Key Takeaways:
-
AI billing platforms predict denial risks before submission, protecting revenue before it is lost.
-
86% of claim denials are preventable with smarter eligibility and coding workflows.
-
Core features include NLP coding, denial analytics, real-time eligibility, and executive KPI dashboards.
-
Platform development costs between $50,000 and $200,000, depending on scope and integration depth.
-
Intellivon builds phased AI billing platforms prioritizing high-impact workflows before expanding platform features.
Healthcare billing problems extend beyond the billing department. Each denied claim, missed eligibility check, coding mistake, and underpayment impacts cash flow, operational growth, and revenue forecasting throughout the organization.
Traditional billing processes were not designed to handle this complexity. Unconnected EHRs, manual coding checks, payer portals, and reactive denial management lead to errors that add up with each billing cycle. As a result, revenue teams spend more time fixing issues than preventing them.
AI healthcare billing platforms change this situation by making billing systems proactive. They predict claim risks, highlight coding problems, confirm eligibility, identify missing documentation, and enhance payment visibility before any revenue is lost. However, creating this platform takes more than just putting together AI features. HIPAA-compliant architecture, EHR integrations, payer-aware logic, audit trails, and revenue dashboards must all function together as one system.
At Intellivon, we assist healthcare companies, RCM providers, and SaaS founders in building AI-powered billing platforms based on real billing operations, rather than generic automation templates. This blog discusses architecture, features, AI use cases, compliance, costs, and development scope.
Why Healthcare Billing Teams Need AI-Driven Platforms Today
Healthcare billing inefficiencies have moved from an operational inconvenience to a measurable financial crisis that manual workflows can no longer absorb.
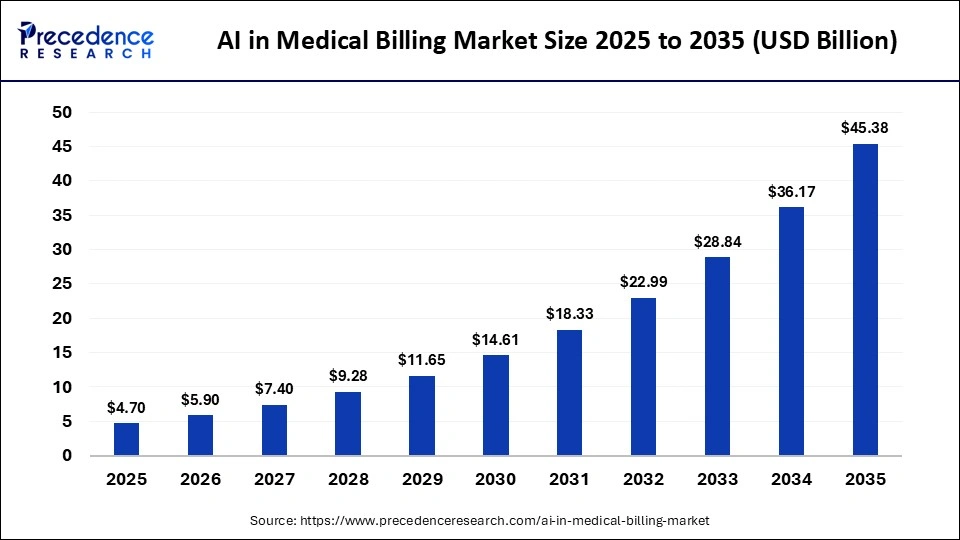
1. Claim Denials Are Creating Unsustainable Revenue Loss
In 2024, 11.81% of all claims were denied, up 2.4% year over year, with outpatient denials costing USD 5,390 per case. Furthermore, 86% of those denials are preventable. A USD 3 million practice still loses between 4 and 5% of annual revenue, approximately USD 150,000, to billing leakage.
Around 80% of medical bills contain errors, and 32% of denials trace directly back to coding mistakes.
2. The Workforce Crisis Is Accelerating The Problem
A 12% shortage of certified coders exists today, projected to reach 30% nationally. Coder demand is simultaneously rising 13% by 2026, and 43% of providers are already understaffed.
In addition, rural teams frequently operate with just one or two billing staff, making recruitment an unrealistic solution at scale.
3. AI Delivers Proven And Immediate Returns
Organizations adopting AI billing platforms report 32% higher coding efficiency, 25% faster billing processes, and 40% fewer denials.
For a USD 3 million practice, AI recovers approximately USD 60,000 annually through denial reduction alone, with payback typically achieved within 6 to 12 months.
The numbers make the case clearly. For healthcare businesses building or modernizing billing infrastructure, AI is no longer a competitive advantage. It is the baseline requirement for financial stability at scale.
What An AI Healthcare Billing Platform Actually Does
An AI billing platform acts as an intelligent operating layer that sits directly on top of legacy medical software. Instead of relying on manual data entry and human audits, this technology uses machine learning to process financial workflows in real time.
It continuously reviews documentation, matches clinical notes with shifting payer rules, and executes administrative tasks without human fatigue. The platform transforms the back office from a reactive cost center into an automated revenue engine.
