Healthcare apps create huge amounts of clinical data every day, but much of it gets stuck in separate systems. Lab results might be stored in one place, prescriptions in another, and patient histories somewhere else. For any enterprise trying to build or grow a healthcare app, this kind of data fragmentation makes it much harder to deliver reliable and compliant care.
HL7 integration fixes this problem by setting a common standard for communication between healthcare apps and EHR systems. When your app can connect easily with hospitals, clinics, labs, and pharmacies, data moves smoothly, work gets done faster, and compliance is easier to manage. Additionally, apps built with HL7 standards are the kind of systems that health networks actually want to use. Getting HL7 integration right from the start avoids expensive rework, vendor problems, and regulatory trouble later on.
Intellivon has experience helping healthcare teams build HL7-compliant apps that are connected, secure, and ready to scale. This blog explains the basics of HL7, how integration works in real-world settings, and practical steps to build it into your healthcare platform.
Why HL7 Integration Matters for Healthcare Apps
Building a healthcare application today is about more than just a clean interface. For any platform to provide value to a hospital, it must speak the same language as the existing infrastructure.
Consequently, Health Level Seven (HL7) standards have become the backbone of modern clinical logic.
Without a standardized way to move data, healthcare remains a series of digital islands. For entrepreneurs, investing in HL7 integration is a strategic move to ensure a product can survive in a regulated ecosystem.
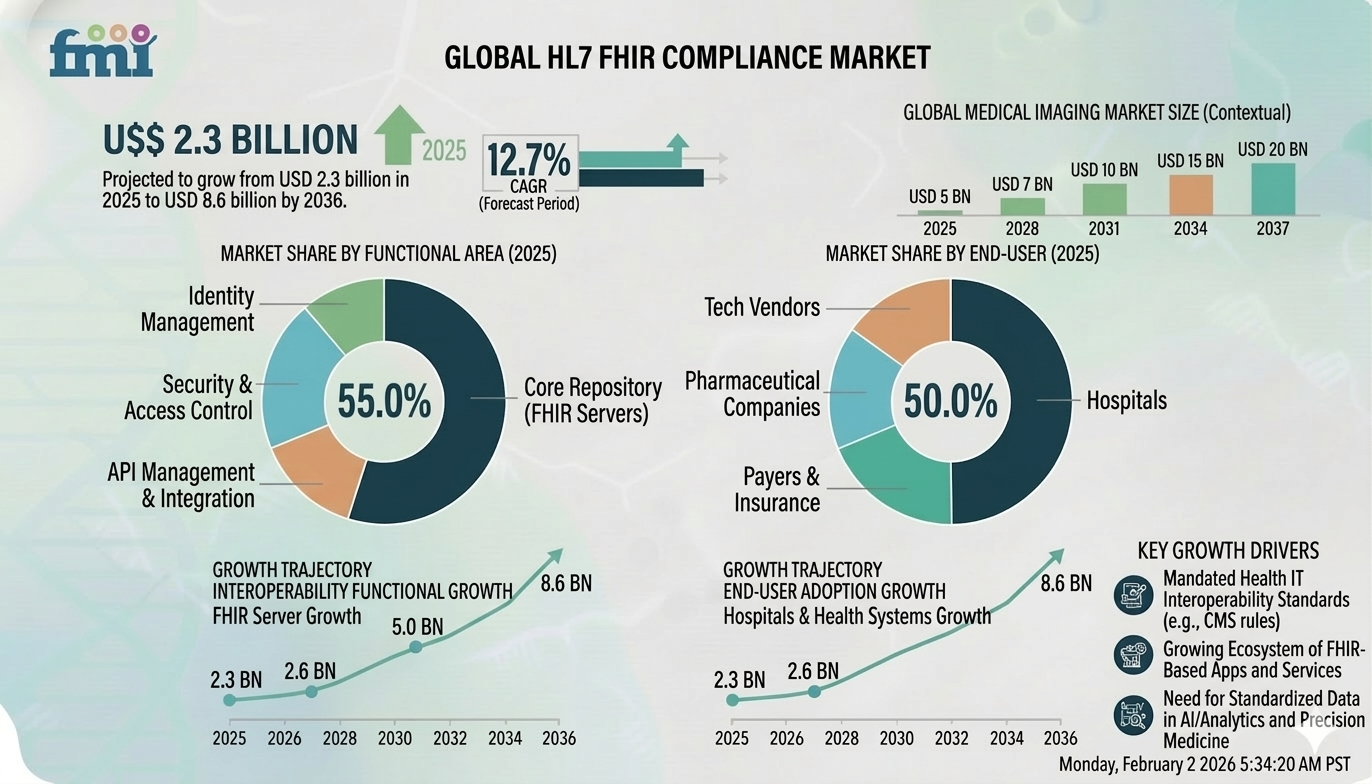
The HL7 integration market is valued at USD 2.3 billion in 2025 and is expected to reach USD 2.6 billion in 2026. Over the next decade, it is projected to grow to USD 8.6 billion by 2036, expanding at a CAGR of 12.7%.
1. Fragmented Health Data
Most medical facilities use dozens of different software systems to manage patient intake and billing. Unfortunately, these systems rarely talk to each other out of the box. This fragmentation creates data gaps where critical information is trapped in one department while another stays in the dark.
