Hospitals rely heavily on EHR systems for documentation, coordination, and clinical decision-making, yet effective usage often depends on how well staff are trained across roles and workflows. Doctors, nurses, and administrative teams interact with EHRs differently, making an EHR training system for hospitals essential to bridge training gaps, prevent delays and errors, ensure consistent data entry, and help teams build confidence and accuracy in real clinical environments.
The most effective EHR training reflects real clinical practice, not isolated instruction, by using simulated workflows, role-based modules, guided scenarios, and feedback mechanisms that prepare staff for real-world usage. System success depends on mirroring clinical routines and remaining flexible to support ongoing learning and onboarding across departments.
In this blog, we explain how to develop an EHR training system for hospitals by examining core features, system architecture, and practical considerations involved in building scalable and effective training solutions for healthcare environments.
Why Hospitals Fail at EHR Training Today?
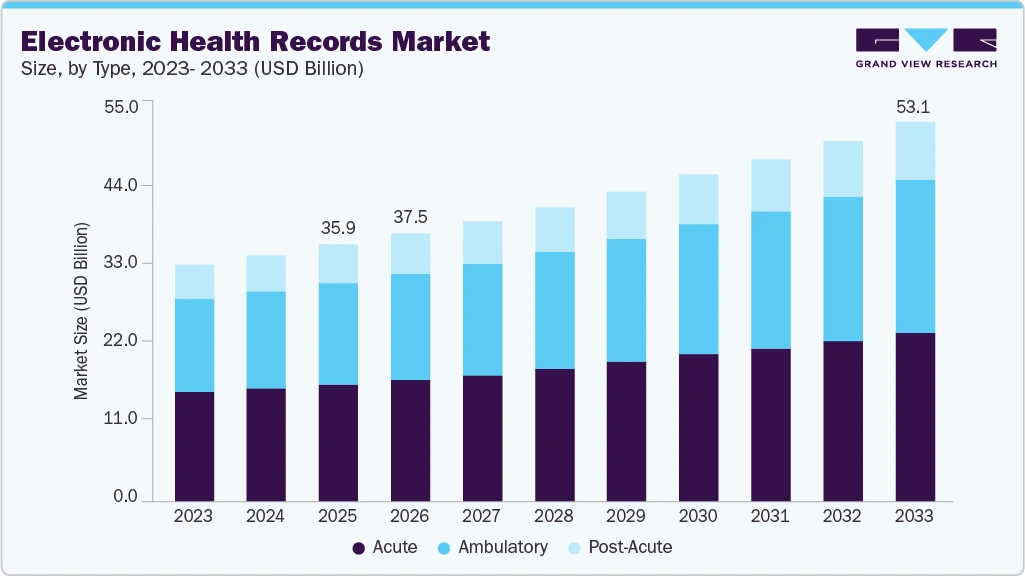
The global healthcare IT market is currently witnessing an unprecedented surge, with the EHR segment alone estimated at USD 35.89 billion in 2025 and projected to reach USD 53.11 billion by 2033, growing at a compound annual growth rate (CAGR) of approximately 5.10%. However, this financial expansion masks a critical operational crisis: hospitals often view software implementation as a one-time event rather than a continuous cultural shift.
Even with massive capital investments in top-tier platforms, the human element remains the most frequent point of failure. A poorly executed EHR training system for hospitals results in technical friction that alienates clinical staff and stunts the digital transformation process before it can yield measurable clinical benefits.
A. Low Adoption Despite Expensive EHR Systems
The acquisition of a premium platform does not guarantee efficient workflows. Implementing a tailored EHR training system for hospitals ensures that high-cost technology becomes a clinical asset rather than a generic obstacle.
This leads to a phenomenon where clinicians rely on unofficial workarounds to bypass the system.
| Challenge | Impact on Adoption |
| Generic Curriculum | Doctors ignore features that do not apply to their specific specialty. |
| Complex Interfaces | Users revert to manual notes when the digital path is not intuitive. |
| Lack of Value Prop | Staff see the EHR as a data entry burden rather than a diagnostic tool. |
| Inadequate Support | Frustration peaks when technical hurdles occur during active patient rounds. |
B. Workflow Gaps between Training and Real Use
The EHR training system for hospitals often fails by teaching features in isolation. This creates a reality gap, leaving staff unprepared for the high cognitive load and pressure of live clinical environments like shift changes.
Effective training architectures bridge this gap by focusing on integrated clinical scenarios:
- Multi-Role Simulations: Training should involve simultaneous inputs from pharmacy, nursing, and lab tech roles to mirror how data actually moves through a hospital.
- Environmental Stressors: Modules should include common interruptions, such as alert fatigue and emergency overrides, to test user proficiency under pressure.
- Data Accuracy Training: Using HL7 and FHIR standards in a sandbox environment allows users to see how their documentation affects downstream billing and clinical decision support.
C. Hidden Costs of Poor EHR Onboarding
The financial burden of an ineffective EHR hospital training system is rarely limited to the initial training budget. Inadequate onboarding creates a ripple effect of operational inefficiencies that can jeopardize the financial health of the entire institution.
- Productivity Loss: Physicians spend excessive hours on documentation after their shifts, leading to burnout and high turnover rates among high-value specialists.
- Revenue Leakage: Incorrect data entry and unfamiliarity with coding requirements lead to a surge in denied insurance claims and delayed reimbursements.
- Compliance Risks: Without rigorous training on HIPAA protocols within the EHR interface, the risk of accidental data breaches and regulatory fines increases significantly.
- Patient Safety Issues: Slow navigation or misinterpreted alerts can lead to medication errors or delayed treatments, which are the most costly failures of all.
What Is an EHR Training System in Practice?
The EHR training system for hospitals is a sophisticated infrastructure that mirrors live clinical environments. It allows staff to master complex documentation and data retrieval tasks in a controlled setting, ensuring proficiency without risking patient safety or data integrity.
