Healthcare leaders in large organizations understand why specialty EHR systems are important. They struggle with what it actually takes to create one that can handle scale. Generic platforms were never designed for the operational needs of oncology networks, behavioral health groups, or multi-site surgical centers. This leads to fragmented workflows, gaps in compliance, and clinical teams working around the system instead of using it.
Specialty EHR systems address this issue by being built around how a specific clinical field functions. Instead of forcing a cardiology practice to use a template meant for primary care, these systems reflect actual workflows, include specialty-specific documentation, and link the appropriate data to support decisions at the right time. This connection between clinical practice and system design is what leads to better outcomes, more efficient operations, and improved ROI.
At Intellivon, we create healthcare platforms designed for this level of accuracy. Our teams have extensive healthcare knowledge, full-stack AI skills, and practical experience with complex, compliance-ready systems in global enterprise settings. In this blog, we’ll discuss the architectural choices, compliance frameworks, AI integration strategies, and development methods that make specialty EHR platforms truly scalable.
Why Generic EHR Systems Fail Specialty Care
Generic EHR systems often struggle in specialty care because they follow a one-size-fits-all design. They lack tailored workflows, specialty templates, and deep integrations required in fields like cardiology, oncology, or dermatology. As a result, clinicians face workflow gaps, manual workarounds, and slower decision-making. Over time, this directly impacts care quality and operational efficiency.
Market trends reflect this shift. Up to 30% of healthcare practices are now replacing their EHR systems, largely due to poor specialty fit. This growing dissatisfaction is pushing enterprises toward specialty-focused EHR platforms built for precision, scale, and long-term adaptability.
1. Workflow gaps in cardiology, oncology, etc.
Specialized departments operate on logic that general EHRs simply cannot replicate. In cardiology, for instance, clinicians need immediate access to longitudinal EKG data and imaging within a single view.
However, generic systems often require multiple logins or fragmented screens to view a single test. This friction creates “cognitive debt,” forcing doctors to manually bridge data gaps. Consequently, these manual workarounds increase the risk of oversight and clinical errors across the enterprise.
2. Limits of one-size-fits-all EHR platforms
The primary limitation of a “one-size-fits-all” platform is its rigid data architecture. These systems are typically designed for the “average” patient encounter, which centers on primary care.
Therefore, a specialty EHR brand must accommodate vastly different data sets, such as Mohs surgery mapping or complex joint-space analysis. Because the underlying database is built for simplicity, it cannot handle the multi-dimensional data required by a specialist. This forces clinicians to shoehorn complex medical data into generic text fields that are impossible to query or analyze later.
3. Impact on care quality and revenue cycles
When documentation is non-intuitive, financial health inevitably suffers. If a specialist cannot easily capture the specific complexity of a procedure, the coding often defaults to a lower level. This results in significant “revenue leakage” because the EHR fails to justify the actual intensity of care provided.
In addition, incomplete data capture leads to frequent claim denials. Therefore, the enterprise loses money on every complex patient encounter simply because the software cannot document the work accurately.
4. Why enterprises outgrow standard EHR tools
As an organization expands, the need for data autonomy becomes paramount. Standard tools often become “walled gardens” that make it difficult to extract data for advanced AI analytics.
Enterprises reach a tipping point where the cost of daily inefficiency exceeds the cost of building a bespoke, scalable solution. Growth-minded leaders realize that their software must be as specialized as their medical staff to remain competitive.
Choosing a digital foundation that aligns with your clinical reality is the only way to ensure long-term growth. Moving toward a specialty-focused architecture is now a strategic necessity for any organization looking to lead.
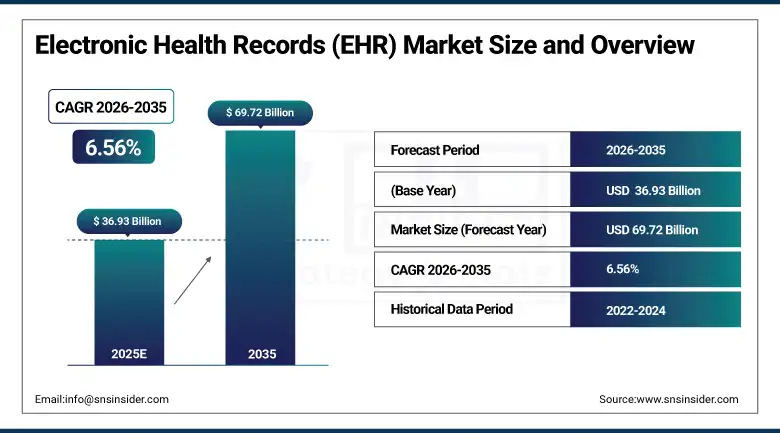
What Is a Scalable Specialty EHR System?
A scalable specialty EHR system is a healthcare platform designed to support deep, specialty-specific clinical workflows while handling growing patient volumes and multi-site operations. It combines tailored templates, diagnostics, and coding systems with a cloud-based infrastructure that scales easily.
As a result, healthcare providers maintain performance, interoperability, and efficiency without replacing systems as their practice expands.
Role of Real-Time Data and Unified Workflows
Static data is a liability in high-acuity specialty care. For enterprises, the shift toward real-time data synchronization and unified workflows is the only way to eliminate clinical lag and financial oversight.
1. Instantaneous Clinical Decision Support
Real-time data integration allows the EHR to function as an active participant in care rather than a passive filing cabinet. In specialties like neurology or cardiology, seconds matter.
Therefore, having live telemetry data or acute lab results stream directly into a unified dashboard enables immediate intervention. This synchronization ensures that every clinician, from the surgeon to the pharmacist, operates on a “single source of truth.”
2. Streamlining Inter-Departmental Handoffs
Unified workflows dissolve the traditional silos between specialty departments and administrative back-offices. When a specialty EHR brand automates the transition from a clinical procedure to a billing event, it removes manual data entry risks.
