Building a healthcare startup involves making many key decisions before seeing your first patient. The choice of an EHR system often comes quickly, but is treated almost as an afterthought. However, this decision, made early and under pressure, shapes clinical workflows, billing practices, compliance, and ultimately how fast the business can grow.
Problems usually emerge later. Within six months, the team might find themselves working around the system instead of using it. At the same time, customization requests start to pile up, and integrations end up taking months. This is a common issue in EHR adoption within startups. This happens when the EHR architecture isn’t seen as a key decision from the beginning.
Intellivon helps healthcare startups avoid this path. They build platforms from scratch, customize Epic and Cerner environments, integrate clinical AI, and ensure FHIR and HL7 compliance from the ground up. This blog details every major decision point in the process, helping your team approach EHR customization with the clarity it needs.
Why Startups Are Building Custom EHR Systems
Choosing between a custom EHR and a vendor solution is a strategic choice about who controls your data, how your workflows evolve, and what your long-term costs look like.
Most hospitals struggle with limited customization in commercial EHR systems. In fact, around 75–80% report frustration with rigid workflows and a lack of flexibility.
As a result, many now look for configurable vendors or fully custom-built platforms that adapt to their care models. In fact, EHR systems customized to specific company requirements are gaining traction where they are treated as a core IP asset and can be easily monetized.
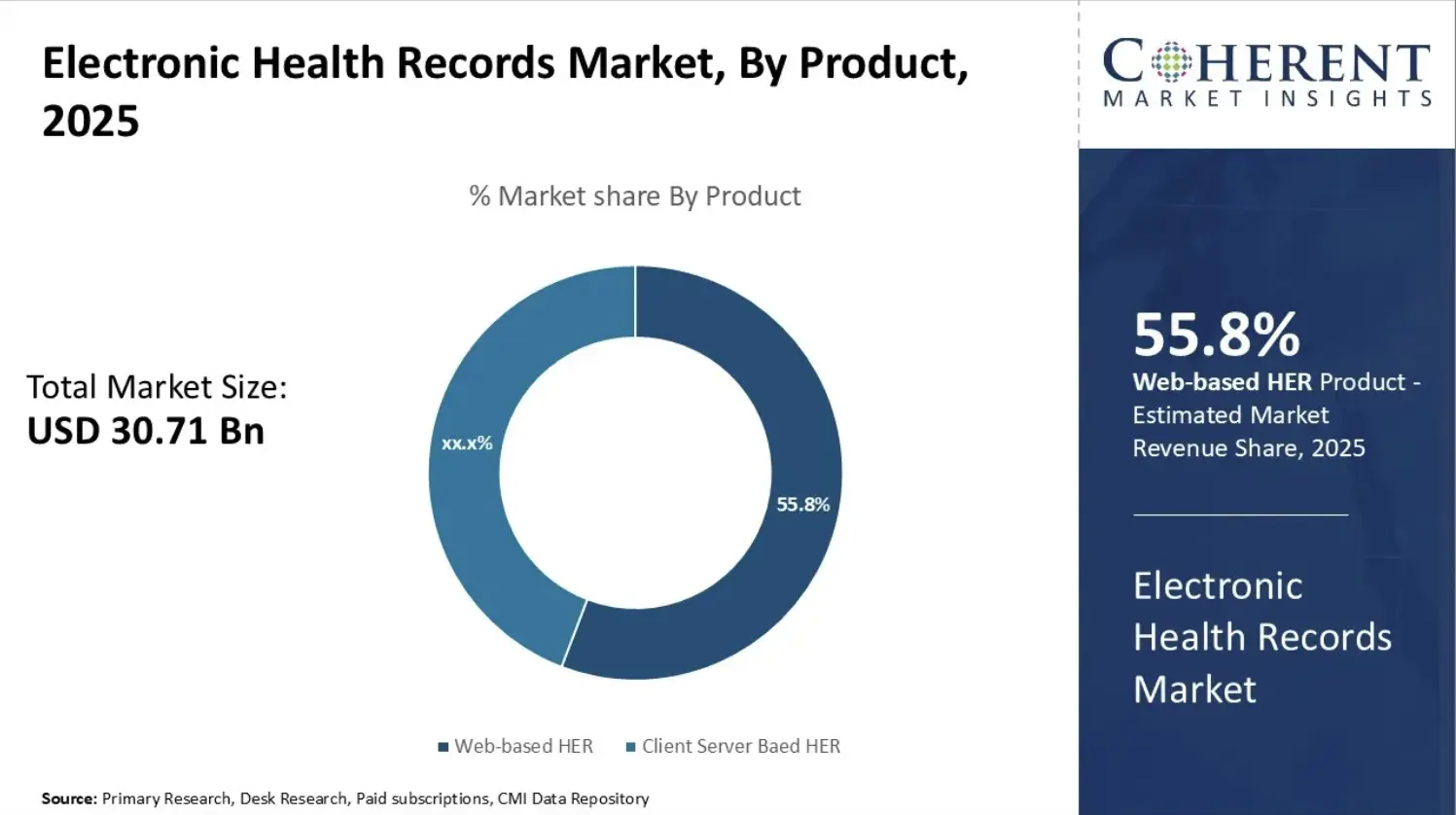
The global EHR software market was valued at approximately USD 30–35 billion in 2025. It is expected to reach the mid-to-high USD 30 billion range by 2032. This reflects a steady CAGR of around 8–10%. As a result, the market continues to expand at a consistent pace, driven by long-term healthcare digitization and system modernization efforts.
