Building on Epic EHR is not just a simple integration project. It requires a commitment that involves compliance, clinical workflows, real-time data exchange, and enterprise scalability, all at the same time. Organizations that underestimate this complexity often find themselves months into development with a product that works in staging but fails under real clinical demands. The choices made early on set the stage for everything that comes next.
Epic powers hospital records in the U.S. Any platform designed to connect with or expand its ecosystem takes on both its vast reach and its strict technical requirements. Getting this wrong can lead to delayed launches, failed audits, and clinical staff who lose trust in the tool entirely. Getting it right means having a platform that works well across health systems, gains procurement trust, and stands up to regulatory checks.
Intellivon has worked extensively inside these builds. We have navigated Epic’s developer ecosystem, FHIR-based APIs, certification rules, and the integration layers that most vendors overlook until it’s too late. That hands-on experience informs everything we will talk about in this blog. What follows is a breakdown of the Epic EHR features that developers and enterprise decision-makers need to understand before starting a build.
Why Developers Choose Epic for EHR Builds
Developers increasingly choose Epic for EHR builds for a clear reason. It is not just about APIs or data models. Instead, Epic has become the standard system across most U.S. hospitals and ambulatory networks.
As a result, integrating with Epic is no longer optional. It is often required to access real clinical workflows, patient data, and operational systems at scale.

This growth reflects a clear shift. Healthcare providers are investing heavily in digital infrastructure to support scalable, data-driven care delivery across systems.
Software developers in healthcare need a stable foundation that handles data security and compliance.
Epic serves as this core infrastructure, allowing technical teams to build specialized tools without reinventing basic record-keeping systems. This approach reduces development risk and speeds up the delivery of new clinical features.
1. Epic’s role in modern healthcare infrastructure
Modern hospitals require a single source of truth for patient data. Epic acts as the central operating system, providing a standardized environment where all clinical information lives.
It already powers over 300 million patient records, making it the largest “single‑version” EHR footprint in the U.S. healthcare ecosystem. Developers value this because it turns fragmented records into a clean, accessible database.
This eliminates the need for engineers to build core storage from scratch, saving significant time during the launch of new digital health tools.
2. Why enterprises don’t replace Epic but extend it
Replacing a core EHR is a massive financial risk. Instead of a “rip and replace” strategy, enterprises extend the system’s capabilities through custom development.
This modular approach allows businesses to keep their stable core while adding modern layers for patient engagement. It protects the original investment while allowing the technology stack to evolve alongside market demands.
3. Where custom development fits into Epic ecosystems
Custom development bridges the gap between a generic software package and specific clinical needs. While the base platform is comprehensive, it cannot cover every unique specialty workflow.
Developers create bespoke solutions like specialized telehealth interfaces or automated billing triggers. These additions help an organization differentiate itself by offering a superior experience for both providers and patients.
By using a stable core and extending it with strategic code, enterprises can innovate without compromising security. This ensures the technology remains a flexible asset for the business.
Understanding Epic EHR Architecture for Developers
Technical leaders must understand that Epic is not a single database, but a sophisticated hierarchy of data environments. For a developer, the architecture determines how quickly an application can retrieve information and how much load the system can handle.
Getting this right is the difference between a high-performing tool and one that causes system lag during peak clinical hours.
1. Core components of Epic’s system design
The system is built on a layered design that separates real-time clinical tasks from long-term data analysis. This ensures that when a doctor is entering a prescription, the system remains fast, even if a business analyst is running a massive report in the background. Key components include:
- The Database Engine: A high-performance hierarchical structure designed for speed.
- The Presentation Layer: The interface where clinicians interact with data (Hyperspace).
- The Integration Engine (Bridges): The gateway that allows external apps to communicate with the core.
- Interconnect: The web service layer that powers mobile and web-based API calls.
2. Chronicles vs Clarity vs Caboodle explained
Understanding where data lives is essential for cost-effective development. Developers must choose the right environment based on whether they need real-time updates or historical trends.
