Key Takeaways:
-
AI RCM predicts claim risk before submission, flags coding gaps, detects underpayments, and prioritizes work queues by recovery potential.
-
Diagnosing the specific revenue leak, whether denials, coding errors, or underpayments, must happen before choosing AI features.
-
Payer-aware logic with denial pattern learning, contract variance detection, and authorization rule mapping separates effective AI RCM from generic billing software.
-
Build costs range from $50,000 for an MVP to $200,000 and above for an enterprise platform with payer integrations and compliance controls.
-
How Intellivon builds AI RCM platforms your enterprise fully owns, with payer-aware automation, denial prediction, and secure integrations from day one.
Healthcare revenue teams are under immense pressure with their current billing systems because of rising denials, stretched-out payer timelines, and undetected underpayments. The financial impact corrodes across every stage as these trends begin to compound over time.
Traditional RCM software organizes the billing workflow. However, it largely reacts after claims are submitted, denials are returned, and revenue has already been lost. That lag is where the real cost lives.
However, an AI RCM software changes the approach entirely. It predicts claim risk before submission, flags documentation gaps during coding, assists coders in real time, detects underpayments after adjudication, and prioritizes work queues based on recovery potential. As a result, revenue teams spend less time firefighting and more time on decisions that actually move collections forward.
Building this kind of software, however, requires careful planning. Mistakes in AI RCM development do not just affect efficiency. Instead, they affect reimbursement accuracy, regulatory compliance, and patient billing integrity. The architecture, data pipelines, and workflow integrations must be scoped correctly from the start. This blog covers how to plan, scope, build, test, and scale AI RCM software that performs in real healthcare environments.
Why Adoption Of AI RCM Platforms Is Booming Right Now
Healthcare organizations are accelerating the adoption of AI-powered RCM platforms as claim denials climb, staffing gaps widen, and reimbursement timelines stretch against rising operational costs. The financial pressure is real, and health systems are responding by investing in infrastructure that can keep up.
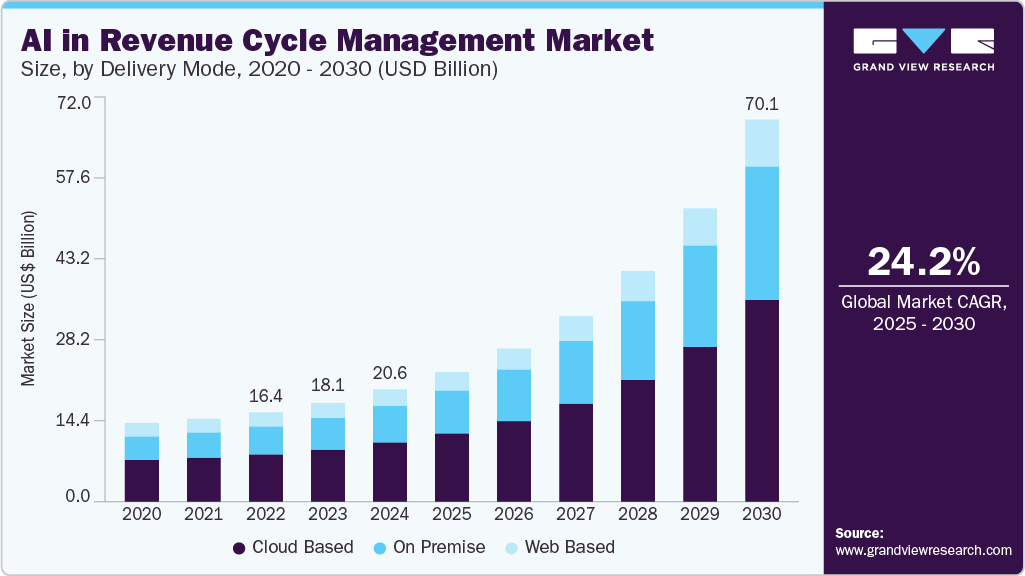
Adoption Trends
AI adoption in revenue cycle management has moved well past the experimentation stage. Around 46% of health systems now use AI within their RCM operations, and an additional 40% are actively running pilots focused on coding assistance, claims review, and denial management. The shift is deliberate, with organizations prioritizing the areas where revenue leakage is most visible and most recoverable.
Hospitals currently hold the largest share of AI RCM adoption, accounting for approximately 45% of market revenue. Payers, however, are growing the fastest, expanding at a CAGR of 27.68% as automated adjudication becomes central to how insurers process and settle claims at scale.
Investor confidence is following that momentum. Waystar’s USD 968 million IPO and strategic acquisitions, such as those executed by R1 RCM, signal that the market views AI-powered revenue cycle infrastructure as a long-term growth category, and not a transitional experiment.
