Patient engagement often seems successful at first glance. However, when it is designed as an experience layer rather than a central healthcare system, its effectiveness decreases as programs expand across services, regions, and patient groups.
Companies invest in patient engagement platforms to improve adherence, access, and continuity of care. Initially, the adoption rate seems high. Over time, though, signs begin to change where notifications become less relevant, and care workflows move away from clinical oversight. However, even though engagement metrics stay consistent, outcomes and operational efficiency do not improve accordingly. This gap shows how engagement is organized within the larger healthcare system.
Developing patient engagement healthcare apps should be seen as building enterprise infrastructure rather than superficial software. This blog discusses how we build patient engagement platforms in terms of governance, compliance, architecture, and long-term scalability. Drawing from Intellivon’s experience in creating enterprise-level patient engagement solutions, it describes how these systems can support ongoing participation, coordinated care delivery, and measurable outcomes without raising clinical, regulatory, or operational risks.
Key Takeaways of the Patient Engagement Solutions Market
The market for patient engagement solutions has grown quickly as healthcare shifts from episodic interactions to continuous digital communication. As a result, health systems now face higher administrative pressure and rising patient expectations.
In addition, coordinated care across services has become harder to manage at scale. Therefore, enterprises are investing in engagement platforms that simplify access and improve operational efficiency.
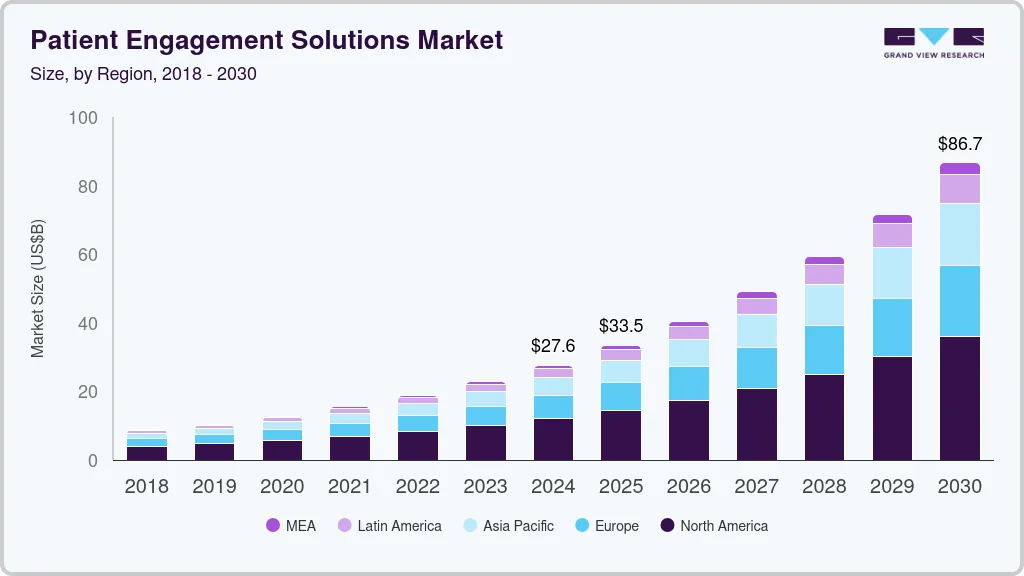
Because of these shifts, the global patient engagement market reached USD 27.63 billion in 2024. Moreover, it is projected to grow to USD 86.67 billion by 2030. This expansion reflects a strong estimated CAGR of 20.97 percent between 2025 and 2030.
Market Insights:
- Federal programs such as Meaningful Use and Promoting Interoperability continue to accelerate enterprise adoption.
- Over 90% EHR penetration across U.S. hospitals enables smoother patient portal integration.
- Chronic disease prevalence affects more than 130 million Americans, increasing demand for ongoing digital engagement.
- Telehealth expansion since COVID-19 has strengthened the need for unified digital access points.
- Value-based care incentives encourage data sharing, coordinated workflows, and measurable patient engagement.
- North America currently holds a 43.8% market share, while Asia-Pacific shows the fastest growth at 21.12% CAGR.
- Analysts project mid-teen to 20% CAGR through 2030 as digital-first care models mature.
Adoption of patient engagement platforms is now widespread across enterprise healthcare. 99% of U.S. acute care hospitals allow patients to view their health data digitally, while 96% support data downloads and 92% enable secure messaging.
In addition, over 80% offer all 4 foundational portal capabilities, and 95% provide access to clinical notes. Mobile access is also common, with 81% offering apps and 70% of those built on FHIR standards.
Because adoption is highest among large, urban, and system-affiliated hospitals, enterprises are positioning engagement platforms as core infrastructure that supports care coordination, digital access, and financial performance as regulatory pressure and patient expectations continue to rise.
What Is a Patient Engagement Healthcare App?
A patient engagement healthcare app is a digital system that helps healthcare organizations stay connected with patients before, during, and after care. It supports everyday actions such as booking appointments, viewing results, messaging care teams, completing forms, and receiving reminders. In addition, it can guide patients through care plans, track follow-ups, and reduce missed visits.