Therefore, clinicians lose time manually searching for records. For an investor, a platform that cannot solve this is a liability because it adds work to an exhausted workforce.
2. HL7 Enables Interoperability
HL7 acts as a universal translator for healthcare information. It provides international standards for transferring clinical data between software applications. By adopting these standards, your app can automatically receive updates when a doctor signs a chart.
Furthermore, interoperability allows your application to be “plug-and-play” ready for the enterprise.
3. Where HL7 Fits
In a modern tech stack, HL7 sits at the integration layer. It acts as the bridge between your app and the hospital’s Electronic Health Record (EHR).
This architecture allows you to scale quickly. Instead of building unique connections for every hospital, you build one robust HL7 interface that adapts to different environments.
4. When To Adopt HL7 Standards
The decision to adopt HL7 should happen during the design phase. If your app handles patient records or billing, you need these standards immediately.
Regulatory bodies often require this for data security. Moreover, large health systems make HL7 compatibility a deal-breaker during procurement.
As organizations move toward data-driven models, they prioritize platforms that reduce friction. Decision-makers are now focusing on how well a new tool fits into a broader digital strategy.
What Is HL7 and How Does It Work in Healthcare Systems?
HL7 is a global set of standards for transferring clinical and administrative data between software applications. Essentially, it serves as a universal language for healthcare IT.
This framework ensures that a pharmacy, a laboratory, and an imaging center all read patient data the same way. Therefore, it removes the need for expensive, custom-coded interfaces for every new connection.
HL7 v2 vs HL7 v3 vs FHIR Explained Simply
Healthcare interoperability has evolved significantly over time. However, not all HL7 standards work the same way. Each version, be it HL7 v2, HL7 v3, or FHIR, was designed for a different era of healthcare systems.
Understanding these differences helps you choose the right approach for building scalable, future-ready healthcare apps.
HL7 v2 vs HL7 v3 vs FHIR Comparison
| Aspect | HL7 v2 | HL7 v3 | FHIR |
| Release Era | Late 1980s | Early 2000s | 2014 onwards |
| Data Format | Pipe-delimited text | XML-based | JSON / XML |
| Architecture Style | Message-based | Model-driven | API-first (RESTful) |
| Ease of Implementation | Moderate (but inconsistent) | Complex and rigid | Easy and developer-friendly |
| Flexibility | High but loosely structured | Strict and standardized | Highly flexible and modular |
| Adoption Level | Widely used in hospitals | Limited adoption | Rapidly growing adoption |
| Real-Time Capability | Limited | Limited | Strong real-time support |
| Best Use Case | Legacy hospital systems | Structured enterprise systems | Modern apps and cloud platforms |
| Integration Complexity | High (custom mapping needed) | Very high | Lower with standardized APIs |
HL7 v2 remains the backbone of most hospital systems today, despite its inconsistencies. In contrast, HL7 v3 attempted to standardize data exchange but introduced complexity that limited widespread adoption.
FHIR changes the approach entirely. It uses modern web technologies, making it easier to build, scale, and integrate healthcare applications in real time.
In practice, most enterprise healthcare systems use a combination of HL7 v2 and FHIR, where HL7 handles internal system communication, and FHIR enables external app connectivity.
How HL7 Data Flows Between Hospital Systems
Healthcare systems rely on continuous data exchange to coordinate care across departments.
HL7 enables this by structuring how clinical data moves between systems like EHRs, lab systems, and billing platforms.
1. Data generated within source systems
Clinical data originates in systems such as EHRs, laboratory systems, or radiology platforms. Events like patient admissions, lab results, or discharge updates trigger HL7 messages.
2. HL7 message creation and formatting
The source system converts this data into HL7 message formats (such as ADT or ORU). These messages follow predefined structures to ensure consistent data exchange.
3. Transmission through interface engines
HL7 messages are routed through interface engines like Mirth or Rhapsody. These systems manage message flow, queue processing, and routing across multiple endpoints.
4. Data transformation and mapping
Since systems store data differently, messages are transformed and mapped. This ensures compatibility between the sending and receiving systems.
5. Data ingestion by target systems
The receiving system processes the HL7 message and updates records accordingly, such as adding patient data or updating clinical results.
HL7 enables structured, event-driven communication across hospital systems. However, real-world implementations often require middleware and transformation layers to ensure accurate, scalable data exchange.
Types of EHR Systems You Need to Integrate With
Understanding the EHR landscape is vital for any strategic healthcare investment. Therefore, your integration strategy must account for the diverse technical architectures found in modern hospitals. Consequently, recognizing which systems dominate specific sectors will help you prioritize your development roadmap.
