Smartwatches, fitness bands, and biosensors generate billions of health data points every day. Through these wearables, patients track their heart rate, oxygen levels, sleep cycles, and glucose in real time. However, many healthcare organizations still do not capture this data in their clinical workflows. This leads to a significant gap in diagnosis and care, impacting both patient outcomes and revenue.
The main issue is fragmentation. Wearable data is stored separately and is not connected to the systems that clinicians actually use. Without a unified, real-time data layer, healthcare organizations cannot respond to signals that could prevent hospital stays, identify early signs of decline, or personalize treatment effectively.
When wearable health data integrates into EHR systems using purpose-built APIs and interoperability frameworks, everything changes. Care teams can see data continuously, making decision-making proactive instead of reactive. This improves patient outcomes and boosts operational efficiency. Intellivon helps healthcare organizations establish this infrastructure from start to finish. In this blog, we will discuss how we achieve this integration.
Why Hospitals Are Investing in Wearable Health Data
Hospitals invest in wearable health data to reduce costs, manage chronic diseases at scale, and move care beyond hospital visits into continuous, remote monitoring models. The global wearable healthcare devices market is valued at about $70–71 billion in 2024. It is projected to reach around $379 billion by 2035, growing at a roughly 16–17% CAGR.
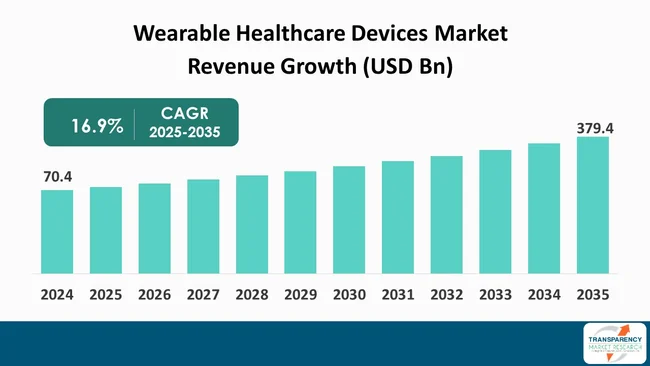
Modern health systems are facing a structural bottleneck that physical infrastructure can no longer solve alone. Therefore, hospitals are pivoting toward wearable integration to manage high-acuity patients without the overhead of physical facility expansion.
1. Growth of Remote Patient Monitoring Programs
Remote patient monitoring (RPM) has evolved from a niche pilot into a core enterprise strategy. Consequently, health systems leverage these programs to capture recurring reimbursement. This shift improves longitudinal patient outcomes at scale.
Furthermore, RPM allows streamlined clinical teams to oversee large populations via automated dashboards. However, the true value lies in the predictive capability of these systems.
They flag deteriorating health status before an emergency visit becomes inevitable. This directly addresses the chronic staffing shortages currently plaguing the industry.
2. Continuous Patient Data
Standard clinical snapshots often miss the intermittent symptoms that define chronic conditions. In contrast, wearables provide a longitudinal view of a patient’s health journey.
This eliminates the “white coat effect” entirely. Moreover, these insights allow specialists to refine medication dosages with surgical precision.
When clinicians possess a 24/7 data trail, they spend less time on discovery. Instead, they focus on high-value decision-making. Thus, continuous monitoring bridges the gap between episodic visits and real-life recovery.
3. Wearables Supporting Preventive Healthcare Models
Preventive care is the most effective hedge against ballooning chronic disease costs. Wearable devices act as sophisticated early-warning systems. They identify subtle trends that escape the naked eye during brief consultations.
For instance, a persistent change in resting heart rate can signal an impending cardiac event. By intervening at this stage, providers avoid high-cost interventions.
Therefore, this investment is fundamentally a move toward long-term risk mitigation. It transforms the provider from a reactive healer into a proactive health partner.
By digitizing the patient journey, enterprises shift from reactive care to a proactive, scalable management model. This transition ensures that hospital resources remain focused on high-complexity cases while maintaining a constant presence in the home.
Why Wearable Data Cannot Connect Directly to EHR
The primary reason for this disconnect is a fundamental mismatch in system architecture and intent.
EHRs were built to be secure, static repositories for billing and discrete clinical events, while wearables are high-frequency data broadcasters that lack the standardized protocols necessary for a “plug-and-play” relationship.
1. Limitations of Direct Wearable-to-EHR Integration
Direct integration often fails because EHR systems are not designed to handle the sheer volume of “noise” generated by wearables. A single smartwatch can produce thousands of data points daily, ranging from heart rate variability to sleep stages.
If this raw data flowed directly into a patient’s chart, it would overwhelm the storage capacity and the user interface. Consequently, clinicians would face “alert fatigue,” where critical health signals are buried under a mountain of insignificant physiological fluctuations.
Furthermore, most EHRs lack the native APIs to authenticate thousands of individual consumer devices securely.
2. Clinical Validation Requirements for Device Data
Before a physician can make a diagnostic decision, the data must be clinically validated. Consumer wearables often use proprietary algorithms to calculate metrics like “readiness” or “stress scores,” which do not always align with medical-grade standards.
