Handling patient data across digital systems requires strict safeguards, especially when information moves between applications, providers, and workflows. HIPAA EHR integration requires foundational data privacy, access control, and auditability, ensuring compliance is natively designed into the system’s architecture rather than added as a secondary layer.
Compliance in HIPAA EHR integration requires well-structured, controlled data flows where encryption, role-based access, secure APIs, audit logs, and consent management align across systems. Platform success depends on enforcing these safeguards while ensuring usability and performance in clinical workflows.
In this blog, we explain how to make a HIPAA-compliant EHR integrated platform by breaking down core compliance requirements, architectural considerations, and practical steps involved in building secure and interoperable healthcare systems.
Why HIPAA-Compliant EHR Platforms Matter Today?
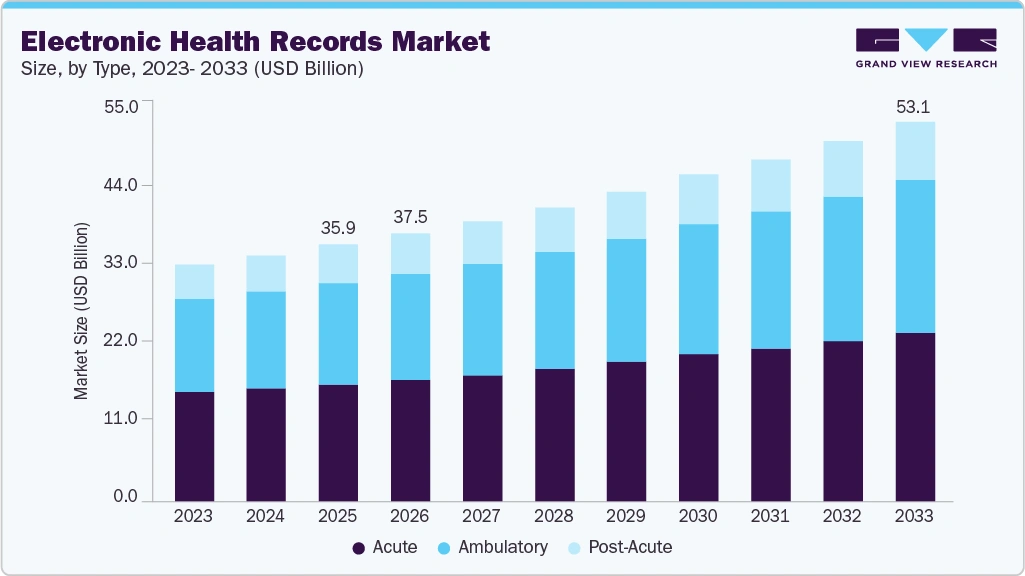
The rapid digitization of healthcare has propelled the EHR market from USD 35.89 billion in 2025 toward a projected USD 53.11 billion by 2033, growing at a 5.10% CAGR HIPAA-compliant integrated platforms now serve as the essential infrastructure for secure, cloud-native medical delivery and operational longevity.
75% of healthcare providers report that their EHR allows them to deliver better patient care through real-time access to comprehensive medical histories. Clinicians save an average of 45 minutes per day on administrative tasks thanks to EHR integration.
Facilities that integrate digital workflows report a 20–30% reduction in medication errors and a 60% decrease in “near-miss” medication events.
With medical errors costing the industry approximately $20 billion annually, EHRs provide a critical buffer by alerting providers to drug interactions and safety risks. Well-planned HIPAA compliance automation can deliver a 300% to 500% ROI by replacing repetitive manual work with secure workflows
A. Rising Risks Around PHI in Digital Healthcare
Protected Health Information (PHI) is a high-value target for cybercriminals because it contains permanent identifiers like social security numbers, medical histories, and insurance details. Unlike a credit card, medical data cannot be “reset” once compromised, leading to long-term identity theft and medical fraud.
The modern threat landscape for digital healthcare includes several critical vulnerabilities:
- Ransomware and Extortion: Healthcare remains the most targeted sector for ransomware. Attackers encrypt patient databases, halting clinical operations and demanding massive payouts to restore access.
- Unsecured API Endpoints: As platforms connect with third-party apps, poorly secured APIs create “backdoors” that allow unauthorized access to sensitive databases.
- Social Engineering and Phishing: Human error remains a significant risk. Sophisticated phishing attempts target healthcare staff to gain administrative credentials.
- Insider Threats: Unauthorized data access by employees, whether accidental or intentional, accounts for a substantial percentage of documented healthcare breaches.
B. Shift Toward Unified Healthcare Data Ecosystems
Modern healthcare providers are moving away from fragmented, standalone software toward integrated ecosystems. A unified platform eliminates data silos, allowing for a longitudinal patient record that flows seamlessly between different care settings.
| Feature | Legacy Siled Systems | Unified Integrated Platforms |
| Data Accessibility | Manual entry and faxing required between departments. | Real-time data availability via FHIR and HL7 APIs. |
| Clinical Efficiency | High “toggle tax” from switching between multiple apps. | Single-pane-of-glass interface for all clinical tasks. |
| Patient Outcomes | Fragmented history leads to potential medical errors. | Comprehensive data allows for better clinical decision support. |
| Interoperability | Limited connection to labs, pharmacies, or insurers. | Native integration with the broader healthcare network. |
The move toward HIPAA EHR integration is fueled by the need for data liquidity across clinical settings. When a platform unifies scheduling, charting, and billing into one compliant environment, it directly reduces administrative friction and enhances the quality of care.
C. Cost of Non-Compliance in Healthcare Systems
Failing to maintain HIPAA compliance carries heavy financial and operational penalties. The Office for Civil Rights (OCR) enforces these regulations strictly, and the consequences extend far beyond simple fines.
The true impact of non-compliance can be categorized into three primary areas:
- Statutory Fines and Legal Penalties: Depending on the level of negligence, HIPAA violations can cost thousands to millions of dollars per year. These fines are often accompanied by mandatory, multi-year corrective action plans.
- Reputational Damage and Loss of Trust: A data breach often leads to a mass exodus of patients and partners. In the healthcare sector, once the reputation for privacy is lost, it is nearly impossible to recover.
- Operational Paralysis: Non-compliance can lead to the termination of Business Associate Agreements (BAAs). Without a valid BAA, a platform is legally prohibited from handling PHI, effectively resulting in a total shutdown of services.

What Is a HIPAA-Compliant EHR Platform?
A HIPAA-compliant EHR platform securely manages PHI using zero-trust principles, ensuring all data interactions are encrypted authenticated and logged to meet federal privacy standards.
This architecture serves as the unified digital backbone for modern medical facilities, streamlining the exchange of information between patients, providers, and third-party entities.
A. Core Components of a Secure EHR Ecosystem
To maintain a secure environment, a modern EHR platform must integrate several high-level technical components that work in unison. These layers ensure that data is not only stored safely but also transmitted and accessed without risk of exposure.
