Key Takeaways:
-
Revenue leakage occurs through eligibility errors, coding gaps, claim rejections, underpayments, and delayed collections at every RCM stage.
-
AI prevents denials before submission, automates coding support, detects underpayments, and prioritizes claims by recovery probability.
-
Agentic AI handles eligibility checks, authorization workflows, and denial queues while keeping humans in control of final decisions.
-
Build costs range from $50,000 for an MVP to $200,000 and above for an enterprise platform with payer integrations and compliance controls.
-
How Intellivon builds AI RCM platforms your enterprise fully owns, with denial prediction, payer-aware automation, and secure integrations from day one.
Revenue cycle management is one of the most important financial operations for a health system, and it is also one of the most disjointed. This is because data leakage occurs at every stage, from patient access and coding mistakes to claim rejections, underpayments, and collections that never finish. For most hospitals and clinics, this leakage is an infrastructure issue more than a billing one.
Rule-based billing software was designed for a simpler payer environment. However, as payer complexity has increased, denial patterns have changed, and reimbursement timelines have lengthened. Static rule sets can no longer keep up. Now, hospitals, digital health companies, and RCM vendors are investing in AI-powered platforms that can anticipate problems, predict outcomes, and act throughout the entire revenue cycle instead of just notifying issues after they arise.
AI should be integrated into RCM workflows, and not just added as a reporting tool. This means having automation, predictive denial modeling, payer intelligence, and compliance controls built into every touchpoint. Intellivon creates secure, scalable AI RCM platforms for organizations that need strong financial infrastructure, not just better billing software. This blog explains how to build one from the ground up.
Why Healthcare Businesses Are Building AI RCM Platforms
Shrinking margins, staffing shortages, and rising payer complexity have made revenue cycle efficiency a boardroom priority rather than a back-office concern. Healthcare businesses are therefore building AI RCM platforms to move faster, capture more revenue, and maintain compliance without proportionally increasing headcount.
Leaders like R1 RCM, Waystar, and athenahealth have already demonstrated what that looks like in practice. Each has embedded AI into core revenue cycle workflows, moving from rule-based automation toward systems that can reason across payer behavior, coding patterns, and claim risk in real time.
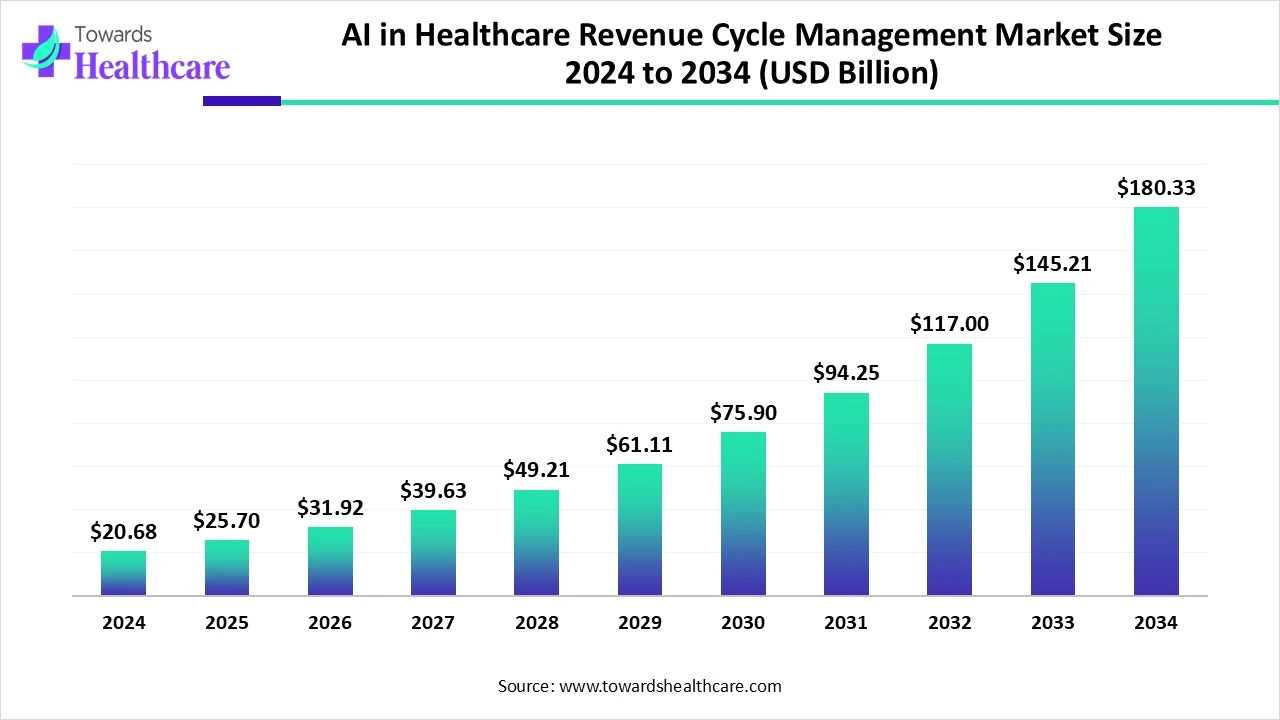
The global AI in revenue cycle management market was valued at USD 20.63 billion in 2024 and is projected to reach USD 70.12 billion by 2030, growing at a CAGR of 24.16% through the same period.
Revenue cycle pressure is no longer manageable through process improvements alone. The problems are structural, and they compound across every stage of the billing cycle.
1. Claim Denials Are Becoming A Revenue Risk
Denials rarely happen for a single reason. Eligibility errors, coding gaps, missing documentation, prior authorization failures, and payer-specific rule changes each create their own rejection pathway.
Furthermore, when resubmissions are delayed, the recovery window shortens, and write-offs increase. Every denial that goes unresolved is direct revenue walking out the door.
2. Manual RCM Workflows Slow Down Cash Flow
Staff-dependent processes create bottlenecks that are difficult to scale. Repetitive claim checks, manual payment posting, delayed follow-ups, and slow denial resolution keep accounts receivable cycles longer than they need to be.
As backlogs grow, moreover, the cost of chasing outstanding payments begins to outweigh the recovery value on lower-balance claims.
3. Patient Payment Responsibility Is Increasing
As high-deductible plans become standard, patients are responsible for a larger share of the bill. However, most billing systems were not designed around the patient financial experience.
Accurate cost estimates, flexible payment plans, digital payment options, clear billing communication, and accessible financial counseling are therefore no longer optional. They directly affect collection rates.
