Healthcare clinics sometimes fail because the systems created to support the care that they provide were never designed for how they really operate. This is because standard EHR platforms seem promising during a demo, but quickly show their limitations. At the same time, the clinical workflows sometimes don’t match reality, and integrations tend to create more issues than they solve.
Deciding to build a custom EHR affects the business structure and workflow of a clinic positively. The difference between a platform that fits your workflows and one that forces you to change yours is significant. Thus, the impact that a custom EHR software has on a clinic can be seen through staff productivity, billing accuracy, patient retention, and ultimately profit.
We build enterprise-grade EHR systems from the ground up, architecting for HIPAA compliance, HL7 and FHIR interoperability, multi-specialty workflows, and the kind of clinical data infrastructure that scales without breaking. This blog draws from that experience and tells you how we build such software step-by-step.
Why Clinics Are Moving Beyond Legacy EHR Systems
Recently, we have been noticing a significant change in the way clinics are adopting new EHR systems. They are moving away from outdated EHR systems because they slow teams down, create security risks, and don’t support modern care needs. Today, nearly 60% of healthcare leaders plan to upgrade their EHR systems in 2026 to escape these problems.
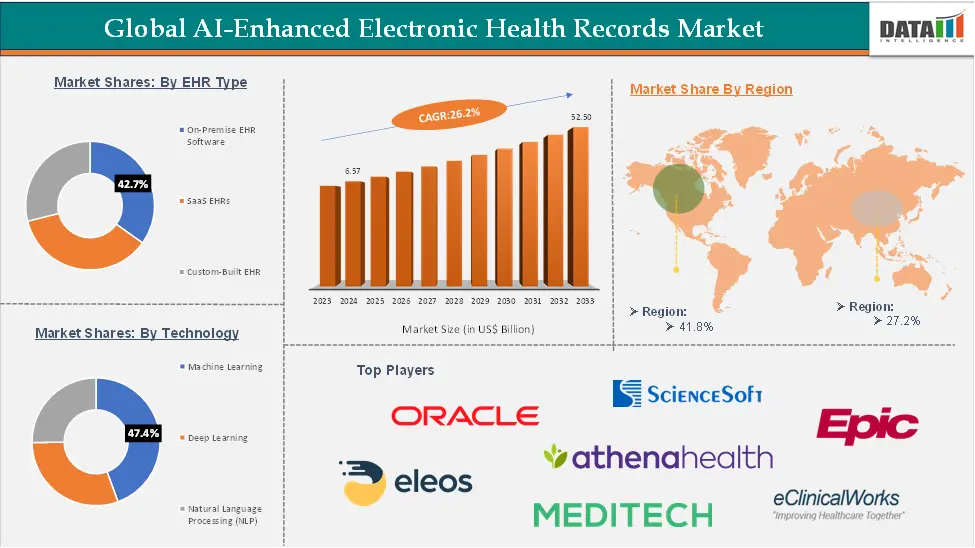
This shift comes from growing cyber threats, stricter regulations, and the level of accuracy patients expect from healthcare enterprises today. Simply put, older systems can’t keep up with how clinics need to operate today. In fact, the global AI-powered EHR systems market reached USD 32.44-33.99 billion in 2025-2026 and is projected to grow to USD 43-52.60 billion by 2030-2034. This is per an extensive report prepared by Data Intelligence.
1. Rigid Systems Slows Workflows
Traditional EHRs often force doctors to follow a linear, inflexible path for every patient. This environment leads to burnout and reduces the time spent on actual care. In a custom environment, the interface adapts to the specific specialty of the clinic.
Therefore, a cardiologist sees different data points than a pediatrician. By removing unnecessary fields, providers can complete charts in half the time. This efficiency is no longer a luxury but a requirement for high-volume practices.
2. Incorrect Data Impacts Care
Legacy systems often struggle to communicate with laboratory software or wearable health devices. When patient data stays in silos, the medical team loses the full picture of a person’s health.
However, a custom EHR integrates these disparate sources into a single, unified view. This connectivity ensures that every specialist has access to the same updated records.
Accurate data leads to fewer medical errors and more precise treatment plans. In 2026, the ability to sync data instantly across platforms is a competitive necessity if you want to stay on top of the game.
3. Billing Inefficiencies Powers Revenue Loss
Manual coding and outdated billing modules often lead to high rejection rates. Legacy software does not update its logic to match changing insurance regulations or complex tax codes. This is a problem.
However, adding a custom billing engine allows clinics to automate the verification of insurance eligibility instantly. In addition, AI-powered scrubbers can check for coding errors before a claim is even submitted.
This proactive approach ensures a steadier cash flow and reduces the burden on administrative staff. Reducing the “days in accounts receivable” directly impacts the bottom line.
4. Legacy Systems Cannot Scale
As a clinic grows, an old system becomes a roadblock to an eventual expansion. This is because these platforms are often hosted on local servers that lack the elasticity of the modern cloud.
However, custom EHR software development allows for modular growth. You can add new features, like telehealth or remote monitoring, without rebuilding the entire foundation.
This insane scalability ensures that the technology grows alongside your business goals at the same speed. Investing in a flexible architecture protects your capital from future technical debt.
Moving beyond legacy systems is a strategic pivot toward operational excellence and sustainable growth. By embracing customized, AI-ready platforms, clinics can finally prioritize patient outcomes over administrative paperwork.
What a Custom EHR Platform Solves for Clinics
Off-the-shelf EHR tools are built for the average clinic. However, most clinics operating at scale are anything but average.
