Key Takeaways:
-
AI diagnostic imaging takes 4 to 6 months for an MVP and 9 to 18 months for an enterprise platform with PACS integration, multi-role workflows, and clinical validation.
-
Timeline shifts significantly by modality: X-ray takes 4 to 8 months, MRI takes 8 to 14 months, and multi-modality platforms take 12 to 24 months.
-
Data readiness, annotation quality, PACS integration scope, and clinical validation depth drive most timeline overruns, not AI model development itself.
-
MVP timelines compress to 120 to 180 days by targeting one modality, one diagnostic condition, and limited PACS integration while building on a modular architecture.
-
How Intellivon builds AI diagnostic imaging systems your enterprise fully owns, with secure image pipelines, clinical workflow design, PACS integration, and compliance-ready architecture from day one.
Every hospital system and healthtech investor asking about AI diagnostic imaging eventually lands on the same question: how long does this actually take to build?
Building an AI diagnostic imaging system takes 4 to 6 months for an MVP and 9 to 18+ months for an enterprise-grade platform. That range exists because the timeline shifts based on imaging modality, data readiness, PACS/RIS integration, clinical validation, and deployment scope.
However, the AI model is only one piece of the system. A production-ready platform also needs DICOM ingestion, image preprocessing, annotation workflows, result visualization, radiologist review, audit trails, access control, and compliance-ready architecture. A single X-ray triage tool moves faster. In contrast, a multi-modality platform covering CT, MRI, and full radiology workflows takes considerably longer and demands a fundamentally different build strategy.
At Intellivon, we build AI diagnostic imaging systems around secure image pipelines, clinical workflow design, PACS/RIS/EHR integration, and scalable deployment infrastructure. This blog, therefore, breaks down the full development timeline by stage, system type, and integration scope, and shows how teams can move from MVP to production without costly rework.
Why AI Diagnostic Imaging Is Becoming So Popular Right Now
AI in medical imaging is currently one of the most aggressive sectors in healthcare technology. Industry forecasts suggest the global market for AI diagnostics will grow at a compound annual rate of 24% to 33% between 2026 and 2035. This rapid expansion stems from a critical need for faster, more precise results in high-pressure fields.
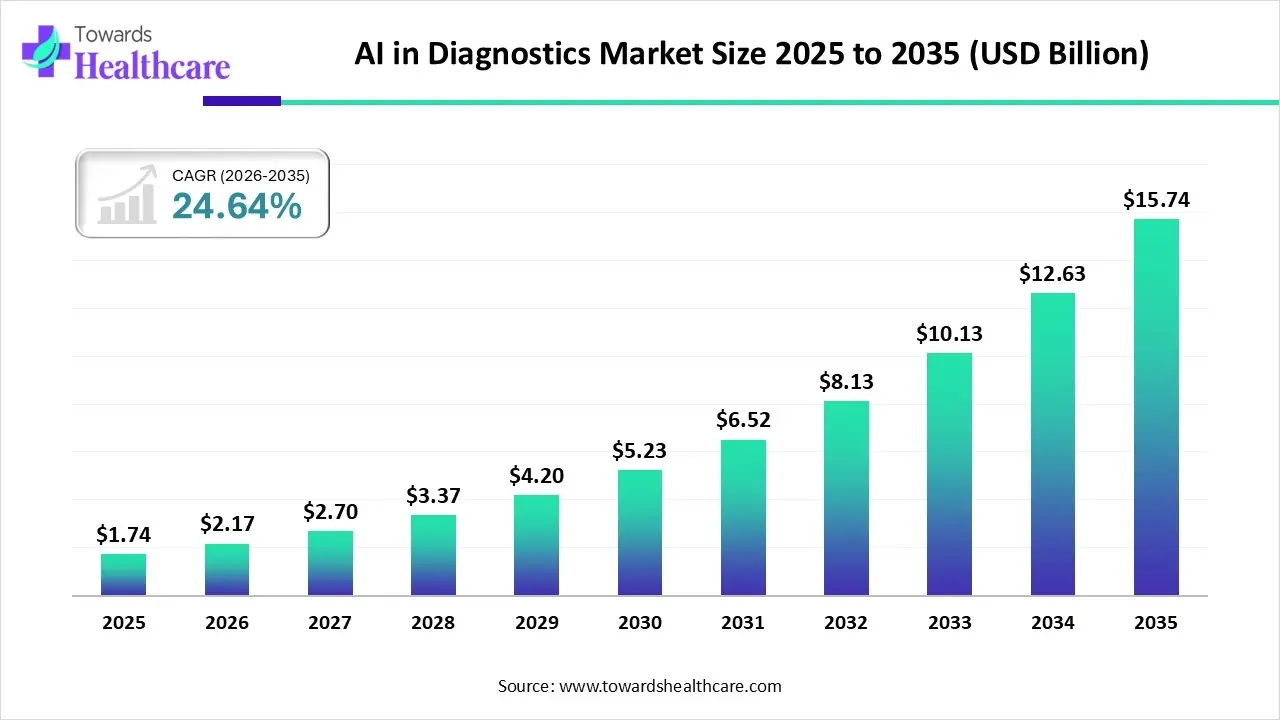
Specifically, cardiology, oncology, and radiology are leading this shift toward automated, data-driven insights.
1. Rising volume of imaging studies
Modern hospitals produce more CT, MRI, and X-ray data than ever before. This surge creates massive pressure on existing radiology teams. AI-assisted triage solves this by automatically flagging urgent cases for immediate review.
These tools allow your practice to manage higher volumes without adding new headcount. This technology effectively removes bottlenecks and keeps patient throughput moving smoothly.
2. Improved accuracy and early detection
Algorithms excel at spotting tiny irregularities that are easy to miss. This is especially vital for identifying early-stage cancers or neurovascular issues. Using AI boosts diagnostic sensitivity and leads to much more reliable treatment paths. It also prevents the need for costly and repetitive follow-up scans.