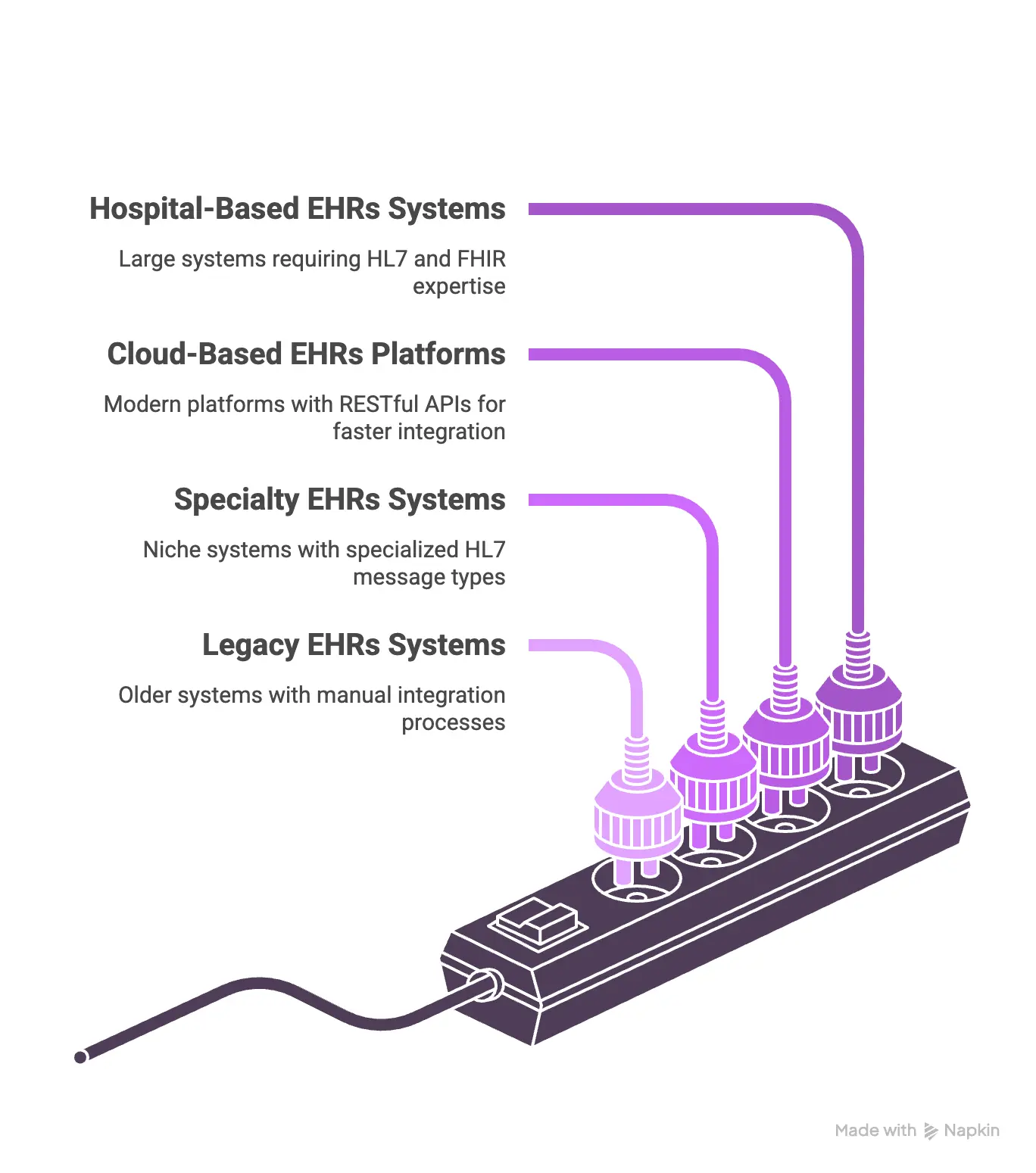
1. Hospital-based EHR systems
Large health systems typically rely on Epic and Oracle Cerner. These systems are massive installations that manage everything from patient billing to surgical scheduling. Integration with these giants usually requires deep familiarity with HL7 v2 messages and, increasingly, FHIR APIs.
Because these systems are so deeply entrenched, they often have strict security protocols. However, successfully connecting to an Epic instance opens the door to the largest patient populations. Therefore, demonstrating the ability to handle these heavyweights signals that your product is ready for the enterprise.
2. Cloud-based EHR platforms
In contrast to traditional systems, cloud-based EHRs like Athenahealth use modern web standards. These platforms are often the preferred choice for smaller practices and innovative startups. They usually offer well-documented RESTful APIs, which makes the initial integration much faster.
Furthermore, these systems scale more naturally with your application. Since the infrastructure is managed in the cloud, you don’t have to worry about hospital-side server maintenance. This lower barrier to entry allows for rapid prototyping and quicker market validation.
3. Specialty EHR Systems
Not every healthcare provider needs a general-purpose EHR. For example, behavioral health and oncology often use “niche” platforms tailored to their specific workflows. These systems might use specialized HL7 message types that aren’t common in general medicine.
If your app targets a specific medical vertical, you must ensure your integration layer can handle these unique data fields. Therefore, a flexible HL7 engine is essential to capture the nuances of specialty care.
4. Legacy EHR Systems
Many smaller hospitals still operate on legacy systems built decades ago. These systems often lack modern APIs and may only support older versions of the HL7 standard. Integrating with them can be a manual process involving flat-file transfers or outdated connections.
However, these legacy environments represent a significant portion of the underserved market. While they present technical hurdles, solving the integration puzzle for these facilities creates a massive competitive advantage. It proves your team has the “in-the-trenches” experience to handle messy healthcare data.
Navigating these different systems requires a nuanced approach to data architecture. By planning for both cutting-edge cloud apps and rigid legacy platforms, you position your enterprise for maximum market reach.
Popular EHR Systems and HL7 Integration Approach
Navigating specific EHR vendors requires a tailored strategy. Each major player has a distinct philosophy regarding data access, meaning a “one-size-fits-all” connector rarely works at the enterprise level.