A. Role-Based Learning for Clinical Staff
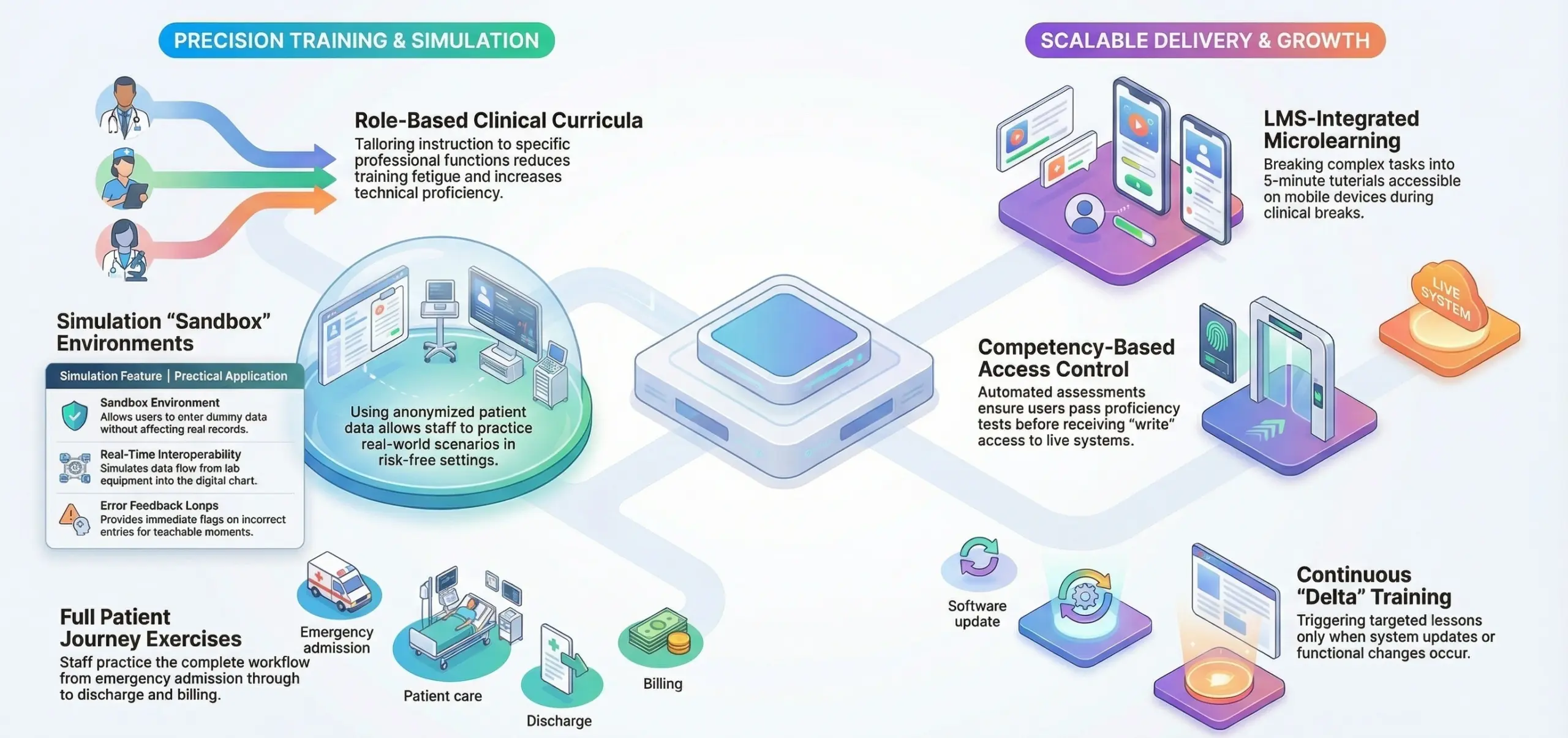
One of the most critical elements of a modern EHR training system for hospitals is the departure from universal instruction. Tailoring curricula to specific professional functions reduces training fatigue while significantly increasing technical clinical proficiency.
- Physician-Centric Workflows: Focuses on rapid order entry, clinical decision support alerts, and voice-to-text integration for efficient charting.
- Nursing and Support Staff: Emphasizes medication administration records (MAR), bedside vitals entry, and patient handoff protocols.
- Administrative and Financial Roles: Concentrates on patient registration accuracy, insurance verification, and HIPAA-compliant data management.
- Specialized Technicians: Prioritizes high-volume data entry and image retrieval for departments like radiology or pathology.
B. Simulation-Driven Training Environments
Static screenshots are insufficient for preparing staff for high-stakes environments. A high-quality EHR training system for hospitals utilizes a sandbox or shadow environment, which is a non-production instance containing anonymized patient data for safe practice.
This allows users to practice real-world scenarios in a risk-free setting.
| Simulation Feature | Practical Application |
| Sandbox Environment | Users can “break” the system or enter dummy data without affecting real patient records. |
| Scenario-Based Exercises | Practicing a full patient journey, from emergency admission to discharge and billing. |
| Real-Time Interoperability | Simulating how data flows via HL7/FHIR from lab equipment into the patient’s digital chart. |
| Error Feedback Loops | The system flags incorrect entries immediately, providing a teachable moment during the simulation. |
C. LMS Integration and Content Delivery Layers
The EHR training system for hospitals relies on a robust Learning Management System (LMS) for scalability. This integration provides structured content delivery while allowing administrators to track progress and verify competency across a massive clinical workforce.
- Microlearning Modules: Breaking down complex EHR tasks into 5-minute video tutorials or interactive guides that can be accessed on a tablet during a break.
- Competency Tracking: Automated assessments that require a passing score before a user is granted “write” access to the live production environment.
- Content Accessibility: Ensuring that training materials are available across multiple devices, supporting a mobile-first approach for clinicians who are constantly on the move.
- Certification Management: Automatically logging completed training hours for regulatory compliance and professional development records.
D. Continuous Learning with System Updates
The EHR training system for hospitals must adapt to frequent software patches and regulatory changes to remain effective. This high-performing infrastructure treats education as a continuous cycle, preventing programs from becoming obsolete shortly after onboarding.
- Delta Training Modules: When a major system update is deployed, the training system triggers short, targeted lessons focusing exclusively on interface or functional changes.
- Just-in-Time Learning: Integration of “help” overlays or tooltips within the live EHR environment provides immediate guidance during active documentation.
- Proactive Skill Gap Analysis: Using built-in analytics, the system identifies users struggling with specific new features and pushes automated refresher content to their dashboards.
- Regulatory Alignment: Continuous updates ensure that staff remain compliant with evolving HIPAA protocols and interoperability standards like FHIR without needing full retraining sessions.
Who Needs an EHR Training Platform the Most?
The demand for a structured EHR training system for hospitals is not uniform across the healthcare landscape. Specific high-stakes organizational profiles face significant risks when training is neglected, making a robust infrastructure essential for maintaining operational stability and clinical safety.
A. Multi-Specialty Hospitals Scaling Operations
As service lines expand into oncology or cardiology, data complexity increases. A flexible EHR training system for hospitals must accommodate these diverse specialty workflows while ensuring all departments maintain a unified and accurate patient record.
- Departmental Precision: Specialized training ensures that surgeons aren’t forced to navigate through primary care templates, reducing clicks and preventing “chart clutter.”
- Standardized Communication: Scaling operations requires that different departments speak the same “digital language,” ensuring that a lab result from one wing is correctly interpreted by a specialist in another.
- Centralized Oversight: A unified platform allows leadership to monitor training completion across multiple locations, ensuring that expansion does not dilute the quality of care or data compliance.
B. Hospitals Switching or Upgrading EHR Systems
Migrating to new or cloud-based platforms is a high-risk transition. Without a dedicated EHR training system for hospitals, the “go-live” period can cause operational paralysis, decreasing patient throughput while increasing staff frustration and burnout.
| Transition Phase | Strategic Training Requirement |
| Pre-Migration | Baseline assessments to identify which staff members will need the most support during the shift. |
| Parallel Testing | Using a sandbox environment to let staff practice with new workflows while the old system is still live. |
| Go-Live Support | Real-time, on-floor access to microlearning modules to resolve “how-to” questions instantly. |
| Post-Live Optimization | Advanced modules to help users move beyond basic entry to utilizing advanced analytics and reporting. |
C. Healthcare Groups with High Staff Turnover
Amidst high clinician burnout and nursing shortages, manual onboarding is unsustainable. A digital EHR training system for hospitals provides a scalable, repeatable process, ensuring every new hire meets institutional standards for data entry and HIPAA compliance efficiently.
- Rapid Onboarding: Automated modules allow new hires to reach clinical “full productivity” in days rather than weeks.
- Institutional Knowledge Retention: A digital system captures best practices and specific hospital protocols, ensuring that when a veteran staff member leaves, their knowledge of “how we do things here” stays within the platform.
