Modern healthcare is not short on data; instead, it is struggling to connect it meaningfully in real-time. Doctors often switch between systems during consultations, and this can quietly slow decisions. Patients may wait while providers piece together fragmented records across tools.
A lot of healthcare institutions have started integrating telehealth in EHR systems because patient demand for remote care is rising, and providers need faster access to unified records. Virtual visits can run inside the same system where the patient’s history already exists. Data from each interaction should update instantly and support more consistent clinical decisions. Over time, this approach can gradually create a more connected and reliable care delivery model.
We’ve worked with multiple healthcare institutions and helped them integrate telehealth with their EHR systems. As we have years of expertise, we’re sharing this blog to discuss the steps to develop telehealth integration with EHR.
Why Telehealth-EHR Integration Is No Longer Optional?
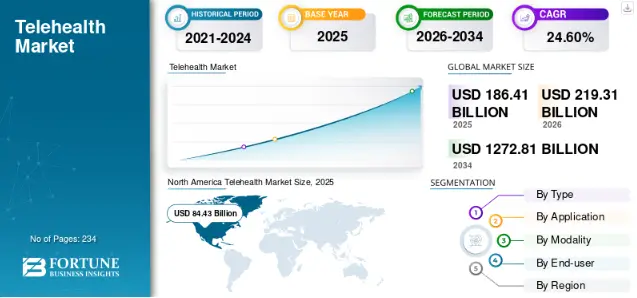
Source: Fortune Business Insights
As North America continues to dominate this space, the shift from standalone video tools to deeply integrated ecosystems has become a mandate for survival. For investors, a platform lacking native EHR connectivity is a strategic liability that ignores the operational needs of high-volume medical practices.
True integration ensures bi-directional data flow between virtual encounters and permanent records, forming the bedrock of scalability and enterprise appeal. By automating workflows, these systems reduce provider burnout, secure audit trails for billing, and eliminate the “shadow costs” of manual data entry. Moving beyond mere convenience, integrated platforms offer a defensible business model that secures data integrity and long-term clinical value.
The Cost of Disconnected Systems
The financial friction of fragmented systems is often obscured until a platform attempts to scale. When telehealth and EHR systems are disconnected, shadow costs accumulate through administrative bloat and data errors.
- Manual Data Re-entry: Clinicians are forced to spend valuable time copying data from the video platform into the EHR. This double-entry system is a waste of expensive labor and an incubator for human error.
- Billing Delays and Denials: Insurance reimbursement hinges on precise documentation. If the telehealth platform does not sync the proof of encounter with the EHR billing module, the resulting lag impacts cash flow.
- Siloed Intelligence: Predictive analytics rely on comprehensive data sets. In a disconnected system, the telehealth platform is blind to historical lab results and medication history. This renders advanced diagnostic tools less effective.
Real-world implementation proves these costs are avoidable. For instance, Kaiser Permanente treats telehealth as a core component of its KP HealthConnect EHR system rather than an add-on. This integration allowed them to handle over 30,000 video visits per day during peak periods without losing data continuity or administrative control.
Modern Patient Expectations
Today’s healthcare consumer compares their medical experience to digital banking and retail. They expect a frictionless journey where their information follows them across every medium.
A patient assumes a doctor has their full history at their fingertips. When a provider must ask for medication lists because the tool does not talk to the EHR, it erodes trust. Integration allows for a personalized experience through automated check-ins and instant access to results. These are the primary drivers of patient retention in a competitive market.
Cleveland Clinic provides a strategic example of meeting these expectations. By embedding their telehealth workflows directly into their Epic EHR platform, they ensured that patients could access “Express Care Online” and have those visits instantly reflected in their global medical record.
Improving Clinical Outcomes
Healthcare is an information business. The quality of a clinical decision is proportional to the accessibility of data at the moment of care. Integration transforms a telehealth session into a high-fidelity clinical encounter.
With a unified system, a physician can review real-time biometric data alongside historical trends during the call. This allows for immediate interventions without toggling between tabs. For chronic disease management, this continuous loop of data prevents hospitalizations. By ensuring data reaches the right person at the right time, integrated platforms move beyond convenience to become essential clinical tools.
