Healthcare organizations need Electronic Health Record systems to handle records, organize the work that doctors and nurses deal with, billing, and ensure they follow the rules, and bring all parts of patient care together. This system is used by every department and every person. It is also a huge part of every time a patient interacts with the organization, so choosing an EHR vendor is a very big decision.
The right Electronic Health Record vendor gives you more than a list of things it can do. They give you a base that helps with sharing data, following the rules, making sure the system can grow, and working smoothly with the systems you already have. All of these things affect how well the system works across departments and over time.
In this blog, we talk about the technical things to consider when evaluating EHR vendors and what healthcare leaders and people who invest in health technology should think about when they choose an EHR vendor, so they can decide with clarity and confidence.
Why EHR Implementations Fail in Real Operations
Most EHR vendor choices fail after they go live. This is because workflows often don’t match real clinical operations, support drops post-implementation, and systems struggle to scale as demand grows.
Most enterprise health projects fail when rigid software meets the reality of complex clinical workflows. Leaders often pick a pretty interface but ignore the weak data engine underneath, leading to massive operational friction.
1. Feature-based selection vs system-level thinking
Procurement teams often use a “checkbox” approach, picking the vendor with the most features. However, a long list of tools doesn’t mean the system actually works together.
System-level thinking focuses on how data flows from the bedside to the billing office. If the architecture is fragmented, even the best features will stay siloed and underused.
2. Hidden risks in legacy vendor architectures
Many established vendors hide old, clunky code behind a modern-looking web portal. This technical debt makes it hard to use modern security or real-time data streaming.
Furthermore, these closed systems often charge high fees just to access your own data. Choosing a legacy vendor creates a “vendor lock-in” that limits your ability to innovate later.
3. Why scalability issues appear post-deployment
A platform might look fast during a small pilot with ten users. However, true bottlenecks appear when five thousand clinicians log in at once.
Scalability includes how the database handles complex requests. If the system slows down during critical care moments, you lose the trust of your medical staff instantly.
4. Cost of poor interoperability decisions
Interoperability is often ignored during the initial sale, but it is the backbone of modern healthcare. When your EHR cannot interact with other apps, your data stays trapped.
This prevents you from using AI diagnostics or advanced patient engagement tools. Consequently, the enterprise loses the chance to perform deep analytics that could lower the cost of care.
5. Customization trap and technical debt
Heavy customization to match old workflows often breaks the vendor’s update path. You end up stuck on an old version of the software that is very expensive to maintain. Instead, look for platforms that offer flexible configuration.
This allows you to change business logic without breaking the core system or creating future debt.
Reliable EHR success depends on choosing an infrastructure that evolves with your growth. Strategic leaders prioritize flexible foundations over static feature lists to ensure lasting stability.
What Enterprise Buyers Actually Need From EHR Vendors
Selecting a platform is easy. However, choosing the right foundation is difficult. Enterprise leaders need a reliable backbone for their entire business.
If the technology is messy, your operations will stay messy. Therefore, you must prioritize long-term stability over short-term features.
1. Unified clinical and operational data layers
Most systems keep medical records and billing data in separate “buckets.” This creates extra work for your staff. Consequently, team members must enter the same information twice.
You need a single layer where all data lives together safely. This lets your doctors focus on patients while your finance team sees accurate revenue. Furthermore, you stop wasting time fixing mistakes between different departments.
2. Real-time data access across systems
In a fast-moving enterprise, old data is useless. You must know what is happening in your clinics right now. Real-time access means your dashboards update the second a patient checks in.
Therefore, you can manage your staff better. You also catch operational problems before they grow. However, if your vendor cannot provide instant data, they are actively slowing down your growth.
3. API-first architecture for long-term flexibility
An API-first design means the system talks to other software easily. You might want to add a new AI tool later. Perhaps you need a custom patient app next year. Without a strong API, you stay locked into only what the vendor offers.
Choosing a flexible architecture now saves you from a total system rebuild later. It gives you the power to innovate on your own terms.
4. Compliance-ready infrastructure from day one
Healthcare laws are very strict. These rules also change often. Hence, you cannot afford a system that treats security as an afterthought. Therefore, you need a platform built with high-level encryption. It must include detailed audit logs from the very start.
This protects you from massive fines. Furthermore, a compliance-ready setup allows you to expand into new regions without worrying about local data laws.
At this stage, the decision is no longer about choosing the right vendor. It is about building the right EHR infrastructure. This is where Intellivon works with healthcare enterprises to design and build scalable, API-first EHR platforms tailored to their operations.