They carry specialty-specific workflows, multi-location data environments, and compliance obligations that generic platforms were never designed to handle cleanly. Custom EHR development addresses the gaps that packaged software leaves open.
1. Unified Patient Records Across Care Workflows
When patient data lives across disconnected systems, care quality suffers. Physicians make decisions without full context, coordinators duplicate data entry, and referrals create information gaps.
A custom EHR centralizes records across departments, specialties, and locations, giving every authorized user a single, accurate view of the patient at any point in the care journey.
2. Automation from Intake to Billing Lifecycle
Manual processes are expensive. From patient intake forms to insurance verification, prior authorizations, and claim submission, every manual touchpoint adds time and error risk.
A well-built EHR automates this entire lifecycle. Therefore, staff spend less time on administration and more time on work that actually requires human judgment.
3. Real-Time Insights for Clinical Decisions
Data that arrives too late has limited value. Custom EHR platforms surface clinical insights at the point of care, flagging drug interactions, surfacing patient history, and supporting diagnosis with structured data.
In addition, leadership gets operational dashboards that reflect what is happening across the organization right now.
4. Built-In Compliance and Data Governance
Compliance cannot be bolted on after the fact. HIPAA, HITECH, and state-level data regulations require controls that are embedded into how the system handles, stores, and transmits data. A custom build lets you define those controls by design, and not by patch.
A custom EHR platform does not just fix what is broken. Instead, it builds the operational foundation that serious healthcare businesses grow on.
Features That Make Custom EHR Worth Building
Building a custom platform is about more than just digital filing. It is about creating a tool that actually understands how your clinic breathes. In 2026, smart features are the bridge between a chaotic waiting room and a streamlined clinical operation.
Investors look for systems that reduce human error while maximizing the number of patients seen per day. These custom modules transform a passive database into an active revenue-generating engine.
1. Smart Scheduling and Patient Flow Automation
Old-school calendars often lead to double bookings or empty slots that drain potential revenue. A smart scheduling system uses historical data to predict “no-shows” and optimizes the daily agenda. Therefore, the staff spends less time on the phone and more time assisting patients.
In addition, automated reminders can be sent via text or email to confirm appointments. This flow ensures that the clinic stays busy without feeling overwhelmed. A smooth front-desk experience is often the first step in building long-term patient loyalty.
2. Digital Intake and Medical History Tracking
Paper forms are a relic of the past that create unnecessary data entry for your team. Custom EHR software development allows patients to complete their intake forms on their own devices before they arrive.
This data flows directly into their medical record without a staff member typing a single word. However, the true value lies in how this history is tracked over time. Dynamic charts highlight trends in vitals or lab results at a glance. At the same time, clearer data helps doctors make faster, more confident decisions during a consultation.
3. E-Prescriptions and Lab System Integrations
Waiting for a faxed lab result or a pharmacy confirmation is a major bottleneck in modern care. A custom EHR connects directly to national pharmacy databases and local diagnostic laboratories.
In addition, doctors can send prescriptions with a single click, reducing the risk of manual errors. This integration ensures that the patient’s record is updated the moment a lab result is ready.
Real-time updates mean faster treatments and a much better experience for the patient. Additionally, strategic connectivity is what separates an elite clinic from a struggling one.
4. Automated Billing and Revenue Cycle Systems
Revenue leakage often happens because of small coding mistakes or missed deadlines in the billing cycle. An automated billing system acts as a 24/7 auditor for your clinic’s finances. It checks for insurance eligibility automatically and flags potential issues before they become denials.
Furthermore, a custom system can offer patients easy online payment options directly through their portal. This transparency speeds up the collection process and improves the clinic’s overall cash flow. Reliable revenue cycles allow leaders to focus on scaling rather than chasing payments.
5. Role-based Dashboards for Clinical Teams
A surgeon, a nurse, and an accountant all need different information to do their jobs effectively. Custom dashboards ensure that every user sees exactly what they need without any distracting clutter.
For example, a nurse might see a list of upcoming vitals, while a manager sees a chart of daily revenue. This focused view reduces “alert fatigue” and helps staff stay productive. In addition, it enhances security by limiting sensitive data access based on specific job roles. Customization ensures the software fits the person, not the other way around.
Investing in these targeted features turns a standard software project into a high-performance business asset. These tools do not just store data; they actively drive the clinic toward higher efficiency and better care.
Inside an AI-Driven EHR Platform Architecture
Building a modern EHR is about creating a living nervous system for a clinic. In 2026, high-performance architecture must handle massive data loads. However, it must also provide instant, actionable insights. Investors need a “future-proof” foundation that adapts as technology evolves.
A well-designed technical stack ensures the platform remains fast and secure. Therefore, this architecture supports both enterprise use and strict compliance.
