Key Takeaways:
-
AI claims platforms reduce cycle time, detect fraud, and support adjuster decisions.
-
Building custom platforms protects proprietary fraud models, risk data, and competitive advantages.
-
Development costs range from $50,000 for MVPs to $200,000 for enterprise infrastructure.
-
NLP, computer vision, and anomaly detection work together to process every claim intelligently.
-
Explainability, bias testing, and human oversight keep AI claims platforms compliant and defensible.
Insurance claims operations rely on speed, accuracy, and defensible decisions. But as claim volumes increase and fraud patterns become harder to spot manually, the gap between what traditional claims software offers and what modern operations need has become a significant issue. Claims teams require a layer of intelligence that reads claim data, understands policy context, flags risks, detects fraud patterns, routes claims to the correct adjuster, and produces decisions that are ready for audits from the start.
Creating that intelligence layer involves much more than just deploying AI models. In fact, claims data pipelines, policy logic engines, document intelligence, human review workflows, explainability frameworks, fraud signal detection, system integrations, and secure infrastructure must all work together. At the same time, the platform architecture is as important as the AI itself.
Organizations that succeed in this area reduce claim cycle times, lower fraud risk, and provide adjusters with the decision support they need. Those who underestimate the complexity of building these systems end up with tools that do not fit into real workflows and provide minimal operational value.
Intellivon builds AI claims intelligence platforms for insurers, MGAs, and claims technology companies that require production-grade infrastructure instead of just proof-of-concept AI. This blog draws from that experience and shows you how we build these platforms from the ground up.
Why Insurance Companies Are Building AI Claims Intelligence Platforms
Insurance companies are accelerating investment in AI claims intelligence platforms because legacy systems were not built for the scale, speed, or complexity that modern claims operations now demand.
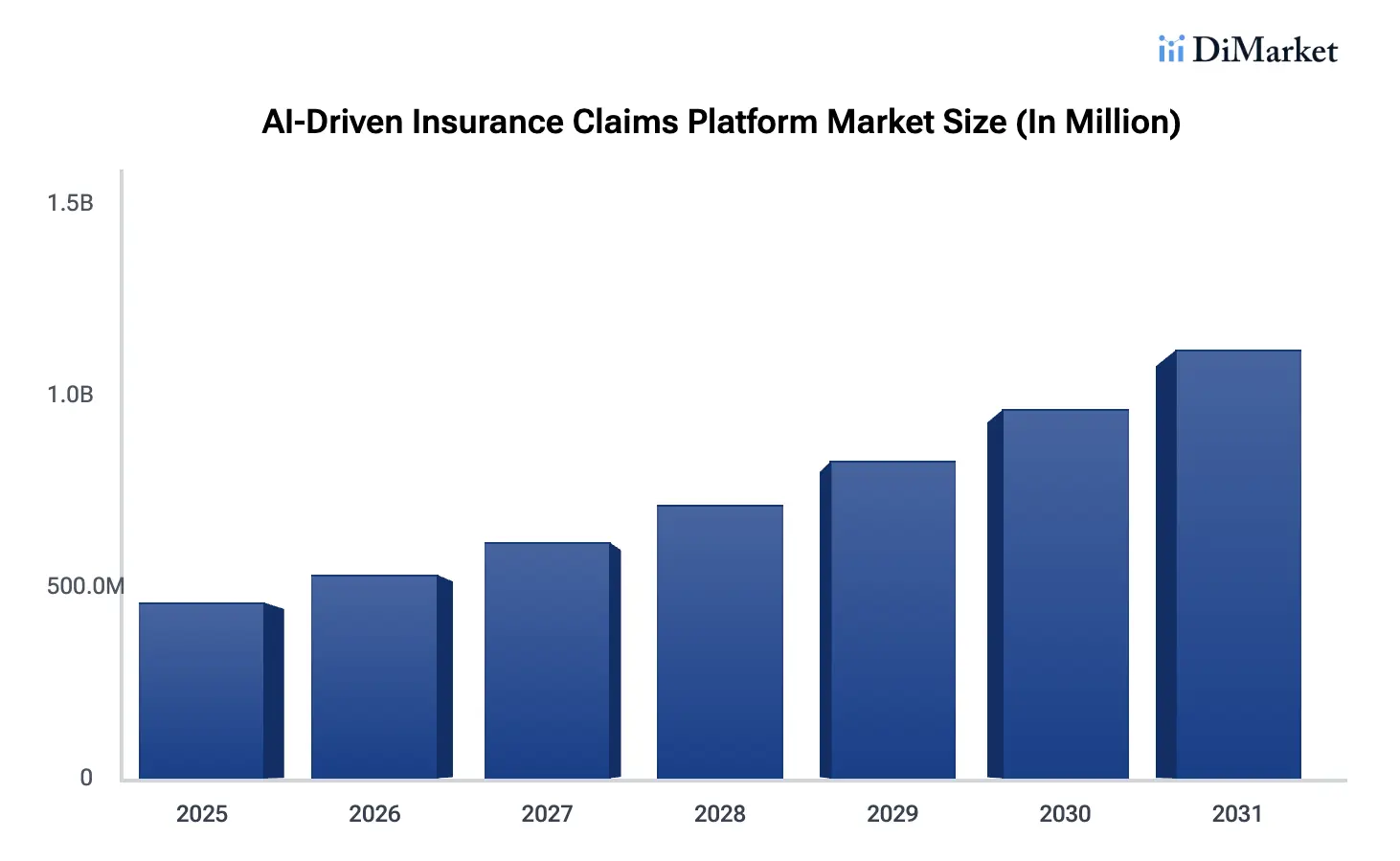
The market reflects that urgency. AI-driven claims platforms were valued at USD 0.46 billion in 2024 and are projected to reach USD 1.29 billion by 2033, growing at a CAGR of 15.9%. Insurers build AI claims intelligence platforms to reduce claim cycle time, detect fraud, improve routing, support adjusters, reduce leakage, and create better customer experiences.
