Key Takeaways:
- AI denial platforms prevent rejections before submission by validating claims against payer rules.
- Denial rates between 15 and 20% cost the industry up to $25 billion annually.
- NLP, generative AI, and machine learning work together to automate appeal drafting and recovery.
- Platform development covers ingestion, prediction, appeal automation, analytics, and audit-ready compliance controls.
- Intellivon engineers intelligent systems that reduce preventable denials and accelerate revenue recovery.
Claim denials represent one of the most recoverable revenue losses in hospital operations, and the window to recover them is shrinking. This is because payers are deploying AI to scrutinize documentation, apply policy rules, and automate rejection decisions faster than hospital billing teams can respond. The cost of reworking, appealing, and resubmitting denied claims has consequently made denial management one of the most expensive inefficiencies in the revenue cycle.
AI denial management software addresses this as infrastructure, and not as a bolt-on tool. It prevents denials before submission by validating claims against payer rules, prioritizes recovery after rejection based on value and appeal probability, automates appeal workflows with supporting documentation, and gives revenue teams payer-level visibility into exactly where and why revenue is leaking.
Building this platform requires claims intelligence, payer behavior modeling, workflow automation, EHR and RCM integrations, explainable decision logic, and audit-ready infrastructure working together across the full denial lifecycle.
Intellivon engineers AI claims denial management platforms for hospitals, health systems, RCM companies, and healthcare SaaS founders who need a system that fights denials with the same intelligence that payers use to issue them. This blog draws from our experience and covers exactly how to build one.
Why Healthcare Businesses Are Building AI Denial Management Platforms
Claim denials have moved from a billing inconvenience to a financial infrastructure problem. As denial rates climb and payer rules grow more complex, healthcare businesses are building AI denial management platforms to protect revenue that manual workflows can no longer recover at scale.
1. The Denial Crisis Crushing Hospital Margins
Denial rates across U.S. providers now sit between 15 and 20%, costing the industry between USD 20 and 25 billion annually in appeals and lost revenue.
Furthermore, 41% of providers are facing denial rates above 10%, a figure that has risen steadily since 2022. Missing data accounts for 50% of denials, while authorization failures drive another 35%.
Hospitals spend USD 19.7 billion each year overturning denials, and 54% of those denials are eventually paid, but only after costly multi-round appeals that delay cash flow and consume staff capacity.
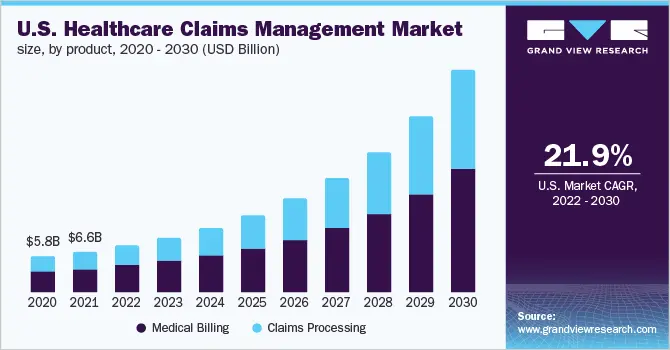
The U.S. healthcare denial management market reached USD 5.13 billion in 2024 and is projected to reach USD 8.93 billion by 2030 at a CAGR of 9.68%. AI-powered segments are expanding considerably faster as platforms like Innovaccer, Waystar, Experian Health, and Goml demonstrate measurable denial reduction at scale.
2. What AI Denial Platforms Actually Deliver
Healthcare organizations adopting AI denial management are reporting 20 to 30% reductions in denial rates and 69% higher resubmission success rates. The operational impact comes from three core capabilities:
- Predictive denial prevention: AI scans claims before submission to flag coding errors, missing documentation, and authorization gaps that account for over 60% of human error-driven rejections
- Automated appeals generation: NLP extracts clinical evidence and generative AI drafts payer-specific appeal letters, cutting rework from weeks to hours
- Root cause analytics: Real-time dashboards surface denial patterns such as missing authorization, driving 35% of cases, enabling revenue teams to fix problems upstream rather than chase them downstream
3. The Market Reflecting That Urgency
AI-powered segments are expanding considerably faster as platforms like Innovaccer, Waystar, Experian Health, and Goml demonstrate measurable denial reduction at scale. For healthcare businesses still relying on manual denial workflows, that competitive gap is becoming a revenue gap.
AI denial management is therefore not a process improvement initiative. It is financial infrastructure, and the organizations building it now are setting the standard that the rest of the market will eventually be measured against.
What Is An AI Claims Denial Management Platform?
An AI claims denial management platform is an infrastructure that manages the full denial lifecycle across prevention, recovery, and analysis.
It validates claims against payer rules before submission to reduce rejection risk, scores denied claims by recovery probability to prioritize appeal effort, automates appeal generation using clinical documentation, and tracks payer behavior patterns to identify where denials are originating.
Unlike standalone denial tracking tools, it connects directly into RCM, EHR, and billing workflows so that denial intelligence feeds back into the claims process rather than sitting in a separate reporting layer.
Building a platform for automated claims management involves more than just basic filtering. It functions as an intelligent layer that sits between the provider and the payer to ensure financial integrity.