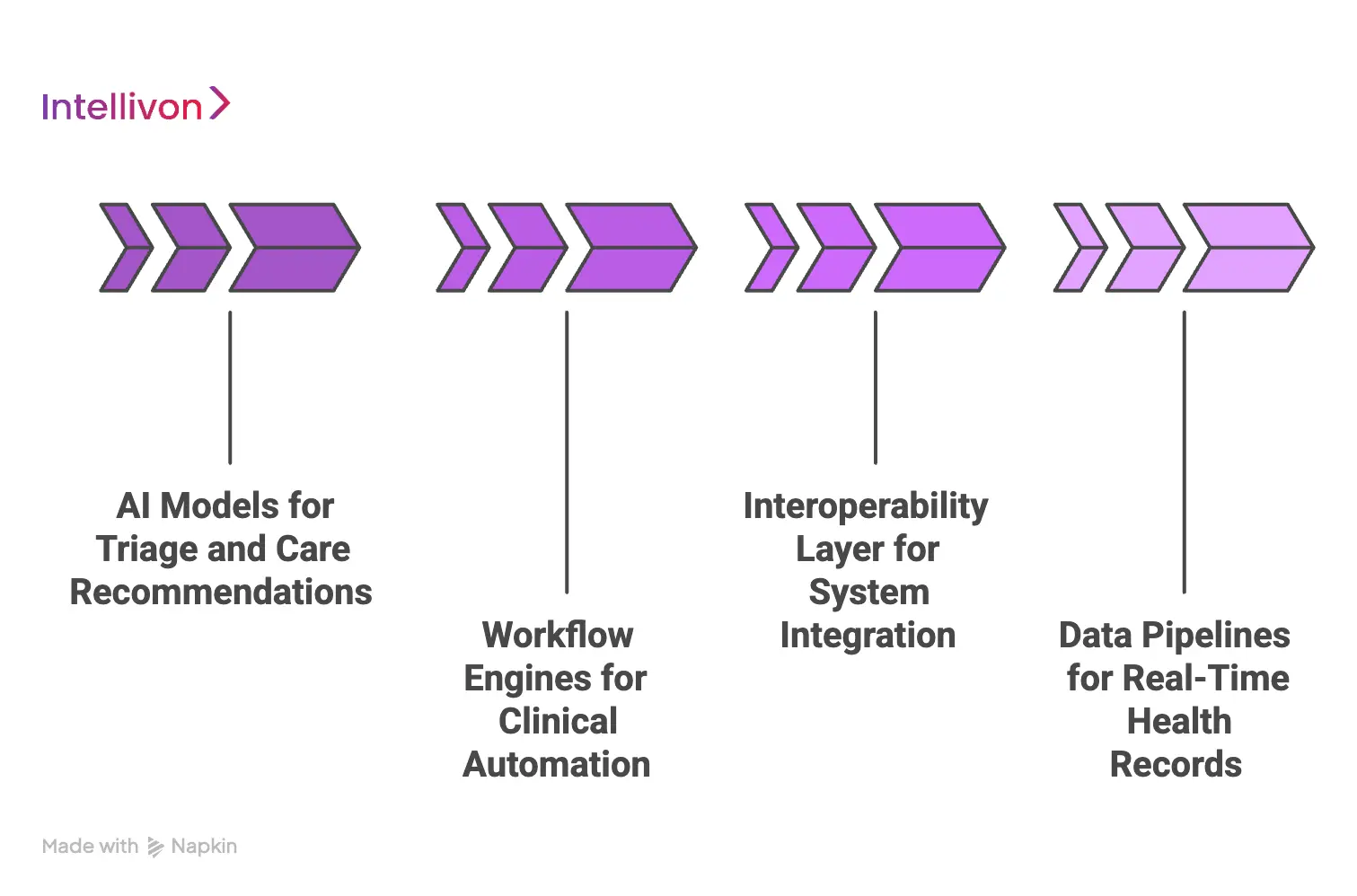
1. AI Models for Triage and Care Recommendations
The intelligence layer acts as a digital co-pilot for the medical team. Instead of just storing symptoms, the system analyzes them against vast databases.
- Predictive Triage: Algorithms rank patient urgency based on digital intake data.
- Decision Support: The system flags drug interactions or missed screenings in real-time.
- Risk Scoring: AI identifies high-risk patients who need proactive follow-up care. Therefore, the clinic can allocate resources where they are needed most. This proactive stance significantly improves patient outcomes. In addition, it reduces legal liability for the practice.
2. Workflow Engines for Clinical Automation
The workflow engine is the “brain” that moves a patient through their journey. It eliminates the need for staff to remember every administrative step.
- Automated Task Routing: When a doctor signs an order, the system pings the technician.
- Status Tracking: The engine monitors how long a patient waits in each stage.
- Trigger-Based Alerts: If a lab result is critical, the system pings the provider. Furthermore, these engines ensure that no patient falls through the cracks. Automation turns a complex clinical process into a repeatable service. Thus, it maximizes daily revenue.
3. Interoperability Layer for System Integration
A clinic does not exist in a vacuum. It must talk to pharmacies, insurance carriers, and other hospitals. The interoperability layer serves as a “universal translator” for these different languages.
By using FHIR standards, the EHR can securely exchange data. This connectivity is vital for maintaining a complete record of a patient’s health. However, it also opens doors for faster insurance authorizations. Strategic integration is what makes your platform essential.
4. Data Pipelines for Real-Time Health Records
Data must flow like water, clean, constant, and accessible. Modern data pipelines ensure information from wearables reaches the chart instantly.
- Stream Processing: Data is validated as it moves through the system.
- Secure Storage: High-level encryption protects sensitive health information at every stage.
- Instant Availability: Doctors never have to wait for a “sync” to see vitals. Reliable pipelines prevent data lag. Consequently, a robust data strategy ensures the platform remains responsive as the clinic grows.
This architectural approach transforms a software tool into a scalable enterprise asset. By focusing on these core layers, you build a system that is technically superior.
HL7 and FHIR Integration in EHR Systems
HL7 and FHIR are the two primary interoperability standards used in EHR systems. At the same time, HL7 enables structured data exchange between legacy healthcare systems. FHIR uses modern REST-based APIs to allow real-time, scalable data sharing across platforms, devices, and care settings.
