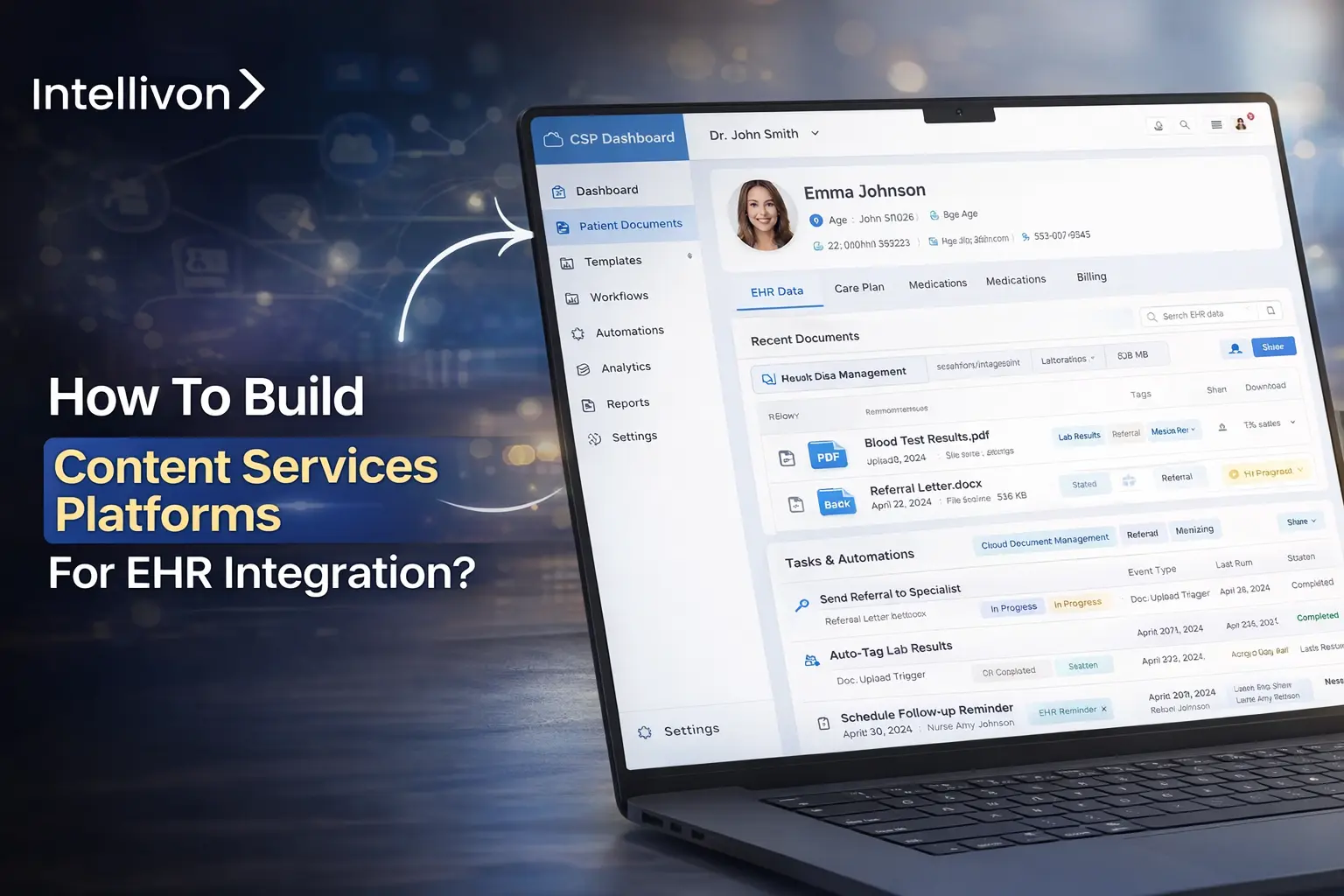
Healthcare data doesn’t stall because clinical notes, imaging files, consent forms, lab reports, and insurance documents constantly move across departments. When systems can’t keep up, the whole operation feels the impact. Healthcare enterprises are struggling because their infrastructure isn’t designed for this volume or complexity.
A content services platform that effectively connects with Electronic Health Records is a current operational need, and leading companies have already integrated these platforms into their workflows. This decision impacts compliance, care delivery speed, revenue cycle health, and how well your teams can perform their jobs. Getting the setup right from the beginning saves both costs and complications later on.
Intellivon has partnered with healthcare enterprises to create enterprise-grade platforms that combine AI, security measures, and integrated architecture. This blog outlines what a scalable content services platform build requires, including architecture choices, compliance issues, and integration hurdles.
Why Content Services Matter in Modern EHR Systems
Content services are no longer optional in modern EHR systems. Instead, they act as a critical differentiator. They convert fragmented, unstructured content, such as scans, notes, consent forms, and emails, into structured, patient-centric data. As a result, healthcare providers can reuse this data across clinical care, billing, and analytics workflows.
