Clinicians face thousands of decisions every day. They often work under time pressure and with incomplete information. Missed warning signs can lead to emergency situations, longer hospital stays, or avoidable complications.
Predictive patient analytics helps by turning scattered clinical data into clear risk forecasts. These forecasts identify subtle signs of deterioration, predict spikes in resource use, and allow for earlier, evidence-based interventions. This approach leads to faster and more confident decision-making.
At Intellivon, we build predictive patient analytics platforms for regulated, high-volume healthcare settings. Our systems are designed to be secure and are built to meet enterprise standards. They work well with existing EHRs like Epic and Cerner, billing systems, and devices, helping health systems improve patient outcomes, streamline operations, and reinforce their compliance with regulations. This blog explains how we create these enterprise-grade platforms from the ground up.
Key Takeaways of the Healthcare Predictive Analytics Market
The healthcare predictive analytics market has moved firmly into enterprise-scale adoption. In 2025, the global market stands between USD 20–28 billion and is projected to expand toward USD 70–150 billion by 2030–2034, reflecting sustained CAGRs of 24–28%.
This growth is not speculative. It is being driven by structural changes in healthcare delivery, rising chronic disease burden, and the rapid digitization of clinical data across large health systems.
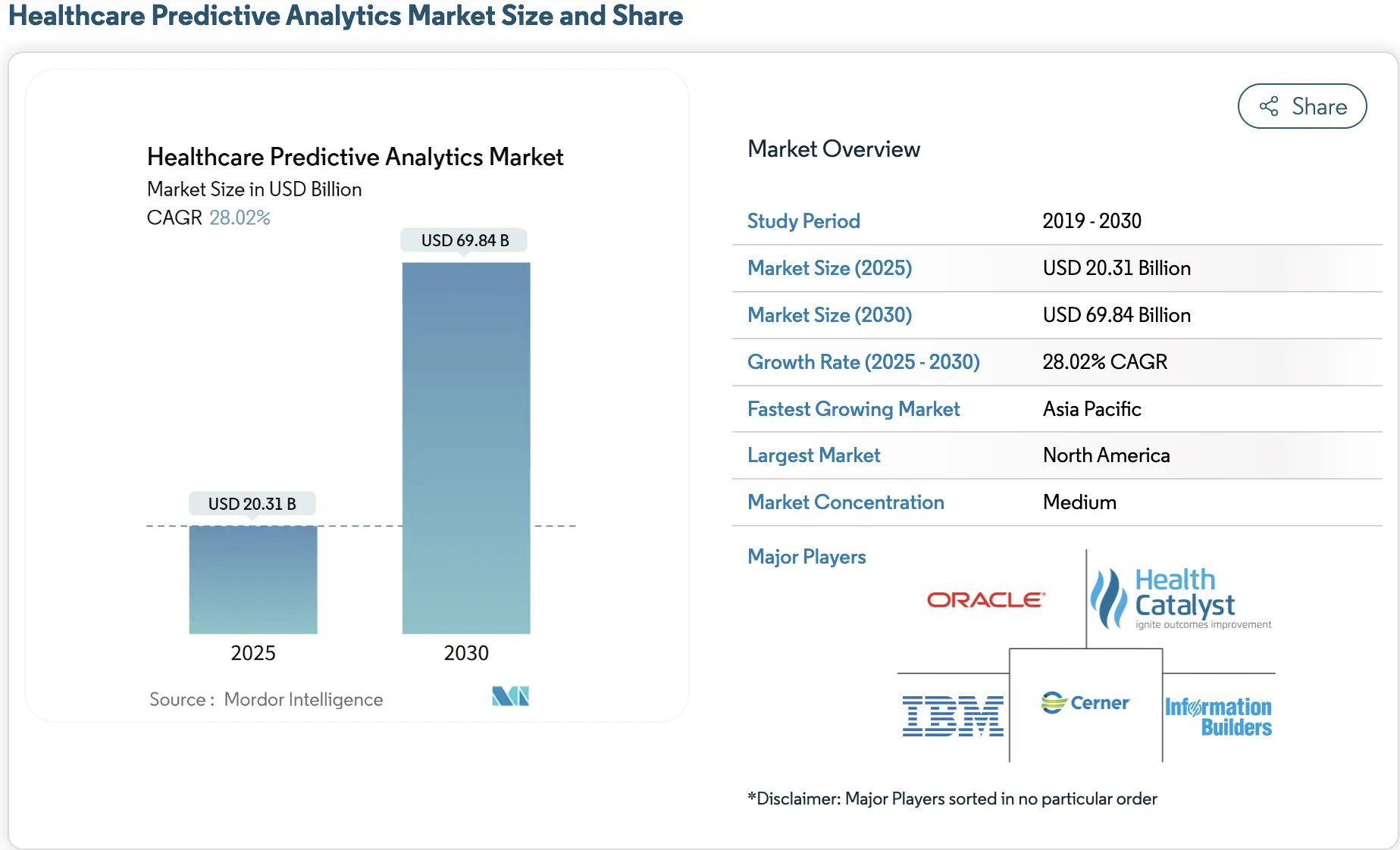
Key Growth Drivers:
- Market expansion is fueled by the shift from fee-for-service to value-based care, where early risk detection directly impacts revenue protection.
- EHR saturation across hospital networks has created massive longitudinal datasets ready for predictive modeling.
- Wearables, remote monitoring devices, and AI-ready sensors are accelerating real-time health data generation.
- Payers are rapidly adopting predictive models for risk adjustment, fraud detection, and high-cost patient identification.
- Population health management is the fastest-growing application segment, with data-driven prevention becoming a board-level priority.
- North America holds nearly half of the total market share, driven by chronic disease prevalence, reimbursement reform, and technology maturity.
- Operational forecasting now rivals clinical prediction as a core enterprise use case, supporting staffing, ICU capacity, and supply chain planning.
- Cloud-native predictive platforms are shortening deployment cycles while improving scalability and compliance posture.