Hospitals must ensure that the data entering the EHR meets strict accuracy thresholds. Without a middle layer to verify the device’s calibration and data integrity, the risk of “garbage in, garbage out” becomes a legal and clinical liability.
Healthcare leaders must prioritize data that is actionable and medically defensible rather than just plentiful.
3. Interoperability Gaps Across Healthcare Systems
Interoperability remains a fragmented landscape despite the progress of HL7 and FHIR standards. Different wearable manufacturers use various data formats, many of which are “walled gardens.”
For instance, a data packet from a Garmin device might be structured differently than one from an Apple Watch or a Medtronic sensor. Without a centralized translation layer, a hospital would need to build and maintain hundreds of individual connections.
This lack of a universal language makes direct integration a logistical nightmare for IT departments already stretched thin by cybersecurity demands.
In summary, the technical and clinical hurdles of direct integration make a middleware approach the only viable path for scalable enterprise health tech. Bridging these gaps is about ensuring data becomes a tool for better outcomes rather than a burden on the system.
Types of Wearable Data Hospitals Integrate into EHRs
Clinical teams now prioritize specific data points to drive better patient outcomes. However, not every metric from a consumer device is useful for a medical record.
Strategically, hospitals focus on high-impact streams that reflect real-world recovery and chronic disease status.
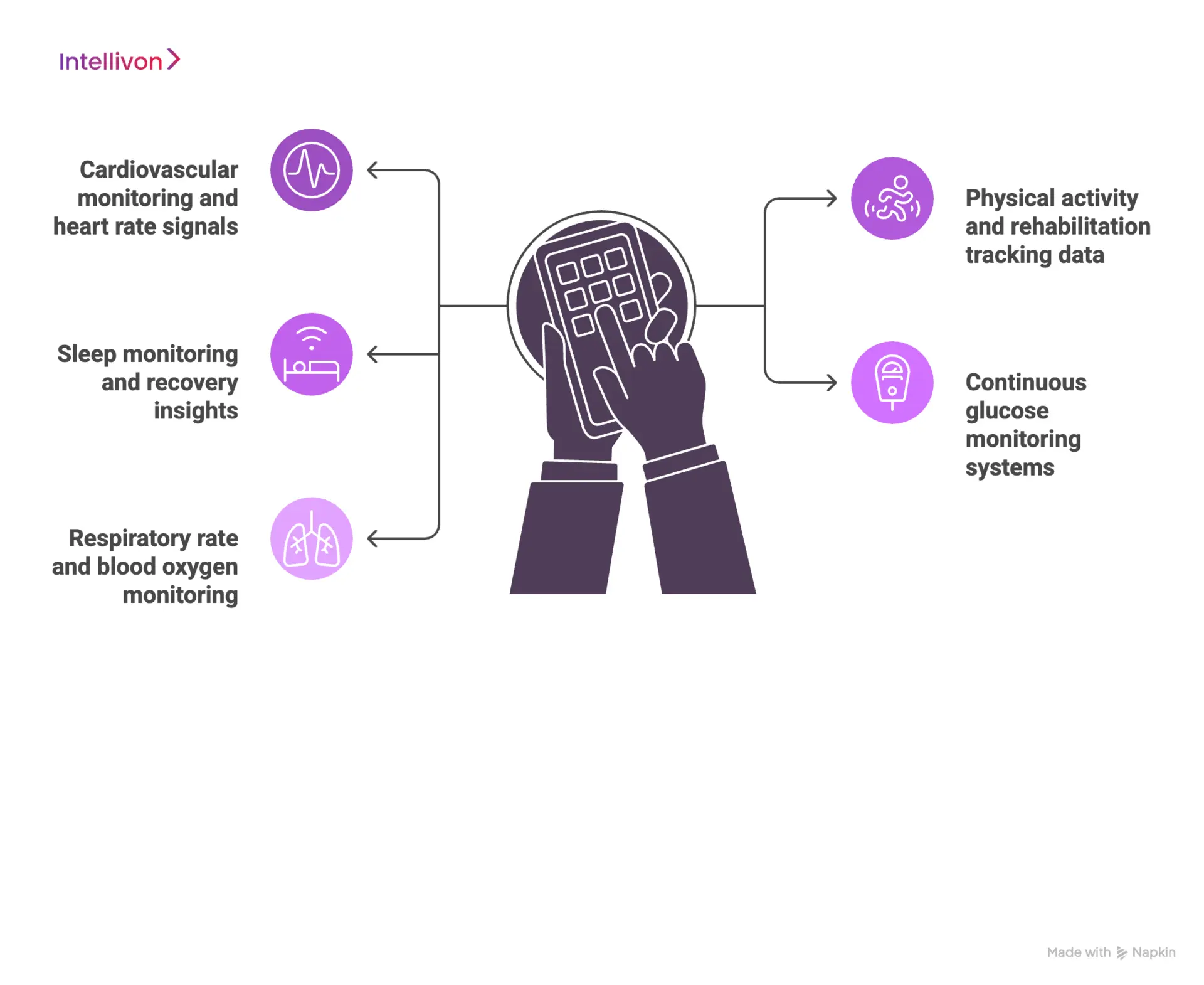
1. Cardiovascular monitoring and heart rate signals
Heart rate tracking is the most common integration in modern cardiology. Specifically, clinicians look for resting heart rate trends and heart rate variability.