CFOs Need Better Revenue Visibility
Financial leaders need more than monthly reports. Days in A/R, clean claim rates, denial rates, net collection performance, underpayment trends, payer behavior patterns, and forecasted cash flow all need to be visible in real time.
Without that visibility, revenue decisions rely on lagging data and assumptions.
AI RCM platforms address each of these pressure points systematically, which is precisely why investment in this infrastructure is accelerating.
What Is An AI Revenue Cycle Management Platform?
An AI revenue cycle management platform is a healthcare financial infrastructure that uses automation, predictive modeling, and payer intelligence to reduce revenue leakage, accelerate reimbursement, and give financial teams real-time visibility across the entire billing cycle.
Unlike traditional billing software, it adapts to payer behavior, flags risk before claims are submitted, and operates across every stage of the patient financial journey.
Traditional RCM Software Vs AI RCM Platforms
Traditional RCM software was built to organize billing workflows. This is why AI RCM platforms are built to optimize revenue outcomes, and the difference shows up at every stage of the cycle.
| Capability | Traditional RCM Software | AI RCM Platform |
| Workflow Logic | Rule-based, static workflows | Predictive, adaptive workflows |
| Claim Review | Manual claim review and checking | AI-assisted claim validation before submission |
| Reporting | Static dashboards with lagging data | Real-time revenue intelligence and forecasting |
| Denial Management | Reactive, post-denial resolution | Proactive denial prevention and risk flagging |
| Operations Model | Staff-heavy, process-dependent | Human-in-the-loop automation at scale |
The gap between the two is financial, and organizations running on traditional RCM infrastructure are leaving measurable revenue on the table every billing cycle.
Where Revenue Leakage Happens Across The RCM Workflow
Building an AI revenue cycle platform turns a reactive billing process into a proactive asset for your enterprise. This system protects your cash flow by stopping financial leaks before they impact your bottom line.
Revenue leakage in RCM happens when eligibility errors, missing authorizations, coding gaps, claim rejections, denials, underpayments, and patient billing delays go unresolved.
1. Front-End Revenue Leakage
The claim lifecycle starts long before a provider sees a patient. Most denials begin at the registration desk through human error. Inaccurate insurance details or missed checks create a domino effect of rework.
When staff fail to verify coverage, the organization carries the cost without a payment guarantee. Addressing these variables during intake is the best way to protect margins.
2. Mid-Cycle Revenue Leakage
Mid-cycle involves turning medical services into billable codes. Revenue leaks here when documentation is incomplete. Clinical updates are often slow and miss specific capture opportunities.
Without automated validation, these errors bypass internal reviews. This results in wasted time for coding teams and more contested claims.
3. Back-End Revenue Leakage
The back end is where unresolved claims often sit. Denied claims represent trapped capital that many firms eventually write off. If teams lack a strategy for contract variance, payers may underpay without being noticed.
These small gaps across thousands of claims create a massive deficit. Efficient management requires a surgical approach to intervention.
4. How AI Helps Prevent Leakage Earlier
AI transforms the workflow by adding risk scoring at the point of entry. The system checks every claim against payer behavior to predict denial chances. This allows your team to fix errors before they reach the insurer.
Consequently, your clean claim rate increases and reduces expensive rework. It ensures your revenue remains secure through the entire process.
By identifying these specific points of failure, business leaders can deploy targeted AI solutions to secure their earnings. Solving these leaks is the first step toward building a truly resilient financial infrastructure.
Core Modules Of An AI Revenue Cycle Management Platform
Designing a high-performance AI RCM platform requires a modular architecture that addresses every touchpoint of the financial journey. By integrating these specific components, your enterprise can ensure a seamless flow of data and capital across the entire healthcare ecosystem.
A strong AI RCM platform includes patient access, eligibility, prior authorization, coding, claims, denials, payment posting, patient billing, analytics, and compliance modules.
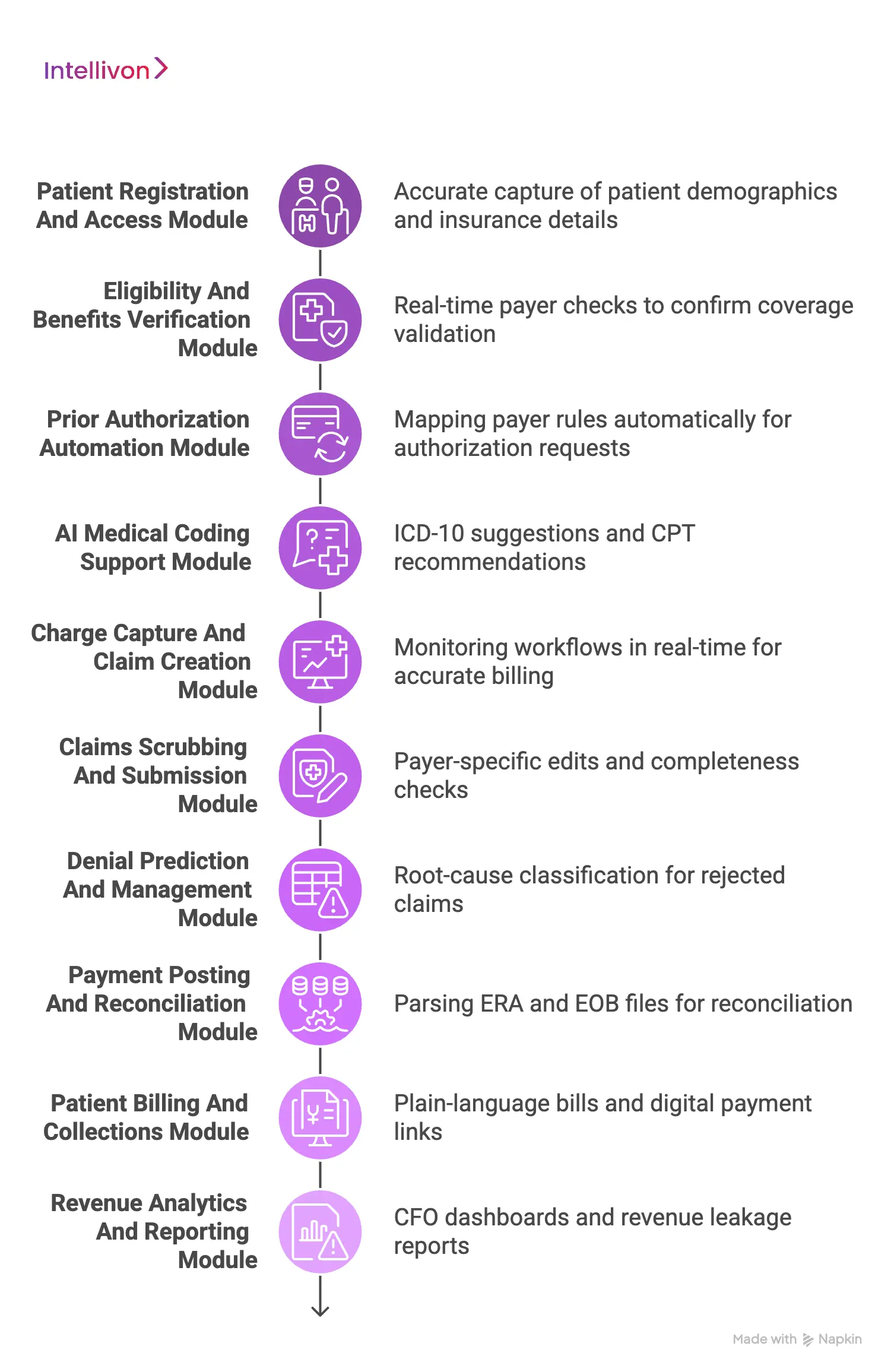
1. Patient Registration And Access Module
A successful revenue cycle begins with the accurate capture of patient demographics and insurance details. Because human error at the front desk causes most downstream issues, this module uses intelligent alerts to flag registration mistakes immediately.