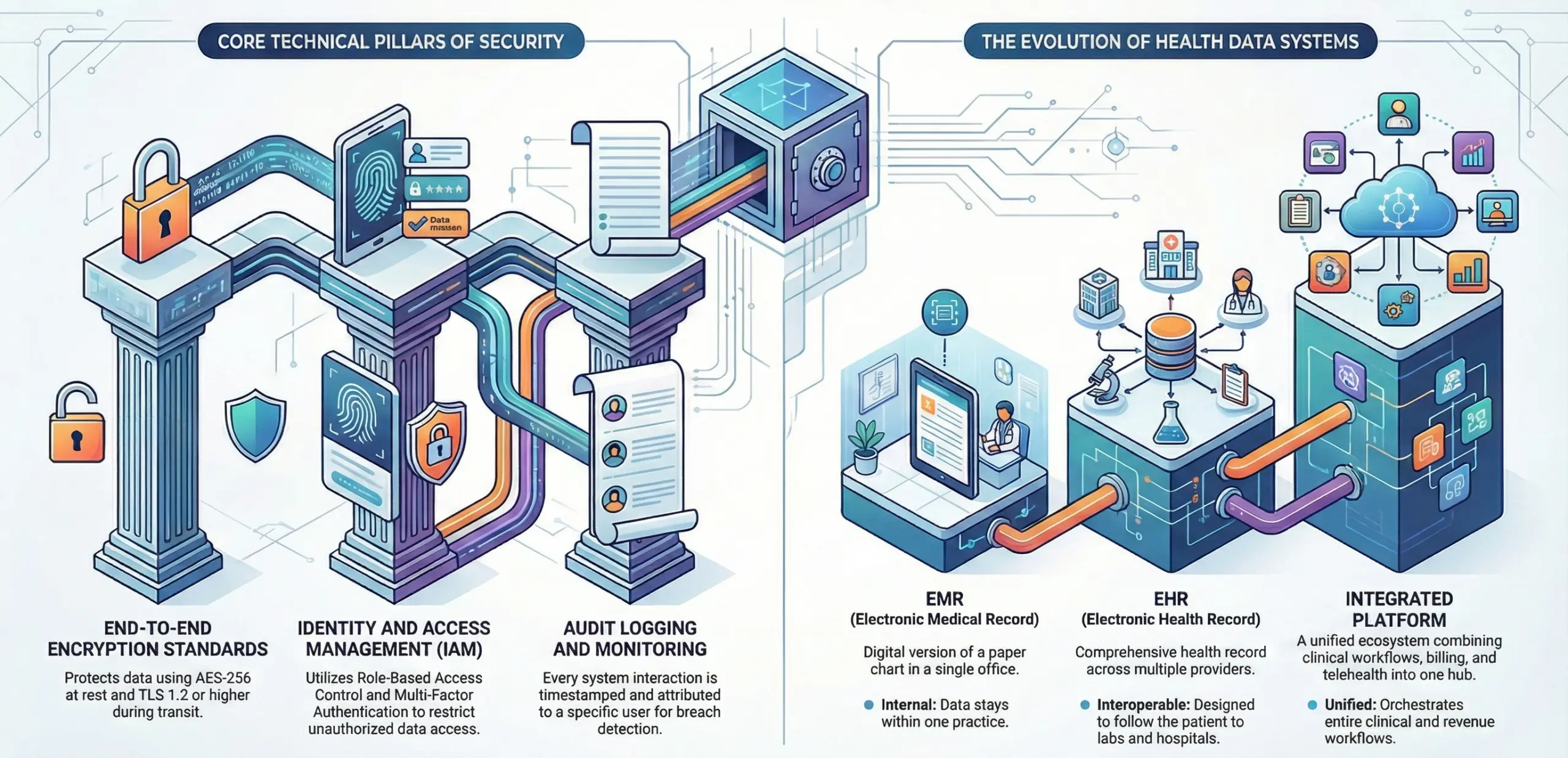
The essential technical pillars include:
- End-to-End Encryption: Data must be protected at rest (using AES-256 standards) and in transit (using TLS 1.2 or higher). This ensures that even if a data packet is intercepted, it remains unreadable.
- Identity and Access Management (IAM): This involves Role-Based Access Control (RBAC) and Multi-Factor Authentication (MFA). It ensures that a billing clerk cannot access clinical notes, and a doctor only sees records relevant to their patients.
- Audit Logging and Monitoring: Every action taken within the system like viewing, editing, or deleting a record must be timestamped and attributed to a specific user. Real-time monitoring tools detect unusual patterns that might indicate a breach.
- Data Redundancy and Disaster Recovery: Compliance requires that PHI remains accessible during emergencies. This involves encrypted cloud backups and failover protocols that allow the system to remain operational during local hardware failures.
B. Role of Compliance in Platform Architecture
Compliance is not a feature added after development; it is the framework that dictates how the entire system is built. In a HIPAA-compliant architecture, every technical decision is mapped back to the three main safeguards required by the law.
- Administrative Safeguards: These involve the policies and procedures governing conduct. The platform must support these by automating risk assessments and managing Business Associate Agreements (BAAs) with integrated partners.
- Physical Safeguards: Even in cloud environments, there must be protocols for facility access and workstation security. Compliance architecture ensures that cloud providers like AWS or Azure meet the physical security standards for data centers.
- Technical Safeguards: This is the software-level enforcement of privacy. It includes automatic log-offs, emergency access procedures, and integrity controls to ensure that PHI is not altered or destroyed in an unauthorized manner.
C. Difference Between EHR, EMR, and Integrated Systems
These terms represent different levels of data utility and connectivity while often used interchangeably. Understanding these distinctions is vital for determining the scope of a development project.
| System Type | Scope and Functionality | Level of Connectivity |
| Electronic Medical Record (EMR) | A digital version of a paper chart in a single clinician’s office. | Internal: Data stays within one practice and is not easily shared. |
| Electronic Health Record (EHR) | A comprehensive record of a patient’s health across multiple providers. | Interoperable: Designed to follow the patient to specialists, labs, and hospitals. |
| Integrated Platform | A full ecosystem combining EHR, billing, telehealth, and patient portals. | Unified: Orchestrates the entire clinical and financial workflow in one hub. |
An integrated platform represents the highest tier of this evolution. It goes beyond mere record-keeping to automate clinical workflows, manage revenue cycles, and facilitate remote patient monitoring, all within a single, compliant environment.
Who Should Build an EHR Integrated Platform?
Organizations outgrowing off-the-shelf software should build custom EHR platforms to bypass workflow bottlenecks. A proprietary ecosystem ensures deeper data ownership, custom clinical logic, and scalable growth without the restrictive licensing constraints of traditional healthcare models.
1. Hospitals and Multi-Specialty Clinics
Large-scale medical institutions often manage high volumes of complex data across diverse departments. For these organizations, a unified platform acts as the glue between disparate services like radiology, pathology, and inpatient care.