The pressure on insurance claims operations is hitting carriers simultaneously across volume, cost, and customer expectation, and legacy infrastructure is not keeping pace.
1. The Operational Crisis Driving Investment
Claim volumes are rising, operational costs are climbing, and customers now expect digital, real-time claims experiences as standard. AI adoption in insurance consequently jumped from 8% in 2024 to 34% in 2025, as carriers recognized that manual processing could not scale to meet those demands.
Organizations deploying AI are already seeing up to 30% reductions in operational costs, which makes the business case for building proprietary platforms increasingly difficult to ignore.
2. Why Carriers Are Building Instead Of Buying
Off-the-shelf solutions cannot deliver the control that serious claims operations require. Therefore, carriers are choosing to build custom AI platforms to protect three critical assets:
- Proprietary data and algorithms: Claims history, fraud patterns, and risk models are core competitive assets. Building in-house keeps that data fully owned and protected.
- Fraud detection precision: Fraud costs the industry tens of billions annually. Custom platforms allow carriers to tune detection models to their specific risk profiles and claim types.
- Customer experience differentiation: Speed and accuracy in claims processing directly impact retention. Generic solutions cannot match the responsiveness that custom AI infrastructure enables.
3. The Technology Gap In Legacy Systems
Traditional core systems were built before cloud architecture and machine learning existed. As a result, they cannot support real-time predictive analytics, generative AI for document processing, or autonomous claims workflows.
This gap is why carriers like Aviva are partnering with AWS, Microsoft Azure, and Google Cloud to build and scale these platforms.
4. Where AI Claims Intelligence Delivers The Most Value
The highest-impact applications currently driving investment include:
- Claims processing automation: Reduces processing time from days to minutes, representing over 25% of the AI insurance market
- Fraud detection and prevention: Flags suspicious patterns in real time before payments are released
- Automated claims triage: Routes simple claims for instant approval and escalates complex cases for human review
- Claims co-pilot tools: The fastest-growing segment, supporting adjusters with real-time recommendations and structured decision support
With AI insurance spend projected to grow over 25% in 2026, building claims intelligence infrastructure has moved from a strategic consideration to a competitive necessity.
What Is An AI Claims Intelligence Platform?
An AI claims intelligence platform is a software infrastructure that automates, analyzes, and supports the end-to-end claims lifecycle.
It processes claim data, applies policy logic, detects fraud, routes decisions, and supports adjuster workflows using machine learning, document intelligence, and real-time risk scoring across every stage of the claims process.
1. Connects Claim Data, Policy Logic, And Adjuster Workflows
The platform serves as connective tissue between disparate data points and settlement logic. It begins at the First Notice of Loss (FNOL) by ingesting data from various channels.
By applying policy rules against incoming facts, the software determines coverage eligibility in seconds. This flow ensures that stakeholders have a consistent version of the truth.
The system effectively manages several critical inputs:
- Evidence Ingestion: Processing claim documents, images, and repair estimates.
- Records Analysis: Reviewing medical history and payment patterns for settlements.
- Risk Evaluation: Flagging fraud indicators by comparing data against known suspicious patterns.
2. Supports Claims Teams Instead Of Replacing Them
Technology serves to augment human expertise rather than render it obsolete. Complex cases require the nuanced judgment and empathy only a professional provides.
Furthermore, regulatory bodies emphasize that human oversight is essential for maintaining fairness. Insurers remain responsible for ensuring that automated processes avoid unfair discrimination.
The platform handles repetitive tasks, so adjusters focus on high-value investigations. It suggests the next best action based on historical data. This collaborative approach leads to higher job satisfaction and better outcomes. The AI provides the evidence, but the human makes the final call.
How An AI Claims Intelligence Platform Works
The underlying power of this platform lies in its ability to convert chaotic data into a structured workflow. It follows a logical sequence that mirrors a human adjuster but operates at a much higher velocity.
An AI claims intelligence platform works by collecting claim data, extracting documents, checking policy rules, scoring claim risk, detecting fraud patterns, routing cases, and supporting adjuster decisions.
