Every large hospital network has a fully functioning EHR system that is loaded with patient data. However, the moment a patient moves between facilities, crosses a border, or starts generating health signals through a wearable, the existing EHR systems in place start failing to coordinate these numbers. Because of this anomaly, clinical decisions are made with incomplete information because the existing systems were never designed to work together.
This is precisely where serious builders and investors are currently directing their attention. They are not focusing on creating another EHR platform, but are interested in the integration layer that allows everything currently in place to function as a unified system across hospital networks, jurisdictions, and the growing network of connected devices providing real-time signals to clinical settings. Get that layer right, and you create something with lasting value in one of the most complex industries in the world.
Intellivon operates at this specific layer of healthcare infrastructure, and that experience will guide everything we cover in this blog. It will cover architecture decisions, interoperability standards, compliance across borders, scalability under real enterprise demands, and how we build such solutions from the ground up.
Why EHR Integration Fails at Enterprise Scale
EHR integration at enterprise scale often fails due to weak governance, mismatched standards, and overlooked organizational gaps. This happens even as healthcare pushes for FHIR adoption and stricter compliance.
Despite strong market growth in interoperability solutions, execution still lags. High failure rates reveal a clear gap between technical potential and real-world implementation.
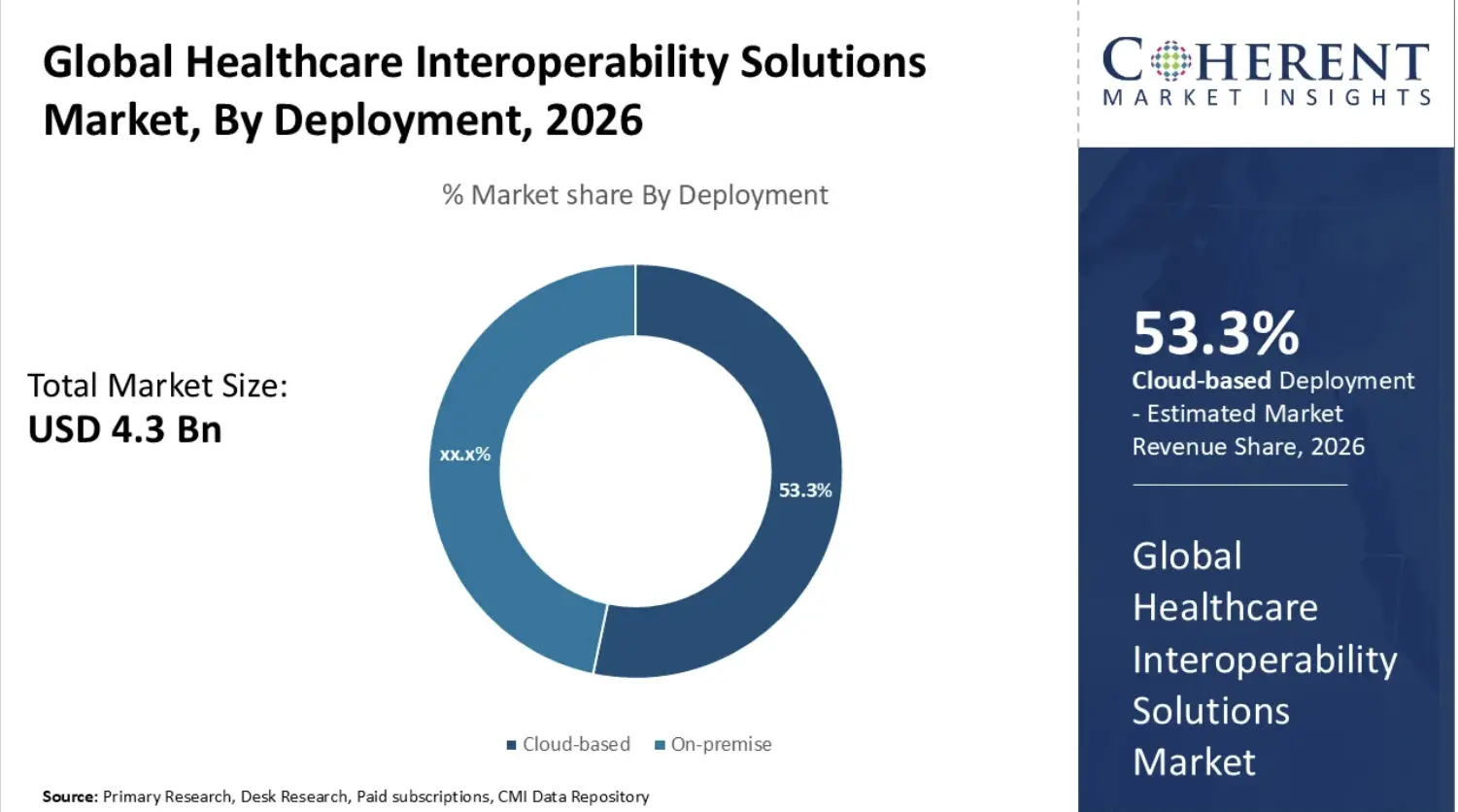
However, enterprise-scale failures still persist. This highlights the need for stronger middleware and better governance across systems.