What is an AI Revenue Cycle Management Software?
AI revenue cycle management software is a healthcare financial platform that uses AI to manage, automate, and optimize the full billing and reimbursement cycle. It covers every stage from patient registration and insurance verification through coding, claims submission, denial management, payment posting, and collections.
Traditional RCM software follows fixed rules. AI RCM software, however, learns from payer behavior, claim outcomes, and coding patterns to make smarter decisions at each stage. It can predict which claims are likely to be denied before submission, flag documentation gaps during coding, detect underpayments after adjudication, and prioritize work queues based on recovery potential.
The result is a system that does not just organize billing workflows. It actively reduces revenue leakage, shortens reimbursement timelines, and gives financial teams the visibility they need to make faster, more accurate decisions.
Build AI RCM Software vs Add AI To Existing RCM
Choosing the right technical path is the most critical hurdle for stakeholders in the healthcare financial space. Many leaders struggle to decide between building a ground-up platform or enhancing their current infrastructure with intelligent modules.
| Feature | Custom AI RCM Software | AI Add-On Module | Legacy Modernization |
| Development Time | 9 to 18 Months | 3 to 6 Months | 6 to 12 Months |
| Initial Cost | High Investment | Moderate | Strategic Reallocation |
| Control | Full Proprietary Logic | Limited by Host System | High Process Control |
| Best For | New SaaS or High Volume | Targeted Efficiency | Stabilizing Operations |
1. When Full Custom AI RCM Software Makes Sense
Founding a new platform is ideal when current billing workflows are unique. Standard software often fails to account for specific payer rules that cause high denial rates.
Revenue leakage is frequently spread across too many disconnected manual steps. A custom build allows for the design of specific work queues for the administrative team.
- Proprietary Value: Enables the launch of a unique SaaS product.
- Deep Integration: Connects directly with EHRs and clearinghouses without middleware.
- Tailored Logic: Supports specialized payer rules that generic tools ignore.
This path provides the highest level of financial intelligence. It ensures long-term competitive differentiation for the enterprise.
2. When An AI Add-On Module Is Enough
A stable billing engine might only require specific enhancements. An add-on module works best for targeted problems like denial prediction or automated medical coding.
There is no need to replace the entire ecosystem to see a major impact. This route offers a much faster deployment timeline.
- API Connectivity: Links easily through standard data exports.
- Risk Mitigation: Lowers the chance of operational downtime during rollout.
- Cost Efficiency: Provides a high return on investment without massive overhead.
The AI layer adds intelligence while keeping familiar interfaces. It is a strategic way to test machine learning in a live environment.
3. When Legacy RCM Modernization Is The Better Route
Established organizations often rely on old systems that manage core tasks well. However, these systems frequently force teams to use manual spreadsheets. Modernization is the right choice when data quality is poor or integrations are limited.
- Performance Wrap: Places a modern API layer over existing databases.
- Real-time Access: Provides the analytics that legacy platforms usually lack.
- Error Reduction: Stabilizes the foundation before moving to full automation.
This approach balances the need for innovation with the reality of technical debt. It allows the business to scale without losing historical data.
4. When Buying A Ready-Made RCM Tool Is Safer
A standard off-the-shelf tool sometimes meets every basic requirement. This is the safest route if billing workflows follow industry norms exactly. It is the best choice when the development budget is strictly limited. Fast deployment often matters more than having unique proprietary features.
- Standardization: Aligns with common clearinghouse and payer formats.
- Low Maintenance: Removes the burden of managing a software team.
- Proven Logic: Uses existing industry benchmarks for performance.
It allows a focus on operations rather than software engineering. Proprietary AI logic is not always a requirement for profitability.
5. How To Decide The Right Development Path
The final decision requires a hard look at current denial rates. High manual workloads usually indicate that a custom or modernized solution is necessary. Long-term goals for product ownership must also be evaluated.
- Current Performance: Analysis of the current denial and leakage rates.
- Growth Targets: Assessment of future volume and scalability needs.
- Resource Availability: Review of the internal technical and financial budget.
Consider compliance requirements and the amount of available training data. The choice must balance the immediate budget against the potential for future revenue growth.
Choose The Right AI RCM Software Product Model
AI RCM software can be developed as an internal provider system, SaaS product, billing company platform, AI add-on, or enterprise automation layer.
The choice of a product model dictates every technical decision from the database schema to the user interface. Therefore, stakeholders must align the software architecture with their specific business goals early in the process.
1. Internal AI RCM Software For Hospitals And Clinics
These systems are built specifically for the unique revenue workflows of a single organization. The primary goal is to improve staff productivity and track revenue leakage in real time.
Because the tool is internal, it integrates deeply with the existing practice management systems. Consequently, the finance team gains a clear view of the entire collection process.