What Is Telehealth Integration Within an EHR?
Telehealth integration is the architectural embedding of virtual care directly into the clinician’s primary workspace. It is not an add-on or a side-by-side window. It is a unified environment where the video interface, patient charts, and diagnostic tools operate as a single cohesive unit.
For a healthcare business, this means building a system where the visit is a data point in a continuous clinical narrative. When a platform is integrated, the physician never leaves the EHR to initiate a call. Data such as visit duration and clinical notes populate the patient’s history automatically. This removes the software toggling that causes administrative fatigue.
Evolving Beyond Video Calls
Basic video consultations are a commodity, while integrated care is a high-value asset. A standard call is only a communication channel. In contrast, an integrated solution treats the video stream as a data-gathering tool.
- Contextual Awareness: The system pulls relevant data like allergies and recent labs into the clinician’s view as the call starts.
- In-App Documentation: Clinicians can chart in real time within the interface using pre-populated templates.
- Resource Optimization: Integration allows for automated virtual rooming where medical assistants intake patients before the doctor joins.
Core Unified Workflow Components
A unified workflow handles the entire patient journey without data leakage. From an investor’s perspective, the strength of a platform lies in the automation of these components.
- Unified Scheduling: Appointments booked through a portal appear instantly in the EHR calendar with secure links.
- Digital Intake: Pre-visit forms and legal consents are signed digitally and saved directly to the patient file.
- Integrated Order Entry: Physicians send e-prescriptions or order lab work without closing the video window.
How Data Sync Happens in Real Time
Real-time synchronization relies on robust API frameworks using industry standards like HL7 or FHIR. This allows the telehealth platform to speak the same language as the EHR.
When a doctor updates a patient’s vitals during a call, that information is sent via an encrypted hook to the EHR database. This ensures the data is immediately available to other providers in the care network.
For a business owner, this technical depth creates stickiness with enterprise clients by guaranteeing data accuracy and fulfilling regulatory requirements.
Must-Have Features in Telehealth-Integrated EHR Systems
The competitive value of EHR systems with telehealth integration lies in reducing manual tasks and streamlining the provider experience. For an entrepreneur, these features represent the technical benchmarks required to achieve high ROI and market penetration.
1. One-Click Patient Visits
Efficiency begins with the user interface. A one-click system allows clinicians to launch a secure session directly from the digital chart. This eliminates the need to manage external meeting IDs or secondary logins. For the enterprise, this reduces technical friction and increases the daily patient volume a provider can manage.
2. Real-Time Chart Access
During a consultation, physicians need a 360-degree view of the patient without losing visual contact. The platform should display historical data, recent lab results, and immunization records alongside the video feed. This ensures clinical decisions are informed by the patient’s full history, significantly reducing diagnostic errors.
3. Automated Clinical Notes
The most significant drain on a provider’s time is charting. Advanced systems use structured data fields that sync automatically. When a clinician enters notes during a call, the system should auto-populate the relevant sections of the record. This ensures the file is updated the moment the session ends, keeping the clinic audit-ready.
4. Integrated Scripts and Billing
A telehealth encounter is not complete until the treatment is ordered and the visit is billed. Integrated tools allow doctors to send scripts to a pharmacy without leaving the video interface. Simultaneously, the system should generate a claim based on visit complexity, ensuring rapid reimbursement and reducing coding errors.
5. Remote Patient Monitoring
The future of virtual care lies in continuous data. Integration with RPM tools allows wearable data, such as heart rate or glucose levels to flow directly into the patient record. This gives clinicians a real-time dashboard of patient health, allowing for proactive interventions before a condition escalates into an emergency.
6. Secure Follow-Up Messaging
Post-visit engagement is critical for patient outcomes and retention. Integrated secure messaging ensures all follow-up communication is encrypted and stored as part of the legal medical record. This provides a clear trail of communication, which is vital for both care coordination and legal defensibility in a professional setting.
How to Develop Telehealth Integration with EHR?
Building a telehealth integration with EHR starts with designing interoperable APIs and data exchange layers that can securely sync patient records in real time. The system should gradually align video workflows with clinical data pipelines so consultations may reliably update records and improve care decisions.