EHR Vendor vs Custom Platform: What Scales Better
Choosing between a standard vendor and a custom platform is a high-stakes architectural decision. Most organizations eventually outgrow the rigid boundaries of off-the-shelf software.
Therefore, understanding the long-term limits of each model is essential for sustainable growth.
Limits of off-the-shelf EHR vendors
Standard vendors provide speed but often sacrifice control. These systems are built for the “average” clinic, not a complex enterprise. Consequently, unique clinical workflows must be forced into the software’s pre-set logic.
This creates massive friction for the medical staff. Furthermore, proprietary codebases make it nearly impossible to extract data for custom analytics without paying heavy integration fees.
When customization becomes mandatory
Generic software works until the business model evolves. Perhaps a unique patient engagement strategy is launched. Maybe a proprietary AI diagnostic tool needs to be integrated.
At this point, the “closed” nature of a standard vendor becomes a bottleneck. Customization becomes mandatory when the technology starts to dictate the business strategy rather than supporting it. Therefore, a shift toward a more flexible architecture is required to maintain a competitive edge.
Total cost of ownership comparison
Off-the-shelf systems appear cheaper at first glance. However, the hidden costs of per-user licensing and integration fees add up quickly. A custom or semi-custom platform requires a larger upfront investment.
Yet, the long-term total cost of ownership is often lower. There are no “success taxes” for adding more locations or users. Consequently, the enterprise gains a predictable cost structure that scales linearly with the business.
Hybrid approach: build on top of core systems
A “rip and replace” strategy is not always necessary. A hybrid approach uses a stable core system but builds a custom layer on top. This provides the security of a proven engine with the flexibility of a bespoke interface.
It allows for the rapid deployment of new features without breaking the underlying record-keeping. Furthermore, this strategy ensures that the enterprise owns the most valuable part of the stack, which is the data orchestration layer.
Key Technical Layers to Evaluate in Any EHR Vendor
Evaluating an EHR requires looking beneath the user interface to the core technical stack. A high-performing system relies on how well these hidden layers communicate. Therefore, a weakness in any single layer will eventually create a bottleneck for the entire enterprise.
1. Data architecture and storage models
Data storage is the foundation of any health platform. Many legacy systems use rigid, relational databases that struggle with unstructured clinical notes. Modern enterprises require a flexible data model that handles diverse information types without slowing down.
Furthermore, the storage must support high-concurrency access across multiple clinic locations. This ensures that the system remains responsive during peak hours when thousands of clinicians are active simultaneously.
2. Integration layer (HL7, FHIR, APIs)
A closed system is a liability in a connected healthcare world. The integration layer must support modern standards like FHIR and HL7 for seamless data exchange. However, true connectivity goes beyond simple file transfers. An advanced platform provides robust, well-documented APIs.
Consequently, third-party tools and internal applications can interact with the core record in real-time. This eliminates the need for expensive, custom-coded “bridges” between different pieces of software.
3. Workflow orchestration engine
An EHR should adapt to the clinic, not the other way around. The orchestration engine manages how tasks move from the front desk to the exam room. If this engine is hard-coded, changing a single step in a clinical protocol becomes a major IT project.
Therefore, leaders should look for a “low-code” or highly configurable engine. This allows the organization to optimize workflows on the fly without breaking the underlying data integrity.
4. Security and access control systems
Security is a non-negotiable requirement for patient trust and legal compliance. A sophisticated system uses Role-Based Access Control (RBAC) to ensure that staff only see what they need.
Furthermore, every action must be captured in a tamper-proof audit log. Encryption should protect data both at rest and during transit. Consequently, the enterprise stays protected against internal errors and external threats while meeting strict global privacy standards.
5. AI readiness and data structuring
Most AI initiatives fail because the underlying data is “messy” or unstructured. A future-proof EHR must capture data in a way that machines can understand immediately. This means using standardized terminologies and structured fields instead of just free-text boxes.
When data is clean and organized, deploying predictive models for patient outcomes or revenue cycles becomes a reality. This readiness turns the EHR from a simple record-keeping tool into a powerful engine for clinical intelligence.
Strategic leaders prioritize architectural integrity to build a data-driven environment that evolves with the enterprise. This is why Intellivon designs scalable, API-first ecosystems that move beyond the limits of traditional software.
Interoperability: Where Most Vendors Break Down
Interoperability failures in EHR systems are usually caused by inconsistent data mapping and restricted API access.
Reliable platforms must support modern standards like FHIR and HL7 to integrate labs, payers, and devices into a single, unified patient record layer.