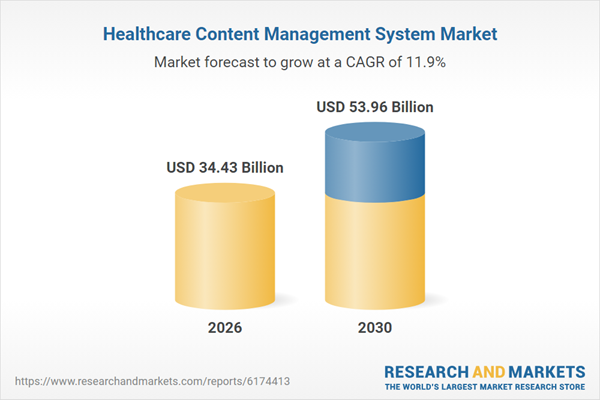
This reflects a strong compound annual growth rate (CAGR) of 12.2%, driven by rising demand for scalable, data-driven healthcare systems.
Modern healthcare environments move too fast for traditional paper-based or siloed digital filing. When clinicians cannot find a specific lab report or a signed consent form within the EHR, patient care slows down, and risks increase.
Content services solve this by acting as the intelligent glue between the patient record and the actual documents. This ensures that every piece of information is indexed, searchable, and available at the point of care without leaving the primary clinical interface.
1. From document storage to clinical data orchestration
Moving beyond simple storage means treating documents as active data points. Clinical orchestration ensures that a specialist’s note from three years ago automatically surfaces when a physician opens a relevant diagnosis screen.
Therefore, the system anticipates the user’s needs by routing the right content to the right person at the right time.
2. Why legacy ECM fails in healthcare workflows
Older Enterprise Content Management (ECM) systems are often too rigid for the fluid nature of medicine. They rely on manual folder structures that do not communicate with modern APIs.
This lack of integration forces staff to jump between applications, which creates massive operational friction and increases the likelihood of data entry errors.
3. Role of content services in interoperability at scale
As healthcare networks grow, sharing data between different facilities becomes a major hurdle. Content services utilize HL7 and FHIR standards to bridge these gaps.
Consequently, this allows a centralized platform to serve as a single source of truth for patient records across multiple geographic locations and disparate software systems.
4. How content impacts clinical and operational decisions
Fast access to a comprehensive patient history directly improves clinical outcomes and reduces hospital readmissions. Operationally, these platforms automate the “revenue cycle” by ensuring all billing documentation is complete.
This efficiency reduces administrative overhead and allows healthcare leaders to reallocate resources toward expanding their service lines and improving patient experiences.
By prioritizing a content services strategy, organizations move from simply managing files to mastering the information that drives clinical excellence. This shift turns a technical necessity into a significant competitive advantage in the healthcare market.
What Is a Content Services Platform in Healthcare?
A Healthcare Content Services Platform (CSP) is a modular, API-first architecture designed to manage unstructured patient data within the EHR ecosystem.
It replaces rigid filing systems with flexible microservices that index, store, and surface medical images or clinician notes in real-time.
By utilizing HL7 and FHIR standards, a CSP ensures that vital documents remain accessible across different hospital departments and geographic locations.
CSP vs ECM In Healthcare Infrastructure
Healthcare enterprises are moving beyond traditional document management. While ECM systems focused on storing files, modern healthcare demands platforms that can actively manage, connect, and activate data across systems.
This is where Content Services Platforms (CSP) come in. They transform static content into usable, interoperable data that supports clinical and operational workflows.
CSP vs ECM: Key Differences
| Factor | ECM (Enterprise Content Management) | CSP (Content Services Platform) |
| Core Purpose | Centralized document storage and archiving | Dynamic content management and data orchestration |
| Data Handling | Primarily unstructured document storage | Handles both structured and unstructured data |
| Integration | Limited integrations with EHR systems | API-first integration with EHR, labs, and billing systems |
| Interoperability | Siloed systems with restricted data flow | Built for HL7, FHIR, and real-time data exchange |
| Scalability | Rigid and difficult to scale | Cloud-native and highly scalable |
| Clinical Use | Passive storage of records | Active role in clinical workflows and decisions |
| Automation | Minimal automation capabilities | AI-driven classification, extraction, and workflows |
| Access Speed | Slower retrieval from document repositories | Real-time access across systems |
| Compliance | Basic compliance support | Advanced compliance, audit trails, and governance |
ECM systems were designed for document storage. However, modern healthcare needs more than that. CSP platforms enable real-time access, interoperability, and intelligent data use.
As a result, they play a direct role in improving care delivery, operational efficiency, and decision-making.
For enterprises building EHR-integrated systems, CSP is a foundational infrastructure.
Where EHR Systems Break Without Content Layers
Standard EHR platforms manage discrete data well, but they often struggle with the unstructured documents that provide clinical context.
Without a unified content layer, these vital records remain trapped in disconnected silos, forcing clinicians to waste time searching multiple systems.
1. Fragmented patient records across departments
A patient’s medical journey rarely stays within one department. However, without a content layer, a cardiologist may never see imaging reports from the emergency room.
This lack of visibility leads to duplicate testing and a fragmented understanding of the patient’s condition. Furthermore, these gaps often result in conflicting treatment plans that compromise safety.
