Key Takeaways:
- Custom RCM software connects patient access, coding, claims, payments, and revenue analytics together.
- Administrative inefficiencies cost hospitals 15 to 30% of potential revenue every billing cycle.
- AI modules handle denial prediction, coding support, underpayment detection, and revenue forecasting automatically.
- Development costs range from $50,000 for basic MVPs to $200,000 for enterprise intelligence platforms.
- Intellivon builds modular RCM platforms that reduce leakage and scale with your operations.
Healthcare businesses operate across one of the most financially complex patient journeys in any industry. From the moment a patient registers to the final payment posted, every step in that journey carries revenue risk, and most organizations are managing that risk across disconnected billing tools that were never built to work together.
Missed eligibility checks, delayed prior authorizations, incomplete documentation, coding gaps, claim rejections, underpayments, and slow patient collections each contribute to a revenue problem that compounds across the cycle. This is why healthcare businesses are moving toward custom RCM software that connects the entire patient financial journey into one system.
Healthcare RCM software is becoming the financial operating system behind modern healthcare businesses. It connects patient access, coding, claims, denials, payments, collections, analytics, compliance, and AI-driven workflows so that revenue teams have the visibility and control to reduce leakage at every stage.
Intellivon builds healthcare RCM platforms for healthcare SaaS companies, RCM vendors, billing companies, clinics, hospitals, and enterprise care networks that need infrastructure that improves revenue visibility, reduces manual work, and scales with their operations. This blog draws from this experience and discusses how to build such software from the ground up.
Why Healthcare Businesses Build Custom RCM Software
Healthcare businesses are moving toward custom RCM software because off-the-shelf solutions cannot accommodate the operational complexity or financial stakes that modern revenue cycle management demands.
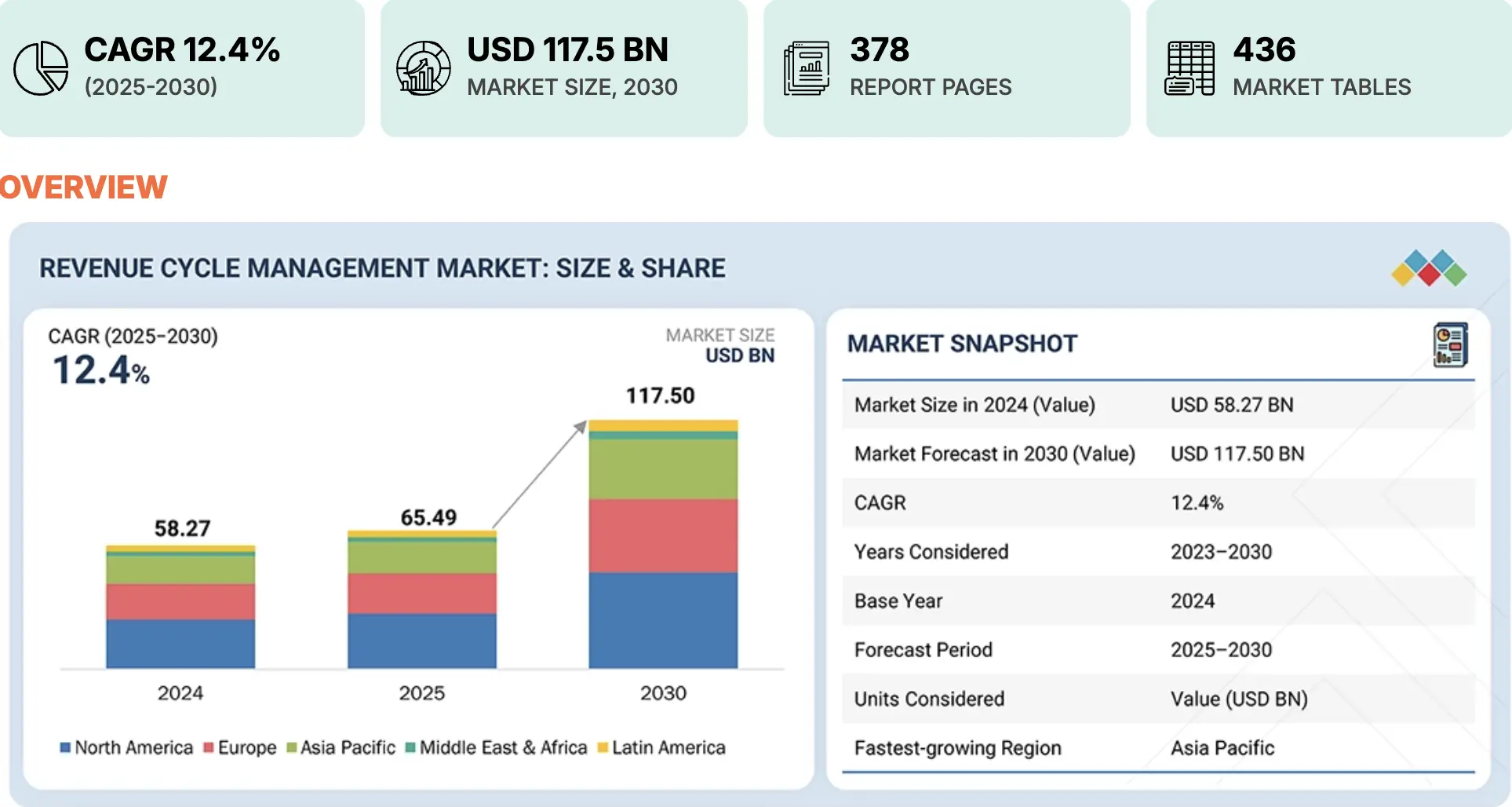
Off-the-shelf RCM solutions were built for the average provider. However, no two healthcare organizations operate the same way, and the financial consequences of that mismatch are measurable.
1. Revenue Cycle Costs Are Crushing Margins
Revenue cycle activities cost hospitals over USD 160 billion annually, with administrative expenses accounting for more than 40% of total hospital expenditures.
Organizations are consequently losing 15 to 30% of potential revenue to administrative inefficiencies, claim denials, and coding errors that generic software cannot adequately address.
2. EHR Integration Gaps Force Custom Builds
Most U.S. hospitals run on Epic or Cerner, yet their native billing modules lack the automation, AI capability, and real-time analytics that modern revenue management demands.
Custom RCM software fills that gap by combining EHR workflows with AI-driven claims automation and centralized payment collections.
3. Unique Payer Mixes Demand Tailored Solutions
Each organization faces distinct payer contracts, coding requirements, and denial patterns based on specialty and geography.
A Medicare-heavy community hospital has fundamentally different denial prevention needs than a specialty surgicenter managing commercial managed care. Custom platforms train on internal data to address those specific conditions.
