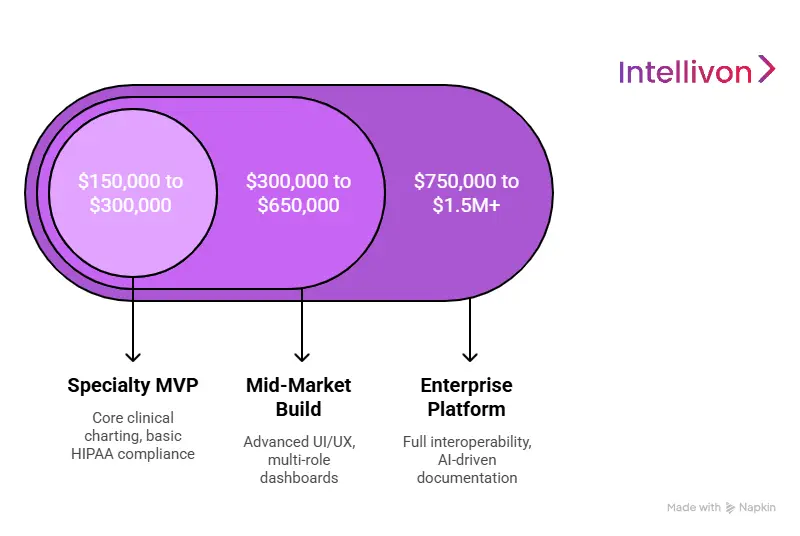
MVP vs Full-Scale Platform Cost
Launching an MVP allows you to enter the market, secure early adopters, and validate your specialty-specific features without over-committing capital. A full-scale platform is a comprehensive ecosystem designed for enterprise-level deployment.
| Development Stage | Estimated Investment | Primary Focus |
| Specialty MVP | $150,000 to $300,000 | Core clinical charting, basic HIPAA compliance, and one primary specialty module. |
| Mid-Market Build | $300,000 to $650,000 | Advanced UI/UX, multi-role dashboards, and basic lab or pharmacy integrations. |
| Enterprise Platform | $750,000 to $1.5M+ | Full interoperability (FHIR), AI-driven documentation, and high-concurrency architecture. |
Cost by Features & Integrations
The specialty in the EHR is where the most significant development costs reside. Every custom tool, such as a 3D body map for dermatology or a DICOM viewer for cardiology, requires specialized engineering and testing.
- Custom Clinical Modules: Budget $40,000 to $80,000 per specialty-specific module. This covers the logic for unique data points like growth charts or range of motion tracking.
- Third-Party Integrations: API connections to labs or imaging hardware typically cost $15,000 to $30,000 each, depending on the complexity of the data handshake.
- AI & Automation: Implementing ambient listening or smart coding assistants can add $50,000 to $120,000 to the initial build, though it significantly increases the platform’s market valuation.
Ongoing Maintenance & Scaling Costs
Post-launch expenses are not just about fixing bugs. They are about maintaining the integrity of the clinical data and staying ahead of evolving healthcare regulations. For a high-performing platform, expect to allocate 15% to 25% of your initial development cost annually for maintenance.
Investor Note:
Scaling costs often include cloud infrastructure, which grows with your patient volume. Budgeting for dedicated security audits and regular HIPAA penetration testing is mandatory to protect the asset from liability and data breaches.
Regular updates to ICD-10 and CPT code libraries also require consistent attention. As you scale to more clinics, the cost of customer support and specialized training modules will become a larger portion of the operational budget. This ensures that the software continues to deliver the high ROI that clinicians expect.
Hidden Costs of Using Generic EHR Systems
The true cost of a generic EHR isn’t the subscription fee; it’s the systemic drain on a practice’s value. Using a tool designed for a general practitioner in a specialty setting creates a “friction tax.” These hidden costs represent a major opportunity for specialized platforms to capture market share by recovering operational losses.
Lost Revenue from Inefficient Billing
Generic systems lack the “medical necessity” triggers required for complex claims, leading to consistent under-billing.
