Key Takeaways:
-
AI radiology ROI comes from faster triage, higher productivity, better throughput, and downstream care capture, not direct reimbursement.
-
Published research shows five-year ROI reaching 451%, rising to 791% when radiologist time savings are included.
-
Hospitals must track turnaround time, follow-up capture, and cost avoidance to measure real financial impact.
-
ROI failures stem from missing baselines, poor PACS integration, low volume, and no downstream workflow to capture findings.
-
How Intellivon builds ROI-driven AI radiology systems your enterprise fully owns, with PACS connectivity and financial impact tracking from day one.
Imaging volumes are increasing faster than radiologists can handle, and the resulting operational pressure is now reflected in hospital financial statements. Because of this, hospital leaders are asking more focused questions about where AI in radiology provides real value and how that value translates financially.
The answer is rarely just one number. AI in radiology shows its return on investment through quicker turnaround times, greater radiologist productivity, fewer bottlenecks, improved care coordination, and better follow-up capture.
A study published in JACR found that an AI radiology platform in a hospital accredited for stroke management delivered a 451% return on investment over five years, and this increased to 791% when factoring in radiologist time savings. However, the same study confirmed that results differ based on scan volume, care setting, and the impact of treatment after scanning.
Thus, what financial leaders, radiology heads, and hospital operators should evaluate goes beyond direct reimbursement. Intellivon designs AI radiology as part of the workflow infrastructure rather than as a separate diagnostic tool. At the same time, sustainable ROI comes from how the system operates across the entire imaging process. This blog explains exactly where that value originates.
How Radiology Delays Affect Hospital Revenue And Operations
Radiology delays extend patient stays, block bed turnover, and create bottlenecks that ripple across hospital operations. As imaging demand continues to climb in hospitals, the gap between scan volume and reporting capacity widens, and the financial pressure that follows lands directly on hospital revenue.
The radiology AI market is expanding in direct response to these backlogs, with workforce shortages and turnaround time failures driving investment across health systems globally. In fact, the global radiology as a service market was valued at USD 4.0 billion in 2022 and is projected to reach USD 11.9 billion by 2030, growing at a CAGR of 14.7% through the same period.
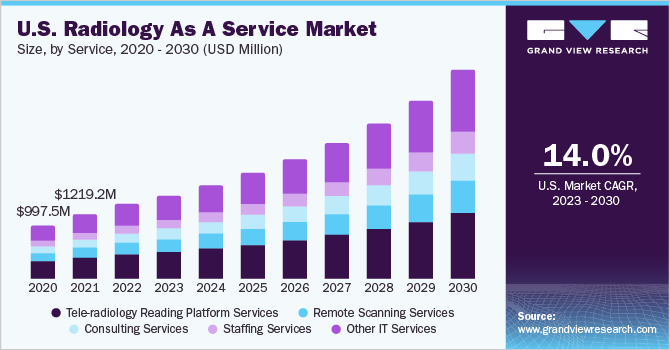
That growth, however, is not incidental. Hospitals and health systems are therefore actively shifting toward cloud-based imaging infrastructure because it delivers advanced diagnostic capability without the cost overhead of traditional on-premise deployments.
As a result, demand for scalable, cloud-based medical imaging services has become one of the strongest signals of where radiology infrastructure is heading.
What ROI Means In AI Radiology For Hospitals
AI radiology ROI includes financial, operational, clinical, and workforce returns created through faster reporting, smarter triage, better throughput, and improved care coordination.
Calculating the true value of medical imaging software requires looking past simple cost savings. While many institutions focus solely on direct revenue, the actual impact appears across the entire workflow of a modern facility.
Assessing AI radiology ROI involves analyzing how automated tools integrate with human expertise to create a more efficient and profitable care environment.
1. Direct Financial ROI
Financial gains stem from better utilization of existing imaging equipment and capturing care pathways more effectively.
- Asset Utilization: Reduces idle time for expensive MRI or CT machines through faster processing.
- Downstream Revenue: Identifies urgent findings that lead to necessary follow-up scans and higher-value procedures.
- Leakage Prevention: Minimizes patient loss caused by delayed or uncertain diagnoses that drive patients elsewhere.
2. Operational ROI
Operational improvements center on the speed and priority of the reporting worklist to maximize daily output.
- Automated Triage: Moves critical cases to the top of the queue without manual intervention.
- Efficiency Gains: Lowers report turnaround times and removes the need for administrative manual routing.
- Throughput: Enables the department to process a higher volume of patients accurately within a standard shift.
3. Workforce ROI
The workforce benefits focus on protecting the clinical staff and optimizing their specialized time.
