Missed appointments, delayed follow-ups, and low patient engagement often stem from gaps in communication rather than a lack of intent. To manage high patient volumes and complex touchpoints, providers are adopting EHR reminder tools that automate outreach, ensuring timely notifications that improve patient adherence and support consistent care beyond the clinic.
The effectiveness of a patient engagement system depends on how well appointment reminders, medication notifications, follow-up messages, and personalized communication align with clinical workflows. These interactions must be deeply integrated with EHR data to ensure that every touchpoint maintains the highest standards of accuracy, privacy, and compliance.
In this blog, we explain how to build an EHR reminder and patient engagement system by examining core features, system architecture, and practical considerations involved in delivering reliable and patient-centric communication within healthcare environments.
Why EHR Reminder Systems Are Now Critical in Care?
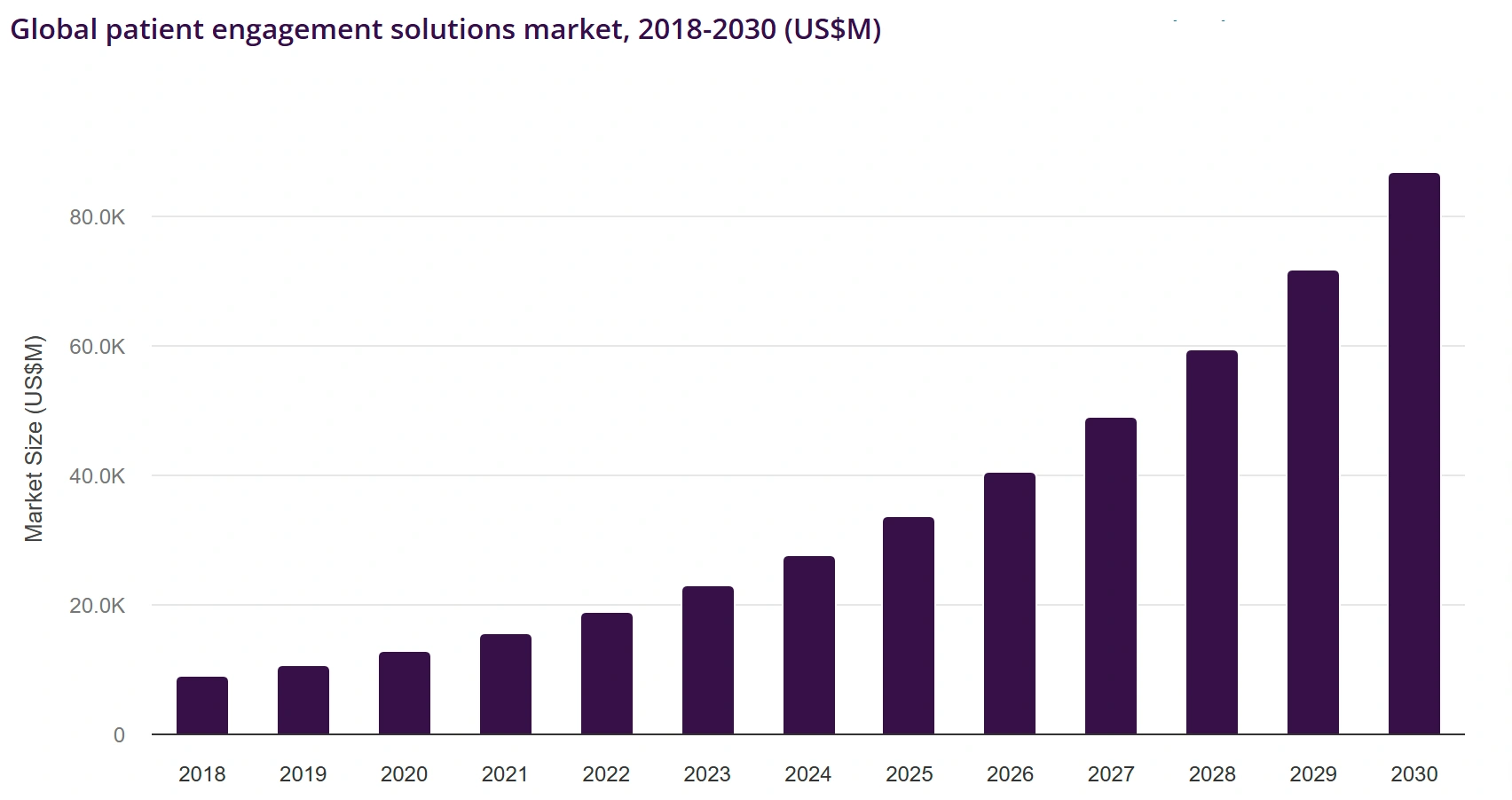
Modern healthcare is shifting toward proactive engagement, fueling the market from USD 27.6 billion in 2024 to reach USD 86.7 billion by 2030 at a 21% CAGR, reflecting a global transition toward continuous, data-driven patient interaction.
While EHRs serve as essential repositories, they often lack real-time engagement capabilities. An integrated layer transforms these static databases into active communication engines, optimizing clinical outcomes and protecting organizational revenue.
High-quality post-discharge engagement has been shown to reduce hospital readmissions by 25% to 33% by addressing gaps in care coordination and medication understanding.
Non-adherence to chronic disease medications (like those for hypertension or diabetes) increases hospitalization and mortality risks by roughly 33% to 38%. Engaged patients are significantly more likely to adhere to these life-saving regimens.
Digital tools can save over 25 staff hours per month by automating reminders and administrative tasks, often delivering an ROI of 6:1 to 15:1 within three years.
A. Rising no-show costs and care gaps in healthcare
The financial and clinical consequences of missed appointments create a dual crisis for healthcare providers. When a patient fails to appear for a scheduled slot, the immediate result is a loss of billable time and underutilized staff. Over time, these gaps lead to significant revenue leakage and fragmented care.
Impact of No-Shows and Care Disruption:
- Revenue Loss: Every missed appointment represents a direct hit to the bottom line, with cumulative annual losses often reaching millions for larger health systems.
- Wasted Resources: Clinical staff and specialized equipment remain idle, yet the overhead costs for the facility remain constant.
- Clinical Risks: Patients who miss follow-up appointments for chronic conditions are at a much higher risk for acute complications and emergency room visits.
- Resource Allocation: Frequent no-shows make it difficult for administrators to accurately predict staffing needs and manage patient flow effectively.
B. Shift toward value-based and patient-centric care
The industry is moving away from fee-for-service models and toward value-based care, where reimbursement is tied directly to patient outcomes. In this environment, the ability to ensure patient adherence to treatment plans is a primary driver of financial success.
| Feature | Fee-for-Service Model | Value-Based Care Model |
| Primary Goal | Volume of visits and tests | Quality of outcomes and efficiency |
| Patient Role | Passive recipient of care | Active partner in health management |
| Success Metric | Number of billable codes | Reduction in readmissions and complications |
| Communication | Episodic and reactive | Continuous and proactive |
To thrive in this landscape, systems must deliver personalized prompts that respect the patient’s lifestyle. By automating outreach for preventive screenings and wellness checks, providers can meet the quality metrics required for maximum reimbursement while fostering long-term loyalty.
C. Why engagement layers are replacing static EHRs
As the global Electronic Health Records (EHR) market scales from $32.4 billion in 2025 to $52.6 billion by 2034, this 62% expansion underscores a massive shift toward healthcare digitization. While standard EHRs prioritize documentation, an integrated engagement layer leverages this data via interoperability standards to drive advanced, real-time patient workflows.
