The wrong EHR decision doesn’t announce itself on day one. It surfaces eighteen months later, in a system that can’t scale, a compliance gap that triggers an audit, or a vendor contract that holds your data hostage. By then, reversing course costs far more than doing it right the first time.
Healthcare organizations today are dealing with a complex landscape. Interoperability requirements are increasingly strict, and AI-based clinical workflows are the new normal. At the same time, healthcare regulations such as HIPAA, HL7 FHIR, and ONC certification are creating multiple layers of compliance that generic platforms handle well only in broad terms. So, the real question isn’t simply “build vs. buy.” It lies in control, scalability, and how far you want your enterprise to scale.
We at Intellivon have helped many enterprises navigate this very decision in the past, creating custom EHR platforms that fit the complex needs of healthcare organizations. In this blog, we provide you with the strategic tools you need to make the right decision with confidence.
Why Enterprises Are Moving Toward Custom EHR
Enterprises are moving toward custom EHR systems to overcome vendor limits, tailor workflows, and gain full control over their data. As interoperability demands grow, off-the-shelf solutions struggle to scale or support specialized care models.
At the same time, the EHR market is expected to reach $36.93B in 2025, reflecting rising demand. Custom platforms help organizations integrate AI, improve system flexibility, and manage long-term costs more predictably.
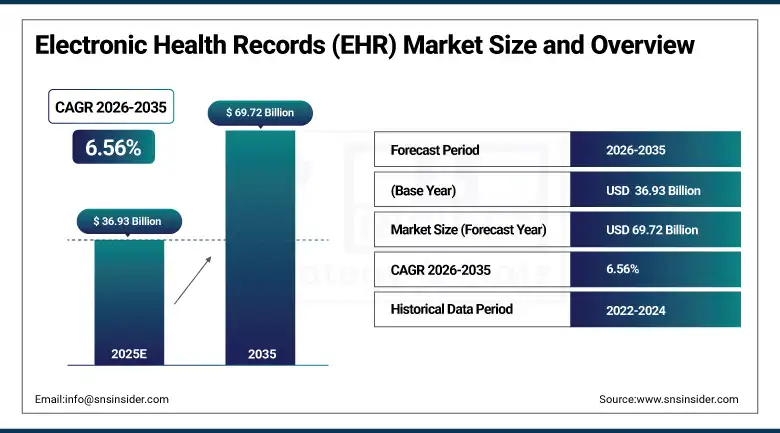
Navigating the choice between off-the-shelf software and a tailored build is a pivotal moment for any healthcare enterprise. While ready-made solutions offer a quick start, the shift toward a custom EHR is driven by the need for a sustainable, competitive edge.
1. Standard systems fail to support complex workflows
Generic platforms are built for the average user, creating friction for specialized departments. When software does not mirror a clinician’s actual steps, productivity drops and burnout rises.
Most standard tools force professionals to adapt to the software rather than the technology supporting the expert.
2. Early EHR choices create long-term limitations
Choosing a vendor based on immediate needs often leads to “vendor lock-in.” If the provider’s roadmap diverges from your strategy, your enterprise remains stuck with obsolete tools.
Building custom ensures you own the intellectual property and maintain the freedom to evolve.
3. Scaling exposes gaps in ready-made platforms
Ready-made platforms struggle with the concurrent user volume required at the enterprise level. Furthermore, licensing fees typically scale per user, creating a financial burden as you grow.
Custom solutions allow for horizontal scaling without the recurring penalty of exponential licensing costs.
4. Faster deployment leads to long-term inefficiencies
The allure of “plug-and-play” promises a rapid launch but often lacks deep integration. Over time, the cost of managing these inefficiencies exceeds the initial savings.
A strategic investment in custom EHR prioritizes long-term operational health over a temporary, limited shortcut.
5. Enterprises need control over data and systems
Standard systems often use closed architectures that make real-time analytics a significant challenge. For an enterprise looking to leverage AI, this lack of access is a deal-breaker.
A custom build allows for higher-level encryption and specific audit trails that meet evolving regulatory demands.
Investing in a custom EHR secures your future against the limitations of generic software. At the same time, it prepares your organization for a more agile, data-driven era of healthcare.
Custom vs Ready-Made EHR: Core Differences
Choosing between a custom-built and ready-made EHR is a long-term infrastructure choice that directly impacts how your organization delivers care, manages data, and scales operations.
At a surface level, ready-made systems offer speed and lower upfront costs. However, as workflows become more complex and integrations grow, these systems often create limitations. In contrast, custom EHR platforms are designed around your workflows, data flows, and long-term operational goals.
The difference rests in control, scalability, and alignment with how your healthcare system actually operates.
Comparison: Custom vs Ready-Made EHR
| Factor | Ready-Made EHR | Custom EHR |
| Cost Structure | Lower upfront cost but recurring license fees | Higher upfront investment with predictable long-term costs |
| Implementation Speed | Faster deployment with pre-built modules | Longer timeline due to system design and development |
| Workflow Fit | Standardized workflows with limited flexibility | Fully aligned with clinical and operational workflows |
| Scalability | Limited by vendor architecture and pricing tiers | Designed to scale across locations, users, and services |
| Integrations | Restricted APIs and integration limitations | Seamless integration with labs, payers, devices, and systems |
| Data Ownership | Vendor-controlled data structures | Full ownership and control over data architecture |
| Customization | Surface-level configuration options | Deep customization across workflows and logic |
| Compliance | General compliance support | Tailored compliance based on system and region |
| Long-Term Flexibility | Difficult to adapt as needs evolve | Built to evolve with new care models and technologies |
The Difference Becomes Clear at Scale
At an early stage, ready-made EHR systems can support basic operations efficiently. However, as organizations grow, add specialties, and integrate more systems, their limitations become more visible.
Custom EHR platforms address these gaps by aligning technology with real-world workflows, and not by forcing teams to adapt to software constraints. As a result, enterprises that plan for long-term scale and flexibility increasingly move toward custom-built systems.
Where Ready-Made EHR Breaks at Scale
The primary challenge of a fixed platform is its inability to evolve alongside an expanding business. As operational complexity grows, the limitations of a one-size-fits-all architecture transition from minor inconveniences to significant financial liabilities.