- Capacity Building: Allows the existing team to manage larger volumes without increasing headcount.
- Burnout Mitigation: Reduces the immense pressure of repetitive reviews and manual report preparation.
- Staff Resilience: Creates a stable environment where clinicians focus on complex diagnostic challenges rather than sorting.
4. Clinical ROI
Clinical returns impact patient health and the long-term reputation of the healthcare facility.
- Early Detection: Identifies subtle anomalies faster to enable immediate treatment decisions.
- Case Escalation: Reduces diagnostic delays in emergency scenarios where every minute is critical.
- Patient Trust: Enhances the overall experience by providing rapid results and high-quality care.
This holistic view helps leaders understand that AI radiology ROI is a combination of measurable hospital outcomes rather than a single financial metric.
Where Hospitals See ROI From AI Radiology
Hospitals see AI radiology ROI through faster triage, improved reporting productivity, higher imaging throughput, reduced operational waste, and stronger downstream care capture.
Identifying exactly where value is generated allows for a more targeted investment strategy. Modern solutions move beyond simple image analysis to restructure the entire departmental workflow. By focusing on high-impact areas, facilities can achieve a measurable return that scales with their patient volume.
1. Faster Critical Case Triage
Traditional first-in-first-out workflows often fail when urgent cases are buried under routine screenings. AI systems act as an always-on secondary viewer that flags likely life-threatening conditions before a human ever opens the file.
- Acute Conditions: Algorithms specifically target stroke, pulmonary embolism, and intracranial hemorrhage with high precision.
- Automated Escalation: Software identifies pneumothorax or acute fractures and instantly moves these studies to the top of the radiologist’s worklist.
- Risk Reduction: Prioritizing urgent cases reduces the window of time during which a critical patient waits without a definitive diagnosis.
2. Reduced Report Turnaround Time
Speed is a primary driver of efficiency in both emergency and inpatient settings. By reducing the manual review delay, hospitals can significantly accelerate the entire care cycle.
- Rapid Reads: AI provides preliminary insights that allow for faster treatment decisions in the ER.
- Wait Time Reduction: Recent data from AJR Online shows that AI worklist reprioritization can reduce wait times for acute findings by nearly 36 percent.
- Improved Flow: Faster results lead to quicker inpatient discharges and better bed management across the hospital.
3. Higher Radiologist Productivity
Automation does not replace the specialist but rather removes the cognitive load of routine tasks. This allows the medical team to process more studies with higher accuracy.
- Pre Analysis: Software handles initial segmentation and measurement of findings like lung nodules or cardiac volumes.
- Drafting Assistance: Structured reporting tools prepopulate findings into the dictated report to save manual entry time.
- Capacity Growth: Studies published in 2025 suggest that AI applications could eventually reduce total interpretation time by up to 33 percent over five years.
4. Better Imaging Throughput
Maximizing the use of existing hardware is the fastest way to increase departmental revenue. AI helps clear bottlenecks that typically slow down the scanning process.
- Modality Efficiency: Faster reporting means machines can be scheduled more tightly without causing a backlog in the waiting room.
- Bottleneck Removal: Real-time tracking identifies where cases are getting stuck in the pipeline.
- Increased Volume: More efficient workflows allow the facility to handle higher patient counts without adding additional shifts.
5. Improved Follow-Up Capture
Long-term revenue is often hidden in the follow-up recommendations that get lost in manual processes. AI ensures that incidental findings are tracked and acted upon.
- Revenue Drivers: A key study in the JACR found that AI identification of necessary treatments and follow-up scans is a major revenue contributor.
- Pathway Continuation: Tracking lung nodules or oncology surveillance ensures patients remain within the hospital system for their long-term care.
- Systemic ROI: One modeling study reported an ROI of up to 451 percent by including the value of additional procedures generated through AI detection.
The integration of these tools transforms the radiology department from a cost center into a proactive driver of hospital growth.
What ROI Range Can Hospitals Realistically Expect?
Hospitals can expect AI radiology ROI to vary widely based on imaging volume, use case, integration depth, reimbursement model, and downstream care pathways.
Hospitals should not expect one universal ROI number for their digital transformation efforts. A high-volume department managing stroke, trauma, oncology, or emergency imaging typically generates a much stronger return than a small facility using AI for a single standalone task.
Success depends on how deeply the technology is woven into the clinical and financial fabric of the organization.
1. Conservative ROI Scenario
In this setting, the hospital usually focuses on basic operational improvements to stabilize a small or mid-sized department.
- Scope: Limited modality focus with one or two specific AI use cases and basic PACS integration.
