Key Takeaways:
- AI billing platforms reduce denials by 40% and recover revenue lost to coding errors.
- Manual billing workflows have no realistic path to scale, given the coder shortage.
- NLP, predictive scrubbing, and denial automation replace reactive billing with proactive revenue protection.
- Development costs range from $50,000 for basic MVPs to $200,000 for enterprise platforms.
- Intellivon builds proprietary AI billing platforms with HIPAA controls, payer logic, and EHR integrations.
Medical billing has turned into a problem for generating revenue. Every delayed claim, missed code, and avoidable denial causes financial loss that builds up throughout the billing cycle. This directly affects cash flow, relationships with payers, and revenue predictability.
Traditional billing tools manage claims and payments fairly well. However, they do not provide revenue teams with enough insights into denial risk, coding gaps, changes in payer rules, or missing documentation. This is where revenue disappears, and where most billing software falls short.
Creating smarter billing systems means making workflows predictable, automated, and controlled throughout the entire process. It also goes beyond just having AI features. Secure PHI workflows, EHR and PMS integrations, payer logic, claim automation, denial management, audit controls, and scalable designs must all be properly planned and built from the start.
Intellivon develops AI medical billing platforms for healthcare SaaS founders, RCM companies, and enterprise care teams who want product ownership instead of the limitations of ready-made software. This blog discusses features, architecture, AI use cases, compliance, costs, and the steps required to build such a platform from scratch.
Why Healthcare Teams Need AI Medical Billing Software
Healthcare billing inefficiencies are no longer a back-office concern. They are a measurable financial problem that compounds across every billing cycle.
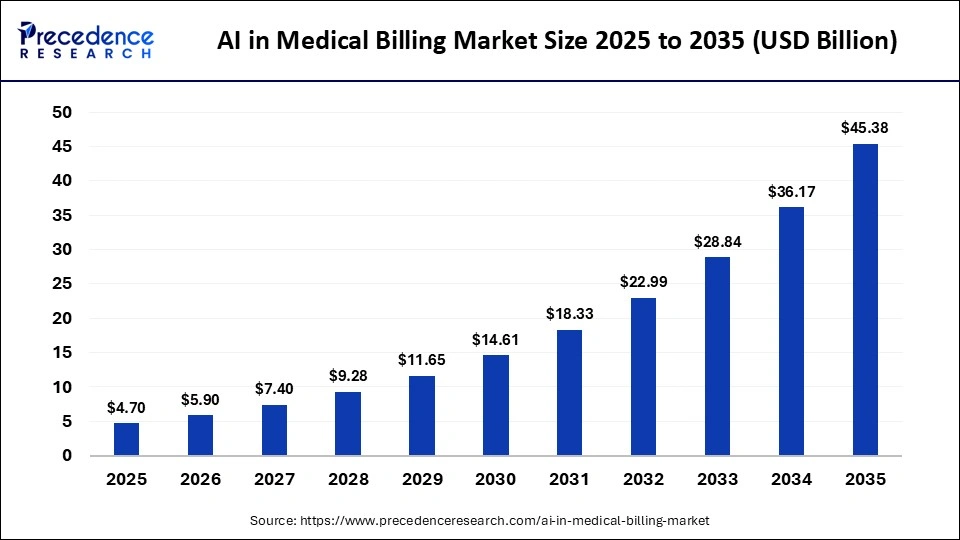
That growth is being driven by rising demand for billing automation, increasing healthcare data volumes, and the urgent need for faster, more accurate revenue cycle management across health systems globally.
1. Claim Denials Are Draining Revenue
In 2024, 11.81% of all claims were denied, up 2.4% year over year, with outpatient denials costing USD 5,390 per case. Furthermore, 86% of those denials are preventable.
A USD 3 million practice, however, still loses between 4 and 5% of annual revenue, approximately USD 150,000, to billing leakage. About 80% of medical bills contain errors, and 32% of denials trace directly back to coding mistakes.
2. Workforce Crisis Makes Manual Billing Unsustainable
A 12% shortage of certified coders exists today, projected to reach 30% nationally, with rural areas absorbing the sharpest impact.
Coder demand is simultaneously rising 13% by 2026, and 43% of providers are already understaffed. Manual billing workflows, therefore, have no realistic path to scale.
3. The Market Opportunity Is Significant
The AI medical billing market was valued at USD 4.70 billion in 2025 and is projected to reach USD 45.38 billion by 2035, growing at a CAGR of 25.44%.
That represents 9.6x growth within a decade, driven by organizations that can no longer absorb the USD 125 billion lost annually to billing errors industry-wide.
4. AI Delivers Proven Financial Returns
Organizations adopting AI billing platforms report 32% higher coding efficiency, 25% improvement in billing processes, and 40% fewer denials.
For a USD 3 million practice, AI can recover approximately USD 60,000 annually just through denial reduction, with payback typically achieved within 6 to 12 months.
The numbers make the case clearly. For healthcare businesses building or modernizing billing infrastructure, AI is the baseline requirement for financial stability at scale.
What Is AI Medical Billing Software Development?
AI medical billing software development is the process of designing and building healthcare billing platforms that use machine learning, NLP, and automation to manage claim submission, coding support, eligibility verification, denial prediction, payment posting, and revenue analytics.
The goal is to replace manual, error-prone billing workflows with intelligent systems that reduce denials, accelerate reimbursements, and give healthcare organizations measurable control over their revenue cycle.
How AI Medical Billing Software Works In Healthcare
The system acts as an intelligent bridge between clinical documentation and insurance reimbursement.
It continuously processes complex data to ensure providers receive accurate payments faster.
