Most hospital executives are making important operational decisions based on data that’s already hours old. ED capacity reaches critical levels at 2 PM, but the dashboard doesn’t update until the nightly batch runs. At the same time, the staffing shortages only show up after patients are already waiting.
Real-time KPI dashboards address a specific issue, which is turning operational data into useful information before problems escalate. The technical challenge lies in integrating feeds from ADT systems, bed management platforms, and staffing software without creating weak point-to-point connections that fail during routine updates.
At Intellivon, we have built real-time dashboards for multi-facility health systems that process over 50,000 transactions daily, achieving refresh rates in less than a second. What sets apart platforms that can scale from those that cannot is their structure.
These systems are designed to handle EMR migrations, onboarding new facilities, and changing regulatory requirements without needing complete rebuilds. In this blog, we will draw from our experience and show you how we build such dashboards from scratch.
Key Takeaways Of The Healthcare Dashboard Tools Market
Healthcare KPI dashboards track key metrics like patient outcomes, operational efficiency, and financial performance. They help teams see what is working and where risks are growing. As healthcare operations become more complex, these dashboards help leaders act faster and make better decisions.
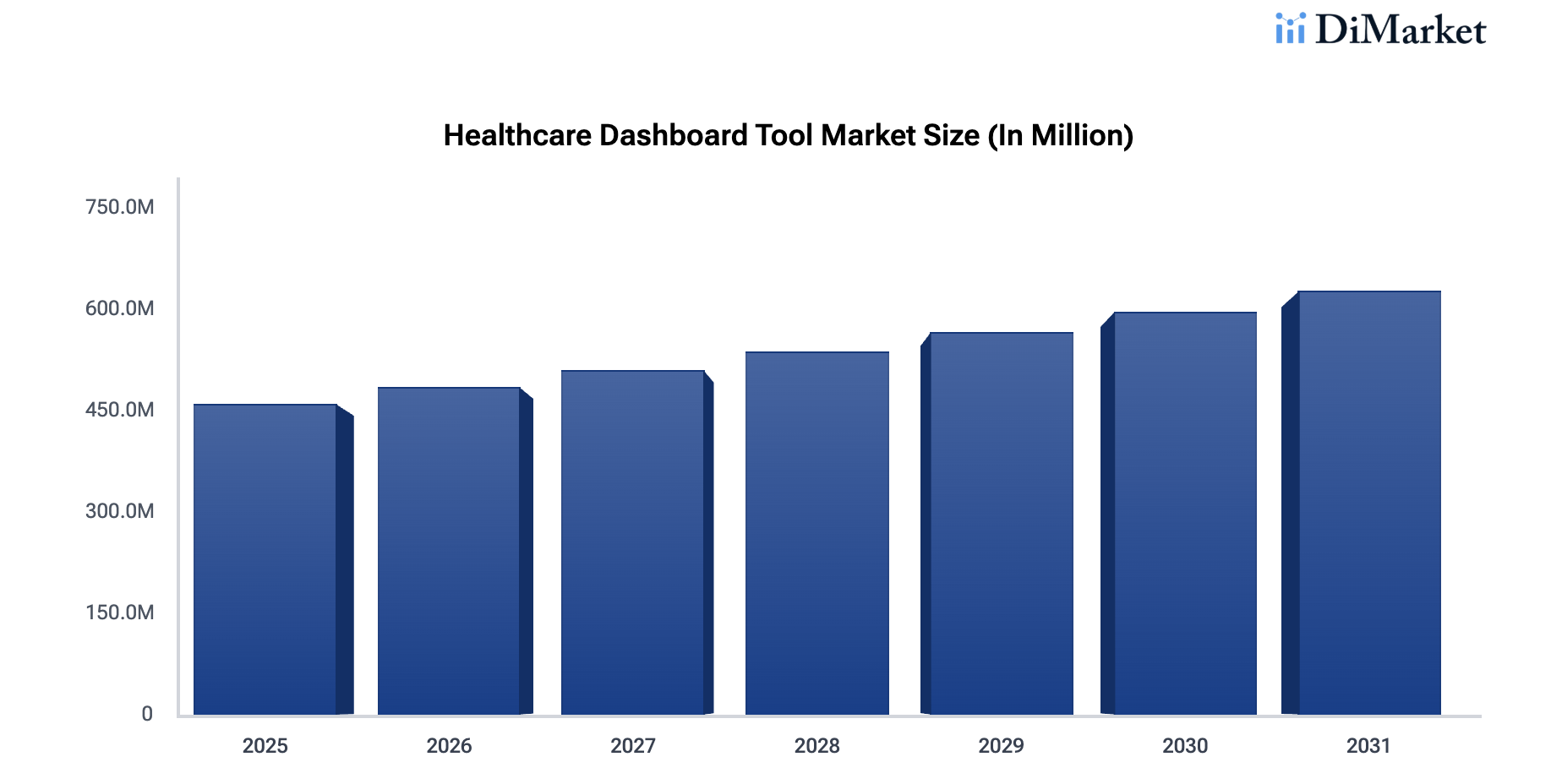
In fact, the global healthcare dashboard tools market was valued at USD 415 million in 2025. It is expected to reach USD 659.2 million by 2033. This reflects a steady CAGR of 5.3% between 2025 and 2033.
Market Insights:
- The shift to value-based care and preventive medicine is increasing the need for real-time KPI monitoring. Healthcare teams need live visibility to manage outcomes and costs effectively.
