Healthcare systems have long been built around departments, so patient data often stayed siloed within separate units, and this structure could slow clinical decisions and gradually affect care quality. As healthcare moves toward integrated and value-based models, the need for connected systems becomes more evident.
Many institutions have begun implementing EHR systems in healthcare ecosystems to improve coordination and real-time access to patient data. EHR systems can unify records across departments and reduce duplication, while workflows become more aligned, supporting more consistent data-driven patient care.
Over the years, we’ve implemented EHR systems for several healthcare institutions, using technologies like healthcare interoperability frameworks and clinical data intelligence systems. As we have this expertise, we’re sharing this blog to discuss how to implement EHR in healthcare ecosystems.
Why EHR Is Now Core to Digital Healthcare Growth?
According to Grand View Research, the global electronic health records market size was estimated at USD 35.89 billion in 2025 and is projected to reach USD 53.11 billion by 2033, growing at a CAGR of 5.10% from 2026 to 2033. This growth reflects a fundamental shift in healthcare digitization. For a strategic investor, an EHR platform is now the central nervous system of a modern medical facility.
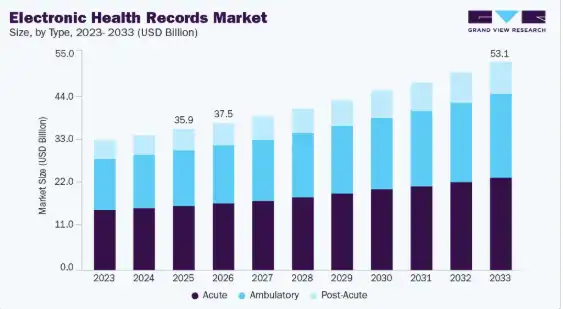
Source: Grand View Research
Market expansion is driven by value-based care models where reimbursement depends on patient outcomes. Providers require a digital infrastructure that aggregates data from sources like wearables and diagnostic labs.
Modern EHRs are innovation platforms. They integrate AI for predictive analytics, streamlined billing, and patient engagement. As the industry transforms, the EHR serves as the foundation for all health-tech development.
Shifting from Silos to Connected Care
Historically, Electronic Medical Records (EMRs) were digital versions of paper charts restricted to single practices. These silos prevented information from following patients across different care settings. Today, demand has shifted toward interoperable systems that facilitate connected care.
Entrepreneurs can solve this fragmentation by using FHIR standards. This ensures data is accessible to primary care, specialists, and emergency rooms simultaneously. Kaiser Permanente proved this value with their “HealthConnect” system, which decreased hip fractures by 37% through proactive screening and improved member retention.
Demand for Real-Time Data Access
Delayed information is a barrier to quality care. Clinicians need immediate lab results for life-saving decisions, and patients expect the same transparency they find in banking.
Strategic investment focuses on:
- Edge Computing: Processing data at the source to reduce latency.
- Mobile Architectures: Secure tablet and smartphone access for providers.
- API Ecosystems: Allowing third-party apps to sync real-time data.
Providing this immediacy positions a platform as a premium solution. In modern healthcare, delayed data is a liability.
Impact on Quality and Revenue
A sophisticated EHR platform influences both clinical outcomes and financial health. Integrated decision support tools alert doctors to drug interactions, elevating the standard of care.
Mayo Clinic showcased this power through a modernization project that reduced hospital-acquired conditions by 30%. It also generated a $300 million revenue increase through improved billing capture and documentation efficiency.
The EHR drives financial efficiency by automating the documentation-to-coding pipeline:
- Precision Billing: Automated coding reduces human error.
- Resource Optimization: Analytics identify bottlenecks to improve staffing.
- Reduced Liability: Detailed documentation defends against malpractice claims.
For an investor, an EHR that optimizes revenue while improving care is a high-ROI transformation tool.
Business Benefits of EHR Implementation in Healthcare
An integrated EHR ecosystem transforms a healthcare provider into a proactive, data-driven enterprise. By centralizing disparate workflows, organizations eliminate the fragmentation that leads to revenue leakage and clinical errors.
A robust EHR supports both high-volume patient throughput and high-margin specialized care within a single framework.
1. Scaling Operational Efficiency
Inefficiency in large networks often stems from manual data entry and fragmented communication. A unified EHR automates routine tasks, allowing staff to focus on higher-value clinical activities.
Geisinger Health serves as a benchmark for this efficiency. By integrating their EHR with a unified patient identification system, they achieved a 98% data match rate. This allowed them to reallocate five full-time employees from manual record cleanup to higher-value clinical support roles, significantly reducing operational overhead.
