Key Takeaways:
-
AI shifts hospitals from reactive billing to proactive claim validation and denial prevention.
-
Nearly 80% of denials are preventable through better coding accuracy and eligibility verification.
-
Core features include coding support, denial prediction, appeal automation, and payer rule validation.
-
Development costs range from $60,000 for MVPs to $350,000 for enterprise hospital deployments.
-
Intellivon builds HIPAA-ready AI claims platforms that integrate directly with EHR and RCM systems.
Payers are becoming quicker, stricter, and more reliant on AI when they review, delay, and deny hospital claims. At the same time, most hospital claims teams are still using workflows based on manual reviews, reactive corrections, and processes that rely on staff. These workflows cannot keep up with the speed of the payers. The resulting revenue gap poses a structural risk, and not merely a billing problem.
An AI claims management software changes this situation by helping hospitals shift from fixing claims reactively to using proactive claim insights. This shift involves validating claims earlier, spotting denial risks before submission, routing complex cases effectively, supporting appeal processes, and tracking revenue performance throughout the entire cycle.
Intellivon develops AI claims management software for hospitals, health systems, RCM companies, healthcare SaaS platforms, and enterprise care networks. Our engineering approach brings together claim intake, document intelligence, coding support, payer validation, denial prediction, workflow automation, appeal management, and secure healthcare integrations into one platform focused on revenue. This blog explains how to build such a system, what it needs to include, what it costs, and how Intellivon builds it from the ground up.
Why Hospitals Are Investing In AI Claims Management Software
Hospital revenue teams are not investing in AI claims management because the technology is new. They are investing because the financial pressure of managing claims manually has become unsustainable at scale.
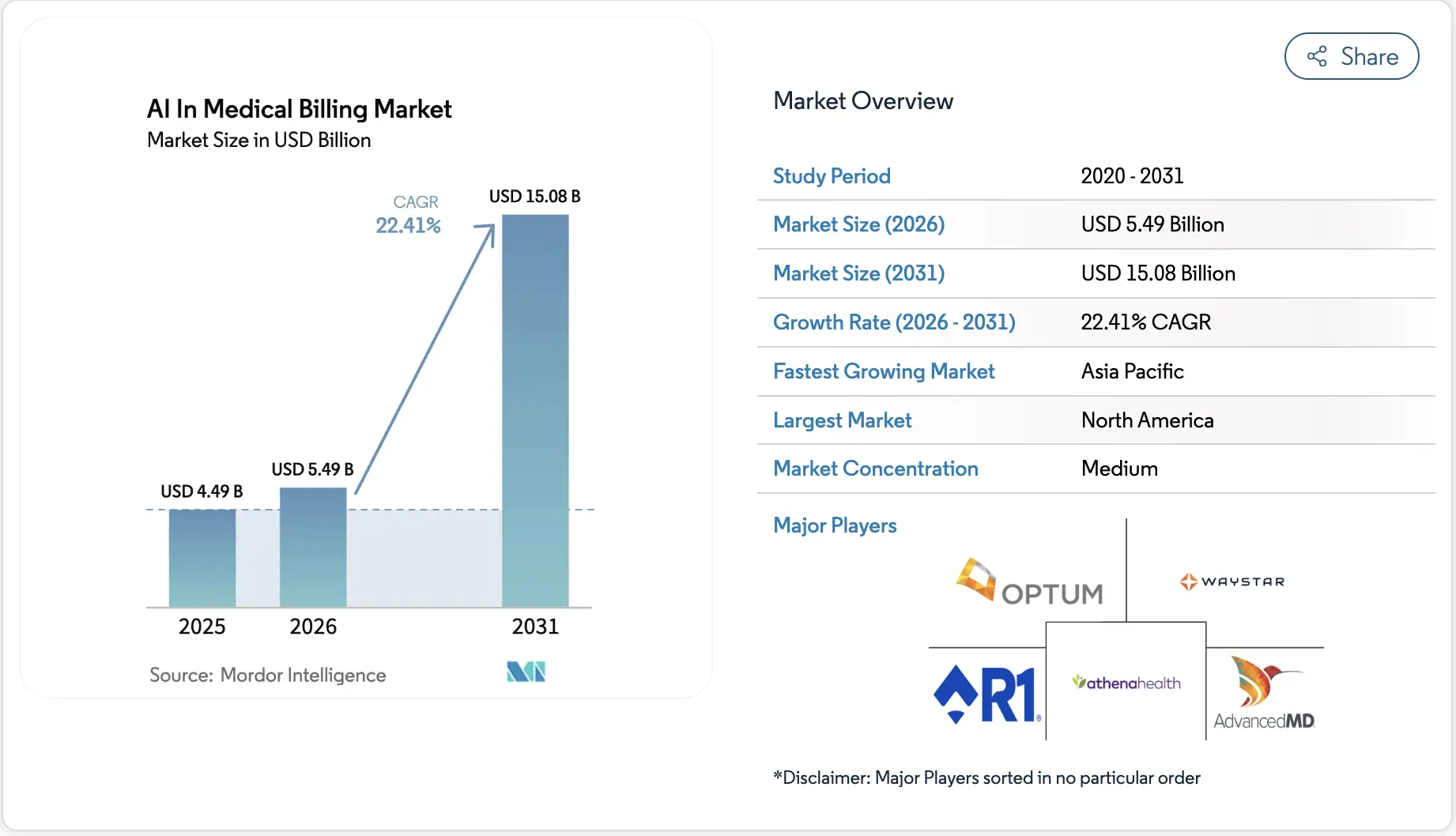
The AI in healthcare RCM market reflects that shift, projected to grow from USD 20.68 billion in 2024 to USD 180.33 billion by 2034 at a CAGR of 24.2%. That growth is being driven by hospitals that have decided AI claims infrastructure is no longer optional.