Consequently, your technical roadmap must account for these vendor-specific nuances to ensure reliable data flow.
| EHR System | Integration Method | Key HL7 Messages | Challenges | Recommended Strategy |
| Epic | HL7 v2 + Care Everywhere | ADT, ORU | Strict governance, closed ecosystem | Work with the Bridge team for mapping and approvals |
| Cerner | HL7 + custom workflows | ADT, ORU, ORM | Data inconsistency across domains | Normalize data using interface engines |
| Athenahealth | APIs (primary) + HL7 | Limited HL7 usage | API-first model reduces HL7 reliance | Use APIs for real-time, HL7 for batch workflows |
| Allscripts | HL7 v2 (legacy-heavy) | ADT, ORU | Older HL7 versions (v2.3) | Build backward-compatible integrations |
1. Integrating with Epic using HL7 interfaces
Epic remains the dominant force in large-scale healthcare. Their integration approach primarily utilizes the Epic Care Everywhere network and traditional HL7 v2 feeds.
- Method: Focuses on ADT (Admission, Discharge, Transfer) and ORU (Observation Result) messages.
- Strategy: Requires coordination with the hospital’s Bridge team to map specific data segments.
2. Cerner HL7 integration workflows and challenges
Cerner (now Oracle Health) often utilizes a more open, yet complex, architecture. While they support standard HL7, their workflows can be highly customized per facility.
- Challenge: Data consistency across different Cerner “domains” can vary.
- Solution: Use an interface engine to normalize incoming Cerner data before it hits your app.
3. Athenahealth API vs HL7 integration differences
Athenahealth is a cloud-native leader. Unlike legacy systems, they strongly prefer RESTful APIs over traditional HL7.
- API Advantage: Faster setup and easier real-time queries.
- HL7 Use Case: Better for high-volume, asynchronous background tasks like batch result uploads.
4. Allscripts integration considerations for apps
Allscripts (Veradigm) provides a flexible environment but often requires navigating multiple legacy codebases.
- Consideration: Ensure your integration can handle older HL7 versions (v2.3) frequently found in their ambulatory setups.
Understanding these vendor profiles allows you to allocate development resources effectively. By mastering these connections, you transform a technical hurdle into a massive competitive moat.
Step-by-Step HL7 Integration Process for Apps
At the enterprise level, EHR integration is a continuous, high-integrity lifecycle. Consequently, we treat every integration as a mission-critical pipeline. This architecture must remain resilient against system updates and clinical workflow changes.
Our methodology ensures that your platform moves from a standalone tool to a deeply embedded clinical asset. Therefore, we utilize a rigorous, expert-led framework for every deployment.
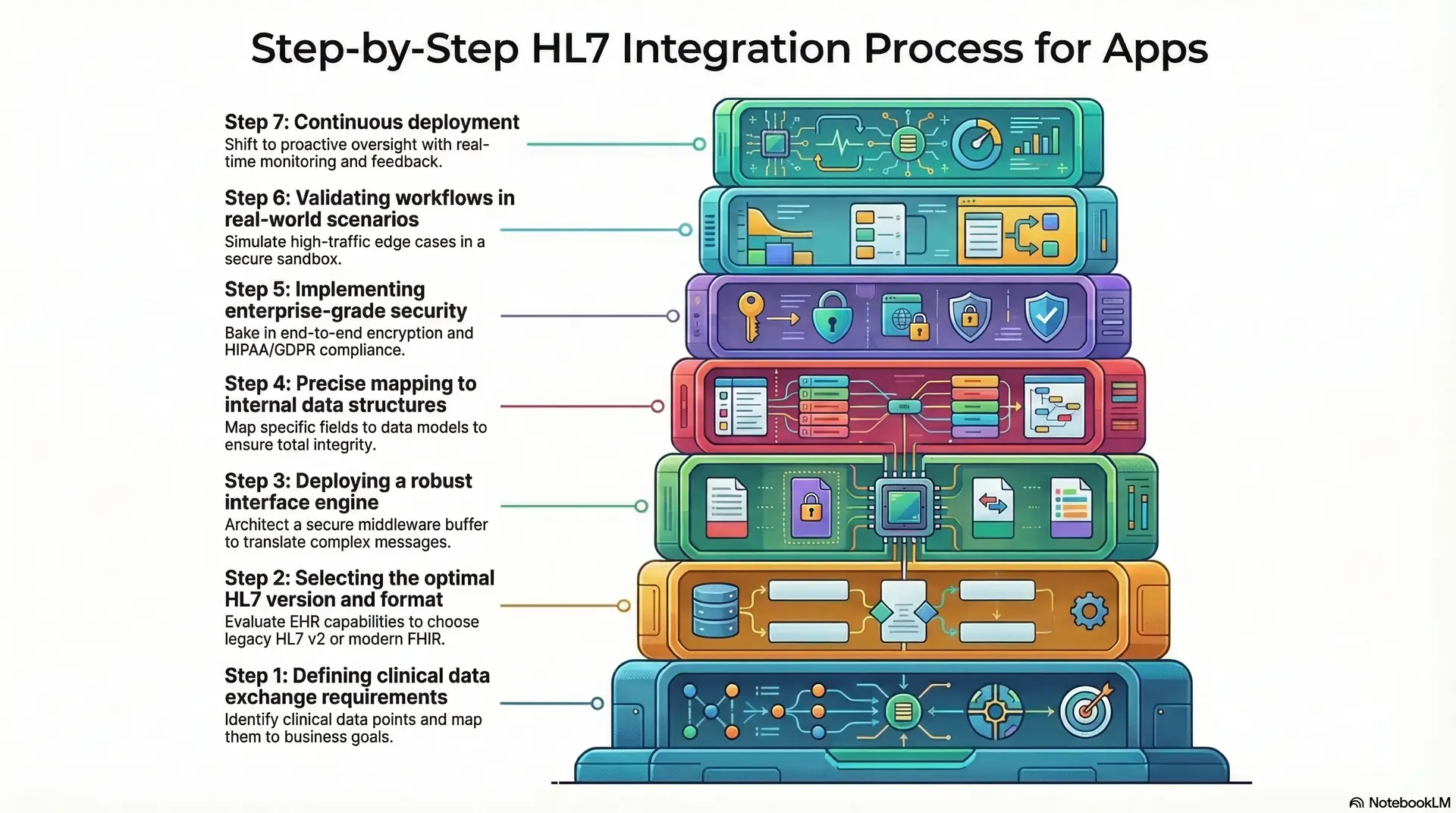
Step 1: Defining clinical data exchange requirements
Before a single line of code is written, we identify the exact clinical data points required. Whether the objective is real-time vital monitoring or asynchronous syncing, we map these needs to your broader business goals.
