Right now, hospitals are dealing with three alarming issues. The first one is that their fee-for-service habits are bleeding into value-based contracts. At the same time, Epic holds years of rich patient data that never reaches the outcomes dashboards or financial risk tools that actually drive performance. Additionally, the poor care coordination quietly compounds reimbursement risk until it shows up as a budget problem nobody saw coming. For organizations managing large patient populations under value-based contracts, that scenario plays out more often than anyone reports.
The real question rests in how a value-based care platform is built that sits on top of Epic’s infrastructure without disrupting clinical operations or adding another disconnected layer. When it’s done right, risk stratification becomes automated, quality metrics flow directly from clinical documentation, and financial performance stops living separately from patient outcomes.
Intellivon specializes in developing enterprise-grade value-based care platforms that integrate with Epic at the infrastructure level. This blog draws from that experience and covers architecture, integration strategy, interoperability standards, and compliance.
Why Value-Based Care Needs Platform Thinking
Value-based care (VBC) requires platform-driven architectures to work at scale. Isolated tools, fragmented data, and manual workflows cannot support coordinated care, shared risk models, or continuous improvement.
As a result, the shift is no longer about adding a single analytics module. Instead, healthcare organizations are building integrated platforms that connect claims, EHR, RPM, social determinants, and care management systems into one unified ecosystem.
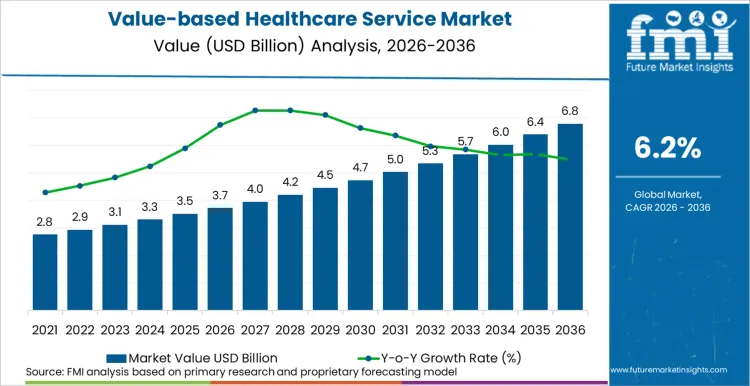
The value-based healthcare services market was valued at USD 3.5 billion in 2025 and is expected to reach USD 3.72 billion in 2026. It is projected to grow further to USD 6.78 billion by 2036, at a CAGR of 6.2%. This growth reflects a broader shift from volume-based billing to outcome-driven reimbursement models across healthcare systems.
Transitioning to a value-based model requires more than just a change in billing. It demands a fundamental shift in how data moves through the healthcare enterprise.
1. Fee-for-service systems break outcome models
Traditional healthcare systems were built to track individual transactions. These legacy frameworks focus on the volume of tests and visits. However, value-based care prioritizes the long-term health of the patient. Therefore, using a fee-for-service architecture to manage risk often leads to financial misalignment.
In addition, volume-based systems lack the predictive tools needed for wellness. They are designed to react to illness rather than prevent it. Consequently, organizations struggle to close care gaps when using outdated software. To succeed, leaders must move toward systems that reward quality and efficiency.
2. Why point solutions fail in VBC programs
Many enterprises try to fix specific problems with isolated apps. While these tools might help with one task, they create data silos. These disconnected systems cannot share information with other clinical departments. As a result, the care team loses the full picture of the patient journey.
Managing a VBC program requires a unified view of every touchpoint. Fragmented tools increase the manual workload for busy clinicians. Furthermore, they often require multiple logins and separate databases. This friction reduces the likelihood of successful adoption across the enterprise.
3. Platform-led care delivery across providers
A platform approach connects every stakeholder in the care continuum. It allows primary doctors and specialists to work from the same data set. Because the information is centralized, transitions of care become much smoother. This connectivity ensures that no patient falls through the cracks during referrals.
In addition, platforms enable real-time tracking of performance metrics. Leaders can see which interventions are lowering costs and improving health. This level of transparency is essential for managing global risk contracts. A robust platform scales as the provider network grows larger.
4. Epic is the system of record in VBC
Integrating with Epic is the most strategic move for any VBC platform. Since Epic holds the vast majority of clinical data, it serves as the source of truth. However, raw data inside an EHR is often difficult to analyze for risk. Therefore, your platform must enhance Epic data with external financial insights.
Epic value-based care integration ensures that clinicians stay within their known workflows. They do not have to leave the EHR to see risk scores or care gaps. This deep integration builds trust and speeds up the decision-making process. By leveraging the existing system of record, you reduce technical debt and implementation time.
A platform-led strategy ensures that your data works for you rather than against you. This approach creates a sustainable foundation for long-term clinical and financial success.
Transitioning to a platform mindset is the only way to scale complex value-based initiatives effectively. By centralizing data and workflows, organizations can finally align their clinical outcomes with their financial goals.
What a Value-Based Care Platform Must Deliver
Building a platform for value-based care requires a shift from transactional data to holistic patient insights. Investors must ensure the infrastructure supports long-term health outcomes while protecting financial margins.
1. Longitudinal patient record across care journeys
A true VBC platform must move beyond the snapshot of a single office visit. Therefore, it should aggregate data from every touchpoint, including hospitals, clinics, and home monitoring. This creates a continuous timeline of a patient’s health history over many years.
