Healthcare organizations nowadays have separate systems. Billing is in one platform, clinical records are in another, and scheduling is in yet another. This results in staff spending hours trying to match up data that should already be linked. At the same time, decisions are delayed because the right information isn’t available in the right place when needed. This is a structural problem more than it is a technical one, and it’s costing healthcare organizations money and quality of care.
All-in-one EHR platforms address this issue at the core. Rather than piecing together different solutions, they combine clinical workflows, administrative tasks, revenue cycle management, and patient engagement into one clear system. The efficiency gains are immediate. However, the bigger benefit comes from what combined data allows, which includes faster diagnoses, stronger compliance, and operational insight that leadership can truly act on.
Intellivon builds these platforms for healthcare enterprises, end-to-end. In this blog, we draw from that experience to show you exactly how we approach each layer, from architecture and core features to compliance frameworks, technology stack, and cost structure, built from the ground up, the way enterprise-grade systems demand.
Why Healthcare Is Moving to Unified EHR Platforms
Modern healthcare organizations are quickly outgrowing the era of disconnected software tools. The shift toward a unified EHR platform is now a strategic necessity for maintaining a competitive edge in 2026.
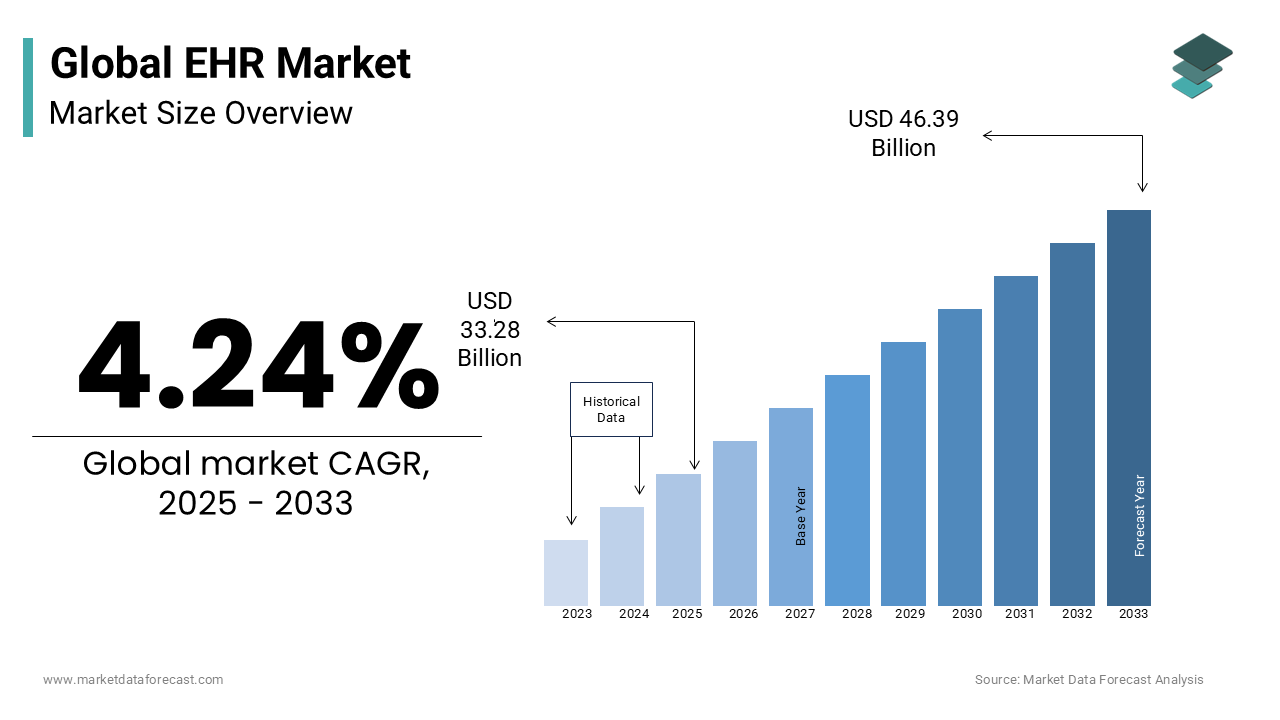
Healthcare is moving toward unified EHR platforms to eliminate data silos, improve interoperability, and enable real-time care delivery. As efficiency and value-based care demands grow, legacy systems struggle to keep up.
Unified platforms solve this fragmentation, helping providers improve outcomes while reducing operational costs.
1. Fragmented systems are slowing clinical and financial workflows
Legacy environments often rely on a patchwork of specialized software that rarely communicates effectively. When clinical data remains trapped in one silo and billing information stays in another, the entire organization suffers from massive friction. Physicians lose valuable hours toggling between screens, while administrative teams struggle with manual data entry.
This fragmentation does more than just frustrate staff; it creates significant financial leakage. Inaccurate coding and delayed documentation frequently lead to denied claims and stalled revenue cycles. By integrating these disparate functions, enterprises can finally synchronize their medical delivery with their fiscal goals.
2. Rising compliance and data accuracy demands
Regulatory bodies are enforcing stricter standards for data integrity and patient privacy every year. Maintaining a dozen different security protocols across multiple vendors is no longer a sustainable strategy for large-scale providers. A single vulnerability in one minor tool can compromise the entire network’s integrity.
A unified platform centralizes governance, making it much easier to implement robust encryption and access controls. This architecture ensures that every piece of patient data is captured accurately at the point of care. Consequently, the risk of human error decreases while the speed of mandatory reporting increases significantly.
3. Why unified platforms are becoming the default in 2026
In 2026, the baseline for healthcare technology is no longer just digital storage but active intelligence. Unified systems allow AI-driven analytics to scan the entire dataset to identify population health trends and operational gaps.
For example, Epic Systems remains a dominant force for large hospital networks because its “One Virtual Patient” model ensures that every provider sees the same data in real-time. This level of insight is impossible to achieve when data is scattered across incompatible databases.
Other innovative players like athenahealth and CureMD are capturing the mid-to-large ambulatory market by offering “all-in-one” cloud suites. These platforms remove the need for third-party billing or patient engagement add-ons by building those features into the core architecture
Therefore, forward-thinking investors are prioritizing platforms that offer a holistic view of the patient journey. These systems support value-based care models, which reward providers for quality outcomes rather than just the volume of services. The move to a single interface is now the standard for those seeking long-term growth.
Investing in a unified architecture is the most direct way to solve the persistent “data silo” problem. This transition empowers leaders to focus on innovation instead of troubleshooting basic connectivity issues.
