The average hospital generates thousands of clinical data points each hour, which include medication changes, discharge summaries, lab results, and referral requests. These are recorded, timestamped, and filed within existing EHR systems that cost millions to set up. Still, a care coordinator managing a high-risk patient has no reliable way to know when a critical lab value changed two hours ago. This is a structural issue that traditional EHR platforms face, and it costs significantly in readmissions, care delays, and lost revenue due to poor documentation.
EHR communication automation platforms fill that gap at the infrastructure level. A well-designed system connects clinical events directly to workflows without waiting for staff to manually provide the information. The platform actively moves information to the right person at the right time, which is something a traditional EHR system cannot do.
At Intellivon, creating enterprise-grade AI systems for compliance-heavy environments is central to our work. This blog draws from our experience and talks about how we build EHR communication automation systems for healthcare companies from the ground up.
Why EHR Systems Malfunction When Scaled
EHR systems often break down as organizations scale. Most platforms were designed for smaller environments, not enterprise-wide operations. As a result, rigid architectures, poor interoperability, and rising system load start to create serious bottlenecks.
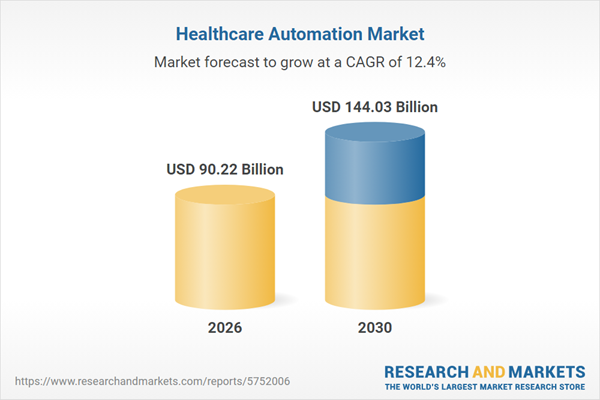
EHR communication automation systems streamline patient and provider interactions using AI-driven messaging, reminders, and integrated portals. They replace manual workflows as healthcare automation grows rapidly, with the market projected to reach $90.22 billion in 2026.
1. Scalability Barriers
Monolithic EHR systems struggle as data volume increases. Database performance slows down, and system response times drop. At the same time, on-premise setups cannot scale quickly. Expanding infrastructure can take weeks or even months.
Cloud migration helps handle traffic spikes and multi-location access. However, many providers still face long-term limitations. In fact, nearly 70% are now looking for future-ready systems to avoid rising infrastructure costs and maintenance overhead.
Integration issues make this worse. When EHR systems fail to connect efficiently with labs, billing platforms, or external tools, performance drops further as usage grows.
2. Interoperability Failures
Data sharing across systems remains a major challenge. Different EHRs use inconsistent data formats, which makes interoperability difficult. Vendor lock-in adds another layer of complexity.
This directly impacts performance. For example, models trained on one hospital’s data can lose accuracy when deployed elsewhere. In one case, AUROC dropped from 94.2% to 86.3%.
The lack of standard adoption, such as FHIR, forces teams to rely on manual workarounds. As networks expand, these inefficiencies multiply. In large hospitals, legacy silos block nearly 36% of scalability efforts.
3. Performance at Scale: What Studies Show
Research across 137 California hospitals shows a clear pattern. Larger facilities only see improvements in cost, length of stay, and readmissions when their EHR systems are built for scale.
However, most systems are not. Predictive models, such as those used for AKI detection, can lose up to 20.5% accuracy across different hospitals. This highlights a deeper issue: poor data portability.
In resource-constrained environments, the problem becomes even harder to solve. Without shared support models that address cost, infrastructure, and staffing, scalability efforts often fail. Most EHR systems fail at scale because they were never designed for it. Enterprises now need flexible, interoperable architectures built to handle real-world complexity.
What Is An EHR Communication Automation System?
In a large-scale medical environment, this system is a specialized software layer that connects every department. It is a sophisticated engine that monitors the EHR for specific triggers.
For example, if a critical lab result is uploaded, the system automatically identifies the attending physician and sends an immediate, secure alert. This automation removes the need for nursing staff to spend hours on the phone tracking down doctors.
Core goal: real-time clinical communication flow
The primary objective is to eliminate “information lag,” which is the gap between a clinical event and the necessary response. By automating the flow of data, the system ensures that clinical decisions happen in real-time.
This flow keeps everyone, from the surgical suite to the billing office, perfectly synchronized. When the communication is automated, the enterprise operates with much higher velocity and significantly fewer medical errors caused by missed messages.
Difference from basic EHR messaging tools
Standard EHR messaging is often just a “digital sticky note” that requires someone to log in and check an inbox.
Automation systems are proactive rather than passive. While a basic tool waits for a user to find the information, an automated system pushes the information out to mobile devices or workstations instantly.
It uses “if-this-then-that” logic to ensure that urgent tasks are escalated if they aren’t acknowledged within a certain timeframe.
| Feature | Basic EHR Messaging | EHR Communication Automation |
| Delivery Style | Passive (User must log in to check) | Proactive (System pushes to device) |
| Response Logic | Manual follow-up required | Automated escalation if unread |
| Data Trigger | Sent manually by a human | Triggered automatically by clinical data |
| Workflow Impact | Creates “inbox fatigue.” | Streamlines real-time action |
| Integration | Limited to the EHR platform | Connects to mobile, IoT, and external apps |
This automated approach ensures that critical updates never sit ignored in a cluttered inbox. By shifting from manual messaging to an intelligent flow, the enterprise can significantly reduce response times and improve patient safety.