Choosing between a standard platform and a bespoke solution is a critical decision. However, this choice often dictates your startup’s long-term scalability and clinical speed. Therefore, founders must evaluate if their current software supports their unique vision.
1. When off-the-shelf systems silently break growth
Generic EHRs usually target the average medical clinic. Consequently, these systems often fail to support disruptive healthcare startups. For example, rigid interfaces can slow down your providers significantly. In addition, basic platforms frequently lack the APIs needed for modern wearable data.
As a result, your unique value proposition becomes buried under manual workarounds. This friction eventually stops true enterprise expansion in its tracks.
2. Signs your startup is outgrowing basic tools
You will likely notice operational friction first in your clinical workflows. For instance, providers might click through ten screens for one prescription.
Furthermore, your “automated” reporting might still require manual Excel exports every week. High patient churn is another clear indicator of software failure.
When the software dictates your protocols instead of supporting them, it becomes a liability. Therefore, recognizing these early red flags is essential for maintaining your competitive edge.
3. The hidden cost of delaying customization
Waiting too long to customize creates massive technical debt. This debt eventually drains your capital and slows down innovation. Moreover, every month spent on a basic system leads to disorganized data.
This makes future migration much more difficult and expensive. You also lose the chance to collect high-quality data for machine learning. Thus, the longer you wait, the harder it is to untangle your operations.
4. When a custom EHR becomes unavoidable
Customization becomes essential when you move into specialized care models. In addition, high-volume telehealth requires a very specific patient journey. If a standard template cannot replicate your workflow, you must build your own architecture.
This move protects your intellectual property and improves clinical outcomes. At this stage, a custom EHR is a fundamental engine for growth. Therefore, it directly increases your investor valuation and market authority.
Investing in a custom foundation ensures your platform remains a powerful asset. It prevents your software from becoming an anchor during rapid scaling phases.
What Actually Breaks Without EHR Customization
Generic platforms often create a “glass ceiling” for healthcare innovation. Therefore, relying on standard software eventually leads to deep operational fractures.
These breaks happen slowly at first, yet they soon compromise your entire clinical delivery. Consequently, your investment in a rigid system turns into a constant source of friction.
1. Fragmented patient data across tools
Standard systems often struggle to speak with external health applications. As a result, your patient data becomes trapped in disconnected silos. For instance, diagnostic results may not sync with treatment plans automatically.
Furthermore, manual data entry increases the risk of human error across your platform. This fragmentation forces clinicians to hunt for information during critical moments. Thus, the lack of a unified data layer weakens your entire service model.
2. Operational chaos in care coordination
Care coordination requires a seamless flow between different medical departments. However, off-the-shelf EHRs usually lack the flexible task-routing tools you need. If your nurses must call doctors to confirm simple status updates, your workflow is broken.
In addition, rigid software cannot adapt to your specific internal protocols. This leads to missed follow-ups and delayed patient care cycles. Therefore, customization is the only way to synchronize your team effectively.
3. Poor clinical decision visibility
Decision-makers need real-time data to improve patient outcomes. Yet, basic systems rarely offer deep, customizable analytics dashboards. You might find yourself guessing about provider efficiency or treatment success rates.
Moreover, without custom reporting, identifying high-risk patient trends becomes nearly impossible. This lack of transparency prevents you from making evidence-based strategic shifts. Consequently, your clinical leadership loses the ability to drive high-level performance.
4. Scaling failures during growth phases
Growth typically amplifies the small inefficiencies in your current software. For example, a system that works for ten patients often crashes with ten thousand. Furthermore, standard EHRs rarely support the rapid onboarding of new medical staff.
If the software is too complex, training costs will skyrocket as you expand. You will also face higher infrastructure costs for features you never use. Thus, failing to customize early makes scaling an expensive and painful process.
Ignoring these technical cracks will eventually lead to a full-scale operational collapse. Therefore, building a custom architecture is the most logical path toward sustainable enterprise growth.
How Founders Should Think About EHR Systems
Successful healthcare leaders view their technology as a strategic moat. Therefore, your digital architecture must do more than just record patient visits.
It should actively accelerate your clinical and business objectives every single day. Consequently, shifting your perspective on software is the first step toward true innovation.