- Enterprise solutions such as Health Catalyst Ignite reflect the market’s shift toward fully managed, production-grade platforms rather than experimental analytics tools.
What matters most to enterprise leaders is that this market growth is translating into measurable outcomes. Large health systems now report improvements in adherence, utilization control, and claims efficiency, while payers achieve faster adjudication and network optimization at scale.
Predictive analytics is now a financial, operational, and clinical performance lever embedded directly into how modern healthcare enterprises compete and grow.
What Is a Predictive Patient Analytics System?
A predictive patient analytics system uses machine learning on EHR, clinical, and operational data to forecast patient risk, disease progression, hospital utilization, and outcomes. Unlike descriptive analytics, it predicts future events and supports early intervention, enabling value-based care, population health management, and enterprise-scale clinical decision intelligence.
Difference Between Descriptive, Diagnostic, Predictive, and Prescriptive Analytics
| Analytics Type | Core Question It Answers | What It Focuses On | Typical Healthcare Examples | Enterprise Value |
| Descriptive Analytics | What happened? | Historical reporting | Past admissions, length of stay, mortality rates, case volumes | Operational visibility and baseline performance tracking |
| Diagnostic Analytics | Why did it happen? | Root-cause analysis | Readmission drivers, staffing delays, treatment gaps, comorbidity impact | Performance optimization and issue resolution |
| Predictive Analytics | What is likely to happen next? | Future risk and probability modeling | Deterioration risk, ICU demand, readmission likelihood, disease progression | Early intervention, cost avoidance, proactive care |
| Prescriptive Analytics | What action should be taken now? | Decision guidance under constraints | Treatment recommendations, optimal discharge timing, staffing adjustments | Workflow automation, outcome optimization, margin protection |
Predictive patient analytics operates at the third maturity layer, but it increasingly powers prescriptive decision systems. It does not replace clinical judgment. Instead, it strengthens it with statistically grounded, real-time foresight that scales across enterprise operations.
Core Objectives of a Predictive Patient Analytics System
A predictive patient analytics system is not built as a generic reporting tool. Each objective addresses a specific enterprise risk area where delayed insight translates into measurable cost and care impact.
1. Patient Risk Stratification
Risk stratification organizes patients by future probability of clinical deterioration rather than by current diagnosis alone. The system continuously recalculates risk tiers using longitudinal EHR data, medication history, lab trends, and behavioral signals.
As a result, intervention becomes targeted instead of reactive, and preventable escalations decline.
2. Disease Progression Forecasting
Disease progression forecasting models how conditions such as diabetes, cardiac disorders, oncology cases, and respiratory illness are likely to evolve over time.
This enables earlier therapy adjustments and reduces late-stage complications that drive avoidable admissions and extended hospital stays.
3. Hospital Utilization Modeling
Utilization modeling predicts near-term demand for beds, ICU capacity, operating rooms, and clinical staff. Instead of relying on static historical averages, the system forecasts utilization using live admission flows, seasonal trends, and patient acuity signals.
This allows hospitals to align staffing and resource allocation with actual demand, reducing both congestion and idle capacity.
4. Outcome Prediction
Outcome prediction estimates the probability of recovery, readmission, complications, or mortality for individual patients. When applied consistently, outcome prediction improves care continuity while lowering downstream treatment costs and readmission exposure.
Predictive patient analytics shifts organizations away from delayed response toward continuous foresight, which is the foundation of sustainable, outcome-driven healthcare operations.
Key Use Cases Of Predictive Patient Analytics Systems
Predictive patient analytics systems are used for readmission risk prediction, chronic disease forecasting, ICU demand planning, treatment outcome prediction, and population health risk scoring. These use cases enable earlier intervention, better capacity planning, lower avoidable costs, and stronger value-based care performance across large healthcare enterprises.
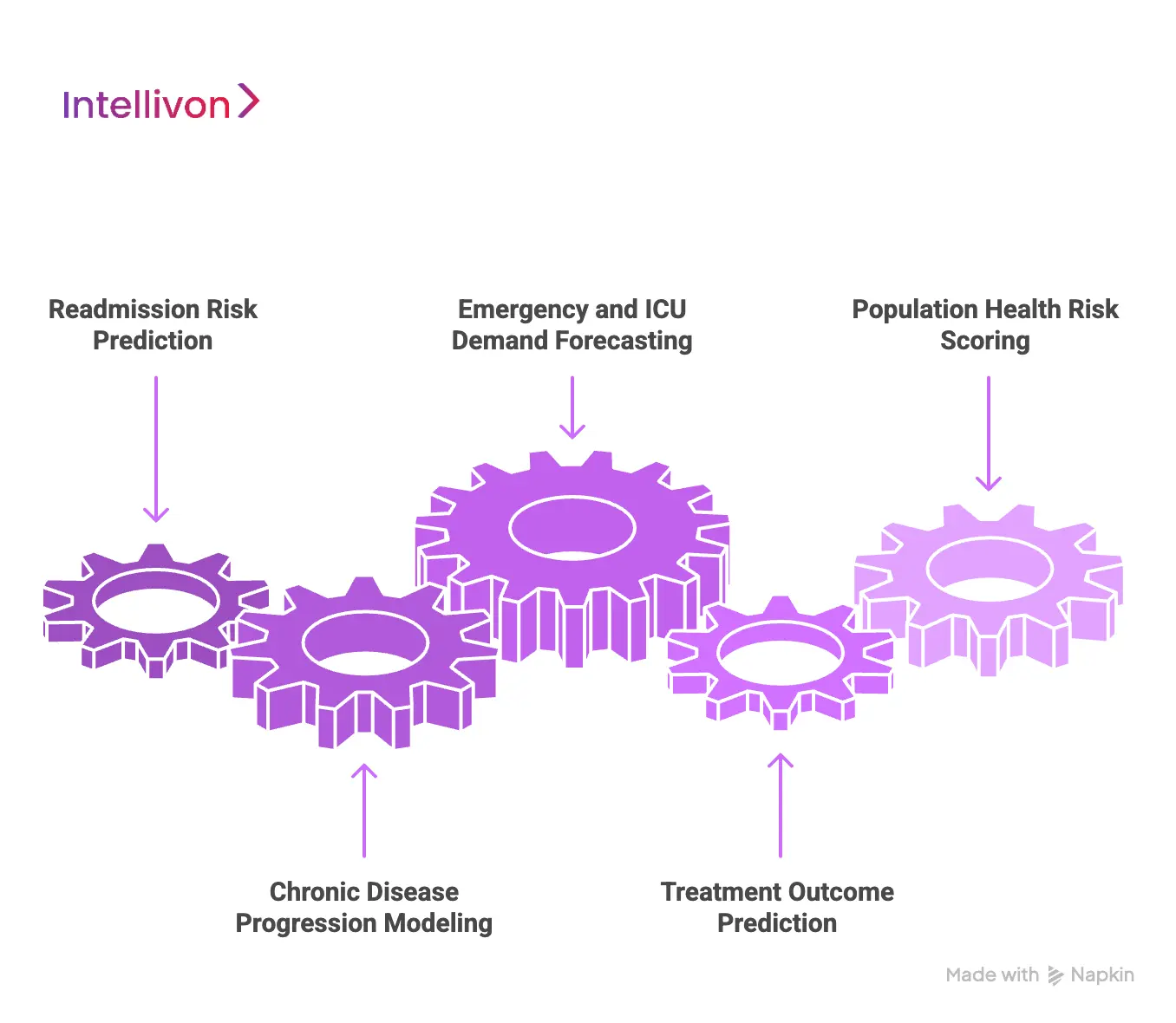
1. Readmission Risk Prediction
Unplanned readmissions remain one of the largest hidden cost centers in hospital operations. Predictive analytics models assess discharge readiness by analyzing diagnosis history, lab stability, medication adherence, prior admissions, and social risk factors. Patients flagged as high risk receive targeted follow-up, home monitoring, or care coordination before they leave the facility.