1. It Prevents Denials Before Claim Submission
Prevention represents the most cost-effective stage of the revenue cycle. By implementing an AI layer at the front end, you can identify errors that human reviewers typically overlook.
This proactive approach ensures that only “clean claims” move forward, which drastically reduces the initial rejection rate.
- Automated Claim Validation: The system scans every field against current coding standards to ensure data integrity.
- Payer-Specific Edits: AI adapts to the unique rules of different insurance carriers to prevent format-related rejections.
- Eligibility Verification: Real-time checks confirm a patient’s active coverage before the provider renders expensive services.
- Documentation Integrity: Natural language processing identifies missing clinical notes or required attachments that support the billed services.
- Prior Authorization Review: The platform cross-references clinical orders with payer requirements to ensure necessary approvals are in place.
2. It Helps Teams Recover Denied Claims Faster
When a denial occurs, the platform transforms from a shield into a recovery engine. It removes the manual burden of sorting through thousands of reason codes. Instead, it prioritizes tasks based on the probability of a successful appeal and the total dollar value at risk.
- Smart Denial Categorization: Machine learning models group denials by root cause so teams can address systemic issues at once.
- Automated Appeal Generation: The system drafts custom appeal letters by pulling relevant clinical data and policy language automatically.
- Intelligent Work Queues: AI routes the most complex cases to senior specialists while automating the simple administrative fixes.
- Resubmission Tracking: The platform monitors the status of every corrected claim to ensure it does not disappear in the payer portal.
3. It Turns Denial Data Into Revenue Cycle Intelligence
Data is the ultimate asset for any investor in this space. An AI platform does not just fix individual claims but provides a macro-view of the entire financial ecosystem. This intelligence allows leaders to make strategic decisions that improve long-term margins.
- Payer Behavior Trends: Track which insurance companies are changing their policies or increasing their denial rates for specific procedures.
- Root-Cause Dashboards: Visualize exactly where the revenue leak is happening, whether it starts in the front office or the billing department.
- Service-Line Insights: Identify which medical departments have the highest overhead due to administrative friction.
- Continuous Process Improvement: The AI learns from every successful appeal to suggest permanent workflow changes for the provider staff.
An AI Claims Denial Management Platform is an enterprise-grade solution that uses machine learning to validate claims, automate appeals, and provide predictive analytics. It functions as a strategic tool for revenue cycle management (RCM) by shifting from reactive billing to proactive financial optimization.
Core Features Of An AI Claims Denial Management Platform
Building an enterprise-grade platform requires a strategic focus on features that maximize reimbursement while minimizing manual labor. These tools must work together to create a seamless flow from the patient encounter to the final payment.
The core features include denial prediction, claim scrubbing, documentation intelligence, appeal automation, payer analytics, work queue management, and RCM integrations.
1. Denial Risk Scoring
The platform evaluates every claim against historical patterns to assign a specific probability of rejection. This allows teams to intervene before the claim ever reaches the insurance carrier.
- Predictive Modeling: Uses machine learning to identify hidden patterns that lead to common rejections.
- Pre-submission Alerts: Flags high-risk claims for immediate correction by the billing staff.
- Probability Weighting: Focuses human attention on claims most likely to be denied.
2. AI-Powered Claim Scrubbing
Standard scrubbing is often too rigid to handle complex healthcare billing. AI-driven scrubbing adapts to the shifting rules of thousands of different payers simultaneously.
- Coding Accuracy: Verifies that ICD-10 and CPT codes align with the latest clinical guidelines.
- Modifier Validation: Checks for the correct use of modifiers to prevent simple administrative denials.
- Authorization Sync: Confirms that the procedure code matches the authorization obtained from the payer.
3. Clinical Documentation Review
Missing evidence is a primary cause of revenue loss. Natural language processing (NLP) scans medical records to ensure the clinical narrative supports the billed services.
- Note Analysis: Searches through physician notes to find specific keywords required for reimbursement.
- Discharge Summaries: Links hospital discharge data to the final bill to ensure consistency.
- Attachment Automation: Identifies which reports or images must be sent with the claim to avoid “missing info” requests.
4. Denial Code Classification
The system translates confusing CARC and RARC codes into actionable business insights. This helps management understand whether a problem is clinical, administrative, or technical.
- Payer Grouping: Normalizes different payer languages into a single, unified view for the user.
- Operational Tagging: Labels denials as “avoidable” or “unavoidable” to guide team strategy.
- Trend Tracking: Monitors if a specific denial code is spiking across a certain specialty or location.
5. Automated Appeal Drafting
Generating manual appeals is the most time-consuming part of the recovery process. The AI automates this by creating professional, evidence-backed documents in seconds.
- Payer-Specific Templates: Use the exact format preferred by the insurance company to speed up processing.
- Evidence Collection: Automatically attaches the specific medical records needed to overturn the denial.
- Policy Integration: Quotes the latest payer policy language directly in the letter to increase success rates.
6. Work Queue Prioritization
Labor is the highest cost in the revenue cycle. The platform ensures that every minute spent by a biller is directed toward the highest possible ROI.
- Dollar Value Routing: Automatically moves high-dollar denials to the top of the specialist’s list.