- Automated Scheduling: Integration with portals reduces no-show rates.
- Lab Integration: Eliminating manual requests speeds up diagnostics by 20% to 30%.
- Standardized Workflows: Unified protocols reduce variance in care and processing.
2. Improving Retention and Satisfaction
Patient loyalty is now a critical metric for healthcare profitability. Modern EHRs improve the consumer experience by providing frictionless access to personal health data.
Intermountain Health optimized this by integrating its Epic EHR with AI-powered communication tools. This allowed patients to resolve 79% of inquiries through self-service portals. The result was an 85% drop in call abandonment rates, directly correlating to higher patient satisfaction and retention.
When patients can view results and message doctors through one interface, engagement rises. High engagement reduces the high cost of patient acquisition for the practice.
3. Enabling Data-Driven Decisions
Data is the most valuable asset in a healthcare ecosystem. A robust EHR provides the analytics needed to identify trends across a population, allowing for:
- Risk Stratification: Identifying high-risk patients before they require emergency care.
- Predictive Staffing: Using flow data to adjust staffing levels and reduce overtime.
- Clinical Research: Aggregating data can create secondary revenue streams through partnerships.
4. Lowering Administrative Costs
While the initial investment is significant, the long-term reduction in manual processing costs is substantial. Facilities save on physical storage, transcriptions, and filing.
More importantly, reducing billing errors ensures the organization captures more revenue for work already performed. Over a 5-year horizon, these savings often exceed the total cost of ownership of the software.
Types of EHR Systems You Can Implement
Integrating the right EHR architecture is a high-stakes decision for any investor looking to build EHR-powered healthcare ecosystems. The choice of system determines the ecosystem’s long-term agility and the cost of maintaining data integrity across a network of providers.
1. Cloud vs On-Premise Platforms
The choice between cloud and on-premise involves a trade off between institutional control and rapid scalability. Most modern digital health entrepreneurs lean toward cloud integration for its lower entry barriers.
| Integration Factor | Cloud-Based (SaaS) | On-Premise |
| Speed to Live | Weeks via web-based APIs | Months; requires physical install |
| Security | Managed by vendor (HIPAA) | Internal IT responsibility |
| Accessibility | Global via secure internet | Restricted to local network |
| Scalability | Near-instant seat expansion | Limited by server capacity |
The Strategic Play: Cloud systems are superior for scaling rapidly across multiple geographical sites. However, large tertiary care centers with extensive legacy infrastructure often require on-premise integration to maintain total data sovereignty and comply with specific local regulations.
2. Specialty-Specific vs General Systems
General EHR systems aim for broad utility, covering everything from pediatrics to geriatrics. While these offer a unified data structure, they often suffer from feature bloat that can alienate specialized clinicians.
Industry Insight:
A cardiologist has data requirements, such as high-resolution imaging and EKG integration that are irrelevant to a mental health professional. Specialty-specific EHRs focus on these niche templates and specific insurance reimbursement codes.
For an investor, integrating a specialty-specific system like Modernizing Medicine for dermatology or Zenoti for medical spas can yield a higher ROI.
Specialists often prefer systems that reduce their documentation time by speaking their specific clinical language.
3. Integrated Systems vs Standalone Apps
When designing a healthcare ecosystem, you must decide if you are integrating an all-in-one hub or a best-of-breed suite of specialized tools.
- Monolithic Integrated Systems: Platforms like Epic or Cerner handle clinical records, billing, and pharmacy in one package. They offer a single source of truth but are notoriously difficult and expensive to weave into a smaller, agile ecosystem.
- Standalone Specialized Apps: This is where modern innovation thrives. Instead of one giant system, you integrate specialized modules such as a remote patient monitoring tool or an AI-driven triage app into a lightweight core via APIs.
Recommendation for Investors: Unless you are managing a massive multi-state hospital group, the modular approach is often more cost-effective.
By integrating high-value standalone applications that solve specific pain points, you create a flexible ecosystem that can evolve as medical technology advances.
Must-Have Features in a Scalable EHR System
To build competitive EHR-powered healthcare ecosystems, you must prioritize features that solve actual clinical friction. A scalable system does not just store data; it translates that data into a streamlined workflow for the provider and a better experience for the patient.
1. Unified Records And Timeline View
A fragmented history is a risk to patient safety. A unified record aggregates data from every touchpoint, including consultations, surgeries, and immunizations, into a single longitudinal view.
Cleveland Clinic, for instance, utilized this unified approach to gain a 360-degree view of patient health across its global locations. By centralizing records, they reduced duplicate testing by 15% and ensured that a patient visiting their London facility had the same data profile as one in Ohio.