2. Clinical workflows slowed by document silos
When clinical documents live in isolated systems, the workflow inevitably grinds to a halt. Consequently, nurses and physicians spend valuable minutes logging into different portals for a single consent form.
This friction directly contributes to clinician burnout and reduces the time spent on actual patient care. In addition, these delays can postpone surgeries, which negatively impacts hospital throughput.
3. Compliance risks due to unmanaged data flows
Insecure document sharing is a major liability for any healthcare enterprise. Therefore, without a centralized platform, staff may resort to using unencrypted email to move patient data.
These practices create massive holes in the audit trail and increase the risk of a HIPAA violation. A robust content layer ensures that every document is tracked and encrypted.
4. Lack of real-time access to patient information
In emergency medicine, every second counts, so waiting for a document to be “pulled” from an archive is not an option. Legacy systems often require manual indexing, meaning a document might not be available for hours.
Modern content services solve this by providing instant access. As a result, providers no longer have to make decisions based on incomplete information.
Organizations must prioritize a unified content strategy to eliminate these systemic breakdowns. Addressing these gaps ensures the EHR delivers on its promise of clinical excellence and operational efficiency.
Key Use Cases of CSP in EHR Integration
A strategic Content Services Platform (CSP) transforms the EHR from a data repository into a comprehensive clinical intelligence hub.
By mapping unstructured documents to structured patient identities, organizations can finally achieve a 360-degree view of the patient journey.
1. Unified patient records across multiple systems
Enterprises often grow through acquisitions, resulting in a fragmented landscape of different EHR brands. However, a CSP acts as a vendor-neutral archive that pulls documents from various systems into a single interface.
Consequently, a physician in a newly acquired clinic can view the full history of a patient treated at the main hospital. This unified view eliminates the need for expensive and risky data migrations between legacy platforms.
2. Automated clinical documentation and indexing
Manual indexing is a significant bottleneck that introduces human error into the medical record. Modern CSPs utilize machine learning to “read” incoming documents and categorize them automatically.
For example, the system can identify a document as a “Cardiology Referral” and extract the patient’s ID. In addition, this automation ensures that records are filed correctly without requiring hours of administrative labor.
3. Claims processing and billing document management
Revenue cycle management relies heavily on the supporting documentation required by payers. Therefore, a CSP links clinical notes directly to billing codes, ensuring that every claim is backed by the necessary medical evidence.
This transparency reduces the frequency of claim denials and speeds up the reimbursement cycle. Moreover, the system can compile all relevant documents for an audit with a single click.
4. Consent, compliance, and audit trail automation
Managing patient consent forms is a high-stakes legal requirement that is often handled poorly with paper files. A digital content layer tracks every version of a consent form and ensures it is signed before a procedure begins.
Furthermore, the platform maintains a forensic-level audit trail of who accessed which document and when. This level of oversight is essential for maintaining HIPAA compliance and protecting the organization.
5. Imaging and diagnostic report integration
Standard EHRs often struggle to display high-resolution medical images alongside clinical text. A CSP integrates with imaging systems to surface diagnostic results directly within the patient’s chart.
Therefore, a clinician can view a radiology report and the corresponding X-ray side-by-side without switching applications. This seamless access leads to faster diagnoses and a more collaborative approach to complex patient cases.
By targeting these specific use cases, healthcare leaders can drive immediate ROI while building a scalable foundation for future innovation. These integrations turn fragmented data into a cohesive asset that supports both clinical excellence and financial stability.
Architecture of a Content Services Platform
A robust CSP architecture must serve as the high-speed connective tissue between the EHR and unstructured medical records. This structure ensures data mobility while maintaining the strict security required for enterprise healthcare.