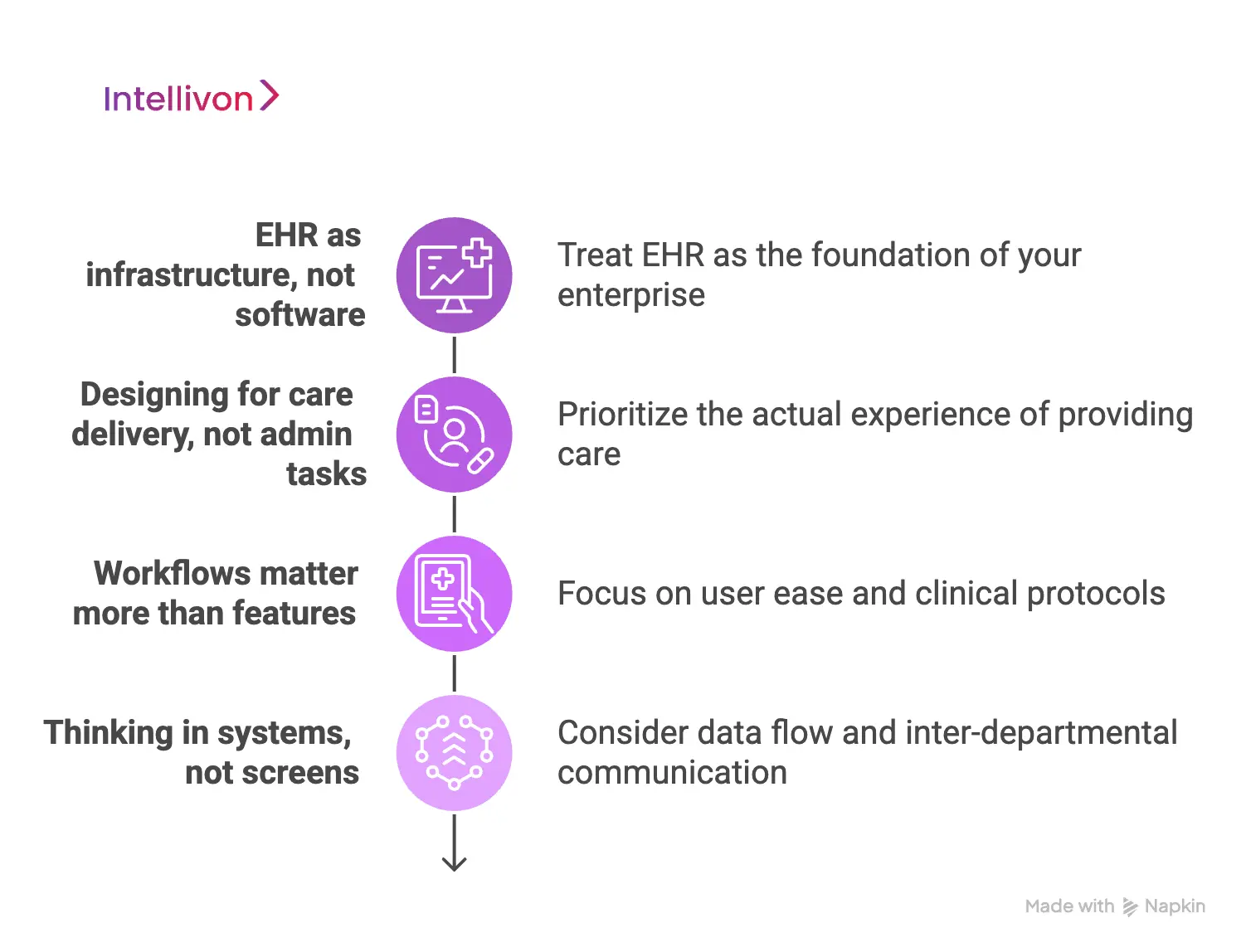
1. EHR as infrastructure, not software
You must treat your EHR as the foundation of your entire enterprise. For example, think of it like the electrical grid of a modern city. If the grid is weak, no amount of high-tech appliances will function properly.
In addition, software updates should never disrupt your core medical services. A custom infrastructure allows for seamless scaling without breaking your internal tools. Thus, investing in a solid base prevents future technical debt from accumulating.
2. Designing for care delivery, not admin tasks
Most legacy systems focus heavily on billing and administrative checkboxes. However, your startup should prioritize the actual experience of providing care. If your doctors spend hours on data entry, they cannot focus on patients.
Therefore, customization allows you to automate the repetitive “paperwork” within the interface. This shift improves provider satisfaction and reduces the risk of clinical burnout. As a result, your platform becomes a tool that clinicians actually enjoy using.
3. Workflows matter more than features
A long list of features often hides a poorly designed product. Instead, you should focus on how easily a user moves through a task. For instance, a “one-click” prescription refill is more valuable than ten complex reporting modules. In addition, your software must mirror your specific clinical protocols exactly.
This alignment ensures that every team member follows the same high standard of care. Therefore, workflow optimization is the most direct path to operational excellence.
4. Thinking in systems, not screens
Avoid the trap of simply adding more buttons to an existing interface. Instead, consider how data flows between different departments in your organization. For example, a lab result should automatically trigger a follow-up task for the nurse. Furthermore, these systems must communicate with your billing and pharmacy partners in real-time.
This holistic approach prevents information from getting stuck in isolated digital corners. Consequently, you create a responsive ecosystem that adapts to patient needs instantly.