1. Fragmented systems across hospitals and departments
Large healthcare networks often grow through acquisitions. This results in a patchwork of disparate software versions and vendors. Communication breaks down when one department uses a specialized oncology module while the main hospital operates on a different legacy platform.
This fragmentation forces clinicians to toggle between screens, which increases cognitive load and slows down patient care. Successful EHR integration solutions must unify these fragments into a single, cohesive interface.
2. Data silos blocking real-time clinical decisions
Information trapped in isolated silos prevents a holistic view of the patient journey. When lab results, imaging, and pharmacy records do not sync instantly, doctors make decisions based on incomplete data.
This lag time creates bottlenecks in emergency departments where every second matters. Breaking these silos is essential for implementing predictive analytics and AI-driven triage tools that rely on a continuous stream of live data.
3. Legacy infrastructure vs modern API expectations
Modern healthcare demands FHIR-based APIs and cloud-native agility. However, many large systems still rely on on-premise servers and outdated messaging protocols.
These legacy frameworks cannot handle the high-velocity data exchange required by mobile health apps or remote monitoring devices. Bridging the gap between old hardware and modern software requirements remains a primary technical hurdle for most IT departments.
4. Compliance risks in multi-system environments
Moving sensitive data across multiple platforms increases the attack surface for cyber threats. Each integration point must strictly adhere to HIPAA and SOC2 standards to avoid massive fines. Inconsistent security protocols across different vendors can lead to inadvertent data leaks.
Maintaining a unified compliance posture requires rigorous encryption and automated auditing at every stage of the data transfer process.
Addressing these foundational failures is the first step toward building a resilient, future-ready healthcare ecosystem.
What Is EHR Integration in the Enterprise Context?
In the enterprise context, EHR integration is the strategic unification of patient data across vast, multi-site networks. It moves beyond simple data sharing to create a single source of truth. This allows disparate systems, from radiology to billing, to communicate in real-time.
By leveraging FHIR and HL7 standards, large health systems ensure that clinicians have immediate access to complete, actionable patient histories at every point of care.
Beyond APIs: System-wide data orchestration
System-wide data orchestration moves past simple point-to-point connections. It creates a coordinated layer that manages how information flows across an entire hospital network. While an API provides the pathway, orchestration provides the intelligence.
It ensures that data reaches the right person exactly when they need it to make a critical decision.
This approach transforms passive data into active clinical triggers:
- Automated Workflow Triggers: An abnormal lab result can instantly alert a specialist, update the patient’s mobile app, and flag the billing department.
- Reduced Clinician Burnout: Intelligent orchestration filters out irrelevant data. This prevents alert fatigue and allows doctors to focus on patient care.
- Unified Operational Visibility: Leadership gains a real-time view of bed availability, staffing levels, and resource allocation across multiple facilities.
Effective orchestration acts as the central nervous system of a large health system. It eliminates manual data entry and ensures that every department operates from the same set of facts. This level of synchronization is what separates a modern digital hospital from a collection of disconnected clinics.
Role of interoperability standards (HL7, FHIR)
Interoperability standards like HL7 and FHIR are the universal languages of healthcare. They allow different software systems to understand each other without custom, expensive coding for every new connection.
For an enterprise, these standards are not just technical requirements; they are strategic assets that protect long-term investments.
These standards offer several distinct advantages for scaling health platforms:
- FHIR (Fast Healthcare Interoperability Resources): This modern, internet-based standard allows mobile apps and cloud services to access EHR data securely. It makes the system modular and ready for future AI integrations.
- Legacy Support (HL7 v2): Most existing hospital systems still rely on older HL7 protocols. Maintaining compatibility ensures that new solutions can still communicate with older, reliable infrastructure.
- Rapid Deployment: Using standardized frameworks reduces the time required to onboard new clinics or integrate third-party diagnostic tools.
By prioritizing these standards, organizations avoid “vendor lock-in.” They build an open ecosystem that can adapt as medical technology evolves. This flexibility is essential for maintaining a competitive edge in a rapidly changing healthcare market.
Types of EHR Integrations Enterprises Build
Building a connected health system is about making sure different tools talk to each other without errors. Leaders must choose integration paths that simplify daily operations and improve the way clinicians work across multiple locations.