What Defines a True All-in-One EHR Platform?
A true all-in-one EHR platform is a single, unified software ecosystem that consolidates clinical documentation, practice management, and revenue cycle tools into one database.
Unlike fragmented systems that rely on messy third-party integrations, this architecture ensures data flows instantly across the entire enterprise. It provides a “single source of truth” for patient records, billing, and scheduling, significantly reducing administrative friction while improving clinical accuracy.
Why Most Integrated Systems Are Still Fragmented
Many healthcare leaders believe they own a unified solution, yet their teams still struggle with data gaps and manual workarounds. In reality, most “integrated” platforms are just separate software products stitched together with unstable digital bridges.
1. The Illusion of the Single Interface
Many vendors grow through acquisitions, buying smaller companies to add features like billing or telehealth to their core EHR. Instead of rebuilding these tools from scratch, they simply link them using APIs or plug-ins.
While the user might see a single login screen, the underlying databases are still completely different. This setup often leads to data lag, where information entered in the clinical portal takes minutes or hours to appear in the billing section.
2. The High Cost of Middleware
When systems aren’t truly unified, they require middleware (extra layers of software) to translate data between modules. This creates a fragile ecosystem where an update to one part of the system can break the connection to another.
For an enterprise, this means constant IT maintenance, higher subscription fees for bridge services, and a higher risk of data corruption during the transfer process.
3. Fragmented Workflows and App Fatigue
Because these sub-systems were built by different teams, the user experience is rarely consistent. A doctor might find that the patient portal looks and feels entirely different from the charting module.
This lack of uniformity causes app fatigue and increases the learning curve for new staff. True unification ensures that every button, menu, and report follows the same logic, making the software feel like a natural extension of the workflow.
True integration is often a marketing term rather than a technical reality. Recognizing the difference between a “stitched-together” system and a natively unified platform is essential for long-term operational success.
Signs Your Current EHR Stack Is Failing
Recognizing the technical decay in your current infrastructure is the first step toward strategic recovery. When an EHR stack begins to fail, the symptoms manifest as operational friction that directly erodes your bottom line.
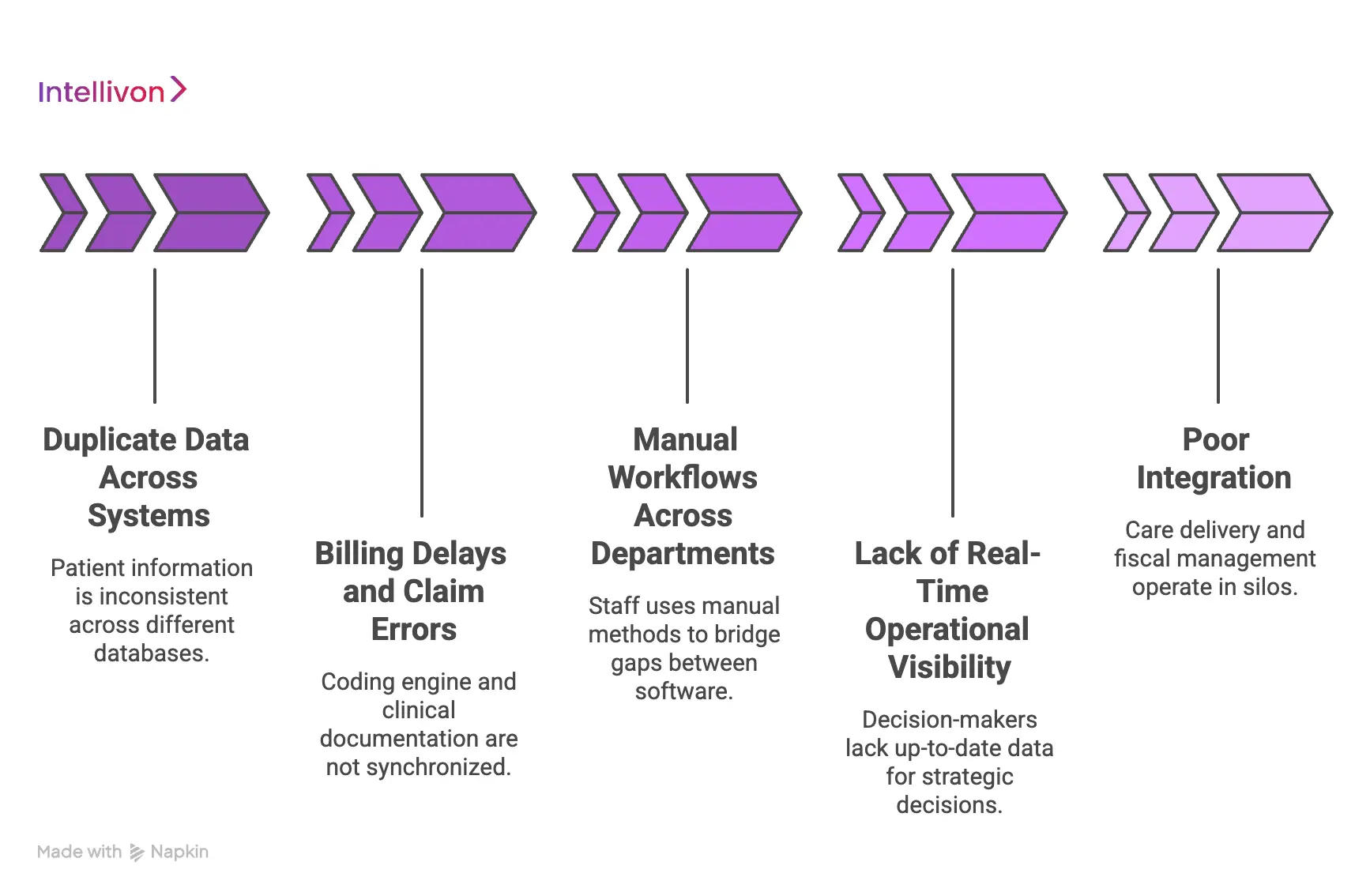
1. Duplicate Data Across Systems
Maintaining multiple databases inevitably leads to record duplication and synchronization errors. When a patient’s address is updated in the clinical portal but remains stagnant in the billing system, the result is a “split identity” that triggers administrative chaos.
These discrepancies force staff to spend hours manually verifying basic information across various screens. Consequently, clinical safety is compromised as doctors may miss critical historical data hidden in an unlinked module.