4. Regulatory Compliance Requires Real-Time Updates
HIPAA, ICD-10/11, and CMS mandates evolve continuously.
Custom RCM platforms, therefore, maintain compliance through proactive rule engines, audit trails, and real-time payer rule updates, including CMS electronic prior authorization mandates effective January 2026.
As AI capabilities mature and regulatory complexity increases, custom RCM platforms will separate financially healthy health systems from those struggling to recover revenue in an increasingly challenging reimbursement landscape.
What Is Healthcare Revenue Cycle Management Software?
Healthcare revenue cycle management software is the financial infrastructure that connects every administrative, clinical, billing, payer, and payment workflow from the moment a patient schedules an appointment to the final payment posted against their account.
RCM software begins before care is delivered and ends after collections close. It manages:
- Patient access: registration, eligibility verification, and prior authorization
- Clinical documentation: coding support, charge capture, and documentation validation
- Claims management: claim scrubbing, submission, and payer adjudication
- Denial and appeals: denial tracking, root cause analysis, and appeal workflows
- Payment and collections: payment posting, patient billing, and balance resolution
- Revenue analytics: visibility into A/R, denial trends, collection rates, and cash flow
RCM software does not just organize billing workflows. Instead, it directly controls how quickly and completely a healthcare organization recovers the revenue it has already earned.
RCM Software Vs Medical Billing Software
Healthcare Revenue Cycle Management (RCM) software acts as the financial engine for modern medical enterprises by automating the entire patient journey from registration to final payment.
This comprehensive system manages clinical and administrative data to ensure providers receive accurate compensation for their services.
| Feature | Medical Billing Software | Healthcare RCM Software |
| Primary Focus | Submitting claims and tracking payments | Managing the entire financial lifecycle |
| Scope | Back-end administrative tasks | Front-end and back-end integration |
| Functionality | Basic coding and billing | AI-driven analytics and denials management |
| Goal | Getting paid for a specific visit | Improving overall enterprise profitability |
While medical billing tools handle simple transactions, RCM platforms provide the strategic infrastructure required to manage complex financial health. Choosing the right architecture allows organizations to minimize revenue leakage and maximize operational efficiency.
Front-End RCM Features Preventing Revenue Leakage
Financial success in healthcare starts long before a doctor sees a patient. Most claim denials stem from simple administrative errors during the initial contact phase.
By implementing robust front-end features, enterprises stop revenue leakage at the source rather than chasing lost funds months later.
1. Patient Scheduling And Intake
Modern scheduling systems do more than just book time slots on a calendar. They serve as the first point of data entry where accuracy is paramount for future billing success.
- Appointment Scheduling: Automated systems allow patients to book visits based on real-time provider availability.
- Provider Mapping: The software ensures the selected service aligns with the specific credentials and contracts of the attending physician.
- Intake Form Automation: Digital forms eliminate manual data entry errors by allowing patients to input their own history and visit reasons securely.
This digital foundation creates a clean patient profile from the start. Consequently, staff members spend less time correcting typos and more time focused on patient care. Integrating these workflows ensures every visit reason maps correctly to a billable service code.
2. Patient Demographic And Insurance Capture
Capturing precise identity and coverage details is the most effective way to prevent identity fraud and billing mismatches. Precise data collection at this stage ensures the payer can identify the member immediately.
- Primary Data Points: The system captures names, dates of birth, and contact details with mandatory field validation.
- Insurance Card Imaging: Mobile uploads or scanners extract policy and group numbers directly from the physical card.
- Duplicate Profile Detection: Advanced algorithms flag similar records to prevent the creation of fragmented medical or financial histories.
Maintaining a single source of truth for patient identity is vital for enterprise scalability. When demographic data remains consistent, the likelihood of a “patient not found” denial drops significantly.
3. Eligibility And Benefits Verification
Verifying coverage in real-time prevents the provider from performing services that the insurance company will not cover. This feature connects directly to payer portals to fetch the most current benefit data.
- Real-Time Status: Instantly confirm if a policy is active or has recently lapsed.
- Financial Breakdowns: Identify specific copays, remaining deductibles, and coinsurance percentages for the scheduled service.
- Exception Alerts: The software flags plan limitations or benefit caps before the patient arrives at the clinic.
Automating this check removes the burden of manual phone calls to insurance companies. Therefore, the administrative team can address coverage issues with the patient before the appointment begins.
4. Prior Authorization Triage
Failing to secure prior authorization is a leading cause of high-value claim denials. A strategic RCM platform identifies which services require a green light from the payer and manages the workflow accordingly.
- Payer Rule Engine: The software automatically identifies procedures that require pre-approval based on the specific insurance plan.
- Document Routing: It gathers clinical notes and required forms to send them to the authorization team or the payer directly.
- Status Tracking: Dashboard views show the real-time progress of every request to ensure no patient is treated without a valid authorization number.
5. Patient Responsibility Estimation
Financial transparency builds trust and increases the likelihood of full payment. By providing an accurate cost estimate, organizations help patients plan for their medical expenses.
- Out-of-Pocket Calculation: The system combines the contracted payer rate with the patient’s specific benefit levels to predict the final bill.
- Payment Planning: Staff can offer structured plans for high-cost procedures based on the generated estimate.
- Transparency Reports: Digital summaries explain exactly why a patient owes a specific amount, reducing future billing disputes.
6. Pre-Visit Payment Collection
Collecting payments at the point of service is significantly more effective than sending invoices through the mail. Digital tools simplify this process by offering flexible payment options.
- Digital Links: Patients receive secure SMS or email links to pay their copay or deductible before their arrival.
- Installment Setup: For larger balances, the system can automate recurring monthly charges.
- Automated Receipts: Instant digital confirmations ensure the patient has a record of the transaction for their own files.
By securing funds early, enterprises improve their cash on hand and reduce the cost of collections. This proactive approach turns the front desk into a vital part of the revenue cycle.
Mid-Cycle RCM Features For Charge Accuracy
Revenue integrity depends entirely on the transition from clinical care to financial data. Mid-cycle healthcare RCM processes ensure that every medical service is documented accurately and translated into the correct billable codes.
Errors in this phase often lead to expensive audits or permanent revenue loss. Consequently, enterprise leaders prioritize mid-cycle software to bridge the gap between the exam room and the billing office.
1. Clinical Documentation Review
Detailed clinical documentation is the foundation of any successful healthcare RCM strategy. If a service is not documented properly, it cannot be billed legally. Software at this stage acts as a safety net for busy providers.
- Missing Documentation Alerts: The system flags encounters where a provider has not finished their notes.
- Medical Necessity Checks: It analyzes whether the documented symptoms justify the performed procedures based on payer rules.
- Provider Note Completeness: AI tools scan for specific keywords required to support high-level billing codes.