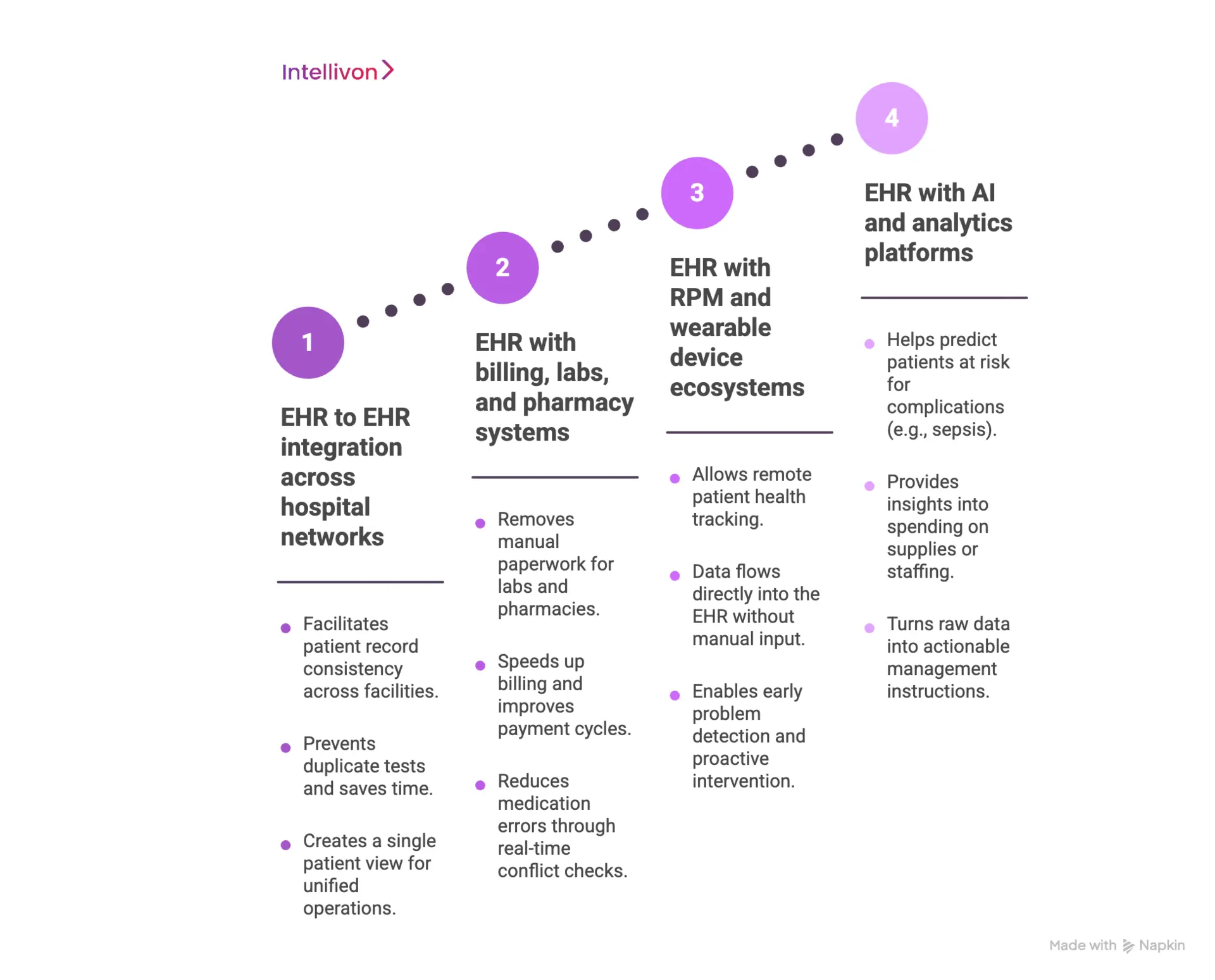
1. EHR to EHR integration across hospital networks
When hospitals merge, they often end up with different software systems that do not communicate. These integrations link platforms like Epic and Cerner, so a patient’s record stays consistent no matter which facility they visit.
This setup stops doctors from ordering the same test twice and saves significant time. By creating a single view of the patient, the entire network operates as one unified organization rather than a group of disconnected offices.
2. EHR with billing, labs, and pharmacy systems
Connecting clinical data to the back office is essential for a healthy bottom line. When the EHR sends data directly to labs and pharmacies, it removes the need for manual paperwork. This automation speeds up the billing process and helps the hospital get paid faster.
It also reduces the chance of dangerous medication errors because the system checks for conflicts in real-time before a prescription is even filled.
3. EHR with RPM and wearable device ecosystems
Remote Patient Monitoring (RPM) lets doctors track patient health from a distance using devices like smartwatches or blood pressure cuffs. Integration flows this data directly into the hospital’s main system without the patient needing to call in their numbers.
This allows the care team to spot a problem early and intervene before it leads to an expensive emergency room visit. It turns the hospital from a reactive service into a proactive health partner.
4. EHR with AI and analytics platforms
AI works best when it has a constant stream of clean data from the EHR. These integrations help the system predict which patients might be at risk for complications like sepsis or heart failure.
Beyond clinical care, analytics tools help leaders see exactly where they are overspending on supplies or staffing. This makes the hospital more efficient by turning raw data into clear instructions for better management.
Choosing the right integration depends on whether you want to focus on saving costs, improving care, or growing your medical network.
What Must Be Designed Before Any Integration Starts
Careful planning is the only way to avoid expensive rework later in the project. Leaders must ensure that the technical blueprint aligns with the operational reality of each department before a single line of code is written.
1. Mapping system dependencies across departments
Every department in a hospital relies on data in a slightly different way. For example, a change in the pharmacy system can unexpectedly break the billing workflow if the dependencies are not mapped out first. Leaders need to see exactly how data moves from the emergency room to the lab and eventually to the insurance provider.