Role in modern digital health infrastructure
Modern healthcare requires a foundation that supports decentralized care and rapid scaling. An automation system serves as the “connective tissue” that allows different software platforms to work as one.
It ensures that even as an organization adds more clinics or telehealth services, the quality of communication remains consistent.
This infrastructure is essential for any enterprise looking to improve patient throughput and reduce the administrative burden on its highly skilled workforce.
By transforming how information moves, these systems turn a static database into a proactive clinical partner. This shift ensures that the technology works for the providers, allowing them to focus entirely on patient recovery.
How Automated EHR Communication Actually Works
This phase of digital transformation is less about replacing human oversight and more about optimizing the data flow between siloed systems. By integrating automation into the core of your EHR, you create a responsive ecosystem that acts on patient data in real-time.
The Enterprise Automation Workflow
- Data Capture and Triggers: The process begins when a specific event occurs within the EHR, such as a lab result upload or a missed appointment. Smart sensors or API listeners detect this change immediately.
- Logic and Routing: The system evaluates the data against pre-set enterprise rules. For example, a high glucose reading might route an urgent notification to a specialist, while a routine refill request goes to a pharmacist.
- Secure Message Generation: Once the path is clear, the system generates a personalized message. It pulls specific patient details from the database to ensure the communication is relevant and actionable.
- Multi-Channel Delivery: The automation engine sends the message through the patient’s preferred channel, whether that is a secure portal, SMS, or encrypted email. This ensures higher engagement rates and fewer missed updates.
- Feedback Loop and Documentation: Every interaction is logged back into the EHR automatically. If a patient confirms an appointment via text, the schedule updates instantly without any manual data entry from your staff.
This structured approach eliminates the “black hole” of manual follow-ups that often plagues large healthcare networks. Consequently, your clinical staff can refocus their energy on complex patient care rather than administrative tracking.
Key Features Enterprises Expect in 2026
Enterprise leaders now look for EHR systems that act as proactive partners rather than passive filing cabinets. These key features ensure that high-volume data translates into immediate, high-value clinical action.
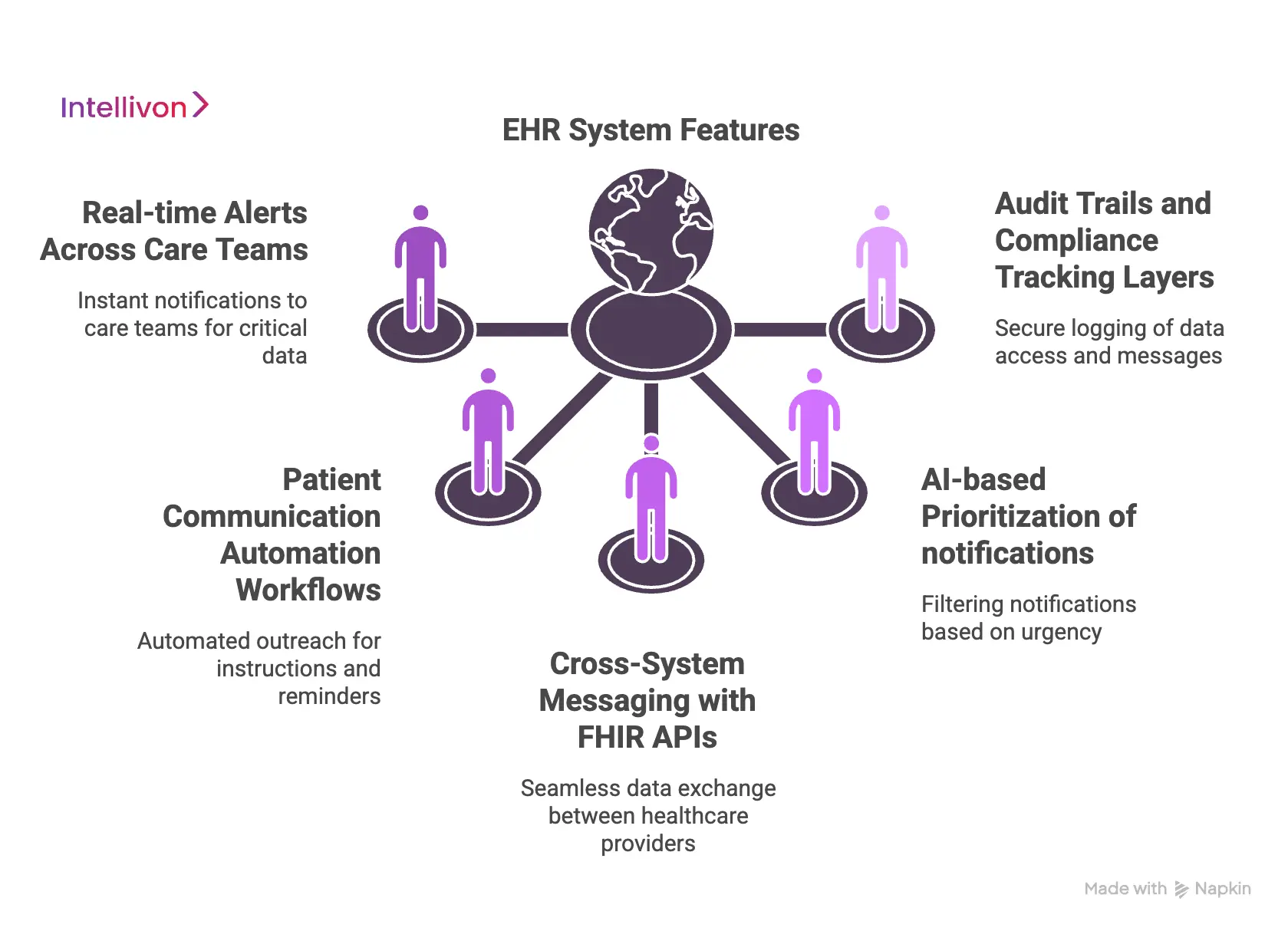
1. Real-time alerts across care teams
Modern systems eliminate the “waiting game” by pushing critical data to the right hands instantly. When a lab result hits a certain threshold, the system notifies the entire care team on their preferred devices.