For enterprises, these apps work best when they connect with EHRs, identity systems, and clinical workflows. Therefore, they act as a managed channel for access, communication, and coordination. When designed well, they improve adherence, reduce administrative load, and support better outcomes at scale.
How Engagement Platforms Differ From Patient Portals
At first glance, patient portals and engagement platforms can appear similar. Both offer digital access to health information and communication tools. However, their purpose and impact differ significantly at the enterprise scale.
Patient portals focus on access while engagement platforms focus on behavior, continuity, and outcomes. This distinction becomes critical as healthcare organizations move from isolated interactions to ongoing digital care management.
Comparison: Patient Portals vs Engagement Platforms
| Aspect | Patient Portals | Patient Engagement Platforms |
| Primary purpose | Provide access to health information | Drive sustained participation across the care journey |
| Scope of use | Transactional and episodic | Longitudinal and continuous |
| Workflow integration | Limited to EHR-linked functions | Embedded across clinical, operational, and care workflows |
| Personalization | Minimal and static | Dynamic, behavior-driven, and context-aware |
| Care coordination | Patient-initiated | System-orchestrated across teams and services |
| Measurement focus | Logins, messages, record views | Adherence, outcomes, utilization, and efficiency |
| Enterprise scalability | Functional at the single-system level | Designed for multi-program, multi-region scale |
As healthcare delivery shifts toward value-based models, enterprises need systems that influence behavior rather than just provide visibility. Therefore, engagement platforms become strategic infrastructure rather than optional digital tools.
Role Of Patient Engagement Apps in Modern Care Delivery Models
Patient engagement platforms play a structural role in how modern care is delivered. They connect patients, clinicians, and operations teams across the entire care journey.
Instead of supporting isolated interactions, these systems help enterprises manage continuity, coordination, and demand at scale. As care models shift toward value, prevention, and hybrid delivery, engagement platforms become the connective layer that keeps workflows aligned.
1. Pre-Care: Access, Intake, and Readiness
Before care begins, engagement platforms act as the primary digital entry point. Patients use them to discover services, schedule appointments, complete intake forms, and verify insurance details.
At the same time, automated reminders and instructions prepare patients in advance, which reduces no-shows and last-minute cancellations.
For enterprises, this improves clinic utilization and lowers front-desk burden. These touchpoints set expectations early and create cleaner handoffs into clinical workflows.
2. During Care: Communication and Coordination
During active care, engagement platforms support secure messaging, visit summaries, care instructions, and real-time updates. Patients can ask follow-up questions, share symptoms, and receive guidance without triggering unnecessary visits.
Care teams use the same channel to coordinate tasks, escalate issues, and maintain visibility across services. As a result, communication stays structured and traceable, even across multidisciplinary teams. This reduces fragmentation during complex care episodes.
3. Post-Care: Follow-Ups and Adherence
After a visit or discharge, engagement platforms help sustain momentum. Patients receive follow-up reminders, medication guidance, and recovery instructions through familiar digital channels. Surveys and check-ins capture early warning signs before complications escalate.
For enterprises, these touchpoints support adherence while reducing avoidable readmissions. Post-care engagement turns episodic treatment into managed continuity.
4. Long-Term Care: Chronic and Preventive Management
For chronic conditions and preventive programs, engagement platforms enable ongoing participation. Patients track progress, receive personalized nudges, and stay connected to care teams over time. Educational content and monitoring tools reinforce self-management behaviors.
Enterprises use these touchpoints to support population health goals and value-based care contracts. Long-term engagement shifts care from reactive to proactive.
Across modern care delivery models, engagement platforms provide consistency where healthcare often fragments. They align access, communication, and follow-up into a single operating layer.
When designed well, these systems reduce operational strain while improving patient experience and outcomes. For enterprises, this role makes engagement platforms foundational to scalable, sustainable care delivery.
Why Patient Engagement Matters for Healthcare Organizations
Patient engagement matters because it directly influences outcomes, operational efficiency, and cost control. For enterprises, engagement platforms help manage demand, improve adherence, and support scalable care delivery.
Patient engagement is no longer a supporting function in healthcare delivery. It directly affects how organizations manage demand, control costs, and deliver consistent outcomes at scale. As care models become more distributed and patient expectations rise, engagement platforms shape how effectively enterprises operate across the entire care lifecycle.
1. Improves Clinical Outcomes
Engaged patients are more likely to follow care plans, attend follow-ups, and report issues early. This improves adherence across chronic, preventive, and post-acute care programs. In addition, structured digital touchpoints help clinicians monitor progress without relying on sporadic visits.
Over time, this continuity reduces avoidable complications and escalation. For enterprises, better outcomes also support value-based care goals.
2. Reduces Operational Friction
Healthcare operations absorb significant effort through calls, rescheduling, paperwork, and manual follow-ups. Engagement platforms move many of these interactions into digital workflows.
As a result, front-desk teams handle fewer interruptions, and clinicians regain focused time. This shift improves throughput without adding staff. Therefore, engagement directly contributes to operational stability at scale.
3. Supports Financial Performance
Patient engagement influences revenue and cost on multiple fronts. Fewer no-shows improve utilization and digital follow-ups reduce low-value visits. Better adherence lowers downstream costs tied to readmissions and complications.
