Key Takeaways:
-
AI reduces missed findings, false positives, and measurement errors by acting as a continuous second reader across CT, MRI, X-ray, ultrasound, and mammography.
-
Real accuracy depends on training data diversity, validated models, secure DICOM pipelines, PACS integration, and explainable outputs that radiologists can verify.
-
Sensitivity, specificity, AUC, and turnaround time determine clinical value, not laboratory accuracy scores alone.
-
Build costs range from $50,000 for a basic MVP to $280,000 and above for an enterprise multi-modality platform with compliance controls and model monitoring.
-
How Intellivon builds AI medical imaging diagnostic systems your enterprise fully owns, with validated models, PACS integration, and compliance-ready architecture from day one.
Medical imaging is one of the most data-rich areas in healthcare. Every CT scan, MRI, and X-ray provides thousands of data points that clinicians use to make important decisions. However, the challenge is that the number of scans is increasing faster than the capacity of radiology. At the same time, subtle abnormalities can be hard to identify consistently under pressure.
AI in imaging diagnostics changes this situation. Instead of replacing radiologists, AI offers an extra layer of analysis. Furthermore, it flags suspicious areas, measures findings accurately, and helps with quicker, more informed reporting across different facilities.
At Intellivon, we create AI imaging solutions that meet the needs of clinical environments where accuracy, compliance, and scalability are critical. In this blog, we discuss how AI improves detection accuracy, reduces reporting differences, fits into clinical workflows, and presents a strong case for investment to healthcare entrepreneurs.
Why Enterprises Are Adopting AI in Medical Imaging Diagnostics Now
AI adoption in medical imaging has moved from early experimentation to mainstream deployment. Healthcare organizations using AI for at least one imaging application have grown from 17% in 2018 to over 50% today. That shift reflects both growing clinical confidence and real efficiency gains that enterprises can measure.
The AI in medical imaging market is projected to grow by USD 5.17 billion between 2024 and 2029, at a CAGR of 28.1%. That growth is not speculative. It is being pulled forward by real clinical demand for faster, more precise diagnostics at scale.
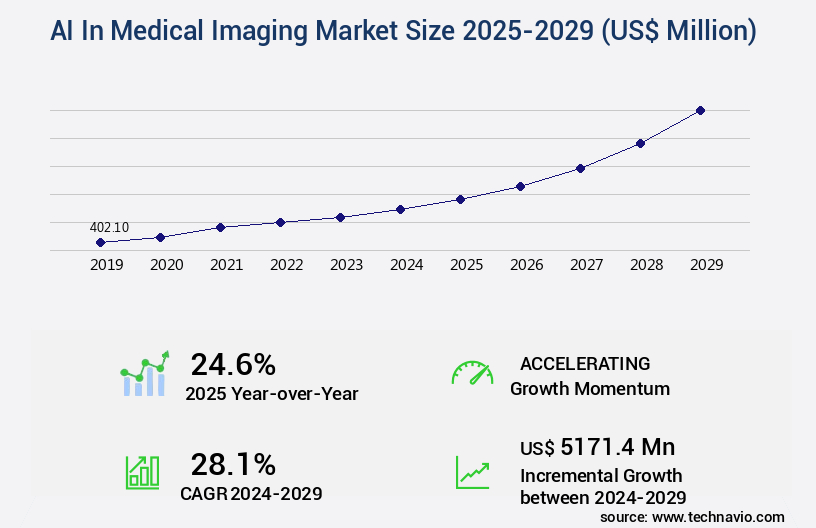
Adoption Statistics
AI imaging adoption has crossed the halfway mark globally. Current deployment stands at 50%, up from 17% in 2018. Nearly one-third of non-users plan to implement within two years, pushing combined adoption to 53%.
- Computer-aided detection leads use cases at 92.6% of adopters
- High-volume centers show adoption rates well above the global average
- Workflow optimization ranks as the second most common application
Top Players
| Company | Key AI Focus | Notable Achievements |
| GE HealthCare | Radiology AI across scanners | 100+ FDA authorizations |
| Siemens Healthineers | Optiq AI, cardio imaging | 64 FDA clearances |
| Philips Healthcare | Spectral CT, cardiac MRI | 45% energy cut, 2x faster exams |
| Aidoc | Critical condition triage | 30% faster turnaround |
| Qure.ai | Stroke, oncology algorithms | Disease-specific platforms |
ROI Evidence
Hospitals deploying AI imaging report measurable financial returns.
- Radiologist productivity improves 20 to 30%
- Turnaround times drop 30 to 50%
- Diagnostic accuracy gains of 5 to 15%
- Broader implementations save USD 55 to 72 million annually
What Does AI Mean In Medical Imaging Diagnostics?
AI in medical imaging diagnostics refers to the use of machine learning and deep learning algorithms to analyze medical images such as X-rays, CT scans, and MRIs. These systems are trained on large datasets to detect abnormalities, measure findings, and prioritize cases.
The goal is to support radiologists with faster, more consistent analysis across high volumes
of imaging data. This technology acts as a force multiplier for existing hospital infrastructure and patient management.
1. AI As A Diagnostic Support Layer
AI operates as a powerful partner rather than a replacement for trained medical professionals. The technology excels at handling repetitive tasks such as measuring the volume of a lesion or segmenting an organ.
Consequently, radiologists can focus their cognitive energy on complex cases that require nuanced human judgment.
- Clinical Triage. Algorithms flag urgent findings like brain hemorrhages and move them to the top of the specialist queue.
- Consistency. Software provides the same level of analytical depth at the end of a long shift as it does at the start.
- Error Reduction. The system acts as a second set of eyes to catch small nodules or subtle fractures.
This collaborative approach ensures that every scan undergoes a rigorous dual-check process. Integration into existing hospital systems must be seamless to avoid creating friction for the staff.
2. AI Across CT, MRI, X-Ray, Ultrasound, Mammography, And PET
Different imaging modalities present unique challenges that require specialized algorithmic training. An X-ray is a flat two-dimensional image, while a CT scan involves thousands of three-dimensional cross-sections.
Therefore, a model designed for bone fractures cannot be used to analyze cardiac blood flow without extensive retraining.
- Modality Specificity. Each scan type has unique physics that the AI must be specifically tuned to interpret.
- Dataset Diversity. Effective platforms require training data from various equipment manufacturers to ensure universal accuracy.
- Enterprise Versatility. A comprehensive suite covering oncology and neurology offers a larger market moat than a single-use tool.
Precise engineering is necessary to ensure the AI understands the specific constraints of each machine. Diverse datasets are essential because they teach the model to recognize variations across different hardware.
3. AI Detection, AI Triage, AI Segmentation, And AI Reporting
Detection involves the core ability of the software to find suspicious patterns like nodules or calcifications. Once detected, the triage function kicks in to reorganize the workflow based on the severity of the findings.
This automated prioritization is a game-changer for high-volume urban trauma centers.
- Pathology Detection. The AI identifies anomalies across the entire image field with high sensitivity.
- Automated Segmentation. Software outlines the exact boundaries of tumors for precise surgical or radiation planning.
- Structured Reporting. The system translates visual findings into standardized text for faster insurance and clinical processing.
Strategic implementation of these four pillars creates a cohesive diagnostic environment. Each function addresses a specific bottleneck in the current medical workflow.
Implementing these diagnostic layers effectively reduces human error and speeds up the delivery of care. This technical depth allows healthcare founders to build scalable platforms that meet the highest standards of medical excellence.
Why Accuracy Is Still A Major Challenge In Medical Imaging
Healthcare enterprises face a growing crisis where diagnostic demand far outpaces the available specialist workforce. This imbalance creates immense pressure on clinical accuracy as teams struggle to maintain quality under extreme throughput requirements.
Investors must recognize that these systemic bottlenecks represent the primary market drivers for AI adoption. Addressing these challenges is the first step toward building a resilient and profitable diagnostic platform.