Platforms like Nextech solve this for plastic surgery by embedding charting logic that justifies higher-level procedures. Similarly, WebPT dominates physical therapy by integrating automated compliance rules specific to rehab, preventing common payment delays.
- Code Slippage: Clinicians default to lower-level codes, losing $20 to $50 per encounter.
- High Denials: Generic tools miss specialty-specific payer rules, increasing rejections by 10% to 15%.
- Admin Bloat: Practices must hire extra staff to manually correct errors a specialized EHR would catch at the point of care.
Staff Burnout Due to Poor UX
The most expensive asset is the provider. When a specialist spends 2 hours every evening finishing charts due to a clunky interface, the practice is burning its most valuable capital.
Economic Impact: Physician turnover is costly. Recruiting a new specialist can exceed $250,000, excluding lost patient revenue during the gap.
- Poor UX trickles down to all staff. Jane App gained traction in mental health by using a “human-first” interface that reduces this emotional burden.
- In oncology, Flatiron Health streamlines workflows by surfacing chemotherapy protocols directly, sparing doctors from digging through irrelevant generic menus.
Time Wasted on Workarounds
When software fails a specialist, staff build “shadow systems.” These workarounds are inefficient, insecure, and create data silos.
- Manual Entry: Transcribing data from diagnostic devices because the EHR lacks native integration.
- Paper Trails: Reverting to paper for specialized measurements, which must be scanned later.
- Third-Party Tools: Paying for extra plug-ins to handle tasks like patient engagement.
Every minute on a workaround is a minute not spent on billable activity. In high-volume clinics, these increments add up to hundreds of hours of lost productivity annually.
Who Should Invest in Specialty EHR Software?
The transition to a specialty EHR is a strategic pivot toward operational excellence. While generic models satisfy basic regulatory needs, they act as a ceiling on growth for high complexity practices. Identifying your investment bracket depends on your data demands and long-term scaling objectives.
Scaling Independent Specialists
For a growing practice, the EHR is the foundational infrastructure. The goal is to commoditize the lead physician’s “clinical secret sauce” so new associates can provide identical efficiency.
- Standardization: Custom templates ensure every provider follows the same high-standard diagnostic protocol.
- Asset Value: A proprietary or specialized platform increases the “book value” of the practice during a private equity exit.
- Example: A surgical group might use ModMed to ensure every surgeon captures the exact range of motion data required for high reimbursement claims.
Overcoming Generic Limitations
Many established clinics reach a breaking point where workarounds cost more than a new system. If staff spend more time on manual data entry than patient interaction, a specialty-first overhaul is required.
| Problem Area | Generic EHR Impact | Specialty EHR Solution |
| Data Entry | Manual transcription from devices. | Automated IoT and device integration. |
| User Interface | Irrelevant fields for every patient. | Context-aware, specialty only fields. |
| Compliance | Templates lack niche detail. | Built in protocols for specific boards. |
| Patient Flow | Linear, rigid scheduling. | Optimized for specialty visit types. |
Operational Insight: When a clinic transitions to a niche tool like WebPT for physical therapy, they often see an immediate reduction in “Days in AR” because documentation is inherently cleaner and more compliant.
HealthTech Startups Targeting Niche Markets
Entrepreneurs should look where the “Goliaths” are weakest. Large EHR providers cannot afford to build deep functionality for every micro-specialty, creating a “Blue Ocean” for verticalized startups.
By focusing on deep clinical logic, a startup achieves high “stickiness” and low churn. Flatiron Health proved this in oncology; by structuring cancer data, something generic EHRs struggle with, they created a platform so valuable it led to a multi-billion dollar acquisition.
Startups should prioritize:
- Unique Data Sets: Capturing information others ignore, like genetic markers or therapy outcomes.
- Workflow Monopolies: Handling a specific surgical workflow from end to end.
- Niche Integration: Connecting the specialist to a specific ecosystem of labs and insurers.