In addition, reclaimed clinician time increases capacity without extending work hours. For large organizations, these gains compound across departments and regions.
3. Strengthens Patient Trust and Retention
Patients now expect healthcare access to match the convenience of other digital services. Engagement platforms provide clarity, responsiveness, and continuity throughout the care journey.
When patients feel informed and supported, trust improves. Over time, this drives retention within competitive healthcare markets. For enterprises, consistent engagement strengthens brand perception and long-term relationships.
4. Enables Scalable, Value-Based Care Models
Modern care delivery depends on coordination across providers, services, and settings. Engagement platforms help orchestrate these interactions through shared workflows and data visibility. They support preventive programs, chronic care management, and population health initiatives.
As value-based models expand, engagement becomes essential infrastructure. Without it, scaling care delivery introduces risk and fragmentation.
Patient engagement shapes how healthcare organizations perform, not just how they communicate. It influences outcomes, capacity, cost control, and patient loyalty at the same time.
Types of Patient Engagement Apps
Patient engagement apps vary by care model, including chronic care, preventive programs, post-discharge support, remote monitoring, behavioral health, and employer-led healthcare. Each type addresses specific operational and clinical needs at enterprise scale.
1. Chronic Disease Management Apps
Chronic disease management apps support long-term conditions such as diabetes, hypertension, and heart disease. They focus on monitoring, medication adherence, education, and regular communication with care teams. These apps help enterprises manage high-risk populations while reducing unnecessary visits.
Real example:
Kaiser Permanente uses its patient engagement platform to support chronic disease programs across millions of members. Digital monitoring and secure messaging help clinicians manage diabetes and cardiovascular care while reducing in-person follow-ups.
2. Preventive Care and Wellness Engagement Platforms
Preventive engagement platforms encourage early action through screenings, vaccinations, and routine check-ups. They help organizations shift care upstream by automating reminders and simplifying access. These platforms often combine education, scheduling, and follow-up in one system.
Real example:
The NHS App in England supports preventive care by enabling vaccination bookings, health reminders, and access to screening information. It plays a central role in national prevention and public health initiatives.
3. Post-Discharge and Recovery Engagement Apps
Post-discharge engagement apps guide patients after surgery or hospitalization. They deliver recovery instructions, reminders, and symptom check-ins. These touchpoints help detect issues early and reduce avoidable readmissions.
Real example:
Mayo Clinic uses digital follow-up tools through its patient engagement systems to support post-surgical recovery. Patients receive discharge instructions and follow-up communication that help teams monitor recovery remotely.
4. Remote Monitoring and Continuous Care Apps
Remote monitoring apps collect patient data through devices, surveys, and regular check-ins. They support continuous care without frequent in-person visits. These apps are critical for managing complex and high-risk patients.
Real example:
The Veterans Health Administration uses remote patient monitoring programs to manage chronic conditions such as heart failure. These engagement tools have helped reduce hospital admissions and improve care continuity across large populations.
5. Behavioral Health and Mental Wellness Engagement
Behavioral health engagement apps support therapy access, self-guided programs, and ongoing check-ins. They prioritize privacy and consistency, which is essential for mental health care delivery at scale.
Real example:
The UK’s NHS Talking Therapies program uses digital engagement tools to support cognitive behavioral therapy access. Patients engage through structured digital pathways that reduce wait times and improve continuity.
6. Employer or Payer-Led Engagement Platforms
Employer and payer-led engagement platforms guide members through benefits, care options, and preventive services. They often act as the digital front door for large populations. These platforms help manage utilization and improve care navigation.
Real example:
UnitedHealthcare’s digital member engagement platforms support appointment scheduling, care navigation, and benefit access. These tools help members choose appropriate care settings and reduce unnecessary emergency visits.
Each category of patient engagement app addresses a specific operational challenge. When implemented correctly, they reduce friction, stabilize care delivery, and improve outcomes. For enterprises, success depends less on features and more on how engagement apps integrate into existing systems and long-term care strategies.
Patient Engagement Portals Can Support 26 More Patients Per Clinician Each Year
Digital engagement often gets framed as a convenience feature. In practice, it plays a direct operational role. When routine interactions shift from phone calls and in-person visits to structured digital channels, clinical teams recover time. Several economic evaluations have measured this shift. The findings show clear value for large healthcare organizations.
1. Fewer Visits/Calls Translate Into Usable Capacity
A multi-year evaluation of MyChart found that active portal users required 14% fewer in-person visits and 19% fewer telephone encounters over a 3-year period.
Patients relied on secure messaging, automated updates, and self-service access for routine needs. As a result, clinicians faced fewer interruptions, and staff processed fewer manual requests.
2. Savings Compound As Adoption Grows
The same study reported USD 89.73 in net savings per patient over 3 years, after accounting for both clinician and patient time. Across a typical panel of 2,000 patients, this translates to USD 171,473 in savings. These gains came from fewer low-value interactions, reduced administrative effort, and smoother care coordination.
3. Clinical Capacity Increases Without Extending Work Hours
The most strategic outcome involved throughput. By moving routine follow-ups and clarifications into portal workflows, clinicians gained enough capacity to support 26 additional patients each year. At a system level, a network with 400 to 500 active physicians could support 10,000 to 13,000 more patients annually without expanding staff.