A well-designed system acts as a silent partner in your growth strategy. Therefore, choosing a custom path ensures your technology evolves alongside your clinical ambitions.
What EHR Customization Really Involves in 2026
Modern EHR development has moved far beyond simple interface adjustments. In 2026, customization focuses on creating a high-performance engine for clinical and business intelligence.
Therefore, leaders must understand the technical layers that transform a static record into a dynamic asset. This approach ensures your platform remains compliant, scalable, and ahead of market shifts.
1. Workflow-driven system architecture
Architecture in 2026 is defined by modular, event-driven design rather than monolithic blocks. This means each clinical service can scale independently based on actual demand. For instance, your intake module should not crash just because your billing department is processing high volumes.
In addition, using an API-first strategy allows for seamless integration with external diagnostic tools. Consequently, a workflow-driven structure ensures that the system bends to your needs, not the other way around.
2. Custom clinical data models
Standard data models often force unique patient data into generic “buckets.” However, custom models allow you to define structured data points specific to your medical specialty. For example, a cardiology startup needs different data fields than a behavioral health platform. By utilizing FHIR (Fast Healthcare Interoperability Resources) standards, you ensure this data remains mobile and secure.
Furthermore, clean data models are the “golden records” required for future AI training. Thus, high-quality data modeling is a prerequisite for any advanced healthcare enterprise.
3. Automation and decision support layers
Automation has shifted from simple rules to intelligent, context-aware assistance. For instance, modern systems can now automatically classify and route incoming faxes using Intelligent Document Processing (IDP). This can reduce manual processing time by up to 89% in specific clinical workflows.
Moreover, Clinical Decision Support (CDS) layers now offer real-time alerts for potential drug interactions or diagnostic anomalies. These tools act as a safety net for busy providers. Therefore, embedding automation directly into the EHR reduces cognitive load and prevents medical errors.
4. Real-time system orchestration
Orchestration is the ability of your system to interpret and act on data instantly. For example, a critical lab result should automatically trigger a nurse’s task and update the patient portal. In addition, orchestration layers manage the flow of information between IoT wearables and the central record.
This ensures that clinicians see the most current patient status without manual refreshing. As a result, your organization moves from reactive firefighting to proactive, data-driven care. This level of synchronization is what separates market leaders from traditional providers.
Building these layers correctly today prevents the “technical debt” that cripples growth tomorrow. Therefore, a deep commitment to technical customization is the only way to build a truly resilient healthcare platform.
Mapping Care Delivery Before Writing Code
Successful platform development begins with a deep understanding of the clinical floor. Therefore, jumping straight into software development without a mapped journey is a recipe for expensive rework.
Founders must visualize every interaction point before the first line of code is ever written. Consequently, this strategic mapping phase ensures your technology actually serves the humans using it.
1. Breaking down real patient journeys
A patient journey is much more than a simple appointment booking. For instance, it includes the anxiety of waiting for results and the clarity of follow-up instructions. You must map every digital and physical touchpoint in your specific care model.
In addition, consider how data moves from the patient’s home device to the clinician’s dashboard. This granular view allows you to identify exactly where software can add the most value. Thus, a well-mapped journey leads to a more intuitive and sticky user experience.
2. Identifying failure points in workflows
Every clinical process has hidden friction points that slow down care. For example, a delay in lab signatures can stall an entire treatment plan for days. However, custom EHR design allows you to build “fail-safes” directly into the system architecture. By identifying these bottlenecks early, you can automate reminders or escalate urgent tasks.
Moreover, fixing these issues in the design phase is ten times cheaper than fixing them after launch. Therefore, rigorous stress-testing of your workflows is a non-negotiable step for enterprise stability.
3. Designing for non-ideal scenarios
Standard EHRs often assume a “perfect” workflow where everything goes according to plan. Yet, healthcare is inherently unpredictable and full of edge cases. For instance, what happens if a patient loses internet connectivity during a remote consultation? Your system must have offline data syncing or automated recovery protocols.
Furthermore, you should design for cases where data is missing or incorrectly entered. This resilience ensures that your platform remains reliable during high-pressure clinical situations. As a result, your startup builds a reputation for mission-critical dependability.
4. Aligning system logic with clinical timelines
Medical decisions operate on specific, high-stakes timelines that software must respect. For example, acute care requires millisecond data refreshes, while chronic care focuses on long-term trends. In addition, your notification logic should prioritize life-critical alerts over routine administrative pings.
If your system ignores these clinical rhythms, it will quickly alienate your providers. Therefore, aligning your backend logic with the reality of the bedside is essential. This alignment creates a seamless harmony between the technology and the life-saving work of your team.
A map is the blueprint for your competitive advantage. Therefore, taking the time to map your care delivery ensures your EHR is built on a foundation of operational truth.
Architecture Decisions That Define Your EHR
Technical choices made during the early stages will dictate your startup’s ability to pivot. Therefore, these high-level architectural decisions are not just IT concerns but core business strategies.