Consequently, this alignment reduces the “denial rate” by ensuring that all clinical documentation meets payer requirements the moment it is generated.
3. Predictive Operational Analytics
A unified data stream provides leadership with a live heat map of enterprise performance. By analyzing patient throughput and resource allocation in real-time, COOs can identify bottlenecks before they impact the bottom line.
In addition, this visibility allows for more agile staffing models, ensuring that high-demand specialty wings are never under-resourced during peak hours.
Ultimately, the marriage of real-time data and unified workflows transforms the EHR into a strategic asset. It empowers clinicians to provide safer care while giving executives the granular transparency needed to drive sustainable growth across the entire enterprise.
Key Features of Specialty EHR Platforms
To transition from a cost center to a value driver, an enterprise EHR must move beyond basic data entry. High-performance specialty platforms integrate clinical intelligence directly into the user interface, ensuring that the software adapts to the physician, not the other way around.
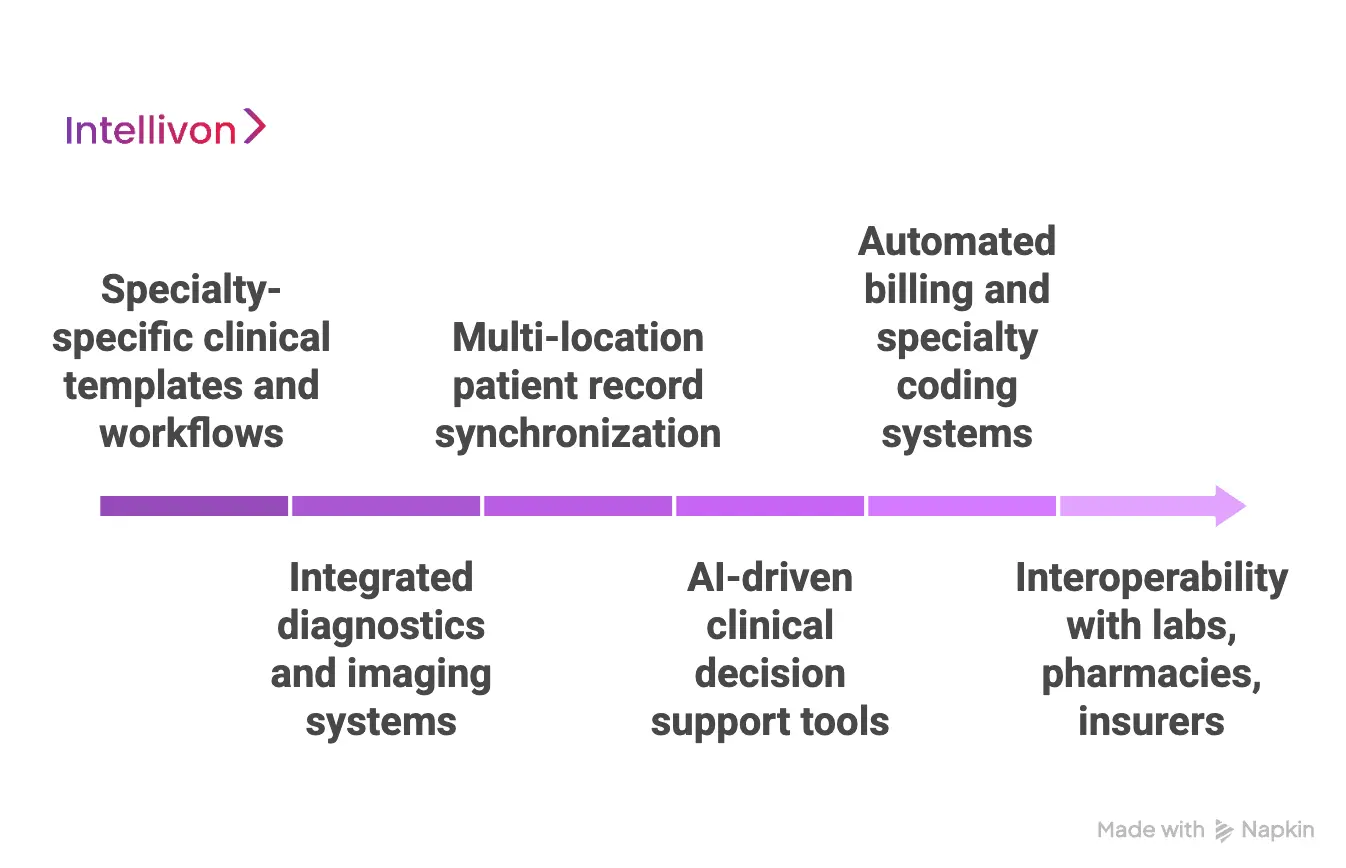
1. Specialty-specific clinical templates and workflows
Generic templates are the primary cause of clinician burnout and data fragmentation. Specialty-specific EHR brands provide pre-configured workflows designed for the unique “path of care” in fields like orthopedics or neurology.
For example, an orthopedic surgeon requires a template that captures range-of-motion data and joint-space measurements as discrete data points. Therefore, using “smart forms” that trigger based on the patient’s diagnosis ensures the enterprise captures the granular data necessary for clinical excellence and accurate reimbursement.
2. Integrated diagnostics and imaging systems
In specialty care, the diagnosis is often inseparable from the image. A scalable EHR platform treats PACS and DICOM data as native components of the record. When a specialist views high-resolution MRIs or retinal scans directly within the patient’s timeline, the “time-to-decision” drops significantly.
This integration eliminates the need for third-party viewers that slow down the clinical encounter. Consequently, the enterprise benefits from increased throughput and a higher standard of diagnostic accuracy.