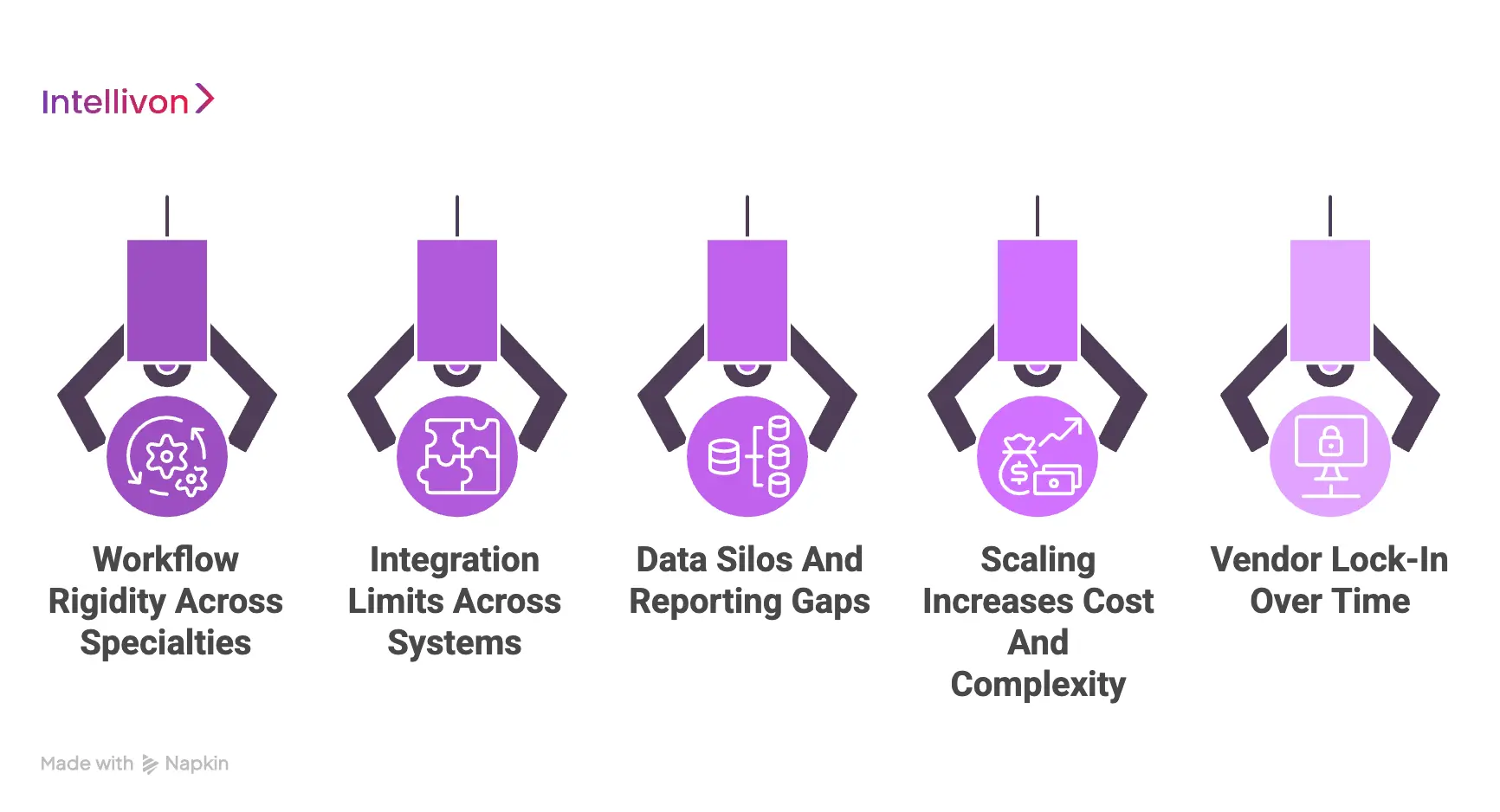
1. Workflow rigidity across specialties
Standardized EHRs are designed for the “median” clinical case, which rarely aligns with the nuanced needs of specialized medicine. For instance, an oncology department requires vastly different data visualization and staging tools than a pediatric clinic. When a platform lacks the flexibility to adapt to these specific workflows, clinicians are forced into manual entry.
This rigidity creates a massive hidden cost in the form of administrative burden. Specialized teams often spend more time fighting the interface than engaging with patients. A system that cannot pivot to meet the unique demands of each department eventually becomes a bottleneck for the entire organization.
2. Integration limits across systems
In an enterprise environment, the EHR must communicate with laboratory information systems (LIS), imaging archives (PACS), and billing engines. Ready-made platforms frequently offer limited “out-of-the-box” integrations that fail to handle custom data fields or real-time syncing.
Consequently, IT teams must build expensive “middleware” to bridge these gaps. These patches are fragile and often break during software updates, leading to system downtime. Without deep, native integration, the enterprise remains a collection of disconnected tools rather than a unified digital ecosystem.
3. Data silos and reporting gaps
Data is only useful if it is accessible, yet many commercial EHRs store information in proprietary formats. This creates data silos where extracting granular insights for population health or financial auditing requires specialized, expensive services from the vendor.
Enterprise leaders need real-time dashboards to make informed decisions. When the reporting layer is shallow, leadership is essentially flying blind. These gaps in data visibility prevent organizations from identifying waste, optimizing resource allocation, or leveraging predictive AI models to improve patient outcomes.
4. Scaling increases cost and complexity
The financial model of most ready-made EHRs is built on per-user or per-seat licensing. While this seems manageable for a small team, it becomes a predatory expense as an enterprise grows. Adding five hundred new staff members can result in a massive, recurring budgetary spike that does not provide any new functionality.
Furthermore, as you add more modules to compensate for missing features, the system architecture becomes bloated. This complexity leads to slower load times and increased training requirements for new hires. At scale, the low starting price of a ready-made solution often evaporates, replaced by a high total cost of ownership.
5. Vendor lock-in over time
Perhaps the most dangerous risk of a ready-made platform is the loss of strategic autonomy. When your entire clinical operation runs on a closed system, switching costs become so high that you are effectively trapped. The vendor gains immense leverage, allowing them to hike prices or slow down support without fear of losing your business.
This lock-in prevents enterprises from adopting newer, more efficient technologies that might emerge in the market. You are tied to the vendor’s development cycle, even if it lags years behind industry standards. A custom EHR removes this dependency, placing the roadmap firmly back into the hands of the organization.
Scaling a healthcare enterprise requires a foundation that expands without friction. Recognizing where ready-made systems fail is the first step toward building a resilient, high-performance infrastructure that supports long-term growth.
When Custom EHR Becomes the Logical Choice
Choosing to build a custom solution is a strategic pivot from a passive consumer to an active architect of your clinical future. When the cost of adapting to a rigid system exceeds the investment of a bespoke build, the logic for a custom EHR becomes undeniable.
For high-growth healthcare enterprises, the transition to custom software is rarely about a single feature. It is a fundamental decision to align technical infrastructure with long-term business objectives and operational excellence.