1. Challenges in multi-system data exchange
Exchanging data between different platforms is rarely a “plug-and-play” process. Most systems use unique ways to label clinical data, which creates confusion during transfers. Consequently, a “blood pressure” reading in one system might not be recognized by another without manual mapping.
This lack of a common language leads to data loss and increased clinical risk. Furthermore, many legacy vendors intentionally limit data exports to prevent customers from switching to a competitor.
2. HL7 vs FHIR: what vendors actually support
While HL7 is the old industry standard, FHIR is the modern, web-based future of healthcare data. Most vendors say they support both, but their FHIR implementations are often limited to basic data sets. However, an enterprise needs deep, bi-directional access to truly innovate.
Therefore, a platform must offer full FHIR support to allow external apps to read and write data safely. This distinction determines whether an organization can use modern tools or remains stuck with slow, batch-file transfers.
3. Integrating labs, payers, pharmacies, and devices
A patient’s health journey involves more than just a clinic visit. It includes data from external labs, insurance claims, pharmacy records, and even wearable devices. Most vendors struggle to pull this outside information into the main clinical view.
Consequently, doctors must log into multiple portals just to see a complete picture of a patient’s health. A high-performing system acts as a central hub that pulls all these external data points into a single workflow.
4. Building a unified patient record layer
The ultimate goal of interoperability is a “single source of truth” for every patient. This layer should exist independently of any specific software module. It ensures that regardless of where a patient is treated, their entire history is available in one place.
Therefore, the architecture must prioritize a unified data layer that stays clean and organized. This approach eliminates duplicate records and ensures that every provider has the most accurate information at the point of care.
Reliable data exchange is the only way to ensure patient safety and operational efficiency across a large enterprise. Strategic leaders prioritize systems that treat connectivity as a core function rather than a paid add-on.
Evaluating Vendor Architecture for Scalability
Scalability is where most EHR systems either perform or break. While many vendors promise flexibility, their architecture often limits real-world growth.
To evaluate this properly, you need to look beyond features and focus on how the system behaves under pressure, across locations, and over time.
1. Monolith vs Microservices in EHR Systems
Most legacy EHR vendors still rely on monolithic systems. While these systems are easier to deploy initially, they struggle as complexity increases.
In contrast, microservices-based EHR platforms break the system into smaller, independent modules. This allows teams to update, scale, and manage components without affecting the entire system.
| Factor | Monolithic EHR Systems | Microservices EHR Systems |
| Architecture | Single unified codebase | Modular, independent services |
| Scalability | Scales as one unit | Scales individual components |
| Deployment | Risky, system-wide updates | Independent, safer deployments |
| Flexibility | Limited customization | High flexibility and adaptability |
| Failure Impact | One issue affects the entire system | Issues isolated to specific services |
If your organization plans to scale, microservices provide long-term stability and flexibility that monolithic vendors cannot match.
2. Handling High Patient Data Volumes
As patient data grows, performance becomes a critical factor. Many EHR vendors struggle with latency and data retrieval speed at scale.
A well-architected system should handle large datasets without slowing down clinical workflows.
| Factor | Traditional Vendor Systems | Scalable Data Architectures |
| Data Handling | Centralized, heavy databases | Distributed and optimized storage |
| Performance | Slows with data growth | Maintains speed at scale |
| Query Speed | Delays in large datasets | Optimized real-time querying |
| Data Processing | Batch-heavy processing | Real-time and event-driven |
| System Load | High strain under peak usage | Load is distributed across services |
Scalable data architecture ensures that performance remains consistent, even as patient volume and data complexity increase.
3. Multi-Location and Multi-Entity Scaling
Healthcare enterprises often operate across multiple hospitals, clinics, and regions. However, many vendor systems are not designed for distributed environments.
As a result, organizations face data silos, inconsistent workflows, and operational inefficiencies.
| Factor | Limited Vendor Systems | Enterprise-Ready Platforms |
| Multi-location Support | Basic or fragmented | Unified across locations |
| Data Consistency | Siloed data across units | Centralized patient records |
| Workflow Management | Inconsistent processes | Standardized workflows |
| Expansion | Difficult to onboard new entities | Seamless scalability |
| Governance | Hard to enforce policies | Centralized control and compliance |
A scalable EHR must support seamless expansion across locations while maintaining consistency and control.
4. Cloud-Native vs On-Premise Tradeoffs
Deployment architecture plays a key role in scalability. While on-premise systems offer control, they often limit agility and expansion.