3. Multi-location patient record synchronization
For enterprises operating across multiple regions, data latency is a significant operational risk. Multi-location synchronization ensures a patient’s record updates in real-time, regardless of where they receive care. If a patient visits a specialty clinic in one city and an infusion center in another, the records must merge instantly.
This “borderless” data flow prevents the duplication of expensive tests and ensures medication reconciliation remains accurate. Therefore, a high-availability cloud architecture is essential for maintaining a global view of patient health.
4. AI-driven clinical decision support tools
Modern specialty EHRs leverage AI for active clinical guidance. These tools act as a “second set of eyes,” scanning vast amounts of patient data to identify subtle trends. For instance, in a cardiology workflow, the system can flag early indicators of heart failure by analyzing historical EKG patterns.
Moreover, these tools automate the “prior authorization” process by matching clinical notes against insurance criteria in real-time. This reduces the administrative burden and ensures treatment plans proceed without delay.
5. Automated billing and specialty coding systems
Revenue cycle management in specialty care is complex due to niche procedure codes. Automated billing systems use natural language processing to “read” clinical notes and suggest accurate CPT codes.
This eliminates manual guesswork that leads to under-coding or audit risks. In addition, these systems understand specialty-specific logic, such as bilateral procedures in ophthalmology. By automating the link between clinical documentation and financial output, the enterprise protects its margins and ensures a predictable cash flow.
6. Interoperability with labs, pharmacies, and insurers
No specialty clinic exists in a vacuum. A scalable EHR serves as a high-speed hub for external data exchange with national lab chains, specialty pharmacies, and insurers.
When a specialist orders a complex biopsy, the results flow back as structured data rather than static PDFs. Furthermore, direct integration with specialty pharmacies ensures complex biologics are authorized and delivered quickly. This interoperability is the foundation of value-based care, allowing for seamless sharing of outcomes data to negotiate favorable payer contracts.
Ultimately, these features define the difference between a record-keeping tool and a strategic clinical engine. By prioritizing these specialized capabilities, an enterprise can secure its operational future and deliver superior patient outcomes at scale.
Core Architecture Behind Scalable EHR Systems
Building a digital foundation for specialty care demands a structural rethink of how medical data moves. Modern enterprise systems must prioritize modularity and resilience to handle the explosive growth of specialty data sets.
1. Cloud-native infrastructure for healthcare scale
Legacy on-premise servers often fail when an enterprise scales across multiple regions or integrates high-resolution diagnostic imaging. Cloud-native infrastructure provides the elasticity needed to handle these fluctuating workloads without compromising speed.
By leveraging auto-scaling groups, the system can allocate more resources during peak clinic hours and scale down during off-peak times.
This approach ensures that performance remains consistent even as the patient database grows into the millions. Therefore, the cloud is a fundamental requirement for operational agility.
2. Microservices vs monolithic EHR architecture
Traditional “monolithic” EHRs are built as a single, massive codebase, which makes even minor updates risky and time-consuming.
In contrast, a microservices architecture breaks the system into smaller, independent services like “billing,” “scheduling,” or “imaging.” This modularity allows developers to update a specific specialty module without taking the entire system offline.
Consequently, the enterprise experiences higher uptime and faster deployment cycles for new clinical features. Moving away from a monolith is essential for specialty EHR brands that want to remain adaptable in a rapidly changing regulatory environment.
3. API-first design for ecosystem integration
An API-first strategy ensures that the EHR serves as a central hub rather than a closed silo. By building robust, well-documented APIs from the start, an enterprise can seamlessly connect with third-party tools like wearable devices or remote monitoring platforms.
This design philosophy allows for “plug-and-play” connectivity with specialized diagnostic software used in fields like ophthalmology or oncology.
In addition, it simplifies the process of data exchange with external health systems and research institutions. Therefore, an open API architecture is the key to future-proofing your clinical ecosystem.
4. HL7 and FHIR for interoperability compliance
Interoperability is not just a feature; it is a federal mandate that dictates how healthcare data must be shared. Utilizing HL7 and specifically FHIR (Fast Healthcare Interoperability Resources) ensures that the system can communicate with any other compliant platform. FHIR uses modern web standards to make data exchange faster and more secure than older protocols.
This standardization is critical for enterprises that need to aggregate data from multiple disparate sources for population health management. Consequently, adhering to these standards reduces the cost of integration and minimizes the risk of compliance penalties.
5. Data pipelines for real-time patient workflows
Scaling a specialty system requires sophisticated data pipelines that process information as it happens. Unlike batch processing, which updates records in chunks, real-time pipelines ensure that a lab result or a vitals update is reflected across all modules instantly.
This immediacy is vital for high-stakes environments where a delay in data could impact a surgical outcome. In addition, these pipelines can feed live data into AI models for “on-the-fly” clinical decision support.
Maintaining a continuous flow of high-quality data is the only way to ensure that the enterprise operates at peak efficiency.
Selecting the right architectural framework is the most significant technical decision an enterprise leader can make. A well-designed backend ensures that the system remains a growth enabler rather than a technical bottleneck as the organization expands.
How Specialty EHR Systems Scale with Growth
Scaling a healthcare enterprise requires a digital foundation that expands alongside your clinical footprint without degrading performance.
A truly scalable system ensures that as you add more clinics or data points, the user experience remains fast, reliable, and clinically intuitive.