- Primary Drivers: Value is generated through faster reads, fewer administrative delays, and a reduced manual workload for the clerical staff.
- Expected Outcome: A moderate return on investment characterized by steady efficiency gains and the elimination of common workflow bottlenecks.
2. Moderate ROI Scenario
Facilities with a more integrated approach see a sharper increase in value by connecting their imaging data across multiple platforms.
- Scope: Multi-modality imaging department with advanced integration across PACS, RIS, and EHR systems.
- Primary Drivers: Value comes from emergency triage support, automated reporting assistance, and dedicated productivity dashboards.
- Expected Outcome: Stronger ROI driven by significant reductions in turnaround times, enhanced radiologist productivity, and better care coordination between departments.
3. High ROI Scenario
The most significant returns are found in large health systems that treat AI as a central pillar of their enterprise strategy.
- Scope: High-volume environments managing complex stroke, oncology, and emergency department workflows.
- Primary Drivers: Revenue is captured through AI-driven follow-up tracking and automated specialist referrals that keep patients within the network.
- Expected Outcome: Exceptional ROI achieved when the software identifies patients needing urgent interventions, specialist review, or long-term surveillance procedures.
4. Why ROI Can Reach 451% Or Higher
While these figures may seem ambitious, they are grounded in recent industry research and standardized financial modeling. A published ROI calculator from 2025 demonstrated a 451% five-year ROI by looking strictly at clinical and operational efficiencies.
When including radiologist time savings, which can range from 14% to 49%, depending on the task, that figure can climb as high as 791%. These benchmarks reflect measurable improvements across waiting, triage, reading, and reporting activities rather than just theoretical benefits.
This data highlights that AI radiology ROI is a measurable outcome for those who implement these tools with a clear strategic vision.
Key Metrics Hospitals Should Track For ROI
Hospitals should track AI radiology ROI through turnaround time, radiologist productivity, scan volume, follow-up completion, patient flow, and cost-per-study improvement.
For any platform to prove its worth, the executive team must look at specific, data-driven indicators that go beyond general satisfaction. Establishing a baseline for these metrics before implementation is essential for measuring the shift from traditional to AI-enhanced operations.
These KPIs provide a clear map of how the technology improves both the clinical mission and the bottom line.
1. Report Turnaround Time
Speed is the most visible metric of a healthy radiology department, especially in high-stakes emergency environments. Reducing the time between scan completion and final report is a primary goal.
- Emergency TAT: Monitor the speed of results for critical findings like large vessel occlusions or pulmonary embolisms.
- Segmented Windows: Track average times for preliminary reads versus final reports to identify where delays occur.
- Critical Case TAT: Measure how quickly life-threatening cases are moved to the top of the queue compared to first-in-first-out historical data.
2. Radiologist Productivity
Productivity metrics should focus on the quality and volume of work performed without increasing staff exhaustion. AI helps clinicians handle more complex cases by taking over routine tasks.
- Case Throughput: Track the number of studies read per shift and the average time spent on specific modalities like CT or MRI.
- Task Automation: Measure the reduction in manual measurements and segmentation tasks now handled by the software.
- After Hours Relief: Analyze the impact of AI on on-call workloads and the speed of preliminary findings during night shifts.
3. Imaging Department Throughput
Maximizing the utilization of expensive imaging assets is a major revenue driver for any health system. Better workflow leads to more scans completed per day.
- Modality Utilization: Identify if MRI or CT machines are being used more consistently throughout the day due to faster processing.
- Wait Time Reduction: Monitor the time a patient spends from arrival to exam completion to ensure a smooth flow.
- Bottleneck Analysis: Use real-time data to find and remove scheduling delays that prevent full department capacity.
4. Follow Up And Referral Capture
Missing a follow-up recommendation is both a clinical risk and a loss of potential revenue. AI ensures that incidental findings are tracked through the entire care pathway.
- Finding Tracking: Monitor the percentage of patients with incidental findings who successfully schedule their recommended follow-up scans.
- Pathway Continuity: Track oncology or stroke patients to ensure they move smoothly into specialist referrals and treatments.
- Revenue Preservation: Calculate the value of procedures and hospitalizations generated through automated follow-up alerts.
5. Cost Avoidance
Operational ROI often comes from what you do not have to spend. Reducing wasted resources and unnecessary overhead directly impacts the margin.
- Outsourcing Reduction: Measure the decrease in spending on external teleradiology services as internal capacity grows.
- Administrative Load: Track the reduction in manual routing and coordination tasks previously handled by administrative staff.
- Waste Mitigation: Lower costs related to duplicate scans or delays that extend a patient’s length of stay in the hospital.