Cloud-native EHR systems, on the other hand, are built to scale dynamically based on demand.
| Factor | On-Premise Systems | Cloud-Native Systems |
| Scalability | Limited by hardware | Elastic, on-demand scaling |
| Infrastructure | Requires manual setup | Managed and automated |
| Cost Model | High upfront investment | Pay-as-you-scale |
| Maintenance | Internal IT dependency | Managed by cloud providers |
| Accessibility | Restricted access | Secure access from anywhere |
Cloud-native architectures provide the flexibility and scalability required for modern healthcare operations.
Scalability rests in maintaining performance, consistency, and control as complexity increases. This is where vendor architecture decisions start to impact long-term success, and where many systems begin to fail.
Security, Compliance, and Risk Evaluation
Maintaining patient trust requires a security architecture that goes beyond simple password protection. A high-stakes enterprise environment must defend against sophisticated cyber threats while meeting strict global legal standards.
Therefore, security cannot be an added feature; it must be the core foundation of the entire system.
1. HIPAA, GDPR, and regional compliance layers
Global enterprises must navigate a complex web of different privacy laws. While HIPAA governs data in the United States, GDPR sets much stricter rules for patient rights in Europe. Consequently, a one-size-fits-all approach to compliance often fails during international expansion.
You need a system that can adapt its data handling rules based on the patient’s physical location. Furthermore, the platform must allow for “right to be forgotten” requests without breaking the core medical record.
2. Data encryption and access control models
Sensitive health data must stay encrypted, whether it is sitting on a server or moving across the internet. However, encryption is only effective if the access controls are equally strong. A modern system uses “least privilege” access, meaning staff only see the specific files needed for their job.
Therefore, a billing clerk cannot access clinical notes, and a nurse only sees their assigned patients. This granular control prevents internal data leaks and limits the damage of a compromised account.
3. Audit trails and governance systems
Every single interaction with a patient record must be recorded in a permanent, unchangeable log. These audit trails are essential for both legal defense and internal quality control. If a record is changed, the system must show who made the change and exactly when it happened.
Consequently, leadership can monitor for unauthorized access in real-time. This level of transparency builds a culture of accountability and ensures the enterprise is always ready for a surprise regulatory inspection.
4. Risk of breaches in legacy EHR systems
Older software was often built before modern cyber-attacks were a common threat. These legacy systems frequently have “backdoors” or unpatched vulnerabilities that hackers can easily exploit. Furthermore, they often lack the ability to integrate with modern multi-factor authentication tools.
Relying on an outdated EHR is a massive financial and reputational risk. Therefore, moving to a modern, security-first architecture is a vital business protection strategy.
Strong security protocols turn a potential liability into a significant competitive advantage for the enterprise. Strategic leaders invest in robust defense layers to ensure long-term clinical safety and financial stability.
Performance Metrics That Actually Matter
A slow EHR is a clinical hazard. System performance directly dictates the pace of care and the productivity of the entire medical staff. Therefore, measuring the right technical benchmarks is essential to ensure operational stability and patient safety.
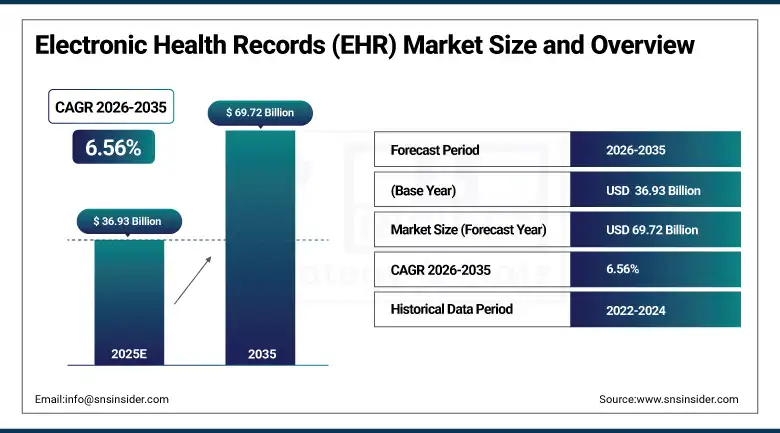
1. System latency in clinical workflows
Latency is the delay between a clinician’s click and the system’s response. In a high-volume clinic, even a two-second lag adds up to hours of lost productivity every week. Consequently, doctors spend more time looking at loading screens than interacting with patients.
This friction is a leading cause of administrative burnout and data entry errors. Therefore, a high-performing system must maintain sub-second response times for all core clinical functions.