1. Radiology Teams Handle Growing Imaging Volumes
Modern hospitals process an unprecedented number of scans as diagnostic imaging becomes the cornerstone of every medical department. This surge often leads to significant reporting delays, which can stall critical patient treatment plans.
- Volume Growth. The total number of CT and MRI scans continues to rise annually across global health systems.
- Workload Pressure. Radiologists are often required to interpret hundreds of images per hour to keep up with demand.
- Systemic Delays. Bottlenecks in the imaging queue can result in longer hospital stays and increased operational costs.
These factors combine to create a landscape where human experts are pushed to their absolute cognitive limits. Maintaining peak performance in such an environment is a significant challenge for any diagnostic center.
2. Small Or Early Findings Can Be Easy To Miss
Early-stage diseases often manifest as incredibly subtle changes in tissue density that are difficult for the human eye to perceive. These tiny markers are the most critical for patient survival but also the most susceptible to being overlooked.
- Oncology. Early tumors and lung nodules can be smaller than a few millimeters in diameter.
- Breast Health. Microcalcifications in mammography often require intense magnification to be identified correctly.
- Trauma. Hairline fractures and small internal bleeds can be masked by surrounding dense tissue or bone.
Detecting these minute details requires a level of focus that is difficult to sustain over a long shift. This vulnerability represents a clear opportunity for algorithmic assistance to improve patient safety.
3. Human Fatigue Can Affect Review Quality
Visual search tasks are notoriously sensitive to the effects of exhaustion and long working hours. When a specialist reviews thousands of images in a single day, the risk of a false negative result naturally increases.
- Cognitive Load. The mental energy required to analyze complex 3D scans leads to rapid decision fatigue.
- Emergency Workload. Overnight shifts in trauma centers often involve high-stakes decisions under suboptimal conditions.
- Repetitive Stress. Constant scanning for the same types of anomalies can lead to habituation.
Mitigating the impact of fatigue is essential for maintaining a high standard of care across a hospital network. AI provides a consistent baseline of performance that does not fluctuate based on the time of day.
4. Diagnostic Interpretation Can Vary Between Readers
Subjectivity remains a persistent hurdle in medical imaging, as different specialists may interpret the same scan differently. These variations can stem from differences in training, years of experience, or specific subspecialty expertise.
- Experience Gaps. Junior residents may lack the nuanced pattern recognition of a veteran radiologist.
- Inter-rater Variability. Multiple readers often disagree on the exact boundaries or severity of a detected lesion.
- Site Inconsistency. A scan interpreted at a rural clinic might receive a different classification than one at a major hospital.
Standardization ensures that every patient receives a high quality of care regardless of which specialist is on duty. AI helps bridge this gap by providing a mathematical and objective assessment of the data.
5. Imaging Data Often Sits In Disconnected Systems
Critical patient information is frequently trapped in isolated silos like the EHR or lab result databases. Without access to a patient’s full medical history, a radiologist might lack the context needed to interpret a confusing image.
- Data Fragmentation. Vital clues from prior scans or pathology reports are often not visible within the primary software.
- Workflow Friction. Manually searching for clinical notes across different platforms wastes valuable time and increases the risk of error.
- Contextual Blindness. An abnormality may look benign without the knowledge of a patient’s recent surgery or laboratory markers.
Connecting imaging AI with a broader clinical context allows for much higher diagnostic confidence. This integration transforms isolated images into a comprehensive map of a patient’s health status.
Solving these systemic challenges requires a strategic shift toward integrated, intelligent infrastructure. This approach improves accuracy and drives significant operational efficiencies for the entire enterprise.
How AI Improves Accuracy In Medical Imaging Diagnostics
AI transforms medical imaging by identifying complex patterns that exist beyond the limits of human perception. These systems analyze pixel-level data to surface early disease signals with incredible consistency and mathematical precision. This transition from subjective observation to data-driven analysis is fundamental for modern diagnostic accuracy.
Strategic investment in these tools allows healthcare providers to scale their diagnostic capabilities while maintaining the highest safety standards. This section explores the specific mechanisms that make AI an indispensable asset for enterprise-grade medical platforms.
1. Detects Subtle Patterns In Medical Images
Sophisticated algorithms excel at identifying minute changes in tissue density and texture that might appear normal to a human observer. These systems process thousands of data points simultaneously to determine if a specific region represents a pathological threat.
- Pixel-Level Analysis. AI evaluates the entire image grid to find anomalies that occupy only a few pixels.
- Texture Recognition. Algorithms identify irregularities in tissue surface patterns that indicate early-stage malignancy.
- Early Disease Signals. Software can detect the subtle loss of gray-white matter differentiation in early neurological cases.
By surfacing these hidden markers, AI provides a significant head start in the treatment of aggressive diseases. This capability is a primary driver for better patient survival rates in oncology and neurology.
2. Reduces Missed Findings With Second-Reader Support
Providing a constant second set of eyes ensures that no critical finding goes unnoticed during a high-speed clinical review. This support is especially vital in busy trauma centers where the volume of scans can lead to oversight.
- Concurrent Review. The software analyzes images in real-time as the specialist opens the file for study.
- Visual Flagging. Suspicious regions are highlighted with digital overlays to draw immediate attention to potential issues.
- False Negative Reduction. Validated models act as a safety net to catch lesions that may be missed during manual reads.
This redundant layer of verification builds immense trust between the technology and the clinical staff. It ensures that the diagnostic output remains robust even during periods of peak hospital activity.
3. Reduces False Positives With Risk Scoring
Overdiagnosis can lead to unnecessary patient anxiety and expensive follow-up procedures that strain hospital resources. AI mitigates this by providing probability-based risk scores that help specialists differentiate between benign and malignant patterns.
- Confidence Scores. Every detection includes a numerical value representing the likelihood of a true positive finding.
- Risk Thresholding. Enterprises can calibrate these thresholds to match the specific clinical requirements of their department.
- Pattern Separation. Advanced models distinguish between harmless anatomical variations and actual disease markers.
Lowering the rate of false positives improves the overall efficiency of the healthcare system. It allows physicians to focus their intervention efforts on patients who truly require medical care.
4. Improves Lesion And Organ Segmentation
Accurate boundary marking is essential for surgical planning and ensuring that radiation therapy targets only the diseased tissue. Manual segmentation is a tedious process that is highly prone to human variability and measurement error.
- Boundary Precision. Algorithms outline the exact edges of tumors with sub-millimeter accuracy for better surgical outcomes.
- Volumetric Calculation. Software automatically calculates the total volume of a lesion to track its size over time.
- Disease Mapping. Multi-dimensional mapping helps specialists visualize the relationship between a tumor and surrounding healthy organs.
These automated measurements provide a level of detail that is difficult to achieve manually. This precision is critical for the success of complex oncological treatments and long-term monitoring.
5. Tracks Changes Across Prior And Current Scans
Monitoring the progression of a chronic condition requires a precise comparison between images taken months or years apart. AI excels at longitudinal tracking by aligning historical data with current scans to identify even the slightest changes.
- Growth Tracking. Algorithms detect minute increases in tumor size that indicate a need for a change in treatment.
- Recurrence Monitoring. Systemic scans are automatically compared to baseline images to catch any signs of returning disease.
- Treatment Response. AI quantifies how a tumor reacts to chemotherapy or radiation by measuring density changes.
Consistent tracking across the patient journey ensures that therapy remains effective and targeted. This historical context is vital for managing long-term health outcomes in complex patient populations.
6. Improves Image Quality Before Interpretation
Poor scan quality can often obscure vital information and lead to a delayed or incorrect diagnosis for the patient. AI tools enhance the raw output of imaging hardware to create sharper and more readable results for the specialist.
- Noise Reduction. Deep learning filters out electronic interference to provide a cleaner view of internal structures.
- Low-Dose Reconstruction. Software can generate high-quality images from low-radiation CT scans to protect patient health.
