Key Takeaways:
- Hospital-grade AI radiology software requires direct PACS, RIS, EHR, and DICOM integration with radiologist-led review and governance built in from day one, not added after.
- Core use cases span abnormality detection, emergency triage, AI-assisted reporting, image segmentation, prior study comparison, and missed finding quality checks across multiple modalities.
- AI Model selection differs by clinical need: computer vision for detection, deep learning for complex scans, segmentation for tumor mapping, NLP for reporting, and multimodal AI for contextual review.
- Build costs range from $60,000 for a basic MVP to $500,000 and above for an enterprise platform with custom AI models, multi-site deployment, and full compliance architecture.
- How Intellivon builds AI radiology software that your hospital fully owns, connecting imaging data, clinical workflows, AI models, and governance controls into one scalable platform.
Hospitals have plenty of AI detection tools. However, they lack AI radiology software that truly fits the way radiology operates. This is because detection alone does not make a clinical product. By 2026, creating hospital-grade AI radiology software will require direct connections to PACS, RIS, EHR, and DICOM systems. This software must support radiologist-led reviews at every stage and include governance before processing any images. Without these elements, what exists is just a prototype, not a platform.
To do this correctly, teams must define the clinical use case, map out existing imaging workflows, integrate with hospital systems, build or connect AI models, design dashboards for radiologist reviews, and implement audit trails that can withstand scrutiny. At the same time, compliance and auditability are essential from the start, and they cannot be afterthoughts.
At Intellivon, we create AI radiology software for secure hospital infrastructure. We connect imaging data, clinical workflows, AI models, and governance controls into one scalable platform. This blog discusses use cases, key features, system architecture, integration needs, compliance frameworks, costs, timelines, and what serious development looks like.
Why Hospitals Need AI Radiology In 2026
The global radiology AI market is currently undergoing a period of rapid institutionalization. Projections indicate multi-billion dollar valuations by 2030, underpinned by a sustained compound annual growth rate (CAGR) of 24% to 25%. In 2026, focus is no longer on experimental adoption, but on operational scalability and clinical reliability.
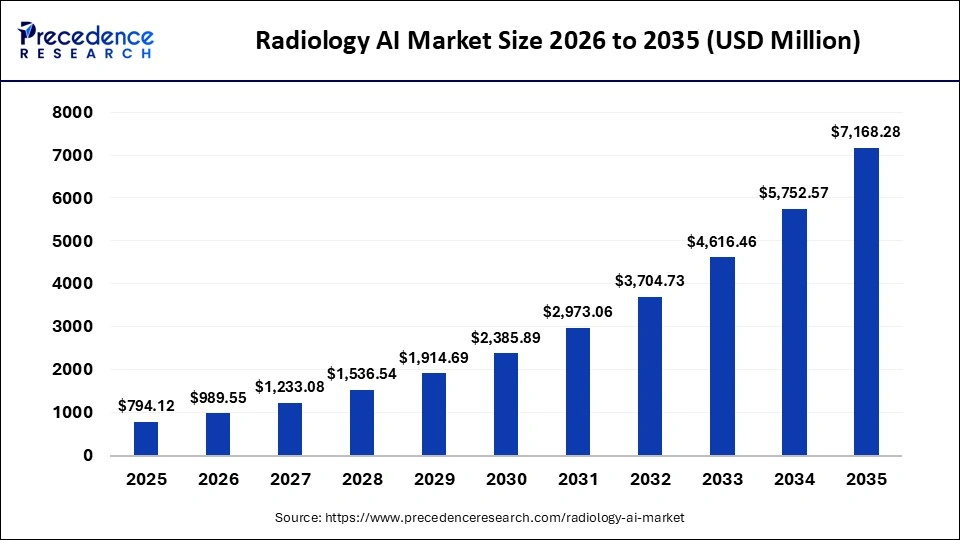
This transition is a direct response to unsustainable imaging volumes and systemic staffing shortages that pose a fundamental threat to diagnostic timelines and patient outcomes.
1. Imaging Volumes Are Increasing
Surging scan volumes in oncology and neurology, driven by an aging population and early-detection protocols, have created permanent structural bottlenecks.
For investors, the value lies in AI-driven worklist prioritization that mitigates these delays and ensures high-stakes studies are addressed during peak-load periods.
2. Radiologist Shortages Affect Turnaround
Chronic staffing gaps and subspecialty backlogs are driving clinician burnout. By implementing intelligent triaging, hospitals can optimize their human capital, allowing highly trained specialists to focus on complex diagnostic interpretations rather than manual, repetitive administrative tasks.
3. Hospitals Need Better Workflow Control
Standalone tools fail in high-pressure environments. In 2026, success requires deep integration with PACS and RIS ecosystems. To be a viable investment, a platform must function as a native layer, enhancing the diagnostic lifecycle without adding operational friction.
4. Governance Is Now A Buying Requirement
Transparency is now a core procurement mandate. Trust is built through “white-box” systems featuring robust audit trails, decision logs, and model-drift monitoring. Platforms must prove clinical accountability through rigorous QA dashboards to meet modern safety standards.
The transition toward integrated, governed AI is a strategic necessity for maintaining diagnostic integrity in 2026. Investors should prioritize platforms that balance technical sophistication with seamless workflow harmony and rigorous accountability.
What Is AI Radiology Software For Hospitals?
AI radiology software uses machine learning and computer vision to analyze medical images, prioritize urgent cases, and support radiologist review inside active hospital workflows.
However, hospital-grade AI radiology software goes further than basic DICOM viewers or standalone detection models. It connects directly with PACS, RIS, and EHR systems, embeds into clinical workflows, and includes governance, audit trails, and radiologist-in-the-loop design as core architecture.
How AI Radiology Software Works
The operational lifecycle of a medical imaging solution is a highly orchestrated technical pipeline designed to convert raw data into diagnostic intelligence. For investors, understanding this flow is critical for assessing platform efficiency and integration potential.