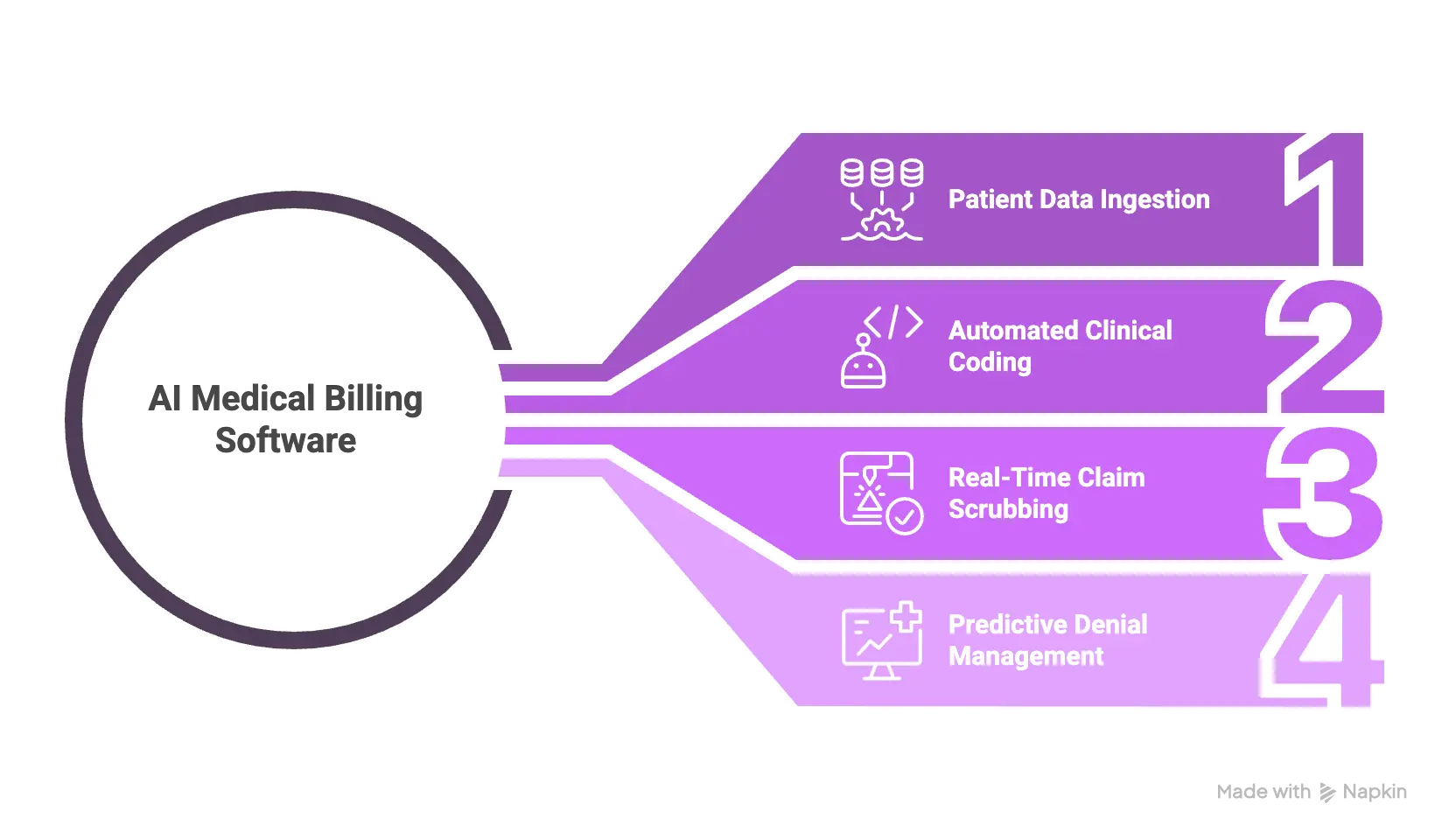
Step 1 Patient Data Ingestion
The platform automatically extracts patient demographics and insurance coverage details during registration. This initial step flags insurance errors before care is delivered. Therefore, providers avoid front-end eligibility denials entirely.
Step 2 Automated Clinical Coding
Advanced NLP models analyze physician notes and electronic health records.
The software translates this medical text into accurate diagnostic and procedural codes. Consequently, this automation reduces human coding bottlenecks significantly.
Step 3 Real-Time Claim Scrubbing
Before submission, the system checks claims against billions of shifting payer rules. Machine learning algorithms identify potential reasons for rejection instantly. As a result, billing teams correct issues prior to sending the claim.
Step 4 Predictive Denial Management
The software tracks submitted claims and predicts adjudication outcomes based on historical patterns. If an insurance company rejects a claim, the platform generates automated appeal workflows. This proactive approach saves hundreds of administrative hours daily.
In short, this technology turns a tedious manual process into an automated revenue engine. Investing in this development allows founders to capture massive market share by solving healthcare’s biggest operational bottleneck.
What Makes AI Billing Different From RCM Tools
Traditional revenue cycle management tools rely on rigid, pre-defined rules that frequently break when insurance policies change. In contrast, AI introduces adaptive learning models that evolve with changing compliance standards automatically.
| Feature Capabilities | Traditional RCM Software | AI-Driven Medical Billing |
| Claim Processing | Requires manual data input and basic rule checks | Automates validation using natural language processing |
| Denial Handling | Flags errors after the insurance company rejects them | Predicts potential denials before submission |
| Adaptability | Demands manual updates for every new billing regulation | Learns changing payer policies through continuous data updates |
| Workflow Efficiency | Relies heavily on human intervention for exceptions | Resolves complex clerical mismatches without human effort |
| Data Insights | Provides static reports on past financial performance | Offers real-time forecasting for future revenue streams |
Therefore, legacy platforms only track financial workflows while modern intelligent software actively optimizes them. Fintech investors can capture a premium market position by replacing these obsolete systems with self-correcting autonomous solutions.
Core Features Of AI Medical Billing Software
An enterprise-grade medical billing platform must execute multi-stage administrative functions without relying on fragile manual interventions.
Integrating advanced AI capabilities ensures that the software remains highly scalable and perfectly compliant with evolving healthcare laws.
Enterprise AI Medical Billing Functional Matrix
| Core Module | Technical Mechanism | Strategic Enterprise Impact |
| Eligibility Verification | Automated payer portal data scraping | Eliminates front-end eligibility claim rejections |
| Coding & Charge Capture | Generative clinical note analysis | Prevents lost revenue from omitted codes |
| Predictive Scrubbing | Real-time machine learning verification | Maximizes the initial first-pass clean claim rate |
| Submission Routing | Autonomous electronic clearinghouse syncing | Shortens standard accounts receivable collection cycles |
| Denial Automation | Automated appeal letter compilation | Recovers lost revenue without adding labor costs |
| Financial Analytics | Enterprise predictive cash flow modeling | Uncovers deep, actionable operational efficiencies |
1. Insurance Eligibility And Benefit Verification
Front-end mistakes represent the single largest driver of preventable medical claim rejections across modern hospital networks. AI medical billing software mitigates this vulnerability by automating comprehensive patient verification protocols during the initial scheduling phase.
- Advanced computer vision models extract structured insurance information from physical coverage cards instantly.
- The system queries dozens of insurance systems simultaneously to verify individual co-pays and deductibles.
- Automated modules flag missing prior authorizations before a patient receives medical treatment.
Therefore, administrative registration teams catch coverage gaps prior to the delivery of expensive clinical care. This proactive oversight protects the hospital line from immediate front-end financial losses.
2. AI Medical Coding And Charge Capture Support
Manual translation of clinical summaries into standardized medical codes creates significant operational bottlenecks for growing billing companies. Ambient AI systems solve this resource constraint by interpreting unstructured clinical records automatically.
- Sophisticated natural language understanding models review complex physician transcripts in real time.
- The application extracts appropriate diagnostic and procedural codes directly from medical notes.
- Context-aware safeguards flag structural inconsistencies between documented care and selected billing codes.
