Healthcare platforms in enterprises fail not because of bad technology, but because of incomplete technology. This might look something like a scheduling tool that doesn’t connect to billing, or an EHR that can’t push data to the front desk. This dilemma results in a system that creates more problems than it can resolve.
Consequently, the features that are built into an EHR and practice management platform determine everything. They shape how fast providers document, how accurately claims get submitted, how well patient data flows across departments, and how confidently a health system scales.
For entrepreneurs and investors evaluating this space, features are the architecture of a product’s market value. The right combination drives adoption, reduces churn, and positions a platform as mission-critical infrastructure inside healthcare organizations.
At Intellivon, we build enterprise-grade healthcare platforms that go beyond surface-level functionality. This blog breaks down the key features that separate average EHR practice management software from solutions that health systems actually depend on.
Why Clinics Are Replacing Legacy Systems Now
Clinics are rapidly replacing legacy EHR systems in 2026 as inefficiencies, compliance risks, and rising patient expectations expose their limitations. Today, 60% of healthcare leaders prioritize EHR modernization. As a result, organizations are shifting to cloud-native platforms built for AI, interoperability, and long-term scalability.
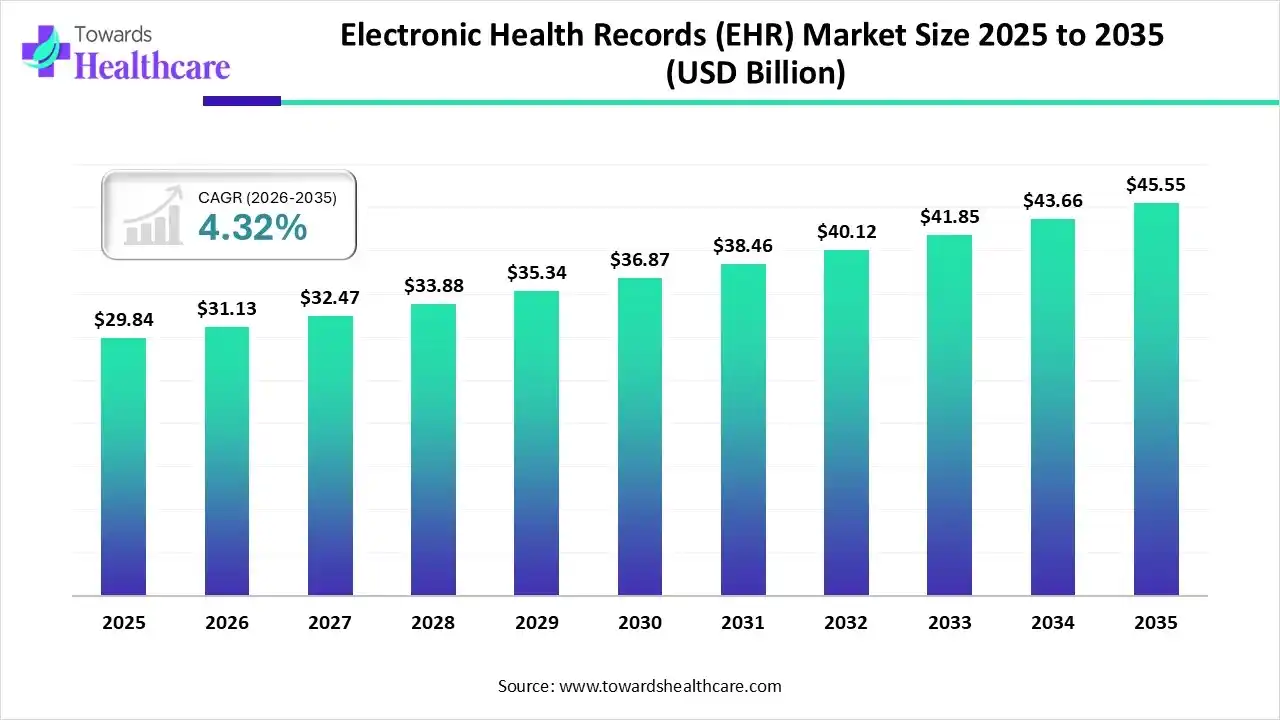
The global electronic health records market is valued at USD 29.84 billion in 2025 and is projected to reach USD 45.55 billion by 2035. This reflects a steady CAGR of 4.32% from 2026 to 2035, driven by growing demand for scalable, digital healthcare infrastructure.
Modern healthcare demands speed and precision that older, fragmented systems simply cannot provide. Therefore, many organizations find that existing infrastructure acts as a bottleneck rather than a foundation. Maintenance costs for aging servers climb while the user experience remains stagnant.
Consequently, the transition to integrated platforms is accelerating as leaders prioritize agility and data-driven decision-making.
1. Rising inefficiencies in disconnected systems
When clinical data sits in one silo and scheduling in another, staff productivity suffers. Employees spend hours manually syncing information across different windows. This fragmentation leads to frequent data entry errors and frustrated providers.
Furthermore, the lack of real-time communication between departments slows down patient throughput. A unified system eliminates these hurdles by creating a single source of truth.
2. Revenue leakage due to poor billing workflows
Financial gaps often stem from a lack of transparency in the revenue cycle. Legacy tools frequently miss unbilled procedures or fail to flag denied claims early. These small leaks turn into significant capital losses over a fiscal year.
However, modern practice management tools automate claim scrubbing to ensure higher first-pass rates. Improved visibility allows your team to resolve payment bottlenecks before they impact the bottom line.
3. Compliance risks in outdated infrastructure
Security threats have evolved, but many older systems lack the robust encryption needed today. Relying on patched software creates vulnerabilities that lead to expensive regulatory fines. In addition, legacy databases struggle to provide the detailed audit trails required for modern audits.
Moving to a contemporary platform ensures your data protection measures stay ahead of both hackers and shifting legal requirements.