- Success Probability: Prioritizes claims that have a high likelihood of being paid upon resubmission.
- Deadline Management: Tracks filing limits to ensure no claim becomes uncollectible due to age.
7. Root-Cause Analytics
Effective platforms stop the “revolving door” of denials by identifying where errors originate. This moves the organization from reactive fixing to proactive prevention.
- Provider Tracking: Identifies if specific clinicians are consistently failing to document necessary details.
- Specialty Analysis: Highlights which medical departments are struggling with specific payer requirements.
- Systemic Fixes: Suggests changes to the front-end registration process to eliminate eligibility errors.
8. Payer Performance Dashboards
Transparency is essential when negotiating with large insurance carriers. These dashboards provide the data needed to hold payers accountable for their behavior.
- Payer Scorecards: Compares the denial rates and payment speeds of different insurance companies.
- Overturn Rates: Measures how often a payer admits an error after an appeal is filed.
- Negotiation Leverage: Uses objective data to support better terms during annual contract renewals.
Investment in an AI claims platform transforms the revenue cycle from a cost center into a predictable, high-margin asset.
How An AI Denial Management Platform Works
Modern denial management requires a sophisticated technical architecture that connects various data silos into a single source of truth. By following a structured six-step workflow, the platform transforms fragmented healthcare data into a streamlined engine for revenue recovery.
An AI denial management platform ingests claim, clinical, payer, and payment data, detects denial risks, recommends corrections, automates appeals, and tracks recovery outcomes.
Step 1: Claim And RCM Data Ingestion
The process begins by pulling data from multiple external and internal sources to create a comprehensive view of every patient encounter. High-performance platforms utilize robust APIs to ensure that information flows in real time without manual entry.
- EHR and PMS Integration: The system pulls clinical notes and scheduling data directly from Electronic Health Records and Practice Management Systems.
- Clearinghouse Connectivity: It ingests data from clearinghouses to track the movement of claims between the provider and the insurance company.
- Billing System Sync: Financial records and patient ledgers are synchronized to ensure every billed dollar is accounted for in the analysis.
- ERA/EOB Processing: The AI parses Electronic Remittance Advice (ERA) and Explanation of Benefits (EOB) files to identify exact payment amounts and rejection reasons.
- Historical Claim History: Ingesting years of past data allows the machine learning models to recognize long-term patterns in payer behavior.
Step 2: Data Normalization And Denial Mapping
Raw data from different payers often arrives in inconsistent formats that make side-by-side analysis nearly impossible. This stage involves cleaning and standardizing the information so that the AI can perform accurate comparisons.
- Standardized Categorization: The platform maps thousands of unique payer codes into a few dozen primary denial categories for easier reporting.
- Payer Code Mapping: It aligns specific carrier reason codes with industry-standard CARC and RARC definitions to remove ambiguity.
- Duplicate Detection: The system identifies redundant claims or double-billings that could lead to unnecessary fraud investigations or rejections.
- Claim Lifecycle Tracking: Every claim is assigned a unique digital footprint to monitor its progress from the initial draft to the final bank deposit.
Step 3: Pre-Submission Denial Risk Analysis
The most critical work happens before the claim ever reaches the insurance company. By running every submission through a predictive model, the platform stops errors before they become costly administrative burdens.
- Predictive Risk Scoring: The AI calculates the probability of a denial based on current payer trends and historical rejection data.
- Pattern Recognition: It identifies combinations of codes or patient demographics that have historically triggered audits or delays.
- Real-Time Simulation: The system simulates the payer’s adjudication engine to see if the claim passes all known clinical and financial rules.
Step 4: Claim Correction And Human Review
AI does not replace human expertise but rather amplifies it by highlighting the specific areas that require professional attention. This collaborative approach ensures that complex medical nuances are always respected during the billing process.
- Intelligent Recommendations: Instead of just flagging an error, the platform suggests the specific correction or missing modifier needed for approval.
- Coder Review Workflows: High-risk claims are automatically routed to certified coders who can verify clinical accuracy within the platform.
- Biller Review Interface: Administrative staff can quickly address simple errors like missing subscriber IDs or incorrect birth dates through a centralized dashboard.
- Exception Handling: The system learns from human overrides to refine its future predictions and reduce false-positive alerts.
Step 5: Appeal Workflow Automation
When a denial is unavoidable, the platform shifts into high gear to recover the funds as quickly as possible. This step removes the repetitive administrative tasks that usually slow down the resubmission process.
- Automated Appeal Drafts: The AI generates a professional appeal letter that is pre-populated with all necessary patient and policy information.
- Evidence Packet Assembly: It automatically gathers the specific clinical notes, lab results, and authorization forms required to prove the case.
- Deadline Monitoring: Integrated calendars track the filing limits for every payer to ensure that no claim expires before it can be appealed.
- One-Click Resubmission: Once a human approves the appeal, the system transmits it directly back to the payer or the clearinghouse.
Step 6: Performance Learning And Model Monitoring
The final stage ensures that the platform gets smarter with every single transaction. By monitoring the outcomes of appeals and shifts in payer behavior, the system stays ahead of the constantly changing healthcare landscape.