1. Why Interoperability Is Critical for Clinics
Disconnected systems create direct clinical risk. When a referring physician cannot access imaging history, care quality drops. When billing cannot read discharge data, revenue cycles stall. Interoperability closes these gaps.
Therefore, the right data reaches the right person at the right moment, across departments, facilities, and external providers.
2. HL7 Integration for Legacy Healthcare Systems
Many established clinics still run infrastructure built on HL7 v2 messaging. Replacing these systems entirely is rarely practical or cost-effective.
However, a well-architected custom EHR builds HL7 integration layers that allow legacy systems to exchange structured data cleanly. This approach protects existing investments while modernizing data flow where it matters most.
3. FHIR APIs for Real-Time Data Exchange
FHIR represents the current direction of healthcare interoperability. Its REST-based architecture allows applications to request and receive patient data in real time.
In addition, FHIR’s modular resource structure makes scaling integrations significantly easier as your platform grows. Mobile apps, patient portals, payer systems, and clinical tools all connect more cleanly through FHIR.
4. Building a Connected Healthcare Ecosystem
Interoperability is the foundation that makes every other feature more valuable. When your EHR connects cleanly with labs, pharmacies, imaging centers, and payer networks, the entire organization operates faster and smarter.
Intellivon designs these integration architectures with long-term scalability in mind. Therefore, adding a new data source never requires rebuilding what already works.
Interoperability done right separates a functional EHR from one that supports genuine enterprise-scale operations. Without it, even the most capable platform becomes an island.
Compliance and Security in EHR Software
In the healthcare sector, data security is not just a technical feature. It is the literal foundation of your business reputation. In 2026, a single data breach can cost a clinic millions in fines and lost trust. Therefore, investors must prioritize a “security-first” architecture from the very first line of code.
High-level compliance ensures that your platform is ready for enterprise-scale adoption. A secure system protects the patient, the provider, and the stakeholder simultaneously.
1. HIPAA compliance for patient data security
Operating in the US healthcare market requires strict adherence to HIPAA regulations. This framework ensures that Protected Health Information (PHI) remains confidential and available.
- Technical Safeguards: Implementing automatic log-offs and unique user IDs.
- Physical Safeguards: Ensuring that servers and data centers meet elite security standards.
- Administrative Actions: Developing clear policies for how staff handle sensitive data.
Therefore, compliance is a continuous process, not a one-time checkbox. It serves as a vital shield against legal and financial risks.
2. Role-based access and audit logging systems
Not every employee needs access to every piece of patient information. Role-based access control (RBAC) ensures that a receptionist only sees scheduling data, while a doctor sees medical charts.
- Granular Permissions: Customizing access levels based on specific job functions.
- Detailed Audit Logs: Tracking every time a file is viewed, edited, or shared.
- Real-time Monitoring: Flagging suspicious activity, such as unauthorized login attempts.
In addition, audit logs provide a clear “paper trail” for regulatory inspections. This transparency builds a culture of accountability within the clinical team.
3. Encryption and secure data storage practices
Data must be unreadable to unauthorized eyes, whether it is sitting on a server or moving across the web. Modern encryption standards act as a final line of defense against cyberattacks.
- Data at Rest: Using AES-256 encryption to protect stored records.
- Data in Transit: Utilizing TLS 1.3 for secure communication between devices.
- Key Management: Storing encryption keys in hardware-backed security modules.
Furthermore, frequent backups ensure that data can be recovered quickly in an emergency. Secure storage is the bedrock of a resilient healthcare platform.
4. Managing sensitive health data at scale
As your clinic grows, the volume of data grows exponentially. Managing this “Big Data” requires a strategy that balances speed with extreme security.
- Database Sharding: Breaking data into smaller, manageable pieces for faster access.
- Anonymization: Removing personal identifiers for research or administrative analytics.
- Cloud Scalability: Using secure, healthcare-compliant cloud providers to handle traffic spikes.
Consequently, a scalable data strategy prevents system slowdowns during peak hours. It ensures the platform remains reliable as you expand to multiple locations.
A robust security posture turns a potential liability into a major competitive advantage. By focusing on these core protections, you build a product that the medical community can trust.
Technology Stack for Custom EHR Platforms
The technology decisions made at the start of an EHR build define how the platform performs years later. Many organizations launch on a stack that handles the current load but buckles under growth.
Therefore, choosing the right architecture is a long-term business decision. It needs to support scale, security, compliance, and integration all at once.