In addition, this record must be accessible to every provider in the network. When a specialist sees a patient, they should instantly see the primary doctor’s notes. Consequently, this transparency prevents duplicate testing and reduces the risk of medical errors. A complete history is the foundation of any successful wellness strategy.
2. Real-time quality and risk scoring engines
Waiting for monthly claims data is a recipe for financial failure in risk-based contracts. Instead, the platform must calculate risk scores in real time as clinical data enters the system. This allows the care team to see which patients are drifting toward a crisis.
Furthermore, these engines should track quality metrics such as HEDIS or MIPS scores automatically. If a patient is missing a screening, the system must flag it immediately. Therefore, providers can close care gaps during the actual patient encounter. This proactive approach ensures the organization hits its performance benchmarks.
3. Care coordination across providers and settings
Value-based care often fails when patients transition between different levels of care. For example, a patient leaving the hospital needs a follow-up appointment within days. The platform must automate these handoffs to ensure no one is lost in the system.
In addition, the software should facilitate communication between community resources and clinical teams. This might include coordinating with social workers or home health aides. When everyone is synchronized, the cost of care drops significantly. Effective coordination is the primary driver of reduced hospital readmissions.
4. Contract-aware workflows for VBC models
Every payer contract has different rules, incentives, and reporting requirements. Therefore, a generic EHR setup is usually not enough to manage multiple VBC agreements. The platform must be “contract-aware” to guide clinicians toward the right actions for each patient.
For instance, the system can suggest specific cost-effective medications based on the patient’s insurance plan. It can also prioritize certain follow-up tasks that are tied to shared savings bonuses. Consequently, the clinical workflow becomes a tool for achieving the best financial outcome. This alignment is critical for maintaining healthy margins in a risk-based environment.
5. Population health analytics and reporting
To manage risk at scale, leaders need to see the big picture across thousands of lives. The platform must include powerful analytics tools that identify trends and outliers in the population. You can see which regions or clinics are performing best and why.
Furthermore, these reports must be easy to share with payers and regulatory bodies. Automated reporting saves hundreds of hours of manual data collection every year. Therefore, the administrative burden of compliance is greatly reduced. High-level insights allow executives to make data-driven decisions about their network strategy.
Delivering value at scale is impossible without a platform that understands both the patient and the contract. By investing in these five core areas, organizations can build a resilient infrastructure that thrives in the evolving healthcare landscape.
Where Epic Fits in VBC Platform Architecture
A value-based care platform is only as strong as its connection to the primary medical record. For most large health systems, that foundation is Epic. Understanding how to build on top of this infrastructure is the key to creating a scalable, high-performance solution.
1. Epic as clinical data backbone for VBC
In a value-based model, you cannot manage what you cannot see. Epic acts as the central warehouse for all clinical interactions and patient history. Therefore, it provides the essential context needed to evaluate health outcomes. By treating Epic as your primary data source, you ensure your platform uses the most accurate information.
2. Using Epic APIs, HL7, and FHIR layers
To move data, you must use a mix of modern and legacy standards. HL7 v2 remains the workhorse for real-time updates like admissions.
However, FHIR APIs are the future of structured data exchange. They allow your platform to query specific resources like conditions with high precision.
3. Integrating with Epic registries and modules
Epic offers specific tools like “Healthy Planet” for population health. Your platform should not compete with these modules but rather enhance them.
For example, you can push social health data into Epic registries to improve risk stratification. This creates a more powerful tool for care managers.
4. Handling data latency and sync challenges
Real-time care requires real-time data, but syncing large amounts of information can be slow. Your architecture must handle these delays without breaking the user experience. Therefore, implementing “webhooks” is essential so your system is notified the instant a change happens. This prevents the need for constant, manual data requests.
5. Extending Epic without disrupting workflows
The biggest mistake is forcing a doctor to log into a second system. Therefore, your platform should live inside the Epic interface using “SMART on FHIR” technology. This allows your custom tools and risk scores to appear as a tab within the patient’s chart. Consequently, you turn data into action at the exact moment a care decision is made.
Successful VBC platforms treat Epic as a partner, not an obstacle. By using the right integration layers and respecting clinical workflows, you create a solution that is both technically sound and highly practical for everyday use.
Epic Integration Models for VBC Platforms
Selecting the proper integration model is a high-stakes decision for any enterprise leader. This choice dictates the speed, cost, and long-term scalability of your platform.