- Chronicles: This is the real-time, “live” database. It is optimized for speed and clinical workflows. If you are building an app that needs to show a patient’s current heart rate, you pull from Chronicles.
- Clarity: This is a relational (SQL) version of the data, extracted from Chronicles daily. It is used for complex reporting that would be too heavy for the live system.
- Caboodle: This is a unified data warehouse. It brings in Epic data and merges it with outside sources (like insurance claims or social data) for high-level business intelligence.
3. Data flows across clinical and operational layers
Data moves through the ecosystem in a structured loop to ensure safety and accuracy. When a clinician enters data into a patient’s chart, it is immediately indexed in Chronicles for real-time viewing. From there, the integration layer pushes this information out to connected third-party apps via APIs.
Furthermore, this data is periodically mirrored into the operational and analytical layers. This flow ensures that the business side of the enterprise has the information it needs for billing and resource planning without slowing down the clinical side.
Consequently, developers must design their “data hooks” to trigger at the right point in this flow to avoid data latency.
4. Why architecture knowledge impact scalability
Scalability in healthcare isn’t just about handling more users; it’s about handling more data complexity without failing. An application that queries the live database too frequently will eventually hit a performance ceiling. Professional developers mitigate this by:
- Optimizing Query Placement: Moving heavy data requests to Clarity instead of Chronicles.
- Using Cached Data: Reducing the number of live API calls for non-essential information.
- Asynchronous Processing: Allowing the EHR to handle clinical tasks while the app processes data in the background.
Strategic architecture knowledge allows an enterprise to grow its user base across multiple hospitals while keeping the user experience snappy. Therefore, investing in developers who understand these nuances prevents the “technical debt” that often kills large-scale digital health projects.
Navigating this architecture requires a specialized approach that respects the system’s limits while pushing its capabilities. When built correctly, these integrations become a seamless part of the enterprise’s digital strategy.
Epic Interoperability Features Developers Must Know
Interoperability is the digital nervous system of a modern healthcare enterprise. For developers, Epic provides a sophisticated toolkit that allows external applications to communicate with the central electronic health record.
Understanding these features is essential for building solutions that sync patient data seamlessly without creating manual work for clinicians.
1. FHIR APIs in Epic: capabilities and limits
Fast Healthcare Interoperability Resources (FHIR) are the modern standard for exchanging health data. Epic’s FHIR APIs allow developers to read and write information, such as medications and lab results, using standard web technologies.
This accessibility makes it simpler to build mobile apps that feel like a natural extension of the patient’s chart. However, developers cannot access every proprietary data point via FHIR, as some complex elements remain restricted.
2. HL7 interfaces for legacy system integration
Many hospital operations still rely on HL7 v2 messaging for event-driven data. These interfaces function as a continuous stream triggered by specific events, such as a patient admission or a filed lab result.
Developers use HL7 to ensure that older software, like billing systems, stays in sync with the main EHR. Because it is an older standard, it requires expert knowledge to map data segments correctly for backend reliability.
3. SMART on FHIR apps within Epic workflows
SMART on FHIR allows developers to “embed” their application directly inside the Epic user interface. This means a doctor can open a specialized tool without ever leaving the patient’s record. It provides a seamless experience that reduces “app fatigue” through:
- Single Sign-On (SSO): Users skip separate logins for the app.
- Context Awareness: The app automatically identifies the active patient.
- UI Integration: Apps appear as native tabs within the EHR.
4. Real-time vs batch data exchange in Epic
Choosing between real-time and batch processing is a critical business decision. Real-time exchange is necessary for clinical alerts where seconds matter, relying on webhooks for instant updates.
In contrast, batch data exchange is better for non-urgent tasks like population health analytics. Moving large volumes during off-peak hours avoids slowing down the system for active doctors.
Mastering these tools ensures your custom software is an integrated part of the larger clinical ecosystem. This connectivity drives enterprise value and improves patient outcomes.