This prevents communication gaps during shift changes and ensures that urgent patient needs never sit in an inbox.
2. Patient communication automation workflows
Automation handles the repetitive outreach that usually drains administrative resources. From post-discharge instructions to preventative screening reminders, the system manages the schedule based on patient history.
It scales your reach without requiring you to hire more coordinators.
3. Cross-system messaging with FHIR APIs
Data must move freely between different hospitals and specialist clinics to be truly useful. Using FHIR (Fast Healthcare Interoperability Resources) standards, these systems speak a universal language.
This allows your automation to pull data from external labs or pharmacies, creating a unified view of the patient journey.
4. AI-based prioritization of notifications
Not every alert is a crisis, so the system must distinguish between them. AI filters the “noise” by ranking notifications based on clinical urgency and patient risk scores.
Consequently, doctors only see what requires their immediate attention, which significantly reduces “alarm fatigue.”
5. Audit trails and compliance tracking layers
Security is a non-negotiable foundation for any enterprise healthcare investment. Every automated message and data access point is logged in a tamper-proof digital ledger.
This ensures you are always ready for a HIPAA audit while protecting the organization from liability.
By prioritizing these features, your organization can move from reactive management to a proactive, data-driven care model. These tools bridge the gap between complex backend data and the human-centric needs of a modern healthcare facility.
Types of EHR Communication You Can Automate
The scope of automation in healthcare has expanded far beyond simple calendar invites. By identifying the highest-friction touchpoints in your current operations, you can deploy targeted logic to handle routine interactions with precision.
1. Appointment reminders and follow-ups
Missed appointments represent a significant revenue leak for any large-scale health system. Automated workflows send reminders via SMS or voice, allowing patients to confirm or reschedule with one click.
However, the real value lies in the follow-up, where the system checks in on patients who missed a visit to bring them back into the care loop.
2. Lab results and diagnostic notifications
Processing lab results manually often creates a bottleneck that delays treatment plans. Automation allows for the immediate release of “normal” results to patient portals, accompanied by clear explanations.
For “abnormal” results, the system can trigger an internal alert for the physician while simultaneously scheduling a follow-up call with the patient.
3. Care coordination across departments
When a patient moves from primary care to a specialist, information often gets lost in transition. Automated triggers ensure that the specialist receives the relevant history before the patient arrives.
This internal “handshake” reduces redundant testing and ensures that every department is working from the same real-time data set.
4. Discharge instructions and recovery tracking
The period immediately after hospital discharge is critical for preventing readmission. Automated systems can send a series of check-ins over a 30-day period, asking patients about their symptoms or medication adherence.
If a patient reports a red-flag symptom, the system alerts the nursing team for an immediate intervention.
5. Billing, claims, and payment communications
Financial transparency is a major factor in patient satisfaction and healthy cash flow. Automation can send real-time cost estimates, explain insurance coverage in plain language, and offer flexible payment plans.
By digitizing these conversations, you reduce the administrative burden on your billing department and accelerate your collection cycles.
Automating these diverse communication paths transforms your EHR from a static record into a dynamic engagement engine. This shift not only improves the patient experience but also reinforces the operational stability of your entire enterprise.
Who Should Build Custom Communication Systems
While off-the-shelf software works for small clinics, large-scale organizations often outgrow generic tools. Custom systems are essential for those who need to own their data logic and create a unique, competitive advantage in the market.
1. Multi-hospital networks with fragmented workflows
Large health systems often struggle with data silos because they operate across multiple locations with different legacy software. Custom automation acts as a unifying layer that pulls data from every site to create a single source of truth.
Therefore, administrators can see patient flow across the entire network without logging into ten different systems.
Real-world Example: Mayo Clinic utilizes advanced custom integrations to ensure that its vast network of specialists and researchers can share life-saving data across different campuses instantly.
2. Specialty care providers with complex journeys
Specialized fields like oncology or fertility require highly specific patient touchpoints that standard EHRs cannot handle. A custom system allows you to build “branching logic” tailored to those specific medical journeys.
This ensures that a patient receives the right prep instructions for a complex procedure at exactly the right hour.
Real-world Example: Memorial Sloan Kettering Cancer Center builds tailored digital pathways to manage the intricate, long-term communication needs of cancer patients undergoing specialized treatments.
3. Digital-first healthcare platforms at scale
Startups and established tech firms that provide virtual-only care need systems that can handle millions of users simultaneously. Custom builds allow these companies to scale their infrastructure without paying “per-seat” licensing fees to third-party vendors. This approach provides the flexibility to pivot their service model as they grow.
Real-world Example: Hims & Hers Health has built a proprietary technology stack that automates the bridge between patient consultations and pharmacy fulfillment at a massive scale.