- Documentation-to-Code Matching: The software verifies that the written narrative supports the selected diagnosis.
These tools reduce the administrative burden on physicians. However, they also ensure that the organization remains compliant with federal and private payer regulations.
2. AI-Assisted Medical Coding
Manual coding is slow and prone to human error. Modern healthcare RCM platforms use AI to suggest the most accurate codes while maintaining a human-in-the-loop approach for quality control.
- Code Recommendations: The system suggests CPT, ICD-10, and HCPCS codes based on clinical documentation.
- Modifier Recommendations: It identifies when a specific modifier is needed to explain special circumstances to the payer.
- Human Review Integration: Certified coders can quickly approve or edit AI suggestions through an intuitive interface.
- Coding Audit Trail: Every change is logged to provide a transparent history for future compliance reviews.
3. Charge Capture Automation
Missing charges are a silent killer of healthcare profitability. Charge capture automation ensures that every consumable item and every minute of provider time is accounted for in the final claim.
- Encounter-to-Charge Mapping: The software automatically links clinical activities to their corresponding financial charges.
- Missed Charge Alerts: It identifies “forgotten” items, such as an injection billed without the accompanying medication code.
- Duplicate Detection: The system flags identical charges submitted for the same encounter to prevent fraudulent billing.
- Specialty Rules: Custom logic applies different rules for surgery, radiology, or primary care to ensure accuracy across departments.
4. Coding Work Queues
Efficiently managing a team of coders requires a structured digital environment. Work queues allow managers to direct resources where they are needed most.
- Task Assignment: The system automatically routes specific cases to coders based on their expertise or current workload.
- High-Value Prioritization: Claims with the highest dollar amounts move to the front of the line to optimize cash flow.
- Productivity Tracking: Leaders can monitor how many charts each coder completes per hour.
- Case Escalation: Incomplete or confusing cases are moved to senior auditors for a second look.
5. Diagnosis And Procedure Validation
Before a claim leaves the building, it must undergo a rigorous validation process. This step confirms that the diagnosis and the procedure make sense together in the eyes of the payer.
- Code Compatibility: The software checks if the selected codes are allowed to be billed together on the same day.
- Alignment Checks: It ensures the procedure performed is a recognized treatment for the diagnosed condition.
- Payer-Specific Edits: The system applies unique rules for Medicare, Medicaid, and private insurers to avoid immediate rejections.
6. Claim Readiness Scoring
Think of claim readiness scoring as a final inspection before shipping a product. It gives administrators a clear “go” or “no-go” signal for every claim.
- Readiness Scores: Every claim receives a numerical score based on its likelihood of being paid on the first submission.
- Risk Flagging: The system highlights risky coding combinations that might trigger an audit.
- Gap Identification: It points out missing fields or documentation that would cause an immediate denial.
Therefore, the billing team only spends time on claims that are truly ready. This precision significantly increases the clean claim rate and reduces the time spent on rework.
Back-End RCM Features For Claims And Collections
The back-end phase represents the critical moment when clinical efforts transform into realized capital. Efficient healthcare RCM systems manage a complex web of communication between providers, payers, and patients.
Success here requires a relentless focus on detail and a proactive approach to recovering every dollar owed. Consequently, top-tier platforms prioritize visibility and automated workflows to handle the high volume of transactions typical in enterprise settings.
1. Claim Creation And Scrubbing
Before a claim ever reaches a payer, it must undergo a rigorous “scrubbing” process to ensure it meets every technical requirement. This internal audit prevents simple errors from turning into costly delays.
- Claim Generation: The system automatically compiles all clinical and demographic data into the standard industry format.
- Payer Rule Validation: It checks the claim against a massive library of specific insurance company rules.
- Error Alerts: If a required field is blank or a code is invalid, the software stops the process and alerts the billing team.
- Duplicate Detection: The platform identifies identical claims to prevent redundant submissions that could flag an account for fraud.
2. Clearinghouse Submission
The clearinghouse acts as the digital post office for healthcare transactions. Seamless integration with this intermediary ensures that claims move swiftly and securely to their destination.
- Electronic Submission: The software transmits batches of claims instantly, reducing the time spent on manual uploads.
- Batch Processing: Thousands of records can be processed simultaneously, ensuring enterprise-level scalability.
- Rejection Handling: If a clearinghouse identifies an issue, the error is fed back into the healthcare RCM dashboard for immediate correction.
- Payer Acknowledgment: The system tracks the exact second a payer receives the claim, providing a clear audit trail.
3. Claim Status Tracking
Visibility is the enemy of stagnant revenue. Advanced tracking allows leaders to see exactly where every dollar sits in the pipeline at any given moment.
- Status Categories: Claims are tagged as Submitted, Accepted, Rejected, Pending, Denied, Paid, Appealed, or Closed.
- Real-Time Updates: The dashboard refreshes as payers process the data, removing the need for manual status checks.
- Workflow Integration: Changing a status can trigger automated next steps, such as moving a denied claim to an appeal queue.
4. Denial Classification
Not all denials are equal. Sophisticated healthcare RCM software categorizes rejections so that teams can focus on the most impactful issues first.
- Reason Code Analysis: The system reads standard CARC and RARC codes to explain exactly why a payer refused a claim.
- Root-Cause Grouping: It identifies patterns, such as a specific doctor consistently failing to provide necessary clinical notes.
- Preventable vs. Non-Preventable: The software separates internal process errors from complex payer disputes.
- Priority Ranking: High-value denials are moved to the top of the work list to protect the largest revenue streams.
5. Appeal Workflow Management
When a payer denies a legitimate claim, the appeal process must be swift and documented perfectly. This module manages the administrative burden of fighting for reimbursement.
- Task Creation: The system automatically assigns a denial to the appropriate specialist for review.
- Document Collection: It gathers the original claim, the denial notice, and the necessary clinical records into a single digital folder.
- Deadline Tracking: Automated alerts ensure that no appeal window is missed due to human oversight.
- Outcome Tracking: The software monitors the success rate of appeals to help refine future submission strategies.
6. Payment Posting And ERA/EOB Processing
Reconciling payments is a high-volume task that is ripe for automation. Accurate posting ensures that financial records reflect the true state of the business.
- Electronic Remittance Advice (ERA): The system automatically ingests digital payment files from payers.
- Explanation of Benefits (EOB): It matches paper or digital EOBs to the corresponding patient accounts.
- Adjustment Tracking: The software records contractual write-offs and patient balances with pinpoint accuracy.
- Exception Handling: Any payments that do not match the expected amount are flagged for manual review.
7. Underpayment Detection
Payers do not always pay the full contracted rate. Underpayment detection ensures that providers are not leaving money on the table due to silent payer errors.
- Contracted Rate Comparison: The system compares every payment against the specific fee schedule stored in the database.