- Feedback Loops: The AI analyzes which appeals were successful and which were rejected to improve its future drafting logic.
- Appeal Outcome Analysis: It tracks the “win rate” for different denial types to help management decide where to focus their recovery resources.
- Payer Behavior Monitoring: If a carrier suddenly changes its policy on a specific procedure, the AI detects the trend and updates the risk models immediately.
- Continuous Model Retraining: Data scientists and algorithms work together to retrain the underlying models on the latest reimbursement data every week.
Implementing these automated steps ensures that every claim follows the path of least resistance toward full reimbursement. This technical workflow creates a reliable foundation for scaling revenue without increasing administrative headcount.
AI Models Used In Denial Management Software
Selecting the right technological stack is vital for building a platform that balances automation with clinical integrity. The most effective systems do not rely on a single algorithm but rather a collection of specialized models working in concert.
AI denial management platforms use machine learning, NLP, rules engines, RPA, generative AI, analytics pipelines, and secure healthcare integrations.
1. Machine Learning For Denial Prediction
Predictive models analyze millions of historical data points to identify which claims are likely to encounter resistance. This allows the system to flag potential issues long before they impact the bottom line.
- Historical Pattern Analysis: The model identifies specific combinations of codes and patient demographics that payers frequently reject.
- Risk Probability Scoring: Every claim receives a score that reflects its likelihood of approval based on current market conditions.
- Trend Identification: The system detects when a payer subtly shifts their adjudication logic so providers can adapt immediately.
2. NLP For Clinical Documentation Review
Natural Language Processing (NLP) bridges the gap between unstructured medical notes and structured billing data. It ensures that the clinical reality of the patient encounter is accurately reflected in the financial submission.
- Entity Extraction: The AI identifies specific diagnoses, procedures, and symptoms within physician narratives.
- Consistency Checking: It cross-references doctor notes against billed codes to ensure the documentation supports the requested payment level.
- Missing Evidence Detection: The system flags instances where a required piece of clinical proof is absent from the file.
3. Rules Engines For Payer-Specific Validation
While AI handles the complex patterns, a deterministic rules engine ensures that basic payer requirements are met with 100% accuracy. This hybrid approach combines the flexibility of machine learning with the rigidity of insurance contracts.
- Contract Logic Enforcement: The system applies specific billing rules negotiated with each individual insurance carrier.
- Standardized Edits: It performs basic checks for formatting, patient eligibility, and provider credentials.
- Hybrid Validation: The engine combines logic-based rules with AI risk scores to provide a comprehensive claim review.
4. Generative AI For Appeal Drafting
Generative models have revolutionized the speed at which administrative teams can respond to denials. However, the focus remains on “augmented intelligence,” where the AI assists the human expert rather than replacing them.
- Dynamic Letter Generation: The AI drafts custom appeal letters that quote specific payer policies and clinical guidelines.
- Evidence Summarization: It condenses long medical records into concise summaries that prove medical necessity to the payer.
- Policy Alignment: The model ensures that the language used in the appeal aligns perfectly with the latest insurance carrier requirements.
5. RPA For Repetitive Claim Tasks
Robotic Process Automation (RPA) handles the high-volume, low-complexity tasks that typically bog down a billing department. This allows skilled staff to focus on complex cases that require human judgment.
- Automated Status Checks: Bots log into payer portals to verify the current status of pending claims without human intervention.
- Data Entry Automation: The system moves information between different software platforms to eliminate manual transcription errors.
- Follow-Up Scheduling: RPA ensures that every denied claim is revisited at the appropriate interval until a final resolution is reached.
6. Analytics Pipelines For Revenue Cycle Reporting
Converting raw data into actionable intelligence requires a robust pipeline that can process information at scale. These pipelines feed the dashboards that help executives make high-level strategic decisions.
- Real-Time Data Processing: The system updates financial metrics as soon as a payment or denial is recorded.
- Attribution Modeling: It identifies which specific interventions or staff members are driving the highest recovery rates.
- Predictive Financial Forecasting: Leadership can use the data to project future cash flows based on current claim volumes and rejection rates.
Modern AI applications in healthcare must remain transparent and auditable to ensure fair adjudication and regulatory compliance. Combining these sophisticated models creates a reliable framework that enhances human decision-making rather than operating in a “black box” environment.
Data To Build An AI Claims Denial Management Platform
The strength of any predictive model depends entirely on the quality and variety of the data it consumes. Building a reliable platform requires access to diverse data sets that capture the entire journey of a claim from creation to final adjudication.
AI denial management platforms need historical claims, denial codes, payer responses, clinical documentation, eligibility data, authorization data, payment data, and appeal outcomes.
1. Historical Claims Data
Past performance is the best predictor of future payer behavior. Ingesting years of claim history allows the AI to understand the baseline for “clean” submissions and identify anomalies that lead to financial friction.
- Core Claim Attributes: The system tracks billed amounts, CPT codes, and ICD-10 codes to identify high-value service patterns.
- Modifier Utilization: It analyzes how specific modifiers impact reimbursement rates across different medical specialties.
- Entity Mapping: Data includes the specific provider, facility, and payer involved to detect localized issues or systemic bias.