1. Claim Intake And FNOL Capture
The journey starts with a seamless digital experience for the policyholder. Instead of waiting for business hours, customers submit details through mobile apps or chatbots that guide them through the necessary steps.
- Omnichannel Access: Supports mobile FNOL, web forms, and chatbot interactions.
- Initial Triage: Automatically classifies the claim type based on user descriptions.
- Direct Upload: Allows instant submission of photos and vital documents at the scene.
2. Document And Image Intelligence
Once the data arrives, the system uses machine learning to “read” and “see” the evidence. It extracts text from messy invoices and identifies the severity of dents or cracks in photos without manual effort.
- Deep Extraction: Uses OCR and NLP to pull data from medical records and bills.
- Visual Analysis: Employs computer vision for damage detection on vehicles or property.
- Smart Review: Automatically flags discrepancies between repair estimates and actual damage.
3. Policy And Coverage Validation
The platform instantly compares the incident details against the legal fine print. This step ensures that the claim is legitimate under the specific terms of the customer’s contract.
- Rule Application: Checks policy terms, exclusions, and coverage limits.
- Financial Accuracy: Automatically applies deductibles and calculates potential payouts.
- Endorsement Check: Accounts for specific add-ons or modifications to the standard policy.
4. Claim Severity And Risk Scoring
By looking at historical data, the AI predicts how expensive or complex a claim might become. This allows the company to prepare its reserves and prioritize resources effectively.
- Value Prediction: Estimates the total claim cost within minutes of filing.
- Severity Levels: Classifies claims into low, medium, or high-complexity categories.
- Instant Alerts: Triggers escalation logic for high-risk or high-value cases.
5. Fraud And Anomaly Detection
The system acts as a digital watchdog, scanning for patterns that a human might miss. It looks beyond the individual claim to see if there is a broader trend of suspicious activity.
- Pattern Recognition: Identifies suspicious claim patterns and duplicate submissions.
- Cost Control: Flags inflated repair costs that sit outside market norms.
- Network Analysis: Detects anomalies in provider or vendor behavior to stop organized fraud.
6. Adjuster Work Queue Intelligence
In the final stage, the platform ensures the right person is working on the right task. It organizes the daily workload so that nothing falls through the cracks and deadlines are met.
- Smart Routing: Assigns claims based on the specific skill set of the adjuster.
- SLA Management: Tracks timelines to ensure the company meets its service promises.
- Strategic Support: Provides investigation recommendations to help adjusters reach a settlement.
This comprehensive workflow transforms the claims department from a reactive cost center into a proactive unit. Every step is designed to maximize accuracy while keeping the customer experience fast and transparent.
Key Features Of An AI Claims Intelligence Platform
Selecting a platform requires looking beyond basic automation to find deep functional intelligence. The most effective systems act as a comprehensive nervous system for the entire claims organization.
Key features of an AI claims intelligence platform include FNOL automation, document intelligence, fraud detection, claim scoring, policy validation, damage assessment, adjuster copilots, settlement intelligence, and audit dashboards.
1. AI-Powered FNOL Intake
The system captures data across every digital touchpoint to create a unified entry point. It instantly parses information from emails, voice transcripts, and mobile app entries to build a structured record.
By classifying the claim type at the moment of impact, the platform ensures the file follows the correct regulatory path. This reduces initial cycle times from hours to mere seconds.
2. Intelligent Document Processing
Advanced models go beyond simple text extraction to understand the context within complex documents. The platform reads handwritten police reports, multi-page medical bills, and dense repair estimates with high precision.
It connects fragmented data points, such as matching a specific line item in an invoice to a policy exclusion. This capability removes the manual burden of data entry from the adjuster’s desk.
3. Policy Coverage Intelligence
Digital systems cross-reference every claim detail against the active policy ruleset in real-time. The engine evaluates limits and deductibles while checking for specific endorsements that might apply to the incident.
Consequently, the organization avoids the risk of paying for uncovered losses or violating contractual terms. This automation provides a reliable safety net for even the most complex commercial policies.
4. Claim Risk Scoring
The platform assigns a dynamic score to every file based on its severity and financial exposure. It uses historical benchmarks to predict which claims are likely to escalate into litigation or high-value payouts.
Decision makers receive instant alerts for files that deviate from standard risk profiles. Therefore, the enterprise can move from reactive processing to a proactive, risk-adjusted management style.
5. AI Damage Assessment
Computer vision models analyze imagery to provide an objective view of physical or financial damage.
- Auto: Identifying total loss potential by analyzing structural vehicle damage from photos.
- Property: Assessing roof damage or flood impact via satellite or drone imagery.
- Health: Reviewing treatment codes against injury descriptions to flag over-treatment.
- Equipment: Checking sensor data from industrial machinery to validate failure claims.
6. Fraud Detection Engine
The software scans for anomalies that signal organized criminal activity or individual opportunism. It identifies duplicate claims submitted under different names and flags inflated repair costs that exceed market averages.
By performing network analysis, the system uncovers hidden links between providers, claimants, and witnesses. These insights stop financial leakage before the settlement process even begins.