This shifts readmission management from retrospective audits to real-time prevention. For enterprises, this directly protects reimbursement, reduces penalty exposure, and improves care continuity metrics.
2. Chronic Disease Progression Modeling
Chronic conditions generate long-term cost and utilization pressure. Predictive analytics forecasts disease progression by learning from years of longitudinal patient data across vitals, labs, therapy response, and lifestyle indicators. Instead of waiting for deterioration, care teams receive early signals that guide therapy adjustments and intervention timing.
This improves long-term disease control while reducing acute exacerbations that drive emergency visits and inpatient stays. At scale, this stabilizes both clinical load and payer risk profiles.
3. Emergency and ICU Demand Forecasting
Emergency departments and ICUs operate under constant capacity risk. Predictive patient analytics estimates near-term demand by correlating live admission flows, acuity scores, seasonal trends, and population health signals. These forecasts inform proactive staffing, bed allocation, and surgical scheduling.
The result is fewer bottlenecks during demand surges and lower idle capacity during slow periods. From an enterprise perspective, this improves throughput without expanding physical infrastructure.
4. Treatment Outcome Prediction
Outcome prediction estimates the likelihood of recovery, complications, or treatment failure for individual patients before critical decisions are finalized. These insights support more accurate triage, therapy selection, and discharge timing. They also guide post-acute care planning and remote monitoring strategies.
When deployed correctly, outcome prediction reduces trial-and-error medicine. It strengthens clinical confidence while lowering avoidable downstream treatment costs.
5. Population Health Risk Scoring
Population health teams use predictive analytics to identify emerging risk clusters across communities and care networks. The system analyzes claims trends, chronic burden, utilization patterns, and social determinants to rank population segments by future care demand and cost exposure.
This enables earlier preventive outreach, targeted screening programs, and payer-provider coordination. At scale, population risk scoring becomes the backbone of value-based care execution.
Each of these use cases delivers value on its own. Together, they reshape how a healthcare enterprise plans, intervenes, and allocates resources. This is why adoption is accelerating across providers, payers, and integrated delivery networks.
How Predictive Patient Analytics Systems Signal Risk 48 Hours Before Onset
In many critical conditions, the difference between recovery and escalation is measured in hours. Yet most clinical systems still react after symptoms become obvious. Predictive patient analytics changes this timeline by identifying subtle physiological shifts far earlier.
By learning from vitals, labs, medications, and behavioral data streams, modern models can surface credible risk signals up to 48 hours before clinical onset in conditions such as sepsis, cardiac events, and respiratory failure.
This early visibility is no longer experimental. It is already improving real hospital outcomes at scale.
1. Clinical Proof That 48-Hour Early Prediction Is Real
In a large multi-site clinical study published in Nature Medicine, machine learning models successfully predicted severe sepsis as early as 48 hours before onset using only routinely collected EHR data. The system continuously evaluated heart rate, blood pressure, laboratory trends, and longitudinal patient context to generate early warnings that clinicians could act on with confidence.
In a separate real-world deployment analysis of an AI-powered sepsis early warning system in live hospital environments, early detection led to a 39.5% reduction in in-hospital mortality and a 32% reduction in length of stay after implementation. These gains came from earlier treatment initiation, not downstream therapy changes.
For enterprise leaders, this matters for one reason. Earlier detection directly converts into lower ICU escalation, shorter inpatient stays, and reduced downstream treatment costs.
2. What Happens Inside the 48-Hour Prediction Window
From a technical and operational standpoint, these early risk signals are not simple threshold-based alerts. They are the output of continuous, multi-layered intelligence pipelines operating across the patient timeline.
Most enterprise-grade predictive patient analytics platforms monitor and correlate:
- Minute-level vital sign drift rather than isolated abnormal values.
- Lab trajectory changes across repeated test cycles.
- Medication response variance over time.
- Subtle deterioration of language embedded in clinical notes using NLP.
- Historical risk profiles from prior admissions and comorbid patterns.
By correlating these signals, the system generates a rolling probability score that evolves with every new data point. Therefore, clinicians do not receive a static warning. They see a dynamic risk curve that reflects the patient’s real-time status.
