Revenue leakage in healthcare rarely makes itself obvious. It builds up quietly, hidden in claim queues that no one audits, in eligibility checks that occur too late, and in denial patterns that repeat month after month without resolution. For healthcare organizations processing thousands of encounters each week, that leakage adds up to something much more damaging than just an operational hassle.
When serious investors and enterprise operators consider healthcare RCM software development, they view it as a system that directly affects whether a healthcare business receives accurate, timely payments at scale. The difference between a well-designed RCM platform and a makeshift billing process is clear in collection rates, staffing costs, and relationships with payers.
Intellivon has addressed this issue at the enterprise level. In this blog, we explain how we build healthcare RCM software that scales with the enterprise. We discuss the critical decisions, common development pitfalls, and what a serious, scalable build looks like from the ground up.
Why Healthcare RCM Needs To Be Revised In 2026
Legacy RCM tools were built for transaction processing, not real-time analytics or AI-driven denial management. As a result, they struggle at enterprise scale.
They slow down workflows, limit visibility, and increase manual effort. Over time, they shift from revenue enablers to cost centers, instead of helping organizations optimize financial performance.
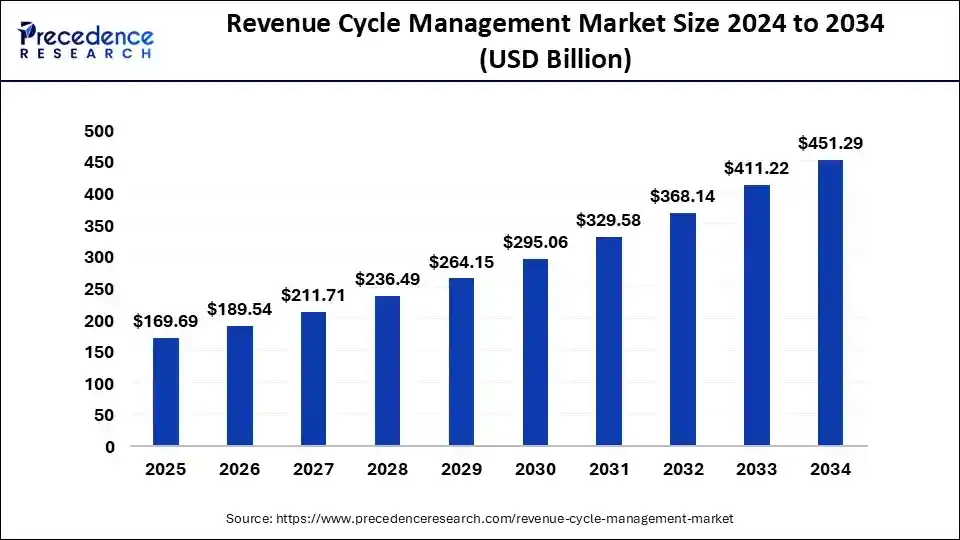
The financial landscape for healthcare providers is shifting toward a model where traditional administrative methods are no longer sustainable. Investing in modernized Revenue Cycle Management (RCM) is now a strategic necessity to protect margins and ensure long-term scalability.
1. Why legacy RCM systems fail at scale
Legacy platforms often operate on rigid architectures that cannot handle the massive data volumes of modern health systems. These aging infrastructures lack the elasticity required to integrate with diverse Electronic Health Record (EHR) updates seamlessly.
Consequently, bottlenecks occur during high-volume periods, leading to delayed billing cycles and increased operational costs. Reliance on manual data entry within these systems creates a significant risk of human error.
Furthermore, outdated security protocols in older software struggle to meet the evolving demands of global data privacy regulations.
2. Revenue leakage across disconnected systems
Information silos are the primary cause of lost profits in large-scale healthcare organizations. When patient registration, clinical documentation, and billing departments use fragmented tools, critical data often disappears during transfers.
These gaps result in undercoding or missed charges that directly impact the bottom line. Therefore, a unified digital thread is essential to capture every dollar earned.
Without a centralized source of truth, auditing becomes an expensive and reactive process rather than a proactive financial safeguard.
3. Rising complexity in payer workflows
Insurance providers constantly update their reimbursement policies, making manual compliance nearly impossible for administrative staff. The variety of documentation requirements across different payers creates a chaotic environment for billing teams.
In addition, the shift toward value-based care introduces new metrics that traditional RCM tools were never designed to track. However, advanced software can ingest these complex rule sets automatically.
This automation ensures that submissions align with the latest criteria, significantly reducing the likelihood of initial claim rejections.
4. Why enterprises shift to custom RCM
Off-the-shelf solutions rarely align with the unique operational workflows of a sophisticated enterprise. Custom-built RCM software allows leaders to bake their specific business logic directly into the application.
This tailored approach enables better control over data ownership and provides deeper insights through proprietary analytics. In addition, custom platforms offer the flexibility to scale features as the organization grows into new markets.
By owning the technology stack, enterprises gain a competitive advantage and avoid the limitations of vendor lock-in.
Modernizing your RCM infrastructure is the most effective way to turn administrative hurdles into a reliable engine for financial growth. Custom solutions provide the precision and agility required to thrive in a highly regulated and competitive market.
What Is A Healthcare RCM Software?
Healthcare Revenue Cycle Management (RCM) software is an enterprise-grade financial platform that automates the patient lifecycle. It unifies clinical and administrative data to manage billing, from initial scheduling to final payment collection.
Consequently, it streamlines claim submissions, tracks reimbursements, and ensures regulatory compliance while minimizing manual errors and revenue loss.
How An RCM Cycle Works End-To-End
Healthcare revenue cycle management starts long before a claim is submitted. It begins when a patient first interacts with a provider and continues until the final payment is collected and recorded. In practice, every stage affects cash flow, claim accuracy, and operational efficiency.
Here is the end-to-end revenue cycle explained as a clear step-by-step process.