4. Shift toward unified clinical + operational platforms
The industry is moving toward a model where clinical care and business operations live under one roof. Leaders recognize that a patient’s medical journey is inseparable from the administrative process. By merging these functions, you create a seamless experience for both the provider and the patient.
This holistic approach simplifies training and reduces the total cost of ownership for your technology stack.
The shift toward modern infrastructure is a proactive move to protect your margins. Updating your core technology ensures you remain competitive in an increasingly digital healthcare market.
What Is EHR + Practice Management Software?
EHR and practice management software is a unified clinical and operational platform built for healthcare organizations. The EHR side handles patient records, clinical documentation, and care workflows. The practice management side covers scheduling, billing, insurance claims, and administrative operations.
Together, they eliminate the disconnect between clinical and business functions, giving healthcare enterprises a single system to deliver care, manage revenue, and maintain compliance.
Clinical vs Operational Systems Explained
Healthcare platforms often split into two layers: clinical systems and operational systems. While both support care delivery, they solve very different problems. However, most clinics struggle because these systems operate in silos. As a result, workflows break, data gets duplicated, and decision-making slows down.
Understanding the difference is critical before building an integrated EHR + practice management platform.
Clinical vs Operational Systems: Key Differences
| Aspect | Clinical Systems (EHR) | Operational Systems (PMS) |
| Primary focus | Patient care and treatment | Clinic operations and revenue |
| Core users | Doctors, nurses, clinicians | Admin staff, billing teams |
| Data handled | Medical records, diagnostics | Appointments, billing, claims |
| Key goal | Improve clinical outcomes | Improve efficiency and cash flow |
| Examples | EHR, CDS tools | Scheduling, billing systems |
| Impact of failure | Poor patient care | Revenue loss and delays |
Clinical and operational systems serve different purposes, but they must work together. Therefore, modern healthcare platforms are moving toward unified EHR + practice management systems.
By integrating both layers, clinics gain real-time visibility, reduce friction, and deliver better care while improving financial performance.
Why Combining Both Systems Matters Today
Historically, EHR and practice management software were sold and deployed as separate products. Clinicians documented in one system while front-desk and billing teams operated in another.
That separation made sense when healthcare was simpler. However, today, it creates serious operational drag.
When both systems run on a unified platform, the impact is immediate:
- Clinical data flows directly into billing, reducing manual entry and claim errors
- Appointment scheduling syncs with provider availability and patient records in real time
- Insurance eligibility checks happen before the patient walks in, not after
- Revenue cycle teams see clinical outcomes that directly affect reimbursement accuracy
- Compliance documentation stays connected to the encounters that generate it
Separately, each system does its job. Together, they create a closed loop where clinical decisions and business operations reinforce each other.
For a platform targeting enterprise healthcare buyers, that integration is the foundation on which everything else is built.
What Problems Does It Actually Solve for Clinics?
Integrated platforms move beyond digitalization to resolve deep-rooted friction. Many clinics currently struggle with disconnected tools. This lack of cohesion creates unnecessary manual labor.
Consequently, operational errors increase. However, a unified EHR aligns every department. Thus, leaders see immediate improvements in staff morale. Similarly, patient service speed improves significantly.
1. Fragmented patient data across systems
When records exist in silos, clinical error risks rise. Doctors may miss allergy alerts. Therefore, patient safety suffers. In addition, staff waste time searching for files. A modern system consolidates data into a single profile. Consequently, providers have the context needed for care. Furthermore, information stays accurate.
2. Delays in billing and claim reimbursements
Slow reimbursement cycles cause cash flow instability. Legacy systems often rely on manual entry. Thus, coding errors occur frequently. Furthermore, tracking unpaid invoices is difficult. However, automated software identifies errors before submission. Therefore, your organization captures revenue faster. Additionally, teams spend less time on appeals.
3. Administrative overload for staff
Healthcare burnout often stems from excessive documentation. Employees spend much of their day on scheduling. However, modern platforms automate these routine processes. In addition, digital intake forms eliminate manual entry. Consequently, the staff focuses on patients. Moreover, overall workflow efficiency increases.
4. Lack of real-time decision visibility
Without centralized data, directors cannot monitor business health. It is difficult to track wait times accurately. Consequently, decisions rely on intuition. However, a unified platform provides real-time dashboards. Thus, visibility empowers quick adjustments. Therefore, you maximize profitability across the organization.
Solving these core problems creates a resilient business model. Finally, your clinic can focus on sustainable growth.
Core EHR Features That Drive Clinical Efficiency
The modern EHR has evolved from a digital filing cabinet into a proactive partner in the exam room. High-performance systems prioritize features that reduce manual data entry and provide context-aware insights. Consequently, clinicians can spend more time engaging with patients rather than navigating complex menus.
By integrating these core capabilities, your practice builds a foundation for long-term operational excellence and scalability.