The strategic advantages for hospitals include:
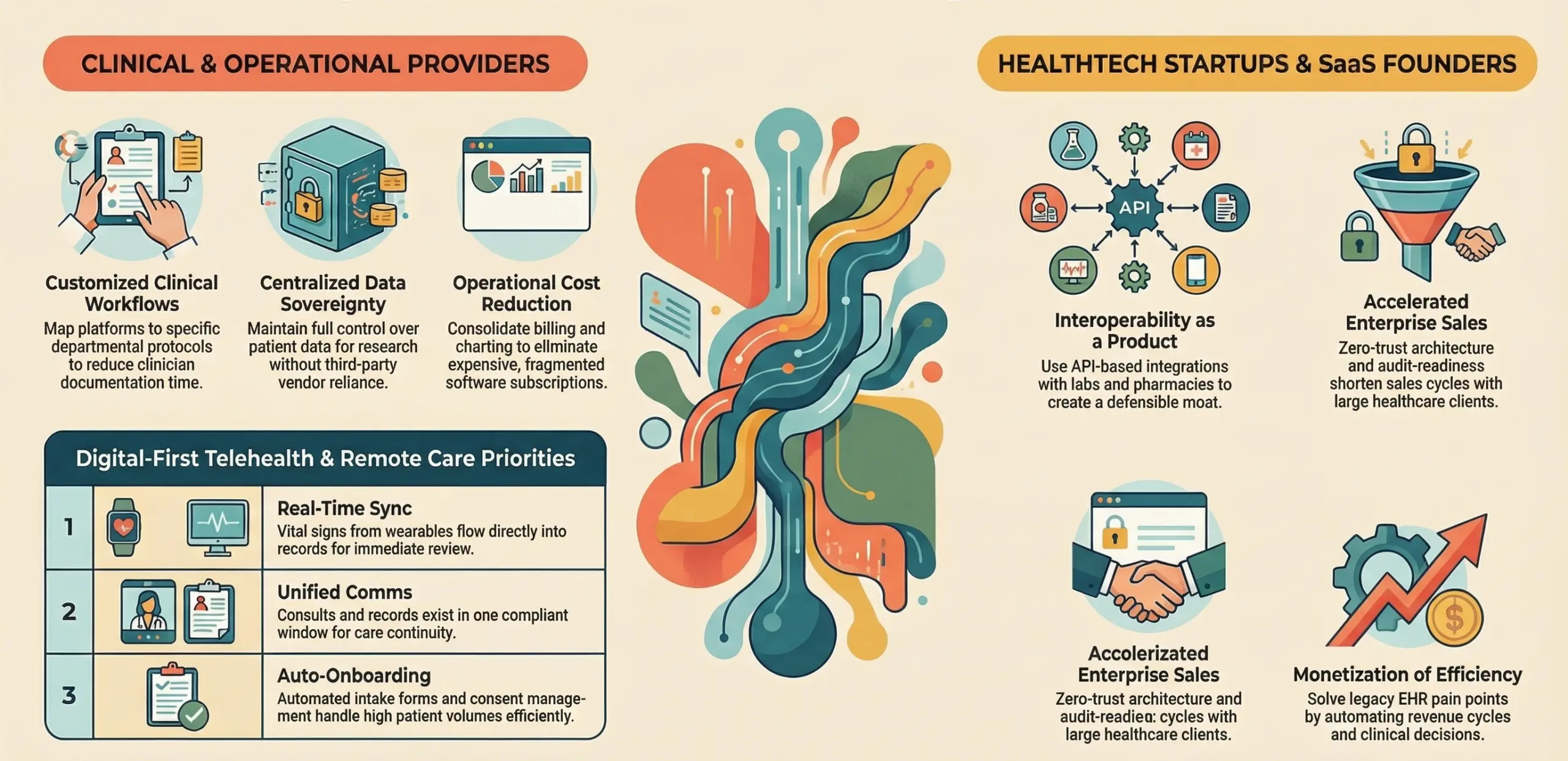
- Customized Clinical Workflows: Unlike generic software, a custom platform can be mapped to the specific departmental protocols of a high-volume hospital, reducing the time clinicians spend on documentation.
- Centralized Data Sovereignty: Hospitals can maintain full control over their patient data repositories, facilitating internal research and population health management without relying on third-party vendors.
- Operational Cost Reduction: By consolidating billing, scheduling, and charting into one hub, hospitals eliminate the need for multiple expensive subscriptions and reduce the IT overhead required to maintain fragmented systems.
2. Telehealth and Remote Care Providers
Telehealth and Remote Patient Monitoring (RPM) providers operate in a digital-first environment where the software is the clinic. For these entities, a HIPAA-compliant EHR platform is not just a tool; it is the delivery mechanism for care.
| Priority | Why an Integrated Platform is Essential |
| Real-Time Data Sync | Vital signs from wearable devices must flow directly into the EHR for immediate clinical review. |
| Integrated Communication | Video consultations, secure messaging, and patient records must exist in one compliant window to ensure continuity. |
| Automated Onboarding | Digital intake forms and consent management must be automated to handle high patient volumes efficiently. |
| Scalable Infrastructure | Cloud-native platforms allow telehealth providers to expand into new states or regions without physical hardware limits. |
3. Healthtech Startups and SaaS Founders
For founders entering the healthcare market, building a HIPAA EHR integration is the baseline requirement for entering the market and gaining provider trust. In a crowded market, the ability to offer a “plug-and-play” EHR integrated solution that is already audit-ready provides a massive competitive advantage.
Key strategic considerations for SaaS founders:
- Interoperability as a Product: A platform that offers seamless API-based integration with labs and pharmacies becomes an indispensable part of the healthcare value chain.
- Reduced Friction for Enterprise Sales: Large healthcare clients prioritize security. A platform built on a zero-trust architecture with ready-to-sign BAAs shortens the sales cycle significantly.
- Monetization of Efficiency: Founders can build value by solving specific “pain points,” such as automating the revenue cycle or providing AI-driven clinical decision support, which are features often lacking in legacy EHRs.
Key Features of a Successful HIPAA EHR Integration
Modern EHR platforms use modular, cloud-native architectures to transform clinical data into secure, actionable insights, ensuring high availability and scalability. The integrated features reduce documentation burdens, allowing clinicians to focus on patients while automating compliance and ROI.

1. End-to-End PHI Encryption and Data Security
Secure PHI using AES-256 encryption and frequent key rotation. Storing keys in Hardware Security Modules (HSMs) ensures data remains mathematically inaccessible, providing a multi-layered defense against physical or cloud breaches.
Utilize TLS 1.2 or 1.3 protocols to prevent man-in-the-middle attacks during transmission. Incorporating data masking and anonymization allows for secure analytics while maintaining the highest standards of patient privacy.
2. Role-Based Access and Identity Management
Implement Role-Based Access Control (RBAC) to enforce the principle of least privilege, ensuring users only access PHI necessary for their specific job functions. This granular control prevents unauthorized data exposure across the organization.
Strengthen security with Multi-Factor Authentication (MFA) and Single Sign-On (SSO) integration. These tools mitigate compromised password risks while reducing “password fatigue” for medical staff moving between various hospital applications.
3. Real-Time Audit Logs and Activity Monitoring
Transparency is a core requirement and maintaining immutable audit logs that document every PHI interaction, including views, edits, and deletions. Storing these in separate, secure environments ensures they remain tamper-proof for compliance and forensic reviews.
Deploy machine learning algorithms for real-time anomaly detection. By identifying suspicious access patterns or irregular geographic logins, the platform can trigger automated alerts to stop potential breaches before data exfiltration occurs.