Identifying these “hand-off” points early prevents service outages during the integration process. This map acts as a guide for the technical team to ensure no critical service is left behind.
2. Defining a unified patient data structure
Data often looks different depending on which software generated it. One system might record a birthdate as MM/DD/YYYY, while another uses YYYY-MM-DD. Without a unified structure, the integrated system will struggle to match records correctly.
Establishing a common data language ensures that a patient’s identity remains consistent across every touchpoint. This step is vital for maintaining clean records and avoiding the dangerous issue of duplicate patient files.
3. Choosing real-time vs asynchronous data flow
Not every piece of information needs to move at the same speed. Vital signs in an ICU require real-time synchronization to save lives. However, monthly financial reports can be processed asynchronously, or in “batches,” to save on system resources.
Deciding which data needs instant delivery helps manage the load on the hospital’s network. This strategic choice balances the need for speed with the reality of technical costs and server performance.
4. Establishing governance and data ownership
Clear rules must define who “owns” the data and who has the right to change it. When multiple systems are linked, it is easy to lose track of which record is the authoritative source. Governance policies set the standards for data quality, security access, and long-term storage.
By deciding these rules early, leadership avoids internal conflicts between IT and clinical staff. Strong governance ensures the integrated platform remains a trusted source of truth for the entire organization.
Setting these ground rules early creates a predictable environment for both the developers and the medical staff.
Core Architecture Behind Scalable EHR Integration
The technical foundation of a healthcare platform determines how well it can grow. A rigid architecture will eventually break under the pressure of new hospital sites or increased patient data. Leaders must invest in a structure that remains flexible as the organization expands.
1. API-first communication across systems
An API-first strategy ensures that every part of the hospital’s digital ecosystem can talk to every other part. Instead of building custom, one-off connections for every new tool, developers create a standardized interface.
This approach allows the IT team to plug in a new pharmacy module or a third-party billing app without rewriting the core EHR code. It drastically reduces the time needed to launch new services and keeps the entire system modular and agile.
2. Middleware for decoupling legacy dependencies
Most large health systems still rely on older “legacy” software that was never meant for the cloud. Middleware acts as a translator between these old servers and modern web applications.
By placing a layer between the two, you “decouple” the systems. This means you can upgrade your patient portal without crashing the underlying database from the 1990s. Middleware provides the stability needed to modernize a hospital’s tech stack at a manageable pace.
3. Event-driven pipelines for real-time updates
In a high-stakes medical environment, data cannot wait for a scheduled “sync” at the end of the day. Event-driven architecture ensures that as soon as a doctor signs a discharge paper, the billing, pharmacy, and transport teams are notified instantly.
The system reacts to specific “events” as they happen. This automation eliminates the lag time that often frustrates clinical staff and ensures that the patient’s digital record is always an accurate reflection of their physical status.
4. Microservices for independent system scaling
Large, “monolithic” software programs are difficult to update because a tiny error in one area can bring down the entire hospital network. Microservices break the platform into smaller, independent pieces, like one service for scheduling and another for lab results.
If the scheduling service experiences a surge in traffic, it can scale up its server power independently without affecting the rest of the system. This granular control keeps the platform fast and reliable even during peak hours.
Building with these modern patterns ensures that the technology remains an asset rather than a bottleneck for the business.
The Integration Layer Most Health Systems Miss
A critical layer often goes missing between the user interface and the database. Many leaders focus only on the connection itself, neglecting the engine that processes the data as it moves. Neglecting this layer leads to fragmented information that clinicians cannot trust.
1. Data transformation and normalization pipelines
Data arrives from different sources in various formats and languages. One clinic might code a procedure differently from the main hospital across town. Transformation pipelines act as a digital translator that converts all incoming data into a single, standardized format.
This process, called normalization, ensures that every system in the network speaks the same language. Without this, your analytics tools will produce inaccurate reports because they are comparing apples to oranges.
2. Patient identity resolution across systems
A single patient might have records in five different systems under slightly different names or addresses. If these records are not linked, a doctor might miss a life-saving piece of medical history. Identity resolution uses smart matching logic to confirm proper patient names.
This layer prevents the creation of dangerous duplicate charts and ensures a complete, longitudinal view of every patient. It is the most vital safety feature of any integrated health platform.
3. Workflow orchestration across departments
Moving data is easy, but managing a clinical workflow is complex. Orchestration is the logic that dictates what happens after a piece of data is received. For example, when a surgeon orders a post-op scan, the system must automatically notify the imaging department, update the bed manager, and alert the billing office.
This layer coordinates these multi-step processes across different departments without human intervention. It turns a passive database into an active assistant for the entire medical staff.
4. Monitoring, logging, and failure recovery
In a large health system, a single broken connection can stall an entire department. A robust integration layer must include “self-healing” features that detect a failure the moment it happens. Detailed logging allows IT teams to see exactly where a message got stuck and why.