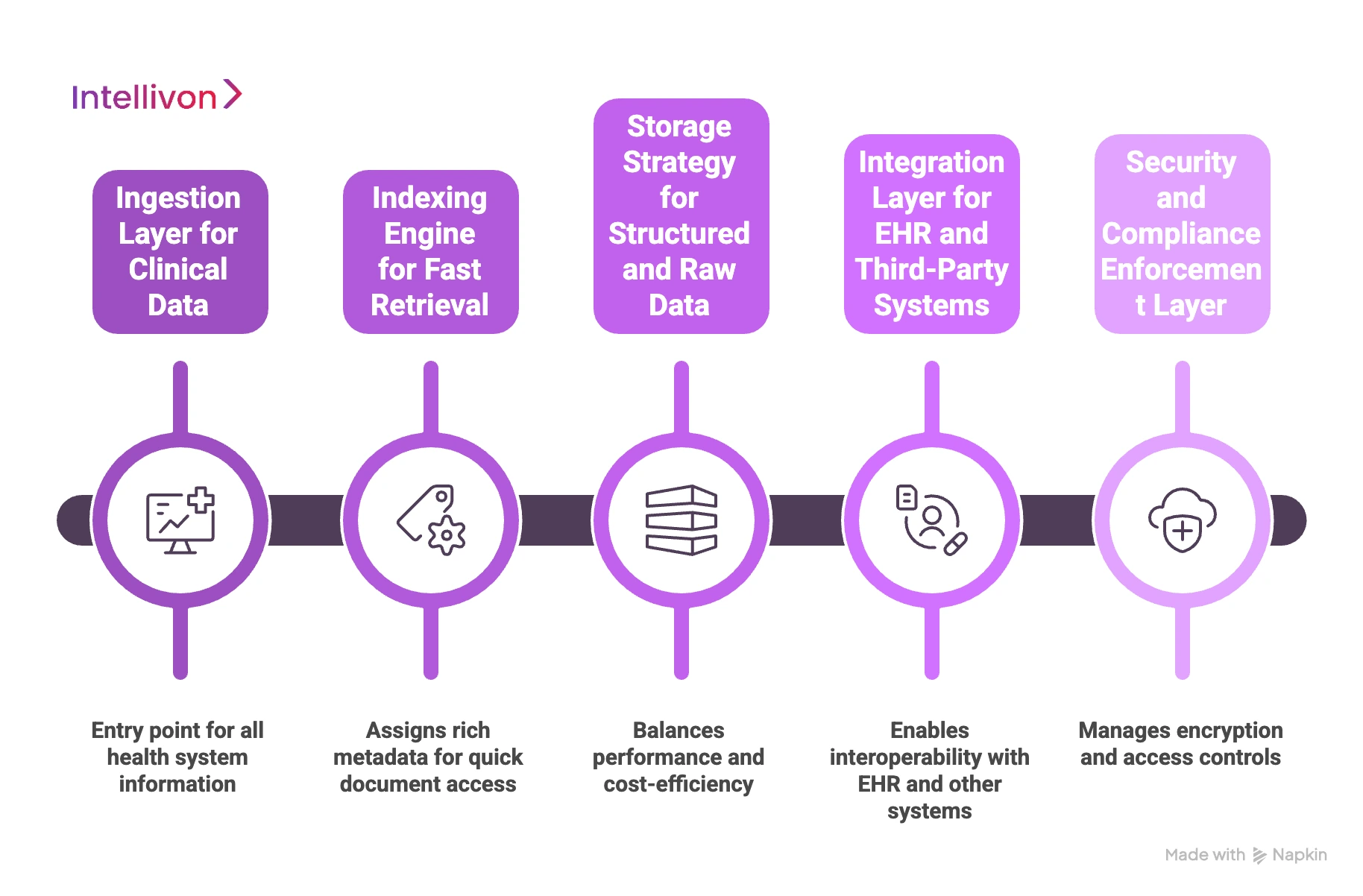
1. Ingestion Layer for Clinical Data
The ingestion layer acts as the entry point for every piece of information entering the health system. It handles diverse inputs, ranging from high-resolution images to simple PDF referral letters.
Consequently, the system validates their integrity and prepares them for processing. This ensures only clean, verified data enters the clinical ecosystem.
2. Indexing Engine for Fast Retrieval
A CSP is only as effective as its ability to find a specific document in seconds. Therefore, the indexing engine assigns rich metadata to every file, including patient demographics and encounter dates.
Furthermore, using a metadata-centric approach allows the system to surface relevant documents automatically based on the user’s current context within the EHR.
3. Storage Strategy for Structured and Raw Data
Enterprise healthcare requires a tiered storage strategy to balance performance with cost-efficiency.
Frequently accessed data resides on high-speed storage for immediate retrieval. In contrast, legacy records move to lower-cost cloud tiers. Moreover, maintaining raw data in its original format preserves its forensic value for future clinical audits.
4. Integration Layer for EHR and Third-Party Systems
Interoperability is achieved through an integration layer that speaks the language of modern healthcare. This layer utilizes FHIR and RESTful APIs to move data between the CSP and the primary EHR.
Consequently, the user experience remains seamless since the clinician never leaves their primary software environment. This integration allows a CSP to function as a native extension.
5. Security and Compliance Enforcement Layer
Security must be baked into every architectural layer rather than added as an afterthought. This component manages encryption both at rest and in transit.
In addition, the system enforces role-based access controls to ensure privacy. This rigorous enforcement of access is critical for maintaining HIPAA compliance and building trust with patients.
An optimized architecture ensures that the CSP is a high-performance engine for clinical data. By focusing on these core layers, organizations build a system that is technically superior and operationally indispensable.
Step-by-Step Development of CSP for EHR
Building an enterprise-grade CSP is not a simple software installation; it is a strategic alignment of data and clinical workflows. Therefore, Intellivon moves through a logical progression from initial assessment to full-scale deployment.
Consequently, this structured path minimizes technical debt and ensures the platform remains scalable as the healthcare landscape evolves.
Step 1: Assess existing healthcare data systems
Our first phase involves a deep audit of your current IT infrastructure and data silos. We identify where unstructured data lives, whether in legacy filing systems or disconnected departmental servers.
Moreover, understanding the limitations of your current EHR is vital for designing a complementary content layer.