4. FHIR-Based Interoperability Framework
Utilize a FHIR-based API framework to eliminate data silos and enable seamless communication with labs, pharmacies, and insurers. This ensures a longitudinal patient record that updates in real-time across the ecosystem.
The modular FHIR architecture supports “Best-of-Breed” third-party integrations, such as AI imaging or genomic tools. This flexibility allows the platform to scale and evolve without requiring a complete database overhaul.
5. E-Prescriptions and Clinical Decision Support
Integrate e-prescribing to eliminate manual errors and accelerate fulfillment via the Surescripts network. Real-time formulary checks ensure medication coverage is verified before the patient leaves the clinical setting.
Leverage Clinical Decision Support (CDS) to provide an intelligent “safety net” at the point of care. The system analyzes data to provide automated alerts for drug interactions, allergies, and overdue screenings.
6. Telehealth and Remote Patient Monitoring
Embed HIPAA-compliant video conferencing to conduct virtual visits while simultaneously updating medical records. This integration ensures clinical continuity and robust documentation necessary for insurance reimbursement and seamless care delivery.
Incorporate Remote Patient Monitoring (RPM) by streaming data from wearable devices directly into the EHR. Automated threshold triggers allow for proactive clinical intervention, significantly improving long-term outcomes for chronic disease management.
7. Automated Billing and Claims Processing
Use automated coding logic to suggest ICD-10 and CPT codes, reducing manual entry and documentation burdens. The system “scrubs” claims for errors before submission, ensuring a clean claim approach that accelerates reimbursement.
Streamline the revenue cycle with real-time eligibility verification and secure patient payment portals. This transparency increases collection rates while providing the organization with accurate data for financial forecasting and resource allocation.
8. Appointment and Workflow Automation System
Automate patient scheduling and digital intake workflows to reduce administrative bottlenecks and human error. Integrated reminders and self-service portals enhance patient engagement while optimizing the clinical daily calendar.
Synchronize front-office tasks with clinical workflows to ensure seamless transitions from check-in to consultation. This unified environment transforms administrative overhead into a driver of operational ROI and improved provider efficiency.
The Ideal Architecture for HIPAA EHR Integration
Modern EHR architecture prioritizes data liquidity and security through a distributed, decoupled stack that ensures system resilience and maintains strict encryption across high-volume clinical workflows.
The following table compares the critical architectural components required to sustain a secure, enterprise-grade integration:
| Architectural Pillar | Technical Implementation | Strategic Business Value |
| Zero-Trust Healthcare Data Architecture Model | Implementing continuous verification where no user or device is trusted by default, utilizing MFA and per-session authentication. | Minimizes the blast radius of potential credential theft and ensures that PHI access is strictly limited to verified, authorized identities. |
| Microservices vs Monolithic System Design | Breaking the platform into independent services (Scheduling, Messaging, Billing) managed via Kubernetes containers. | Enables independent scaling of high-demand modules and allows for rapid feature updates without risking total system downtime. |
| Cloud Infrastructure | Deploying on AWS Nitro or Azure Health Data Services with pre-configured HIPAA BAA and automated encryption. | Leverages billions in provider security investments to ensure geographic redundancy, 99.9% uptime, and out-of-the-box regulatory alignment. |
| Secure API Layer for Data Exchange | Utilizing an API Gateway with OAuth2, OpenID Connect, and TLS 1.3 for all FHIR-based clinical data transfers. | Protects the “handshake” between the EHR and the engagement layer, preventing unauthorized data interception or “man-in-the-middle” attacks. |
HIPAA-Compliant EHR Integrated Platform Development Process
Building a HIPAA-compliant EHR requires aligning software engineering with federal mandates to prioritize data integrity. This structured roadmap ensures the resulting infrastructure is technically robust, commercially viable, and prepared for the complex, regulated healthcare market.
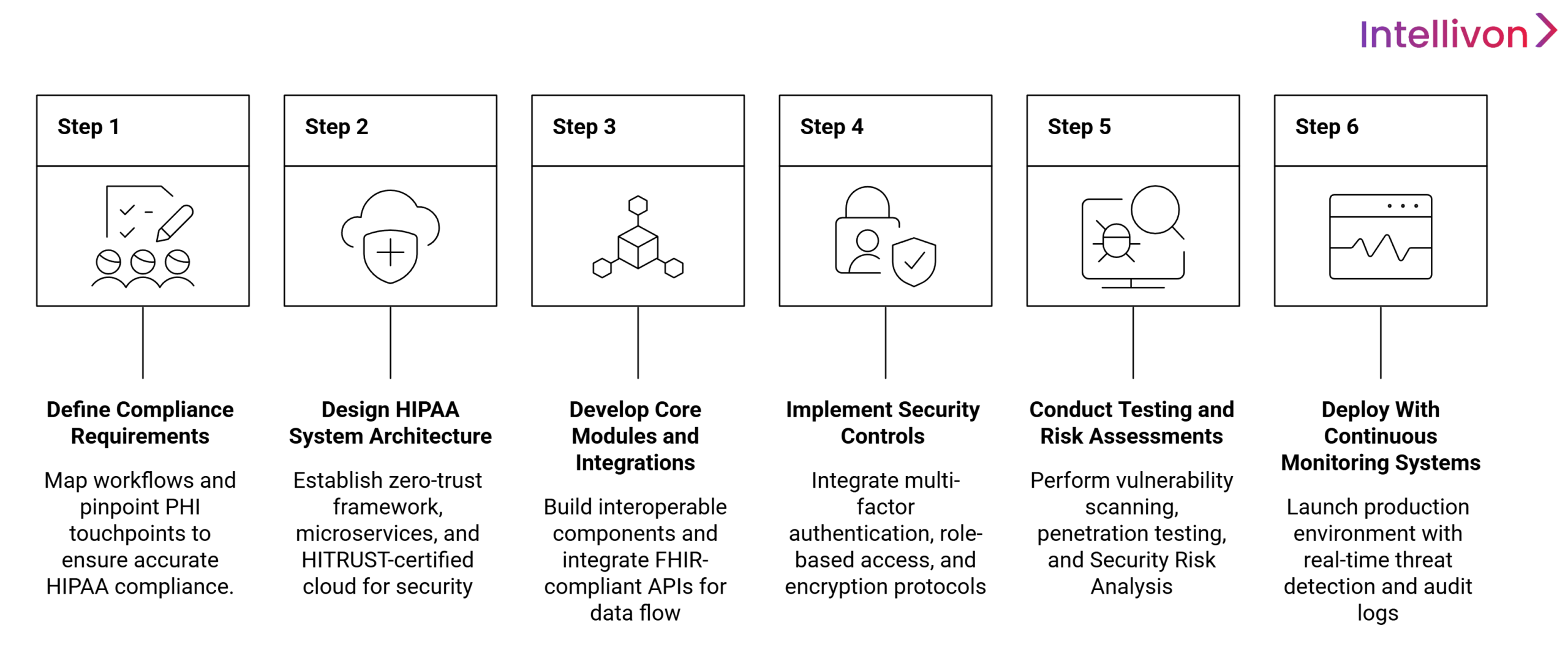
1. Define Use Cases and Compliance Requirements
Strategic planning for HIPAA EHR integration begins with a comprehensive map of clinical workflows and administrative needs. Specificity in identifying Protected Health Information touchpoints allows for precise application of HIPAA Technical Safeguards. A well-defined scope prevents feature creep and ensures that every module serves a clear, compliant purpose within the care delivery model.