A rigid foundation will eventually stifle innovation and increase your operational costs. Consequently, selecting the right framework is essential for building a resilient, enterprise-grade healthcare platform.
1. Monolith vs microservices in healthcare
Traditional monolithic systems bundle all functions into a single, massive codebase. However, this approach often leads to “deployment hell,” where one small update breaks the entire EHR.
In contrast, a microservices architecture breaks the system into smaller, independent units.
For instance, your billing service can be updated without touching your clinical notes module. In addition, this modularity allows your engineering team to scale specific features based on real-time demand. Thus, microservices provide the agility required for a fast-growing healthcare enterprise.
| Factor | Monolithic Architecture | Microservices Architecture |
| System Structure | Single, tightly integrated codebase | Independent, modular services |
| Deployment | Full system redeploy required for updates | Services can be deployed independently |
| Risk of Failure | One bug can impact the entire system | Failures are isolated to specific services |
| Scalability | Scales as one unit, often inefficient | Scales specific services based on demand |
| Development Speed | Slows down as the system grows | Faster parallel development across teams |
| Flexibility | Hard to modify individual components | Easy to update or replace services |
| Integration Capability | Limited and complex integrations | Designed for seamless integrations |
| Maintenance | Becomes harder over time | Easier to manage and evolve |
| Best Fit | Small, early-stage systems | Growing, complex healthcare platforms |
2. API-first vs tightly coupled systems
A tightly coupled system integrates all components so closely that they cannot function alone. This often results in a “closed loop” that prevents third-party integrations. On the other hand, an API-first strategy treats every internal function as a connectable service.
For example, you can easily plug in a new AI-driven radiology tool via a secure endpoint. Furthermore, this openness makes your platform more attractive to health system partners. Therefore, prioritizing APIs from the start ensures your EHR remains a central hub in the digital health ecosystem.
| Factor | Tightly Coupled Systems | API-First Architecture |
| System Design | Components depend heavily on each other | Each function is exposed as an independent service |
| Integration | Difficult to integrate third-party tools | Easy plug-and-play integrations |
| Flexibility | Changes impact multiple components | Changes remain isolated and controlled |
| Scalability | Hard to scale individual features | Scale services independently |
| Innovation Speed | Slower due to dependencies | Faster adoption of new technologies |
| Ecosystem Readiness | Closed system, limited extensibility | Open ecosystem, partner-friendly |
| Vendor Lock-In | High risk of lock-in | Reduced dependency on single systems |
| Use Case Example | Hard to add new clinical tools | Easily integrate AI, wearables, labs |
| Long-Term Viability | Becomes rigid over time | Adapts with evolving healthcare needs |
3. Data architecture for patient records
Patient data must be stored in a way that balances extreme security with high availability. For example, using a “Document-Store” model can offer more flexibility for varied clinical notes. However, a relational database might be better for tracking strict medication dosages and history.
In addition, your architecture must support “Data at Rest” and “Data in Transit” encryption to meet HIPAA standards. This dual approach protects your most valuable asset while ensuring clinicians have instant access. As a result, a robust data layer becomes the single source of truth for your entire organization.
4. Designing for interoperability from day one
Interoperability is no longer an optional feature; it is a regulatory requirement in 2026. Therefore, your system must support HL7 FHIR standards to exchange data with hospitals and labs. If your EHR cannot “speak” the same language as the rest of the industry, it will quickly become obsolete.
Moreover, building for interoperability allows you to aggregate longitudinal patient records from multiple sources. This comprehensive view leads to better diagnostic accuracy and improved patient outcomes. Consequently, being “interop-ready” is a massive competitive advantage when pitching to large enterprise clients.
Integration Strategy Most Startups Get Wrong
Connectivity is often treated as a final checklist item rather than a core feature. Therefore, many founders underestimate the technical friction of linking to established medical networks.
This oversight usually leads to significant data delays and frustrated clinical users. Consequently, a proactive integration strategy is what separates a functional tool from an enterprise-grade platform.
1. Why integrations fail post-launch
Most failures occur because developers treat integrations as “set and forget” tasks. However, external APIs frequently change their data schemas without much warning. If your system cannot handle these sudden shifts, your entire data flow will break instantly.
In addition, many startups fail to account for the “latency” of legacy hospital servers. This results in slow loading times that disrupt the clinician’s workflow. Thus, failing to build a resilient monitoring layer is a common and expensive mistake.
2. Handling HL7, FHIR, and legacy systems
Modern healthcare requires a “bilingual” approach to data exchange. While FHIR is the modern standard, many large hospitals still rely on older HL7 v2 messages. Therefore, your custom EHR must be able to translate between these different languages seamlessly.
For instance, using a “middleware” engine can map old data fields into your new architecture. Moreover, ignoring legacy systems will lock you out of the most lucrative enterprise markets. As a result, supporting both old and new standards is a strategic necessity for growth.
3. Integrating labs, pharmacies, and wearables
Connecting to third-party providers involves more than just a simple data link. For example, a lab integration must handle complex “LOINC” codes for accurate test results. In addition, pharmacy links require real-time “Surescripts” certification to ensure legal compliance.