- Audit Readiness: For hospitals relying on temporary staff, having a digital trail of training completion is vital for defending against malpractice claims or regulatory audits.
- Consistency of Care: Standardized training ensures that a traveling nurse in the ICU follows the exact same documentation protocols as a staff nurse, preventing errors caused by differing previous experiences.
Core Features of a High-Impact EHR Training System
The EHR training system for hospitals must function as a dynamic, workflow-integrated layer. Prioritizing user-centric design transforms these platforms from mandatory compliance tasks into vital tools that facilitate seamless patient care and clinical excellence.
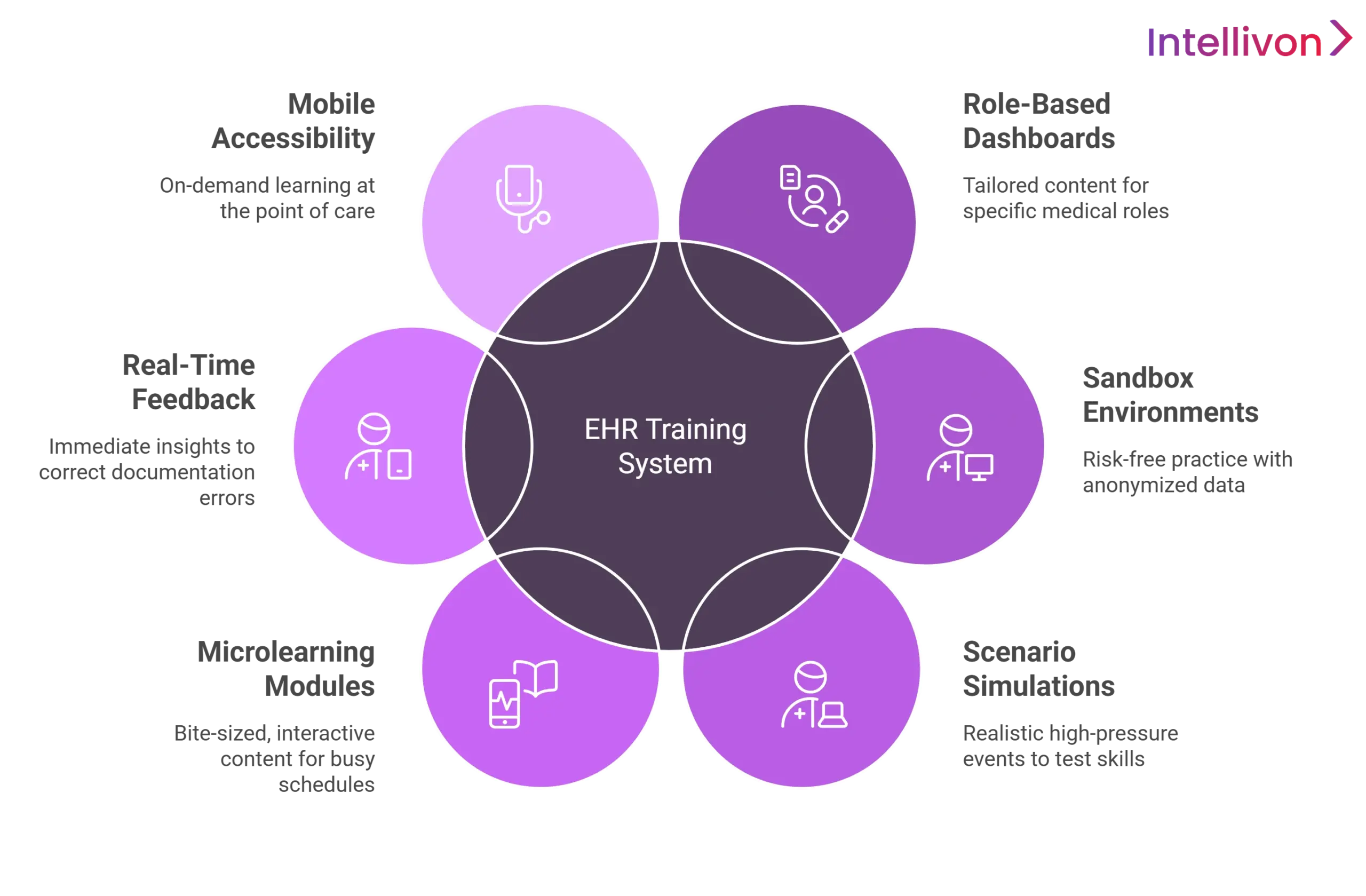
1. Role-Based Dashboards and Learning Paths
The EHR training system for hospitals uses role-based dashboards to filter content by credentials. This targeted approach ensures clinicians only see relevant modules and templates, significantly reducing unnecessary training time.
These personalized learning paths guide users from basic navigation to advanced clinical decision support. By focusing on professional identity, the system increases user engagement through specialty-specific tools like operative note templates.
2. Sandbox EHR Environments for Safe Practice
The sandbox EHR environment provides a risk-free mirror of the live system. This non-production instance allows staff to practice complex order entries and documentation using anonymized patient data without consequences.
Confidence grows as clinicians navigate this protected digital space. Users can freely test workflows and fail safely, ensuring they master the interface before interacting with a high-stakes EHR training system for hospitals’ production environment.
3. Scenario-Based Clinical Simulations
Traditional tutorials often fail because they lack clinical context. These scenario-based simulations recreate high-pressure events like code blues or rapid admissions to test cognitive load and technical speed simultaneously.
Staff members engage with realistic patient journeys rather than isolated buttons. This method ensures the EHR training system for hospitals effectively translates software knowledge into real-world muscle memory and improved patient safety outcomes.
4. Interactive Videos and Microlearning Modules
Long, static lectures frequently lead to information fatigue. These microlearning modules deliver bite-sized, interactive content that clinicians can consume in minutes, fitting seamlessly into the busy rhythms of a hospital shift.
Active participation is encouraged through embedded quizzes and clickable demonstrations. Modern EHR training system for hospitals architectures prioritize these short formats to ensure better knowledge retention and faster skill acquisition for medical staff.
5. Real-Time Feedback and Performance Tracking
Immediate insights are vital for correcting documentation errors. The system uses real-time feedback to alert users of mistakes instantly, reinforcing correct data entry habits during the learning process itself.
Administrators utilize granularity in tracking to identify specific skill gaps across departments. This data-driven approach within the EHR training system for hospitals allows for targeted interventions and verified competency mapping before full system access.
6. Mobile-First and On-Demand Accessibility
Clinical work is inherently mobile and rarely tethered to a desk. These mobile-first platforms ensure that every guide and video is fully responsive, allowing for just-in-time learning directly at the point of care.
Support remains available 24/7 to accommodate diverse shift rotations. By providing on-demand resources, the EHR training system empowers clinicians to find instant solutions without waiting for IT assistance or scheduled classroom sessions.
Advanced Capabilities That Improve Adoption Rates
The EHR training system for hospitals requires adaptive technological layers to achieve true clinical mastery. These advanced capabilities transform static platforms into active support tools, leveraging automation to eliminate redundant instruction and shorten proficiency timelines.