4. Enterprises integrating RPM and telehealth systems
Organizations using Remote Patient Monitoring (RPM) deal with a constant stream of data from wearable devices. A custom communication engine is needed to filter this data and only alert a doctor when a patient’s vitals show a dangerous trend.
This prevents staff from being overwhelmed by non-critical data pings.
Real-world Example: Dexcom integrates its continuous glucose monitoring data directly into healthcare ecosystems, requiring custom automated triggers to alert care teams of hypoglycemic events in real-time.
Investing in a custom build is a strategic move for any leader who views technology as a core asset rather than a utility. It ensures your infrastructure is built to support your specific business goals, not the limitations of a vendor’s roadmap.
Custom vs Built-In EHR Messaging: Real Difference
Several EHR platforms come with built-in messaging features. On paper, they seem sufficient. However, as organizations scale, these tools start to show clear limitations.
Built-in messaging is designed for basic communication within a single system. It works well for simple alerts or internal notes. But it lacks the flexibility required for complex workflows, multi-system coordination, and real-time automation.
Custom EHR communication systems take a different approach. Instead of treating messaging as a feature, they treat it as infrastructure. This allows enterprises to design communication flows around actual clinical and operational needs, not vendor constraints.
As a result, the choice rests on control, scalability, and long-term efficiency of the system rather than just its features.
Custom vs Built-In Messaging Comparison
| Factor | Built-In EHR Messaging | Custom EHR Communication System |
| Scope | Limited to internal EHR workflows | Designed for cross-system communication |
| Flexibility | Fixed workflows controlled by the vendor | Fully customizable workflows and rules |
| Integration | Basic integrations are often restricted | Deep integrations via APIs (FHIR, HL7) |
| Scalability | Struggles with multi-site operations | Built for enterprise-scale environments |
| Automation | Minimal automation capabilities | Advanced rule-based and AI-driven automation |
| Real-Time Communication | Often delayed or batch-based | Event-driven, real-time communication |
| Control | Vendor-dependent roadmap | Full ownership of the system and logic |
| Compliance | Standard compliance features | Custom compliance aligned to org needs |
| User Experience | Generic interface | Tailored for workflows and roles |
| Long-Term Cost | Lower upfront, higher limitations later | Higher upfront, better long-term ROI |
Built-in messaging may work for smaller setups, but it quickly becomes a bottleneck at scale. Custom communication systems give enterprises the control, flexibility, and integration depth needed to support real-world healthcare operations.
Step-by-Step: Build EHR Automation System
Building a sophisticated automation layer requires a blend of clinical insight and engineering precision. This process ensures that every automated interaction is as reliable and secure as a face-to-face consultation.
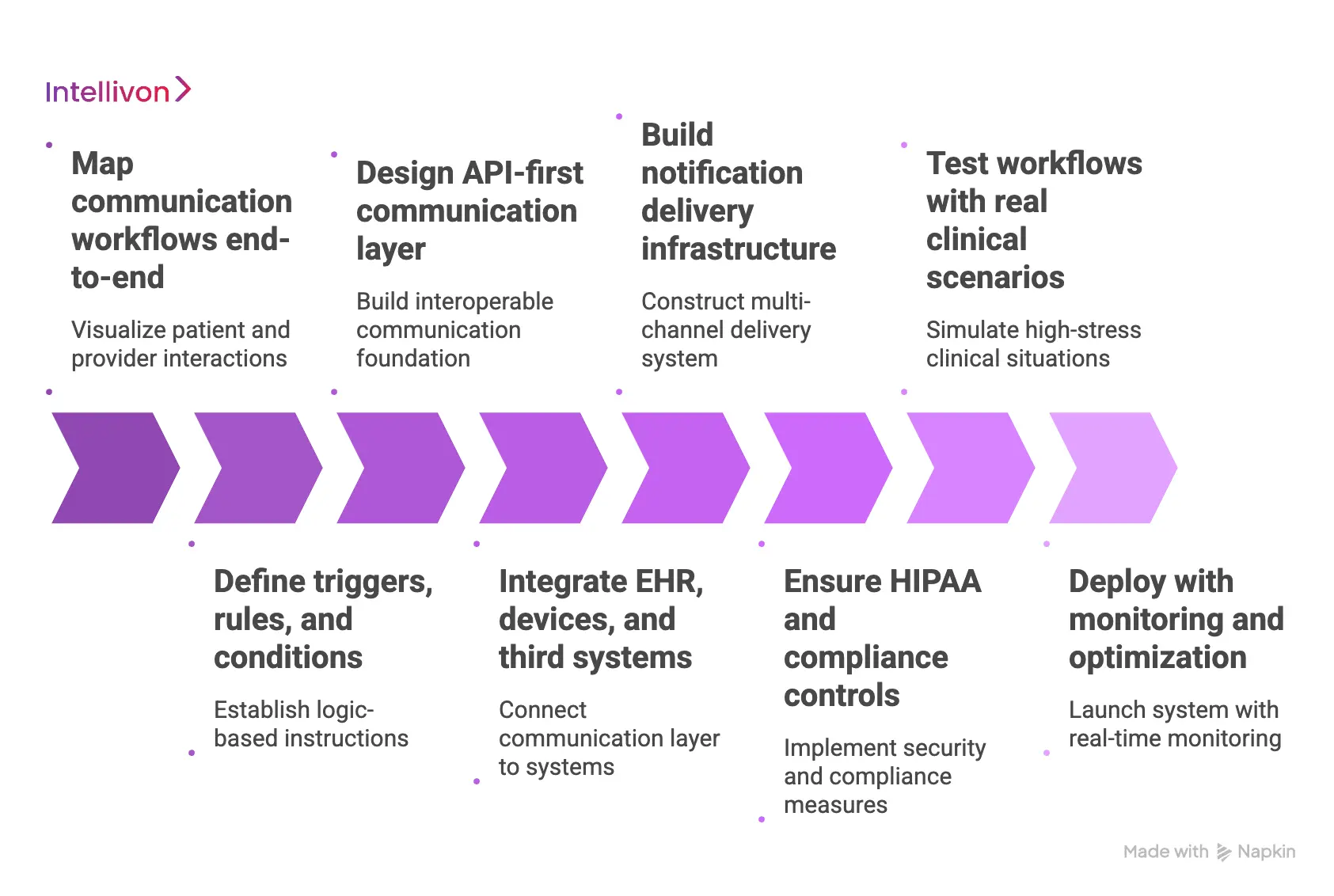
Step 1: Map communication workflows end-to-end
We begin by visualizing every touchpoint a patient or provider has with your system. This involves identifying where manual handoffs currently fail or slow down.