Taken together, these results highlight a structural advantage that often goes overlooked. Patient engagement portals reshape administrative demand, stabilize clinical workloads, and expand system capacity.
When applied across large networks, the impact becomes meaningful enough to influence financial performance and long-term planning.
Core Features of a Patient Engagement Healthcare App
Enterprise patient engagement healthcare apps combine secure access, workflow integration, personalization, and governed AI to support scalable care delivery, compliance, and measurable outcomes.
At enterprise scale, patient engagement apps succeed when features support real care delivery, not just digital interaction. These platforms must balance usability with governance, flexibility, and long-term scalability. Below are the core features enterprises expect when patient engagement becomes part of the healthcare infrastructure.
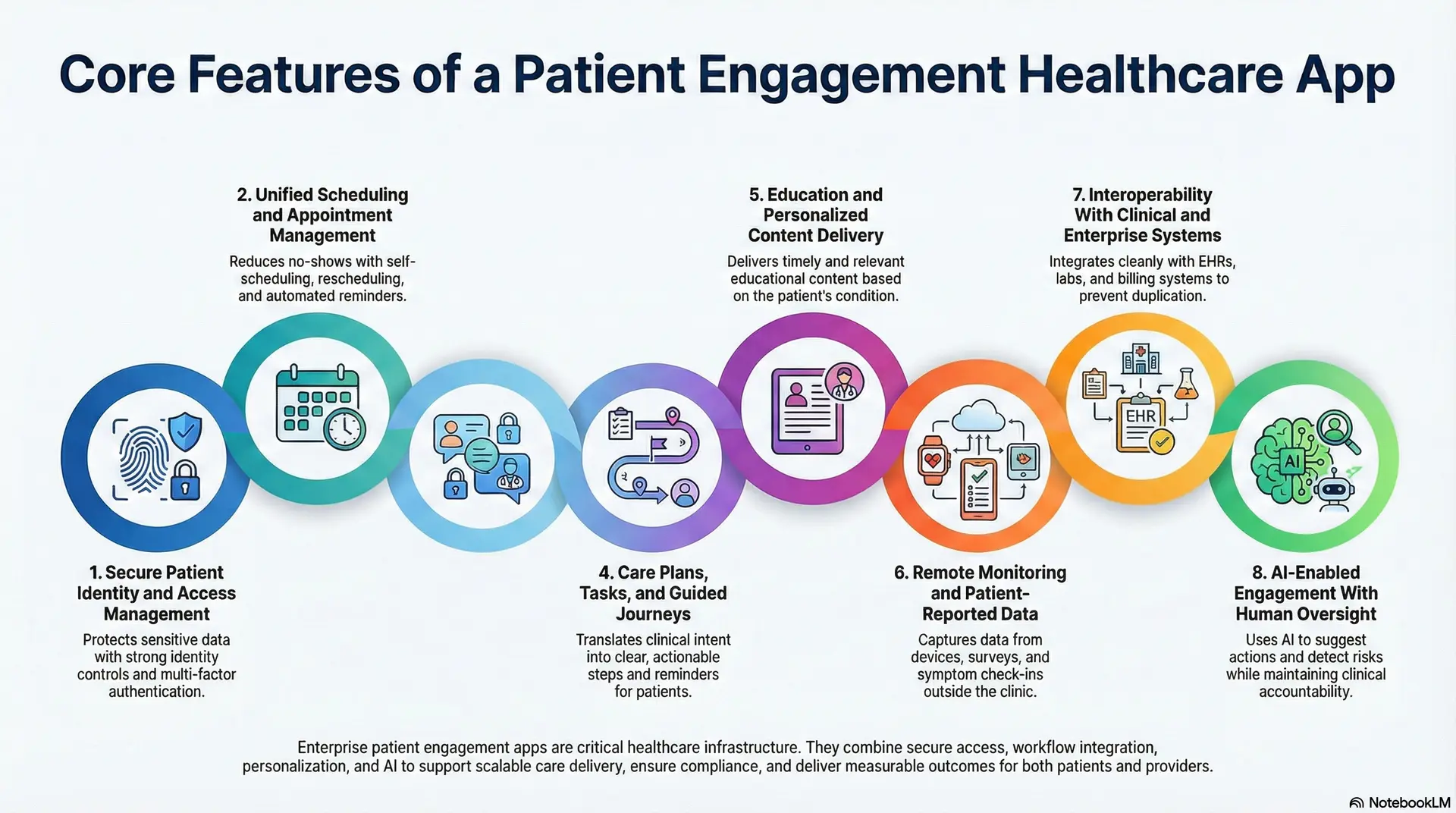
1. Secure Patient Identity and Access Management
Enterprise engagement apps require strong identity controls from the start. Patients must access services securely across devices, locations, and care settings. Role-based access, proxy management, and multi-factor authentication protect sensitive data.
These controls also support regulatory compliance and audit readiness. As programs scale, consistent identity management prevents fragmentation.
2. Unified Scheduling and Appointment Management
Scheduling remains one of the highest-impact engagement features. Enterprise platforms support self-scheduling, rescheduling, waitlists, and automated reminders. These tools reduce no-shows and smooth clinic operations.