- Data Acquisition & Ingestion: The process begins when an imaging modality (CT, MRI, X-ray) captures a scan. This data is transmitted to the hospital’s imaging environment, where the software securely pulls DICOM files from the PACS or RIS.
- Neural Processing & Analysis: Advanced AI models execute automated segmentation, classification, and scoring. By analyzing pixel-level data, the system identifies anomalies that may be imperceptible to the human eye.
- Intelligent Triage & Reporting: High-confidence positive findings are instantly prioritized on the radiologist’s worklist. Clinicians review these insights via a specialized dashboard, allowing for AI-assisted structured reporting and seamless syncing with hospital records.
Strategic Imaging Applications
- Acute Care: Stroke triage via CT, fracture detection, and emergency case prioritization.
- Oncology: Lung nodule detection, tumor segmentation, and mammography screening support.
- Long-term Monitoring: Brain MRI analysis, chest X-ray abnormality detection, and automated quality checks to prevent diagnostic oversights.
AI Radiology Software Vs DICOM Viewers
For an investor, it is critical to distinguish between a commodity tool and a high-value clinical asset. While a standard DICOM viewer is a fundamental requirement for image visualization, it remains a passive utility.
In contrast, AI radiology software represents an active intelligence layer that transforms the diagnostic process from a manual inspection into a data-driven, assisted workflow.
The following table highlights the strategic and technical differences that justify the higher valuation and complexity of AI-integrated platforms:
| Feature | DICOM Viewer | AI Radiology Software |
| Main Role | Static image visualization | Automated analysis and case prioritization |
| Intelligence Layer | Limited or non-existent | Deep learning-based detection and scoring |
| Workflow Value | Basic access to imaging data | High-velocity assisted review and triage |
| Clinical Support | Manual clinician inspection | AI-supported decision assistance |
| Integration Needs | Standard DICOM viewing | Multi-point (PACS, RIS, EHR, Reporting) |
| Governance Needs | Basic access logs | Audit trails and active model monitoring |
| Buyer Value | Viewing efficiency | Measurable ROI via speed and quality gains |
A DICOM viewer serves only as a window into the scan. On the other hand, an AI radiology software acts as a specialized assistant. By flagging potential findings and structuring audit-ready workflows, AI solutions provide the operational scalability that modern healthcare enterprises require to remain solvent and safe.
The value of AI lies in its transition from a “point-and-click” tool to an autonomous clinical partner. Therefore, investing in the latter offers a defensible market position centered on improved patient outcomes and systemic efficiency.
Core Use Cases Of AI Radiology Software
AI radiology software serves as a multi-functional diagnostic layer that addresses abnormality detection, emergency triage, and operational automation.
By implementing these solutions, healthcare enterprises transform imaging departments into proactive, high-precision hubs that align clinical safety with business ROI goals.
1. AI-Based Abnormality Detection
Abnormality detection utilizes deep learning to identify deviations from healthy anatomical baselines, highlighting areas for immediate review. This digital “second set of eyes” identifies lung opacities, fractures, tumors, brain hemorrhages, and breast lesions.
Strategic positioning emphasizes that AI augments, rather than replaces, clinical judgment. By surfacing findings such as nodules or pneumonia, the software reduces the search fatigue that often leads to human error in high-volume environments.
2. Emergency Case Triage
In acute care, AI-driven triage automatically moves high-risk cases, like stroke, intracranial hemorrhage, or pulmonary embolism, to the top of the worklist. This ensures life-threatening conditions are addressed in minutes rather than hours.
This helps hospitals reduce delays for trauma-related abnormalities and improves response coordination across emergency teams. Improving “door-to-needle” time significantly enhances patient outcomes while lowering the institutional costs associated with delayed interventions.
3. AI-Assisted Radiology Reporting
Reporting assistance streamlines the diagnostic lifecycle by extracting objective data and auto-populating structured findings. It supports impression drafting, measurement extraction, and voice dictation, ensuring findings sync directly with RIS and EHR systems.
By automating finding summaries and prior-study comparisons, the software reduces repetitive documentation. This allows radiologists to maintain high-velocity throughput without sacrificing the detail or accuracy of the final clinical report.
4. Image Segmentation And Measurement
Segmentation models identify and outline regions of interest, such as tumor boundaries or organ structures. This provides precise lung volume analysis and lesion tracking that is often more consistent than manual 2D measurements.
These tools are vital for oncology and neurology, where brain structure analysis and bone fracture regions require high-granularity mapping. Accurate segmentation ensures that clinical decisions are based on quantifiable, repeatable data.
5. Prior Study Comparison
AI tracks chronic disease progression by comparing current scans with historical data to monitor changes in lesion size or tumor growth. This is essential for longitudinal oncology imaging workflows and chronic disease monitoring.
Automated follow-up scan comparison alerts clinicians to subtle changes over time that might be missed during a manual side-by-side review, ensuring that treatment plans are adjusted based on the most accurate trajectory of the disease.
6. Quality Checks For Missed Findings
Acting as a second review layer, AI performs consistency checks between the image and the final report. It monitors for missed abnormalities and provides QA dashboards to track department-level quality and peer-review accuracy.
These safety nets help reduce diagnostic oversights and provide administrators with actionable data for quality tracking. By maintaining a high standard of clinical oversight, hospitals protect themselves against liability while improving overall patient care.
| Use Case | Hospital Value |
| Abnormality Detection | Supports faster, more accurate scan review |
| Emergency Triage | Prioritizes critical, life-threatening cases |
| Reporting Assistance | Reduces repetitive documentation and errors |
| Segmentation | Improves measurement accuracy for complex cases |
| Prior Comparison | Tracks clinical changes and disease progression |
| QA Checks | Helps reduce missed findings and oversight |
| Worklist Automation | Improves overall radiology department throughput |
Defining these use cases allows hospitals to identify the specific AI radiology architecture they need to build. Investors should focus on platforms that offer these high-value applications as a cohesive, integrated ecosystem.