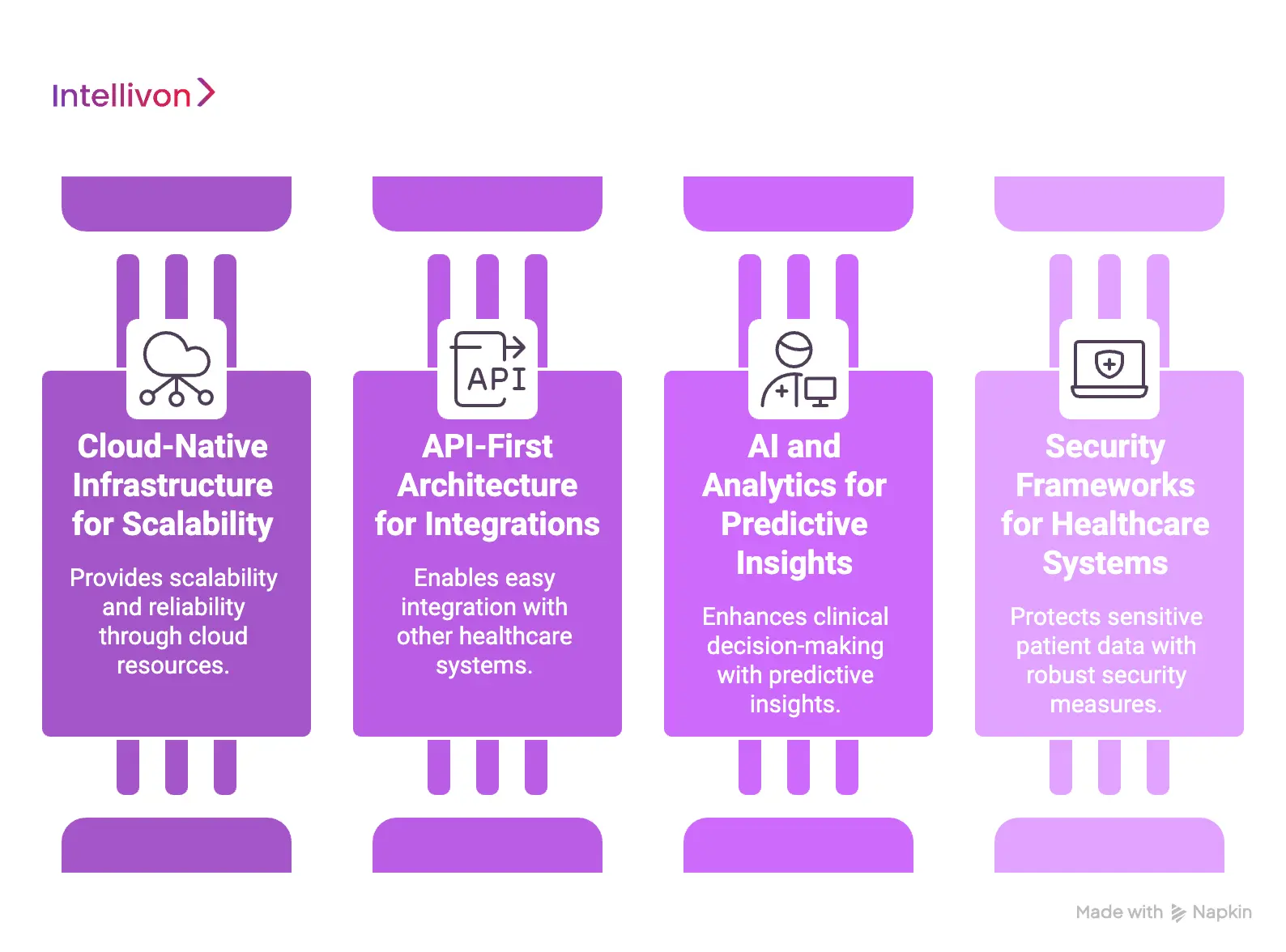
1. Cloud-Native Infrastructure for Scalability
Cloud-native architecture gives EHR platforms the flexibility that on-premise systems cannot match. Resources scale up during peak clinical hours and down when demand drops. In addition, multi-region deployment ensures uptime even when individual nodes fail.
Platforms built on AWS, Azure, or Google Cloud Healthcare API also carry built-in compliance tooling.
Key advantages of cloud-native EHR infrastructure:
- Elastic scaling without hardware procurement cycles
- Built-in disaster recovery and automated failover
- Reduced infrastructure management burden on internal teams
- Faster deployment of updates across multiple locations
2. API-First Architecture for Integrations
An API-first approach means every core EHR function is accessible through a well-defined interface. Therefore, connecting a new lab system or telehealth tool does not require custom development each time. Instead, it requires a clean API call.
This reduces integration costs significantly over time. In addition, it future-proofs the platform as new tools plug in without disrupting existing workflows.
3. AI and Analytics for Predictive Insights
AI is no longer an advanced feature in healthcare software. It is rapidly becoming a baseline expectation. A well-built EHR embeds AI at the workflow level, surfacing drug interaction alerts, predicting readmission risk, and flagging documentation gaps.
However, AI value depends entirely on data quality. Therefore, we build the underlying data architecture first, ensuring models operate on clean, structured inputs.
Practical AI applications in custom EHR platforms:
- Predictive risk scoring for high-acuity patients
- Automated clinical documentation through NLP
- Revenue cycle anomaly detection
- Population health trend analysis across patient cohorts
4. Security Frameworks for Healthcare Systems
Healthcare data is among the most targeted in any industry. A single breach carries financial penalties, reputational damage, and years of operational disruption.
Therefore, security cannot be added after development. It must be designed into the system from the start.
A production-grade EHR security framework includes:
- End-to-end encryption for data at rest and in transit
- Role-based access controls tied to clinical functions
- Audit logging for every data access and modification event
- Automated vulnerability scanning and penetration testing protocols
- Multi-factor authentication across all user entry points
The right technology stack determines how far and how fast the platform can grow without accumulating technical debt that demands a full rebuild.
Custom vs Off-the-Shelf EHR for Clinics
Clinics often start with off-the-shelf EHR systems because they are quick to set up and require lower upfront investment. However, as operations grow, these systems begin to show limitations.
As a result, many clinics start evaluating custom EHR platforms that align better with their workflows, integrations, and long-term goals.