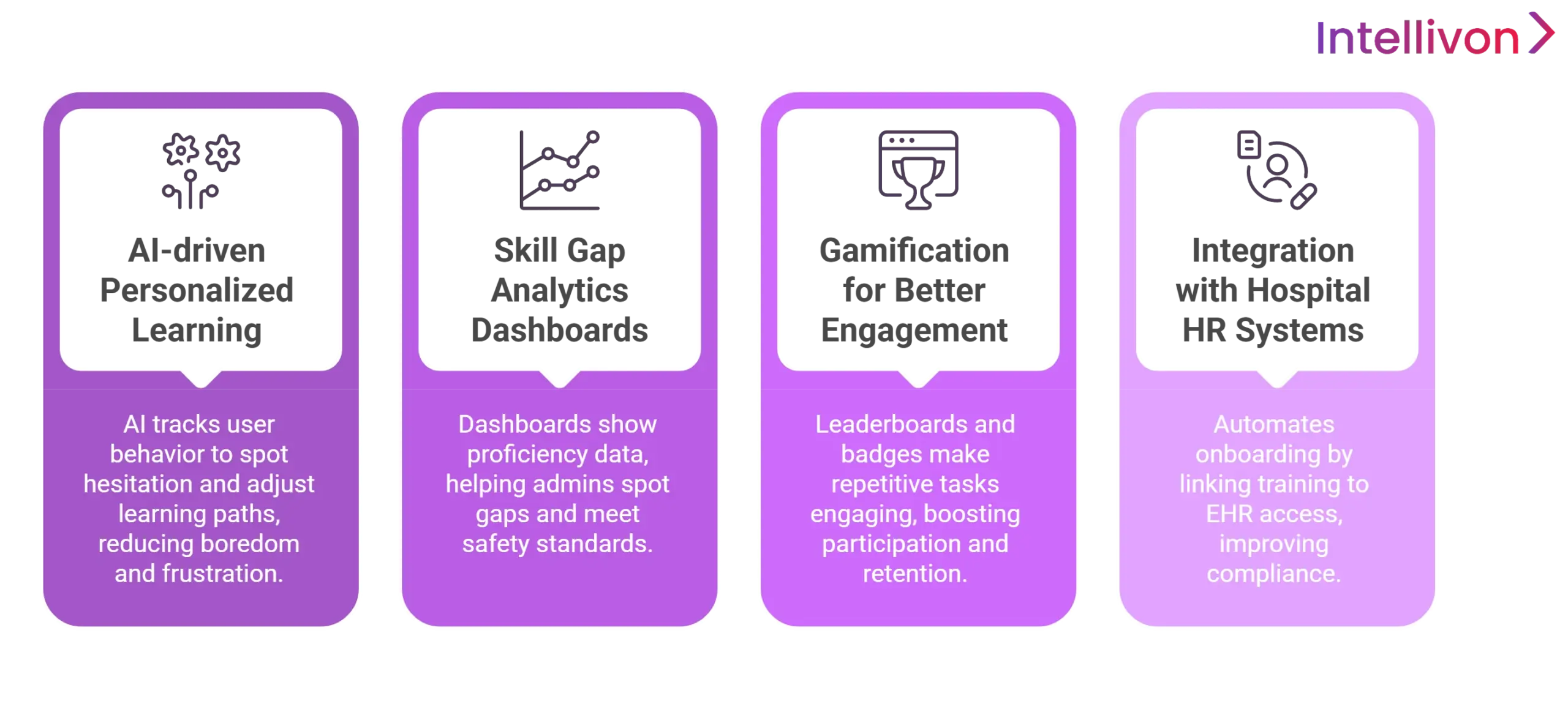
1. AI-driven Personalized Learning Paths
AI-driven engines analyze user interactions to identify hesitation patterns. By automatically recalibrating learning paths, the platform prioritizes challenging modules while bypassing mastered sections, eliminating the boredom-frustration cycle to ensure efficient training hours and specialist buy-in.
2. Skill Gap Analytics and Reporting Dashboards
Reporting dashboards visualize real-time proficiency data, allowing administrators to identify specific departmental weaknesses. These granular analytics enable data-driven interventions, ensuring every clinician meets safety benchmarks while providing leadership with verified competency mapping across the entire hospital network.
3. Gamification for Better Engagement
Gamification elements like leaderboards and achievement badges transform repetitive tasks into a rewarding experience. This layer increases voluntary participation and retention, ensuring the EHR training system for hospitals feels like a professional milestone rather than a standard administrative burden.
4. Integration with Hospital HR Systems
The HR system integration automates onboarding and credentialing by linking training completion directly to live EHR access. This closed-loop accountability reduces overhead and ensures only verified, trained staff can perform clinical documentation, significantly bolstering regulatory HIPAA compliance.
How EHR Training Systems Integrate With Hospital IT?
An effective EHR training system for hospitals must be deeply integrated into existing technical infrastructure, communicating fluently with both core electronic records and broader IT.
This integration ensures realistic data, seamless transitions to live environments, and secure patient information protection.
A. LMS and EHR Platform Integration Architecture
The backbone of a scalable training strategy is the technical bridge between the Learning Management System (LMS) and the EHR itself. This architecture allows for a “single pane of glass” experience where administrative data and clinical skill acquisition are synchronized in real time.
- Single Sign-On (SSO) Implementation: Streamlines access by allowing clinicians to use their standard hospital credentials to enter the training portal, reducing login fatigue.
- Automated Provisioning: When a user completes a required module in the LMS, the system automatically triggers the creation or update of their user profile in the EHR production environment.
- Bi-Directional Data Flow: Progress from the EHR sandbox such as accuracy in order entry is fed back into the LMS to update the user’s competency transcript.
- API-First Design: Utilizing robust APIs ensures that as the hospital upgrades its primary software, the training layer remains compatible and functional without manual re-coding.
B. Using HL7 and FHIR in Training Environments
Modern medicine relies on interoperability to provide high-fidelity instruction, an EHR training system for hospitals must simulate data exchange across clinical systems using standard HL7 and FHIR protocols, ensuring realistic data flow.
| Protocol Feature | Application in Training |
| HL7 Messaging | Simulates the arrival of lab results or imaging reports into the patient’s chart, teaching users how to interpret external data. |
| FHIR Resources | Enables training on modern app-based integrations, such as mobile vitals tracking or patient-facing portals. |
| Inter-Departmental Sync | Teaches how an order placed in the ER triggers a notification in the Pharmacy or Radiology department. |
| Data Normalization | Ensures that users understand how inconsistent data from outside sources is standardized within the hospital’s primary system. |
C. Syncing Real Workflows into Training Modules
Technical proficiency is useless if it doesn’t align with the actual physical movement of patients and staff through the facility. The integration process involves “mapping” live hospital workflows directly into the digital training modules to ensure the software supports, rather than hinders, clinical care.
- Workflow Mirroring: Capturing the exact steps of a high-volume process, such as a surgical intake or a pediatric immunization, and recreating those steps within the training simulation.
- Custom Template Syncing: Automatically importing the specific documentation templates and “smart phrases” used by the hospital’s departments into the sandbox environment.
- Alert Logic Calibration: Training users on the specific clinical decision support alerts and the local protocols for responding to them that they will encounter in the live system.
- Hardware Integration: Ensuring the training system accounts for the use of physical peripherals, such as barcode scanners for medication or bedside biometric monitors.
D. Data Security and HIPAA Compliance Layers
Security is the most critical integration point for any EHR training system for hospitals. Even in a simulated environment, the platform must uphold the rigorous standards of HIPAA to prevent the accidental exposure of Protected Health Information (PHI) and to train staff on the importance of data privacy.