7. Adjuster Copilot
A dedicated digital assistant provides summaries and suggests the next-best action for every open file. It drafts settlement notes and communication templates to ensure consistent messaging across the department.
The copilot reviews thousands of pages of documentation to highlight the most relevant facts for the human handler. This support allows adjusters to manage higher file volumes without sacrificing quality or accuracy.
8. Claims Analytics Dashboard
Executives gain a high-level view of departmental health through a suite of real-time performance metrics.
- Efficiency: Tracking cycle times and claim volumes to identify operational bottlenecks.
- Financials: Monitoring leakage rates, payout trends, and reserve accuracy.
- Performance: Evaluating individual adjuster performance against departmental SLAs.
- Trends: Visualizing fraud rates and emerging risk patterns across different regions.
9. Audit And Explainability Layer
Modern systems must provide a clear trail of how every automated decision was reached. This layer addresses concerns regarding AI hallucinations and bias by ensuring every output is traceable to a specific data source.
Regulatory exposure is minimized because the platform provides the “why” behind every recommendation. Continuous monitoring ensures that the models remain accurate and fair as market conditions evolve.
This suite of features ensures that every decision is backed by data and fully traceable for regulatory compliance. By integrating these tools, an enterprise can significantly reduce operational leakage while improving the policyholder experience.
AI Claims Intelligence Platform Development Process
Building a high-performance intelligence layer requires a structured, multi-phase engineering approach. We focus on creating a system that integrates deeply with your existing operations while ensuring every automated decision is defensible.
AI claims intelligence platform development includes workflow discovery, claims data mapping, AI model planning, system architecture, integration development, testing, compliance setup, and deployment.
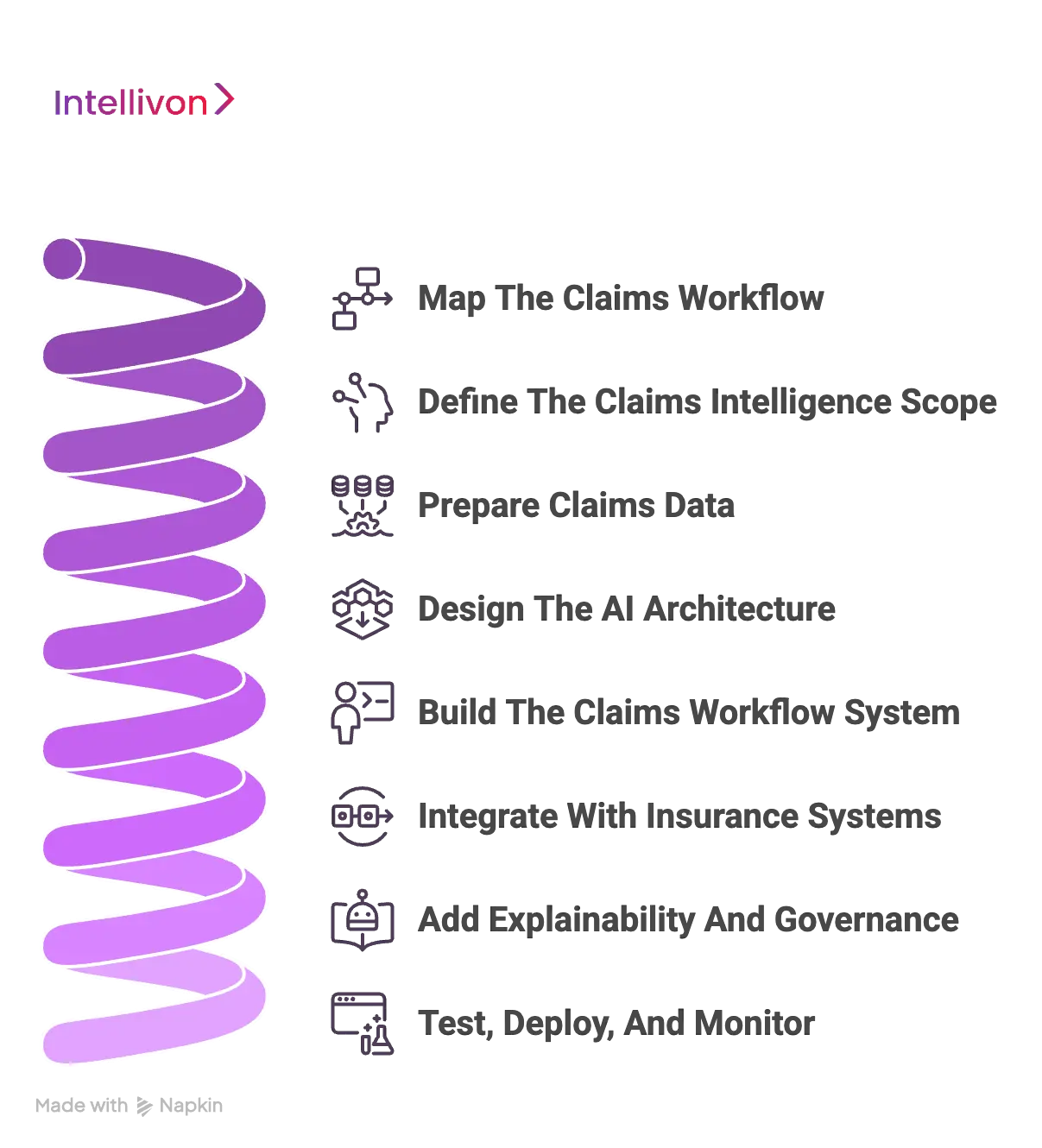
Step 1: Map The Claims Workflow
We begin by deconstructing your current lifecycle to identify every manual touchpoint and decision node. This mapping ensures the AI understands the specific nuances of your departmental logic.