- Outcome Tracking: The final status of every historical claim provides the “ground truth” needed to train machine learning models.
2. Denial And Remittance Data
Understanding why a claim was rejected is just as important as knowing it was denied. Granular remittance data allows the platform to categorize problems and suggest precise administrative fixes.
- Reason Code Analysis: The AI parses CARC and RARC codes to understand the specific justification provided by the insurance carrier.
- ERA and EOB Parsing: Digital and paper-based remittance files are converted into structured data for deep comparative analysis.
- Payer Commentary: The system captures free-text comments from adjusters, which often contain clues for successful appeals.
- Rejection Timing: Tracking how long a payer takes to issue a rejection helps in forecasting cash flow volatility.
3. Clinical Documentation
Modern insurance carriers increasingly deny claims based on a perceived lack of “medical necessity.” Therefore, the platform must have access to the underlying clinical narrative to prove that the services provided were appropriate.
- Physician Narratives: NLP models analyze progress notes and consultation reports to extract supporting evidence for billed codes.
- Diagnostic Reports: Lab results and imaging findings are cross-referenced to ensure they justify the level of care provided.
- Discharge Summaries: These documents provide a high-level overview of the patient’s condition, which is essential for complex inpatient appeals.
- Evidence of Necessity: The system flags specific clinical markers that align with payer-defined criteria for reimbursement.
4. Eligibility And Authorization Data
Front-end errors regarding insurance coverage are the leading cause of avoidable denials. Integrating eligibility data ensures that the provider is billing the right payer for a covered service at the right time.
- Real-Time Coverage Checks: The platform verifies active insurance status and benefit limits before the patient leaves the facility.
- Prior Authorization Tracking: It confirms that the necessary approval numbers are present and match the services performed.
- Referral Validation: The system ensures that required primary care referrals are documented for HMO and restrictive PPO plans.
- Benefit Exclusions: Automated checks identify services that are specifically excluded from a patient’s unique policy.
5. Appeal Outcomes
Learning from success is the fastest way to optimize a recovery engine. By tracking which appeals work and which do not, the AI constantly refines its drafting logic and prioritization strategy.
- Success Rate Metrics: The system identifies which arguments and evidence combinations lead to the highest number of overturned denials.
- Recovery Accounting: It tracks the actual dollars recovered versus the amount originally billed to measure true ROI.
- Resubmission Timing: Data on when a corrected claim was sent versus when it was paid helps optimize workflow speed.
- Write-off Analysis: Understanding why certain claims are eventually written off helps prevent similar losses in future billing cycles.
6. Payer Rules And Policy Data
Insurance companies frequently change their “rules of engagement” without direct notice to providers. A robust platform ingests external policy data to keep the internal validation logic current.
- Filing Limit Tracking: The system monitors the unique time windows each payer allows for original submissions and subsequent appeals.
- Payer-Specific Edits: It incorporates the unique formatting and coding rules required by different commercial and government carriers.
- Documentation Standards: The platform stays updated on the specific clinical trials or studies a payer requires to support new treatments.
- Contractual Obligations: It cross-references payments against negotiated fee schedules to detect underpayments or “silent” denials.
Maintaining a clean and comprehensive data lake ensures that the platform remains an authoritative source of truth for the organization.
This data-first approach allows for a transparent and auditable system that withstands both internal scrutiny and external payer audits.
Architecture For AI Claims Denial Management Software
The technical foundation of an AI claims platform must be built for massive scale and absolute precision. A modular architecture ensures that data flows securely from clinical systems through the intelligent processing layers to the final reporting dashboard.
The architecture includes data ingestion, normalization, AI scoring, rules validation, workflow automation, appeal generation, dashboards, integrations, and audit controls.
1. Data Ingestion Layer
Reliable architecture begins with the ability to consume disparate data types from multiple healthcare systems. This layer acts as the entry point, translating varied formats into a unified stream for the internal processing engines.
- API Connectors: High-speed interfaces link directly with Electronic Health Records (EHR) and Practice Management Systems (PMS).
- Clearinghouse Feeds: The system ingests 837 (claims) and 835 (remittances) EDI files to track the entire claim lifecycle.
- Legacy Integrations: Custom adapters ensure that older billing systems can still contribute data without manual exports.
- Payer Direct Links: Secure portals allow for the direct retrieval of payer-specific policy updates and eligibility responses.
2. Claims Intelligence Layer
This is the “brain” of the platform where machine learning models and deterministic rules intersect. This layer evaluates every claim against a backdrop of billions of historical data points to ensure accuracy.
- Denial Prediction Engine: Machine learning models calculate the risk score for every claim before it is transmitted.
- Documentation Cross-Reference: NLP algorithms verify that the clinical evidence justifies the specific codes being billed.
- Payer Rule Validation: A centralized library of insurance policies ensures the claim meets every specific requirement of the carrier.
- Real-Time Adjudication Simulation: The system predicts how the payer’s internal logic will respond to the current claim structure.
3. Workflow Automation Layer
Once a denial or a high-risk claim is identified, it must be routed to the correct specialist immediately. This layer eliminates the confusion of manual spreadsheets by automating task distribution based on expertise and priority.