When connected to EHR workflows, scheduling becomes predictable rather than reactive. This improves capacity planning across departments.
3. Two-Way Communication and Secure Messaging
Effective engagement depends on structured communication, not unmonitored chat. Enterprise apps provide secure messaging tied to care contexts, teams, and escalation rules.
Patients can ask questions and share updates without triggering unnecessary visits. Care teams retain visibility and control over responses. This balance protects clinician time while maintaining access.
4. Care Plans, Tasks, and Guided Journeys
Patient engagement apps should guide action, not just share information. Care plans translate clinical intent into clear steps for patients. Tasks, reminders, and milestones keep progress visible.
Enterprises use these journeys to standardize care delivery across programs. As a result, adherence improves without manual follow-up.
5. Education and Personalized Content Delivery
Education becomes effective when it is timely and relevant. Enterprise platforms deliver content based on condition, stage of care, and patient context. This reduces confusion and supports informed decision-making.
Over time, personalized education reinforces self-management behaviors. It also reduces repetitive clinician explanations.
6. Remote Monitoring and Patient-Reported Data
Modern engagement apps capture data beyond clinic walls. Device integrations, surveys, and symptom check-ins feed into care workflows. Enterprises use this data to identify risk early and prioritize interventions.
When governed properly, remote data supports continuous care without overwhelming teams. Here, visibility improves while workload stays manageable.
7. Interoperability With Clinical and Enterprise Systems
Enterprise engagement apps must integrate cleanly with EHRs, labs, pharmacies, billing systems, and identity platforms. Standards such as FHIR support consistent data exchange and interoperability prevents duplication and manual work.
It also ensures engagement fits into existing operations rather than creating parallel systems.
8. AI-Enabled Engagement With Human Oversight
AI supports personalization, risk detection, and workflow prioritization. However, enterprises require clear boundaries. Engagement apps use AI to suggest actions, not replace judgment.
Escalation rules and explainability protect clinical accountability. This approach enables intelligence without increasing regulatory or operational risk.
Each feature contributes to how engagement functions within the healthcare system. When designed in isolation, even strong features fail to deliver impact. When designed together, they form a stable operating layer. For enterprises, this integrated approach turns patient engagement apps into a scalable, reliable infrastructure.
How AI Is Used in Patient Engagement Apps
AI in patient engagement apps supports personalization, risk detection, and workflow prioritization. At enterprise scale, its value comes from governed use with human oversight and clear accountability.
AI plays a growing role in patient engagement apps, but its value depends on how carefully it is applied. At enterprise scale, AI should support decision-making, reduce manual effort, and improve continuity of care. It should never operate as an uncontrolled automation layer.
When designed with governance and oversight, AI strengthens engagement without increasing clinical or regulatory risk.
1. Personalization at Scale Without Manual Effort
AI helps engagement apps tailor content, reminders, and care prompts based on patient context. This includes condition type, care stage, past behavior, and risk profile. As a result, patients receive messages that feel relevant instead of generic.
For enterprises, this reduces disengagement without requiring manual segmentation. Personalization improves consistency across large populations.
2. Predictive Risk Identification and Early Intervention
AI models can analyze patient activity, reported symptoms, and historical data to flag early risk. These signals help care teams intervene before issues escalate. Instead of reacting to missed visits or complications, teams can act earlier.
This approach supports better outcomes while controlling costs. Predictive insights become especially valuable in chronic and post-discharge care.
3. Intelligent Routing and Workflow Prioritization
Engagement apps generate large volumes of patient interactions. AI helps route messages, tasks, and alerts to the right team at the right time. Low-risk requests move through automated pathways, while high-risk cases escalate to clinicians.
This keeps workloads manageable and response times predictable. For enterprises, workflow prioritization protects clinician capacity.
4. Adherence Support and Behavioral Nudging
AI supports adherence by identifying patterns that signal drop-off. It adjusts reminder timing, frequency, and format based on patient response. These nudges encourage follow-through without overwhelming users.
Over time, this improves medication adherence and follow-up completion. Behavioral support becomes scalable without increasing staff involvement.
5. Continuous Learning From Engagement Data
As engagement apps operate, they generate valuable data on patient behavior and outcomes. AI analyzes this data to refine engagement strategies over time. Programs improve as models learn which touchpoints drive action.
Enterprises use these insights to optimize care delivery. Learning loops strengthen long-term performance.
Why Governance and Human Oversight Matter
AI must operate within defined boundaries in healthcare environments. Enterprises require explainability, audit trails, and escalation rules. AI should recommend actions rather than making clinical decisions.
Human oversight ensures accountability remains clear. When governed properly, AI enhances engagement while maintaining trust.
AI allows patient engagement apps to scale without losing relevance or control. It reduces manual work while improving responsiveness and outcomes. However, its value depends on disciplined design. For enterprises, AI becomes a force multiplier only when it aligns with governance, workflows, and long-term strategy.
How We Build Patient Engagement Platforms at Intellivon
Intellivon builds patient engagement platforms through a governance-first, architecture-led process that aligns care models, integrates enterprise systems, and scales engagement without adding clinical or regulatory risk.