2. Billing Delays and Claim Errors
A failing EHR stack creates a massive disconnect between the point of care and the revenue cycle. If the coding engine doesn’t talk to the clinical documentation in real-time, the probability of “clean claims” drops significantly.
This lack of synergy leads to a high volume of denials and a bloated Days Sales Outstanding (DSO) metric. Finance teams are then left chasing revenue that should have been captured automatically at the moment of the encounter.
3. Manual Workflows Across Departments
If your staff still relies on spreadsheets, sticky notes, or manual data exports to bridge gaps between software, your system has failed. These “manual bridges” are the most expensive way to run a healthcare enterprise because they rely on human intervention for tasks that should be automated.
This labor-intensive approach not only slows down patient throughput but also increases the likelihood of burnout among high-value clinical staff.
4. Lack of Real-Time Operational Visibility
Decision-makers cannot steer an organization using data that is two weeks old. In a fragmented stack, generating a comprehensive report requires pulling data from several different vendors and manually consolidating it.
This delay prevents leadership from reacting to emerging trends, such as sudden shifts in patient volume or declining reimbursement rates. Without a live dashboard, you are essentially flying the enterprise blind in a high-stakes market.
5. Poor Integration Between Clinical and Financial Systems
The most dangerous gap in any healthcare organization is the wall between care delivery and fiscal management. When these two worlds operate in silos, the business cannot accurately calculate the true cost of care for specific patient populations.
This misalignment makes it nearly impossible to succeed in value-based care contracts where financial success is tied directly to clinical performance. A unified platform is the only way to ensure these two departments speak the same language.
Identifying these failure points is essential for justifying the shift toward a more resilient, unified architecture. Addressing these gaps today prevents a total operational breakdown tomorrow.
Core Modules in a Unified EHR Platform
A truly unified platform functions like a central nervous system for a healthcare enterprise. By integrating these core modules into a single database, organizations eliminate the “data silos” that typically throttle growth and clinical efficiency.
1. Clinical Documentation and Charting
The clinical module is where healthcare providers spend the majority of their day. In a unified system, charting is intuitive and fast, pulling in historical data, lab results, and previous notes automatically.
This eliminates the need for redundant data entry and allows doctors to focus on the patient rather than the screen. Because the documentation is linked to the entire system, a note signed by a physician instantly updates the billing and pharmacy modules.
2. Appointment Scheduling and Intake
Efficiency begins the moment a patient books an appointment. An integrated scheduling module syncs with the patient portal and the clinical calendar in real-time. When a patient fills out intake forms digitally, that data flows directly into their medical record without manual transcription.
This automation reduces wait times and ensures that the clinical team has all necessary information before the patient even walks through the door.
3. ePrescription and Pharmacy Systems
Modern prescribing must be both fast and safe. A unified ePrescription module checks for drug-to-drug interactions and insurance formulary compliance instantly. This ensures that the patient receives the most effective medication covered by their plan.
By sending prescriptions directly to the pharmacy from the patient’s chart, the system reduces errors and improves medication adherence, which is a key metric for value-based care.
4. Billing and Revenue Cycle Management
A native billing engine is the heartbeat of a profitable enterprise. Instead of exporting data to a third-party biller, a unified system captures charges at the point of care. This “charge capture” happens automatically based on the clinical documentation.
Consequently, the time between a patient visit and a submitted claim is reduced from days to minutes, significantly improving the organization’s cash flow and reducing administrative overhead.
5. Insurance and Claims Processing
Managing insurance complexity is a major hurdle for large-scale providers. An integrated claims module performs real-time eligibility checks before the appointment even begins.
It automatically scrubs claims for errors before submission, which leads to a much higher “first-pass” acceptance rate. This proactive approach prevents the costly cycle of denials and resubmissions that plagues fragmented systems.
6. Analytics and Decision Support Systems
Data is only valuable if it is actionable. A unified platform provides a live dashboard that tracks both clinical outcomes and financial performance simultaneously.
Leadership can see exactly which departments are most efficient and where patient care gaps exist. These insights allow for data-driven decisions that improve the overall health of both the patients and the business.
Consolidating these modules into a single interface is the only way to achieve true operational excellence. This structural alignment ensures that every department is working from the same information at all times.
How All-in-One EHR Platforms Work in Practice
Understanding the operational mechanics of a unified system reveals how it transforms a chaotic clinical environment into a synchronized enterprise. This step-by-step progression shows how data flows natively from the first patient touchpoint to the final financial reconciliation.
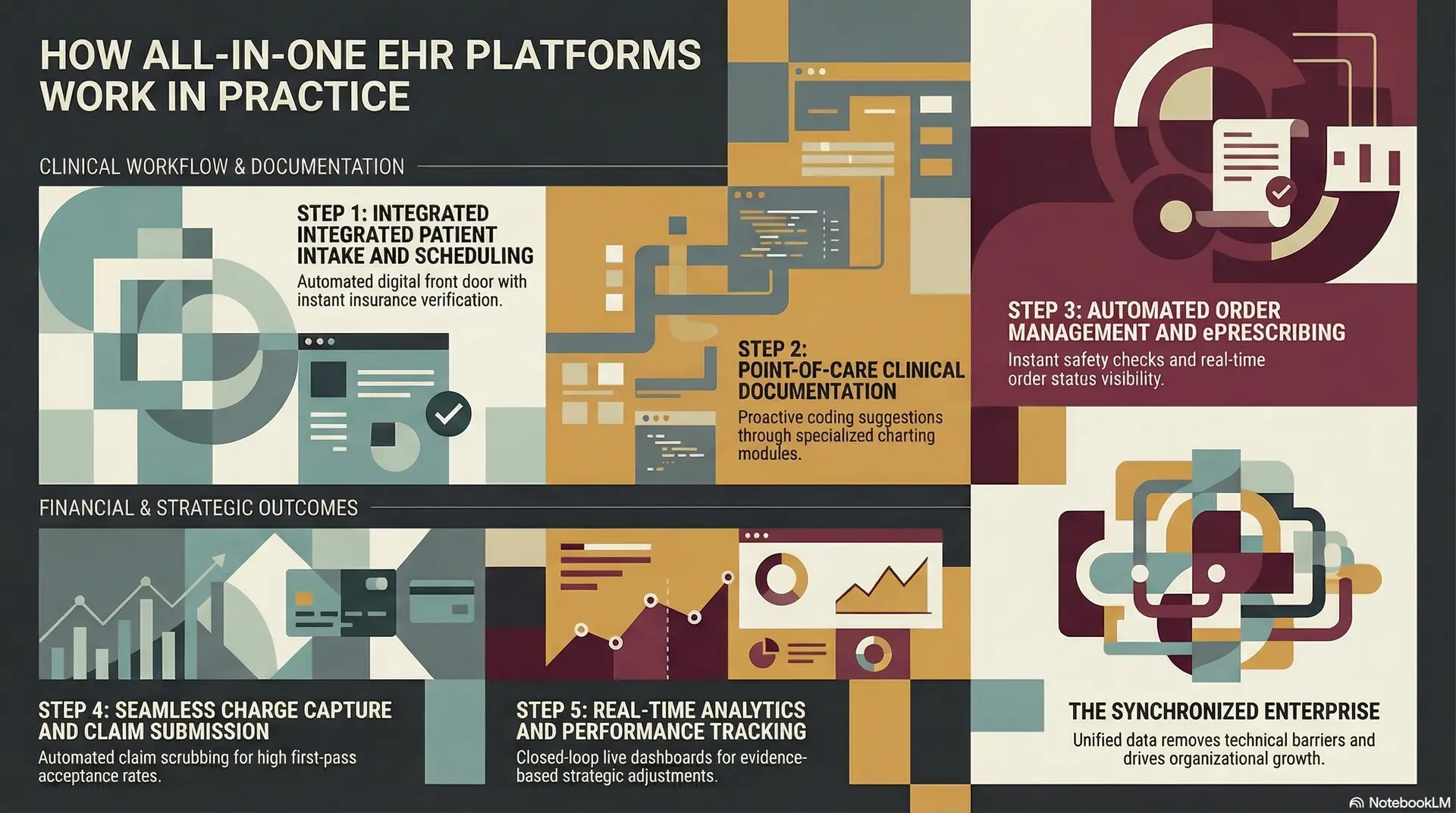
Step 1: Integrated Patient Intake and Scheduling
The process begins with an automated digital front door. When a patient books an appointment through a portal, the system immediately verifies insurance eligibility against live payer databases.