1. Automates Eligibility, Claims, Coding, And Payments
The primary function of the software is to remove friction from the four core pillars of medical revenue management. It shifts these processes from slow, error-prone manual reviews to instantaneous automated cycles.
- Real-Time Eligibility Verification: The system checks insurance coverage automatically before a patient even walks through the clinic door. It verifies active benefits, co-pays, and prior authorization requirements instantly to prevent future payment delays.
- Autonomous Medical Coding: NLP models scan doctor notes and translate clinical narratives into accurate medical codes. This process eliminates human typing errors and matches the precise rules required by insurance companies.
- Clean Claim Generation: The platform compiles all required patient documentation into a digital file that meets specific insurance formats. It submits these files electronically within seconds of a patient visit.
- Frictionless Payment Processing: The software routes patient balances to digital wallets and automated payment plans. It tracks every transaction automatically and matches incoming payments to open invoices without manual tracking.
2. Uses AI To Predict Denials Before Claim Submission
Traditional billing systems only reveal a problem after an insurance company rejects a claim. This platform flips that reactive model by using predictive analytics to identify errors while the claim is still a draft.
- Payer Rule Matching: The software analyzes historical data to learn the specific, shifting criteria that individual insurance companies use to reject payments. It flags mismatched codes or missing documentation before submission.
- Risk Scoring Models: Every outgoing claim receives a dynamic probability score regarding its likelihood of approval. High-risk claims go directly to an administrative dashboard for quick human review.
- Automated Correction Suggestions: When the system identifies a potential denial, it does not just flag the error. It actively suggests the exact modification or missing file needed to guarantee immediate approval.
3. Connects Billing Data Across Healthcare Systems
Medical data often remains trapped inside siloed software products that cannot communicate with one another. This platform acts as a universal translator to unify financial information across entire healthcare networks.
- Universal Software Integration: The system connects directly with various EHR and practice management systems. It extracts necessary data smoothly without requiring hospitals to replace their existing infrastructure.
- Centralized Financial Dashboards: Executives can view the financial health of multiple clinics or hospital departments in one single location. This clear view removes blind spots and simplifies cash flow forecasting.
- Instant Payer Communication: The software maintains a direct, continuous digital bridge with insurance databases. This connection allows for immediate status updates and eliminates the need for phone calls to check on claim progress.
Building an AI healthcare billing platform removes structural inefficiencies by replacing manual administration with proactive financial intelligence.
This integration secures predictable revenue streams and prepares enterprise operations for scalable digital growth.
Core Features Every AI Healthcare Billing Platform Needs
An enterprise-ready AI billing platform must do more than just process digital forms. To capture market share and attract institutional investment, your software needs robust, highly specialized capabilities that directly solve revenue leakage.
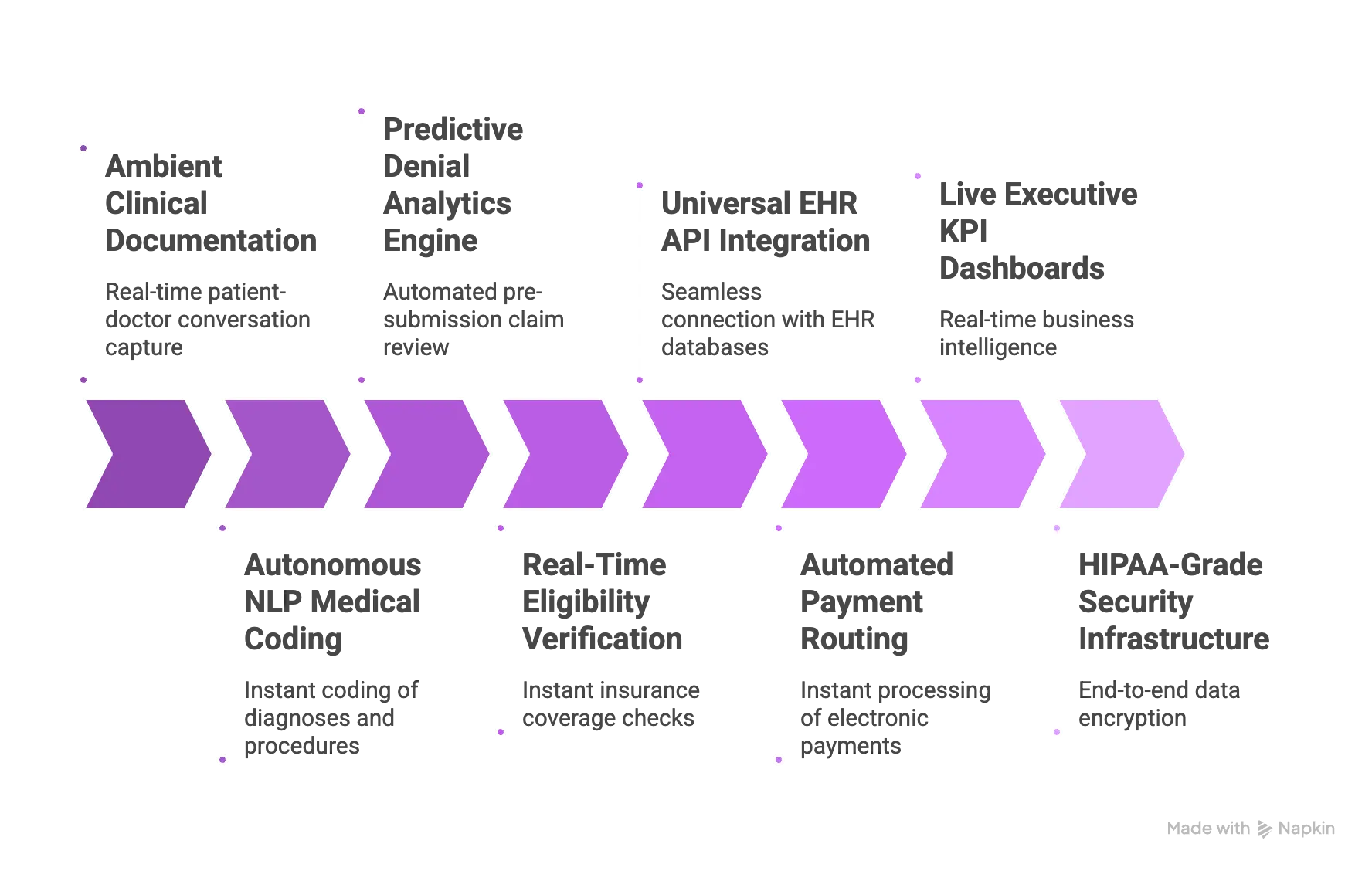
1. Ambient Clinical Documentation
The software securely listens to patient-doctor conversations in real time to capture accurate clinical data. It automatically generates structured summaries, which creates richer data for subsequent billing steps without increasing administrative workloads.
- Speech-to-Text Processing: Advanced audio algorithms filter out background noise to record medical consultations with high precision.