By mapping the “happy path” and potential outliers, we ensure the automation covers the entire patient lifecycle without gaps.
Step 2: Define triggers, rules, and conditions
The system needs clear instructions on when to act. We establish logic-based triggers, such as “If a lab result is >X and the patient is in Category Y, then notify Specialist Z.” These rules act as the brain of your communication engine, ensuring every message is contextually appropriate.
Step 3: Design API-first communication layer
Modern healthcare relies on interoperability. We build a robust API layer that allows your communication engine to “talk” to different databases and third-party apps seamlessly.
This foundation ensures that your system can scale and integrate with future technologies without requiring a total rewrite.
Step 4: Integrate EHR, devices, and third-party systems
Here, we connect the communication layer to your core EHR and peripheral devices like wearable monitors. Therefore, data flows in real-time from a patient’s blood pressure cuff directly into the automation engine.
This integration eliminates the need for manual data entry and reduces the risk of human error.
Step 5: Build notification delivery infrastructure
A message is only useful if it is received. We construct a multi-channel delivery system that supports secure SMS, encrypted email, and push notifications.
This infrastructure is designed for high deliverability and includes “failover” logic to try alternative channels if the first attempt fails.
Step 6: Ensure HIPAA and compliance controls
Security is baked into every line of code. We implement end-to-end encryption, strict access controls, and comprehensive logging to meet HIPAA and SOC2 standards.
This ensures that sensitive patient health information (PHI) is protected at rest and in transit, maintaining your organization’s integrity.
Step 7: Test workflows with real clinical scenarios
Before going live, we run the system through rigorous simulations. We test how the automation handles high-stress scenarios, such as a sudden influx of ER patients or a network outage. This phase confirms that the logic holds up under real-world clinical pressure.
Step 8: Deploy with monitoring and optimization
Deployment is just the beginning. We launch the system with advanced telemetry to monitor performance and user engagement in real-time. This allows for continuous refinement, ensuring the system evolves alongside your clinical needs and business goals.
Building a system of this caliber requires a partner who understands the high stakes of enterprise healthcare. At Intellivon, we specialize in delivering cutting-edge, AI-powered automation that turns these complex steps into a seamless reality for your organization. We engineer growth and clinical excellence and breathe life into your existing systems.
Architecture Behind EHR Communication Systems
The technical backbone of a high-performance EHR system must be both elastic and resilient. A modern architecture ensures that as your patient volume grows, your communication speed remains constant and your data remains secure.
1. API-first communication orchestration layer
An API-first approach treats every function as a modular service that can be easily updated or replaced. This orchestration layer acts as a central hub, managing how different parts of the system interact with each other.
Therefore, you can add a new telehealth vendor or a pharmacy partner without needing to reconfigure your entire core database.
2. Event-driven architecture for real-time updates
Unlike traditional systems that check for updates at set intervals, event-driven architecture reacts the moment a “trigger” occurs. When a nurse enters a vital sign into the EHR, an event is published instantly to the message bus.
This triggers the communication engine to evaluate if an alert is needed, reducing latency from minutes to milliseconds.
3. Integration with HL7 and FHIR standards
Interoperability depends on using industry-standard protocols like HL7 and FHIR. These frameworks provide a consistent data format for exchanging health information across different platforms.
By building on these standards, your system ensures that data from an outside lab is perfectly readable by your internal automation logic.
4. Cloud-native infrastructure for scalability
Cloud-native design allows your system to scale resources up or down based on real-time demand. During a seasonal flu spike, the infrastructure automatically allocates more computing power to handle increased message volumes.
This “pay-as-you-go” model ensures high availability while keeping operational costs optimized for your actual usage.
5. Data pipelines and message queue systems
Reliable communication requires robust data pipelines that prevent information loss during peak traffic. Message queues like RabbitMQ or Kafka hold outgoing notifications in a digital “waiting room” until the delivery service is ready to process them.
This ensures that even if a network goes down, no critical patient alert is ever deleted or forgotten.
This architectural rigor ensures that your system is not just a tool for today, but a scalable platform for the next decade. Building on this foundation allows your enterprise to innovate faster while maintaining a rock-solid technical environment.
Integrations Required for Full Automation
Achieving a fully automated ecosystem requires a “hub-and-spoke” integration strategy. By connecting your central communication engine to these external pillars, you eliminate the manual data silos that typically slow down enterprise healthcare operations.