- MRI Acceleration. AI reduces the time a patient must spend in an MRI machine while maintaining high resolution.
Higher image quality directly supports a more accurate and confident diagnosis by the clinical team. This improvement also enhances patient comfort by making the imaging process faster and less invasive.
Deploying these advanced imaging layers creates a formidable technological moat for any diagnostic enterprise. This strategic depth ensures that your platform delivers superior clinical value and operational reliability.
Key AI Technologies That Improve Diagnostic Accuracy
Technical innovation in medical imaging relies on a specific stack of algorithms designed to mimic and enhance human visual perception. These underlying architectures ensure that software remains reliable across diverse clinical environments.
Understanding these core components is essential for any enterprise looking to build a defensible diagnostic platform. This section breaks down the strategic technologies that drive accuracy in modern diagnostic workflows.
1. Computer Vision For Image Pattern Recognition
Computer vision serves as the foundation for modern imaging software by enabling machines to interpret visual data. It focuses on extracting meaningful information from raw pixels to understand human anatomy.
- Feature Extraction. The system identifies specific edges and shapes that define potential pathologies.
- Density Analysis. Algorithms measure variations in pixel intensity to detect calcifications or fluid accumulations.
- Texture Recognition. Software analyzes surface characteristics to differentiate between healthy and diseased states.
These basic recognition tasks allow the AI to build a comprehensive map of the scan. Consequently, the system can identify deviations from a normal anatomical baseline with extreme precision.
2. Deep Learning For Complex Medical Image Analysis
Deep learning takes pattern recognition further by using neural networks to learn from vast libraries of medical data. These models improve over time as they are exposed to more diverse examples of rare diseases.
- Neural Networks. Convolutional Neural Networks are specifically designed to process the grid-like structure of medical images.
- Vision Transformers. Advanced architectures analyze the relationship between different parts of an image to understand context.
- Modality Training. Models are specifically tuned for the unique physics of CT, MRI, or X-ray hardware.
This depth of analysis allows the software to handle complex diagnostic tasks that require a nuanced understanding of biology. It represents the highest level of machine intelligence currently available in the medical field.
3. Segmentation Models For Precise Region Mapping
Segmentation is the process of partitioning a digital image into multiple segments to simplify its analysis. This technology is vital for identifying the exact physical space occupied by a tumor or an organ.
- Boundary Mapping. Algorithms provide pixel-perfect outlines of lesions for surgical and radiation planning.
- Volumetric Analysis. The system calculates the three-dimensional volume of structures to monitor growth or shrinkage.
- Structural Isolation. Software can digitally remove healthy tissue to focus exclusively on a diseased region.
Precise mapping reduces the margin of error in critical medical interventions. This technical capability ensures that treatments are as targeted and effective as possible for every patient.
4. Classification Models For Diagnostic Decision Support
Classification algorithms assign a category to an image based on the specific features they detect. This technology helps streamline the radiologist’s workflow by providing an immediate initial assessment of the findings.
- Severity Grading. The AI classifies a finding as mild, moderate, or severe based on established clinical criteria.
- Priority Triage. Systems automatically label scans as urgent to ensure critical cases are handled first.
- Multi-Class Diagnosis. Advanced models can identify and categorize multiple pathologies within a single scan.
These automated labels provide a structured starting point for the final human review. This organization is a key driver of operational efficiency in high-volume diagnostic centers.
5. Anomaly Detection For Rare Or Unexpected Findings
Anomaly detection focuses on identifying patterns that do not conform to expected anatomical norms. This serves as a vital safety net for spotting rare conditions that a specialist might not encounter frequently.
- Outlier Identification. The system flags any data point that deviates significantly from a standard healthy dataset.
- Safety-Net Review. AI acts as a constant monitor to ensure that unusual findings receive a second look.
- Unknown Abnormality Flagging. Models can alert a radiologist to a suspicious region even if they cannot specifically name the disease.
This broad-spectrum monitoring protects against the risk of overlooking a rare but critical diagnosis. It provides an additional layer of security for both the patient and the provider.
6. Predictive Analytics For Risk And Progression
Predictive models use current imaging data to forecast how a disease might evolve over time. This forward-looking approach allows for a more proactive and personalized strategy for patient care.
- Progression Modeling. Algorithms estimate the likely growth rate of a tumor based on historical data patterns.
- Recurrence Risk. Software identifies subtle markers that suggest a high probability of a disease returning.
- Follow-Up Planning. Analytics help clinicians determine the optimal timing for the next scan based on individual risk.
Integrating predictive insights into the diagnostic process shifts the focus from reactive treatment to proactive health management. This strategic foresight is a significant value add for any enterprise healthcare platform.
Investing in these core technologies creates a robust framework for high-precision medical diagnostics. This technical maturity allows leading organizations to set new benchmarks for patient care and clinical accuracy.
Where AI Improves Accuracy Across Imaging Modalities
Technological advances in medical imaging have tailored AI applications to the unique physical properties of each diagnostic format. This specificity ensures that algorithms can address the precise challenges of various scan types with maximum reliability.
Investors should prioritize platforms that demonstrate high performance across multiple modalities to capture the broadest market share. This section illustrates how intelligence is specifically applied to the primary pillars of diagnostic imaging.
1. AI In CT Scan Diagnostics
Computed Tomography generates massive datasets that require rapid and precise analysis to manage patient throughput effectively. AI excels at interpreting these complex three-dimensional volumes to surface life-threatening conditions within seconds.
- Vascular Emergencies. Algorithms detect pulmonary embolisms and aortic dissections with high sensitivity to speed up emergency interventions.
- Neurological Care. Specialized stroke workflows identify brain hemorrhages and vessel occlusions to minimize permanent tissue damage.
- Dose Optimization. Advanced reconstruction tools allow for ultra-low-dose scans that protect patients while maintaining diagnostic clarity.
Recent findings from MGM Malar Hospitals in Chennai highlight this impact by showing that AI-enhanced reconstruction can slash radiation exposure by up to 80%.
This breakthrough allows for safer lung cancer screenings without compromising the accuracy needed to catch early-stage tumors.
2. AI In MRI Diagnostics
Magnetic Resonance Imaging provides exceptional soft tissue contrast but is often limited by long scan times and complex interpretation.
AI addresses these bottlenecks by accelerating the acquisition process and automating the segmentation of intricate anatomical structures.
- Tumor Segmentation. Systems provide precise volumetric mapping of brain tumors to track growth and plan surgical approaches.
- Neurological Mapping. Deep learning models identify subtle biomarkers for neurodegenerative diseases like Alzheimer’s and multiple sclerosis.
- Artifact Reduction. Algorithms filter out motion artifacts caused by patient movement to prevent the need for repeat scans.
These improvements make MRI a more efficient and accessible tool for complex diagnostic challenges. By reducing the time a patient spends in the machine, healthcare providers can significantly increase their daily scan capacity.
3. AI In X-Ray Diagnostics
X-rays remain the most widely used imaging modality globally and serve as the first line of defense in most clinical settings. AI integration provides a vital safety net by flagging critical findings on routine chest and musculoskeletal films.
- Triage Automation. Software automatically prioritizes scans showing signs of pneumonia, tuberculosis, or a collapsed lung.
- Fracture Detection. Algorithms highlight subtle hairline fractures that might be difficult to see on standard monitors.
- Public Health Screening. Large-scale AI deployments allow for rapid tuberculosis screening in regions with limited access to specialist radiologists.
The widespread nature of X-ray imaging makes this a prime area for high-impact AI deployment. This technology ensures that even at the primary care level, patients benefit from expert-grade diagnostic oversight.
4. AI In Mammography Diagnostics
Breast cancer screening requires a high level of precision to identify tiny calcifications while minimizing the risk of false positives. AI acts as a sophisticated double-reader that supports specialists in navigating the complexities of dense breast tissue.