Types Of AI Radiology Software to Build
Before committing capital, investors must define the product scope, as the architecture and regulatory pathway vary significantly between a specialized tool and an enterprise platform.
Selecting the right software type ensures the development roadmap aligns with specific clinical demands and long-term scalability.
1. AI Triage Software For Critical Cases
Triage software is engineered for speed, specifically detecting urgent pathologies and reordering review queues to prioritize life-threatening findings. It acts as a digital safety net, ensuring that high-stakes scans do not sit at the bottom of a busy worklist.
- Best For: Emergency departments, level-one trauma centers, and high-volume teleradiology providers.
- Key Features: Critical finding detection, urgency scoring, real-time alert routing, and automated radiologist notifications.
2. AI Reporting Assistant For Radiologists
Reporting assistants focus on reducing the high cognitive load of documentation by automating repetitive tasks and ensuring consistency across clinical reports. They transform the radiologist’s role from manual data entry to high-level oversight.
- Best For: Specialized imaging centers and teleradiology networks seeking to increase report throughput.
- Key Features: Structured report support, finding summaries, automated measurement extraction, and seamless RIS/EHR synchronization.
3. AI Quality Control Platform
QA platforms serve as governance layers, allowing medical directors to monitor diagnostic accuracy and model performance across an entire institution. These systems are essential for maintaining clinical standards and managing liability.
- Best For: Enterprise healthcare networks and compliance-focused teams requiring rigorous oversight.
- Key Features: Audit dashboards, false positive/negative tracking, peer review support, and active model performance monitoring.
4. AI Workflow Automation System
This system focuses on the “plumbing” of the radiology department, managing how cases are routed and tracked throughout the diagnostic lifecycle. It optimizes operational efficiency by matching the right case to the right specialist at the right time.
- Best For: Large diagnostic chains and multi-site radiology networks with complex operational logic.
- Key Features: Intelligent case routing, SLA tracking, multi-role dashboards, and automated escalation logic.
5. Full-Scale Radiology AI Platform
A full-scale platform is the most ambitious build, integrating ingestion, deep-learning analysis, reporting, and governance into a unified ecosystem. It is the foundational infrastructure for any institution aiming for a completely AI-augmented imaging strategy.
- Best For: Healthtech companies and hospitals building long-term, scalable AI infrastructure.
- Key Features: End-to-end DICOM ingestion, integrated analysis, radiologist dashboards, and comprehensive enterprise integrations.
| Software Type | Best For | Complexity |
| AI Triage Software | Emergency case prioritization | Medium |
| Reporting Assistant | Radiologist productivity | Medium |
| QA Platform | Quality and governance | Medium-high |
| Workflow Automation | Operational efficiency | High |
| Full AI Radiology Platform | Enterprise-scale deployment | High |
Selecting the software type dictates the baseline budget and technical requirements. Once the scope is defined, the next decision involves choosing the specific features that make the system usable in real-world hospital conditions.
Features Hospitals Need Beyond AI Detection
For a medical imaging solution to achieve clinical adoption, it must transcend the “black-box” algorithm and function as a sophisticated enterprise tool. Investors must ensure the platform addresses the logistical realities of a radiology department, specifically interoperability, accountability, and the human-in-the-loop workflow.
Without these core features, even the most accurate AI remains an isolated curiosity rather than a billable medical device.
1. DICOM Image Upload And Processing
The technical entry point for any radiology solution is its ability to handle Digital Imaging and Communications in Medicine (DICOM) files. The platform must ingest high-resolution studies, manage metadata, and perform image preprocessing to ensure uniformity across various hardware manufacturers.
- Capabilities: Comprehensive DICOM file support, modality identification (CT, MRI, X-ray), and automated patient-study mapping to maintain data integrity.
2. PACS And RIS Integration
AI tools fail when they force radiologists to leave their primary workspace. Integration with the Picture Archiving and Communication System (PACS) and Radiology Information System (RIS) is a non-negotiable requirement for 2026.
- Workflow Harmony: The system must support PACS query/retrieve and automated image routing, ensuring that findings are synchronized with RIS scheduling and EHR report modules without manual intervention.
3. AI Detection And Risk Scoring
Raw detection is insufficient, and the software must provide context through risk scoring and confidence levels. This allows radiologists to distinguish between subtle incidental findings and acute, life-threatening pathologies.
- Insight Layer: Features include urgency ranking, heatmaps for anatomical overlays, and explainability support to show why the AI flagged a specific region, fostering clinical trust.
4. Radiologist Review Workflow
The platform must facilitate a “human-in-the-loop” architecture. At the same time, radiologists require a dedicated dashboard where they can quickly review AI outputs and either validate or reject them.
- Control Mechanisms: A robust case list with approve/reject options, integrated image viewers, and escalation protocols for complex cases ensures the clinician remains the final decision-maker.
5. AI-Assisted Reporting
To drive ROI, the software must significantly reduce the time spent on documentation. Hence, by auto-populating structured report templates with AI-extracted measurements, the system eliminates repetitive data entry.
- Efficiencies: Support for finding summaries, impression drafting, and voice dictation compatibility ensures that the final output is ready for immediate RIS/EHR export.
6. Critical Alerting System
Urgent findings must be communicated through a tiered alerting system that avoids “notification fatigue.” Therefore, the system must intelligently route alerts to the correct roles based on the severity of the finding.
- Accountability: Critical result tracking, alert acknowledgment logs, and SLA monitoring ensure that life-saving information is acted upon within established clinical windows.
7. Audit Logs And Decision History
In a regulated healthcare environment, every action, both AI and human, must be traceable. At the same time, audit logs provide the forensic trail necessary for legal protection and clinical quality reviews.
- Transparency: Comprehensive logs of AI outputs, radiologist overrides, and timestamped user activity history are essential for regulatory compliance and institutional governance.
8. Model Monitoring Dashboard
AI performance can degrade over time due to “model drift” or changes in hospital equipment. Therefore, a monitoring dashboard provides real-time visibility into the health of the algorithm.