- Variance Alerts: If a payer pays even one percent less than the contract dictates, the software flags the discrepancy.
- Recovery Queues: These underpayments are routed to a dedicated team focused on recovering the missing funds.
8. Patient Billing And Collections
As high-deductible plans become more common, the patient has become a significant payer. This final step in the healthcare RCM cycle focuses on professional and effective communication.
- Digital Statements: Patients receive clear, easy-to-read invoices via email or secure portals.
- Payment Links: Embedded “Pay Now” buttons allow for instant settlement of balances.
- Installment Plans: The system manages recurring monthly payments for patients with high out-of-pocket costs.
- Communication Tracking: Every text, email, and phone call is logged to ensure a consistent and respectful patient experience.
Investing in high-grade RCM infrastructure transforms financial uncertainty into a scalable engine for business growth.
Core Modules Of Healthcare RCM Software
A robust healthcare RCM system functions as a modular ecosystem where each component addresses a specific financial risk.
By segmenting the revenue cycle into specialized modules, enterprises can pinpoint operational bottlenecks and deploy targeted automation. This structural approach ensures that the transition from a clinical appointment to a financial asset is seamless and transparent.
| RCM Module | What It Does | Business Value |
| Patient Intake | Captures patient and insurance data | Reduces front-end errors |
| Eligibility Verification | Checks coverage and benefits | Prevents avoidable claim issues |
| Prior Authorization | Tracks authorization needs and status | Reduces approval delays |
| Coding Support | Helps coders validate codes | Improves claim accuracy |
| Claim Scrubbing | Checks claims before submission | Improves clean claim rate |
| Denial Management | Routes and tracks denied claims | Improves recovery speed |
| Payment Posting | Matches payments with claims | Reduces reconciliation work |
| Patient Billing | Manages patient balances | Improves collections |
| Analytics | Tracks revenue KPIs | Improves financial visibility |
Selecting a platform with these core modules allows a business to maintain high financial integrity across multiple departments.
When these modules communicate effectively, the organization benefits from a significantly lower cost to collect and a more predictable revenue stream.
Prior Authorization Built Into Modern RCM Software
Modern healthcare RCM software must address the complexities of prior authorizations to prevent high-value claim rejections. New regulatory standards demand that these workflows move away from manual faxes and toward automated, real-time data exchange.
By integrating these checks directly into the billing cycle, enterprises ensure clinical services are pre-approved for reimbursement.
1. Prior Authorization Requirement Detection
The system automatically cross-references the planned procedure with the patient’s specific insurance policy to determine if an approval is necessary. This prevents the provider from performing services that might later be deemed “unauthorized” by the payer.
- Payer Rule Matching: The software checks the unique plan, provider credentials, and service codes against a live database of insurer requirements.
- Real-Time Alerts: Staff receive an immediate notification if a scheduled appointment requires a green light from the insurance company.
- Proactive Triage: By catching these requirements during the scheduling phase, the organization avoids last-minute cancellations or unpaid visits.
2. Required Documentation Checklist
Gathering the correct clinical evidence is the most time-consuming part of the authorization process. A modern platform provides a clear roadmap of exactly what the payer needs to approve the request.
- Clinical Justification: The system identifies necessary medical notes and lab reports required to prove the procedure is medically necessary.
- Comprehensive File Management: It organizes imaging records, referral forms, and insurance documents into a single submission packet.
- Accuracy Checks: Automated validation ensures that no document is missing before the request is transmitted to the payer.
3. Authorization Request Tracking
Transparency is vital when managing dozens of pending approvals. A centralized dashboard allows the administrative team to monitor the status of every request without logging into multiple payer portals.
- Lifecycle Statuses: Requests are categorized as Submitted, Pending, Approved, Denied, Expired, or “Additional Information Requested.”
- Expiry Alerts: The software warns staff when an approved authorization is nearing its end date so they can re-request it if needed.
- Status Syncing: Real-time updates ensure the clinical team knows exactly when they can proceed with the scheduled treatment.
4. Authorization-To-Claim Matching
Even with an approval, a claim can still be denied if the authorization number is not recorded correctly on the final bill. This module automates the link between the two to ensure financial accuracy.
- Automated Linking: The system pulls the valid authorization number directly into the corresponding claim fields.
- Submission Guards: It prevents any claim from being sent if a required authorization is missing or has already expired.
- Denial Prevention: This simple check virtually eliminates the “no authorization” denial category, which is traditionally one of the most expensive errors to fix.
5. FHIR-Based Prior Authorization API Readiness
Interoperability is the future of healthcare finance. Utilizing the Fast Healthcare Interoperability Resources (FHIR) standard allows for direct, secure communication between providers and insurance companies.
- API-Driven Exchange: Data flows directly between the RCM software and the payer’s system, bypassing slow manual portals.
- Documentation Transfer: Large clinical files move instantly, reducing the turnaround time for high-stakes medical decisions.
- Interoperability Standards: Adopting FHIR ensures the enterprise remains compliant with the CMS 2027 mandates for electronic data exchange.
These integrated features turn prior authorization from a logistical nightmare into a streamlined, predictable part of the business. Consequently, enterprises can focus on patient outcomes while the software secures the underlying revenue.
Healthcare Data Standards Used In RCM Software Development
Technical credibility in the healthcare sector rests on the seamless integration of various data standards. These protocols ensure that financial information remains consistent across different systems, platforms, and payer environments.
Without these standards, the modern healthcare RCM ecosystem would collapse under the weight of incompatible data formats.
1. HL7 For Healthcare Data Exchange
Health Level Seven (HL7) serves as the traditional backbone for exchanging clinical and administrative data. It allows different software applications, such as EHRs and billing systems, to share vital patient information.
- Encounter Data: It transmits the essential details of a patient’s visit to the billing office.
- System Integration: This standard enables legacy hospital systems to communicate with modern financial platforms.
- Patient Demographics: HL7 messages carry the core identity data required to start the revenue cycle.
2. FHIR For Modern API-Based Interoperability
Fast Healthcare Interoperability Resources (FHIR) represent the next generation of data exchange. Unlike legacy standards, FHIR uses a modern API approach that makes it easier to share specific pieces of information, such as prior authorization status or insurance coverage.
- Resource-Based Architecture: It allows developers to request specific “resources” like a patient’s coverage rather than an entire medical record.
- Payer-Provider Workflows: This standard facilitates the real-time communication required for 2027 CMS compliance.
- Modern Accessibility: FHIR is built for mobile and cloud-based environments, ensuring high-speed data access.
3. X12 EDI For Claims And Payment Transactions
Electronic Data Interchange (EDI) is the specific language used for the actual submission of claims. The X12 standard ensures that every financial transaction between a provider and a payer follows a strict, predictable format.