- Insurance details: Captures and stores primary and secondary coverage data.
- Duplicate patient detection: Advanced matching logic ensures a single, accurate record for every patient.
- Registration error alerts: Real-time notifications prevent incomplete files from moving forward.
2. Eligibility And Benefits Verification Module
This module performs real-time payer checks to confirm coverage validation before any service is rendered. It automatically detects deductibles, co-pays, and plan limitations so that financial expectations are clear from the start.
- Real-time payer checks: Instantly verifies active coverage status through direct API links.
- Deductible detection: Identifies the exact remaining amount the patient must pay.
- Automated staff task creation: Generates work orders when coverage mismatches are found.
3. Prior Authorization Automation Module
Managing authorizations is often the most labor-intensive part of the cycle, yet AI simplifies this by mapping payer rules automatically. The system detects requirement triggers and generates a document checklist to support every request submission.
- Payer rule mapping: Keeps a live database of which procedures need prior approval.
- Status tracking: Monitors the progress of requests to prevent service delays.
- CMS-0057-F readiness: Ensures compliance with new federal interoperability and authorization standards.
4. AI Medical Coding Support Module
Intelligent coding support provides ICD-10 suggestions and CPT recommendations based on the existing provider notes. The software identifies documentation gaps and performs modifier checks to ensure full compliance with current regulations.
- Documentation gap detection: Flags clinical notes that lack enough detail for specific billing codes.
- Modifier checks: Suggests correct codes to prevent denials based on procedural variations.
- Human coder review: Facilitates a quick audit trail where experts can approve AI suggestions.
5. Charge Capture And Claim Creation Module
This module bridges the gap between the medical encounter and the financial charge by monitoring workflows in real-time. It issues missing charge alerts and performs service-code matching to ensure every procedure is accounted for accurately.
- Encounter-to-charge workflows: Tracks the patient journey to ensure every visit is billed.
- Missing charge alerts: Notifies billing teams when a service lacks a corresponding fee.
- Claim-line validation: Checks each individual item for accuracy before the final claim is built.
6. Claims Scrubbing And Submission Module
Before a claim reaches the clearinghouse, the scrubber applies payer-specific edits and checks for completeness. It uses AI risk scoring to determine which claims are likely to be rejected and identifies duplicate submissions before they cause delays.
- Payer-specific edits: Customizes validation rules based on the unique requirements of each insurer.
- AI risk scoring: Ranks claims based on their probability of immediate acceptance.
- Clearinghouse integration: Provides a direct pipeline for electronic data interchange (EDI).
7. Denial Prediction And Management Module
The power of an AI RCM platform lies in its ability to perform root-cause classification for every rejected claim. The system assigns a denial risk score to each file and offers specific appeal recommendations to the billing team.
- Root-cause classification: Groups denials by reason to find systemic issues in the workflow.
- Appeal recommendation: Generates template-based responses for faster claim recovery.
- Payer-level intelligence: Aggregates data to show which insurers have the highest denial rates.
8. Payment Posting And Reconciliation Module
Automating the reconciliation process involves parsing ERA and EOB files to match 835 remittances with open invoices. This module quickly detects underpayments and maps adjustment codes to keep the general ledger balanced.
- ERA/EOB parsing: Converts complex digital and paper files into readable data.
- Underpayment detection: Compares paid amounts against contracted rates to find missing money.
- Finance reconciliation: Syncs the billing system with the bank deposits for total accuracy.
9. Patient Billing And Collections Module
Modern platforms prioritize the patient experience by offering plain-language bills and digital payment links. The system tracks payment preferences and suggests installment plans based on collection risk segmentation.
- Digital payment links: Allow patients to pay via mobile or web with one click.
- Installment plans: Automatically calculate monthly payments for high-balance accounts.
- Collection risk segmentation: Focuses staff energy on accounts with a high likelihood of payment.
10. Revenue Analytics And Reporting Module
Executive decision makers need CFO dashboards that provide a clear view of days in A/R and cash forecasts. This module tracks payer performance and generates revenue leakage reports to identify where the organization is losing money.
- CFO dashboards: Displays high-level KPIs like net collection rates and total outstanding debt.
- Days in A/R: Tracks how long it takes for the business to turn a claim into cash.
- Revenue leakage reports: Pinpoint specific departments or doctors where money is being lost.
These interconnected modules work together to create a robust financial engine that maximizes efficiency and minimizes waste. Investing in this comprehensive architecture ensures your platform remains competitive in an increasingly complex regulatory environment.
How To Build An AI RCM Platform Step By Step
Building a high-performance AI RCM platform requires a structured engineering approach that balances technical innovation with clinical accuracy.
We view this transition as a phased evolution where each stage builds the necessary intelligence to protect enterprise margins.
Step 1: Map The Existing Revenue Cycle Workflow
We began by performing a thorough audit of how money and data move through the legacy ecosystem. This phase involved identifying every staff handoff and pinpointing where delays occur between the EHR and the billing software.
By understanding these dependencies, we built a solution that solves actual bottlenecks rather than theoretical ones.
- Patient intake process: We mapped the journey from the first appointment call to the registration desk.
- Claim creation process: Our team documented the transition from clinical notes to billable encounters.
- Staff handoffs: We identified points where human error was most likely to occur during data transfer.
- EHR dependencies: We analyzed how legacy software limitations impacted data extraction for billing.