Key Epic EHR Features That Enable Custom Development
Strategic development within the Epic ecosystem requires leveraging specific entry points designed for external innovation. These features act as the “hooks” that allow third-party applications to become a native part of the clinical experience.
1. Open.epic and developer access ecosystem
Open.epic serves as the primary gateway for developers to explore technical capabilities without heavy initial investment. This public resource provides the documentation and sandboxes necessary to understand how to move data safely.
It lowers the barrier to entry by offering standardized specifications for FHIR and other integration methods. For an enterprise, this means technical teams can prototype and validate ideas in a controlled environment before committing to full-scale implementation.
2. App Orchard: building and listing integrations
The App Orchard, now the Connection Hub, is the formal marketplace for developers looking to scale solutions across multiple health systems.
This ecosystem provides advanced support, including deeper API access and official validation of security and performance. Joining this program allows an enterprise to:
- Gain Visibility: List products in a directory seen by global clinical leaders.
- Access Premium APIs: Use specialized data points not available in public tiers.
- Ensure Compliance: Benefit from rigorous reviews to build trust with hospital CIOs.
3. Embedded apps inside clinician workflows
Successful custom developments are those that do not require clinicians to change their daily behavior. Using SMART on FHIR, developers can place tools directly into the “Hyperspace” interface as a native tab.
This allows a specialist to view a custom risk-scoring dashboard or a specialized imaging viewer without ever leaving the patient’s chart. Embedding eliminates the friction of switching windows, which is a major factor in reducing burnout.
4. Event-driven triggers and automation support
Modern healthcare requires software that reacts in real-time to changing patient conditions through event-driven triggers. Epic supports triggers, such as a lab result being filed, to initiate automated workflows in external applications.
For example, an automation could trigger a home-care follow-up the moment a patient is discharged. This capability transforms the EHR into an active engine that drives operational efficiency and proactive patient care across the enterprise.
Clinical Workflow Features Developers Can Extend
Custom development allows enterprises to transform standard documentation tools into high-performance clinical assets. By extending these native features, developers can tailor the EHR to meet specific specialty needs and operational goals.
1. Smart forms, templates, and documentation tools
Smart forms and templates are the primary interface for clinical data entry. Developers can extend these by building dynamic components that pull real-time data from external sources, such as specialized medical devices or remote monitoring apps.
This automation reduces the manual burden on clinicians, ensuring that documentation is both accurate and comprehensive. For an enterprise, this results in cleaner data for billing and more consistent patient records across different care settings.
2. Clinical decision support customization
Clinical Decision Support (CDS) systems provide real-time guidance to doctors at the point of care. Developers can customize these systems by integrating proprietary algorithms or AI models that trigger specific alerts based on a patient’s unique profile.
For example, a custom CDS tool could flag potential drug interactions or suggest advanced screenings for high-risk patients. These enhancements help organizations standardize high-quality care and reduce the likelihood of costly medical errors.
3. Order sets and care pathway automation
Order sets and care pathways define the standardized steps for treating specific conditions. Developers can automate these pathways by creating “smart” triggers that suggest the next logical step in a treatment plan based on a patient’s progress.
This ensures that clinical teams follow evidence-based protocols while allowing for flexibility in complex cases. Automation in this area significantly increases hospital throughput and improves the predictability of patient outcomes.
4. Reducing clinician friction through UX layers
One of the most valuable extensions a developer can build is a simplified user experience (UX) layer. By creating custom dashboards that aggregate the most relevant data for a specific specialty, developers can eliminate “click fatigue.”
These layers allow clinicians to find critical information, like recent vitals or pending labs, in a single view. Reducing this friction directly impacts provider satisfaction and allows them to spend more time with patients rather than the software.
Strategic extensions of clinical workflows turn the EHR into a proactive tool for care delivery. These technical enhancements drive both clinical excellence and long-term operational sustainability for the enterprise.
Revenue Cycle Features Developers Integrate With
Integrating financial workflows with clinical data is the key to maintaining a healthy enterprise bottom line. Developers can automate the complex exchange of information between payers and providers, reducing the time it takes to get paid.