- 837 Claims: This is the standard format for submitting healthcare claims electronically.
- 270/271 Eligibility: These transactions allow the system to check if a patient is covered in real time.
- 835 Remittance: Payers use this format to send payment details and denial reasons back to the provider.
4. ICD, CPT, And HCPCS Code Sets
Universal coding sets allow the entire industry to speak the same language regarding medical conditions and treatments. Accurate use of these codes is the primary requirement for getting paid the correct amount.
- ICD-10: These codes describe the patient’s diagnosis or medical condition.
- CPT: These codes identify the specific medical procedures performed by the provider.
- HCPCS: This set covers medical supplies, durable equipment, and services not found in CPT.
5. ERA And EOB Data
Electronic Remittance Advice (ERA) and Explanation of Benefits (EOB) are the documents that explain what was paid and why. Handling this data correctly is the key to accurate financial reconciliation.
- Adjustment Tracking: These files show contractual write-offs and any discounts applied by the payer.
- Denial Reasons: They contain standardized codes that explain exactly why a claim was rejected.
- Patient Responsibility: The system uses this data to calculate the final bill for the patient.
6. Secure REST And GraphQL APIs
While healthcare-specific standards handle the clinical data, modern web APIs manage the internal workings of the RCM platform. These tools allow for fast, flexible, and secure development.
- Partner Integrations: REST APIs allow the RCM software to connect with third-party tools like payment gateways.
- Analytics Services: GraphQL allows dashboards to fetch complex financial datasets efficiently without overloading the system.
- Platform Security: These APIs utilize secure authentication to ensure that sensitive financial data is only accessible to authorized users.
Implementing these standards ensures that an RCM platform is both legally compliant and technically scalable. Therefore, enterprises can build a future-proof infrastructure that adapts to the changing demands of healthcare finance.
Healthcare RCM Software Integrations You Need
No healthcare RCM platform can operate as an island in a modern medical enterprise. Success requires a deep, bi-directional flow of data between various clinical and financial systems to ensure data integrity.
These integrations eliminate the need for manual data entry, which is the primary cause of administrative errors and revenue leakage.
1. EHR And EMR Integrations
Integrating with Electronic Health Records (EHR) is the most critical step for any revenue cycle strategy. This connection allows the billing system to pull clinical evidence directly from the provider’s notes to support every claim.
- Major Platforms: The system should offer native connectors for Epic, Oracle Health/Cerner, Athenahealth, eClinicalWorks, and Practice Fusion.
- Data Synchronization: It must capture patient demographics, encounter data, and detailed clinical notes in real time.
- Custom Environments: Support for custom or specialty-specific EHRs ensures the platform can scale with unique enterprise needs.
2. Practice Management System Integrations
Practice management tools handle the operational pulse of the facility. Linking these with your healthcare RCM software ensures that the front office and the back office are always in sync.
- Workflow Alignment: Scheduling and appointment data flow directly into the billing queue to prepare for eligibility checks.
- Resource Mapping: The integration matches specific providers to their contracted insurance entities to ensure valid claims.
- Account Visibility: Staff can view patient balances and billing history directly within the scheduling interface.
3. Clearinghouse Integrations
The clearinghouse is the gateway to the insurance world. A direct integration streamlines the submission process and provides immediate feedback on the technical health of your claims.
- EDI Workflows: The system manages the electronic data interchange for claim submissions, rejections, and eligibility requests.
- Real-Time Feedback: It pulls claim status and Electronic Remittance Advice (ERA) files directly back into the RCM dashboard.
- Error Handling: Instant rejection alerts allow the billing team to fix and resubmit claims within minutes instead of days.
4. Payer API And Portal Integrations
Modern RCM platforms are moving away from manual portal logins. Direct API connections with major payers allow for instant verification of benefits and faster claim processing.
- Benefit Deep-Dives: Access granular details on copays, deductibles, and specific plan limitations without leaving the platform.
- Prior Authorization: Automate the submission of authorization requests and track their progress through direct payer links.
- Denial Intelligence: Fetch detailed denial reasons and payment statuses to accelerate the appeal process.
5. Payment Gateway Integrations
Simplifying the payment process for patients is the fastest way to improve collection rates. Integrating secure payment gateways allows for flexible, consumer-friendly financial interactions.
- Flexible Collections: Support for copayments, payment links via SMS, and structured installment plans for high balances.
- Automated Reconciliation: Every transaction is automatically matched to the patient’s ledger to ensure accurate accounting.
- Financial Safety: Secure processing of refunds and credits maintains patient trust and financial compliance.
6. Document Management Integrations
Healthcare RCM involves a massive volume of physical and digital paperwork. A centralized document management integration ensures that every claim is backed by the necessary proof.
- Evidence Storage: Securely store and link insurance cards, medical records, and imaging files to specific patient encounters.
- Appeal Support: The system automatically bundles authorization files and EOBs when drafting an appeal letter.
- Clinical Attachments: Seamlessly transmit required documentation to payers alongside the electronic claim.
7. Accounting And ERP Integrations
The final step in the revenue cycle is translating medical billing into enterprise financial health. Integrating with accounting and ERP systems ensures that the CFO has a clear view of the bottom line.
- Revenue Recognition: The software identifies earned revenue versus pending claims to provide accurate financial forecasting.
- AR Management: Detailed accounts receivable data flows into the general ledger for streamlined month-end closing.
- Enterprise Dashboards: High-level reporting tools combine clinical and financial data to show the true cost to collect.
By prioritizing these integrations, organizations create a cohesive digital environment that supports growth. This interconnected strategy reduces the administrative burden on staff and ensures a more predictable cash flow for the entire enterprise.
Healthcare RCM Software Development Process
Building an enterprise-grade healthcare RCM platform requires a rigorous, phased approach that balances technical precision with clinical reality. Our development methodology focuses on creating a high-performance financial engine that eliminates manual friction.
By following a structured lifecycle, we ensure that the final product is compliant, scalable, and deeply integrated into the provider’s daily operations.