Enterprises need a governed engagement system that fits real care delivery and scales without creating operational risk. At Intellivon, patient engagement platforms are built as enterprise healthcare infrastructure, designed to support access, coordination, and measurable outcomes across programs and populations.
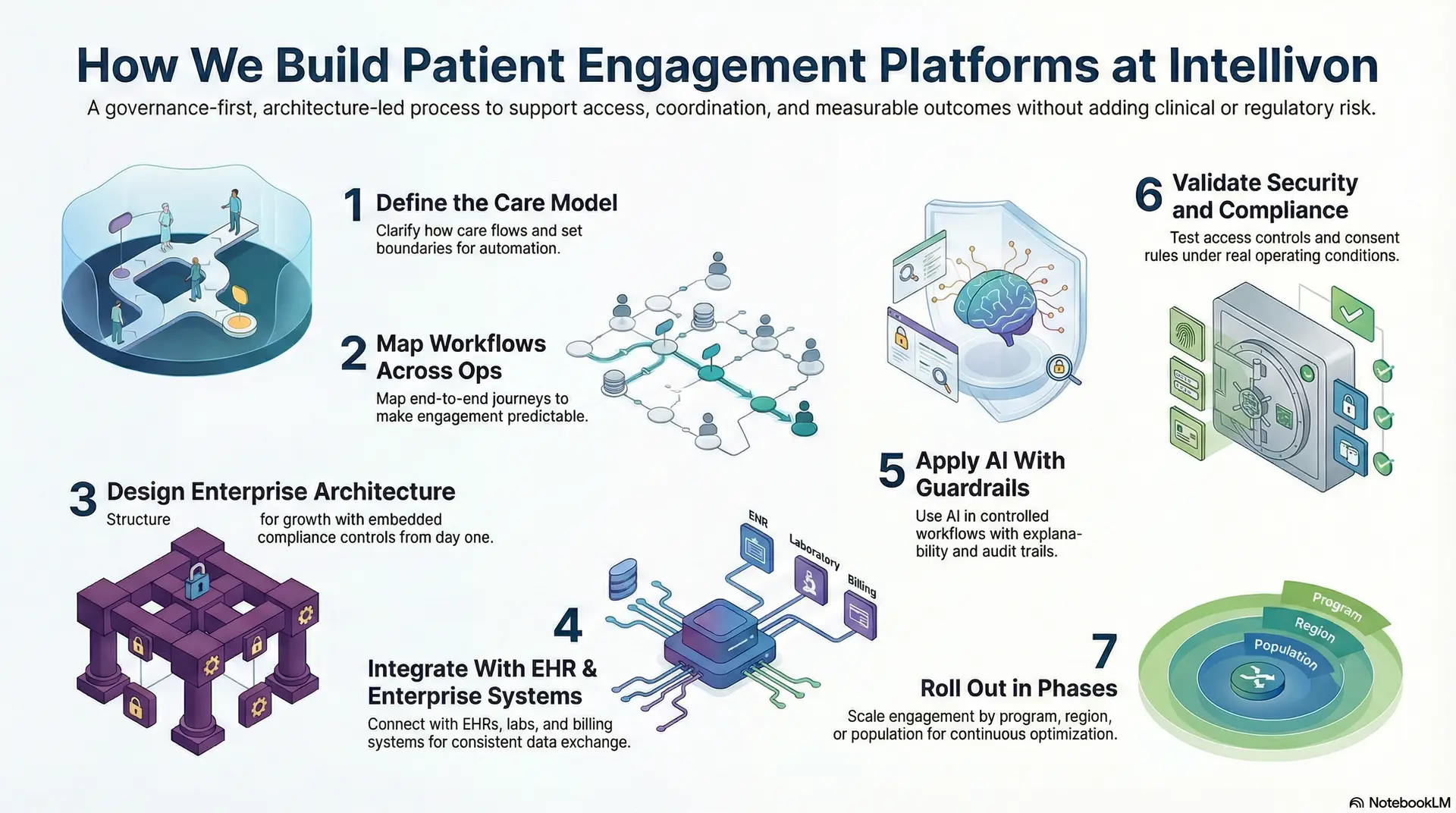
Step 1: Define the Care Model
The work starts by clarifying how care should flow across services. Clinical use cases, ownership models, and escalation rules are defined early.
This ensures the platform supports real-world operations, not assumptions. In addition, decision boundaries are set for what automation can handle and where clinicians must stay in control. These definitions reduce downstream rework and adoption resistance.
Step 2: Map Workflows Across Ops
Engagement fails when workflows remain vague. Therefore, Intellivon maps end-to-end journeys across access, visits, follow-ups, and long-term care. Each touchpoint connects to the right team and system.
Intake, scheduling, messaging, and care tasks are aligned to reduce manual burden. As a result, engagement becomes predictable, not fragmented.
Step 3: Design Enterprise Architecture
The platform architecture is structured for growth from day 1. Identity, consent, data, workflows, and integration layers remain clearly separated. This supports modular rollout across regions and programs.
Compliance controls are embedded into workflows rather than added later. Therefore, auditability, traceability, and policy enforcement stay intact as scale increases.