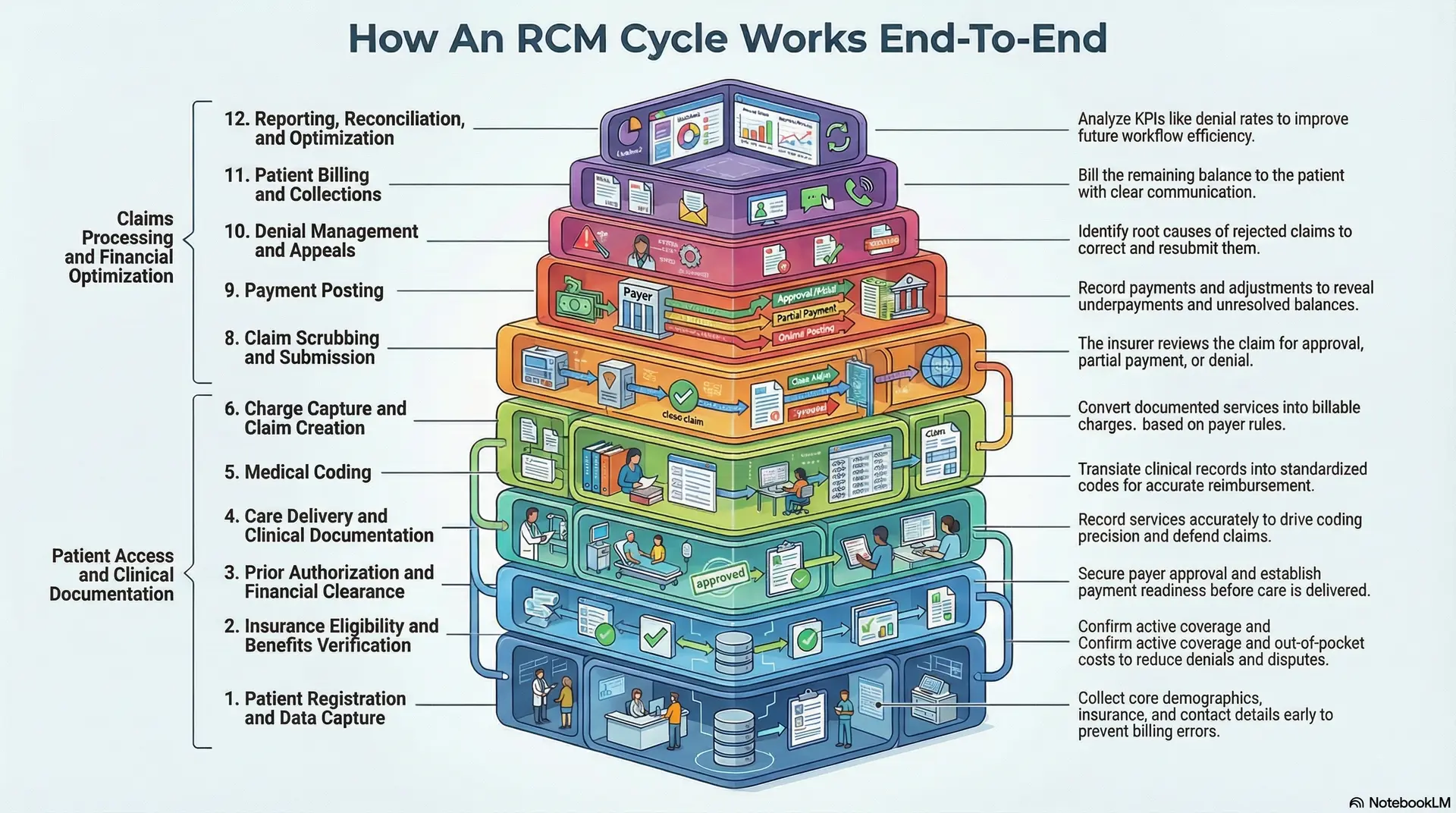
Step 1: Patient Registration and Data Capture
The revenue cycle starts when the patient books an appointment or arrives for care. At this stage, the provider collects core details such as demographics, insurance information, contact details, and referral data if required.
This step may look administrative, but it directly affects billing. Even a small data error can lead to claim rejections, payment delays, or compliance issues later. Therefore, strong RCM systems validate patient data early and reduce avoidable mistakes from the start.
Step 2: Insurance Eligibility and Benefits Verification
Once patient details are captured, the next step is to verify insurance coverage. The provider checks whether the policy is active, what services are covered, whether prior authorization is needed, and how much the patient must pay out of pocket.
This stage protects both revenue and patient experience. When eligibility is verified in advance, providers reduce denied claims and avoid billing disputes. At the same time, patients get more clarity on their financial responsibility before treatment begins.
Step 3: Prior Authorization and Financial Clearance
For many procedures, treatments, and specialist services, payer approval is required before care is delivered. The RCM workflow must confirm these authorizations on time and document them properly.
In parallel, providers often review co-pays, deductibles, and expected balances. This helps the organization establish financial clearance before the visit. As a result, teams reduce downstream delays and improve collection readiness.
Step 4: Care Delivery and Clinical Documentation
After administrative and insurance checks are completed, care is delivered. However, from an RCM perspective, treatment alone is not enough. The services provided must be documented accurately in the clinical system.
Documentation drives the next stages of the cycle. It must clearly reflect diagnoses, procedures, treatment complexity, and physician notes. If documentation is incomplete or inconsistent, coding errors increase, and claims become harder to defend.
Step 5: Medical Coding
Once the encounter is documented, coding teams translate clinical records into standardized medical codes. These may include diagnosis codes, procedure codes, and modifiers required for billing.
Coding is one of the most sensitive points in the revenue cycle. If the codes do not match the documentation, the claim may be denied, delayed, or underpaid. Therefore, enterprises often invest in coding automation, validation tools, and audit workflows to improve accuracy without slowing down throughput.
Step 6: Charge Capture and Claim Creation
After coding, the organization converts clinical services into billable charges. These charges are reviewed, assembled, and prepared for claim generation based on payer requirements and contract rules.
This step ensures that every eligible service is captured correctly. Missed charges reduce revenue, while incorrect charges increase denial risk. Strong RCM systems create a cleaner path from documentation to billing by standardizing charge capture workflows.