- Risk Stratification. Systems categorize findings based on their probability of malignancy to guide follow-up biopsy decisions.
- Interval Cancer Detection. AI identifies subtle changes across consecutive years of screening to find cancers that appear between regular appointments.
- Consistency. Software provides an objective assessment that reduces the variability often seen between different human readers.
Implementing these tools improves the early detection rates that are critical for patient survival. This focus on preventive health represents a significant opportunity for sustainable growth in the diagnostic market.
5. AI In Ultrasound Diagnostics
Ultrasound is a highly operator-dependent modality where the quality of the scan relies heavily on the skill of the technician. AI provides real-time guidance and automated measurements to standardize results across different clinical settings.
- Fetal Monitoring. Algorithms automatically measure key growth metrics during prenatal scans to ensure healthy development.
- Cardiac Assessment. Deep learning tools calculate ejection fractions and heart wall thickness with greater speed than manual methods.
- Real-Time Feedback. Systems guide the probe placement for less experienced users to ensure the highest quality images are captured.
Standardizing ultrasound results reduces the need for patients to return for secondary imaging. This operational efficiency lowers costs and improves the overall patient experience within the healthcare system.
6. AI In PET And Nuclear Imaging
Positron Emission Tomography involves mapping metabolic activity to identify active disease sites at the molecular level. AI enhances this process by improving the signal-to-noise ratio and providing quantitative biomarkers for treatment response.
- Metabolic Mapping. Software distinguishes between inflammatory processes and active malignant growth with high accuracy.
- Staging Support. Algorithms identify the spread of disease across the body to help oncologists determine the best course of action.
- Recurrence Detection. High-sensitivity models find small clusters of metabolic activity that indicate the early return of cancer.
Quantitative imaging biomarkers allow for a much more data-driven approach to oncology and chronic disease management. This technical depth is essential for the future of personalized medicine and precision healthcare.
Deploying specialized AI across these various modalities ensures a comprehensive approach to modern medical diagnostics. This versatile technical stack creates a powerful competitive advantage for any enterprise-grade imaging platform.
How AI Reduces Diagnostic Errors In Radiology Workflows
Diagnostic errors often stem from a combination of systemic pressure and the limits of human visual fatigue. AI provides a standardized layer of oversight that maintains peak analytical performance regardless of clinical volume or time of day.
Investors must understand that reducing errors is a direct path to lowering hospital liability and improving long-term patient retention. This section highlights how algorithmic precision mitigates the most common risks in modern radiology.
1. Reducing False Negatives
A false negative occurs when a disease is present but remains undetected during the initial review of the scan. AI serves as a vigilant second reader that specifically monitors for subtle lesions and early-stage abnormalities that might be overlooked.
- Second-Reader Alerts. The software highlights suspicious pixels in real-time to ensure no region is dismissed prematurely.
- High-Risk Monitoring. Algorithms maintain high sensitivity for critical conditions like small pulmonary nodules or hairline fractures.
- Subtle Pattern Detection. Deep learning models recognize the faint shadows of early disease that fall below the threshold of human perception.
Minimizing these missed findings is the most impactful way to improve clinical outcomes and survival rates. This capability transforms the diagnostic process into a more resilient and reliable system for every patient.
2. Reducing False Positives
Unnecessary follow-ups and biopsies caused by false positives create a massive financial and emotional burden for patients and providers. AI improves the specificity of diagnostics by applying probability-based validation to every detected pattern.
- Confidence Thresholds. Systems provide a numerical likelihood for each finding to help specialists prioritize actual threats.
- Benign vs. Suspicious. Advanced classification models distinguish between harmless anatomical variations and genuine pathologies.
- Pattern Validation. The software cross-references visual data with known disease signatures to confirm the validity of a flag.
Better accuracy in these classifications prevents the strain of overdiagnosis on the healthcare ecosystem. Consequently, hospitals can allocate their resources more effectively toward patients who require immediate intervention.
3. Reducing Delayed Diagnosis
In emergency medicine, the time between a scan and a final report can be the difference between recovery and permanent damage. AI automates the prioritization of the imaging queue by routing urgent cases to the top of the specialist’s list.
- Critical Finding Alerts. Systems instantly notify the clinical team if a scan shows signs of acute conditions like a brain bleed.
- Urgent Case Routing. Algorithms sort the global worklist so that the most severe cases receive the earliest attention.
- Emergency Prioritization. AI ensures that trauma scans are analyzed ahead of routine check-ups, regardless of when they were taken.
Faster review cycles lead to quicker treatment starts and shorter overall hospital stays for the patient. This operational speed is a vital metric for any enterprise-grade healthcare platform.
4. Reducing Measurement Errors
Manual measurements are inherently subjective and often vary significantly between different radiologists or even different shifts. AI automates these quantitative tasks to ensure that every lesion and organ is measured with mathematical exactness.
- Automated Volumetrics. The software calculates the three-dimensional volume of tumors to provide a more accurate picture of disease burden.
- Consistent Tracking. Algorithms use the same logic for every scan to ensure that growth or shrinkage is measured accurately over time.
- Structural Metrics. AI provides precise data on organ size and wall thickness that is difficult to achieve with manual calipers.
Standardized measurements are essential for monitoring the effectiveness of oncology treatments and chronic disease progression. This data-driven approach removes the guesswork from critical clinical decisions.
5. Reducing Multi-Site Reporting Variation
Large healthcare networks often struggle with inconsistent diagnostic quality across different clinics and hospital branches. AI provides a centralized logic that ensures a scan in a rural facility is interpreted with the same rigor as one in a major urban center.
- Shared Protocols. Every site within the network uses the same validated AI models for initial scan analysis.
- Standardized Scoring. The software provides a uniform language for reporting findings to ensure clarity across the entire medical team.
- Centralized Monitoring. Administrators can track diagnostic performance and accuracy metrics across all locations from a single dashboard.
Consistency across the enterprise builds a stronger brand reputation and ensures a high standard of care for all patients. This technical alignment is a key strategic advantage for growing healthcare organizations.
Solving these error-prone bottlenecks requires a commitment to intelligent, integrated diagnostic workflows. This approach secures the highest level of clinical integrity while driving significant financial value for the enterprise.
How AI Supports Radiologists Without Replacing Them
AI functions as a highly specialized assistant that enhances the professional capabilities of medical experts. It takes over the most taxing visual tasks while leaving the final clinical judgment to the experienced radiologist.
Strategic implementation of these tools builds a sustainable environment where technology and human expertise work in harmony. This collaborative model is essential for any enterprise seeking to scale its diagnostic services without compromising on quality.
1. AI Acts As A Second Reader
Providing an independent review of every scan ensures that the primary reader has a reliable safety net for every case. The software scans the entire image field to identify potential threats that might be subtle or located in peripheral areas.
- Independent Review. Algorithms analyze the pixels without being influenced by the clinical history or previous findings of the doctor.
- Suspicious Markers. Digital overlays highlight specific regions of interest to guide the specialist’s attention immediately.
- Radiologist Confirmation. The physician maintains full control by reviewing the AI suggestions and deciding whether to include them in the final report.
This dual-layer approach significantly reduces the risk of oversight during long shifts or high-volume periods. Consequently, it builds a higher level of trust between the diagnostic center and the referring physicians.
2. AI Prioritizes Critical Scans
Identifying life-threatening conditions immediately allows the clinical team to intervene during the most critical windows of treatment. AI imaging diagnostics automatically move high-risk cases to the top of the worklist to ensure they receive immediate attention.
- Stroke and Hemorrhage. Systems detect brain bleeds and vessel blockages within seconds to activate emergency response teams.
- Pulmonary Embolism. Automated alerts notify the radiologist of blood clots in the lungs before they even open the study.
- Trauma Triage. High-impact injuries are identified in the queue to ensure that surgical teams have the data they need right away.