- In addition, AI is helping predict trends in bed occupancy, staffing needs, and readmission risks. This allows teams to plan resources earlier and reduce operational pressure.
- At the same time, cloud adoption, telehealth growth, and interoperability requirements such as the 21st Century Cures Act are accelerating the demand for connected, real-time data systems.
About 71% of hospitals used predictive AI in 2024, up from 66% in 2023. These models are used for things like readmission risk, treatment planning, scheduling, and billing automation.
What Are Real-Time Hospital KPI Dashboards?
Real-time hospital KPI dashboards are digital tools that show live performance data across clinical, operational, and financial areas. They pull data continuously from hospital systems and update metrics as events happen.
This helps teams detect risks early, respond faster, and manage resources better. Therefore, hospitals can improve patient care, reduce delays, and control costs using accurate, up-to-date operational insights across departments and decision levels.
Why Real-Time KPI Dashboards Are Becoming Mission-Critical for Hospitals
Healthcare operations are becoming faster, more complex, and more data-dependent. Therefore, hospitals need live visibility into performance across care delivery, operations, and finances.
Static reports no longer support daily decision cycles. Real-time KPI dashboards help teams detect risks early, respond faster, and maintain stable performance during demand changes.
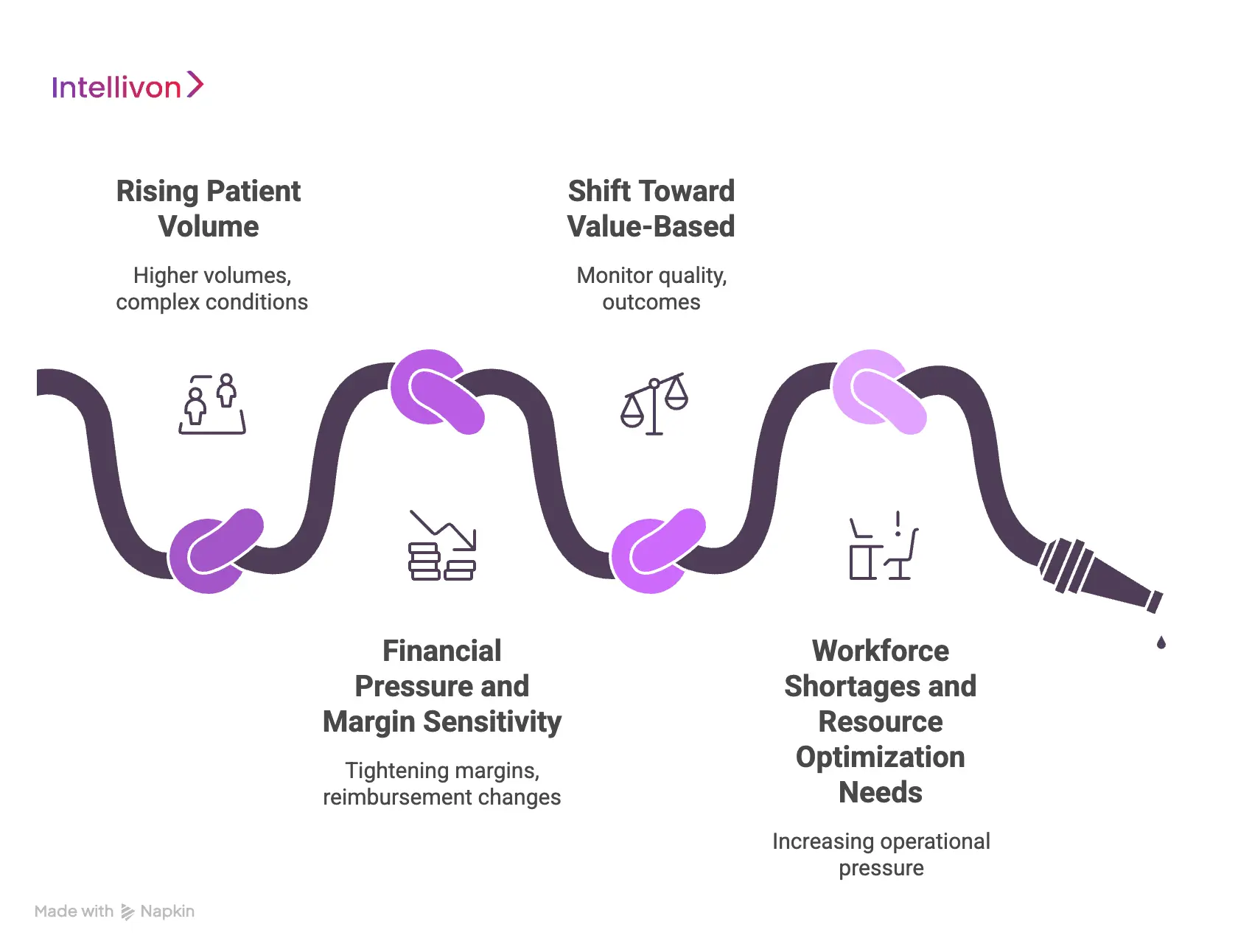
1. Rising Patient Volume
Hospitals are managing higher patient volumes with more complex conditions. In addition, care coordination now involves multiple departments and external partners.
Real-time dashboards help teams track patient flow, bed capacity, and care delays as they happen. This improves response speed and reduces operational bottlenecks.