2. Design HIPAA-First System Architecture
A zero-trust framework serves as the blueprint for HIPAA EHR integration. Microservices architecture facilitates the isolation of sensitive data, while the selection of HITRUST-certified cloud providers ensures physical security. This design phase establishes the foundation for end-to-end encryption and high-availability database clusters.
3. Develop Core Modules and Integrations
Modular engineering focuses on creating interoperable components for charting, scheduling, and billing. The integration of FHIR-compliant APIs enables the platform to communicate with external diagnostic laboratories and pharmacies. This development stage transforms raw clinical requirements into a functional, data-fluid ecosystem that supports real-time medical decision-making.
4. Implement Security and Compliance Controls
Technical enforcement of privacy standards involves the deep integration of multi-factor authentication and role-based access. Granular permission levels ensure the principle of least privilege is maintained across the organization. Automated encryption protocols for data at rest and in transit are finalized to eliminate potential vulnerabilities.
5. Conduct Testing and Risk Assessments
Rigorous vulnerability scanning and penetration testing identify potential entry points for unauthorized access. A formal Security Risk Analysis (SRA) evaluates the platform against HIPAA’s Administrative, Physical, and Technical Safeguards. These evaluations ensure that the system is resilient, stressed and fully prepared for external audits.
6. Deploy With Continuous Monitoring Systems
Final deployment transitions the platform into a production environment equipped with real-time threat detection and immutable audit logs. Automated monitoring tools track system performance and user activity to identify anomalies instantly. This proactive stance ensures long-term stability and immediate response to any potential security incidents.
Cost to Build a HIPAA-Compliant EHR Platform
The total investment for HIPAA EHR integration requires a strategic balance between essential compliance and high-end feature sets. By leveraging pre-built healthcare modules and focused MVP scopes, the initial capital requirement can be streamlined without compromising the security integrity of the platform.
| Development Phase | MVP Level | Enterprise Level | Key Deliverables |
| Discovery & Compliance Architecture | $12,000 – $18,000 | $30,000 – $50,000 | Technical Blueprints, HIPAA Mapping, & Zero-Trust Design |
| Security, Identity & IAM | $20,000 – $30,000 | $55,000 – $80,000 | MFA, RBAC, AES-256 Encryption, & BAA Documentation |
| Core EHR & Clinical Modules | $40,000 – $65,000 | $120,000 – $200,000 | Charting, Scheduling, Intake, & Clinical Workflows |
| FHIR/HL7 Interoperability | $25,000 – $40,000 | $80,000 – $120,000 | API Gateway, Lab/Pharmacy Sync, & Data Exchange |
| Revenue Cycle & Billing | $15,000 – $25,000 | $50,000 – $75,000 | ICD-10 Coding, Claims Scrubbing, & Payment Gateway |
| QA, Auditing & Risk Assessment | $8,000 – $15,000 | $35,000 – $50,000 | SRA Reports, Pen-Testing, & Immutable Audit Logs |
| Total Estimated Investment | $80,000 – $133,000 | $220,000 – $375,000+ | A Fully Audit-Ready Healthcare Ecosystem |
Critical Cost-Affecting Factors
Strategic budgeting for a healthcare platform requires an understanding of the variables that drive development hours and infrastructure costs. The following factors are the primary determinants of the final expenditure:
- Integration Complexity: Connecting single labs takes 80–120 hours, while full-scale interoperability hubs syncing national pharmacies and clearinghouses can exceed 500+ development hours.
- Data Migration: Transitioning 10,000+ patient records to FHIR-compliant databases requires intense scrubbing, typically adding 15%–20% to the total project timeline.
- Security Sophistication: Beyond foundational encryption, AI-driven anomaly detection and automated threat response systems can increase the security budget by $30,000–$50,000.
- Audits & Documentation: Achieving audit-ready status via third-party security assessments and formal HIPAA certifications costs between $15,000 and $40,000.
- Cloud Scaling: Supporting 1,000+ concurrent users requires high-availability clusters, resulting in monthly DevOps and hosting fees of $2,500 to $8,000+.
HIPAA Compliance Requirements Explained Simply
HIPAA compliance is a continuous operational framework, not a one-time checkbox. By integrating Administrative, Physical, and Technical safeguards into a platform’s DNA, organizations ensure data integrity and proactive audit-readiness while maintaining essential patient trust.
1. Administrative Safeguards You Must Implement
Administrative safeguards represent the “management” layer of HIPAA. They focus on the policies, procedures, and people-side of data protection, ensuring that the organization has a clear roadmap for handling sensitive information.
- Risk Analysis and Management: Organizations must conduct regular, formal assessments to identify where PHI is vulnerable and implement a plan to mitigate those risks.
- Workforce Training: Every individual with access to the platform must undergo documented training on privacy protocols and the specific security features of the software.
- Information Access Management: This involves establishing formal procedures for authorizing, supervising, and terminating access to PHI, ensuring that an employee’s access is revoked immediately upon their departure.
- Contingency Planning: The platform must have a documented strategy for data backup and disaster recovery, ensuring that clinical operations can continue even in the event of a system failure or natural disaster.
2. Physical Safeguards for Data Protection
Physical safeguards govern the actual environment where data is stored and accessed. While most modern platforms are cloud-based, the responsibility for physical security remains a shared obligation between the software provider and the cloud host.
- Facility Access Controls: Access to physical locations where servers or workstations are located must be restricted to authorized personnel only, typically managed through keycards or biometric scanners.
- Workstation Security: Policies must dictate how computers and mobile devices are positioned and used. For example, screens should not be visible to unauthorized passersby, and devices must have automatic lock timers.
- Device and Media Controls: There must be a strict protocol for the disposal of hardware. If a laptop or server is retired, the data must be “wiped” using forensic-grade methods to ensure PHI cannot be recovered.
- Inventory Management: Organizations must maintain a detailed record of every hardware asset that has access to the network, tracking its movement and current user throughout its lifecycle.
3. Technical Safeguards and Encryption Standards
Technical safeguards are the software-level protections that prevent unauthorized digital access to PHI. These are the “teeth” of the HIPAA Security Rule and require the most rigorous engineering focus.
- Access Control and Unique User IDs: Every user must have a unique identifier. The system must also include emergency access procedures, allowing authorized users to gain access to data during a critical medical crisis.
- Integrity Controls: The platform must implement mechanisms to ensure that PHI is not altered or destroyed in an unauthorized manner. This often involves digital signatures or checksums to verify data “freshness.”
- Transmission Security: This focuses on protecting data as it moves across networks. Encryption standards like TLS 1.2+ are mandatory for any data leaving the internal firewall, ensuring that intercepted packets remain unreadable.
- Audit Controls: The software must include hardware, software, or procedural mechanisms that record and examine activity in information systems that contain or use PHI.