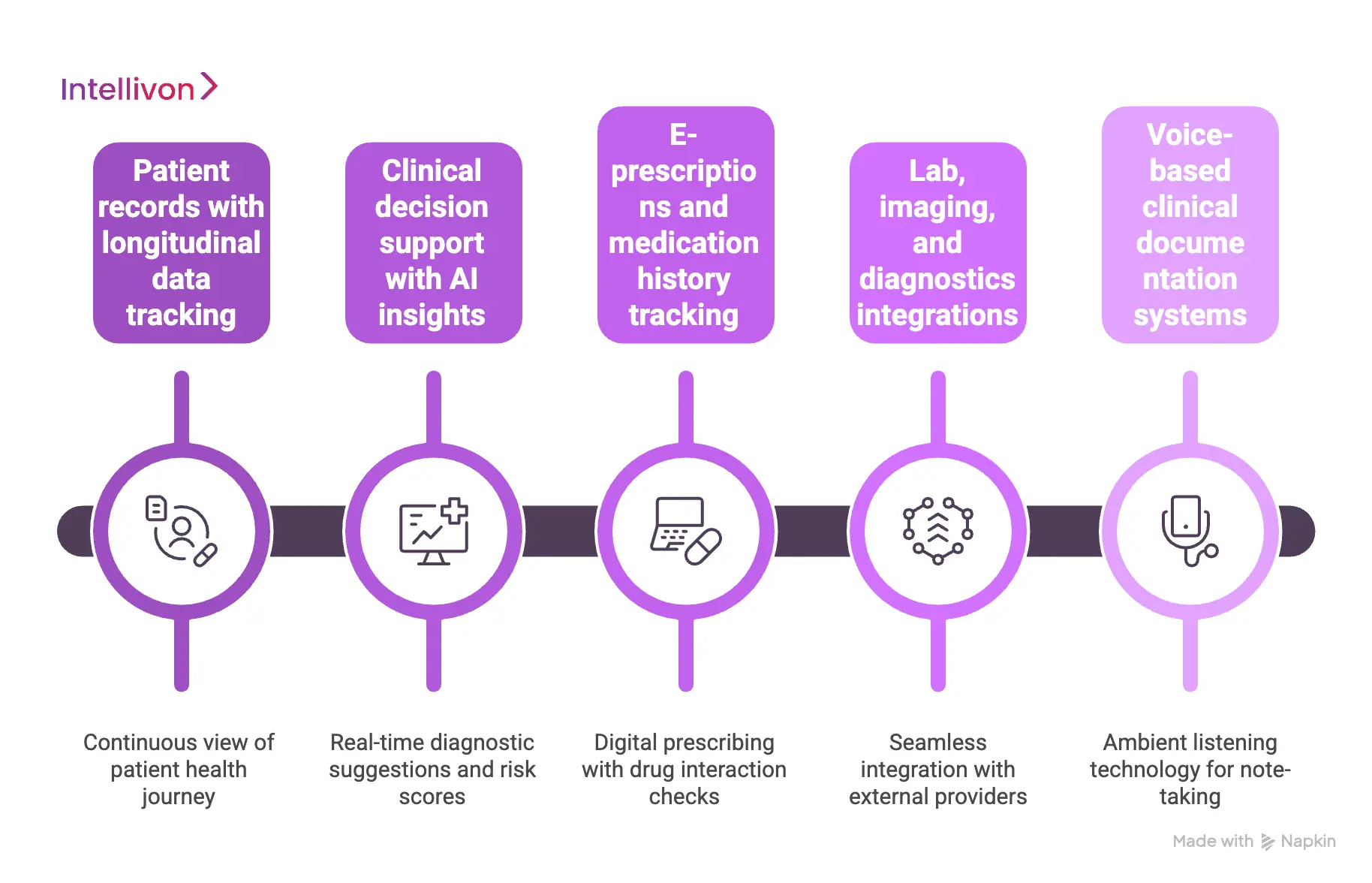
1. Patient records with longitudinal data tracking
A longitudinal record provides a continuous view of a patient’s health journey over several years. Unlike fragmented charts, this feature connects data from multiple providers, hospitals, and pharmacies into one timeline.
Therefore, clinicians can easily track disease progression and identify subtle functional changes. This comprehensive history eliminates the need for repeat testing and ensures that no critical past event is overlooked.
2. Clinical decision support with AI insights
AI-driven decision support acts as a real-time safety net during every encounter. These systems analyze current patient data against vast medical databases to provide diagnostic suggestions and risk scores.
For instance, the software can flag early indicators of sepsis or heart failure before symptoms become critical. In addition, these insights help standardize care quality across your entire medical group.
3. E-prescriptions and medication history tracking
Digital prescribing significantly reduces medication errors caused by illegible handwriting or miscommunication. These tools automatically check for potential drug interactions and patient allergies in real time.
Furthermore, tracking a patient’s medication history helps providers identify patterns of non-adherence or potential substance misuse. This transparency ensures that every new prescription is both safe and clinically appropriate for the patient’s profile.
4. Lab, imaging, and diagnostics integrations
Seamless integration with external laboratories and imaging centers accelerates the diagnostic process. Results flow directly into the patient’s chart as soon as they are finalized.
Thus, providers no longer need to chase down faxes or manual reports. This immediate access allows for faster treatment adjustments and improves the overall patient experience.
5. Voice-based clinical documentation systems
Ambient listening technology is revolutionizing how clinicians record their notes. These systems transcribe doctor-patient conversations and automatically generate structured clinical summaries.
Consequently, physicians can remain eye-to-eye with their patients instead of typing on a laptop. This shift drastically reduces the documentation burden and lowers the risk of physician burnout.
Investing in these high-impact features transforms your EHR into a strategic asset. Finally, your team can achieve peak productivity while maintaining the highest standards of patient safety.
Practice Management Features That Drive Revenue
Modern practice management is shifting from basic bookkeeping to advanced revenue orchestration. High-performing platforms now use intelligent automation to handle high-friction tasks like scheduling and collections. Consequently, your administrative team can focus on strategic growth rather than manual data entry.
By implementing these revenue-focused capabilities, you ensure your organization remains profitable in an increasingly complex reimbursement landscape.
1. Smart scheduling and appointment optimization
Inefficient scheduling is a leading cause of lost revenue due to gaps and last-minute no-shows. Smart systems use predictive models to identify patients with a high probability of missing their appointments.
Therefore, the software can automatically suggest double-booking or send targeted reminders to high-risk slots. Furthermore, real-time optimization tools can instantly fill cancellations from a digital waitlist. This proactive approach ensures maximum provider utilization and protects your daily billable hours.
2. Automated billing and coding workflows
Manual coding is often prone to human error, leading to frequent undercoding and lost income. Automated billing tools now analyze clinical documentation in real time to suggest the most accurate codes. Thus, your organization can ensure that all services rendered are fully captured and billed.
In addition, these workflows reduce the time spent on manual audits and corrections. Speeding up the billing cycle directly improves your cash flow and reduces the burden on your financial staff.
3. Insurance eligibility and claim tracking
Verifying insurance coverage manually is a slow process that often leads to denied claims. Modern platforms perform instant, automated eligibility checks before the patient even arrives at the clinic. Consequently, front-desk staff can address coverage issues or collect co-pays immediately.