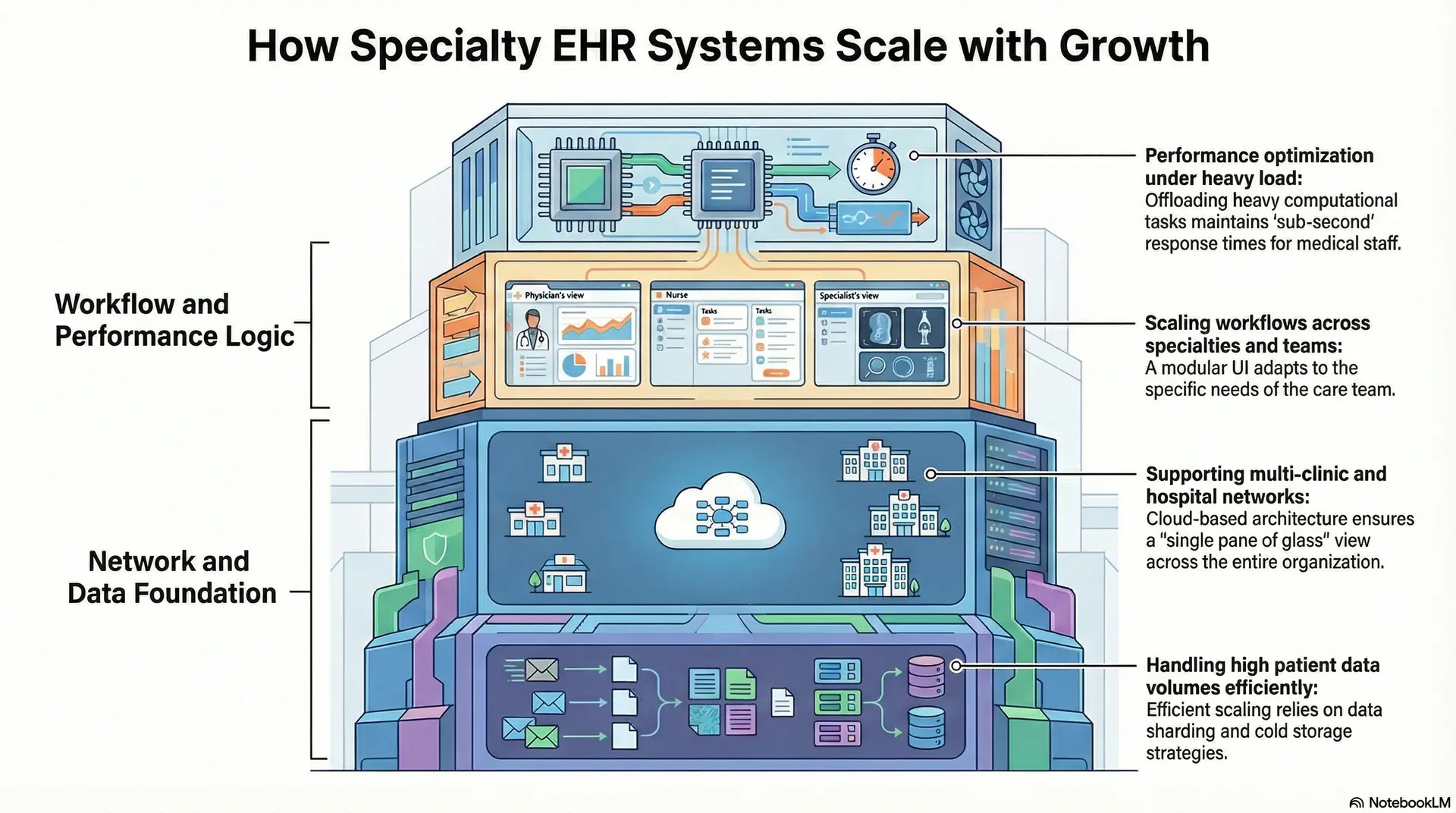
1. Supporting multi-clinic and hospital networks
Managing a distributed network of clinics requires a centralized data strategy that provides a “single pane of glass” view across the entire organization. Therefore, a cloud-based architecture is essential for ensuring that a specialist in one location has the same real-time access as a surgeon in another.
- Centralized Credentialing: Streamline provider access across multiple facilities through a unified identity management system.
- Standardized Clinical Protocols: Deploy consistent specialty-specific templates across the network to ensure uniform care quality.
- Global Resource Scheduling: Optimize patient throughput by viewing provider availability across all integrated hospital wings.
Consequently, multi-clinic synchronization reduces administrative overhead and prevents the creation of data silos that typically plague growing specialty EHR brands.
2. Handling high patient data volumes efficiently
As an enterprise grows, the sheer volume of high-resolution imaging, genomic data, and longitudinal records can strain traditional databases.
Efficient scaling relies on “data sharding” and cold storage strategies that keep active patient records immediately accessible while archiving older data.
- Blob Storage for Imaging: Utilize scalable object storage for massive DICOM and PACS files to prevent database bloat.
- Indexed Search Architectures: Implement advanced indexing to ensure that clinicians can retrieve specific patient history in milliseconds, regardless of database size.
- Automated Data Tiering: Move inactive records to lower-cost storage tiers to optimize operational expenses without losing data integrity.
In addition, these strategies ensure that the system remains responsive even when managing millions of unique patient encounters. Therefore, data volume becomes a strategic asset for research rather than a technical liability.
3. Scaling workflows across specialties and teams
A scalable system must be “specialty-aware,” allowing a cardiology workflow to coexist seamlessly with an oncology module on the same platform.
This requires a modular UI that adapts to the specific needs of the care team currently logged in.
- Role-Based Access Control (RBAC): Tailor the interface to surface only the most relevant data for specific specialists and nursing staff.
- Dynamic Workflow Logic: Automate task handoffs between different departments, such as moving a patient from diagnostic imaging to a surgical consult.
- Cross-Specialty Data Mapping: Ensure that core vitals and allergy lists are shared across all specialty modules while maintaining niche-specific documentation.
This flexibility allows the enterprise to onboard new specialty lines quickly, reducing the time-to-market for new clinical services. Consequently, the EHR acts as a catalyst for service line expansion.
4. Performance optimization under heavy load
System latency is the primary enemy of clinical efficiency during peak hours. High-performance specialty EHR brands utilize content delivery networks (CDNs) and edge computing to process data closer to the clinician.