- Custom Dashboards: Displays financial health metrics for internal billing teams.
- Provider Reporting: Tracks performance across multiple clinical locations.
- Process Visibility: Monitors how quickly staff resolve outstanding claims.
This model is best for hospitals and large diagnostic centers. Furthermore, it serves specialty clinics and enterprise healthcare groups that want total control over their data.
2. AI RCM SaaS For Healthcare Companies
A SaaS model requires a multi-tenant architecture to support many different clients on one platform. Developers must build a scalable cloud infrastructure that handles subscription management and provider onboarding.
Additionally, the software should track usage-based AI workflows for billing purposes. This ensures the platform stays profitable as it grows.
- Scalable Core: Supports rapid growth for many different healthcare clients.
- Product Analytics: Provides insights into how users interact with the tool.
- Onboarding Flows: Streamlines the setup process for new digital health companies.
This path is ideal for healthtech founders and healthcare SaaS startups. It is also the right choice for RCM product companies looking to enter the market.
3. AI RCM Platform For Billing Companies
Medical billing companies need a platform that manages multi-client claim queues effectively. The software must handle client-specific payer rules while tracking staff assignments and productivity.
Therefore, the system includes robust service level agreement tracking. This helps the business maintain high trust with its clients.
- Client Portals: Provides transparent reporting for the billing company’s customers.
- Recovery Workflows: Streamlines the process of contesting denied claims.
- SLA Dashboards: Ensures the team meets its contractual performance targets.
Consequently, this model is best for RCM service providers and revenue cycle BPOs. It empowers outsourced billing teams to work more efficiently across diverse accounts.
4. AI Add-On For Existing Healthcare Software
Sometimes the most strategic move is to build a specialized intelligence layer. This AI add-on connects to existing EHR or practice management software through APIs.
It provides specific functions like claim risk scoring or denial prediction without replacing the host system. This approach allows for a faster rollout.
- Coding Support: Assists human coders by suggesting the most accurate ICD-10 codes.
- Underpayment Detection: Identifies when payers underpay based on contract terms.
- Intelligence API: Delivers predictive insights to other healthcare software platforms.
This model is excellent for EHR vendors and billing software providers. Consequently, it allows them to add modern AI features to their current product offerings.
5. AI Automation Layer For Enterprise RCM Teams
An automation layer works on top of existing tools to eliminate repetitive tasks. It connects payer portals and claim queues to speed up manual workflows.
This approach is beneficial because it supports staff without requiring a full system replacement. It serves as a bridge between legacy systems and modern efficiency.
- Repetitive Task Automation: Handles data entry and payment posting automatically.
- Portal Integration: Aggregates data from various payer websites into one view.
- Rapid Adoption: Minimizes training time since the core systems remain the same.
This strategy is best for enterprises with high manual workloads. It is also perfect for hospitals that want to avoid the risks of a major platform migration.
The product model decides the architecture and the total development cost. Selecting the right model ensures that the AI roadmap supports the long-term business vision.
Turn Revenue Cycle Operations Into Software Requirements
AI RCM software requirements should come from real revenue cycle workflows, including patient access, eligibility, authorization, coding, claims, denials, payments, and reporting.
Translating complex billing tasks into functional software specifications is the foundation of a successful build. Each stage of the revenue cycle requires specific data inputs and logic to ensure the AI RCM software delivers measurable value.
1. Patient Access Requirements
The initial point of contact sets the stage for the entire financial outcome. Therefore, the software must prioritize accurate data capture during the registration process. This includes advanced duplicate patient detection to prevent fragmented records.
- Insurance Capture: Systems need to digitize and validate insurance cards instantly.
- Demographic Alerts: The platform should flag missing or incorrect address information immediately.
- Responsibility Estimation: Providing patients with clear cost estimates based on their specific plan.
Effective patient access workflows reduce front-end errors that lead to later denials. Consequently, the system must link appointments directly to financial tasks for better visibility.
2. Eligibility And Benefits Requirements
Real-time verification is a non-negotiable requirement for modern healthcare platforms. The software must communicate with payers to confirm coverage status before any service is rendered. This prevents the provider from performing non-reimbursable work.
- Benefit Visibility: Displaying co-pays and remaining deductibles for the staff.
- Mismatch Detection: Highlighting discrepancies between provided info and payer records.
- Task Creation: Generating a follow-up action if coverage appears inactive or expired.
Maintaining detailed payer response logs is also essential for auditing purposes. These logs prove that the organization performed due diligence before starting treatment.
3. Prior Authorization Requirements
Managing authorizations is often the most labor-intensive part of the revenue cycle. Therefore, the software requires a robust rule engine to detect which procedures need prior approval. This prevents the clinical team from proceeding without a valid authorization number.