1. Claims management and billing workflows
Efficient claims management requires a seamless connection between the clinical record and the billing office. Developers build custom interfaces that automatically scrub data for errors before a claim is even submitted to a payer.
This real-time validation prevents common mistakes that lead to denials, such as missing diagnostic codes or incorrect patient identifiers. For an enterprise, this means a faster revenue cycle and less manual labor spent on fixing old billing entries.
2. Coding automation and payer integrations
The transition from clinical notes to billable codes is often a bottleneck in hospital operations. Developers can extend Epic’s native capabilities by integrating AI-driven coding engines that suggest the most accurate ICD-10 or CPT codes based on physician documentation.
These integrations can also connect directly to payer portals to check coverage limits in real-time. This automation ensures that the organization captures the full value of the services provided while maintaining strict compliance.
3. Prior authorization workflows in Epic
Prior authorization is one of the most significant administrative burdens in modern healthcare. Developers can build automated “checkpoints” within the EHR that identify when a procedure requires insurance approval and automatically pull the necessary clinical proof.
By digitizing this exchange, an enterprise can reduce treatment delays and improve the patient experience. This technical bridge between the hospital and the insurance company turns a manual, multi-day process into a near-instant digital transaction.
4. Connecting financial data with clinical systems
True business intelligence comes from seeing the relationship between clinical outcomes and financial performance. Developers create unified data layers that allow executives to see which departments are most efficient and where resource waste is occurring.
By mapping the cost of care directly to the patient’s recovery timeline, leaders can make data-driven decisions about future investments. This level of transparency is essential for moving toward value-based care models where quality is tied to reimbursement.
Strategic financial integrations transform the EHR from a simple ledger into a sophisticated engine for growth. These technical solutions ensure that the business remains profitable while delivering high-quality care.
Security and Compliance Features in Epic EHR
Protecting patient data is a non-negotiable requirement for any enterprise-grade healthcare application.
For developers, Epic provides a rigorous security framework that ensures every data interaction meets federal regulations while maintaining system integrity.
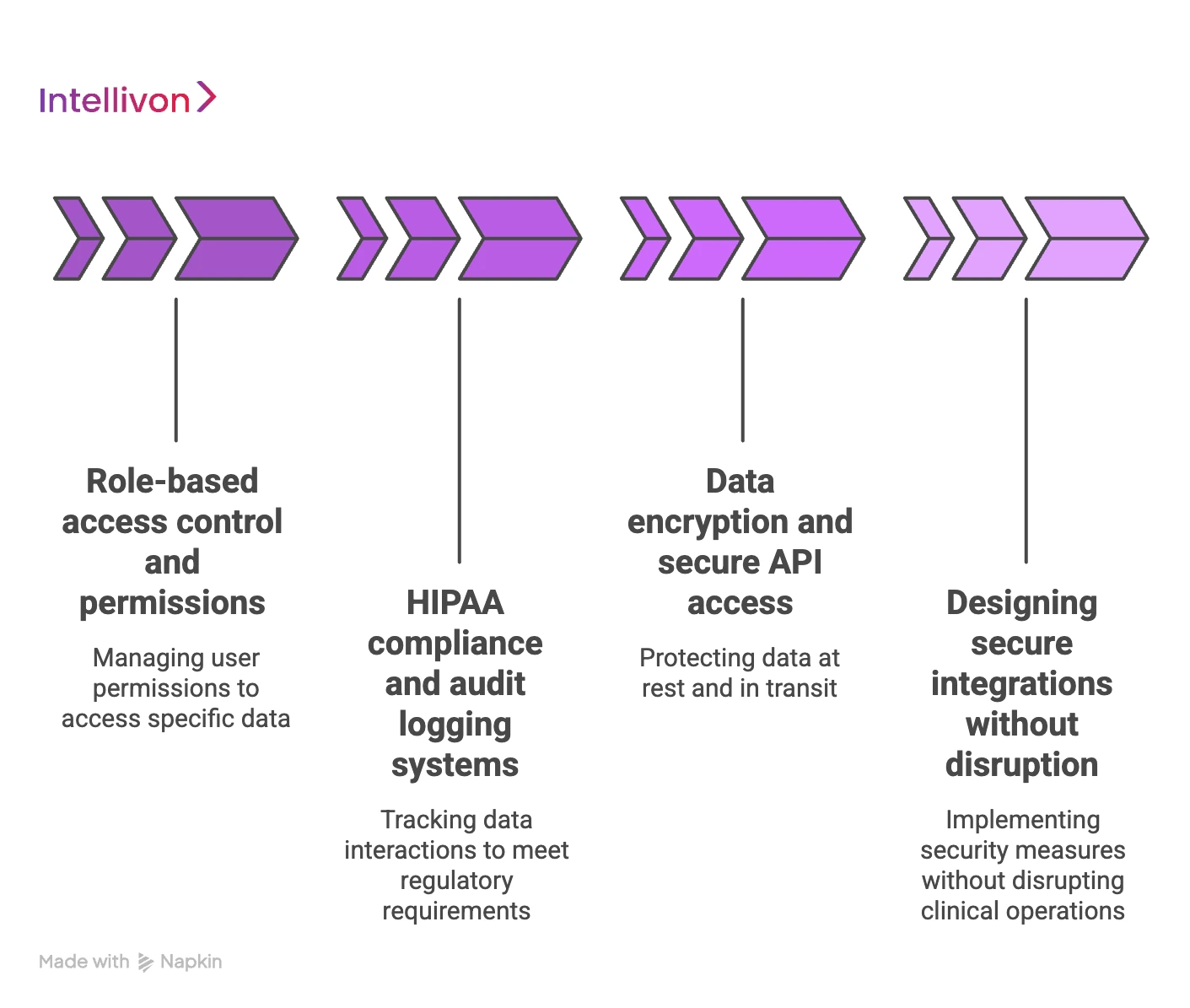
1. Role-based access control and permissions