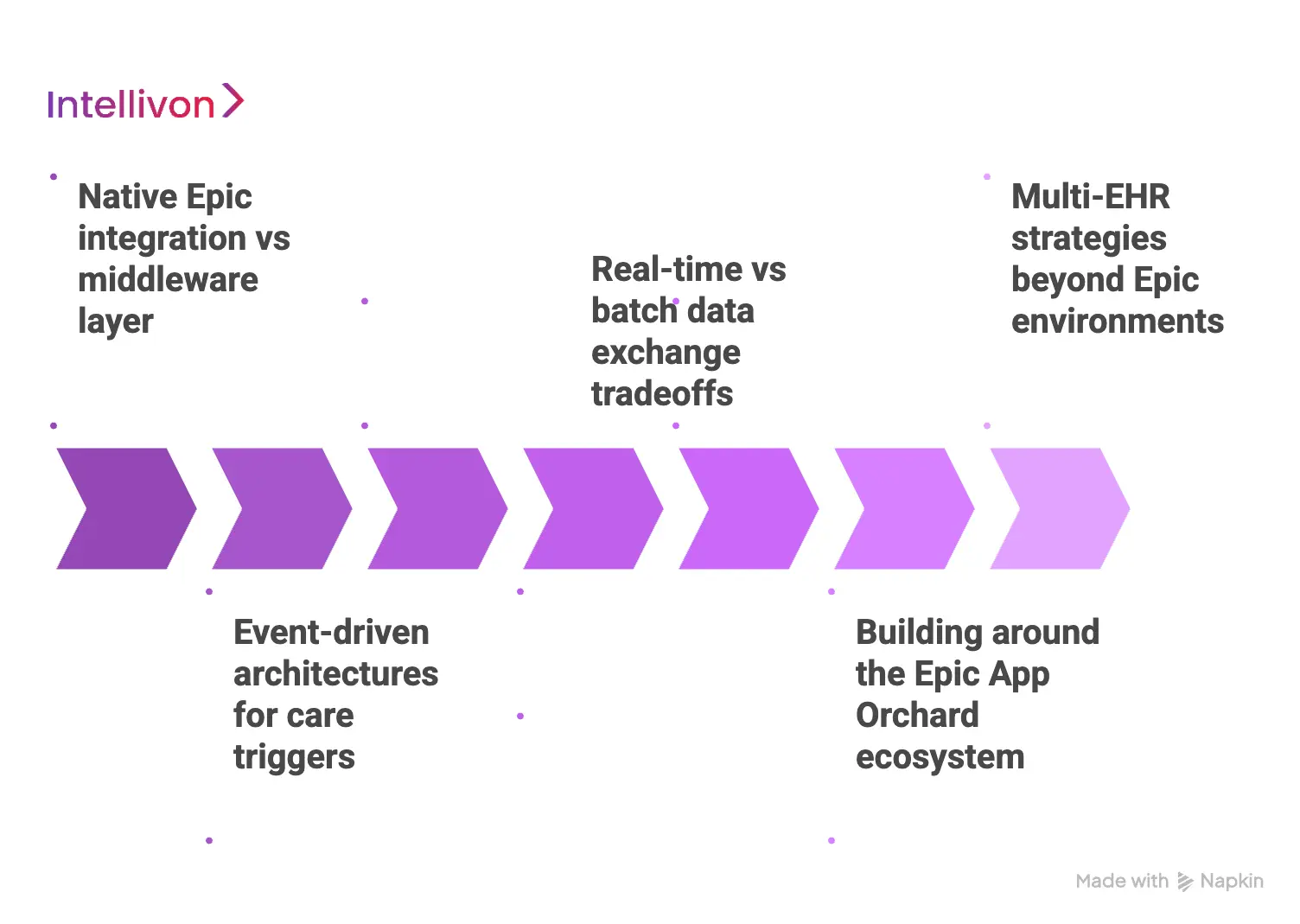
1. Native Epic integration vs middleware layer
A native integration lives directly within the Epic environment using SMART on FHIR. This approach offers the most seamless experience for clinicians. Therefore, users never leave their primary workspace. However, native builds can be restrictive for aggregating non-Epic data.
In addition, a middleware layer acts as a neutral data hub. It collects information from various systems before sending it to your platform. This model is often more flexible for complex Value-Based Care (VBC) calculations.
2. Real-time vs batch data exchange tradeoffs
Real-time exchange is essential for immediate clinical interventions. For example, a doctor needs a high-risk alert during a patient visit. However, real-time syncing requires more bandwidth. Therefore, it is best reserved for critical data points.
In contrast, batch processing is more efficient for large-scale population health analytics. You can move massive amounts of claims data overnight. Furthermore, batching is often more cost-effective. Finding the right balance between these two methods is key to system stability.
3. Event-driven architectures for care triggers
Modern VBC platforms thrive on event-driven designs. This means the system stays quiet until a specific event occurs, like a patient discharge. Once triggered, the platform automatically starts a post-discharge care workflow.
Therefore, no manual intervention is needed to begin the next phase. In addition, these architectures reduce the noise that clinicians often face. They only receive notifications when an action is truly required. Consequently, this targeted approach improves the efficiency of care management teams.
4. Building around the Epic App Orchard ecosystem
The Epic App Market (formerly App Orchard) provides a governed path for integration. It offers standardized APIs and security protocols that Epic has already vetted. Therefore, using this ecosystem speeds up the trust-building process with hospital IT departments. It signals that your platform meets high enterprise standards.
Furthermore, being part of the official market simplifies the deployment process. You can leverage existing Epic frameworks to install and update your tools. However, you must align your development roadmap with Epic’s evolving API versions.
5. Multi-EHR strategies beyond Epic environments
While Epic is a dominant player, most large networks still use multiple EHR systems. Therefore, your platform must be able to speak to Cerner or Meditech. A multi-EHR strategy protects your investment against future market shifts. You are not locked into a single vendor’s ecosystem forever.
In addition, an EHR-agnostic data layer allows you to normalize information from these different sources. This ensures your risk scores are consistent across the whole network. Consequently, your platform becomes more valuable to large integrated delivery networks.
The ideal strategy combines the native feel of Epic with the power of an independent data layer. By mastering these models, organizations build a resilient infrastructure that supports high-performance value-based care. This technical foundation allows for rapid scaling and consistent clinical outcomes across any provider network, regardless of the underlying record system.
Core Modules of a VBC Platform with Epic
A high-performance value-based care platform functions as a strategic intelligence layer. It sits above the raw clinical data to provide the specific insights needed for risk-based contracting.