1. Multi-location and multi-team operations
Managing a fragmented network of clinics requires a unified source of truth that standard platforms struggle to provide. A custom EHR centralizes data while allowing for localized configurations that reflect the specific regulatory or operational needs of different regions.
This ensures consistent care quality and reporting across the entire organization.
2. Complex clinical and operational workflows
If your organization handles specialized treatments or unique patient journeys, a “standard” interface is a liability. Custom builds allow for the creation of precise modules, such as advanced oncology tracking or complex surgical scheduling, that mirror your exact protocols.
This specificity reduces cognitive load for staff and minimizes the risk of procedural errors.
3. Real-time integrations across ecosystems
Modern healthcare does not exist in a vacuum. Your EHR must communicate instantly with labs, pharmacies, and wearable devices. Custom architecture prioritizes open APIs and HL7/FHIR standards, ensuring that data flows without friction.
This connectivity eliminates manual data entry and provides clinicians with a comprehensive, real-time view of patient health.
4. Automation, AI, and data-driven decisions
Ready-made systems often treat AI as a superficial add-on. In contrast, a custom EHR allows you to bake predictive analytics and automated administrative tasks directly into the core engine.
Whether it is predicting patient no-shows or automating complex billing cycles, native AI integration transforms the EHR from a digital filing cabinet into a proactive business tool.
5. Need for long-term system ownership
Owning your software is a play for financial and strategic autonomy. By building custom, you eliminate the risk of vendor insolvency or unexpected price hikes.
You own the code, the data, and the roadmap, ensuring that your most critical business tool evolves at the pace of your own ambition, not a third party’s schedule.
A custom EHR is the foundation for an enterprise that refuses to be limited by “average” software. It is an investment in a system that grows with you, rather than one you eventually outgrow.
What a Custom EHR Platform Actually Includes
A bespoke platform is A cohesive environment where clinical excellence meets operational efficiency. By designing each component from the ground up, an organization ensures that every module speaks the same language, eliminating the friction common in “bolted-on” commercial suiteS.
1. Clinical records and patient data systems
The core of any EHR is the longitudinal patient record. In a custom build, this goes beyond basic charts to include specialized data fields tailored to your specific medical protocols.
Whether it is tracking complex oncology biomarkers or integrating high-resolution imaging directly into the patient timeline, a custom system ensures that the data clinicians need is exactly where they expect it. This precision reduces charting time and allows for a more focused patient-provider interaction.
2. Scheduling and care coordination workflows
Managing the movement of patients across multiple facilities and departments requires more than a digital calendar. Custom EHRs include intelligent scheduling engines that account for provider availability, room equipment, and patient preparation requirements.
Furthermore, care coordination tools allow different teams, from surgery to post-op recovery, to collaborate in real-time. This synchronization ensures that transitions of care are seamless, reducing the risk of administrative bottlenecks or missed follow-ups.
3. Billing, claims, and revenue systems
Revenue cycle management (RCM) is often where ready-made systems fail due to rigid billing logic. A custom EHR integrates billing directly into the clinical workflow, capturing every billable event as it occurs.
By building a bespoke claims engine, enterprises can automate coding suggestions, verify insurance eligibility instantly, and reduce claim denials. This direct link between clinical action and financial recording ensures a healthier bottom line and a more transparent billing process for patients.
4. Role-based dashboards and access control
An enterprise functions on specialized information. A CFO needs financial KPIs, while a head nurse needs floor-wide patient status updates. Custom platforms utilize sophisticated role-based access control (RBAC) to present specific, actionable dashboards for different user types.
This ensures that every professional sees only the data relevant to their role, which enhances security and prevents information overload. It turns raw data into a strategic tool for every level of the organization.
5. Centralized data and orchestration layer
The most critical, yet often invisible, part of a custom EHR is the orchestration layer. This is the “brain” that connects the EHR to external laboratories, pharmacies, and state health registries.
By using a centralized architecture, the system can process incoming data from various sources and trigger automated actions, such as alerting a doctor to a critical lab result. This layer ensures that the EHR remains an open, scalable hub that can easily adopt new technologies or AI tools as they emerge.
A custom EHR is a comprehensive business asset that integrates clinical precision with financial intelligence. It transforms the way an enterprise operates by providing a unified, high-performance foundation for every department.
Core Components of a Scalable EHR System
A modular architecture ensures that a surge in data volume does not degrade the user experience for clinicians. By isolating the data, logic, and presentation layers, developers can update individual components without risking a total system failure.
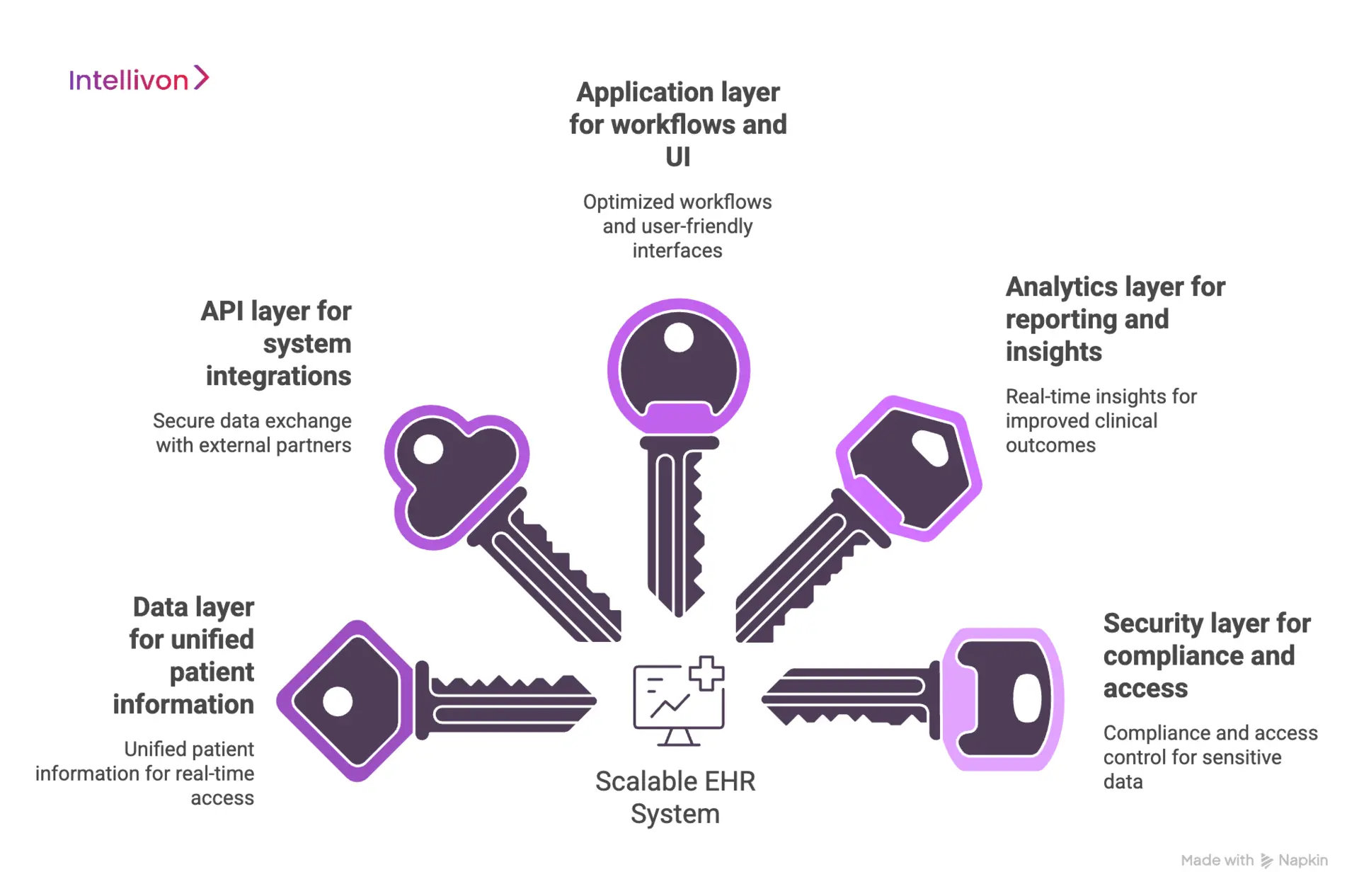
1. Data layer for unified patient information
The foundation of a high-performance EHR is a robust, non-relational or hybrid data store. Traditional databases often struggle with the irregular, unstructured nature of medical notes and high-resolution imaging.