- Structured Summary Generation: The system synthesizes the conversation into organized clinical notes, highlighting symptoms and diagnoses.
2. Autonomous NLP Medical Coding
Advanced NLP reads complex, unstructured medical texts. The engine accurately extracts diagnoses and procedures, mapping them instantly to standardized ICD-10, CPT, and HCPCS codes with zero manual intervention.
- Contextual Semantic Mapping: The AI understands medical context, preventing misinterpretation of abbreviations or complex clinical terms.
- Instant Standardized Coding: The platform assigns the exact digital codes required by insurance databases within seconds.
3. Predictive Denial Analytics Engine
This component acts as an automated pre-submission reviewer. It uses machine learning models trained on historical payer behavior to identify documentation gaps or coding mismatches, which block errors before submission.
- Pre-Submission Inspection: The software evaluates outgoing claims against millions of active payer rules to flag errors early.
- Risk Scoring Dashboards: Every claim receives a clear probability score regarding its likelihood of approval before final submission.
4. Real-Time Eligibility Verification
The platform executes automatic coverage checks before care is delivered. It instantly pulls active insurance benefits, copays, and prior authorization requirements to completely eliminate front-end administrative friction.
- Instant Benefit Retrieval: The system communicates directly with insurance databases to confirm patient coverage details instantly.
- Prior Authorization Automation: The AI identifies required approvals ahead of time, reducing the risk of non-payment.
5. Universal EHR API Integration
A robust middleware layer connects smoothly with major EHR databases. It synchronizes scheduling, charting, and financial data without requiring a disruptive overhaul of the clinic’s existing infrastructure.
- Bidirectional Data Syncing: Information flows continuously between the billing platform and the core hospital software.
- Zero-Disruption Deployment: The system works alongside legacy software, avoiding costly and time-consuming technical overhauls.
6. Automated Payment Routing
The system processes electronic remittance advice and transfers funds automatically. It instantly matches incoming digital payments to open medical invoices and sets up automated patient payment plans effortlessly.
- Instant Invoice Reconciliation: Incoming deposits are automatically matched to outstanding claims, eliminating manual ledger updates.
- Flexible Payment Adjustments: The software creates customized installment schedules for patients based on outstanding balances.
7. Live Executive KPI Dashboards
Decision-makers gain full visibility through real-time business intelligence tools. The interface monitors critical metrics, including first-pass clean claim rates, active collection trends, and detailed denial root-cause breakdowns.
- Visual Financial Metrics: Interactive charts display collection performance, aging accounts, and revenue trends clearly.
- Root-Cause Tracking: The dashboard groups rejected claims by specific error types to highlight process inefficiencies.
8. HIPAA-Grade Security Infrastructure
The platform features end-to-end data encryption for information at rest and in transit. Multifactor authentication, HIPAA-grade security, strict access logs, and automated compliance auditing preserve data privacy and protect against expensive regulatory penalties.
- End-to-End Encryption: All sensitive patient records are fully scrambled during transmission and storage.
- Automated Audit Trails: The system logs every user action automatically to maintain total compliance transparency.
Investing in these eight core features allows software developers to deliver a reliable product that drastically lowers hospital overhead costs.
This robust technical foundation ensures high operational stability, making the application highly attractive to large enterprise buyers looking for an immediate return on investment.