1. EHR systems like Epic, Cerner, athenahealth
The primary Electronic Health Record (EHR) serves as the “source of truth” for all patient data. Integration with market leaders like Epic or Cerner involves building secure bridges that allow your automation engine to read and write data in real-time.
This ensures that any automated message sent to a patient is based on the most current clinical notes available.
2. Labs, pharmacies, and diagnostic systems
Automation loses its value if it stops at the hospital doors. By integrating directly with national lab chains and pharmacy networks, your system can trigger notifications the moment a prescription is ready or a test result is finalized.
This digital handshake speeds up the “time-to-treatment” and reduces the administrative burden on your nursing staff.
3. Patient apps and engagement platforms
To meet modern expectations, your system must deliver information where patients already spend their time. Integrating with mobile health apps and patient portals allows for rich, interactive communication beyond simple text.
Consequently, patients can view their charts, upload photos of symptoms, or confirm appointments within a single, secure interface.
4. Insurance and billing systems
Connecting your communication layer to clearinghouses and insurance providers streamlines the financial journey. Automated triggers can verify eligibility in seconds or notify a patient of their co-pay before they even arrive at the clinic.
This integration reduces claim denials and improves the overall transparency of healthcare costs for the end-user.
5. IoT devices and remote monitoring tools
The rise of “hospital-at-home” models makes IoT integration a necessity for 2026. Data from wearable heart monitors or smart scales flows directly into your automation logic.
If a device detects a concerning trend, the system can automatically alert the care team and send a “check-in” message to the patient simultaneously.
These integrations transform a fragmented collection of tools into a unified, intelligent network. When these systems talk to each other, your organization can provide a level of care that is both deeply personal and massively scalable.
Security and Compliance in Communication Systems
Maintaining the integrity of patient data is the cornerstone of patient trust. A secure communication architecture ensures that every automated alert or message meets the highest standards of privacy and legal protection.
1. HIPAA-compliant messaging architecture design
Designing for HIPAA requires more than just a secure server; it demands a system-wide approach to data handling. We architect the messaging layer to ensure that Protected Health Information (PHI) is never exposed in insecure environments. This includes:
- Decoupled Data Storage: Separating message metadata from the actual clinical content to reduce the “blast radius” of a potential breach.
- Secure Transport Layers: Utilizing TLS 1.3 for all data moving between the EHR and the communication engine.
- Automated Expiry: Setting time-to-live (TTL) parameters on sensitive notifications so they do not sit indefinitely on a recipient’s device.
2. End-to-end encryption for patient data
Encryption must be active at every stage of the data lifecycle to be truly effective. We implement AES-256 encryption for data at rest within your databases and end-to-end encryption for data in transit.
Therefore, even if a data packet is intercepted, the information remains unreadable to unauthorized parties. This standard is non-negotiable for protecting the enterprise from the catastrophic financial and reputational costs of a data leak.
3. Role-based access and audit logging
A robust system must strictly control who can see what and when. Role-Based Access Control (RBAC) ensures that a billing clerk cannot access clinical notes, while a specialist sees only what is relevant to their consultation.
- Granular Permissions: Customizing access levels based on specific job functions within the healthcare network.
- Immutable Audit Trails: Creating a permanent, time-stamped record of every person who accessed or sent a piece of patient data.
- Real-time Monitoring: Using automated tools to flag unusual access patterns, such as a user logging in from an unrecognized geographic location.
4. Consent management and data governance
Patients must have clear control over how and where they receive their health information. Our systems integrate dynamic consent management, allowing patients to opt-in or opt-out of specific communication channels instantly.
Consequently, your organization stays compliant with evolving privacy laws like the TCPA (Telephone Consumer Protection Act) while respecting the individual preferences of every patient in your care.
By embedding these security protocols into the very fabric of your automation, you protect your organization’s most valuable asset: its reputation. A secure system is a reliable system, providing the peace of mind necessary to scale your digital operations.
Cost to Build EHR Communication Automation System
The cost of building an EHR communication automation system depends on how deeply it connects with your existing workflows and systems. In most cases, enterprises are not building standalone tools. They are building a communication layer that sits across clinical, operational, and patient-facing systems.
At an early stage, organizations can start with a focused automation system. This typically covers high-impact workflows such as patient reminders, internal alerts, or care coordination. As complexity grows, the system expands to support multi-channel communication, real-time workflows, and deeper integrations.
For most organizations, the investment falls between $50,000 and $150,000, depending on scope, integrations, and automation depth.
Estimated Cost Breakdown
| Component | Starter System ($50K–$80K) | Growth System ($80K–$120K) | Advanced System ($120K–$150K) |
| Core Communication Engine | Basic rule-based workflows | Multi-step workflows | Advanced orchestration workflows |
| EHR Integration (FHIR/HL7) | 1 system integration | 2–3 systems integrated | Multi-system integration with sync |
| Notification Delivery System | SMS or email alerts | Multi-channel (SMS + email) | Real-time alerts with escalation |
| Workflow Automation Logic | Predefined triggers | Configurable workflows | Dynamic rule-based workflows |
| Patient Communication Layer | Appointment reminders | Engagement workflows | Personalized communication journeys |
| Care Team Communication | Internal alerts | Department coordination | Cross-team workflow communication |
| AI & Smart Routing | Not included | Basic prioritization | Smart routing and alert filtering |
| Dashboard & Monitoring | Basic logs | Workflow tracking dashboards | Real-time monitoring dashboards |
| Security & Compliance | HIPAA-ready basics | Role-based access control | Advanced audit logs and encryption |
| Infrastructure (Cloud/Backend) | Standard cloud setup | Scalable backend setup | Light event-driven architecture |
| Testing & QA | Basic testing | Workflow validation | Scenario-based testing |
| Deployment & Support | Initial deployment | Deployment + short support | Deployment + optimization support |
What Drives the Cost Up
- Integration Depth: The more systems you connect, the higher the complexity. Integrating EHRs, labs, billing platforms, and patient apps requires custom APIs and data mapping.