1. Patient risk stratification engine design
Effective risk management begins with identifying the right patients for intervention. Therefore, your platform must use advanced algorithms to score patients based on clinical and social factors.
This engine should pull data directly from Epic to ensure scores are always current. In addition, it must categorize patients into low, medium, and high-risk tiers. Consequently, care managers can prioritize their time on the individuals who need the most support.
2. Care gap detection and closure workflows
Care gaps represent missed opportunities for both health and revenue. For example, a diabetic patient who has not had an eye exam represents a significant risk. Your platform must automatically flag these omissions within the Epic provider workspace.
Therefore, the doctor can address the gap during a scheduled visit. Furthermore, these workflows should track the status of the gap until it is officially closed. This closing of the loop is essential for hitting quality performance targets.
3. Provider performance tracking dashboards
In a value-based model, leaders must understand how individual clinicians contribute to the overall goal. These dashboards should compare providers against peers on metrics like readmission rates and quality scores. This transparency encourages best practices across the entire organization.
In addition, the data must be presented in a clear and actionable format. Therefore, clinical leaders can identify which teams need additional training or resources. This level of oversight is critical for managing a profitable network.
4. Cost and utilization tracking modules
Controlling costs requires deep visibility into how patients use healthcare resources. This module must track expensive events like emergency room visits and out-of-network referrals. By integrating claims data with Epic clinical data, you get a complete view of the total cost of care.
Furthermore, it should identify high-cost outliers that are draining the organization’s margins. Therefore, you can develop targeted strategies to redirect care to more affordable settings. This financial intelligence is the backbone of shared savings success.
5. Patient engagement and remote monitoring
The patient’s journey does not end when they leave the clinic. Therefore, your platform must include tools for remote monitoring and proactive communication. This might involve digital surveys or syncing data from home medical devices. In addition, these engagement tools should push relevant alerts back into the Epic system for review.
Consequently, the care team can intervene early if a patient’s condition starts to decline. This continuous connection is the most effective way to prevent avoidable hospitalizations.
These core modules transform fragmented data into a unified strategy for population health. By building these capabilities on top of Epic, organizations create a powerful system that drives both clinical excellence and financial sustainability. This modular approach allows investors to scale their technology as their value-based care programs grow in complexity and size.
Designing Data Pipelines for Epic VBC Systems
A data pipeline is the plumbing of your healthcare platform. It moves vital information from Epic to your analytics engine. For investors, a reliable pipeline is the only way to ensure that clinical decisions are based on facts rather than guesses.
1. Ingesting ADT, clinical, and claims data
Your platform needs three types of data to work well. Admission, Discharge, and Transfer (ADT) feeds tell you when a patient enters the hospital. Clinical data from Epic shows what happened during the visit.
Finally, claims data from insurance companies reveal the total cost. Therefore, your pipeline must pull all three into one place. In addition, these feeds must be secure and reliable. Consequently, the care team always has the most recent story for every patient.
2. Normalizing data across fragmented sources
Data comes in many different formats and languages. For example, one clinic might code a lab result differently from another. Your system must translate these various codes into a single standard. This process is called normalization.
Therefore, when you look at a report, the information is consistent across the whole network. In addition, clean data makes it much easier to build accurate risk models. Furthermore, it prevents the confusion that happens when different systems use different terms for the same thing.
3. Building patient identity resolution systems
One of the biggest hurdles is making sure the name of the patient in Epic is the same as in the insurance file. A patient identity system matches these records using details like birth dates or addresses. Therefore, you avoid creating duplicate profiles for the same person.
In addition, this ensures that every piece of medical history is attached to the right individual. Consequently, your clinical scores remain accurate. A strong matching system is the only way to maintain a true longitudinal record over time.
4. Ensuring data quality and governance
Bad data leads to bad medical decisions. Therefore, your pipeline must include automatic checks to catch errors or missing values. Data governance is the set of rules that decides who can see and change this information.
In addition, it ensures that your platform stays compliant with privacy laws like HIPAA. Furthermore, regular audits help keep the data clean as the system grows. High data quality builds trust with the doctors who rely on your platform every day.
5. Creating near real-time analytics layers
Waiting weeks for a report is not an option in value-based care. Therefore, your pipeline should process data as soon as it arrives. This “near real-time” layer allows you to spot a rising risk before it becomes a crisis.
In addition, it lets you track your progress toward financial goals every day. Furthermore, fast analytics mean that your care triggers are always based on the latest facts. Consequently, your organization can pivot quickly to address new challenges in the patient population.
Building a solid data pipeline is the most important technical investment for a value-based platform. By simplifying how data moves from Epic to your analytics tools, you create a foundation for long-term growth and clinical success. This infrastructure ensures that your enterprise remains competitive in an increasingly data-driven healthcare market.
Real Challenges in Epic-Based VBC Platforms
Building on Epic provides a strong foundation, but it also comes with specific hurdles that can stall a value-based care program. Understanding these real-world obstacles is the first step toward creating a resilient and profitable platform.
1. Data access limitations within Epic
While Epic holds vast amounts of information, getting that data out in a usable way is not always easy. Therefore, developers often face strict rules about how many times they can query the system.
These limits can slow down your real-time risk scores if the pipeline is not designed well. In addition, some high-value data points may stay hidden in unstructured doctor notes. Consequently, your platform needs a plan to extract this “dark data” without crashing the primary EHR.