A chronological timeline allows clinicians to see trends in a patient’s health at a glance. Instead of digging through digital folders, a doctor can visualize how a specific chronic condition has progressed over several years. This leads to faster and more accurate diagnoses.
2. EPrescriptions And Medication Tracking
Manual prescriptions are prone to errors and pharmacy delays. Integrated ePrescription modules allow doctors to send orders directly to a patient’s preferred pharmacy.
For example, CVS Health integrated its pharmacy management systems with EHR provider networks to streamline this exact process. This integration allowed for real-time prescription fill alerts, helping providers identify non-adherent patients immediately.
Beyond convenience, these tools track medication adherence. They automatically check for potential drug to drug or drug-to-allergy interactions. This proactive safety layer is a non-negotiable requirement for any modern healthcare ecosystem.
3. Lab And Diagnostic Integrations
Efficiency is lost when staff must manually upload lab results. A scalable EHR integrates directly with Laboratory Information Systems (LIS) and imaging centers.
- Automatic Sync: Results flow into the patient record the moment they are verified.
- Abnormal Value Alerts: The system flags critical results to ensure immediate follow-up.
- Trend Analysis: Providers can graph lab values over time to monitor the effectiveness of a treatment plan.
4. Decision Support And Clinical Alerts
Clinical Decision Support acts as an intelligent assistant for the physician. It uses data-driven algorithms to provide real-time alerts and evidence-based recommendations during the patient encounter.
Mount Sinai Health System implemented advanced CDS alerts within its EHR to target sepsis, a leading cause of hospital mortality. The system analyzed vitals in real time and alerted clinicians to early warning signs. This intervention led to a 40% reduction in sepsis-related deaths within their facilities.
- Preventive Care Alerts: Reminds the doctor if a patient is due for a screening or vaccination.
- Protocol Guidance: Suggests the latest clinical pathways for specific diagnoses.
- Risk Assessment: Flags patients who show early indicators of high-risk conditions like sepsis or heart failure.
5. Billing And Revenue Cycle Tools
An EHR must be as proficient at business as it is at medicine. Integrated RCM ensures that clinical work is translated into financial claims without delay.
By utilizing automated coding tools, the system maps clinical notes to the correct ICD-10 and CPT codes. This reduces upcoding risks and downcoding revenue loss. Integrated billing also allows for real-time insurance eligibility checks to ensure the facility gets paid for the services it provides.
6. Role-Based Access And Permissions
Data security is a legal and ethical mandate. In a large ecosystem, not every user needs access to every data point. Role-based access control ensures that access is granted based on necessity.
- Nurses and Medics: Access to vitals and medication administration records.
- Billing Staff: Access to financial and demographic data but not clinical notes.
- Administrators: Access to high-level reporting and audit logs.
Strict permissioning protects patient privacy and ensures compliance with global standards like HIPAA or GDPR. This protects your investment from costly legal exposure.
How to Implement EHR in a Healthcare Ecosystem?
Implementing an EHR in a healthcare ecosystem starts with establishing interoperable data layers so systems can securely exchange clinical information. It should then gradually standardize workflows and may integrate real-time processing so care delivery becomes more consistent and efficient.
We’ve supported several healthcare providers in building EHR-integrated ecosystems, and here is the approach followed.
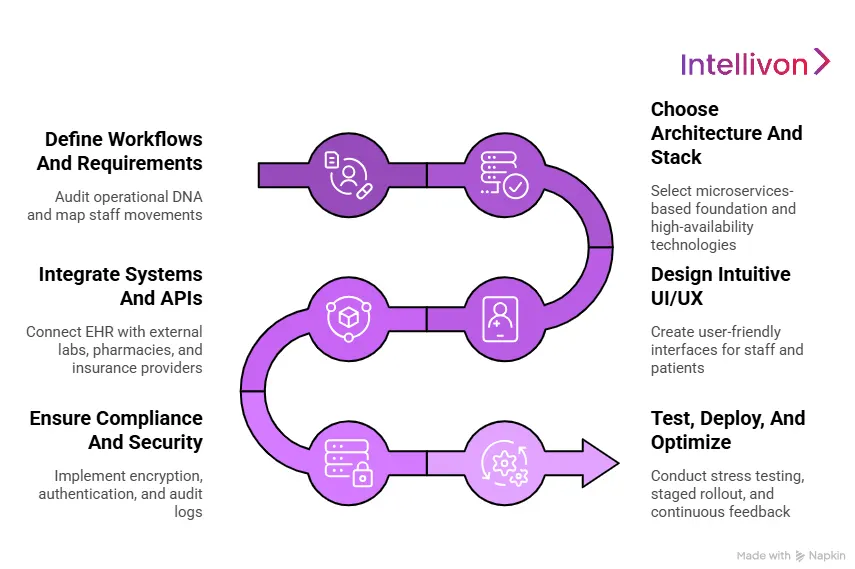
1. Define Workflows And Requirements
We begin by auditing your operational DNA. Our team maps the precise movements of your doctors, nurses, and staff to identify bottlenecks in patient intake and discharge. By defining requirements based on real-world behavior, we ensure the ecosystem solves genuine friction rather than adding digital overhead.