This initial step ensures that the clinical team isn’t flying blind regarding coverage or prior authorizations. Because the intake forms are native to the EHR, the data the patient enters populates their medical record instantly without any manual transcription from the front desk staff.
Step 2: Point-of-Care Clinical Documentation
During the encounter, the physician works within a specialized charting module that is aware of the patient’s entire history. As the doctor documents findings, the system uses natural language processing to suggest relevant ICD-10 codes in real-time.
This “proactive coding” ensures that clinical intent is captured accurately at the moment of care. There is no need to “sync” this note with a separate billing system because they both sit on the same underlying data table.
Step 3: Automated Order Management and ePrescribing
When a provider orders a lab test or sends a prescription, the unified platform performs an instant safety check. It cross-references the order with the patient’s current medications, known allergies, and insurance formulary.
This automation reduces the “callback” loop between pharmacies and clinics, saving hours of administrative time every week. The order status is visible to the entire care team immediately, providing a transparent view of the patient’s treatment plan.
Step 4: Seamless Charge Capture and Claim Submission
The most significant shift happens when the clinical note is signed. In a fragmented system, a biller would have to pull this data into a separate software.
The system scrubs the claim against thousands of payer-specific rules before it ever leaves the building. This high first-pass acceptance rate means the organization gets paid faster and with significantly less manual intervention from the finance department.
Step 5: Real-Time Analytics and Performance Tracking
Finally, every data point collected, from the wait time in the lobby to the final payment received, is fed into a live dashboard. Leadership can monitor key performance indicators (KPIs) like clinician productivity and revenue leakage without waiting for end-of-month reports.
This closed-loop system allows for rapid strategic adjustments based on hard evidence rather than anecdotal feedback.
This integrated lifecycle ensures that every department is an active participant in the enterprise’s success. By removing technical barriers, the platform allows the staff to focus on high-value tasks that drive growth and patient satisfaction.
Monolithic vs Modular vs Unified EHR Systems
Choosing the right EHR architecture is a critical decision for any healthcare organization. It directly impacts scalability, performance, integration flexibility, and long-term costs.
Traditionally, enterprises relied on monolithic systems or stitched together modular tools. However, both approaches create limitations as organizations scale.
Today, unified EHR platforms are emerging as the preferred model. They combine the control of a single system with the flexibility modern healthcare operations demand.
Let’s break down how these three approaches compare.
Comparison Table
| Factor | Monolithic EHR Systems | Modular EHR Systems | Unified EHR Platforms |
| Architecture | Single, tightly coupled system | Multiple independent systems connected via integrations | Single platform with unified data architecture |
| Data Management | Centralized but rigid | Distributed across systems | Single source of truth across all modules |
| Scalability | Difficult to scale specific features | Scalable but depends on integrations | Scales efficiently across modules and workloads |
| Flexibility | Low flexibility | High flexibility but fragmented | High flexibility within a unified structure |
| Integration Needs | Minimal external integrations | Heavy reliance on APIs and third-party tools | Limited external dependencies |
| Performance | Slows down as the system grows | Depends on integration efficiency | Optimized with real-time data flow |
| Maintenance | Complex and risky updates | Ongoing integration maintenance required | Easier to manage with centralized control |
| Cost Over Time | High due to upgrades and rigidity | High due to integration and licensing costs | Lower due to reduced dependencies |
| User Experience | Often outdated and rigid | Inconsistent across systems | Seamless and consistent across workflows |
| Best Fit | Small to mid-sized setups with stable needs | Organizations needing flexibility across tools | Enterprises needing scale, speed, and control |
Monolithic systems offer control but struggle to adapt. Modular systems provide flexibility but introduce complexity through integrations.
In contrast, unified EHR platforms strike the right balance. They centralize data, streamline workflows, and reduce operational overhead without sacrificing scalability.
For enterprises building long-term healthcare infrastructure, unified platforms are becoming the most practical and future-ready choice.
Unified Platforms as the Scalable Approach
A unified platform offers the best of both worlds by providing a single database with a modular user interface. Every department uses a specialized toolset, but all the data lives in one central, cloud-native repository. This structure ensures that a change in one area is reflected across the entire enterprise in milliseconds.
This architecture is built for the scale of 2026, supporting massive data sets without sacrificing system speed. It allows leadership to deploy new AI features or telehealth modules without worrying about compatibility issues. The result is a fluid, high-performance environment that grows alongside your patient population.
What Enterprises Should Choose in 2026
For any organization looking to remain competitive, the choice must be a unified, cloud-first architecture. Investing in legacy monoliths or fragmented modular stacks creates long-term liabilities that hinder digital transformation. A unified system provides the data liquidity required to succeed in high-stakes, value-based care environments.