Wearable data adds another layer of complexity due to the massive volume of heart rate or sleep metrics. Furthermore, your system must filter this “noise” to show only what is clinically relevant. Therefore, deep integration requires a sophisticated understanding of specialized medical data sets.
4. Building a scalable integration layer
A scalable layer acts as a universal adapter for your entire EHR. Instead of building a new connection for every partner, you should use a standardized “Gateway” approach. For instance, this allows you to swap one lab provider for another without rewriting your core code.
In addition, a central hub makes it easier to monitor security and data privacy across all connections. This modularity reduces your long-term maintenance costs significantly. Consequently, a well-built integration layer becomes a powerful engine for rapid market expansion.
Mastering the “handshake” between systems is the only way to ensure your platform remains useful. Therefore, investing in a robust integration layer protects your clinical reputation and your investors’ capital.
Designing for Scale From Day One
Scalability is a fundamental requirement for any venture-backed healthcare startup. Therefore, your digital foundation must handle a thousand patients as easily as ten. If your system slows down under pressure, your operational costs will skyrocket.
Consequently, building for future volume today is the most efficient use of your current capital.
1. Supporting rapid patient growth
Rapid growth often places immense strain on traditional database structures. However, a custom EHR uses horizontal scaling to distribute this load across multiple servers. For instance, your patient portal should remain responsive even during a viral marketing surge.
In addition, automated load balancing ensures that no single point of failure disrupts your care delivery. Thus, an elastic architecture allows you to onboard thousands of new users without any performance lag.
2. Multi-location and multi-provider scaling
Expanding to new regions requires a system that understands complex organizational hierarchies. For example, a clinic in New York may have different regulatory workflows than one in California. Therefore, your EHR must support “Multi-tenancy” logic to keep data separate yet accessible.
In addition, role-based access control allows you to add new providers with specific permissions instantly. This modularity ensures that your administrative overhead does not grow faster than your revenue.
3. Handling increasing data complexity
As you scale, the sheer variety of data types will become a significant technical challenge. For instance, you may need to store high-resolution medical images alongside simple text notes. However, a custom data lake can organize this information for rapid retrieval and analysis.
Moreover, your system must handle the increasing frequency of real-time telemetry from patient wearables. This capability prevents your data storage from becoming a cluttered and expensive graveyard of information.
4. Avoiding costly re-architecture
Many startups are forced to rebuild their entire platform after reaching a certain size. This “Total Rewrite” usually happens because the original software was too rigid. However, using a microservices approach from the start prevents this catastrophic scenario. By isolating different functions, you can upgrade specific parts of the system without starting over.
Furthermore, this foresight saves millions in future development costs and avoids weeks of operational downtime. Therefore, smart architecture is the ultimate insurance policy for your long-term growth.
Building for the future is about preparing for the inevitable. Therefore, a scalable EHR is the strongest signal you can send to your investors and partners.
Compliance and Security as System Design Layers
Security in healthcare is not a feature you add later. Instead, it must be the very foundation of your entire software architecture. Therefore, founders who treat compliance as an afterthought often face massive legal and financial risks.
Consequently, building security into every layer of your system is a non-negotiable requirement for enterprise trust.
1. Designing HIPAA-ready architectures early
HIPAA compliance requires more than just a simple password on a database. For instance, your system must track every single time a patient record is viewed. In addition, you must ensure that data is encrypted both at rest and during transit.
However, a custom architecture allows you to automate these administrative safeguards from the start. This proactive approach prevents costly security breaches before they can even happen. Thus, a HIPAA-ready design is the first line of defense for your startup’s reputation.
2. Data security models for healthcare startups
Modern data security relies on a “Zero Trust” model for every user. This means that no person or device is trusted by default, even inside your network. For example, a doctor should only see the specific records for their current patients.
Furthermore, multi-factor authentication should be a mandatory requirement for all system access points. This granular control protects your most sensitive assets from both internal and external threats. Therefore, a robust security model is a fundamental part of your business value.
3. Auditability and access control systems
Audit trails provide a transparent history of every action taken within your EHR. For instance, if a record is changed, the system must log who made the edit and when. In addition, role-based access control (RBAC) ensures that staff members only see what they need.
A nurse might see clinical notes, while a billing clerk only sees financial data. This separation of duties reduces the risk of accidental or intentional data exposure. Consequently, high auditability is a key requirement for passing enterprise-level security reviews.
4. Avoiding compliance bottlenecks at scale
As you grow, manual compliance checks will become a major operational bottleneck. However, a custom system can automate regular security audits and reporting tasks. For example, you can schedule automatic permission reviews for every employee in your organization. In addition, cloud-based security tools can detect unusual data patterns in real-time.
This automation allows your team to focus on growth rather than constant paperwork. As a result, your compliance strategy remains efficient even as your patient volume doubles.
Compliance is the price of entry into the high-stakes world of healthcare. Therefore, building these layers early ensures your platform is ready for the most demanding enterprise clients.