1. The Revenue Crisis Hospitals Face
Claim denials have reached levels that directly threaten hospital cash flow. With 19% of claims denied on average, the administrative cost of reworking, appealing, and resubmitting rejected claims compounds across every billing cycle.
Furthermore, 80% of those denials are preventable with better coding accuracy and eligibility verification. However, manual workflows cannot consistently deliver that accuracy at volume, which is why hospitals are losing 15 to 30% of potential revenue to administrative inefficiencies alone.
Why AI Delivers Measurable ROI
Hospitals adopting AI claims management are reporting 40 to 50% reductions in denial rates and 30% faster payment cycles. The financial drivers behind those results include:
- Denial prediction and prevention: AI analyzes historical claims data to flag high-risk submissions before payers reject them
- Automated medical coding: NLP and generative AI extract billable procedures from clinical notes, reducing coding errors from 20% to under 5%
- Real-time claims scrubbing: Validation against payer rules prevents compliance issues that trigger audits or payment delays
Why Hospitals Build Custom Rather Than Buy Generic
Generic software cannot account for the unique payer mixes, service lines, and denial patterns each hospital carries. Additionally, with coding and billing vacancies exceeding 20%, AI must handle routine claims autonomously while integrating directly into existing EHR infrastructure such as Epic, Cerner, and Meditech.
Custom-built platforms trained on internal data consistently outperform off-the-shelf alternatives in denial prevention accuracy.
What Is AI Claims Management Software For Hospitals?
AI claims management software is a revenue protection infrastructure that manages the full claim lifecycle from intake to payment reconciliation. It handles eligibility verification, prior authorization checks, medical coding support, documentation validation, claim scrubbing, and denial risk scoring before submission.
After adjudication, it supports appeal workflows, automates payment posting, and surfaces RCM analytics that give revenue teams visibility into exactly where the cycle is losing money. Unlike generic billing automation, it is built around how hospital claims actually move through payer systems.
How It Differs From Traditional Claims Software
Legacy systems operate as digital filing cabinets with basic rule engines. These platforms flag errors based on rigid instructions. However, AI solutions thrive on fluidity. They observe how insurers respond to codes and adjust logic automatically.
| Feature | Traditional Software | AI Claims Software |
| Logic | Static rules | Self-learning algorithms |
| Detection | Manual checks | Pattern recognition |
| Workflow | Reactive | Proactive |
Traditional tools record history while AI predicts outcomes. Intelligent systems flag potential denials before submission. This allows teams to correct gaps immediately and prioritize high-value claims.
Modern software transforms billing into a high-performance engine for financial health.
Core Features Of AI Claims Management Software For Hospitals
Enterprise AI claims management systems utilize a unified stack of NLP, predictive modeling, and OCR to automate the revenue cycle.
By integrating real-time payer rule engines with automated appeal workflows, hospitals can achieve a clean claim rate exceeding 95% while drastically reducing the cost to collect.
Executive leaders must view AI claims management as a multidimensional engine rather than a single tool. This software integrates deep learning across every touchpoint of the billing journey to eliminate manual friction and financial leakage.
1. AI Claim Intake And Document Processing
The system begins by transforming unstructured data from discharge summaries, physician notes, and lab reports into actionable intelligence. Using advanced OCR and Document AI, the platform extracts critical details from EOBs and referral forms.
This creates a structured data layer that ensures physician intent and clinical evidence are perfectly captured for the billing cycle.
2. Eligibility And Coverage Verification
Automated verification engines check patient eligibility and policy status in real-time before the encounter even begins.
- Pre-visit validation: Confirms insurance coverage and plan-specific limits instantly.
- Benefits verification: Identifies secondary insurance and deductible balances to prevent backend surprises.
3. AI-Assisted Medical Coding Support
The software provides a safety net for ICD-10, CPT, and HCPCS coding by matching procedures directly to clinical documentation.
It identifies coding gaps and detects diagnosis-procedure mismatches, ensuring that the final submission reflects the full complexity of the care provided.
4. Payer Rule Validation
AI engines maintain a live library of payer-specific rules and prior authorization requirements.
By checking claims against current contract-based conditions and medical necessity rules, the system ensures compliance with the shifting landscape of various insurance carriers.
5. Denial Risk Prediction
Machine learning models analyze historical denial patterns to assign a risk score to every claim.
The software flags high-risk payer combinations or authorization gaps before submission, allowing the team to address clinical denial risks while the documentation is still fresh.
6. Claim Scrubbing And Error Detection
This feature acts as a final filter to catch missing fields, duplicate claims, or invalid patient data.
It identifies policy mismatches and incomplete documentation, ensuring only “clean” claims move forward to the clearinghouse.
7. Smart Work Queue Routing
Instead of a first-in-first-out approach, the system routes tasks based on strategic value.
- High-value priority: Pushes large-dollar claims to the front.
- Specialist queues: Directs complex clinical denials to senior reviewers for faster resolution.
8. AI Appeal Management
When denials occur, the AI classifies the reason and suggests the best evidence for an appeal.
It supports draft generation for appeal letters and tracks strict payer deadlines to ensure no revenue is lost to administrative oversight.
9. Payment Posting And Reconciliation
The platform automates the processing of 835 remittance data to detect underpayments or contract variances.
By flagging payment mismatches and write-off trends, it ensures that the hospital receives every cent dictated by its contracts.
10. Claims Analytics Dashboard
A centralized command center tracks the health of the entire revenue cycle. Leadership gains instant visibility into Days in AR, revenue leakage, and staff productivity, turning raw billing data into high-level strategic insights.
Implementing these core features allows a hospital to transform its financial department into a data-driven powerhouse. These capabilities ensure long-term solvency and provide the transparency required for effective enterprise scaling.