Step 2: Define content workflows and lifecycle
Once we understand the data, we map out how that information moves through your organization. Consequently, this step defines the lifecycle of a document from its initial ingestion to its final archival.
Our strategists consult with your clinicians to ensure the digital workflow mirrors the physical reality of patient care.
Step 3: Design interoperability architecture
Interoperability is the most critical technical hurdle in any healthcare software project. Therefore, Intellivon designs architectures that utilize modern standards like HL7 and FHIR to ensure seamless communication.
A decoupled design allows the content layer to function independently while remaining deeply integrated into your UI.
Step 4: Build APIs and integration connectors
With the architecture defined, our focus shifts to creating the secure “hooks” that link your systems. We build RESTful APIs that allow the EHR to request specific documents on demand.
Furthermore, using standardized connectors simplifies the process of adding third-party diagnostic tools to your ecosystem later.
Step 5: Implement AI for document processing
Manual data entry is a significant source of error and administrative cost. Consequently, Intellivon integrates AI-driven Optical Character Recognition (OCR) to automatically categorize documents and extract key patient data.
This automation ensures that a scanned lab report is instantly indexed under the correct patient profile.
Step 6: Ensure HIPAA and compliance readiness
Security and compliance are rigorously tested before the platform handles any real patient records. This involves implementing end-to-end encryption and conducting thorough penetration testing on all API endpoints.
In addition, we ensure the system generates detailed audit logs that track every interaction with Protected Health Information.
Step 7: Deploy and scale across systems
The final step is the phased rollout of the CSP across your entire healthcare network. Intellivon provides a significant advantage by leveraging our expertise in high-scale AI and enterprise cloud architecture.
Consequently, our partnership allows your organization to move from a pilot to a global clinical ecosystem with confidence.
Following these steps ensures the development of a platform that is both technically robust and clinically impactful. A methodical execution transforms fragmented data into a strategic asset that drives better patient outcomes.
Technologies Used in CSP Development
Selecting a modern technology stack is the difference between a fragmented database and a truly interoperable clinical ecosystem. A cloud-native approach ensures high performance, total security, and seamless EHR integration for enterprise-scale healthcare providers.
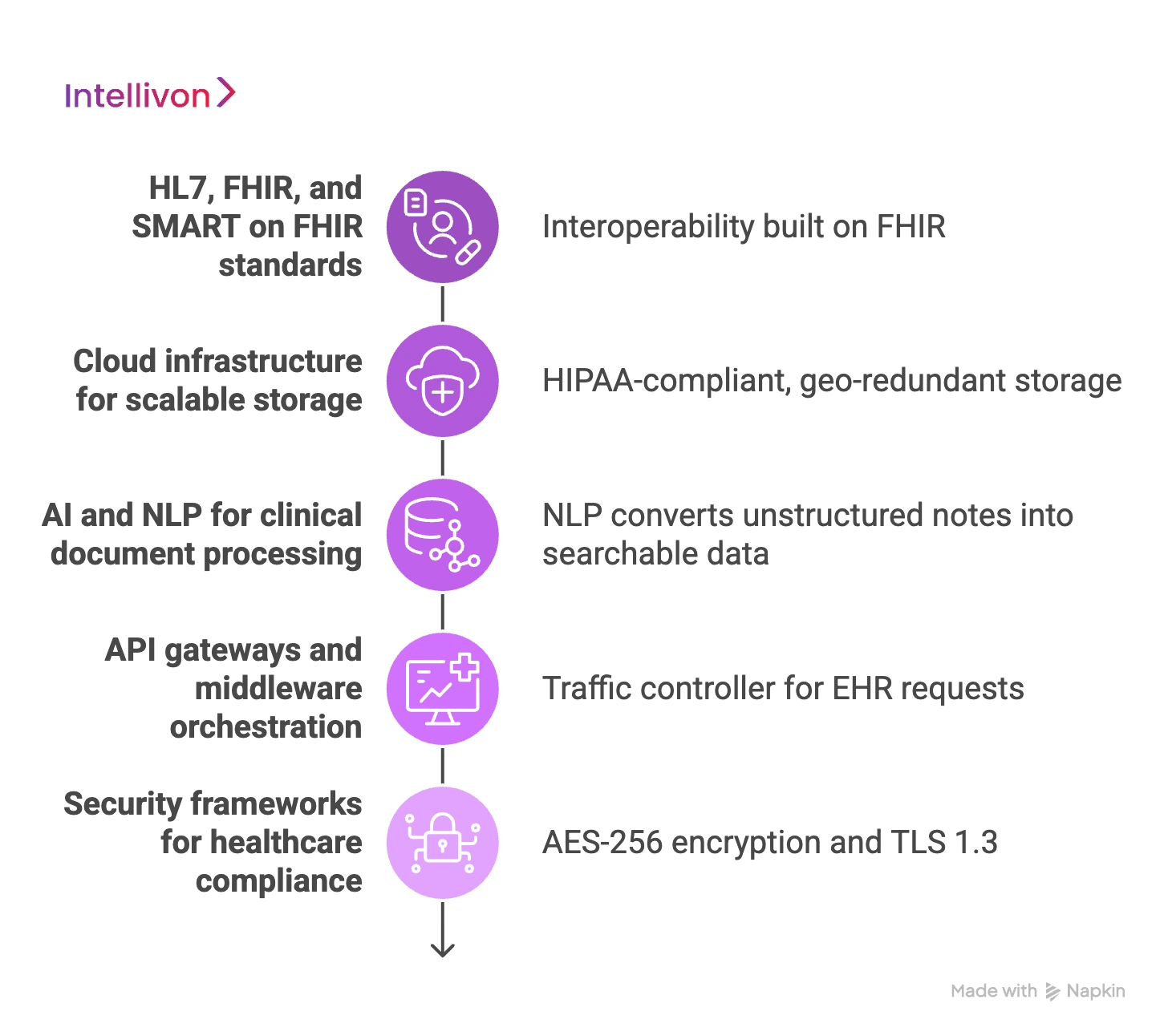
1. HL7, FHIR, and SMART on FHIR standards
Interoperability is built on the language of FHIR (Fast Healthcare Interoperability Resources). This standard allows the CSP to exchange data with any modern EHR without the need for custom, fragile code.