Decision-makers should prioritize vendors that prove their “all-in-one” claim through a shared data schema rather than just a shared login. This ensures your technology remains an asset that drives growth instead of a barrier that creates frustration.
Choosing the right system today defines your operational limits for the next ten years. A unified approach is the only way to ensure your enterprise stays resilient in an unpredictable market.
Business Impact of Unified EHR Platforms
Unified EHR platforms drive ROI by collapsing the cost of data reconciliation and accelerating Revenue Cycle Management (RCM) velocity.
Enterprises typically see a 15–20% reduction in administrative overhead within the first year of full consolidation.
1. Reduction in operational costs
Maintaining multiple software contracts and the IT staff required to bridge them is a massive, hidden drain on capital. A unified platform eliminates the need for expensive middleware and third-party integration consultants.
Therefore, the total cost of ownership drops as the organization moves to a single, predictable subscription model.
2. Faster billing and claim cycles
Revenue leakage often results from “data lag” between the clinical encounter and the back-office billing team. In a unified system, the bill is ready the moment the physician signs the chart.
This immediate synchronization removes the manual “chase” for missing documentation that typically stalls the revenue cycle.
3. Improved provider productivity
Physician burnout is a leading cause of operational inefficiency and high staff turnover. Fragmented systems force doctors to act as data entry clerks, toggling between various windows.
A unified interface restores the provider’s focus by providing all necessary tools within a single, logical workflow.
4. Better compliance and audit readiness
In a highly regulated market, fragmented data is a massive legal liability. When records are scattered, responding to a government audit can take weeks of manual labor. A unified platform provides a single, immutable audit trail for every action taken within the system.
5. Enhanced patient experience
Modern patients expect a digital experience that mirrors retail or banking. A unified platform offers a seamless journey, from online booking to transparent billing via a single portal. This level of professional consistency builds deep trust and long-term loyalty.
The business case for a unified EHR goes far beyond simple software replacement. It is a fundamental shift toward a more profitable, resilient, and patient-centered enterprise model.
Real Challenges Before Building an EHR Platform
Moving toward a unified architecture requires a clear-eyed assessment of the technical hurdles already present within your organization. Identifying these bottlenecks early is the only way to ensure the new platform delivers a true return on investment.
1. Legacy System Fragmentation
Many enterprises operate on a patchwork of software that was never designed to work together. This fragmentation means that your clinical, billing, and scheduling tools exist as isolated islands of data.
Consequently, your IT department spends more time managing “bridges” between these systems than they do on actual innovation. This technical debt slows down every department and prevents the organization from adopting modern, AI-driven tools.
2. Data Inconsistency Across Departments
When information is manually entered into multiple systems, errors are inevitable. A patient’s medication list might be updated in the clinical chart but remain outdated in the pharmacy or billing module.
These discrepancies create a split reality that compromises patient safety and leads to massive administrative headaches. Therefore, a primary challenge is consolidating these conflicting records into a single, reliable source of truth.
3. Compliance Complexity
The regulatory landscape for healthcare data is becoming increasingly strict and difficult to navigate. Managing HIPAA, SOC2, or GDPR compliance across five different vendors is a high-stakes liability.
A single security gap in one minor tool can put the entire enterprise at risk of a major data breach. This complexity makes it nearly impossible to maintain a consistent security posture across a fragmented software stack.
4. Lack of Interoperability
The inability to share data seamlessly with external labs, pharmacies, and other hospital networks is a major operational barrier. Many legacy systems use proprietary formats that do not talk to the rest of the healthcare ecosystem.
This lack of interoperability forces staff to rely on outdated methods like faxing or manual data entry to share patient records. Consequently, the speed of care delivery is throttled by the limitations of the software.
5. Scaling Limitations in Current Systems
Older EHR architectures often struggle to handle the high data volumes required by modern, large-scale enterprises. As your patient population grows, these systems become slower, leading to screen lag and frustrated providers.
Because they aren’t cloud-native, scaling often requires massive capital investments in local server hardware. This rigidity prevents the business from expanding quickly into new markets or adding specialized service lines.
Addressing these foundational challenges is the first step toward building a platform that actually works for your business. Recognizing these pain points allows you to design a solution that is resilient, compliant, and ready for growth.
Architecture Behind All-in-One EHR Platforms
Building a high-performance EHR requires a departure from legacy software engineering. The architecture must prioritize data liquidity and high availability while maintaining the rigorous security standards required for healthcare.
1. Single Database vs Distributed Systems
A unified platform relies on a single-database schema to ensure every module pulls from the same source of truth. In a distributed or fragmented system, data must be synchronized between different databases, which often leads to “data lag” and synchronization errors.
| Factor | Single Database Architecture | Distributed Systems |
| Data Structure | One unified database across all modules | Multiple databases across different systems |
| Source of Truth | Single source of truth for all workflows | Multiple versions of the same data |
| Data Consistency | Real-time consistency across teams | Prone to data lag and sync issues |
| Data Flow | Instant updates across all modules | Requires synchronization between systems |
| Error Risk | Minimal duplication and mismatch errors | Higher risk of inconsistencies and conflicts |
| Operational Visibility | Complete, real-time system visibility | Fragmented view across departments |
| System Complexity | Simpler data management | Complex data coordination and maintenance |
| Scalability Impact | Scales with structured architecture | Scaling increases sync complexity |
| Common Issue | Rare data conflicts | Frequent “split-identity” problems |
| Best Fit | Enterprises needing unified workflows | Legacy systems with disconnected tools |
2. API-First Architecture for Scalability
An API-first approach means that the core functions of the EHR are built as accessible services from the very beginning. This design allows the platform to connect easily with third-party tools, such as advanced diagnostic AI or specialized telehealth hardware.
Because the internal modules communicate through these same APIs, the system remains modular and easy to update without risking a total system failure. Therefore, the enterprise can scale its capabilities by “plugging in” new features as the market evolves.
3. Cloud-Native Infrastructure Design
True all-in-one platforms are built specifically for the cloud rather than being lifted and shifted from local servers. This cloud-native design allows for elastic scaling, meaning the system automatically adjusts its processing power based on the current user load.
Consequently, providers never experience screen lag during peak hours, and the organization only pays for the computing resources it actually uses. This architecture also provides built-in redundancy, ensuring that the system remains online even during localized hardware failures.