This strategic alignment prevents “scope creep” effectively. Furthermore, it ensures development resources are focused exclusively on high-value data streams.
Step 2: Selecting the optimal HL7 version and format
Interoperability requires navigating a fragmented landscape of standards. We evaluate the target EHR’s capabilities to determine the superior choice. Frequently, we implement a hybrid approach between legacy HL7 v2 and modern FHIR APIs.
This flexibility ensures your application maintains compatibility across diverse healthcare environments.
Step 3: Deploying a robust interface engine
We avoid the fragility of “point-to-point” connections. Instead, we architect a robust interface engine. This acts as a permanent, secure buffer between your app and the hospital infrastructure.
Moreover, this middleware translates complex messages into a clean, actionable format for your internal systems.
Step 4: Precise mapping to internal data structures
HL7 messages are notoriously “noisy” and filled with redundant segments. Our engineers meticulously map specific fields to your application’s data model. Therefore, we ensure total data integrity at every step.
This prevents the clinical mismatches that occur when handling high-volume patient information.
Step 5: Implementing enterprise-grade security
Security is baked into our architecture, not added as an afterthought. We implement end-to-end encryption and multi-factor authentication protocols.
Consequently, every integration point is fully HIPAA or GDPR compliant. This approach protects both the patient data and your enterprise’s reputation.
Step 6: Validating workflows in real-world scenarios
Testing goes far beyond simple connectivity checks. We simulate high-traffic environments and complex “edge cases.”
By validating these workflows in a secure sandbox, we guarantee performance. Clinicians can then rely on the data for real-time decision-making without hesitation.
Step 7: Continuous deployment
Once a connection is live, our work shifts into proactive oversight. We implement real-time monitoring to catch message failures or latency bottlenecks.
This continuous feedback loop allows us to resolve issues quickly. Thus, we optimize performance as your clinical data needs scale.
By treating integration as an evolving lifecycle, Intellivon provides a foundation for long-term scalability. We leverage our enterprise-grade AI and deep integration expertise to turn technical hurdles into a high-performance competitive advantage.
Key Components of HL7 Integration Architecture
Building a resilient HL7 architecture is a strategic investment in technical stability. At the enterprise level, we avoid fragile, direct connections between systems. Instead, we architect a modular environment that absorbs the complexities of diverse hospital infrastructures.
This approach ensures that your application remains scalable and secure as your clinical data requirements evolve. Therefore, our architectural framework prioritizes high availability and total data integrity.
1. Interface Engines for Message Processing
The interface engine is the central nervous system of any healthcare integration strategy. It serves as a sophisticated router that accepts, parses, and delivers HL7 messages. Consequently, this engine eliminates the need for manual data handling.
We utilize industrial-grade engines to manage high-volume message traffic without latency. Furthermore, a robust engine provides the logging and queuing necessary to prevent data loss during system downtime.
2. Data Transformation and Mapping Layers
HL7 messages are notoriously inconsistent across different EHR vendors. Therefore, we implement a dedicated transformation layer to normalize this data. This component translates non-standard vendor segments into a clean, unified format.
We meticulously map every clinical field, from patient identifiers to complex lab results. Consequently, your developers can focus on building features rather than debugging inconsistent data packets.
3. API Gateways and Interoperability Layers
Modern healthcare apps must bridge the gap between legacy HL7 and modern web standards. We deploy advanced API gateways that act as a secure front door for your data exchange. Moreover, they allow your platform to support both HL7 v2 and FHIR standards simultaneously.
This interoperability layer ensures that your app remains compatible with both legacy hospital systems and cutting-edge cloud platforms. Thus, you achieve maximum market reach.
4. Security, Compliance, and Audit Systems
Security is the most critical component of any healthcare architecture. Since we handle sensitive Protected Health Information (PHI), our systems include automated audit trails and end-to-end encryption.