2. Choose Architecture And Stack
We build for the future. Our architects select a microservices-based foundation that handles millions of records without latency. We prioritize technologies that support high availability, ensuring your ecosystem remains responsive and reliable even during peak hospital hours or rapid network expansion.
3. Design Intuitive UI/UX
User experience is a clinical safety requirement. We design interfaces that eliminate alert fatigue by prioritizing critical data points like vitals and allergies. For your patients, we create frictionless portals that make navigating medical histories and scheduling as simple as modern banking.
4. Integrate Systems And APIs
We ensure your EHR does not exist in a silo. Our engineers integrate your core platform with external labs, pharmacies, and insurance providers via secure, industry-standard APIs. By leveraging FHIR and HL7 protocols, we transform standalone records into a fully connected healthcare marketplace.
5. Ensure Compliance And Security
Security is the cornerstone of institutional trust. We implement end-to-end encryption, multi-factor authentication, and comprehensive audit logs. Our rigorous approach ensures your ecosystem meets or exceeds global standards like HIPAA and GDPR, protecting you from legal and financial risk.
6. Test, Deploy, And Optimize
We move from staging to production with surgical precision. After rigorous stress testing in simulated environments, we manage a staged rollout to minimize service disruption. Post-deployment, we establish a continuous feedback loop with your staff to refine features and optimize performance based on live clinical data.
Cost to Implement EHR in Healthcare Ecosystem
The financial roadmap for an EHR implementation is rarely linear. While a basic setup can be cost-effective, a high-performance ecosystem that supports real-time data exchange and advanced clinical tools requires a more significant commitment. Here is how we break down the financial landscape in USD.
Core Drivers In EHR Development
The primary drivers of your budget are the complexity of clinical workflows and the choice of deployment. Building a custom ecosystem offers more control but carries higher initial development costs compared to integrating a licensed SaaS platform.
- Software Development: For custom builds, expect $150,000 to $500,000 for an initial enterprise-grade version. Licensing for a pre-built SaaS typically ranges from $200 to $700 per provider per month.
- Engineering Talent: Skilled healthcare developers, including API experts, security specialists, and UI/UX designers, typically cost $100 to $180 per hour for US-based teams.
- Infrastructure: Cloud hosting on platforms like AWS or Azure usually costs $1,000 to $10,000 per month, depending on data volume.
Cost By Features And Scale
As you move from a single clinic to a multi-facility ecosystem, costs scale alongside the complexity of the integrations. Each node added to the network, whether a pharmacy, a lab, or a third-party billing app, requires dedicated engineering.
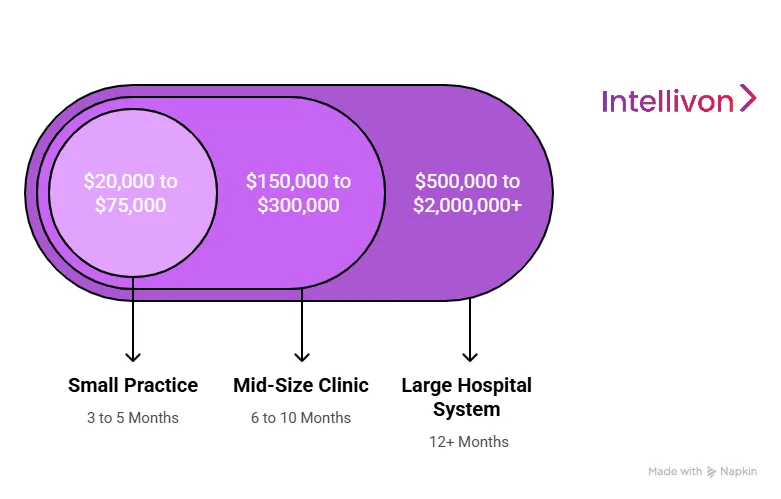
| Scale / Type | Estimated Cost Range (USD) | Deployment Time |
| Small Practice (1 to 5 Providers) | $20,000 to $75,000 | 3 to 5 Months |
| Mid-Size Clinic (up to 25 Providers) | $150,000 to $300,000 | 6 to 10 Months |
| Large Hospital System | $500,000 to $2M+ | 12+ Months |
| Specialty Modules (e.g., Oncology) | $10,000 to $50,000 (each) | Varies |
Budget Planning And Hidden Factors
The sticker price of an EHR is often just the beginning. We advise our clients to budget an additional 15% to 20% of the initial cost for the first year of maintenance and support.