7. Clinical Outcome Indicators
Ultimately, the success of the investment is reflected in how it changes the patient’s journey through the facility.
- Time to Treatment: Measure the window between a critical scan and the start of life-saving interventions.
- Emergency Department Flow: Monitor the ED length of stay and how faster radiology results accelerate discharge or admission decisions.
- Safety Metrics: Track the reduction in diagnostic delays and the speed of critical result communication to referring physicians.
Establishing these specific benchmarks allows leadership to transform abstract technology goals into a transparent performance roadmap.
Consequently, tracking these indicators ensures the investment remains aligned with both clinical excellence and the long-term financial health of the enterprise.
What Costs Affect AI Radiology ROI?
AI radiology ROI depends on software development, PACS integration, model deployment, cloud infrastructure, compliance, monitoring, training, and ongoing support costs.
Understanding the investment required for a medical imaging platform is crucial for calculating a realistic break-even point. While high-end enterprise systems can reach millions, a strategically developed solution tailored for specific high-impact use cases offers a more accessible entry point.
Below is a breakdown of the typical capital allocation for an agile, enterprise-grade AI radiology platform.
Investment Overview Table
| Development Phase | Estimated Cost (USD) | Key Deliverables |
| Core AI Platform & Logic | $30,000 – $50,000 | Model selection, validation, and clinical UI |
| Integration & Interoperability | $10,000 – $30,000 | DICOM routing, HL7/FHIR, and PACS hooks |
| Infrastructure & Security | $5,000 – $20,000 | Cloud setup, GPU pipelines, and encryption |
| Compliance & Governance | $5,000 – $20,000 | HIPAA controls and performance monitoring |
| Total Estimated Investment | $50,000 – $120,000 | Ready-to-deploy enterprise solution |
1. AI Model And Platform Development Cost
The foundation of your return lies in the precision of the model and its clinical utility. This phase focuses on selecting the right architecture and validating it against diverse datasets to ensure high sensitivity.
- Strategic Selection: Choosing between pre-trained models or custom-developed logic to solve specific clinical problems.
- Clinical Review: Building the features that allow radiologists to interact with AI findings seamlessly.
- Validation Work: Ensuring the model performs consistently across different imaging hardware and patient demographics.
2. PACS, RIS, And EHR Integration Cost
A standalone AI is a liability while an integrated AI is an asset. Significant resources must be allocated to ensure the software communicates perfectly with the existing hospital infrastructure.
- Data Routing: Setting up DICOM listeners to capture and process images the moment they leave the scanner.
- Workflow Sync: Matching orders within the RIS and ensuring results are delivered back to the EHR in a standardized format.
- Seamless Access: Integrating AI overlays directly into the PACS viewer so clinicians do not have to switch windows.
3. Infrastructure And Deployment Cost
Processing high-resolution medical images requires specialized hardware and robust data pipelines. Consequently, the choice between cloud and on-premise setups significantly impacts long-term scalability.
- GPU Utilization: Provisioning the high-performance computing power needed for real-time image analysis.
- Image Pipelines: Building secure tunnels that move massive files through the analysis engine without latency.
- Scalability Planning: Ensuring the system can handle a sudden surge in scan volume without a drop in performance.
4. Compliance And Security Cost
In healthcare, security is not just a feature but a non-negotiable requirement. Protecting Protected Health Information (PHI) is a major part of the development and operational budget.
- Privacy Controls: Implementing strict HIPAA-compliant access controls and end-to-end encryption.
- Auditability: Maintaining detailed logs of who accessed which data and when for regulatory reviews.
- Data Retention: Configuring storage rules that comply with both medical record laws and hospital policies.
5. Monitoring And Governance Cost
Performance in the lab does not always translate to performance in the clinic. Ongoing monitoring ensures that the AI remains accurate as patient populations or imaging protocols change.
- Model Drift: Tracking performance over time to ensure the algorithm does not lose accuracy.
- Governance Dashboards: Implementing systems that allow clinical leads to audit AI decisions versus human findings.
- Feedback Loops: Creating a mechanism where radiologists can flag errors to improve the system iteratively.
This structured investment approach ensures that every dollar spent contributes directly to a measurable clinical or financial outcome.
Why Direct Reimbursement Is Not The Whole ROI Story
Investors often start the conversation by asking if a specific tool has a dedicated billing code. While direct payment is a factor, it rarely represents the full economic impact of the technology.
Relying solely on one-to-one reimbursement models overlooks the massive structural value that integrated software brings to a high-volume health system.