Furthermore, implementing SMART on FHIR enables “pluggable” apps that run directly within the EHR interface. Consequently, this ensures that clinicians have a unified experience regardless of which platform they are using.
2. Cloud infrastructure for scalable storage
Healthcare data volumes are expanding exponentially, requiring a storage strategy that can grow without massive upfront hardware costs. Leveraging enterprise cloud providers like AWS or Azure provides HIPAA-compliant, geo-redundant storage.
In addition, using object storage allows the platform to handle massive DICOM images and raw telemetry data with ease. This cloud-first approach ensures that patient records are always available, even during regional hardware failures.
3. AI and NLP for clinical document processing
Unstructured physician notes contain vital clinical insights that are often lost in static PDFs. Therefore, integrating Natural Language Processing (NLP) allows the system to “read” these documents and convert them into searchable data.
This technology can identify symptoms, medications, and diagnoses within a block of text. Moreover, this AI layer reduces the need for manual data entry, allowing administrative staff to focus on higher-value patient coordination tasks.
4. API gateways and middleware orchestration
An API gateway serves as the traffic controller for all requests moving between the EHR and the content services layer. It manages authentication, rate limiting, and request routing to ensure the system remains responsive.
Consequently, this middleware layer shields the core database from direct external exposure. By orchestrating these requests efficiently, the platform maintains the low latency required for real-time clinical decision support.
5. Security frameworks for healthcare compliance
Security is integrated through advanced encryption frameworks and identity management protocols. Utilizing AES-256 encryption for data at rest and TLS 1.3 for data in transit meets strict HIPAA requirements.
Furthermore, role-based access control (RBAC) ensures that only authorized personnel can view sensitive clinical records. This rigorous security posture is essential for protecting the organization from cyber threats and maintaining patient trust.
By combining these advanced technologies, organizations build platforms that are both resilient and future-proof. This technological depth ensures that the investment provides long-term value in an increasingly digital healthcare landscape.
Integration With Leading EHR Systems
Effective EHR integration is a strategic necessity that bridges the gap between siloed clinical data and actionable patient insights.
By leveraging a unified Content Services Platform (CSP), enterprises can achieve a seamless flow of information across the industry’s most widely used platforms.
1. Integrating with Epic using content services
Epic remains a cornerstone of the healthcare market, and its “App Orchard” ecosystem provides robust pathways for content integration. Utilizing these APIs allows a CSP to embed document links directly within the Hyperspace interface.
Furthermore, this integration ensures that when a physician opens a patient’s chart, all related external PDFs or images are instantly available. Consequently, this deep embedding reduces the need for clinicians to toggle between different software applications during a consultation.
2. Cerner integration and document workflows
Cerner’s Millennium platform relies heavily on its “Ignite” APIs to facilitate third-party data exchange. Therefore, a CSP must be configured to synchronize clinical documents with Cerner’s PowerChart environment in real-time.
This synchronization ensures that a scanned radiology report from an outside clinic is automatically indexed and searchable within the patient’s primary record. In addition, these automated workflows significantly reduce the administrative burden on nursing staff who previously handled manual uploads.
3. Athenahealth and cloud-native CSP models
As a cloud-native EHR, Athenahealth is ideally suited for integration with modern, web-based content services. The platform’s open API architecture allows for rapid deployment of document management tools without the need for on-premise hardware.
Moreover, this cloud-to-cloud connection ensures high availability and low latency for providers in remote or outpatient settings. Consequently, organizations using Athenahealth can scale their content services footprint globally with minimal technical friction.
4. Handling vendor-specific data limitations
Every EHR vendor has specific constraints regarding data formats and API rate limits. Consequently, the CSP must act as a sophisticated “buffer” that translates and optimizes data before it reaches the primary system.
This might involve converting proprietary image formats into standardized PDFs or DICOM files for better compatibility. Furthermore, a robust integration strategy includes error-handling protocols to manage system downtime or data synchronization failures without losing critical patient information.