Faster notification leads to better patient outcomes and more efficient use of emergency room resources. This capability is a cornerstone of modern, high-performance trauma centers.
3. AI Automates Repetitive Measurements
Manual tracking of disease progression is one of the most time-consuming and error-prone tasks in the radiology department. AI automates these calculations to provide report-ready values with incredible speed and accuracy.
- Tumor Volumetrics. The software outlines the three-dimensional boundaries of a mass to provide an exact measurement of its size.
- Progression Tracking. Algorithms compare current scans with historical data to calculate the exact percentage of growth or shrinkage.
- Organ Segmentation. Automated tools provide precise metrics on organ health that are critical for chronic disease management.
Automating these tasks frees up the specialist to focus on the nuanced interpretation of the data. This shift improves the overall throughput of the department while maintaining a high standard of quantitative accuracy.
4. AI Improves Report Consistency
Variations in reporting styles can lead to confusion for the referring doctors and make it difficult to track patient health over time. AI encourages the use of structured findings and standardized language across the entire enterprise.
- Standardized Language. The system suggests specific clinical terms to ensure that reports are clear and professional.
- Measurement Templates. Automated values are inserted directly into standardized templates to reduce manual data entry errors.
- Audit-Ready Data. Consistent reporting makes it much easier for administrators to review clinical performance and compliance.
Clear and consistent communication is vital for maintaining a high quality of care across a large hospital network. This technical alignment ensures that every patient record is accurate and easy to interpret for the entire medical team.
5. AI Lets Specialists Focus On Complex Cases
Routine scans often consume a disproportionate amount of a senior radiologist’s time and cognitive energy. By automating the triage and preliminary review of these cases, AI allows experts to dedicate their skills to the most challenging diagnoses.
- Triage Automation. Routine negative scans are identified quickly so the specialist can focus on the cases that require deep analysis.
- Cognitive Relief. Reducing the burden of repetitive visual search tasks prevents the burnout of highly skilled medical staff.
- Resource Allocation. Senior radiologists can spend more time on multidisciplinary consultations and complex surgical planning.
Efficiently managing the workload of a medical team is a major operational advantage for any healthcare business. This strategic use of technology ensures that human talent is applied where it provides the most value.
Integrating these support layers allows for a more resilient and scalable diagnostic infrastructure. This approach demonstrates that AI is not a threat to the profession but a necessary evolution for modern medical excellence.
What Makes An AI Medical Imaging System Accurate In Real Clinical Use?
Real-world accuracy depends on moving beyond laboratory performance to achieve reliability within complex hospital environments. A robust system must maintain its precision despite variations in hardware, patient demographics, and data quality.
Investors should evaluate platforms based on their ability to handle these environmental variables without losing diagnostic integrity. This section outlines the technical and operational requirements for a high-performance clinical AI deployment.
1. High-Quality Imaging Data
The foundational accuracy of any algorithm is directly linked to the diversity and cleanliness of the information used during its development. Consequently, a model trained only on a single demographic or scanner type will likely fail when deployed globally.
- Diverse Datasets. Training data must include various ethnicities, ages, and body types to prevent algorithmic bias.
- Hardware Agnostic. Systems need exposure to images from all major manufacturers like GE, Siemens, and Philips to ensure universal compatibility.
- Expert Labeling. High-quality ground truth relies on meticulous annotation by multiple board-certified specialists to minimize errors.
Ensuring this data breadth allows the software to recognize disease patterns across a wide range of clinical scenarios. This versatility is a critical indicator of a platform’s long-term commercial viability.
2. Clinically Validated AI Models
Laboratory metrics like sensitivity and specificity provide a starting point, but external validation is what proves true clinical utility. Therefore, an enterprise solution must demonstrate consistent performance across different healthcare networks and independent studies.
- Key Metrics. Accuracy is measured through Area Under the Curve (AUC), precision, and recall to ensure a balanced diagnostic performance.
- External Validation. Independent researchers must test the model on data it has never seen before to confirm its reliability.
- Real-World Testing. Performance is monitored in active clinical settings to account for the pressures of a live hospital environment.
Rigorous validation builds the necessary trust for wide-scale adoption by healthcare administrators and clinicians alike. This transparency is what separates professional-grade tools from experimental software.
3. Secure DICOM Image Pipelines
Medical imaging relies on the DICOM standard for the transmission and storage of visual data across different platforms. A secure and efficient pipeline is necessary to ingest, normalize, and route these massive files without data loss.
- Metadata Normalization. Systems must clean and standardize tags from different machines to ensure the AI interprets the orientation and scale correctly.
- De-identification. Privacy is maintained by automatically removing patient-identifiable information before processing the data in the cloud.
- Quality Checks. Automated filters identify and reject blurry or incomplete scans that do not meet the threshold for accurate analysis.
Establishing a robust data pipeline ensures that the AI receives the highest quality input for every analysis. This technical infrastructure is the backbone of any scalable medical imaging enterprise.
4. PACS, RIS, And EHR Integration
For AI to be useful, it must reside where the radiologist already works rather than requiring a separate login or window. Seamless integration with Picture Archiving and Communication Systems (PACS) and Electronic Health Records (EHR) is a non-negotiable requirement.
- Workflow Connection. Findings should appear directly within the specialist’s existing reporting interface to avoid workflow friction.
- Interoperability. Utilizing standards like HL7 and FHIR allows the AI to pull clinical context from lab results and prior medical notes.
- Report Syncing. Automated measurements and findings are pushed directly into the final report to save time and reduce manual entry errors.
Deep integration ensures that the technology actually saves time rather than adding to the administrative burden. This connectivity is what enables the AI to provide a truly holistic diagnostic assessment.
5. Explainable AI Outputs
Clinicians are often hesitant to trust “black box” algorithms that provide a diagnosis without showing their work. Explainable AI provides visual and data-driven evidence to help the specialist understand why the system reached a specific conclusion.
- Visual Heatmaps. Color-coded overlays indicate exactly which pixels the AI identified as suspicious or pathological.
- Confidence Scores. The system provides a probability rating to help the doctor weigh the importance of each finding.
- Region Annotations. Detailed notes explain the specific textures or densities that triggered an alert.
Transparency in decision-making allows the doctor to validate the AI’s logic quickly and confidently. This collaborative verification is essential for maintaining the highest standards of patient safety.
6. Human-In-The-Loop Review
The final diagnostic decision must always remain with the medical professional to ensure accountability and clinical nuance. A human-in-the-loop system allows the radiologist to override or correct the AI while capturing that feedback for future improvements.
- Clinical Override. Specialists can easily dismiss false positives or add findings that the AI may have missed.
- Feedback Loops. The system learns from every human interaction to refine its detection capabilities over time.
- Governance Workflows. Clear protocols define the relationship between algorithmic suggestions and the final medical record.
This balance between automation and human oversight is the cornerstone of responsible medical innovation. It ensures that the technology serves as a tool for excellence rather than a substitute for professional judgment.
7. Continuous Model Monitoring
Accuracy can degrade over time as hospital equipment is updated or patient populations shift, a phenomenon known as model drift. Constant monitoring is necessary to ensure the system remains as precise on day 1,000 as it was on day 1.
- Performance Dashboards. Administrators track accuracy metrics in real-time to identify any sudden drops in sensitivity or specificity.
- Retraining Triggers. Systems automatically alert developers when updated datasets are needed to account for new scanner technologies.
- Alert Performance. The frequency of alerts is analyzed to ensure the system is not causing notification fatigue for the staff.
Proactive maintenance keeps the diagnostic platform at the cutting edge of clinical performance. This ongoing optimization protects the initial investment and ensures continued trust from the medical community.
Building a system that excels across these technical pillars requires a deep understanding of both engineering and medicine. This comprehensive approach is what allows Intellivon to deliver enterprise-grade solutions that redefine the limits of diagnostic accuracy.