Your team can act earlier and with much higher clinical confidence.
3. Workflow efficiency and cost savings
Repetitive manual tasks like organ segmentation and measurement take up valuable time. AI tools automate these processes to give radiologists their time back. This focus on high-level analysis speeds up the entire reporting cycle.
Your facility benefits from lower operational costs and smarter resource allocation. Efficiency gains here directly impact your bottom line.
4. Growing support for value‑based care
Healthcare is shifting toward population-scale and outcomes-driven models. Payers now reward providers who can demonstrate long-term patient health improvements. AI-enhanced imaging aligns perfectly with these preventive-care strategies. It provides the precise data needed for accurate risk stratification.
This ensures your organization remains compliant and profitable in a value-based market.
Investing in these diagnostic tools transforms a standard imaging department into a proactive clinical asset. This shift creates a scalable foundation for both improved patient care and sustainable business growth.
What is an AI Diagnostic Imaging System?
An AI diagnostic imaging platform is a specialized ecosystem that converts raw medical images into actionable clinical insights. It is far more than just an algorithm. Moreover, a complete system includes image ingestion, preprocessing, and secure annotation workflows.
It also features model training, clinical validation, and seamless integration with existing hospital reporting tools. At the same time, high-level security and continuous monitoring ensure the platform remains accurate and compliant in live medical environments.
How Long Does AI Diagnostic Imaging System Development Usually Take?
An AI diagnostic imaging system typically requires 4 to 6 months for a functional Minimum Viable Product (MVP). Developing a full-scale enterprise platform generally takes 9 to 18 months.
These timelines depend on several factors beyond just coding. You must account for data curation, clinical validation, and rigorous regulatory compliance. A basic diagnostic system focuses on core detection, while enterprise versions offer deep integration and scalability.
Quick Timeline Estimate By Project Type
| AI Diagnostic Imaging System Type | Estimated Timeline | Best Fit |
| Proof of Concept | 8–12 weeks | Testing feasibility with limited image data |
| MVP Diagnostic Imaging Tool | 4–6 months | Single modality, limited workflow, early validation |
| AI-Assisted Radiology Platform | 6–9 months | PACS-connected platform with review workflow |
| Enterprise Diagnostic Imaging System | 9–18 months | Multi-user, integrated, secure, scalable system |
| Regulated AI Medical Device Platform | 12–24 months | Systems requiring deep clinical validation |
Understanding the Development Variables
The complexity of your target modality is the primary driver of these estimates. Different types of medical data require vastly different levels of engineering effort:
- X-ray and Ultrasound: These systems often move faster. The 2D nature of the data allows for simpler preprocessing and lower computational costs.
- CT and MRI: These involve massive 3D datasets. They require sophisticated AI orchestration to handle hundreds of “slices” per study.
- Digital Pathology: This represents the highest complexity. High-resolution slides create enormous files that demand specialized data pipelines and high-end GPU clusters.
Furthermore, the “AI model” is actually a small part of the total roadmap. Most of your time will be spent on the following mission-critical layers:
- Data Curation: Acquiring and cleaning high-quality, diverse datasets is the biggest bottleneck. You need thousands of verified images to avoid algorithmic bias.
- Workflow Integration: The system must connect to existing PACS (Picture Archiving and Communication Systems) and HL7/FHIR interfaces. If it breaks the radiologist’s current flow, they will not use it.
- Regulatory Compliance: Navigating FDA or CE marking is not optional. This phase requires rigorous clinical trials and documentation that can add 6 to 12 months to the launch date.
So, the real question is not only how long development takes. It is the type of diagnostic imaging system you are trying to build.
What Makes AI Diagnostic Imaging Development Time-Intensive?
Diagnostic imaging platforms require more time than general software because they involve massive data pipelines, strict HIPAA security, and clinical validation against “ground truth” labels provided by medical specialists.
Building a medical AI tool is much harder than creating a standard phone app. You aren’t just dealing with buttons and menus. You are handling massive, sensitive medical files that require perfect accuracy. These systems need high-grade data, careful cleaning, and testing by actual doctors.
Every layer of the process adds time because safety is the top priority. Skipping these steps can lead to wrong diagnoses and major business risks.
1. Needs More Than Standard App Development
Most health apps just manage simple tasks like scheduling or payments. An imaging platform is different because it must “think” like a radiologist. The system has to ingest huge image files and run complex math to find health issues.
It also needs a way for doctors to review and sign off on what the AI finds. This requires a much deeper level of engineering than a typical dashboard or website.
2. Data Quality Often Controls The Timeline
The speed of your launch depends entirely on how good your medical images are. If the data is messy, the AI will make mistakes. We focus on several critical factors to ensure the system is reliable:
- Accurate Labels: Real doctors must mark exactly where a problem is in thousands of images.
- Scanner Differences: The AI must work whether the scan came from an old machine or a brand-new one.
- Removing Privacy Info: Every image must be scrubbed of names and IDs to stay legal and secure.
- High Resolution: Medical scans are very large. Moving them quickly requires specialized “pipes” in the software.
- Handling Gaps: If you don’t have enough examples of a rare disease, the AI needs extra training time.
3. Clinical Validation Adds Time But Reduces Risk
Before any patient uses the tool, it undergoes a “stress test” called clinical validation. We run the AI on old cases where we already know the outcome. This proves the system is accurate in the real world, not just in a lab.
Testing locally is vital because an AI might act differently depending on the hospital’s equipment. At the same time, constant feedback loops with radiologists help us catch errors early. This process builds a platform that doctors actually trust and use.
This technical depth is exactly why general software teams often fail in healthcare. Success requires a partner who knows that clinical accuracy is the only way to protect your investment.
AI Diagnostic Imaging Development Timeline By Stage
Creating a reliable medical AI platform requires a structured, multi-step journey. This process ensures the final product is not just a smart algorithm, but a tool doctors can actually trust. Each stage has specific goals and timeframes to manage the technical and clinical needs of a healthcare environment.