How AI Claims Management Software Works In A Hospital Workflow
The operational flow of AI claims software follows a linear path of data ingestion, enrichment, and intelligent routing. By shifting the validation process to the pre-submission phase, the system creates a “closed-loop” revenue cycle that minimizes human intervention and maximizes first-pass acceptance rates.
Integrating AI into the hospital workflow changes the lifecycle of a claim from a manual task to an automated pipeline.
This transition ensures that data flows seamlessly between departments without the typical bottlenecks found in traditional billing environments.
Step 1: Claim Data Is Collected From Hospital Systems
The process begins with the aggregation of data from various siloed platforms. The AI engine connects directly to the Electronic Health Record (EHR) and Hospital Information System (HIS) to pull relevant patient data.
- System Integration: It gathers inputs from the Practice Management System (PMS) and existing RCM tools.
- Centralized Repository: Data from the billing system and document repositories are consolidated to create a comprehensive view of the patient encounter.
Step 2: AI Extracts And Structures Claim Information
Once the data is collected, the system uses Natural Language Processing (NLP) and OCR to convert unstructured notes into structured fields. The platform performs document classification to distinguish between a physician note and a lab report.
Consequently, entity extraction identifies specific dates, dosages, and procedures, while code mapping prepares the data for formal submission.
Step 3: The System Validates Claims Before Submission
Before a claim ever reaches a payer, the software performs a rigorous internal audit. It validates patient eligibility and ensures that all prior authorizations are attached and active.
The AI cross-references diagnosis codes with procedure codes to verify clinical logic. This step ensures documentation completeness and strictly adheres to the most recent payer-specific rules.
Step 4: AI Scores Denial Risk
Every claim is assigned a numerical risk score based on historical data and current payer behavior.
- Low-risk claims: These are “clean” and move directly to the clearinghouse for immediate submission.
- Medium-to-High-risk claims: These are flagged for specific issues like missing documentation or coding mismatches.
- Human review triggers: The system automatically pauses high-risk claims, requiring a specialist to intervene before the claim is sent and potentially denied.
Step 5: Claims Are Routed To The Right Team
The software utilizes smart routing to ensure the right eyes see the right problems. Instead of a generic billing queue, issues are sent to specialized departments based on the error type.
- Coding Team: Receives claims with ICD-10 or CPT discrepancies.
- Clinical Documentation Team: Handles cases where physician notes lack the detail required for medical necessity.
- Appeals Team: Automatically receives denied claims with pre-populated evidence for a faster rebuttal.
Step 6: Dashboards Track Outcomes
The final stage involves continuous monitoring through an executive-level command center. Leaders can track approval rates and identify the most common denial reasons across different payers.
The dashboard highlights payer trends and the direct revenue impact of current workflows. This visibility allows management to identify and fix workflow delays before they affect the hospital’s bottom line.
This structured workflow ensures that no claim is left to chance. By automating the heavy lifting of data validation and routing, the hospital operates with a level of precision that manual processes simply cannot match.
The result is a streamlined financial operation that supports the primary mission of patient care.
AI Use Cases In Hospital Claims Management
Real-world AI applications in healthcare revenue cycles focus on shifting from retrospective recovery to prospective prevention.
By utilizing machine learning for denial prediction and NLP for documentation audits, hospitals can reduce administrative waste and recapture millions in otherwise lost revenue.
The practical application of AI in claims management is no longer a theoretical concept. Leading health systems are currently deploying these specific use cases to insulate their balance sheets from the rising complexity of payer requirements.
1. AI Denial Prediction
Hospitals can now predict which claims are likely to be denied before they ever leave the facility. The system analyzes coding gaps, payer-specific historical risks, and missing documentation to assign a probability score to each submission.
For instance, Cloudmed (now part of nThrive/FinThrive) uses predictive analytics to identify hidden insurance coverage and potential denial triggers. This allows billing teams to intervene early, ensuring that high-risk claims are perfected rather than rejected.
2. AI Claim Scrubbing
Automated scrubbing goes beyond basic field checks to ensure total alignment with intricate payer rules. The platform scans for invalid codes, duplicate entries, and subtle policy mismatches that human reviewers often miss.
Waystar utilizes smart automation to scrub millions of claims, significantly increasing the first-pass clean claim rate. By filtering out errors at the source, hospitals avoid the costly cycle of resubmission and administrative rework.
3. AI Prior Authorization Support
Missing or incorrect authorizations are a primary driver of clinical denials. AI platforms check whether a procedure requires prior authorization in real-time and flag missing approval documents before submission.
Companies like Olive have pioneered automated authorization workflows that connect directly to payer portals. This ensures that the clinical team and the billing office are always in sync regarding the status of required permissions.
4. AI Clinical Documentation Review
AI reviews clinical notes, discharge summaries, and diagnosis data to ensure the claim has sufficient supporting evidence. Using Natural Language Processing, the software identifies if the physician’s notes justify the level of care billed.
3M Health Information Systems employs advanced NLP to help clinicians improve documentation integrity. This ensures that the severity of the patient’s condition is accurately reflected, which is vital for proper reimbursement in value-based care models.
5. AI Fraud And Anomaly Detection
The system flags unusual claim patterns, duplicate submissions, and abnormal billing combinations that could indicate internal errors or external fraud.
CGI ProperPay uses sophisticated algorithms to identify these anomalies for both payers and providers. By detecting high-risk claim behavior before it becomes a legal or financial liability, hospitals can maintain compliance and protect their reputation with major insurers.
6. AI Appeal Letter Support
When a denial occurs, AI accelerates the rebuttal process by summarizing the denial reason and suggesting the strongest evidence for the appeal. It can even draft templates tailored to the specific payer’s language.
Akasa uses AI to automate these repetitive tasks within the revenue cycle. This allows specialized staff to focus on the nuances of the case rather than spending hours on manual data entry and letter drafting.