2. Financial Pressure and Margin Sensitivity
Healthcare margins are tightening due to rising costs and reimbursement changes. Therefore, hospitals must monitor revenue cycle performance continuously.
Real-time KPI visibility helps detect claim delays, denial spikes, and billing gaps early. This supports faster financial recovery and better cash flow stability.
3. Shift Toward Value-Based
Healthcare payment models are moving toward outcomes and quality metrics. As a result, hospitals must monitor quality indicators and patient outcomes continuously. Real-time dashboards help teams correct performance issues before they impact quality scores or reimbursement outcomes.
4. Workforce Shortages and Resource Optimization Needs
Staff shortages are increasing operational pressure across hospitals. Therefore, leaders need real-time insight into staffing gaps, overtime risks, and workload imbalance. Live dashboards help teams adjust staffing decisions quickly and maintain safe care delivery levels.
Real-time KPI dashboards are becoming essential because hospitals must operate with live performance visibility. They help organizations protect patient outcomes, maintain financial stability, and manage operations proactively in a rapidly changing healthcare environment.
What “Real-Time” Means in Hospital KPI Dashboards
In healthcare, real-time means data updates fast enough to support immediate decisions. In addition, live data helps hospitals manage care delivery, staffing, and revenue performance more accurately.
As operations become more complex, real-time visibility is becoming essential for stable hospital performance.
1. Live Data From Multiple Hospital Systems
Real-time dashboards collect data continuously from EHRs, devices, and operational platforms. As patient and workflow events happen, metrics update automatically. Therefore, teams always see the latest operational and clinical conditions.
In addition, this reduces dependence on manual reporting and delayed data extracts. As a result, leaders can respond faster to capacity or care delivery changes. This improves coordination across departments and reduces operational blind spots.
2. Event-Based KPI Tracking
Real-time dashboards monitor events such as admissions, discharges, transfers, and clinical alerts. When these events occur, KPIs update immediately. Therefore, teams can detect patient flow risks much earlier. In addition, staff can respond quickly to care delays or operational bottlenecks.
As a result, hospitals can reduce wait times and improve patient throughput. This also helps teams manage sudden demand spikes more effectively.
3. Near-Instant Performance Visibility
In most hospitals, real-time means updates happen within seconds or minutes. This is critical for emergency care, bed management, and staffing adjustments. Therefore, teams can act before performance metrics start declining.
In addition, faster visibility supports better resource allocation during peak demand. As a result, hospitals can maintain stable operations even during high patient volumes. This improves both care quality and patient experience.
4. Decision-Ready Data, Not Just Fast Data
Real-time dashboards focus on showing data that teams can act on immediately. They highlight risks, workflow delays, and performance gaps. Therefore, leaders can make faster clinical and operational decisions. In addition, finance teams can detect revenue risks earlier.
As a result, hospitals can shift from reactive management to proactive operations. This improves long-term operational and financial stability.
Real-time hospital KPI dashboards help hospitals see and act on performance data as events happen. Therefore, teams can prevent delays, reduce risks, and improve coordination across departments.
Core Real-Time KPIs Hospitals Should Track
Hospitals track KPIs to protect patient outcomes, financial stability, and daily operations. However, not all metrics need real-time monitoring. Real-time KPI dashboards should focus on signals that help teams act immediately.
Therefore, hospitals must prioritize KPIs linked to patient risk, capacity pressure, revenue leakage, and workforce strain. In addition, tracking fewer high-impact KPIs improves decision speed and reduces alert overload.