How AI Medical Imaging Accuracy Is Measured
Quantifying the performance of AI imaging diagnostics requires a rigorous set of statistical metrics that go beyond simple accuracy percentages. These variables allow enterprise leaders to evaluate how well a system performs in high-stakes clinical scenarios where every detail matters.
Understanding these metrics is essential for selecting a platform that balances patient safety with operational efficiency. This section breaks down the core mathematical pillars used to validate modern diagnostic software.
1. Sensitivity
Sensitivity measures the ability of the algorithm to correctly identify every instance where a disease is actually present. Consequently, a high sensitivity score is non-negotiable for screening programs where missing a single case of cancer or stroke could be fatal.
- True Positive Rate. This metric reflects the percentage of sick patients who are correctly identified by the software.
- Emergency Impact. High sensitivity ensures that life-threatening conditions like intracranial hemorrhages are never overlooked in the triage queue.
- Safety Net. This score represents the reliability of the AI as a second reader to prevent human oversight.
Maximizing sensitivity is the primary goal for early-stage detection tools in oncology and neurology. This ensures that the diagnostic platform captures even the most subtle signals of disease.
2. Specificity
Specificity measures the ability of the system to correctly identify healthy patients as being free of disease. Therefore, high specificity is critical for reducing the number of false alarms that lead to unnecessary biopsies and patient anxiety.
- True Negative Rate. This indicates how often the AI correctly confirms that a scan is normal and requires no intervention.
- Alert Quality. High specificity prevents the specialist from becoming desensitized to AI flags due to constant false positives.
- Overdiagnosis Prevention. Proper calibration ensures that benign anatomical variations are not labeled as suspicious findings.
Maintaining high specificity protects the hospital from the costs associated with redundant follow-up procedures. It ensures that clinical resources are focused entirely on patients who truly need medical attention.
3. Precision And Recall
Precision and recall provide a deeper look into the reliability and thoroughness of the detection model. At the same time, precision focuses on the quality of the positive alerts, while recall measures the system’s ability to find all relevant cases within a dataset.
- Finding Reliability. Precision tells you what percentage of the AI’s flags were actually correct upon human review.
- Missed Case Reduction. Recall is mathematically similar to sensitivity and ensures that the system is not blind to rare pathologies.
- Clinical Usefulness. Balancing these two metrics ensures the software provides actionable insights without overwhelming the radiologist.
A platform with high precision and recall creates a more efficient workflow for the entire diagnostic team. This technical balance is a key driver for successful enterprise adoption.
4. AUC And Confidence Thresholds
The Area Under the Curve (AUC) is a comprehensive metric that evaluates the overall ability of a model to distinguish between normal and abnormal states. It allows developers to tune the confidence thresholds to match the specific needs of a clinical department.
- Model Discrimination. An AUC score close to 1.0 indicates a nearly perfect ability to separate healthy and diseased scans.
- Threshold Tuning. Administrators can adjust the system to be more aggressive in detection or more conservative to avoid false positives.
- Performance Balance. Proper tuning ensures the model operates at its peak efficiency across different imaging modalities.
This flexibility allows the technology to adapt to the unique risk profiles of various medical specialties. It ensures the software remains a relevant tool as clinical requirements evolve over time.
5. False Positive And False Negative Rates
These rates quantify the errors that occur during the diagnostic process and represent the primary risks that AI aims to mitigate. Monitoring these values is essential for managing clinical liability and maintaining high standards of patient care.
- Clinical Risk. High false negative rates are dangerous as they lead to delayed treatments and poor patient outcomes.
- Workflow Burden. High false positive rates lead to notification fatigue, where specialists begin to ignore the AI’s input.
- Patient Anxiety. Reducing these errors directly improves the patient experience by providing more accurate and definitive results.
Minimizing these error rates is a core objective for any enterprise healthcare strategy. This focus on reliability builds long-term trust with both clinicians and patients.
6. Real-World Workflow Metrics
Beyond statistical math, the true value of AI imaging diagnostics is measured by its impact on the daily operations of a hospital. These metrics demonstrate the return on investment by showing how the technology improves overall productivity.
- Report Turnaround Time. High-performance systems significantly reduce the time between a scan being taken and the final report being signed.
- Critical Case Response. AI ensures that emergency findings are flagged and treated in a fraction of the usual time.
- Radiologist Productivity. Automation of measurements and triage allows specialists to handle higher volumes with less cognitive strain.
Tracking these metrics allows healthcare founders to visualize the tangible benefits of digital transformation. This operational data is the most compelling argument for the widespread deployment of diagnostic AI.
Summary Of Core Diagnostic Metrics
The following table provides a quick comparison of the primary metrics used to assess AI performance in a clinical setting.
| Metric | Primary Focus | Clinical Goal |
| Sensitivity | Finding all true cases | Minimize missed diagnoses (False Negatives) |
| Specificity | Avoiding false alarms | Minimize unnecessary follow-ups (False Positives) |
| Precision | Alert accuracy | Ensure that flags are highly reliable |
| AUC | Overall discrimination | Maximize the system’s ability to separate healthy vs. sick |
| Workflow ROI | Operational speed | Reduce turnaround time and specialist fatigue |
Implementing a measurement framework based on these metrics ensures that your diagnostic platform meets the highest standards of clinical excellence.
How To Build An AI Medical Imaging System That Improves Accuracy
Building a resilient AI platform requires a sophisticated blend of medical expertise and enterprise-grade engineering. At Intellivon, we follow a rigorous, stage-gated development process to ensure that every algorithm delivers clinical-grade precision. This systematic approach transforms raw imaging data into a high-performance diagnostic asset for your healthcare organization.
Investors and founders must look beyond the model itself to the entire infrastructure supporting it. The following steps outline our strategic blueprint for developing AI imaging diagnostics that thrive in real-world clinical environments.
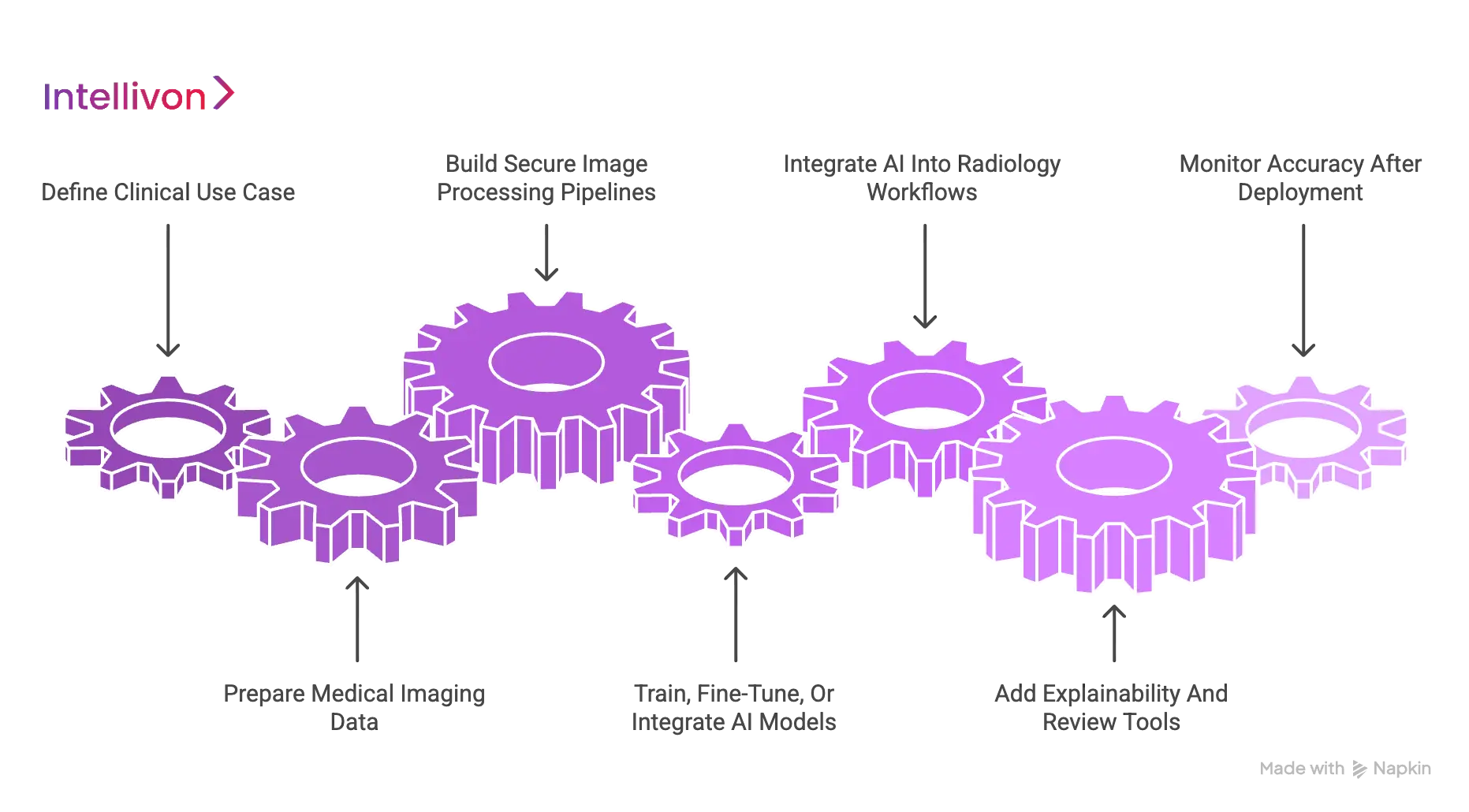
1. Define The Clinical Use Case
Every successful project begins with a narrow and well-defined clinical objective. We identify the specific disease state and imaging modality where AI can provide the highest return on investment and clinical impact.