A modern data layer uses a unified schema to aggregate information from disparate sources into a single “golden record.” This approach eliminates duplication and ensures that every department accesses the same real-time patient history.
2. API layer for system integrations
Connectivity is the lifeblood of the modern healthcare ecosystem. A dedicated API layer acts as a sophisticated traffic controller, managing the secure exchange of data between the EHR and external partners like labs or pharmacies.
By strictly adhering to FHIR (Fast Healthcare Interoperability Resources) standards, the system remains future-proof. This layer allows the enterprise to plug in new third-party tools or AI services without rewriting the core codebase.
3. Application layer for workflows and UI
The application layer is where the business logic resides, translating raw data into meaningful clinical actions. In a custom build, this layer is optimized for speed and responsiveness across different devices.
Furthermore, the user interface (UI) is designed around the specific ergonomics of a hospital floor or an outpatient clinic. Consequently, the software feels like a natural extension of the professional’s hand, rather than a digital obstacle.
4. Analytics layer for reporting and insights
Decision-makers need interpreted intelligence. An independent analytics layer processes vast amounts of historical data without slowing down the primary clinical database.
This component powers real-time dashboards that track key performance indicators, such as patient throughput or medication adherence rates. It provides the high-level visibility needed to identify operational waste and improve clinical outcomes across the entire network.
5. Security layer for compliance and access
Security in healthcare is not a feature but a fundamental requirement. A dedicated security layer manages complex encryption protocols, multi-factor authentication, and granular audit logs.
This system ensures that only authorized personnel can access sensitive Protected Health Information (PHI). Moreover, it automates compliance with regional regulations, such as HIPAA or GDPR, by maintaining a transparent and immutable record of every data interaction.
A well-structured EHR architecture provides the stability needed for rapid growth. By investing in these core layers, an enterprise builds a resilient digital backbone that can support thousands of concurrent users across multiple geographic locations.
How Custom EHR Systems Actually Work
The primary function of a high-tier EHR is to orchestrate data movement between the point of care and the administrative back-end. By utilizing a modular framework, a custom system ensures that every clinical action triggers a corresponding operational or financial event in real-time.
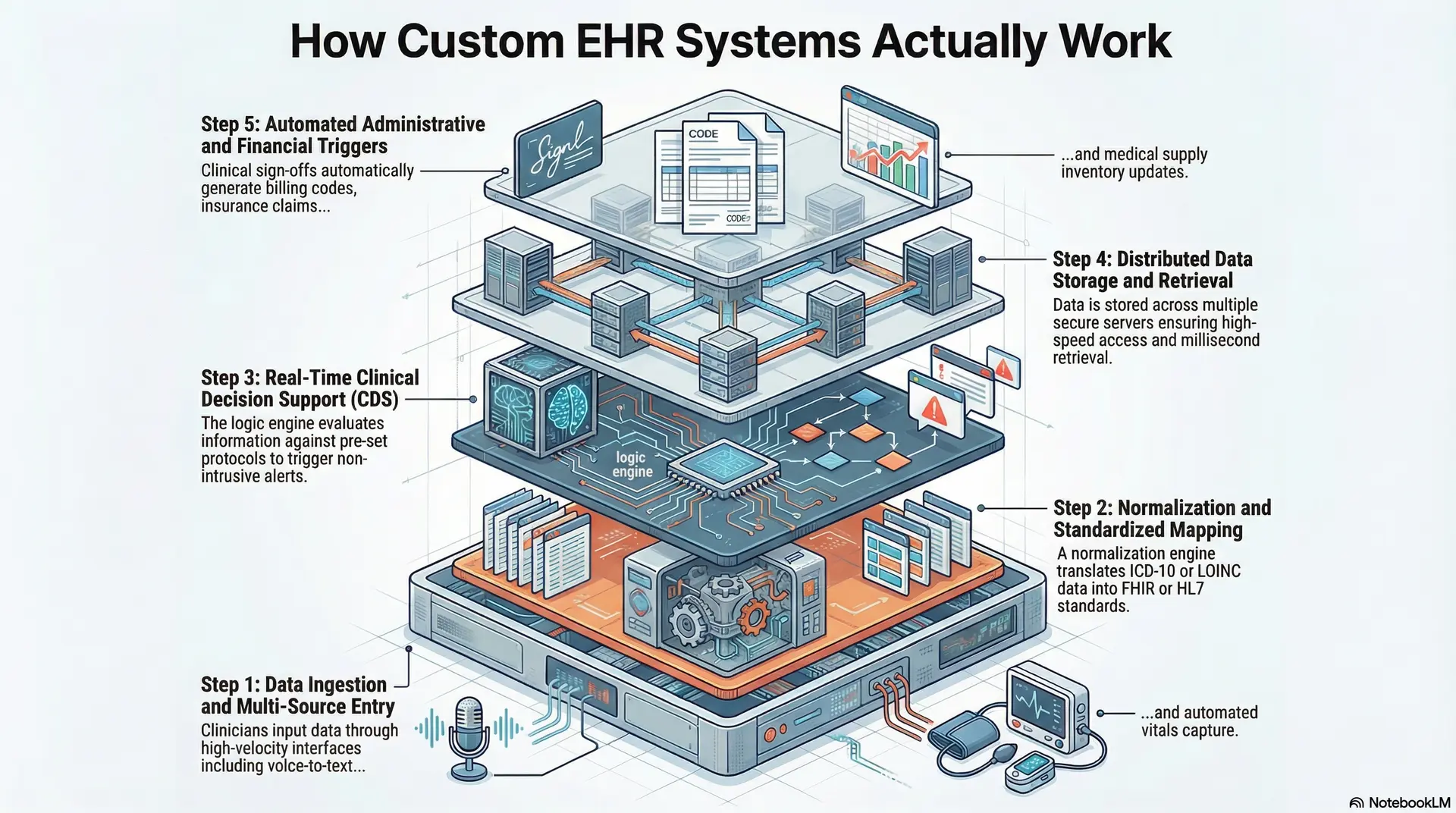
Step 1: Data Ingestion and Multi-Source Entry
The process begins at the point of care, where clinicians input data through specialized, high-velocity interfaces. Unlike generic software, a custom system allows for diverse input methods, including voice-to-text, tablet-based sketching, and automated vitals capture from bedside monitors.