Managing who can see specific patient data is the first line of defense in healthcare security. Developers work within Epic’s “Security Classes” to ensure that an application only accesses the information necessary for a user’s specific job function.
For example, a billing clerk using a custom app should not be able to view sensitive mental health notes. By mapping custom app permissions to these native roles, an enterprise can prevent internal data leaks and ensure that staff only interact with relevant clinical records.
2. HIPAA compliance and audit logging systems
Every interaction with a patient’s electronic record must be tracked to meet HIPAA requirements. Epic’s internal audit engines, such as “Chronicles Data Audit,” automatically log every time a user views, edits, or deletes a piece of information.
Developers must ensure their external integrations pass these audit signals back to the core system. This transparency is vital during a regulatory audit, as it provides a complete, undeniable trail of how data moved between the EHR and the third-party tool.
3. Data encryption and secure API access
Data must be protected both while it sits in the database and while it travels across the network. Epic uses industry-standard encryption (AES-256) for data at rest and TLS for data in transit through its Interconnect web services.
Developers must use OAuth 2.0 for secure API authentication, ensuring that only authorized applications can request patient records. This multi-layered approach to encryption prevents “man-in-the-middle” attacks and keeps the organization’s most sensitive digital assets safe from external threats.
4. Designing secure integrations without disruption
Security should never come at the expense of clinical speed or system uptime. Developers achieve this balance by using “non-persistent” data strategies, where sensitive information is processed in memory rather than being stored on external servers.
This reduces the “attack surface” of the new application and simplifies the compliance burden for the IT department. By building “security-first” integrations, an enterprise can innovate rapidly without risking the massive fines or reputational damage associated with a data breach.
Robust security features turn the EHR into a fortress that protects both the patient and the business. These technical safeguards provide the confidence needed to scale digital health solutions across a global enterprise.
Data Analytics and Reporting Capabilities in Epic
Transforming raw clinical data into actionable business intelligence is a core requirement for modern healthcare leadership. For developers, Epic provides a multi-tiered reporting environment that separates real-time operational needs from long-term strategic analysis.