To better understand the difference, here’s a quick comparison of both approaches:
| Factor | Off-the-Shelf EHR | Custom EHR |
| Setup Time | Quick to deploy | Requires development time |
| Initial Cost | Lower upfront cost | Higher initial investment |
| Customization | Limited to templates | Fully tailored to workflows |
| Workflow Fit | Clinics adapt to the system | System adapts to the clinic |
| Integrations | Predefined, limited | Fully flexible integrations |
| Scalability | Limited as the clinic grows | Built for long-term scaling |
| Ownership | Vendor-controlled | Fully owned by the clinic |
| Compliance Control | Standard features | Custom governance controls |
1. Flexibility and workflow customization
Off-the-shelf EHR systems follow fixed workflows. Clinics often need to adjust their processes to match the software, which can slow down care delivery.
In contrast, custom EHR platforms are built around real clinical workflows. This allows care teams to operate more efficiently, with fewer manual steps and better coordination.
2. Integration and interoperability limitations
Most off-the-shelf systems support only predefined integrations. Connecting with labs, pharmacies, billing tools, or third-party platforms can become restrictive over time. On the other hand, custom EHR platforms are designed for interoperability from the start.
They support standards like HL7 and FHIR, enabling seamless data exchange across systems.
3. Long-term cost vs operational efficiency
Off-the-shelf EHR solutions are easier to adopt initially. However, clinics often face hidden costs due to inefficiencies, workarounds, and additional tools.
Custom EHR platforms require a higher upfront investment, but they reduce operational friction. Over time, this leads to better efficiency, fewer errors, and improved financial performance.
4. Scalability for growing clinic networks
As clinics expand to multiple locations or handle higher patient volumes, off-the-shelf systems may struggle to keep up. Performance limitations and rigid structures can slow growth. In comparison, custom EHR platforms are built to scale.
They support complex workflows, larger data volumes, and multi-location operations without compromising performance.
When a custom EHR becomes the better choice
Custom EHR platforms become a practical choice when clinics reach a certain level of complexity.
This includes multi-location operations, high patient volumes, and the need for deep integrations. It also applies to clinics operating under strict compliance requirements or planning long-term expansion.
In the early stages, off-the-shelf systems can work well. However, as clinics grow, these systems often create limitations. Custom EHR platforms move beyond basic software and become core clinical infrastructure. Therefore, clinics gain the control, flexibility, and scalability needed to support long-term growth.
How We Build Custom EHR Platforms For Enterprises
Building a premium EHR requires more than just coding skills. It requires a deep understanding of clinical logic and high-level data security.
At Intellivon, we specialize in creating elite, AI-powered solutions for large-scale healthcare enterprises. Our process focuses on reducing technical debt while maximizing long-term ROI for investors.
We build scalable business assets that evolve with the medical industry. Therefore, our roadmap is designed to move from concept to clinic with precision.
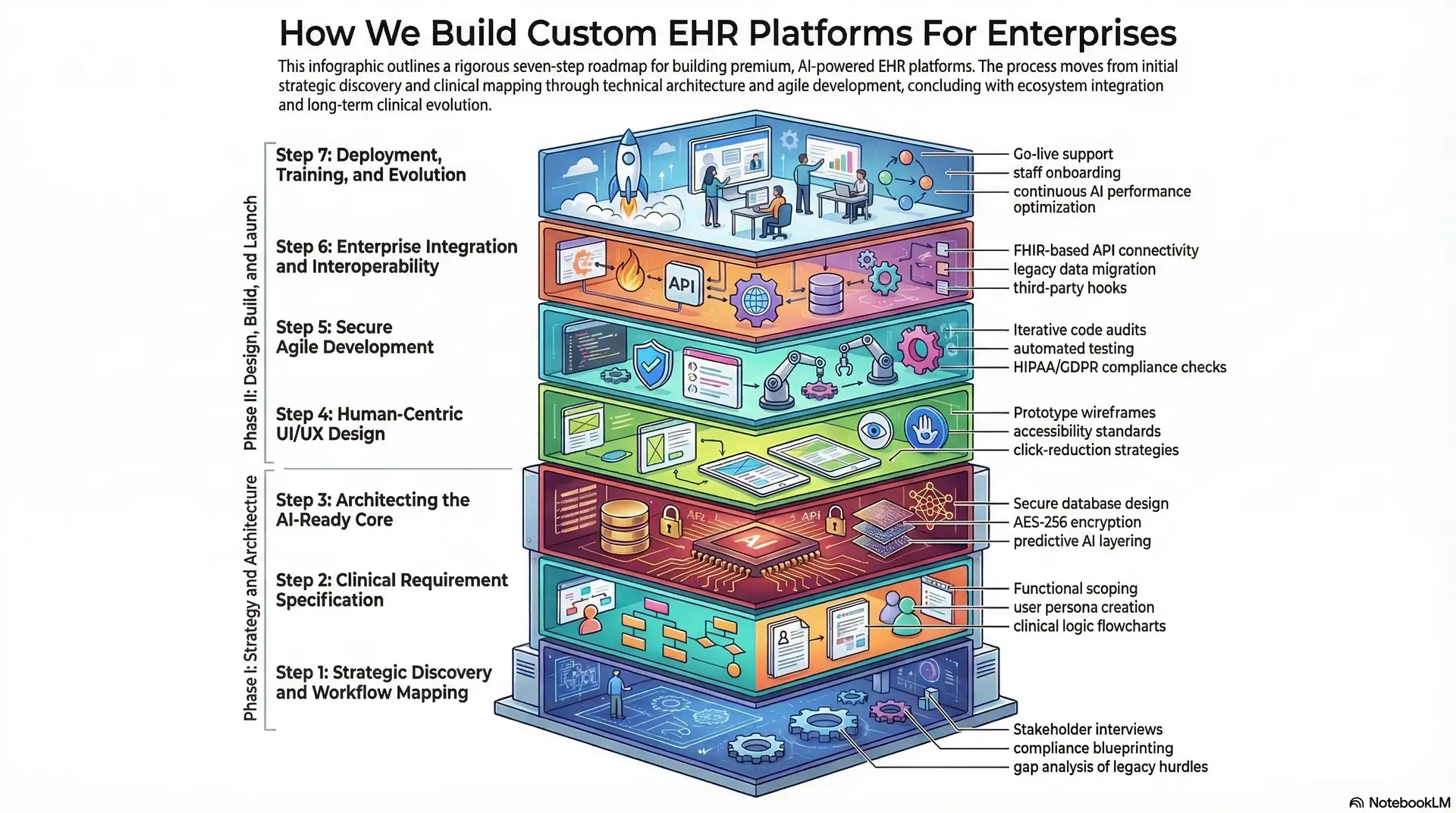
Step 1: Strategic Discovery and Workflow Mapping
We begin by analyzing the unique operational hurdles of your enterprise. Every clinic has a specific “pulse” that generic software often ignores. Our consultants dive deep into your current daily routines to find hidden inefficiencies.