3. Why This Early Signal Changes Enterprise Economics
When risk is identified two days earlier, the clinical response window shifts dramatically. Care teams can stabilize patients on general wards instead of escalating them into the ICU. Labs and imaging become targeted instead of exploratory. Staffing can be proactive instead of reactive.
At an enterprise level, the financial impact compounds across:
- Lower ICU utilization rates.
- Shorter average length of stay.
- Fewer emergency escalations.
- Reduced readmission exposure.
- Higher throughput without proportional staffing increases.
Therefore, 48-hour early risk detection is not only a clinical advantage. It is a structural, operational, and financial lever for large healthcare systems.
Enterprise Predictive Patient Analytics System Pipeline Architecture
An enterprise predictive patient analytics pipeline includes data ingestion from EHR and devices, normalization and interoperability, secure lakehouse storage, and real-time plus historical data access layers.
This architecture enables scalable risk prediction, live clinical alerts, and large-scale model training across healthcare systems.
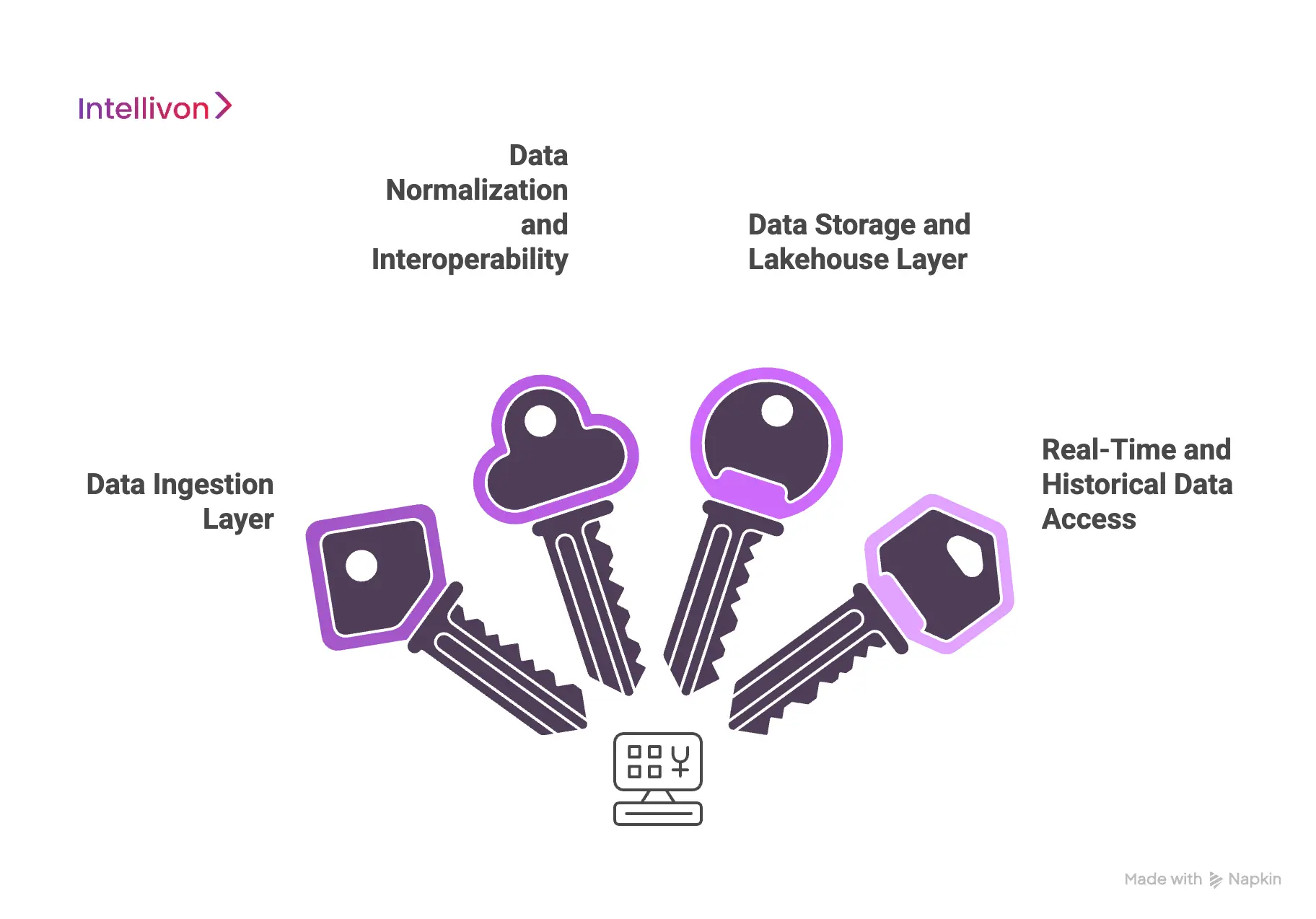
1. Data Ingestion Layer
The ingestion layer is responsible for pulling data from dozens of heterogeneous systems across the enterprise. These include EHR platforms, laboratory systems, imaging repositories, claims engines, and medical devices. Data enters through HL7 and FHIR interfaces, secure APIs, and event streams.
Hospitals typically operate in both batch and real-time modes. Batch ingestion supports historical modeling and reporting. Streaming ingestion supports live risk scoring and bedside decision support. A mature pipeline handles both without creating latency or duplication.
2. Data Normalization and Interoperability
Once ingested, data must be normalized before it can be used for modeling. Healthcare data arrives in inconsistent formats, naming conventions, and clinical coding standards. This layer resolves schema conflicts, maps terminologies, and aligns records across systems.
Clinical ontology alignment ensures that laboratory values, diagnoses, medications, and procedures are represented consistently across facilities. Without this step, predictive models learn noise instead of signal. Interoperability here directly determines model reliability and cross-hospital scalability.
3. Data Storage and Lakehouse Layer
Enterprise predictive platforms require storage systems that can handle both structured and unstructured healthcare data at scale. This includes vitals, lab results, images, clinical notes, claims, and device telemetry. A lakehouse architecture allows these diverse data types to live in a unified environment.