1. Using Clarity for enterprise reporting
Clarity is a relational database that receives a daily extract of clinical data from the live Chronicles system. Developers use it to build complex, high-volume reports that would otherwise slow down the performance of the active EHR.
By writing SQL-based queries against Clarity, an enterprise can analyze long-term trends in patient outcomes or financial performance. This allows decision-makers to identify inefficiencies in specific departments and adjust staffing or resource allocation based on verified historical data.
2. Caboodle for data warehousing and BI
Caboodle acts as the unified data warehouse for the entire enterprise, bringing together Epic data and external sources. Developers use this platform to merge clinical records with financial claims, social determinants of health, and even third-party research databases.
This consolidation provides a “360-degree view” of the organization’s performance that is essential for participating in value-based care contracts. Consequently, Caboodle serves as the foundation for sophisticated business intelligence tools that drive high-level strategic planning and investment.
3. Real-time dashboards for operational insights
Operational leaders need to know what is happening in their facilities right now, not what happened yesterday. Developers build real-time dashboards using “Radar” and “Reporting Workbench” to display live metrics like emergency room wait times or current bed capacity.
These tools pull data directly from the transactional layer, allowing managers to intervene the moment a bottleneck occurs. This immediate visibility is what allows a high-volume hospital to maintain flow and safety during peak periods of patient activity.
4. Predictive analytics integration opportunities
The most advanced enterprises are moving from descriptive reporting to predictive modeling. Developers can integrate custom machine learning models into the Epic workflow to predict patient risks, such as the likelihood of sepsis or a 30-day readmission.
By surfacing these scores directly within the clinician’s view, the system moves from being a passive record-keeper to a proactive clinical partner. These integration opportunities allow an organization to stay ahead of clinical crises and significantly reduce the overall cost of care.
Data analytics features turn a vast ocean of clinical information into a precise map for business growth. These technical capabilities ensure that every strategic decision is backed by the full weight of the organization’s data.
Limitations of Epic for Custom Development
Acknowledging the technical boundaries of the Epic environment is vital for realistic project scoping and resource allocation. For developers, navigating these constraints is as important as mastering the features, as it prevents costly pivots mid-build.
1. Closed ecosystem challenges for developers
Epic is fundamentally a proprietary system, which creates a “walled garden” effect for outside engineering teams. Unlike open-source platforms, developers cannot modify the core codebase or access underlying database schemas without strict oversight from the vendor.
This lack of direct control means that certain deep-level optimizations or UI overhauls are simply not possible for third-party tools. For an enterprise, this requires a shift in strategy from “building inside” to “building alongside” the EHR to achieve true flexibility.
2. API limitations and approval dependencies
While FHIR has opened many doors, the breadth of available APIs is still curated by Epic’s internal product roadmap. Developers often find that specific clinical data points or specialized financial fields are not yet exposed through standard web services.
Furthermore, moving an application from a local sandbox to a live production environment requires a multi-stage approval process through the Connection Hub. This dependency on vendor timelines can introduce delays in the development lifecycle, requiring leaders to plan for longer integration phases.
3. Performance constraints in large deployments
Scaling an integrated application across dozens of hospitals introduces a significant load on the Interconnect web service layer. If a custom app makes too many high-frequency API calls, it can trigger rate-limiting protocols designed to protect the EHR’s core stability.
Developers must spend considerable time optimizing “chatty” applications to ensure they do not cause latency for doctors during peak hours. Failure to manage these performance thresholds can lead to a degraded user experience or, in extreme cases, temporary suspension of the app’s access.
4. Why external platforms are often required
To bypass these native limitations, many enterprises choose to build the “heavy lifting” components on external cloud platforms like AWS or Azure. By hosting proprietary algorithms and large-scale data processing outside of the EHR, developers can use modern DevOps tools that are not available within Epic.
The EHR then serves as the secure “viewer” or data source, while the external platform provides the computational power. This hybrid architecture allows for greater innovation while maintaining the necessary clinical connection to the patient record.
