Key Takeaways:
-
AI reduces workload through urgent triage, normal case filtering, automated measurements, and draft report generation.
-
Evidence shows AI cut mammography workload by 44 percent and PE reporting time by 22 minutes at scale.
-
AI tools fail when they create separate dashboards, trigger alert fatigue, or disconnect from PACS and RIS.
-
Fastest gains come from chest X-ray automation, stroke triage, PE detection, and oncology follow-up reporting.
-
How Intellivon builds AI radiology systems your enterprise fully owns, with PACS integration and reporting automation from day one.
Radiology teams today handle more than just scan volume. Complex cases, urgent reporting queues, fragmented patient histories, repetitive measurements, and an increasing administrative load have stretched reporting timelines. This directly impacts care delivery and hospital throughput.
Reporting time is not only a concern for radiologists. It influences emergency response, bed allocation, surgical scheduling, and treatment decisions. When reports are delayed, the entire care process slows down. AI can lessen the radiologist’s workload by removing friction throughout the reporting cycle, not just during image interpretation.
It helps prioritize urgent studies, summarize clinical history, prefill structured reports, automate measurements, flag potential missed findings, and push results back into PACS, RIS, and EHR systems. These actions lead to real-time savings.
However, this only works when AI is integrated into actual radiology operations. An algorithm that sits outside the workflow provides little benefit. Intellivon designs AI radiology systems focused on measurable time savings, creating each part based on how radiologists work in reality, not how vendors think they work. This blog explains how we build such platforms from the ground up.
Why the Radiologist Workload Is Increasing
Imaging demand is growing faster than the radiology workforce can keep pace with. Demographic shifts, rising chronic disease prevalence, and expanding diagnostic protocols have collectively pushed scan volumes to levels that existing staffing models were never designed to handle. As a result, top-performing radiologists are absorbing a disproportionate share of the increase, which accelerates burnout and strains the economics of running a radiology department at scale.
Market analyses consistently project that this shortage will persist. The gap, therefore, is not a temporary staffing problem. It is a structural pressure that health systems need to plan around, not wait out.
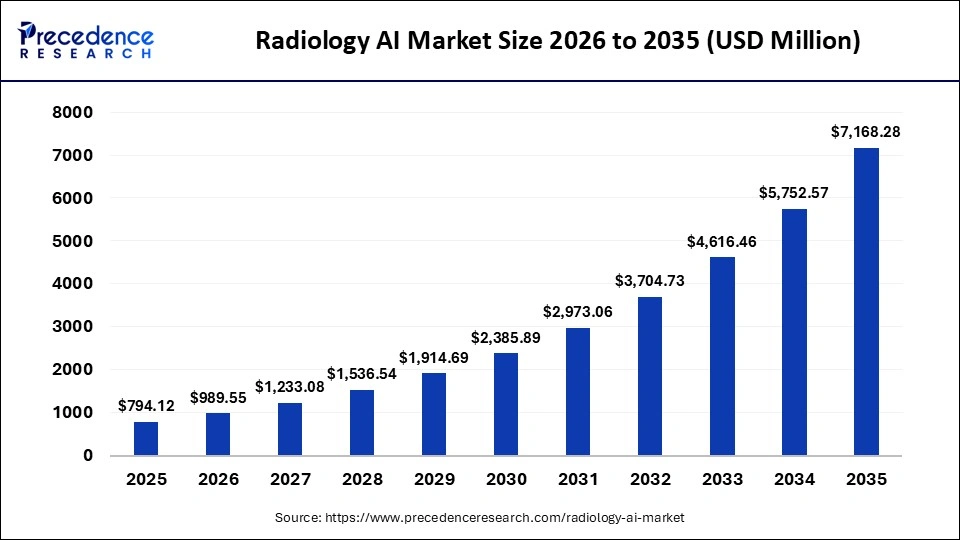
The global radiology AI market is projected to grow from USD 989.55 million in 2026 to approximately USD 7,168.28 million by 2035, expanding at a CAGR of 24.61%. That trajectory reflects how seriously health systems are now investing in AI as core radiology infrastructure, not a peripheral tool.
Radiology departments are not simply busier. Instead, they are structurally overwhelmed, and the gap keeps widening.
1. Imaging Volumes Are Rising Faster Than Capacity
Aging populations require more frequent scans. Chronic conditions like diabetes, cardiovascular disease, and cancer demand ongoing imaging to monitor progression.
Advanced modalities such as CT and MRI are now standard across more clinical pathways, and follow-up imaging has become routine rather than an exception.
Furthermore, emergency imaging volumes have climbed steadily across most health systems. The workforce, however, has not grown at the same pace, and that imbalance is what makes this a capacity crisis rather than a temporary surge.
2. Radiologists Handle More Than Image Reading
Reading images is only one part of the job. Before opening a scan, radiologists review clinical history, compare prior studies, and assess referral context. During interpretation, they take measurements and evaluate findings across multiple sequences.
After reading, they draft structured reports, communicate critical results, and respond to queries from referring physicians. As a result, the time each case actually demands extends well beyond interpretation alone.
3. Reporting Delays Affect Hospital Flow
When reports are delayed, the impact moves across the entire care chain. Emergency department decisions stall, inpatient discharges slow, and surgical planning gets pushed back.
In addition, oncology teams cannot finalize treatment decisions without confirmed findings. Consequently, patients wait longer, beds stay occupied, and hospital throughput takes a measurable hit.
4. Burnout Is A Workflow Problem
Repetitive reads, constant interruptions, after-hours reporting pressure, and manual documentation compound over time. Fragmented systems, moreover, force radiologists to toggle between PACS, RIS, and EHR platforms just to piece together patient context.
That cognitive load, sustained across a full shift, therefore accelerates fatigue far faster than volume alone ever would.
This is not a staffing problem hospitals can hire their way out of. It is a workflow problem, and AI is increasingly the most viable path to solving it.
How AI Reduces Radiologist Workload
AI reduces radiologist workload by automating repetitive tasks, prioritizing urgent studies, summarizing clinical context, assisting with measurements, and reducing reporting friction.