1. Many Radiology AI Tools Lack Direct Payment Codes
FDA clearance indicates safety and efficacy, but it does not guarantee that payers will cover the cost of the scan. In fact, most imaging software currently operates without a specific Category I payment code.
- Coding Reality: As of early 2026, while there are over 26 CPT codes for clinical AI, only a small fraction receive reliable national reimbursement.
- Temporary Status: Many tools carry Category III codes, which are primarily used for data collection rather than guaranteed payment.
- Internal Value: Because reimbursement lags behind innovation, the most successful hospitals focus on how AI creates value inside existing global payment or diagnostic-related group (DRG) workflows.
2. Workflow ROI Can Be More Important
Efficiency gains often outweigh the search for new billing codes by expanding the total capacity of the department. When a specialist can handle more volume without additional hours, the margin per study increases naturally.
- Throughput Optimization: Faster preliminary reads and automated triage allow the facility to process a higher volume of patients every day.
- Backlog Reduction: Systems that flag urgent cases prevent the costly administrative spiral of manual worklist management.
- Asset Efficiency: Reducing avoidable delays ensures that high-cost hardware like MRI suites stays productive throughout every shift.
3. Downstream Revenue Matters
The most significant financial returns often happen after the initial scan is completed. By identifying subtle findings early, AI acts as a feeder system for other high-value hospital services.
- Care Pathways: A single AI-detected finding can trigger follow-up imaging, specialist consultations, and interventional procedures.
- Leakage Prevention: Automated tracking ensures that patients stay within the hospital network for their long-term treatment and surveillance.
- Revenue Multipliers: Research has shown that additional clinically beneficial treatments performed due to AI identification are major contributors to a 451 percent five-year ROI.
4. Evidence Still Matters For Reimbursement
While the market currently emphasizes efficiency, building a strong evidence base is the only way to secure future dedicated payments. Payers require rigorous documentation of how a tool changes the clinical course for a patient.
- Outcome Studies: Capturing real-world data on how AI reduces the length of stay or improves recovery rates is essential.
- Utilization Tracking: Documenting the frequency and accuracy of AI findings provides the “economic impact” data that insurance companies demand.
- Performance Governance: Standardized monitoring ensures the software remains a reliable clinical partner as patient demographics evolve.
Focusing on the broader impact allows entrepreneurs to see that AI radiology ROI is about system-wide growth rather than just a collection of billing codes.
AI Radiology Use Cases With Strong ROI Potential
The strongest AI radiology ROI often comes from high-volume, time-sensitive, and downstream-heavy use cases such as stroke, PE, oncology, fractures, and follow-up management.
Strategic investors should focus on applications where minutes saved translate directly into better outcomes or increased billable activity. High-impact use cases solve specific operational pain points while simultaneously opening new revenue streams through enhanced diagnostic precision.
By targeting these specific clinical areas, a facility ensures its medical imaging software provides immediate and scalable value.
1. Stroke Imaging And Neuro Triage
In neurology, time is brain tissue, making neuro-triage one of the most profitable areas for automation. These systems act as an early warning mechanism that bypasses traditional manual sorting.
- Rapid Alerts: Software identifies large vessel occlusions and intracranial hemorrhages in seconds to notify stroke teams immediately.
- Treatment Routing: Faster detection enables quicker administration of life-saving interventions like thrombectomy or tPA.
- System Impact: Reducing the time to treatment lowers the long-term cost of care and improves the hospital’s status as a primary stroke center.
2. Pulmonary Embolism Detection
Pulmonary embolism (PE) represents a significant diagnostic challenge in busy emergency departments. AI tools ensure these high-risk cases do not sit at the bottom of a growing worklist.
- Critical Triage: Algorithms scan CT pulmonary angiograms to flag potential clots for priority review.
- Escalation Logic: The system automatically moves positive scans to the top of the radiologist’s queue to trigger faster care team escalation.
- Risk Mitigation: Early intervention reduces the likelihood of catastrophic outcomes and lowers the liability associated with diagnostic delays.
3. Chest X-Ray Triage
Chest X-rays are the highest volume study in most hospitals, but often have the lowest individual margin. Automation creates ROI here by managing the sheer scale of the workload.
- Normal vs. Abnormal: AI can instantly separate clear scans from those needing attention to let specialists focus on the complex cases.
- High Volume Support: In the ICU and ED, these tools identify pneumothorax or misplaced lines to prevent complications.
- Backlog Relief: Clearing the “normal” queue faster allows the entire department to maintain a steady and predictable patient flow.
4. Oncology Imaging Follow-Up
Oncology requires meticulous longitudinal tracking that is prone to human error and administrative gaps. AI provides a structured way to manage these high-value, long-term patients.