Step 2: Define The AI Use Cases
We focused our strategy on high-impact automation rather than trying to fix everything at once. Therefore, we prioritized use cases like denial prediction and coding support that offered the fastest return on investment.
By defining these goals early, we aligned our development team with the specific business outcomes that matter most to stakeholders.
| AI Use Case | Business Impact | Primary User |
| Denial Prediction | Reduces rework costs and accelerates cash flow. | Billing Manager |
| Coding Support | Increases accuracy and prevents compliance audits. | Medical Coder |
| Underpayment Detection | Captures lost revenue from contract variances. | CFO / Controller |
Step 3: Build The Data Foundation
We recognized that an AI platform is only as strong as the data that feeds its learning models. At the same time, we aggregated diverse datasets, including clinical documentation, remittance files, and deep denial histories, to create a comprehensive training environment.
This foundation allowed our system to recognize the subtle patterns that lead to underpayments or delayed reimbursements.
- Claims data: We gathered historical records of every submission made over the last five years.
- Payer rules: We built a live database of specific requirements from different insurance carriers.
- Remittance files: We tracked 835 data to understand exactly how much was paid versus billed.
- Payment timelines: Our team analyzed the average duration between claim submission and fund arrival.
Step 4: Clean And Normalize RCM Data
RCM data is notoriously messy because it often contains duplicate records and inconsistent naming conventions across different payers.
We focused on historical claim cleanup and standardized all fields so the AI could process information without confusion. Because clean data is the primary driver of accuracy, we treated this phase as a non-negotiable requirement for a reliable platform.
- Duplicate records: We merged multiple patient files into a single source of truth.
- Inconsistent payer names: We normalized varied entries for the same insurance company into a single ID.
- Missing denial codes: Our process filled in gaps where historical data lacked clear reasons for rejection.
- Standardized fields: We ensured all dates, currencies, and codes followed a uniform format.
Step 5: Design The Platform Architecture
We designed the architecture to support a complex backend that handles heavy data processing while providing a simple frontend for the end-user.
At the same time, we built a robust rules engine that works alongside the AI model layer to ensure every claim passes through a strict validation gate. However, we also included an audit logging layer to track every change for compliance purposes.
| Component | Function | Technical Focus |
| Workflow Engine | Directs tasks between bots and humans. | Logic & Orchestration |
| Data Warehouse | Stores normalized historical and live data. | Scalability & Speed |
| Security Layer | Protects PHI with enterprise encryption. | HIPAA Compliance |
Step 6: Build AI Automation Models
In this stage, our data scientists developed predictive models that score claim risk and detect anomalies in real-time. We leveraged NLP for coding assistance to help bridge the gap between doctor notes and complex ICD-10 requirements.
These models continuously learn from new data, meaning the platform becomes more effective at detecting revenue leakage over time.
- Predictive denial models: We built logic to foresee rejections before claims leave the office.
- NLP coding assistance: Our AI reads clinical notes to suggest the most accurate billing codes.
- Anomaly detection: We implemented triggers to flag unusual patterns indicating fraud or errors.
- Revenue leakage detection: We identified specific areas where capital was consistently lost.
Step 7: Integrate With Healthcare Systems
We understood that a standalone platform is useless if it cannot talk to existing EHR or practice management systems. At the same time, we built secure pipelines using payer APIs and clearinghouse integrations to ensure a smooth flow of electronic data. Consequently, connecting these systems allowed for automated payment posting and real-time updates to patient portals and accounting software.
- EHR/EMR systems: We established direct integration for real-time clinical data extraction.
- Clearinghouses: Our team built secure pipelines for large-scale electronic claim submission.
- Payment gateways: We enabled secure digital transactions for patient co-pays.
- Accounting systems: We synced billing data with the general ledger for total transparency.
Step 8: Add Human-In-The-Loop Review
Even with advanced automation, we included human oversight to handle complex exceptions and maintain high confidence thresholds.
This module ensures that billing specialists can review AI-generated appeals or coding suggestions before they are finalized. By maintaining clear audit trails, we built trust in the system while ensuring that final decisions are always backed by professional expertise.
- Exception routing: We designed the system to send complex cases to human specialists automatically.
- Confidence thresholds: We set strict limits where the system must ask for help if it is unsure.
- Coder approval: We allowed experts to validate AI-suggested codes with a single click.
- Audit trails: Our platform records every human intervention for future training and compliance.
We ensure that your AI RCM platform is not just a tool but a resilient financial engine built for the future of healthcare.
AI Features That Make RCM Platforms More Effective
Smart RCM platforms succeed by moving beyond basic automation and embedding intelligence into every layer of the financial process.
These specific AI features act as a dynamic roadmap that guides teams toward higher collection rates and more predictable cash flows.
1. Denial Prediction Before Claim Submission
Waiting for a rejection letter is a waste of time and staff resources. Modern systems use risk scoring to check every claim against known payer patterns before they ever leave the facility. By finding these red flags early, the software provides preventive alerts and specific correction steps that boost the number of claims paid on the first attempt.
- Payer-specific patterns: The AI tracks how specific insurance companies change their rules in real-time.
- Historical denial learning: Models study past rejections to prevent the same mistakes from recurring.
- Claim correction recommendations: The system suggests the exact changes needed to satisfy payer requirements.
2. AI-Assisted Medical Coding
Medical coding is a complex hurdle, so AI tools now act as a digital second pair of eyes to ensure accuracy. The platform reviews clinical notes to provide code suggestions while checking for modifier errors and compliance gaps.
This approach does not just lower error rates; it increases coder speed by handling the repetitive parts of the workflow.
3. Prior Authorization Intelligence
Authorization delays can stop a provider’s schedule and lead to massive revenue loss. We solve this by using intelligence that detects when an approval is needed and flags missing documents automatically.
The platform matches every procedure against live payer rules, so the team knows exactly where an approval stands in the pipeline.
4. Automated Claim Follow-Up Prioritization
Not all outstanding claims have the same value, and treating them equally leads to wasted effort. A prioritization engine ranks claims based on recovery probability, appeal deadlines, and total dollar value.
Therefore, staff spend their energy on the most important accounts rather than getting stuck on old claims that likely won’t be paid.
5. Underpayment And Contract Variance Detection
Hidden underpayments drain resources if they are not caught and disputed immediately. Efficient systems compare remittance data against actual contract rates to find every small discrepancy.