Modern radiology departments face a widening gap between imaging volume and available specialist hours.
By integrating an AI radiology workflow, enterprises can shift the burden of manual data processing to intelligent algorithms, allowing the clinical team to focus on high-level diagnostic synthesis.
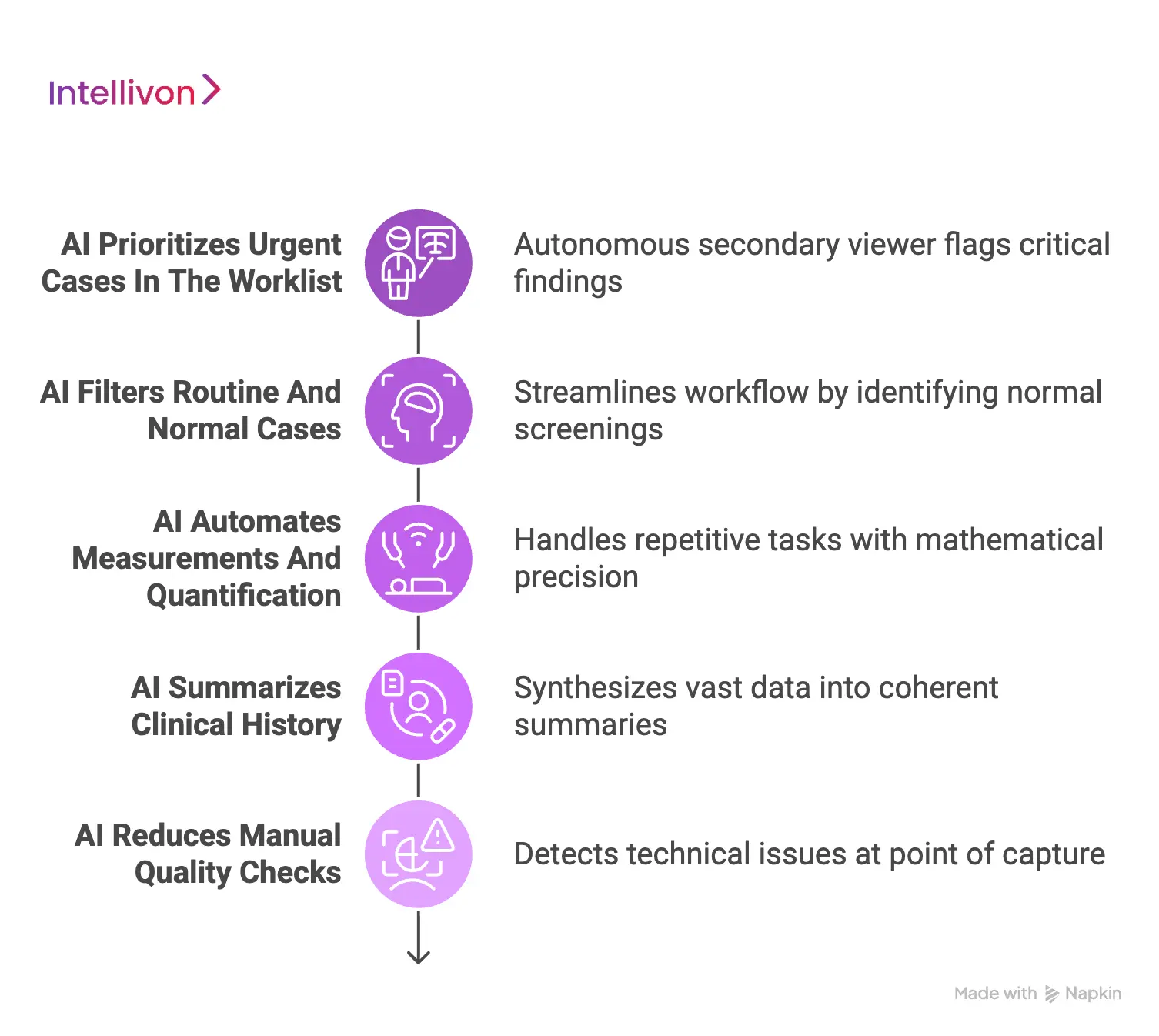
1. AI Prioritizes Urgent Cases In The Worklist
Traditional worklists operate on a first-come, first-served basis, which can leave life-threatening pathologies buried under routine screenings.
AI triage tools act as an autonomous secondary viewer that flags critical findings the moment a scan is completed.
- Acute Detection: Algorithms target stroke, pulmonary embolism, intracranial hemorrhage, and pneumothorax with high precision.
- Dynamic Escalation: Software identifies trauma cases or critical chest findings and instantly moves these studies to the top of the reporting queue.
- Time Savings: A JACR study on pulmonary embolism found that AI deployment led to significant work-hour turnaround-time savings by flagging high-risk studies early.
2. AI Filters Routine And Normal Cases
A significant portion of daily volume involves routine screenings that show no pathology.
AI helps clear the “noise” so that human expertise is directed where it is most needed.
- Screening Prioritization: AI identifies normal chest X-rays and low-urgency cases to streamline the workflow.
- Risk-Based Focus: This filtering does not replace the final sign-off but ensures radiologists spend more time on complex, high-risk cases.
- Negative Findings: By flagging clear negative findings, the system reduces the cognitive fatigue associated with reviewing hundreds of identical routine scans.
3. AI Automates Measurements And Quantification
Manual measurement of lesions and tumors is one of the most time-consuming aspects of radiology.
AI handles these repetitive tasks with mathematical precision, ensuring consistency across longitudinal studies.
- Clinical Accuracy: Software automates lesion measurement, tumor size comparison, and nodule tracking.
- Advanced Segmentation: AI provides organ segmentation and stroke volume scoring that would take a human several minutes to calculate manually.
- Consistency: Automated quantification reduces inter-observer variability, which is critical for tracking oncology patient progress over time.