Consequently, providers eliminate expensive human coding backlogs while boosting overall compliance. This advanced layer prevents structural revenue leakage by identifying billable clinical items that human operators routinely overlook.
3. Claim Scrubbing And Billing Error Detection
Submitting flawed claims to insurance networks results in expensive administrative rejections and delayed cash collections.
Predictive auditing layers act as automated gatekeepers, validating financial submissions before they ever leave the healthcare organization.
- The software checks every compiled claim against billions of shifting commercial payer regulations.
- Machine learning algorithms analyze historical rejection trends to assign an accurate denial risk score.
- The platform isolates non-compliant submissions automatically and suggests specific corrections to billing staff.
As a result, health organizations regularly achieve exceptionally high first-pass clean claim ratios. Preventing errors at the submission stage significantly minimizes downstream administrative overhead.
4. Automated Claim Submission And Status Tracking
Managing manual follow-up workflows across diverse insurance portals strains internal billing department resources. Autonomous AI orchestration engines remove this burden by managing the entire transactional lifecycle independently.
- The system batches and transmits validated claims to clearinghouses via secure electronic data interfaces.
- Software robots systematically monitor payer networks to track claim processing statuses in real time.
- The system surfaces slow or stalled claims automatically to prevent filing deadline expirations.
Therefore, financial managers maintain total visibility over their outstanding claims without dedicating human hours to manual tracking. This persistent automation dramatically stabilizes incoming corporate cash flow.
5. Denial Management And Appeal Workflow Automation
Resolving rejected medical insurance claims manually costs healthcare networks hundreds of millions of dollars in administrative overhead. AI Agentic automation resolves this friction by managing the entire post-adjudication lifecycle independently.
- Algorithms interpret electronic remittance advice files to categorize the root cause of every denial.
- The system compiles localized appeal arguments by cross-referencing relevant patient records with payer rules.
- Automated queues dispatch completed appeal packets directly to insurance companies for re-evaluation.
AI-driven appeal generation reduces the average time spent resolving complex billing disputes by more than 60%.
Consequently, billing teams recover critical revenue that would otherwise be abandoned due to restrictive labor constraints. This automated defense significantly protects enterprise operational margins.
6. Payment Posting, AR Tracking, And Revenue Analytics
Reconciling multi-payer electronic remittances against bank deposits manually introduces significant operational risk and potential accounting errors.
Automated ledger engines maintain absolute transactional precision across complex corporate health networks.
- Embedded modules match inbound clearinghouse files with specific bank deposits automatically.
- Machine learning tools convert legacy paper documentation into searchable, structured financial records.
- Dynamic analytical dashboards forecast future cash collections while pinpointing persistent operational inefficiencies.
Ultimately, enterprise executives gain clear, real-time insights into their macro-level financial health. Replacing outdated accounting spreadsheets with proactive analytical intelligence enables predictable long-term corporate growth.
AI Use Cases In Medical Billing Software
Implementing targeted AI use cases allows healthcare enterprises to transform reactive reimbursement workflows into proactive revenue generation models.
These advanced applications deploy specialized machine learning algorithms to solve systemic operational inefficiencies across the entire software ecosystem.
1. Predictive Denial Risk Scoring For Claims
Submitting healthcare claims without assessing their rejection probability forces administrative teams into a costly cycle of reactive appeals.
An advanced AI medical billing software deploys predictive scoring engines to evaluate every claim before it leaves the facility.
- Neural networks evaluate hundreds of data points within a compiled claim against historical payer adjudication patterns.
- The system assigns a precise percentage-based denial risk score to each invoice prior to electronic transmission.
- High-risk submissions are diverted automatically to senior specialists with specific recommendations for technical correction.
2. AI-Assisted Coding From Clinical Documents
Manual medical coding is highly susceptible to human fatigue, leading to costly under-coding or non-compliant over-coding. Ambient intelligence models streamline this process by serving as an automated, highly accurate co-pilot for human coding teams.
- Natural language processing models extract clinical semantic concepts from unstructured doctor notes and discharge summaries.
- The application maps these clinical findings directly to the most accurate, compliant diagnostic and procedural codes.
- Real-time audit trails explain the logical clinical reasoning behind every automated code suggestion.
This supportive layer minimizes compliance audit liabilities while maximizing charge capture precision.
3. Automated Missing Data And Error Detection
Incomplete patient demographic profiles or incorrect insurance group numbers trigger immediate, automated rejections from insurance clearinghouses.
Smart AI medical billing data imputation engines identify and resolve these omissions before they disrupt the revenue cycle.
- Advanced heuristic algorithms scan complex claim files to pinpoint missing subscriber IDs or invalid modifier combinations.
- The platform automatically queries internal health records to find and populate missing demographic data fields.
- Real-time alerts block flawed invoices from entering the submission queue until the critical data gaps are resolved.
Resolving data gaps programmatically ensures a highly fluid transactional pipeline.
4. Smart Work Queues For Billing Teams
Traditional billing departments organize their daily tasks using basic alphabetical lists or static, unoptimized receipt dates.
Dynamic workflow orchestration optimizes labor allocation by prioritizing outstanding accounts based on true financial impact.
- Machine learning models calculate the exact collection probability and potential dollar value for every outstanding invoice.
- The platform populates smart work lists that automatically route high-priority, high-value claims to available staff.
- Task assignments shift dynamically in real time based on changing payer deadlines and team performance metrics.
This structural optimization ensures that human effort is always focused on the highest-return activities.
5. Underpayment Detection And Revenue Leakage Alerts
Insurance payers frequently underpay contractually agreed-upon rates, a trend that routinely goes unnoticed due to complex fee schedules.
Modernized AI medical billing platforms feature underpayment detection modules that act as automated financial auditors to safeguard corporate revenue margins.
- Digital contract modeling engines digitize and store complex, multi-tiered commercial payer fee structures.
- The software cross-references every inbound electronic remittance against the exact contract terms automatically.
- The platform flags underpayments instantly and generates automated demand letters to recover the missing funds.
Implementing automated contract auditing allows financial leaders to capture every dollar of contractually owed revenue.
In conclusion, continuous variance monitoring plugs the hidden financial leaks that quietly drain large healthcare operations. Funding a platform with native underpayment detection gives fintech founders an unassailable financial value proposition.
Technical Architecture For AI Billing Platforms
An enterprise-grade AI medical billing platform requires a highly resilient, multi-tiered infrastructure to process sensitive clinical data at scale.
The underlying architecture must seamlessly balance high-throughput computational processing with stringent enterprise security protocols.