Investor Note: One of the highest hidden costs is Data Migration. Moving years of messy legacy records into a structured new system can cost between $5,000 and $25,000 for mid-sized setups, potentially reaching six figures for large hospital networks.
Other silent budget eaters include staff training, which can cost $1,000 to $5,000 per employee, and the productivity dip during the first few weeks of the go-live phase. By planning for these variables early, we help you avoid mid-project funding gaps and ensure a smoother path to ROI.
Designing Patient-Centric EHR Experiences
To build EHR-centric healthcare ecosystems, we shift the focus from data entry to data empowerment. A successful ecosystem relies on two pillars: patient accessibility and clinician efficiency. Our design philosophy prioritizes clarity and speed to drive high adoption across your organization.
1. Patient Data Access
Modern healthcare centers on the patient’s right to their data. We design secure, user-friendly portals for viewing medical history, lab results, and immunizations in real time.
Kaiser Permanente proved the value of this approach by achieving high patient portal enrollment, which significantly improved health outcomes for patients with chronic conditions like diabetes.
Instead of using complex jargon, we use data visualization to help patients understand health trends. Seeing a three-year graph of cholesterol levels makes a patient more likely to adhere to treatment plans and engage in preventative care.
2. Intuitive Clinician Dashboards
Clinician burnout often stems from interfaces that require too many clicks. Our dashboard design focuses on cognitive load reduction, surfacing high-priority data like allergies, medications, and vitals on a single, clean screen.
- Dynamic Layouts: Screens that adapt to the patient’s condition or the doctor’s specialty.
- One-Click Navigation: Fast access to e-prescribing or lab orders.
- Visual Hierarchies: Color-coded alerts that flag critical values without overwhelming the user.
3. Engagement and Real-Time Insights
Real-time data is the lifeblood of a proactive ecosystem. By integrating wearable data and remote monitoring, we allow your EHR to provide insights between office visits.
Mayo Clinic successfully integrated remote monitoring into its EHR ecosystem, allowing its care teams to manage cardiac patients from home and reducing hospital readmission rates.
Clinical Value: When a system identifies an irregular heart rate from a wearable and flags it for the doctor, the EHR evolves from a passive record into a life-saving tool. This engagement builds deep trust within your healthcare ecosystem.
Automating Clinical Workflows with EHR Systems
To optimize EHR-backed healthcare ecosystems, automation must transition from a luxury to a core infrastructure component. Replacing repetitive manual labor with intelligent, background processes allows clinicians to focus on patients rather than screens.
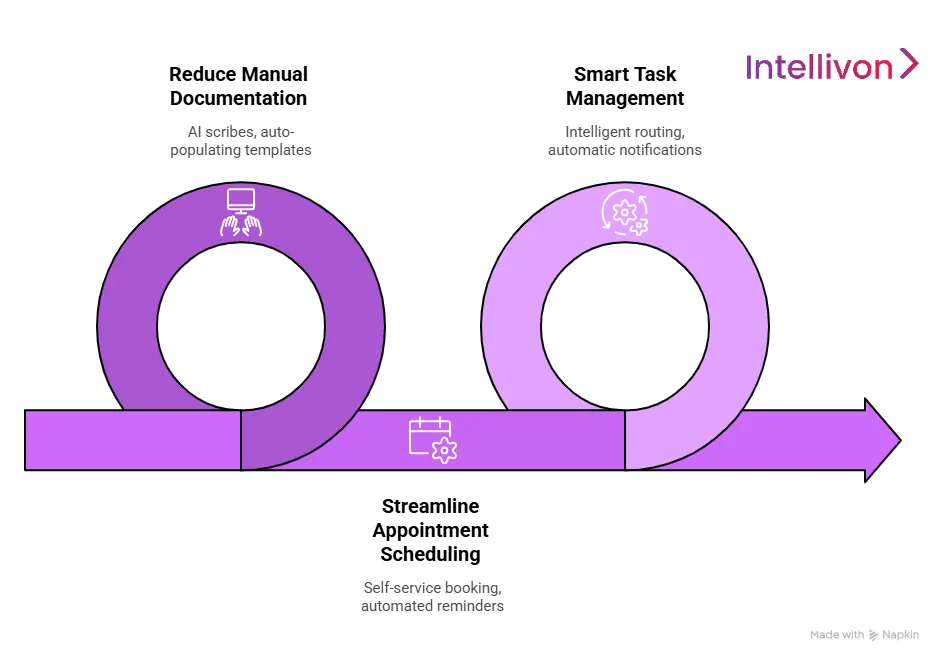
1. Automating Clinical Workflows
Automation serves as the engine of a modern healthcare network. Removing friction from daily operations helps organizations increase patient throughput while simultaneously reducing staff burnout. Efficiency is built into the ecosystem through the following strategic layers.