Moreover, integrated claim tracking provides a transparent view of every submission’s status. This visibility allows your team to intervene early if a claim is stalled, preventing revenue from aging out.
4. Revenue cycle management dashboards
Without centralized data, identifying financial bottlenecks is nearly impossible for enterprise leaders. Revenue cycle dashboards provide real-time visibility into key performance indicators like days in accounts receivable.
Therefore, you can quickly spot trends in denials or slow-paying payers across multiple locations. This data-driven insight empowers you to make informed decisions about staffing and payer contracts. Having a clear financial map ensures you are always moving toward higher profitability.
5. Patient communication and reminders system
Consistent communication is vital for reducing no-shows and improving patient retention. Automated systems send personalized reminders via text, email, or voice based on the patient’s preference. In addition, these tools can handle post-visit follow-ups and satisfaction surveys automatically.
Thus, you build stronger patient relationships without increasing your administrative headcount. A reliable communication loop ensures that your schedule stays full and your patient base remains loyal.
Maximizing your revenue requires a shift from reactive billing to proactive financial management. Finally, these tools provide the structural support needed to scale your operations profitably.
Advanced Features Clinics Now Expect in 2026
The landscape of healthcare technology has shifted from passive record-keeping to proactive medical intelligence. Enterprise leaders now prioritize systems that can think, predict, and automate.
By adopting these forward-looking features, your organization can future-proof its operations while delivering superior patient value. Therefore, staying ahead of these trends is critical for maintaining a market-leading position.
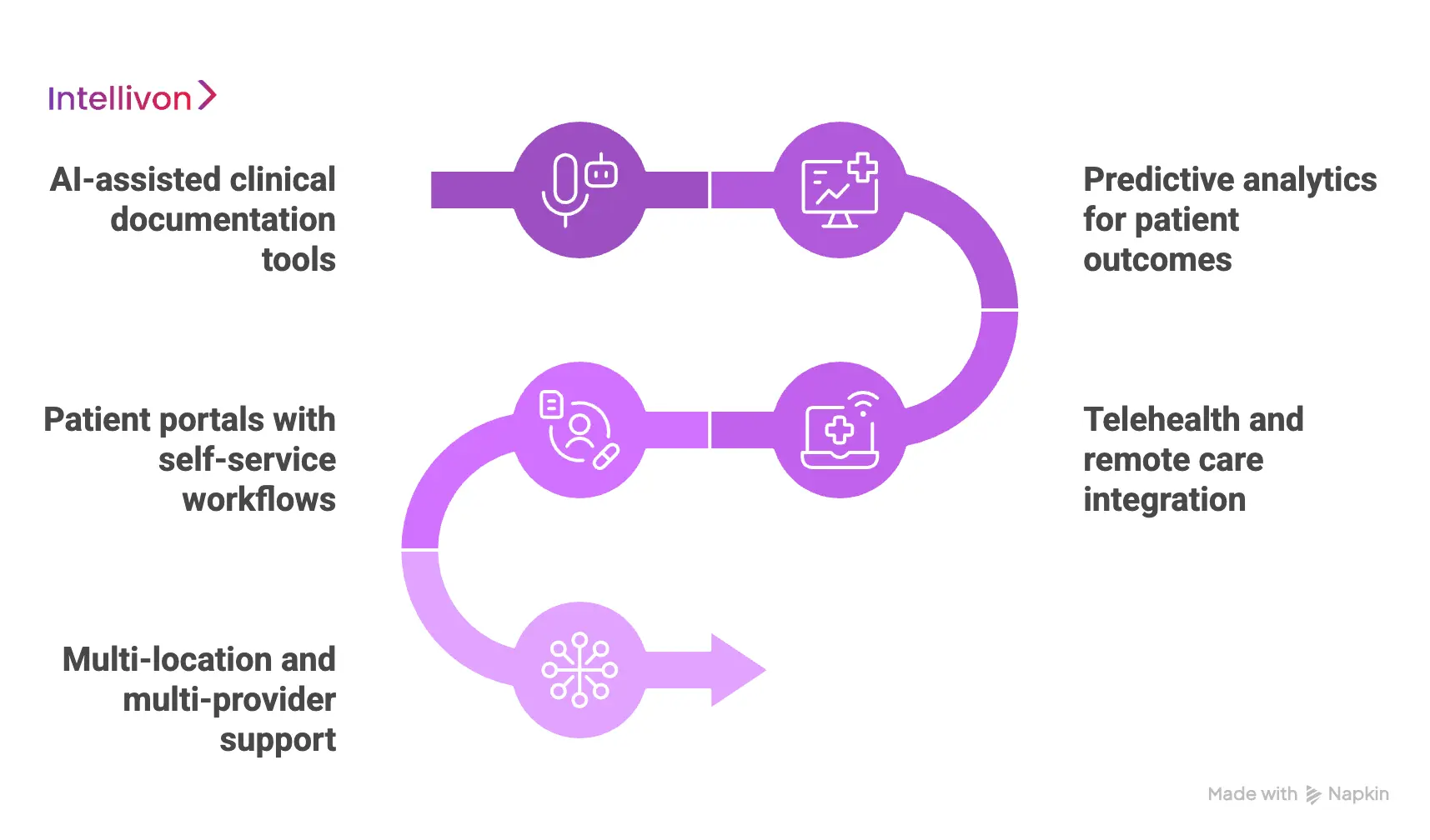
1. AI-assisted clinical documentation tools
Ambient voice technology is the most significant breakthrough in clinical efficiency this year. These tools listen to patient encounters and automatically generate structured SOAP notes in real time. Thus, providers can eliminate hours of “pajama time” spent on documentation after shifts.
Furthermore, these systems are now sophisticated enough to suggest appropriate billing codes based on the conversation. This automation drastically reduces physician burnout and improves the accuracy of the medical record.