Step 4: Integrate With EHR and Enterprise Systems
A patient engagement platform is only as strong as its interoperability. Intellivon integrates the platform with EHRs, labs, pharmacies, billing systems, and identity providers. Standards such as FHIR support consistent data exchange and reduce duplication.
In addition, data flows are designed to remain governed and observable. This prevents parallel systems from forming over time.
Step 5: Apply AI With Guardrails
AI improves personalization, prioritization, and early risk detection. However, it must operate within defined rules. Intellivon implements AI in controlled workflows with explainability, audit trails, and escalation paths.
AI supports care teams by suggesting actions and highlighting risk. Clinicians retain final authority where it matters.
Step 6: Validate Security and Compliance
Before launch, the platform goes through security testing and compliance validation. Access controls, consent rules, and logging are tested under real operating conditions.
In addition, workflows are reviewed with clinical and operations teams to reduce friction. This step prevents surprises after rollout. It also improves stakeholder confidence.
Step 7: Roll Out in Phases
Enterprises scale engagement through phased adoption, not big-bang launches. Intellivon supports rollout by program, region, or population segment. Engagement metrics are tracked alongside outcomes, utilization, and operational impact.
Therefore, optimization remains continuous rather than reactive. Over time, the platform evolves as care models and regulations change.
What This Approach Delivers
This process creates a platform that stays reliable as complexity increases. Engagement remains consistent across teams, services, and patient populations. In addition, governance and compliance remain stable as the platform scales. For enterprise leaders, this reduces risk while improving outcomes, capacity, and long-term performance.
Cost to Build a Patient Engagement Healthcare App
At Intellivon, patient engagement healthcare apps are built as regulated care coordination infrastructure, not as surface-level communication tools. The focus stays on platforms that can operate reliably across providers, regions, and evolving care models. Every design decision considers scale, governance, and operational risk from the start.
When budget constraints exist, scope is refined with intent. However, security controls, consent logic, interoperability, and auditability are never reduced. As a result, enterprises avoid remediation costs later. Predictability replaces rework, and long-term ROI remains protected as engagement programs expand.
Estimated Phase-Wise Cost Breakdown
| Phase | Description | Estimated Cost Range (USD) |
| Discovery & Engagement Strategy | Care model definition, engagement goals, population scope, regulatory assessment, KPI alignment | $7,000 – $14,000 |
| Enterprise Architecture Design | Engagement workflows, identity and consent layers, integration mapping, scale planning | $9,000 – $17,000 |
| Consent & Governance Framework | Consent models, access policies, audit workflows, compliance enforcement | $8,000 – $15,000 |
| Backend & Enterprise Integrations | EHRs, scheduling systems, messaging services, labs, identity providers, interoperability APIs | $15,000 – $28,000 |
| Frontend & Role-Based Interfaces | Patient, clinician, and admin interfaces with accessibility and security controls | $11,000 – $20,000 |
| Engagement Logic & Care Journeys | Reminders, tasks, messaging rules, escalation paths, adherence workflows | $10,000 – $18,000 |
| Security & Privacy Engineering | Encryption, access controls, logging, monitoring, zero-trust enforcement | $10,000 – $18,000 |
| Testing & Compliance Validation | Functional testing, security validation, consent checks, audit readiness | $7,000 – $12,000 |
| Deployment & Scale Readiness | Cloud deployment, observability, performance tuning, failover planning | $8,000 – $14,000 |
Total initial investment: $85,000 – $180,000
Ongoing maintenance and optimization: ~15–20% of the initial build per year
Hidden Costs Enterprises Should Plan For
Even well-scoped patient engagement programs face pressure when indirect cost drivers are overlooked. Planning for these early protects budgets, timelines, and compliance posture as adoption grows.
- Integration complexity increases as EHRs, scheduling tools, devices, and third-party systems expand
- Compliance overhead grows due to recurring audits, reporting requirements, and regulatory updates
- Data governance requires continuous consent validation, access reviews, and correction workflows
- Cloud costs rise with increased messaging volume, monitoring data, and analytics workloads
- Change management includes onboarding for clinicians, operations teams, and support staff
- Continuous monitoring becomes essential as engagement volume and regulatory scrutiny increase
Best Practices to Avoid Budget Overruns
Based on Intellivon’s experience delivering enterprise patient engagement platforms, these practices consistently lead to controlled costs and predictable outcomes.
- Start with a focused engagement scope before expanding populations or programs
- Embed consent management, auditability, and security into the core architecture
- Use modular components that scale without redesign
- Design engagement workflows around real care operations, not assumptions
- Maintain continuous observability across performance, usage, and compliance
- Plan for regulatory evolution rather than one-time certification
Ready to Plan Your Engagement Platform Investment?
Request a tailored proposal from Intellivon’s healthcare team to receive a delivery roadmap aligned with your budget constraints, compliance exposure, and long-term patient engagement strategy.
Which Patient Management Apps Have Proven Successful in Healthcare?
Several patient management apps demonstrate how digital engagement can function reliably at the enterprise and national scale. Platforms such as Epic MyChart, HealtheLife, OceanMD, the NHS App, and MediRecords with HotDoc show how engagement systems perform when embedded into real healthcare operations.