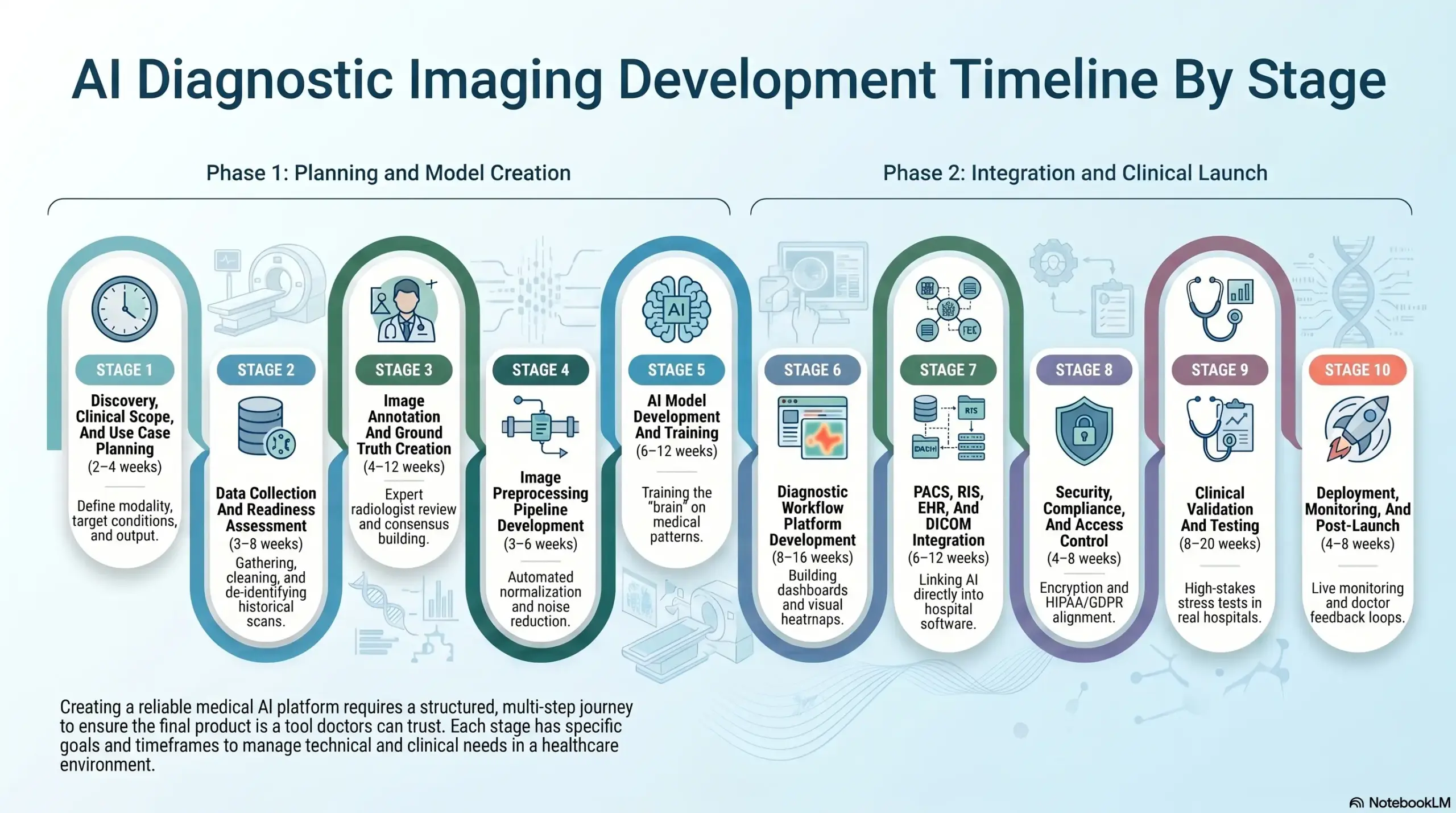
Stage 1 — Discovery, Clinical Scope, And Use Case Planning
Estimated timeline: 2–4 weeks
This initial phase defines the “what” and “why” of your project. You must decide exactly what the AI will look for and how it fits into a doctor’s day. Choosing a clear focus early prevents expensive changes later.
- Select Modality: Will the system analyze X-rays, CT scans, or MRIs?
- Target Conditions: Examples include lung nodules in CT scans, fractures in X-rays, or stroke signs in brain scans.
- Define Output: Should the AI just flag urgent cases (triage), find a tumor (detection), or outline it (segmentation)?
- Map Workflow: Identify exactly where the radiologist will see the AI’s results.
Stage 2 — Data Collection And Readiness Assessment
Estimated timeline: 3–8 weeks
The AI needs thousands of historical images to learn. This stage involves gathering those scans and making sure they are usable. If a hospital’s data is messy or unorganized, this phase can take much longer.
| Activity | Description |
| Data Gathering | Collecting old studies from various imaging machines. |
| Quality Check | Removing blurry scans or incomplete files. |
| Privacy Check | Stripping patient names and IDs to stay legal. |
| Format Review | Ensuring all files follow the standard DICOM format. |
Stage 3 — Image Annotation And Ground Truth Creation
Estimated timeline: 4–12 weeks
This is often the biggest timeline driver. Real doctors must manually “tag” images so the AI knows what a healthy scan looks like versus a sick one. This “ground truth” is the foundation of the system’s accuracy.
- Expert Review: Radiologists draw boxes or masks around areas of interest.
- Consensus Building: Multiple doctors review the same image to ensure the labels are 100% correct.
- Dataset Splitting: Dividing images into groups for training, testing, and final validation.