2. Interoperability gaps across provider networks
Value-based care often involves doctors who use different software systems. However, these systems do not always speak the same language as Epic. This creates gaps in the patient’s story when they move between a hospital and a private clinic. Therefore, your platform must act as a bridge to fill these holes.
Furthermore, if a referral happens outside your main network, the data might not follow the patient. This lack of connection makes it very difficult to track total care costs.
3. Aligning clinical and financial datasets
Doctors look at blood pressure, while finance teams look at insurance claims. These two worlds rarely meet in a single database. Therefore, a major challenge is merging clinical facts with financial data. In addition, claims data is often delayed by several weeks or months.
This “claims lag” means your financial picture is always slightly behind the clinical reality. Consequently, your platform must find ways to predict costs before the final bill arrives.
4. Scaling across multiple care organizations
What works for one hospital might not work for another, even if they both use Epic. Every organization has its own unique way of setting up its workflows and data fields. Therefore, a “one size fits all” platform will likely fail during a large rollout. In addition, managing different security rules across multiple sites adds a layer of technical pain.
Furthermore, you must ensure that your analytics stay accurate as the patient population grows. Scaling requires a flexible architecture that can adapt to local clinical habits.
5. Managing compliance across data flows
Moving patient data between Epic and an external platform brings heavy legal responsibilities. You must ensure that every byte of information is encrypted and tracked. Therefore, your platform must meet strict HIPAA and SOC2 standards to protect patient privacy.
In addition, you need to manage “consent” to ensure patients have agreed to share their data. Furthermore, these rules can change depending on the state or the specific payer contract. Consequently, staying compliant is a constant task that requires dedicated technical oversight.
Acknowledging these challenges allows you to build a more robust and realistic platform from day one. This proactive approach ensures that your technology remains a reliable asset as you navigate the complexities of risk-based contracting and large-scale provider networks.
AI in Value-Based Care Platforms with Epic
Integrating AI with Epic data transforms a passive record into a predictive engine. This layer of intelligence allows leaders to stay ahead of clinical risks and financial fluctuations.
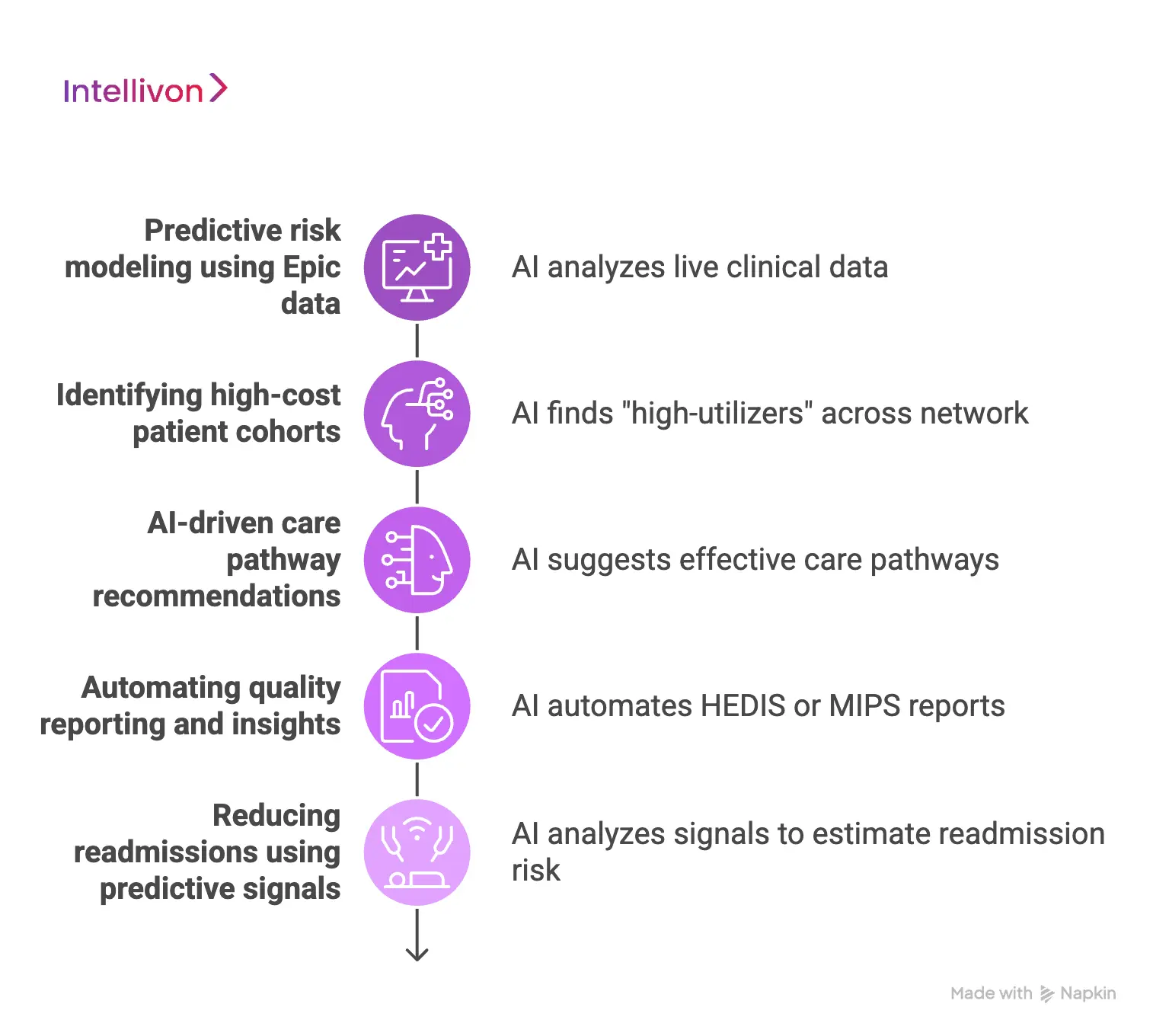
1. Predictive risk modeling using Epic data
Traditional risk models often look backward at old insurance claims. However, AI can look at live clinical data sitting inside Epic today. This includes lab results, vital signs, and even doctor notes.