Compliance Requirements For AI Healthcare Billing Platforms
Building a healthcare product requires absolute adherence to strict legal frameworks. Because medical billing platforms process both highly sensitive personal data and financial transactions, regulatory oversight is intense.
Investors must treat compliance as a foundational technical requirement rather than an afterthought to avoid catastrophic penalties.
1. HIPAA Data Privacy
The platform must implement rigorous safeguards to protect patient identity and clinical records from exposure.
Data Minimization: The AI only accesses specific data fields required to process a claim, masking unnecessary clinical histories during evaluation.
2. SOC 2 Type II Security
Fintech buyers demand independent validation that your cloud infrastructure can withstand sophisticated cyber threats over extended observation periods.
Continuous Monitoring Automated software tracks infrastructure vulnerabilities and flags unusual data access patterns instantly.
3. PCI-DSS Level 1 Payments
If your platform processes credit cards or bank transfers for patient balances, it must secure payment gateways.
Tokenized Processing: The software converts sensitive payment data into secure, single-use digital tokens rather than storing raw card numbers.
4. Explainable AI Coding
If your software uses machine learning to assign billing codes, you must prove how the algorithm reached conclusions.
Logic Documentation: The system documents the exact clinical data points the AI used to choose a specific medical code for future audits.
5. Human-In-The-Loop Audits
When a human billing specialist corrects an automated AI coding suggestion, the platform must record the change.
Override Tracking: The system saves the original AI output, the human modification, and the reason for the adjustment.
6. HITRUST CSF Certification
This framework harmonizes multiple regulations into a single healthcare-specific security standard to streamline compliance across different markets.
Unified Risk Management. Achieving this certification proves to enterprise hospital networks that your software meets the global standard for healthcare data safety.
Prioritizing regulatory compliance protects your capital investment and creates an immediate competitive advantage.
Enterprise healthcare buyers will completely bypass innovative products if they lack verified certifications, making compliance the ultimate gatekeeper for enterprise software adoption.
How To Design Secure AI Healthcare Billing Architecture
An enterprise-grade AI healthcare billing platform requires a highly resilient, multi-tiered infrastructure to process sensitive clinical data at scale.
The underlying architecture must seamlessly balance high-throughput computational processing with stringent enterprise security protocols.
Enterprise AI Medical Billing Technology Stack
| Architecture Layer | Core Technologies and Frameworks | Strategic Enterprise Function |
| Data Layer | PostgreSQL, AWS Aurora, Redis, AWS KMS | Secures and isolates protected health information |
| Integration Layer | HL7 FHIR APIs, Mirth Connect, REST | Syncs clinical documentation with external records |
| Gateway Layer | X12 EDI Engines, Change Healthcare APIs | Handles secure transactional routing to clearinghouses |
| AI Model Layer | Python, PyTorch, BERT, OpenAI API | Executes medical coding and predictive denial scoring |
| Automation Layer | Apache Airflow, Celery, Node.js | Drives automated claims routing and background tasks |
| Security Layer | OAuth 2.0, AWS CloudTrail, Okta | Enforces zero-trust access and immutable audit tracking |
1. Secure PHI Data Layer For Healthcare Workflows
The foundational data architecture must isolate protected health information (PHI) while maintaining rapid data accessibility. At the same time, financial investors must prioritize absolute cryptographic security at this layer to prevent catastrophic data liabilities.
- Hardware-Level Encryption: Database engines utilize advanced hardware-level encryption algorithms to secure medical records both at rest and during transit.
- In-Memory Caching: High-speed caching systems handle volatile transaction data to optimize platform speed during peak operating hours.
- Automated Data Partitioning: Storage layers deploy automated data partitioning strategies to isolate tenant records across large hospital networks.
2. EHR, EMR, And Practice Management Integrations
An intelligent platform cannot operate in isolation from the clinical systems that generate healthcare data. Seamless ingestion requires standardized communication protocols to pull data directly from electronic health records.
- Real-Time FHIR APIs: Fast Healthcare Interoperability Resources (FHIR) APIs establish real-time data pipelines between clinical systems and the billing software.
- Specialized Integration Engines: Advanced integration tools translate legacy healthcare data formats into clean, modern database structures automatically.
- Continuous Bidirectional Syncing: Sync modules update administrative records across all connected clinical platforms instantly to eliminate data lag.
This absolute integration removes manual human entry errors from the initial stage of the revenue cycle.
3. Clearinghouse, Payer API, And ERP Integrations
The financial core of the software must communicate efficiently with diverse insurance networks and corporate enterprise resource planning ledgers. This connectivity accelerates cash collection by utilizing direct, automated transactional channels.
- EDI Mapping Modules: Electronic data interchange mapping modules translate internal billing data into standard X12 clearinghouse formats.
- Modern Payer APIs: Application programming interfaces bypass slow legacy clearinghouses to verify immediate claim status updates.
- Financial Webhooks: Automated webhooks feed real-time collection data directly into the hospital’s enterprise resource planning (ERP) systems.
Implementing robust integration gateways guarantees maximum transactional velocity for the entire enterprise.