We have worked with several healthcare organizations to develop telehealth integration with EHR systems, and here is how it is done.
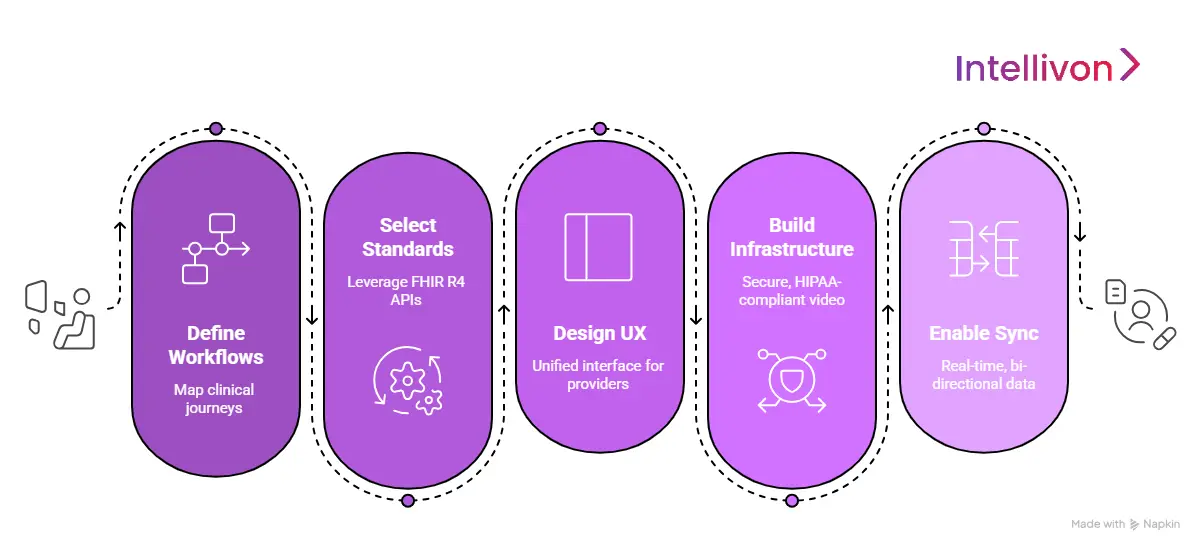
1. Defining High-Impact Workflows
We begin by mapping the specific clinical journeys unique to your business model. Whether targeting primary care or chronic management, we identify every friction point from intake to discharge. This ensures our development efforts solve actual operational bottlenecks.
2. Selecting Interoperability Standards
Longevity in health tech requires a FHIR-first approach. We leverage modern standards like FHIR R4 and secure RESTful APIs to ensure your platform communicates with major providers like Epic or Cerner. These universal protocols ensure your platform remains compliant with 2026 regulations.
3. Designing a Unified UX
Our design philosophy centers on a single pane of glass experience. For providers, we build interfaces that keep the video feed and patient chart in one view. For patients, we create a mobile-first digital front door that makes joining a visit as simple as answering a text.
4. Building Secure Infrastructure
Security is the foundation of patient trust. We deploy HIPAA-compliant, encrypted video infrastructure using WebRTC and medical-grade SDKs for high fidelity in low-bandwidth areas. This includes secure waiting rooms and encrypted file-sharing modules that meet the highest privacy standards.
5. Enabling Real-Time Data Sync
We bridge the gap between consultation and documentation through automated, bi-directional sync. When a doctor updates a diagnosis during a call, our system triggers secure webhooks that update the EHR instantly. This eliminates manual re-entry and ensures the clinical record is always live.
6. Validating Security and Performance
Before launch, we conduct rigorous stress tests and compliance audits. This includes end-to-end penetration testing and SOC2 Type II verification to ensure the system scales to thousands of concurrent users. This validation satisfies institutional requirements and paves the way for market expansion.
Cost to Develop Telehealth Integration with EHR
Estimating costs for telehealth integrated EHR systems depends on data complexity rather than just video functionality. A basic MVP starts lower, but a sophisticated, bi-directional system for clinics typically ranges from $150,000 to $350,000. This ensures the platform is a core medical tool, not just a call app.