This decoupled architecture offers several strategic advantages:
- Agility: Developers can update communication logic and user interfaces without disturbing the core clinical database.
- Behavioral Insights: Unlike a static record, an engagement layer tracks interaction data, such as message open rates and click-through actions, to refine future outreach.
- Consumer Experience: These systems provide the seamless, mobile-first experience patients have come to expect from other industries like retail or banking.
- Scalability: By using cloud-native infrastructures, these layers can manage millions of automated triggers across SMS, email, and push notifications simultaneously.
What Is an EHR Reminder & Engagement System?
An EHR Reminder tools & Engagement System bridges clinical data and patient action by turning EHR insights into timely, automated communication, ensuring care plans are followed while improving adherence, engagement, and overall patient outcomes.
A. From Passive EHRs to Active Care Platforms
The shift from passive EHRs to active care platforms with EHR Reminder tools transforms healthcare delivery by replacing manual outreach with real-time, logic-based triggers, enabling timely communication and reducing missed care opportunities.
Key Differences in System Logic:
- Data Liquidity: Instead of information sitting idle, an active platform identifies specific data points such as a missed lab result or an upcoming wellness exam and moves that information into a communication workflow.
- Trigger-Based Outreach: Actions are not dependent on staff memory; they are automated based on clinical protocols, ensuring no patient falls through the cracks.
- Two-Way Interaction: Unlike one-way portals, these platforms allow patients to confirm appointments, reschedule, or ask brief clarifying questions, creating a continuous loop of information.
B. Core Functions Beyond Basic Notifications
Modern EHR reminder tools go beyond basic reminders by managing the entire patient journey, from scheduling to post-discharge follow-ups, using advanced tools that reduce administrative workload while improving care precision and patient outcomes.
| Core Function | Practical Application | Strategic Value |
| Medication Adherence | Automated alerts for refills and dosage timings based on the pharmacy integration. | Reduces readmission rates for chronic disease patients. |
| Preventive Care Prompts | Identifying patients due for vaccinations or screenings based on age and history. | Drives revenue through high-value preventive services. |
| Post-Visit Surveys | Collecting Net Promoter Scores (NPS) and clinical feedback immediately after a consultation. | Enhances reputation management and quality of care metrics. |
| Educational Content | Sending targeted videos or articles related to a patient’s specific diagnosis or upcoming procedure. | Increases health literacy and reduces pre-surgical anxiety. |
C. Where It Fits in Modern Health Ecosystems
The EHR reminder tools in modern health ecosystems connect EHRs, telehealth platforms, and patient apps, acting as an orchestration engine that ensures consistent communication and prevents fragmented or conflicting patient messaging across channels.
Integration Touchpoints:
- Telehealth Integration: Automatically sending secure links and technical setup instructions 15 minutes before a virtual visit.
- Wearable Data Sync: Triggering a notification to a care manager if a patient’s wearable device detects an anomaly, such as a spike in blood pressure.
- Billing and Payments: Integrating with financial systems to send friendly reminders about outstanding balances or to offer payment plan options.
- Pharmacy Networks: Coordinating with external pharmacies to alert patients when a prescription is ready for pickup, closing the loop on the treatment cycle.
By positioning the engagement system as the central nervous system of patient interaction, organizations can create a unified experience that feels personalized rather than institutional.
Key Problems EHR Reminder Tools Solve for Providers
An EHR-integrated engagement system solves communication gaps between clinics and patients by automating administrative tasks, reducing inefficiencies, and enabling providers to focus more on clinical care while maintaining operational and financial performance.
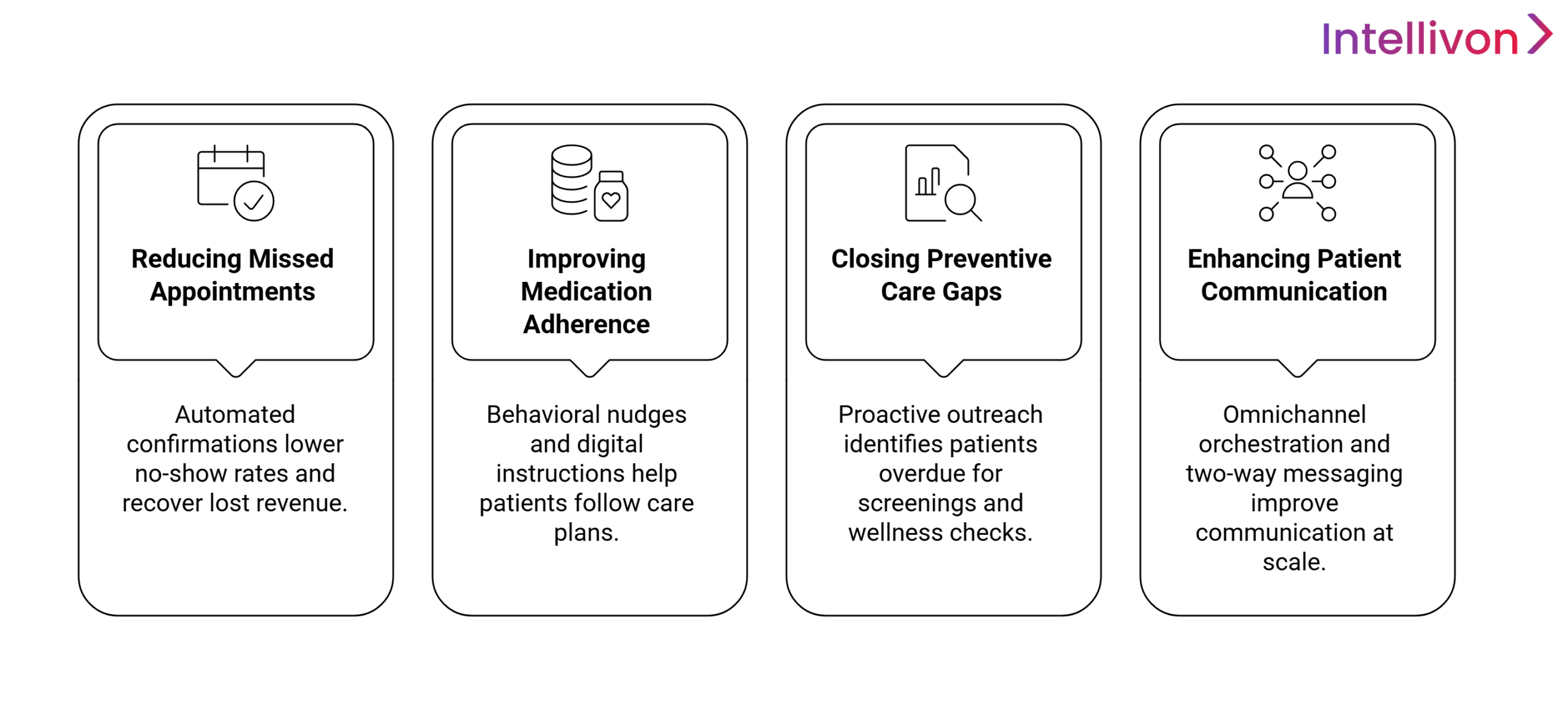
1. Reducing Missed Appointments and Revenue Loss
The financial stability of a practice depends on a predictable patient schedule. When appointments are missed without notice, the overhead costs of the facility remain, but the revenue disappears. Automated EHR reminder tools intervene by providing a multi-touch confirmation workflow that significantly lowers no-show rates.