Step 7: Claim Scrubbing and Submission
Before a claim is sent to the payer, it goes through validation checks. This process, often called claim scrubbing, identifies missing data, coding mismatches, formatting issues, or payer-specific errors.
Once the claim passes these checks, it is submitted through the appropriate channel, often via a clearinghouse. This step is critical because clean claims are more likely to be paid faster. In contrast, poor claim quality creates rework, delays, and administrative waste.
Step 8: Payer Adjudication
After submission, the payer reviews the claim. The insurer decides whether the claim should be approved, partially paid, denied, or routed back for more information.
This stage is largely outside the provider’s direct control, which is why earlier workflow quality matters so much. Clean documentation, accurate coding, and correct payer rules improve the chances of first-pass acceptance. As a result, organizations reduce denial volumes and accelerate reimbursements.
Step 9: Payment Posting
When the payer processes the claim, the payment is posted into the system. The provider records what was paid, what was adjusted, and what balance remains the patient’s responsibility.
Payment posting closes the loop between expected and actual reimbursement. It also reveals underpayments, contractual variances, and unresolved balances. Therefore, this step is not just clerical. It is essential for financial visibility and follow-up action.
Step 10: Denial Management and Appeals
Not every claim is paid the first time. Some are denied due to coding errors, missing authorizations, documentation gaps, or payer-specific issues. When that happens, the RCM team must identify the root cause, correct the issue, and resubmit or appeal the claim.
This is where many organizations lose revenue. If denial management is reactive, teams only fix surface problems. However, when systems track patterns and causes, providers can improve upstream workflows and reduce repeat denials over time.
Step 11: Patient Billing and Collections
After payer payment is processed, the remaining balance is billed to the patient. This may include co-pays, deductibles, co-insurance, or non-covered services.
Patient collections are now a core part of the revenue cycle. Clear billing statements, flexible payment options, and timely follow-ups improve both cash flow and patient satisfaction. On the other hand, poor billing communication often leads to delayed collections and a weaker financial experience.
Step 12: Reporting, Reconciliation, and Optimization
The final stage of the revenue cycle is analysis. Organizations review KPIs such as denial rates, days in accounts receivable, first-pass claim rate, net collection rate, and reimbursement trends.
This step turns RCM from a billing function into a strategic financial system. By analyzing where money is delayed, lost, or under-collected, enterprises can improve workflows across the entire cycle. In other words, reporting is not the end of the process. It is what helps the next cycle perform better.
An end-to-end revenue cycle is a connected system that links patient access, clinical documentation, claims processing, payments, and financial analysis.
When even one stage breaks, revenue slows down. That is why enterprise RCM software must support the full cycle, not just isolated billing tasks.
Where RCM Systems Break in Real Hospitals
Operational friction within a hospital often stems from a mismatch between clinical excellence and administrative infrastructure. Even the most prestigious institutions face financial strain when their underlying software cannot keep up with the physical pace of care.
1. Billing gaps across teams and systems
Large hospitals frequently rely on a patchwork of software that does not communicate effectively. When the front desk uses one system and the billing office uses another, data synchronization becomes a manual burden. This fragmentation creates “dark data” where patient insurance updates or co-pay details are lost in transition.
2. Delays between clinical and finance teams
The lag between a medical procedure and the generation of a bill is a major liquidity killer. Clinical staff prioritizes patient outcomes, often leaving detailed coding for later in the shift. However, if the RCM software is not integrated with the clinical EHR, the finance team must wait for manual exports to begin their work.
3. Revenue loss from workflow inefficiencies
Inefficient workflows act as a slow leak in a hospital’s balance sheet. Manual claim scrubbing and repetitive data entry consume hundreds of staff hours that could be better utilized for patient advocacy. Furthermore, without automated alerts for missing documentation, claims are often sent to payers with incomplete information.
Addressing these breaks requires a strategic shift toward unified, intelligent platforms that prioritize accuracy and speed.
Key Features of Enterprise RCM Software
A robust RCM platform is a strategic asset for financial predictability. It replaces reactive administration with a proactive, data-driven financial engine.
1. Eligibility verification and pre-auth
Verifying insurance at entry prevents future denials. High-end RCM systems connect to payer databases to confirm benefits instantly. This automation extends to prior authorizations, removing significant administrative bottlenecks.
2. Medical coding with AI accuracy
AI analyzes clinical notes to suggest accurate medical codes. This reduces reliance on manual teams and minimizes audit risks. Consequently, the accuracy of submissions increases, leading to higher first-pass clean claim rates.
3. Claims management and tracking
Modern platforms track claims from generation to final payment. If a claim stalls, the system provides immediate visibility for intervention.
Therefore, you maintain a transparent, real-time view of every transaction in the pipeline.
4. Denial management workflows
Software categorizes denials by reason and routes them to specialists automatically. This replaces chaotic manual chasing with a systematic recovery process.
In addition, identifying root causes allows for long-term fixes in clinical workflows.
5. Payment processing and reconciliation
Centralized gateways simplify managing diverse payment streams. The software automates reconciliation by matching incoming funds with outstanding invoices.
This precision ensures ledger accuracy without manual accounting labor.
6. Revenue analytics and dashboards
Custom dashboards transform raw data into actionable intelligence. Decision-makers can monitor KPIs like Net Collection Ratio at a glance.
Consequently, the software becomes a vital tool for driving sustainable enterprise growth.
Investing in these core features ensures your organization maintains liquidity in an increasingly complex environment. These tools provide the technical foundation for scalable, error-free financial operations.
Our Step-by-Step Process for Developing an RCM Software
Building an enterprise-grade RCM platform requires a methodical approach that balances technical precision with financial logic. We follow a structured development lifecycle to ensure the final product effectively bridges the gap between clinical services and revenue capture.