- Performance Metrics: Hospitals track accuracy trends, false-positive/negative rates, and confidence score distributions to ensure the AI remains reliable across varying case volumes and modalities.
| Feature | Why It Matters |
| DICOM Ingestion | Enables secure, standardized clinical image handling |
| PACS/RIS Integration | Ensures the tool fits existing hospital workflows |
| AI Scoring | Quantifies findings to help prioritize urgent reviews |
| Radiologist Dashboard | Keeps humans in control of the final diagnosis |
| Reporting Support | Reduces documentation burden and manual errors |
| Critical Alerts | Speeds up the response time for urgent, high-risk cases |
| Audit Logs | Supports governance, liability protection, and review |
| Model Monitoring | Tracks long-term AI reliability and clinical safety |
These features require a robust technical foundation, making architecture one of the most critical components of the development process. Investors must ensure the underlying stack is built for high-concurrency and deep medical interoperability.
Hospital Integrations Needed For Radiology AI
A radiology AI solution is only as valuable as its connectivity. For enterprise-scale deployment, the software must navigate the complex “web” of hospital IT, ensuring data flows seamlessly between diagnostic devices and clinical records.
Technical debt often stems from poor interoperability. Therefore, investors must prioritize a modular integration strategy that supports both legacy standards and modern APIs.
1. PACS Integration
The Picture Archiving and Communication System (PACS) is the central repository for medical images. Deep integration allows the AI platform to perform automated DICOM query/retrieve functions, pulling studies for analysis and routing findings back to the clinician’s primary workstation.
- Technical Scope: Success requires robust study synchronization and image routing that maintains high fidelity across multi-vendor PACS environments.
- Operational Impact: By ensuring viewer compatibility, the AI results appear as a native layer in the radiologist’s current environment, eliminating the need to toggle between different software applications.
2. RIS Integration
The Radiology Information System (RIS) manages the business logic of the department, including scheduling and order status. Integrating with the RIS ensures that the AI is aware of the patient exam details and the specific radiologist assigned to the case.
- Workflow Continuity: The system tracks the study lifecycle, from “ordered” to “completed,” allowing the AI to trigger analysis the moment a scan is finalized.
- Strategic Value: This connectivity ensures that AI findings are linked to the correct billing and administrative codes, streamlining the entire radiology operation.
3. EHR Integration
The Electronic Health Record (EHR) provides the critical patient context that raw imaging data lacks. By integrating with the EHR, the AI can correlate imaging findings with medical history, clinical notes, and existing diagnosis codes.
- Clinical Depth: Access to longitudinal care records allows the AI to support more nuanced interpretations, such as comparing a current lung nodule to a history of smoking or prior malignancies.
- Delivery: Final reports are pushed directly into the patient’s record, ensuring all members of the care team have immediate access to AI-augmented insights.
4. HL7 And FHIR Integration
Healthcare messaging standards like HL7 and FHIR are the “languages” hospitals use to communicate. While HL7 is the legacy standard for triggered events (like a new order), FHIR provides modern, web-based APIs for more flexible data exchange.
- Interoperability Planning: Utilizing FHIR APIs allows for faster development and easier scaling across different healthcare networks.
- Data Exchange: These standards ensure that patient demographics and report delivery are handled securely and accurately, reducing the risk of data silos.
5. Modality Worklist Integration
Modality worklist integration connects the AI platform directly to the imaging devices, such as CT or MRI scanners. This ensures that the imaging order details are perfectly matched to the patient-study at the point of acquisition.
- Accuracy Gains: This integration significantly reduces manual entry errors by the technologist, ensuring the AI analyzes the correct scan for the correct clinical indication.
- Coordination: It facilitates better modality coordination, ensuring that high-priority emergency scans are flagged for AI analysis before the patient even leaves the table.
6. Reporting System Integration
The final output of a radiologist’s work is the report. AI findings must support these reporting workflows by auto-populating structured findings and providing impression support without forcing a separate login.
- Efficiency Drivers: Compatibility with voice dictation and automated RIS/EHR sync ensures that measurements and findings are transferred with 100% accuracy.
- Approval Flow: The system supports a final approval flow where the radiologist validates the AI-generated content before it is finalized in the hospital’s clinical records.
| Integration | Role In Radiology AI |
| PACS | Retrieves and routes imaging studies for analysis |
| RIS | Supports scheduling and manages the reporting lifecycle |
| EHR | Adds patient context and stores final clinical records |
| DICOM | Enables standardized medical image and metadata exchange |
| HL7 | Supports hospital-wide messaging and event triggers |
| FHIR | Enables modern, API-driven clinical data exchange |
| Modality Worklist | Connects scan orders directly to imaging devices |
| Reporting Tools | Moves AI findings into the final clinical documentation |
Once integrations are mapped, our development team can start building the software in a structured sequence. This technical foundation is what allows a platform to move from a lab environment to a revenue-generating clinical tool.
How To Build AI Radiology Software Step By Step
Building a market-ready AI radiology solution requires more than just an algorithm; it demands a robust, regulated, and interoperable ecosystem. At Intellivon, we utilize an “Integration-First” development philosophy.
This ensures that the high-fidelity AI models we build are not isolated tools but are deeply woven into the hospital’s digital fabric.
By following a structured nine-step roadmap, we mitigate technical debt and ensure that every platform is ready for the rigors of a clinical environment.