Therefore, the system can predict which patients might get sicker in the next thirty days. In addition, these models get smarter as they ingest more data over time. Consequently, your clinical team can act before a minor health issue turns into a major crisis.
2. Identifying high-cost patient cohorts
A small group of patients usually accounts for the majority of healthcare spending. Therefore, your platform must use AI to find these “high-utilizers” across your entire network. The system looks for patterns in how these individuals use the emergency room or specialty care.
In addition, it identifies social factors like a lack of transportation that might drive up costs. Furthermore, knowing who these patients are allows you to design specific programs to help them. This targeted approach is the fastest way to protect your financial margins.
3. AI-driven care pathway recommendations
Standardizing care is the best way to ensure high quality and low costs. Therefore, AI can suggest the most effective “care pathway” based on a patient’s unique history in Epic. If a patient has multiple chronic conditions, the system recommends a tailored plan of action.
In addition, these suggestions appear directly in the provider’s workflow to save time. Furthermore, the AI tracks whether following these paths actually leads to better health outcomes. Consequently, you can constantly refine your clinical strategies based on real-world evidence.
4. Automating quality reporting and insights
Reporting on quality metrics is often a manual and painful process for clinical staff. However, AI can automatically find the data needed for HEDIS or MIPS reports within the EHR. It scans the record to see if screenings were done or if medications were prescribed correctly.
Therefore, the administrative burden on your nurses and doctors is greatly reduced. In addition, automated insights show you exactly where your organization is falling short of its goals. This transparency allows you to fix problems long before the reporting deadline arrives.
5. Reducing readmissions using predictive signals
Preventing a patient from returning to the hospital is a top priority in value-based care. Therefore, AI analyzes “predictive signals” during the initial hospital stay to estimate the risk of a quick return. These signals might include a change in heart rate or a delay in physical therapy.
In addition, the system alerts the care transition team to provide extra support after discharge. Furthermore, it can suggest home monitoring for patients with the highest risk scores. Consequently, you can significantly lower your readmission rates and avoid expensive payer penalties.
AI turns the vast amount of data in Epic into a clear and actionable roadmap for value-based success. By moving from reactive care to predictive intelligence, organizations can finally master the balance between patient health and financial risk. This technological edge is what allows modern healthcare enterprises to thrive in a competitive landscape.
Compliance and Security in VBC Platforms
Security is the foundation of trust for any healthcare enterprise. When building on top of Epic, your platform must protect sensitive data while allowing the right people to access it.
1. HIPAA and PHI data handling practices
Protecting patient health information (PHI) is a legal and ethical must. Therefore, every byte of data moving between Epic and your platform must be encrypted. This includes data “at rest” in your database and “in transit” across the network.
- Encryption Standards: Use AES-256 for stored data and TLS 1.2 or higher for transfers.
- Data Minimization: Only pull the specific patient fields needed for your risk models.
- Business Associate Agreements: Ensure all vendors sign formal HIPAA contracts.
- Secure Deletion: Have a clear policy for removing data when it is no longer required.
In addition, your team must undergo regular security training to prevent human error. Consequently, you reduce the risk of costly data breaches. High security standards are the first thing an investor looks for in a health tech platform.
2. Role-based access across care teams
In a large network, not everyone should see every piece of data. Therefore, your platform must use role-based access control (RBAC). This means a billing clerk sees different information than a heart surgeon.
- Clinician View: Full access to medical history and real-time risk scores.
- Care Manager View: Access to care gaps and social health data.
- Financial Officer View: Access to total cost and utilization reports only.
- Patient View: Access to their own personal health summaries.
Furthermore, these roles should sync directly with the existing permissions in Epic. This prevents the need for manual account setup for every new staff member. Consequently, your system remains organized and secure as the organization grows.
3. Audit trails for clinical and financial data
If a data point changes, you must know who changed it and why. Therefore, an immutable audit trail is essential for both clinical and financial records. This log tracks every login, data view, and modification made within the platform.
- Timestamping: Record the exact second an action occurs.
- User Identity: Link every action to a specific verified user account.
- Source Tracking: Note whether data came from Epic, a claim, or a manual entry.
- Alerting: Trigger notifications for suspicious or unauthorized access attempts.
In addition, these logs are vital during a formal government or payer audit. They prove that your organization follows strict data integrity rules. Furthermore, they help technical teams troubleshoot errors in the data pipeline quickly.
4. Secure API integrations with Epic systems
Connecting to Epic requires more than just a username and password. Therefore, you must use modern security protocols like OAuth 2.0 and OpenID Connect. These tools allow your platform to verify its identity without sharing secret credentials.
- Token-Based Access: Use short-lived tokens to pull data from Epic APIs.
- Scoped Permissions: Request access only to specific “scopes” like “Patient.Read.”
- API Gateways: Use a secure gateway to manage and monitor all incoming traffic.