Every data transaction is logged, creating a transparent record for HIPAA compliance. Therefore, your enterprise remains protected against both external threats and regulatory risks.
By engineering these components into a unified architecture, Intellivon ensures your healthcare platform is ready for the rigors of the enterprise. We provide the technical depth required to turn complex data into a strategic asset.
HL7 Integration Challenges and How to Solve Them
Identifying the technical barriers to a seamless EHR integration solution is only half the battle. For enterprise leaders, the real value lies in how those obstacles are systematically dismantled.
Intellivon approaches these challenges with a dual focus on engineering excellence and clinical operational stability. Therefore, we transform high-risk integration hurdles into stable, high-performance data pipelines that drive long-term business growth.
1. Inconsistent Data Formats Across EHR Systems
Standardization remains the most persistent challenge in healthcare. Although HL7 provides a framework, different EHR vendors often implement “Z-segments” or custom fields that deviate from the norm. Consequently, a message that works for one hospital may fail in another.
Our Solution: We implement a robust data normalization layer that automatically detects and corrects these inconsistencies. By using AI-driven mapping tools, we ensure that every incoming data packet is cleaned and structured before it enters your application. This results in a “single source of truth” across all your integrated provider networks.
2. Legacy Systems Lacking Modern APIs
Many established provider networks still operate on-premise systems that do not support RESTful APIs or modern web protocols. This creates a massive “data wall” that blocks real-time connectivity. Therefore, traditional integration methods often lead to slow, batch-processed data that lacks clinical relevance.
Our Solution: We deploy custom-built middleware “wrappers” that translate legacy HL7 v2 messages into modern FHIR resources. This allows your platform to communicate with decades-old infrastructure without requiring a full system overhaul. Thus, you gain the benefits of modern cloud connectivity while maintaining compatibility with legacy hospital environments.
3. Complex Message Mapping and Transformations
Mapping thousands of clinical data points between disparate systems is a labor-intensive and error-prone process. Moreover, manual mapping slows down the deployment of new integrations significantly.
Our Solution: We utilize advanced transformation engines that automate the heavy lifting of data mapping. Our library of pre-configured templates for major EHRs like Epic and Cerner accelerates the “go-live” process. Consequently, we reduce manual errors and ensure that your integration remains accurate and reliable at scale.
4. Security Risks in Clinical Data Exchange
Transmitting Protected Health Information (PHI) across networks introduces significant vulnerabilities. Without enterprise-grade security, your integration points become prime targets for data breaches and ransomware. Therefore, maintaining compliance with HIPAA or GDPR is a continuous operational requirement, not a one-time checkbox.
Our Solution: We embed security directly into the integration architecture using end-to-end encryption (TLS 1.2+) and granular access controls. Every transaction is tracked through an automated audit system, providing full transparency for regulatory reviews. This proactive security posture minimizes risk and builds deep trust with your healthcare partners.
5. Real-Time Data Sync and Latency Issues
High-latency data exchange can render a healthcare application useless in emergency or acute care settings. If a clinician has to wait minutes for a lab result to sync, the platform becomes a bottleneck rather than a tool.
Our Solution: We architect high-concurrency message queues that process thousands of transactions per second with sub-second latency. By using edge computing and optimized data routing, we ensure that your application always displays the most current clinical information. This real-time performance is what sets an enterprise-grade solution apart from a standard app.
By systematically addressing these technical barriers, Intellivon removes the friction associated with healthcare data exchange. We provide the expertise needed to turn these complex challenges into a seamless, high-value integration experience.
Compliance Requirements for HL7 Integration
Navigating the regulatory landscape is a critical hurdle for any healthcare enterprise. For investors, compliance is not merely a legal checkbox; it is a fundamental protector of brand equity and market valuation.
Therefore, we architect every HL7 integration with a “security-first” mindset to ensure your platform passes every hospital IT audit.