By mastering these vendor-specific integrations, healthcare leaders can unlock the full potential of their existing EHR investments. This technical synergy is essential for creating a truly data-driven clinical environment that scales with the enterprise.
Cost to Build CSP for EHR Integration
At Intellivon, Content Services Platforms (CSP) for EHR integration are built as an enterprise healthcare infrastructure, not as document management layers added to fragmented systems. The goal is to create a unified platform that captures, structures, and distributes healthcare content across clinical and operational workflows.
However, building a CSP for EHR integration goes beyond storing documents. It requires designing data ingestion pipelines, interoperability layers, metadata frameworks, and AI-driven processing systems. As a result, healthcare organizations gain real-time access to patient data, improve workflow efficiency, and ensure compliance at scale.
Estimated Phase-Wise Cost Breakdown
| Phase | Description | Estimated Cost Range (USD) |
| Discovery & Workflow Planning | Define content types, workflows, EHR integration scope, and use cases | $8,000 – $15,000 |
| System Architecture & Data Design | Design CSP architecture, metadata models, and data pipelines | $10,000 – $20,000 |
| Content Ingestion & Processing Layer | Build pipelines for documents, scans, emails, and clinical inputs | $8,000 – $18,000 |
| EHR Integration Development | Integrate with Epic, Cerner, or other systems via FHIR/HL7 APIs | $10,000 – $25,000 |
| AI & Automation Layer | Implement document classification, OCR, and data extraction | $7,000 – $18,000 |
| Search, Retrieval & UX Development | Build interfaces for fast content access and workflow interaction | $7,000 – $15,000 |
| Compliance, Security & Testing | Ensure HIPAA compliance, encryption, audit logs, and validation | $5,000 – $12,000 |
| Deployment & Scaling Setup | Cloud deployment, performance tuning, and scalability setup | $5,000 – $12,000 |
Estimated Total Cost
For most healthcare organizations, the cost to build a CSP for EHR integration typically ranges between:
$60,000 – $160,000
Key Factors That Influence Cost
- Volume and types of content (documents, imaging, emails)
- Complexity of EHR integrations (Epic, Cerner, multi-system setups)
- Level of AI automation required for document processing
- Real-time data access and interoperability requirements
- Compliance, security, and audit requirements
- Scalability across hospitals, clinics, or regions
Get a Precise Cost Breakdown
Every CSP platform is different. The final cost depends on your data complexity, integration scope, and workflow requirements.
Talk to Intellivon’s experts to get a tailored cost estimate for your healthcare platform.
Security and Compliance in CSP Platforms
Securing sensitive medical data is a high-stakes requirement that defines the integrity of any enterprise healthcare platform.
A robust Content Services Platform (CSP) must integrate defense-in-depth strategies to protect patient privacy while ensuring data remains accessible to authorized providers.
1. HIPAA compliance and data protection layers
Maintaining HIPAA compliance during data transfers is achieved through end-to-end encryption. These protocols protect data both at rest and in transit, ensuring that unauthorized parties cannot intercept sensitive information.
Furthermore, modern architectures include automated data masking to ensure that Protected Health Information (PHI) is only visible when absolutely necessary for care.
2. Role-based access control and encryption
Enterprise environments utilize sophisticated Role-Based Access Control (RBAC) engines that integrate with hospital identity providers. This manages “least privilege” access, ensuring staff members only see information relevant to their specific job function.
Consequently, access is automatically granted or revoked based on the user’s department, backed by military-grade encryption keys.
3. Audit logs and traceability mechanisms
Traceability is maintained through an auditing layer that records every “view,” “edit,” or “download” action with a tamper-proof timestamp. These logs are consolidated into a searchable dashboard, providing a forensic-level trail of every document interaction.
Moreover, this allows compliance officers to generate comprehensive reports in seconds during a regulatory audit.
4. Managing sensitive patient data at scale
To manage high volumes, platforms utilize AI-driven tools that scan and “tag” sensitive information as it enters the system. This automation identifies PHI within millions of unstructured PDFs or images instantly.
Therefore, the system applies higher security headers to high-risk documents without manual intervention.
Building a secure CSP ensures that your clinical data remains a fortified asset. At Intellivon, we specialize in developing these cutting-edge, enterprise-grade AI solutions to help you scale securely.
Future of Content Services in Healthcare Systems
The future of healthcare technology is shifting from simple record-keeping to proactive, intelligent data ecosystems. As content services platforms evolve, they will serve as the cognitive engine behind modern EHRs, turning static documents into real-time clinical intelligence.
1. AI-driven clinical documentation automation
Documentation burdens are a primary cause of clinician burnout in modern health systems. Future content services will utilize advanced generative AI to “listen” to clinical encounters and draft structured notes in real-time.
Furthermore, these systems will automatically index and cross-reference these notes with existing patient records. This automation ensures that the medical record is always current and accurate without requiring hours of manual input from the provider.
2. Real-time data exchange across care networks
Interoperability will move from a periodic data “pull” to a continuous, real-time stream of information between facilities. Consequently, a patient’s health data will be instantly available to any authorized provider across the global care network.