2. Reducing Manual Documentation
Documentation is the primary time-sink in modern medicine. Implementing tools that capture data at the source reduces the need for “after-hours” charting and manual entry.
- Voice-to-Text Integration: AI scribes transcribe consultations directly into structured clinical notes.
- Auto-Populating Templates: Smart forms pull previous vitals, active medications, and family history into new encounter notes automatically.
- OCR for External Records: Optical Character Recognition scans paper records from outside facilities and categorizes data into the correct EHR fields.
Efficiency Win: Automating the data entry process can lead to a 30% reduction in time spent on daily administrative tasks, effectively returning hours to the provider’s schedule for direct patient care.
3. Streamlining Appointment And Coordination
Manual scheduling is prone to human error and high no-show rates. The patient lifecycle is automated from the initial booking to the final follow-up.
- Self-Service Scheduling: Patients book via the portal with real-time sync to the provider’s calendar.
- Automated Reminders: SMS and email alerts are triggered 48 hours and 2 hours before the appointment.
- Waitlist Automation: If a cancellation occurs, the system automatically notifies the next patient on the waitlist to fill the slot.
- Referral Tracking: Automatic notifications reach the receiving specialist and the referring doctor once an appointment is booked or completed.
4. Smart Task Management
Efficiency is often lost during the hand-off between different departments. Systems using intelligent routing ensure no task falls through the cracks.
| Task Category | Manual Approach | Automated Ecosystem |
| Refill Requests | Nurse checks fax and calls doctor. | System flags request; doctor signs in one click. |
| Lab Follow-up | Staff manually calls the patient. | Results trigger an automated portal message. |
| Prior Auth | Hours spent on the phone with payers. | Auto-submission of clinical data to insurance. |
| Vitals Alerts | Manual review of nursing logs. | System pings physician if vitals hit trigger zones. |
Implementing these “if-this-then-that” logic flows ensures staff members always focus on the highest priority items. This smart management layer transforms the EHR from a passive database into an active operations manager.
Using EHR Data for Smarter Healthcare Decisions
Harnessing EHR data turns a static digital archive into a dynamic engine for medical progress. By applying advanced processing to existing records, healthcare systems can move from reactive care to predictive medicine. This shift ensures that every data point captured serves a purpose in the long-term clinical strategy.
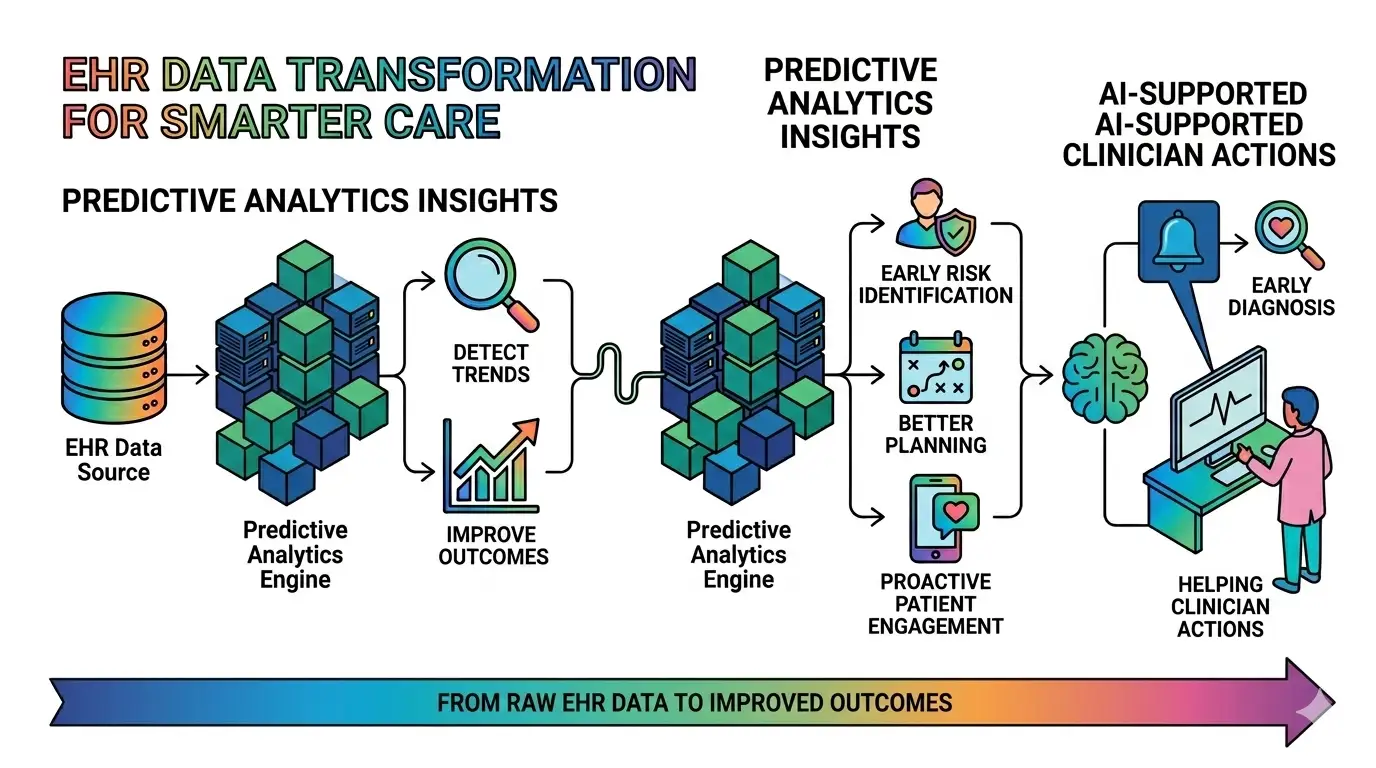
1. Actionable Clinical Insights
Raw data is a liability until it is processed into a clear narrative. Clinical dashboards now translate thousands of disparate data points into easy-to-read visualizations.