Enterprise AI Medical Billing Technology Stack
| Architecture Layer | Core Technologies and Frameworks | Strategic Enterprise Function |
| Data Layer | PostgreSQL, AWS Aurora, Redis, AWS KMS | Secures and isolates protected health information |
| Integration Layer | HL7 FHIR APIs, Mirth Connect, REST | Syncs clinical documentation with external records |
| Gateway Layer | X12 EDI Engines, Change Healthcare APIs | Handles secure transactional routing to clearinghouses |
| AI Model Layer | Python, PyTorch, BERT, OpenAI API | Executes medical coding and predictive denial scoring |
| Automation Layer | Apache Airflow, Celery, Node.js | Drives automated claims routing and background tasks |
| Security Layer | OAuth 2.0, AWS CloudTrail, Okta | Enforces zero-trust access and immutable audit tracking |
1. Secure PHI Data Layer For Healthcare Workflows
The foundational data architecture must isolate protected health information (PHI) while maintaining rapid data accessibility.
At the same time, financial investors must prioritize absolute cryptographic security at this layer to prevent catastrophic data liabilities.
- Database engines utilize advanced hardware-level encryption algorithms to secure medical records both at rest and during transit.
- In-memory caching systems handle volatile transaction data to optimize platform speed during peak operating hours.
- Storage layers deploy automated data partitioning strategies to isolate tenant records across large hospital networks.
2. EHR, EMR, And Practice Management Integrations
An intelligent platform cannot operate in isolation from the clinical systems that generate healthcare data. Seamless ingestion requires standardized communication protocols to pull data directly from electronic health records.
- Fast Healthcare Interoperability Resources (FHIR) APIs establish real-time data pipelines between clinical systems and the billing software.
- Specialized integration engines translate legacy healthcare data formats into clean, modern database structures automatically.
- Continuous bidirectional syncing modules update administrative records across all connected clinical platforms instantly.
This absolute integration removes manual human entry errors from the initial stage of the revenue cycle.
3. Clearinghouse, Payer API, And ERP Integrations
The financial core of the software must communicate efficiently with diverse insurance networks and corporate enterprise resource planning ledgers. This connectivity accelerates cash collection by utilizing direct, automated transactional channels.
- Electronic data interchange mapping modules translate internal billing data into standard X12 clearinghouse formats.
- Modern payer application programming interfaces bypass slow legacy clearinghouses to verify immediate claim status updates.
- Financial webhooks feed real-time collection data directly into the hospital’s enterprise resource planning (ERP) systems.
Implementing robust integration gateways guarantees maximum transactional velocity for the entire enterprise.
4. AI Model Layer For Coding And Denial Prediction
The intelligence tier forms the core competitive advantage of the modern AI medical billing platform. This layer runs highly specialized machine learning models that analyze clinical text and calculate financial risks.
- Natural language processing (NLP) models interpret unstructured doctor notes to extract appropriate diagnostic and billing codes.
- Machine learning classifiers evaluate historical data to predict exactly which insurance company will reject a claim.
- Model management pipelines handle continuous training cycles to adapt to shifting regulatory and healthcare policies.
Investing in a robust machine learning layer ensures the platform remains highly accurate in a shifting market.
5. Workflow Automation Layer For Billing Operations
The automation engine acts as the operational nervous system, managing complex background tasks without human intervention.
This framework handles the automated execution of administrative tasks based on real-time triggers.
- Distributed task queues manage thousands of background tasks simultaneously without degrading the platform’s user experience.
- Automated workflow orchestration tools manage complex multi-step processes like automated appeal routing and bulk filing.
- Real-time event notifications trigger instant communication alerts when critical financial anomalies require senior human review.
Fintech founders can leverage this automation to operate a highly scalable billing system with low overhead.
6. Compliance, Audit Logs, And Access Controls
Enterprise healthcare applications must maintain absolute regulatory compliance to survive rigorous institutional procurement processes. The security layer enforces tight guardrails around every data interaction within the platform.
- Centralized identity providers manage secure multi-factor authentication and role-based access controls for all users.
- Immutable audit logging services record every single data modification and patient record access event permanently.
- Automated compliance monitoring tools continuously scan cloud infrastructure to detect and fix security vulnerabilities instantly.
In conclusion, robust compliance architecture transforms a standard software application into an enterprise-grade financial asset. Building verifiable, high-security infrastructure builds deep trust with the conservative buyers who dominate the healthcare market.
HIPAA And Compliance Needs For AI Billing Software
Navigating the stringent landscape of healthcare compliance is non-negotiable when launching an enterprise administrative platform.
Incorporating robust regulatory guardrails directly into your software blueprint protects your venture from catastrophic legal penalties and builds institutional trust.
1. PHI Encryption, Access Control, And Audit Logs
Safeguarding protected health information requires continuous cryptographic protection across your entire database ecosystem. Fintech developers must implement a zero-tolerance approach to data security to satisfy institutional procurement officers.
- Database engines maintain absolute data isolation by encrypting sensitive patient records at rest and during transit.
- Immutable, write-once audit logs record every instance of file access, user login, and data alteration permanently.
- Automatic session timeouts and multi-factor authentication prevent unauthorized exposure on shared workplace terminals.
Therefore, your platform establishes an unalterable digital paper trail for every single piece of clinical data it processes. This rigorous defense mechanism completely insulates your healthcare clients from devastating federal audit failures.
2. Role-Based Permissions For Billing Teams
A massive operational hazard in healthcare centers is internal staff accessing patient data outside their specific job requirements. Implementing tight, automated permission parameters ensures data exposure remains strictly on a need-to-know basis.
- Administrative dashboards restrict data access based on clear corporate roles like medical coder, billing clerk, or financial auditor.
- Granular security configurations block standard billing employees from viewing sensitive, non-billing clinical documentation.
- Executive management overrides require secondary security approvals to prevent internal collusion or data theft.
Consequently, your application minimizes the internal surface area vulnerable to data leaks and accidental compliance violations. This structured access model aligns perfectly with the HIPAA principle of minimum necessary disclosure.
3. Secure AI Model Workflows For Healthcare Data
Utilizing LLMs introduces unique compliance risks, particularly regarding data retention and unauthorized model training. Engineering a compliant machine learning pipeline requires isolating data completely from public AI infrastructure.
- APIs connecting to external machine learning models must operate under strict zero-data-retention agreements.
- Internal data scrubbing microservices strip out direct patient identifiers before sending text to artificial intelligence engines.
- Open-source machine learning models are deployed within your isolated cloud environment to prevent data leakage.
As a result, patient records are never absorbed into public models or used for unauthorized training cycles. Building these secure algorithmic pathways ensures your proprietary technology remains fully compliant with modern data privacy laws.
4. Vendor, Hosting, And Data Governance Requirements
Building an enterprise billing system requires establishing a fully compliant web of infrastructure partners and clear corporate policies. Every third-party utility you integrate must mirror your strict compliance stance exactly.
- Cloud hosting solutions must be anchored entirely on healthcare-compliant infrastructure with signed Business Associate Agreements.