When the platform detects a variance, it starts recovery workflows and alerts the team to trends that might require a contract review.
| Feature | Primary Function | Business Value |
| Contract Comparison | Matches paid amounts to rates. | Recovers hidden capital. |
| Adjustment Review | Validates why a fee was lowered. | Stops systemic losses. |
| Payer Alerts | Flags recurring payment errors. | Improves payer negotiations. |
6. Patient Payment Prediction
Managing the patient portion of the bill requires a mix of data and empathy. Predictive models segment balances based on payment likelihood and recommend the best installment plans for that specific person.
By timing reminders correctly and personalizing the experience, you increase collections while keeping the patient relationship strong.
7. Revenue Forecasting Dashboards
Decision makers need more than just a look at the past; they need to see what is coming next. Forecasting dashboards analyze expected reimbursements and cash flow trends to provide visibility into future performance.
These tools highlight the real impact of denials and help leaders adjust their strategy before a cash crunch happens.
By focusing on these high-impact features, an enterprise can build a platform that turns financial data into a competitive advantage. These tools ensure that every dollar earned is a dollar actually collected.
Where Agentic AI Fits In Revenue Cycle Management
Agentic AI introduces a layer of autonomous reasoning that moves beyond basic “if-then” automation.
Instead of just following a fixed script, these agents can evaluate context and execute specific steps to assist human teams, ensuring that workflows remain fluid and responsive to payer changes.
1. AI Agents For Eligibility And Benefits Checks
These agents act as a digital concierge for the patient access department by verifying insurance details long before the patient arrives. They proactively scan for coverage mismatches and calculate precise deductibles and co-pays.
When data is missing, the agent does not just stop; it creates a targeted task for the staff to address the specific gap.
- Coverage mismatch detection: Automatically flags when a patient’s plan does not align with the scheduled service.
- Staff task creation: Routes specific administrative needs directly to the right desk for resolution.
- Patient access support: Ensures that the front-end team has all financial clearance data ready for the patient.
2. AI Agents For Prior Authorization Workflows
Managing authorizations involves a high volume of back-and-forth communication that agentic AI is uniquely suited to handle. The agents verify requirements, create document checklists, and monitor status updates across various payer portals.
They also provide summaries of payer communications so that clinical staff can quickly understand why a request might be delayed.
- Document checklist creation: Lists every specific clinical file needed for a successful approval submission.
- Payer communication summaries: Distills complex insurance updates into clear, actionable bullet points for the team.
- Exception routing: Identifies complex cases that fall outside standard rules and sends them to a senior specialist.
3. AI Agents For Claim Follow-Up
Rather than having billing staff manually check the status of every claim, agents perform these checks in the background and update work queues. They prioritize aging claims and suggest the next-best-action based on the latest payer response.
This ensures that the team focuses on the accounts with the highest probability of immediate payment.
- Payer response summaries: Interprets coded responses from insurers to explain why a claim is pending.
- Next-best-action suggestions: Recommends whether to call the payer, resubmit, or provide more data.
- Follow-up reminders: Keep high-value accounts from falling through the cracks by alerting staff to deadlines.
4. AI Agents For Denial Work Queues
When a denial occurs, agentic AI quickly classifies the reason and prepares the foundation for an appeal. It detects missing documents and assigns a recovery priority score so the billing department knows which rejections are worth the most effort.
Furthermore, it alerts specialists to repeat denial patterns that suggest a larger systemic issue with a specific payer.
- Appeal draft support: Populates appeal letters with the specific data points needed to overturn a denial.
- Recovery priority scoring: Ranks denials by dollar value and the likelihood of a successful appeal.
- Specialist assignment: Matches complex denials with the specific team member who has the most expertise in that area.
5. Why Human Oversight Still Matters
While agentic AI handles the heavy lifting, human experts remain the ultimate decision-makers to ensure total compliance and accuracy. Professionals provide the final sign-off on appeals and handle unique financial exceptions that require a nuanced touch.
By maintaining strict confidence thresholds, the system only acts on what it knows for certain and asks for help whenever a situation becomes ambiguous.
- Coding accuracy: Human coders verify AI suggestions to maintain high-quality clinical documentation standards.
- Compliance review: Legal and billing experts ensure all automated actions align with evolving healthcare regulations.
- Audit history: Every action taken by an agent is logged, providing a clear trail for internal and external reviews.
Integrating agentic AI into the revenue cycle is about empowering human teams with better data and faster execution. This partnership ensures that the enterprise remains agile while maintaining the highest levels of financial integrity.
Key Integrations For AI RCM Platform Development
An enterprise-grade RCM platform must function as a central nervous system that communicates effortlessly with every external healthcare entity. Building these secure pipelines ensures that data flows without friction, which is the only way to achieve true automation at scale.
AI RCM platforms need secure integrations with EHRs, clearinghouses, payers, coding systems, payment gateways, patient portals, and analytics tools.