| Workflow Stage | Key Activities | Automation Potential |
| Intake | Data entry, FNOL, initial triage | High (90%+) |
| Verification | Policy check, coverage validation | High (100%) |
| Evaluation | Damage assessment, medical review | Medium (Hybrid) |
| Payment | Reserve setting, fraud check, payout | High (80%) |
- Discovery: We shadow your best adjusters to capture the “tacit knowledge” they use for complex decisions.
- Gap Analysis: Identifying where claims currently languish in the queue allows us to target specific bottlenecks.
- Standardization: We help you unify disparate processes across different lines of business for a cleaner data pipeline.
Step 2: Define The Claims Intelligence Scope
Once the workflow is clear, we define which intelligence modules will drive the most immediate ROI. Most enterprises prioritize fraud intelligence and document extraction to clear high-volume backlogs.
- Priority Ranking: We categorize features into “Essential” for day-one operations and “Advanced” for future scaling.
- Module Selection: You might choose to focus on auto-damage computer vision first before moving into complex medical NLP.
- Resource Planning: Defining the scope helps us align your internal IT and claims experts with our development timeline.
Step 3: Prepare Claims Data
Quality output requires high-fidelity input, so we aggregate diverse datasets from your historical archives. We ingest past claim files, adjuster notes, and payout data to train models on your specific risk appetite.
- Data Cleansing: Removing duplicates and correcting errors in historical records to prevent “garbage in, garbage out” scenarios.
- Labeling: Our experts tag historical claims (e.g., “Fraudulent” or “Total Loss”) to provide a baseline for the AI to learn.
- Aggregation: We bring together structured data from databases and unstructured data like photos, voice recordings, and handwritten notes.
Step 4: Design The AI Architecture
Our architects build a robust pipeline that balances raw processing power with human-centric design. We implement a multi-layered system that handles data ingestion and intelligent processing simultaneously.
| Layer | Component | Function |
| Ingestion | API Gateways | Captures data from mobile apps and web portals |
| Intelligence | NLP & Computer Vision | Reads documents and analyzes photos for damage |
| Reasoning | ML Models | Predicts severity and scores fraud risk levels |
| Control | Rules Engine | Applies strict policy limits and legal constraints |
- Scalability: We use cloud-native microservices so your platform can handle spikes in claims after a major storm or event.
- Modularity: Each engine is independent, allowing you to update your fraud models without touching the document reader.
Step 5: Build The Claims Workflow System
We develop the interface where your team will interact with the AI insights daily. This includes building intuitive dashboards and prioritized work queues that highlight the most urgent files.
- Work Queues: Claims are sorted by urgency and adjuster skill set rather than just by arrival time.
- Notification Engine: Real-time alerts sent via email or internal messaging for high-priority escalations.
- Role-Based Access: Ensuring that only authorized personnel can view sensitive medical or financial records.
Step 6: Integrate With Insurance Systems
A platform is only as good as its connectivity, so we ensure seamless data flow across your entire tech stack. We build secure API integrations with your core insurance platforms and CRMs.
- Core Connectivity: Deep integration with Guidewire, Duck Creek, or custom legacy mainframes.
- Third-Party Data: Connecting to ISO ClaimSearch, police databases, or medical provider networks.
- Payment Orchestration: Linking to financial systems for automated EFT or check issuance once a claim is approved.
Step 7: Add Explainability And Governance
We treat regulatory compliance as a core feature rather than an afterthought. Following NAIC guidelines, we build in documentation and testing frameworks that keep you in control of every algorithmic decision.
- The “Why” Factor: For every automated decision, the system generates a human-readable explanation for adjusters.
- Bias Mitigation: We run regular audits to ensure the AI does not develop unfair patterns based on demographic data.
- Governance Frameworks: Establishing clear protocols for when a human must override an AI recommendation.
Step 8: Test, Deploy, And Monitor
Before going live, we conduct rigorous testing for model accuracy and system performance. We monitor false positive rates in fraud detection to ensure legitimate customers are not inconvenienced.
- User Acceptance Testing (UAT): Real adjusters test the system to ensure the interface is intuitive and helpful.
- Performance Monitoring: Tracking system uptime and API response times during peak load simulations.
- Iterative Training: We continue to feed new data into the system post-launch to keep accuracy levels high as market trends change.
This rigorous development process ensures your platform is not just a tool, but a strategic asset. By following this roadmap, we deliver a solution that scales with your growth and withstands regulatory scrutiny.