- IP Whitelisting: Only allow data requests from known and trusted server addresses.
In addition, regularly rotating your security keys prevents unauthorized long-term access. This technical rigor ensures that your connection to the EHR remains a closed loop. Consequently, you protect the entire health system from external cyber threats.
5. Data governance across multi-org networks
Managing data across different hospitals requires a clear set of shared rules. Therefore, data governance defines how information is defined, collected, and shared. This is especially important when combining data from multiple Epic “instances” or different EHR brands.
- Master Data Management: Create a single definition for “active patient” or “high risk.”
- Data Stewardship: Assign individuals to be responsible for the quality of specific data sets.
- Consent Management: Track which patients have opted into sharing their data.
- Quality Metrics: Set benchmarks for data accuracy and completeness across all sites.
Furthermore, a strong governance framework prevents “data silos” from forming within the network. It ensures that everyone is playing by the same rules regardless of their location. Consequently, your analytics stay consistent and reliable across the entire enterprise.
A secure and compliant platform is a requirement for any value-based care investment. By mastering these security layers, you protect your patients and your financial interests at the same time.
How We Build the VBC Platform With Epic Integration
Building an enterprise-grade platform requires a disciplined and phased approach. At Intellivon, we follow a rigorous seven-step framework to ensure your Value-Based Care (VBC) solution is both technically sound and clinically impactful.
Step 1: Strategic Discovery and Roadmap Design
Every successful project begins with a clear understanding of your specific payer contracts and clinical goals. Therefore, we start by identifying the key performance indicators that drive your shared savings.
We analyze your existing Epic configuration to find potential data gaps early. In addition, we define the user personas who will interact with the platform daily. Consequently, this roadmap serves as our source of truth throughout the development process.
Step 2: Technical Architecture and Security Setup
Security is not an afterthought in healthcare technology. Therefore, we establish a HIPAA-compliant cloud environment with SOC2-grade encryption from day one. We configure the OAuth 2.0 handshake to allow for a secure connection with your Epic instance.
In addition, we set up the data governance rules that will manage information flow across your network. This solid foundation ensures that your patient data remains protected at every stage.
Step 3: Data Mapping and Pipeline Engineering
Moving data from Epic into a VBC engine requires precise mapping of clinical fields. We use HL7 and FHIR standards to ensure that lab results and diagnoses move without errors.
Therefore, we build automated pipelines that ingest ADT feeds and claims data in real-time. In addition, we implement identity resolution tools to match patients across different data sources. Consequently, your clinical team always works with a single, accurate patient record.
Step 4: Embedding Insights into Epic Workflows
A platform is only useful if doctors actually use it. Therefore, we use SMART on FHIR to embed our risk scores and care gaps directly into the Epic patient chart.
This prevents clinicians from having to log into a separate system to see vital information. In addition, we design custom “In-Basket” alerts to notify care managers of urgent events. Furthermore, these tools feel like a native part of the EHR experience.
Step 5: AI Integration and Risk Stratification
Once the data is flowing, we deploy our proprietary AI models to identify high-risk patient cohorts. These models analyze longitudinal history to predict future hospitalizations or rising costs. Therefore, you can move from reactive treatment to proactive population health management.
In addition, the AI identifies specific care pathways that offer the best clinical outcomes for the lowest cost. Consequently, your organization can optimize its resources with surgical precision.
Step 6: Rigorous Testing and Clinical Validation
We never “go live” without extensive testing in a non-production environment. Therefore, we perform end-to-end dry runs to ensure that every data trigger and alert works perfectly. We involve your lead clinicians in User Acceptance Testing (UAT) to gather feedback on the interface.
In addition, we stress-test the data pipelines to handle high-volume traffic without latency. This phase ensures the platform is reliable and ready for the high stakes of patient care.
Step 7: Deployment and Continuous Optimization
The final step is a phased rollout across your provider network. Therefore, we provide comprehensive training and support to ensure high adoption rates among staff. We monitor system performance and data accuracy in real-time to catch any early issues.
In addition, we use performance analytics to refine the AI models as more data becomes available. Consequently, your platform grows more valuable and effective with every passing month.
This seven-step process ensures that your investment in value-based care technology delivers measurable results. By combining technical expertise with a deep understanding of clinical workflows, Intellivon builds platforms that truly move the needle on health and finance.
Cost to Build VBC Platform with Epic Integration
At Intellivon, value-based care platforms are built as enterprise healthcare infrastructure, not as analytics dashboards layered onto Epic. The objective is to create a system that continuously ingests clinical and financial data, aligns it with VBC contracts, and drives outcome-based workflows across providers.
However, building a reliable VBC platform with Epic integration requires more than connecting APIs. It involves data normalization, identity resolution, real-time analytics, and contract-aware logic. As a result, healthcare organizations gain unified visibility into patient outcomes, cost performance, and care delivery efficiency.