Signs Your Practice Needs a Specialty EHR Software
Identifying the right time to transition to specialty EHR software is critical for maintaining operational health. When a generic system begins to feel like a hurdle rather than a tool, it is likely leaking revenue and productivity. Recognizing these specific red flags allows you to quantify the need for an upgrade before clinical quality or staff morale suffers.
1. High Documentation Time
When clinicians spend more time clicking than treating, the EHR has failed. Generic systems force doctors to navigate irrelevant tabs to find specialty-specific fields.
If providers consistently stay late for “pajama time” charting, the system lacks the macros and templates required for your niche. Transitioning to a tool like Nextech for ophthalmology can cut charting time significantly by using drawing tools that automatically generate clinical text.
2. Coding Errors & Denials
Generic EHRs often lack the nuanced rules engine required for specialty billing. This results in “down-coding” to stay safe or frequent “hard denials” from payers who require specific clinical justifications.
High denial rates are a symptom of software that doesn’t prompt for mandatory specialty data. For example, WebPT helps rehab therapists avoid these traps by flagging missing functional limitation G-codes before a claim is submitted, ensuring a higher first-pass clean claim rate.
3. Poor Clinical Workflows
Software should mirror the physical movement of your clinic. If your team uses “sticky notes,” spreadsheets, or paper charts to track specialized data, your EHR is a poor fit.
This friction is evident in fields like mental health or pediatrics, where longitudinal tracking is key. Platforms like PCC for pediatrics integrate growth charts and immunization registries directly into the workflow. This eliminates the need for external workarounds and ensures the clinical record remains a single source of truth.
How Specialty EHR Software Reduces Admin Overhead?
Specialty EHR software reduces admin overhead by aligning workflows with specific clinical processes, which helps automate documentation, orders, and routine tasks. It reduces manual data entry through integrations and smart templates, improving accuracy and saving time.
It also enables faster coordination across care teams, which minimizes delays and reduces repetitive administrative work.
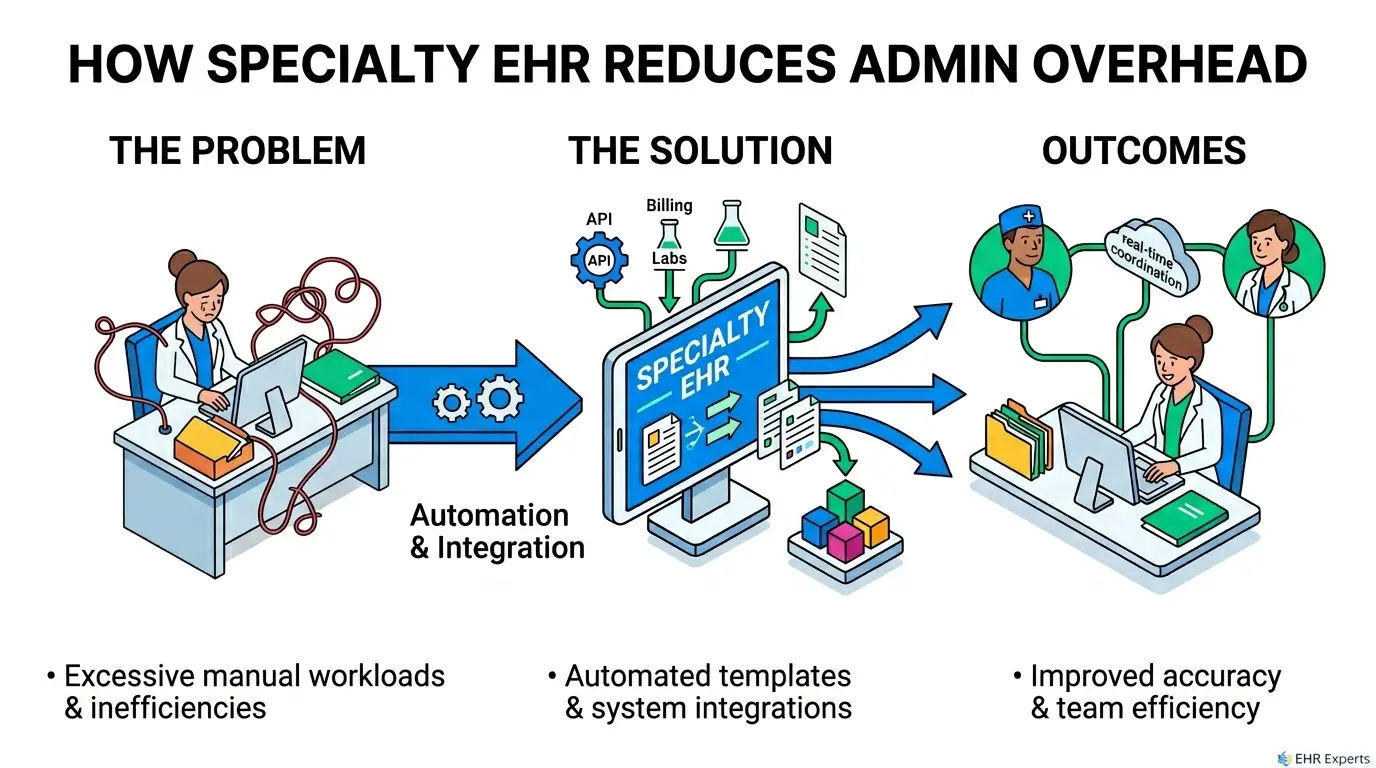
Automating Repetitive Clinical Tasks
Generic systems treat every patient encounter as a blank slate, forcing doctors to re-enter data or click through irrelevant screens. Specialized systems use “smart logic” to predict the next step in a specific clinical pathway.