- Document Checklists: Listing the exact clinical notes required for each specific payer.
- Status Tracking: Monitoring the progress of submitted requests until they are approved.
- Expiry Alerts: Warn the team if an authorization is about to expire before the procedure.
Capturing denial reasons at this stage is also critical for long-term improvement. It helps the organization map out payer-specific rules more accurately over time.
4. Coding And Charge Capture Requirements
The software must bridge the gap between clinical documentation and financial billing. This requires a deep understanding of ICD-10 and CPT code sets. The system should review clinical charts to find any missing charges that were not captured manually.
- Modifier Validation: Ensuring that modifiers are applied correctly to avoid simple rejections.
- Medical Necessity: Checking if the documented diagnosis supports the billed procedure.
- Coder Approval: Providing a workflow where human experts can review and finalize AI suggestions.
Automated charge capture ensures that every service is accounted for correctly. Consequently, this reduces the risk of compliance issues during external audits.
5. Claims And Denial Requirements
Submitting clean claims is the primary goal of any RCM platform. Therefore, the software must include a claim scrubbing engine with payer-specific edits. This engine acts as a final filter before the claim reaches the clearinghouse.
- Risk Scoring: Assigning a probability score to each claim based on historical patterns.
- Denial Classification: Automatically sorting denials into categories like “Technical” or “Clinical.”
- Appeal Workflows: Generating the necessary documents to contest a denial quickly.
Scoring the probability of recovery helps teams focus on the most valuable claims first. This strategic approach ensures that resources are not wasted on low-value appeals.
6. Payment Posting And Reconciliation Requirements
The software must handle the complex task of parsing electronic remittance advice files. This ensures that payments are applied to the correct patient accounts without manual entry. Furthermore, the system should automatically check for any contract variances.
- Adjustment Mapping: Converting cryptic payer codes into readable descriptions for the finance team.
- Underpayment Detection: Flagging any payment that falls below the agreed-upon contract rate.
- Accounting Sync: Pushing finalized payment data directly into the general ledger.
Effective reconciliation keeps the financial records accurate and up to date. It also provides a clear view of the actual cash flow versus the expected revenue.
7. Patient Billing And Collection Requirements
Patient responsibility is a growing portion of total healthcare revenue. Therefore, the software must offer a seamless experience for patients to settle their balances. This includes sending digital payment links directly to their mobile devices.
- Installment Plans: Allowing patients to set up automated monthly payments for high balances.
- Reminder Automation: Sending gentle triggers before a payment becomes overdue.
- Collection Scoring: Identifying which accounts are most likely to pay without intervention.
Maintaining detailed communication logs ensures that the staff can resolve disputes efficiently. A transparent billing process builds trust and improves the overall collection rate.
A strong AI RCM product does not start with generic features. It starts by converting every step of the revenue operations into clear software requirements.
Decide What AI Should And Should Not Automate
AI RCM software should automate low-risk tasks first, support medium-risk decisions with review, and require human approval for high-risk billing and coding actions.
Strategic automation requires a clear understanding of the risks associated with every billing decision. Successful founders do not try to automate every task immediately. Instead, they build a tiered system that protects the organization from compliance errors and financial loss.
1. Low-Risk AI Automation Areas
Low-risk tasks are the most logical starting point for any AI RCM software project. These features focus on data organization and alerting rather than final decision-making. They act as a digital assistant that helps the staff work faster without changing the underlying claim data.
- Eligibility Alerts: Flagging when a patient’s insurance does not match the provider records.
- Missing Fields: Highlighting blank spots in a claim form before it moves to the next stage.
- Work Prioritization: Sorting the daily task list so the team tackles high-value claims first.
These areas are safer because they support human decisions rather than replacing them. Consequently, they reduce manual labor while maintaining a high level of oversight. They provide immediate dashboard insights that help leaders understand the current state of operations.
2. Medium-Risk AI Automation Areas
Medium-risk automation involves predictive modeling and scoring. These tools help the team identify patterns that a human might miss. However, the results still require a final look by a professional to ensure the logic holds up in a real-world scenario.
- Denial Prediction: Using historical data to guess which claims might be rejected.
- Payment Forecasting: Estimating when the cash will actually hit the bank account.
- Recovery Probability: Scoring which denied claims are worth the time and effort to appeal.
These features require specific controls like confidence scores and exception handling. Therefore, the system must provide a review queue for any prediction that falls below a certain threshold. Performance tracking and manual overrides ensure the model stays accurate over time.
3. High-Risk AI Automation Areas
High-risk areas involve actions that directly impact the legal and financial standing of the organization. Because these tasks involve coding and payer communication, they require the highest level of scrutiny. Mistakes here can lead to audits or accusations of fraudulent billing.