This initial stage ensures that the patient record is populated with high-fidelity information without slowing down the medical professional. Consequently, the system captures a more accurate and comprehensive view of the patient’s status from the very first minute.
Step 2: Normalization and Standardized Mapping
Once data enters the system, the orchestration layer must translate it into a universal format. Healthcare data often arrives in different languages, such as ICD-10 for diagnoses or LOINC for lab results.
A custom EHR uses a normalization engine to map this information to FHIR or HL7 standards automatically. This step is critical because it allows the system to remain “interoperable,” meaning it can share and receive data from any other certified medical platform.
Without this translation, an enterprise remains a collection of disconnected data islands.
Step 3: Real-Time Clinical Decision Support (CDS)
After the data is normalized, the system’s logic engine evaluates the information against pre-set clinical protocols. For example, if a physician prescribes a medication that conflicts with a patient’s known allergy, the EHR triggers an immediate, non-intrusive alert.
This “intelligence layer” operates in the background, providing a safety net that reduces human error. Furthermore, custom systems allow leaders to embed their own unique institutional best practices directly into these automated workflows.
Step 4: Distributed Data Storage and Retrieval
To handle the scale of an enterprise, a custom EHR typically uses a distributed storage model. This means the system stores data across multiple secure servers to ensure that a hardware failure at one location does not result in a total blackout.
When a clinician searches for a record, the retrieval engine locates the data in milliseconds. This high-speed access is essential in emergency departments where every second counts. Proper storage architecture also ensures that large files, such as MRI scans, do not slow down the primary text-based records.
Step 5: Automated Administrative and Financial Triggers
The final step in the cycle is the transition from clinical action to business outcome. As the doctor signs off on a treatment plan, the custom EHR automatically generates the necessary billing codes and insurance claims.
It also updates the inventory for any medical supplies used during the procedure. This automation eliminates the need for a separate “coding” department to manually review every chart. Instead, the system ensures that the revenue cycle remains as fast and accurate as the clinical care provided.
The beauty of a custom EHR lies in its invisible complexity. By managing these steps seamlessly, the system allows healthcare leaders to focus on patient outcomes and business growth rather than technical friction.
Key Integrations in Modern EHR Platforms
The true power of a modern EHR lies not in its standalone features, but in its ability to serve as a central nervous system for the entire healthcare enterprise.
A custom platform excels by creating seamless, real-time links between clinical actions and the vast ecosystem of third-party services that define 21st-century medicine.
1. Lab and diagnostic systems integration
In a standard EHR, lab results often arrive as static PDFs that require manual review and data entry. A custom-integrated system, however, utilizes automated data mapping to ingest results directly into the patient’s digital chart.
This allows for real-time longitudinal tracking of biomarkers and immediate clinician alerts for critical values. Furthermore, by automating the “order-to-result” loop, enterprises can significantly reduce turnaround times and eliminate the administrative errors that occur during manual transcription.
2. Pharmacy and prescription systems
Modern prescribing requires a direct link to Pharmacy Benefit Managers (PBM) and retail pharmacy networks to ensure patient safety and cost-effectiveness.
Custom integrations enable real-time “Electronic Prior Authorization” (ePA) and instant drug-drug interaction checks against the patient’s full history. Consequently, clinicians can see out-of-pocket costs for patients at the point of care, which improves medication adherence.
This level of connectivity transforms the prescription process from a simple order into a data-driven clinical intervention.
3. Insurance and claims platforms
Revenue leakage often stems from the gap between clinical documentation and insurance adjudication. By integrating directly with payer portals and claims clearinghouses, a custom EHR can perform real-time eligibility verification before the patient even sees a doctor.
Instead of waiting weeks for a denial, the system flags coding inconsistencies or missing documentation instantly. This “clean claim” approach accelerates the reimbursement cycle and reduces the burden on your billing department, directly impacting the organization’s bottom line.
4. Remote monitoring and IoT devices
The hospital of the future extends into the patient’s home via the Internet of Medical Things (IoMT). Custom EHRs are built to handle the continuous stream of data from wearable heart monitors, glucose sensors, and smart scales.
Rather than overwhelming clinicians with raw data, the integration layer uses “edge analytics” to filter for anomalies and only alert care teams when a patient’s vitals trend outside of safe parameters. This proactive monitoring allows for early intervention, reducing hospital readmission rates and improving chronic disease management.
5. External EHR and hospital systems
Enterprises frequently operate in a multi-vendor environment where they must exchange data with outside specialists or public health registries. While generic platforms often charge “data tax” for these exchanges, a custom build utilizes open standards like HL7 and FHIR to ensure seamless interoperability.
This allows for a “CommonWell” or “Carequality” style connection, where a patient’s records follow them regardless of the facility they visit. Achieving this level of transparency is essential for high-stakes care coordination and population health management.
Strategic integrations turn an EHR from a digital record into a proactive healthcare engine. By connecting every facet of the medical ecosystem, an enterprise ensures its technology works as hard as its clinical teams to deliver superior care.
AI in Custom EHR Systems
The strategic advantage of a custom EHR lies in its ability to leverage “Native AI” across every layer of the patient journey.
By embedding machine learning models directly into the database architecture, organizations can achieve a level of automation that generic, third-party plug-ins simply cannot match.