Feature and Complexity Costs
Budgets are usually split across four development pillars. Understanding these is essential for assessing capital deployment:
- Core Architecture ($80,000 to $150,000): Covers the backend, video engine, and clinical dashboard.
- Interoperability & Mapping ($30,000 to $75,000): Ensures the tool and EHR speak the same language via FHIR/HL7.
- Compliance & Security ($20,000 to $40,000): HIPAA audits and SOC2 verification. Security is a non-negotiable expense.
- QA & Load Testing ($15,000 to $25,000): Ensures 99.9% uptime during peak clinical hours.
Cost Impact Factors
Budget variances are driven by three strategic choices:
Bi-Directional vs. One-Way Sync: One-way sync is cheaper, but bi-directional sync allows doctors to update charts during a call. This doubles the development effort but triples the market value.
The number of connected systems also creates an exponential effect. Integrating with one EHR like Epic is a controlled cost. Connecting to multiple legacy systems requires a middleware layer that can push costs toward $500,000. Team location also shifts hourly rates from $30 to over $150.
Timeline and Team Structure
Professional integration is a marathon. A robust MVP takes 6 to 9 months, while a full enterprise rollout can take 12 months.
A specialized team is required to hit these milestones:
| Role | Responsibility |
| Project Manager | Aligns clinical needs with technical output. |
| Integration Architect | Manages FHIR/HL7 mapping and APIs. |
| Backend Engineers (2-3) | Build the secure, scalable engine. |
| UX/UI Designer | Creates the clinician interface. |
| DevOps & Security | Maintains HIPAA-compliant cloud infra. |
| QA Engineer | Conducts bug-squashing and latency testing. |
Architecture Behind Telehealth-EHR Integration
When we design telehealth embedded EHR systems for our clients, we move away from monolithic builds. Instead, we utilize a modular architecture where the video interface and the data layer are decoupled. This allows for independent scaling and ensures that a spike in video traffic never compromises the integrity of the patient’s medical records.
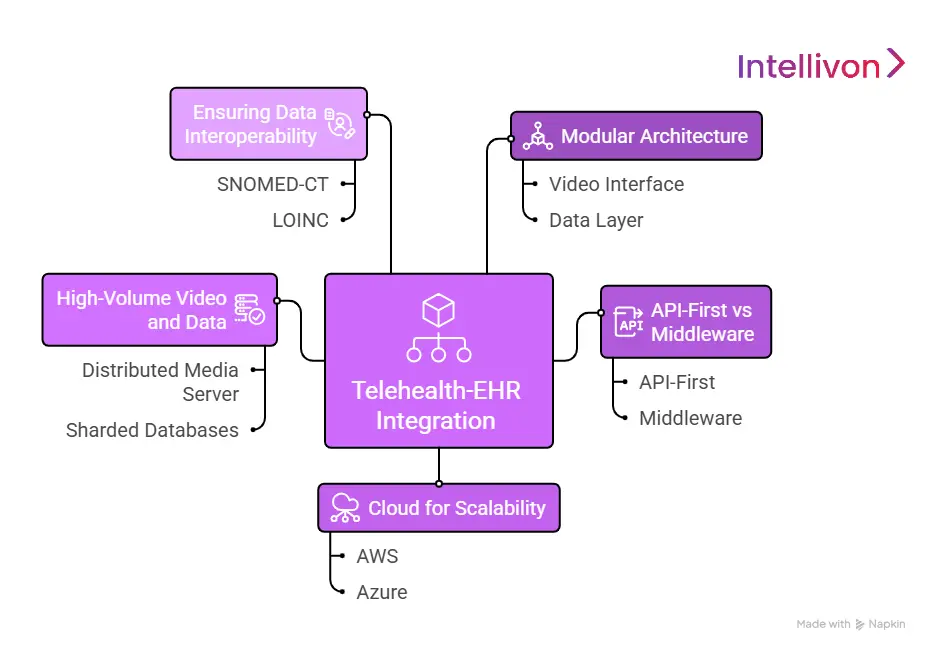
API-First vs Middleware
An API-first approach uses direct, secure connections like FHIR or REST to link the telehealth tool to the EHR. This is ideal for modern EHRs that offer robust developer portals. In contrast, middleware-based integration uses an intermediary layer to translate data between older legacy systems and your platform.