7. AI Underpayment Detection
The system compares actual payments with expected reimbursement based on complex contracts and payer rules. This identifies instances where a hospital was paid less than the contracted rate.
Experian Health provides tools that specialize in contract management and underpayment recovery. By flagging these variances immediately, hospitals can recover earned revenue that would otherwise be lost to “silent” underpayments.
Deploying these use cases creates a robust financial defense for any healthcare institution. These technologies ensure that every service provided is accurately documented, billed, and paid. Strategic investment in these areas fundamentally changes the profitability profile of a hospital system.
Key Integrations Required For Hospital Claims Management Software
For an enterprise-grade AI solution to deliver on its promise, it must coexist within a complex web of existing hospital technology. A fragmented system is a failing system. True efficiency is achieved when the AI layer acts as a nervous system, connecting every department to a central financial objective.
1. EHR And EMR Integration
The EHR is the primary source of truth for patient care. The claims platform must pull clinical data directly to justify every billed service.
- Clinical Justification: Automatic extraction of clinical notes and discharge summaries to support medical necessity.
- Data Accuracy: Direct sync of diagnosis data and encounter history to eliminate manual transcription errors.
- Longitudinal View: Access to patient records ensures that recurring treatments are billed consistently over time.
2. HIS And PMS Integration
Hospital Information Systems (HIS) and Practice Management Systems (PMS) handle the administrative pulse of the facility. Integration here ensures that the financial journey starts correctly at the front desk.
- Workflow Continuity: Seamlessly links patient registration and admission data to the billing record.
- Scheduling Alignment: Syncs appointments and department-level workflows to track billable events as they happen.
- Operational Sync: Ensures that admission data matches the final claim to prevent identity or eligibility rejections.
3. RCM And Billing System Integration
Integrating with the core Revenue Cycle Management (RCM) infrastructure allows the AI to enhance existing billing workflows rather than replacing them.
- Advanced Charge Capture: Identifies missing charges by comparing clinical logs with the billing system’s output.
- Dynamic Coding: Facilitates real-time coding workflows and automated claim creation.
- Financial Tracking: Streamlines payment posting and denial management by updating the central billing ledger instantly.
4. Clearinghouse Integration
The clearinghouse acts as the gateway to the insurance world. A direct integration allows for a high-speed feedback loop between the hospital and the payer.
- EDI Standardization: Manages 837 claim submissions and 835 remittance advice with zero manual handling.
- Instant Feedback: Captures claim status updates and rejection reports the moment they are issued.
- Payer Response Loop: Automatically routes payer responses back into the AI engine for immediate analysis.
5. Payer Portal Integration
Directly querying payer portals bypasses the delays of traditional clearinghouse loops and phone calls.
- Real-Time Verification: Performs eligibility checks and authorization status updates in seconds.
- Direct Interaction: Enables automated appeal submission and denial updates directly within the insurer’s environment.
- Proactive Monitoring: Constantly polls for claim status changes to reduce the time a claim sits in “pending” status.
6. Document Management Integration
Hospitals generate mountains of paperwork that often live outside the structured EHR fields. Integrating with document systems captures this “hidden” evidence.
- Evidence Retrieval: Automatically attaches scanned forms, referral letters, and lab reports to claims.
- Unstructured Data Capture: Uses AI to read insurance documents and medical records stored in PDF or image formats.
- Audit Readiness: Maintains a central repository of all supporting documentation for easy retrieval during payer audits.
7. Analytics And BI Integration
Data is only valuable if it is actionable. Integrating with Business Intelligence (BI) tools transforms raw claim numbers into a strategy.
- Strategic Oversight: populates revenue dashboards with real-time data on denial trends and claim aging.
- Performance Benchmarking: Tracks payer performance and department-level reporting to identify systemic bottlenecks.
- Leakage Identification: Highlights specific areas of revenue leakage, allowing leaders to reallocate resources where they have the most impact.
A robust integration strategy ensures that the AI software is not just an add-on, but a foundational component of the hospital’s infrastructure. This connectivity is what separates a generic tool from an enterprise-grade financial engine.
Ultimately, these integrations create a transparent, high-velocity environment where every stakeholder has the data they need to drive the hospital’s mission forward.
AI Claims Management Software Architecture
A resilient AI claims architecture leverages a modular, microservices-based design to handle massive data throughput.
By combining FHIR-standard data ingestion with advanced ML inference layers, the system ensures sub-second processing speeds and enterprise-grade reliability for high-volume hospital environments.
Building a platform of this scale requires a sophisticated engineering approach that balances high-performance computing with extreme data sensitivity.
The architecture must be robust enough to handle millions of transactions while remaining flexible enough to adapt to daily changes in insurance regulations.
1. Data Ingestion Layer
The foundation of the architecture is a high-availability ingestion layer designed to communicate with disparate legacy systems. This layer ensures that data flows into the AI engine without latency or loss.
- Protocol Support: Utilizes HL7 and FHIR standards for seamless clinical data exchange alongside EDI 837/835 for financial transactions.
- Modern Connectivity: Employs RESTful APIs for real-time data sync and SFTP for secure batch uploads of historical records.
- Data Normalization: Automatically standardizes varying data formats from different hospital departments into a unified schema.
2. Document Intelligence Layer
Once raw data enters the system, the Document Intelligence layer translates visual and textual information into structured intelligence.
- Advanced Extraction: Uses high-precision OCR to pull data from complex claim forms and scanned medical records.
- Classification & Recognition: Employs specialized models for medical document classification and Named Entity Recognition (NER) to identify specific clinical terms.
- Reliability Controls: Every extraction is assigned a confidence score. If the score falls below a set threshold, the system triggers a manual verification request to ensure 100% accuracy.