Security is enforced at this layer through encryption, access controls, and data lineage tracking. Storage is designed for dual use. It supports large-scale offline model training as well as low-latency access for real-time inference.
4. Real-Time and Historical Data Access
Predictive systems operate in two time horizons at once. Historical data trains models and supports long-term forecasting. Real-time data powers live risk detection and operational alerts. A well-designed architecture separates these workloads while keeping them logically connected.
Offline training environments handle heavy computation without disrupting live systems. Online inference services deliver risk scores directly into clinical and operational workflows with strict latency guarantees. This separation protects both system stability and decision reliability.
For healthcare leaders, architecture is not a technology decision alone. It is a business risk decision. A fragile pipeline produces delayed insights, inconsistent predictions, and audit exposure. A resilient pipeline delivers continuous intelligence that clinicians trust and executives can act on.
AI & Machine Learning Models Used in Predictive Patient Analytics Platforms
Predictive patient analytics platforms use supervised machine learning for risk prediction, deep learning for time-series and medical imaging, NLP for clinical notes, and ensemble models for higher accuracy. These AI models forecast patient deterioration, readmissions, ICU demand, and treatment outcomes at enterprise scale.
At enterprise scale, accuracy alone is not enough. Models must also be interpretable, stable under data drift, and safe for clinical deployment.
1. Supervised Learning Models
Supervised machine learning models form the backbone of most risk prediction engines. These models learn from labeled historical outcomes such as readmissions, ICU transfers, complications, and mortality.
Logistic regression remains widely used for its transparency and regulatory comfort. Random forest and gradient boosting models, such as XGBoost, deliver higher accuracy for complex, non-linear risk patterns. These models are commonly used for readmission risk, deterioration scoring, and payer-side risk adjustment.
From an enterprise perspective, these models offer the right balance between performance, explainability, and clinical acceptance.
2. Deep Learning Models
Deep learning models are deployed where traditional machine learning reaches its limits. Long Short-Term Memory networks analyze continuous streams of vitals, waveforms, and lab sequences to detect deterioration patterns that unfold over hours or days.
Convolutional Neural Networks are used for imaging-based prediction across radiology, cardiology, and pathology. These models extract high-dimensional features from scans and link them directly to risk and outcome forecasts.
Deep learning improves sensitivity for early detection. However, it demands stronger governance, validation, and monitoring due to its higher complexity.
3. Natural Language Processing Models
A large share of clinically relevant information still exists inside unstructured physician notes, discharge summaries, and nursing documentation. Natural language processing models convert this free text into structured risk signals.
Entity extraction identifies symptoms, diagnoses, medications, and clinical intent. Context modeling captures disease severity, uncertainty, and care transitions. These insights often surface risks that structured fields miss, especially in early deterioration scenarios.
For enterprises, NLP significantly expands the predictive surface area without adding a new data capture burden for clinicians.
4. Ensemble and Hybrid AI Models
High-performing predictive platforms rarely rely on a single model. They use ensemble architectures that combine multiple models across structured data, time-series streams, imaging, and text.
Hybrid models improve robustness by averaging predictions across different learning approaches. They reduce false positives, stabilize outputs across data drift, and perform better across diverse patient populations.
At scale, this layered modeling strategy is what enables consistent performance across hospitals, departments, and demographic segments.
Enterprises that prioritize explainability, validation, and continuous performance monitoring consistently achieve higher adoption and stronger clinical impact. Predictive patient analytics succeeds when models become part of daily decision-making, not isolated research assets.
Regulatory Compliance in Predictive Patient Analytics Systems
Regulatory compliance in predictive patient analytics requires HIPAA and GDPR alignment, encryption at rest and in transit, role-based access control, audit logs, consent management, and de-identification workflows. These controls ensure patient privacy, legal defensibility, and safe enterprise-scale deployment of AI-driven healthcare prediction systems.
1. Healthcare Data Protection and Privacy Regulations
Predictive systems process large volumes of protected health information across clinical, administrative, and behavioral domains. Regulatory frameworks such as HIPAA, GDPR, HITRUST, and ISO 27001 define how this data must be stored, processed, and shared.
At an enterprise level, compliance means more than encryption and access controls. It requires provable safeguards for data minimization, purpose limitation, cross-border transfer governance, and breach response. These protections must extend across cloud infrastructure, APIs, and downstream analytics services.
2. Encryption and Identity Governance
All sensitive health data must be encrypted both at rest and while in transit. However, encryption alone is not sufficient. Predictive platforms must also enforce strict identity and access governance across users, systems, and service accounts.
Role-based and attribute-based access control ensure that clinicians, analysts, and administrators see only the minimum data required for their function. Privileged access is tightly audited and reviewed continuously. This segregation of duties protects patient privacy while supporting enterprise-scale operations.
3. Auditability, Traceability, and Data Lineage
Predictive analytics decisions increasingly influence clinical pathways, discharge timing, and payer actions. Every prediction must therefore be traceable back to its data sources and model version. Audit logs record who accessed data, which model generated a prediction, and what information was used at the time.
Data lineage tracking ensures that training datasets, feature pipelines, and inference outputs can be reconstructed during regulatory reviews or legal inquiries. This is essential for defending both clinical decisions and financial outcomes during audits.
4. Consent Management and Data Minimization
Not all patient data can be used freely for predictive modeling. Predictive platforms must respect patient consent directives across treatment, analytics, and secondary use cases. Consent must be dynamically enforced as data moves through pipelines rather than locked at ingestion.
Data minimization practices ensure that models receive only what is necessary for the prediction task. This reduces regulatory exposure, lowers breach impact, and simplifies cross-border data governance.
5. De-Identification and Pseudonymization Workflows
Predictive model training often uses large population datasets. To protect patient identity, these datasets must undergo de-identification or pseudonymization before being used in non-production environments.