4. AI Summarizes Clinical History
Reviewing fragmented patient histories is essential for context, but creates a massive administrative drain. AI tools can synthesize vast amounts of data into a coherent summary for the radiologist.
- EHR Extraction: Systems pull relevant lab values and prior diagnoses directly from the Electronic Health Record.
- Longitudinal Context: AI summarizes previous imaging context and highlights significant changes since the last scan.
- Efficiency Gains: Nature identifies clinical history summarization as a primary time-saving opportunity, removing the need for manual record digging.
5. AI Reduces Manual Quality Checks
Suboptimal image quality often leads to rejected studies and wasted modality time. AI can detect technical issues at the point of capture before the patient even leaves the facility.
- Artifact Detection: Algorithms identify motion artifacts or incorrect positioning in real-time.
- Technical Compliance: The system flags low-quality images or contrast timing issues immediately.
- Cost Avoidance: Nature notes that catching these errors early prevents expensive repeat scans and reduces frustration for both patients and clinicians.
The integration of these tools transforms the radiology department from a cost center into a proactive driver of hospital growth. This efficiency allows for higher patient volumes while maintaining the highest standards of diagnostic accuracy.
How AI Reduces Radiology Reporting Time
AI reduces radiology reporting time by generating draft reports, pre-filling structured templates, standardizing findings, and reducing repetitive documentation.
While workload reduction focuses on the queue, reporting efficiency targets the final bottleneck: the dictation and documentation phase.
By integrating intelligent automation into the reporting interface, enterprises can significantly accelerate the transition from image interpretation to a finalized clinical result.
1. AI Generates Draft Reports For Review
The transition from a blank screen to a finished report is often the most time-consuming part of a radiologist’s day. AI assists by providing a sophisticated starting point that the specialist simply needs to verify and refine.
- Impression Suggestions: Algorithms analyze the pixels and suggest high-level findings for the radiologist to approve.
- Modality-Specific Templates: The system automatically selects the correct reporting structure based on whether it is a CT, MRI, or X-ray.
- Radiologist-Controlled Editing: The human remains the final authority, utilizing the AI draft as a high-quality foundation rather than a finished product.
- Evidence of Impact: A pilot study using simulated AI draft reports demonstrated that assisted reporting reduced average time from 573 seconds to 435 seconds. While this represents promising evidence, it highlights a clear trend toward significant time savings.
2. AI Prefills Structured Reporting Templates
Structured reporting is the gold standard for clinical clarity, but manual entry into these templates can be tedious. AI eliminates this friction by populating findings directly into the required fields.
- Auto-Filled Sections: Data from the image analysis, such as lesion measurements, is pushed directly into the template.
- Standardized Language: The system ensures that descriptions follow recognized medical lexicons, reducing the need for manual wording adjustments.
- Performance Benchmarks: A 2026 Radiology study showed that chest radiograph reporting dropped from 88 seconds for free-text to just 25 seconds when using AI-prefilled structured reporting.
- Efficiency Gains: This dramatic reduction in time per study allows for significantly higher departmental throughput without increasing physician stress.
3. AI Reduces Repetitive Dictation
Much of a radiologist’s vocal effort is spent on “normal” findings and standard follow-up language that varies little between patients. AI identifies these patterns and automates the boilerplate content.
- Recurrent Phrasing: The software recognizes standard impressions and comparison statements, pre-loading them into the report.
- Normal Findings: For negative studies, AI can prepopulate the entire report, leaving only a quick verification for the specialist.
- Comparison Support: Automated statements regarding how a current scan relates to previous imaging reduce the need for manual cross-referencing and dictation.
4. AI Improves Report Consistency
Variability in reporting can lead to confusion among referring physicians and delays in treatment. AI acts as a leveling force that ensures every report meets a specific enterprise standard.
- Standard Terminology: By enforcing consistent language, AI improves the quality of communication with downstream clinical teams.
- Reduced Variation: Whether a study is read at 8:00 AM or 8:00 PM, the structured impressions remain uniform and professional.
- Data Integrity: Cleaner, standardized reports create better downstream data for hospital analytics and future research initiatives.
5. AI Flags Missing Report Details
Incomplete reports lead to administrative back-and-forth and potential liability. AI monitors the report in real-time to ensure every critical detail is present before it is signed.
- Completeness Checks: The system flags missing laterality (left vs. right), size measurements, or severity scores.
- Critical Result Language: AI ensures that life-threatening findings are described using the specific terminology required for hospital alerts.
- Follow-Up Gaps: If a finding typically requires a 6-month follow-up, the system prompts the radiologist to include that specific recommendation.
Reporting time improves when AI reduces documentation friction rather than trying to replace radiologist judgment. This technical synergy allows for a faster, more reliable diagnostic cycle that benefits the entire healthcare ecosystem.
Real Proof That AI Can Reduce Workload And Time
Real-world evidence shows AI can reduce radiologist workload and reporting time when deployed through triage, screening, and reporting workflows.
Abstract promises of efficiency mean little to an enterprise without empirical data to back them up. Fortunately, recent clinical trials and large-scale deployments have provided the hard metrics necessary to prove that AI is a tangible asset for modern radiology.
These results demonstrate that when the right technology meets a specific clinical pressure point, the gains in productivity and safety are undeniable.
1. MASAI Trial Reduced Mammography Reading Workload
The MASAI (Mammography Screening with Artificial Intelligence) trial stands as one of the most robust pieces of evidence for AI-driven efficiency. This randomized controlled trial enrolled over 80,000 women to compare AI-supported screening against the traditional double-reading standard.
The results were a landmark for the industry, proving that AI can handle massive volumes without compromising clinical integrity.
- Workload Reduction: The study found that AI-supported mammography screening reduced the screen-reading workload by a staggering 44.3%.
- Safety Profile: The trial reported similar cancer detection rates compared to standard double reading, with no increase in the false-positive rate.
- Scalability: This proves AI can manage high-volume screening triage at scale, allowing human readers to focus on complex cases.
- Strategic Impact: For an investor, this represents a near-halving of the labor required for one of the most common imaging procedures in healthcare.