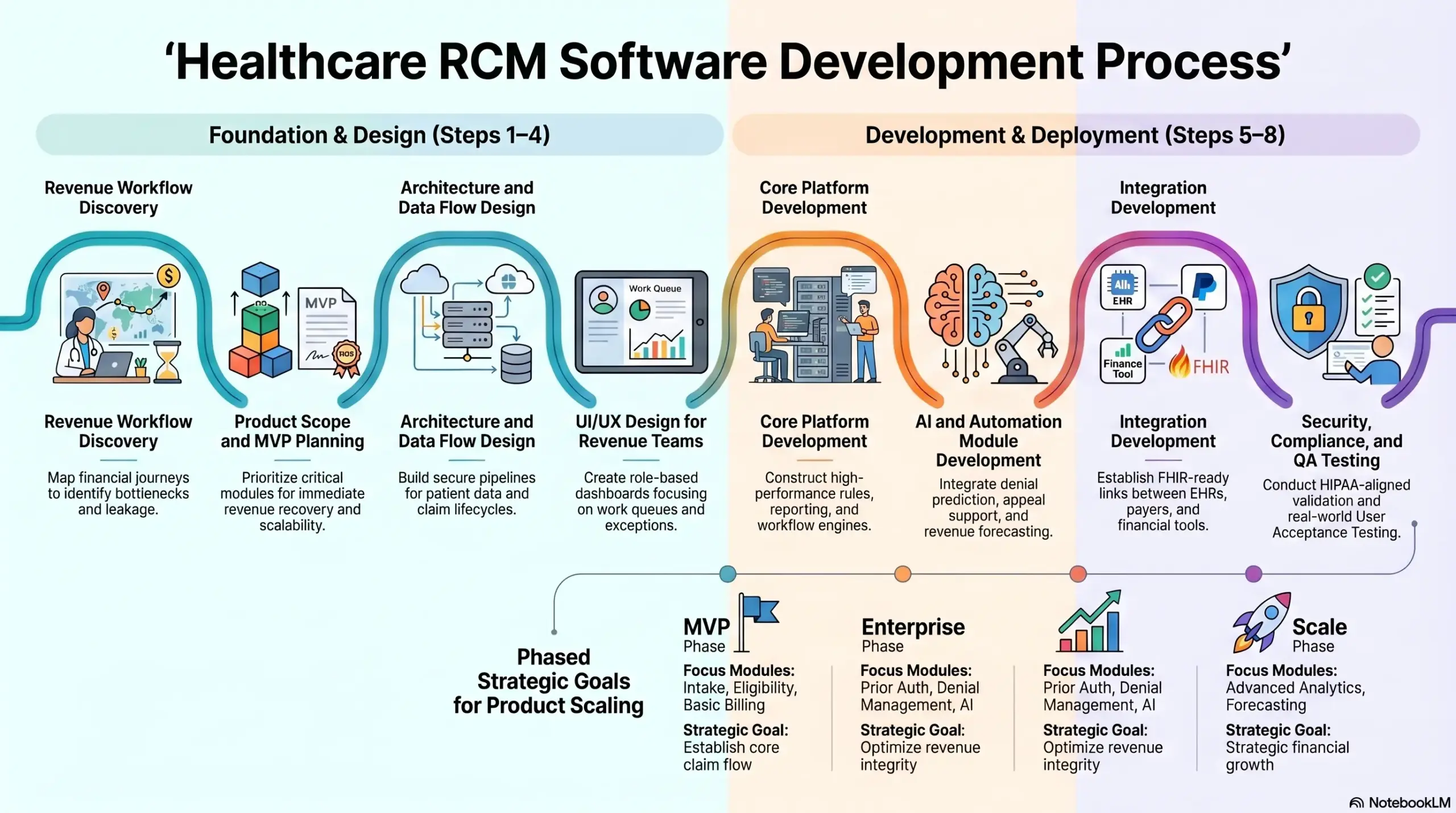
Step 1: Revenue Workflow Discovery
We begin by mapping the entire financial journey to identify where capital is being lost. This discovery phase allows us to build a solution that addresses specific institutional bottlenecks rather than applying a generic template.
- Workflow Audit: We analyze current intake, coding, and billing processes to find manual workarounds that slow down the cycle.
- Leakage Assessment: Our team identifies common denial reasons and payer mix challenges that impact the bottom line.
- User Role Mapping: We define the specific needs of registrars, coders, and billers to ensure the software supports their unique tasks.
Step 2: RCM Product Scope And MVP Planning
Strategic planning ensures that the most critical financial modules are prioritized for early impact. We create a roadmap that balances immediate revenue recovery with long-term enterprise scalability.
| Phase | Focus Modules | Strategic Goal |
| MVP | Intake, Eligibility, Basic Billing | Establish core claim flow |
| Enterprise | Prior Auth, Denial Management, AI | Optimize revenue integrity |
| Scale | Advanced Analytics, Forecasting | Strategic financial growth |
Step 3: Architecture And Data Flow Design
A robust architecture is the only way to handle the massive data volumes inherent in healthcare. We design high-speed data pipelines that manage the movement of sensitive information between patients, providers, and payers.
- Patient Data Flow: Secure pathways for demographic and clinical data from the EHR to the billing engine.
- Claim Lifecycle: Logic that tracks a claim from initial creation through submission, adjudication, and final payment.
- Audit Trail: Immutable logs for every data change to ensure complete transparency for compliance and internal reviews.
Step 4: UI/UX Design For Revenue Teams
Efficient billing requires a clean interface that highlights exceptions rather than overwhelming users with data. Our designs focus on role-based dashboards that prioritize high-value tasks and urgent deadlines.
- Work Queues: Intelligent lists that sort claims by urgency, dollar value, or denial type.
- Exception Handling: Visual alerts that point specifically to the error on a claim, reducing research time.
- Manager Views: High-level heatmaps that show department-wide productivity and outstanding accounts receivable.
Step 5: Core Platform Development
The core platform serves as the central brain of the RCM operation. We build high-performance backends and flexible rules engines that can adapt to changing payer requirements without requiring a full code rewrite.
- Rules Engine: A customizable framework that allows administrators to update payer-specific billing rules on the fly.
- Reporting Engine: Specialized databases designed for lightning-fast retrieval of complex financial KPIs.
- Workflow Engine: Automation logic that moves claims through the system based on their current status and required actions.
Step 6: AI And Automation Module Development
We integrate intelligence directly into the workflow to move from reactive billing to predictive revenue management. These modules use machine learning to identify patterns that standard algorithms miss.
- Denial Prediction: AI models that score claims based on their likelihood of being rejected by specific payers.
- Appeal Support: Tools that automatically summarize denial reasons and suggest the most effective clinical arguments for recovery.
- Revenue Forecasting: Predictive analytics that model future cash flow based on historical payment timelines and seasonal trends.
Step 7: Integration Development
Interoperability is the hallmark of a successful RCM deployment. We build secure, FHIR-ready connectors that link the financial platform to the broader healthcare ecosystem.
- Clinical Links: Bi-directional integrations with EHRs like Epic and Cerner for seamless documentation capture.
- Payer Gateways: Direct API links to insurance portals for real-time eligibility and claim status updates.
- Financial Tools: Connections to payment gateways and accounting ERPs to ensure the general ledger is always accurate.
Step 8: Security, Compliance, And QA Testing
Security is embedded into every layer of our development process. We conduct rigorous testing to ensure the platform meets all HIPAA standards and protects sensitive financial data.
- HIPAA-Aligned Testing: Validating that all data at rest and in transit is encrypted and access is strictly controlled.