Stage 4 — Image Preprocessing Pipeline Development
Estimated timeline: 3–6 weeks
Before the AI “sees” an image, the software must clean it up. This is like preparing ingredients before cooking. We build pipelines that automatically handle things like noise reduction and image alignment.
- Normalization: Making images from different machines look consistent.
- Resolution Handling: Ensuring the AI can read both high and low-detail scans.
- Secure Storage: Setting up a safe place to hold these massive image files.
Stage 5 — AI Model Development And Training
Estimated timeline: 6–12 weeks
This is where the actual “brain” of the system is built. Engineers use specialized math and computers to teach the model how to recognize medical patterns.
- Architecture Selection: Choosing the best AI structure for the specific job.
- Training: Running the model through thousands of images to improve its “vision.”
- Performance Metrics: We track how well it works using several key scores:
- Sensitivity: How good is it at finding every sick patient?
- Specificity: How good is it at not bothering healthy patients?
- Accuracy: Overall correctness in its predictions.
Stage 6 — Diagnostic Workflow Platform Development
Estimated timeline: 8–16 weeks
The AI model needs a home. This stage focuses on building the dashboard and tools that doctors will use every day. Intellivon builds this entire ecosystem to ensure the AI results are easy to see and act upon.
- User Dashboard: A clean screen for doctors to track cases.
- Visual Overlays: Using “heatmaps” to show the doctor exactly where the AI sees a problem.
- Audit Logs: Keeping a digital record of every action for safety and legal reasons.
Stage 7 — PACS, RIS, EHR, And DICOM Integration
Estimated timeline: 6–12 weeks
Radiologists do not want to log into a separate website to see results. The AI must live inside their existing software (like PACS or RIS). This is why seamless integration is the only way doctors will actually use the tool.
- System Connection: Linking the AI directly to hospital imaging archives.
- Report Sync: Automatically pushing AI findings into the final medical report.
- Workflow Productivity: Ensuring the AI speeds up the day instead of adding more clicks.
Stage 8 — Security, Compliance, And Access Control
Estimated timeline: 4–8 weeks
Healthcare data is highly protected, and that is why security cannot be an afterthought. We build deep layers of protection to ensure patient privacy is never compromised.
- Encryption: Locking data so it cannot be stolen while moving or sitting in storage.
- Role-Based Access: Ensuring only authorized doctors can see specific patient scans.
- HIPAA/GDPR Alignment: Building the system to follow global privacy laws from day one.
Stage 9 — Clinical Validation And Testing
Estimated timeline: 8–20 weeks
This is a high-stakes stress test. We prove the system works in a real hospital setting, not just a quiet lab. This step reduces your business risk by catching errors before they affect patients.
| Testing Type | Goal |
| Retrospective | Testing the AI on thousands of past cases with known outcomes. |
| Multi-Site | Checking if the AI works across different hospitals and equipment. |
| Bias Testing | Ensuring the AI is fair and accurate for all types of patients. |
Stage 10 — Deployment, Monitoring, And Post-Launch Optimization
Estimated timeline: 4–8 weeks for launch
Once the system goes live, the work continues. AI systems need constant watching because medical data and equipment change over time. We monitor the tool to ensure it stays accurate and fast.
- Live Monitoring: Tracking how fast the AI gives results.
- Drift Detection: Checking if the AI is becoming less accurate over time.
- Feedback Loops: Collecting doctors’ comments to make the system better every month.
This 10-stage process is how Intellivon delivers enterprise-grade AI that actually works in a clinical setting. By following this roadmap, we turn complex medical data into a scalable growth engine for your business.
Timeline Breakdown For Different AI Diagnostic Imaging Systems
Development speed depends heavily on the type of medical images your system needs to analyze. While basic 2D scans move quickly through the pipeline, complex 3D datasets require significantly more engineering and validation time.
Choosing the right modality early helps you set realistic expectations for your board and investors.
Quick Timeline Reference by Imaging Type
| Imaging Modality | Estimated Development Time | Data Complexity |
| X-ray Systems | 4–8 Months | Low (2D Images) |
| CT Scan Analysis | 6–12 Months | Medium (3D Slices) |
| Ultrasound Tools | 6–12 Months | Medium (Video/Real-time) |
| MRI Diagnostic | 8–14 Months | High (Multi-sequence) |
| Pathology Imaging | 9–18 Months | Very High (Whole-slide) |
| Multi-Modality Platform | 12–24 Months | Extreme (Unified Ecosystem) |
1. Timeline for Building an AI X-Ray Diagnostic System
Estimated timeline: 4–8 months
X-ray projects are often the fastest to market because the data is less complex. Since these are standard 2D images, the AI can process them without massive computing power. However, you still need high-quality labels from doctors to ensure the system is safe for clinical use.
- Common Use Cases: Detecting bone fractures, screening for pneumonia, or spotting chest abnormalities.
- Why It Is Faster: Lower image file sizes and simpler processing steps compared to 3D scans.
- Key Focus: Validation is still essential to ensure the AI works across different clinic locations and machine brands.
2. Timeline for Building an AI CT Scan Analysis System
Estimated timeline: 6–12 months
CT scans are much more detailed than X-rays because they contain hundreds of 3D slices. The AI must analyze every single layer to find small issues like internal bleeding. This depth requires more infrastructure and a longer testing phase to ensure nothing is missed.
- Common Use Cases: Stroke triage, lung nodule detection, and identifying pulmonary embolisms.
- Technical Needs: High-speed processing to handle the large volume of data in each study.
- Validation: Requires slice-level analysis to ensure the AI points the doctor to the exact location of the problem.
3. Timeline for Building an AI MRI Diagnostic System
Estimated timeline: 8–14 months
MRI systems deal with a very high variation in how images look. Different sequences and planes of view make it harder for an AI to learn patterns quickly. Because of this complexity, the preprocessing and validation cycles are much longer than those of other modalities.
- Common Use Cases: Brain tumor segmentation, neurological analysis, and musculoskeletal imaging.