- Precision Tracking: Software automates lesion measurements and tumor tracking to ensure consistent comparisons across multiple years.
- Reminders and Alerts: Automated systems flag when a patient is due for surveillance, ensuring they return to the facility for their care.
- Workflow Automation: Reducing the manual effort of finding historical scans and measuring nodules increases the number of oncology cases a radiologist can handle per shift.
5. Fracture And Trauma Detection
Trauma centers benefit from AI by reducing the rate of missed findings during high-pressure shifts. This improvement directly impacts both patient safety and orthopedic referral volumes.
- X-ray Triage: AI identifies subtle fractures that might be missed by non-specialists in a crowded emergency room.
- Orthopedic Referrals: Faster and more accurate diagnosis leads to immediate specialist consultations and surgical planning.
- Patient Movement: Quicker disposition from the ED improves overall bed turnover and reduces boarding times for trauma patients.
6. Report Automation And Structured Reporting
The final stage of the radiology process is often the most time-consuming. Streamlining the creation of the final report offers a direct boost to daily productivity.
- Draft Assistance: AI can prepopulate reports with measurements and findings to save significant dictation time.
- Standardization: Structured templates ensure that referring physicians receive clear and consistent data to drive their treatment plans.
- Time Savings: Eliminating repetitive manual data entry allows the medical staff to focus on clinical interpretation rather than clerical work.
Selecting high-impact use cases like stroke triage or oncology tracking ensures that the technology addresses the most time-sensitive and revenue-dense areas of the hospital.
Consequently, focusing on these proven applications allows leadership to secure a faster path to a measurable AI radiology ROI while simultaneously elevating the standard of patient care.
Why Some AI Radiology Investments Fail To Show ROI
AI radiology investments fail when hospitals buy standalone tools without workflow integration, baseline metrics, clinician adoption, governance, or measurable business outcomes.
High-profile technology failures in healthcare rarely stem from poor algorithms. Instead, they occur when advanced software is dropped into an environment that is not prepared to measure or manage its impact.
Understanding these common pitfalls allows investors to build a more resilient implementation strategy that prioritizes long-term utility over short-term novelty.
1. No Baseline ROI Metrics
It is impossible to prove a return on investment if the organization does not know its starting point. Without a clear financial and operational baseline, even the most successful pilot program remains an anecdotal success.
- Missing Benchmarks: Many facilities fail to record pre-AI turnaround times or cost-per-study figures before the software goes live.
- Leakage Ignorance: Hospitals often lack data on how many patients currently miss their follow-up appointments, making it hard to credit AI for improvements.
- Ill-Defined Success: A project without specific, numerical goals for productivity and patient flow often loses its executive support during the first budget review.
2. Poor PACS And RIS Integration
The quickest way to kill clinical adoption is to force a radiologist to change their workflow for a single tool. Software that operates in a silo is often ignored or actively avoided by the medical team.
- Workflow Friction: Forcing clinicians to use separate dashboards or duplicate logins creates a “cognitive tax” that slows down their day.
- Alert Fatigue: Systems that push too many notifications without clinical context cause specialists to tune out even the most critical findings.
- Adoption Barriers: If the AI findings do not appear directly within the primary viewer, the tool becomes a burden rather than a benefit.
3. Low Imaging Volume
The economic engine of AI radiology ROI is volume. A sophisticated model used on a handful of cases per month will rarely generate enough value to cover its development and integration costs.
- Niche Limitations: Investing in narrow use cases that only appear occasionally results in a very slow payback period.
- Underutilization: Expensive GPU infrastructure and cloud pipelines must be offset by high-frequency processing to remain financially viable.
- Scale Requirements: Strategic investors should target areas like chest X-rays or emergency CT scans where the sheer scale of the workload justifies the automation.
4. No Downstream Workflow Capture
Identifying a finding is only the first half of the value chain. ROI is lost when a hospital fails to notify the care team or schedule the necessary follow-up treatment.
- Broken Chains: If the AI flags a lung nodule but there is no automated referral path, the potential for downstream revenue disappears.
- Patient Navigation: Without a system to guide the patient through the next steps of their treatment, the clinical insight never translates into a business outcome.
- Tracking Gaps: Facilities must be able to track a patient from the initial AI flag all the way to the final specialist consultation or procedure.
5. Weak Model Monitoring
Performance in a controlled test environment does not always match real-world clinical use. Neglecting the ongoing governance of the system can lead to significant clinical and financial risks.
- Performance Drift: Algorithms can lose accuracy as imaging protocols change or patient demographics shift over time.