3. AI And ML Layer
This is the brain of the platform where predictive models analyze the processed data to drive decision-making. This layer moves beyond simple “if-then” logic to identify subtle patterns in payer behavior.
- Predictive Modeling: Runs denial prediction and claim anomaly detection to stop revenue loss before it happens.
- Strategic Logic: Handles coding recommendations and appeal prioritization based on the likelihood of successful recovery.
- Continuous Learning: The models constantly retrain on new claim outcomes, becoming more accurate as more data passes through the system.
4. Rules Engine
The Rules Engine acts as a digital compliance officer, enforcing thousands of payer-specific mandates in real-time.
- Policy Enforcement: Manages current coding policies and authorization logic for hundreds of insurance carriers.
- Contract Intelligence: Performs automated contract checks to ensure reimbursement conditions are met.
- Regulatory Alignment: Hard-codes compliance rules to protect the facility from audit risks and legal discrepancies.
5. Workflow Automation Layer
This layer transforms AI insights into physical actions by orchestrating the movement of tasks across the organization.
- Dynamic Routing: Automatically directs claims to the appropriate team through intelligent task routing and approval flows.
- Efficiency Tracking: Manages exception handling and the entire appeal workflow while monitoring strict SLA tracking.
- Bot Orchestration: Uses robotic process automation to handle repetitive data entry, freeing up staff for complex clinical reviews.
6. Dashboard And Reporting Layer
The reporting layer translates complex backend operations into a clear, visual command center for hospital leadership.
- Real-time Visibility: Provides live views of claim status, denial trends, and immediate revenue risk.
- Management Tools: Tracks team workload and staff productivity to optimize departmental resources.
- Payer Analytics: Generates payer scorecards that highlight which insurers are most likely to delay or deny specific procedure types.
7. Security And Compliance Layer
Given the sensitivity of healthcare data, security is not a feature but the core framework of the entire architecture.
- Access Control: Implements strict Role-Based Access Control (RBAC) and multi-factor authentication.
- Data Protection: Ensures end-to-end encryption for data at rest and in transit, supplemented by sophisticated data masking for non-clinical users.
- Audit Integrity: Maintains immutable audit logs and consent controls to satisfy rigorous HIPAA and SOC2 compliance monitoring requirements.
An architecture built on these principles provides the stability and scalability required for global healthcare enterprises. It ensures that the software is not just a tool, but a reliable infrastructure asset for the long term.
Engineering excellence at this level is what enables a hospital to transform its financial future.
Compliance And Security Requirements For AI Claims Software
Enterprise AI claims platforms must adhere to a “security-by-design” philosophy to mitigate the inherent risks of processing Protected Health Information (PHI).
By combining HIPAA-compliant encryption with explainable AI models, hospitals can ensure that every automated decision is both secure and fully auditable by federal regulators.
Risk mitigation is the primary concern for any healthcare executive when introducing automation into the revenue cycle. A platform is only as valuable as its ability to protect the institution from data breaches and regulatory penalties.
Therefore, the architecture must prioritize transparency and ironclad security protocols at every touchpoint.
1. HIPAA-Ready Data Protection
The software must provide a fortified environment for PHI through multiple layers of technical safeguards.
- Encryption Standards: All data must be secured using AES-256 encryption at rest and TLS 1.2 or higher for data in transit.
- Secure Storage: Information is housed in Tier 4 data centers that meet rigorous physical and digital security standards.
- Persistence Controls: Automated audit logs track every instance of data access, ensuring that PHI protection remains continuous and verifiable for compliance officers.
2. Role-Based Access Control
Security is maintained by ensuring that individuals only access the data necessary for their specific function.
- Billing and Coding Teams: Access is limited to patient financial records and relevant clinical notes for claim justification.
- Administrators and Auditors: Granted high-level visibility for workflow oversight and compliance reporting without needing deep clinical access.
- Specialized Roles: Physicians and appeal teams see only the data required to resolve specific clinical or documentation gaps, preventing unnecessary data exposure.
3. Audit Trails For Every Claim Action
Transparency is maintained through an immutable ledger that records every interaction within the system.
- Modification Tracking: The system logs every claim edit, noting the user, the timestamp, and the specific field changed.
- AI Accountability: Every AI recommendation and subsequent user approval is captured to provide a clear history of the decision-making process.
- Submission History: All appeal submissions and payment updates are tracked, creating a comprehensive paper trail for internal reviews or external audits.
4. Explainable AI For Revenue Teams
To build trust and maintain compliance, the AI cannot operate as a “black box.” It must provide clear justifications for its actions.
- Logic Disclosure: When a claim is flagged, the system identifies exactly which payer rule or historical pattern triggered the alert.
- Actionable Insights: The software specifies what data was missing and provides a recommended course of action based on the identified gap.
- Confidence Scoring: Each recommendation includes a confidence level, allowing staff to understand the certainty behind the AI’s logic.
5. Secure Healthcare Integrations
Connectivity with external systems is managed through hardened protocols to prevent unauthorized data interception.
- Standardized Security: Utilizes secure authentication for all API, EDI, and FHIR-based data exchanges.
- Protocol Integrity: Employs HL7-compliant encryption to ensure that clinical data remains private as it moves between the EHR and the claims platform.
- Active Monitoring: Continuous surveillance of all integration points detects and blocks suspicious activity in real-time, maintaining a secure perimeter around the hospital’s data ecosystem.
By embedding these security measures into the core of the platform, hospitals can confidently scale their AI initiatives. These protocols do more than protect data; they provide the peace of mind required to innovate in a highly regulated landscape.
Ultimately, a secure system is the only sustainable foundation for long-term digital transformation.
Cost To Develop AI Claims Management Software For Hospitals
AI claims management software development for hospitals can cost between $60,000 and $350,000+, depending on AI features, claim workflow complexity, integrations, compliance needs, and enterprise scale.