2. AI Triage Reduced PE Reporting Time During Work Hours
Urgent workflows present a different challenge: it is not just about volume, but the speed of intervention. A comprehensive study published in the Journal of the American College of
Radiology (JACR) analyzed 11,252 CT pulmonary angiography exams to measure how AI impacts the clock during critical episodes. The data highlighted a specific “sweet spot” where AI provides the highest return on investment.
- Work-Hour Efficiency: Report turnaround time for PE-positive cases dropped from 68.9 minutes to 46.7 minutes after AI implementation.
- Measured Savings: The observed savings of 22.2 minutes per critical case provide a significant buffer for emergency departments.
- Contextual Performance: Interestingly, off-hour savings were not statistically significant, suggesting that AI delivers the most value when the system is under peak pressure.
- Pressure Point Relief: This shows that AI works best when it aligns with the highest-volume periods of the day, effectively smoothing out the “rush hour” of the radiology department.
3. ARA Health Reported 20% Lower Reporting Time
While clinical trials provide controlled data, enterprise-level case studies show how these tools perform in the messy reality of private practice. ARA Health Specialists, a massive group serving 13 hospitals and 30 outpatient centers, recently transitioned to advanced AI reporting tools.
Their experience reading nearly 100,000 studies per month offers a blueprint for large-scale digital transformation.
- Median Gains: The group reported a 20% median reduction in reporting time across their entire diagnostic staff.
- High-Performer Impact: The data was even more impressive for top-decile radiologists, who achieved reporting speeds approximately 60% faster than their previous baseline.
- Widespread Adoption: Efficiency improved for 79% of the radiologists in the group, indicating that the technology is intuitive enough for broad clinical use.
- Operational Scale: When a group processes six-figure volumes monthly, a 20% time saving translates into thousands of hours of recovered capacity every year.
4. Failed AI Deployments Prove Integration Matters
To build real trust with decision-makers, we must acknowledge that AI is not a “plug-and-play” magic wand. A prospective single-center study reported by Radiology
Business found that a specific commercial AI triage tool failed to improve turnaround times for intracranial hemorrhage cases. In fact, the positive-exam turnaround time was slightly higher with the AI tool in place.
- The Integration Gap: This failure highlights that software alone is not the solution; the friction often lies in how the tool talks to existing PACS and RIS systems.
- Validation Requirements: Without rigorous site-specific validation, an AI tool can become a distraction rather than a helper.
- Behavioral Alignment: If the AI doesn’t match the natural workflow of the radiologist, it creates “triage fatigue” that actually slows down the diagnostic process.
- Intellivon’s Approach: This data makes a compelling case for a partner like Intellivon. We understand that AI only reduces workload when it is meticulously integrated and monitored to align with human behavior.
The difference between a successful deployment and a costly failure lies in the strategic execution of the AI radiology workflow. When implemented with technical precision, these tools deliver the massive ROI and time savings evidenced by the MASAI and ARA Health results.
AI Workload Reduction Across The Radiology Workflow
AI reduces workload across ordering, scheduling, image acquisition, interpretation, reporting, quality control, and follow-up communication.
To truly transform a department, stakeholders must look beyond the diagnostic booth. AI delivers maximum enterprise value when it is treated as an end-to-end operational layer rather than a standalone tool for image analysis.
By automating touchpoints throughout the entire clinical journey, facilities can eliminate the micro-frictions that collectively drain staff energy and departmental resources.
1. Before The Scan
Efficiency begins long before the patient enters the gantry. AI helps management anticipate needs and ensure that every scheduled slot is used effectively, reducing administrative overhead for coordinators and technologists.
- Imaging Order Checks: Algorithms verify imaging appropriateness, ensuring the requested scan matches the clinical indication.
- Protocol Selection: Automated systems suggest the most effective scan protocols based on the patient’s history and the referring physician’s query.
- Demand Prediction: Nature highlights that AI can forecast patient volume, allowing leadership to distribute workloads evenly across the department.
- Modality Utilization: Intelligent scheduling tools minimize machine downtime by optimizing the sequence of different scan types throughout the day.
2. During Image Acquisition
The quality of the output is determined at the source. AI tools integrated into the modality hardware act as a real-time quality coach for the technologist, ensuring the data is clinical-grade on the first attempt.
- Image Quality Checks: Systems detect suboptimal contrast or positioning in real-time, allowing for immediate adjustments.
- Motion Artifact Detection: AI identifies patient movement that would otherwise render a scan unreadable, preventing the “drift” that leads to rejected studies.
- Reconstruction Assistance: Advanced algorithms speed up the image reconstruction process, shortening the time a patient must remain inside the machine.
- Repeat Scan Reduction: By catching technical errors instantly, AI drastically reduces the rate of expensive and frustrating patient callbacks for re-imaging.
3. During Interpretation
This is the core of the AI radiology workflow, where the algorithm acts as a tireless assistant to the specialist. It organizes the mental workspace so the radiologist can focus on high-complexity decision-making.
- Worklist Prioritization: Urgent pathologies are moved to the top of the queue, ensuring critical patients are seen first.
- Lesion Detection: AI provides “second-look” support by flagging subtle nodules or fractures that might be missed during a high-volume shift.
- Normal Case Triage: The system identifies healthy scans, allowing for a rapid “quick-look” and sign-off to clear the backlog.
- Measurement Support: Automated quantification of organ volumes and lesion sizes removes the need for manual, pixel-level clicking.
4. During Reporting
The reporting phase is often where the most time is lost to administrative friction. AI transforms this stage from a manual data entry task into a high-level verification process.
- Draft Reports: Software pre-generates findings and impressions based on the image analysis, giving the doctor a 90% completed document to review.
- Structured Templates: AI enforces enterprise-wide reporting standards by auto-filling specific fields in a structured format.
- Missing Detail Alerts: The system monitors the report for laterality, size, or severity gaps, ensuring the final output is legally and clinically sound.