- Robust Data De-identification: Sophisticated algorithms are used to “scrub” real patient data before it enters the training sandbox, replacing sensitive identifiers with synthetic but clinically realistic alternatives.
- Access Control Auditing: The system tracks every interaction within the training environment, mirroring the audit logs found in live EHRs to teach clinicians about digital accountability.
- Secure Cloud Hosting: For platforms hosted off-site, end-to-end encryption ensures that training data is protected from external breaches during transit and at rest.
- Compliance Certification: The system includes built-in assessments that specifically test a user’s knowledge of privacy protocols, such as locking workstations and verifying patient identity before data entry.
Step-by-Step Process to Build the System
The EHR training system for hospitals requires a phased engineering approach aligning technical architecture with clinical reality. This strategic process ensures the platform functions as a vital extension of the hospital’s mission.
Each stage must be validated against the dual metrics of technical accuracy and user adoption to ensure long-term viability.
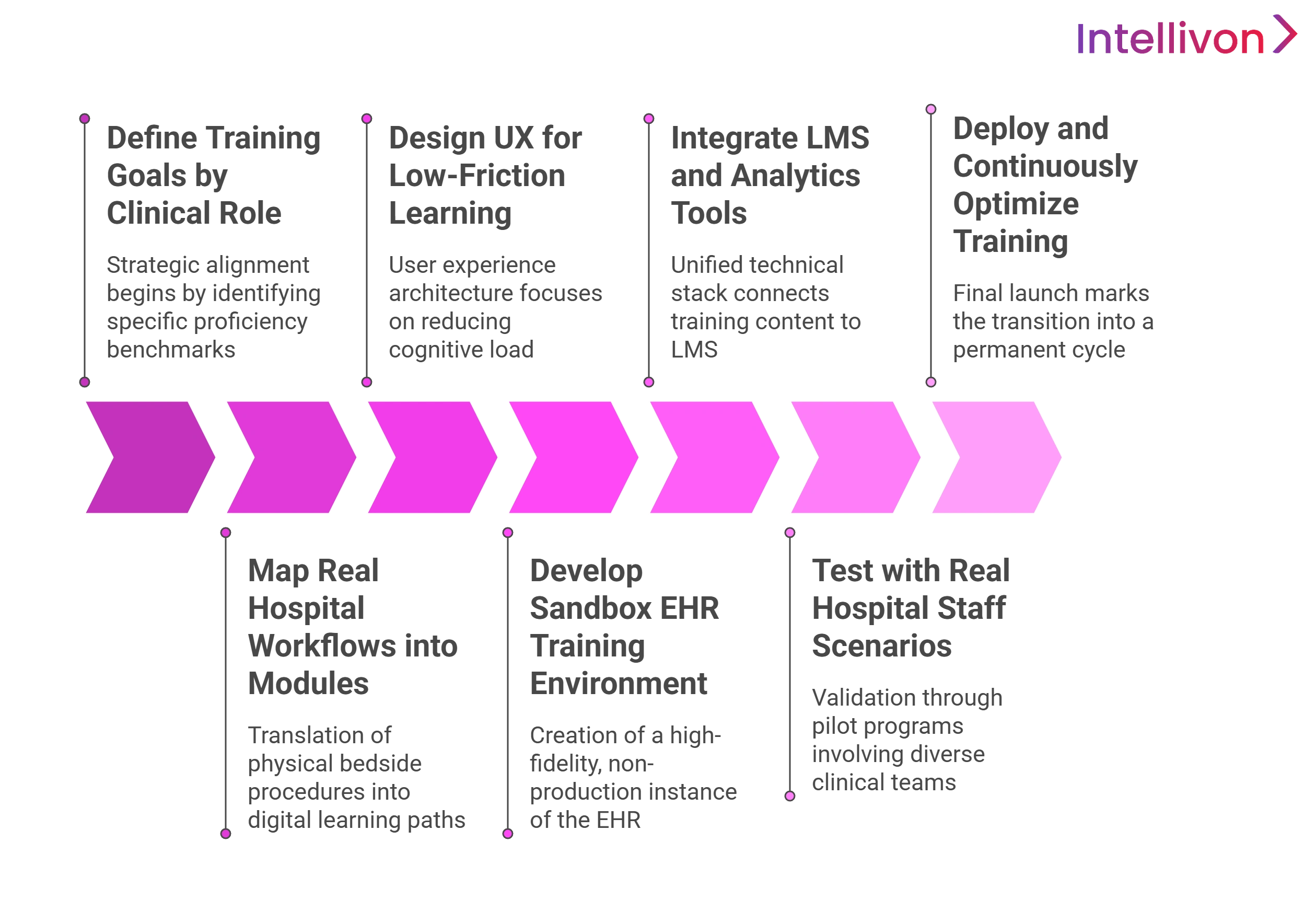
1. Define Training Goals by Clinical Role
Strategic alignment begins by identifying specific proficiency benchmarks for every department. This foundational phase ensures that the curriculum targets high-impact clinical outcomes rather than generic software features, allowing for measurable improvements in documentation speed and data accuracy across various medical specialties.
2. Map Real Hospital Workflows into Modules
The translation of physical bedside procedures into digital learning paths is essential for maintaining clinical relevance. This step involves a deep dive into departmental protocols to ensure that every simulated task reflects the actual sequences performed by staff during live patient care.
3. Design UX for Low-Friction Learning
User experience architecture focuses on reducing the cognitive load for already overstressed healthcare providers. A clean, intuitive interface ensures that clinicians spend their limited time mastering the EHR functionality itself rather than struggling to navigate the training platform’s own menus and internal structure.
4. Develop Sandbox EHR Training Environment
The creation of a high-fidelity, non-production instance of the EHR provides a risk-free space for technical experimentation. This environment uses de-identified data and mirrors the live system’s interoperability layers, allowing users to build muscle memory without compromising real-world patient safety.
5. Integrate LMS and Analytics Tools
A unified technical stack connects the training content to a central Learning Management System for automated oversight. This integration enables real-time tracking of user progress, competency verification, and the generation of detailed skill gap reports that inform administrative decision-making and resource allocation.
6. Test with Real Hospital Staff Scenarios
Validation through pilot programs involving diverse clinical teams identifies potential friction points before a full-scale rollout. These stress tests ensure the system handles complex, multi-role simulations and accurately reflects the high-pressure environment of an active hospital wing during peak operational hours.
7. Deploy and Continuously Optimize Training
The final launch marks the transition into a permanent cycle of performance monitoring and content refinement. Systematic updates ensure the platform remains aligned with new EHR patches, shifting regulatory requirements, and evolving clinical best practices, maintaining a state of constant readiness.