4. AI Model Layer For Coding And Denial Prediction
The intelligence tier forms the core competitive advantage of the modern AI medical billing platform. This layer runs highly specialized machine learning models that analyze clinical text and calculate financial risks.
- Natural Language Processing: NLP models interpret unstructured doctor notes to extract appropriate diagnostic and billing codes.
- Machine Learning Classifiers: Predictive classifiers evaluate historical data to predict exactly which insurance company will reject a claim.
- Model Management Pipelines: Pipelines handle continuous training cycles to adapt to shifting regulatory and healthcare policies.
Investing in a robust machine learning layer ensures the platform remains highly accurate in a shifting market.
5. Workflow Automation Layer For Billing Operations
The automation engine acts as the operational nervous system, managing complex background tasks without human intervention. This framework handles the automated execution of administrative tasks based on real-time triggers.
- Distributed Task Queues: Scalable queues manage thousands of background tasks simultaneously without degrading the platform’s user experience.
- Workflow Orchestration Tools: Automation software manages complex multi-step processes like automated appeal routing and bulk filing.
- Real-Time Event Notifications: Event-driven monitors trigger instant communication alerts when critical financial anomalies require senior human review.
Fintech founders can leverage this automation to operate a highly scalable billing system with low overhead.
6. Compliance, Audit Logs, And Access Controls
Enterprise healthcare applications must maintain absolute regulatory compliance to survive rigorous institutional procurement processes. The security layer enforces tight guardrails around every data interaction within the platform.
- Centralized Identity Providers: Access engines manage secure multi-factor authentication and role-based access controls for all users.
- Immutable Audit Logging: Specialized logging services record every single data modification and patient record access event permanently.
- Automated Compliance Monitoring: Cloud security tools continuously scan cloud infrastructure to detect and fix security vulnerabilities instantly.
In conclusion, robust compliance architecture transforms a standard software application into an enterprise-grade financial asset.
Step-By-Step AI Healthcare Billing Platform Development
Building a market-ready AI medical billing platform requires balancing strict regulatory constraints with cutting-edge automation engineering.
At Intellivon, we follow a rigorous, deployment-tested framework to transform complex healthcare data into highly scalable, automated fintech assets.
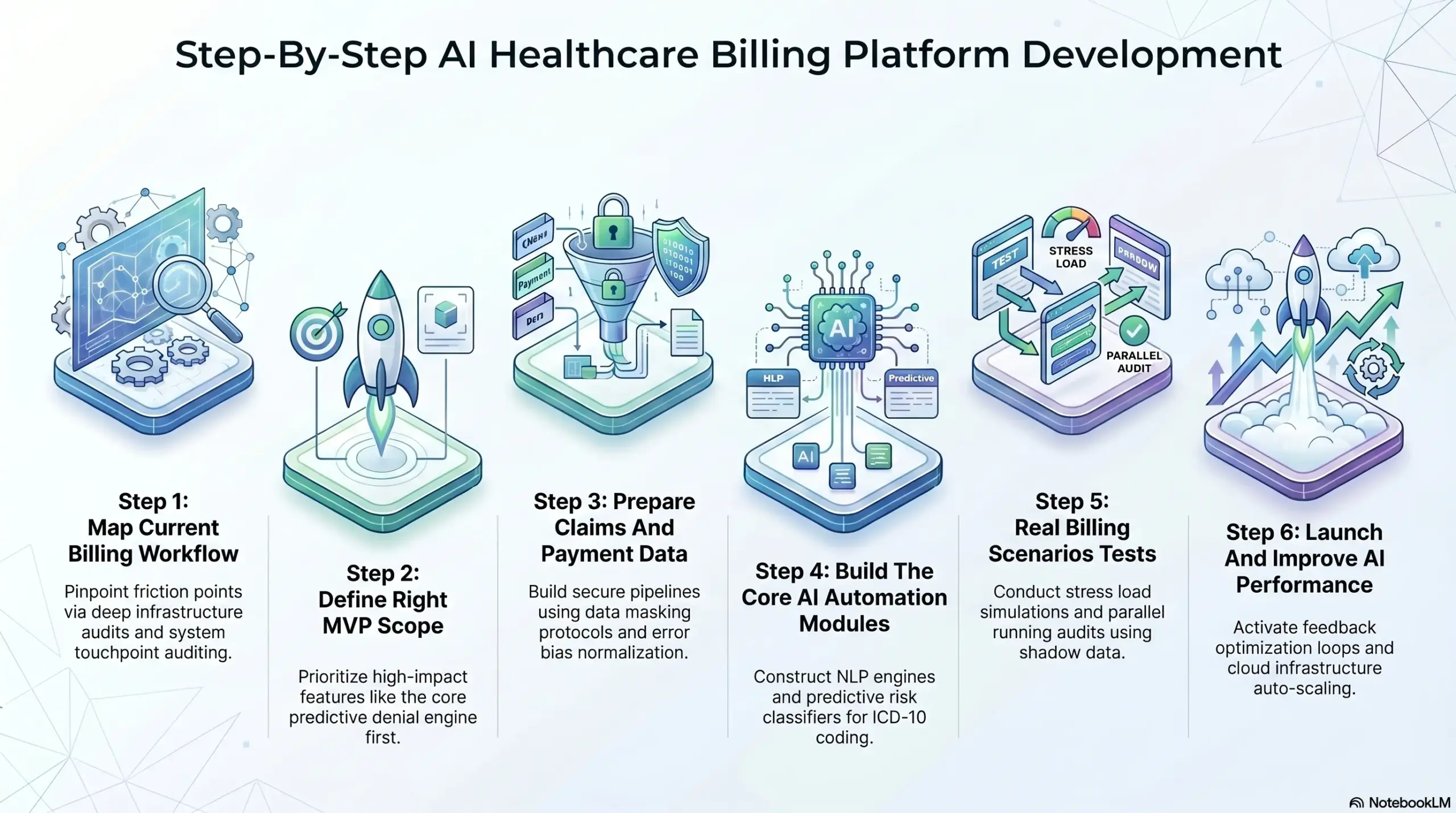
Step 1: Map Current Billing Workflow
We begin by analyzing exactly where hospitals lose money and time under their current legacy revenue cycle.