- API Security: Stress-testing every integration point to prevent unauthorized data access or leaks.
- User Acceptance (UAT): Real-world testing with actual billing teams to ensure the software solves their practical daily challenges.
By following this precise development lifecycle, we transform fragmented financial tasks into a unified, high-output revenue machine. This methodology ensures that every line of code serves the ultimate goal of maximizing provider profitability and operational efficiency.
How Much Does Healthcare RCM Software Development Cost?
Estimating the investment for healthcare RCM software requires balancing immediate feature requirements with long-term enterprise scalability. The total cost fluctuates based on the depth of AI integration, the complexity of payer rules, and the number of external system connections.
Therefore, decision-makers must view these figures as a roadmap for aligning technical investment with expected revenue recovery.
| Software Scope | Estimated Cost | Best For |
| Basic RCM MVP | $50,000–$80,000 | Clinics, startups, and focused billing automation |
| Mid-Level RCM Platform | $80,000–$130,000 | Billing companies, specialty practices, RCM vendors |
| AI-Powered RCM Software | $130,000–$170,000 | Healthcare SaaS, hospitals, multi-location providers |
| Enterprise RCM Intelligence | $170,000–$200,000 | Health systems, large RCM companies, complex teams |
1. Basic RCM MVP Cost
A Minimum Viable Product focuses on the foundational elements of the revenue cycle. This entry-level investment is designed to digitize manual processes and establish a clean data flow for small to mid-sized clinical operations.
- Core Intake: Digital patient registration and insurance card data capture.
- Eligibility Checks: Basic real-time verification of insurance coverage status.
- Claim Tracking: A central dashboard to monitor the status of submitted claims.
- Reporting: Simple financial summaries to track monthly billing performance.
2. Mid-Level RCM Platform Cost
Mid-level solutions introduce advanced automation and specialized work queues to handle higher claim volumes. This tier is ideal for organizations looking to reduce their days in accounts receivable through more aggressive denial management.
- Claim Scrubbing: Automated rule engines that check for errors before submission.
- Denial Management: Tools to categorize, route, and track rejected claims for faster recovery.
- Payment Posting: Automated matching of payer remittances to patient accounts.
- Clearinghouse Integration: Seamless electronic data interchange for batch claim processing.
3. AI-Powered RCM Software Cost
Investing in AI moves the platform from tracking revenue to predicting and protecting it. This cost reflects the development of custom machine learning models trained on historical billing data.
- Denial Prediction: AI scoring to identify high-risk claims before they are sent.
- Coding Support: Natural language processing to suggest accurate codes from clinical notes.
- Prior Authorization Support: Intelligent tracking of approval needs to prevent unauthorized service denials.
- Underpayment Detection: Automated variance analysis to flag when payers underpay contracted rates.
4. Enterprise RCM Intelligence Platform Cost
At the enterprise level, the software must manage complex, multi-entity environments with diverse payer contracts. This high-scale deployment focuses on deep interoperability and sophisticated financial governance.
- Multi-Entity Support: Centralized management for health systems with multiple locations and departments.
- AI Governance: Advanced controls for managing automated decision-making and compliance risks.
- Revenue Forecasting: Predictive models that project future cash flow based on macro-level payment trends.
- Custom Payer Workflows: Bespoke automation logic designed around the specific requirements of major national insurers.
While the initial development cost is a significant factor, the long-term ROI is found in the reduction of lost revenue and administrative overhead. Consequently, a well-planned RCM platform often pays for itself through improved clean claim rates and faster reimbursement cycles.
How To Use AI Safely In Healthcare RCM Software
Deploying AI within the revenue cycle requires a balanced approach between automation and clinical oversight. While AI significantly increases efficiency, it must operate within a framework of safety and transparency to prevent financial or compliance risks.
Establishing these guardrails ensures that technology serves as a reliable co-pilot for your billing and administrative teams.
1. Keep Humans In The Loop
The most effective healthcare RCM strategies use AI to augment human expertise rather than replace it. This ensures that complex cases involving medical nuance receive the necessary professional judgment before final submission.
- AI Suggestion Logic: The system provides recommendations for coding or denial responses that staff can quickly verify.
- Professional Responsibility: Certified coders and billing specialists remain the final authority on all claims and appeals.
- Approval Workflows: High-value transactions or sensitive patient communications require a manual “sign-off” to move forward in the cycle.
2. Make AI Recommendations Explainable
For AI to be useful, users must understand the logic behind its suggestions. Explainable AI (XAI) eliminates the “black box” problem by showing exactly which data points triggered a specific alert or recommendation.
- Risk Indicators: The software highlights the specific documentation gaps that make a claim likely to be denied.
- Regulatory Mapping: It points to the exact payer rule or federal regulation that justifies a suggested billing code.
- Actionable Guidance: Instead of just flagging an error, the AI provides clear instructions on what the staff needs to correct.
3. Track Model Accuracy
AI models are not static and can experience “drift” as payer behaviors and healthcare regulations change over time. Continuous monitoring is essential to maintain the integrity of your financial predictions and automations.
- Granular Performance: Tracking accuracy rates across different payers and medical specialties to identify specific areas for improvement.
- Error Analysis: Regularly reviewing false positives and false negatives to refine the model’s decision-making logic.
- Drift Detection: Automated alerts notify developers when the model’s performance begins to deviate from established benchmarks.
4. Maintain Audit Trails
Transparency is the foundation of healthcare compliance. A robust RCM platform records every interaction between the AI and the human user to provide a complete history of the financial lifecycle.
- Interaction Logs: The system stores the original AI recommendation alongside the final decision made by the human staff member.
- Temporal Tracking: Timestamps and user IDs are attached to every change to ensure a clear chain of custody for all data.
- Support Documentation: Every decision is linked back to the supporting clinical or financial data used at the time of the action.
5. Avoid Fully Automated Compliance
Certain areas of the revenue cycle are too sensitive for full automation due to the high risk of audit or legal repercussions. Maintaining human control in these areas protects the organization from systemic compliance failures.
- High-Stakes Coding: Human coders must review complex surgical or diagnostic codes to ensure they accurately reflect the provider’s notes.
- Clinical Appeals: Responses to medical necessity denials require the nuanced argument that only a clinical expert can provide.
- Financial Responsibility: Patient billing and collection strategies should always be overseen by staff to maintain a positive patient experience.
By following these safety protocols, enterprises can harness the power of AI without compromising their financial or ethical standards. This structured approach builds trust in the technology while securing the long-term stability of the revenue cycle.
ROI Of Healthcare RCM Software Development
Investing in custom healthcare RCM software transforms the billing department into a strategic value driver. By replacing manual friction with unified automation, enterprises see a direct impact on their net patient revenue.