- Workflow Complexity: Simple reminders are easy to build. However, multi-step care coordination workflows across departments require more logic, testing, and refinement.
- Real-Time Capabilities: Systems that rely on instant alerts and event-driven workflows need stronger backend infrastructure and messaging systems.
- Compliance and Security: Healthcare systems must meet strict standards. HIPAA compliance, encryption, audit logs, and access controls all add to the development effort.
- Automation Intelligence: Adding smart routing, prioritization, or AI-driven alerts increases both system capability and cost.
Hidden Costs Enterprises Often Miss
- Data migration from legacy systems
- Staff training and onboarding
- Ongoing maintenance and upgrades (15–20% annually)
- Compliance audits and security updates
- Infrastructure scaling as usage grows
These costs shape the long-term investment, not just the initial build.
At this investment level, the goal is not to build a full enterprise platform from day one. The focus is to solve critical communication gaps with a scalable foundation that can evolve over time.
Common Mistakes Enterprises Make While Building
Building a custom communication engine is a high-stakes investment. Many organizations fail because they treat automation as a quick software patch rather than a fundamental shift in their digital infrastructure.
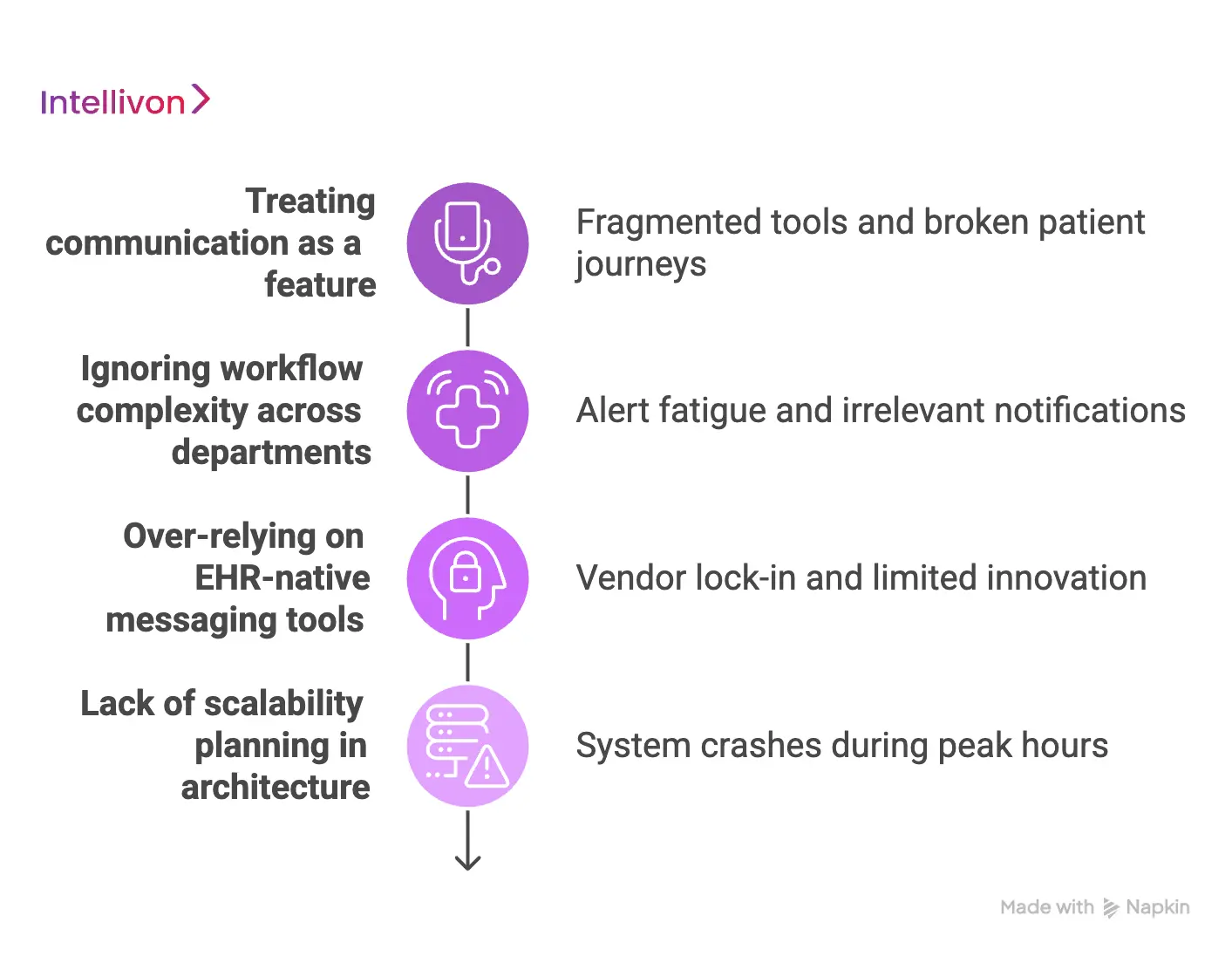
1. Treating communication as a feature
Many leaders mistakenly view automated messaging as a simple “add-on” to their existing EHR. When you treat communication as a minor feature, you end up with fragmented tools that don’t talk to each other. This leads to broken patient journeys and data gaps that frustrate both clinicians and patients.