1. Clinical decision support systems
Standard decision support often relies on rigid, rule-based alerts that lead to “alarm fatigue” for busy clinicians. In a custom EHR, AI-driven support systems analyze a patient’s full longitudinal history, including genomics and social determinants of health, to provide highly nuanced recommendations.
Consequently, the system only alerts the physician when a specific, high-risk deviation occurs, such as a subtle trend toward sepsis. This precision ensures that the technology acts as an expert consultant rather than a digital nuisance.
2. Automated documentation and note creation
Physician burnout is frequently tied to the “pajama time” spent on manual data entry after hours. Custom platforms integrate ambient voice recognition and Natural Language Processing (NLP) to capture clinician-patient conversations in real-time.
The AI automatically parses these dialogues into structured SOAP notes, extracting discrete data points for the patient’s record. Instead of typing for hours, the provider simply reviews and signs off on the generated content. This shift restores the human element to the medical encounter and drastically increases daily patient throughput.
3. Predictive analytics for patient outcomes
The ability to foresee a medical crisis before it manifests is the “holy grail” of population health management. Custom EHRs utilize predictive modeling to scan thousands of data points across the enterprise to identify patients at high risk for readmission or chronic disease escalation.
These models provide actionable “risk scores” that allow care coordination teams to intervene early with preventative measures. Furthermore, because the AI is trained on your organization’s specific patient demographic, its accuracy far exceeds that of generalized industry models.
4. Workflow automation and prioritization
In a high-volume hospital, deciding which task to tackle next is often a chaotic process. AI-integrated EHRs act as an intelligent air-traffic controller, prioritizing nurse task lists and physician rounds based on real-time acuity data.
For instance, if a lab result indicates a critical electrolyte imbalance, the system automatically elevates that patient to the top of the care team’s dashboard. This dynamic prioritization ensures that resources are always deployed where they are needed most, reducing wait times and improving overall safety.
5. Revenue cycle intelligence and optimization
Financial leakage is often the result of “human-in-the-loop” errors during complex coding and billing processes. Custom AI modules perform “autonomous coding” by scanning clinical notes and mapping them to the most accurate, high-reimbursement ICD-10 and CPT codes.
Additionally, the system uses predictive algorithms to identify which insurance claims are likely to be denied before they are even submitted.
This allows the billing team to correct issues proactively, significantly reducing the “Days in Sales Outstanding” (DSO) and stabilizing the enterprise’s cash flow.
Integrating AI into a custom EHR is a move from reactive management to predictive excellence. It empowers healthcare leaders to make data-driven decisions that enhance both clinical outcomes and the organization’s long-term financial health.
Use Cases of Custom EHR in Healthcare
Strategic leaders deploy custom EHRs when the “median” functionality of commercial software creates a barrier to expansion. By building for specific use cases, organizations can capture market share and deliver superior patient outcomes that standardized tools cannot support.
1. Multi-specialty hospital systems
Managing a network that includes everything from cardiology to labor and delivery requires a unified but flexible digital core. A custom EHR allows each department to have its own tailored interface while sharing a centralized patient record.
Consequently, a surgeon in the OR can see real-time updates from a consultation in the neurology wing without switching between fragmented modules.
2. Telehealth and remote care platforms
Virtual care requires more than just a video link; it needs a system that integrates scheduling, digital consenting, and asynchronous messaging into the clinical record. Custom builds allow for a “digital-first” patient journey, where AI-driven intake forms prepare the clinician before the call begins.
This seamless integration ensures that telehealth is a core part of the care continuum rather than a detached service.
3. Value-based care delivery models
In a value-based model, profitability depends on managing patient risk and outcomes rather than the volume of services. Custom EHRs integrate HEDIS and MIPS tracking directly into the workflow, alerting clinicians to care gaps in real-time.
Instead of retroactive reporting, the system proactively guides the care team toward the most cost-effective and clinically sound interventions.
4. Chronic care and monitoring programs
Managing long-term illnesses like diabetes or hypertension requires continuous data loops from wearable devices. A custom platform automates the ingestion of this data, using “exception-based” alerting to notify care managers only when a patient’s trends become dangerous.
This allows a small team of coordinators to manage thousands of high-risk patients efficiently, reducing emergency room visits and hospital readmissions.
5. Specialty clinics with complex workflows
Fertility clinics, oncology centers, and behavioral health facilities have highly specific regulatory and documentation needs. Custom software reflects these exact protocols, such as cycle tracking or complex chemotherapy dosing, with high-fidelity accuracy.
By removing the “noise” of irrelevant fields found in generic systems, specialty teams can focus entirely on the nuances of their specific medical field.
A custom EHR is the ultimate tool for a healthcare enterprise that refuses to be constrained by average technology. It provides the architectural freedom to lead the market in specialized, high-impact care delivery.
Architecture Behind Enterprise EHR Systems
High-performance healthcare operations depend on an underlying architecture that can process millions of data points without latency. For an enterprise, the “bones” of the system determine whether the platform will be a strategic asset or a constant technical bottleneck.
1. API-first architecture explained
An “API-first” approach means the system is designed from day one to talk to other software. Instead of building a closed box, developers create secure “gateways” that allow external apps, labs, and insurance payers to exchange data instantly.
This modularity ensures that your EHR is never isolated. It functions as a hub that can easily integrate with the latest diagnostic tools or remote monitoring devices. For a business leader, this means your technology investment remains “future-proof” as the medical ecosystem evolves.
2. Cloud-native deployment models
Deploying an EHR “in the cloud” (via AWS, Azure, or Google Cloud) offers a level of security and scalability that on-premise servers cannot match. Cloud-native systems use “auto-scaling,” which automatically adds computing power during busy morning rounds and scales back at night to save costs.
Furthermore, cloud providers offer geographically redundant backups, ensuring that a natural disaster at one location doesn’t result in the loss of critical patient records. This model shifts the burden of hardware maintenance away from your internal team, allowing them to focus on innovation.
3. HL7 and FHIR interoperability standards
Interoperability is the ability of different health systems to share and understand data. HL7 (Health Level Seven) and the newer FHIR (Fast Healthcare Interoperability Resources) are the universal languages of medical data.
A custom EHR built on these standards ensures that a patient’s record from a local clinic can be perfectly read by a specialist in your network. This “data liquidity” eliminates the need for faxing records or manual data entry. It creates a seamless experience for both the patient and the provider, which is essential for high-quality care coordination.
4. Designing for scale and uptime
At the enterprise level, “downtime” is not just a technical issue; it is a clinical risk and a financial disaster. Designing for scale involves using “load balancers” to distribute user traffic evenly across servers, preventing any single point of failure.
Additionally, custom systems utilize “stateless architecture,” which allows users to stay logged in even if their connection switches between different data centers. This focus on 99.99% uptime ensures that your clinicians always have access to life-saving information, regardless of the system load or external network conditions.