Strategic Advantages of Automated Scheduling:
- Smart Confirmation Buffers: The system sends reminders at high-impact intervals such as 72 hours, 24 hours, and 2 hours before the visit, allowing patients to confirm or cancel early enough for the slot to be refilled.
- Waitlist Automation: When a cancellation is detected, the platform can automatically notify the next patient on the waitlist, ensuring the provider’s calendar remains optimized.
- Cost Recovery: By reducing no-shows by even 10% to 15%, a mid-sized practice can recover hundreds of thousands of dollars in annual revenue that would otherwise be lost to empty exam rooms.
2. Improving Medication and Care Plan Adherence
Patient non-adherence is a primary driver of hospital readmissions and poor clinical outcomes. Many patients struggle to follow complex medication schedules or post-discharge instructions once they leave the clinical setting. An EHR reminder tools extend the reach of the provider into the patient’s daily life.
Mechanisms for Driving Adherence:
- Behavioral Nudges: Timely SMS or push notifications remind patients to take specific dosages, reducing the likelihood of missed treatments.
- Digital Discharge Instructions: Instead of easily lost paper handouts, patients receive mobile-friendly summaries and “how-to” videos tailored to their recovery plan.
- Refill Synchronization: Integration with pharmacy data allows the system to alert patients when their medication is running low, prompting them to request a refill before they run out.
3. Closing Preventive Care and Follow-Up Gaps
Many patients only interact with healthcare providers when they are symptomatic, leading to missed opportunities for early intervention. The EHR reminder tools use data to identify patients who are overdue for screenings, vaccinations, or routine wellness checks.
Benefits of Proactive Outreach:
- Automated Population Health: The system segments the patient database by age, risk factors, or history to send targeted alerts for mammograms, colonoscopies, or flu shots.
- Chronic Disease Management: Patients with long-term conditions receive automated prompts for necessary lab work or quarterly check-ups, ensuring their condition is monitored consistently.
- Closing the Referral Loop: If a patient is referred to a specialist, the system tracks whether that appointment was scheduled and nudges the patient if they haven’t taken action.
4. Enhancing Patient Communication at Scale
Manual patient outreach is unscalable; a clinic’s staff can only make a finite number of phone calls per day. The EHR reminder tools allow a small administrative team to manage the communication needs of thousands of patients simultaneously without increasing headcount.
Operational Efficiency Gains:
- Omnichannel Orchestration: The system manages preferences automatically, sending a text to one patient and an email to another, ensuring the message is delivered via the most effective channel.
- Two-Way Messaging Hubs: Secure chat interfaces allow patients to ask simple administrative questions, which the system can often resolve using AI or route to the correct department.
- Standardized Messaging: Centralizing communication ensures that every patient receives consistent, high-quality information that reflects the provider’s brand and clinical standards.
Must-Have Features for a Scalable EHR Reminder Platform
A scalable EHR reminder tools and engagement platform uses a modular, real-time architecture to support complex workflows and deliver seamless, data-driven automation. These features ensure flexibility, interoperability, and reliable performance as patient demands grow.
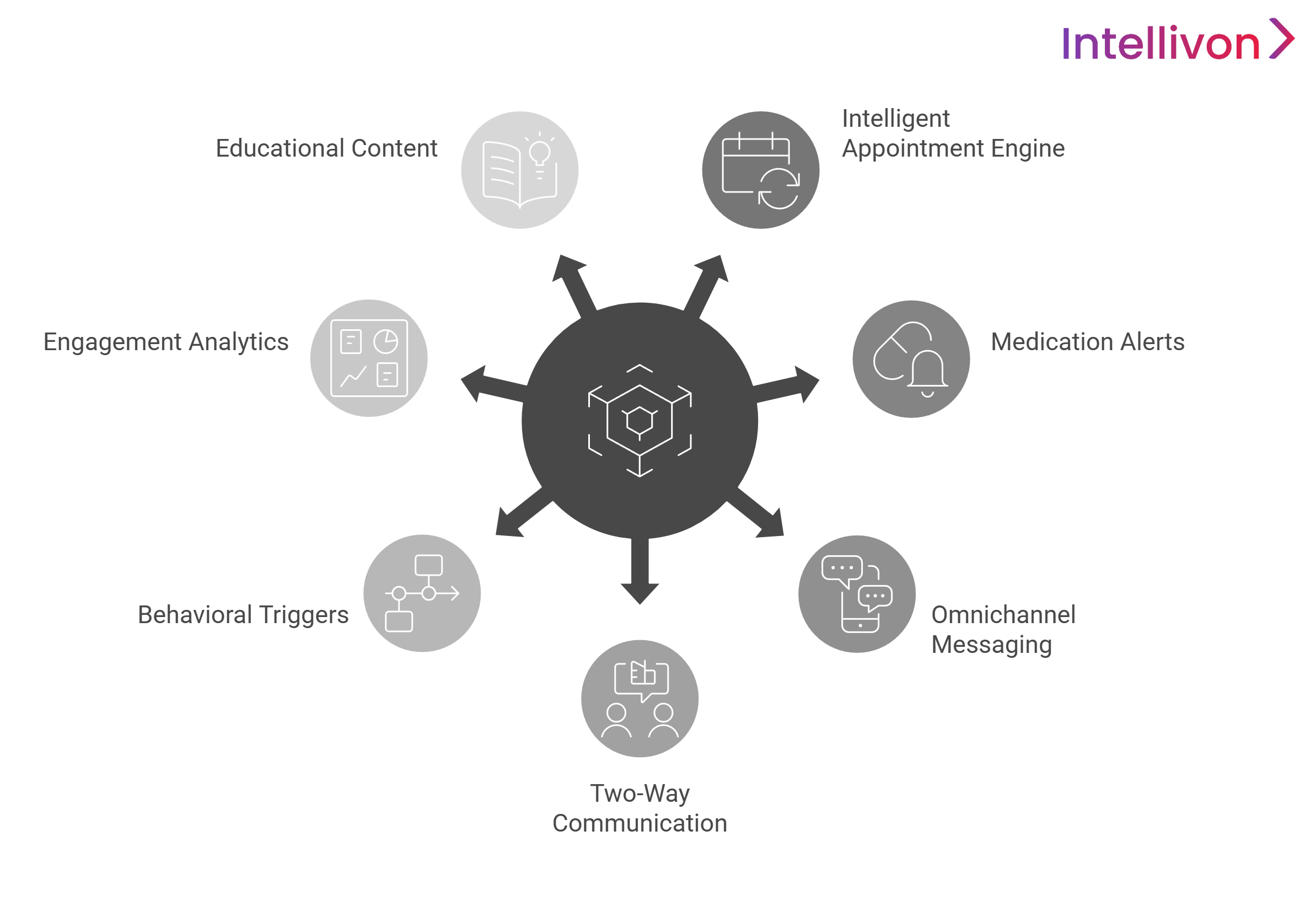
1. Intelligent Appointment Reminder Engine
The intelligent engine uses real-time EHR synchronization to identify bookings and cancellations, preventing outdated notifications. Custom cadence settings such as “Save the Date” alerts and tiered confirmation prompts ensure patients receive logic-driven outreach via their preferred methods.
Smart logic updates EHR statuses instantly upon SMS confirmation, eliminating manual calls. Automated rescheduling workflows then capture cancelling patients, minimizing revenue leakage and maintaining care continuity.