- Intelligent Routing: Claims are sent to coders, billers, or appeal specialists based on the specific type of error detected.
- Escalation Logic: High-value claims or those approaching filing deadlines are automatically moved to supervisor queues.
- Collaborative Interfaces: Finance teams and clinical staff can communicate within the claim file to resolve documentation gaps.
- Automated Follow-ups: The system reminds users of pending tasks to ensure no revenue is lost due to administrative delays.
4. Appeal Management Layer
Recovering denied revenue requires a structured approach to documentation and communication. This layer standardizes the appeal process to increase the speed and success rate of every resubmission.
- Packet Assembly: The system automatically bundles the appeal letter with the specific clinical notes and lab results needed for proof.
- Deadline Tracking: A rigorous calendar management system monitors payer-specific appeal windows to prevent “timely filing” rejections.
- Response Monitoring: The platform tracks when a payer acknowledges an appeal and updates the recovery status in real time.
- Digital Resubmission: Corrected claims are sent back through the clearinghouse or payer portal with a single click.
5. Analytics And Reporting Layer
Transparency is the only way to measure the true impact of an AI investment. This layer converts the mountain of claim data into clear visual insights that drive executive decision-making.
- Trend Dashboards: Leadership can visualize denial spikes by payer, specialty, or specific medical location.
- Preventability Metrics: The system distinguishes between avoidable administrative errors and complex clinical denials.
- Recovery Performance: Real-time tracking shows the exact dollar amount recovered compared to the cost of the labor involved.
- Cash Flow Impact: Analytics project future revenue based on current appeal success rates and historical payment speeds.
6. Security And Compliance Layer
In healthcare technology, security is not a feature but a non-negotiable requirement. This layer ensures that every byte of data is protected according to the highest industry and legal standards.
- HIPAA Controls: Every part of the architecture is designed to maintain the privacy of Protected Health Information (PHI).
- Role-Based Access (RBAC): Users only see the specific data required for their job function to minimize security risks.
- End-to-End Encryption: Data is encrypted both while sitting in the database and while moving between different systems.
- Immutable Audit Trails: The platform records every view, edit, and transmission to provide a complete history for regulatory audits.
A well-architected platform provides a resilient environment where AI can thrive while maintaining the strict security standards healthcare requires. This structured approach ensures that the system is not only smart but also reliable and fully auditable.
Key Integrations Needed For AI Denial Management Platforms
A denial management platform cannot operate in isolation. Its effectiveness depends on its ability to talk to the existing healthcare ecosystem and pull data from the various systems where patient and financial information lives.
AI denial management platforms must integrate with EHRs, practice management systems, clearinghouses, billing software, payer portals, document systems, and analytics tools.
1. EHR Integration
The Electronic Health Record (EHR) is the primary source of clinical truth. Integration with major players like Epic, Oracle Health, or Athenahealth allows the AI to pull the clinical documentation necessary to prove medical necessity during an appeal.
- Clinical Data Access: The system retrieves physician notes and lab results to build comprehensive evidence packets.
- Bidirectional Flow: Updates made within the denial platform can sometimes be pushed back to the EHR to maintain clinical consistency.
- Custom Interface Support: Robust APIs ensure that even proprietary or highly customized EHRs can share data with the AI engine.
2. Practice Management And Billing Systems
These systems handle the operational side of the clinic or hospital. Integrating here ensures that the AI understands the financial context of every claim and can track it through the entire accounts receivable (A/R) cycle.
- Charge Capture Sync: The platform monitors charges as they are created to identify potential coding errors immediately.
- Coding Integration: AI suggestions are fed directly into the billing workflow to improve the accuracy of initial submissions.
- Payment Posting: Real-time visibility into payment posting allows the system to identify partial payments or “under-reimbursements” that act as silent denials.
3. Clearinghouse Integration
Clearinghouses act as the middleman between providers and payers. Direct integration allows the platform to see rejections in real time and verify that claims are formatted correctly before they reach the insurance company.
- EDI 837/835 Parsing: The system automatically processes standardized claim and remittance files to track every transaction.
- Real-Time Status Tracking: Automation ensures that the status of a claim is updated as soon as the clearinghouse receives a response.
- Eligibility Gateway: Integrating with clearinghouse eligibility tools allows for instant verification of patient coverage before care is provided.
4. ERA/EOB Processing
Electronic Remittance Advice (ERA) and Explanation of Benefits (EOB) files contain the specific reasons for a denial. Automating the ingestion of these files eliminates the need for manual data entry and speeds up the start of the appeal process.
- Automated Code Extraction: The AI identifies CARC and RARC codes within the files to categorize the denial automatically.
- Payment Matching: The system matches incoming payments to the original claim to identify any discrepancies or missing funds.
- Intelligent Appeal Routing: Based on the extracted denial reason, the platform routes the claim to the correct specialist for immediate action.
5. Payer Portal Integration
Many insurance companies require providers to use their specific web portals for status checks and documentation submission. AI-driven bots can navigate these portals to perform repetitive tasks that would otherwise take hours for a human.
- Automated Status Scrapping: Bots log into portals to check on pending claims and update the internal dashboard.
- Digital Document Uploads: The platform can automatically upload clinical evidence packets directly to the payer’s system.