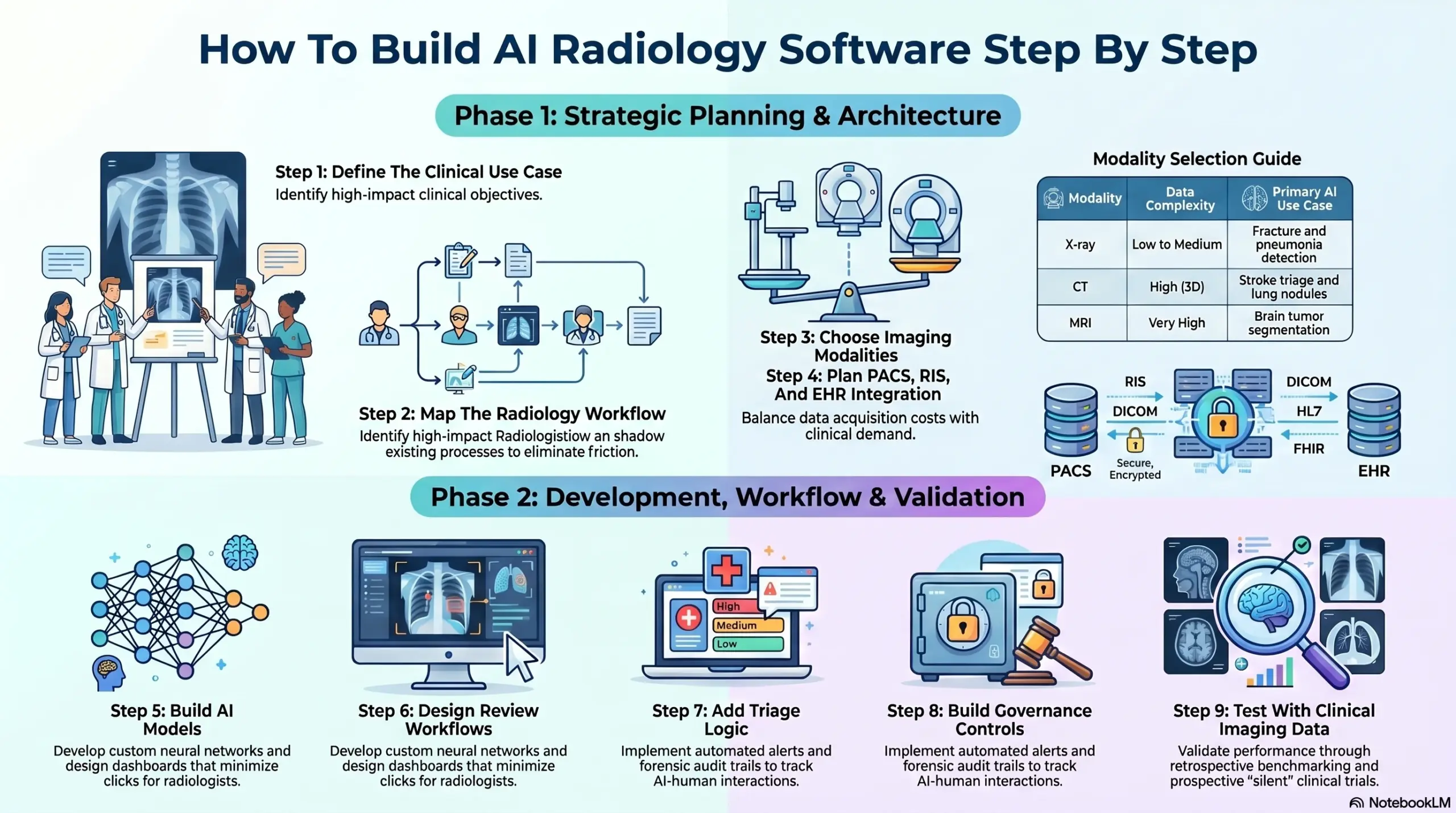
Step 1: Define The Clinical Use Case
Every project at Intellivon begins with identifying a high-impact clinical objective. Developing “generic” radiology AI often leads to unfocused products that fail to achieve regulatory clearance or buyer interest.
We focus on specific pathologies where AI offers the highest ROI, such as reducing “door-to-needle” time for stroke patients or increasing the sensitivity of breast cancer screenings.
- Strategic Objectives: We define success metrics early, such as target sensitivity/specificity rates or expected reduction in turnaround time (TAT).
- Focused Examples: Fracture detection in high-volume trauma centers, lung nodule tracking for oncology clinics, or automated measurement for cardiac MRI.
Step 2: Map The Radiology Workflow
We perform a comprehensive “shadowing” of the existing diagnostic process to ensure our software eliminates friction.
Understanding how a scan moves from the modality to the radiologist’s eyes allows us to identify the exact point where AI intervention adds the most value.
- Workflow Mapping Components:
- Capture: Identifying the imaging modality and technologist protocols.
- Storage: Mapping the DICOM transfer path from the scanner to the PACS.
- Assignment: Understanding how cases are currently routed to subspecialists.
- Escalation: Defining the criteria for “critical” alerts and how they are communicated to emergency teams.
Step 3: Choose Imaging Modalities
The choice of modality dictates the complexity of the data pipeline and the specific machine learning architecture required.
Intellivon assists investors in selecting modalities that align with their market entry strategy, balancing data acquisition costs with clinical demand.
| Modality | Data Complexity | Primary AI Use Case |
| X-ray | Low to Medium | Fracture, pneumonia, and chest abnormality detection |
| CT | High (3D) | Stroke triage, pulmonary embolism, and lung nodules |
| MRI | Very High (Multi-sequence) | Brain tumor segmentation and neurodegenerative tracking |
| Mammography | High (Dense tissue) | Lesion detection and breast density scoring |
| Ultrasound | Medium (Dynamic) | Obstetric measurements and cardiovascular fluid flow |
Step 4: Plan PACS, RIS, And EHR Integration
Interoperability is the most common failure point in healthtech. We architect the data flow before building the UI, ensuring the platform speaks the native language of hospital IT.
This includes planning for multi-vendor PACS environments and ensuring HIPAA-compliant data encryption in transit.
- Technical Planning:
- DICOM Integration: Configuring C-MOVE and C-STORE commands for image retrieval.
- HL7/FHIR: Setting up the messaging infrastructure for patient demographics and order updates.
- Security: Implementing OAuth2 and specialized VPN tunnels for secure hospital-to-cloud communication.
Step 5: Build Or Integrate AI Models
At this stage, we decide between building bespoke neural networks or integrating high-performing third-party models.