The cost to develop AI claims management software for hospitals depends on how deeply the platform connects with real revenue cycle workflows. A simple claim validation MVP will cost less than a full claims intelligence system with denial prediction, coding support, payer rule checks, appeal automation, and EHR/RCM integrations.
Once the core problem is clear, the software scope becomes easier to estimate.
| Software Scope | Estimated Cost | Best For |
| Basic AI Claims MVP | $60,000–$100,000 | Startups, small hospitals, and focused claim validation |
| Mid-Level Claims Automation Platform | $100,000–$180,000 | Multi-specialty hospitals, billing teams, and RCM companies |
| Advanced AI Claims Management System | $180,000–$280,000 | Hospitals need denial prediction, coding support, and integrations |
| Enterprise Claims Intelligence Platform | $280,000–$350,000+ | Health systems, multi-location hospitals, and enterprise RCM operations |
What Affects The Development Cost?
Several factors shape the final development cost:
- The number of AI modules: OCR, NLP, denial prediction, coding support, and appeal automation increases the scope.
- Claim workflow complexity: Inpatient, outpatient, emergency, diagnostics, and specialty claims need different logic.
- EHR and RCM integrations: Connecting with hospital systems, billing platforms, and clearinghouses adds development effort.
- Payer rule engine: The platform may need payer-specific rules for authorization, coding, eligibility, and documentation.
- Dashboard complexity: Basic claim tracking costs less than executive-level revenue, denial, and payer analytics.
- Data migration: Historical claims, denial records, payment files, and documents may need cleanup.
- Compliance requirements: Role-based access, encryption, audit logs, and PHI protection increase engineering scope.
- Deployment model: Cloud, private cloud, multi-location, and enterprise-grade deployments affect the budget.
Hidden Costs Hospitals Should Plan For
Hospitals should also budget for:
- Data cleanup: Old claim records may be incomplete, duplicated, or poorly structured.
- Payer rule updates: Insurance rules, authorization needs, and coding policies change often.
- Legacy integration: Older hospital systems may need custom connectors or middleware.
- Staff training: Billing, coding, and denial teams need time to adopt the platform.
- AI monitoring: Models need regular checks for accuracy, drift, and payer pattern changes.
- Compliance testing: Security, access, audit logs, and PHI handling must be verified.
- Maintenance: The platform will need updates, bug fixes, security patches, and feature improvements.
Hospitals should not treat AI claims management software as a one-time build. It works best as a long-term claims intelligence system that improves reimbursement speed, reduces denials, and gives revenue teams better control.
At Intellivon, we help hospitals define the right scope before development begins. This keeps the budget focused on the workflows that directly improve claim accuracy, denial prevention, and revenue cycle performance.
Development Timeline For AI Claims Management Software
For entrepreneurs and investors, understanding the lifecycle of this development is critical for managing capital and expectations.
Building in the healthcare sector involves unique hurdles that do not exist in traditional fintech or general enterprise SaaS.
| Development Stage | Estimated Timeline |
| Discovery and workflow mapping | 2–4 weeks |
| Product architecture and UX planning | 3–5 weeks |
| MVP development | 12–20 weeks |
| AI model development and testing | 8–16 weeks |
| EHR/RCM/clearinghouse integrations | 8–20 weeks |
| Compliance and security testing | 4–8 weeks |
| Pilot rollout | 4–8 weeks |
| Enterprise rollout | 6–12+ months |
Execution speed is often dictated by the quality of the initial discovery phase. Identifying exactly where the revenue leakage occurs allows the engineering team to prioritize the features that deliver the fastest ROI.
Why Hospital Claims Software Takes Longer Than Generic SaaS
Building for hospitals requires navigating a complex web of dependencies that go beyond simple code. Unlike a standard app, a claims platform must achieve perfect synchronization with clinical realities and regulatory mandates.
- Legacy Integrations: Many hospitals still rely on older, on-premise systems that lack modern APIs. Consequently, building custom bridges for data exchange takes significant engineering effort.
- Healthcare Data Complexity: The variety of data types—ranging from structured ICD-10 codes to unstructured physician notes—requires extensive data cleaning and normalization before the AI can even begin to process it.
- Compliance Testing: Security audits for HIPAA and SOC2 are non-negotiable. Every feature must undergo rigorous stress testing to ensure zero data leakage.
- Payer-Specific Rules: Because each insurance carrier has unique requirements, the rules engine must be manually validated against hundreds of different contract types.
- Clinical Documentation Dependencies: The software must be tuned to understand specific clinical workflows. This ensures that the AI’s suggestions do not create additional administrative burdens for doctors and nurses.
These complexities mean that the development process is iterative. Successful deployment requires a partner who understands both the technical architecture and the nuances of the medical billing environment.
By accounting for these factors early in the roadmap, investors can ensure the platform is built for long-term stability and enterprise adoption. Careful planning during these phases prevents the “technical debt” that often plagues rushed healthcare software projects.
Step-By-Step Process To Develop AI Claims Management Software
Building a high-performance intelligence layer is a structured, multi-phase engineering approach.
We focus on creating a system that integrates deeply with your existing operations while ensuring every automated decision is defensible, accurate, and scalable across a global healthcare enterprise.
Step 1: Hospital Claims Workflow Discovery
We begin by deconstructing your current claim lifecycle to identify every manual touchpoint and decision node.
This mapping ensures the AI understands the specific nuances of your departmental logic and the unique “unwritten rules” of your payer contracts.
- Workflow Mapping: We analyze historical denial patterns and billing bottlenecks to identify where revenue is currently leaking.
- System Audit: We review your team roles and existing systems like the EHR and HIS to ensure a seamless technical fit without disrupting clinical workflows.