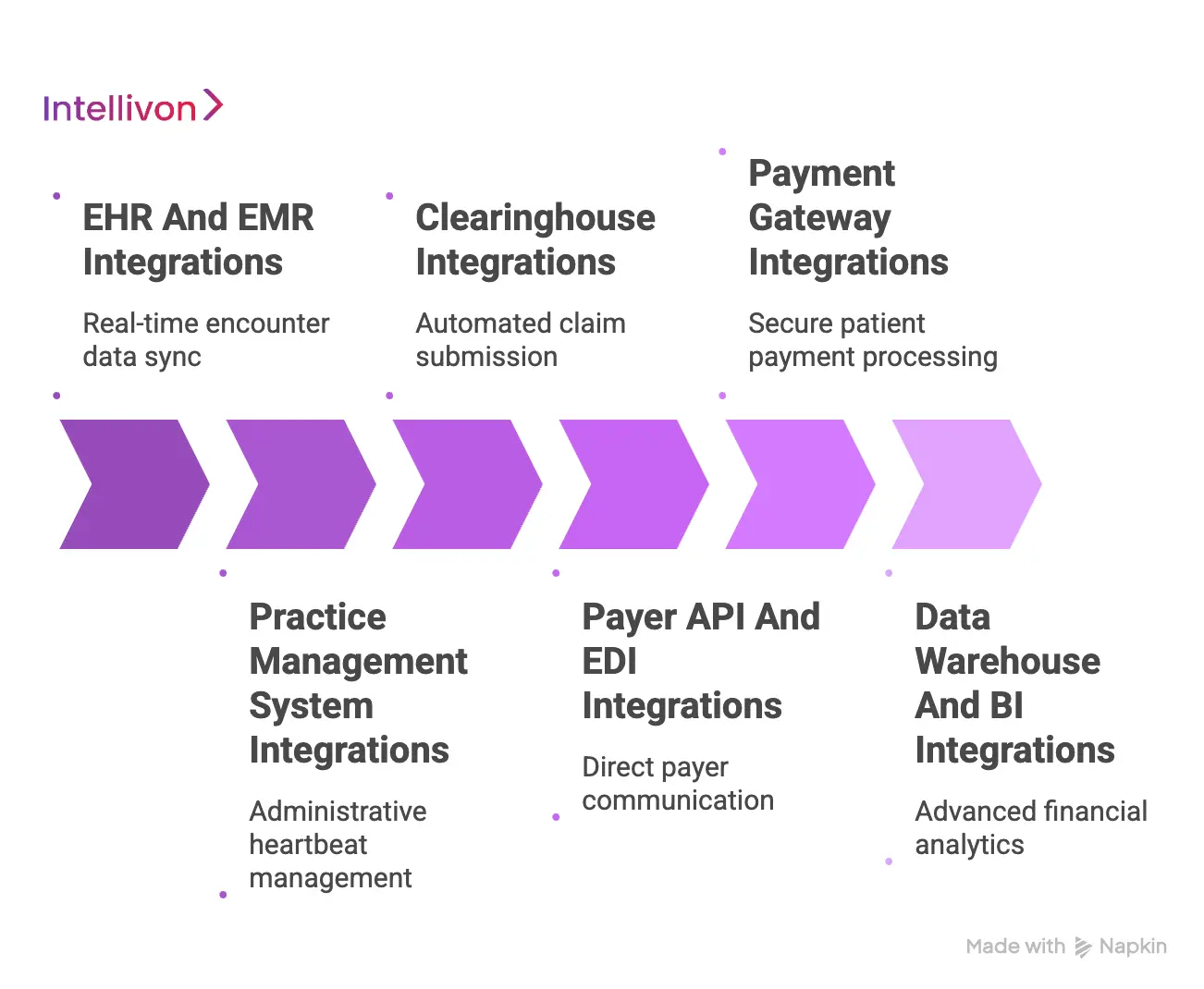
1. EHR And EMR Integrations
The Electronic Health Record is the primary source of truth for all clinical encounters. To build a robust AI platform, you must establish deep integrations with major players like Epic, Oracle Health/Cerner, and Athenahealth.
These connections allow for real-time encounter data sync and direct documentation access, which are essential for accurate coding and claim creation.
- Platform Coverage: Integration with eClinicalWorks, Meditech, and NextGen ensures your solution fits into diverse hospital environments.
- Encounter Data Sync: Automatically pulling patient visit details prevents manual entry errors.
- Documentation Access: Allows the AI to read physician notes for more precise clinical evidence.
2. Practice Management System Integrations
While the EHR handles the clinical side, the Practice Management System (PMS) manages the administrative heartbeat of the facility. Integrating with the PMS allows your platform to oversee scheduling data and provider details while tracking patient balances.
This link is vital for ensuring that charges are captured immediately after an appointment status changes to completed.
3. Clearinghouse Integrations
Clearinghouses act as the middleman between your platform and thousands of different insurance payers. By establishing a direct pipeline, you can automate claim submission and receive instant notifications regarding rejections.
This integration also handles the ingestion of ERA files, which is necessary for the AI to understand why a claim was paid or denied.
- Claim Status: Real-time monitoring of where a claim sits in the payer’s review process.
- Payer Response Tracking: Categorizing electronic responses to identify systemic issues across different insurers.
4. Payer API And EDI Integrations
The most sophisticated platforms are moving toward direct Payer APIs and FHIR standards to bypass traditional delays. These integrations handle X12 270/271 for eligibility and X12 835 for remittance advice.
Furthermore, utilizing prior authorization APIs allows the system to request and receive approvals in seconds rather than days.
- X12 837 Claims: The industry standard for sending professional and institutional claims.
- X12 276/277: Automated loops that check and report on the current status of any submitted claim.
5. Payment Gateway Integrations
To secure the patient-facing side of the revenue cycle, your platform requires a secure payment gateway integration. This enables the processing of card payments and ACH transfers while supporting automated installment plans for high-balance accounts.
A clean integration here ensures that refunds and reconciliations are handled with total financial transparency.
6. Data Warehouse And BI Integrations
Final financial reporting relies on consolidating all this data into a centralized warehouse for advanced analytics. Connecting to Business Intelligence (BI) tools allows your platform to feed executive dashboards with live revenue reports and payer trends.
Consequently, these forecasting models provide decision-makers with the clarity needed to plan future investments and growth.
- Finance Analytics: Deep-dive reports on net collection rates and total outstanding debt.
- Forecasting Models: Predictive tools that estimate future cash flow based on current billing volume.
By prioritizing these specific integrations, you ensure that your AI RCM platform is not an isolated tool but a fully connected financial engine. This connectivity is what ultimately drives higher margins and operational efficiency for the modern enterprise.
Compliance And Regulatory Readiness For AI RCM Platforms
Regulatory alignment is a non-negotiable requirement for any healthcare financial platform. Because the landscape of patient privacy and federal mandates evolves rapidly, your architecture must be built with compliance as a core feature rather than a secondary addition.
AI RCM platforms ensure compliance through HIPAA-compliant encryption, CMS-0057-F readiness for authorizations, price transparency workflows, and explainable AI governance.
1. HIPAA And PHI Protection
Protecting Protected Health Information (PHI) requires a multi-layered defense strategy. Every data point processed by the AI must remain encrypted both at rest and in transit to prevent unauthorized access.
Furthermore, strict data minimization ensures that the system only processes the specific information needed to complete a billing task.
- Secure AI processing: Ensures that machine learning models do not store or leak sensitive identifiers.
- Role-based access: Limits data visibility based on the specific job function of the user.
- Audit logs: Tracks every instance where PHI is accessed or modified for total accountability.
2. Prior Authorization API Readiness
Federal mandates like CMS-0057-F require a shift toward automated, transparent authorization workflows. Your platform must support payer API readiness to allow for the instant exchange of clinical documentation.
This ensures that the organization maintains an audit-ready approval history while reducing the time patients wait for care.
- Payer API readiness: Facilitates direct digital communication with insurance carriers for faster approvals.
- Denial reason capture: Digitizes the specific reasons for an authorization rejection to improve future submissions.
- Authorization status tracking: Provides real-time visibility into the progress of pending requests.
3. Price Transparency And Patient Estimates
Modern regulations demand that providers give clear, upfront cost estimates to patients before services are rendered. By automating Good Faith Estimate workflows, your platform helps the enterprise stay compliant with the No Surprises Act.
This visibility into payment responsibility builds patient trust and significantly reduces back-end collection hurdles.
- Shoppable service pricing: Provides patients with clear costs for common medical procedures.