- Trend Identification: Visual graphs of a patient’s vital signs and lab results help providers spot subtle shifts in health before they become critical.
- Medication Effectiveness: Systems analyze historical data to determine which pharmaceutical interventions have the highest success rates for specific patient demographics.
- Provider Performance: Leadership can monitor departmental efficiency, identifying which protocols yield the best recovery times.
2. Predictive Population Health
Scaling an EHR across a population allows for the identification of massive health trends. Predictive analytics can forecast the spread of infectious diseases or identify regional spikes in chronic conditions.
- Risk Stratification: Algorithms categorize patients into high, medium, and low risk groups based on social determinants of health and history.
- Resource Allocation: Systems predict future hospital admission rates, allowing administrators to adjust staffing levels and bed availability in advance.
- Preventative Outreach: Automated systems identify patients who have missed essential screenings and trigger personalized communication to close gaps in care.
3. Early Diagnosis With AI Models
Integrating Artificial Intelligence directly into the EHR workflow provides a “second set of eyes” for the clinician. AI models scan the background of every patient encounter to find patterns that the human eye might miss.
HCA Healthcare effectively utilized its vast data ecosystem to implement the Sepsis Prediction and Optimization of Therapy tool. This system continuously monitors patient data and has been credited with helping clinicians detect sepsis up to 18 hours earlier than traditional methods, significantly lowering mortality rates across their facilities.
Diagnostic Support:
When an AI model flags a specific combination of lab values and history as a potential early indicator of kidney disease, it prompts the physician to order further testing. This early intervention is the key to moving from managing late-stage illness to preventing it entirely.
Reducing Medical Errors Through Smart EHR Design
In any EHR-powered healthcare ecosystem, the primary goal of design is the elimination of preventable harm. Smart architecture doesn’t just store information; it acts as a safety net, catching human oversights before they reach the patient. By embedding clinical intelligence into the user interface, organizations can drastically lower the risk of adverse events.
1. Alerts For Drug Risks
Medication errors are among the most common and dangerous risks in a clinical setting. Smart EHR systems use real-time cross-referencing to protect patients from harm.
- Automated Cross-Checks: The system scans the patient’s entire history for drug-to-drug, drug-to-allergy, and drug-to-food interactions.
- Dose Calculation Safety: Built-in calculators prevent decimal point errors or incorrect unit measurements, particularly in pediatric care.
- Alert Fatigue Prevention: To ensure clinicians don’t ignore warnings, alerts are tiered by severity so that only the most critical risks trigger a “hard stop” in the workflow.