- Main Challenge: The AI must be trained to handle multi-plane imaging without losing accuracy.
- Strategy: Expect a longer data preparation phase to account for the unique way MRI machines capture data.
4. Timeline for Building an AI Ultrasound Diagnostic System
Estimated timeline: 6–12 months
Ultrasound imaging is unique because the quality of the scan depends on the person holding the probe. The AI must be smart enough to handle blurry or moving images in real-time. This requires a heavy focus on usability and workflow design.
- Common Use Cases: Cardiac imaging, fetal assessment, and thyroid or breast screening.
- Workflow Design: The AI results often need to appear immediately while the doctor is still with the patient.
- Requirement: Strong focus on noise reduction to clean up the grainy nature of live ultrasound feeds.
5. Timeline for Building an AI Pathology Imaging System
Estimated timeline: 9–18 months
Pathology involves whole-slide images that are incredibly large. These files are much bigger than a standard MRI or CT scan. Managing these huge datasets requires specialized storage and extremely high-end computing clusters.
- Common Use Cases: Cancer detection, cell counting, and tissue classification.
- Annotation Needs: Doctors must spend significant time labeling tiny cell structures across massive digital slides.
- Infrastructure: Your team will need to build heavy-duty data pipelines to move these files without crashing the system.
6. Timeline for Building A Multi-Modality AI Imaging Platform
Estimated timeline: 12–24 months
A multi-modality platform is the ultimate enterprise solution. It combines different types of scans into one unified workflow for a whole hospital system. Because it handles everything from X-rays to MRIs, the validation and integration burden is very high.
- Scope: Multiple AI models running inside a single, secure dashboard.
- Integrations: Deep connections with PACS, RIS, and EHR systems across several hospital sites.
- Architecture: Requires a scalable cloud or hybrid deployment that can grow as the hospital adds more departments.
Building these specialized systems requires enterprise-grade clinical expertise. Intellivon specializes in navigating these modality-specific challenges to ensure your platform delivers clear ROI. By aligning your development timeline with the specific needs of your imaging data, we help you build a reliable, enterprise-grade solution.
What Factors Can Increase The Development Timeline?
Several variables can stretch your roadmap beyond the initial estimates. Development involves aligning technical performance with clinical safety and hospital IT requirements. Understanding these time multipliers allows you to budget more accurately and avoid common launch delays.
1. Imaging Modality And Diagnostic Complexity
The specific task you ask the AI to perform dictates much of the schedule. A system that simply flags a scan as “normal” or “abnormal” (classification) is faster to build than one that must draw a 3D boundary around a tumor (segmentation).
Tasks like quantitative measurement or diagnosing multiple conditions simultaneously add significant layers of testing and refinement.
2. Dataset Size, Quality, And Availability
The speed of your project is tethered to your data. If you already have thousands of clean, labeled images from diverse sources, you can move quickly. However, timelines often expand when you must:
- Negotiate access to hospital archives.
- Clean up inconsistent data from different scanner brands.
- Find enough examples of rare conditions to ensure the AI isn’t biased.
- Bridge gaps where historical data is missing or incomplete.
3. Annotation And Radiologist Review Requirements
Reliable AI requires a “ground truth” established by experts. Having senior radiologists review and label every scan in your training set takes time and can be expensive.
While this phase can feel like a bottleneck, it is the only way to build clinical trust and ensure the model performs accurately in a real-world medical setting.
4. AI Model Type And Performance Target
Your performance goals directly impact the training duration. If you require extremely high sensitivity to ensure zero missed cases, the engineering team must spend more time on “performance tuning.”
- Detection: Finding the location of an issue.
- Quantification: Measuring the size or volume.
- Prioritization: Sorting the worklist for the doctor.
- Multi-model decisioning: Running several models at once for a comprehensive review.
5. PACS, RIS, And EHR Integration Scope
Integration can be a major variable. On the other hand, connecting to a single department’s imaging archive is relatively straightforward.
However, if the platform must support multiple hospital sites, different electronic health record (EHR) systems, and various radiology workflows, the engineering complexity increases. Each new connection requires unique testing to ensure data flows securely and without lag.
6. Compliance And Regulatory Expectations
Medical AI is often classified as “Software as a Medical Device.” This means you cannot simply launch and iterate like a standard consumer app. You must maintain strict documentation and quality controls throughout the entire lifecycle.
Regulatory bodies look for systems that can safely learn and improve over time, which requires a rigorous framework for monitoring and updates.
6. Deployment Model: Cloud, On-Premise, Or Hybrid
Where the software “lives” affects your speed to launch.
- Cloud Deployment: Generally, the fastest, as the infrastructure is ready to scale immediately.
- On-Premise: Often takes longer because it must pass through rigorous hospital IT and security reviews.
- Hybrid Systems: Offer a balance but require more complex architecture planning to manage how data moves between the hospital and the cloud.
7. Number Of User Roles And Clinical Workflows
The more people who need to use the system, the more features you have to build. A tool used only by a radiologist is simpler than one that must also serve technicians, referring physicians, and hospital administrators.
Each role needs its own dashboard, access permissions, and notification settings to ensure the right information reaches the right person.
8. Validation Depth And Real-World Testing
Deeper validation is a time investment in safety. Testing the AI across multiple hospital environments, rather than just one, ensures it can handle variations in image quality and patient populations.
This makes the platform much more “enterprise-ready” and significantly reduces the risk of failure after the official launch.
Understanding these variables allows you to build a realistic roadmap that prioritizes clinical safety over raw speed. By addressing these factors early, you ensure your platform is robust enough to handle the high-stakes demands of a live hospital environment.
Can You Build An AI Diagnostic Imaging MVP Faster?
A 120-to-180-day development cycle is achievable by focusing on a single modality and one diagnostic condition, utilizing pre-labeled datasets and limited PACS integrations to prove clinical feasibility.