2. Predictive analytics for patient outcomes
Modern EHRs now utilize machine learning to identify at-risk patients before a crisis occurs. By analyzing longitudinal data, these systems flag early indicators for chronic conditions like heart failure or diabetes. Therefore, your care teams can intervene with preventive strategies that significantly lower readmission rates.
In addition, predictive models help optimize resource allocation by forecasting patient volume. This data-driven foresight directly translates into better clinical outcomes and lower long-term costs.
3. Telehealth and remote care integration
Virtual care has evolved into a permanent, hybrid model that balances in-person and remote visits. Seamless integration allows telehealth sessions to launch directly from the patient’s chart with one click.
Moreover, the software now synchronizes with wearable devices to track vitals like glucose levels or heart rate. This continuous monitoring ensures that providers have a real-time view of patient health between office visits. Consequently, your practice can manage chronic diseases more effectively while offering unmatched patient convenience.
4. Patient portals with self-service workflows
Patients now expect a consumer-centric experience that mirrors modern retail or banking. Self-service portals allow individuals to book appointments, pay bills, and complete intake forms from their mobile devices.
Therefore, your front-desk staff spends significantly less time on administrative phone calls. Furthermore, secure messaging features enable quick, HIPAA-compliant communication for non-urgent inquiries. These digital touchpoints increase patient engagement and loyalty while streamlining your internal operations.
5. Multi-location and multi-provider support
For expanding enterprises, a unified system that manages multiple sites is essential for consistent growth. Centralized dashboards allow leaders to monitor performance and utilization across every clinic location.
In addition, role-based access controls ensure that data remains secure while remaining accessible to the right team members. This scalability allows you to add new providers and locations without the friction of fragmented software. A unified infrastructure provides the stability needed for rapid, large-scale expansion.
Adopting these advanced features transforms your practice into a highly efficient, data-driven organization. Finally, these tools provide the competitive edge required to lead in the modern healthcare economy.
What Makes a High-Performance EHR Platform?
Performance in the healthcare sector is measured by technical stability and clinical agility. Many systems struggle under the weight of massive datasets. However, a high-performance platform maintains lightning-fast responsiveness even during peak hours.
Consequently, providers can focus on patients without being slowed by loading screens. By prioritizing these structural pillars, your organization ensures its technology investment remains a long-term asset.
1. Speed and real-time data processing capability
In a clinical setting, every second spent waiting for a screen to load is a second lost. High-performance systems utilize modern cloud architectures to deliver instantaneous data retrieval. Therefore, clinicians can pull up complex imaging or multi-year lab trends in real time.
Furthermore, real-time processing ensures that critical alerts reach the provider exactly when needed. This speed directly correlates with higher daily patient throughput and improved physician satisfaction.
2. Interoperability with external systems
No medical facility operates in total isolation from the broader healthcare ecosystem. A high-performance platform must communicate seamlessly with external labs, pharmacies, and specialty networks. Thus, data flows across different systems without the need for manual faxing.
In addition, using standardized protocols like FHIR ensures that your data remains portable and secure. This connectivity allows for a collaborative care model that improves patient safety across all touchpoints.
3. Role-based access and workflow automation
Efficiency improves when every staff member has a workspace tailored to their specific responsibilities. Role-based access ensures that front-desk staff, nurses, and billing specialists see only relevant data.
Consequently, this focus reduces cognitive clutter and minimizes the risk of unauthorized data exposure. Moreover, integrated workflow automation handles repetitive tasks like appointment confirmations. This intelligent delegation allows your human capital to focus on complex clinical problem-solving.
4. Scalability across growing clinic networks
A system that works for one office may fail when expanded to twenty locations. High-performance platforms are built to scale horizontally without degrading the user experience. Therefore, adding new providers or facilities becomes a simple administrative task rather than a technical overhaul.
Furthermore, centralized management tools allow for standardized protocols across the entire network. This consistency is vital for maintaining brand quality and operational control during periods of rapid growth.
Building your practice on a high-performance foundation eliminates the technical debt that plagues many growing organizations. Finally, these capabilities provide the resilience needed to lead in a data-driven market.
Architecture Behind Modern EHR Systems
Modern EHR systems have transitioned from rigid, local databases to dynamic, cloud-based ecosystems. This shift allows for the rapid deployment of new features without disrupting daily clinical operations. However, the complexity of managing these environments requires a deep understanding of distributed systems.
Consequently, enterprise leaders prioritize architectures that balance high availability with robust data protection. By focusing on these core structural elements, you build a platform that scales effortlessly alongside your clinical business.
1. Monolith vs microservices in healthcare
Traditional monoliths house the entire application in a single codebase, making updates slow and risky. If one component fails, the entire system often goes down. However, a microservices architecture breaks the platform into independent, modular units like billing, scheduling, and charting.
Therefore, developers can update the billing module without touching clinical data. This isolation increases system resilience and allows for faster innovation. Furthermore, it enables teams to use optimized technologies for specific tasks, ensuring that each feature performs at its absolute peak.
2. API-first design for interoperability
An API-first approach treats the integration layer as a primary product rather than an afterthought. This strategy ensures that your EHR can connect with any third-party tool, from wearable devices to genomic databases. Thus, data exchange becomes standardized and predictable across the entire healthcare ecosystem.
In addition, using RESTful APIs or GraphQL allows for more efficient data retrieval and reduced latency. This connectivity is essential for creating a truly patient-centric experience that follows the individual across various care settings and specialized providers.
3. Cloud-native vs on-premise deployment
On-premise systems require significant upfront capital for hardware and ongoing maintenance. Furthermore, scaling these systems often involves physical upgrades and downtime. Conversely, cloud-native deployments offer near-infinite scalability and lower total cost of ownership.
Therefore, you can adjust your server capacity in real time based on patient volume. Cloud providers also offer superior disaster recovery and security features that are difficult to replicate in-house. This shift allows your IT team to focus on clinical workflows rather than managing physical server racks.