Identifying these specific friction points allows us to build target parameters for the automation engine.
| Evaluation Area | Traditional Human Process | Intellivon Automated Target |
| Data Ingestion | Manual scanning of clinic papers | Instant digital extraction |
| Verification | Disconnected phone checks | Live insurance API pings |
- Process Bottleneck Discovery: We run deep infrastructure audits to pinpoint the exact steps where manual billing errors occur most frequently.
- System Touchpoint Auditing: Our team maps out every piece of software currently touching clinical records to plan secure integration channels.
Step 2: Define Right MVP Scope
To maximize your initial investment, we narrow the platform focus down to a high-impact Minimum Viable Product. This ensures you launch a functional application quickly without drowning in unnecessary features.
| Dev Focus | Excluded from Initial MVP | Included in High-Impact MVP |
| Scope | Cross-border insurance processing | High-volume regional claims |
- High-Value Feature Selection: We prioritize building the core predictive denial engine first, as preventing rejected claims yields the fastest financial return.
- Target Market Selection: We design the first version specifically for mid-sized medical groups where administrative volume is heavy but integration hurdles are manageable.
Step 3: Prepare Claims And Payment Data
An AI model is only as smart as the information used to train it. We build secure data pipelines to clean, organize, and sanitize historical clinical records.
| Data Treatment | Raw Ingested Records | Structured Machine Input |
| Format | Unstructured doctor text | Normalized JSON datasets |
- Data Masking Protocols: We remove personal patient identifiers from the training datasets to maintain strict regulatory compliance.
- Error Bias Normalization: Our engineers clear out duplicate or corrupt historical billing entries to prevent training the AI on past human mistakes.
Step 4: Build The Core AI Automation Modules
Next, our development teams construct the specialized natural language processing engines and predictive analytics layers. This is where we create your core proprietary intellectual property.
| Core Engines | Natural Language Processing | Predictive Risk Classifiers |
| Output | Accurate ICD-10 medical codes | Real-time claim denial scores |
- Model Pipeline Construction: We build custom machine learning frameworks trained specifically on specialized healthcare terminology.
- Payer Logic Calibration: We program the software to automatically adjust its evaluation criteria based on changing insurance company guidelines.
Step 5: Real Billing Scenarios Tests
We never deploy an unproven application into a live hospital network. At the same time, we subject the newly created billing platform to intensive, isolated testing using historical shadow data.
| Testing Stage | Initial Synthetic Simulation | Live Shadow Data Testing |
| Metric | Code accuracy benchmarks | First-pass clean claim rates |
- Stress Load Simulation: We push thousands of complex, error-filled claims through the system simultaneously to verify that the validation gates block every mistake.
- Parallel Running Audits: The software processes real claims in the background alongside human billers to compare speed, accuracy, and operational efficiency directly.
Step 6: Launch And Improve AI Performance
During the final launch phase, we connect the platform to live production systems and activate continuous optimization cycles. This turns your application into an evolving enterprise asset.
| Scaling Phase | Day 1 Go-Live Operations | Continuous Scaling Cycle |
| Focus | System integration safety | Autonomous accuracy refinement |
- Feedback Optimization Loops: When human billers correct a rare system error, the software logs that interaction to automatically retrain and smarten the model.
- Infrastructure Auto-Scaling: We engineer the underlying cloud architecture to automatically expand its processing power as your client portfolio grows.
Executing this deployment process successfully converts a complex software project into a highly valuable, market-ready fintech platform.
Partnering with Intellivon ensures your application is engineered to the highest industry standards, turning your initial development capital into a highly scalable, recurring revenue asset.
Cost to Build AI Healthcare Billing Software
AI healthcare billing platform development costs between $50,000 and $200,000, depending on AI features, integrations, compliance needs, billing workflows, and platform scale.
The cost to build an AI healthcare billing platform depends on how complex the platform needs to be. A focused MVP with claim tracking and basic automation costs less than a full AI billing platform with coding support, denial prediction, payer integrations, audit controls, and revenue dashboards.