How We Build a Customized Startup-Ready EHR System
At Intellivon, we recognize that enterprise-grade AI and healthcare software must be built for the long term. Therefore, our methodology focuses on clinical precision and high-scale performance from the very first day.
We engineer a strategic asset for your business. Consequently, our seven-step process ensures your platform is ready for the most demanding global markets.
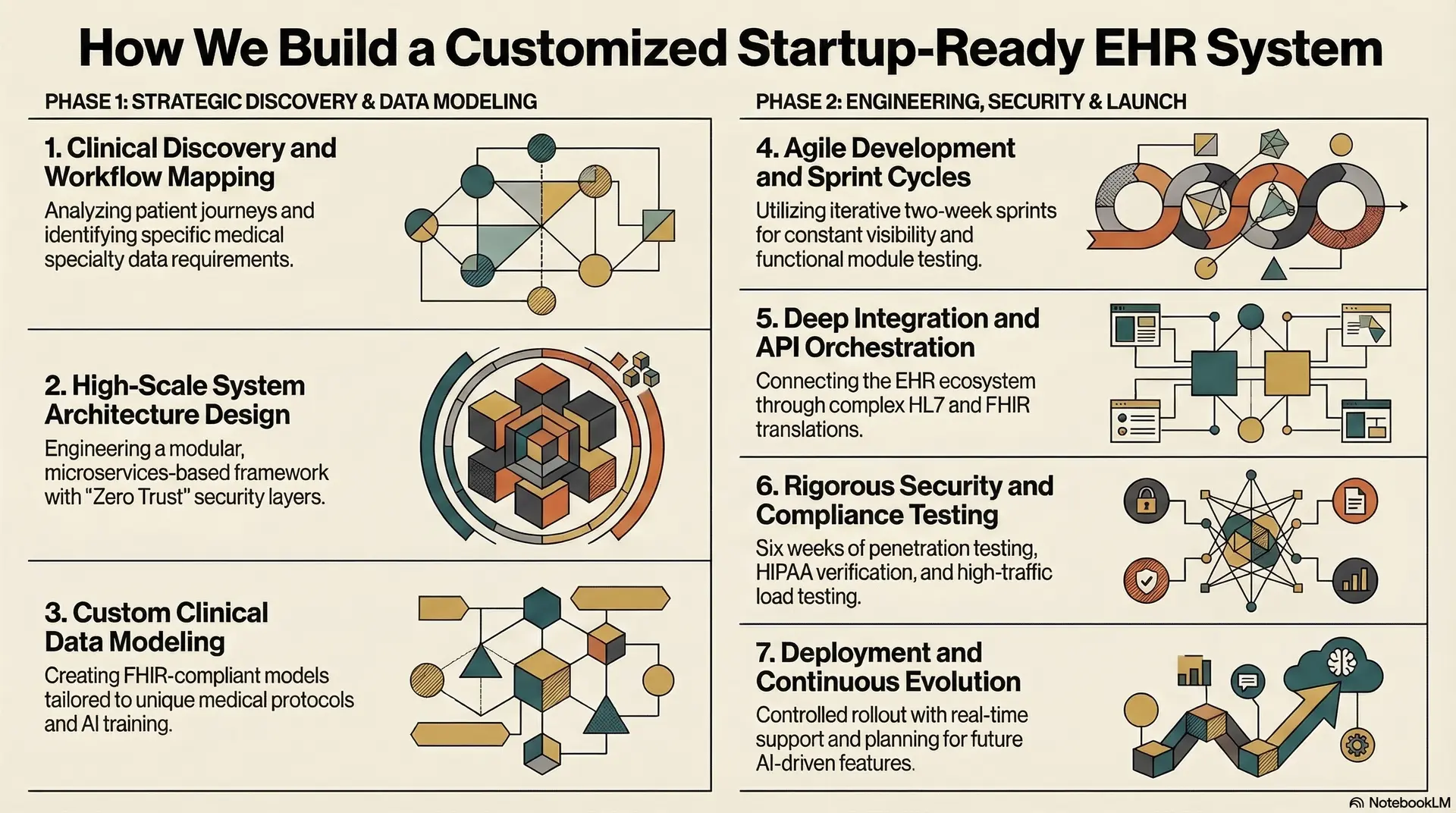
1. Clinical Discovery and Workflow Mapping
We begin by deeply analyzing your specific patient journeys and provider requirements. For instance, we map every single touchpoint from the first intake form to final billing. In addition, we identify the exact data fields your medical specialty requires for daily operations.
This phase typically lasts three to five weeks of close collaboration. Thus, a solid discovery phase prevents expensive mid-project shifts.
2. High-Scale System Architecture Design
Our engineers design a modular, microservices-based framework to ensure your platform never slows down. However, we also prioritize data security by building “Zero Trust” layers into the backend.
For example, we decide how your database will handle millions of real-time health records. Furthermore, we design the API layer to support future AI integrations seamlessly. As a result, your architecture remains flexible as your startup grows.
3. Custom Clinical Data Modeling
Standard data “buckets” are often too rigid for disruptive healthcare startups. Therefore, we create custom FHIR-compliant data models that fit your unique medical protocols.