- Payer Mix Analysis: Understanding your specific payer mix allows us to prioritize the rules engines that will yield the highest ROI during the initial launch.
| Phase | Key Activity | Stakeholders Involved |
| Discovery | Deep-dive into denial data and manual touchpoints | CFO, Billing Manager, IT Lead |
| Mapping | Visualizing the “as-is” vs “to-be” workflow | RCM Director, Solution Architect |
| Gap Analysis | Identifying documentation and coding blind spots | Coding Lead, Compliance Officer |
Step 2: AI Module Selection
Once the workflow is clear, we define which intelligence modules will drive the most immediate value. Most hospitals prioritize document extraction and denial prediction to clear high-volume backlogs and stabilize cash flow.
- Core Extraction: Selecting high-precision OCR and NLP modules specifically trained on medical terminology and payer forms.
- Predictive Analytics: Implementation of denial prediction and anomaly detection to flag high-risk claims before they are submitted.
- Operational Support: Integration of coding support and appeal automation to reduce the cognitive load on your billing specialists.
Step 3: Data Preparation
Quality output requires high-fidelity input. We aggregate diverse datasets from your historical archives to train the models on your specific patient demographics and local payer behaviors.
- Historical Aggregation: We ingest years of claim records, denial logs, and payment data to create a robust baseline for the machine learning models.
- Clinical Enrichment: Inclusion of physician notes, lab reports, and discharge summaries to train the NLP engine on nuanced clinical documentation standards.
- Data Cleansing: We rigorously remove duplicates and correct errors in historical records to prevent the “garbage in, garbage out” scenario that plagues many AI projects.
Step 4: Product Architecture
Our architects build a robust pipeline that balances raw processing power with human-centric design.
This multi-layered system handles data ingestion and intelligent processing simultaneously, ensuring zero latency during peak billing cycles.
- Scalable Infrastructure: We utilize cloud-native microservices and secure APIs to ensure the platform grows with your hospital’s transaction volume.
- Intelligence Pipelines: Construction of dedicated pipelines for real-time risk scoring, medical necessity checks, and documentation gap detection.
- Enterprise Dashboard: Structuring the command center to provide executive-level visibility into “at-risk” revenue and department-level productivity.
| Layer | Technology Focus | Primary Function |
| Ingestion | FHIR / HL7 / EDI APIs | Real-time data sync with EHR and HIS |
| Inference | NLP & Predictive ML Models | Denial risk scoring and clinical note analysis |
| Orchestration | Workflow Automation Engines | Smart task routing and appeal drafting |
| Presentation | BI Dashboards & Work Queues | Strategic oversight and daily task management |
Step 5: MVP Development
We develop the core interface where your team will interact with AI insights daily. This phase focuses on delivering a functional “clean claim” engine as quickly as possible to prove the concept and begin recapturing revenue.
- Core Engine: Building the claim intake, validation engine, and fundamental AI risk scoring modules.
- Review Interface: Developing the “Human-in-the-Loop” queue where specialists can easily approve or override AI recommendations.
- Baseline Reporting: Providing a clear view of initial performance metrics, including first-pass clean claim rates.
Step 6: AI Model Training And Testing
During this phase, we subject the models to rigorous stress tests using real-world scenarios to ensure clinical and financial accuracy meets enterprise standards.
- Accuracy Benchmarking: We test the model against thousands of historical denial outcomes to verify that its predictions are statistically significant.
- Bias & Fairness Audits: We run regular checks to ensure the AI logic does not develop unfair patterns based on demographic data or specific provider groups.
- Continuous Refinement: Implementing feedback loops where human reviewer actions are fed back into the system to sharpen the AI’s decision-making logic over time.
Step 7: Integration With Hospital Systems
A platform is only as good as its connectivity. We ensure a seamless data flow across your entire tech stack to eliminate the manual data entry that leads to human error.
- Bidirectional Sync: Secure integration with EHR (Epic, Cerner, etc.) and RCM platforms for real-time data exchange.
- Payer Gateways: Linking the system directly to clearinghouses and payer portals for automated status updates and faster submissions.
- Financial Reconciliation: Ensuring the PMS and billing records stay perfectly updated as the AI moves claims through their lifecycle.
Step 8: Compliance And Security Testing
We treat regulatory compliance as a core feature rather than a final checklist item. Following HIPAA, SOC2, and international data standards, we build in the frameworks that keep you in control.
- Security Hardening: Implementation of strict role-based access controls, end-to-end encryption, and sophisticated PHI handling protocols.
- Penetration Testing: Rigorous third-party testing to identify and patch potential vulnerabilities before the system is deployed.
- Explainability Layers: Ensuring every AI-driven action includes a clear “reasoning” trail that can be understood by auditors and revenue teams alike.
This rigorous development process ensures your platform is not just another piece of software, but a strategic financial asset. By following this roadmap, we deliver a solution that scales with your growth, withstands regulatory scrutiny, and delivers a measurable impact on your bottom line.
By finalizing this step-by-step implementation, the hospital moves from a state of reactive billing to a model of total revenue intelligence. This structured approach guarantees that the resulting AI ecosystem is resilient, transparent, and fully aligned with the hospital’s long-term operational goals.
Challenges In AI Claims Management Software Development
The transition to an AI-driven revenue cycle is not without its friction. While the ROI is significant, enterprise leaders must anticipate and solve for specific structural challenges that can impede the performance of the software.
1. Incomplete Or Inconsistent Claim Data
AI models are only as effective as the data that feeds them. In many hospitals, patient information is scattered across the EHR, scanned PDFs, and siloed billing systems.
This fragmentation leads to “data noise,” where missing clinical notes or inconsistent field entries make it difficult for the AI to predict outcomes with high accuracy.
The Solution: Implement an automated data-cleansing layer during the ingestion phase. By using NLP to extract and structure data from unstructured documents before it hits the model, we ensure the AI works with a “single source of truth” that is both clean and comprehensive.