At Intellivon, we break the development cost into clear phases. This helps founders and CTOs understand where the budget goes and how each phase supports the final product.
AI Healthcare Billing Platform Development Cost Breakdown
| Development Phase | Estimated Cost | What It Includes |
| Discovery And Product Strategy | $5,000–$12,000 | Workflow mapping, feature planning, AI use case selection, compliance planning, product roadmap |
| UI/UX Design And Prototyping | $8,000–$18,000 | User journeys, billing dashboards, claim screens, admin panels, clickable prototypes |
| MVP Backend And Core Platform | $20,000–$45,000 | User roles, patient data, claim workflows, billing logic, admin controls, and database setup |
| AI Billing Features | $15,000–$40,000 | Coding support, claim error detection, denial risk scoring, document review, smart work queues |
| Healthcare Integrations | $12,000–$35,000 | EHR, EMR, PMS, clearinghouse, payer API, payment, and ERP integrations |
| HIPAA And Security Controls | $8,000–$22,000 | PHI protection, encryption, access control, audit logs, secure hosting, compliance workflows |
| Testing And Quality Assurance | $7,000–$18,000 | Functional testing, integration testing, AI output validation, security checks, bug fixing |
| Deployment And Launch Support | $5,000–$10,000 | Cloud deployment, production setup, monitoring, launch support, and technical documentation |
Total Estimated Cost: $50,000–$200,000
Cost By Platform Scope
| Platform Scope | Estimated Cost | Best For |
| Basic AI Billing MVP | $50,000–$75,000 | Startups, small clinics, early SaaS validation |
| Mid-Level AI Billing Platform | $75,000–$120,000 | Growing healthcare companies and RCM teams |
| Advanced AI Billing Software | $120,000–$160,000 | Billing companies, SaaS platforms, and multi-specialty clinics |
| Enterprise AI Billing Platform | $160,000–$200,000 | Hospitals, healthcare groups, RCM vendors, enterprise teams |
How Intellivon Helps Control Cost
Intellivon helps healthcare founders and CTOs avoid building too much too early.
Instead of starting with every feature, we prioritize the workflows that create faster revenue impact.
A practical first version may focus on:
- Claim error detection
- Eligibility verification
- Denial risk scoring
- Billing work queues
- Revenue dashboards
- One or two key integrations
Then, the platform can scale into AI coding support, appeal automation, payment intelligence, ERP synchronization, and enterprise reporting.
This phased approach keeps the initial investment focused. It also helps teams move from MVP to full AI billing infrastructure without wasting budget on features users do not need yet.
Real AI Healthcare Billing Platform Use Cases
Implementing an AI billing system introduces immediate operational advantages across diverse healthcare environments.
These six real-world applications demonstrate how advanced automation transforms daily clinical workflows into high-performance financial operations.
1. Autonomous Medical Coding For Emergency Departments
Emergency departments handle unpredictable patient volumes and highly complex, unstructured clinical documentation.
This platform utilizes advanced NLP to translate frantic doctor notes into precise billing codes instantly.
- Contextual Chart Parsing: The AI reads completely unstructured physician narratives to extract underlying diagnoses and render treatments accurately.
- Instant Code Assignment: The system assigns exact ICD-10 and CPT codes within seconds, eliminating manual data entry queues.
- Accelerated Billing Cycles: Processing records autonomously immediately after patient discharge shrinks the time between care delivery and claim submission.
2. Predictive Denial Management For Multi-Specialty Clinics
Multi-specialty clinics face high denial rates because different medical specialties must satisfy wildly different insurance rules. The platform uses predictive analytics to inspect outgoing claims and fix errors before they leave the building.
- Payer Behavioral Tracking: The software continuously monitors historical insurance payments to learn the hidden, shifting rules that cause rejections.
- Pre-Submission Risk Scoring: Every compiled claim receives a dynamic probability score showing its exact likelihood of immediate approval.
- Proactive Correction Prompts: When the system flags a high-risk claim, it highlights the missing clinical documentation needed to guarantee payment.
3. Real-Time Eligibility Verification For Ambulatory Surgery Centers
Ambulatory surgery centers lose significant revenue when they perform expensive procedures on patients whose insurance benefits have quietly expired. This module automates front-end verification to secure payments before treatment begins.
- Automated Scheduler Pings: The system monitors the digital patient calendar and automatically queries insurance databases forty-eight hours before appointments.
- Granular Benefit Ingestion: The software extracts exact co-pays, remaining deductibles, and specific network coverage limits instantly.
- Instant Front-Desk Alerts: Staff receive clear notifications regarding patient out-of-pocket liabilities, allowing them to collect payments at check-in.
4. Prior Authorization Automation For Oncology Networks
Oncology treatments require expensive, specialized medications that always require complex insurance pre-approvals, frequently delaying vital patient care.
The platform automates this administrative process by matching clinical records to payer guidelines.
- Guideline Criteria Matching: The AI cross-references the patient’s medical chart against the insurance company’s specific clinical policy rules.
- Packet Compilation: The software gathers required lab results, imaging reports, and doctor notes into a secure digital submission packet automatically.
- Status Tracking Loops: Continuous digital communication loops monitor the insurance portal to secure approvals without requiring manual phone calls.