AI Models Used In Claims Intelligence Platforms
Modern claims platforms rely on a sophisticated stack of specialized models working in unison. Each model addresses a specific data type to ensure no detail remains hidden during the evaluation process.
AI claims intelligence platforms use NLP, OCR, computer vision, predictive analytics, anomaly detection, rules engines, and generative AI to support claims decisions.
1. NLP For Claim Notes And Documents
Natural Language Processing allows the system to understand the human element within a file. It processes unstructured text to identify the core facts of an incident without requiring a manual read-through.
- Summarization: Condensing hundreds of pages of adjuster notes into a concise situational overview.
- Classification: Categorizing documents automatically based on their linguistic content.
- Extraction: Identifying specific policy language or legal clauses that impact the current claim.
- Sentiment Analysis: Detecting potential claimant frustration or litigation risk through written communication.
2. OCR For Document Extraction
Optical Character Recognition serves as the foundation for digital data entry. It converts static images of documents into searchable and editable data points that the platform can analyze.
- Financial Documents: Reading and validating line items within invoices and repair estimates.
- Medical Records: Extracting treatment codes and dates from complex hospital bills.
- Official Reports: Parsing police reports and claim forms to populate core database fields.
- Accuracy Checks: Comparing extracted data against known templates to ensure 100% fidelity.
3. Computer Vision For Damage Assessment
This technology provides the “eyes” of the platform by analyzing visual evidence submitted via photos or video. It objectively measures physical loss to provide a baseline for financial settlements.
- Auto & Property: Identifying specific parts that require repair or replacement based on impact patterns.
- Roofing: Utilizing drone or satellite imagery to detect hail or wind damage across large areas.
- Equipment: Monitoring industrial machinery for signs of wear or sudden failure.
- Quality Control: Automatically rejecting blurry or fraudulent photos that do not meet evidentiary standards.
4. Predictive Analytics For Claim Severity
By looking at historical trends, these models forecast the eventual cost and complexity of a new submission. This foresight allows leadership to manage reserves and staff workloads more effectively.
| Model Goal | Data Inputs | Output |
| Payout Prediction | Past settlements, market rates | Estimated total claim cost |
| Complexity Scoring | Injury types, legal involvement | Difficulty rating (1-10) |
| Litigation Risk | Claimant behavior, attorney history | High/Low alert for legal suit |
5. Anomaly Detection For Fraud
This proactive engine searches for outliers that deviate from standard human or business behavior. It acts as a shield for the company’s capital by identifying bad actors early in the lifecycle.
- Pattern Recognition: Spotting organized groups that file similar claims across different regions.
- Duplicate Detection: Flagging multiple submissions for the same incident or identical photos used in different files.
- Vendor Monitoring: Identifying repair shops or providers that consistently submit inflated estimates.
- Network Analysis: Visualizing hidden connections between claimants, witnesses, and service providers.
6. Generative AI For Adjuster Support
Generative models serve as a high-level assistant that handles the heavy lifting of content creation. This technology allows adjusters to focus on the final decision while the AI handles the documentation.
- Communication: Drafting professional and empathetic messages to policyholders during stressful times.
- Settlement Notes: Creating detailed justifications for payout amounts based on the gathered evidence.
- Checklists: Generating customized investigation steps based on the unique facts of the claim.
- Warning: Generative AI is a supportive tool and must never make final claim decisions autonomously. Human governance is mandatory to prevent bias and ensure legal accountability.
The integration of these models creates a comprehensive intelligence layer that enhances every aspect of the claims process. By utilizing the right tool for each data type, the platform remains accurate, fast, and reliable.
How Much Does It Cost To Develop An AI Claims Intelligence Platform?
Understanding the financial commitment is vital for any enterprise looking to modernize its claims infrastructure. While costs vary based on complexity, the following estimates provide a clear roadmap for strategic budgeting.
The cost to develop an AI claims intelligence platform usually ranges from $50,000 to $200,000, depending on AI scope, integrations, data quality, and compliance needs.
| Platform Scope | Estimated Cost | Best For |
| AI Claims MVP | $50,000–$80,000 | Targeted automation or proof of concept |
| Mid-Level Intelligence | $80,000–$140,000 | Growing insurers, TPAs, and brokers |
| Enterprise Infrastructure | $140,000–$200,000 | Multi-region carriers and complex workflows |
The final price tag depends on several critical factors beyond just software development. High-quality data preparation and the number of legacy system integrations often influence the total investment.
Additionally, the specific depth of the fraud detection engine and the complexity of the policy rules will dictate the engineering hours required.
Scaling the system for thousands of daily claims also adds infrastructure costs. Therefore, starting with a well-defined MVP allows leaders to prove value before expanding.
Cost By Feature
| Feature | Estimated Cost |
| FNOL Intake System | $8,000–$15,000 |
| Document Intelligence | $12,000–$25,000 |
| Policy Coverage Validation | $10,000–$20,000 |
| Claim Risk Scoring | $15,000–$30,000 |
| Fraud Detection Engine | $20,000–$40,000 |
| Adjuster Copilot | $15,000–$30,000 |
| Analytics & Audit Layer | $10,000–$20,000 |
Investing in these modular components ensures that your capital is directed toward the features with the highest impact. This structured approach allows your organization to build a scalable, future-proof asset that pays for itself through reduced leakage.