4. Role-Based Access and Security Layers
Security in a unified EHR is handled through sophisticated, multi-layered access controls that follow the principle of least privilege. A billing clerk, for example, can access financial records but is restricted from viewing sensitive clinical notes.
These permissions are managed centrally, making it simple to audit who accessed what data and when. In addition to encryption at rest and in transit, these role-based layers protect the enterprise from internal data leaks and external cyber threats.
5. HL7 and FHIR Interoperability Standards
To succeed in a modern healthcare landscape, a platform must “speak” the universal languages of medical data. Fast Healthcare Interoperability Resources (FHIR) and HL7 standards allow the EHR to exchange information seamlessly with external labs, pharmacies, and other hospital networks.
This connectivity ensures that the patient’s medical history follows them wherever they go, regardless of what software the other provider is using. Adhering to these global standards is no longer optional; it is a requirement for participating in value-based care models.
The technical integrity of the platform defines the operational limits of the business. Investing in a modern, standards-based architecture ensures that your technology remains a competitive advantage for years to come.
Step-by-Step Process to Build an All-In-One EHR Platform
Developing a unified EHR involves a six-stage lifecycle: scope definition, unified schema design, clinical module development, RCM integration, interoperability testing, and cloud scaling.
Partnering with a specialized firm like Intellivon accelerates this timeline by leveraging pre-built AI frameworks and compliant cloud architectures.
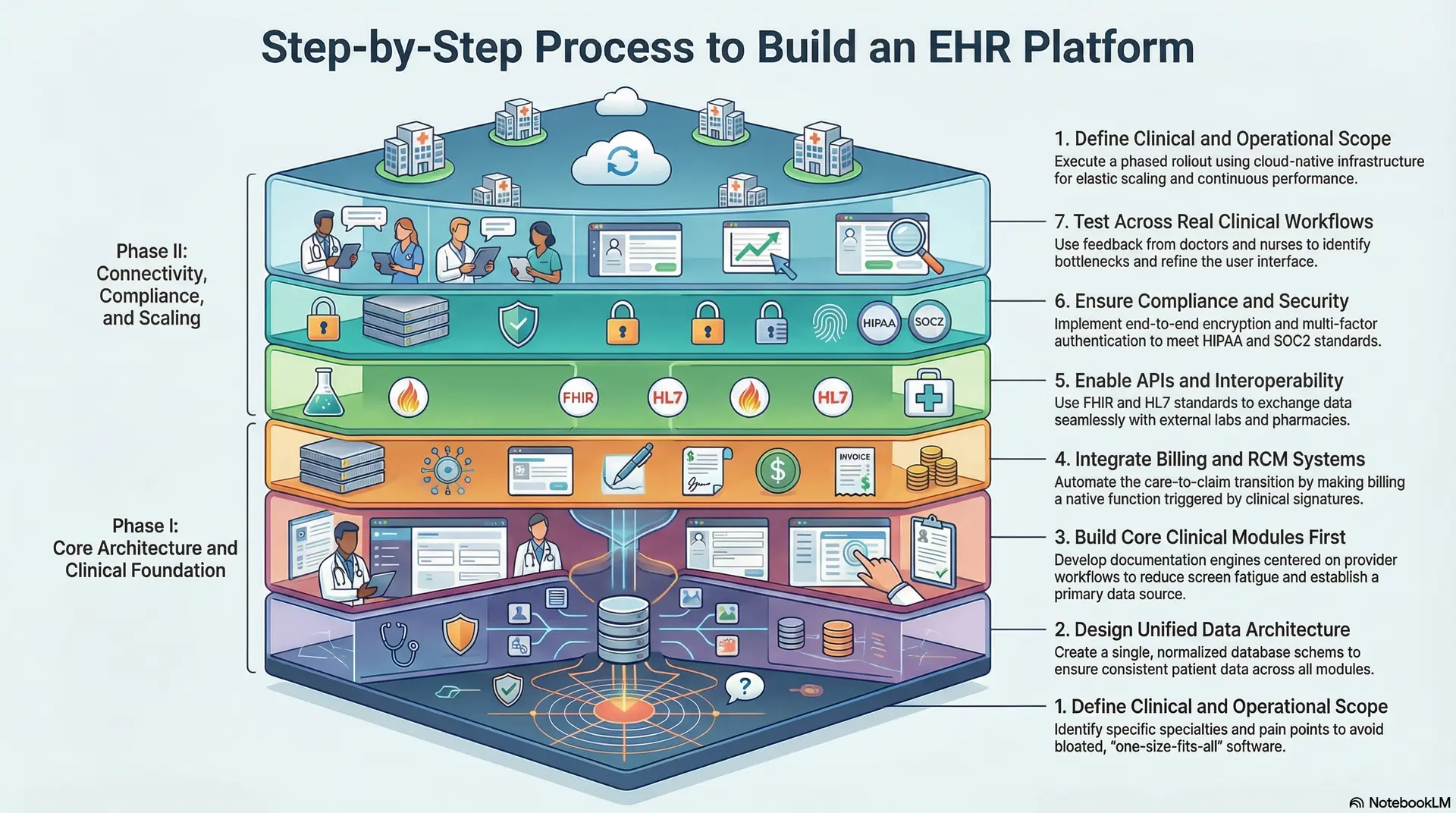
Step 1: Define Clinical and Operational Scope
Before writing a single line of code, leadership must determine which medical specialties and business workflows the platform will support. A “one-size-fits-all” approach often leads to bloated software that serves no one well.
Therefore, identifying specific “pain points”, such as slow patient intake or high claim denial rates, is essential for setting development priorities. This discovery phase ensures the engineering team builds features that solve real-world problems for clinicians and administrators alike.
Step 2: Design Unified Data Architecture
The most critical technical step is creating a single, normalized database schema that all modules will share. Unlike fragmented systems, a unified architecture ensures that a patient’s address, medication list, and balance remain consistent across the entire platform.
Consequently, this eliminates the need for internal “data bridges” that often break during system updates. Designing for data liquidity at this stage prevents expensive technical debt as the enterprise grows.
Step 3: Build Core Clinical Modules First
The heart of the system is the clinical charting and documentation engine. This module must be designed with the provider’s workflow in mind, using intuitive layouts that reduce “screen fatigue.”
By building the clinical core first, you establish the primary source of truth for all subsequent data points. Intellivon specializes in incorporating AI-driven documentation tools at this stage, allowing physicians to dictate notes that are automatically converted into structured, coded data.