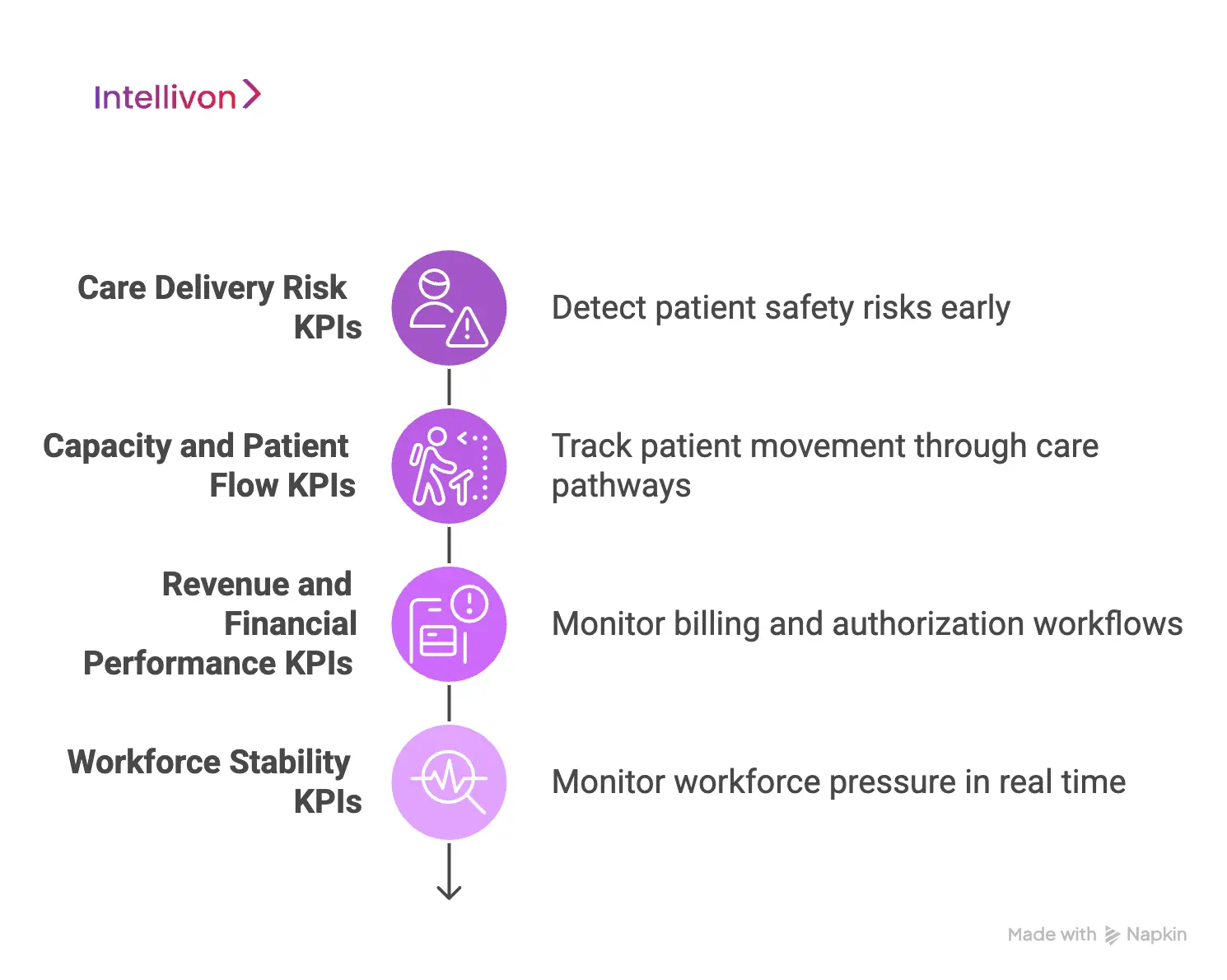
1. Care Delivery Risk KPIs
These KPIs help hospitals detect patient safety risks early. Therefore, teams can intervene before care quality declines. In addition, real-time monitoring supports faster clinical coordination across departments.
As patient volumes and complexity increase, these metrics help maintain safe care delivery standards.
Key Real-Time KPIs Include:
- Emergency department wait time drift
- Length of stay deviation patterns
- ICU bed capacity risk levels
- Clinical deterioration alert delays
These metrics help hospitals protect patient outcomes and reduce preventable complications.
2. Capacity and Patient Flow KPIs
Patient flow directly impacts care quality, staff workload, and revenue. Therefore, hospitals must track how quickly patients move through care pathways. In addition, real-time flow visibility helps teams prevent bottlenecks during demand surges.
As a result, hospitals can maintain stable operations even during peak patient loads.
Key Real-Time KPIs Include:
- Bed turnover time
- Patient boarding time
- Transfer delays between departments
- Operating room utilization drift
These metrics help hospitals maximize throughput while maintaining care quality.
3. Revenue and Financial Performance KPIs
Revenue cycle delays can create hidden financial losses. Therefore, hospitals need real-time visibility into billing and authorization workflows. In addition, early detection of revenue risks improves cash flow stability.
As reimbursement models become more complex, real-time monitoring becomes more valuable.
Key Real-Time KPIs Include:
- Discharge-to-bill time lag
- Prior authorization queue aging
- Denial rate spike detection
- Charge capture completion gaps
These metrics help hospitals reduce revenue leakage and improve financial predictability.
4. Workforce Stability KPIs
Staffing stability directly impacts patient safety and operational cost. Therefore, hospitals must monitor workforce pressure in real time.
In addition, early detection of staffing risks helps prevent burnout and overtime spikes. As workforce shortages continue, these metrics support safer staffing decisions.
Key Real-Time KPIs Include:
- Nurse-to-patient ratio risk levels
- Shift coverage gaps
- Overtime surge patterns
- Workload imbalance indicators
These metrics help hospitals maintain safe staffing while controlling labor costs.
The most valuable real-time KPIs are the ones that help teams act immediately. Therefore, hospitals should focus on metrics linked to patient risk, flow delays, revenue performance, and staffing stability.
In addition, tracking the right KPIs helps reduce alert fatigue and improve decision confidence. As healthcare operations become more complex, real-time KPI monitoring is becoming essential for stable and efficient hospital performance.
Architecture Required to Build Real-Time Hospital KPI Dashboards
Building real-time hospital KPI dashboards requires more than visualization tools. It needs a strong data and processing foundation. Therefore, hospitals must design architecture that can move, process, and display data continuously.
In addition, the system must support compliance, security, and audit tracking. As real-time decision needs increase, architecture stability becomes critical for long-term performance. Below is a simplified layer-based architecture used in enterprise hospital environments.
1. Data Source Layer
This layer includes all systems where hospital data is generated. These systems produce clinical, operational, and financial data every second. Therefore, real-time dashboards must connect to multiple data sources at the same time.
In addition, data must be captured without disrupting clinical workflows. As hospitals expand digital systems, this layer continues to grow.
Typical Data Sources Include:
- Electronic Health Records (EHRs)
- Medical devices and monitoring systems
- Laboratory and imaging systems
- Bed management and scheduling platforms
- Revenue cycle and billing systems
This layer ensures dashboards receive accurate raw data from across the hospital ecosystem.