2. Downtime impact on care delivery
System downtime is the most expensive risk an enterprise can face. When the EHR goes offline, clinical operations grind to a halt, and patient safety is compromised. However, many vendors only guarantee “network” uptime rather than “application” uptime.
An enterprise needs a platform with a redundant, high-availability architecture that ensures constant access to records. Furthermore, a clear disaster recovery plan must be in place to handle unexpected outages without data loss.
3. Data sync speed across systems
In a multi-clinic network, data must move instantly between different locations. If a lab result is updated in one facility, it should be visible across the entire enterprise immediately. Slow synchronization leads to duplicate testing and fragmented clinical decisions.
Therefore, the underlying data architecture must support real-time streaming rather than old-fashioned batch processing. This speed ensures that every provider always works with the most current patient information.
4. User load handling during peak hours
Many systems perform well during a morning pilot but crash during the mid-day rush. Peak hour handling measures how the database reacts when thousands of users log in simultaneously.
A rigid system will slow down or “lock up” under heavy traffic. Consequently, your staff faces frustrating delays during the busiest parts of their shift. A modern, cloud-native platform scales its resources automatically to maintain high speeds regardless of the total user count.
Measuring these technical metrics provides a clear picture of the system’s true operational value. Strategic leaders prioritize high-performance infrastructure to ensure their technology never becomes a barrier to quality care.
Vendor Evaluation Checklist for CTOs and CIOs
Financial leaders evaluate EHR vendors using a four-pillar framework: pre-shortlist questioning, proposal red flag identification, deep technical due diligence, and verified scalability proof.
This ensures the platform supports long-term interoperability and enterprise-level user loads.
1. Questions to ask before shortlisting vendors
A shortlist should only include vendors that meet modern architectural standards. Asking the right questions early prevents wasting time on legacy systems. Consequently, the following queries help filter out weak candidates:
- Does the platform support bi-directional FHIR APIs for all data fields?
- How does the system handle data residency across different global regions?
- Is the pricing model based on users, locations, or data volume?
- What is the historical application uptime over the last three years?
2. Red flags in vendor proposals
Marketing materials often hide technical limitations behind vague corporate language. However, certain “red flags” signal future operational pain. Furthermore, spotting these early saves the enterprise from expensive long-term mistakes:
- Proprietary Data Formats: Proposals that mention “custom data exports” often mean your data is trapped.
- High Integration Fees: Charging for every API connection is a sign of a closed ecosystem.
- Vague Scalability Claims: General statements about “cloud power” without specific concurrency tests are risky.
- Manual Update Paths: If updates require system downtime, the architecture is likely outdated.
3. Technical due diligence framework
Due diligence must go beyond a simple feature demo. Technical leaders should perform a deep “under the hood” inspection. This process ensures the system can actually handle the complexity of a multi-clinic network. Therefore, the evaluation team must review the API documentation and database schemas.
They should also verify the vendor’s security certifications and disaster recovery protocols. Consequently, this step eliminates the risk of discovering major flaws after the contract is signed.
4. Proof of scalability and integration success
The final test of any system is its performance in a real-world environment. Vendors must provide proof of success at a similar or larger scale. Furthermore, they should demonstrate how their platform integrates with third-party billing and lab systems.
Asking for a live “stress test” or a reference call with a high-volume client is essential. This verification confirms that the technology can grow as fast as the business without breaking.
A disciplined checklist ensures that the final selection is based on data rather than a sales pitch. Strategic leaders use these benchmarks to build a technology stack that empowers clinical excellence.
Cost of Choosing the Wrong EHR Vendor
Selecting the wrong vendor creates a “technical debt” that compounds every year. Initial savings on a cheaper license often disappear when the system fails to meet real-world demands.
Therefore, the true cost of a bad choice is measured in lost time and expensive emergency fixes.
1. Integration rework costs
A closed system requires expensive “middleware” just to talk to other software. When a vendor does not offer open APIs, every new connection becomes a custom project. Consequently, the organization pays developers to build “bridges” that break every time the software updates.
This cycle of constant rework drains the IT budget. Furthermore, it prevents the business from adopting new medical technologies quickly.
2. Operational inefficiencies over time
Small delays in a clinical workflow might seem minor at first. However, these seconds of friction turn into thousands of wasted hours across a large enterprise. Staff members often develop “workarounds” to bypass clunky software features.
This leads to data silos and manual spreadsheet tracking outside the EHR. Therefore, the system intended to improve efficiency actually becomes the primary cause of operational slowdowns.