Data pipelines for real-time sync
Real-time synchronization is vital for maintaining a consistent view of patient health across multiple locations. Modern data pipelines use event-driven architectures to move information instantly between different modules.
Consequently, a lab result updated in one facility is immediately visible to a specialist in another. This eliminates the “stale data” problem that often leads to clinical errors or repetitive testing. Moreover, these pipelines support advanced analytics by feeding clean, structured data into machine learning models for real-time diagnostic insights.
A robust architecture is the primary moat against technical obsolescence in a fast-moving market. Finally, these structural choices ensure your platform remains fast, secure, and ready for the future of AI-driven care.
Compliance Requirements You Cannot Ignore
Navigating the complex landscape of healthcare regulations is a non-negotiable aspect of platform development. Therefore, integrating compliance into the core architecture is essential for protecting both patient trust and institutional capital.
1. Compliance Requirements You Cannot Ignore
Regulatory standards in healthcare are evolving rapidly to keep pace with digital transformation. Many organizations treat security as a final layer. However, high-performance systems embed compliance directly into every data transaction.
Consequently, these platforms reduce the risk of catastrophic data breaches and legal liabilities. By prioritizing these legal pillars, your organization ensures that its digital expansion remains ethical and sustainable.
2. HIPAA and global data privacy standards
Maintaining HIPAA compliance is the baseline for any medical platform operating within the United States. These rules ensure that Protected Health Information (PHI) remains confidential and accessible only to authorized users.
Furthermore, global entities must often adhere to GDPR or regional standards that dictate strict data residency requirements. Therefore, your platform must support localized data hosting and specific consent management workflows. In addition, staying updated on shifting international laws is vital for cross-border healthcare delivery.
3. Role of audit trails and data logging
Comprehensive audit trails provide a transparent record of every interaction within the patient record. These logs must capture who accessed the data, what changes were made, and when the event occurred.
Thus, your organization can quickly identify and investigate any suspicious activity or unauthorized access. Moreover, detailed logging is a primary requirement for successful regulatory audits and forensic analysis. This level of transparency builds a culture of accountability across your entire clinical and administrative staff.
3. Encryption and secure data storage models
Data must be protected both at rest and in transit using industry-standard encryption protocols. High-performance systems often utilize AES-256 encryption for stored data and TLS 1.3 for active communication. However, modern platforms are also exploring homomorphic encryption to allow for data analysis without decrypting the actual PHI.
This advanced approach adds an extra layer of security for research and analytics. Therefore, your storage model should prioritize multi-layered defense strategies to thwart sophisticated cyber threats.
4. Handling sensitive patient data at scale
As your patient volume grows, the complexity of managing sensitive data increases exponentially. Scaling requires automated data classification tools that identify and flag high-risk information across the entire network.
Consequently, you can apply stricter access controls to the most vulnerable data points. In addition, implementing zero-trust architecture ensures that every access request is verified regardless of its origin. This proactive stance is necessary for maintaining integrity while managing millions of records across global clinic chains.
Security is not a static goal but a continuous operational process. Finally, building a compliant infrastructure provides the peace of mind needed to focus on clinical innovation and market expansion.
How Integration Impacts Platform Performance
Seamless connectivity across the healthcare ecosystem is the primary driver of modern platform efficiency. Therefore, understanding the technical and operational impact of these integrations is essential for long-term scalability.
1. How Integration Impacts Platform Performance
Modern EHR performance is no longer measured in isolation but by how well it communicates with external entities. Fragmented data exchange leads to clinical delays and administrative friction.
However, a deeply integrated system ensures that information flows at the speed of care. Consequently, providers can make faster decisions based on a complete view of the patient. By prioritizing these high-impact connection points, your organization builds a resilient digital foundation.
2. EHR integration with labs and pharmacies
Direct connections with laboratories and pharmacies eliminate the need for manual data entry and paper-based orders. When a provider orders a test, the request is transmitted instantly to the lab. Thus, results are returned directly into the patient’s chart as soon as they are finalized.
Furthermore, e-prescribing tools check for drug interactions against the patient’s current medication list in real time. This immediate feedback loop reduces medical errors and significantly improves patient safety.
3. Connecting billing systems and insurers
Synchronizing your practice management software with insurance payers is vital for financial health. Integrated eligibility checks allow staff to verify coverage before a patient even enters the exam room.
Therefore, your organization can collect accurate co-pays and reduce the number of denied claims. Moreover, real-time claim tracking provides visibility into the status of every submission. This automation speeds up the reimbursement cycle and ensures a predictable cash flow for the enterprise.
4. Wearables and remote monitoring devices
The rise of the Internet of Medical Things (IoMT) allows for continuous patient monitoring outside the clinic walls. Integrating data from wearables provides clinicians with a longitudinal view of vitals like heart rate.
Consequently, providers can identify health trends and intervene before a condition becomes critical. In addition, this remote data sync supports chronic disease management and reduces the need for frequent in-person visits. This shift enhances patient convenience while optimizing provider time.
5. Third-party healthcare app integrations
A flexible platform must support a diverse ecosystem of specialized third-party applications. Using standardized APIs allows you to plug in tools for niche functions like mental health tracking. Thus, you can customize your digital environment without the need for extensive custom coding.
Furthermore, these integrations ensure that data remains unified across all touchpoints. Maintaining an open architecture allows your platform to adapt to new medical innovations as they emerge.
Successful integration transforms a static record system into a dynamic care coordination hub. Finally, these connections provide the operational agility needed to thrive in a connected healthcare market.
Cost to Build EHR + PMS Software in 2026
At Intellivon, EHR + practice management platforms are engineered as enterprise healthcare infrastructure, not as tools layered onto fragmented systems. The objective is to create a unified platform that manages clinical workflows, automates operations, and integrates seamlessly across the healthcare ecosystem.
However, building such a platform is about designing the right architecture. Therefore, the cost depends on workflow complexity, integrations, and compliance depth. As a result, even within a focused budget range, scope decisions play a critical role.