These metrics often signal early autonomic stress or potential cardiac events. Consequently, integrating EKG-capable watch data allows for continuous atrial fibrillation monitoring.
This shift moves care from reactive office visits to proactive remote surveillance.
2. Physical activity and rehabilitation tracking data
Recovery after surgery depends heavily on physical movement. Therefore, surgeons track step counts and gait symmetry through wearable sensors. If a patient’s mobility drops, the EHR triggers an automated alert for the care team.
This data provides an objective view of a patient’s progress at home. As a result, providers can intervene early if a rehabilitation plan is failing.
3. Sleep monitoring and recovery insights
Sleep architecture serves as a powerful proxy for systemic health. For example, deep sleep and REM cycles correlate with neurological recovery and mental health. Consequently, physicians use this data to manage chronic pain or depressive disorders.
Integrating these insights offers a holistic view of the patient’s lifestyle. This context helps doctors adjust treatments based on actual rest patterns.
4. Continuous glucose monitoring systems
Continuous Glucose Monitors (CGMs) provide a full “movie” of metabolic health. In contrast, traditional finger-prick tests only offer a single snapshot in time. Therefore, syncing CGM data with the EHR is vital for diabetes management.
It allows endocrinologists to see how diet and exercise impact blood sugar in real-time. This integration significantly reduces the risk of dangerous hypoglycemic episodes.
5. Respiratory rate and blood oxygen monitoring
Monitoring blood oxygen is essential for managing chronic lung conditions. Specifically, it helps track patients with COPD or asthma during flare-ups. In addition, respiratory rate serves as an early warning sign for pneumonia or heart failure.
Automating this data flow ensures that home oxygen therapy is adjusted accurately. Thus, patients receive the right level of care without unnecessary hospital visits.
In summary, selecting the right data types is the foundation of a successful remote monitoring strategy. When hospitals map these streams correctly, they transform raw numbers into a clear narrative of patient health.
How Wearable Health Data Flows into Hospital Systems
A reliable data pipeline requires more than a simple Bluetooth connection. For an enterprise, the focus is on a secure, multi-stage architecture.
This ensures data integrity from the patient’s home to the hospital’s server. Each step must maintain strict compliance while filtering out unnecessary noise.
1. Patient wearable devices and sensor networks
The process begins at the “edge” with the patient’s hardware. These sensors track physiological signals such as heart rate or glucose levels. Most devices operate within a Personal Area Network using low-energy protocols.
Consequently, they transmit encrypted packets to a nearby receiver. This initial step is critical for success. Therefore, the quality of the raw signal determines the accuracy of all clinical downstream analysis.
2. Mobile health apps and device data gateways
The smartphone acts as a primary gateway for the wearable data. Specifically, a dedicated mobile app aggregates the raw sensor information. However, these apps do more than just relay data. They also perform initial “edge” processing to save bandwidth.
This means the app can flag immediate anomalies before the data leaves the patient. Therefore, the mobile layer serves as the first filter for data quality and security.
3. Cloud health data processing platforms
Once data leaves the phone, it enters a secure, HIPAA-compliant cloud environment. These platforms serve as the heavy-lifting engine for the entire integration. In this stage, proprietary algorithms normalize the data into a standard format.
Furthermore, the cloud layer manages the massive scale of incoming streams. As a result, the hospital does not manage the storage burden of raw, high-frequency telemetry.
4. Healthcare interoperability integration layers
The refined cloud data must now be translated into a clinical language. This is where integration engines play a vital role. These systems use the FHIR standard to map data into clinical “Resources.”
Specifically, they ensure that a heart rate data point fits perfectly into a medical record field. Consequently, this layer bridges the gap between consumer tech and medical-grade software. This translation is essential for system-wide compatibility.
5. EHR ingestion and clinical monitoring dashboards
The final destination is the Electronic Health Record system itself. However, hospitals rarely dump all this data into the main chart. Instead, they use secondary dashboards or population health modules.
These interfaces highlight only the most critical trends for the staff. Therefore, clinicians can focus on patients who need immediate attention. This prevents the staff from being overwhelmed by healthy, routine data points.
In summary, building this flow is a strategic investment in long-term patient engagement. When executed correctly, it turns a passive monitoring tool into a proactive clinical asset. This infrastructure allows hospitals to scale their care delivery without increasing their physical footprint.
Architecture for Wearable Data Integration Platforms
A high-performance architecture functions like a specialized refinery. It takes raw, unrefined signals from a patient and converts them into high-value clinical intelligence.
Each layer of the stack must be designed for maximum uptime and absolute data fidelity.