- Coding Suggestions: Recommending ICD-10 or CPT codes based on clinical notes.
- Appeal Generation: Drafting the legal text for a claim reconsideration.
- Authorization Submissions: Directly sending requests to payers for procedure approval.
Every high-risk action must include detailed recommendation explanations. The software should maintain a version history for every change made by the AI. Furthermore, a compliance review stage is essential to ensure every submission meets current regulatory standards.
4. Where Human Approval Is Non-Negotiable
Certain financial and legal decisions should never be left entirely to an algorithm. Human expertise is vital for complex situations that require nuanced judgment or ethical considerations. This ensures that the organization remains accountable for its most sensitive actions.
- Financial Write-offs: Deciding when to stop pursuing a debt and take a loss.
- Final Claim Edits: Correcting a claim right before it is officially submitted.
- Contract Recovery: Taking formal action against a payer for systemic underpayment.
Human approval is also necessary for any compliance-sensitive recommendations. This layer of protection builds trust with both the internal staff and the external payers. It ensures that the software remains a tool for humans rather than a replacement for them.
5. How To Build Confidence Thresholds
Confidence thresholds allow the software to route tasks based on the certainty of the AI output. High-confidence results can move through the system with minimal intervention. Conversely, low-confidence outputs are escalated to a senior manager for a deep dive.
- Auto-Routing: Moving certain claims forward when the AI is 99% sure of the data.
- Staff Review: Sending tasks to a junior member when the confidence is moderate.
- Escalation: Alerting a specialist when the AI is confused by a complex case.
Tracking manual overrides provides a constant feedback loop for the developers. This data helps the machine learning model learn from its mistakes. Over time, the system becomes more accurate, and the need for human intervention slowly decreases.
The goal is not full automation from the very first day. Instead, the focus is on safe automation that improves revenue performance without creating unnecessary compliance risk.
Build The AI RCM MVP Around One Revenue Outcome
An AI RCM MVP should focus on one high-value revenue outcome, such as reducing denials, improving clean claims, detecting underpayments, or speeding claim follow-up.
Launching a massive platform all at once often leads to high costs and slow delivery. Therefore, successful founders focus on a Minimum Viable Product that solves one specific financial pain point. This approach allows for faster market entry and a clearer return on investment.
1. MVP Option 1: Denial Prediction MVP
This model is ideal for organizations struggling with a growing backlog of rejected claims. The primary goal is to stop revenue loss before the claim even leaves the office. By analyzing historical data, the software can flag high-risk claims for immediate review.
- Risk Scoring: Evaluates the likelihood of a denial based on past payer behavior.
- Correction Alerts: Notifies the billing staff of specific errors that need fixing.
- KPI Dashboards: Provides leadership with clear visibility into the preventable denial rate.
Focusing on denial prediction is a strategic move for RCM companies managing large volumes. Consequently, it reduces the heavy workload associated with the appeal process. It turns a reactive billing cycle into a proactive revenue strategy.
2. MVP Option 2: AI Claim Scrubbing MVP
A claim scrubbing MVP is perfect for businesses that face frequent technical rejections. This tool acts as a final gatekeeper to ensure every submission meets the exact requirements of different payers. It focuses on the technical accuracy of the claim data.
- Payer Edits: Applies specific rules for each insurance company to avoid rejections.
- Readiness Score: Gives a simple “go” or “no-go” signal for every claim in the queue.
- Field Detection: Automatically finds missing or mismatched data points.
This option is great for SaaS teams building validation tools for the broader market. Therefore, it improves the first-pass acceptance rate and lowers the cost of manual review. It ensures that the cash flow remains steady and predictable.
3. MVP Option 3: Eligibility Automation MVP
Many billing issues start at the front desk before the patient even sees a doctor. An eligibility MVP focuses entirely on the registration and insurance verification process. It ensures that the provider is only treating patients with active and valid coverage.
- Real-time Checks: Instantly verifies coverage during the patient check-in process.
- Visibility: Shows the exact co-pay and deductible amounts to the front-desk staff.
- Task Creation: Automatically alerts the team if a plan has limitations or requires a referral.
This model is best for clinics with high registration error rates. In addition, it significantly reduces the front-desk workload. It stops the most common type of denial at the very beginning of the cycle.
4. MVP Option 4: AI Coding Support MVP
Coding is a specialized and expensive task that often creates bottlenecks in the billing process. An AI coding support MVP helps humans work faster by suggesting the most likely codes based on clinical notes. It is particularly valuable for high-volume specialty practices.
- Note Ingestion: Scans clinical documents to find relevant diagnoses and procedures.
- Gap Alerts: Highlights when a doctor has not provided enough detail for a specific code.