This level of connectivity eliminates the need for duplicate testing and ensures that specialists have immediate access to emergency department records. Therefore, the healthcare journey becomes a single, continuous narrative rather than a series of disconnected events.
3. Predictive analytics powered by unified data
When clinical documents are unified within a single content layer, they become a goldmine for predictive insights. Future platforms will scan millions of unstructured records to identify early warning signs of chronic diseases or potential outbreaks.
Moreover, these analytics will provide decision-makers with real-time data on hospital throughput and resource allocation. This transition from reactive to proactive management is essential for improving patient outcomes and maintaining financial stability.
4. Rise of cloud-native healthcare platforms
The infrastructure of healthcare is rapidly moving away from on-premise servers toward flexible, cloud-native architectures. These platforms offer the elasticity needed to manage the massive influx of data from wearable devices and high-resolution imaging.
In addition, cloud-native systems provide superior disaster recovery and global accessibility for decentralized care teams. This shift ensures that the enterprise can scale its technology footprint rapidly to meet the demands of a growing patient population.
Embracing these future-ready technologies ensures that healthcare organizations remain competitive and clinically effective. A unified, intelligent content strategy is the foundation upon which the next era of medicine will be built.
Conclusion
Building a Content Services Platform for EHR integration is a strategic investment in clinical efficiency and data integrity. Therefore, shifting from fragmented storage to a unified digital ecosystem ensures your organization remains competitive and compliant. Consequently, this transformation allows leaders to focus on growth while providing clinicians with the real-time insights they need.
Intellivon provides the cutting-edge, enterprise-grade AI solutions required to build this future-proof infrastructure. Our expertise in high-scale clinical data orchestration ensures your platform scales seamlessly across global care networks. Contact Intellivon today to design a custom content strategy that turns your unstructured data into a powerful clinical asset.
Build a CSP for EHR Integration With Intellivon
At Intellivon, Content Services Platforms (CSP) for EHR integration are built as an enterprise healthcare infrastructure, not as document repositories layered onto disconnected systems. The objective is to create a unified platform that captures, structures, and distributes clinical content across workflows, enabling seamless data flow across care, billing, and operations.
Each platform is designed to support the full content lifecycle. This includes data ingestion, document processing, metadata management, EHR synchronization, workflow automation, and real-time access to patient information. As a result, healthcare organizations reduce data silos, improve clinical efficiency, and enable faster, more informed decision-making.
Our engineering approach focuses on AI-first, API-driven architectures combined with interoperability standards like HL7 and FHIR. This ensures seamless integration with EHR systems, labs, imaging platforms, and third-party healthcare applications without disrupting existing operations.
Why Intellivon for CSP + EHR Development
- Clinical infrastructure, not just content storage: Platforms are designed to activate healthcare data, not just store documents in isolated systems.
- Built for interoperability from day one: Seamless integration with EHRs and external systems ensures consistent, real-time data exchange across the healthcare ecosystem.
- AI-driven content processing and automation: Automate document classification, extraction, and workflows to reduce manual effort and improve accuracy.
- Real-time access to patient-centric data: Enable clinicians and staff to access unified, up-to-date patient information across systems instantly.
- Scalable and compliance-ready architecture: Support multi-location healthcare environments while meeting HIPAA and global regulatory requirements.
Whether you are building a new CSP or modernizing legacy content systems, Intellivon helps you design, develop, and scale with confidence.
Talk to Intellivon’s healthcare experts to get a tailored roadmap and cost estimate for your CSP platform.
FAQs
Q1. What is a content services platform in healthcare?
A1. A content services platform (CSP) manages and organizes healthcare content across systems. It handles documents, images, emails, and clinical notes in one place.
Unlike traditional systems, CSP converts unstructured content into structured, usable data. As a result, providers can access, share, and use patient information across care, billing, and analytics workflows.
Q2. How does CSP integrate with EHR systems?
A2. CSP integrates with EHR systems using APIs and interoperability standards like HL7 and FHIR. It connects content from multiple sources directly to patient records.
For example, scanned documents or lab reports are automatically indexed and linked to the correct patient. This ensures real-time access to complete, up-to-date information within the EHR.
Q3. How long does CSP development take
A3. CSP development typically takes between 3 and 6 months. However, the timeline depends on integration complexity and platform scope.
For instance, multi-system EHR integrations or AI-driven automation can extend development time. On the other hand, simpler deployments with limited workflows can be completed faster.
Q4. What data can CSP platforms manage?
A4. CSP platforms manage both structured and unstructured healthcare data. This includes patient records, clinical notes, scanned documents, imaging files, emails, and consent forms.
In addition, they handle metadata, audit logs, and workflow data. As a result, organizations get a complete, unified view of patient information across systems.
Q5. How much does CSP development cost
A5. The cost to build a CSP for EHR integration typically ranges from $60,000 to $160,000. However, the final cost depends on several factors.
These include the number of integrations, volume of content, level of AI automation, and compliance requirements. Therefore, most enterprises require a tailored estimate based on their specific workflows and scale.