4. Business Associate Agreements (BAA) Explained
A Business Associate Agreement (BAA) is a legally binding contract that is foundational to the HIPAA ecosystem. Under HIPAA, any third-party service provider that touches, stores, or transmits PHI on behalf of a “Covered Entity” (like a doctor’s office) is considered a Business Associate.
The BAA serves several critical functions:
- Liability Shifting: It establishes that the third party (e.g., a cloud provider or a billing service) is directly liable for HIPAA compliance and can be fined by the OCR for its own breaches.
- Permitted Uses: It clearly defines the only ways in which the Business Associate is allowed to use the PHI provided to them.
- Breach Notification: It mandates a specific timeline often much shorter than the federal 60-day limit, for the associate to report any security incidents back to the primary healthcare provider.
- Data Return/Destruction: It outlines what happens to the data once the contract ends, ensuring that no PHI remains in the hands of the third party after the partnership is over.
Interoperability Using FHIR and HL7 Standards
Interoperability transforms static databases into dynamic ecosystems. By adopting FHIR standards, your HIPAA EHR integration becomes more resilient and capable of real-time data exchange across the healthcare ecosystem.
A. Why FHIR Is Critical for Modern Healthcare Apps
Fast Healthcare Interoperability Resources (FHIR) represents the next generation of data exchange, utilizing modern web technologies like RESTful APIs and JSON. Unlike older, rigid standards, FHIR is designed for the mobile-first, cloud-native world, allowing developers to request specific data “resources” rather than bulky, entire records.
Key advantages of a FHIR-based architecture include:
- Granular Data Access: Developers can pinpoint specific elements such as a single medication or an allergy, reducing bandwidth and increasing system speed.
- Rapid Development Cycles: Using familiar web standards like HTTP and JSON shortens the learning curve for software engineers and accelerates the time-to-market.
- Modular Scalability: FHIR’s “plug-and-play” nature allows for the easy addition of third-party apps, such as patient portals or AI-driven diagnostic tools.
- Mobile Integration: FHIR is natively compatible with iOS and Android health kits, enabling seamless syncing between consumer wearables and clinical records.
B. How HL7 Enables Legacy System Integration
Health Level Seven (HL7) Version 2 remains the “workhorse” of existing hospital infrastructure. Most legacy systems, particularly in large inpatient facilities, still rely on HL7 messages for basic communication regarding admissions, discharges, and transfers (ADT).
This allows the new platform to integrate with existing hospital systems and access key data without a full infrastructure overhaul.
| Feature | HL7 v2 (Legacy) | FHIR (Modern) |
| Data Format | Pipe-delimited (non-human readable) | JSON / XML (developer-friendly) |
| Exchange Method | Trigger-based “Push” messaging | RESTful API “Pull” or “Push” |
| Complexity | High; requires specialized interface engines | Lower; uses standard web protocols |
| Primary Use | Internal hospital system communication | Cross-platform and mobile health apps |
C. Real-Time Data Exchange Across Ecosystems
The ultimate goal of interoperability is the creation of a real-time data loop that connects every member in the care journey. In a fully integrated ecosystem, data moves actively to where it is most needed, ensuring that clinical decisions are based on the most current information available.
The strategic impact of real-time exchange includes:
- Elimination of Duplicate Testing: Real-time access to external lab results prevents redundant and costly procedures.
- Instant Clinical Alerts: Data from remote monitoring devices can trigger automated emergency responses if patient vitals cross a specific threshold.
- Coordinated Transitions of Care: When a patient is moved from a hospital to a rehab center, their full history including active medications and imaging, is available to the new facility before they arrive.
- Pharmacy and Payer Sync: Electronic prescriptions and prior authorizations are processed instantly, reducing the time patients wait for critical treatments.
Tech Stack for HIPAA-Compliant EHR Platforms
A robust tech stack ensures high performance and regulatory compliance. Using enterprise frameworks and healthcare-specific cloud services creates an agile, secure system supporting rapid data processing.
The following table outlines the recommended technologies for building a high-performance, HIPAA-compliant EHR engagement layer:
| Tech Layer | Recommended Stack | Strategic Value & Compliance Role |
| Frontend & Backend Technologies | React / Next.js (Frontend) Node.js / Python (Django) (Backend) | Provides a responsive, mobile-first user experience while the backend handles complex FHIR resource mapping and asynchronous notification logic with high efficiency. |
| Secure Databases and Encryption Layers | PostgreSQL (RDS) with AES-256 Redis (for Caching) | Ensures all Protected Health Information (PHI) is encrypted at rest and in transit, while maintaining high-speed access for real-time scheduling and patient lookups. |
| DevOps, Monitoring, and Compliance Tools | Docker / Kubernetes AWS CloudWatch / Datadog Vanta / Drata | Automates the deployment of secure microservices, provides real-time audit logs for HIPAA tracking, and maintains a continuous state of “audit-readiness.” |
Common Mistakes to Avoid in EHR Development
Building a HIPAA-compliant EHR platform is complex, with common pitfalls around security, interoperability, and data privacy. Our developers address these challenges with robust architecture, compliance-first design, and proven best practices to ensure scalable, secure healthcare solutions.
1. Ignoring Compliance in Early Development Stages
Challenge: Treating HIPAA EHR integration as a post-launch add-on rather than a core development requirement leads to structural vulnerabilities.
Solution: Our developers embed HIPAA Technical Safeguards into the initial sprint, utilizing automated compliance-as-code tools and zero-trust frameworks to ensure every data interaction is natively secure from day one.
2. Poor API Security and Data Leakage Risks
Challenge: Exposed or weakly authenticated API endpoints create “backdoors” for unauthorized PHI access, especially when connecting with third-party labs, pharmacies, or wearables.
Solution: We implement OAuth 2.0, OpenID Connect, and granular scopes for all FHIR-based exchanges, while our engineers conduct rigorous penetration testing to validate that no data leaks occur during transmission.
3. Lack of Scalability in System Design
Challenge: Monolithic architectures often crash or lag when patient volumes increase, leading to clinical workflow disruptions and high costs for emergency server migrations.
Solution: Our team builds using microservices and HITRUST-certified cloud auto-scaling, ensuring the platform handles thousands of concurrent users seamlessly while maintaining consistent speeds for real-time clinical data processing.
How Intellivon Builds Secure EHR Platforms?
Intellivon engineers high-performance healthcare ecosystems where security is the architectural foundation. Our approach streamlines complex regulatory requirements into a scalable digital backbone, ensuring every clinical workflow remains data-fluid, audit-ready, and patient-centric.
A. Compliance-First Development Approach
We embed HIPAA safeguards directly into the source code using a zero-trust framework. This proactive strategy automates encryption and access controls, ensuring that your platform remains fully compliant and ready for federal audits from day one.
B. Experience in Healthcare App Development
Our team possesses deep domain expertise in navigating the complexities of medical software. We have successfully delivered high-stakes solutions that bridge the gap between intuitive user experiences and the rigorous technical demands of modern clinical environments.
C. Proven Framework for Secure Integrations
We utilize a standardized, FHIR-driven integration engine to connect your EHR with labs, pharmacies, and insurers. This framework ensures seamless, real-time data exchange across the healthcare ecosystem while maintaining the highest levels of transmission security.