Launching a Minimum Viable Product (MVP) within a shorter timeframe is possible if you focus on a specific, high-impact problem. By narrowing the scope, you can validate your core technology and business model without waiting years for a full-scale rollout.
This approach allows you to gather real-world feedback and secure further investment while the system begins to deliver measurable value.
What A 4–6 Month MVP Can Include
A successful MVP focuses on the absolute essentials required to prove the system works. It should provide a clear path from image ingestion to a verified result. By keeping the features lean, you ensure the core AI model receives the attention it needs to be accurate.
- One Imaging Modality: Focus specifically on X-ray, CT, or MRI rather than trying to handle all three.
- One Diagnostic Use Case: Target a single abnormality, such as detecting a specific type of fracture or a certain lung condition.
- Basic Ingestion: A simple way to upload images or a limited connection to a single imaging archive.
- Result Visualization: A clean screen where a radiologist can see the AI findings and provide a quick review.
- Performance Testing: Initial data showing the tool meets your basic accuracy and safety targets.
What Should Not Be Forced Into The First MVP
Attempting to build too much too soon is the leading cause of project failure. Overcomplicating the first version adds massive technical debt and extends the timeline indefinitely. Save these complex features for later versions once the primary tool is stable:
- Multi-Site Rollout: Stick to one clinic or department initially to manage variables effectively.
- Full Automation: The MVP should assist a doctor, not attempt to replace the entire reporting workflow.
- Custom Dashboards: Avoid building excessive administrative tools that do not contribute to the actual diagnosis.
- Too Many Conditions: Trying to find ten different diseases at once will dilute the quality of your training data.
How Intellivon Helps Reduce MVP Timelines
Building on the right foundation is the key to speed. We help you skip the trial-and-error phase by providing a structured path to a working product. At the same time, our approach ensures that even a fast-tracked system remains enterprise-ready from day one.
- Clear Scope Definition: We help you identify the specific use case that offers the highest ROI with the least technical friction.
- Data Readiness Assessment: We quickly evaluate your current image archives to see what can be used for training immediately.
- Modular Architecture: We use reusable imaging pipelines that handle the heavy lifting of data movement and security automatically.
- Integration-First Planning: We ensure your MVP is built to connect with hospital systems later, so you do not have to rebuild from scratch.
- Early Validation Framework: We start the testing process early, giving you confidence in the model’s accuracy long before the final launch.
A faster MVP should not mean a weaker system. Instead, it should mean a narrower system built on the right foundation.
How To Reduce Development Time Without Increasing Risk
Reducing the development cycle requires a shift in strategy from broad experimentation to narrow, high-impact execution. You can cut months off your timeline by focusing on the underlying data and engineering architecture before the first line of AI code is even written.
This proactive approach ensures you build a system that is both fast to market and clinically safe.
1. Start With One High-Value Diagnostic Use Case
A common mistake is trying to build a system that can see everything at once. One focused use case beats a broad idea every time. By narrowing your focus, you can gather higher-quality data and move through the validation phase much faster.
- Chest X-ray Triage: Automatically flagging abnormal scans for immediate review.
- CT Stroke Detection: Identifying signs of bleeding in brain scans within seconds.
- MRI Tumor Segmentation: Outlining the exact boundaries of a lesion for surgery planning.
- Ultrasound Fetal Support: Automating standard measurements to save the technician time.
2. Audit Imaging Data Before Development Begins
Your project will stall if your engineers spend months cleaning messy data. At the same time, you must audit your image archives before development begins to identify gaps early.
- Quantity: Do you have enough examples of both healthy and sick cases?
- DICOM Consistency: Are the files in a standard format that the AI can read?
- Scanner Variation: Does your data come from multiple types of machines or just one?
- Privacy Needs: Is there a clear process to remove all patient names and IDs?
3. Build The AI Pipeline And Platform In Parallel
The AI model and the software platform around it should be developed at the same time. The engineering team can build the secure image ingestion layer and the doctor’s dashboard while the data scientists train the algorithm.
This parallel workstream ensures that once the model is ready, it already has a home to live in.
4. Plan PACS And RIS Integration Early
Waiting until the end of the project to think about hospital integration is a major risk. You need to know how the AI will talk to existing hospital software from day one.
Planning for DICOM and HL7 connections early prevents you from having to rebuild your entire data structure later in the project.
5. Use Modular Architecture For Future Expansion
Build your system in separate pieces rather than one giant block of code. This modular approach makes it easier to update the AI model without breaking the entire platform.
- Ingestion Layer: Handles the incoming images from the hospital.
- Inference Layer: Where the actual AI math happens.
- Review Workflow: The screen where the doctor sees and approves the result.
- Reporting Layer: Automatically sends the findings to the patient’s record.
6. Keep Clinical Review In The Loop
Radiologists should be involved in every stage of development. Their feedback on how the results are displayed or how the AI behaves reduces the need for expensive rework.
When doctors help build the tool, the final product is much more likely to be adopted and trusted by other medical professionals.
7. Avoid Overbuilding The First Version
Focus on building for scalability rather than building every possible feature. Your first version should be strong, safe, and accurate, but it does not need ten different custom dashboards or fully automated reporting. Launching a lean, high-quality system allows you to start generating ROI while you plan for the next round of features.
Balancing speed and safety is the hallmark of a successful enterprise AI strategy. By focusing on modular design and early data audits, you create a scalable platform that meets the rigorous demands of modern healthcare. This foundation ensures your investment is protected as you move from a narrow MVP to a comprehensive diagnostic solution.
Common Timeline Mistakes That Delay AI Diagnostic Imaging Projects
Most project delays do not stem from the AI model failing to learn. Instead, they happen because of a lack of foresight regarding how the system will exist in a high-pressure hospital environment.
Avoiding these common traps ensures your development stays on track and your final product actually reaches the clinical floor.