Estimated Phase-Wise Cost Breakdown
| Phase | Description | Estimated Cost (USD) |
| Discovery & Workflow Mapping | Define workflows, billing logic, and system scope | $5,000 – $10,000 |
| UI/UX & Product Design | Design clinician dashboards and admin interfaces | $8,000 – $15,000 |
| Core EHR Development | Patient records, charting, prescriptions | $15,000 – $40,000 |
| Practice Management Modules | Scheduling, billing, and basic RCM workflows | $10,000 – $30,000 |
| Integrations | Labs, pharmacies, and essential third-party systems | $5,000 – $20,000 |
| Compliance & Security | Basic HIPAA-ready setup, encryption, and access control | $3,000 – $10,000 |
| Testing & Deployment | QA, rollout, and initial onboarding | $4,000 – $10,000 |
Total Estimated Cost Range
- MVP for small clinics: $50,000 – $80,000
- Growth-stage platform: $80,000 – $120,000
- Advanced custom system: $120,000 – $150,000
This range typically supports a scalable, cloud-based platform with essential EHR + PMS capabilities. However, advanced AI features, deep integrations, or multi-location scaling may extend beyond this range.
What Impacts Cost Within This Range?
Even within a $50K–$150K budget, key decisions influence the final cost:
- Workflow depth: Specialty-specific logic increases complexity
- Integration scope: Each external system adds development effort
- Automation level: AI and smart workflows raise initial costs
- Compliance needs: Higher security = higher implementation effort
- Scalability planning: Future-ready systems cost more upfront
Why Low-Cost Builds Often Fail
Many vendors optimize for cost, not longevity. As a result, clinics end up with systems that:
- Cannot scale beyond a single location
- Break during integrations
- Fail compliance audits
At Intellivon, the focus remains on building lean but scalable systems. This ensures that even within a controlled budget, the platform can evolve without requiring a complete rebuild.
A $50,000–$150,000 investment can deliver a strong EHR + PMS foundation, if it is built with the right architecture. Therefore, clinics should prioritize scalability, integrations, and compliance from day one.
Want a precise cost breakdown for your platform? Speak with Intellivon’s experts to map your workflows and get a tailored estimate aligned with your growth roadmap.
How Intellivon Builds EHR + Practice Management Platforms Differently
At Intellivon, we move beyond the standard “feature-list” development model to create integrated ecosystems designed for high-stakes medical environments. Our methodology bridges the gap between complex regulatory requirements and intuitive user experiences.
Consequently, our partners receive a platform that is not only compliant but also operationally superior from day one. By following a rigorous, architecturally-driven process, we ensure that every deployment is built to handle the future of AI-driven healthcare.
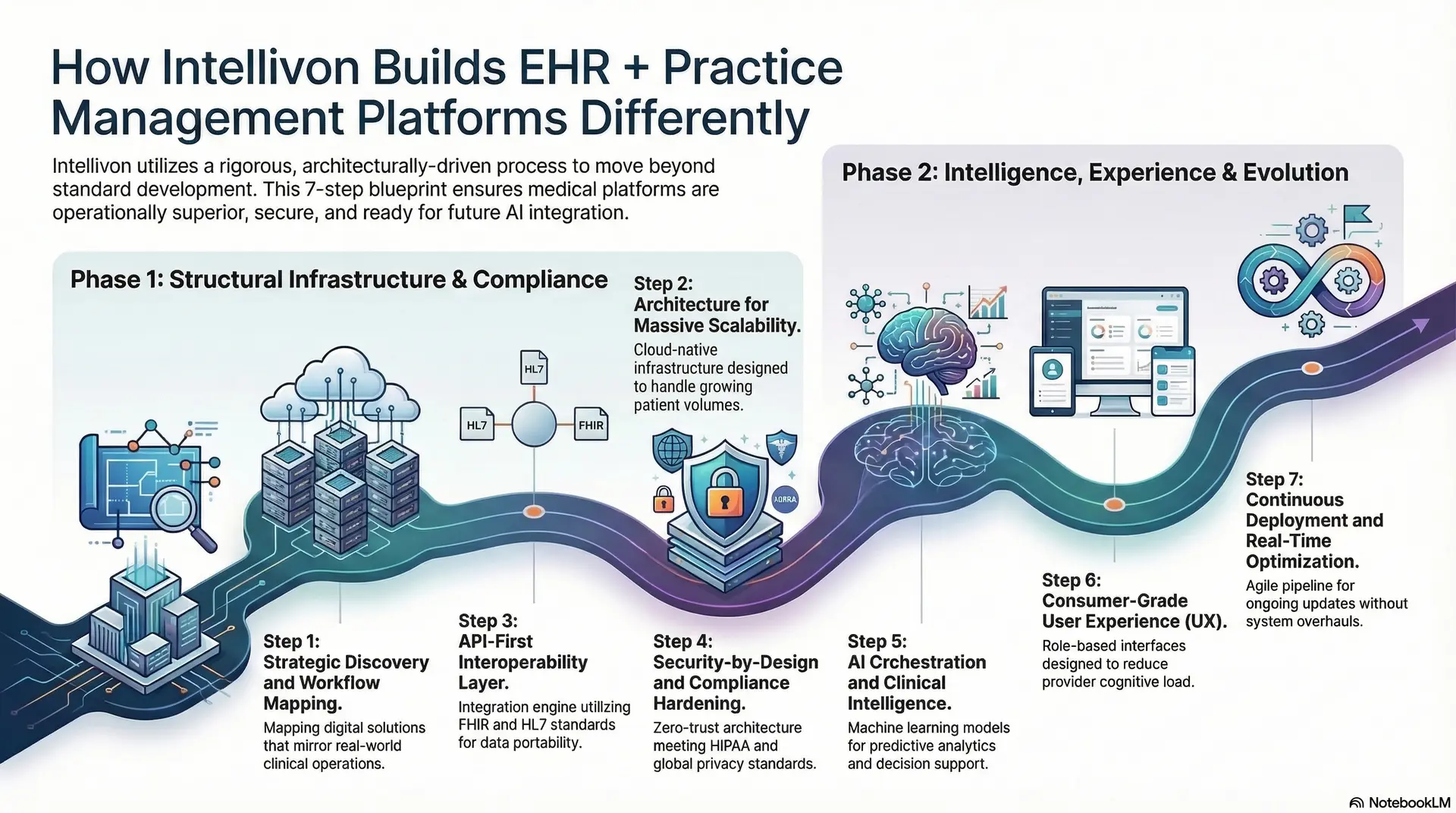
Step 1: Strategic Discovery and Workflow Mapping
We begin by deconstructing your specific clinical and administrative bottlenecks through deep-dive sessions. Therefore, we don’t just build software; we map a digital solution that mirrors your real-world operations. This phase identifies the key performance indicators that will drive your platform’s ROI.