- Machine-readable data: Ensures that pricing information is accessible to regulatory bodies and consumer tools.
- Estimate audit logs: Records exactly what the patient was quoted to resolve future billing disputes.
4. Coding And Billing Compliance
AI-driven coding must adhere to the latest ICD-10, CPT, and HCPCS standards to avoid costly audits. The system should automatically flag medical necessity issues and perform modifier checks before a claim is finalized.
Therefore, maintaining an audit-ready coding history is vital for defending the organization during external payer reviews.
- Modifier checks: Automatically applies the correct billing modifiers based on the procedure context.
- Medical necessity rules: Matches diagnosis codes with procedures to ensure they meet payer guidelines.
- Coding recommendation review: Requires human sign-off on AI-suggested codes to maintain accuracy.
5. AI Governance And Explainability
Black-box AI is a liability in healthcare. Therefore, your platform must offer explainable denial prediction and recommendation history. Decision-makers need to see model confidence scores to understand why the AI flagged a specific claim.
Continuous bias monitoring and model drift tracking ensure that the system remains fair and accurate over time.
- Human approval logs: Documents every time a staff member accepts or overrides an AI suggestion.
- Error analysis: Identifies where the model might be making systemic mistakes for targeted retraining.
- Explainable denial prediction: Provides clear reasons why a claim is at risk of being rejected.
6. Security Controls For Enterprise RCM Platforms
Enterprise-grade security requires robust access controls like Single Sign-On (SSO) and Multi-Factor Authentication (MFA). Encryption must be the standard for all data pipelines, and activity monitoring should trigger alerts for any unusual behavior.
Regular data backups and secure integration protocols ensure the platform remains resilient against potential cyber threats.
- MFA and SSO: Ensures that only verified personnel can enter the financial ecosystem.
- Activity monitoring: Scans for internal and external threats in real-time.
- Secure integrations: Validates that every third-party connection meets the same high security standards.
Building a platform with these safeguards ensures that your enterprise can scale without the fear of regulatory penalties. Compliance-first engineering is the most effective way to protect both your patients and your profits.
AI RCM Platform Architecture
Building an enterprise-grade AI RCM platform requires a decoupled, resilient architecture that handles high-volume data transactions with millisecond latency.
This multi-layered approach ensures that each component can scale independently while maintaining the strict security protocols necessary for healthcare finance.
1. Frontend Layer For RCM Teams
The frontend serves as the command center for various user roles, from medical coders to CFOs. It must provide a responsive, intuitive interface that prioritizes urgent tasks, such as high-value denial appeals or pending authorization requests.
By using modular dashboard components, different teams can visualize the specific KPIs that drive their daily productivity.
- Role-based dashboards: Custom views for billing specialists, coders, and executives.
- Claim queues: Real-time lists of claims requiring manual intervention or review.
- Denial worklists: Prioritized rejections categorized by recovery probability and dollar value.
- Tech Stack: React.js or Angular for the UI framework, Tailwind CSS for styling, and D3.js or Recharts for complex data visualizations.
2. Backend Services Layer
The backend architecture follows a microservices pattern, where individual services manage specific domains like claims, payments, or patient data. This prevents a failure in one area from taking down the entire system.
These services communicate via high-speed APIs to ensure that data flows seamlessly from the point of service to final reconciliation.
- Claims and Payer Services: Logic for managing the lifecycle of medical claims and insurance interactions.
- Notification service: Triggers alerts for missing documentation or urgent denial deadlines.
- Tech Stack: Node.js, Python (FastAPI), or Go for service development; Docker and Kubernetes for orchestration; and Redis for high-speed caching.
3. Model Monitoring And Feedback Layer
Launching an AI model is only the beginning; maintaining its accuracy requires constant oversight. This layer tracks prediction accuracy and monitors for “model drift,” which happens when payer behaviors change, and the AI’s logic becomes outdated.
Staff feedback loops allow the system to learn from rejected recommendations, creating a continuous improvement cycle.
- Prediction accuracy tracking: Comparing AI denial predictions against actual payer outcomes.
- Retraining triggers: Automated alerts that signal when a model’s performance falls below a set threshold.
- Tech Stack: Prometheus and Grafana for monitoring, Weights & Biases or MLflow for model tracking, and custom feedback capture tools.
4. AI Model Layer
This layer houses the specialized machine learning models that provide the “intelligence” of the platform. These include NLP models for document classification and predictive models for revenue forecasting.
Each model is trained on vast datasets of historical claims and payer responses to identify patterns that humans might miss.
- Denial prediction model: Foresees rejections based on hundreds of claim variables.
- Payer behavior model: Analyzes how specific insurers respond to different types of clinical documentation.
- Tech Stack: PyTorch or TensorFlow for model training, Scikit-learn for traditional ML, and Hugging Face for NLP-based coding assistance.
5. Rules Engine Layer
The rules engine provides a rigid validation gate that works alongside the fluid logic of the AI. It handles the “hard rules” of healthcare, such as specific payer requirements, CPT coding constraints, and federal compliance mandates.
This ensures that every claim is technically perfect before it is ever submitted for reimbursement.
- Payer and Compliance rules: Up-to-date databases of insurer-specific billing guidelines.
- Claim edits: Automated checks that prevent common errors like mismatched modifiers or missing IDs.
- Tech Stack: Drools, Camunda, or custom-built Python-based rule engines with versioned logic.
6. Workflow Orchestration Layer
Efficiency depends on getting the right task to the right person at the right time. The orchestration layer manages task routing, exception queues, and SLA tracking to ensure that no claim sits idle.
It handles escalation logic, automatically moving a task to a supervisor if a deadline is approaching.
- Task routing: Assigning claims to specialists based on their expertise and current workload.
- SLA tracking: Monitoring how long it takes to resolve denials or appeals.
- Tech Stack: Apache Airflow, Temporal.io, or AWS Step Functions for managing complex, long-running workflows.
7. Integration Layer
The integration layer is the gateway to the outside world, connecting the platform to EHRs, clearinghouses, and payer portals. It must support multiple data standards, including legacy HL7 and modern FHIR APIs.
Secure connectors ensure that patient data and financial records move across these systems without compromising security.
- FHIR and X12 EDI: Standards for exchanging clinical and financial healthcare information.
- Clearinghouse connectors: Direct pipelines to major hubs like Availity or Change Healthcare.
- Tech Stack: Mirth Connect for HL7/EDI processing, Apigee for API management, and Azure Integration Services or AWS AppSync.
8. Data And Analytics Layer
This layer is responsible for storing, processing, and analyzing the massive amounts of data generated by the revenue cycle. An operational database handles daily transactions, while a data lake or warehouse stores historical data for long-term trend analysis.