- Service Level Agreements mandate routine SOC 2 Type II audits to verify ongoing operational security posture.
- Data retention policies automatically purge or anonymize financial archives according to individual state medical record laws.
In conclusion, absolute compliance governance transforms a simple software application into a bulletproof enterprise asset. Founders who invest heavily in these verification protocols gain a massive advantage over cheap, non-compliant alternatives.
How We Build AI Medical Billing Software Step-by-Step
At Intellivon, we follow a rigorous, enterprise-grade engineering methodology to design, build, and deploy high-performance AI medical billing platforms.
We break down the complex development lifecycle into transparent, manageable phases so non-technical founders can track their investment with absolute clarity.
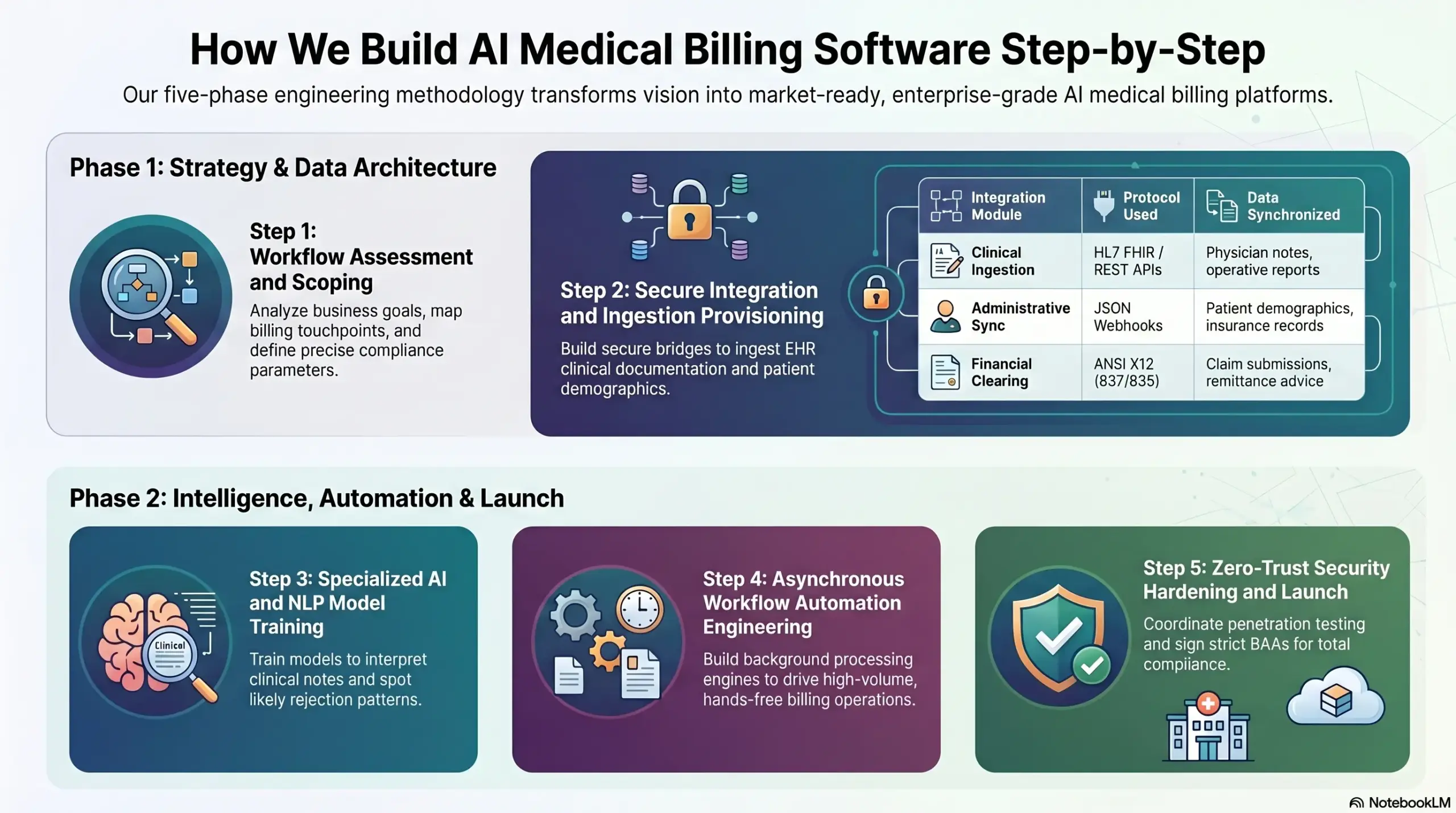
Step 1: Healthcare Workflow Assessment and Scoping
Before writing a single line of code, our strategic consultants analyze your specific business goals, operational bottlenecks, and target user personas.
We map out every touchpoint in the billing lifecycle to ensure the technical architecture perfectly mirrors real-world healthcare needs.
- We conduct deep discovery sessions to evaluate your existing practice management systems and pinpoint revenue leakage areas.
- Our analysts define the precise compliance parameters, target medical specialties, and clearinghouse routing rules required for your product.
- We establish clear engineering benchmarks, including first-pass clean claim targets and processing speed requirements.
Therefore, we eliminate development guesswork and ensure your capital is spent building high-value, highly marketable features. This meticulous upfront planning sets a bulletproof foundation for your entire software investment.
Step 2: Secure Integration and Ingestion Provisioning
A billing platform is only as good as its data access pipeline.
Intellivon engineers build secure, low-latency integration bridges to ingest raw clinical documentation and patient demographics directly from electronic health records.
| Integration Module | Protocol Used | Data Synchronized |
| Clinical Ingestion | HL7 FHIR / REST APIs | Physician notes, operative reports, and lab results |
| Administrative Sync | JSON Webhooks | Patient demographics, insurance coverage records |
| Financial Clearing | ANSI X12 (837/835) | Claim submissions, electronic remittance advice |
- We deploy specialized interface engines to translate fragmented, legacy medical data into clean database structures.
- Our teams configure automated data synchronization loops to ensure records update across all systems in real time.
- We implement strict front-end validation gates to catch missing or malformed data before it reaches your core processing engine.
Consequently, your platform operates as a seamless extension of the provider’s existing software ecosystem. This deep connectivity eliminates manual data entry and sets the stage for autonomous processing.
Step 3: Specialized AI and NLP Model Training
This phase is where we build your core intellectual property and competitive market advantage. We configure, fine-tune, and validate the advanced artificial intelligence models that handle automated medical coding and predictive denial scoring.
[Clinical Text] ➔ [Intellivon NLP Engine] ➔ [ICD-10 / CPT Codes] ➔ [Predictive Denial Scoring Model]
- Our data scientists train NLP models to accurately interpret unstructured clinical notes and doctor charts.
- We feed historical claim data into machine learning classifiers to teach the software how to spot likely rejection patterns.