Enterprise-grade platforms maintain strict separation between identifiable clinical systems and anonymized analytics workloads. Re-identification keys are held in protected vaults with restricted access. This design supports innovation without compromising legal and ethical safeguards.
For healthcare enterprises, compliance maturity often determines whether predictive analytics remains a limited pilot or becomes a system-wide clinical intelligence layer.
How We Develop a Predictive Patient Analytics System
Building a predictive patient analytics system is not a software project alone. It is an enterprise transformation initiative that touches clinical workflows, data governance, security posture, and financial performance. At Intellivon, we follow a structured, compliance-first delivery framework that moves predictably from clinical intent to production-grade intelligence.
Each phase is designed to reduce risk early, protect regulatory posture, and ensure that predictions translate into daily operational decisions.
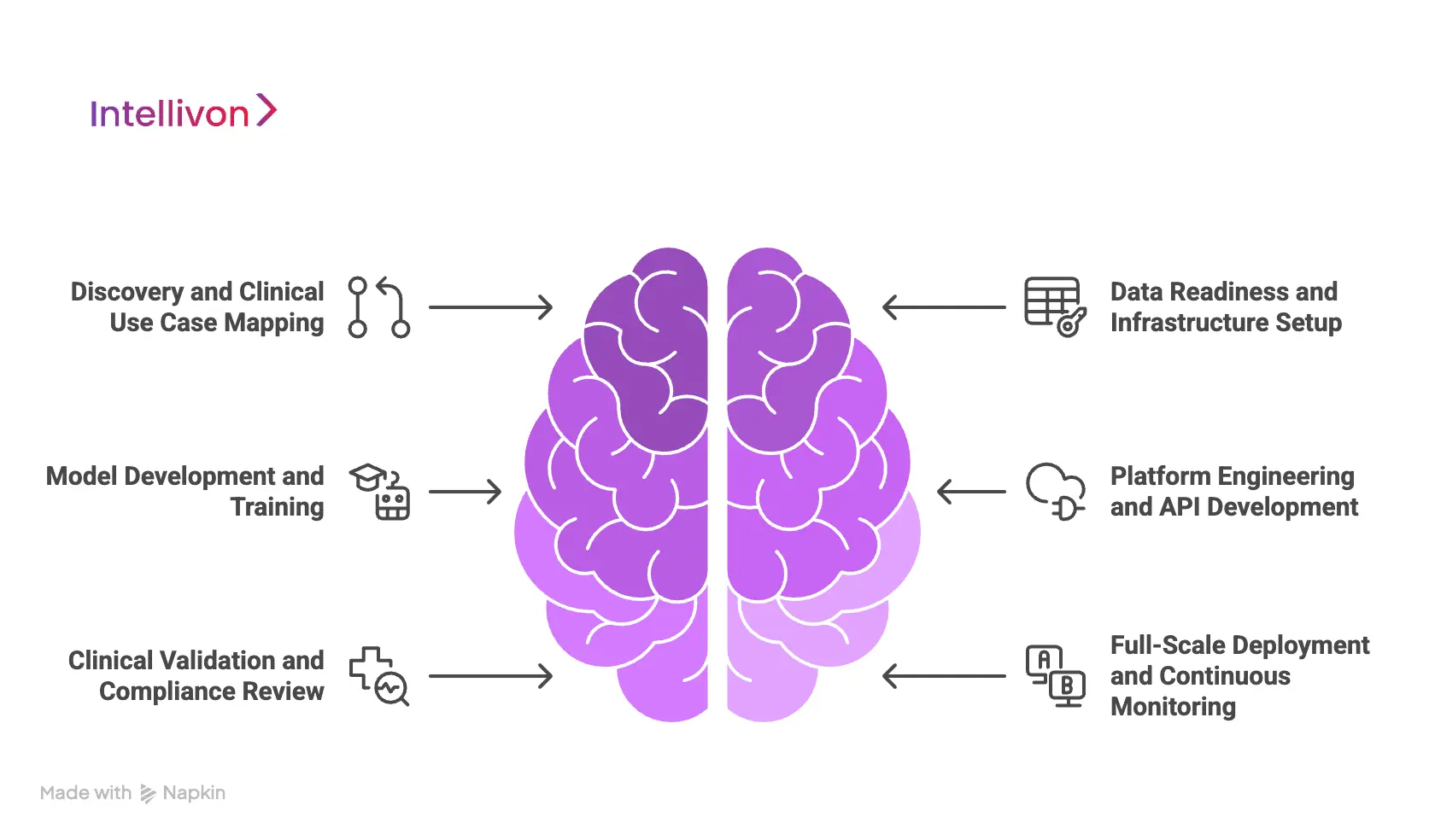
Phase 1: Discovery and Clinical Use Case Mapping
Every engagement begins with clinical and business discovery. We work closely with operational leaders, clinical stakeholders, and IT teams to define the exact outcomes the system must influence. These may include readmission reduction, ICU demand control, chronic disease stabilization, or payer risk optimization.
We map current workflows, escalation paths, and decision bottlenecks. This prevents the system from becoming a standalone analytics tool with no operational impact. At this stage, success metrics, data boundaries, and compliance constraints are also established.
Phase 2: Data Readiness and Infrastructure Setup
Once use cases are locked, we assess data readiness across EHRs, lab systems, claims engines, imaging platforms, and connected devices. This phase identifies data gaps, quality issues, and integration complexity across legacy systems.
We then design the ingestion, interoperability, and storage architecture using secure, scalable cloud and hybrid infrastructure. Legacy systems are integrated without disruptive rip-and-replace strategies. This protects business continuity while enabling modern analytics at scale.
Phase 3: Model Development and Training
With clean, governed data in place, our data science teams move into feature engineering and model development. We select algorithms based on the prediction horizon, explainability requirements, and regulatory exposure of each use case.
Models are trained on longitudinal patient data, validated against historical outcomes, and stress-tested for bias, drift, and stability. Clinical reviewers participate in validation to ensure model behavior aligns with real-world decision logic.