Automated recovery protocols can then resubmit the data once the connection is restored. This transparency ensures that no patient record is ever lost in transit due to a temporary server glitch.
Investing in this hidden layer is what transforms a basic data link into a high-performance enterprise solution.

Integrating With Epic, Cerner, and Legacy Systems
Interacting with the “big two” requires a specialized strategy that balances their rigid structures with your need for innovation. Most enterprises find that a direct modification of these core systems is too risky and expensive. Instead, successful teams build around them, using their strengths while bypassing their limitations.
1. Extending Epic without touching core systems
Epic is the dominant force in the market, but its core is notoriously difficult to change. Smart developers use the “Epic App Orchard” and specialized web services to build custom tools that sit on top of the main platform.
This allows a health system to add a unique patient portal or an AI diagnostic tool without altering the underlying Epic code. It keeps your custom features separate, which makes future Epic version updates much smoother and less likely to break your integrations.
2. Working within Cerner’s ecosystem constraints
Cerner (now Oracle Health) offers a different set of challenges, often requiring a deep understanding of its Millennium architecture. Integration here usually involves working within the “Cerner Ignite” APIs to ensure data flows reliably between the EHR and outside apps.
Because Cerner can be more restrictive with third-party access, developers must focus on highly efficient, standardized data calls. This approach ensures that your custom solution doesn’t slow down the main EHR interface for doctors during a busy shift.
3. Connecting legacy systems through API layers
Many older hospital systems were built before modern “cloud-native” standards existed. To bring these systems into the modern era, we wrap them in a modern API layer. This layer acts as a facade that translates old data formats into clean, JSON-based information that new apps can understand.
It allows a 20-year-old billing system to talk to a brand-new mobile app as if they were built in the same decade. This strategy saves millions by extending the life of existing hardware.
4. Managing closed systems and vendor limitations
Some niche software vendors make it intentionally difficult to export data to protect their market share. Overcoming these closed systems requires creative engineering, such as using Robotic Process Automation (RPA) or secure file transfers when APIs are unavailable.
Leaders must navigate these vendor limitations by insisting on data-sharing clauses in new contracts. In the meantime, building bridge technologies ensures that no department remains a data island, even if their software provider is uncooperative.
By mastering these specific vendor environments, an organization can finally achieve the single pane of glass view that clinicians need.
Key Components of an EHR Integration Layer
A robust integration layer acts as the specialized engine room of a hospital’s digital strategy. It ensures that data from a thousand different sources is cleaned, secured, and delivered to the right screen in milliseconds.
1. Data ingestion and transformation pipelines
Data enters a health system in massive volumes and inconsistent formats. Ingestion pipelines act as the front door, collecting information from labs, imaging centers, and bedside monitors. Once inside, transformation logic reworks this raw data into a usable structure that matches the primary EHR.
This step is vital because it removes “noise” and ensures that clinicians see only high-quality, relevant information. Without these pipelines, the system becomes a digital junkyard of unreadable files.
2. Interoperability engine (FHIR, HL7 adapters)
The interoperability engine is the central translator for the entire enterprise. It uses specific “adapters” to speak both the old language of HL7 and the modern, web-based language of FHIR. This engine allows a 15-year-old on-premise server to communicate perfectly with a brand-new cloud-based AI tool.
By managing these protocols in one place, the IT team can add or remove apps without breaking the whole network. This modularity is what makes a health system truly “future-proof.”
3. Identity and patient matching systems
Matching the right data to the right person is the most critical safety task in healthcare. Identity systems use complex algorithms to compare names, birthdays, and social security numbers across different databases.
If a patient visits a satellite clinic under a nickname, the matching system identifies them and links the visit to their main hospital record. This prevents “ghost” files and ensures that a doctor has the full medical history before prescribing a new medication.
4. Security and compliance enforcement layers
In a world of constant cyber threats, every data transfer must be shielded by an invisible security layer. This component handles end-to-end encryption and ensures that only authorized staff can view sensitive patient files.
It also maintains a detailed “audit log” that tracks who accessed what data and when. For leadership, this layer is the primary defense against HIPAA violations and expensive data breaches. It builds the trust necessary to operate a large-scale digital health platform.
When these components work in harmony, the technology fades into the background, allowing doctors to focus entirely on the patient.
Step-by-Step EHR Integration Development Process
At Intellivon, we treat EHR integration as a strategic engineering challenge rather than a simple software installation. Our approach ensures that data flows securely without disrupting life-critical clinical operations.
This seven-step methodology defines how we move from initial discovery to a fully optimized enterprise solution.