Case Study: Building a Scalable EHR System
This case study illustrates how a multi-specialty provider transitioned from fragmented, paper-heavy systems to a unified, cloud-native EHR. The project eliminated data silos to accelerate patient care while ensuring strict federal privacy compliance.
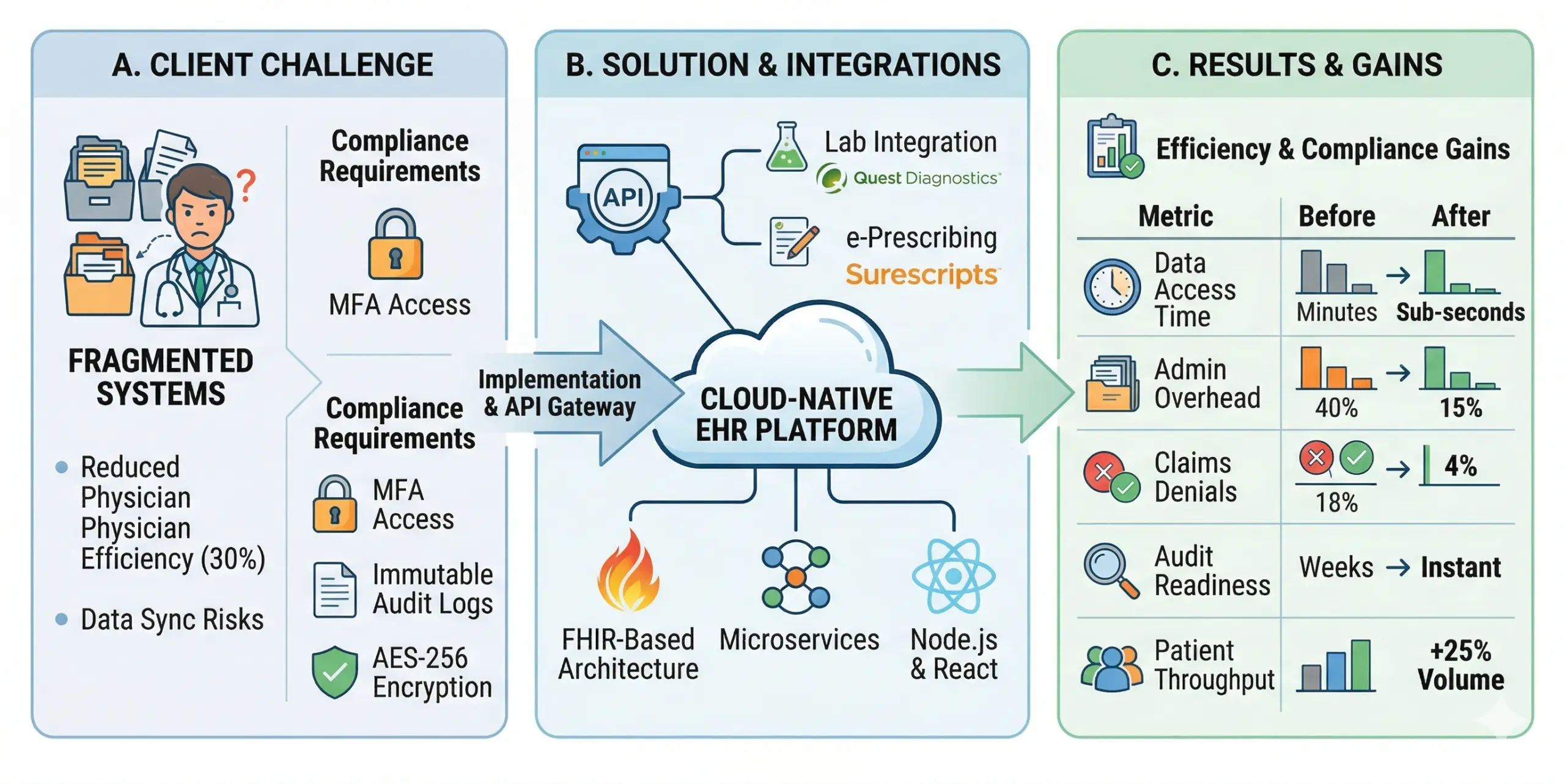
A. Client Challenge and Compliance Requirements
The client struggled with a disjointed infrastructure where patient records were scattered across multiple legacy systems, leading to a “toggle tax” that reduced physician efficiency by 30%. This fragmentation created significant risks for data synchronization errors and made it nearly impossible to maintain a clear audit trail for HIPAA reporting.
To mitigate these risks, the following compliance requirements were established:
- Zero-Trust Identity Management: Implementation of Multi-Factor Authentication (MFA) across all staff access points to prevent unauthorized credential usage.
- Immutable Audit Logging: A requirement for a non-erasable record of every instance where Protected Health Information (PHI) was viewed or modified.
- End-to-End Encryption: Mandatory AES-256 encryption for data at rest and TLS 1.2+ for all external communications with labs and pharmacies.
- Business Associate Management: Automated tracking and storage of BAAs for all third-party integrated service providers.
B. Solution Architecture and Key Integrations
The architecture utilizes a modular, microservices-based framework to ensure high availability and data integrity. This design enables seamless API connectivity with external diagnostic labs and pharmacies while maintaining strict HIPAA isolation.
- Situation: The provider needed a centralized platform capable of handling high-volume patient data while integrating seamlessly with external diagnostic and financial partners.
- Task: Our objective was to design a FHIR-based microservices architecture that could scale dynamically and ensure 100% data integrity during real-time exchanges.
- Action: We deployed a HITRUST-certified cloud environment, utilizing Node.js and React for a high-performance interface. Our team integrated a custom FHIR API gateway to sync with Surescripts for e-prescribing and Quest Diagnostics for automated lab results.
- Result: The platform successfully unified the clinical workflow, reducing patient intake time by 50% and providing a single, compliant source of truth for the entire medical staff.
C. Results in Efficiency and Compliance Gains
Implementing the integrated platform transformed manual administrative processes into automated, audit-ready workflows. These gains reflect a significant reduction in operational friction, allowing the clinical team to prioritize high-quality patient care.
| Performance Metric | Pre-Implementation Status | Post-Implementation Result |
| Administrative Overhead | 40% of staff time spent on data entry. | Reduced to 15% via automated charting. |
| Claim Denial Rate | 18% due to manual coding errors. | Dropped to 4% with ICD-10 automation. |
| Data Accessibility | 5-minute average to retrieve records. | Sub-second real-time data retrieval. |
| Audit Readiness | 2 weeks to compile compliance reports. | Instant, one-click audit log generation. |
| Patient Throughput | Limited by manual scheduling bottlenecks. | 25% increase in daily patient volume. |
How to Choose the Right EHR Development Partner
Choosing the right HIPAA-compliant EHR partner ensures secure, compliant, and scalable healthcare infrastructure long-term. A successful partnership is built on technical transparency and shared accountability, who prioritizes transparency, interoperability standards, and compliance-by-design to avoid risks, rework, and long-term system inefficiencies.