1. Reduced Preventable Denials
Preventable denials account for nearly 90% of all rejected claims. Modern RCM platforms eliminate these errors by enforcing strict data validation at the point of entry.
- Eligibility Validation: Automated checks ensure coverage is active before services are rendered, reducing eligibility-related denials by up to 30%.
- Prior Authorization: Verification modules confirm required approvals are in place, preventing high-value rejections.
- Clean Claim Rate: Advanced scrubbers help enterprises achieve a 95% or higher clean claim rate, compared to the industry average of roughly 80%.
2. Faster Claim Submission
Time is a critical factor in the revenue cycle. Automation shrinks the “discharge-to-bill” time from weeks to mere hours, ensuring a more predictable cash flow.
- Automated Work Queues: Claims move instantly to the next stage without waiting for manual administrative oversight.
- Batch Processing: Thousands of records are scrubbed and transmitted simultaneously for massive enterprise scalability.
- Efficiency Gains: Organizations typically see a 25% reduction in days in accounts receivable (AR), directly improving liquid cash reserves.
3. Lower Manual Follow-Up
Manual follow-up on claims is a significant expense in healthcare administration. Task routing ensures staff only intervene when human judgment is truly required.
- Task Routing: The system identifies which denials are likely to be overturned and assigns them to specialists automatically.
- Automated Status Updates: Constant communication with payer portals removes the need for staff to spend hours on phone calls.
- Labor Savings: Enterprises report a 40% decrease in manual administrative touches per claim, allowing for a leaner billing team.
4. Better Payment Recovery
Silent revenue loss occurs when payers reimburse less than the contracted amount. Underpayment detection modules act as a financial safety net.
- Payer Variance Tracking: The software flags any payment that deviates from the agreed-upon fee schedule.
- Appeal Prioritization: High-value denials move to the front of the queue to ensure maximum recovery of significant funds.
- Revenue Lift: Detecting underpayments and missed charges can result in a 3% to 7% increase in total collected revenue annually.
5. Improved Patient Collections
As patient responsibility rises, the ability to collect from individuals is vital. Digital-first billing strategies treat the patient like a modern consumer.
- Transparent Balances: Clear, itemized digital statements reduce patient confusion and payment disputes.
- Flexible Options: Offering installment plans and SMS payment links increases the likelihood of balance settlement.
- Collection Impact: Modern RCM tools can boost patient collection rates by 20% while improving overall satisfaction scores.
6. More Accurate Revenue Forecasting
A clear view of the financial future allows enterprise leaders to make confident growth decisions. Real-time analytics replace guesswork with data-driven predictions.
- Cash Flow Forecasts: Predictive models analyze historical payer speed to show when revenue will hit the bank.
- AR Aging Predictions: The system identifies accounts at risk of becoming uncollectible before they reach the 90-day mark.
- Decision Support: Accurate forecasting allows CFOs to better manage capital expenditures and facility expansions.
By focusing on these key performance indicators, an enterprise can transform its financial trajectory. This combined effect creates a resilient organization capable of navigating the complexities of modern healthcare.
Conclusion
Advanced healthcare RCM software transforms complex financial challenges into a streamlined engine for sustainable growth. By integrating predictive AI, robust data standards, and automated workflows, enterprises can significantly reduce revenue leakage while improving operational efficiency.
Prioritizing these technical innovations ensures your organization remains resilient against shifting regulatory demands and payer behaviors. Ultimately, modernizing your revenue cycle is the most effective way to secure long-term profitability and success.
Build Healthcare RCM Software With Intellivon
At Intellivon, we build healthcare revenue cycle management software for hospitals, specialty clinics, RCM companies, billing service providers, healthcare SaaS platforms, provider networks, and enterprise healthcare teams.
Our engineering approach connects patient registration, eligibility verification, charge capture, coding support, claim scrubbing, claim submission, denial management, payment posting, patient billing, analytics, and secure healthcare integrations into one connected RCM system.
A. Build RCM Workflows Around Real Healthcare Operations
RCM software only works when it fits the way healthcare teams manage claims, payments, denials, and patient billing every day. We design workflows around patient access teams, coders, billers, denial specialists, finance leaders, and administrators.
We build workflows for:
- patient registration
- eligibility verification
- charge capture
- claim scrubbing
- coding review
- claim submission
- denial follow-up
- payment posting
- patient billing
B. Integrate With Your Healthcare, Billing, And Payment Systems
A healthcare RCM platform becomes valuable when it connects with the systems where patient, claim, payer, payment, and clinical data already live. We build secure integrations that keep revenue cycle workflows connected and easier to manage.
We integrate with:
- EHR systems
- practice management systems
- billing platforms
- Clearinghouses
- payment gateways
- payer systems
- ERA/EOB systems
- document systems
- analytics tools
C. Make RCM Software Secure, Scalable, And Compliance-Ready
Healthcare revenue systems handle sensitive patient, financial, and claims data. We build RCM platforms with secure architecture, role-based access, audit trails, encryption, PHI protection, workflow controls, and scalable deployment.
We focus on:
- HIPAA-ready architecture
- secure PHI handling
- role-based access
- audit-ready workflows
- encrypted data pipelines
- human review controls
- scalable cloud deployment
Want to build healthcare RCM software for your hospital, RCM company, billing platform, or healthcare SaaS business? Contact Intellivon to design a secure, scalable revenue cycle management system around your workflows.
Things To Know About Healthcare RCM Platforms
Q1. What is healthcare revenue cycle management software?
A1. Healthcare revenue cycle management software helps healthcare organizations manage patient registration, eligibility checks, coding, claim submission, denial management, payment posting, collections, and financial reporting. A custom RCM platform connects these workflows into one system so providers can reduce billing errors, improve cash flow, and track revenue performance clearly.
Q2. How much does healthcare RCM software development cost?
A2. Healthcare RCM software development usually costs between $60,000 and $350,000+, depending on features, integrations, automation level, compliance needs, and enterprise scale. A basic platform costs less, while AI-powered RCM software with EHR, clearinghouse, payment, denial, and analytics integrations requires a higher investment. Competitor cost ranges also vary widely based on complexity.
Q3. What features should healthcare RCM software include?
A3. A strong healthcare RCM platform should include patient registration, insurance eligibility verification, charge capture, medical coding support, claim scrubbing, claim submission, denial management, payment posting, patient billing, analytics dashboards, and compliance controls. Advanced platforms can also include AI denial prediction, workflow automation, and revenue forecasting.
Q4. How long does it take to build healthcare RCM software?
A4. A focused RCM MVP can take around 3–5 months, while a full enterprise RCM platform may take 8–14+ months. The timeline depends on workflow complexity, AI modules, integrations, security requirements, user roles, reporting needs, and how much legacy system modernization is involved.