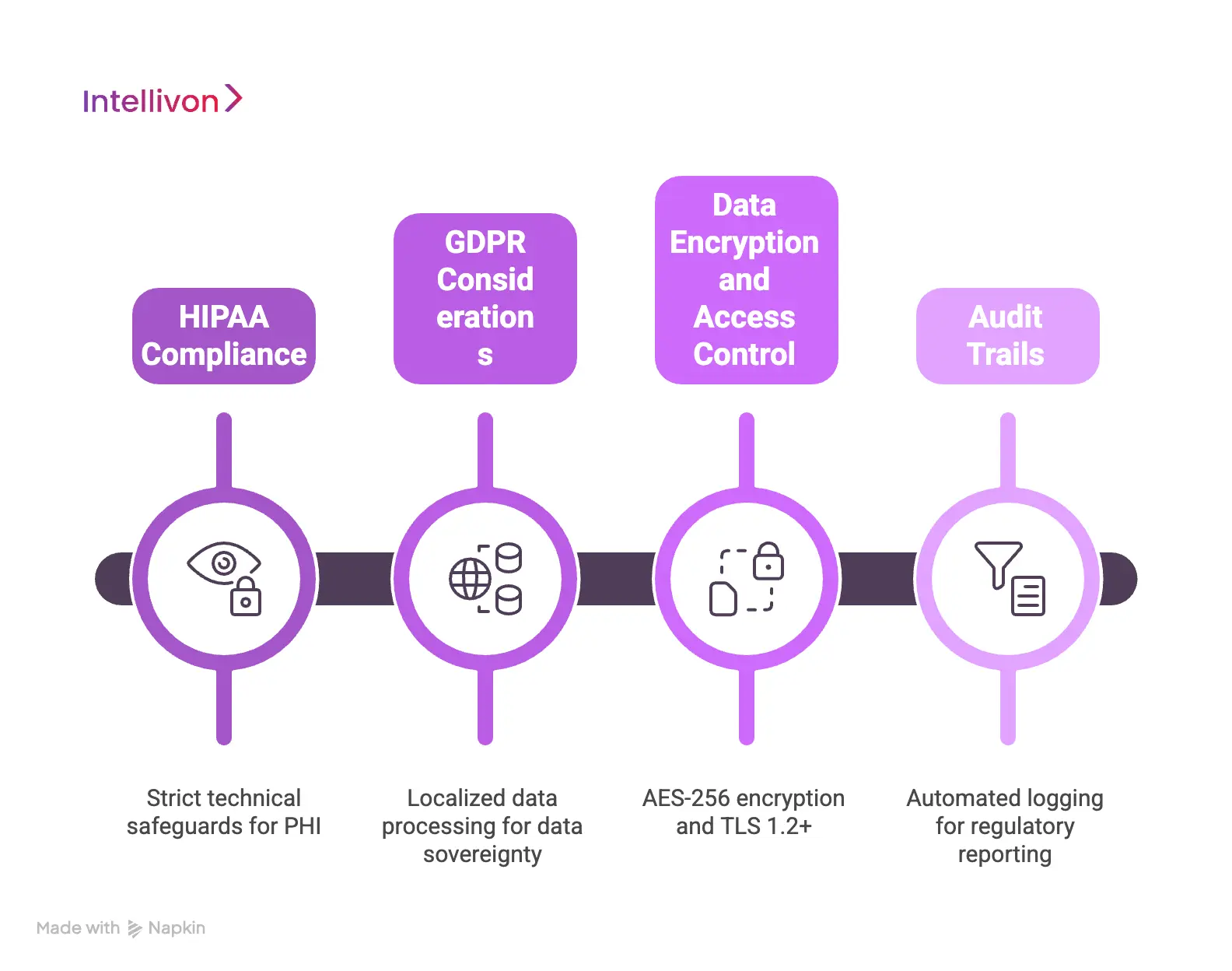
1. HIPAA Compliance
In the United States, HIPAA remains the gold standard for protecting patient privacy. Any application touching Protected Health Information (PHI) must adhere to strict technical safeguards. Consequently, we implement rigorous data-handling protocols for every connection.
Our integration logic ensures that PHI is never transmitted in an insecure manner. Furthermore, we automate the de-identification of data where full records are not clinically necessary. This approach maintains high integrity while reducing your organization’s total liability.
2. GDPR Considerations
For platforms operating in Europe, GDPR introduces a higher layer of complexity regarding data sovereignty. Unlike many generic solutions, our architecture allows for localized data processing.
This ensures that sensitive health information stays within specific geographic boundaries as required by law. Consequently, we help your enterprise navigate the data portability requirements central to HL7 interoperability. Thus, your app remains globally compliant from day one.
3. Data Encryption and Access Control
Security must exist both in transit and at rest. We utilize AES-256 encryption for data storage and TLS 1.2+ for every HL7 message moving across the network.
Moreover, we implement Role-Based Access Control to ensure only authorized personnel interact with clinical data. This granular approach prevents unauthorized internal access. Therefore, your system remains a fortress against both external threats and internal errors.
4. Audit Trails
Transparency is the final pillar of a compliant integration. We implement automated audit trails that log every interaction within the HL7 pipeline. These logs provide the necessary documentation for regulatory reporting and forensic analysis.
Consequently, your enterprise stays ready for any compliance review without manual preparation.
By embedding these standards into the core data pipeline, Intellivon mitigates the risk of catastrophic data breaches. We ensure your partners can scale across health systems without the fear of non-compliance penalties.
Cost to Build an HL7 EHR Integration Solution
At Intellivon, HL7 EHR integration solutions are engineered as enterprise interoperability infrastructure, not as simple connectors between healthcare systems. The objective is to build a platform that enables reliable, secure, and real-time clinical data exchange across fragmented healthcare environments.
However, HL7 integration is not just about connecting systems. It involves message standardization, data transformation, compliance controls, and system orchestration. As a result, healthcare providers gain unified data access while reducing integration failures, delays, and clinical risks.
Estimated Phase-Wise Cost Breakdown
| Phase | Description | Estimated Cost (USD) |
| Discovery & Integration Planning | Identify EHR systems, HL7 message types, and data exchange workflows | $8,000 – $15,000 |
| Architecture & HL7–FHIR Design | Define integration architecture, middleware, and interoperability layers | $10,000 – $20,000 |
| Interface Engine Setup | Configure Mirth/Rhapsody, message routing, and queue systems | $12,000 – $25,000 |
| HL7 Message Mapping & Transformation | Map HL7 segments to internal data models or FHIR resources | $15,000 – $30,000 |
| API & Interoperability Layer | Build FHIR APIs and external system access layers | $10,000 – $20,000 |
| Security & Compliance Implementation | HIPAA, encryption, access controls, and audit logging | $8,000 – $18,000 |
| Testing & Validation | Validate workflows, simulate clinical scenarios, fix edge cases | $7,000 – $15,000 |
| Deployment & Monitoring Setup | Production deployment, monitoring, and performance tuning | $5,000 – $12,000 |
Total Estimated Cost Range
$50,000 – $150,000+
The final cost depends on:
- Number of EHR systems integrated (Epic, Cerner, etc.)