2. Data Integration and Streaming Layer
This layer moves data from source systems into real-time processing pipelines. Therefore, data must be transferred quickly and securely.
In addition, the system must handle large volumes of clinical and operational events. As hospital activity changes throughout the day, streaming systems must scale automatically.
Key Capabilities Include:
- HL7 and FHIR data integration
- Event streaming and message processing
- Real-time data transformation and normalization
- Change data capture from operational systems
This layer ensures continuous data flow without delays or data loss.
3. Real-Time Processing and Analytics Layer
This layer converts raw data into meaningful KPIs and alerts. Therefore, the system must process data instantly as events happen.
In addition, rules and clinical logic must be applied to detect risks. As predictive analytics adoption increases, this layer supports AI-driven insights.
Key Functions Include:
- KPI calculation engines
- Clinical threshold monitoring
- Predictive risk detection models
- Alert trigger and notification logic
This layer turns data into decision-ready intelligence.
4. Dashboard and Visualization Layer
This layer displays KPIs in an easy-to-understand format. Therefore, dashboards must show only the most important metrics. In addition, role-based views help teams see data relevant to their work.
As hospitals move toward command center models, this layer becomes a decision interface.
Key Capabilities Include:
- Real-time KPI dashboards
- Role-based access views
- Command center monitoring screens
- Mobile and remote dashboard access
This layer helps teams monitor performance and act quickly.
5. Governance, Security, and Compliance Layer
Healthcare data requires strict security and audit controls. Therefore, real-time dashboard systems must include governance from the start.
In addition, access control and audit logging must work continuously. As regulatory requirements grow, this layer protects hospitals from compliance risks.
Key Capabilities Include:
- PHI data protection and encryption
- Role-based data access control
- Audit trail logging
- Consent and regulatory compliance monitoring
This layer ensures safe and compliant real-time data usage.
Real-time hospital KPI dashboards depend on strong, well-designed architecture. Therefore, hospitals must build systems that support continuous data movement, processing, and secure access.
In addition, layered architecture improves scalability and reliability. As real-time decision-making becomes standard in healthcare, strong architecture will determine long-term dashboard success.
Governance, Compliance Requirements for Real-Time KPI Dashboards
Real-time hospital KPI dashboards must protect sensitive data while supporting fast decisions. Therefore, governance and compliance cannot be added later. They must be built into the architecture from the beginning.
In addition, real-time systems must track how data is used, who accesses it, and how decisions are made. As regulatory pressure increases, strong governance helps hospitals avoid legal, financial, and reputational risks. Below are the core governance and compliance areas hospitals must address.
1. Data Privacy and PHI Protection
Healthcare dashboards process protected health information continuously. Therefore, data must be encrypted during transfer and storage.
In addition, access must be limited to authorized users only. As more systems connect in real time, privacy controls must work across all data flows.
Key Requirements Include:
- End-to-end data encryption
- Secure data transmission protocols
- PHI masking where required
- Continuous data access monitoring
This ensures patient data stays protected while supporting real-time analytics.
2. Role-Based Access and Identity Control
Not every user should see all hospital data. Therefore, dashboards must provide role-based data access.
In addition, identity verification must work across systems and locations. As remote access and multi-site operations grow, identity control becomes more important.
Key Requirements Include:
- Role-based dashboard views
- Multi-factor authentication
- Identity federation across systems
- Session monitoring and access logging
This ensures the right data is visible to the right people at the right time.
3. Audit Trails and Decision Traceability
Hospitals must track how data is used and how decisions are made. Therefore, dashboards must log user activity continuously.
In addition, audit logs must support compliance reporting and investigations. As real-time decision systems expand, audit traceability becomes critical.
Key Requirements Include:
- User activity logging
- KPI access and modification tracking
- Alert response documentation
- Automated compliance reporting
This helps hospitals demonstrate regulatory compliance and operational accountability.
4. Regulatory Compliance and Data Governance Policies
Healthcare dashboards must follow regional and national healthcare regulations. Therefore, systems must support regulatory reporting and policy enforcement.
In addition, governance frameworks must define how data is stored, shared, and retained. As healthcare regulations evolve, dashboards must adapt without disrupting operations.
Key Requirements Include:
- HIPAA and regional data compliance controls
- Data retention and deletion policies
- Consent-based data sharing controls
- Cross-border data governance monitoring
This ensures hospitals remain compliant while expanding digital capabilities.
5. Real-Time Risk Monitoring and Security Threat Detection
Real-time systems must detect security risks as they happen. Therefore, dashboards must integrate with security monitoring tools. In addition, anomaly detection helps identify unusual access or data activity.
As cyber threats increase in healthcare, real-time security monitoring becomes essential.
Key Requirements Include:
- Real-time access anomaly detection
- Security event monitoring integration
- Automated threat alerting
- Incident response workflow integration
This protects hospitals from cyber risks while maintaining real-time operations.
Governance and compliance are critical for real-time hospital KPI dashboards. Therefore, hospitals must build privacy, access control, and audit tracking into the system architecture.
In addition, strong governance improves data trust and decision confidence.
AI and Predictive Intelligence in Real-Time Hospital KPI Platforms
AI is helping hospitals move from monitoring performance to predicting risks. Therefore, real-time KPI dashboards are now becoming early warning systems. In addition, predictive intelligence helps hospitals prepare for demand changes before they happen.