- API-First: Best for modern, cloud-native EHRs; lower latency; easier to maintain.
- Middleware: Best for large hospital networks; handles legacy protocols; acts as a universal translator.
Cloud for Scalability
We utilize auto-scaling cloud infrastructure, typically AWS or Azure, to manage fluctuating patient volumes. By using serverless functions and containerized microservices, the system can spin up additional resources during peak hours and scale down at night. This ensures 99.9% uptime while optimizing cloud costs for our clients.
High-Volume Video and Data
Handling thousands of simultaneous video feeds requires a distributed media server architecture. We implement WebRTC protocols with a STUN/TURN server configuration to bypass firewalls and reduce latency.
Technical Note: For patient data, we use sharded databases that distribute the processing load. This ensures that retrieval of clinical charts remains instantaneous even under heavy load, preventing the dreaded “spinning wheel” during a live consultation.
Ensuring Data Interoperability
Interoperability is achieved by strictly adhering to the standard pillars of health data exchange.
We map all incoming telehealth data to standardized terminologies like SNOMED-CT for clinical findings and LOINC for lab results. This ensures that the data generated in your platform is readable by any other healthcare system, fulfilling the promise of a unified longitudinal patient record.
Turning Telehealth Into a Native EHR Workflow Layer
The efficiency of modern EHR systems is measured by the speed at which a clinician can transition from reviewing data to treating a patient.
A one-click architecture removes the technical barriers that traditionally haunt telehealth sessions. By embedding the “Join Visit” trigger directly into the patient’s digital chart, the software transforms a complex video call into a simple clinical event.
Why Add-On Tools Fail at Scale
Standalone apps often create data silos that frustrate clinicians and complicate billing. When a telehealth tool operates outside of the core EHR systems, it forces providers to manually transfer notes and update charts after the visit. This redundancy leads to:
- Data Fragmentation: Critical patient history is trapped in a secondary app.
- Increased Burnout: Double documentation adds hours to the clinical day.
- Compliance Risk: Disconnected logs make audit trails difficult to verify.
Embedding Virtual Care Into Daily Routines
Successful integration means the virtual visit is a natural extension of the physical clinic schedule. When telehealth is embedded, a doctor can see a list of in-person and remote patients in a single queue. Launching a session happens within the existing charting environment, allowing the provider to maintain clinical focus without switching browser tabs.
Major institutions have already demonstrated the power of this native approach. For example,
- Cleveland Clinic transitioned its Express Care Online directly into its primary Epic environment. This allows clinicians to pull up longitudinal data and order labs during a video call without ever leaving the patient’s chart.
- Similarly, Kaiser Permanente utilizes integrated video layers to ensure that every virtual interaction is captured in its central database, allowing for seamless follow-ups between primary care and specialty departments.
A Single Interface for All Interactions
The single pane of glass philosophy is the benchmark of high-quality health tech. This design brings together the video feed, the longitudinal patient record, and the prescription module into one view.
Workflow Impact: By unifying the interface, a clinician can review lab results and update the treatment plan in real time during the conversation. This ensures the patient record is updated the moment the session ends, keeping the clinic efficient and audit-ready.
Enabling One-Click Virtual Visits from Patient Charts
Efficiency in telehealth integrated EHR systems is defined by how quickly clinicians move from reviewing data to delivering care. A one-click architecture removes the technical barriers that traditionally haunt virtual care. By embedding the “Join Visit” trigger directly into the patient’s digital chart, the software transforms a complex video call into a simple clinical event.