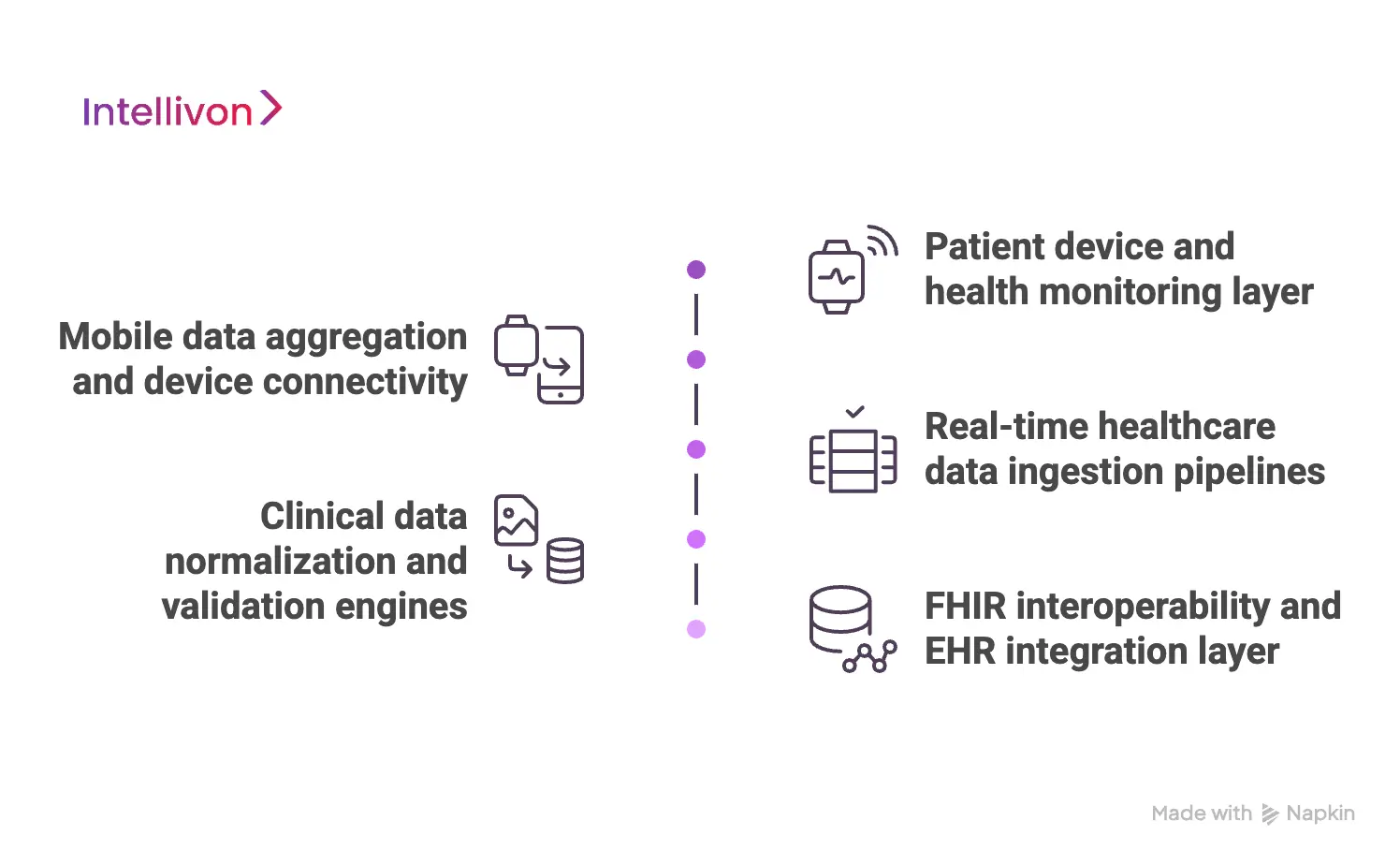
1. Patient device and health monitoring layer
The foundation of the architecture is the “Edge Layer.” This includes a variety of sensors like smartwatches, continuous glucose monitors, and blood pressure cuffs. These devices collect high-frequency data points in real-world settings.
However, the architecture must account for intermittent connectivity and varying battery lives. Therefore, the device layer must support local data caching to prevent information loss. This ensures that a patient’s health narrative remains continuous even during cellular outages.
2. Mobile data aggregation and device connectivity
The mobile application serves as the primary gateway and local processing hub. Specifically, it manages the secure Bluetooth pairing and data syncing from the wearable. In addition, the mobile layer handles user identity management and consent.
This ensures that the person wearing the device is the same person in the medical record. Consequently, the app performs a vital “sanity check” on the data before it ever hits the network. Therefore, the mobile gateway is the first line of defense for data integrity.
3. Real-time healthcare data ingestion pipelines
Once data is transmitted, it enters a high-throughput ingestion pipeline. These pipelines are often built on technologies like Apache Kafka or AWS Kinesis. They are designed to handle millions of simultaneous events without latency.
Specifically, the system must sort and prioritize data based on clinical urgency. For example, a heart rate spike should be processed faster than a routine step count update. As a result, the enterprise can support real-time monitoring at a massive scale.