- Load Balancing: Distribute incoming traffic across multiple server clusters to prevent any single point of failure during high-volume periods.
- Database Read-Replicas: Use secondary database copies for reporting and analytics to keep the primary database free for clinical documentation.
- Asynchronous Processing: Handle non-critical tasks, like generating patient statements or syncing to external registries, in the background.
By offloading heavy computational tasks, the system maintains “sub-second” response times for the medical staff. Therefore, the enterprise can confidently scale its patient volume without fearing a total system slowdown.
Transitioning from a localized clinic to a massive healthcare network requires a system that views growth as a design requirement. By prioritizing these scaling mechanisms, leaders can ensure their digital infrastructure supports, rather than hinders, their long-term vision.
Types of Specialty EHR Systems Enterprises Build
Enterprises are moving away from horizontal platforms toward verticalized solutions that mirror the clinical reality of each department. By building modular, department-specific systems, organizations ensure that every specialist works within a digital environment tailored to their precise medical logic.
1. Oncology EHR systems with treatment workflows
Oncology requires managing complex, long-term data that standard systems simply cannot provide. A specialized oncology module focuses on the “staged” nature of cancer care, integrating chemotherapy infusion scheduling with real-time lab monitoring.
- Dynamic Dose Calculation: Automatically adjusts chemotherapy doses based on fluctuating patient weight and toxicity levels.
- Staging Visualization: Provides a clear timeline of cancer progression and treatment response over multiple years.
- Toxicity Tracking: Flags adverse reactions immediately to ensure patient safety during aggressive treatments.
Consequently, specialty EHR brands in this space prioritize oncology-specific flowsheets that visualize the entire treatment arc at a glance.
2. Cardiology EHR systems with imaging integration
In cardiology, the diagnostic image is the core of the patient record. A high-performance cardiology EHR treats telemetry streams and high-resolution images as native inputs rather than external attachments.
- Native DICOM Viewing: Allows doctors to view echocardiograms and angiograms directly within the patient’s chart.
- Side-by-Side Comparison: Overlays current cardiac scans with historical data to track heart function changes over time.
- Procedural Coding: Automatically captures complex codes for interventional procedures like catheterizations.
Therefore, narrowing the gap between the imaging suite and the documentation layer drastically improves diagnostic speed for the enterprise.
3. Mental health EHR systems with therapy tracking
Mental health platforms require a unique balance of high-level privacy and detailed tracking for behavioral outcomes. Unlike surgical fields, these systems focus heavily on qualitative data and long-term counseling progress.
- Outcome Tracking Scales: Integrates standardized tools like PHQ-9 or GAD-7 directly into the session notes.
- Granular Privacy Controls: Restricts sensitive therapy notes while allowing core medical data to flow to primary care.
- Tele-health Integration: Provides a secure, built-in video platform for remote counseling sessions.
In addition, these systems transform behavioral health from a fragmented service into a data-driven clinical pillar for the organization.
4. Orthopedic EHR systems with rehab workflows
Orthopedic surgery is a true success of the enterprise, which depends on tracking the subsequent rehabilitation. These systems bridge the gap between the operating room and the physical therapy clinic.
- Range-of-Motion Mapping: Uses digital tools to record and visualize joint flexibility progress during recovery.
- Surgical Log Integration: Connects specific surgical hardware data with post-operative therapy protocols.
- Device Interoperability: Syncs data from wearable recovery trackers to monitor patient activity levels at home.
By closing the loop between the surgeon and the therapist, the enterprise ensures better long-term outcomes for every patient.
5. Multi-specialty EHR platforms for hospital groups
For large-scale hospital groups, the challenge is maintaining specialty-specific depth while ensuring a unified patient record. Multi-specialty platforms solve this by using a “shared core” with distinct “clinical skins” for different departments.
- Department-Specific UIs: A neurologist and a pediatrician see entirely different, relevant screens while using the same database.
- Unified Revenue Cycle: Consolidates billing and claims data from all specialties into a single executive dashboard.
- Cross-Department Handoffs: Automates the transition of a patient from a specialty consult to a general hospital admission.
Consequently, a well-architected multi-specialty platform becomes the central nervous system of a modern, diversified healthcare enterprise.
Strategic investment in these specialized architectures allows an enterprise to dominate niche markets while maintaining a cohesive operational standard. By selecting the right “clinical skin” for each department, leaders drive both clinician satisfaction and organizational growth.
Compliance Requirements for Specialty EHR Systems
In the enterprise healthcare sector, regulatory adherence is not merely a legal checkbox but the foundation of patient trust and operational continuity.
Building a specialty EHR requires a sophisticated compliance framework that scales across jurisdictions without compromising data accessibility.
1. HIPAA compliance and patient data protection
For any specialty EHR brands operating within the United States, HIPAA remains the gold standard for protecting Protected Health Information (PHI).
Beyond simple encryption, enterprises must ensure that specialty-specific data, such as psychiatric notes or genomic sequences, receives layered protection.
- Encryption at Rest and Transit: Utilizing AES-256 for stored data and TLS 1.3 for data moving between clinics.
- Business Associate Agreements (BAAs): Ensuring every third-party cloud provider or AI vendor integrated into the EHR signs a formal risk-sharing agreement.
- De-identification Protocols: Automating the removal of identifiers for specialty research or population health analytics.
Therefore, HIPAA compliance must be “baked into” the code rather than treated as an afterthought. Consequently, this proactive stance shields the enterprise from devastating data breaches and federal fines.
2. GDPR and regional healthcare data regulations
Global healthcare enterprises must navigate a fragmented landscape of international data laws, with GDPR being the most stringent. Unlike domestic rules, these regulations often grant patients the “right to be forgotten,” which is technically challenging in a complex specialty record.
- Data Residency: Ensuring that patient data stays within specific geographic borders to meet local “sovereignty” laws.