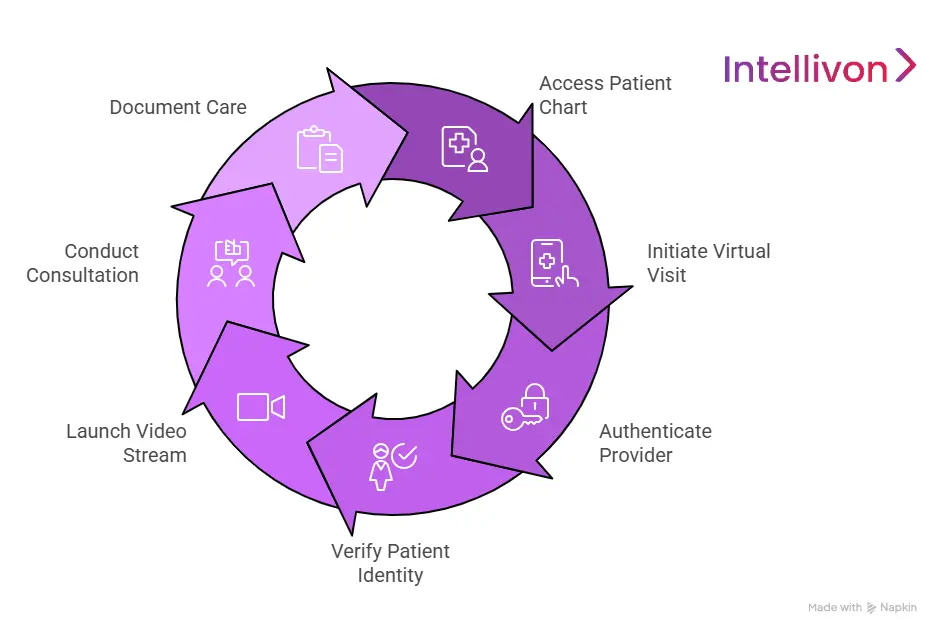
Launching Consultations Within the EHR
A native integration ensures that the video window exists as a component of the existing medical record. There are no secondary logins or external meeting links to manage. When a provider clicks the visit icon, the system automatically:
- Authenticates the provider’s credentials.
- Verifies the patient’s identity via the EHR record.
- Opens a secure, encrypted video stream in a dedicated frame.
Reducing Time-to-Consultation
Minimizing the “digital distance” between the doctor and patient is critical for high-volume clinics. Every second spent searching for a link is a second lost to patient care.
| Feature | Standalone Tool | Integrated EHR System |
| Login Process | Separate username/password | Single Sign-On (SSO) |
| Meeting Setup | Copy/paste link to the patient | Automated SMS/Email trigger |
| Visit Start Time | 2 to 4 minutes | Under 15 seconds |
Eliminating Context Switching
Context switching is the primary driver of cognitive load and medical errors. When a provider has to toggle between a video app and a patient’s history, they lose the ability to maintain eye contact and clinical focus.
Efficiency Rule: A professional telehealth-EHR interface should allow the provider to view lab results, document symptoms, and see the patient simultaneously.
By keeping all tools in one view, the system eliminates the “tab-shuffling” that leads to burnout. This unified approach ensures that the provider remains present with the patient while the EHR systems handle the data synchronization in the background.
Automating Documentation, Billing, and Prescriptions
The true ROI of integrated EHR systems lies in eliminating manual data entry. When a clinician closes a virtual visit, the system should already have the documentation, billing, and prescriptions queued for final approval. This automation ensures the provider stays focused on the patient rather than on a keyboard.
Capturing Session Notes
Traditional virtual care requires providers to toggle between video and the chart. Integrated systems remove this hurdle with a sidebar for real-time charting. Major institutions have already refined this process:
- Mayo Clinic: By integrating video directly into their unified platform, specialists can document complex cases while maintaining a high-definition visual connection.
- Jefferson Health: Their JeffConnect system ensures every virtual consult is automatically appended to the patient’s longitudinal record, removing the risk of lost notes between systems.
Auto-Generating Billing Codes
Billing is often where standalone tools fail, leading to lost revenue. Integration allows the system to calculate complexity and duration to suggest correct CPT codes.
The Billing Flow:
- Time Tracking: The system logs the exact duration of the encounter.
- Code Suggestion: Based on the diagnosis, the system suggests codes like 99213 or 99214.
- Validation: The platform checks for telehealth modifiers to ensure claims aren’t rejected.