Build A Claims Intelligence Platform That Adjusters Actually Use
Technology often fails in the insurance sector because it adds more screens rather than solving actual problems. A successful platform must prioritize the human experience to ensure the frontline team embraces the new tools.
A usable claims intelligence platform should reduce adjuster workload, explain recommendations, prioritize urgent claims, summarize documents, and keep humans in control.
1. Keep The Workflow Inside Existing Claims Operations
Forcing adjusters to toggle between different software windows disrupts their focus and slows down the entire process. The intelligence layer should ideally live inside your core claims system as a native extension.
By embedding AI insights directly where the adjuster already works, you reduce friction and increase the speed of adoption.
- Integrated UI: Displays risk scores and document summaries within the standard claim view.
- Direct Sync: Updates the core system records automatically without manual copy-pasting.
- Minimal Training: Leverage familiar interfaces to shorten the learning curve for staff.
2. Show Why AI Flagged A Claim
Adjusters are naturally skeptical of “black box” decisions that do not explain the underlying logic. The system must provide clear evidence for why it categorized a claim as high-risk or potentially fraudulent.
When a professional understands the specific risk factors involved, they are much more likely to trust the system’s output.
3. Let Adjusters Accept, Reject, Or Override AI Suggestions
Insurance remains a field where human judgment is the final authority for complex cases. The platform should empower adjusters by giving them the final say on any automated recommendation.
Tracking these overrides provides an invaluable feedback loop that helps the engineering team refine the machine learning models.
| User Action | Purpose | Long-term Benefit |
| Accept | Confirms AI accuracy | Validates the current model logic |
| Reject | Flags a false positive | Prevents future errors in similar cases |
| Override | Adds human nuance | Captures “tacit knowledge” for training |
4. Reduce Administrative Work First
The fastest way to win over a skeptical team is to remove the tasks they dislike the most. Start by automating document extraction, summarizing long medical histories, and routing simple files instantly.
When adjusters see that the AI handles the “busy work,” they will view the platform as a partner rather than a replacement.
5. Track Adoption Metrics
Success is measured by how often the tools are used to make better, faster decisions. We monitor specific key performance indicators to ensure the platform is delivering real-world value to the team.
- Usage Rates: Measuring how many adjusters actively use the AI insights daily.
- Override Frequency: Identifying if certain models are consistently being corrected by humans.
- Cycle Time: Tracking the reduction in time from FNOL to final settlement.
- Productivity: Observing the increase in file volume handled by each adjuster without added stress.
Focusing on these adoption drivers ensures that your investment results in a more efficient and satisfied workforce. A platform that adjusters love is a platform that delivers a massive return on investment.
Compliance For AI Claims Intelligence Platforms
Regulatory scrutiny in the insurance sector is intensifying as automation becomes the industry standard. A robust governance framework ensures that your platform remains a strategic asset rather than a legal liability.
AI claims platforms need governance controls for explainability, fairness, privacy, security, audit logs, model monitoring, human oversight, and third-party AI risk.
1. Human Oversight
The most critical safeguard is maintaining a “human-in-the-loop” architecture for high-stakes decisions. AI should act as a sophisticated recommendation engine that surfaces the most relevant data for an adjuster.
This ensures that the final authority for settlement or denial remains with a qualified professional. This approach satisfies regulatory requirements while preserving the empathy necessary for complex claimant interactions.
2. Explainable AI
Transparency is non-negotiable when an algorithm influences financial outcomes. Every claim score or risk flag must be accompanied by visible reasons that a human can easily interpret.
If a system identifies a high probability of fraud, it must highlight the specific data points that triggered the alert. Consequently, your team can defend its decisions during internal audits or external regulatory inquiries.
3. Bias And Fairness Testing
Algorithms can inadvertently pick up historical biases present in training data. We implement rigorous testing protocols to ensure that outcomes remain fair across all protected groups and claim categories.
- Outcome Audits: Regularly reviewing settlement trends to identify any unintended disparities.
- Data Masking: Preventing sensitive demographic variables from influencing the core decisioning logic.
- Parity Checks: Comparing AI performance across different regions to ensure consistent application of policy rules.
4. Audit Logs
A comprehensive digital paper trail is essential for both accountability and continuous improvement. The platform must track who reviewed, approved, or overrode every AI-generated suggestion.
These logs provide a clear history of the decision-making process for every individual file. Therefore, leadership can identify training gaps or system errors before they escalate into systemic issues.
5. Data Security
Protecting sensitive policyholder information is the foundation of customer trust. We utilize enterprise-grade encryption for all claim documents, medical records, and payment data.
- Encryption: Securing data both at rest and during transit across the platform.
- Access Control: Limiting data visibility based on specific adjuster roles and seniority.
- Compliance Standards: Aligning the infrastructure with SOC2, GDPR, or HIPAA requirements where applicable.