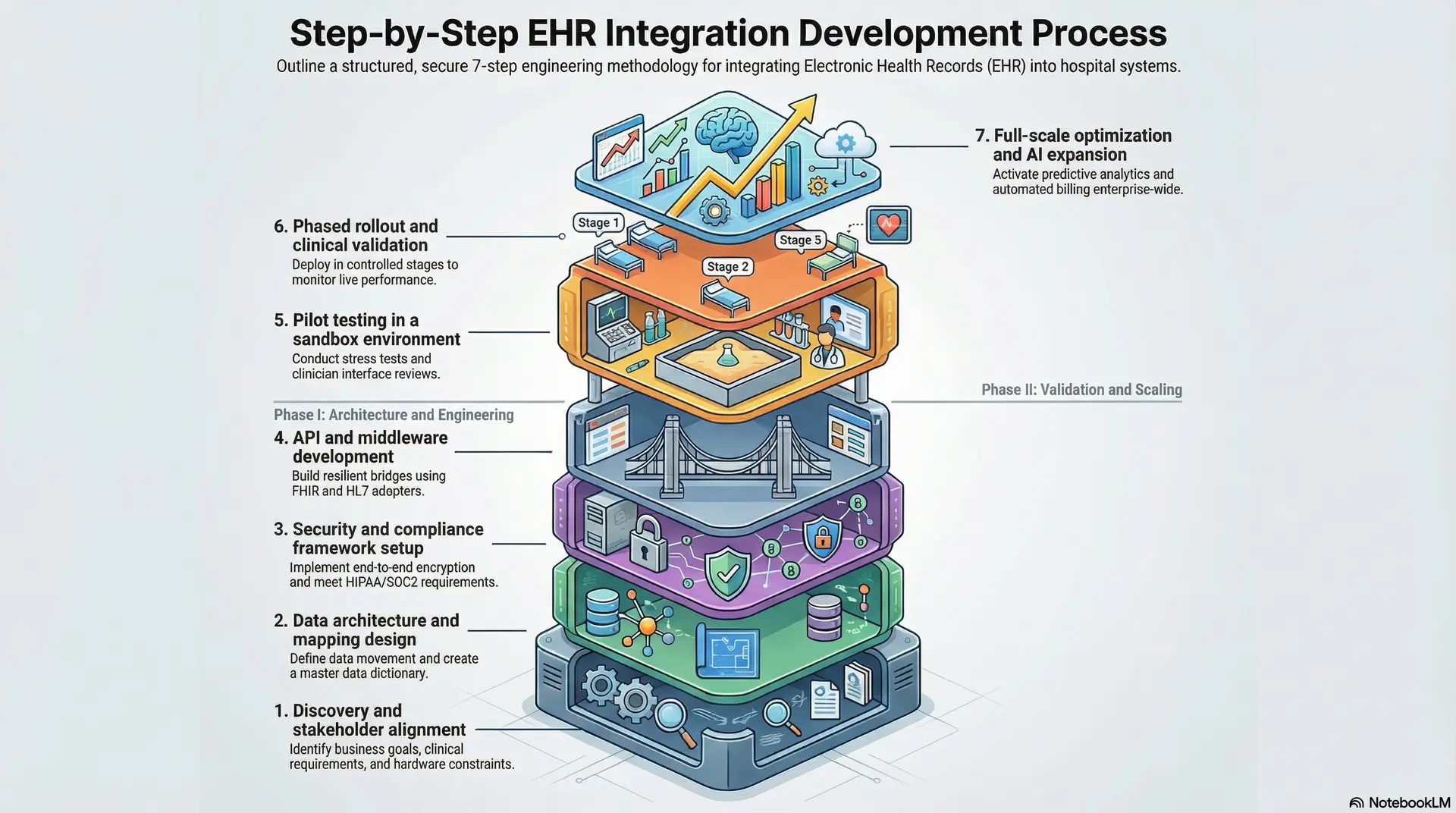
1. Discovery and stakeholder alignment
Our process begins by identifying your specific business goals and clinical requirements. We work with your leadership to prioritize the workflows that will benefit most from automation.
During this phase, our team maps out every existing software version and hardware constraint across your hospital network. This deep dive ensures our solution solves real-world bottlenecks rather than adding digital complexity.
2. Data architecture and mapping design
Once goals are clear, we define exactly how data moves between your disparate systems. At the same time, we create a master “data dictionary” to standardize terminology across every department in the enterprise.
Our mapping ensures a “blood pressure” reading in a remote clinic perfectly matches the format in your main hospital EHR. This foundational step prevents the data corruption that often leads to clinical errors.
3. Security and compliance framework setup
We establish a rigorous security perimeter before a single line of code is written. Our engineers implement end-to-end encryption and multi-factor authentication for every data access point.
We ensure the entire architecture meets strict HIPAA and SOC2 requirements for patient privacy. By building security into the DNA of the integration layer, we protect your organization from future cyber threats.
4. API and middleware development
This is the core engineering phase where we build the “translation” layer for your systems. We utilize FHIR and HL7 adapters to create a resilient bridge between legacy servers and modern applications.
By using a middleware approach, we build new features without risking the stability of your core EHR. This decoupled architecture allows for faster updates and easier maintenance as your health system grows.
5. Pilot testing in a sandbox environment
We never move an integration into production without extensive testing in a mirrored, non-clinical environment. Our team runs “stress tests” to see how the system handles high volumes of data during peak hospital hours.
We invite your clinicians to test the interface to ensure it fits naturally into their daily routines. This “sandbox” phase identifies friction points before they can ever impact patient care.