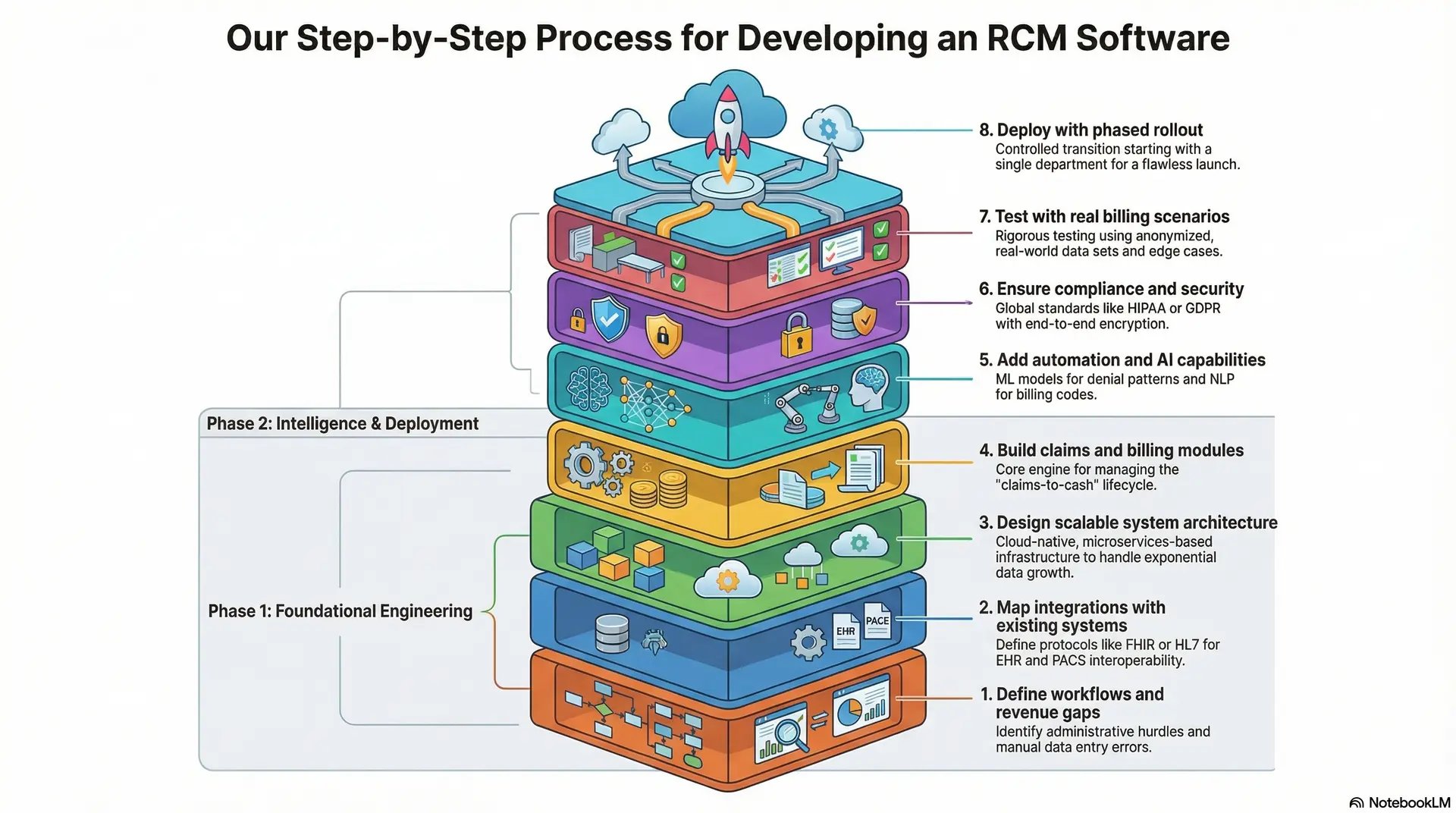
1. Define workflows and revenue gaps
We begin by conducting a deep audit of your current administrative hurdles. We identify exactly where manual data entry causes delays or where claims consistently fall through the cracks.
Consequently, this discovery phase sets the functional requirements for the entire build. Mapping these gaps allows our developers to create features that specifically target high-frequency error points.
2. Map integrations with existing systems
Your RCM software must communicate with EHRs, LIS, and PACS systems. Therefore, we define data exchange protocols like FHIR or HL7 as a critical step for seamless interoperability.
This ensures that patient data flows into the billing module without manual re-entry. In addition, mapping these connections early prevents costly architectural changes during the later stages of development.
3. Design a scalable system architecture
For an enterprise solution, the underlying infrastructure must handle exponential data growth. We choose a cloud-native, microservices-based architecture to allow individual modules to scale independently based on demand.
This design choice ensures the platform remains responsive even during peak billing cycles. Furthermore, a modular approach makes it easier to update specific features without taking the entire system offline.
4. Build claims and billing modules
This phase focuses on the core engine that generates and manages medical claims. We program complex payer rules and reimbursement logic directly into the software’s foundation.
However, the interface remains intuitive so billing staff can navigate complex financial data easily. These modules act as the primary interface for managing the “claims-to-cash” lifecycle, requiring the highest levels of transactional accuracy.
5. Add automation and AI capabilities
Integrating AI transforms the platform from a recording tool into a predictive powerhouse. We build machine learning models to analyze historical denial patterns and flag high-risk claims before submission.
Consequently, this reduces the administrative burden of manual claim scrubbing. In addition, AI-driven natural language processing extracts relevant billing codes from clinical notes, further increasing efficiency and accuracy.
6. Ensure compliance and security
Healthcare data demands the highest level of protection to meet global standards like HIPAA or GDPR. During this stage, we implement end-to-end encryption, multi-factor authentication, and robust audit trails.
Therefore, every data access point is strictly monitored and logged within the system code. Building security into the DNA of the application protects your enterprise from both data breaches and regulatory penalties.
7. Test with real billing scenarios
Before going live, we subject the software to rigorous testing using anonymized, real-world data sets. This process uncovers how the system handles complex edge cases, such as split-billing or secondary insurance claims.