A. Key Questions to Ask Before Hiring
A rigorous vetting process begins with targeted inquiries that reveal a partner’s technical depth and operational maturity. These questions are designed to separate generalist agencies from specialized healthcare engineering firms.
- “Can you provide a sample Business Associate Agreement (BAA)?” A partner ready for healthcare work should have a standard BAA ready for review, indicating they understand their legal liability.
- “How do you handle data isolation in a multi-tenant architecture?” This reveals their understanding of preventing data leakage between different clinics or departments within the cloud.
- “What is your experience with FHIR and HL7 v2 standards?” Specialized partners should be able to discuss specific integration engines and API management strategies they have previously deployed.
- “How is security testing integrated into your CI/CD pipeline?” Ensure they perform automated vulnerability scans and penetration testing throughout the development lifecycle, not just at the end.
B. Evaluating Healthcare Domain Expertise
Healthcare expertise requires deep familiarity with clinical workflows and “gray areas” like eRx, EPCS, and ICD-10 coding. Partners who understand SOAP notes and longitudinal records build products that ensure high adoption and ROI.
C. Importance of Compliance and Security Experience
In EHR development, compliance is an environment, not a feature. Partners must provide audit-ready systems featuring zero-trust networks, key rotations, and disaster recovery protocols to prevent costly legal fees and safeguard institutional reputation.
Future Trends in HIPAA-Compliant EHR Platforms
EHR platforms are evolving into intelligent, decentralized systems that enable predictive care, automation, and enhanced data security. Future-ready architecture ensures scalability, stability, and innovation, making EHRs central to modern digital healthcare ecosystems.
A. AI in Clinical Decision Support Systems
Artificial Intelligence is transforming Clinical Decision Support (CDS) from a rule-based alerting system into a sophisticated diagnostic partner. Modern AI models can analyze unstructured data such as physician notes and medical imaging to identify subtle patterns that traditional systems might overlook.
- Automated Risk Scoring: AI algorithms can process real-time vitals and historical records to generate “sepsis alerts” or “cardiac risk scores” hours before clinical symptoms become apparent.
- Natural Language Processing (NLP): Advanced NLP tools reduce the documentation burden by converting verbal physician-patient interactions into structured, compliant EHR entries automatically.
- Precision Medicine Integration: AI facilitates the use of genomic data at the point of care, suggesting personalized treatment plans based on a patient’s specific genetic markers and history.
B. Blockchain for Secure Healthcare Data Sharing
Blockchain offers a decentralized, tamper-proof ledger for managing consent and records. In HIPAA-compliant contexts, it stores cryptographic “hashes” of data interactions rather than the PHI itself, ensuring integrity without compromising patient privacy.
| Feature | Traditional Centralized EHR | Blockchain-Enabled EHR |
| Data Ownership | Controlled by the hospital or provider. | Controlled by the patient via private keys. |
| Audit Trails | Internal logs that can be vulnerable to tampering. | Immutable, distributed ledger of every access event. |
| Interoperability | Complex API mapping between different systems. | Unified data index accessible by authorized nodes. |
| Consent Management | Often manual or siloed in separate documents. | Smart contracts automate and enforce data permissions. |
C. Predictive Analytics for Patient Outcomes
Predictive analytics shifts clinical focus from reactive to proactive care. By aggregating vast patient data, integrated platforms forecast population health trends and individual trajectories, enabling precise, intervention-based care models.
The strategic application of predictive modeling includes:
- Readmission Prevention: Identifying patients at high risk of post-discharge complications, allowing for targeted remote monitoring and follow-up care.
- Chronic Disease Management: Using historical trends to predict the progression of conditions like diabetes, enabling clinicians to adjust care plans before a crisis occurs.
- Resource Allocation: Forecasting patient inflow and bed demand, which helps hospitals optimize staffing and reduce administrative bottlenecks.
- Revenue Cycle Forecasting: Analyzing claim history to predict denial patterns, allowing the billing department to correct systemic issues before they impact cash flow.
Build Your HIPAA-Compliant EHR With Intellivon
Engineering a healthcare platform that balances rigid federal compliance with fluid clinical workflows requires more than just technical proficiency; it requires a partner dedicated to the high-stakes reality of modern medicine.
Intellivon specializes in transforming complex regulatory requirements into intuitive, high-performance digital ecosystems. By choosing to build with us, you are not just hiring a development team but securing a strategic alliance focused on data integrity, scalable architecture, and the long-term success of your healthcare venture.
Why Partner With Us:
The decision to develop a custom EHR is a vital investment for your enterprise’s future. We provide the expertise to navigate healthcare law and software engineering, ensuring your platform is a market-ready asset from the start.
- End-to-End Compliance Support: We manage the full lifecycle from zero-trust design to audit-ready documentation ensuring all HIPAA safeguards are natively integrated into your system’s DNA.
- Custom Healthcare Solutions: We build bespoke modules for charting, billing, and interoperability precisely mapped to the unique clinical workflows of clinics, hospitals, or startups.
- FHIR-First Interoperability: We create data-fluid ecosystems using FHIR and HL7 standards enabling seamless, real-time exchange with pharmacies, labs, and insurance clearinghouses.
Get a Free Consultation With Our Experts and navigating the path to a HIPAA-compliant platform starts with a clear, actionable strategy. We offer a comprehensive consultation to discuss your vision, evaluate your compliance needs, and provide a realistic roadmap for development, integration, and launch.
Conclusion
Developing a HIPAA EHR integration is a sophisticated architectural undertaking where technical precision meets stringent federal mandates. Success requires a strategic fusion of zero-trust security, FHIR-driven interoperability, and intelligent workflow automation. By prioritizing a compliance-first philosophy for your HIPAA EHR integration, you mitigate existential legal risks while establishing a resilient, scalable digital backbone for modern healthcare. As the industry shifts toward unified data ecosystems, a robust, audit-ready platform becomes your most significant competitive advantage, ensuring long-term operational excellence and superior patient-centric care in an evolving medical landscape.
FAQs
Q.1. How much does it cost to build a HIPAA-compliant EHR?
A.1. Building a secure EHR platform typically ranges from $80,000 to over $350,000+. Costs depend on integration complexity, specialized security features, and scaling requirements. Investing in compliance-by-design early prevents expensive legal penalties and structural refactoring during the market launch phase.
Q.2. What are the primary technical requirements for HIPAA compliance?
A.2. A compliant platform must feature AES-256 encryption, multi-factor authentication, and granular role-based access controls. Additionally, maintaining detailed, tamper-proof audit logs and ensuring secure FHIR-based data exchange are federal mandates. These technical safeguards protect data integrity and ensure overall system availability.
Q.3. How does role-based access control (RBAC) protect patient data?
A.3. RBAC ensures users only access information necessary for their specific job functions. By mapping digital permissions to real-world medical hierarchies, the system prevents unauthorized data exposure, reduces internal insider threats, and maintains strict compliance with the HIPAA Privacy Rule.
Q.4. Why is FHIR-based interoperability essential for new healthcare platforms?
A.4. FHIR standards allow your platform to act as a universal translator between diverse medical systems. By adopting these protocols, you eliminate data silos and ensure patient information is accessible at the point of care, which drives user adoption and ROI.