Step 4: Integrate Billing and RCM Systems
Once the clinical engine is stable, the focus shifts to the Revenue Cycle Management (RCM) layer. In a unified platform, billing is not an add-on but a native function that triggers the moment a clinical note is signed.
This integration ensures that every billable action is captured accurately without manual intervention. By automating the transition from care to claim, the organization significantly reduces its Days Sales Outstanding (DSO) and improves overall cash flow.
Step 5: Enable APIs and Interoperability
A modern EHR must communicate with the broader healthcare world through FHIR and HL7 standards. Building an API-first architecture allows the platform to exchange data seamlessly with external labs, pharmacies, and imaging centers.
This connectivity ensures that the enterprise is ready for value-based care models where shared data is a requirement. Therefore, interoperability is treated as a core feature rather than a secondary consideration for the development team.
Step 6: Ensure Compliance and Security
In 2026, healthcare data security must be proactive rather than reactive. This step involves implementing end-to-end encryption, multi-factor authentication, and sophisticated role-based access controls.
The platform must be engineered to meet HIPAA, SOC2, and other global regulatory standards by default. Our deep expertise in healthcare compliance ensures that every layer of the infrastructure is “audit-ready” and protected against emerging cyber threats.
Step 7: Test Across Real Clinical Workflows
Before a wide-scale rollout, the system must be rigorously tested in a live clinical environment. This phase identifies “bottlenecks” that only appear during high-volume patient hours, such as slow chart loading or confusing navigation menus.
Feedback from actual doctors and nurses is used to refine the user interface for maximum efficiency. Testing ensures that the platform is a tool for care delivery rather than an obstacle to it.
Step 8: Deploy and Scale Across Facilities
The final stage is the phased rollout across the organization’s locations. Using a cloud-native infrastructure allows for “elastic scaling,” meaning the system can support more users without a decrease in performance.
Continuous monitoring and automated updates ensure the platform remains secure and efficient as the enterprise expands. Partnering with a scale-ready firm like Intellivon provides the technical backbone needed to manage this transition without operational downtime.
Following this structured path transforms the complexity of EHR development into a manageable, strategic asset. By prioritizing a unified design, leaders ensure their technology investment drives both clinical excellence and financial growth.
Cost to Build an All-in-One EHR Platform
Building an all-in-one EHR platform is not a fixed-cost project. The total investment depends on how deeply the system integrates clinical workflows, administrative operations, and revenue cycle management into a single architecture.
Unlike fragmented solutions, a unified platform requires strong data foundations, compliance layers, and scalable infrastructure from day one. As a result, costs are shaped more by system complexity than just feature count.
1. Cost Breakdown by Modules and Complexity
| Component | Scope | Estimated Cost |
| Clinical Module | Charting, EMR, decision support | $15,000 – $30,000 |
| Scheduling & Intake | Appointments, patient onboarding | $8,000 – $15,000 |
| ePrescription System | Drug databases, pharmacy integration | $8,000 – $18,000 |
| Billing & RCM | Claims, invoicing, payment workflows | $15,000 – $35,000 |
| Insurance Integration | Eligibility checks, claims validation | $10,000 – $20,000 |
| Analytics & Reporting | Dashboards, operational insights | $8,000 – $18,000 |
Modules are built as part of a unified system, and not separate tools.
2. Infrastructure and Cloud Costs
| Component | Scope | Estimated Cost |
| Cloud Hosting (AWS/GCP/Azure) | Servers, storage, scaling | $5,000 – $15,000/year |
| Database Management | High-availability, backups | $3,000 – $10,000 |
| API and Integration Layer | Internal and external APIs | $5,000 – $12,000 |
A cloud-native setup ensures scalability, but costs increase with data volume, user load, and real-time processing needs.
3. Compliance and Security Costs
| Component | Scope | Estimated Cost |
| HIPAA Compliance Setup | Encryption, access control | $5,000 – $15,000 |
| Audit Logs & Monitoring | Tracking and governance systems | $3,000 – $8,000 |
| Security Testing | Penetration testing, audits | $3,000 – $7,000 |
Healthcare platforms cannot compromise on compliance. These are mandatory investments, not optional add-ons.
Hidden Costs Enterprises Often Miss
- Data migration from legacy systems
- Workflow redesign across departments
- Integration cleanup and dependency removal
- Ongoing maintenance and version upgrades
- Training and onboarding for staff
These costs often increase total project budgets by 20–30%
Estimated Total Cost Range
| Platform Scope | Estimated Cost |
| MVP (Core Modules Only) | $40,000 – $70,000 |
| Mid-Level Platform | $70,000 – $120,000 |
| Enterprise-Grade Platform | $120,000 – $200,000+ |
Most healthcare organizations underestimate the cost of building a unified EHR platform because they compare it to modular systems. However, the real value comes from eliminating long-term integration costs, reducing operational inefficiencies, and improving revenue cycles.
At Intellivon, EHR platforms are built as long-term infrastructure, not short-term software projects. This approach ensures that the system scales with your organization without requiring constant rebuilds or integrations.
Compliance Requirements for EHR Platforms
Navigating the labyrinth of healthcare regulations is the highest hurdle for any enterprise looking to deploy a unified platform. In 2026, compliance is no longer a checkbox exercise but a continuous, high-stakes operational requirement that defines your market reputation.
1. HIPAA and Data Privacy Standards
The Health Insurance Portability and Accountability Act remains the foundational pillar for any medical software in the United States. A unified EHR must ensure that Protected Health Information (PHI) is encrypted both at rest and during every transmission.
In 2026, this extends beyond simple passwords to include multi-factor authentication and automated session timeouts. Therefore, the architecture must support granular privacy controls that allow patients to manage their own data sharing preferences.
2. HL7 and FHIR Requirements
Interoperability is now a legal mandate under the 21st Century Cures Act. Platforms must utilize Fast Healthcare Interoperability Resources (FHIR) to allow for the seamless exchange of data between different healthcare providers.
This standardized digital language ensures that a patient’s records are accessible across labs, hospitals, and pharmacies without technical friction. Consequently, developers must prioritize an API-first design that natively supports these global data exchange protocols.
3. Audit Trails and Data Governance
A robust EHR must maintain an immutable record of every interaction within the system. This audit trail tracks who accessed which record, what changes were made, and exactly when the event occurred.
Strong data governance policies ensure that information remains accurate and consistent across the entire enterprise. These logs are essential during federal audits or legal discovery, providing a single source of truth for the organization’s operational integrity.
4. Security Best Practices
Modern security goes far beyond basic firewalls to include Zero-Trust architectures and real-time threat monitoring. Systems must be designed to detect and neutralize unauthorized access attempts before they reach the core database.