2. Changing Payer Rules
Insurance companies update their medical necessity policies and coding requirements constantly. A static system becomes obsolete within months, leading to a sudden spike in denials. Keeping a manual track of thousands of changing rules across hundreds of payers is an impossible task for human teams.
The Solution: Use a dynamic, cloud-based rules engine that updates in real-time. By leveraging web-scraping and API-based monitoring of payer portals, the software can automatically adjust its validation logic as soon as a policy change is detected.
3. Legacy Hospital System Integration
Many large health systems operate on a patchwork of disconnected legacy software, some of which may be decades old. These systems often lack the modern APIs required for real-time data exchange, creating “digital dead zones” where information gets stuck.
The Solution: Build modular “middle-layer” connectors. Instead of attempting a risky and expensive overhaul of the legacy HIS, the AI platform uses custom adapters (HL7/FHIR bridges) to pull and push data without disrupting the stability of the underlying core systems.
4. Low Adoption By Billing Teams
Introducing AI can be met with resistance if the staff feels the software is a “black box” that adds more work or threatens their job security. If the tool is too complex or forces a radical change in daily habits, adoption rates will plummet, and the system will fail to deliver results.
The Solution: Design the software to fit existing workflows. The AI should act as a “copilot” that sits within the current billing interface, providing suggestions and automating repetitive tasks like data entry, rather than forcing the team to learn a completely new platform.
5. AI Explainability Issues
Revenue teams cannot act on a flag if they do not understand the logic behind it. If a claim is marked as “high risk” without an explanation, the staff is likely to ignore the warning, leading to avoidable denials.
The Solution: Prioritize “Explainable AI” (XAI). Every flag or recommendation must be accompanied by a clear, human-readable justification. For example, “Flagged due to missing prior authorization for CPT 93000 based on recent Aetna policy update.”
6 Compliance And PHI Risk
In a healthcare environment, there is zero room for error regarding data privacy. Managing massive datasets across various AI modules increases the “attack surface” for potential breaches, making PHI protection a massive engineering challenge.
The Solution: Implement a “Security-First” architecture. This includes end-to-end encryption, automated data masking for non-clinical users, and immutable audit logs that track every touchpoint. Regular penetration testing and automated compliance monitoring ensure that the system stays protected against evolving threats.
Solving these challenges is what separates a generic AI tool from a high-impact enterprise asset. By addressing these hurdles early in the development lifecycle, we build a platform that is not only smart but also resilient and trustworthy.
Ultimately, overcoming these barriers creates a transparent environment where technology and human expertise work in perfect harmony.
Conclusion
Modern hospitals must transition from reactive billing to proactive, AI-driven revenue intelligence to remain solvent. Automating complex workflows like denial prediction and clinical documentation review eliminates administrative friction and secures earned revenue.
This strategic shift provides the financial stability required to enhance patient care. Adopting these intelligent systems is now a necessity for any healthcare enterprise seeking long-term operational excellence.
Builds AI CMS Software With Intellivon
At Intellivon, we develop AI CMS software for hospitals, health systems, RCM companies, healthcare SaaS platforms, billing companies, and enterprise care networks.
Our systems help teams reduce avoidable denials, improve claim accuracy, speed up reimbursements, and manage claims workflows with better visibility.
A. Help You Define The Right Claims Software Scope
We start by identifying where AI can create the highest revenue impact before development begins.
- MVP planning
- Claim workflow discovery
- AI module selection
- Denial pattern analysis
- Payer mix review
- Product roadmap planning
B. Build AI Workflows Around Hospital Claims Operations
We design AI workflows around real hospital revenue cycle tasks, not generic automation.
- Claim intake automation
- OCR and document processing
- Claim validation
- Denial risk scoring
- Coding support
- Appeal workflow automation
C. Integrate With Your Healthcare Systems
We connect the platform with the systems your billing, coding, finance, and clinical teams already use.
- EHR and EMR systems
- HIS and PMS platforms
- RCM and billing software
- Clearinghouses
- Payer portals
- Payment systems
- Document management tools
D. Make Claims AI Secure, Explainable, And Scalable
We build AI claims systems with the controls hospitals need for PHI, compliance, and enterprise use.
- Role-based access
- Audit trails
- Data encryption
- AI confidence scores
- Human review queues
- Secure APIs
- Model monitoring
If your hospital wants to reduce denials, automate claim review, improve reimbursement speed, or build a custom AI claims management platform, Intellivon can help you build the right system from the ground up.
Contact Intellivon to build AI CMS software that protects hospital revenue and simplifies claims operations.
Things To Know About CMS Platforms
Q1. Can AI claims management software actually reduce hospital denials?
A1. Yes, but only when it prevents errors before submission. AI can flag missing documents, coding mismatches, eligibility gaps, authorization issues, and payer-specific claim rules. Hospitals should use it as a pre-submission risk layer, not just a post-denial tracking tool after revenue has already been delayed.
Q2. Will AI replace hospital billing and coding teams?
A2. No. AI helps billing and coding teams handle repetitive checks faster, but it still needs human review. Hospital claims involve clinical context, payer disputes, documentation judgment, compliance, and exceptions. The strongest systems use AI to support coders, not replace final billing decisions.
Q3. What should hospitals look for in AI claims management software?
A3. Hospitals should look for eligibility verification, claim scrubbing, denial prediction, payer rule validation, appeal workflows, reporting, analytics, and EHR/RCM integration. The software should also include audit trails, role-based access, and human review queues so teams can trust every AI recommendation before acting.
Q4. Can poorly designed AI claims software increase denials?
A4. Yes. If AI coding or claim automation works without proper validation, it can create incorrect claims, documentation gaps, and more denials. Hospitals need explainable AI, confidence scores, clean data, payer-specific rules, human approval steps, and continuous monitoring to keep the system safe and accurate.