- Impression Suggestions: Intelligent prompts suggest the most likely diagnostic conclusion, reducing the cognitive load of phrasing complex results.
5. After Reporting
The value of a report is only realized if it leads to the correct clinical action. AI ensures that findings do not fall through the cracks of a fragmented healthcare system.
- Critical Alert Routing: The system automatically pushes life-threatening results to the referring physician’s mobile device or EHR dashboard.
- Follow-Up Tracking: AI monitors incidental findings, like a small lung nodule, and ensures a follow-up scan is scheduled for six months later.
- Referral Coordination: Automated workflows can trigger referrals to oncology or surgery based on specific keywords in the finalized report.
- Quality Dashboards: Management can track model performance and departmental turnaround times to ensure the investment continues to deliver ROI.
This holistic approach ensures that AI is not just a feature, but the backbone of a modern, scalable radiology enterprise. By optimizing every stage of the workflow, organizations can achieve a level of operational excellence that was previously impossible.
AI Use Cases That Reduce Reporting Time Fastest
The fastest reporting-time gains usually come from high-volume, repetitive, and time-sensitive radiology workflows where AI can remove recurring manual steps.
For an enterprise looking to maximize ROI, the strategy must prioritize high-frequency workflows where even a small percentage of time saved per study aggregates into significant operational gains.
By targeting these specific clinical use cases, leadership can ensure that the technology addresses the most persistent bottlenecks in the diagnostic pipeline.
1. Chest X-Ray Reporting Automation
Chest radiographs represent the highest volume of imaging in most hospitals, making them the most impactful area for automation. AI systems excel at categorizing these studies quickly to prevent backlogs in both inpatient and outpatient settings.
- Normal/Abnormal Triage: Algorithms can instantly separate clearly negative scans from those requiring complex review.
- Critical Alerts: The system provides immediate pneumothorax alerts, ensuring that a collapsed lung is treated before the radiologist even opens the file.
- Bedside Workflow Support: AI assists with ICU line and tube checks, providing rapid feedback on the placement of life-support equipment.
- Reporting Support: Structured reporting templates pre-filled by AI reduce the time spent on repetitive “clear” findings.
2. Stroke And Neuro Triage
In neurology, the mantra is “time is brain.” AI tools in this domain are designed to shave minutes off the diagnostic process, directly impacting the patient’s long-term recovery and reducing hospital stay durations.
- Large Vessel Occlusion (LVO): Automated detection of major arterial blockages allows for immediate surgical intervention.
- ASPECTS Support: AI provides standardized scoring for early ischemic changes, removing the subjectivity and time required for manual assessment.
- Stroke Team Alerts: Positive findings trigger simultaneous notifications across the entire care team, bypassing the traditional phone-tree delays.
- Escalation Speed: By flagging intracranial hemorrhage (ICH) early, the system ensures that neurosurgical consults happen in minutes rather than hours.
3. Pulmonary Embolism Triage
Pulmonary embolism (PE) is a high-stakes diagnosis that often arrives through the emergency department. AI ensures that these critical scans do not sit at the bottom of a high-volume worklist.
- CTPA Prioritization: The software scans CT pulmonary angiograms in the background and moves positive cases to the top of the reporting queue.
- Emergency Support: Rapid identification of clots in the pulmonary arteries allows the ER staff to begin anticoagulation therapy sooner.
- Communication Speed: Faster critical communication reduces the “dead time” between image acquisition and life-saving treatment decisions.
4. Mammography Screening Support
Screening programs are defined by massive volumes of mostly normal scans. AI serves as a high-performance filter that allows radiologists to spend more time on suspicious lesions.
- Risk-Score Triage: Algorithms assign a risk score to every mammogram, helping doctors prioritize the most suspicious cases first.
- Reading Support: AI can act as the “second reader” in double-reading protocols, maintaining high sensitivity while reducing the need for two separate human interpretations.
- Normal Case Prioritization: By flagging likely normal studies, the system allows for a faster “quick-read” workflow, significantly lowering the per-study interpreting time.
5. Oncology Follow-Up Reporting
Oncology patients require frequent longitudinal scans to track treatment progress. This is an exceptionally manual process that AI is uniquely equipped to handle through automated data comparison.
- Tumor Measurement: AI automates the 3D measurement of lesions, ensuring mathematical precision that is impossible with manual calipers.
- RECIST-Style Support: Software tracks tumor changes according to standardized criteria, prepopulating the comparison data into the report.
- Follow-Up Recommendations: The system tracks the timeline for the next scan and generates the appropriate recommendation language for the referring oncologist.
6. Musculoskeletal And Trauma Reads
In a busy emergency or orthopedic setting, identifying small fractures is both time-consuming and prone to human error during fatigue. AI acts as a tireless safety net for the surgical team.
- Fracture Detection: Advanced algorithms flag subtle or occult fractures in X-rays, particularly in difficult areas like the wrist or ribs.
- ED Workload Support: Rapid triage of trauma cases ensures that orthopedic surgeons receive the necessary information for stabilization immediately.
- Referral Acceleration: By speeding up the initial read, the facility can move patients through the ED and into specialized care pathways more efficiently.
Strategic deployment in these high-impact areas transforms the radiology department into a proactive engine of hospital efficiency. This targeted approach ensures that the investment delivers immediate, measurable value to both clinicians and the bottom line.
Why Some AI Tools Fail To Reduce Workload
AI tools fail to reduce workload when they create extra dashboards, false alerts, workflow interruptions, low trust, or additional verification burden.
The promise of automation often hits a wall when the technology is not aligned with the physical and cognitive reality of the medical professional. For an enterprise, an AI tool that adds even thirty seconds of administrative friction per study is an operational failure.
True workload reduction only occurs when the technology reduces the total number of steps required to reach a diagnostic conclusion.
1. Standalone AI Dashboards Add More Work
One of the most common pitfalls in health-tech procurement is the “portal problem.” If a radiologist has to leave their primary diagnostic environment to check a secondary screen, the tool has already lost the battle for efficiency.