Therefore, we establish clear accuracy targets and risk thresholds before a single line of code is written.
- Disease Focus. Selecting high-impact areas such as oncology, neurology, or emergency trauma.
- Modality Specificity. Determining if the system will optimize CT, MRI, X-ray, or Ultrasound workflows.
- Workflow Mapping. Identifying exactly where the AI intervention occurs to minimize friction for the medical staff.
| Component | Strategic Goal |
| Target Users | Radiologists, surgeons, or emergency physicians |
| Accuracy Targets | Defining acceptable sensitivity and specificity levels |
| Regulatory Path | Mapping out the FDA or CE certification requirements early |
2. Prepare Medical Imaging Data
The reliability of a diagnostic system is only as good as the data used to train it. We manage complex DICOM datasets through a secure and structured governance framework.
This ensures that every image used in development is accurately labeled by board-certified specialists and stripped of sensitive patient identifiers.
- Annotation Workflows. Implementing multi-reader validation to ensure ground-truth labels are beyond reproach.
- Data Diversity. Sourcing images from various scanner manufacturers to prevent hardware-specific bias.
- Governance. Maintaining strict compliance with global data privacy regulations like HIPAA and GDPR.
This meticulous preparation phase prevents algorithmic drift and ensures the model can handle the messiness of real-world medical data. Quality data is the primary fuel for clinical-grade accuracy.
3. Build Secure Image Processing Pipelines
An enterprise platform requires a robust pipeline to ingest and route massive imaging files without compromising speed or security. We build automated architectures that handle DICOM ingestion and metadata normalization at scale.
This allows for seamless communication between the hospital hardware and the AI processing engine.
- DICOM Ingestion. Creating secure gateways that handle high-volume data transfers from hospital servers.
- Quality Gates. Automated checks identify and reject sub-optimal scans before they reach the analysis stage.
- Storage Architecture. Designing high-availability systems that ensure diagnostic results are always accessible.
Managing the flow of information is just as critical as the analysis itself. A secure pipeline ensures that the right data reaches the right algorithm with zero latency.
4. Train, Fine-Tune, Or Integrate AI Models
We deploy a variety of architectural approaches depending on the complexity of the diagnostic task. This involves training deep learning models for detection, segmentation, and classification.
Furthermore, we fine-tune these architectures using transfer learning to achieve peak performance with smaller, specialized medical datasets.
- Detection Models. Training systems to find nodules, fractures, or hemorrhages with high sensitivity.
- Segmentation. Developing U-Net or transformer-based models for precise anatomical boundary marking.
- Validation. Conducting rigorous internal and external testing to confirm the model meets its accuracy targets.
This technical layer provides the core intelligence of the platform. We focus on creating models that are not only accurate but also robust against noise and artifacts common in clinical imaging.
5. Integrate AI Into Radiology Workflows
For AI to be effective, it must be invisible within the clinician’s existing software environment. We specialize in deep integrations with PACS, RIS, and EHR systems.
This connectivity allows the AI to pull the necessary clinical context and push results directly into the final medical report.
- PACS/RIS Connection. Ensuring that AI markers and findings appear directly on the radiologist’s primary monitor.
- Interoperability. Using HL7 and FHIR standards to sync findings with the patient’s broader medical history.
- Worklist Prioritization. Automatically re-ordering the reporting queue based on the severity of the AI findings.
Integration is the bridge between a laboratory experiment and a functional clinical tool. By removing workflow friction, we ensure high adoption rates among medical professionals.
6. Add Explainability And Review Tools
We prioritize transparency by providing radiologists with the visual evidence they need to trust the AI’s output. This includes heatmaps and bounding boxes that highlight exactly where the algorithm detected an abnormality.
Furthermore, we include human-in-the-loop features that allow for clinical overrides and feedback.
- Visual Indicators. Using digital overlays to draw immediate attention to suspicious regions.
- Confidence Scores. Providing a probability rating for each finding to assist in the final diagnostic decision.
- Feedback Capture. Building tools that allow doctors to correct the AI, creating a continuous loop of improvement.
Explainability transforms the “black box” of AI into a collaborative diagnostic partner. This trust-building layer is essential for the long-term success of any medical imaging platform.
7. Monitor Accuracy After Deployment
Accuracy is not a static metric but an ongoing commitment to quality. We implement continuous monitoring dashboards that track model performance against real-world clinical outcomes.
This allows us to identify and address any signs of model drift before they impact patient care.
- Drift Monitoring. Tracking whether changes in hospital equipment or patient demographics affect the system’s precision.
- Accuracy Dashboards. Providing administrators with real-time views of turnaround times and error rates.
- Retraining Cycles. Establishing automated triggers to update the model with new data as the clinical environment evolves.
Post-deployment monitoring ensures that the initial investment continues to deliver value over the long term. This rigorous oversight is a hallmark of the enterprise-grade solutions provided by Intellivon.
Following this structured development path allows healthcare founders to build platforms that are both medically sound and commercially scalable. This technical maturity is why organizations trust us to lead their digital transformation in medical imaging.
Cost To Build An AI Medical Imaging Diagnostic System?
The cost to build an AI medical imaging diagnostic system depends on how deeply AI is embedded into the clinical workflow. A simple MVP may only support image upload, one modality, and basic AI-assisted detection.
However, an enterprise-grade diagnostic imaging system needs secure DICOM pipelines, PACS/RIS integration, AI model validation, explainable outputs, radiologist review tools, compliance controls, and continuous monitoring.
For healthcare businesses, the real investment is not only in the AI model. It is in building a system that can safely process medical images, return usable findings, support clinical review, and scale across real diagnostic environments.
| AI Medical Imaging Diagnostic System Type | Estimated Development Cost |
| Basic AI Imaging MVP | $50,000–$90,000 |
| Single-Modality AI Diagnostic Support Platform | $90,000–$150,000 |
| AI-Assisted Radiology Workflow Platform | $150,000–$200,000 |
| Multi-Modality AI Medical Imaging Platform | $200,000–$250,000 |
| Enterprise AI Medical Imaging Diagnostic System | $250,000–$280,000+ |
Factors Affecting AI Medical Imaging Development Cost
Several factors can increase or reduce the total development cost. The most important ones include:
- Imaging modality: X-ray-based systems are usually faster to build than complex multi-modality platforms involving CT, MRI, mammography, ultrasound, and PET workflows.