These examples highlight what separates scalable patient management apps from basic portals. They operate inside clinical workflows, support daily operations, and remain dependable as usage grows across regions and populations.
1. Epic MyChart
Epic MyChart is one of the most widely adopted patient management apps in the United States. It connects directly with Epic’s clinical ecosystem and supports scheduling, lab results, visit summaries, proxy access, e-visits, and secure messaging.
Large healthcare enterprises use MyChart to centralize patient communication and manage appointments more efficiently. Its tight integration with Epic allows organizations to maintain a single patient record across inpatient, outpatient, and virtual care settings. As a result, patient interactions remain consistent across the care continuum.
2. Cerner HealtheLife
HealtheLife integrates with Cerner Millennium and provides core patient management capabilities, including medical record access, secure messaging, care plan updates, and appointment coordination.
Health systems adopt HealtheLife because it aligns naturally with Cerner-based workflows. Clinical documentation stays synchronized, while patients gain structured access to orders, visit instructions, and results. Many enterprises also use it as a foundation for digital front-door strategies across multi-hospital environments.
3. OceanMD
OceanMD is widely used across Canada as a patient management platform focused on intake, scheduling, digital forms, referrals, and secure communication. Its modular design supports interoperability with provincial systems and multiple EHRs.
Healthcare organizations rely on OceanMD to reduce administrative overhead and modernize front-desk operations. Digital forms replace paper workflows, improving data accuracy and reducing staff workload during peak hours.
4. NHS App
The NHS App operates at a national scale and serves millions of users across England. It supports appointment booking, prescription refills, medical record access, and secure identity verification through NHS login.
Public health authorities and care providers use the app as a unified patient management layer for access and communication. It supports vaccination programs, national health initiatives, and coordinated service delivery. Its success demonstrates how patient management apps can function across an entire country.
When patient management apps align with enterprise operations, they become a dependable infrastructure that supports access, coordination, and long-term care delivery.
Conclusion
Patient engagement apps have become a defining capability for modern healthcare enterprises. When designed as core infrastructure, it improves outcomes, stabilizes operations, and supports long-term growth. However, success depends on disciplined architecture, governance, and execution.
Organizations that approach engagement strategically gain measurable advantages in scale, efficiency, and trust. With the right partner, patient engagement platforms become enablers of sustainable, enterprise-wide transformation rather than short-term digital initiatives.
Build a Patient Engagement App With Intellivon
At Intellivon, patient engagement apps are built as enterprise care coordination platforms, not as basic communication layers. Every architectural and delivery decision prioritizes governance, interoperability, and regulatory alignment. This ensures engagement platforms function reliably across providers, regions, and evolving care models, not just at initial rollout.
As engagement programs expand across populations, services, and delivery channels, stability becomes essential. Workflow integrity, performance, and compliance remain consistent as scale increases. Organizations maintain control over patient interactions without introducing fragmentation, clinician burden, or regulatory exposure.
Why Partner With Intellivon?
- Enterprise-grade engagement architecture designed for regulated, multi-provider healthcare environments
- Proven delivery across health systems, payers, employer-led programs, and digital care platforms
- Compliance-by-design approach covering privacy, consent management, auditability, and data residency
- Secure role-based access with end-to-end traceability across patients, clinicians, and administrators
- Governed AI enablement for personalization, risk identification, and workflow prioritization
- Modular, cloud-native infrastructure built for phased rollout and cross-region scaling
Book a strategy call to explore how Intellivon can help you build and scale a patient engagement app with control, compliance, and long-term enterprise value.
FAQs
Q1. What makes a patient engagement healthcare app enterprise-ready?
A1. An enterprise-ready patient engagement app goes beyond basic access features. It integrates with EHRs, identity systems, and care workflows while supporting consent management, auditability, and scalability. These platforms operate reliably across regions and populations. Governance and interoperability define enterprise readiness, not UI alone.
Q2. How is a patient engagement app different from a standard patient portal?
A2. Patient portals focus on viewing information and completing simple transactions. Patient engagement apps actively guide behavior through reminders, care journeys, messaging workflows, and follow-ups. They support longitudinal care rather than isolated interactions. At enterprise scale, engagement apps influence outcomes, capacity, and operational efficiency.
Q3. Is AI safe to use in patient engagement healthcare apps?
A3. AI is safe when applied with clear governance and human oversight. In patient engagement apps, AI supports personalization, risk detection, and workflow prioritization. It should recommend actions, not make clinical decisions. Enterprises require explainability, audit trails, and escalation controls to maintain accountability.
Q4. How long does it take to build a patient engagement healthcare app?
A4. Timelines depend on scope, integrations, and compliance requirements. Most enterprise patient engagement platforms take several months to design, integrate, and validate. Phased rollouts help organizations launch faster while managing risk. Planning for scale early prevents delays later.
Q5. What outcomes should enterprises expect from patient engagement apps?
A5. Well-designed engagement apps improve adherence, reduce administrative load, and stabilize care delivery. Enterprises often see fewer missed visits, better follow-up completion, and improved patient satisfaction. Over time, these platforms also support capacity growth and value-based care goals.