- Separate Logins: Managing multiple credentials for different AI vendors creates unnecessary mental drag.
- Extra Screens: Physically turning away from the primary workstation to view results breaks the diagnostic flow.
- Manual Result Checking: If the system does not push results directly into the primary viewer, doctors must manually “pull” the data, adding steps to every study.
- Low Adoption: When a tool makes the job harder or slower, clinicians will simply stop using it, rendering the investment a sunk cost.
2. False Positives Create Alert Fatigue
An algorithm that is over-sensitive can become a burden. While missing a finding is a clinical risk, flagging every minor irregularity as a crisis creates a different kind of danger, which is desensitization.
- Non-Urgent Alerts: If the system “cries wolf” too often, radiologists begin to ignore the notifications, including the critical ones.
- Verification Burden: Every AI flag requires a human to verify it. If most of those flags are false positives, the “assistant” is actually creating more work.
- Reduced Confidence: High false-positive rates erode the medical team’s trust in the technology, leading to a rejection of the AI radiology workflow entirely.
- Delayed Adoption: Alert fatigue is the primary reason why sophisticated algorithms fail to scale within large hospital systems.
3. AI Outputs Do Not Match Reporting Style
Efficiency is lost when the AI-generated content requires extensive manual editing. If a draft report is phrased in generic “AI-speak” that doesn’t match the specialist’s medical lexicon, it becomes faster to delete the draft and start over.
- Unusable Drafts: Reports that lack the nuance of a specific sub-specialty require complete manual rewriting.
- Generic Impressions: If the AI cannot provide specific, actionable impressions, it fails to provide the high-level synthesis that decision-makers need.
- Specialty Alignment: A neuroradiologist and a musculoskeletal specialist use different descriptive styles; a “one-size-fits-all” AI output fails both.
- No Personalization: Without the ability to mirror the facility’s existing reporting standards, the AI remains an outsider in the clinical workflow.
4. Poor Integration Slows Radiologists Down
Technical debt and fragmented infrastructure are the enemies of speed. If the AI is not deeply embedded into the existing software stack, it creates a series of “micro-frictions” that aggregate into significant delays.
- PACS/RIS Disconnect: If the AI results don’t sync with the Picture Archiving and Communication System, the data remains siloed.
- EHR Context Gaps: When the AI lacks access to the Electronic Health Record, its findings may lack the necessary clinical context for a complete diagnosis.
- DICOM Routing Issues: Delays in how images are routed to the AI server can mean the “urgent” result arrives after the human has already finished the read.
- Viewer Friction: Any delay in the loading or rendering of AI overlays on the primary diagnostic monitor directly translates to lost revenue.
5. No Monitoring Means No Improvement
AI is not a “set and forget” solution. Because healthcare data is dynamic, models can experience “drift” where their accuracy or efficiency degrades over time if not properly governed.
- Model Drift: Changes in patient populations or referral patterns can lead to a drop in algorithm performance.
- Workflow Drift: As a department evolves, an AI tool that worked on day one may become a bottleneck by day three hundred.
- Modality Differences: An AI that works perfectly on a new 3T MRI might struggle with data from an older 1.5T machine, requiring constant calibration.
- Governance Dashboards: Without a centralized way to monitor accuracy and ROI, leadership has no way to prove the technology is still delivering value.
AI only reduces workload when it reduces steps. If it adds steps, radiologists will avoid it. Successful implementation requires a partner who understands the difference between a high-performing algorithm and a high-performing workflow.
How Intellivon Builds AI Systems That Reduce Radiologist Workload
Reducing radiologist workload requires a connected radiology system where image data, worklists, clinical context, AI outputs, reporting tools, and hospital integrations work together inside the radiologist’s daily workflow.
At Intellivon, we build AI radiology systems for hospitals, diagnostic imaging chains, teleradiology providers, and radiology SaaS platforms.
Our process focuses on reducing manual steps, improving reporting speed, supporting radiologist decisions, and making workload reduction measurable from day one.
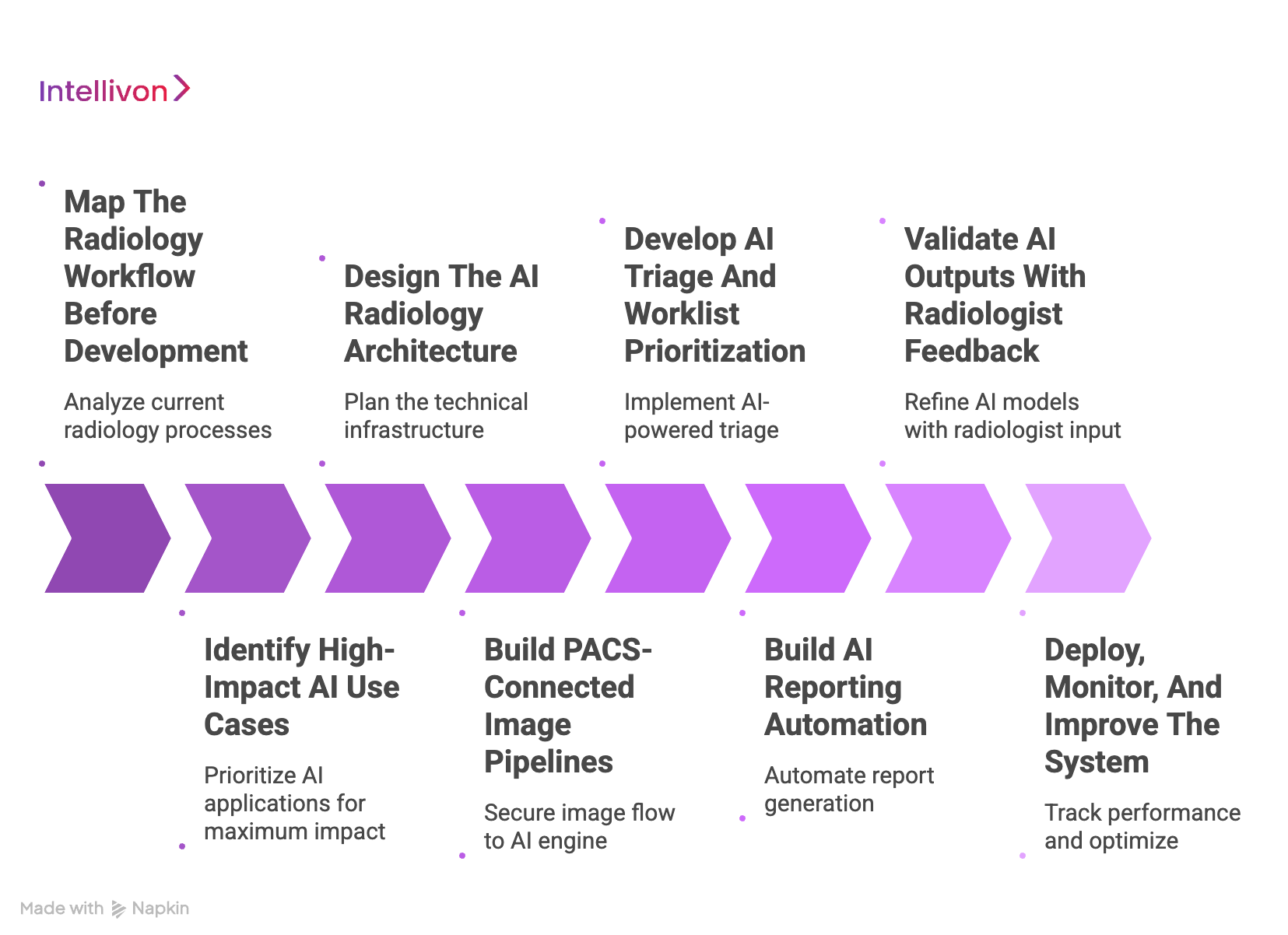
Step 1: Map The Radiology Workflow Before Development
Before building the AI system, Intellivon studies how radiologists currently receive, review, prioritize, report, and communicate imaging results. We believe that technology must adapt to the physician, not the other way around.