Understanding these limitations allows an enterprise to build more resilient and scalable technology stacks. By planning for these technical hurdles early, leaders can ensure their digital health investments deliver long-term value without hitting a ceiling.
When to Build on Epic vs Build Around Epic
Choosing the right development path is a high-stakes decision that dictates both your speed to market and long-term maintenance costs. For an enterprise, the choice depends on whether a feature needs to live inside the clinician’s existing workflow or requires specialized computing power.
1. Use cases for embedded Epic development
Embedded development is the gold standard for tools that require high clinician adoption and immediate patient context. Features like clinical calculators, risk-scoring alerts, and specialized documentation forms perform best when they are native to the Hyperspace interface.
By building “on” Epic using SMART on FHIR, developers eliminate the need for users to manage multiple logins or manually search for patients. This seamless integration is essential for any tool used during a live patient encounter where every second of provider attention is critical.
2. When external platforms make more sense
External platforms are the logical choice for data-heavy applications that involve complex AI modeling or large-scale consumer engagement. If your solution requires processing terabytes of imaging data or managing millions of patient-generated health records from wearables, the EHR is not the right hosting environment.
Building “around” Epic on a cloud provider like AWS or Google Cloud allows developers to use modern database technologies and elastic scaling. This approach keeps the EHR “lean” and prevents the custom app from competing for core system resources.
3. Hybrid architecture for enterprise scalability
A hybrid architecture offers the best of both worlds by combining a secure clinical “viewer” with a powerful external “engine.” In this model, the user interface lives inside Epic as an embedded app, but the heavy data processing and proprietary logic happen on a separate, high-performance server.
This separation of concerns allows an enterprise to update its proprietary algorithms weekly without needing to go through a full EHR change-control cycle. Consequently, the hybrid model is the preferred strategy for scaling advanced digital health platforms across multiple global regions.
Selecting the right architecture is the foundation of a successful healthcare technology strategy. This decision ensures that your investment remains agile enough to adapt to future clinical and business needs.
How Intellivon Extends Epic Beyond Native Limits
Enterprises often hit a performance or feature ceiling when relying solely on out-of-the-box electronic health record tools.
Intellivon bridges this gap by engineering sophisticated middleware and AI layers that transform a static record system into a dynamic growth engine.
1. API-first platforms built around Epic systems
Intellivon specializes in building decoupled, API-first architectures that interact with the Epic Connection Hub without being restricted by its native UI. By treating the EHR as a secure data vault rather than a rigid cage, we allow organizations to:
- Deploy High-Frequency Apps: Build consumer-facing portals that handle millions of requests without hitting EHR rate limits.
- Modernize Tech Stacks: Use React or Flutter for the front-end while maintaining a secure FHIR-based back-end.
- Rapid Prototyping: Launch new clinical features in weeks by hosting complex logic on external cloud environments.
2. Creating unified clinical + operational layers
True enterprise efficiency requires a “single pane of glass” that merges patient health data with real-time business metrics. Our engineers create unified data fabrics that pull clinical insights from Chronicles and financial trends from Clarity into a high-performance executive dashboard.
This integration allows leadership to see the direct financial impact of clinical protocols in real-time. Consequently, the organization moves from fragmented reporting to a centralized command center that drives both patient safety and institutional profitability.
3. AI-driven workflows on top of Epic data
While the base EHR provides basic alerts, our system implements advanced AI orchestration to predict and prevent clinical crises before they occur.
Our teams integrate proprietary machine learning models, such as predictive sepsis monitors or automated discharge planners, directly into the clinician’s workflow via CDS Hooks.
This technical layer processes vast amounts of historical data to provide “next-best-action” recommendations that are far more nuanced than native templates. These AI-driven workflows turn data gravity into a competitive advantage for high-volume medical centers.
4. Seamless integration without system disruption
The primary concern for any CIO is maintaining system uptime during the rollout of new technology. Intellivon utilizes a “Sidecar” deployment strategy that ensures our custom tools run parallel to the core EHR without affecting its stability.