- One-Click Charting: Pre-configured templates for common specialty complaints (e.g., a “Glaucoma Follow-up” in Nextech) allow providers to finish charts in seconds rather than minutes.
- Auto-Generated Orders: When a specific diagnosis is entered, the system automatically queues the correct labs, prescriptions, and follow-up instructions typical for that niche.
- Example: In a pediatric setting, PCC automatically calculates medication dosages based on the latest weight entry, removing the need for manual math and double-checking.
Reducing Manual Data Entry Errors
Manual data entry is the “silent killer” of clinical efficiency. When staff must transcribe results from a diagnostic device into a generic text field, the risk of transposition errors skyrockets.
The Integration Advantage: A specialty-focused EHR acts as a hub for niche medical hardware. Instead of a technician typing numbers into a box, the data flows directly from the device to the patient’s digital record.
| Feature | Generic EHR Impact | Specialty EHR Impact |
| Lab Results | PDF attachment; manual typing. | Direct data mapping to discrete fields. |
| Imaging | External viewer required. | Native DICOM support within the chart. |
| Vitals | Manual entry by nursing staff. | Bluetooth/IoT sync from monitors. |
Streamlining Care Team Collaboration
A specialty clinic is an ecosystem of surgeons, nurses, therapists, and billers. When the software understands these specific roles, communication becomes instantaneous rather than a series of phone calls or physical “handoffs.”
- For instance, Jane App streamlines the transition from a therapy session to front-desk checkout by automatically updating the billing queue the moment a practitioner signs a note.
- In complex environments like oncology, Flatiron Health allows the infusion nurse and the oncologist to view the same real-time treatment plan, ensuring that chemotherapy doses are adjusted instantly based on the morning’s lab results without a single internal email.
How Custom EHRs Improve Patient Experience?
The ultimate measure of any clinical tool is its impact on the patient. While generic systems turn doctors into data entry clerks, specialty EHR software is designed to disappear. By streamlining technical tasks, these platforms return the focus to the human connection and transform a cold encounter into a collaborative journey.
1. Faster Consultations
Patients judge care quality bysoftware is, eye contact, and engagement. Generic EHRs with endless nested menus force doctors to hunt for data during the exam, breaking the rapport.
- Intelligent Surfacing: Custom systems pull relevant history to the front based on the specific appointment type.
- Voice to Chart: Specialized ambient listening understands niche terminology, allowing the doctor to speak naturally while the system charts.