- Approval Flow: Keeps the final decision in the hands of a certified human coder.
Founders choosing this path can see an immediate boost in coder productivity. Furthermore, it reduces the risk of expensive compliance audits. It ensures that every service provided is documented and billed at its full value.
5. MVP Option 5: Underpayment Detection MVP
Contracted rates are complex, and payers often make mistakes when calculating payments. An underpayment MVP compares every incoming payment against the agreed-upon fee schedule. This is a high-value tool for finance teams managing multiple payer contracts.
- Rate Comparison: Flags any payment that is even a few dollars below the contract.
- Variance Alerts: Identifies systemic payment issues with specific insurance companies.
- Recovery Tasks: Creates a workflow for staff to chase down the missing revenue.
This model is highly attractive to hospitals and multi-location providers. Consequently, it helps recover thousands of dollars that might otherwise be ignored. It provides a level of financial oversight that is impossible to achieve manually.
The initial development phase should focus on one core revenue outcome. A targeted MVP provides the proof of concept needed to scale into a full enterprise-grade solution.
Plan Integrations Before Finalizing The Development Scope
AI RCM software integrations should be planned early because EHR, clearinghouse, payer, payment, and accounting connections affect cost, timeline, and product design.
Integrations form the nervous system of any revenue cycle platform. If the software cannot communicate with existing tools, then the AI logic remains isolated and ineffective. Therefore, founders must define the technical scope of these connections before the first line of code is written.
1. EHR And EMR Integration Scope
The EHR is the primary source of all clinical and demographic data. High-quality AI RCM software must pull encounter data and documentation directly from these systems. This ensures that the billing process starts with the most accurate information available.
- Major Platforms: Planning for connections with systems like Epic, Oracle Health, and Athenahealth.
- Data Points: Extracting patient demographics and clinical notes for automated coding.
- Synchronization: Ensuring that clinical updates are reflected in the billing queue in real time.
Integrating with the top EHR vendors allows the software to serve a wider range of healthcare providers. It eliminates the need for manual data entry and reduces the risk of human error.
2. Practice Management System Integration Scope
Practice management systems handle the operational side of the clinic, like scheduling and registration. The RCM tool needs this data to link appointments to specific financial outcomes. Consequently, the system can track whether a patient was checked in correctly before a claim is created.
- Registration Data: Pulling insurance information captured during the patient check-in.
- Charge Data: Gathering all service charges associated with a specific appointment.
- Billing History: Reviewing past patient balances to assess collection risks.
This connection provides a complete view of the patient journey from the front desk to final payment. It helps the organization identify where process breakdowns occur in the daily workflow.
3. Clearinghouse Integration Scope
Clearinghouses act as the bridge between providers and thousands of different insurance companies. Therefore, the software must integrate deeply with these hubs to manage claim submissions and status updates. This is where the platform receives its most critical performance feedback.
- Claim Status: Automatically pulling rejection messages to alert the billing staff.
- ERA Files: Ingesting electronic remittance advice for automated payment posting.
- Resubmission: Streamlining the workflow for fixing and resending denied claims.
Effective clearinghouse integration ensures that the organization can track every transaction in real time. It provides a transparent log of all communication between the provider and the payer.
4. Payer And X12 EDI Integration Scope
Standardized EDI transactions are the language of healthcare finance. The software must be capable of processing X12 formats for eligibility, claims, and remittances. Furthermore, it should provide a way to interact with payer portals for more detailed information.
- Transaction Types: Supporting 270/271 for eligibility and 837 for claim submission.
- Remittance: Processing 835 files to understand how claims were adjudicated.
- Payer APIs: Connecting directly to modern payer interfaces for faster data exchange.
Mastering these protocols ensures that the platform is compatible with the entire insurance ecosystem. It allows for a higher level of automation in verifying coverage and checking claim status.
5. FHIR API Readiness
The industry is rapidly moving toward FHIR standards for better data interoperability. Modern RCM platforms must prepare for these API based workflows to remain competitive. This is especially relevant for managing complex prior authorization tasks.
- CMS Compliance: Aligning with rules like CMS-0057-F to improve digital data exchange.
- Authorization Flows: Using APIs to send and receive approval documents instantly.
- Interoperability: Preparing for payer-to-payer data exchange requirements.
Being FHIR-ready future-proofs the software against upcoming regulatory changes. It enables a more seamless flow of documentation between providers and payers.
6. Payment Gateway Integration Scope
A seamless payment experience is vital for improving patient collections. The software should integrate with reliable gateways to handle credit cards and ACH transactions safely. Therefore, the system must also manage refunds and recurring payment plans.
- Payment Links: Sending secure digital links to patients via text or email.
- Digital Receipts: Automatically generating and storing proof of payment for the patient.