2. Medication Alerts With Adherence Tracking
This module utilizes automated alerts to remind patients of dosages, cross-referencing EHR medication lists for accuracy. By tracking adherence patterns, the system identifies non-compliant patients, allowing for timely clinical interventions and improved outcomes.
Care teams receive real-time adherence reports, highlighting patients who consistently miss doses. This proactive monitoring transforms a passive prescription into an active, tracked treatment plan that significantly reduces the risk of medication-related readmissions.
3. Omnichannel Messaging (SMS, Email, Push)
An omnichannel delivery layer ensures patients receive critical information via their preferred channels. By diversifying outreach through SMS, email, and push notifications, the system maximizes open rates and ensures that urgent health updates are never missed.
The platform maintains cross-channel synchronization, ensuring a consistent message across all devices. This unified communication strategy improves patient accessibility and allows providers to reach diverse demographics through the most effective digital touchpoints available.
4. Two-Way Patient Communication Hub
This hub enables secure, two-way dialogue between patients and providers, moving beyond one-way blasts. Patients can ask questions or clarify instructions, fostering a collaborative care environment that strengthens the provider-patient relationship and increases trust.
Integrated directly with the EHR inbox, these messages are routed to the appropriate staff members. This centralized communication flow reduces phone tag, accelerates response times, and ensures all patient interactions are documented for clinical continuity.
5. Behavioral Triggers and Smart Workflows
Behavioral triggers initiate automated workflows based on specific patient actions or data changes within the EHR reminder tools. Whether a missed lab result or a high blood pressure reading, the system automates follow-up without manual staff effort.
These smart workflows guide patients through complex care journeys by providing the right information at the right time. By responding to individual patient behaviors, the system creates a personalized experience that drives higher engagement and better health literacy.
6. Patient Feedback and Engagement Analytics
The analytics engine captures and visualizes patient engagement data, from message open rates to satisfaction scores. These real-time insights allow administrators to identify bottlenecks in the care funnel and optimize outreach strategies for maximum impact.
Automated post-visit surveys collect immediate feedback, helping providers address concerns before they escalate. This data-driven approach enables continuous service improvement and provides tangible proof of the platform’s return on investment and clinical efficacy.
7. Educational Content and Care Nudges
Care nudges deliver bite-sized, relevant educational content tailored to a patient’s specific diagnosis or upcoming procedure. These micro-learning moments empower patients with the knowledge needed to manage their health effectively between scheduled clinical visits.
The system ensures patients are properly prepared by automating the delivery of pre-operative or post-operative instructions. This preventive education reduces anxiety, minimizes surgical cancellations, and promotes long-term behavioral changes that lead to sustained wellness.
Advanced Features of EHR Patient Reminder System That Drive Real Engagement
Advanced EHR reminder tools use AI and real-time data to deliver personalized communication that reduces message fatigue and improves outcomes. These features drive predictive outreach, stronger patient trust, and higher adherence for better retention and population health.
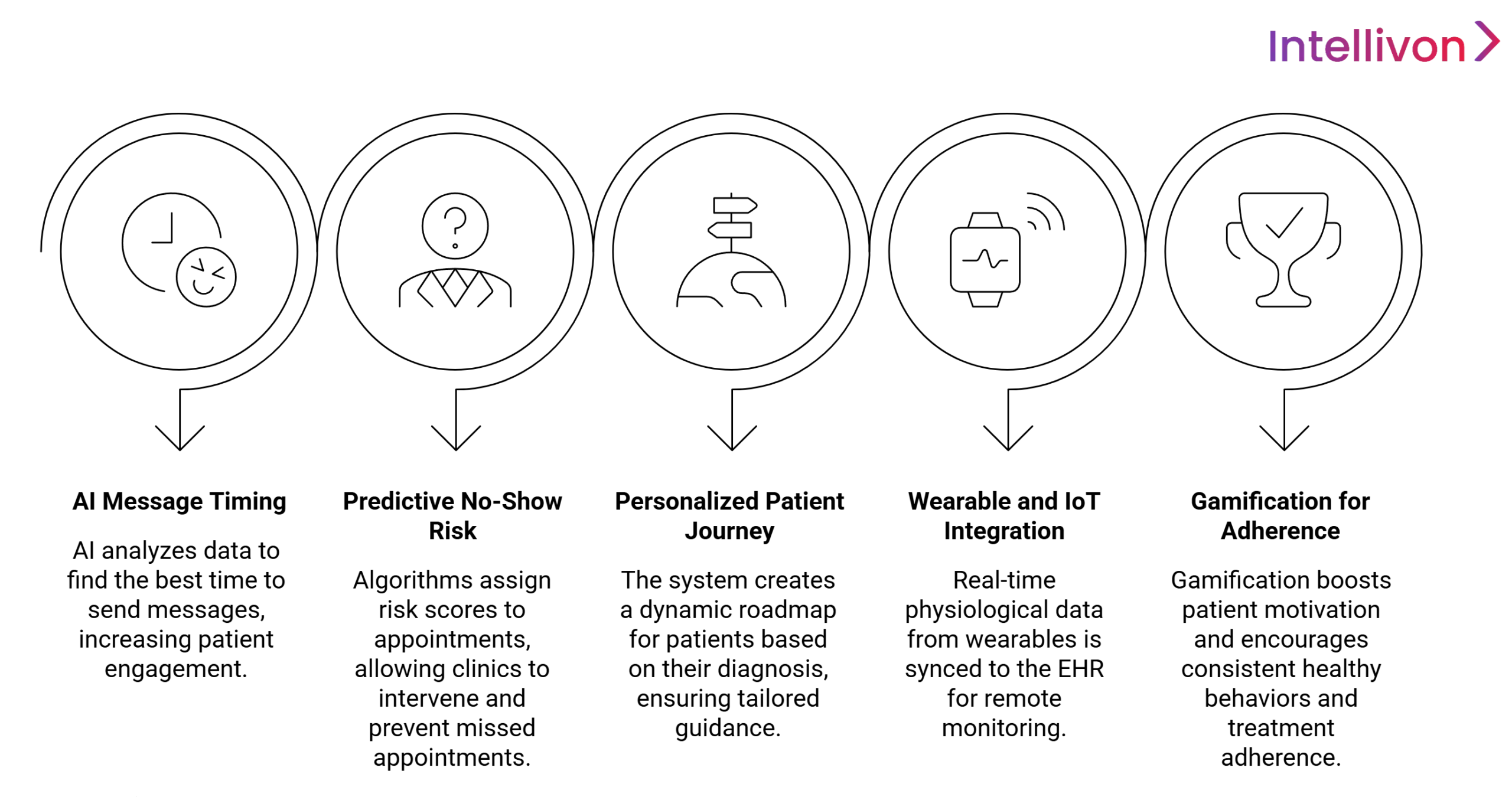
1. AI-Based Message Timing Optimization
AI-based timing optimization analyzes historical data to identify each patient’s golden window for engagement. By replacing traditional batch-sending with predictive, staggered delivery, the system ensures critical prompts arrive when patients are most likely to act, maximizing conversion rates.
2. Predictive No-Show Risk Scoring
Predictive algorithms analyze historical attendance and socioeconomic factors to assign a risk score to every appointment. By identifying high-risk patients in advance, clinics can implement targeted interventions like personalized transportation assistance or additional phone reminders to protect schedules.