We use non-persistent data processing and asynchronous API calls to keep the Hyperspace environment fast and responsive for frontline staff. This approach guarantees that innovation never comes at the cost of clinical performance or system reliability.
By pushing the boundaries of what is possible within the EHR ecosystem, Intellivon empowers healthcare leaders to innovate without technical compromise. Our solutions ensure your digital infrastructure evolves as fast as your business goals.
Conclusion
Modernizing your clinical infrastructure requires a balance between a stable core and agile, custom extensions. By strategically building on and around Epic, your enterprise can unlock new revenue streams and operational efficiencies without risking system stability.
Intellivon provides the cutting-edge, enterprise-grade AI solutions and technical expertise needed to transform your EHR into a high-performance growth engine. Contact us today to build the future of integrated healthcare.
Build Epic-Integrated Platforms With Intellivon
At Intellivon, Epic-integrated platforms are built as an enterprise healthcare infrastructure, not add-ons. The focus is to unify Epic data with operational workflows, enabling scalable, real-time care across systems.
Each platform works alongside Epic without disrupting its core. This includes FHIR and HL7 integrations, workflow automation, external app layers, AI-driven decision support, and real-time synchronization.
Our approach combines API-first, cloud-native architecture with interoperability standards. As a result, organizations extend Epic seamlessly across clinical, financial, and operational systems while maintaining compliance and performance.
Why Intellivon for Epic-Integrated Platforms?
- Build Around Epic, Not Against It: Extend capabilities without modifying Epic’s core. This reduces risk, avoids vendor lock-in issues, and ensures long-term upgrade compatibility.
- Deep FHIR and HL7 Expertise: Accelerate integration with proven interoperability frameworks. We design reliable data exchange across EHRs, labs, payers, and third-party healthcare systems.
- AI-Driven Clinical and Operational Workflows: Layer intelligent automation on top of Epic data. Enable faster decision-making, reduce manual effort, and improve care coordination across departments.
- Enterprise-Grade Scalability and Performance: Platforms are built to support multi-hospital systems, high patient volumes, and complex workflows without compromising speed, reliability, or data consistency.
If you’re planning to extend Epic with custom workflows, analytics, or patient-facing applications, Intellivon can help you design and deploy a scalable, future-ready platform.
FAQs
Q1. What APIs does Epic provide for developers?
A1. Epic provides APIs primarily through its FHIR-based ecosystem via App Orchard. These APIs allow developers to access patient data, scheduling, clinical records, and workflows. In addition, Epic supports HL7 interfaces for legacy integrations. However, access is controlled and requires approval, which means development must align with Epic’s governance and interoperability standards.
Q2. Can developers fully customize Epic EHR?
A2. No, Epic cannot be fully customized at the core level. Developers can extend functionality through APIs, SMART on FHIR apps, and external platforms. As a result, most enterprise teams build around Epic rather than modifying it directly. This approach ensures system stability while still enabling advanced workflows and integrations.
Q3. How long does Epic integration take?
A3. Epic integration timelines typically range from 3 to 9 months, depending on complexity. Simple FHIR-based integrations can be completed faster, while HL7 interfaces and multi-system integrations take longer. In addition, approval processes, testing cycles, and compliance requirements can extend timelines in enterprise environments.
Q4. What are Epic’s biggest development limits?
A4. Epic’s biggest limitations include restricted API access, approval dependencies, and limited flexibility within its core system. Developers often face constraints when trying to implement custom workflows or real-time data processing. Therefore, many enterprises build external platforms to overcome these limitations while still leveraging Epic’s core capabilities.
Q5. How much does Epic-based development cost?
A5. Epic-based development typically ranges from $50,000 to $300,000+, depending on scope. Costs vary based on integration complexity, number of systems involved, compliance requirements, and custom feature development. Enterprise-grade platforms with AI, analytics, and multi-system integrations fall on the higher end of the range.