4. Clinical data normalization and validation engines
Raw data from different manufacturers rarely looks the same. Therefore, a robust normalization engine is required to “clean” the incoming streams. This layer removes artifacts and validates the data against medical-grade thresholds.
Furthermore, it applies business logic to convert raw units into standard clinical measurements. Specifically, it ensures that every data point is timestamped and attributed correctly. Consequently, this engine prevents “dirty data” from reaching the clinical decision-makers.
5. FHIR interoperability and EHR integration layer
The final layer is the interoperability gateway, which speaks the language of the EHR. Modern systems utilize the FHIR (Fast Healthcare Interoperability Resources) standard for this purpose.
This layer maps the normalized data into specific HL7 FHIR “Resources” like Observation or DeviceMetric. Furthermore, it manages the secure API handshake with the hospital’s core systems.
As a result, the integration remains stable even if the hospital switches EHR vendors. This decoupling is essential for long-term strategic flexibility.
Ultimately, a well-architected platform reduces the burden on IT and clinical teams alike. It provides a single, secure pipe for all remote patient data. This allows the enterprise to focus on care delivery rather than troubleshooting hardware connectivity.
Interoperability Standards for Wearable Integration
The industry has moved toward open, web-based standards to solve the connectivity crisis. These frameworks allow different systems to talk to each other securely and predictably. Consequently, they form the backbone of any modern remote patient monitoring strategy.
1. FHIR APIs for healthcare interoperability
The Fast Healthcare Interoperability Resources (FHIR) standard is the modern gold standard. It uses a RESTful API approach, which is familiar to any software developer. Specifically, it breaks down health data into modular “Resources.”
These can be easily queried, updated, or deleted as needed. Therefore, hospitals can pull specific wearable metrics without downloading the entire patient history. This efficiency is vital for maintaining high system performance.
2. HL7 messaging frameworks in hospital systems
While FHIR is the future, legacy HL7 v2 messaging still dominates many internal hospital workflows. These frameworks use “push” notifications to send data between labs, pharmacies, and the EHR. Consequently, integration platforms must often translate modern wearable data back into HL7 formats.
This ensures that the new technology remains compatible with older infrastructure. Thus, supporting both standards is necessary for a seamless enterprise-wide rollout.
3. SMART on FHIR clinical application frameworks
SMART on FHIR allows developers to create “plug-and-play” apps that run inside the EHR. For example, a clinician could open a specialized view of a patient’s glucose trends directly from the chart.
This framework handles the complex authentication and authorization through OAuth2. As a result, doctors do not need to log into multiple portals to see wearable data. Therefore, it significantly reduces the cognitive load on clinical teams.
4. IoT healthcare protocols
Beyond the EHR, devices use specific IoT protocols like MQTT or CoAP for data transmission. These protocols are designed for low-power sensors that may have weak internet connections. Specifically, they use a “publish-subscribe” model to move data efficiently with minimal overhead.
Furthermore, they support robust encryption to protect sensitive data at the source. Consequently, these protocols ensure that the “edge” of the network remains secure and reliable.
In summary, interoperability standards are the “rules of the road” for digital health. By adhering to these frameworks, enterprises ensure their systems remain flexible and future-proof. This technical alignment is the first step toward a truly connected care ecosystem.
Clinical Systems Powered by Wearable Data Platforms
The true value of an integration platform lies in its ability to power specialized clinical workflows. These systems use filtered wearable data to drive automated interventions and predictive modeling.
As a result, hospitals can move from reactive treatment to proactive wellness management across various specialties.
1. Remote patient monitoring for chronic care
Remote Patient Monitoring (RPM) platforms act as a continuous safety net for high-risk patients. Specifically, these systems track vitals like blood pressure and weight for patients with hypertension or heart failure. If a metric trends outside of a safe range, the system triggers a clinical alert.
Therefore, care managers can intervene before a patient requires an emergency room visit. This proactive approach significantly reduces readmission rates and lowers the overall cost of care.
2. Cardiac monitoring and early risk alerts
Wearable platforms have revolutionized how hospitals manage cardiac health at scale. By integrating continuous EKG and heart rate data, clinicians can identify asymptomatic arrhythmias like Atrial Fibrillation.
Furthermore, advanced algorithms can detect subtle changes in heart rate variability that precede cardiac stress. Consequently, these early risk alerts allow for lifestyle or medication adjustments in real-time. Thus, the hospital can prevent major cardiac events through early detection.
3. Post-surgical recovery monitoring systems
The period immediately following discharge is the most vulnerable time for surgical patients. Therefore, hospitals use wearable sensors to monitor mobility, wound temperature, and oxygen levels.
If a patient remains sedentary for too long, the system encourages movement to prevent blood clots. In addition, tracking heart rate and temperature can provide early signs of post-operative infection.
As a result, surgical teams can monitor the recovery of dozens of patients from a single centralized dashboard.
4. Diabetes management using wearable data
Continuous Glucose Monitor (CGM) integration is the most mature application of wearable data in modern medicine. These systems provide a constant stream of metabolic data directly to the endocrinologist’s portal.