Step 2: Architecture for Massive Scalability
Our engineers design a cloud-native, microservices-based infrastructure to ensure your system never slows down as your patient volume grows. Thus, you gain a platform that supports horizontal scaling across multiple regions and clinic networks. We prioritize high availability and disaster recovery at the structural level.
Step 3: API-First Interoperability Layer
We build a robust integration engine that allows your EHR to speak fluently with labs, pharmacies, and external specialty networks. In addition, we utilize FHIR and HL7 standards to ensure seamless data portability. This connectivity is essential for a unified, patient-centric care model.
Step 4: Security-by-Design and Compliance Hardening
Security is baked into our code, not added as a final layer. We implement zero-trust architectures, AES-256 encryption, and automated audit logging to meet HIPAA and global privacy standards. Consequently, your enterprise is protected against evolving cyber threats and regulatory risks.
Step 5: AI Orchestration and Clinical Intelligence
We integrate advanced machine learning models for predictive analytics and ambient voice documentation. Therefore, your platform moves from passive record-keeping to proactive decision support. This step significantly reduces clinician burnout and improves diagnostic accuracy across your organization.
Step 6: Consumer-Grade User Experience (UX)
Our design team focuses on reducing the “cognitive load” for providers through intuitive, role-based interfaces. Moreover, we develop seamless patient portals that offer self-service scheduling and billing. A clean, modern UX ensures high adoption rates and minimal training time for your staff.
Step 7: Continuous Deployment and Real-Time Optimization
The final step is establishing an agile pipeline for continuous updates and performance monitoring. Thus, your platform evolves alongside medical innovations without requiring massive system overhauls. We provide ongoing support to ensure your technology remains a competitive advantage.
Our process is designed to turn your vision into a high-performance reality. Finally, these steps provide the clarity and technical depth needed to lead the healthcare market.
Conclusion
Building a high-performance EHR and Practice Management platform is a strategic investment in your organization’s future. Therefore, choosing a partner who understands both clinical depth and technical scalability is essential. Modern solutions must prioritize intelligence, security, and seamless integration to drive true ROI.
Consequently, your digital infrastructure becomes a growth engine. Finally, let Intellivon transform your vision into a market-leading reality with our elite development expertise.
Build an EHR + PMS Platform With Intellivon
At Intellivon, EHR + practice management platforms are built as an enterprise healthcare infrastructure, and not as software layered onto disconnected clinical and administrative systems. The objective is to create a unified platform that aligns care delivery, operational workflows, and revenue systems into a single, scalable environment.
Each platform is designed to support the full clinical and operational lifecycle. This includes patient records, clinical decision support, scheduling, billing, insurance workflows, and real-time data visibility across departments. As a result, healthcare organizations reduce administrative friction, improve care coordination, and accelerate revenue cycles.
Our engineering approach focuses on AI-first, API-driven architectures combined with interoperability standards like HL7 and FHIR. This ensures seamless integration with EHRs, labs, pharmacies, insurers, and third-party healthcare systems without disrupting ongoing operations.
Why Intellivon for EHR + PMS Development
- Clinical infrastructure, not just software: Platforms are built to support long-term healthcare operations, not short-term feature requirements.
- Designed for interoperability from day one: Seamless integration with healthcare ecosystems ensures continuous data flow and system reliability.
- AI-powered workflow optimization: Automate documentation, billing, and decision-making with intelligent systems.
- Built for scale and compliance: Architects support multi-location growth while meeting global healthcare regulations.
Whether you are modernizing legacy systems or launching a new healthcare platform, Intellivon helps you design, build, and scale with confidence.
Talk to Intellivon’s healthcare experts to get a tailored roadmap and cost estimate for your EHR + PMS platform.
FAQs
Q1. What is EHR and practice management software?
A1. EHR and practice management software is a unified platform that combines clinical and administrative functions. It manages patient records, treatment workflows, scheduling, billing, and insurance processes in one system. As a result, clinics improve care delivery while streamlining operations and revenue management.
Q2. How long does it take to build such software?
A2. Building EHR + PMS software typically takes 4 to 9 months, depending on complexity. A basic MVP can be launched in 3–5 months, while advanced systems with integrations, AI features, and compliance layers require more time. Therefore, timelines vary based on scope and scalability needs.
Q3. What features are essential in EHR systems?
A3. Essential EHR features include patient records, clinical documentation, e-prescriptions, lab integrations, and decision support tools. In addition, modern systems include scheduling, billing, and patient communication features. Together, these ensure efficient workflows, accurate data management, and improved patient outcomes.
Q4. How much does EHR software development cost?
A4. The cost to build EHR software typically ranges from $50,000 to $150,000 for a scalable MVP. However, the final cost depends on features, integrations, compliance requirements, and customization. More advanced systems with AI and multi-location support can increase the investment.
Q5. Can EHR systems scale with clinic growth?
A5. Yes, modern EHR systems are designed to scale with clinic growth. Cloud-native and API-driven architectures allow clinics to add new locations, providers, and integrations without rebuilding the system. As a result, organizations can expand operations while maintaining performance and compliance.