As healthcare data volumes grow, AI helps teams detect patterns that are difficult to identify manually. Below are the key ways AI supports real-time hospital KPI platforms:
1. Predicting Patient Flow and Capacity Demand
AI models can analyze historical and real-time data together. Therefore, hospitals can predict patient admissions, discharge delays, and bed demand earlier. In addition, predictive models help hospitals prepare for seasonal spikes and emergency surges.
As patient demand becomes less predictable, forecasting helps maintain stable operations.
Common Predictive Use Cases Include:
- Bed occupancy forecasting
- Emergency department volume prediction
- Discharge delay risk prediction
- ICU capacity risk forecasting
This helps hospitals prevent overcrowding and maintain patient care quality.
2. Early Detection of Clinical Deterioration Risks
AI can monitor clinical signals and patient data continuously. Therefore, dashboards can detect early signs of patient deterioration. In addition, predictive alerts help clinical teams intervene earlier.
As real-time monitoring improves, hospitals can reduce preventable complications.
Common Predictive Use Cases Include:
- Sepsis risk prediction
- Readmission risk prediction
- Patient deterioration risk alerts
- Medication risk interaction monitoring
This improves patient outcomes and reduces emergency escalations.
3. Workforce and Staffing Demand Prediction
AI can analyze staffing patterns, patient volumes, and workload trends. Therefore, hospitals can predict staffing shortages earlier. In addition, predictive workforce planning helps reduce overtime and burnout risk.
As staffing challenges continue, predictive planning supports safer staffing decisions.
Common Predictive Use Cases Include:
- Shift demand forecasting
- Over time, risk prediction
- Nurse workload balancing prediction
- Department staffing pressure alerts
This helps hospitals manage labor costs and maintain care quality.
4. Revenue Risk and Financial Performance Prediction
AI helps hospitals detect financial risks before they impact revenue. Therefore, dashboards can predict claim delays, denial risks, and billing gaps. In addition, predictive financial analytics helps improve cash flow planning.
As reimbursement complexity increases, predictive finance monitoring becomes more valuable.
Common Predictive Use Cases Include:
- Claim denial risk prediction
- Prior authorization delay prediction
- Billing backlog risk alerts
- Revenue leakage pattern detection
This supports stronger financial performance and faster revenue recovery.
AI and predictive intelligence are transforming real-time hospital KPI dashboards. Therefore, hospitals can move from reactive monitoring to proactive decision-making.
As healthcare complexity grows, AI-powered KPI platforms will help hospitals operate more efficiently and improve long-term performance.
How We Develop Real-Time Hospital KPI Dashboards
At Intellivon, we develop real-time hospital KPI dashboards as enterprise data platforms, not reporting tools.
Therefore, every implementation starts with understanding how decisions are made inside the hospital. In addition, we focus on building systems that support real-time operations, compliance, and long-term scalability. Below is the structured approach we follow.
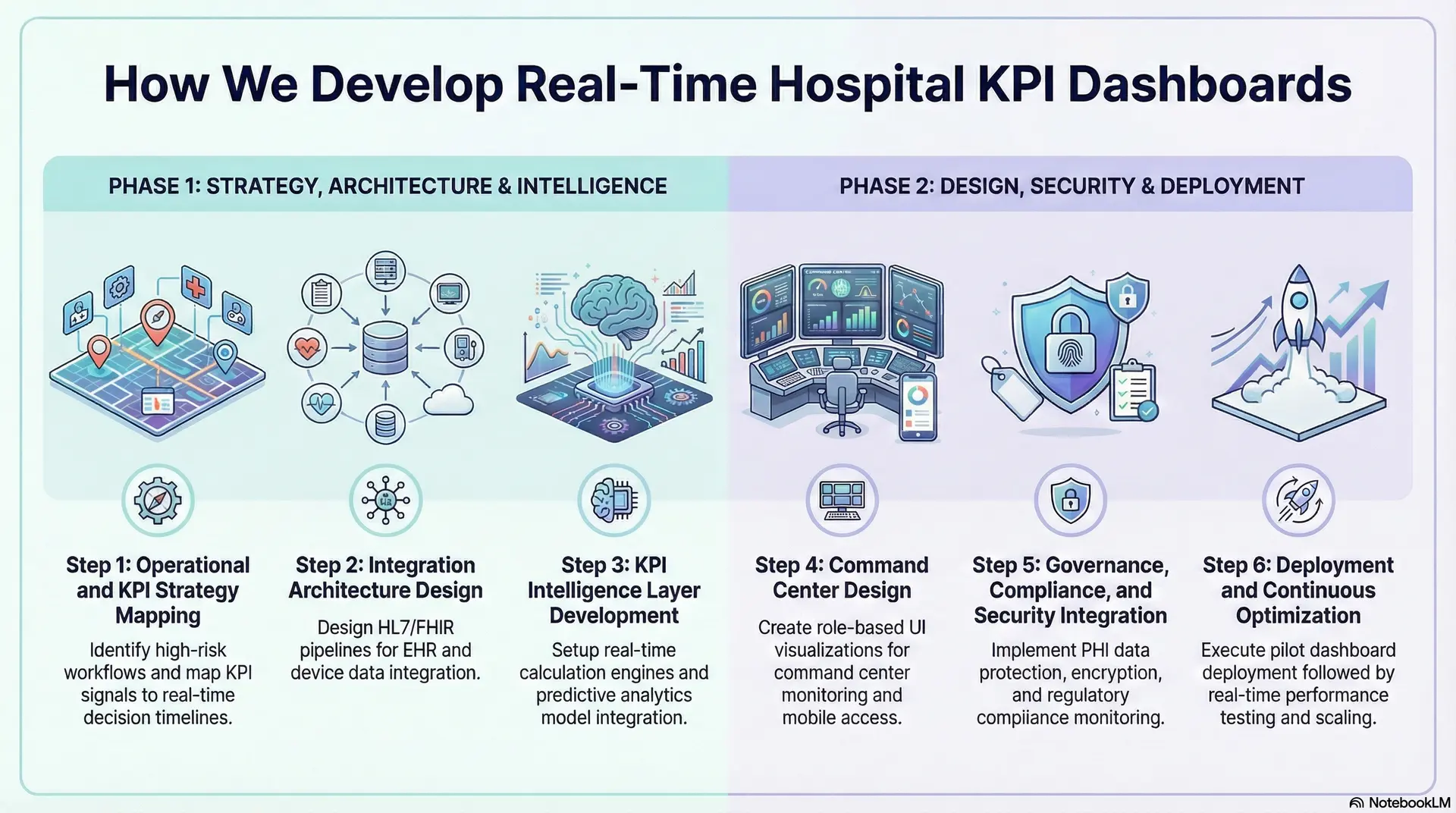
Step 1: Operational and KPI Strategy Mapping
We start by understanding how the hospital operates day to day. Therefore, we identify which decisions require real-time visibility.