3. Personalized Patient Journey Mapping
The system creates a dynamic roadmap based on specific diagnoses, ensuring patients receive the right guidance at each clinical milestone. This tailored approach automates the delivery of preparation steps and recovery goals, fostering a seamless care experience through individual journeys.
4. Integration With Wearables and IoT Data
The platform feeds real-time physiological data by syncing with wearable devices directly into the EHR. This constant stream of biometric insights allows for remote monitoring, enabling providers to detect anomalies and intervene before minor health shifts escalate into emergency situations.
5. Gamification for Long-Term Adherence
Gamification mechanics like progress bars and achievement badges incentivize consistent health behaviors and treatment compliance. By transforming routine tasks into a rewarding achievement system, the platform taps into psychological drivers that sustain long-term patient motivation and wellness.
How FHIR Enables Seamless EHR Integration in Patient Reminder System?
FHIR enables seamless EHR integration by providing a standardized, flexible framework for data exchange, replacing rigid legacy systems and allowing engagement platforms to communicate efficiently with Electronic Health Records.
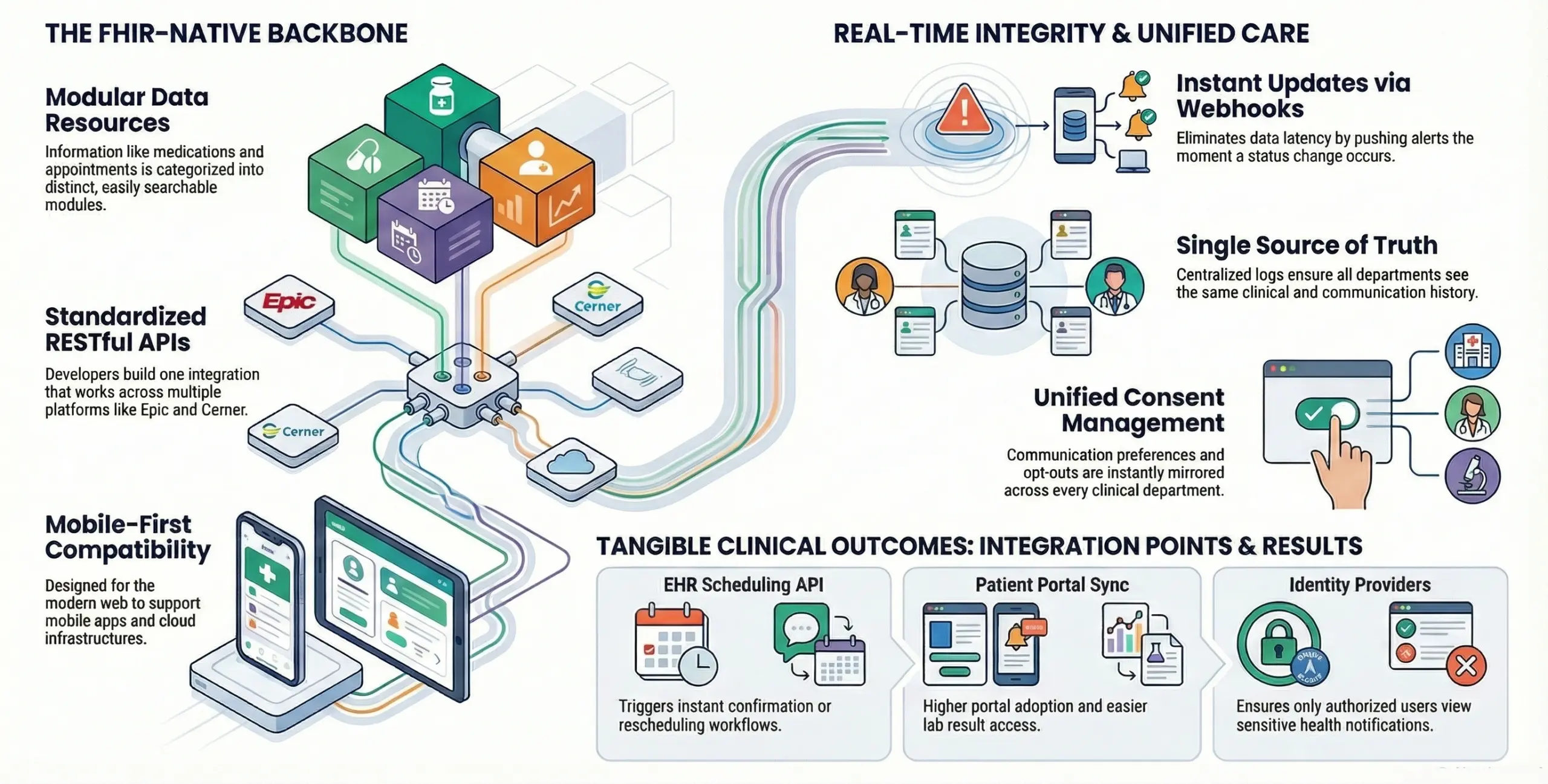
A. Why FHIR Is the Backbone of Interoperability
FHIR revolutionizes healthcare data exchange by treating medical information as a set of modular “resources.”Unlike older standards that required complex, custom-built interfaces for every hospital, FHIR uses modern web technologies to make data easily accessible and searchable.
Strategic Advantages of a FHIR-Based Core:
- Modular Data Handling: Information such as “Patient,” “Medication,” or “Appointment” is categorized into distinct resources, allowing the system to request only the specific data needed for a reminder.
- Reduced Development Time: Using standardized RESTful APIs means developers can build one integration that works across multiple FHIR-compliant EHRs like Epic, Cerner, or Allscripts.
- Future-Proofing: As regulations like the CMS Interoperability and Patient Access final rule evolve, having a FHIR-native backbone ensures the platform remains compliant with federal data-sharing mandates.
- Mobile-First Compatibility: FHIR was designed for the modern web, making it natively compatible with the mobile apps and cloud infrastructures used for patient engagement.
B. Connecting With EHRs, APIs, and Portals
A truly integrated engagement system acts as a sophisticated bridge between the provider’s internal database and the patient’s external interface. This connection is maintained through a series of secure API calls that trigger actions based on clinical updates.
| Integration Point | Purpose | Outcome |
| EHR Scheduling API | Monitors the calendar for new or changed bookings. | Triggers instant confirmation or rescheduling workflows. |
| Patient Portal Sync | Bridges the gap between the secure portal and mobile notifications. | Higher portal adoption and easier access to lab results. |
| Third-Party Health APIs | Connects to external labs, pharmacies, or imaging centers. | Provides a unified view of the patient’s care journey beyond one clinic. |
| Identity Providers | Uses OAuth2/OpenID Connect for secure patient authentication. | Ensures only the authorized user can view sensitive health notifications. |
C. Real-Time Sync Across Healthcare Systems
Data latency is a significant risk in patient communication. If a patient cancels an appointment at 10:00 AM, but the reminder system doesn’t sync until noon, the patient may receive a redundant notification that creates confusion. Real-time synchronization prevents these friction points.
How Real-Time Sync Maintains System Integrity:
- Webhooks for Instant Updates: Instead of “polling” the EHR every few hours, the system uses webhooks to receive instant alerts the moment a status change occurs.
- Conflict Resolution: Intelligent logic ensures that if a patient updates their phone number in the portal, it is immediately mirrored across the reminder engine and the EHR.
- Consistent Patient Experience: Real-time sync ensures that no matter where the patient interacts with the system, they see the most current and accurate version of their care plan.