Specifically, they allow for “time-in-range” analysis, which is a more accurate measure of health than a single A1c test. Furthermore, patients receive immediate feedback on how their diet and exercise affect their glucose.
This closed-loop communication improves patient adherence and long-term health outcomes.
5. Population health monitoring infrastructure
At the enterprise level, wearable data feeds into large-scale population health dashboards. These systems aggregate anonymized data to identify health trends across specific zip codes or demographics.
Specifically, CFOs and COOs use this data to allocate resources where they are needed most. For example, a spike in respiratory issues in a certain area might prompt the opening of a mobile clinic.
Consequently, wearable integration becomes a tool for strategic community health planning.
In summary, wearable data platforms are the engine behind modern, distributed healthcare systems. They allow providers to extend their reach far beyond the clinical setting. By empowering these systems, hospitals can deliver higher-quality care to more patients with greater efficiency.
How We Integrate Wearable Data Into EHR Systems
Implementing a seamless connection between wearable technology and an Electronic Health Record (EHR) requires a disciplined, multi-layered strategy. For the enterprise, this is not a one-time setup but a scalable architecture designed for long-term growth.
At Intellivon, we specialize in orchestrating these complex AI-driven integrations, ensuring that data moves securely from a patient’s wrist to a clinician’s dashboard with zero friction. This roadmap prioritizes security, data accuracy, and provider experience.
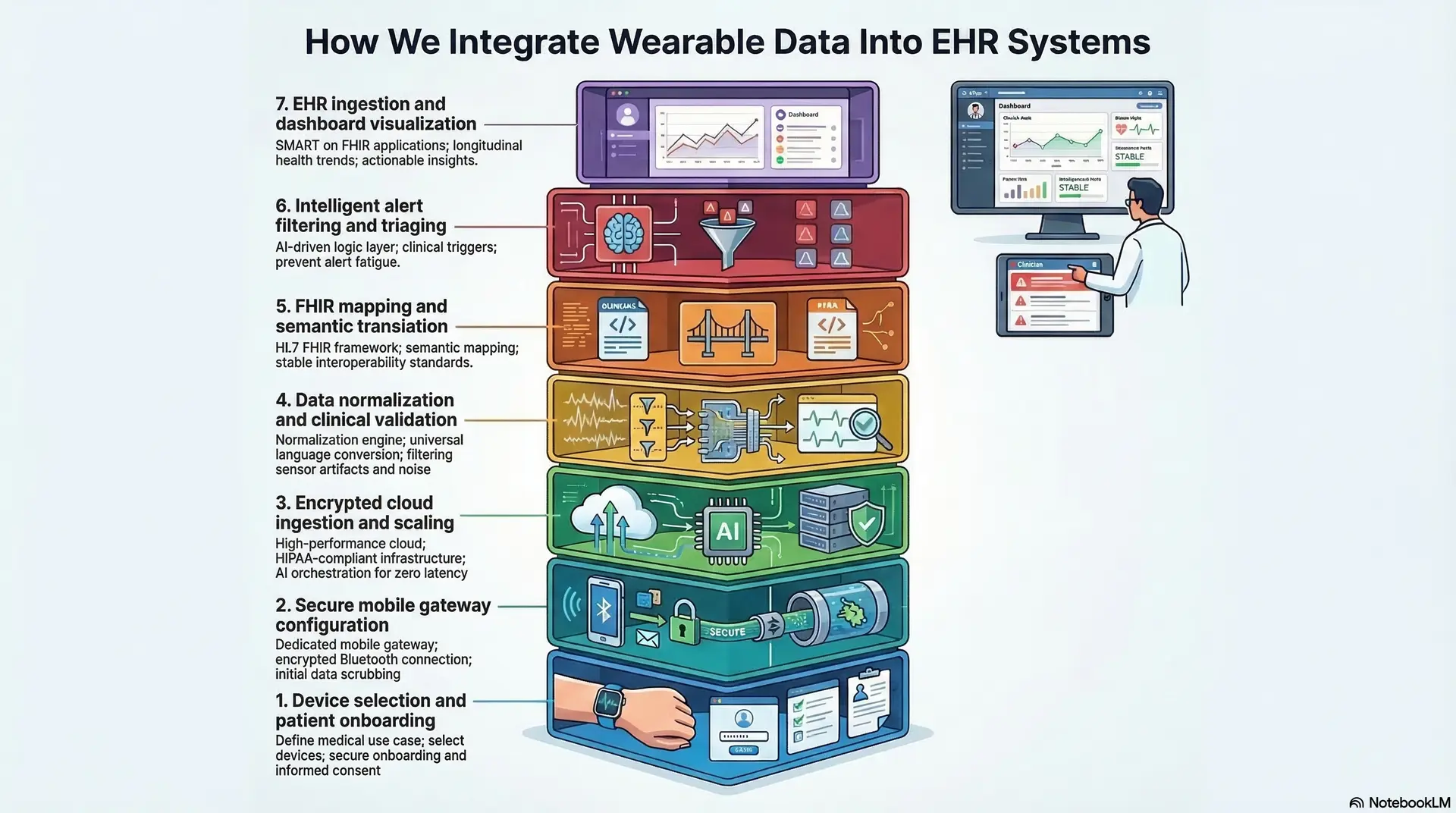
1. Device selection and patient onboarding
The process begins by defining the specific medical use case. We help enterprises select the right devices, such as EKG-capable watches or continuous glucose monitors, based on clinical needs. Once selected, patients are onboarded through a secure mobile interface.