- We engineer isolated, zero-data-retention model pipelines to ensure all algorithmic training complies fully with patient privacy laws.
Building this advanced AI layer commands premium market valuations for your product.
Step 4: Asynchronous Workflow Automation Engineering
With the integrations and models in place, Intellivon builds the background processing engines that drive high-volume, hands-free billing operations.
This layer replaces slow clerical tasks with instantaneous, automated computational routines.
- We build robust, distributed task queues to handle thousands of complex claim checks simultaneously without slowing down the user interface.
- Our developers design dynamic, self-sorting work queues that automatically route high-priority billing exceptions to senior human operators.
- We code automated background agents that track claims across insurance portals and flag processing stalls instantly.
Therefore, your platform breaks the dependency on large administrative teams to scale operational volume. This supreme automation efficiency allows your clients to maximize their revenue capture with minimal overhead.
Step 5: Zero-Trust Security Hardening and Launch
The final step focuses on protecting your product against security vulnerabilities and ensuring it sails through strict corporate procurement audits. We apply a multi-layered security framework across every component of the completed software ecosystem.
- We enforce strict role-based access controls and manage secure identity verification via trusted enterprise authentication systems.
- Our team runs exhaustive automated vulnerability scans and coordinates comprehensive penetration testing to harden the application.
- We sign strict BAAs and provide immutable audit trails to guarantee total compliance with healthcare laws.
In conclusion, our comprehensive deployment methodology transforms your initial vision into a bulletproof, market-ready corporate asset.
Partnering with Intellivon ensures your software is engineered to the highest standards of enterprise performance, safety, and scale.
AI Medical Billing Software Development Cost
AI medical billing software development costs between $50,000 and $200,000, depending on AI features, integrations, compliance needs, billing workflows, and platform scale.
The cost to build AI medical billing software depends on how complex the platform needs to be. A focused MVP with claim tracking and basic automation costs less than a full AI billing platform with coding support, denial prediction, payer integrations, audit controls, and revenue dashboards.
At Intellivon, we break the development cost into clear phases. This helps founders and CTOs understand where the budget goes and how each phase supports the final product.
AI Medical Billing Software Development Cost Breakdown
| Development Phase | Estimated Cost | What It Includes |
| Discovery And Product Strategy | $5,000–$12,000 | Workflow mapping, feature planning, AI use case selection, compliance planning, product roadmap |
| UI/UX Design And Prototyping | $8,000–$18,000 | User journeys, billing dashboards, claim screens, admin panels, clickable prototypes |
| MVP Backend And Core Platform | $20,000–$45,000 | User roles, patient data, claim workflows, billing logic, admin controls, and database setup |
| AI Billing Features | $15,000–$40,000 | Coding support, claim error detection, denial risk scoring, document review, smart work queues |
| Healthcare Integrations | $12,000–$35,000 | EHR, EMR, PMS, clearinghouse, payer API, payment, and ERP integrations |
| HIPAA And Security Controls | $8,000–$22,000 | PHI protection, encryption, access control, audit logs, secure hosting, compliance workflows |
| Testing And Quality Assurance | $7,000–$18,000 | Functional testing, integration testing, AI output validation, security checks, bug fixing |
| Deployment And Launch Support | $5,000–$10,000 | Cloud deployment, production setup, monitoring, launch support, and technical documentation |
Total Estimated Cost: $50,000–$200,000
Cost By Platform Scope
| Platform Scope | Estimated Cost | Best For |
| Basic AI Billing MVP | $50,000–$75,000 | Startups, small clinics, early SaaS validation |
| Mid-Level AI Billing Platform | $75,000–$120,000 | Growing healthcare companies and RCM teams |
| Advanced AI Billing Software | $120,000–$160,000 | Billing companies, SaaS platforms, and multi-specialty clinics |
| Enterprise AI Billing Platform | $160,000–$200,000 | Hospitals, healthcare groups, RCM vendors, enterprise teams |
How Intellivon Helps Control Cost
Intellivon helps healthcare founders and CTOs avoid building too much too early.
Instead of starting with every feature, we prioritize the workflows that create faster revenue impact.
A practical first version may focus on:
- Claim error detection
- Eligibility verification
- Denial risk scoring
- Billing work queues
- Revenue dashboards
- One or two key integrations
Then, the platform can scale into AI coding support, appeal automation, payment intelligence, ERP synchronization, and enterprise reporting.
This phased approach keeps the initial investment focused. It also helps teams move from MVP to full AI billing infrastructure without wasting budget on features users do not need yet.
Build Vs Buy: Which Option Makes Sense?
Enterprise technology leaders must decide whether to license an existing billing engine or commit capital to build proprietary software. This strategic choice directly dictates long-term profit margins, software scalability, and corporate valuation.
When Off-The-Shelf Billing Software Works
Commercial off-the-shelf billing applications provide a fast, predictable path to market deployment for low-volume medical operations. Licensing existing platforms works well when the standard revenue cycle requires no unique workflow customization.
- Standard medical clinics with basic, predictable fee structures can launch pre-built software with minimal configuration overhead.
- Small administrative teams with tight initial cash reserves benefit from low upfront setup costs compared to custom software development.
- Operations that do not require proprietary intellectual property or custom product branding find adequate utility in public software packages.
Therefore, commercial platforms serve as a practical starting point for businesses with generic administrative needs. This route avoids upfront engineering timelines but binds your company to recurring per-user licensing fees permanently.
2. When Custom AI Billing Software Is Better
Developing custom technology becomes highly necessary when an organization scales to handle massive transactional volumes across diverse health networks.
Bespoke platforms unlock structural cost efficiencies that off-the-shelf applications simply cannot replicate.
- Growing revenue cycle management firms use custom software to break the dependency on expensive, per-seat vendor licensing models.
- Digital health innovators build proprietary systems to securely control their raw transactional data pipelines and clinical analytics.
- Specialized medical networks utilize custom software to automate highly specific regional insurance billing and compliance workflows.
Consequently, proprietary engineering transforms an operational expense into a highly defensible corporate asset.
Building a custom system guarantees complete operational freedom and significantly maximizes your enterprise market valuation.
How Founders Should Compare Build And Buy
Fintech investors must objectively weigh immediate financial constraints against long-term strategic growth goals. Evaluating specific operational parameters ensures your selected path aligns perfectly with your macro corporate roadmap.
- Calculate your total cost of ownership by comparing upfront engineering investments against lifetime per-transaction vendor fees.
- Assess your data sovereignty needs to determine if your platform requires strict, isolated patient database custody.
- Review your product roadmap to ensure vendor software updates will not limit your ability to introduce unique platform features.
In conclusion, buying provides immediate speed, but building builds unassailable, high-margin enterprise value.
Strategic leaders invest in custom engineering to secure a permanent, highly scalable competitive advantage in the healthcare market.