Phase 4: Platform Engineering and API Development
Validated models are then embedded inside a secure, microservices-based platform. We build real-time inference pipelines, integrate with EHR systems, and expose prediction services through hardened APIs.
Risk scores are delivered directly into clinical and operational workflows rather than into isolated dashboards. This ensures that intelligence reaches the point of action without adding friction to daily operations.
Phase 5: Clinical Validation and Compliance Review
Before system-wide deployment, the platform undergoes pilot implementation in controlled clinical environments. Predictions are observed alongside existing workflows to validate reliability, safety, and usability.
Parallel compliance audits verify encryption controls, access governance, consent enforcement, and audit logging. Only after regulatory, clinical, and security sign-off does the platform move into scaled production.
Phase 6: Full-Scale Deployment and Continuous Monitoring
Production rollout expands across departments, facilities, and populations based on enterprise priorities. Live monitoring tracks model performance, user adoption, data drift, and system reliability.
We implement continuous retraining pipelines and governance dashboards to keep predictions accurate as care patterns evolve. Operational and financial performance metrics are reviewed regularly to validate ongoing ROI.
Healthcare enterprises partner with Intellivon because we engineer these platforms as regulated, mission-critical systems rather than experimental AI projects. Our solutions are secure by design, enterprise-grade by architecture, and built for seamless integration with complex legacy environments.
Cost to Develop a Predictive Patient Analytics System
Building a predictive patient analytics system is a strategic, board-level investment even at pilot scale. Costs span secure data integration, AI model development, real-time pipelines, clinical validation, cybersecurity, testing, and regulatory alignment.
At Intellivon, we design phased cost models aligned with budget cycles, compliance obligations, and near-term ROI goals. Early phases focus on fast clinical and financial value realization without compromising HIPAA, GDPR, and patient safety requirements.
Estimated Phase-Wise Cost Breakdown
| Phase | Description | Estimated Cost (USD) |
| Discovery & Compliance Blueprint | Clinical workflow analysis, use-case prioritization, HIPAA/GDPR alignment, predictive feasibility mapping | 6,000 – 12,000 |
| Data Integration & Interoperability Design | EHR integration (single system), lab and claims feeds, data normalization, API security | 10,000 – 18,000 |
| Predictive Data Pipeline & Lakehouse Setup | Secure data ingestion, structured/unstructured storage, streaming + batch pipelines | 12,000 – 22,000 |
| AI Model Development & Validation | Risk prediction model setup, tuning, bias testing, baseline MLOps | 14,000 – 28,000 |
| Security, IAM & Compliance Controls | Role-based access, encryption, audit trails, consent enforcement | 7,000 – 14,000 |
| Clinical Dashboards & Workflow Integration | Risk visualization, EHR embedding, operational analytics | 6,000 – 12,000 |
| Testing, QA & Clinical Safety Validation | Functional testing, data accuracy checks, security validation | 5,000 – 10,000 |
| Pilot Deployment, Training & Stabilization | Clinical onboarding, live pilot rollout, tuning and monitoring | 6,000 – 12,000 |
Total Initial Investment Range: USD 66,000 – 128,000
Annual Maintenance and Optimization
- 12–20% of initial build cost per year
- Approx. USD 8,000 – 22,000 annually
Hidden Costs Healthcare Organizations Should Plan For
- Additional integrations as more departments, devices, or EHRs are connected.
- Regulatory documentation updates as privacy and AI governance rules evolve.
- Cloud usage growth as real-time data volume and inference frequency increase.
- Clinical change management and retraining during scale-up.
- Model re-tuning and drift correction as patient behavior and care patterns shift.
Best Practices to Stay Within the USD 70K–150K Budget
Enterprises that consistently control predictive analytics spend tend to:
- Start with one high-impact use case only, such as readmissions or ICU demand.
- Avoid multi-EHR and multi-region deployment in phase one.
- Use a modular model and pipeline design to add new predictions later without rework.
- Enforce security and compliance from day one, not after pilots.
- Track clinical and financial ROI weekly during the first 90 days.
Connect with our team to receive a tailored cost estimate for your hospital or payer environment. We align scope, AI depth, security controls, and integrations to deliver measurable clinical and financial ROI without unnecessary spend.
Examples of Predictive Patient Analytics Systems
Enterprise adoption of predictive patient analytics is no longer limited to innovation labs. It is now embedded into daily clinical, operational, and financial decision-making across large hospital networks, payer ecosystems, and population health programs. The platforms below illustrate how predictive analytics functions at true enterprise scale, with measurable clinical and economic impact.
1. Epic Cognitive Computing
Epic’s predictive analytics capabilities are deeply embedded within one of the world’s most widely used EHR ecosystems. Its machine learning models operate directly inside clinical workflows to predict deterioration, sepsis, readmissions, and ICU transfers in real time.
The system continuously learns from structured EHR data, vitals, lab trends, medications, and historical utilization patterns. Risk scores appear within native clinician dashboards rather than external analytics tools, which drives daily adoption.
Health systems using Epic’s predictive models have reported:
- Earlier detection of sepsis and patient deterioration.
- Lower rates of unplanned ICU escalation.
- Faster clinical response without increasing alert fatigue.
Here, analytics becomes part of routine bedside decision support rather than a retrospective reporting layer.
2. Health Catalyst
Health Catalyst operates one of the most mature enterprise healthcare analytics platforms for population health and operational forecasting. Its predictive engines integrate clinical, claims, cost, and social determinants data across full care networks.
The platform is widely used for:
- Readmission risk modeling.
- Length-of-stay forecasting.
- Chronic disease risk stratification at scale.
Large integrated delivery networks using Health Catalyst have achieved:
- Sustained reductions in avoidable readmissions.
- Higher bed utilization efficiency.
- Faster identification of high-cost patient cohorts.
In this model, predictive analytics directly links clinical intervention with financial performance management.
3. Cerner (Oracle Health)
Cerner’s predictive analytics capabilities span acute care, population health, and revenue cycle operations. The platform streams live patient data from hospital EHRs and applies time-series deterioration models at enterprise scale.