How Intellivon Solves This: We approach communication as a core orchestration layer. Our architects build a centralized “brain” that manages every interaction across your entire enterprise, ensuring a unified and reliable experience.
2. Ignoring workflow complexity across departments
A message flow that works for a radiology department might be completely ineffective for an oncology clinic. Overlooking these departmental nuances creates “alert fatigue” for staff and irrelevant notifications for patients. Therefore, a one-size-fits-all approach often does more harm than good in a complex hospital network.
How Intellivon Solves This: We conduct deep-dive workflow audits before writing a single line of code. Our team builds “branching logic” into your system, allowing different departments to have custom communication rules while staying on the same platform.
3. Over-relying on EHR-native messaging tools
Standard EHRs are excellent databases, but their built-in messaging tools are often rigid and difficult to customize. Relying solely on these native features limits your ability to innovate or integrate with modern tools like remote monitoring devices. This creates a “vendor lock-in” that can stall your digital growth for years.
How Intellivon Solves This: We build “EHR-agnostic” layers that sit on top of your current system. This gives you the freedom to create advanced, custom workflows that your native EHR simply cannot support, while still keeping your data perfectly synced.
4. Lack of scalability planning in architecture
Enterprises often build systems that work for 1,000 patients but crash when they scale to 100,000. Using outdated server models or poorly designed data pipelines leads to system latency and message failures during peak hours. This lack of foresight can turn a successful pilot program into a technical nightmare.
How Intellivon Solves This: We utilize cloud-native, microservices-based architectures. This allows your system to scale horizontally and automatically, ensuring that whether you are sending ten messages or ten million, the performance remains lightning-fast.
Avoiding these common pitfalls requires a partner who looks beyond the code to the broader business strategy. At Intellivon, we ensure your automation is built to last, providing the technical resilience needed to support your enterprise’s long-term vision.
Conclusion
Building an automated EHR communication system is a strategic investment in operational resilience and patient trust. By moving beyond manual workflows, your enterprise can reduce administrative burnout while delivering personalized, real-time care at scale.
This digital transformation turns complex data into actionable insights, creating a competitive advantage in a value-based healthcare economy. Prioritizing a robust, secure, and scalable architecture ensures your organization remains a leader in clinical excellence and long-term growth.
Build EHR Communication System With Intellivon
At Intellivon, EHR communication automation systems are built as healthcare infrastructure, not as messaging features layered onto existing platforms. The focus is to create a unified communication layer that connects clinical workflows, operational systems, and patient interactions in real time.
Each system is designed around how your organization actually communicates. As a result, teams reduce manual effort, improve response time, and maintain consistency across departments.
Our approach combines API-first, cloud-native architecture with interoperability standards like HL7 and FHIR. This ensures seamless integration with EHRs, labs, pharmacies, insurers, and third-party systems without disrupting ongoing operations.
Why Intellivon for EHR Communication Automation
- Built as a Communication Layer, Not a Feature: We design systems that sit across your entire healthcare stack, enabling real-time coordination instead of isolated messaging.
- API-First, Workflow-Driven Architecture: Every communication flow is structured through configurable workflows, allowing flexibility as your operations evolve.
- Deep Integration Expertise: From EHRs to labs and billing systems, we ensure reliable, secure, and scalable integrations across all touchpoints.
- Designed for Scale and Compliance: Our systems are built to handle growing workloads while meeting strict healthcare security and compliance requirements.
Start Building Your Communication System
- Turn fragmented communication into structured workflows.
- Enable real-time coordination across teams and systems.
- Build a scalable, compliant communication layer that grows with your organization.
Talk to Intellivon’s experts to design your EHR communication automation system.
FAQs
Q1. What is an EHR communication automation system?
A1. An EHR communication automation system automates how information flows between patients, providers, and healthcare systems. It uses predefined workflows and triggers to send alerts, reminders, updates, and notifications in real time. Instead of relying on manual coordination, the system ensures the right message reaches the right person at the right time. This improves care delivery, reduces delays, and removes repetitive administrative work.
Q2. How long does it take to build this system?
A2. The development timeline depends on system complexity and integrations. A basic automation system can take 8 to 12 weeks to build. However, systems with multiple integrations, real-time workflows, and advanced automation typically take 3 to 6 months. Timelines increase further if the platform supports multiple facilities or complex care coordination workflows.
Q3. What integrations are required for automation?
A3. EHR communication automation systems rely on multiple integrations to function effectively. At a minimum, they connect with the core EHR platform using standards like FHIR or HL7. Beyond that, most systems integrate with labs, pharmacies, billing platforms, patient apps, and communication channels like SMS or email providers. Advanced setups may also include IoT devices, remote monitoring tools, and analytics systems.
Q4. How secure are automated communication systems
A4. These systems are built with strict security and compliance requirements. Most follow healthcare standards such as HIPAA and include encryption, role-based access control, and audit logging. In addition, communication data is protected both in transit and at rest. Properly designed systems also include consent management and monitoring mechanisms to ensure data privacy at every stage.
Q5. How much does it cost to build such systems
A5. The cost depends on the scope, integrations, and level of automation. For most organizations, building a focused communication automation system ranges between $50,000 and $150,000. Smaller systems cover basic workflows and limited integrations, while higher-end builds support real-time communication, multi-system orchestration, and advanced automation.