- Stakeholder Interviews: We speak with clinicians and administrators to identify true pain points.
- Compliance Blueprinting: Mapping out the specific regulatory requirements for your target market.
- Gap Analysis: Comparing your current legacy hurdles against modern, AI-driven possibilities. Therefore, the foundation of your project is rooted in real-world utility. This phase ensures that the final product solves actual business problems.
Step 2: Clinical Requirement Specification
Once we understand the workflow, we translate those needs into technical requirements. This step ensures that the development team and the medical staff are on the same page. We document every data field, user role, and integration point required for success.
- Functional Scoping: Defining exactly what the software must do to support patient care.
- User Persona Creation: Designing unique interfaces for doctors, nurses, and billing specialists.
- Logic Flowcharts: Visualizing how data moves from a patient’s check-in to their final discharge. In addition, this clarity prevents “feature creep” that can bloat budgets. We focus on the high-value features that drive immediate clinical impact.
Step 3: Architecting the AI-Ready Core
Once the strategy is clear, our engineers build a robust and secure technical foundation. We prioritize a “decoupled” architecture that allows for modular growth over time. This means you can add new features without breaking the existing system.
- Database Design: Creating high-performance schemas that handle massive patient loads.
- Security Integration: Implementing AES-256 encryption and Zero Trust access protocols.
- AI Layering: Building the hooks for predictive triage and automated billing engines. Furthermore, we ensure the system is ready for massive data throughput. A strong core prevents future performance bottlenecks as your clinic expands.
Step 4: Human-Centric UI/UX Design
Healthcare software is notorious for being difficult to use. We change that by designing interfaces that prioritize speed and reduce cognitive load for providers. Our goal is to make documentation feel natural rather than a chore.
- Prototype Wireframes: Creating interactive models so you can feel the software flow early.
- Accessibility Standards: Ensuring the platform is easy to navigate on tablets and desktops.
- Click-Reduction Strategy: Minimizing the steps required to complete common clinical tasks. Therefore, your staff spends less time staring at screens and more time with patients. A great design is the secret to high software adoption rates.
Step 5: Secure Agile Development
Our development team works in short sprints to build the platform piece by piece. This “Agile” approach allows us to show you progress every few weeks. We maintain a constant feedback loop to ensure the build stays aligned with your vision.
- Code Audits: Performing regular checks to ensure the software is clean and secure.
- Automated Testing: Using scripts to find and fix bugs before they reach the user.
- Compliance Checks: Verifying that every new feature meets HIPAA or GDPR standards. In addition, this iterative process allows us to pivot quickly if clinical needs change. We build with flexibility in mind to protect your long-term investment.
Step 6: Enterprise Integration and Interoperability
A clinic does not exist in a vacuum. It must talk to pharmacies, labs, and insurance carriers seamlessly. We ensure your platform speaks fluently to the entire healthcare ecosystem using modern standards.
- API Connectivity: Setting up secure FHIR-based links for instant data exchange.
- Legacy Data Migration: Moving your old patient records into the new system without data loss.
- Third-Party Hooks: Integrating with payment gateways, telehealth tools, and wearable devices. Consequently, your EHR becomes the central hub of your medical operations. This connectivity is what makes your platform an essential enterprise asset.
Step 7: Deployment, Training, and Evolution
The final step is moving the software into the live clinical environment. We provide comprehensive onboarding to ensure your team feels confident using the new tools. However, our partnership does not end at the launch.
- Go-Live Support: Having our experts on standby during the first week of operation.
- Staff Onboarding: Providing clear manuals and video training for all user roles.
- Continuous Optimization: Monitoring performance and adding new AI features as needed. Strategic support ensures that your launch is smooth, secure, and ready to generate revenue. At Intellivon, we stay by your side to ensure long-term operational success.
Our seven-step approach turns a complex development journey into a predictable business victory. By partnering with experts, you ensure your investment delivers a high-performance clinical tool.
Cost to Build Custom EHR Software for Clinics
At Intellivon, custom EHR platforms are built as clinical infrastructure, not as software layered onto fragmented systems. The objective is to create a unified platform that manages patient data, workflows, and integrations across the entire care lifecycle.