Instant ePrescriptions
Sending a prescription should not require leaving the video window. In a fully integrated environment, the eRx module is a native component of the interface.
| Action | Manual Workflow | Integrated Workflow |
| Pharmacy Search | Ask patient; check secondary app | Pulled from patient profile |
| Drug Interaction | Manual check | Real-time EHR history cross-reference |
| Submission | External portal | One-click digital transmission |
This seamless loop ensures that by the time the patient hangs up, their medication is already being processed at their pharmacy.
Ensuring Every Interaction Is Instantly Documented in EHR Systems
Adopting EHR systems with telehealth integration is the only way to prevent the inevitable data loss that occurs when virtual care is decoupled from the primary record.
This professional-grade integration makes the documentation process invisible and automatic. It ensures that the moment a session ends, the patient’s longitudinal record is already accurate and up to date.
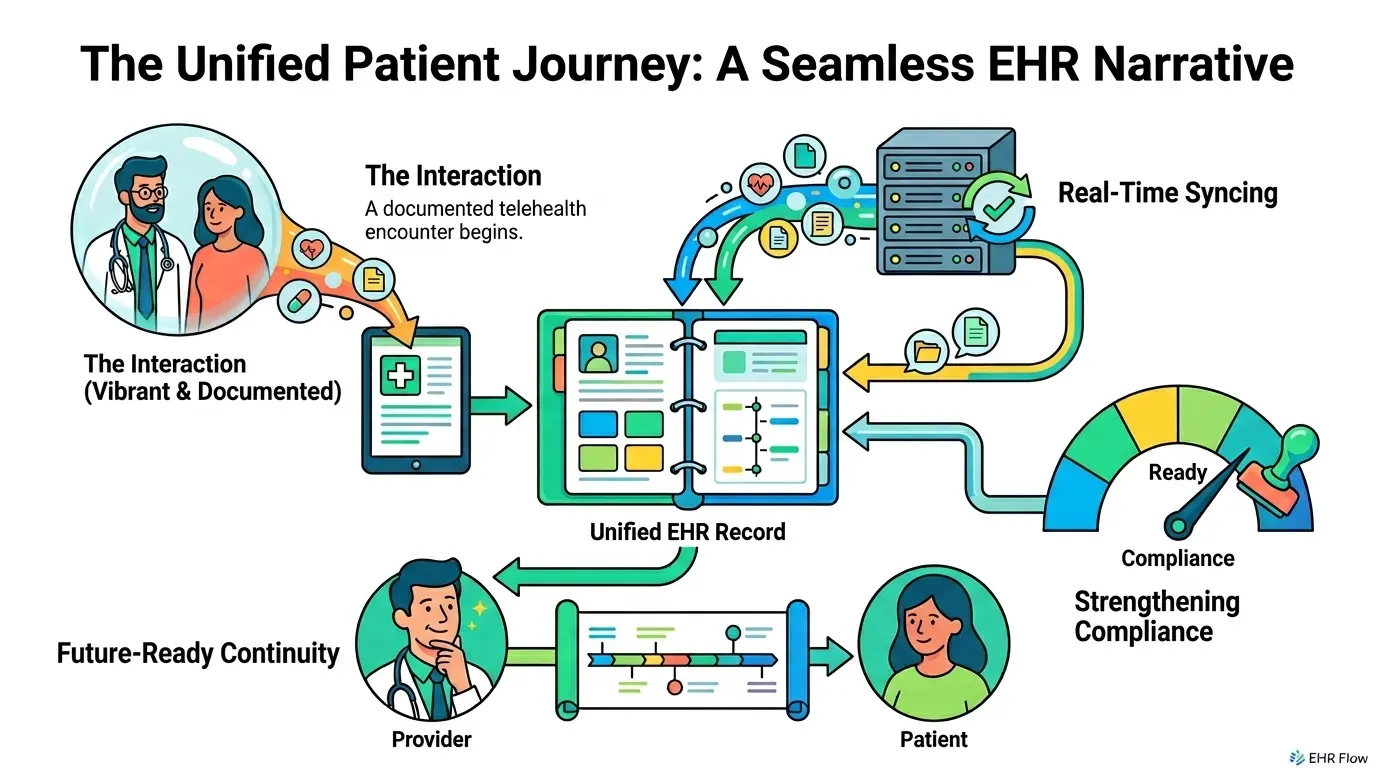
Auto-Saving Visit Records
Real-time synchronization eliminates the documentation gap that occurs when providers wait until the end of the day to update charts.