D. Avoiding Data Silos in Patient Communication
One of the greatest frustrations for patients is “fragmented” communication, where they receive different messages from the billing department, the specialist, and the primary care doctor. An integrated FHIR layer eliminates these silos by creating a “Single Source of Truth.”
Methods for Breaking Down Information Silos:
- Centralized Communication Logs: Every SMS, email, and call is logged back into a single activity feed accessible to all authorized clinical staff.
- Cross-Departmental Workflows: Information from a specialist’s referral is automatically used to trigger a follow-up reminder from the primary care office.
- Unified Consent Management: If a patient opts out of SMS for billing, the system ensures that preference is respected across all clinical departments simultaneously.
- Longitudinal Data Aggregation: By pulling data from various sources into one engagement stream, the system provides a holistic view of the patient’s adherence and interaction history.
Architecture of a Modern Engagement Platform
A modern engagement platform uses cloud-native, distributed architecture to replace legacy systems, ensuring scalability, high availability, security, and real-time data synchronization under growing patient loads.
The following table outlines the foundational architectural pillars required to support a sophisticated, investor-grade EHR engagement layer:
| Architectural Component | Technical Implementation | Strategic Business Value |
| Cloud-Native Infrastructure (AWS or Azure) | Utilizing HIPAA-eligible services like AWS Nitro or Azure Health Data Services for encrypted compute and storage. | Provides infinite horizontal scaling while offloading security compliance to the cloud provider, ensuring the system grows alongside increasing patient loads. |
| Event-Driven Notification Systems | Implementing message brokers like Apache Kafka or RabbitMQ to trigger alerts based on specific EHR “events” (e.g., a new lab result). | Ensures notifications process asynchronously, preventing system bottlenecks during peak hours and guaranteeing no critical patient alert is ever lost. |
| Microservices for Scalability and Flexibility | Decoupling core functions (Scheduling, Messaging, Billing, Consent) into independent, containerized services using Docker and Kubernetes. | Enables rapid deployment of new features without risking platform stability, allowing individual services to remain fully operational during targeted updates. |
| Data Pipelines for Real-Time Patient Insights | Deploying ETL (Extract, Transform, Load) pipelines to stream de-identified engagement data into analytics engines like Snowflake or BigQuery. | Converts raw logs into actionable business intelligence, allowing providers to identify high-risk patient cohorts and optimize the ROI of outreach strategies. |
Security and Compliance You Cannot Ignore for EHR Reminder Tools
Security in healthcare is fundamental, requiring a security-first approach to protect PHI across both storage and communication channels. A multi-layered defense strategy ensures compliance, builds provider trust, and minimizes legal and financial risks.
1. HIPAA Compliance for PHI Protection
The Health Insurance Portability and Accountability Act (HIPAA) sets the gold standard for sensitive patient data protection. Compliance requires a combination of administrative, physical, and technical safeguards to ensure the confidentiality, integrity, and availability of PHI.
- Business Associate Agreements (BAAs): Every vendor, from cloud providers to SMS gateways, must sign a BAA to legally share data protection responsibility across the entire supply chain.
- Data Minimization: Systems must transmit only the minimum necessary information to perform tasks, such as omitting clinical diagnoses from SMS reminders to significantly reduce exposure risk.
- Technical Safeguards: Implementation of automated log-offs and unique user identification ensures precise tracking of record access within the dashboard, maintaining rigorous session management.
2. End-to-End Encryption and Secure Messaging
Standard SMS and unencrypted email are inherently insecure channels. To remain compliant while providing a modern experience, an engagement platform must utilize high-level encryption standards for all data transfers.
- In-Transit Security: All API calls between the EHR and engagement layer utilize TLS 1.3 encryption. This standard secures data during transmission, effectively preventing man-in-the-middle attacks and unauthorized interception.
- At-Rest Protection: Databases containing patient identifiers use AES-256-bit encryption. This ensures that even if physical storage is compromised, the sensitive data remains entirely unreadable to unauthorized parties.
- Secure Link Strategies: Systems bypass the risks of SMS-based health data by using expiring, authenticated links. Patients must verify their identity before accessing care instructions or lab results, ensuring end-to-end privacy.
3. Consent Management and Patient Permissions
Patient autonomy is a critical component of both regulatory compliance and a positive user experience. A scalable system must include a centralized engine to manage how, when, and if a patient wants to be contacted.
| Permission Type | Implementation Method | Regulatory Requirement |
| Opt-In/Opt-Out | Keyword triggers (e.g., “STOP” to unsub) and web-based preference centers. | TCPA (Telephone Consumer Protection Act) compliance. |
| Channel Preference | Allowing patients to choose between SMS, Email, or Voice for different alert types. | Patient-centric engagement standards. |
| Granular Consent | Separating consent for marketing/wellness tips from critical clinical alerts. | GDPR and HIPAA “Right to Restrict” provisions. |
4. Role-Based Access and Audit Logging
Not every user of the platform needs access to every piece of patient data. Role-Based Access Control (RBAC) ensures that administrative staff, nurses, and IT managers have permissions tailored strictly to their job functions.
- Principle of Least Privilege: A front-desk user may see appointment times and phone numbers, while a clinical researcher may only see de-identified outcome data.
- Immutable Audit Trails: The system must record every instance of data access, modification, or transmission. These logs must be “read-only” and stored in a secure location to provide a clear forensic trail in the event of an audit or security incident.
- Real-Time Monitoring: Advanced systems use automated tools to flag unusual access patterns, such as an employee viewing an unusually high number of patient records in a short timeframe.
5. Zero-Trust Architecture for Healthcare Apps
Traditional “perimeter-based” security is no longer sufficient for cloud-connected healthcare apps. A Zero-Trust architecture operates on the assumption that threats could exist both outside and inside the network, requiring continuous verification of every user and device.
- Identity Verification: Implementing Multi-Factor Authentication (MFA) for all provider-facing dashboards is a non-negotiable requirement for Zero-Trust.
- Micro-Segmentation: By isolating the messaging service from the core database, a breach in one area does not grant the attacker access to the entire system.
- Device Health Checks: The system can verify that a clinician’s tablet or laptop meets specific security standards (e.g., updated OS, disk encryption) before allowing it to connect to the engagement layer.
- Least-Privilege Orchestration: Every API request is individually authenticated and authorized, ensuring that the engagement layer only pulls the specific “Patient Resource” it needs for a single notification.
Step-by-Step Process to Build the EHR Patient Reminder System
The development of a high-performance engagement layer requires a phased approach that prioritizes clinical utility and data integrity. By moving from core notification logic to sophisticated AI integration, developers ensure the platform remains stable while adapting to complex provider needs.
1. Define Use Cases and Target Patient Groups
Patient demographics and specific clinical goals dictate the underlying logic of the system. High-risk chronic cohorts require different touchpoints than pediatric wellness groups. Precise segmentation ensures that the engagement strategy addresses unique barriers to care and specific reimbursement requirements.
2. Design Engagement Flows and User Journeys
The orchestration of automated triggers across the patient lifecycle prevents communication gaps. Mapping every interaction from the initial booking to post-discharge follow-up creates a cohesive experience. Each journey must account for diverse preferences in channel, frequency, and message tone.
3. Build MVP With Core Reminder Features
A Minimum Viable Product focuses on the most immediate revenue-protecting functions, such as automated SMS appointment confirmations. This foundational layer establishes the essential handshake between the scheduling engine and the notification service, providing immediate operational value and measurable ROI.