- Consent Management: Building granular interfaces where patients can opt-in or out of specific specialty data-sharing programs.
- Privacy Impact Assessments: Conducting regular technical audits to ensure that new specialty modules don’t leak data across borders.
This ensures that the enterprise can expand its footprint into new markets without rebuilding its entire data architecture.
3. Audit trails and clinical data governance
High-stakes specialties like oncology or surgery require a transparent record of every data interaction to maintain clinical integrity. Data governance ensures that the information within the EHR is accurate, consistent, and used ethically across the organization.
- Immutable Audit Logs: Recording exactly who accessed a record, what they changed, and when they did it, using non-rewritable storage.
- Data Stewardship Roles: Appointing clinical leads to oversee the “truth” of specialty-specific data sets, such as orthopedic implant registries.
- Version Control: Maintaining a history of clinical notes so that the “state of knowledge” at the time of a surgical decision is always retrievable.
Therefore, robust audit trails are a critical defense during malpractice litigation or internal quality reviews. This level of transparency fosters a culture of accountability across all medical teams.
4. Secure data storage and access control systems
Scalable systems must balance “need-to-know” privacy with the “need-to-act” speed required in emergency specialty care. Advanced access control ensures that a billing clerk cannot see a patient’s psychotherapy notes, while a trauma surgeon has instant access to their blood type.
- Multi-Factor Authentication (MFA): Requiring biometric or token-based secondary verification for all enterprise logins.
- Role-Based Access (RBAC): Defining permissions based on job function, ensuring clinicians see only the data relevant to their specialty.
- Just-In-Time Access: Providing temporary, elevated permissions for consulting specialists who are not part of the primary care team.
By implementing these “Zero Trust” principles, the enterprise minimizes the internal threat vector. Consequently, the EHR becomes a secure fortress that protects both the patient’s privacy and the organization’s reputation.
Navigating the complex world of healthcare regulation requires a partner who understands the intersection of law and technology. By prioritizing these compliance pillars, an enterprise ensures that its digital growth is both rapid and legally resilient.
How We Build A Specialty EHR System
Building an enterprise-grade platform is a high-stakes engineering feat that requires a deep understanding of clinical nuances and technical scalability. At Intellivon, we follow a rigorous, battle-tested methodology to transform complex specialty requirements into seamless digital experiences.
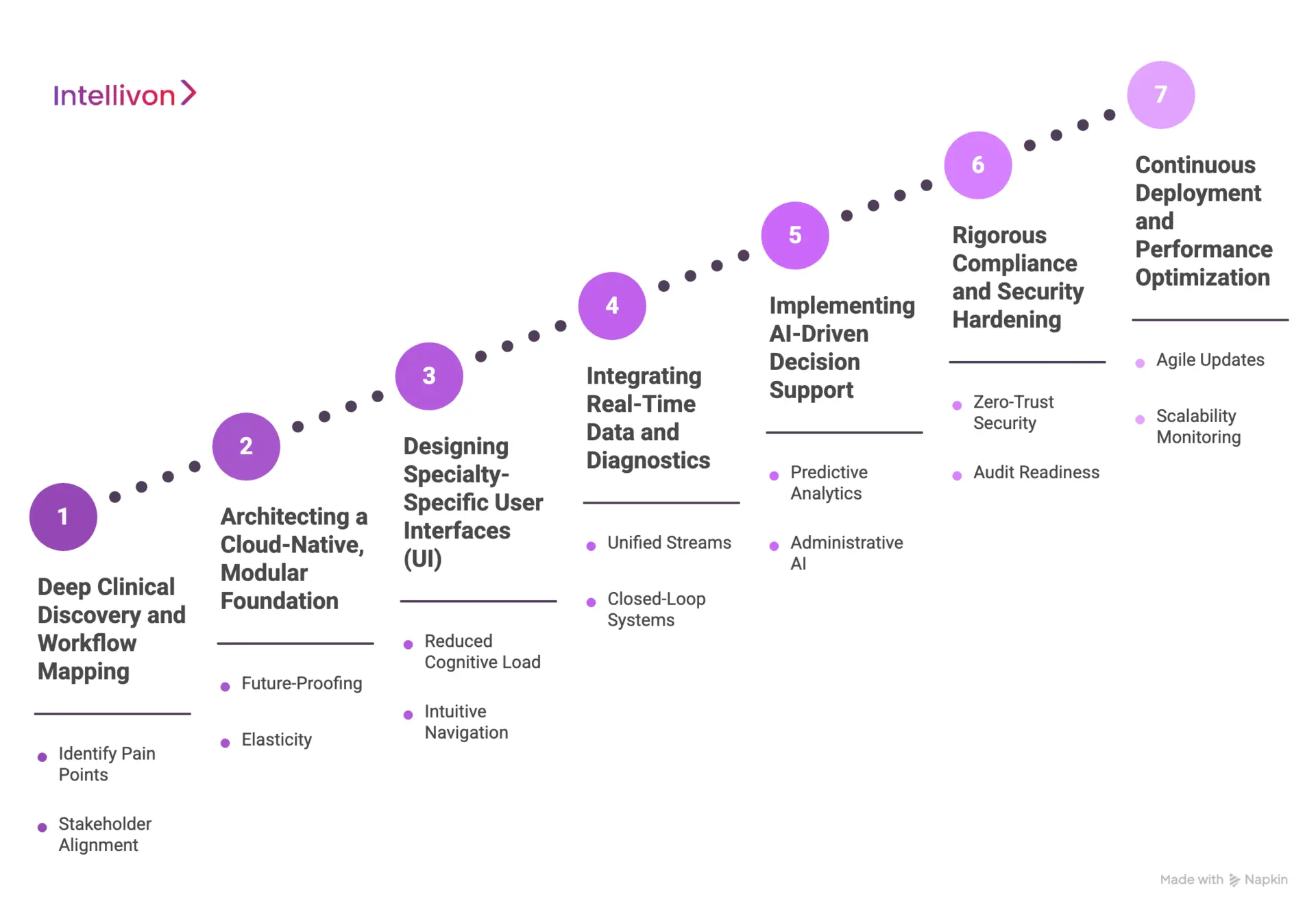
Step 1: Deep Clinical Discovery and Workflow Mapping
The process begins by embedding our strategists within your specialty departments to observe the “day-in-the-life” of your clinicians. We move beyond generic requirements to map the specific decision trees of an oncologist or the rapid-fire data needs of a cardiologist.