This step ensures that the device is correctly paired and the patient has provided informed consent for data sharing. Consequently, the foundation for high-quality data is established at the very start.
2. Secure mobile gateway configuration
Data must be captured locally before it is sent to the hospital. Specifically, we deploy a dedicated mobile gateway that acts as a secure intermediary. This app manages the encrypted Bluetooth connection with the wearable device.
In addition, it performs initial data scrubbing to remove any redundant or corrupted packets. Therefore, the mobile layer ensures that only clean, authenticated data leaves the patient’s environment.
3. Encrypted cloud ingestion and scaling
Once the data is transmitted, it enters a high-performance cloud environment. This infrastructure is designed to handle the massive velocity of incoming streams from thousands of users simultaneously.
At this stage, Intellivon’s AI orchestration layers manage the workload to ensure zero latency. Furthermore, the cloud environment is fully HIPAA-compliant to protect sensitive health information. As a result, the hospital’s internal servers are never overwhelmed by raw telemetry.
4. Data normalization and clinical validation
Raw data from different manufacturers often uses proprietary formats. Therefore, we apply a normalization engine to convert various signals into a universal language. This step involves validating the data against medical-grade thresholds.
Specifically, we filter out “noise” like sensor artifacts caused by movement. Consequently, this ensures that the information reaching the doctor is clinically accurate and reliable.
5. FHIR mapping and semantic translation
To talk to an EHR, the normalized data must be mapped to specific interoperability standards. We utilize the HL7 FHIR (Fast Healthcare Interoperability Resources) framework for this translation.
Each data point is converted into a FHIR “Observation” or “DiagnosticReport” resource. This semantic mapping ensures that the EHR understands exactly what the data represents. Therefore, the integration remains stable even if the hospital updates its core clinical software.
6. Intelligent alert filtering and triaging
Clinicians cannot review every single heart rate update. Specifically, we implement an AI-driven “logic layer” that monitors for specific clinical triggers. If a patient’s vitals trend toward a danger zone, the system generates a high-priority alert.
Conversely, routine data is summarized and stored without interrupting the clinical workflow. As a result, this prevents alert fatigue and allows nurses to focus on patients who need immediate care.
7. EHR ingestion and dashboard visualization
The final step is the secure injection of data into the clinical workflow. We integrate these insights directly into the EHR via SMART on FHIR applications or dedicated portals. This allows physicians to view longitudinal health trends without leaving the patient’s chart.
Finally, we provide intuitive dashboards that highlight actionable insights. This closes the loop between remote monitoring and active clinical intervention.
In summary, integrating wearable data is a strategic evolution for any modern healthcare enterprise. It transforms the way care is delivered by providing a continuous, data-driven view of the patient. By following this rigorous seven-step framework, hospitals can scale their digital health initiatives with confidence.
Challenges Hospitals Face in Integrating Wearable Data
Navigating the transition from traditional care to a data-driven model requires a deep understanding of existing system limitations. Addressing these challenges is where strategic partnerships become the deciding factor between a pilot program and a permanent, scalable solution.
1. Data overload and clinical signal filtering
The sheer volume of data generated by a single wearable device can be staggering. Clinicians are already burdened by administrative tasks and cannot manage thousands of new data points per patient. Consequently, without a filtering mechanism, critical health signals are often lost in the noise. Therefore, “alert fatigue” becomes a significant risk to patient safety.
How Intellivon fixes this: We deploy advanced AI orchestration layers that act as a sophisticated “clinical sieve.” Our algorithms analyze raw telemetry in real-time to identify and highlight only the clinically significant deviations. Specifically, we suppress routine data while escalating high-priority alerts directly to the care team’s workflow.
2. Device fragmentation across wearable vendors
The wearable market is highly fragmented, with dozens of manufacturers using proprietary data formats. This lack of standardization makes it difficult for hospitals to offer a “bring your own device” (BYOD) program. Historically, IT departments had to build custom connectors for every new device. As a result, scaling a monitoring program becomes a costly and slow process.
How Intellivon fixes this: Our platform features a vendor-agnostic ingestion engine. We provide a unified API that abstracts the complexity of different hardware providers. Whether a patient uses an Apple Watch, a Garmin, or a specialized medical sensor, our system normalizes that data into a single, clean format. Consequently, your enterprise can support a diverse device ecosystem without increasing IT overhead.
3. Interoperability across legacy hospital systems
Many hospitals still operate on legacy EHR architectures that were not built for modern web APIs. These systems often lack the native ability to ingest high-frequency external data. Therefore, bridging the gap between a modern cloud-based wearable platform and a 20-year-old on-premise EHR is a major technical barrier. This friction often results in data silos that prevent a holistic view of the patient.