Whether we are developing custom U-Net architectures for segmentation or using ResNet for classification, our focus is on creating a “transparent” engine that provides confidence scores for every finding.
- Development Areas:
- Object Detection: Highlighting specific anomalies like a rib fracture.
- Segmentation: Outlining the exact boundaries of a tumor to calculate volume.
- Classification: Labeling a study as “Normal” or “Abnormal” to support worklist prioritization.
Step 6: Design Radiologist Review Workflows
A radiologist’s time is their most valuable asset. Intellivon designs dashboards that minimize clicks. We focus on “natural” viewing experiences where AI overlays, such as heatmaps, can be toggled on and off without obstructing the original diagnostic image.
- Dashboard Features:
- Synchronized Viewers: Comparing the current scan with historical studies automatically.
- Approve/Reject Logic: Enabling one-click validation of AI findings.
- Heatmap Overlays: Visualizing the AI’s “attention” to show exactly where it detected an anomaly.
Step 7: Add Reporting And Triage Logic
The value of AI is realized when it influences action. We build the “if-this-then-that” logic that governs how AI outputs are used. For example, if the AI detects a large intracranial hemorrhage, the system automatically triggers a “Code Brain” alert to the stroke team.
- Reporting Assistance:
- Auto-Population: Injecting measurements directly into the RIS report template.
- Finding Summaries: Generating a concise narrative of the detected pathologies.
- Triage Scoring: Assigning a numerical urgency score to each case to reorder the worklist.
Step 8: Build Governance And Audit Controls
For institutional buyers, governance is a non-negotiable requirement. We build comprehensive audit trails that record every interaction between the AI and the human. This provides the forensic evidence needed for peer review, quality assurance, and liability protection.
- Control Systems:
- Decision Logs: Tracking every time a radiologist overrode an AI suggestion.
- Model Monitoring: Dashboards that track “accuracy drift” as new hardware or protocols are introduced to the hospital.
- Activity History: Time-stamped logs of when a study was received, analyzed, and reviewed.
Step 9: Test With Clinical Imaging Data
The final step is a multi-stage validation process. We move from retrospective testing (using historical, known data) to prospective “silent” trials where the AI runs in the background of a live environment without influencing clinical decisions yet.
| Validation Type | Purpose | Main Metric |
| Retrospective | Benchmarking against “Ground Truth” | Sensitivity & Specificity |
| Workflow Testing | Measuring impact on reporting speed | Turnaround Time (TAT) |
| Security Audit | Ensuring data privacy compliance | Pen-test success rate |
| UAT | Ensuring the dashboard meets clinician needs | User satisfaction score |
This step-by-step approach ensures that the resulting software is not just a technical achievement, but a defensible clinical asset.
The development process also depends heavily on the type of AI models used inside the radiology software, which dictates the specific hardware and data requirements for the project.
AI Models Used In Radiology Software
The efficacy of a radiology AI solution is determined by its underlying model architecture, yet the model itself is not the entire product. It is a specialized engine sitting within a complex ecosystem of DICOM ingestion, PACS/RIS integration, and clinician-facing dashboards.
At Intellivon, we view the model as a modular layer, where the choice of architecture dictates the project’s cost, regulatory validation pathway, and eventual clinical utility.
1. Computer Vision Models For Image Detection
Computer vision (CV) models are the primary “eyes” of the system, trained to identify visual patterns within 2D and 3D medical images. These models analyze pixel-level intensities to detect anomalies in X-rays, CT scans, and mammograms that might be missed during a rapid manual review.
- Workflow Integration: CV models operate within the AI inference layer. Once an image is preprocessed, the model flags regions of interest (ROI) and transmits these coordinates to the radiologist’s review dashboard.
- Strategic Use Cases: Essential for fracture detection, lung opacity identification, and screening support in high-volume mammography workflows.
- Development Considerations: Success requires that training data match real-world hospital noise and image quality. At Intellivon, we ensure that CV outputs are returned as heatmaps or visual overlays that radiologists can verify in seconds.
2. Deep Learning Models For Complex Scan Analysis
While basic CV identifies patterns, deep learning (DL) models utilize neural networks to analyze subtle, complex features across massive datasets. These models are necessary when the software must classify abnormalities by severity or process high-dimensional data like multi-sequence MRIs.
- Infrastructure Impact: Deep learning often demands high-performance compute environments. They are typically utilized for stroke triage and tumor classification, where simple pattern matching is insufficient.
- Cost & ROI: While DL increases initial development costs due to the need for larger annotated datasets and GPU-intensive training, the clinical accuracy it provides often justifies the investment for enterprise-scale platforms.
- Intellivon’s Approach: We treat DL as a component of the full platform. The model must be seamlessly connected to audit logs and monitoring systems to track performance drift in real-time.
3. Segmentation Models For Region Mapping
Segmentation models go beyond detection by outlining the precise boundaries of anatomical structures or abnormalities. This allows for the transition from qualitative observation (“there is a tumor”) to quantitative data (“the tumor volume is 4.2 cubic centimeters”).
- Clinical Value: Segmentation is the gold standard for oncology follow-up workflows, brain structure mapping, and organ volume analysis.
- Technical Rigor: These models require pixel-level annotation, which is significantly more expensive and time-consuming than simple image-level labeling. Poorly defined masks can quickly erode radiologists’ trust.
- Financial Impact: Segmentation adds complexity to the visualization layer, requiring contours or masks that must perfectly align with the original DICOM images in the viewer.
4. NLP Models For Radiology Reports
Natural Language Processing (NLP) models focus on the textual data within the radiology department rather than the images. They serve as a bridge between the AI’s visual findings and the final clinical documentation stored in the RIS or EHR.
- Operational Role: NLP sits in the reporting layer, extracting findings from prior reports and supporting the drafting of impressions. This reduces the cognitive load of documentation without removing the radiologist’s oversight.
- Precision Requirements: NLP outputs must adhere to standardized medical terminology (e.g., BI-RADS or LI-RADS). At Intellivon, we build NLP tools that allow for human edits, ensuring the radiologist remains the final author.