- Identify Pain Points: We isolate the manual workarounds currently slowing down your staff.
- Stakeholder Alignment: We ensure that the digital roadmap aligns with both clinical outcomes and executive ROI goals.
Step 2: Architecting a Cloud-Native, Modular Foundation
Once the logic is clear, we design a microservices-based backend that allows your enterprise to scale without friction. This modular approach ensures that your system remains agile, allowing for independent updates to billing, imaging, or patient portal modules.
- Future-Proofing: We prioritize an API-first design to ensure long-term compatibility with emerging medical tech.
- Elasticity: Our infrastructure is built to handle massive data bursts, such as high-resolution imaging uploads, without latency.
Step 3: Designing Specialty-Specific User Interfaces (UI)
We believe that a “one-size-fits-all” screen is the primary cause of documentation fatigue. Our design team builds custom “clinical skins” that surface only the most relevant data for each specialty.
- Reduced Cognitive Load: We eliminate irrelevant fields, allowing doctors to finish charts in record time.
- Intuitive Navigation: We use data visualization tools to make longitudinal patient trends easy to spot at a glance.
Step 4: Integrating Real-Time Data and Diagnostics
A specialty EHR is only as good as the data it pulls in. We build deep integrations with your existing lab systems, imaging suites (PACS/DICOM), and wearable devices.
- Unified Streams: We ensure that diagnostic data flows directly into the patient chart as structured, searchable information.
- Closed-Loop Systems: Our integrations allow for automated follow-up tasks based on real-time lab triggers.
Step 5: Implementing AI-Driven Decision Support
We move the EHR from a passive log to an active clinical partner by embedding AI directly into the workflow. This isn’t just about automation; it’s about providing clinicians with a “second set of eyes.”
- Predictive Analytics: We deploy models that flag early indicators of chronic conditions or acute risks.
- Administrative AI: We automate the prior-authorization and coding processes to slash administrative overhead.
Step 6: Rigorous Compliance and Security Hardening
Before a single line of code goes live, we subject the system to exhaustive security audits and compliance checks. We ensure that your platform meets the highest global standards for data protection.
- Zero-Trust Security: We implement multi-factor authentication and role-based access to protect sensitive PHI.
- Audit Readiness: We build immutable logs that make internal and external audits simple and stress-free.
Step 7: Continuous Deployment and Performance Optimization
Our partnership doesn’t end at launch. We provide ongoing support and performance tuning to ensure the system evolves as your enterprise grows.
- Agile Updates: We push feature enhancements without system downtime.
- Scalability Monitoring: We constantly optimize the database to maintain sub-second response times as your patient volume expands.
Building a specialty platform is a journey toward operational excellence and superior care. With a dedicated partner like Intellivon, your enterprise can move from legacy limitations to a future-ready digital ecosystem.
Common Mistakes in Specialty EHR Development
Even the most well-funded healthcare initiatives can falter if they prioritize generic software standards over clinical reality. Avoiding these structural pitfalls is essential for any enterprise looking to build a sustainable and high-performing digital ecosystem.
1. Ignoring specialty-specific workflow depth
Many developers make the mistake of assuming that “a chart is a chart,” regardless of the medical field. However, ignoring the granular data needs of a neurologist or an oncologist leads to immediate clinician burnout and massive data gaps. If the system doesn’t capture the specific metrics a specialist needs to make a decision, it becomes a digital paperweight.
How we solved it: At Intellivon, we utilize clinical shadowing during the discovery phase. By observing live specialty encounters, we build smart workflows that automate the specific documentation requirements of each niche, ensuring the software speaks the doctor’s language from day one.
2. Choosing rigid architectures early on
Enterprises often fall into the trap of building “monolithic” systems that are difficult to update or scale. A rigid architecture means that a single change in the billing module could potentially crash the entire imaging system. This lack of modularity stifles innovation and forces the organization into expensive, multi-year rewrite cycles.
How we solved it: We implement a microservices-first approach for all specialty EHR brands we develop. This architecture allows us to isolate different clinical functions, meaning we can upgrade your cardiology module or add a new AI tool without ever taking your primary patient database offline.
3. Underestimating compliance complexity
Compliance is often treated as a final “check-box” rather than a core design principle. Underestimating the complexity of HIPAA, GDPR, or specialty-specific data laws can lead to catastrophic security breaches and federal investigations. Many systems fail because they cannot handle the right to be forgotten or granular consent management.
How we solved it: We treat compliance as living code. Our platforms include automated compliance engines that track global regulatory shifts in real-time. We bake zero-trust security and immutable audit trails into the foundation, ensuring your enterprise is always audit-ready without manual intervention.
4. Poor integration planning with legacy systems
A new specialty EHR must coexist with decades of legacy data. Poorly planned integrations lead to “data silos” where the new system cannot communicate with old lab records or pharmacy databases. Consequently, this fragmentation forces staff to double-enter data, which invites human error.
How we solved it: We utilize an “API-Gateway” strategy and FHIR-based data mapping to bridge the gap between old and new. This ensures a seamless flow of information from legacy servers into your modern specialty dashboard, providing a unified “360-degree” view of every patient across the entire enterprise.