6. Phased rollout and clinical validation
We avoid the risks of a “big bang” launch by rolling out the integration in controlled phases. At the same time, we typically start with a single department or outpatient clinic to monitor performance in a live setting.
This allows us to make real-time adjustments based on actual usage patterns. We measure success by how accurately data moves and the measurable time saved for your medical staff.
7. Full-scale optimization and AI expansion
Once the foundation is stable, we scale the system across your entire enterprise. This is the stage where we activate advanced features like AI-driven predictive analytics and automated billing.
Intellivon stays embedded with your leadership to refine these data pipelines for maximum efficiency. We ensure your platform is not just functional, but a strategic asset driving long-term institutional growth.
Following this disciplined path ensures your investment results in a reliable, high-performance system that your clinicians and patients can trust.
Cost to Build EHR Integration Systems in 2026
At Intellivon, EHR integration systems are built as an enterprise healthcare infrastructure, not as connectors layered onto fragmented systems. The objective is to create a unified integration layer that enables real-time data exchange across clinical, operational, and financial systems.
However, building a reliable EHR integration system requires more than connecting APIs. It involves designing scalable data pipelines, ensuring interoperability across systems, and embedding compliance into the architecture. As a result, healthcare organizations gain real-time visibility, reduce operational inefficiencies, and enable coordinated care across departments.
Estimated Phase-Wise Cost Breakdown
| Phase | Description | Estimated Cost Range (USD) |
| Discovery & System Mapping | Define integration scope, workflows, and system dependencies | $8,000 – $15,000 |
| Architecture & Data Design | Design data models, FHIR/HL7 layers, and infrastructure | $10,000 – $20,000 |
| Integration Layer Development | Build APIs, middleware, and orchestration pipelines | $10,000 – $25,000 |
| EHR & System Integration | Integrate with Epic, Cerner, labs, billing, and legacy systems | $8,000 – $20,000 |
| Data Transformation & Sync | Enable real-time or batch data processing and normalization | $5,000 – $15,000 |
| Compliance, Security & Testing | Implement HIPAA compliance, encryption, and validation | $5,000 – $12,000 |
| Deployment & Scaling Setup | Cloud deployment, monitoring, and performance optimization | $4,000 – $10,000 |
Estimated Total Cost
For most healthcare organizations, the cost to build an EHR integration system typically ranges between:
$50,000 – $150,000
Key Factors That Influence Cost
- Number of systems being integrated (EHR, labs, billing, etc.)
- Complexity of EHR platforms (Epic, Cerner, legacy systems)
- Real-time vs batch data processing requirements
- Level of workflow automation across departments
- Compliance and security requirements
- Scalability across hospitals, providers, and locations
Get a Precise Cost Breakdown
Every EHR integration system is different. The final cost depends on your system landscape, data complexity, and scale. Talk to Intellivon’s experts to get a tailored cost estimate for your integration system.
Security and Compliance in EHR Integrations
Security is the most critical pillar of any healthcare platform. A single data breach can lead to massive financial penalties and a total loss of patient trust.
For a large enterprise, compliance is not a one-time checkmark but a continuous operational requirement that must be built into the core of the integration.
1. HIPAA, GDPR, and regional compliance layers
Large health systems often operate across state or national borders, requiring a multi-layered approach to privacy laws. While HIPAA sets the standard in the US, global organizations must also account for the strict “right to be forgotten” rules within GDPR.
We build automated compliance layers that tag and handle data differently based on its geographic origin. This ensures that your platform remains legally compliant regardless of where the patient is treated or where the data is stored.
2. Data encryption and access control systems
Protecting patient records requires more than just a password. We implement end-to-end encryption for data both at rest and in transit between systems. Access control systems utilize “least privilege” logic, meaning a billing clerk only sees financial data while a doctor sees clinical records.
By using multi-factor authentication and biometric locks, we ensure that sensitive information is only accessible to verified personnel on authorized devices.
3. Audit trails and governance frameworks
Transparency is the best defense against internal and external security threats. A robust audit trail records every single interaction with a patient’s file, like who viewed it, what they changed, and when it happened.
These logs are stored in a tamper-proof environment to ensure they remain a reliable source of truth for federal auditors. Strong governance frameworks define these rules clearly, so every department understands its responsibility in maintaining the integrity of the health system’s data.
4. Managing third-party data risks
Integrating with outside labs, wearable devices, or AI vendors introduces new points of vulnerability. We treat every third-party connection as a potential risk that must be isolated and monitored.
Our integration layer includes “sandboxing” features that prevent a breach in a third-party app from spreading to your core EHR. We also conduct rigorous security assessments of every vendor to ensure their standards match your enterprise-level requirements.
By prioritizing these security measures, you turn a potential liability into a foundation of trust for your patients and staff.
Real Enterprise Use Cases of EHR Integration
Integrating theoretical solutions into high-stakes medical environments requires proof of impact. Many of the world’s leading health systems have already moved past basic connectivity to achieve true digital maturity.
These real-world examples demonstrate how strategic integration delivers measurable returns on investment and superior patient care.