A robust architecture is the invisible engine of enterprise success. By prioritizing microservices and open standards, healthcare leaders ensure their organization operates on a foundation of stability, security, and limitless scalability.
Cost of Custom vs Ready-Made EHR in 2026
Evaluating the investment requires a move beyond simple procurement metrics. An enterprise must weigh the immediate savings of a subscription against the compounding costs of technical debt and restricted scalability that often accompany off-the-shelf products.
Why does ready-made look cheaper upfront?
Ready-made solutions attract decision-makers with low initial capital requirements. The “as-a-service” model allows organizations to shift costs to OpEx, often starting at just a few thousand dollars per month.
These vendors provide a pre-built infrastructure, which drastically reduces the time and money spent on the initial design phase. For a smaller clinic, this is a logical entry point. However, for an enterprise, this “speed to market” often masks a lack of depth in specialized clinical workflows.
What custom EHR development costs include
Building a bespoke platform is a significant capital investment that covers much more than just coding. A professional enterprise build includes:
- Discovery and Workflow Mapping: 15–20% of the budget is spent ensuring the software mirrors your exact clinical protocols.
- Architectural Engineering: Building a scalable, microservices-based foundation that handles thousands of concurrent users.
- Compliance and Security Hardening: Native integration of HIPAA, GDPR, and FHIR standards from the ground up.
- Quality Assurance: Rigorous testing cycles to ensure 99.99% uptime in high-stakes medical environments.
Hidden costs in licensing and scaling
The “hidden” financial burden of ready-made EHRs lies in their scaling logic. Most vendors charge per user, per month, which means your software bill grows as your company succeeds. Furthermore, any deviation from the “standard” setup results in heavy professional service fees.
- The Integration Tax: Connecting a ready-made EHR to a new lab or pharmacy often requires paid “connectors” or expensive middleware.
- The Customization Trap: Modifying a fixed platform is often more expensive than building from scratch because developers must work around proprietary restrictions.
- Data Access Fees: Some vendors charge for high-volume data exports, effectively making you pay to access your own institutional intelligence.
ROI comparison over time
The return on investment for a custom EHR is found in operational efficiency and the elimination of recurring fees. While the first year is expensive, the subsequent years see a dramatic drop in costs.
| Feature | Ready-Made (SaaS) | Custom Built |
| Upfront Cost | Low ($20k – $100k) | High ($600k – $1.5M+) |
| Scaling Cost | Increases per user/site | Flat (Infrastructure only) |
| Integration | Paid “Add-ons” | Native & Unlimited |
| Ownership | Vendor-owned IP | Enterprise-owned IP |
| Maintenance | Included (Fixed Roadmap) | 15–20% of Build (Your Roadmap) |
Year 1-2: Ready-made systems appear more cost-effective due to lower initial spend.- Year 3: The “Crossover Point”, where cumulative licensing and integration fees often begin to exceed the cost of the custom build.
- Year 5+: Custom owners enjoy a significantly lower TCO, as they are not penalized for growth and can pivot their technology without vendor permission.
Strategic budgeting in 2026 demands a long-term view. While ready-made systems solve for “now,” a custom EHR is a financial and operational hedge against the future, turning a necessary expense into a powerful, proprietary business asset.
How We Develop Custom EHR Platforms for Enterprises
Developing an enterprise-grade EHR is a high-stakes engineering feat that requires a blend of clinical insight and technical rigor. At Intellivon, we have refined a battle-tested methodology that ensures your platform is not just functional but a strategic driver of institutional growth.
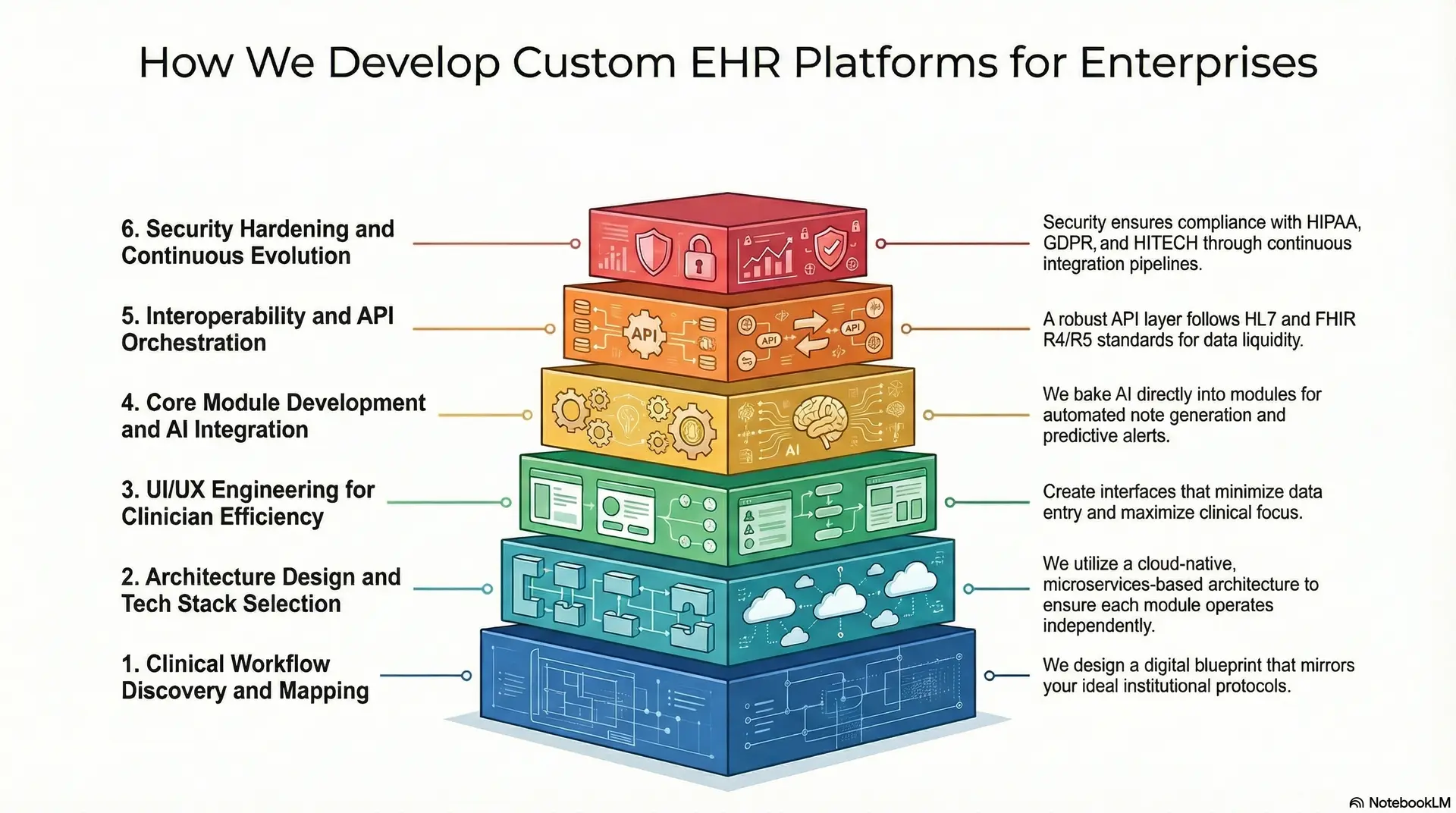
Step 1: Clinical Workflow Discovery and Mapping
We begin by embedding our analysts into your clinical environment to observe the “unspoken” nuances of your daily operations.