- PACS and RIS Mapping: We analyze the existing Picture Archiving and Communication System (PACS) and Radiology Information System (RIS) to identify technical bottlenecks.
- Performance Baselines: Our team establishes a clear baseline for current report turnaround times and modality-wise reporting loads.
- Pain Point Identification: We interview clinical staff to uncover manual steps that slow reporting or cause friction in emergency case routing.
- Systemic Audit: By documenting the movement of every study, we ensure the final AI solution removes real workload instead of adding another tool radiologists must manage.
Step 2: Identify High-Impact AI Use Cases
Intellivon helps hospitals choose AI use cases that can create measurable workload and reporting-time improvements. We prioritize high-volume and high-stakes categories to ensure a rapid return on investment.
- Triage Prioritization: We focus on areas like chest X-ray triage, stroke and neuro detection, and pulmonary embolism alerts, where time is of the essence.
- Automation Focus: Our systems are designed for mammography screening support and oncology follow-up, where repetitive tasks drain the most resources.
- Quantification Tools: We integrate measurement and segmentation automation to handle the tedious pixel-level work that typically slows down interpretation.
- Strategic Selection: This phase ensures the AI system starts with workflows where automation can reduce repetitive review and urgent-case delays.
Step 3: Design The AI Radiology Architecture
After defining the use case, Intellivon designs the technical architecture that connects medical imaging data, AI models, hospital systems, and reporting workflows. We build for the future, ensuring the system is both secure and scalable.
- Image Flow Design: We map the DICOM image flow from the modality to the inference engine and back to the viewer.
- Integration Points: Our architects define specific connection points for PACS, RIS, and EHR systems to ensure seamless data exchange.
- Deployment Flexibility: Whether the facility requires on-premise security or cloud-based scalability, we design the infrastructure to match.
- Roadmap Clarity: This rigorous planning gives hospital leadership a clear development roadmap and a defined budget before engineering begins.
Step 4: Build PACS-Connected Image Pipelines
Intellivon builds secure image pipelines that move scans from imaging systems to the AI engine and back into the radiologist’s workflow. We eliminate the need for secondary logins or external browsers.
- DICOM Ingestion: We develop robust ingestion layers that handle high-volume image routing without latency.
- Metadata Normalization: Our systems ensure that study matching and metadata are consistent across different modalities and imaging sites.
- Result Formatting: AI outputs are converted into PACS-ready formats, such as DICOM SR or secondary captures, for immediate viewing.
- Workflow Continuity: By delivering results directly into the primary diagnostic viewer, we keep radiologists inside their existing environment and prevent “context switching” fatigue.
Step 5: Develop AI Triage And Worklist Prioritization
Intellivon builds AI-powered triage workflows that help radiologists identify urgent studies faster. This layer acts as a digital safety net that continuously monitors the incoming volume.
- Critical Finding Detection: Algorithms are trained to recognize life-threatening pathologies and flag them the moment they are processed.
- Dynamic Reordering: We build logic that reorders the worklist based on severity scores, moving high-risk cases to the top of the queue.
- Alert Routing: The system pushes critical alerts to the appropriate care teams, ensuring the escalation workflow is triggered without manual intervention.
- Operational Balance: This reduces reporting delays for high-risk cases and improves the overall distribution of workload across the radiology team.
Step 6: Build AI Reporting Automation
We develop reporting automation features that reduce repetitive documentation and speed up report creation. We move the radiologist from “data entry operator” to “clinical validator.”
- Draft Generation: Our systems provide draft findings and impressions based on the AI’s analysis, pre-filling up to 90% of the report.
- Structured Templates: We integrate findings directly into the required fields of structured reporting templates, ensuring enterprise-wide consistency.
- Measurement Insertion: Automated lesion tracking and measurements are pushed directly into the text, eliminating manual typing errors.
- Efficiency Gains: These features allow radiologists to spend less time on routine report elements and more time on high-complexity clinical interpretation.