Selecting the right development path requires a partner who anticipates these errors before they impact your ROI. By avoiding these common traps, your organization can move from a fragmented past to a streamlined, scalable future.
Future Trends in Specialty EHR Systems
The next decade of healthcare will be defined by systems that anticipate clinical needs rather than just recording them.
For enterprises, staying ahead of these shifts is the only way to maintain a competitive edge in an increasingly data-driven specialty market.
1. AI-driven diagnostics and predictive care
Artificial Intelligence is evolving from a back-office automation tool into a frontline diagnostic partner. In specialties like radiology or pathology, AI algorithms can now flag micro-calcifications or cellular anomalies that the human eye might miss.
Therefore, the EHR of the future acts as a real-time “triage” engine, highlighting high-risk patients for immediate physician review. Consequently, this shift toward predictive care allows hospital groups to intervene earlier, reducing long-term treatment costs.
2. Remote monitoring and IoT integrations
The “hospital at home” model is becoming a reality through the seamless integration of IoT devices. Specialty EHR brands are now building native pipelines for data from wearable cardiac monitors and continuous glucose sensors.
- Ambient Data Streaming: Provides a continuous view of patient health between clinic visits.
- Automated Alerting: Notifies care teams the moment vitals deviate from a personalized baseline.
- Chronic Disease Management: Enhances the precision of long-term treatment plans for complex conditions.
3. Patient-centric data access platforms
Modern patients expect the same digital transparency in healthcare that they receive in banking. Future-ready EHRs are moving toward “open-access” models where patients own and control their specialty data through secure mobile portals.
This goes beyond viewing lab results and includes sharing records with consulting specialists instantly. By empowering patients, enterprises foster deeper trust and improve treatment adherence.
4. Blockchain for healthcare data security
Blockchain technology offers a decentralized approach to record-keeping that eliminates vulnerabilities found in centralized databases. By using a distributed ledger, specialty systems ensure every entry is immutable and transparently audited.
This is particularly valuable for tracking the chain of custody for sensitive genomic data. Therefore, incorporating blockchain adds an extra layer of structural integrity that is nearly impossible for external actors to compromise.
The future of specialty care is intelligent, connected, and secure. Embracing these trends today ensures your enterprise architecture is ready for the clinical demands of tomorrow.
Conclusion
Building a scalable specialty EHR system is not just a technology decision, it is a long-term infrastructure strategy. Enterprises that invest in specialty-driven architecture gain better workflows, faster care delivery, and stronger scalability.
In contrast, generic systems create limitations over time. By focusing on flexibility, interoperability, and performance from day one, healthcare organizations can build systems that grow with them instead of replacing them later.
Build a Specialty EHR System With Intellivon
At Intellivon, specialty EHR systems are built as enterprise healthcare infrastructure, not as extensions of generic platforms. The focus is to design systems that align deeply with specialty-specific clinical workflows while scaling seamlessly across locations, users, and data volumes.
Each platform is engineered to support the full specialty care lifecycle. This includes tailored clinical templates, diagnostic integrations, decision support systems, scheduling, billing, and analytics, all unified within a single data architecture. As a result, healthcare teams operate with precision, reduce manual effort, and deliver faster, more coordinated care.
Our approach combines AI-first, API-driven architecture with interoperability standards like HL7 and FHIR. This ensures seamless integration with labs, imaging systems, pharmacies, and existing healthcare infrastructure without creating fragmented dependencies.
Why Intellivon for Specialty EHR Systems?
- Specialty-Driven Architecture, Not Generic Systems: Design platforms around real clinical workflows for specialties like cardiology, oncology, and more. This ensures accuracy, usability, and better clinical outcomes.
- Unified Data Architecture Across Workflows: Create a single source of truth for patient data across departments and specialties. This improves coordination, reduces errors, and enables real-time decision-making.
- API-First and Scalable Infrastructure: Build systems that scale with patient volumes, specialties, and locations. Expand capabilities without rebuilding core architecture as your organization grows.
- Compliance-Ready by Design: Integrate HIPAA, HL7, and FHIR standards from the start. Ensure secure data exchange, regulatory alignment, and audit readiness across all operations.
- Built for High-Performance Clinical Environments: Engineer platforms to handle complex workflows, large datasets, and multi-site operations without compromising speed, reliability, or system stability.
If you’re planning to build or upgrade a specialty EHR system, Intellivon can help you design a platform that evolves with your clinical and operational growth.
FAQs
Q1. What is a specialty EHR system?
A1. A specialty EHR system is designed for specific medical fields like cardiology, oncology, or dermatology. It includes tailored workflows, templates, and integrations that match specialty care processes. As a result, clinicians work faster, reduce manual errors, and deliver more accurate, context-specific care compared to generic EHR systems.
Q2. How long does EHR development take?
A2. EHR development typically takes 6 to 12 months, depending on complexity, features, and integrations. Basic systems take less time, while enterprise-grade platforms with specialty workflows and compliance layers require longer. Clear requirements and phased development can significantly speed up the process.
Q3. What integrations are required in EHR?
A3. EHR systems require integrations with labs, pharmacies, imaging systems, billing platforms, and insurance providers. In addition, interoperability standards like HL7 and FHIR enable seamless data exchange. These integrations ensure real-time workflows, reduce manual entry, and improve overall system efficiency.
Q4. How secure are specialty EHR systems?
A4. Specialty EHR systems are highly secure when built with compliance in mind. They include encryption, role-based access control, audit logs, and secure APIs. In addition, standards like HIPAA and GDPR ensure patient data protection, secure storage, and controlled data sharing across systems.
Q5. How much does it cost to build an EHR?
A5. The cost to build an EHR system typically ranges from $50,000 to $150,000+, depending on features, specialty requirements, and integrations. More complex, enterprise-grade systems with scalability and compliance layers can increase costs. However, custom solutions reduce long-term inefficiencies and scaling limitations.