Testing ensures that the automation logic holds up under the pressure of diverse payer requirements. Consequently, this phase minimizes the risk of technical glitches disrupting your actual revenue stream.
8. Deploy with phased rollout
A phased deployment strategy allows your enterprise to transition smoothly without risking total operational downtime. Intellivon specializes in these high-stakes migrations, providing the technical oversight needed for a flawless launch.
We start with a single department or facility to refine workflows based on live feedback. Therefore, this controlled approach ensures the software is fully optimized before a total enterprise-wide adoption.
Following this rigorous development roadmap ensures your investment results in a high-performance financial ecosystem. A well-executed build provides the transparency and control necessary to dominate the modern healthcare market.
Tech Stack for RCM Software Development
Selecting the right technology stack is a high-stakes decision that dictates the scalability and security of your financial ecosystem. We prioritize modern, battle-tested frameworks that ensure high availability and rapid data processing.
1. Backend and frontend technologies
We build robust backends using Python (Django/FastAPI) or Node.js to handle complex financial logic and high-concurrency requests. These languages offer extensive libraries for data validation and secure transaction management.
On the frontend, we utilize React.js or Angular to create intuitive, responsive dashboards for billing specialists. Consequently, this combination provides a seamless user experience while maintaining the power needed for heavy data entry.
2. Cloud infrastructure and deployment
For enterprise-grade reliability, we deploy on AWS or Microsoft Azure, leveraging their dedicated healthcare compliance blueprints.
We use Docker and Kubernetes for containerization, ensuring that the platform can scale resources automatically during peak billing cycles.
This cloud-native approach guarantees 99.9% uptime and simplified disaster recovery. Therefore, your financial data remains accessible and protected against hardware failures or localized outages.
3. AI and automation tools in RCM
We integrate TensorFlow or PyTorch to develop custom machine learning models for denial prediction and automated claim scrubbing. In addition, Natural Language Processing (NLP) tools like AWS Comprehend Medical are used to extract ICD-10 codes from unstructured clinical notes.
These AI layers act as a force multiplier for your administrative staff. Consequently, the system identifies potential errors with a precision that manual review simply cannot match.
4. APIs and interoperability standards
Data fluidity is maintained through strict adherence to HL7 and FHIR standards. We build secure RESTful APIs to facilitate real-time communication between your RCM, EHR, and external payer portals.
This ensures that eligibility checks and claim status updates happen instantaneously without manual file exports. In addition, we utilize integration engines like Mirth Connect to translate data formats across legacy systems.
Choosing the correct stack ensures your software remains relevant and maintainable for a decade rather than a few years. Our technical selection process prioritizes long-term ROI and the highest standards of data integrity.
Why Your RCM Data Structure Matters More
A fragmented data architecture is the silent killer of institutional profitability. For an enterprise, the way information is organized and stored directly dictates the speed of the “claims-to-cash” cycle and the accuracy of financial reporting.
1. Disconnected data leads to revenue loss
When patient registration, clinical documentation, and billing modules operate on disparate schemas, data integrity suffers. Information often degrades during manual transfers between these silos, leading to missing modifiers or incorrect patient identifiers.
Consequently, these small discrepancies result in high denial rates and expensive administrative rework.
2. Building a single financial truth
We focus on creating a centralized data warehouse that serves as the definitive source for all financial and clinical interactions. This “single version of truth” ensures that every department, from the front office to the CFO, is viewing the exact same metrics.
In addition, a structured data environment allows for more granular auditing and compliance tracking.
3. Real-time vs delayed processing
Legacy systems often rely on “batch processing,” where claims are bundled and sent at the end of the day or week. However, modern healthcare demands real-time processing to capture eligibility changes and authorization requirements instantly.
We build systems that validate data at the point of entry, providing immediate feedback to clinical and administrative staff. This shift from reactive to proactive data handling significantly reduces “Days in AR” and improves organizational liquidity.
Therefore, real-time data flow transforms the revenue cycle from a slow-moving back-office task into a high-velocity financial engine.
The integrity of your data structure is the foundation upon which all AI and automation tools are built. Without a clean, unified architecture, even the most advanced software will struggle to deliver a measurable return on investment.
RCM Integrations You Cannot Ignore
A standalone billing tool is a liability in a modern healthcare enterprise. To achieve true financial velocity, your RCM must act as a central nervous system, connecting every clinical and external touchpoint through seamless, automated integrations.
1. EHR integration for clinical sync
The EHR is the primary source of all billable clinical events. Therefore, a bi-directional sync is essential to ensure that procedure codes flow instantly into the billing module. Consequently, this eliminates manual data extraction and reduces the risk of transcription errors.
2. Clearinghouse integration for claims
We integrate directly with leading clearinghouses to automate the submission and tracking of electronic claims. This connection provides instant feedback on “scrubbing” errors before a claim reaches the payer. Furthermore, it allows for the automated retrieval of Electronic Remittance Advice.
3. Payer systems and eligibility checks
Direct API connections to major payer portals verify insurance coverage in real-time during patient check-in. This integration confirms active benefits, co-pay amounts, and deductible status instantly. Consequently, you significantly reduce the likelihood of “service not covered” denials.
4. Payment gateways and collections
We integrate secure, PCI-compliant payment gateways that support credit cards and digital wallets. Every transaction is automatically posted back to the patient’s account in the RCM. This automation reduces administrative burdens and accelerates the overall collection cycle.
5. Analytics systems for forecasting
Your RCM data must feed into advanced business intelligence platforms for predictive forecasting. These systems identify trends, such as shifting denial patterns or seasonal volume fluctuations. Therefore, you can make data-driven decisions regarding staffing and strategic expansion.
Strategic integration is the difference between a fragmented administrative process and a unified financial engine. By connecting these critical systems, you create a transparent, high-efficiency ecosystem capable of scaling with your enterprise.
Compliance in RCM Software Development
In the healthcare sector, regulatory compliance is the baseline for any technical investment. For enterprise leaders, a security breach is a fundamental threat to organizational reputation and patient trust.