Step 7: Validate AI Outputs With Radiologist Feedback
Before full deployment, our experts validate AI outputs with radiologists to make sure the system supports clinical judgment instead of disrupting it. We prioritize trust above all else.
- Feedback Loops: We hold review sessions to analyze false positives and false negatives, refining the model for the specific patient population of the site.
- Usability Testing: Our engineers monitor how radiologists interact with the AI interface to ensure it fits their natural reporting behavior.
- Quality Checks: We run extensive tests on report draft quality and alert accuracy to minimize the risk of “alert fatigue.”
- System Refinement: This collaborative approach ensures that the final system is viewed as a helpful colleague rather than an intrusive technical hurdle.
Step 8: Deploy, Monitor, And Improve The System
After deployment, we track performance so hospitals can measure workload reduction, reporting-time gains, and AI reliability over time. We believe in data-driven governance.
- Analytics Dashboards: We provide real-time dashboards for turnaround time, reporting speed, and overall radiologist productivity.
- Adoption Metrics: Management can track how often AI suggestions are accepted, providing insight into the system’s clinical utility.
- Performance Monitoring: Our tools monitor for model drift and accuracy changes across different modalities or imaging sites.
- Continuous Optimization: This ensures the system continues to scale effectively and provides the necessary proof of ROI for long-term strategic growth.
With this process, Intellivon helps hospitals move beyond standalone AI tools and build radiology systems that reduce measurable workload inside daily operations.
From image routing and AI triage to reporting automation and performance monitoring, every layer is designed to help radiologists work faster, reduce repetitive tasks, and maintain clinical control.
Conclusion
Adopting an AI radiology workflow is a strategic necessity for enterprises facing rising imaging volumes and specialist shortages. By automating reporting, prioritizing critical findings, and removing administrative friction, these systems transform departments into high-efficiency hubs.
When technology aligns with clinical behavior, it delivers measurable ROI through faster turnaround times and improved patient outcomes. Integrating these tools allows for sustainable growth while ensuring physicians remain focused on high-level diagnosis.
Build AI Radiology Workload Solutions With Intellivon
At Intellivon, we build AI radiology systems for hospitals, diagnostic imaging chains, teleradiology providers, healthtech companies, and radiology SaaS platforms.
Our focus is to reduce manual work, speed up reporting, improve case prioritization, and help radiologists work with better support inside their existing workflow.
A. Mapping Radiology Workflows Before Development
We first study how radiologists receive, review, prioritize, report, and communicate imaging results.
This helps us identify where the workload actually builds up. It could be delayed worklists, repetitive measurements, manual report drafting, missing clinical context, urgent case overload, or too many disconnected systems.
What we cover:
- PACS and RIS workflow mapping
- Current turnaround time baseline
- Modality-wise reporting load
- Radiologist pain points
- Emergency and routine case routing
- Manual steps are slowing down reports
This gives hospitals a clear view of where AI can reduce real workload instead of becoming another tool radiologists must manage.
B. Developing AI Reporting Automation
Reporting time often increases because radiologists repeat the same documentation steps across hundreds of studies. Intellivon builds AI reporting features that reduce this repetitive work while keeping radiologists in full control.
The system can generate draft reports, fill structured templates, insert measurements, support prior comparisons, and suggest report language for review.
What we cover:
- Draft report generation
- Structured reporting templates
- Auto-filled findings
- Measurement insertion
- Impression suggestions
- Prior-study comparison support
- Editable radiologist review interface
This helps radiologists spend less time on routine documentation and more time on clinical interpretation.
C. Integrating AI With PACS, RIS, And EHR Systems
AI should not force radiologists to open separate dashboards or manually copy findings into reports. That adds friction and lowers adoption.
Intellivon integrates AI outputs directly into PACS, RIS, EHR, and reporting workflows so radiologists can access insights where they already work.
What we cover:
- DICOM image routing
- PACS integration
- RIS order matching
- HL7 and FHIR workflows
- EHR context connection
- Viewer-ready AI outputs
- Report-ready result delivery
This makes AI easier to use and helps hospitals avoid workflow disruption.
D. Reducing Manual Review And Repetitive Tasks
Many workload issues come from small tasks that repeat across every scan. These tasks may look minor, but they add up across large imaging volumes.
Intellivon builds AI features that automate or assist with repetitive review steps without removing radiologist oversight.
What we cover:
- Lesion measurement support
- Nodule tracking
- Organ segmentation
- Normal and abnormal case sorting
- Image quality checks
- Missing detail alerts
- Follow-up recommendation support
This reduces the manual effort around each case and helps radiologists move through reports faster.
If your hospital or radiology platform wants to reduce reporting delays, support radiologists, and build AI directly into imaging workflows, contact Intellivon to discuss your use case and development roadmap.

FAQs
Q1. How does AI reduce radiologist workload?
A1. AI reduces workload by prioritizing urgent scans, summarizing clinical context, automating measurements, pre-filling report sections, flagging missing details, and reducing repetitive review tasks. It works best when integrated directly into PACS, RIS, and reporting systems, so radiologists do not need extra dashboards.
Q2. Can AI reduce radiology reporting time?
A2. Yes. AI can reduce reporting time by generating draft reports, filling structured templates, inserting measurements, suggesting impressions, and helping radiologists focus on complex findings. Radiologists still review and approve the final report, but AI removes many repetitive documentation steps that slow down reporting.
Q3. Why do some AI radiology tools fail to save time?
A3. Some tools fail because they create false positives, extra clicks, separate dashboards, poor report drafts, or confusing alerts. If radiologists must spend more time checking AI outputs than reading the scan, the tool increases workload. AI must remove workflow steps, not add new ones.
Q4. Which radiology workflows benefit most from AI?
A4. High-volume and time-sensitive workflows benefit most. These include chest X-rays, stroke triage, pulmonary embolism detection, mammography screening, trauma imaging, oncology follow-ups, and structured reporting. These areas often involve urgent prioritization, repetitive measurements, or heavy documentation, making them strong candidates for AI support.