Its predictive functions include:
- Early deterioration detection.
- Utilization and capacity forecasting.
- Payer-side risk and denial prediction.
Healthcare networks using Cerner’s predictive intelligence have reported:
- Earlier clinical escalation in high-risk patients.
- Lower ICU congestion during seasonal demand surges.
- Improved revenue capture through proactive utilization management.
In this architecture, analytics becomes a shared control layer across both care delivery and financial workflows.
4. Optum (UnitedHealth Group)
Optum runs one of the largest predictive healthcare analytics infrastructures globally. Its models analyze hundreds of millions of patient records across claims, pharmacy, behavioral health, and clinical datasets.
The platform focuses on:
- Population risk stratification.
- High-cost patient forecasting.
- Preventive intervention targeting the national scale.
Optum’s predictive systems power:
- Proactive outreach to high-risk members weeks before hospitalization.
- Earlier chronic disease stabilization.
- Large-scale reduction in avoidable emergency utilization across payer networks.
This is predictive analytics operating at a national population scale rather than within a single hospital.
5. Philips (Clinical Command Center)
Philips’ Clinical Command Centers use real-time predictive analytics to orchestrate operations across entire hospital campuses. These platforms aggregate live feeds from EHRs, medical devices, imaging systems, and bed management tools into centralized command environments.
Predictive models are used for:
- ICU and bed demand forecasting.
- Patient deterioration detection.
- Inter-unit transport and throughput optimization.
Hospitals deploying Philips command centers have achieved:
- Faster patient transfers between units.
- Reduced emergency department boarding times.
- Higher utilization of high-acuity beds.
Across all these examples, success does not come from algorithms alone. It comes from how predictive intelligence is embedded into everyday clinical and operational workflows. Each of these platforms succeeds because predictions trigger real actions, not just visualizations.
Conclusion
Predictive patient analytics is no longer an innovation layer. It is becoming the operating intelligence that defines how modern healthcare systems manage risk, capacity, outcomes, and cost. Enterprises that invest now move from reactive care to foresight-driven decision making. They intervene earlier, stabilize utilization, and align clinical performance with financial sustainability across the full care continuum.
At Intellivon, we build predictive patient analytics platforms as secure, enterprise-grade systems engineered for legacy integration, regulatory trust, and measurable ROI. If your organization is ready to shift from hindsight to foresight, we are ready to design, deploy, and scale that intelligence with you.
Build a Predictive Patient Analytics Platform With Us
At Intellivon, we build predictive patient analytics platforms that combine clinical-grade AI, compliance-first architecture, and enterprise-scale reliability. Our systems forecast patient risk, disease progression, utilization demand, and outcomes across care delivery, operations, and population health while integrating seamlessly with existing hospital IT ecosystems.
Each platform is engineered to meet the demands of modern healthcare enterprises: secure, interoperable, scalable, and designed for measurable clinical and financial ROI from day one.
Why Partner With Intellivon?
- Compliance-First Architecture: Every deployment aligns with HIPAA, GDPR, HITRUST, FDA SaMD, where applicable, EU AI Act, and regional healthcare data protection frameworks.
- Healthcare-Tuned Predictive AI Models: Our machine learning and deep learning models are trained on real-world clinical, operational, and claims data patterns.
- Seamless Legacy System Interoperability: We integrate directly with EHR, HIS, LIS, RIS, PACS, RCM, and ERP platforms using FHIR, HL7, DICOM, and secure enterprise APIs.
- Scalable Cloud-Native and Hybrid Infrastructure: Multi-hospital deployments, high availability, elastic scalability, and low-latency inference.
- Continuous Model Optimization: Built-in MLOps pipelines monitor model performance, detect drift, and retrain intelligently.
- Zero-Trust Security Framework: Encryption at every layer, identity-first access governance, network segmentation, and continuous threat detection.
- Human-in-the-Loop Governance: Clinical override controls, approval workflows, and role-based dashboards.
- Proven Enterprise Delivery Expertise: With deep experience delivering enterprise-grade healthcare AI systems.
Book a strategy call with Intellivon to explore how a custom-built predictive patient analytics platform can reduce avoidable risk, improve utilization efficiency, strengthen regulatory posture, and scale reliably across your healthcare enterprise.
FAQs
Q1. What data is required to build a predictive patient analytics system?
A1. A predictive patient analytics system requires four primary data categories: clinical data from EHR systems, administrative and claims data, patient-generated health data from devices and wearables, and social determinants of health. Clinical data includes vitals, labs, medications, diagnoses, and notes.
Q2. How accurate are predictive patient analytics models in hospitals?
A2. Accuracy depends on data quality, model design, and clinical integration. In production hospital environments, well-validated predictive models commonly achieve AUROC scores between 0.85 and 0.95 for tasks such as sepsis detection, readmission prediction, and deterioration forecasting.
Q3. How long does it take to deploy predictive patient analytics in a hospital?
A3. A focused enterprise-grade pilot typically deploys within 12 to 20 weeks. This includes use-case discovery, data integration, model training, compliance validation, and live workflow integration. Full multi-department or multi-hospital rollout generally spans 6 to 12 months, depending on legacy system complexity, regulatory scope, and change management requirements.
Q4. What regulations apply to predictive healthcare analytics platforms?
Predictive healthcare analytics platforms must comply with HIPAA for U.S. patient data, GDPR for EU data protection, HITRUST and ISO 27001 for security governance, and increasingly the EU AI Act for clinical AI systems. Additional regulatory review may apply if models qualify as FDA Software as a Medical Device. Enterprises must also enforce consent management, audit trails, data minimization, and explainability.
Q5. What is the ROI of predictive patient analytics for large hospitals?
Large hospitals typically realize ROI through reduced readmissions, shorter length of stay, lower ICU escalation, and improved staffing efficiency. Mature deployments often deliver measurable financial returns within 9 to 18 months. Clinical ROI includes earlier intervention, improved outcomes, and higher care continuity. Financial ROI compounds over time as predictive systems expand into population health and payer coordination.