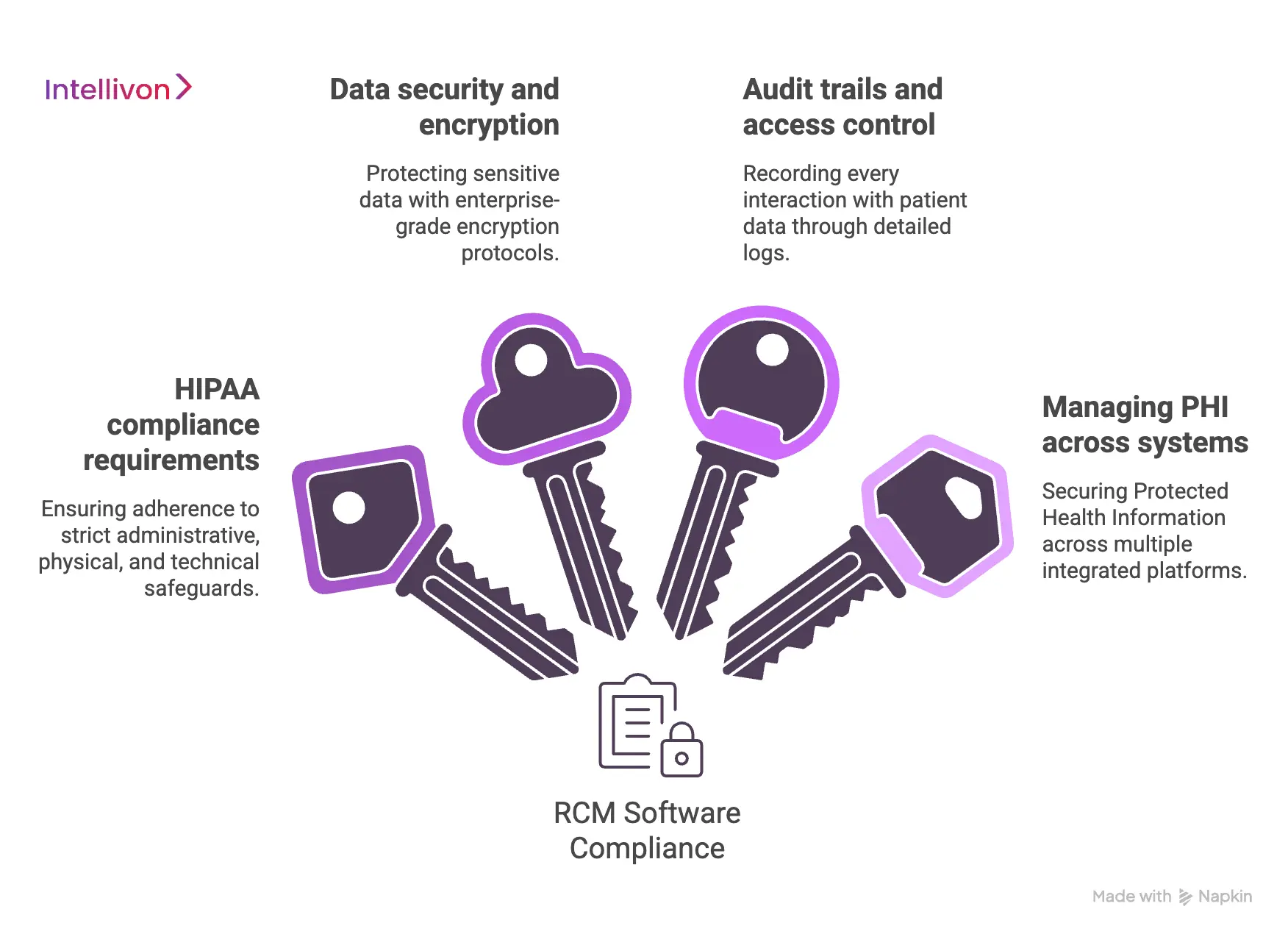
1. HIPAA compliance requirements
Adhering to HIPAA is the non-negotiable standard for any U.S.-based healthcare platform. We ensure that every module, from patient registration to final billing, adheres to strict administrative, physical, and technical safeguards.
Therefore, our development process includes signing Business Associate Agreements (BAAs) with all sub-service providers. Consequently, this legal and technical framework protects the enterprise from massive civil penalties. In addition, we implement specific workflows to manage patient rights, such as data access and amendment requests.
2. Data security and encryption
We protect sensitive financial and medical data using enterprise-grade encryption protocols. Data at rest is secured with AES-256, while all data in transit is shielded by TLS 1.3. This multi-layered approach ensures that even if a database is intercepted, the information remains unreadable.
Furthermore, we utilize hardware security modules (HSMs) to manage encryption keys securely. Therefore, your digital assets are protected against both external hackers and internal vulnerabilities.
3. Audit trails and access control
A robust RCM must record every interaction with patient data through detailed audit trails. We implement Role-Based Access Control (RBAC) to ensure that staff only see the information necessary for their specific job.
Consequently, a billing clerk cannot access deep clinical histories, and a physician cannot modify financial ledgers. Every login, file view, and data modification is timestamped and logged. These logs are immutable, providing a clear map for internal audits or federal investigations.
4. Managing PHI across systems
Securing Protected Health Information (PHI) becomes more complex when data flows between multiple integrated platforms. We utilize “tokenization” to replace sensitive identifiers with non-sensitive equivalents during data exchange. This ensures that PHI is only decrypted at the final destination when absolutely necessary.
Furthermore, we conduct regular vulnerability assessments and penetration testing to identify potential leak points. Therefore, your integrated ecosystem remains a fortress, keeping patient privacy intact while maintaining high operational speed.
Prioritizing compliance during the development phase prevents the catastrophic costs of a data breach. A secure, compliant RCM is the only way to safeguard your enterprise’s future in an increasingly regulated digital world.
AI in RCM Software: Where It Adds Value
Integrating AI into the revenue cycle moves your enterprise from reactive accounting to predictive financial management. AI acts as a continuous optimization layer that identifies patterns human auditors frequently overlook.