Real Examples Of AI Medical Billing Software
Reviewing established market leaders allows enterprise investors to understand the practical execution and commercial viability of intelligent revenue infrastructure.
These real-world platforms demonstrate how integrating machine learning systematically stabilizes cash flow and reduces administrative overhead across diverse healthcare environments.
1. athenahealth (athenaOne)
This cloud-based enterprise suite integrates EHR directly with a massive, network-driven artificial intelligence rules engine.
The platform analyzes aggregated data across millions of daily medical encounters to optimize financial performance.
- The system deploys machine learning models to continuously absorb shifting payer guidelines across its massive provider network.
- Automated staff assistants handle repetitive tasks like note-taking, clinical text documentation, and standard review replies.
- Real-time billing validation mechanisms automatically flag compliance variances before a claim leaves the digital ecosystem.
Therefore, the platform leverages collective network intelligence to shield individual practices from unexpected regulatory updates. This network-wide automation ensures exceptionally low error rates for large ambulatory care groups.
In short, athenahealth proves how macro-level transactional data can be harnessed to optimize micro-level practice revenue. Investors can look to this model to understand the immense value of network-scale predictive training.
2. Waystar
Operating as a high-volume enterprise clearinghouse, this platform integrates advanced machine learning models directly into the primary transaction layer.
The software focuses on automating the end-to-end data transmission pipeline between healthcare providers and public insurers.
- Agentic workflows handle autonomous eligibility checks and real-time benefits verification during patient registration.
- The system utilizes predictive scoring algorithms to flag complex claims that run a high risk of rejection.
- Automated post-adjudication engines interpret remittance advice documents to streamline cash posting.
Consequently, large hospital networks compress their standard collection cycles by eliminating manual clearinghouse back-and-forth. This strategic automation allows billing agencies to scale transaction volumes effortlessly without increasing headcount.
Ultimately, Waystar demonstrates how embedding AI into the transactional architecture maximizes operational velocity. Building a platform with similar clearinghouse capabilities creates a highly defensible fintech product.
3. PracticeSuite
This comprehensive all-in-one practice management and billing platform embeds native automation directly into its core financial workflows.
The software is engineered to simplify complex administrative tasks for solo practices and large medical billing companies alike.
- The application integrates NLP tools to ensure precise clinical validation across electronic data forms.
- Embedded workflows automatically route complex billing exceptions to dedicated specialists based on predictive collection parameters.
- Real-time financial dashboards provide executive users with instantaneous forecasting regarding future cash flow pipelines.
As a result, healthcare organizations minimize manual clerical oversight while protecting themselves against revenue leakage. This highly unified design enables lean administrative teams to operate with elite financial efficiency.
In conclusion, PracticeSuite highlights the immense market demand for unified, easy-to-use cloud-based revenue software. Investing in a holistic platform structure allows founders to capture premium subscription revenue from expanding clinics.
4. Claimocity
This highly specialized platform targets inpatient physicians and mobile hospitalist networks who require rapid charge capture tools at the point of care.
The software utilizes AI to eliminate the delayed data tracking that routinely causes hospital revenue loss.
- Mobile voice-recognition tools analyze clinical dictations on the fly to generate structured billing codes immediately.
- Real-time continuous audit engines review physician charts to identify missing billable services automatically.
- The software coordinates dynamic billing schedules to ensure physicians meet strict institutional filing deadlines.
Therefore, the platform prevents silent financial erosion by capturing complex hospital transactions the moment they occur. This niche optimization delivers immediate, measurable return on investment to high-utilization medical specialists.
Consequently, Claimocity underscores the immense value of building targeted, specialty-centric administrative solutions. Crafting a mobile-first intelligent capture engine allows fintech developers to solve specific, high-cost operational bottlenecks.
5. AdvancedMD
Engineered specifically for independent practices and expanding group networks, this unified software suite combines clinical data tracking with intelligent claim correction technology.
The platform features an industry-recognized automated scrubbing engine to optimize initial submission success.
- The software checks compiled insurance claims against thousands of automated, payer-specific rules at the point of submission.
- Integrated eligibility verification tools run background checks automatically to ensure patient coverage remains completely active.
- Machine learning algorithms analyze historical denial trends to recommend specific text corrections to administrative staff.
Ultimately, healthcare organizations achieve consistently high first-pass clean claim ratios while reducing manual phone follow-ups to insurers. Preventing transaction errors before submission permanently stabilizes operational cash flow.
In summary, AdvancedMD proves that proactive, pre-submission checking is vastly superior to reactive post-denial sorting. Funding a platform with native pre-submission validation provides fintech entrepreneurs with an unassailable sales proposition.
Business Benefits Of AI Medical Billing Software
Investing in custom AI medical billing software development allows fintech entrepreneurs and healthcare operators to capture substantial economic value.
By transforming manual, error-prone clerical workflows into optimized automated pipelines, these intelligent systems deliver immediate and compounding business returns.
1. Reduced Days Sales Outstanding (DSO)
Legacy billing methodologies rely on slow human processing loops that tie up critical institutional capital for months at a time. Automated revenue engines break this operational dependency by executing administrative tasks instantaneously.
- Advanced validation layers verify insurance eligibility and run background checks before a patient even leaves the clinic.
- Automated claim submission modules package and route clean invoices to clearinghouses within seconds of chart finalization.
- Predictive tracking bots scan payer portals continuously to uncover and resolve processing stalls before they cause payment delays.
Therefore, healthcare enterprises compress their reimbursement cycles and capture outstanding cash weeks faster than traditional agencies. This dramatic acceleration in capital velocity provides operators with the liquid resources required to fund aggressive institutional expansion.
In short, reducing DSO transforms stagnant accounts receivable into active, working capital. Investors who fund this technological enhancement create an incredibly high-yield financial tool for large hospital networks.
2. Improved First-Pass Clean Claim Rates
Every initial claim denial forces billing staff into an expensive, multi-week cycle of manual review, correcting, and resubmitting. Moving the validation checkpoint to the front of the submission pipeline permanently shields operations from these administrative setbacks.
- Machine learning algorithms scan data strings for missing fields or incorrect insurance numbers prior to transmission.
- AI models check every invoice against billions of active, payer-specific compliance constraints in real time.
- The system routes flawed entries back to front-office staff automatically with clear, contextual instructions for immediate fix.
Consequently, healthcare organizations frequently achieve first-pass clean claim acceptance rates well above 95%. Eliminating bulk rejections at the source drastically minimizes downstream administrative friction.
Ultimately, maximizing the initial acceptance rate secures an incredibly predictable and reliable revenue pipeline. Building this preventive guardrail gives technology startups a powerful, data-backed value proposition when pitching enterprise clients.
3. Elimination of Silent Revenue Leakage
Healthcare providers quietly lose millions of dollars annually because commercial insurance companies routinely underpay contractually agreed-upon rates. Because manual contract auditing is incredibly tedious, these profitable financial margins are frequently abandoned entirely.