- Authorization Monitoring: Tracking the status of prior authorizations within the portal ensures that no services are provided without approval.
6. BI And Finance Systems
Revenue cycle data must eventually reach the executive suite. Integrating with Business Intelligence (BI) and finance software ensures that leadership has a clear view of how denials are impacting the organization’s overall financial health.
- CFO-Level Reporting: The platform feeds data into executive dashboards to show the direct impact of recovery efforts on the balance sheet.
- Denial Cost Analysis: Finance teams can see the exact cost of labor and lost interest associated with denied claims.
- Budgeting Insights: Accurate recovery forecasts help the organization plan for future investments and staffing needs with greater confidence.
A connected platform ensures that data flows naturally between departments and systems. This connectivity removes the silos that typically cause delays in the revenue cycle and allows for a more agile response to payer challenges.
How To Build An AI Claims Denial Management Platform Step By Step
Building a high-performance intelligence layer is a structured, multi-phase engineering approach.
We focus on creating a system that integrates deeply with your existing operations while ensuring every automated decision is defensible, accurate, and scalable across a global healthcare enterprise.
Step 1: Define The Denial Management Scope
The first move in a successful deployment involves identifying the architectural destination of the project. Whether you are launching a lean MVP or a full-scale enterprise modernization project, the scope dictates the data requirements and integration depth.
- MVP Development: Focus on high-frequency denial types to prove rapid ROI within a single department.
- Internal Tooling: Customizing the platform to fit the specific legacy constraints of a private hospital group.
- SaaS Platform: Engineering for multi-tenancy and global scalability to serve a diverse client base.
- RCM Add-on: Designing a lightweight intelligence layer that enhances current billing software without a total overhaul.
Step 2: Map The Current Revenue Cycle Workflow
A technical solution is only effective if it aligns with the actual movement of a claim. We deconstruct the lifecycle from patient access to reporting to ensure the AI intervenes at the most impactful decision nodes.
- Patient Access: Mapping how registration data is captured to prevent front-end eligibility errors.
- Coding and Submission: Analyzing the transition from clinical documentation to the final claim file.
- ERA Posting: Reviewing how electronic remittance advice is ingested and where manual follow-up stalls.
- Appeals Management: Visualizing the current path of a denied claim to identify lost revenue opportunities.
Step 3: Identify High-Value Denial Categories
Not all rejections represent an equal threat to the balance sheet. We prioritize categories that combine high dollar volume with a high probability of successful recovery through automation.
- Eligibility and Authorization: Tackling the most common administrative errors that lead to immediate rejections.
- Medical Necessity: Using NLP to defend complex clinical decisions against payer scrutiny.
- Coding and Documentation: Identifying gaps in physician notes that trigger audits or down-coding.
- Timely Filing: Implementing guardrails to ensure no claim expires due to simple administrative delays.
Step 4: Prepare And Normalize Claims Data
Intelligence requires a foundation of clean and structured information. We ingest historical claims and payer responses to create a unified data lake that powers the predictive engine.
- Data Cleansing: Removing duplicates and correcting formatting errors in years of historical billing records.
- Code Normalization: Mapping inconsistent payer reason codes to a standardized internal taxonomy.
- Outcome Linking: Connecting finalized payment data to original submissions to teach the AI what “success” looks like.
- Documentation Linking: Attaching clinical PDFs and reports to their relevant claim files for holistic analysis.
Step 5: Build The Denial Prediction Engine
This core module allows the platform to anticipate payer behavior before a claim is ever sent. By training on payer-specific patterns, the system flags high-risk submissions for immediate correction.
- Pattern Recognition: Identifying the subtle combinations of codes and modifiers that lead to certain denials.
- Risk Probability: Assigning a numerical score to every claim to prioritize human review for the most “at-risk” submissions.
- Trend Detection: Monitoring shifts in payer adjudication logic to update prediction models in real-time.
Step 6: Add Payer Rules And Claim Validation Logic
While machine learning finds patterns, deterministic rules provide the rigid accuracy needed for contract compliance. This hybrid approach ensures every claim meets the hard-coded requirements of the insurance carrier.
- Contractual Edits: Building a library of specific billing rules negotiated with individual payers.
- Technical Validation: Ensuring 100% adherence to EDI 837 formatting standards to avoid technical rejections.
- Logic Overrides: Allowing for deterministic “stop” commands when a claim clearly violates a fundamental payer policy.
Step 7: Build Appeal Automation Workflows
Recovery becomes a high-speed process when the manual burden of letter writing is removed. The platform generates evidence-backed appeal packets that are ready for submission in seconds.
- Draft Generation: Creating professional, payer-specific appeal letters that quote the relevant clinical evidence.
- Evidence Checklists: Automatically identifying and bundling the required lab results or physician notes for each case.
- Task Assignment: Routing appeals to the specific staff members best equipped to handle them based on value and complexity.
Step 8: Integrate With RCM And Healthcare Systems
Connectivity is the bridge between AI insights and operational action. We ensure a seamless flow of data across the entire hospital tech stack to eliminate manual entry.
- EHR Connectivity: Building secure, bidirectional links to pull clinical notes and push claim status updates.