- Reconciliation: Matching gateway transactions directly to the patient’s billing record.
Providing flexible payment options reduces the friction for patients who want to settle their bills. This directly improves the organization’s cash flow and lowers the cost of collections.
7. Accounting And ERP Integration Scope
The final stage of the revenue cycle is the transfer of financial data to the general ledger. Therefore, the software needs a clean sync with accounting tools to ensure the books remain accurate. This reduces the workload on the finance team during the month-end close.
- Ledger Sync: Pushing finalized payments and adjustments into the accounting system.
- Revenue Reports: Generating high-level financial summaries for the executive team.
- Audit History: Maintaining a clear trail of every financial transaction for tax and legal purposes.
Connecting with ERP systems provides the CFO with a unified view of the company’s financial health. It ensures that the RCM data matches the actual bank deposits.
8. Patient Portal Integration Scope
Patient engagement is a key factor in modern revenue cycle management. The software should push billing statements and cost estimates directly to the patient portal. This gives patients the transparency they need to manage their healthcare expenses.
- Estimate Visibility: Showing patients their expected out-of-pocket costs before a procedure.
- Communication Logs: Tracking all interactions regarding billing questions or disputes.
- Plan Setup: Allowing patients to manage their own installment plans online.
A robust portal integration empowers patients to take control of their financial responsibilities. It leads to higher satisfaction and faster payment cycles for the provider.
Integrations are not just a backend technical detail. They ultimately decide how useful the software becomes in the daily reality of RCM operations.
Make The Software HIPAA-Ready And Billing-Compliant
AI RCM software must protect PHI, support secure access, maintain audit trails, follow billing rules, and prepare for evolving payer and price transparency requirements.
This proactive approach protects the enterprise from massive legal liabilities and builds essential trust with provider organizations.
1. PHI Protection
Protecting Protected Health Information is the most critical technical requirement for any AI RCM software. Every piece of data must be shielded using industry-standard encryption protocols both while stored and while moving between systems. Furthermore, the platform should practice data minimization by only accessing the patient details necessary for a specific billing task.
- Encryption Standards: Utilizing robust AES-256 encryption at rest and TLS 1.3 for data in transit.
- Masking Logic: Obscuring sensitive patient names and identifiers during the AI training or processing phase.
- Vendor Controls: Ensuring that any third-party AI or cloud provider meets the same high security standards.
Secure AI processing ensures that patient privacy is never compromised for the sake of automation. Consequently, it allows the organization to leverage modern machine learning while staying within the boundaries of federal law.
2. Role-Based Access Control
The software must ensure that users only have access to the data required for their specific jobs. Implementing a least-privilege design prevents unauthorized access and reduces the risk of internal data breaches.
Therefore, permissions should be granular and tied to specific functional roles within the revenue cycle.
- Billing Users: Access to claim queues and payer correspondence without seeing full clinical histories.
- Coders: Permissions to view clinical charts and document suggestions for final approval.
- Finance Admins: High-level access to revenue reports and contract settings without patient-level detail.
Role-based controls simplify the management of large administrative teams. Additionally, they provide a clear structure for auditing user activity across the entire platform.
3. Secure Authentication
Accessing a financial platform requires more than just a simple password. Modern healthcare systems must utilize multi-factor authentication and single sign-on to prevent unauthorized logins.
Therefore, the platform should monitor all session activity to detect and block suspicious behavior instantly.
- Identity Management: Integrating with enterprise SSO providers to centralize user management.
- Session Control: Automatically timing out inactive users to prevent unauthorized access at workstations.
- Activity Alerts: Notifying administrators immediately if a login occurs from an unrecognized device or location.
Strong authentication policies are the first line of defense against cyber threats. Consequently, they ensure that the financial data remains in the hands of authorized personnel only.
4. Coding And Billing Audit Trails
Transparency is essential for passing both internal and external financial audits. The software must maintain a permanent record of every change made to a claim or a billing code.
This history should include the original AI recommendation and the name of the human who gave final approval.
- Edit History: Tracking every modification to a claim from creation to final adjudication.
- Approval Logs: Documenting who authorized specific coding changes or financial write-offs.
- Compliance Reporting: Generating automated summaries that prove the organization is following billing rules.
Comprehensive audit trails protect the business during payer disputes or government investigations. They provide the evidence needed to justify every dollar collected by the organization.
5. Prior Authorization API Readiness
Federal regulations are rapidly pushing for more transparent and automated authorization processes. The software must be ready to exchange documents and approval data via modern APIs.
This alignment with FHIR standards ensures that the platform can communicate directly with payer systems.
- Document Exchange: Securely sending clinical notes required for procedure approval.
- Status Tracking: Maintaining a real-time history of all pending and approved authorizations.