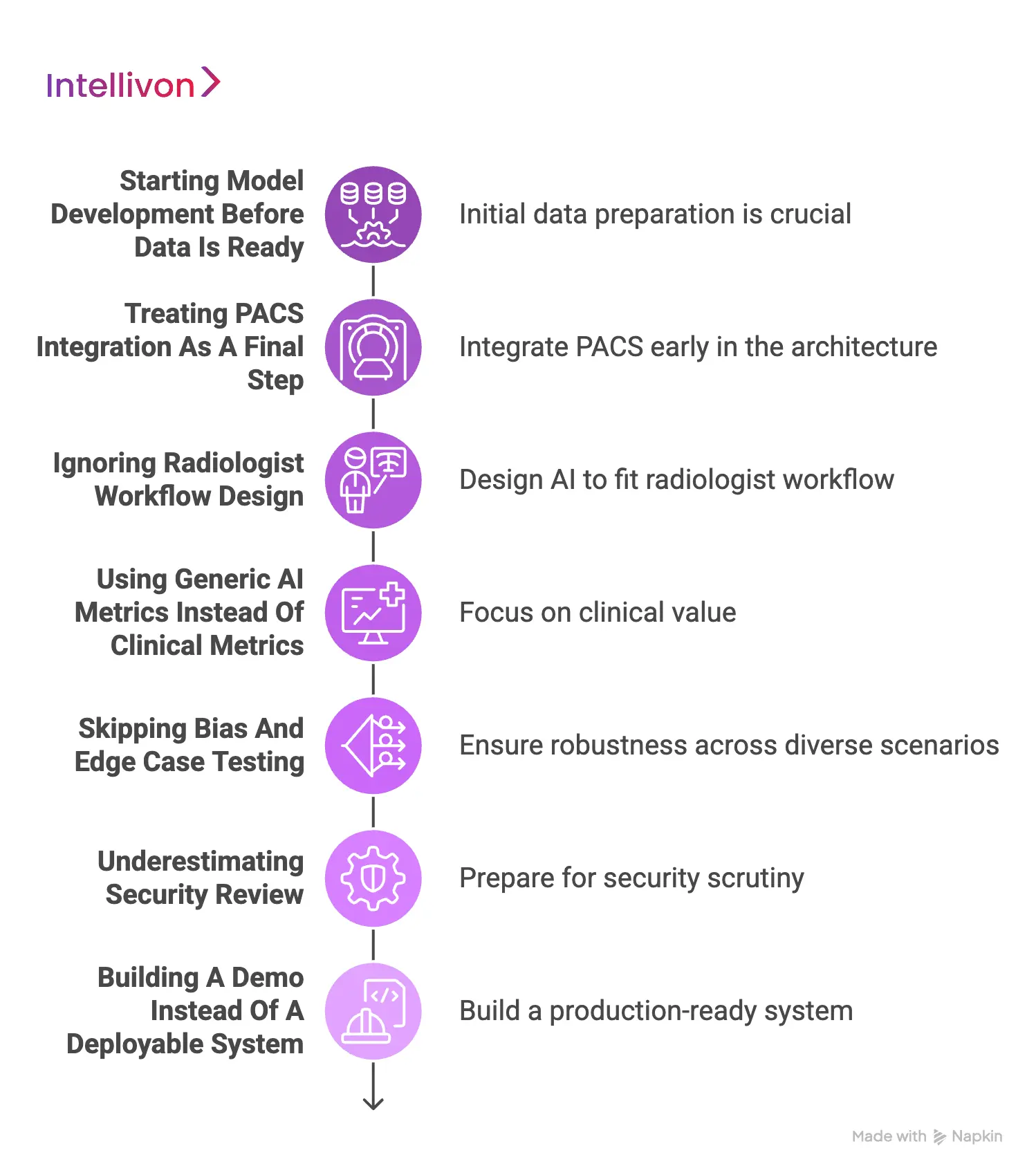
1. Starting Model Development Before Data Is Ready
It is tempting to start training a model as soon as you have a few hundred images. However, if your data readiness is poor, you will eventually have to start over.
Training on messy, unverified, or biased data leads to a tool that fails clinical testing. Investing the first few months in deep data cleaning and expert labeling prevents massive rework later.
2. Treating PACS Integration As A Final Step
Integration is not a simple plug-and-play task to be handled at the end of the roadmap. The way images move from a hospital archive into your AI dictates how you should build your entire software architecture.
If you treat this as a final step, you may find that your system is too slow or incompatible with the hospital’s existing network, forcing a complete redesign.
3. Ignoring Radiologist Workflow Design
Even the most accurate AI will fail if it makes a doctor’s job harder. Radiologists work in high-speed environments where every click matters. If your AI findings are buried in a separate menu or require a different login, the tool will be ignored.
Successful systems are built to fit naturally into the existing radiology reading flow, enhancing speed rather than interrupting it.
4. Using Generic AI Metrics Instead Of Clinical Metrics
Traditional tech metrics like raw accuracy do not always tell the whole story in healthcare. To build trust with enterprise buyers, you must focus on clinical metrics that prove real-world value.
- Sensitivity and Specificity: How many sick patients did the AI miss?
- False Positives: How much extra work did the AI create by flagging healthy scans?
- Turnaround Time: Did the tool actually help the hospital deliver results faster?
- Triage Accuracy: Was the most urgent case moved to the top of the list correctly?
5. Skipping Bias And Edge Case Testing
An AI might work perfectly on data from one specific scanner but fail on images from another brand. Skipping tests on diverse patient groups or different machine types creates a significant safety risk.
You must test for edge cases, such as low-resolution scans or unusual patient anatomy, to ensure the tool is robust enough for any hospital setting.
6. Underestimating Security Review
Hospital IT and compliance teams are the gatekeepers of patient data. They require extensive documentation on how you encrypt data and who has access to it. These reviews can take months and often involve deep audits of your cloud or on-premise setup.