How Intellivon fixes this: We utilize deep expertise in FHIR and HL7 standards to build robust interoperability bridges. Specifically, we create customized integration layers that speak the language of your specific legacy systems. Furthermore, we ensure that the data flow is bi-directional. This allows the wearable data to enrich existing patient records without requiring a total system overhaul.
4. Regulatory concerns around patient data
Security and compliance are non-negotiable in healthcare. Moving sensitive patient data from a consumer device through a public network into a hospital creates multiple points of vulnerability. Furthermore, evolving HIPAA and GDPR regulations place a heavy burden of proof on the hospital. As a result, many organizations hesitate to integrate wearables due to the perceived legal risk.
How Intellivon fixes this: We bake security into the very core of our integration architecture. Every data point is encrypted both at rest and in transit using enterprise-grade protocols. In addition, we provide comprehensive audit trails and automated compliance reporting. This ensures that your integration meets or exceeds all current regulatory requirements, giving your legal and risk teams total peace of mind.
5. Scaling infrastructure for millions of signals
A successful remote monitoring program can quickly scale from a few hundred patients to hundreds of thousands. Most traditional hospital IT infrastructures are not designed to handle this kind of exponential data growth. Specifically, the storage and processing costs can spiral out of control if the architecture is not optimized for the cloud. Therefore, hospitals need a way to scale their capabilities without a corresponding spike in capital expenditure.
How Intellivon fixes this: We leverage cloud-native, serverless architectures that scale automatically based on demand. Specifically, our ingestion pipelines are built to handle millions of simultaneous signals with high availability. Consequently, you only pay for the capacity you use. This allows your enterprise to grow its remote care programs sustainably and predictably.
In summary, while the challenges of integration are significant, they are not insurmountable. By identifying these bottlenecks early and applying specialized technical solutions, hospitals can turn these obstacles into competitive advantages.
Conclusion
The future of healthcare depends on seamless data mobility. By bridging the gap between wearables and EHRs, enterprises unlock proactive care and operational excellence. This transformation reduces provider burnout while improving patient outcomes.
Consequently, organizations that adopt these AI-driven integrations today will lead the market tomorrow. Intellivon is your strategic partner for this transition. We build the secure, scalable infrastructure your enterprise needs to thrive.
Build an EHR-Integrated Wearable Data Platform With Intellivon
At Intellivon, wearable health data platforms are engineered as a clinical data infrastructure, not as simple device integrations layered onto hospital systems. Our platforms enable hospitals to ingest, normalize, and deliver continuous wearable health data directly into EHR environments.
Each solution is designed for regulated healthcare ecosystems. Wearable integration platforms must handle continuous patient data streams, maintain clinical data accuracy, and ensure compliance with healthcare interoperability standards. As a result, hospitals gain real-time patient visibility while keeping their existing EHR workflows intact.
Why Partner With Intellivon?
- FHIR-Native Interoperability Architecture: Our platforms use FHIR-based APIs and healthcare interoperability frameworks to integrate wearable health data into EHR systems without disrupting existing clinical workflows.
- Real-Time Health Data Streaming Infrastructure: We build event-driven data pipelines that ingest wearable signals continuously, enabling clinicians to monitor patient vitals and receive alerts for abnormal health patterns.
- Clinical Data Normalization and Validation: Wearable signals must be converted into clinically meaningful data. Our systems validate, normalize, and map device signals into structured EHR-compatible formats.
- Governance-First Healthcare Data Architecture: Every platform includes audit trails, access controls, and consent management frameworks to ensure compliance with HIPAA and healthcare data governance requirements.
- Scalable Remote Patient Monitoring Platforms: Our architecture supports thousands of connected devices and patients, enabling hospitals to scale remote care programs without compromising performance or data security.
If your organization plans to integrate wearable health data into clinical systems, Intellivon can help you design and build a secure, scalable, and interoperability-ready platform tailored for modern healthcare environments.
FAQs
Q1. How do hospitals connect wearables to EHR systems?
A1. Hospitals connect wearables to EHR systems through integration platforms that collect device data, process it using APIs, and send structured data into the EHR. Most systems use interoperability standards like FHIR to ensure the data fits clinical workflows.
Q2. What standards support wearable health integration?
A2. Wearable health integration typically uses standards such as FHIR APIs, HL7 messaging, and SMART on FHIR frameworks. These standards allow wearable data to be structured and shared securely across healthcare systems.
Q3. Is wearable data reliable for clinical decisions?
A3. Wearable data can support clinical decisions when it is validated, filtered, and normalized before entering the EHR. Hospitals often use analytics and clinical rules to separate meaningful health signals from raw device data.
Q4. How secure is patient-generated health data?
A4.Patient-generated health data is secured using encryption, identity verification, and access controls. Hospitals also follow healthcare regulations like HIPAA to ensure patient data remains protected throughout the integration process.
Q5. How long does wearable integration take to build?
A5. Building a wearable integration platform usually takes 4–8 months, depending on device integrations, interoperability requirements, and EHR system complexity. Large hospital systems may require longer timelines.