6. Third-Party AI Risk
Modern platforms often rely on a network of external APIs and vendor models. It is vital to maintain a central registry that tracks the performance and documentation of these third-party components.
We conduct regular testing of external inputs to ensure they meet your internal standards for accuracy and reliability. This oversight prevents “upstream” errors from compromising your internal claims intelligence.
By prioritizing these governance pillars, you build a platform that is as ethical as it is efficient. This level of rigor transforms compliance from a hurdle into a competitive advantage.
Conclusion
Transitioning to an AI claims intelligence platform is a strategic pivot toward long-term operational resilience. It allows your enterprise to eliminate processing bottlenecks while maintaining the human oversight essential for fair settlements.
This technology does not just save costs; it transforms the claimant experience and protects your capital through advanced risk detection. Adopting these intelligent systems today ensures your organization remains a leader in an increasingly data-driven insurance landscape.
Build AI Claims Intelligence Platforms With Intellivon
At Intellivon, we build AI claims intelligence platforms for insurers, TPAs, insurtech companies, brokers, health claims platforms, P&C carriers, and enterprise insurance teams.
Our engineering approach connects document intelligence, claim risk scoring, fraud detection, damage assessment, policy validation, adjuster copilots, analytics dashboards, and secure integrations into one claims decision infrastructure.
This helps your team reduce manual review, improve claim routing, detect high-risk cases earlier, and make claims operations easier to monitor.
A. Define The Right Claims Intelligence Scope
Intellivon helps you define the right build scope before development begins. We study your claim types, insurance lines, operational bottlenecks, data sources, user roles, and business goals to decide what should be built first.
This includes:
- MVP planning for focused claims intelligence validation
- AI module selection for fraud, routing, or document review
- Insurance line mapping for health, auto, property, or specialty claims
- Claims workflow discovery across intake, review, settlement, and closure
- Product roadmap planning for claims SaaS platforms
- Enterprise modernization planning for legacy claims systems
This approach helps you avoid overbuilding, reduce development risk, and invest first in the claims workflows that create measurable operational value.
B. Build AI Workflows Around Real Claims Operations
Intellivon builds AI workflows around how claims teams actually work. We design systems that capture claim details, process documents, score risk, flag fraud indicators, prioritize adjuster queues, and support settlement decisions with clear context.
We build workflows for:
- FNOL intelligence to classify and route claims faster
- Document processing for invoices, reports, forms, and evidence files
- Fraud scoring based on patterns, anomalies, and claim history
- Claim severity prediction for better prioritization and reserve planning
- Adjuster work queues based on risk, urgency, value, and complexity
- Settlement support with summaries, recommendations, and review notes
This helps your platform move beyond basic claims automation. It gives claims teams the intelligence they need to review cases faster and make better decisions with human oversight.
C. Make Claims AI Explainable, Secure, And Scalable
Intellivon designs AI platforms with governance-ready architecture. We create systems that protect sensitive claim data, show clear AI reasoning, track human decisions, and support long-term model performance.
Our approach includes:
- Role-based access for adjusters, managers, investigators, and admins
- Audit logs to track reviews, decisions, overrides, and system actions
- Model monitoring to measure accuracy, drift, and decision quality
- Explainable AI outputs that show why a claim was flagged or scored
- Human-in-the-loop controls for sensitive or high-value claim decisions
- Secure cloud deployment for scalable claims operations
This helps your claims intelligence platform stay reliable as claim volume grows, workflows expand, and more teams depend on AI-supported decision-making.
If you are planning to develop an AI claims intelligence platform, contact Intellivon to define your build scope, estimate development cost, and create a claims system designed for real insurance operations.
Common Queries
Q1. Can AI replace human claims adjusters?
A1. An AI claims intelligence platform should support claims teams, not replace them. It can summarize documents, score claim risk, flag fraud indicators, recommend next actions, and route simple cases faster. However, complex coverage, liability, negotiation, litigation, and settlement decisions should still stay under licensed human review and audit control.
Q2. What should insurers automate first in claims intelligence?
A2. The best starting module depends on your biggest claims bottleneck. Many insurers begin with document intelligence, FNOL triage, fraud scoring, or adjuster work queue automation. These modules reduce manual review quickly, prove value faster, and create clean operational data before expanding into settlement intelligence, reserve recommendations, and full claims decisioning.
Q3. Can AI detect fake evidence and fraudulent claims?
A3. Yes, but only when the platform combines image checks, metadata review, fraud rules, historical patterns, and human investigation. AI can flag duplicate photos, suspicious damage evidence, manipulated documents, unusual claim timing, and provider anomalies. It should not reject claims automatically. It should help SIU teams review risky cases much faster.
Q4. How do insurers keep AI claims decisions safe?
A4. A safe claims intelligence platform needs explainable AI outputs, human-in-the-loop review, role-based access, audit logs, override tracking, data privacy controls, and model monitoring. These controls help insurers understand why a claim was flagged, who reviewed it, what changed, and whether the AI is creating biased or inaccurate claim outcomes later.