5. Multimodal AI Models For Contextual Review
The most advanced radiology platforms utilize multimodal AI to combine image data with patient metadata, lab results, and historical clinical notes. This creates a context-aware system that mimics the holistic thinking of a senior consultant.
- The Contextual Edge: By correlating a scan with a patient’s medical history or previous biopsy results, the AI can provide a nuanced risk score rather than a generic abnormality flag.
- Integration Complexity: These models require deep EHR and RIS connectivity. The data normalization process is more intensive, as the system must ingest and harmonize disparate data types (text, images, and structured lab data).
- Strategic Positioning: Multimodal AI is best suited for healthcare networks aiming for a “Center of Excellence” status, where decision support is integrated across the entire patient journey.
| AI Model Type | Radiology Use | Product Layer |
| Computer Vision | Detects visible image patterns | AI inference layer |
| Deep Learning | Learns complex imaging features | AI model layer |
| Segmentation | Outlines anatomy or abnormalities | Image review layer |
| NLP | Supports radiology reports | Reporting layer |
| Multimodal AI | Combines images and clinical context | Advanced decision layer |
Strategic Buyer Guidance
Selecting the right model architecture is a business decision that defines the product’s market scope.
A basic triage tool may only require a deep learning classification model, whereas a comprehensive oncology platform necessitates a combination of segmentation, NLP, and multimodal context.
| Buyer Goal | Suitable Model Type |
| Detect abnormalities in X-rays | Computer vision or deep learning |
| Prioritize urgent CT scans | Deep learning and triage models |
| Measure tumors or lesions | Segmentation models |
| Reduce reporting workload | NLP models |
| Compare scans with patient history | Multimodal AI |
| Build a full radiology AI platform | A combination of multiple models |
At Intellivon, we help partners navigate these choices based on their clinical use cases and long-term scalability goals.
How Much Does Building AI Radiology Software Cost?
AI radiology software development can cost anywhere from $60,000 to $500,000+, depending on the imaging modality, AI model complexity, PACS/RIS/EHR integrations, governance requirements, deployment model, and validation scope.
A basic MVP with image upload, a pre-trained AI model, and a simple review dashboard may start between $60,000 and $120,000. However, a hospital-grade AI radiology platform with PACS connectivity, DICOM workflows, AI-assisted reporting, model monitoring, audit trails, and multi-site deployment can cost $300,000 to $500,000+.
| Software Type | Estimated Cost |
| Basic AI radiology MVP | $60,000–$120,000 |
| PACS-integrated AI radiology system | $120,000–$250,000 |
| AI reporting and workflow platform | $180,000–$350,000 |
| Enterprise radiology AI platform | $300,000–$500,000+ |
What Increases AI Radiology Software Cost?
The cost of AI radiology software does not depend only on the number of screens. It depends on the depth of AI, data, integration, compliance, and clinical workflow complexity.
The biggest cost drivers include:
- Multiple imaging modalities
- Custom AI model training
- Large imaging datasets
- Radiologist annotation requirements
- PACS, RIS, and EHR integration
- DICOM and DICOMweb complexity
- Real-time triage workflows
- AI explainability features
- Heatmaps and visual overlays
- Clinical validation planning
- HIPAA-ready security controls
- FDA SaMD documentation support
- Hybrid or on-premise deployment
- Multi-site hospital scaling
- Model monitoring dashboards
- Long-term maintenance and updates
For example, a single-use X-ray detection MVP will cost less because the image workflow is simpler. A multi-modality platform for CT, MRI, X-ray, and mammography will cost more because it needs different preprocessing logic, model pipelines, review workflows, and validation methods.
Similarly, software that only displays AI results will cost less than a platform that connects with PACS, updates RIS workflows, exports reports to EHR systems, and tracks every decision through audit logs.
Cost By Development Area
| Development Area | Estimated Cost Impact |
| Discovery and workflow planning | $8,000–$25,000 |
| UI/UX and radiologist dashboard | $15,000–$50,000 |
| DICOM image handling | $20,000–$60,000 |
| PACS integration | $30,000–$90,000 |
| RIS/EHR integration | $25,000–$80,000 |
| AI model integration | $30,000–$100,000 |
| Custom AI model development | $80,000–$200,000+ |
| Reporting workflow | $25,000–$75,000 |
| Governance and audit controls | $30,000–$100,000 |
| Testing and validation | $25,000–$120,000 |
These ranges can overlap because every hospital environment is different. A project with clean data, one modality, and limited integration needs will stay closer to the lower end. A project with multiple departments, custom AI models, legacy systems, and compliance-heavy workflows will move toward the higher end.
MVP Vs Enterprise Platform Cost
| Cost Area | Basic MVP | Enterprise Platform |
| Estimated cost | $60,000–$120,000 | $300,000–$500,000+ |
| Imaging scope | One modality | Multiple modalities |
| Image input | Manual upload | PACS/DICOM-based ingestion |
| AI model | Pre-trained or limited model | Custom or multi-model system |
| Dashboard | Simple review interface | Role-based clinical workflows |
| Reporting | Basic output | RIS/EHR-connected reporting |
| Governance | Limited logs | Full audit and monitoring |
| Deployment | Cloud MVP | Cloud, hybrid, or on-premise |
| Best for | Pilot projects | Hospital-grade deployment |
A basic MVP helps teams test feasibility. An enterprise platform helps hospitals operationalize AI across real radiology workflows.
Intellivon’s Cost Approach
At Intellivon, we estimate AI radiology software cost by looking at the complete clinical and technical environment, not just the feature list.
We assess the imaging modality, PACS/RIS/EHR requirements, DICOM workflows, AI model scope, reporting needs, governance layer, security requirements, and deployment model before defining the final budget.
This helps hospitals and healthtech companies avoid underbuilt AI tools that work in demos but fail inside real clinical environments.
Our approach focuses on building AI radiology software that can integrate with hospital systems, support radiologist-led review, protect patient data, and scale across departments or locations.