1. Multi-hospital patient data synchronization
Large-scale mergers often leave health systems with a fragmented digital landscape. Organizations like Mayo Clinic have successfully unified patient records across multiple states using sophisticated data synchronization layers.
By ensuring that a patient’s history is available at any clinic within their network, they eliminated redundant testing and improved diagnostic accuracy. This level of synchronization allows a specialist in one city to review live data from a primary care visit in another, ensuring a seamless care experience.
2. Automated insurance and billing workflows
Manual billing is a primary cause of revenue leakage in large enterprises. Cleveland Clinic has utilized deep EHR integration to automate the prior authorization and claims submission process. By connecting their clinical data directly to payer portals, they reduced the time spent on administrative paperwork by thousands of hours annually.
This automation speeds up the “record-to-revenue” cycle and ensures that the financial health of the organization remains as stable as its clinical outcomes.
3. Remote patient monitoring integration
Extending care beyond the hospital walls is a top priority for modern health leaders. Kaiser Permanente has integrated vast streams of data from remote monitoring devices directly into its central EHR. This allows their care teams to track chronic conditions like hypertension or diabetes in real-time without requiring an office visit.
When a device flags an abnormal reading, the system automatically alerts the physician, allowing for immediate intervention that often prevents an expensive emergency room admission.
4. AI-driven clinical decision support systems
AI is most effective when it sits directly inside the clinician’s workflow. HCA Healthcare has integrated advanced predictive analytics into its EHR to help identify early signs of sepsis.
Their system, known as SPOT (Sepsis Prediction and Optimization of Therapy), monitors patient vitals and lab results 24/7 to alert nurses before a crisis occurs. This integration of AI-driven support has saved thousands of lives by turning passive data into proactive, life-saving medical alerts.
These examples show that when technology is correctly integrated, it becomes a powerful engine for both clinical excellence and financial growth.
Conclusion
EHR integration at scale is not just about connecting systems. It is about building a reliable data foundation that supports care, operations, and growth. When done right, it reduces complexity, improves decision-making, and prepares systems for future expansion.
However, success depends on strong architecture and execution. Health systems that invest in the right approach move faster, operate better, and stay ready for what comes next.
Build EHR Integration Platform With Intellivon
At Intellivon, EHR integration platforms are built as enterprise healthcare infrastructure, not as connectors layered onto fragmented systems. The objective is to create a unified integration layer that enables real-time data flow across clinical, operational, and financial systems.
Each platform is designed to support end-to-end data exchange across the healthcare ecosystem. This includes EHR integration, lab and pharmacy connectivity, billing system synchronization, workflow orchestration, and real-time data processing. As a result, healthcare organizations gain a single, consistent view of data while reducing manual dependencies and operational delays.
Our engineering approach focuses on API-first, cloud-native architectures combined with interoperability standards like HL7 and FHIR. This ensures seamless integration with EHR systems, legacy platforms, third-party tools, and emerging healthcare technologies without disrupting existing operations.
Why Intellivon for EHR Integration Development
- Built as infrastructure, not integrations: Platforms are designed to unify systems and workflows, not just connect endpoints.
- Interoperability-first architecture: Seamless data exchange across EHRs, labs, billing systems, and external platforms.
- Real-time data orchestration: Enable faster clinical and operational decisions with continuous data flow.
- Scalable and compliant by design: Architectures support multi-hospital systems while meeting strict regulatory requirements.
Whether you are integrating systems across hospitals or building a centralized data layer, Intellivon helps you design, build, and scale with confidence.
Talk to Intellivon’s healthcare experts to get a tailored roadmap and cost estimate for your EHR integration platform.
FAQs
Q1. What is EHR integration in healthcare systems?
A1. EHR integration connects electronic health records with other clinical, operational, and financial systems. This includes labs, pharmacies, billing platforms, and third-party tools. The goal is to enable seamless data exchange across systems. As a result, providers get a unified view of patient information and reduce manual data entry across workflows.
Q2. How long does EHR integration take to build?
A2. EHR integration timelines depend on system complexity and scale. For most healthcare organizations, projects typically take 3 to 6 months. Smaller integrations may take less time. However, multi-hospital or enterprise setups can take longer due to data mapping, compliance, and testing requirements.
Q3. What systems can integrate with EHR platforms?
A3. EHR platforms can integrate with a wide range of healthcare systems. This includes labs, pharmacies, billing systems, insurance platforms, and remote monitoring devices. They can also connect with analytics tools, AI systems, and legacy hospital software. As a result, organizations create a connected healthcare ecosystem instead of isolated systems.
Q4. How secure are EHR integration solutions?
A4. EHR integration solutions are designed with strong security and compliance measures. This includes data encryption, role-based access control, and audit logging. In addition, systems are built to meet regulations like HIPAA and GDPR. When implemented correctly, they ensure secure data exchange across all connected platforms.
Q5. How much does EHR integration cost?
A5. The cost of EHR integration typically ranges between $50,000 and $150,000 for most healthcare organizations. However, the final cost depends on the number of systems, data complexity, and compliance requirements. Larger, multi-system integrations may require higher investment due to scale and customization.