- Automated contract management modules digitize complex, multi-tiered payer fee schedules into secure relational databases.
- The application cross-references every single inbound electronic remittance against exact contract matrices automatically.
- The platform flags payment variances instantly and compiles automated appeal documents to recover the outstanding funds.
As a result, health systems plug the hidden leaks that quietly drain corporate profitability over high-volume transaction portfolios. Capturing every single dollar of owed revenue directly stabilizes the enterprise’s bottom line.
4. Significant Reduction in Administrative Overhead Costs
Hiring, training, and retaining large teams of specialized human medical coders represents a massive, non-scalable operational expense. Integrating intelligent processing workflows decouples corporate scaling from linear headcount growth.
- NLP models interpret unstructured doctor notes to automate standard medical coding tasks.
- Smart task allocation queues ensure human staff focus exclusively on high-value, complex exception management.
- Background software robots handle bulk electronic data filing and routine clearinghouse messaging without human intervention.
Therefore, business process outsourcing firms and medical networks scale their transaction capacity exponentially while keeping operational overhead completely flat. This extreme efficiency significantly boosts overall corporate margins.
5. Enhanced Financial Predictability
Managing a large healthcare enterprise without accurate cash flow forecasting forces leadership into a reactive, defensive operational posture. Predictive data pipelines convert historical billing patterns into clear, actionable business intelligence.
- Data engines analyze past payer behavior to forecast the exact day an inbound bank deposit will land.
- Predictive models evaluate existing accounts receivable balances to alert leadership of upcoming seasonal cash dips.
- Analytical dashboards highlight changing collection trends across specific medical departments to optimize asset allocation.
Replacing outdated accounting spreadsheets with proactive analytical intelligence enables predictable long-term corporate growth.
In summary, data-driven foresight transforms the entire revenue cycle from an unpredictable variable into a highly stable strategic roadmap. Funding a platform with native predictive analytics allows fintech founders to build an unassailable position in the market.
Build AI Medical Billing Software With Intellivon
At Intellivon, we help healthcare founders, CTOs, RCM companies, SaaS teams, and enterprise healthcare businesses build AI medical billing platforms that support real revenue operations.
With 500K+ engineering hours, ex-MAANG engineers, and deep experience across AI, SaaS, healthcare, enterprise platforms, API integrations, and ERP-connected systems, we help you move from product idea to scalable billing infrastructure.
A. Product Strategy For Healthcare Founders And CTOs
Before development starts, we help you define what your AI medical billing platform should solve first.
Our team maps your billing workflow, claim lifecycle, payer touchpoints, user roles, integration needs, compliance requirements, and revenue leakage points. This helps us create a focused development roadmap instead of a bloated feature list.
We help you decide:
- Which billing workflows should be automated first
- Which AI use cases will create the fastest revenue impact
- Which integrations are needed for the first version
- Which features belong in the MVP
- Which compliance controls must be planned from day one
B. Custom AI Billing Software Development Services
We can help you build platforms for claim automation, AI-assisted coding, denial prediction, eligibility verification, payment tracking, AR analytics, and billing team workflows.
Your platform can include:
- Claim creation and validation
- AI-assisted medical coding
- Denial risk scoring
- Billing work queues
- Appeal workflow automation
- Payment posting support
- Revenue leakage alerts
- Admin and user dashboards
- Role-based access controls
- Audit-ready activity logs
Instead of forcing your team into a fixed product, we build software that matches your billing process, specialty needs, payer logic, and growth plan.
C. Healthcare, Payer, Clearinghouse, And ERP Integrations
AI medical billing software only works when data moves correctly across the healthcare revenue cycle.
That is why Intellivon plans integrations early. We help connect your billing platform with EHR systems, EMR systems, practice management systems, payer APIs, clearinghouses, payment gateways, document systems, and ERP or finance platforms.
These integrations help your platform manage:
- Patient and provider data
- Insurance eligibility checks
- Claim submission workflows
- Payer response tracking
- Denial and appeal updates
- Payment and reconciliation data
- Finance and revenue reporting
We also support complex API and ERP integration needs for businesses that want billing intelligence connected with wider finance operations.
D. Enterprise AI Engineering With Ex-MAANG Talent
Intellivon brings enterprise AI engineering experience across backend systems, SaaS platforms, cloud infrastructure, API-heavy products, automation workflows, and secure data architecture.
Our engineering team helps you build with:
- Scalable backend architecture
- Secure healthcare data pipelines
- AI model integration
- Cloud deployment planning
- API-first development
- Role-based access control
- Performance testing
- Monitoring and optimization
This helps your AI medical billing platform move beyond a basic automation tool and become a reliable revenue infrastructure layer.
Ready To Build AI Medical Billing Software?
If you are planning to build an AI medical billing platform for healthcare teams, RCM operations, SaaS users, or enterprise revenue workflows, contact Intellivon to help you define the right roadmap.
We will help you identify the best AI use cases, plan the architecture, prioritize integrations, define the MVP, and build a scalable platform around real billing outcomes.
Final Thoughts
Building an automated financial ecosystem requires a structured, step-by-step approach focused on solving immediate revenue bottlenecks. Aligning engineering cycles with measurable metrics like lower rejection rates transforms abstract code into a high-value software asset.
A strategic development roadmap ensures your capital optimizes the highest-return activities first. Choosing an experienced, enterprise-grade engineering partner guarantees that your platform launches smoothly, remains perfectly compliant, and successfully dominates the healthcare market.
Things To Know About AI Medical Billing Softwares
Q1. Can AI fully automate medical billing?
A1. AI can automate parts of medical billing, but it should not fully replace human review. It works best for eligibility checks, claim scrubbing, coding support, denial prediction, payment posting, and repetitive follow-ups. Complex payer rules, audits, appeals, and documentation issues still need trained billing teams.
Q2. What problems can AI medical billing software solve?
A2. AI medical billing software can reduce claim errors, missed codes, delayed submissions, denial backlogs, underpayments, and manual follow-up work. It helps billing teams catch issues earlier, prioritize high-risk claims, review documentation faster, and improve reimbursement workflows without depending only on spreadsheets or manual checks.
Q3. Is AI medical billing software useful for small practices?
A3. Yes, but the scope should be practical. Small practices usually need AI for eligibility checks, claim validation, denial alerts, payment tracking, and basic revenue dashboards first. A focused system can reduce billing workload, improve cash flow visibility, and help teams avoid preventable claim errors.
Q4. How does AI help reduce claim denials?
A4. AI helps reduce denials by checking claims before submission. It can flag missing patient details, coding mismatches, prior authorization gaps, payer-specific rule issues, duplicate claims, and weak documentation. This gives billing teams time to correct claims before they become denials.