1. AI in coding and error reduction
Manual coding is often the largest source of compliance risk and revenue leakage. Therefore, we utilize NLP to scan clinical documentation and suggest the most specific ICD-10 and CPT codes.
This automation reduces the “human touch” required for standard procedures, significantly lowering the margin of error. Consequently, your claims are more accurate upon first submission, which drastically reduces the need for expensive back-end corrections.
2. Predictive denial management
Rather than waiting for a rejection, our AI models analyze claims against millions of historical payer interactions to predict denials before they happen. The system flags potential issues, such as missing modifiers or inconsistent data, allowing for immediate pre-submission fixes.
This proactive approach transforms the billing department from a “claims chaser” into a high-precision financial gatekeeper. In addition, the AI learns from every successful appeal to improve future predictions.
3. Automation in claims workflows
Routine administrative tasks, such as status checks and data entry, are perfectly suited for Robotic Process Automation (RPA). We build “digital workers” that navigate payer portals to verify claim status 24/7 without manual intervention.
This constant monitoring ensures that stalled claims are identified and addressed within hours rather than weeks. Therefore, your staff can dedicate their time to resolving complex medical necessity disputes instead of performing repetitive data lookups.
4. Revenue forecasting using AI
For decision-makers, AI-driven forecasting provides a crystal-clear view of future cash flow based on real-time billing performance. The software analyzes historical reimbursement rates, seasonal patient volume, and payer behavior to project monthly revenue with high precision.
Consequently, you can plan capital expenditures and strategic expansions with a level of confidence that traditional spreadsheets cannot provide. Therefore, AI turns your raw financial data into a powerful tool for long-term institutional growth.
The true value of AI lies in its ability to scale your operations without proportionally increasing your headcount. It provides the technical intelligence required to maintain peak financial performance in a volatile healthcare market.
Real RCM Systems Used by Providers
Selecting a platform requires a deep understanding of how different architectures align with specific enterprise goals. Each of these market leaders offers a unique technical focus, ranging from labor-intensive hybrid models to pure-play AI automation.
1. AGS Health: Hybrid RCM at scale
AGS Health operates on a hybrid model that combines high-touch human expertise with proprietary technology. The system works by deploying large-scale clinical coding teams who utilize a centralized workflow platform to process high-volume claims.
This approach is particularly effective for complex multi-specialty groups requiring manual intervention for nuanced denials. Consequently, it provides a safety net for organizations not yet ready for full automation.
2. Quadax: Claims-focused infrastructure
Quadax is built around a powerful EDI (Electronic Data Interchange) engine designed for high-velocity claim scrubbing and submission.
It works by routing clinical data through a series of rigorous “payer-specific” rule sets before it reaches the clearinghouse.
This architecture ensures that errors are caught at the earliest possible stage in the cycle. Therefore, it is a preferred choice for large laboratories and hospital systems with massive transactional volumes.
3. GeBBS: Cost-optimized RCM operations
GeBBS focuses on driving down the “cost-to-collect” through a globally distributed delivery model and integrated technology.
The platform works by automating eligibility and patient access workflows while offshoring more labor-intensive back-office tasks.
This strategy allows health systems to maintain high margins even as reimbursement rates fluctuate. In addition, their “iCode” AI tool assists manual coders in increasing daily output and accuracy.
4. CureAR: AI-driven RCM automation
CureAR represents the next generation of autonomous RCM, focusing heavily on reducing human touches. It works by utilizing advanced machine learning to predict payer behavior and automatically resolve low-level denials without staff involvement.
The system continuously “learns” from previous successful appeals to refine its internal logic. Consequently, it is an ideal solution for tech-forward enterprises looking to scale their operations without increasing administrative headcount.
5. PracticeSuite: RCM with visibility
PracticeSuite provides an end-to-end cloud platform that prioritizes transparent financial reporting and patient engagement. It works by unifying the clinical record with the billing ledger in a single, browser-based interface.
This allows administrators to track “Days in AR” and collection trends in real-time from any device. Furthermore, its integrated patient portal simplifies the collection of out-of-pocket costs.
Therefore, it offers the high level of visibility required for modern medical practice management.
Choosing the right partner depends on whether your enterprise prioritizes human-led complexity or AI-driven efficiency. Each platform provides a different path toward stabilizing and growing your organization’s financial health.
RCM Challenges and How Systems Solve Them
The gap between providing care and receiving payment is often filled with technical and administrative friction. Modern enterprise systems are designed to transform these chronic challenges into streamlined, predictable financial workflows.
1. High denial rates and automation fixes
Denials are frequently the result of simple data mismatches or missed payer deadlines. Advanced RCM platforms solve this by implementing automated “rules engines” that validate every claim against specific payer requirements before submission.
Consequently, the system identifies missing modifiers or incorrect patient IDs in milliseconds. Therefore, your staff only intervenes in complex medical necessity cases rather than fixing repetitive clerical errors.
This proactive filtering significantly reduces the volume of rejected claims and stabilizes monthly cash flow.
2. Data inconsistency and integration layers
When clinical and financial systems do not speak the same language, data integrity quickly degrades. We solve this by building robust integration layers using FHIR and HL7 standards to synchronize data across the enterprise.
This ensures that a change in patient insurance at the front desk is reflected instantly in the billing module. In addition, automated data mapping eliminates the need for manual exports and re-entry.
Consequently, the “single source of truth” remains intact, preventing the costly errors associated with fragmented information silos.
3. Slow reimbursements and workflow gaps
Lag time in the revenue cycle is often caused by “dark periods” where a claim sits idle between departments. Modern systems solve this through automated task routing and real-time status tracking.
When a clinician signs a chart, the system triggers a billing event immediately without manual notification. Furthermore, digital assistants perform 24/7 status checks on submitted claims to identify delays early.
Therefore, your organization can address stalled payments within hours, significantly reducing “Days in AR” and increasing overall liquidity.
4. Compliance risks and system design
Regulatory shifts can turn a standard billing practice into a legal liability overnight. We address this by building “compliance-by-design” into the software architecture, ensuring that every transaction follows the latest HIPAA and OIG guidelines.