At this stage, we map the actual movement of patients, data, and decision-making across departments. By identifying current bottlenecks, we design a digital blueprint that mirrors your ideal institutional protocols.
Step 2: Architecture Design and Tech Stack Selection
Scaling an enterprise requires a foundation that can handle millions of concurrent transactions. We utilize a cloud-native, microservices-based architecture (using AWS, Azure, or Google Cloud) to ensure each module operates independently.
This “decoupled” approach allows us to update your billing engine or patient portal without ever risking a total system blackout.
Step 3: UI/UX Engineering for Clinician Efficiency
A common failure in EHR design is “click fatigue.” Our design team focuses on high-velocity ergonomics, creating interfaces that minimize data entry and maximize clinical focus.
We prioritize “one-click” actions and intuitive dashboards that adapt to different roles, ensuring that a surgeon, a nurse, and a billing clerk each have a specialized view optimized for their specific tasks.
Step 4: Core Module Development and AI Integration
During the build phase, we develop the primary clinical, administrative, and financial engines in parallel. Unlike standard systems, we bake AI and machine learning directly into these modules.
This enables features like automated SOAP note generation, predictive sepsis alerts, and autonomous medical coding, turning the EHR into a proactive assistant rather than a static database.
Step 5: Interoperability and API Orchestration
A modern EHR must communicate fluently with the outside world. We build a robust API layer strictly following HL7 and FHIR R4/R5 standards. This ensures your platform can instantly exchange data with labs, pharmacies, imaging centers, and government registries.
At Intellivon, we prioritize “bi-directional data liquidity,” meaning your system stays at the center of the healthcare ecosystem.
Step 6: Security Hardening and Compliance Auditing
Security is not an afterthought in our process. We implement end-to-end encryption, multi-factor authentication (MFA), and granular role-based access control (RBAC).
Before any code is deployed, it undergoes rigorous vulnerability scanning and third-party compliance audits to ensure it meets or exceeds HIPAA, GDPR, and HITECH requirements.
Step 7: Deployment, Training, and Continuous Evolution
The final step is a phased rollout designed to minimize operational disruption. We provide comprehensive training for your staff and stay on-site during the “Go-Live” period to ensure a smooth transition.
Post-launch, we maintain a continuous integration (CI/CD) pipeline, allowing your platform to evolve with new medical breakthroughs and shifting regulatory demands.
At Intellivon, we build the digital future of your healthcare enterprise. Our process ensures that your custom EHR is a proprietary asset that provides a permanent competitive advantage and a superior standard of care.
Conclusion
Choosing between custom and ready-made EHR systems is not just about cost or speed. It is about building a system that supports how your organization delivers care today and scales tomorrow.
While ready-made platforms work in the short term, their limits become clear with growth. Custom EHR platforms provide control, flexibility, and long-term value, making them the better choice for enterprises planning to scale efficiently.
Build the Right EHR Platform With Intellivon
At Intellivon, EHR platforms are built as enterprise healthcare infrastructure, not as software layered onto fragmented systems. The goal is to create a unified platform that connects clinical workflows, operational processes, and data systems into one scalable environment.
Each solution is designed around how your organization actually operates. This includes clinical documentation, scheduling, billing, integrations, analytics, and automation, all aligned within a single architecture. As a result, teams reduce manual effort, improve coordination, and gain real-time visibility across departments.
Our approach focuses on AI-first, API-driven systems combined with interoperability standards like HL7 and FHIR. This ensures seamless integration with labs, pharmacies, insurers, devices, and existing EHR systems without disrupting ongoing operations.
Why Intellivon for Custom EHR Development
- Architecture-first approach: We design systems for long-term scale, not short-term fixes, ensuring your platform supports growth from day one.
- Workflow-driven development: Every system is built around your clinical and operational workflows, not forced into predefined templates.
- Seamless interoperability: We enable real-time data exchange across healthcare systems using HL7, FHIR, and modern API frameworks.
- Built for scale and performance: Our platforms support multi-location operations, high data volumes, and complex care models without performance trade-offs.
- Continuous evolution and support: We ensure your EHR system evolves with new requirements, technologies, and regulatory changes over time.
If you are evaluating whether to build or move beyond your current EHR, Intellivon helps you design and develop a platform that fits your operations today and scales with your future growth.
FAQs
Q1. What is custom vs ready-made EHR?
A1. A custom EHR is built specifically for an organization’s workflows, integrations, and data needs. In contrast, a ready-made EHR is a pre-built system with standard features designed for general use. While ready-made systems offer faster setup, custom EHR platforms provide better workflow alignment, deeper integrations, and long-term flexibility.
Q2. Is custom EHR better for large systems?
A2. Yes, custom EHR systems are often better suited for large healthcare organizations. This is because they support complex workflows, multi-location operations, and extensive integrations. As organizations scale, custom platforms provide greater control over data, processes, and system performance compared to ready-made solutions.
Q3. How long does a custom EHR take to build?
A3. Custom EHR development typically takes between 6 and 12 months, depending on system complexity, integrations, and feature requirements. Larger enterprise platforms with advanced workflows, AI features, and multiple integrations may take longer to design, develop, and deploy.
Q4. Is a ready-made EHR cheaper long term?
A4. Ready-made EHR systems may appear cheaper initially due to lower upfront costs. However, over time, recurring license fees, upgrade costs, and integration limitations can increase total expenses. Custom EHR platforms require a higher initial investment but often deliver better long-term value through scalability and reduced dependency on vendors.
Q5. Can a custom EHR integrate existing systems?
A5. Yes, custom EHR platforms are designed to integrate seamlessly with existing systems such as labs, pharmacies, insurance platforms, and other EHRs. Using standards like HL7 and FHIR, custom solutions enable real-time data exchange, ensuring better interoperability and coordinated care across systems.