3. Compliance and legal risks
Security flaws in an outdated platform are a massive liability. If a vendor fails to keep up with regional privacy laws, the enterprise faces heavy fines. Furthermore, a single data breach can destroy patient trust and damage the brand permanently.
Consequently, the cost of a “cheap” system is often much higher than a secure one. Legal defense and regulatory penalties can quickly exceed the original price of a premium platform.
4. Long-term scalability limitations
Many systems hit a “ceiling” where they can no longer handle more users or data. When this happens, the only solution is a total system replacement. This process is incredibly disruptive to clinical care and extremely expensive.
However, a scalable architecture grows with the business without requiring a complete rebuild. Therefore, choosing a limited platform today guarantees a massive capital expense in the near future.
A strategic investment in the right infrastructure prevents these hidden financial drains. Leaders prioritize long-term stability to ensure their technology remains an asset rather than a liability.
Conclusion
Choosing the right EHR vendor is not just a software decision. It is a long-term infrastructure decision that impacts scalability, integration, and performance. While vendors may meet initial needs, many fall short as complexity grows.
That is why enterprises increasingly look beyond vendor solutions. Instead, they invest in EHR platforms built around their operations. By focusing on architecture, not just features, organizations can build systems that support growth, adaptability, and better care delivery over time.
Build an EHR Platform With Intellivon
At Intellivon, EHR platforms are built as enterprise healthcare infrastructure, not as software layered onto fragmented clinical and operational systems. The objective is to create a unified platform that connects patient data, workflows, and integrations into a single, scalable environment.
Each platform is designed to support the full clinical and operational lifecycle. This includes patient records, clinical documentation, decision support, scheduling, billing, interoperability, and real-time data access. As a result, healthcare organizations gain complete visibility, reduce administrative burden, and improve care delivery across systems.
Our engineering approach focuses on AI-first, API-driven architectures combined with interoperability standards like HL7 and FHIR. This ensures seamless integration with EHRs, labs, pharmacies, payers, and third-party systems without disrupting existing operations.
Why Intellivon for EHR Platform Development
- Clinical infrastructure, not just software: Platforms are built to support long-term healthcare operations, not short-term feature requirements.
- Designed for interoperability from day one: Seamless integration with healthcare systems ensures consistent, real-time data exchange across the ecosystem.
- Built for scalability and performance: Architectures support high data volumes, multi-location operations, and complex workflows without compromising speed or reliability.
- AI-ready and future-proof systems: Structured data layers enable advanced analytics, automation, and decision support capabilities.
Whether you are replacing a legacy system or building a new EHR platform, Intellivon helps you design, build, and scale with confidence.
Talk to Intellivon’s healthcare experts to get a tailored architecture roadmap and cost estimate for your EHR platform.
FAQs
Q1. What should I look for in an EHR vendor?
A1. You should look beyond features and evaluate the system’s architecture, scalability, and integration capabilities. A strong EHR vendor should support interoperability (HL7, FHIR), handle high data volumes, and align with your clinical workflows. In addition, assess post-go-live support, security standards, and the ability to customize or extend the system as your organization grows.
Q2. How do I evaluate EHR vendor architecture?
A2. Start by understanding whether the system is monolithic or microservices-based. Then, evaluate its integration layer, data architecture, and scalability under real-world conditions. Check how it handles interoperability, real-time data exchange, and multi-location operations. Most importantly, ensure the architecture can evolve with your organization’s needs without requiring major system overhauls.
Q3. What is API-first EHR development?
A3. API-first EHR development means designing the system with APIs at its core, allowing seamless integration with other healthcare systems. Instead of building isolated modules, every function is accessible through APIs. This enables faster integrations with labs, devices, billing systems, and third-party tools. As a result, organizations gain flexibility, scalability, and better control over their healthcare ecosystem.
Q4. How long does EHR implementation take?
A4. EHR implementation timelines vary based on complexity and scope. Basic vendor deployments may take 3 to 6 months, while enterprise-level implementations can take 6 to 12 months or more. Custom-built EHR platforms may take longer initially, but they reduce future rework by aligning with your workflows and integration requirements from the start.
Q5. Should enterprises build or buy EHR systems?
A5. Enterprises can buy EHR systems for faster deployment and lower upfront effort. However, as integration complexity and scalability needs increase, vendor systems may become limiting. Building a custom EHR platform offers greater flexibility, control, and long-term ROI. The right choice depends on your operational complexity, growth plans, and need for system ownership.