4. Integrate With EHR Using FHIR APIs
Secure data exchange via FHIR resources enables the platform to pull real-time clinical context. This integration point is the most critical technical milestone, ensuring that patient records, medication lists, and provider schedules remain synchronized without manual data entry.
5. Test With Real Patient Scenarios
Rigorous validation in simulated clinical environments identifies potential friction in the user interface. Testing ensures that edge cases, such as last-minute cancellations or insurance updates, trigger the correct automated responses without compromising the accuracy of the underlying medical record.
6. Scale With AI and Advanced Automation
Machine learning models optimize message delivery timing and predict patient no-show risks as the user base expands. This advanced tier of development transforms the system into a proactive care partner that continuously learns from historical engagement data and behavioral patterns.
Cost to Build an EHR Patient Engagement Platform
The cost to build an EHR patient engagement platform varies based on features, integrations, compliance, and scalability, depending on overall system complexity and architecture.
The table below outlines estimated costs by platform capabilities, helping stakeholders plan budgets and prioritize feature investments.
| Development Phase | MVP Level | Enterprise Level | Key Deliverables |
| Platform Infrastructure | $25,000 – $40,000 | $70,000 – $120,000 | HIPAA-compliant cloud setup, FHIR-native DB, and secure API gateway. |
| Communication Engine | $20,000 – $35,000 | $60,000 – $95,000 | Automated multi-channel triggers, two-way messaging, and push orchestration. |
| EHR Integration Layer | $35,000 – $55,000 | $100,000 – $180,000 | FHIR R4/R5 resource mapping, OAuth2/SMART authorization, and real-time sync. |
| Security & Compliance | $20,000 – $30,000 | $50,000 – $90,000 | End-to-end encryption, BAA management, audit trails, and RBAC systems. |
| Intelligence & Analytics | $25,000 – $45,000 | $80,000 – $150,000+ | Data normalization, risk-scoring models, and executive ROI dashboards. |
| Total Estimated Cost | $125,000 – $205,000 | $260,000 – $335,000+ | Full-Scale Care Engagement Ecosystem |
Cost-Affecting Factors During Development
The total expenditure for a healthcare platform is rarely a flat fee; it is influenced by technical debt, regulatory hurdles, and the breadth of the intended user base. Understanding these variables allows for better budget allocation and prevents unexpected scope creep during the engineering cycle.
Primary Drivers of Development Costs:
- Interoperability Complexity: Integrating FHIR-ready EHRs costs $35,000–$50,000, but legacy HL7 v2 systems often require custom middleware that can double the budget.
- Regulatory Compliance Audits: While HIPAA is standard, formal SOC2 Type II or HITRUST certifications add $25,000–$65,000 in third-party auditing and documentation costs.
- Volume of PHI Processing: High-volume systems handling 1M+ monthly notifications require sophisticated auto-scaling, increasing monthly DevOps overhead by 20%–30%.
- AI and Machine Learning Depth: Custom predictive models increase timelines by 4–6 months and add roughly $90,000 to the payroll for specialized data science expertise.
- Third-Party API Fees: SMS and voice messaging costs are major operational expenses; high-volume platforms must factor in a 15%–20% margin for recurring delivery fees.
Timeline to Develop and Launch the Platform
Healthcare development timelines are often dictated by integration complexity and compliance audits. A tiered approach enables a faster initial launch of core features, allowing organizations to realize ROI while developing advanced AI capabilities.
A. MVP Development Timeline (8–12 Weeks)
The initial phase establishes a secure communication bridge, prioritizing FHIR resource mapping and HIPAA-eligible infrastructure to launch a functional prototype with core notification capabilities.
- Weeks 1–4: Infrastructure & Mapping: Focuses on cloud deployment and mapping essential EHR data resources to ensure seamless system interoperability.
- Weeks 5–8: Prototype Development: Building the engine to pull real-time appointment data and trigger automated, basic SMS notifications.
- Weeks 9–12: Testing & Compliance: Conducting end-to-end testing for data encryption and ensuring strict adherence to patient opt-out preferences.
B. Full Product Rollout Timeline
Transitioning to a comprehensive platform involves iterative development of advanced communication hubs, wearable integrations, and predictive models, utilizing a soft launch strategy to refine triggers before system-wide deployment.
- Months 1–3: Advanced Feature Integration: Development focuses on the two-way communication hub, wearable API syncing, and deploying machine learning models for predictive risk scoring.
- Months 4–5: Soft Launch & Refinement: Rolling the system out to a single department to calibrate automated triggers and refine message templates based on real-world patient responses.
- Month 6: Full System Deployment: Executing the enterprise-wide rollout across the entire health system, supported by optimized workflows and scaled cloud infrastructure.
C. Factors That Impact Time to Market
Launch timelines are often delayed by EHR vendor credentialing and the inherent complexity of clinical workflows. While simple reminders deploy quickly, multi-stage care journeys require significantly more development and administrative rigor.
Key Drivers of Timeline Variance:
- EHR Vendor Responsiveness: The time required to get API production keys from vendors like Epic or Cerner can vary significantly.
- Data Mapping Requirements: Customizing FHIR resources to match the specific way a clinic records “Patient” or “Observation” data can add weeks to the integration phase.
- Compliance Documentation: Preparing for a formal HIPAA audit or HITRUST certification requires extensive policy writing that runs parallel to the coding process.
- Third-Party Approvals: Registering 10-digit long code (10DLC) or Short Codes for SMS delivery involves carrier approval times that are outside of the developer’s control.
D. Key Milestone Summary
This key milestone summary outlines the critical phases from initial discovery to full market scale, providing a structured roadmap to balance rapid MVP deployment with long-term advanced feature integration.
| Milestone Phase | Estimated Duration | Primary Focus |
| Phase 1: Discovery & Architecture | 2–3 Weeks | Technical scoping, FHIR resource identification, and HIPAA cloud setup. |
| Phase 2: MVP Core Build | 6–8 Weeks | API integration, basic notification engine, and secure data pipelines. |
| Phase 3: Integration Testing | 2–4 Weeks | Sandbox testing with EHR data, security audits, and UAT (User Acceptance Testing). |
| Phase 4: Advanced Feature Set | 12–16 Weeks | AI risk models, two-way messaging hub, and wearable data integration. |
| Phase 5: Full Market Scale | Ongoing | Continuous optimization, multi-EHR expansion, and population health analytics. |
Real Use Cases Across Healthcare Segments
The versatility of an engagement layer allows it to solve distinct operational challenges across the medical spectrum. By tailoring automated workflows to specific clinical settings, organizations can address the unique friction points that lead to revenue loss and patient dissatisfaction.
1. Hospitals Managing High Patient Volumes
Large-scale health systems utilize automated orchestration to synchronize thousands of departmental interactions. Centralized communication hubs prevent message duplication while ensuring that critical pre-operative instructions reach the correct patient population at scale.
Real-World Example: Mayo Clinic integrated an engagement platform with Epic EHR to automate follow-ups. Using “care pathways,” they reduced manual outreach by 60% and improved patient recovery tracking across high-volume surgical departments.
2. Clinics Reducing Daily No-Show Rates
Private practices employ intelligent reminder cadences to stabilize their daily revenue streams. Automated multi-channel confirmations allow administrative staff to focus on high-value clinical tasks rather than manual outbound calling for appointment verification.
Real-World Example: VillageMD utilized bidirectional SMS integrated with practice management software to tackle chronic no-shows. This deployment achieved a 20% reduction in no-show rates across hundreds of locations, recovering millions in potentially lost clinical revenue.