- Result: The consultation feels like a conversation rather than an interrogation. Patients leave feeling heard instead of being treated like a data point.
2. Personalized Care Plans
A specialized system interprets data within the context of a specific condition. This leads to data-driven, highly individualized care plans that generic systems simply cannot support.
The Precision Factor: Specialized software tracks unique biomarkers or progress metrics. This allows for course corrections in treatment long before a generic system would flag an anomaly.
| Feature | Impact on Patient Trust |
| Visual Progress | Patients see improvement through specialized graphs or image overlays. |
| Niche Education | Automated delivery of handouts specific to the exact diagnosis. |
| Error Prevention | Real-time alerts for contraindications specific to specialty medications. |
3. Better Follow Ups with Structured Data
The patient experience continues after they leave. Custom EHRs use structured data to ensure the loop is closed on every aspect of care, automating the tedious tasks that often fall through the cracks.
- Automated Recalls: The system identifies patients due for screenings based on their unique clinical history.
- Remote Monitoring: Data from wearables or home equipment flows directly into the portal for proactive outreach.
- Pharmacy Coordination: Prescriptions are sent with specialty instructions attached, reducing confusion at the counter.
By leveraging structured data, the practice ensures a consistent, high-touch experience. This proactive approach builds long-term loyalty and significantly improves clinical outcomes.
Why Choose Intellivon for Specialty EHR Software?
Selecting a partner for specialty EHR software is a high-stakes decision for operational health. Intellivon provides the technical precision and clinical insight to turn complex challenges into seamless digital tools. We build the modern infrastructure required for high-performing specialty practices.
Proven HealthTech Experience
We architect robust platforms that handle sensitive data with zero friction. With over 500,000 hours of coding experience, our team of ex-MAANG/FAANG developers applies world-class engineering rigor to your clinical needs. This ensures your platform is built on an elite foundation from day one.
Workflow-First Design
Generic software forces your team to adapt; we build the tool to adapt to you. Our design centers on the unique physical and digital movements of your specific clinic. By eliminating redundant clicks, we create an interface that acts as a natural extension of the provider, not a barrier.
Compliance-Ready & Scalable
Security and growth are non-negotiable in healthcare. Our approach prioritizes HIPAA compliance and encryption at every layer while ensuring the architecture is ready to scale. Whether managing one clinic or a national enterprise, our systems expand without compromising performance.
Conclusion
Developing specialty EHR software is an investment in the long-term viability of a practice. By moving away from rigid, generic systems, providers can reclaim their time, secure their revenue, and focus entirely on patient outcomes. With the right technical partner to bridge the gap between complex coding and clinical intuition, a custom solution becomes the most powerful asset in a specialist’s toolkit.
FAQs
Q1: How to develop an EHR system?
A1: Developing an EHR requires a phased approach: discovery to map specialty workflows, choosing a secure tech stack, and building a HIPAA-compliant architecture. The process involves designing intuitive UI/UX, integrating with labs or pharmacies, and conducting rigorous security testing before deployment to ensure data integrity and regulatory adherence.
Q2: What are the 4 types of EMR?
A2: Electronic Medical Records generally fall into four categories: General EMRs for primary care, Specialty-Specific EMRs tailored for niches like cardiology, Cloud-Based EMRs accessible via the web, and On-Premise EMRs hosted on local servers. Each varies in its ability to handle complex data and workflow customization.
Q3: What are the 5 components of the EHR system?
A3: A robust EHR consists of five core pillars: Administrative System (scheduling/billing), Clinical Documentation (notes/charting), Order Management (prescriptions/labs), Decision Support (alerts/clinical logic), and Patient Engagement (portals/communication). These work together to centralize the patient journey.
Q4: What is the difference between an EHR and an EMR?
A4: An EMR is a digital version of a patient’s chart used within a single practice, primarily for diagnosis and treatment. An EHR is designed to be interoperable, allowing patient data to move securely between different healthcare providers, specialists, and laboratories to provide a holistic view of the patient’s health.