- AI model complexity: A simple classification model costs less than a system that includes detection, segmentation, risk scoring, anomaly detection, and longitudinal scan comparison.
- Dataset availability: If the client already has clean, labeled imaging data, development becomes faster. If the system needs dataset preparation, annotation, de-identification, and quality review, the cost increases.
- PACS/RIS integration: Integrating with hospital imaging systems requires DICOM routing, result formatting, viewer compatibility testing, and workflow validation. This adds cost but is essential for real clinical use.
- Compliance requirements: Healthcare systems need strong data protection, access control, audit logs, encryption, and regulatory-aligned workflows. These controls increase development effort.
- Clinical validation scope: The more the system needs to be tested across datasets, radiologists, scanners, locations, and patient groups, the higher the validation cost.
- Deployment model: Cloud deployment, on-premise deployment, and hybrid deployment have different infrastructure, security, and maintenance requirements.
- Monitoring and retraining: Production AI imaging systems need model performance tracking, drift detection, feedback loops, and retraining workflows to maintain accuracy over time.
How Intellivon Helps Control AI Medical Imaging Development Cost
At Intellivon, we help healthcare companies control development costs by defining the right scope before engineering begins. Instead of building every feature at once, we identify the most valuable imaging modality, clinical use case, workflow requirement, and integration path.
For early-stage products, we can start with a focused MVP that validates one diagnostic workflow. For enterprise clients, we design scalable architecture from the beginning so the platform can later support more modalities, AI models, users, and hospital integrations.
Our approach helps clients avoid expensive rework by planning:
- The right AI model strategy
- Secure DICOM image pipelines
- PACS/RIS integration requirements
- Radiologist review workflows
- Compliance controls
- Deployment architecture
- Monitoring and retraining needs
- Future scalability roadmap
This keeps the system practical, clinically usable, and ready for long-term growth.
For healthcare companies planning to build an AI diagnostic imaging system, the best approach is to start with a clear clinical use case, build the right imaging data pipeline, validate AI outputs carefully, and scale the platform only after the workflow proves reliable.
Conclusion
AI integration marks a fundamental shift toward data-driven precision in clinical workflows. By mitigating human fatigue and identifying subtle pathologies, these systems significantly elevate the standard of diagnostic accuracy. Organizations that prioritize validated models and seamless integration will lead the next generation of healthcare delivery.
Ultimately, this technology empowers specialists to provide faster, more reliable outcomes, ensuring that patient safety remains the cornerstone of modern medical imaging innovation.
Build Accurate AI Medical Imaging Systems With Intellivon
At Intellivon, we build AI medical imaging systems for hospitals, diagnostic imaging chains, teleradiology providers, healthtech enterprises, and medical imaging startups.
Our engineering approach focuses on secure image pipelines, diagnostic AI models, radiologist review workflows, PACS/RIS integration, scalable deployment, and enterprise-grade compliance.
A. Designing Accuracy-Focused Imaging AI Architecture
We define how medical images will move through the system, where AI models will run, how diagnostic outputs will be reviewed, and how results will return to clinical workflows.
Our imaging AI architecture planning includes:
- Clinical use case planning for focused diagnostic accuracy improvement
- Imaging modality selection across X-ray, CT, MRI, ultrasound, or mammography
- Workflow mapping across image intake, AI analysis, review, reporting, and escalation
- AI model strategy for detection, segmentation, classification, or risk scoring
- Data flow architecture for secure image processing and result delivery
- Deployment model planning across cloud, on-premise, or hybrid environments
This ensures the system is not built as a disconnected AI tool. It becomes a clinical-grade diagnostic support platform that fits real hospital and radiology operations.
B. Building Secure DICOM Image Pipelines
We build secure DICOM pipelines that prepare imaging studies for AI analysis, radiologist review, reporting, and long-term clinical use.
Our DICOM image pipeline development includes:
- DICOM ingestion from modalities, PACS, VNA, or external imaging sources
- Metadata normalization for consistent patient, study, and scan information
- De-identification workflows to protect PHI before AI model processing
- Image routing based on modality, body region, urgency, or AI use case
- Secure storage with encryption, access control, and audit visibility
- Image quality checks for corrupted, incomplete, or unsupported studies
This gives healthcare enterprises a reliable foundation for AI-assisted diagnostic imaging at scale.
C. Developing AI Diagnostic Support Models
Intellivon develops and integrates AI models that support radiologists with detection, segmentation, classification, risk scoring, and diagnostic review.
Our AI diagnostic support model development includes:
- Detection models for identifying suspicious findings in medical images
- Segmentation models for outlining tumors, lesions, organs, or disease regions
- Classification models for categorizing scan findings and abnormality types
- Risk scoring systems to support clinical prioritization and review urgency
- Model validation workflows to test accuracy, consistency, and reliability
- Explainable AI outputs through confidence scores, markers, and visual highlights
This allows AI to improve diagnostic accuracy while keeping radiologists in control of final clinical decisions.
D. Integrating AI Into Radiology Workflows
AI imaging systems only create value when they work inside the radiology workflow. Intellivon builds integration layers that connect AI outputs with PACS, RIS, EHR, reporting systems, and review interfaces.
Our radiology workflow integration includes:
- PACS integration for returning AI findings into existing image review systems
- RIS integration for worklist updates, case tracking, and reporting workflows
- EHR connection for linking imaging insights with broader patient records
- Reporting workflow support for structured findings and clinical documentation
- Radiologist review panels for accepting, rejecting, or editing AI outputs
- Feedback loops to capture clinical corrections and improve system performance
This ensures AI results reach clinicians where they already work, instead of forcing them into separate tools or disconnected dashboards.
Build Your AI Medical Imaging System With Intellivon
If you are planning to build an AI medical imaging system for hospitals, diagnostic networks, teleradiology teams, or healthtech users, Intellivon can help you define the right use case, design the architecture, and develop a secure enterprise-ready platform.
From DICOM pipelines and AI diagnostic models to PACS/RIS integrations, radiologist review tools, reporting workflows, compliance controls, and model monitoring, we build AI imaging systems that fit real clinical operations.
Contact Intellivon to build an AI medical imaging system that improves diagnostic accuracy, supports radiologists, and scales with your healthcare business.
FAQs
Q1. How does AI improve accuracy in medical imaging diagnostics?
A1. AI improves accuracy by analyzing scans for subtle patterns, highlighting suspicious regions, measuring lesions consistently, comparing prior images, and helping radiologists prioritize urgent cases. It works best as a clinical support layer, not as a standalone replacement for medical professionals.
Q2. Can AI reduce missed findings in radiology?
A2. Yes. AI can reduce missed findings by acting as a second reader during image review. It can flag small lesions, early disease signs, fractures, bleeds, or suspicious regions that may need closer radiologist attention during high-volume workflows.
Q3. Which medical imaging modalities benefit most from AI?
A3. AI can support CT, MRI, X-ray, mammography, ultrasound, and PET imaging. The strongest use cases depend on the disease, scan type, data quality, clinical workflow, and whether the AI model has been trained and validated for that specific modality.
Q4. Is AI more accurate than radiologists?
A4. AI may outperform humans in specific, narrow imaging tasks, but it should not be treated as a full replacement for radiologists. The strongest clinical value comes when AI supports radiologists with detection, triage, segmentation, measurement, and decision support.
Q5. What makes an AI medical imaging system reliable?
A5. A reliable AI imaging system needs high-quality data, clinically validated models, explainable outputs, secure DICOM pipelines, PACS/RIS integration, radiologist review, audit logs, and continuous model monitoring after deployment.