3. Chronic Care and Remote Patient Monitoring
Long-term health management relies on consistent behavioral nudges and physiological data integration. Persistent engagement workflows ensure that patients with hypertension or diabetes remain adherent to their treatment plans between quarterly office visits.
Real-World Example: Ochsner Health’s “Digital Medicine” program uses wireless devices to monitor chronic conditions. Automatically triggering “pharmacist nudges” for out-of-range readings, the system helped 71% of patients achieve blood pressure control within just 90 days.
4. Telehealth Platforms Improving Retention
Virtual care providers leverage automated technical check-ins to ensure seamless digital encounters. High-frequency communication during the “waiting room” phase reduces patient abandonment rates and builds trust in the reliability of the remote care model.
Real-World Example: Teladoc Health uses an engagement engine to automate “pre-visit” requirements. By delivering secure entry links and hardware checks 10 minutes before sessions, they maintained high “visit completion” rates, even during peak pandemic system surges.
Common Mistakes to Avoid in Development
Building effective EHR reminder and patient engagement systems is complex, and common mistakes can hinder outcomes and user adoption. Our developers proactively address these pitfalls with smart design, compliance focus, and user-centric solutions.
1. Ignoring Patient Experience and UX Design
Challenge: Overly complex interfaces and fragmented navigation lead to high abandonment rates, preventing patients from completing essential tasks like scheduling or viewing results.
Solution: Our developers prioritize a mobile-first, “zero-friction” design philosophy, utilizing rapid prototyping and usability testing to ensure every patient touchpoint is intuitive, accessible, and requires minimal cognitive load.
2. Weak Integration With Existing EHR Systems
Challenge: Poorly executed data synchronization creates information silos, resulting in redundant notifications or outdated appointment details that confuse patients and frustrate clinical staff.
Solution: We implement robust FHIR-native connectors and custom webhooks to ensure bi-directional, real-time data flow, allowing the engagement layer to act as a seamless extension of the core EHR.
3. Overlooking Compliance Early in Development
Challenge: Treating security as an afterthought leads to expensive architectural reworks or catastrophic data breaches that jeopardize the organization’s legal standing and reputation.
Solution: Our team embeds HIPAA-compliant protocols and “Privacy by Design” principles from day one, utilizing automated compliance scanning and encrypted data-at-rest to ensure a baseline of total security.
4. Lack of Personalization in Engagement Flows
Challenge: Generic, high-frequency messaging causes “notification fatigue,” leading patients to opt out of the system and ignore critical clinical alerts or follow-up prompts.
Solution: We utilize behavioral data and patient preference mapping to tailor the timing, tone, and channel of every message, ensuring each interaction feels relevant and supportive rather than intrusive.
Monetization Models for EHR Patient Engagement Platform
EHR reminder and patient engagement platforms earn through subscriptions, usage-based pricing, and value-added services while supporting scalable, compliant healthcare solutions. These monetization models boost ROI, improve patient retention, and enable sustainable, flexible, and data-driven growth.
1. SaaS Subscription for Healthcare Providers
Standard recurring fees give hospitals predictable budgets and developers steady revenue for maintenance. Pricing is usually tiered into Basic, Pro and Enterprise based on providers and locations or clinical modules.
Real-World Example: Doctolib primarily operates on a pure SaaS subscription model, charging healthcare professionals a fixed monthly fee (ranging from approximately €129 to €249) for access to its booking, telemedicine, and practice management suite.
2. Per-Patient or Per-Message Pricing
Usage-based models link platform costs to outreach volume, making them a flexible “pay-as-you-grow” option for smaller practices. Providers pay only for actual engagement, such as SMS segments, automated voice calls, or active patient records.
Real-World Example: Klara often utilizes a custom pricing structure that can include usage-based components, where the total cost is influenced by the practice’s total patient volume and the specific number of automated “conversations” or messages processed by the system.
3. Value-Based Care Revenue Models
Performance-linked pricing aligns platform incentives with clinical goals like reduced readmissions. In this model, providers share a percentage of value-based care savings or pay “bonuses” for meeting specific performance benchmarks.
Real-World Example: Phreesia monetizes its platform via “Network Solutions,” where life sciences companies and payers fund targeted patient engagement. This model capitalizes on improved medication adherence and clinical outcomes driven by the platform’s automated interactions.
4. Integration Partnerships With Health Systems
Strategic partnerships involve high-value, long-term agreements where the platform becomes the exclusive communication layer for massive health networks. These deals typically bundle custom development fees with per-user licensing for thousands of clinical staff.
Real-World Example: Luma Health frequently secures large-scale enterprise partnerships with systems like Banner Health or Cook County Health, where the platform is integrated deeply into the health system’s existing infrastructure via long-term, multi-million dollar institutional contracts.
Why Healthcare Startups Choose Intellivon?
Selecting a development partner is a high-stakes decision that dictates the long-term scalability and security of your platform. Intellivon combines deep domain expertise with an agile approach to deliver investor-grade healthcare solutions.
We focus on bridging the gap between complex clinical data and meaningful patient engagement, ensuring your product is built on a foundation of technical excellence and regulatory rigor.
A. Proven Expertise in HIPAA-Compliant Systems
Security is embedded into every line of code we write, ensuring total protection of Protected Health Information (PHI). Our teams utilize zero-trust architectures and advanced encryption to meet stringent regulatory standards.
B. Experience With FHIR and EHR Integrations
We specialize in seamless data exchange using the HL7 FHIR standard to connect with major EHRs like Epic and Cerner. This ensures your platform maintains real-time synchronization across the entire healthcare ecosystem.
C. End-to-End Product Strategy and Development
Our collaborative approach covers everything from initial discovery and UI/UX design to full-scale engineering. We align your product roadmap with market demands to ensure a successful launch and sustainable growth.
D. Scalable and Secure Cloud Deployments
We build infrastructures that scale effortlessly, utilizing AWS and Azure Health Data Services with your user base. Our DevOps protocols guarantee high availability and performance while maintaining 100% compliance in the cloud.
Conclusion
Building an EHR Reminder and Patient Engagement System is more than a technical project; it is a strategic investment in the future of value-based healthcare. By automating the touchpoints that occur between clinical visits, providers can significantly reduce revenue loss from no-shows, improve medication adherence, and foster deeper patient loyalty. As the industry moves toward a more proactive, data-driven model, the organizations that prioritize a seamless, integrated patient experience will be the ones that lead the market.
FAQs
Q.1. What are the must-have compliance features for healthcare apps?
A.1. The platform requires immutable audit trails, unique user identification, and automated session log-offs beyond basic HIPAA encryption. You must also execute Business Associate Agreements with every sub-vendor in your cloud stack.
Q.2. How to integrate a patient engagement system with an EHR?
A.2. The industry standard is utilizing FHIR APIs for real-time data exchange. This allows your system to securely pull appointment data and push patient responses directly into workflows within Epic or Cerner.
Q.3. How does predictive analytics improve patient attendance?
A.3. Predictive models analyze historical data to identify patients at high risk for no-shows. This allows the platform to trigger intensified, personalized outreach or alternative scheduling options specifically for those individuals.
Q.4. What is the role of a BAA in EHR patient engagement software?
A.4. A Business Associate Agreement is a legal contract required by HIPAA. It ensures that third-party vendors, such as cloud providers or messaging APIs, maintain strict security standards while handling your patients’ data.