This data provides the fuel for BI dashboards and the training sets for future AI models.
- Analytics pipelines: Moving and transforming data from raw encounters into actionable insights.
- Model training datasets: Curated, cleaned data used to improve the accuracy of the AI layer.
- Tech Stack: PostgreSQL or MongoDB for operations; Snowflake, BigQuery, or Redshift for the data warehouse; and Apache Spark for heavy data processing.
By structuring the architecture this way, an enterprise can build a platform that is not only powerful but also adaptable to the ever-changing healthcare landscape. This technical depth is what ultimately ensures a high return on investment and long-term operational success.
How Much Does It Cost To Build An AI RCM Platform?
The cost to build an AI RCM platform usually ranges from $50,000 to $200,000+, depending on AI workflows, integrations, compliance, and platform scope.
Building an AI revenue cycle management platform costs more than a standard billing system because it must support healthcare finance workflows, payer logic, AI automation, secure integrations, and compliance controls in one connected environment.
| AI RCM Platform Type | Estimated Cost | Best For |
| AI RCM MVP | $50,000–$80,000 | Startups or healthcare teams validating one revenue workflow |
| Mid-Level AI RCM Platform | $80,000–$140,000 | Clinics, billing companies, or SaaS teams needing AI automation and integrations |
| Enterprise AI RCM Platform | $140,000–$200,000+ | Hospitals, RCM providers, and multi-location healthcare groups need deeper workflow coverage |
Key Factors That Affect AI RCM Platform Cost
The final development cost depends on workflow complexity, AI scope, integration depth, and compliance requirements. A focused denial prediction platform costs far less than a full AI RCM ecosystem with coding support, payer integrations, payment reconciliation, and executive analytics.
The biggest cost drivers usually include AI model complexity, data readiness, healthcare integrations, reporting depth, and the number of operational workflows.
Cover:
- Number of RCM workflows
- AI model complexity
- EHR and EMR integration depth
- Clearinghouse integration
- Payer API and X12 EDI requirements
- Prior authorization workflows
- Data cleanup and migration
- Role-based access requirements
- Compliance and audit controls
- Reporting and dashboard depth
How To Reduce AI RCM Development Cost Without Hurting ROI
The best way to control development cost is to avoid building too many workflows too early. Most successful AI RCM products start with one measurable revenue outcome and expand after proving ROI.
Healthcare businesses can usually reduce risk and cost by validating a focused MVP first instead of launching a full enterprise platform immediately.
Cover:
- Start with one AI workflow
- Prioritize high-impact revenue problems
- Reuse existing healthcare systems where possible
- Limit integrations in the first release
- Use human review instead of full automation initially
- Roll out features in phases
- Track ROI before expanding scope
AI RCM platform cost depends less on the number of screens and more on workflow complexity, payer integrations, AI depth, compliance requirements, and operational scope.
Conclusion
Building an AI revenue cycle platform is a strategic investment that transforms healthcare financial operations from reactive to predictive. By integrating intelligent modules and agentic workflows, enterprises can protect their margins and eliminate systemic revenue leakage.
This technology does not just save costs; it creates a resilient, scalable infrastructure for long-term growth. Now is the time to leverage these advanced tools to ensure every clinical service translates into realized value.
Build An AI Revenue Cycle Platform With Intellivon
At Intellivon, we build AI-powered revenue cycle management platforms for hospitals, specialty clinics, healthcare SaaS companies, billing providers, telehealth platforms, diagnostic networks, and enterprise healthcare teams. Our engineering approach focuses on real revenue workflows, payer-aware automation, secure healthcare integrations, and measurable financial outcomes.
Whether you want to launch a focused AI RCM MVP or develop a full enterprise platform, Intellivon helps you plan, build, integrate, and scale a solution designed for real healthcare operations.
A. Build AI Around Real Financial Outcomes
Our AI workflows are designed to improve measurable revenue metrics instead of generating unnecessary alerts or disconnected analytics.
- Denial prediction
- AI claim scrubbing
- Coding support workflows
- Underpayment detection
- Payment forecasting
- Claim prioritization
- Revenue leakage visibility
B. Develop Payer-Aware Revenue Systems
AI RCM platforms work best when they understand payer-specific rules, authorization requirements, reimbursement behavior, and denial trends.
- Payer-specific claim logic
- Prior authorization intelligence
- Contract variance detection
- Payer performance tracking
- Denial pattern analysis
- Appeal workflow support
C. Integrate With Healthcare And Finance Infrastructure
Revenue cycle platforms depend on reliable data exchange between clinical, billing, payment, and finance systems. We build secure integrations that keep workflows connected across the organization.
- EHR and EMR systems
- Practice management software
- Clearinghouses
- X12 EDI workflows
- FHIR APIs
- Payment gateways
- Accounting and ERP systems
D. Scale Beyond The MVP
Most successful AI RCM platforms start with one focused workflow before expanding into broader automation and analytics. We help healthcare teams scale safely after launch.
- Workflow optimization
- New AI modules
- Payer rule updates
- Model retraining
- KPI dashboards
- Enterprise rollout support
- Multi-location scaling
If you are planning to build an AI revenue cycle management platform, contact Intellivon to develop a secure, scalable, and revenue-focused solution built for real healthcare operations.
Common Queries
Q1. How does AI improve revenue cycle management?
A1. AI improves revenue cycle management by predicting denials, checking claim errors, supporting medical coding, automating eligibility checks, prioritizing follow-ups, detecting underpayments, and forecasting revenue. It helps healthcare teams prevent revenue leakage before claims fail, instead of only reacting after denials or payment delays happen.
Q2. What features should an AI RCM platform include?
A2. An AI RCM platform should include patient registration, eligibility verification, prior authorization, coding support, charge capture, claims scrubbing, denial prediction, payment posting, patient billing, collections, analytics, audit logs, and compliance controls. The best platforms connect these modules into one workflow, not separate tools.
Q3. How much does it cost to build an AI RCM platform?
A3. An AI RCM platform can cost around $60,000–$100,000 for an MVP, $100,000–$180,000 for a mid-level system, and $180,000–$320,000+ for an enterprise platform. Cost depends on AI features, EHR integrations, payer connections, compliance needs, and automation depth.
Q4. How long does it take to build an AI RCM platform?
A4. A focused AI RCM MVP usually takes 4–6 months. A mid-level platform can take 6–9 months. A full enterprise platform with EHR integrations, payer APIs, AI models, denial workflows, payment reconciliation, and compliance controls may take 9–18+ months.