- API Alignment: Preparing for digital workflows that eliminate the need for faxing or manual portal entries.
Being API ready reduces the time spent waiting for payer approvals. Consequently, it speeds up the patient care cycle and improves the overall efficiency of the revenue department.
6. Patient Estimate And Price Transparency Workflows
New mandates require providers to provide clear and accurate cost estimates to patients before service. The software must generate these estimates based on the patient’s specific plan and the provider’s contracted rates.
This transparency is now a regulated requirement rather than an optional feature.
- Cost Estimation: Calculating the exact out-of-pocket responsibility for shoppable services.
- Price Lists: Generating machine-readable pricing data that meets the latest 2026 CMS requirements.
- Clarity: Providing patients with a simple history of their past estimates and payments.
Compliance with price transparency rules builds patient trust and reduces billing disputes. Furthermore, it protects the provider from the latest enforcement actions that began earlier this year.
Compliance should shape the software architecture from the very beginning. It should never appear as a checklist at the end of the development process.
Conclusion
Selecting the right development path transforms revenue cycle management from a defensive struggle into a strategic advantage. By prioritizing data integrity, payer-specific intelligence, and phased automation, organizations can eliminate leakage and ensure sustainable growth.
Implementing these enterprise-grade solutions provides the transparency and efficiency required to lead in the modern healthcare market. Now is the time to build a resilient financial foundation that scales alongside your business ambitions.
Build AI Revenue Cycle Management Software With Intellivon
Building AI revenue cycle management software takes more than adding automation to billing tasks. It requires a healthcare finance system that understands patient access, payer rules, coding workflows, claims, denials, payments, compliance, and revenue performance.
At Intellivon, we help healthcare companies, RCM providers, billing companies, digital health startups, specialty clinics, and enterprise healthcare teams build AI-powered RCM software around real operational workflows.
A. We Design Payer-Aware AI Automation
Payer behavior directly affects reimbursement timelines, denial rates, underpayments, and operational workload. Our AI workflows are designed around payer-specific rules, denial trends, authorization requirements, and reimbursement patterns.
This helps healthcare organizations move from reactive billing operations to predictive revenue management.
- Payer-specific claim rules
- Denial prediction
- Prior authorization logic
- Contract variance detection
- Underpayment alerts
- Payer performance dashboards
B. We Integrate With Healthcare And Finance Systems
Revenue cycle software depends on reliable interoperability between clinical systems, billing systems, payers, payment infrastructure, and finance operations. We build secure integrations that keep workflows connected across the healthcare revenue cycle.
Our approach focuses on clean data exchange, transaction reliability, workflow continuity, and scalable interoperability.
- EHR/EMR
- Practice management systems
- Clearinghouses
- Payer APIs
- X12 EDI
- FHIR APIs
- Payment gateways
- Accounting systems
C. We Add Security, Compliance, And AI Governance
Healthcare finance software must support auditability, explainability, secure access, and human oversight from the start. We design AI RCM systems with governance controls that help organizations maintain trust, visibility, and compliance while scaling automation.
This creates a safer environment for AI-assisted billing, coding, payment, and denial workflows.
- HIPAA-ready architecture
- PHI protection
- Role-based access
- Audit logs
- Human review
- Model monitoring
- Explainable AI workflows
If you are planning to develop AI revenue cycle management software, contact Intellivon to build a secure, scalable, and revenue-focused system designed for real healthcare operations.
Common Queries
Q1. How does AI improve revenue cycle management software?
A1. AI improves revenue cycle management software by predicting denials, validating claims, assisting medical coding, detecting underpayments, prioritizing work queues, and automating repetitive billing tasks. This helps healthcare organizations reduce manual work, improve clean claim rates, speed reimbursement, and gain better visibility into revenue performance.
Q2. What features should AI RCM software include?
A2. AI RCM software should include patient access workflows, eligibility verification, prior authorization support, coding assistance, claim scrubbing, denial prediction, payment posting, patient billing, underpayment detection, payer analytics, audit logs, and compliance controls. The best platforms connect these workflows instead of operating as disconnected modules.
Q3. How much does AI revenue cycle management software development cost?
A3. AI RCM software development usually costs between $50,000 and $200,000+, depending on workflow scope, AI complexity, healthcare integrations, compliance requirements, and reporting needs. A focused MVP costs less, while enterprise systems with payer-aware automation and advanced analytics require a larger investment.
Q4. Can AI RCM software integrate with EHRs and clearinghouses?
A4. Yes. AI RCM software can integrate with EHRs, EMRs, practice management systems, clearinghouses, payer APIs, X12 EDI workflows, payment gateways, accounting systems, and patient portals. These integrations help clinical, billing, claims, payment, and financial data move securely across revenue workflows.