Conclusion
The future of diagnostic imaging depends on moving beyond standalone algorithms toward integrated, hospital-grade ecosystems. Successful investment requires a focus on interoperability, rigorous governance, and seamless clinical workflows that prioritize physician trust.
By aligning technical architecture with real-world operational demands, entrepreneurs can deliver scalable solutions that transform radiology from a manual bottleneck into a high-velocity, data-driven department. Prioritize clinical utility and regulatory readiness to ensure long-term market leadership.
Build AI Radiology Software With Intellivon
At Intellivon, we build AI radiology software that fits real hospital environments. Our team develops platforms that connect with PACS, RIS, EHR, DICOM workflows, reporting systems, and clinical review processes, so AI can support radiologists inside the workflows they already use.
We help hospitals, imaging networks, healthtech companies, and MedTech teams build secure AI radiology platforms that improve case prioritization, reporting speed, workflow visibility, and long-term model performance.
A. Building AI Radiology Systems For Hospitals
Hospitals need AI radiology software that improves clinical operations without adding friction for radiologists. We design platforms that support urgent case triage, image review, reporting, governance, and secure deployment across hospital environments.
- AI triage systems: We build triage workflows that prioritize critical scans and help radiologists review urgent cases faster.
- PACS/RIS integration: Our systems connect with existing imaging and radiology infrastructure to avoid disconnected AI dashboards.
- Radiologist review workflows: We design human-in-the-loop review systems where radiologists can validate, edit, approve, or override AI outputs.
- Reporting workflows: We build structured reporting support, finding summaries, and RIS/EHR-connected documentation flows.
- Governance dashboards: We add audit trails, QA views, model monitoring, and performance tracking for clinical oversight.
- Secure deployment: We support cloud, hybrid, and on-premise deployment based on hospital security and IT requirements.
This helps hospitals use AI as part of daily radiology operations, not as a separate tool that sits outside the clinical workflow.
B. Developing AI Imaging Products For Healthtech Teams
Healthtech and MedTech companies need AI radiology products that can move from MVP to a scalable platform without rebuilding the architecture later. Intellivon helps teams define the right product scope, build the first working version, and prepare the platform for clinical workflow expansion.
- MVP development: We build focused AI radiology MVPs for one modality, use case, or workflow.
- AI model integration: We integrate pre-trained, fine-tuned, or custom AI models into secure imaging workflows.
- Product architecture: We design scalable backend systems for image ingestion, AI inference, review, and reporting.
- Clinical workflow design: We create dashboards and review flows that match how radiologists actually work.
- Compliance-ready engineering: We build audit logs, access control, documentation support, and validation-ready workflows.
- Scalable platform development: We structure the system so new modalities, models, and hospital integrations can be added later.
This gives product teams a stronger foundation than a demo-level AI tool. It helps them build software that can support pilots, partnerships, and enterprise healthcare adoption.
C. Integrating Radiology AI Into Enterprise Platforms
Enterprise healthcare platforms often need AI modules that connect with existing systems instead of replacing them. Intellivon builds API-based AI radiology components that can fit into larger healthcare, imaging, hospital management, or clinical workflow platforms.
- API-based AI modules: We build AI services that can analyze imaging data and return structured outputs to existing platforms.
- Imaging workflow automation: We automate case routing, prioritization, review status updates, and escalation workflows.
- Enterprise integrations: We connect AI radiology modules with PACS, RIS, EHR, reporting systems, and internal healthcare platforms.
- Security controls: We implement role-based access, encrypted data flows, secure APIs, and access logs.
- Model monitoring: We add dashboards to track AI performance, drift, false positives, false negatives, and usage patterns.
- Long-term scaling: We design the platform to support higher scan volumes, more users, multiple facilities, and future AI models.
This approach helps enterprise teams add radiology AI without creating fragmented systems or weakening operational control.
D. Why Choose Intellivon For Radiology AI Development?
AI radiology software must perform in real clinical conditions. That means the system needs strong engineering, secure integrations, usable workflows, and governance from the beginning.
Intellivon brings together AI development, healthcare software engineering, system integration, cloud architecture, and enterprise-grade security to build radiology AI platforms that are ready for real-world use.
Our approach focuses on:
- Building AI around hospital workflows, not forcing hospitals around AI
- Connecting imaging data with PACS, RIS, EHR, and reporting systems
- Keeping radiologists in control of review and final decisions
- Designing audit-ready workflows for better governance
- Supporting secure deployment across hospital environments
- Creating scalable architecture for future modalities and AI models
If your hospital, imaging network, healthtech company, or enterprise healthcare team is planning to build AI radiology software in 2026, Intellivon can help you design, develop, integrate, and scale a secure platform built for real clinical workflows.
Contact Intellivon to discuss your AI radiology software development project.
FAQs
Q1. What is the first step to building AI radiology software?
A1. The first step is defining the clinical use case. Hospitals should decide whether the software will support triage, abnormality detection, reporting, segmentation, or workflow automation. This helps the development team plan imaging data, AI models, PACS/RIS integration, radiologist review flows, and governance requirements from the start.
Q2. Can AI radiology software integrate with existing PACS?
A2. Yes. AI radiology software can integrate with existing PACS using DICOM, DICOMweb, secure APIs, and image routing workflows. This allows scans to move between imaging systems, AI models, radiologist dashboards, and reporting tools without forcing teams to manually upload or manage images.
Q3. Does AI radiology software replace radiologists?
A3. No. AI radiology software supports radiologists by prioritizing urgent cases, flagging possible findings, assisting with reports, and improving workflow speed. Final interpretation, validation, and reporting should remain radiologist-led, especially in hospital environments where clinical accountability and patient safety are critical.
Q4. What features should hospital radiology AI include?
A4. Hospital radiology AI should include DICOM image ingestion, PACS/RIS integration, AI detection, confidence scores, radiologist review dashboards, critical alerts, reporting support, audit logs, access controls, and model monitoring. These features help the software work inside real imaging workflows instead of becoming another disconnected AI tool.