Cost to Develop EHR Training System for Hospitals
The cost to develop an EHR training system for hospitals depends on technical complexity and institutional scale. This financial roadmap categorizes investment levels across different development phases and deliverables.
| Development Phase | MVP Level | Enterprise Level | Key Deliverables |
| Discovery & Architecture | $15,000 – $25,000 | $40,000 – $70,000 | System SRS, Role-based Workflow Maps, FHIR Strategy |
| Sandbox Development | $30,000 – $50,000 | $100,000 – $250,000+ | Non-production EHR instance, De-identified Data Sets |
| Content & Simulations | $20,000 – $40,000 | $80,000 – $150,000 | Interactive SCORM modules, Scenario Simulations |
| LMS & IT Integration | $10,000 – $20,000 | $35,000 – $80,000 | SSO, HRIS Sync, API-based Performance Tracking |
| UI/UX & Mobile Layer | $12,000 – $18,000 | $30,000 – $60,000 | Role-based Dashboards, iOS/Android Accessibility |
| QA & Clinical Testing | $8,000 – $15,000 | $25,000 – $50,000 | HIPAA Compliance Audit, UAT with Medical Staff |
| Total Estimated Cost | $95,000 – $168,000 | $310,000 – $550,000+ | A Fully Validated Training Infrastructure |
Cost-Affecting Factors During Development
The total capital expenditure for a high-performance EHR training system for hospitals is influenced by the depth of technical integration and the volume of specialized clinical content required.
These variables dictate the engineering hours and the level of medical subject matter expertise needed to ensure the platform meets regulatory and operational standards.
- Integration and API Complexity: Real-time bi-directional sync between an LMS and systems like Epic or Oracle Cerner increases development hours by 30% to 50% due to rigorous security handshakes and data mapping.
- Simulated Data Depth: Creating 500+ de-identified patient profiles using HL7 standards adds $20,000 to $40,000 in data engineering costs, providing significantly more backend logic than basic static systems.
- Clinical Role Breadth: Supporting 15+ medical specialties requires vast libraries of unique order sets; every five additional roles increase content creation costs by 15% to 20%.
- Regulatory Auditing Layers: Implementing HIPAA-compliant click-tracking for legal audit trails adds 10% to 15% to the budget but is essential for reducing hospital liability.
- Multi-Facility Scalability: Developing a multi-tenant architecture for 10+ locations requires robust cloud infrastructure, increasing initial DevOps and hosting setup by $15,000 to $30,000.
How Intellivon Builds EHR Training Platforms?
Intellivon engineers a high-performance EHR training system for hospitals by merging clinical insight with advanced software architecture. This approach ensures technical reliability while prioritizing user adoption through intuitive, role-specific digital learning environments.
1. Domain-First Approach to Healthcare Workflows
Strategic development begins with mapping clinical reality into digital logic. This methodology ensures the training system mirrors the high-pressure environment of active wards, prioritizing efficient patient documentation and accurate order entry for every medical specialty.
2. Custom-Built Simulation Environments
High-fidelity sandbox instances provide a risk-free space for clinicians to master complex EHR tasks. These environments utilize de-identified data and replicate real-world system responses, allowing staff to build muscle memory without impacting live patient records.
3. Scalable Architecture for Hospital Networks
Multi-tenant cloud infrastructure enables seamless deployment across expansive healthcare systems. This scalable design supports thousands of concurrent users while maintaining centralized oversight, ensuring consistent training standards and data integrity across every facility within the network.
4. Compliance-First development strategy
Engineering protocols prioritize HIPAA standards and interoperability requirements from the initial code. By integrating robust audit trails and secure data exchange layers, the platform guarantees that all training activities remain fully aligned with federal regulations.
Real Use Case: EHR Training System Implementation
A mid-size regional hospital with 250 beds struggled with a fragmented digital rollout, leading to a 40% increase in documentation time and significant clinician pushback against their newly implemented EHR platform.
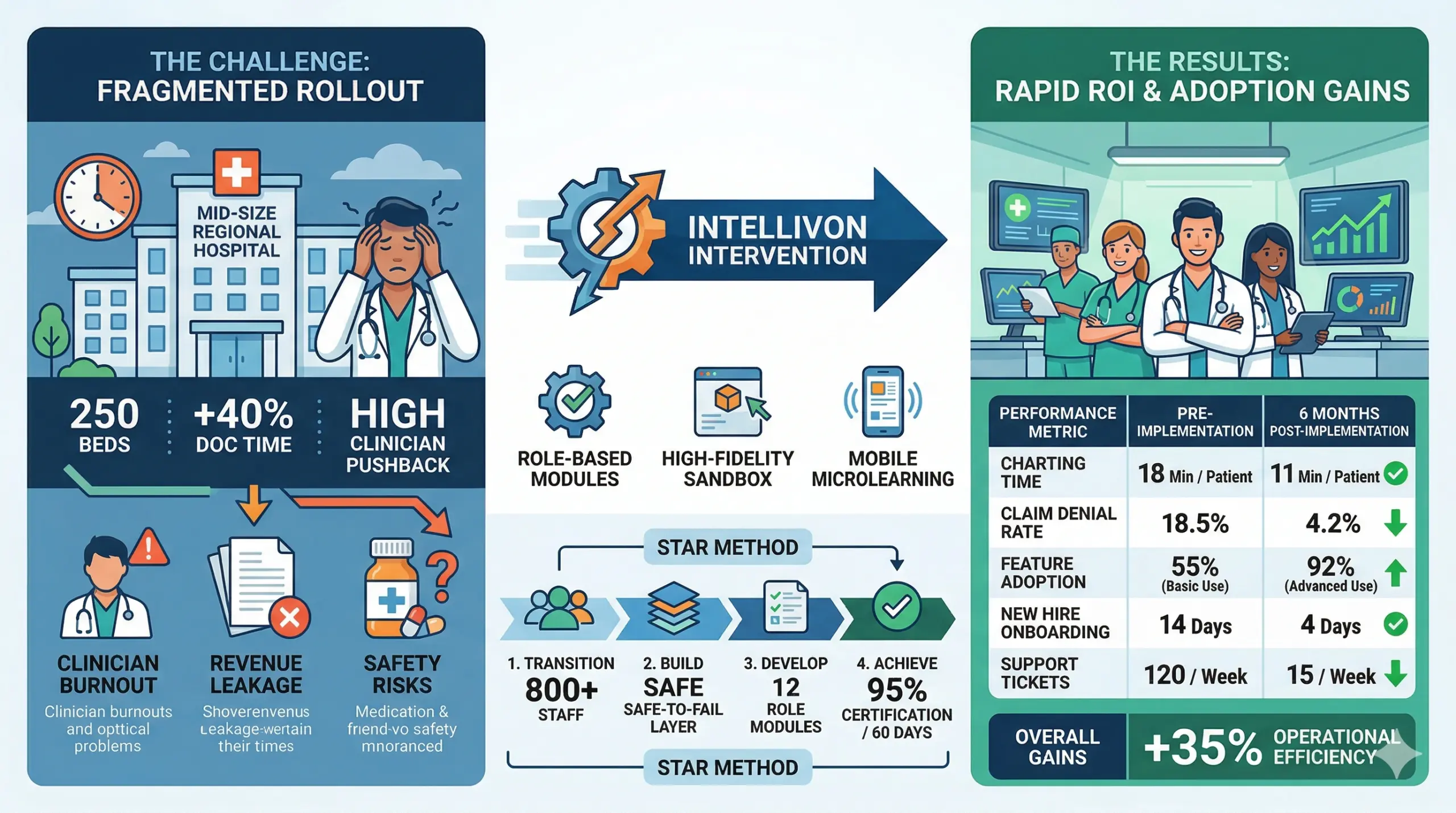
A. Problem Faced by a Mid-Size Hospital
The facility experienced a severe decline in operational throughput following an EHR upgrade, as staff relied on manual workarounds due to a lack of role-specific training and system confidence.