In addition, we work with clinical, operational, and finance teams to define high-impact KPIs. As a result, dashboards are built around real decision workflows, not generic metrics.
Key Activities Include:
- Identifying high-risk operational workflows
- Mapping KPI signals to decision timelines
- Defining real-time alert thresholds
- Aligning KPI definitions across departments
This ensures dashboards support real hospital operations from day one.
Step 2: Integration Architecture Design
Next, we design how data will move across systems in real time. Therefore, we map all required clinical, operational, and financial data sources.
In addition, we design integration pipelines using healthcare data standards. As hospitals expand digital ecosystems, this step ensures reliable data connectivity.
Key Activities Include:
- EHR and device data integration planning
- HL7 and FHIR interface design
- Event streaming architecture setup
- Data quality and validation controls
This ensures dashboards receive accurate and continuous data.
Step 3: KPI Intelligence Layer Development
We then build the processing layer that converts raw data into decision-ready KPIs. Therefore, the system processes events as they happen.
In addition, we apply clinical rules and predictive intelligence models. As real-time data volume grows, this layer ensures performance and stability.
Key Activities Include:
- Real-time KPI calculation engine setup
- Clinical and operational threshold logic development
- Predictive analytics model integration
- Alert and notification workflow design
This turns data into real-time operational intelligence.
Step 4: Command Center Design
Next, we build dashboards that support fast and clear decision-making. Therefore, we design role-based dashboard views. In addition, we optimize dashboards for command center environments and mobile access.
As hospitals move toward centralized monitoring models, this step improves usability and adoption.
Key Activities Include:
- Real-time dashboard UI and visualization design
- Role-based access view configuration
- Command center monitoring layout development
- Mobile and remote dashboard enablement
This ensures teams can act quickly using clear and reliable data.
Step 5: Governance, Compliance, and Security Integration
We embed governance and compliance controls directly into the platform. Therefore, privacy, audit tracking, and access control work continuously.
In addition, security monitoring integrates with real-time data pipelines. As healthcare regulations evolve, this step protects long-term system compliance.
Key Activities Include:
- PHI data protection and encryption implementation
- Role-based data access configuration
- Audit trail and decision logging setup
- Regulatory compliance monitoring integration
This ensures safe and compliant real-time dashboard operations.
Step 6: Deployment and Continuous Optimization
Finally, we deploy dashboards in phases to reduce operational risk. Therefore, hospitals can validate KPIs before full rollout.
In addition, we continuously monitor performance and improve predictive models. As hospital needs change, the platform evolves without disruption.
Key Activities Include:
- Pilot dashboard deployment and validation
- Real-time performance testing
- KPI accuracy and alert tuning
- Continuous improvement and system scaling
This ensures long-term dashboard reliability and performance.
Developing real-time hospital KPI dashboards requires strategy, architecture, and operational alignment. Therefore, hospitals need partners who understand both technology and healthcare workflows.
At Intellivon, we build real-time KPI platforms that support safer care delivery, stronger financial performance, and stable operations.
Common Mistakes Hospitals Make When Building KPI Dashboards
Many hospitals invest in KPI dashboards but fail to get real operational value. This usually happens because dashboards are built as reporting tools instead of decision systems.
Therefore, teams see data but cannot act on it fast enough. In addition, poor integration, weak governance, and unclear KPI strategy reduce dashboard trust. As real-time decision needs increase, avoiding these mistakes becomes critical for long-term success.
1. Building Dashboards Only for Reporting
Many hospitals design dashboards to show historical performance trends. However, real-time operations need live decision signals. When dashboards focus only on reporting, teams cannot prevent risks early.
Therefore, dashboards become passive monitoring tools instead of operational support systems.