- Clearinghouse Integration: Connecting to submission gateways for real-time tracking of claim movement.
- Finance Systems: Ensuring the billing records and general ledger stay perfectly synchronized with AI interventions.
Step 9: Test With Real Denial Teams
Real-world validation ensures the tool actually improves the daily life of the billing staff. We subject the platform to rigorous testing with veteran specialists to refine the user interface and logic.
- Prediction Validation: Comparing AI risk scores against the actual intuition of senior billers.
- Usability Testing: Measuring the time reduction in appeal drafting compared to the old manual process.
- Feedback Integration: Using direct staff input to sharpen the AI’s suggestions and reduce false-positive alerts.
Step 10: Monitor ROI And Improve The System
The final stage focuses on scaling the financial impact and ensuring long-term performance. We track every metric that matters to the CFO to prove the ongoing value of the investment.
- Denial Reduction: Measuring the drop in initial rejections after the pre-submission engine goes live.
- Recovery Rate: Tracking the percentage of denied revenue that is successfully recaptured through automated appeals.
- Clean Claim Rate: Monitoring the increase in claims paid on the first pass without human intervention.
This rigorous development process ensures your platform is not just another piece of software but a strategic financial asset. By following this roadmap, we deliver a solution that scales with your growth and delivers a measurable impact on your bottom line.
Conclusion
Building an automated claims infrastructure turns a reactive billing process into a strategic financial asset. This technology eliminates manual bottlenecks and secures predictable cash flow for the enterprise.
By prioritizing data-driven recovery and proactive risk management, healthcare leaders can finally close the gap on revenue leakage.
Scaling this solution ensures long-term operational resilience and a significant return on investment. Start your transformation now to optimize every dollar in your revenue cycle.
Build AI Claims Denial Management Platforms With Intellivon
At Intellivon, we build AI-powered claims denial management platforms for healthcare SaaS companies, RCM providers, billing companies, hospitals, provider networks, payer-facing platforms, and enterprise healthcare teams.
Our engineering approach connects denial prediction, claim validation, clinical documentation intelligence, appeal automation, payer analytics, work queue management, dashboard reporting, and secure healthcare integrations into one claims decision infrastructure.
This helps your team reduce preventable denials, recover revenue faster, prioritize high-value claims, and make denial performance easier to monitor.
A. Help You Define The Right Denial Management Scope
Not every denial platform needs to start as a full enterprise system. We help you define the right MVP, AI modules, workflows, and roadmap based on your users, denial volume, claim types, and revenue cycle maturity.
We help with:
- MVP planning
- AI module selection
- denial category mapping
- RCM workflow discovery
- product roadmap planning
- enterprise modernization planning
B. Build AI Workflows Around Real Claims Operations
Denial management does not work when AI sits outside the revenue cycle. We design workflows around how billing teams, coders, denial specialists, appeal teams, and finance leaders actually manage claims.
We build workflows for:
- pre-submission denial scoring
- claim correction recommendations
- clinical documentation review
- appeal task routing
- denial work queues
- recovery tracking
C. Integrate With Your Healthcare And RCM Systems
A denial platform is only useful when it can connect with the systems where claims, payments, documentation, and payer responses already live.
We integrate with:
- EHR systems
- practice management systems
- billing platforms
- clearinghouses
- payer portals
- ERA/EOB systems
- document systems
- analytics tools
D. Make Denial AI Explainable, Secure, And Scalable
Healthcare teams need AI they can trust, review, and audit. We build denial intelligence systems with explainable recommendations, role-based access, audit trails, PHI protection, secure data pipelines, and model monitoring.
We focus on:
- HIPAA-ready architecture
- explainable AI outputs
- audit-ready workflows
- secure PHI handling
- human review controls
- scalable cloud deployment
Want to build an AI claims denial management platform for your healthcare, RCM, or billing business? Contact Intellivon to design a secure, scalable denial intelligence system around your workflows.
Things To Know About Claims Denial Management Platforms
Q1. Can an AI claim denial management platform prevent denials before submission?
A1. Yes, if it is built as a prevention layer, not just a denial tracker. The platform can flag missing authorizations, coding issues, eligibility gaps, documentation errors, and payer-specific risks before claims go out. This helps teams fix avoidable problems earlier and reduce rework after denial.
Q2. How does AI help denial teams manage appeals faster?
A2. AI can read denial reasons, classify denial codes, suggest missing evidence, draft appeal templates, and route cases by deadline or claim value. However, appeal teams should still review the output. The best platforms support human judgment instead of sending automated appeals without verification.
Q3. Why do hospitals need denial management software instead of Excel?
A3. Excel can track denied claims, but it cannot predict denial risk, connect with EHR or RCM systems, assign work queues, monitor appeal deadlines, or show payer trends automatically. A denial management platform gives teams one workflow for prevention, resolution, reporting, and revenue recovery.
Q4. Can AI denial management automation create billing errors?
A4. Yes, poorly designed automation can create errors if it uses bad data, vague denial codes, or unchecked AI recommendations. Hospitals need explainable AI, audit trails, confidence scores, payer rule validation, and human review queues. This keeps automation useful without risking more denials or compliance issues.