5. Propensity-To-Pay Patient Collection Models
Rising deductibles mean that patients owe a larger share of their medical bills, but manual collection efforts are expensive and inefficient.
The platform utilizes machine learning to customize patient financial outreach based on historic payment behaviors.
- Financial Profile Analysis: The software evaluates historical settlement patterns to predict an individual’s likelihood of paying their balance in full.
- Customized Installment Generation: The system automatically generates realistic, interest-free monthly payment plans tailored to the patient’s financial bracket.
- Automated Communication Routing: Digital reminders deploy through the patient’s preferred communication channels, boosting collection rates while reducing administrative overhead.
6. Automated Multi-Payer Contract Management
Hospitals routinely lose money when insurance companies underpay them relative to the complex, negotiated reimbursement contracts on file.
The software tracks incoming payments against active legal contracts to flag underpayments automatically.
- Digital Fee Schedule Mapping: The software parses complex, multi-year payer contracts to build an immutable database of negotiated reimbursement rates.
- Remittance Match Audits: The system checks every incoming electronic payment deposit against the exact contract rate expected for that specific procedure code.
- Automated Variance Appeals: When an insurance company underpays a claim, the software automatically generates and submits an appeal to recover the missing cash.
This wide-ranging operational utility ensures that your initial software investment captures immediate market demand from major healthcare networks looking to secure their financial margins.
Build AI Healthcare Billing Platforms With Intellivon
At Intellivon, we build AI-powered healthcare billing platforms for healthcare SaaS companies, billing service providers, RCM vendors, specialty clinics, hospitals, provider networks, and enterprise healthcare teams.
Our engineering approach connects eligibility checks, charge capture, AI-assisted coding, claim scrubbing, denial prediction, payment posting, patient billing, payer analytics, dashboard reporting, and secure healthcare integrations into one connected billing infrastructure.
A. Build AI Billing Workflows Around Real Healthcare Operations
AI healthcare billing software works best when it fits how billing teams, coders, claim specialists, front-office staff, and finance leaders manage revenue every day.
We design workflows that support real operational tasks instead of forcing teams into rigid systems.
We build workflows for:
- Eligibility verification
- Charge capture
- AI coding support
- Claim scrubbing
- Claim submission
- Denial alerts
- Payment posting
- Patient billing
- Revenue reporting
B. Integrate With Existing Healthcare Payment Systems
A healthcare billing platform becomes valuable when it connects with the systems where patient, claim, payer, payment, and documentation data already live.
We build secure integrations that keep billing workflows connected across the full revenue cycle.
We integrate with:
- EHR/EMR systems
- Practice management systems
- Billing platforms
- Clearinghouses
- Payment gateways
- ERA/EOB systems
- Document systems
C. Make Billing AI Secure, Explainable, And Reviewable
Healthcare billing AI must be accurate, controlled, and easy to audit. We build AI workflows with human review, confidence scores, explanation layers, audit trails, access controls, PHI protection, and compliance-ready monitoring.
We focus on:
- HIPAA-ready architecture
- Secure PHI handling
- Human approval
- Confidence scores
- Explainable AI outputs
- Audit-ready workflows
- Override tracking
- Model monitoring
If you are planning to build an AI healthcare billing platform, Intellivon can help you define the right scope, design a secure architecture, integrate healthcare systems, and develop AI workflows that support real billing and revenue outcomes.
Contact Intellivon to discuss your AI healthcare billing platform roadmap.
Conclusion
Investing in an AI healthcare billing platform solves systemic revenue leakage for enterprise operations. By replacing outdated manual workflows with proactive financial intelligence, this technology secures predictable cash flows and drives scalable growth.
Founders who launch these highly compliant, automation-driven solutions establish an indispensable asset within the lucrative healthcare fintech ecosystem.
Things To Know About AI Billing Softwares
Q1. How Much Does AI Healthcare Billing Software Cost?
A1. AI healthcare billing software usually costs between $50,000 and $200,000, depending on features, AI complexity, integrations, compliance needs, and platform scale. A focused MVP costs less, while advanced platforms with denial prediction, payment intelligence, EHR integrations, and analytics require higher investment.
Q2. How Long Does AI Billing Platform Development Take?
A2. AI billing platform development usually takes 4 to 9 months, depending on the scope. A basic MVP with billing automation and claim validation can launch faster. A more advanced platform with AI coding support, denial prediction, payment workflows, and multiple healthcare integrations takes longer.
Q3. Can AI Healthcare Billing Software Be HIPAA-Compliant?
A3. Yes, AI healthcare billing software can be HIPAA-compliant when it includes secure PHI handling, encryption, role-based access, audit logs, user permissions, data backup, and compliance-ready workflows. HIPAA should be planned from the architecture stage, not added after development.
Q4. Which Integrations Matter Most For Billing Platforms?
A4. The most important integrations include EHR/EMR systems, practice management systems, clearinghouses, payer systems, payment gateways, ERA/EOB systems, document management tools, and analytics dashboards. These integrations help billing teams manage claims, payments, denials, and patient billing from one connected platform.