How We Solve This
At Intellivon, we design dashboards around real-time decision workflows. In addition, we map KPIs to actions teams must take immediately. As a result, dashboards support daily operational decisions, not just performance reporting.
2. Tracking Too Many KPIs
Some hospitals try to monitor too many metrics at once. However, this creates alert fatigue and confusion. When teams receive too many signals, they start ignoring dashboards. Therefore, decision speed and data trust both decline.
How We Solve This
We focus on high-impact KPIs linked to patient risk, flow stability, and revenue performance. In addition, we design alert prioritization models. As a result, teams see fewer but more meaningful signals.
3. Ignoring Real-Time Data Integration Challenges
Hospitals often underestimate the complexity of real-time data integration. However, data delays, mismatched formats, and incomplete records reduce dashboard accuracy. Therefore, teams lose confidence in real-time insights.
How We Solve This
We build integration architecture using healthcare data standards and real-time streaming pipelines. In addition, we apply data validation and quality monitoring. As a result, dashboards deliver accurate and reliable real-time data.
4. Weak Governance and Compliance Controls
Some hospitals add security and compliance controls after deployment. However, real-time systems require governance from the start. Without strong controls, hospitals face privacy and regulatory risks. Therefore, dashboards may fail compliance audits.
How We Solve This
We embed governance, access control, and audit logging into the platform architecture. In addition, we design dashboards to support regulatory reporting. As a result, hospitals maintain compliance while using real-time data.
5. Poor Dashboard Adoption and Training Strategy
Even well-built dashboards fail if teams do not trust or understand them. However, many hospitals focus only on technical deployment. Therefore, adoption remains low, and ROI is limited.
How We Solve This
We support phased rollout, user training, and workflow-based dashboard design. In addition, we align dashboards with real user needs. As a result, teams adopt dashboards faster and trust real-time data.
Hospitals often struggle with KPI dashboards because they focus on tools instead of decision workflows. Therefore, successful dashboard programs require strong integration, governance, and KPI strategy.
Conclusion
Real-time KPI dashboards help hospitals move from delayed reporting to faster, data-driven decisions. Therefore, teams can reduce risks, improve patient outcomes, and protect financial performance. In addition, real-time visibility helps hospitals manage staffing, patient flow, and revenue operations more effectively.
As healthcare becomes more complex, real-time KPI platforms will support both operational stability and long-term growth. With the right partner, hospitals can turn real-time data into a strong competitive advantage.
Build Real-Time Hospital KPI Dashboard Platforms With Intellivon
At Intellivon, real-time hospital KPI dashboard platforms are built as regulated healthcare data infrastructure designed for continuous, decision-ready visibility across clinical, operational, and financial systems.
Every architecture and delivery decision prioritizes governance, data accuracy, identity control, and audit-ready KPI access. As real-time monitoring expands across departments, facilities, and partner systems, platforms maintain performance, reliability, and compliance without creating data silos or operational risk.
Why Partner With Intellivon?
- Enterprise-grade real-time KPI platform architecture for multi-EHR, multi-department, and multi-facility healthcare environments
- Proven delivery across hospital networks, command centers, and enterprise performance monitoring programs
- Compliance-by-design architecture with automated audit logging, access control, and regulatory traceability
- Advanced real-time data orchestration across clinical, operational, and financial hospital systems
- Real-time KPI monitoring across streaming, event-driven, and API-based healthcare data models
- Scalable KPI onboarding and governance-driven metric lifecycle management workflows
- AI-ready KPI infrastructure supporting predictive analytics, automation, and operational forecasting
Book a strategy call to explore how Intellivon can help you design and scale real-time hospital KPI dashboard platforms with confidence, compliance control, and long-term enterprise value.
FAQs
Q1. What is a real-time hospital KPI dashboard?
A1. A real-time hospital KPI dashboard shows live performance data across clinical, operational, and financial areas. It updates metrics continuously as events happen. Therefore, hospitals can detect risks early and respond faster.
In addition, real-time dashboards help improve patient outcomes, operational efficiency, and revenue performance using current data instead of delayed reports.
Q2. How are real-time KPI dashboards different from traditional hospital dashboards?
A2. Traditional dashboards usually show historical or batch-processed data. However, real-time dashboards update metrics within seconds or minutes. Therefore, teams can act immediately instead of reviewing past performance.
In addition, real-time dashboards support live operational decisions, which help hospitals prevent delays, reduce risks, and improve patient flow.
Q3. What data sources are needed to build real-time hospital KPI dashboards?
A3. Real-time hospital dashboards require data from EHRs, medical devices, laboratory systems, scheduling platforms, and revenue cycle tools. In addition, integration standards such as HL7 and FHIR help connect systems.
Therefore, hospitals can combine clinical, operational, and financial data into a single real-time performance view.
Q4. How do hospitals ensure compliance when using real-time KPI dashboards?
A4. Hospitals ensure compliance by using encryption, role-based access control, audit logging, and consent management. In addition, governance policies define how data is accessed and shared.
Therefore, hospitals can use real-time data safely while meeting regulatory requirements such as HIPAA and regional healthcare privacy laws.
Q5. How long does it take to implement a real-time hospital KPI dashboard platform?
A5. Implementation time depends on system complexity, data integration needs, and hospital size. Most enterprise implementations take several months from design to full deployment.
However, phased rollouts allow hospitals to start using real-time KPIs earlier. Therefore, hospitals can begin seeing operational improvements before full platform completion.