- Governance Gaps: A 2025 JAMA Network Open systematic review highlighted that while radiology dominates FDA approvals, less than 2 percent of devices were supported by prospective clinical trials.
- Documentation Gaps: Many cleared devices lack detailed public data on demographics or study designs, making it essential for hospitals to conduct their own continuous internal audits.
Addressing these failure points transforms a technology project into a robust enterprise solution. Consequently, a focus on integration and measurement ensures the platform delivers on its promise of a high-yield AI radiology ROI.
How We Calculate AI Radiology ROI For Healthcare Enterprises
Determining the financial viability of a new imaging platform requires more than a simple comparison of costs and revenue. At Intellivon, we use a structured framework to ensure every dollar invested generates a clear and defensible return.
This seven-step process transforms complex clinical data into a transparent business case that resonates with healthcare boards and private investors.
Step 1: Establish The Performance Baseline
Before a single line of code is deployed, we must understand the current limitations of your imaging department. This step involves a deep dive into your existing operational data to set a benchmark for future comparison.
- Current Volume: We analyze the number of scans processed per modality across all shifts.
- Reporting Metrics: Our team measures average turnaround times for routine versus emergency cases.
- Economic Gaps: We identify current follow-up leakage and the total spend on external teleradiology services.
Step 2: Define High-Yield Use Cases
Not all AI applications offer the same financial potential for every facility. We work with your clinical leads to select the specific workflows that will drive the highest impact.
- Triage Focus: Evaluating the ROI potential of stroke, pulmonary embolism, or chest X-ray triage.
- Longitudinal Growth: Assessing how oncology tracking or fracture detection can build sustainable downstream revenue.
- Operational Fit: Ensuring the selected AI use case matches your specific patient demographics and equipment inventory.
Step 3: Model Workflow Integration
Efficiency is lost if the technology does not fit naturally into the hands of the clinician. We design the integration path to ensure the software acts as a productivity multiplier rather than a distraction.
- PACS Deep Links: Creating a seamless connection so AI findings appear directly in the primary viewing environment.
- Automated Routing: Setting up logic that moves critical cases to the top of the worklist without manual oversight.
- Unified Access: Minimizing friction by eliminating separate logins or redundant data entry tasks.
Step 4: Estimate Direct Financial Gains
This phase focuses on the hard numbers that move the needle for your bottom line. We calculate how specific speed and accuracy gains translate into billable growth.
- Capacity Expansion: Estimating the revenue from additional cases handled due to reduced reporting times.
- Revenue Capture: Quantifying the value of necessary follow-up scans and specialist referrals identified by the AI.
- Cost Reduction: Calculating the savings from decreased outsourcing and lower administrative overhead.
Step 5: Account For Total Ownership Costs
Transparency regarding the investment is essential for long-term trust. We provide a comprehensive view of all expenditures, keeping your total project cost between $50,000 and $120,000.
- Development and Logic: Covering the initial build, model validation, and clinical review features.
- Technical Infrastructure: Accounting for cloud processing, GPU pipelines, and high security storage.
- Governance and Security: Including the costs for HIPAA compliance, PHI protection, and ongoing performance monitoring.
Step 6: Execute A Controlled Pilot
A phased rollout allows us to validate the ROI assumptions in a real-world clinical setting before a full enterprise launch. This step minimizes risk and allows for tactical adjustments.
- Baseline Comparison: Comparing the first three months of AI-assisted operation against your historical data.
- User Feedback: Gathering direct insights from radiologists to optimize the reporting interface and notification logic.
- Performance Audit: Verifying the accuracy of the model to ensure it meets the required clinical standards.
Step 7: Scale And Track Longitudinal Impact
True AI radiology ROI is measured in years rather than months. We provide the analytics tools needed to track performance as your facility grows and technology evolves.
- Impact Tracking: Reviewing 12-month financial results to verify the initial business case.
- Scalability Planning: Assessing the 3-year impact on your ability to handle larger patient volumes or more facilities.
- Long-term Projections: Modeling the 5-year ROI to ensure the platform remains a growth enabler for the entire enterprise.
This comprehensive methodology allows Intellivon to act as a strategic partner rather than a simple vendor. Consequently, our clients move forward with the confidence that their investment is grounded in operational reality and fiscal responsibility.
We also build AI-powered radiology platforms for your enterprise from the ground up within the cost we mentioned above. Our solutions are 100% ROI and scalability-driven.
Book a quick consultation call with our experts at Intellivon to get a quote and a strategic roadmap for your AI radiology platform.
Conclusion
Maximizing ROI in AI radiology requires a shift from viewing software as a cost center to treating it as a strategic growth engine. By prioritizing deep workflow integration and tracking high-impact clinical metrics, hospitals can unlock significant gains in both productivity and downstream revenue.