Failing to prepare for this security scrutiny early in the timeline is one of the most common reasons for a delayed launch.
7. Building A Demo Instead Of A Deployable System
There is a big difference between an AI demo that looks good in a meeting and a production system that works 24/7 in a hospital. Many teams focus only on the algorithm, leaving the actual infrastructure as an afterthought.
This is where the experience of a partner like Intellivon becomes a critical advantage. We focus on building production-grade infrastructure from day one, ensuring your platform is ready for deployment, not just a proof-of-concept demonstration.
Success in medical AI requires a balance of technical skill and clinical understanding. By avoiding these common pitfalls, you protect your investment and build a diagnostic tool that provides lasting value to both doctors and patients.
Conclusion
Building an AI diagnostic imaging system is a complex journey that rewards precision over speed. Success depends on a strategic balance between clinical-grade data, expert annotation, and seamless hospital integration.
By focusing on a narrow, high-value MVP and following a structured development roadmap, enterprise leaders can mitigate risks and ensure scalability. Ultimately, the right foundation transforms medical data into a powerful, sustainable engine for better patient outcomes and growth.
Build AI Diagnostic Imaging Systems With Intellivon
At Intellivon, we build AI diagnostic imaging systems for hospitals, diagnostic labs, radiology platforms, healthtech companies, and medical imaging startups. Our approach focuses on real clinical workflows, secure image pipelines, AI-assisted review, scalable deployment, and integration with existing healthcare systems.
Whether you want to launch a focused MVP in 4–6 months or build a production-ready enterprise imaging platform over 9–18+ months, Intellivon helps you define the right scope, reduce development risk, and build a system that is ready for real healthcare environments.
A. Building The AI Imaging Pipeline
Our engineering team designs the full AI imaging pipeline, from DICOM ingestion to model inference and result visualization. This allows radiologists and clinical teams to review AI outputs within a structured, usable workflow.
This includes:
- DICOM image ingestion and metadata extraction
- Image preprocessing for modality-specific quality control
- Annotation workflows for model training and validation
- AI model development for detection, classification, or segmentation
- Real-time or batch inference pipelines
- AI result visualization through overlays, scores, and review screens
This ensures the AI system is not just technically functional, but clinically usable.
B. Designing Clinical Review Workflows
Our platforms can include radiologist dashboards, case prioritization, AI overlays, reporting support, review status tracking, and human-in-the-loop feedback. These workflows help care teams use AI as a decision-support layer while maintaining clinical control.
Workflow capabilities can include:
- Radiologist reviews dashboards
- Case prioritization for urgent scans
- AI overlays, heatmaps, and confidence indicators
- Review status and approval workflows
- Reporting support and structured findings
- Feedback loops for model improvement
This helps enterprises move beyond AI demos and build systems that fit real diagnostic environments.
C. Integrating With Existing Healthcare Systems
At Intellivon, we build integration-ready architectures for PACS, RIS, EHR, EMR, and DICOM-based workflows. This allows your AI imaging system to fit into current radiology operations instead of forcing teams to switch between disconnected tools.
Integration areas include:
- PACS integration for image retrieval and routing
- RIS integration for radiology workflow alignment
- EHR/EMR connectivity for patient and report data
- DICOM routing and image exchange
- Report synchronization across systems
- Multi-site support for enterprise imaging networks
This reduces adoption friction and helps the platform become part of the clinical workflow from the start.
D. Making The Platform Secure And Scalable
We design systems with role-based access, encrypted storage, audit trails, secure deployment, model monitoring, and long-term scalability.
This helps healthcare enterprises prepare for real-world usage, larger imaging volumes, new AI models, and future multi-site expansion.
Security and scalability features include:
- Role-based access control for clinical and admin users
- Audit trails for AI outputs, user actions, and review history
- Encrypted image storage and secure data transfer
- Cloud, on-premise, or hybrid deployment architecture
- Model monitoring for performance, drift, and errors
- Scalable architecture for new modalities, users, and sites
This gives your AI diagnostic imaging system the foundation to grow beyond the first release.
Build Your AI Diagnostic Imaging System With Intellivon
If you are planning to build an AI diagnostic imaging system, Intellivon can help you define the right timeline, technical roadmap, AI architecture, integration scope, and deployment strategy.
From MVP planning to enterprise rollout, we build diagnostic imaging platforms that combine AI models, clinical workflows, secure image pipelines, PACS/RIS integrations, validation support, and scalable infrastructure.
Contact Intellivon to plan and build an AI diagnostic imaging system that is secure, clinically usable, and ready for enterprise deployment.
FAQs
Q1. How long does it take to build an AI diagnostic imaging system?
A1. An AI diagnostic imaging MVP usually takes 4–6 months, while an enterprise-grade platform can take 9–18+ months. The timeline depends on imaging modality, data readiness, annotation quality, AI model complexity, PACS/RIS integration, validation needs, compliance scope, and deployment environment.
Q2. Is AI segmentation useful in diagnostic imaging platforms?
A2. Yes, AI segmentation can be useful when it supports specific clinical tasks like lesion detection, tumor boundary mapping, organ measurement, or disease progression tracking. However, its value depends on image quality, annotation accuracy, validation depth, and how smoothly the output fits into the radiologist’s review workflow.
Q3. Does an AI diagnostic imaging system need PACS and RIS integration?
A3. Yes, PACS and RIS integration are important for real clinical adoption. Without integration, radiologists may need to move between disconnected tools, which slows workflows. A well-built system should retrieve images, process AI outputs, support review, and sync reports within the existing imaging environment.
Q4. Should AI diagnostic imaging platforms use cloud or on-premise deployment?
A4. Both can work. Cloud deployment supports faster scaling, easier updates, and flexible compute. On-premise deployment gives hospitals more local control over imaging data and infrastructure. Many enterprises choose a hybrid model to balance security, latency, compliance, storage costs, and multi-site accessibility.