- Clinician Burnout: Physicians averaged 2.5 hours of overtime daily solely for chart completion, leading to high turnover among senior specialists.
- Revenue Leakage: Inaccurate ICD-10 coding resulted in a 15% spike in insurance claim denials within the first quarter of the system’s launch.
- Patient Safety Risks: Inconsistent use of the medication reconciliation module created gaps in the longitudinal patient record, increasing the potential for adverse drug events.
B. Solution Architecture and Training Modules
Intellivon deployed a custom-engineered EHR training system for hospitals, featuring a high-fidelity sandbox environment and AI-driven learning paths tailored to the specific clinical workflows of each department.
- Situation: The hospital needed to transition 800+ staff members from basic awareness to technical mastery without disrupting active patient care during a high-census period.
- Task: Our goal was to build a scalable, “safe-to-fail” training layer that mirrored their specific Epic configuration and integrated directly with their existing HRIS for automated credentialing.
- Action: We developed 12 role-based modules, implemented a FHIR-integrated sandbox with 1,000 de-identified patient profiles, and deployed a mobile-first microlearning layer for “just-in-time” support on the floor.
- Result: The platform achieved 95% staff certification within 60 days, providing a standardized, repeatable onboarding process that eliminated the need for expensive, off-site classroom sessions.
C. Results in Adoption and Efficiency Gains
Post-implementation analytics revealed a dramatic shift in both technical proficiency and organizational sentiment, confirming that the tailored EHR training system for hospitals delivered a rapid return on investment.
| Performance Metric | Pre-Implementation | 6 Months Post-Implementation |
| Average Charting Time | 18 Minutes / Patient | 11 Minutes / Patient |
| Claim Denial Rate | 18.5% | 4.2% |
| EHR Feature Adoption | 55% (Basic Use) | 92% (Advanced Use) |
| New Hire Onboarding | 14 Days | 4 Days |
| Help Desk Tickets | 120 / Week | 15 / Week |
Timeline to Build an EHR Training Platform
Establishing a robust EHR training system for hospitals follows a structured development lifecycle designed to balance speed with clinical safety. The schedule is dictated by the complexity of the integrated data layers and the depth of role-specific content required to meet the operational demands of a modern healthcare facility.
A. MVP Development Timeline
Building a Minimum Viable Product typically requires 12 to 18 weeks of concentrated engineering. This phase focuses on the core architecture, including the initial sandbox environment and primary clinical workflows.
- Discovery & Logic Mapping: Finalizing the functional requirements and user roles within the first 4 weeks.
- Sandbox Environment Setup: Developing a non-production EHR instance with de-identified patient data for safe practice.
- Core Module Creation: Building the essential training paths for high-volume roles like nursing and general practitioners.
- Basic LMS Integration: Connecting the content to a central tracking system for initial competency verification.
B. Full-Scale Deployment Timeline
Expanding the platform to support 20+ clinical specialties and full enterprise integration usually extends the timeline by another 16 to 24 weeks. This period involves deep-tier API connections and simulations.
- Advanced Role-Based Paths: Developing specialized content for niche departments such as Oncology, Cardiology, and Labor & Delivery.
- Interoperability Stress Testing: Ensuring HL7 and FHIR data exchanges function correctly across simulated lab and pharmacy interfaces.
- Enterprise SSO Integration: Rolling out Single Sign-On capabilities to streamline access for the entire hospital workforce.
- Comprehensive UAT: Conducting User Acceptance Testing with diverse clinical teams to refine the interface and workflow logic.
C. Optimization and Scaling Phase
The transition from a single facility to a multi-hospital network typically occurs over 8 to 12 weeks. This phase centers on cloud infrastructure scaling and performance tuning based on analytics.
- Multi-Tenant Architecture Setup: Configuring the system to support multiple hospital locations with centralized administrative oversight.
- Skill-Gap Analytics Refinement: Using initial performance data to automate the delivery of targeted refresher modules to struggling departments.
- Continuous Content Updates: Implementing a “Delta Training” pipeline to push out updates for new EHR patches or regulatory changes.
- Performance Benchmarking: Comparing post-training EHR adoption rates against baseline metrics to quantify institutional ROI.
Key Timeline Summary
| Project Milestone | Typical Duration | Key Delivery Outcome |
| Discovery & Workflow Mapping | 3 – 5 Weeks | Validated functional requirements and role definitions. |
| Core Architecture & Sandbox | 8 – 12 Weeks | Functional non-production EHR instance with de-identified data. |
| Content & Simulation Design | 6 – 10 Weeks | High-fidelity, interactive clinical learning modules. |
| Integration & Security Testing | 4 – 6 Weeks | Verified SSO, HIPAA compliance, and API stability. |
| Pilot Testing & UAT | 3 – 5 Weeks | Feedback-driven refinements from actual clinical staff. |
| Enterprise-Wide Launch | 2 – 4 Weeks | Fully operational training access across all departments. |
Build vs Buy: What Hospitals Should Choose
Deciding between a custom-engineered or pre-packaged EHR training system for hospitals is a high-stakes pivot. While off-the-shelf options are faster, they often lack the flexibility to mirror specific, proprietary medical workflows.
A strategic evaluation must balance the immediate need for a platform against the long-term requirement for a system that evolves alongside the hospital’s unique clinical architecture.
A. When to Build a Custom Solution
A custom-built infrastructure is the superior choice for healthcare networks with specialized service lines or proprietary clinical protocols. Building from the ground up allows for the precise integration of local medical standards that a generic product simply cannot accommodate.
- Proprietary Workflow Integration: Custom systems allow for the exact mirroring of internal hospital processes, ensuring training matches the live environment 1:1.
- Deep EHR Customization: Hospitals using heavily modified versions of Epic or Cerner require a training layer that reflects those specific modifications and custom templates.
- Unrestricted Scalability: Building ensures the hospital owns the intellectual property, eliminating per-user licensing fees as the organization expands its workforce.
- Unique Interoperability Needs: Custom builds can be engineered to communicate with niche third-party diagnostic tools via specialized HL7/FHIR hooks that standard tools may not support.
B. When off-the-shelf tools fall short
Generic training platforms often struggle with the “last mile” of clinical relevance. While they provide basic software orientation, they frequently fail to provide the deep, role-specific simulation required to reduce documentation errors in a high-pressure environment.
| Feature Gap | Impact on Hospital Operations |
| Static Content | Off-the-shelf videos become obsolete the moment a hospital updates its internal EHR templates. |
| Generic Simulations | Standard tools lack the “sandbox” fidelity needed to practice high-risk orders safely. |
| Rigid Reporting | Basic LMS tools often fail to provide the granular skill-gap analytics required for clinical auditing. |
| Poor Mobile UX | Many legacy products are not optimized for the tablet-based, “on-the-go” reality of modern nursing. |
C. Long-term ROI comparison
The long-term ROI of a custom EHR training system for hospitals is realized through reduced physician burnout and billing inaccuracies. High initial costs are offset by eliminated licensing fees and operational efficiency, resulting in a lower Total Cost of Ownership.
- Reduction in “Pajama Time”: Better-trained clinicians finish charts faster, directly lowering turnover costs and recruitment expenses.
- Decreased Claim Denials: Precise training on coding and documentation leads to a measurable uptick in successful insurance reimbursements.
- Elimination of Seat Licenses: A one-time investment in a custom platform removes the recurring financial burden of scaling a workforce across multiple facilities.