This includes regular vulnerability scanning and end-to-end encryption for all mobile and cloud-based touchpoints. Maintaining a high security posture is the only way to build lasting trust with both providers and the patients they serve.
Mastering these compliance requirements is the only way to safeguard the long-term viability of your technology investment. A secure, compliant foundation is the ultimate competitive advantage in the modern healthcare economy.
Top 5 All-In-One EHR Platforms (2026)
Beyond Epic and Oracle, platforms like Praxis EMR, CureMD, and blueBriX are defining the 2026 EHR landscape. These systems prioritize AI-driven “concept processing” and specialty-specific database schemas to eliminate the rigid templates that typically cause provider burnout.
1. Praxis EMR
Unlike traditional systems that rely on restrictive templates, Praxis EMR uses an AI-driven “Concept Processor” that learns from each physician’s unique documentation style.
As a provider charts, the system recalls past cases and suggests text in their own words, significantly speeding up the documentation process. This template-free approach ensures that clinical notes remain original and legally robust.
Consequently, it has become a top choice for practitioners who value clinical freedom alongside automated efficiency.
2. CureMD
CureMD offers a robust, SMART cloud platform that natively integrates EHR, practice management, and medical billing into a single ecosystem. It stands out for its high level of specialty-specific customization, allowing oncology or dermatology practices to use workflows designed for their unique needs.
Because the system is built on a unified database, financial data flows instantly from the clinical note to the billing queue. This architectural clarity makes it an ideal solution for mid-sized enterprises looking to maximize their revenue cycle velocity.
3. blueBriX
For organizations managing complex mental health and substance-use care, blueBriX provides a highly specialized, unified environment. It is engineered to handle strict regulatory requirements, such as 42 CFR Part 2, which generic EHRs often struggle to manage.
The platform combines telehealth, analytics, and care coordination into one interface, ensuring that every member of a multi-disciplinary team is aligned. Therefore, it is rapidly becoming the standard for large-scale behavioral health facilities seeking operational consistency.
4. NuvertOS
NuvertOS is emerging as a powerful cloud-based “Brain” for hospitals, covering everything from pharmacy and labs to IPD and OPD management. Its primary strength lies in its rapid implementation timeline and zero-hidden-cost model, which appeals to growing hospital chains.
The platform uses predictive AI to manage bed availability and nursing notes in real-time, providing leadership with a 360-degree view of hospital operations. This level of transparency is essential for maintaining high-quality care during rapid organizational expansion.
Choosing a lesser-known, specialized platform can often provide a more tailored fit for an enterprise’s unique clinical goals. These innovators are proving that a unified, AI-first approach is the most effective way to drive long-term growth and provider satisfaction.
Conclusion
Building an all-in-one EHR platform is not just a technology decision. It is a shift toward a unified, scalable healthcare infrastructure. While fragmented systems create delays and inefficiencies, a unified platform brings consistency, speed, and control across operations.
However, success depends on strong architecture and execution. With the right partner, healthcare organizations can build systems that scale, stay compliant, and support long-term growth without operational bottlenecks.
Build an All-in-One EHR Platform With Intellivon
At Intellivon, all-in-one EHR platforms are built as enterprise healthcare infrastructure, not as tools layered onto disconnected systems. The focus is to unify clinical, operational, and financial workflows into a single platform that enables real-time visibility and scalable care delivery.
Each platform is designed to support the full healthcare lifecycle. This includes clinical documentation, scheduling, billing, insurance processing, analytics, and workflow automation, all powered by a single, unified data architecture. As a result, teams operate on consistent data, reduce manual work, and move faster across departments.
Our approach combines API-first, cloud-native architecture with interoperability standards like HL7 and FHIR. This ensures seamless integration where required, without creating long-term dependencies on fragmented systems.
Why Intellivon for All-in-One EHR Platforms?
- Unified Architecture, Not Patchwork Systems: Build a single source of truth across clinical, operational, and financial workflows. This eliminates data silos and ensures consistent, real-time system performance.
- Deep Healthcare Workflow Expertise: Design platforms aligned with real clinical and administrative processes. This improves usability, reduces friction, and ensures faster adoption across teams.
- API-First and Scalable Infrastructure: Enable flexibility and future expansion without rebuilding core systems. Scale across facilities, services, and patient volumes with ease.
- Compliance-Ready by Design: Integrate HIPAA, HL7, and FHIR standards from the ground up. Ensure secure data exchange, audit readiness, and regulatory compliance at every level.
- Built for Long-Term Performance: Platforms are engineered to handle high data loads, complex workflows, and multi-location operations without compromising speed or reliability.
If you’re planning to build or replace an EHR system with a unified platform, Intellivon can help you design and deploy a scalable, future-ready solution.
FAQs
Q1. What is an all-in-one EHR platform?
A1. An all-in-one EHR platform is a unified system that combines clinical records, scheduling, billing, and insurance workflows into a single database. Unlike fragmented solutions, it creates a single source of truth. As a result, patient data flows seamlessly across departments, reducing manual work, improving accuracy, and enabling real-time visibility into both care delivery and operations.
Q2. How long does EHR development take?
A2. EHR development timelines depend on system complexity and scope. A basic MVP with core modules typically takes 4–6 months. In contrast, a full-scale, enterprise-grade platform can take 8–14 months. Factors such as integrations, compliance requirements, and workflow customization also impact timelines. A structured architecture approach can significantly reduce delays and rework.
Q3. What features should a unified EHR include?
A3. A unified EHR should include clinical documentation, appointment scheduling, ePrescription, billing and revenue cycle management, insurance processing, and analytics. In addition, it should support interoperability through HL7 and FHIR, role-based access control, and real-time data synchronization. These features ensure seamless workflows, compliance, and scalability across healthcare operations.
Q4. How much does EHR development cost?
A4. The cost to build an EHR platform varies based on features, integrations, and scale. An MVP may cost between $40,000 and $70,000, while a mid-level platform ranges from $70,000 to $120,000. Enterprise-grade systems can exceed $120,000. However, unified platforms reduce long-term costs by eliminating third-party dependencies and improving operational efficiency.
Q5. Can EHR systems scale across hospitals?
A5. Yes, modern EHR platforms are designed to scale across multiple hospitals and locations. With cloud-native infrastructure and API-first architecture, these systems can handle high patient volumes, complex workflows, and distributed teams. When built correctly, they maintain performance, data consistency, and compliance as the organization grows.