Automated audit trails record every instance of PHI access, providing a transparent map for internal or federal reviews. In addition, the system automatically updates its coding logic to reflect annual changes in ICD-10 or CPT requirements.
Consequently, your enterprise remains protected from both data breaches and expensive regulatory penalties.
Addressing these challenges requires moving beyond patchwork fixes toward a unified, intelligent infrastructure. A well-designed RCM system protects your organization’s long-term financial health and operational integrity.
Best Practices for Building RCM Software
Successful RCM development is a financial engineering project. Approaching the build with a strategic, “business-first” mindset ensures the final platform delivers measurable ROI and long-term operational stability.
1. Design workflows before development
Before writing a single line of code, you must map the entire patient financial journey. We identify every touchpoint, from scheduling and eligibility to final payment posting, to uncover existing bottlenecks. Consequently, this prevents the common mistake of simply digitizing a broken manual process.
Therefore, your development team can build features that actively solve for high-frequency error points. Designing these logical paths early ensures the software architecture supports the actual speed of a busy healthcare enterprise.
2. Prioritize integrations early
An RCM system that cannot communicate with your EHR or laboratory system is a liability. Therefore, we define all data exchange protocols and API requirements during the discovery phase. This early focus on interoperability prevents expensive architectural changes later in the development cycle.
In addition, mapping these connections ensures that data flows seamlessly between clinical and financial modules. Consequently, you achieve a “single source of truth” that eliminates the need for manual data entry and reduces the risk of costly billing gaps.
3. Build for compliance from day one
In healthcare, security cannot be an afterthought; it must be baked into the software’s DNA. We implement HIPAA-compliant safeguards, such as end-to-end encryption and multi-factor authentication, from the very first sprint.
Consequently, this protects your organization from the devastating financial and reputational costs of a data breach. Furthermore, building automated audit trails ensures that every access to patient data is recorded and immutable.
Therefore, your enterprise remains prepared for federal audits or internal security reviews without requiring manual intervention.
4. Test using real-world billing data
A platform that works in a vacuum often fails when faced with the chaos of actual payer requirements. We utilize anonymized, high-volume billing data to stress-test the system’s automation and scrubbing logic.
This process uncovers how the software handles complex edge cases, such as secondary insurance or split-billing scenarios. Therefore, you can refine the “rules engine” to ensure high first-pass clean claim rates before going live.
Consequently, this rigorous testing phase minimizes the risk of technical glitches disrupting your actual cash flow during deployment.
Adhering to these best practices ensures your RCM software is a robust, scalable, and secure financial asset. A well-planned build provides the transparency and precision necessary to thrive in a highly competitive and regulated market.
Conclusion
Healthcare RCM defines how efficiently revenue flows across the organization. As systems grow more complex, disconnected tools create delays, errors, and lost income.
Building a custom RCM platform gives enterprises control, visibility, and scalability across the entire cycle. The focus should not be on managing transactions, but on creating a system that continuously improves financial performance.
Build Your Own RCM Software With Intellivon
At Intellivon, RCM software is built as an enterprise financial infrastructure, not as a billing tool layered onto fragmented systems. The goal is to create a unified platform that connects patient access, clinical data, claims workflows, and financial operations into a single, scalable environment.
Each platform is designed around your existing workflows. This includes eligibility verification, coding, claims processing, denial management, payment reconciliation, and real-time revenue tracking. As a result, teams reduce manual effort, improve claim accuracy, and accelerate cash flow across the organization.
Our engineering approach focuses on API-first, cloud-native architecture combined with interoperability standards. This ensures seamless integration with EHRs, clearinghouses, payer systems, and financial tools without disrupting ongoing operations.
Why Build With Intellivon
- Infrastructure, Not Add-Ons: We build systems that replace fragmented tools with a unified revenue engine, giving you full control over workflows, data, and financial performance.
- Workflow-First Development: Every system is designed around how your teams operate, ensuring that automation supports real billing scenarios, not generic software assumptions.
- AI-Driven Revenue Optimization: We embed AI across the cycle to reduce denials, improve coding accuracy, and identify revenue gaps before they impact cash flow.
- Built for Scale Across Systems: Our platforms support multi-hospital networks, clinics, and specialty practices with consistent performance, centralized control, and flexible configurations.
If your current RCM setup feels fragmented, reactive, or difficult to scale, it is time to rethink the foundation. Contact our experts to build a system that gives you control over revenue, not just visibility into it.
FAQs
Q1. What is healthcare RCM software?
A1. Healthcare RCM software manages the full financial lifecycle of patient care, from registration to final payment. It connects workflows such as eligibility checks, coding, claims submission, denial management, and collections. As a result, providers reduce billing errors, improve claim success rates, and gain better visibility into revenue performance across the organization.
Q2. How long does RCM development take?
A2. RCM software development typically takes 4 to 9 months, depending on complexity. A basic system with core billing workflows can be built faster, while enterprise platforms with integrations, automation, and AI features take longer. Timelines also depend on the number of systems involved and how customized the workflows need to be.
Q3. What integrations are required?
A3. RCM systems require integration with EHR platforms, clearinghouses, payer systems, and payment gateways. In addition, many enterprises connect analytics tools and financial systems for reporting. These integrations ensure that clinical data, billing workflows, and payments move seamlessly across systems without manual intervention.
Q4. How much does RCM software cost?
A4. The cost to build RCM software typically ranges from $50,000 to $150,000 for mid-to-large systems. However, the final cost depends on features, integrations, compliance requirements, and the level of customization. While upfront investment may be higher than ready-made tools, custom systems often deliver better long-term ROI by reducing revenue leakage and manual effort.
Q5. Can RCM systems scale across hospitals?
A5. Yes, modern RCM systems are designed to scale across multi-hospital networks and clinics. With cloud-based architecture and centralized workflows, organizations can manage billing, claims, and reporting across locations. This ensures consistent processes, better control over revenue, and the flexibility to grow without rebuilding systems.