2. Standardized Data Entry
Fragmented or non-standardized notes lead to misinterpretation and diagnostic errors. Forcing structure at the point of entry ensures that every provider in the ecosystem speaks the same clinical language.
- Standardized Terminology: Using drop-down menus with SNOMED CT or ICD-10 codes ensures data is searchable and unambiguous.
- Mandatory Fields: Critical data points, such as weight or allergy status, must be confirmed before a provider can proceed to the ordering phase.
- Dynamic Templates: Forms adapt to the specific specialty, ensuring that the right questions are asked for the right condition every time.
3. Real-Time Decision Support
Medical errors often occur when decisions are based on old information. In a fast-moving ecosystem, data latency can be fatal.
| Feature | Manual Process | Smart EHR Design |
| Lab Results | Calling the lab for updates. | Instant push notifications to the care team. |
| Vitals Tracking | Charting on paper every hour. | Real-time sync with bedside monitors. |
| Protocol Updates | Checking physical handbooks. | Automated clinical pathways based on latest data. |
For example, Intermountain Health successfully utilized real-time data integration within their EHR to manage specialized protocols for complex cases.
By ensuring that every clinician across their multi-hospital network saw the exact same lab results and vitals the second they were recorded, they achieved a significant reduction in mortality rates for patients with acute respiratory distress.
Safety Insight:
When a lab result is updated in the system, it is pushed instantly to the mobile devices of the entire care team. This prevents a physician from making a treatment decision based on a blood panel that is six hours old, ensuring the plan of care always matches the patient’s current physiological state.
Why Choose Intellivon for EHR Implementation in Healthcare?
Choosing the right partner for an EHR-powered healthcare ecosystem is a strategic decision impacting patient safety and long-term ROI. Intellivon brings a high-performance engineering culture to the medical field, ensuring digital infrastructure is as resilient as it is innovative.
Proven Healthcare App Expertise
With over 500,000 hours of coding experience, our team of ex-MAANG/FAANG developers brings a level of technical rigor rarely found in healthcare IT. Having navigated clinical data nuances across dozens of successful deployments, this talent ensures platforms are built using the high-availability principles of the world’s largest tech giants.
Custom Solutions For Scalability
One-size-fits-all EHRs often create more problems than they solve. Custom architectures are designed to grow from a single clinic to a multi-national network without performance loss. Using microservices and modular design, the ecosystem can integrate new AI tools or telehealth modules as the business evolves.
Compliance-First Global Standards
Security is never an afterthought. A compliance-by-design approach is adopted to meet or exceed global standards such as HIPAA, GDPR, and PIPEDA. Every line of code is written with data privacy in mind, utilizing end-to-end encryption and robust audit trails to protect institutions from legal and financial risks.
End-To-End Support
Partnership extends from initial ideation and workflow mapping to post-launch optimization. Support does not end at deployment; continuous monitoring and iterative updates are provided based on real-world user feedback. This ensures the EHR remains a cutting-edge asset rather than a legacy burden.
Conclusion
Implementing a modern EHR within a healthcare ecosystem requires a precise balance of technical rigor and clinical empathy. By prioritizing patient-centric design, automating burdensome workflows, and leveraging data for real-time decision support, institutions can transform a standard database into a life-saving asset. Partnering with a high-performance engineering team like Intellivon ensures that this transition is not only seamless and compliant but also built to scale alongside the future of medicine.
FAQs
Q1: How do you implement an EHR system?
A1: Implementation begins with a comprehensive workflow analysis to align the software with clinical needs. This is followed by data migration, where legacy records are cleansed and moved into the new structured database. Finally, staff undergoes intensive training before a phased “go-live” to ensure the transition minimizes disruption to patient care.
Q2: What are the 4 types of EMR?
A2: Electronic Medical Records generally fall into four categories: Cloud-based, which offer remote access via the internet; On-premise, which are hosted on local servers; Open-source, providing customizable source code; and Proprietary, which are specialized, closed-source systems developed by specific vendors for clinical use.
Q3: What are the 5 components of the EHR system?
A3: A robust EHR consists of Administrative and Billing tools for scheduling and insurance; Clinical Documentation for patient notes and history; Order Management for prescriptions and lab tests; Decision Support for safety alerts and clinical guidelines; and Patient Portals for secure data access and engagement.
Q4: What are the benefits of implementing EHR in healthcare?
A4: EHRs significantly improve patient safety by reducing medication errors through automated interaction alerts. They also boost operational efficiency by streamlining documentation and providing real-time access to patient data across different departments. Ultimately, these systems empower better clinical outcomes by turning raw data into actionable insights for the care team.