Success lies in selecting scalable, evidence-based solutions that align with long-term enterprise goals while consistently delivering measurable improvements in patient outcomes and operational efficiency.
Build ROI-Driven AI Radiology Systems With Intellivon
At Intellivon, we build AI radiology systems for hospitals, diagnostic imaging chains, teleradiology providers, healthtech companies, and radiology SaaS platforms. Our focus is simple: help healthcare teams reduce reporting delays, improve radiologist productivity, increase imaging throughput, and measure financial impact from the start.
A. Designing ROI-Focused AI Radiology Workflows
We start by understanding where the hospital is losing time, money, and capacity inside the radiology workflow.
This includes reporting delays, manual routing, critical case backlogs, missed follow-ups, repeat work, and radiologist workload pressure. Based on this assessment, we define the AI use cases that can create measurable operational and financial value.
What we cover:
- Radiology workflow mapping
- Current turnaround time benchmarks
- Cost-per-study analysis
- Imaging volume assessment
- Use case prioritization
- ROI measurement planning
This helps hospitals avoid random AI adoption and focus on systems that solve real business and clinical problems.
B. Building Secure Medical Imaging Pipelines
AI radiology depends on clean, secure, and well-structured imaging data. Intellivon builds medical imaging pipelines that move scans from hospital systems to AI models without disrupting radiologist workflows.
We design the system around DICOM ingestion, secure image routing, metadata normalization, study matching, and result delivery. This allows AI outputs to reach the right workflow at the right time.
What we cover:
- DICOM ingestion
- Image routing
- Metadata normalization
- Study matching
- Secure storage
- AI model processing
- PACS-ready result delivery
This gives hospitals a reliable foundation for AI-assisted radiology operations.
C. Integrating AI With PACS, RIS, And EHR Systems
AI creates ROI only when radiologists can use it inside their existing workflow. If the system forces teams to open another dashboard or manually check AI results, adoption drops.
Intellivon integrates AI radiology systems with PACS, RIS, and EHR platforms so radiologists can review AI findings, prioritize cases, and complete reports without unnecessary workflow friction.
What we cover:
- PACS integration
- RIS order matching
- EHR data connection
- HL7 and FHIR workflows
- Worklist updates
- Viewer-ready AI outputs
- Result exchange
This helps hospitals reduce extra clicks, avoid duplicate work, and improve radiologist adoption.
D. Scaling AI Across More Radiology Workflows
Once the first use case proves value, Intellivon helps hospitals expand AI across more modalities, departments, and locations.
A hospital may start with stroke triage, chest X-ray automation, or oncology follow-up support. From there, the system can scale into emergency imaging, trauma workflows, mammography, reporting automation, and multi-site radiology operations.
What we cover:
- Multi-modality expansion
- Multi-site deployment
- Additional AI use cases
- Centralized monitoring
- Enterprise access controls
- Scalable cloud or on-premise setup
- Long-term optimization
This allows hospitals to turn AI radiology from a single-use tool into a measurable imaging infrastructure.
If your hospital or radiology platform wants to build an AI radiology system that improves productivity, reduces reporting delays, and tracks ROI from day one, contact Intellivon to discuss your workflow, use case, and development roadmap.
FAQs
Q1. How do hospitals measure ROI from AI radiology?
A1. Hospitals measure AI radiology ROI through faster report turnaround, higher imaging throughput, fewer manual tasks, reduced outsourcing, better follow-up capture, and improved patient flow. The strongest ROI comes when AI is connected to PACS, RIS, EHR, and reporting workflows instead of working as a separate tool.
Q2. Does AI radiology always deliver financial ROI?
A2. No. AI radiology delivers ROI only when it solves a measurable workflow problem. Hospitals need enough imaging volume, clear use cases, strong integration, radiologist adoption, and performance tracking. If AI adds false alerts or extra steps, it can reduce efficiency instead of improving financial returns.
Q3. What affects the ROI of AI radiology solutions?
A3. AI radiology ROI depends on scan volume, use case complexity, integration depth, infrastructure cost, clinical adoption, reporting-time savings, and downstream care impact. A high-volume emergency, stroke, oncology, or chest imaging workflow usually has stronger ROI potential than a narrow, low-volume use case.
Q4. Is AI radiology ROI only about cost savings?
A4. No. Cost savings are only one part of ROI. Hospitals can also gain value from faster diagnosis, improved radiologist productivity, higher scan throughput, better follow-up completion, stronger patient flow, and reduced reporting delays. The best ROI comes from financial, operational, and clinical gains working together.