- Complexity of HL7 message mapping
- Need for HL7–FHIR transformation layers
- Real-time vs batch data processing requirements
- Compliance and security requirements
HL7 vs FHIR Integration Cost Considerations
HL7-based integrations often require more custom mapping and middleware, which increases complexity. In contrast, FHIR-based systems reduce development effort but still require HL7 bridging for legacy systems.
As a result, most enterprise solutions involve hybrid HL7–FHIR architectures, which slightly increase upfront cost but significantly improve scalability and future readiness.
Hidden Costs in HL7 Integration Projects
Many healthcare teams underestimate the following:
- Rework due to inconsistent HL7 message formats
- Delays caused by EHR vendor approvals (Epic, Cerner)
- Ongoing maintenance for message updates and workflows
- Infrastructure scaling for high-volume data exchange
Get a Custom HL7 Integration Cost Estimate
Every healthcare system has unique integration requirements. Therefore, a fixed estimate rarely reflects real-world complexity.
Connect with Intellivon’s experts to get a tailored cost breakdown based on your EHR systems, workflows, and scalability goals.
Conclusion
HL7 integration is the fundamental infrastructure for any successful healthcare enterprise. By bridging the gap between isolated data silos and real-time clinical care, you transform your platform into an indispensable medical asset. Therefore, investing in a robust, compliant integration strategy today ensures long-term scalability and market leadership.
Partner with Intellivon to navigate these complexities with confidence. We deliver cutting-edge, enterprise-grade AI and integration solutions that turn technical hurdles into sustainable growth. Reach out to our strategists today to architect your seamless EHR integration.
Build HL7 Integration Solutions With Intellivon
At Intellivon, HL7 integration solutions are built as enterprise interoperability infrastructure, not as point-to-point connectors layered onto fragmented healthcare systems. The goal is to enable seamless, secure, and scalable data exchange across EHRs, clinical systems, and modern healthcare applications.
Each solution is designed to handle the full integration lifecycle. This includes HL7 message ingestion, transformation, FHIR enablement, real-time data exchange, and compliance enforcement. As a result, healthcare organizations gain reliable interoperability without compromising performance, security, or scalability.
Our engineering teams focus on building hybrid HL7–FHIR architectures that bridge legacy hospital systems with modern, API-driven applications. Therefore, enterprises can modernize their healthcare platforms while maintaining compatibility with existing infrastructure.
Why Partner With Intellivon?
- Enterprise-Grade Interoperability Architecture: We design integration systems with interface engines, transformation layers, and API gateways to ensure consistent, scalable, and high-performance data exchange across healthcare environments.
- Deep Experience With Major EHR Systems: Our teams have worked with Epic, Cerner, Athenahealth, and other leading platforms, enabling faster integrations and reducing vendor-specific implementation risks.
- HL7–FHIR Hybrid Integration Expertise: We build systems that translate HL7 messages into FHIR resources, allowing healthcare apps to achieve real-time interoperability while maintaining legacy system compatibility.
- Security and Compliance by Design: Every solution includes HIPAA-compliant data handling, encryption, role-based access control, and audit-ready infrastructure to meet enterprise regulatory requirements.
- Scalable and Future-Ready Infrastructure: Our architectures support high-volume data exchange, multi-system integrations, and future expansion as healthcare ecosystems grow more complex.
Talk to Intellivon’s experts to design a scalable HL7–FHIR integration solution tailored to your healthcare systems and growth roadmap.
FAQs
Q1. What is HL7 integration in healthcare apps?
A1. HL7 integration enables healthcare apps to exchange clinical data with systems like EHRs, lab systems, and billing platforms. It standardizes how data such as patient records, lab results, and admissions are shared. As a result, apps can access real-time clinical information and support coordinated care delivery.
Q2. How long does HL7 integration take?
A2. HL7 integration typically takes 6 to 16 weeks, depending on complexity. Simple integrations with one system can be completed faster, while multi-EHR or HL7–FHIR integrations take longer. Timelines also depend on vendor approvals, data mapping complexity, and testing requirements.
Q3. What systems can HL7 connect to?
A3. HL7 can connect to a wide range of healthcare systems, including EHRs (Epic, Cerner), laboratory systems, radiology systems, billing platforms, and pharmacy systems. It acts as a standard communication layer between clinical and operational systems.
Q4. Is HL7 still relevant compared to FHIR?
A4. Yes, HL7 remains highly relevant because most hospital systems still rely on HL7 v2. However, FHIR is growing rapidly for modern, API-based integrations. In practice, healthcare apps use both, where HL7 handles internal data exchange, and FHIR enables external app connectivity.
Q5. How secure is HL7 data exchange?
A5. HL7 itself does not define security, but secure implementations use encryption (TLS), access controls, and secure transport protocols. When combined with HIPAA-compliant infrastructure, HL7 integrations can safely handle sensitive patient data across systems.