However, building a reliable EHR system requires more than feature development. It involves designing secure data architectures, enabling interoperability with healthcare systems, and ensuring compliance with regulatory standards.
As a result, clinics gain a scalable platform that improves efficiency, reduces errors, and supports long-term growth.
Estimated Phase-Wise Cost Breakdown
| Phase | Description | Estimated Cost Range (USD) |
| Discovery & Workflow Mapping | Define clinical workflows, data flows, and system requirements | $8,000 – $15,000 |
| UI/UX Design | Design intuitive interfaces for doctors, staff, and admin teams | $6,000 – $12,000 |
| Backend Development | Build core EHR logic, data models, and APIs | $20,000 – $40,000 |
| Integrations (HL7, FHIR, Labs, Billing) | Connect external healthcare and financial systems | $10,000 – $25,000 |
| AI & Automation Modules | Implement scheduling, decision support, and analytics | $8,000 – $20,000 |
| Compliance & Security Layer | HIPAA compliance, encryption, and audit systems | $5,000 – $15,000 |
| Testing & Deployment | QA, performance testing, and production rollout | $5,000 – $10,000 |
Total Estimated Cost Range
For most clinics, the cost to build a custom EHR platform typically ranges between:
$60,000 – $150,000
The final cost depends on system complexity, number of integrations, and scalability requirements.
Key Factors That Affect EHR Development Cost
- Feature complexity: Advanced modules like AI-driven workflows or analytics increase development scope
- Integration requirements: Connecting with labs, pharmacies, and billing systems adds cost
- Compliance needs: Security, encryption, and regulatory requirements impact architecture design
- Scalability: Multi-location or high-volume systems require stronger infrastructure
- Customization level: Fully tailored workflows require a deeper development effort
Cost vs Value for Clinics
While custom EHR systems require higher upfront investment, they reduce long-term inefficiencies caused by rigid systems. Clinics benefit from streamlined workflows, fewer errors, and better control over operations.
As a result, custom EHR platforms shift from being a cost center to becoming a core operational asset that supports growth, compliance, and patient care outcomes.
Connect with Intellivon experts to get a tailored cost breakdown based on your clinic’s workflows, integrations, and scale.
Conclusion
Investing in custom EHR software is a strategic pivot toward long-term operational excellence. By moving beyond rigid legacy systems, clinics can finally prioritize patient outcomes over administrative burdens. A tailored, AI-ready platform ensures your medical enterprise remains scalable and secure.
This transition minimizes technical debt while maximizing clinical efficiency. Therefore, choosing a specialized development approach is the logical next step for growth-focused healthcare leaders seeking sustainable market advantages.
Launch a Custom EHR Platform With Intellivon
At Intellivon, custom EHR platforms are engineered as enterprise clinical infrastructure, not as software layered onto disconnected systems. The goal is to create a unified platform that manages patient data, automates workflows, and integrates seamlessly across the healthcare ecosystem.
Each solution is designed to support the full patient lifecycle, from smart scheduling and digital intake to clinical decision support and automated billing. As a result, clinics gain real-time visibility, reduce administrative burden, and deliver faster, more accurate care.
Our approach focuses on AI-first, API-driven architectures combined with interoperability standards like HL7 and FHIR. This ensures seamless integration with labs, pharmacies, billing systems, and existing healthcare infrastructure, without disrupting ongoing operations.
Why Partner With Intellivon?
- Clinical Infrastructure, Not Just Software: Platforms are built to support long-term clinical operations, not short-term feature requirements.
- AI-Driven Workflow Automation: Automate scheduling, documentation, billing, and decision-making across care workflows.
- Integration-Ready Architecture: Seamless connectivity with healthcare systems, devices, and third-party platforms.
- Compliance-First Engineering: Built with HIPAA-compliant security, encryption, and governance frameworks from day one.
- Scalable for Growing Clinics: Designed to support multi-location clinics and high patient volumes without performance trade-offs.
Custom EHR platforms are no longer optional for clinics aiming to scale efficiently. Therefore, building the right system early can define long-term operational success.
Connect with Intellivon’s experts to build a custom EHR platform tailored to your clinic’s workflows, integrations, and growth roadmap.
FAQs
Q1. What is custom EHR software for clinics?
A1. Custom EHR software is a tailored digital system designed around a clinic’s specific workflows, patient management needs, and integrations. Unlike generic EHR tools, it adapts to how a clinic operates, enabling better efficiency, data control, and scalability across clinical and administrative processes.
Q2. How long does it take to build EHR software?
A2. The timeline depends on complexity and integrations. A basic EHR MVP can take 3–5 months, while a full-scale, enterprise-grade platform may take 6–12 months. Factors like compliance requirements, AI features, and interoperability needs can extend development time.
Q3. What integrations are needed in EHR systems?
A3. EHR systems typically integrate with labs, pharmacies, billing systems, insurance providers, and telehealth platforms. They also support standards like HL7 and FHIR for seamless healthcare data exchange. Integration needs vary based on the clinic’s services and scale.
Q4. How secure are custom EHR platforms?
A4. Custom EHR platforms are built with strong security measures, including data encryption, role-based access controls, audit logs, and HIPAA compliance frameworks. This ensures patient data remains protected while meeting regulatory requirements and reducing the risk of breaches.
Q5. How much does it cost to build an EHR?
A5. The cost to build a custom EHR platform typically ranges between $60,000 and $150,000. The final cost depends on features, integrations, compliance requirements, and system complexity. Clinics can scale the platform over time based on their needs and budget.