Estimated Phase-Wise Cost Breakdown
| Phase | Description | Estimated Cost (USD) |
| Discovery & VBC Program Mapping | Define care models, contracts, KPIs, patient cohorts, and Epic data requirements | $8,000 – $15,000 |
| Epic Integration Planning & Access Setup | API strategy (FHIR/HL7), App Orchard alignment, data access approvals, integration design | $10,000 – $20,000 |
| Data Architecture & Pipeline Engineering | Build ingestion for ADT, clinical, and claims data with normalization and governance layers | $12,000 – $25,000 |
| Patient Identity & Record Unification | Implement MPI, patient matching logic, and longitudinal record creation across systems | $8,000 – $18,000 |
| Core VBC Module Development | Risk stratification, care gap detection, cost tracking, and provider performance modules | $15,000 – $30,000 |
| AI & Predictive Analytics Layer | Develop risk scoring models, utilization prediction, and readmission forecasting systems | $8,000 – $20,000 |
| Care Workflow & Automation Engine | Build contract-aware workflows, alerts, and escalation systems for providers | $7,000 – $15,000 |
| Security, Compliance & Audit Systems | Implement HIPAA controls, role-based access, audit logs, and secure Epic integrations | $5,000 – $12,000 |
| Testing, Deployment & Optimization | End-to-end testing, Epic validation, performance tuning, and production rollout | $5,000 – $10,000 |
Total Estimated Cost
$60,000 – $150,000+
What Drives Cost in Epic-Integrated VBC Platforms
- Epic Integration Complexity: Access layers, API limits, and App Orchard requirements directly impact effort. Deeper integrations increase cost.
- Data Fragmentation Across Systems: Combining Epic data with claims, labs, and external providers requires robust pipeline engineering.
- VBC Contract Complexity: More contract types (bundled payments, shared risk, capitation) increase workflow and logic complexity.
- Real-Time vs Batch Processing Needs: Real-time care gap detection and alerts require more advanced infrastructure than batch reporting systems.
- Scale of Patient Population: Larger populations require stronger data infrastructure, performance tuning, and analytics capabilities.
Cost Optimization Insight
Most healthcare organizations overspend by trying to build everything at once. Instead, Intellivon recommends a phased platform approach:
- Start with core VBC modules + Epic integration
- Then expand into AI, automation, and advanced analytics
This reduces upfront investment while accelerating time-to-value.
Talk to Intellivon’s experts for a tailored cost breakdown based on your VBC model, Epic environment, and integration scope.
Conclusion
Value-based care platforms demand infrastructure that aligns data, workflows, and outcomes. Epic provides the foundation, but true impact comes from how systems are extended, connected, and operationalized.
Therefore, healthcare organizations must think beyond tools and invest in scalable platforms. With the right architecture, they can improve outcomes, control costs, and succeed in value-driven models with long-term confidence.
Build an Epic-Integrated VBC Platform with Intellivon
At Intellivon, value-based care platforms are engineered as enterprise clinical and financial infrastructure, not as tools layered onto Epic. The goal is to create a unified platform that connects patient data, care workflows, and reimbursement models into a single, outcome-driven system.
Each platform is designed to support the full VBC lifecycle. This includes patient risk stratification, care gap detection, provider performance tracking, and contract-aware workflows. As a result, healthcare organizations gain real-time visibility into outcomes, costs, and operational efficiency across care networks.
Our approach focuses on FHIR-first, API-driven architectures combined with deep Epic integration expertise. This ensures seamless connectivity with Epic systems, external providers, labs, and payer systems, without disrupting existing clinical workflows.
Why Healthcare Leaders Choose Intellivon
- Built for Value-Based Models: Platforms align clinical workflows with financial outcomes and payer contracts.
- Deep Epic Integration Expertise: Proven experience with Epic APIs, HL7, FHIR, and App Orchard ecosystems.
- End-to-End Data Infrastructure: From ingestion to analytics, systems are designed for real-time decision-making.
- Scalable Across Care Networks: Architectures support multi-provider, multi-location healthcare environments.
- Compliance-First Engineering: HIPAA-ready systems with secure, audit-ready data handling at every layer.
Build Your VBC Platform with Confidence
Whether you are launching a new value-based program or scaling existing initiatives, Intellivon helps you design, integrate, and deploy platforms that deliver measurable outcomes.
Talk to Intellivon’s experts to plan your EHR-integrated VBC platform.
FAQs
Q1. What is a value-based care platform?
A1. A value-based care (VBC) platform is a system that helps healthcare providers track patient outcomes, manage costs, and align care delivery with payer contracts. It connects clinical, operational, and financial data to support outcome-based reimbursement models. As a result, providers can identify care gaps, improve patient outcomes, and reduce unnecessary spending across populations.
Q2. How does Epic support VBC programs?
A2. Epic supports VBC programs by acting as the central system of record for patient data. It provides access to clinical data, registries, and workflows needed for care management. In addition, Epic enables integration through FHIR APIs and HL7 interfaces. However, most VBC capabilities require extending Epic with external platforms for analytics, automation, and contract management.
Q3. How long does Epic integration take?
A3. Epic integration typically takes 8 to 16 weeks, depending on the scope and complexity. Basic integrations using FHIR APIs are faster, while deeper integrations involving multiple data sources, workflows, and real-time processing take longer. Therefore, timelines depend on data access approvals, integration depth, and the overall architecture of the VBC platform.
Q4. What data is needed for VBC platforms?
A4. VBC platforms require a combination of clinical, financial, and operational data. This includes patient records, diagnoses, lab results, claims data, utilization metrics, and provider performance data. Additionally, data from external systems such as labs, pharmacies, and wearables may be required. This unified dataset enables accurate risk scoring, care gap detection, and outcome tracking.
Q5. How much does it cost to build VBC software?
A5. The cost to build a VBC platform with Epic integration typically ranges from $60,000 to $150,000+. Costs vary based on integration complexity, number of modules, data infrastructure, and AI capabilities. For example, real-time analytics and multi-provider scaling increase development effort. As a result, most enterprises start with a core platform and expand over time.