- Live Data Sync: Every action taken during the call, from updating a problem list to logging vitals, is pushed to the EHR immediately.
- Media Linking: Video recordings or snapshots taken during the consult are automatically tagged and stored within the specific encounter folder.
- Session Metadata: The system logs technical details like start and end times and participant IDs, creating a robust digital footprint for every visit.
Maintaining Compliance Through Logs
Accurate, automated logging is the strongest defense during a clinical or financial audit.
- Audit Trails: Integrated systems generate a chronological log of who accessed the record and what changes were made during the telehealth session.
- Consent Documentation: Patient consent for virtual care is captured digitally and stored as a mandatory legal artifact within the EHR.
- Version Control: Any post-visit edits to the clinical notes are tracked as separate versions, preserving the integrity of the original consultation data.
Improving Continuity of Care
Unified records ensure that a patient’s journey is seamless, regardless of whether they are seen in person or on a screen.
- Unified Patient View: Providers at Mayo Clinic use integrated systems to ensure that a specialist in one department can immediately see the notes from a telehealth urgent care visit.
- Informed Referrals: When a virtual primary care doctor refers a patient to a specialist, the specialist has instant access to the telehealth recording and notes.
- Handoff Efficiency: Institutions like Jefferson Health use these integrated logs to facilitate smoother handoffs between shift changes, as all remote interaction data is centralized.
Why Choose Intellivon for Telehealth Integration with EHR?
Selecting the right partner for telehealth EHR integration is a strategic decision. It impacts both clinical safety and business scalability. Intellivon provides the technical depth to turn complex medical workflows into seamless digital experiences.
Integrated Care Expertise
With over 500,000 hours of coding experience, our team specializes in high-concurrency platforms. Having delivered over 500 AI and healthcare projects, we build clinical-grade systems that bridge video calls and deep EHR data.
Compliance-Ready Development
Security is built into our code foundation, not added later. Led by ex-MAANG/FAANG developers, our process adheres to HIPAA, SOC2, and GDPR standards. This ensures every byte of patient data is encrypted and protected.
End-to-End Delivery
Our partnership extends from initial strategy through post-launch optimization. By managing the full lifecycle, including legacy mapping and load testing, we ensure stability under high volumes. This approach guarantees a reliable and innovative solution.
Conclusion
Developing EHR systems with telehealth integration requires a transition from fragmented silos to a unified digital architecture. Success depends on selecting a partner that understands the intersection of clinical workflows, high-concurrency engineering, and strict data security. By prioritizing a “native-first” approach, organizations can reduce provider burnout, ensure continuous compliance, and deliver a superior patient experience that scales alongside their clinical needs.
FAQs
Q1: What are the three types of telemedicine?
A1: Telemedicine generally includes store-and-forward, remote monitoring, and real-time interactive services. Store-and-forward involves sharing data like images for later review. Remote monitoring tracks patient vitals from a distance. Real-time interactive telemedicine is the most common, involving live video or audio consultations.
Q2: What is a telehealth integrated EHR system?
A2: An EHR system with telehealth integration is a unified platform where virtual care is built into the medical record. Instead of using separate apps, clinicians launch visits and view charts in one interface. This ensures every virtual interaction is instantly captured in the patient’s permanent history.
Q3: What is the difference between telemedicine and telehealth?
A3: Telemedicine refers specifically to remote clinical services, such as a doctor diagnosing a patient via video. Telehealth is a broader term that includes telemedicine plus non-clinical elements like provider training and administrative meetings. Essentially, all telemedicine is telehealth, but not all telehealth is telemedicine.
Q4: What are the three types of EHRs?
A4: The three primary types are cloud-based, on-premise, and open-source configurations. Cloud-based systems offer high scalability for remote care via the internet. On-premise systems are installed on local servers for total data control. Open-source systems allow for deep customization of the source code to fit unique clinical workflows.