- Risk Mitigation: A high-fidelity training system acts as a financial safeguard against the catastrophic costs of medical errors and HIPAA non-compliance fines.
Key Metrics to Measure EHR Training Effectiveness
The effectiveness of a modern EHR training system for hospitals is validated through rigorous data analysis. By tracking key performance indicators, leadership can quantify operational impact and obtain the empirical evidence needed to refine clinical workflows.
These metrics provide the empirical evidence needed to refine training modules and ensure that the digital infrastructure is actively supporting the hospital’s clinical mission.
1. EHR adoption rate improvement
Success is measured by the transition from forced compliance to organic system utilization across all departments. Monitoring how frequently staff utilize advanced features versus manual workarounds indicates the true level of digital integration.
- Feature Penetration: Tracking the percentage of clinicians using advanced clinical decision support tools and automated order sets.
- Reduction in Shadow Systems: Measuring the decline in paper-based notes and unofficial spreadsheets used to bypass the EHR interface.
- System Log Activity: Analyzing the duration and frequency of active sessions to identify high-engagement departments versus those requiring additional support.
2. Reduction in documentation errors
Data integrity is the cornerstone of both patient safety and revenue cycle management. A high-fidelity training environment directly correlates with a decrease in the technical friction that leads to charting mistakes.
- Coding Accuracy: Monitoring the alignment between clinical documentation and ICD-10/CPT coding to reduce insurance claim denials.
- Alert Response Efficiency: Measuring the ratio of acted-upon clinical alerts versus ignored or overridden warnings to combat alert fatigue.
- Data Completion Rates: Tracking the frequency of “hard-stop” bypasses where mandatory patient data fields are left blank or filled with placeholder text.
3. Time-to-proficiency for staff
The speed at which a new hire or a legacy staff member reaches full operational capacity is a critical metric for hospital productivity. Efficient training systems significantly compress the onboarding timeline.
- Onboarding Acceleration: Calculating the number of days from initial system access to the point where a clinician can manage a full patient load independently.
- Help Desk Ticket Volume: Tracking the decrease in “how-to” technical support requests following the implementation of new training modules.
- Assessment Scores: Using sandbox performance data to verify that users meet minimum competency benchmarks before entering the live production environment.
4. Impact on patient care efficiency
The ultimate goal of an EHR training system for hospitals is to return time to the clinician for direct patient interaction. Training effectiveness is visible in the streamlining of digital tasks.
- Average Charting Time: Measuring the reduction in minutes spent on documentation per patient encounter, particularly during high-volume shifts.
- Patient Throughput: Analyzing whether improved EHR proficiency leads to faster discharge processing and reduced wait times in emergency departments.
- Clinician Satisfaction Levels: Using internal surveys to correlate training quality with a reduction in “pajama time” and overall digital burnout.
Future Trends in EHR Training Systems
The evolution of the EHR training system for hospitals is moving toward an immersive, anticipatory architecture. Teaching methods are shifting from reactive processes to proactive, technology-enhanced environments that adapt to a clinician’s immediate needs and cognitive state.
1. AI-based adaptive learning systems
These platforms leverage machine learning to analyze “clickstream” data, identifying exactly where a clinician hesitates during a CPOE (Computerized Physician Order Entry) sequence. The system then recalibrates the curriculum to address that specific friction point.
Real-World Example: Obrio or uPerform integrating with Epic Hyperdrive. If a resident consistently triggers “Best Practice Advisories” (BPAs) but fails to document the required justification, the AI pushes a 60-second “Micro-Sim” to their mobile device that specifically recreates that high-friction documentation bridge.
2. VR-based clinical simulations
Virtual Reality transitions the training from a 2D screen to a spatial experience, allowing staff to practice the physical coordination of using an EHR while managing a patient in a high-acuity setting.
Real-World Example: Oxford Medical Simulation (OMS) used in conjunction with a Cerner Millennium sandbox. In this setup, a nurse wears a VR headset to manage a simulated patient in septic shock; they must physically turn to a virtual workstation, navigate the EHR to find the “Lactic Acid” lab results, and initiate the “Sepsis Bundle” order set while the virtual patient’s vitals fluctuate in real time.
3. Real-time training within live EHR systems
This involves “Digital Adoption Platforms” (DAPs) that act as an intelligent GPS layer sitting on top of the production EHR. They provide step-by-step guidance only when a user initiates a rare or highly complex task.
Real-World Example: WalkMe or AppLearn deployed over Oracle Health (Cremer) provides interactive “Walk-Thru” bubbles for rare tasks like “Organ Donation Notification.” This highlights non-intuitive UNOS (United Network for Organ Sharing) fields on-screen, ensuring immediate regulatory compliance.
Ready to Build Your EHR Training System?
The transition from a legacy system to a high-performance EHR training system for hospitals is a critical leap toward operational excellence and clinical safety. At Intellivon, we specialize in bridging the gap between complex healthcare IT and the professionals who use it every day.
Our team develops custom, role-specific training infrastructures that integrate seamlessly with your existing EHR and HR ecosystems, ensuring that your digital transformation leads to measurable ROI rather than clinician burnout.
Whether you are scaling a multi-specialty network or migrating to a new EHR platform, we provide the technical expertise and clinical insight needed to build a “safe-to-fail” environment that drives 100% adoption.
We don’t just build software; we engineer the human-centric layer that makes your multi-million dollar technology investment actually work for your staff and your patients.
Take the first step toward a more efficient, compliant, and digitally fluent hospital.
- Consult with Our Healthcare IT Experts: Discuss your specific workflow challenges and integration needs.
- Get a Custom Development Roadmap: Receive a detailed timeline and cost breakdown tailored to your facility’s scale.
- See Our Simulation Tech in Action: Explore how our sandbox environments and AI-driven paths can transform your onboarding process.
Contact with our experienced developers of Intellivon today to start building your Custom EHR Training Platform
Conclusion
Building an EHR training system for hospitals is a transformative investment that bridges the gap between complex technology and clinical excellence. By moving beyond static instruction and adopting adaptive, integrated, and data-driven platforms, healthcare institutions can significantly reduce burnout and improve patient safety. This engineering approach ensures that your digital infrastructure becomes a supportive partner in care delivery rather than a hurdle. Ultimately, a well-executed training strategy secures higher adoption rates, protects your financial health, and empowers your workforce to focus on what matters most: superior patient outcomes.
FAQs
Q.1. What features define a top EHR training system for hospitals?
A.1. High-impact platforms must include role-based learning paths, sandbox environments for safe practice, and real-time analytics. These features ensure staff gain proficiency without risking actual patient data or clinical safety.
Q.2. Is a custom EHR training system for hospitals HIPAA compliant?
A.2. Yes, custom builds prioritize security by design. These systems use HL7 and FHIR protocols to simulate data exchange while ensuring all training activities meet strict HIPAA auditing and encryption standards.
Q.3. What are the primary benefits of an EHR training system?
A.3. A dedicated EHR training system for hospitals significantly improves patient safety by reducing documentation errors. It also minimizes clinician burnout by streamlining complex workflows and ensuring staff feel confident using digital tools.
Q.4. Why is a sandbox environment necessary for EHR training?
A.4. A sandbox environment allows clinicians to practice high-stakes tasks without affecting live patient records. This safe space is essential for building muscle memory and testing workflows before interacting with real clinical data.