For instance, a cardiology platform needs different data structures than a mental health app. Moreover, clean data modeling is essential for training future proprietary AI models. Thus, we ensure your data is a structured, high-value business asset.
4. Agile Development and Sprint Cycles
The core development phase utilizes two-week sprints to provide constant visibility into our progress. Therefore, you can see functional modules long before the final launch date. For example, your team might test the patient portal while we build the pharmacy link.
In addition, this iterative approach allows us to pivot quickly based on early feedback. Consequently, your product evolves in a controlled, high-quality environment.
5. Deep Integration and API Orchestration
We connect your EHR to the broader healthcare ecosystem, including labs, pharmacies, and wearables. However, we do not just link systems; we orchestrate the flow of information. For instance, a critical lab result can automatically trigger a clinician’s high-priority task.
Furthermore, we handle the complex HL7 and FHIR translations required for hospital interoperability. Therefore, your system becomes a truly connected hub for modern care.
6. Rigorous Security and Compliance Testing
Security is a non-negotiable layer of our development process at Intellivon. During this six-week phase, we conduct deep penetration tests to find any potential vulnerabilities.
In addition, we verify that every data transaction meets 100% of HIPAA and SOC2 standards. We also perform “Load Testing” to ensure your system handles peak patient traffic. As a result, you launch with total confidence in your platform’s integrity.
7. Deployment and Continuous Evolution
The final step is a controlled rollout followed by ongoing performance monitoring. Therefore, we stay with you to ensure a smooth transition for your clinical staff. For example, we provide real-time support during the first weeks of live patient care.
Moreover, we help you plan the next phase of AI-driven features and updates. Thus, Intellivon acts as your long-term strategic partner in healthcare innovation.
Choosing the right partner is the most important decision for your technical roadmap. Therefore, our structured approach ensures your EHR is not just functional, but market-dominant.
Conclusion
Customizing an EHR is not just a product decision. It shapes how your startup delivers care, scales operations, and controls clinical data. Off-the-shelf tools may work early, but they often limit growth.
In contrast, a well-designed custom EHR aligns with your workflows, integrations, and long-term goals. Therefore, startups that invest early in the right architecture build stronger, more scalable healthcare platforms.
Build a Custom EHR Platform With Intellivon
At Intellivon, EHR platforms are engineered as an enterprise clinical infrastructure, not as systems layered onto fragmented healthcare environments. The goal is to create a unified platform that manages patient data, automates workflows, and enables seamless care delivery across providers, systems, and settings.
Each solution is designed to support the full patient lifecycle. This includes smart scheduling, clinical documentation, decision support, care coordination, and automated billing. As a result, healthcare organizations gain real-time visibility, reduce operational inefficiencies, and deliver faster, more accurate care.
Our approach focuses on AI-first, API-driven architectures combined with interoperability standards like HL7 and FHIR. This ensures seamless integration with EHR systems, labs, pharmacies, billing platforms, and existing healthcare infrastructure without disrupting ongoing operations.
Why Partner With Intellivon?
- Clinical Infrastructure, Not Just Software: Built to support long-term clinical operations across complex healthcare ecosystems.
- AI-Driven Workflow Automation: Automates documentation, scheduling, billing, and care coordination to reduce manual effort.
- Integration-Ready Architecture: Connects seamlessly with healthcare systems, devices, and third-party platforms.
- Compliance-First Engineering: Designed with HIPAA-compliant security, encryption, and governance frameworks.
- Scalable for Enterprise Healthcare Systems: Supports multi-location providers and high patient volumes without performance bottlenecks.
Custom EHR platforms are no longer optional for organizations aiming to scale care delivery and improve clinical outcomes. Therefore, building the right system early directly impacts efficiency, compliance, and long-term scalability.
Connect with Intellivon’s experts to build an EHR platform tailored to your workflows, integrations, and growth roadmap.
FAQs
Q1. What is EHR customization for startups
A1. EHR customization means building or modifying an EHR system to match your startup’s specific care workflows, data needs, and integrations. Instead of adapting your operations to rigid software, the system is designed around how your care model actually works.
Q2. How long does custom EHR take to build
A2. Custom EHR development typically takes 4 to 9 months. The timeline depends on workflow complexity, integrations, compliance requirements, and the level of automation needed. MVP versions can launch faster, while full-scale systems require more time.
Q3. What features should a startup EHR include
A3. A startup EHR should include patient records, scheduling, clinical documentation, billing, and integrations with labs or pharmacies. In addition, it should support workflows, real-time data access, and scalability to handle growth.
Q4. How much does it cost to build an EHR
A4. The cost to build a custom EHR usually ranges from $40,000 to $150,000. It depends on features, integrations, compliance needs, and system complexity. More advanced platforms with AI and automation increase overall costs.
Q5. Can custom EHR systems scale with growth
A5. Yes, custom EHR systems are designed to scale. With the right architecture, they can support more patients, providers, and locations without performance issues. This makes them suitable for startups planning rapid growth.