Key Takeaways:
-
AI RCM platforms cost between $70,000 and $420,000, depending on scope and integrations.
-
Nearly 90% of claim denials are avoidable with predictive AI scrubbing and automation.
-
Modular architecture lets enterprises prioritize high-value workflows before scaling into full cycle automation.
-
Hidden costs like data cleanup, model retraining, and compliance audits must be budgeted early.
-
Intellivon builds HIPAA-compliant AI RCM platforms your organization fully owns and scales confidently.
Building an AI revenue cycle management platform usually costs between USD 50,000 and USD 250,000. The price depends on the project’s scope, integrations, and the level of AI features needed. This cost range exists because AI RCM platforms differ significantly from standard billing tools.
Standard billing software handles form submissions automatically. In contrast, an AI RCM platform needs specific workflows that consider payers, EHR, and PMS integrations, coding intelligence, real-time claim scrubbing, denial prediction models, automated payment posting, compliance checks, and an infrastructure ready for audits. Each of these elements adds complexity, which increases development costs.
However, this investment is not random. Organizations that set up this infrastructure properly recover their costs through fewer denials, quicker reimbursement cycles, and reduced operational expenses for their revenue teams.
Intellivon creates AI RCM platforms for healthcare organizations and digital health companies that require reliable financial systems, rather than basic billing software with an AI label. This blog explains where the costs come from, what factors cause the differences, and how to plan a build that provides measurable returns.
How Much Does It Cost To Build An AI RCM Platform?
The cost to build an AI revenue cycle management platform ranges from $70,000 to $420,000+, depending on AI features, healthcare integrations, compliance needs, automation depth, and enterprise scale.
This is also because the market has seen a significant boom, where the global AI in Revenue Cycle Management (RCM) platform market is valued at USD 20.6–20.8 billion in 2024 and is growing at a CAGR of 24.2% (2025–2034), projected to reach USD 181.7 billion by 2034.
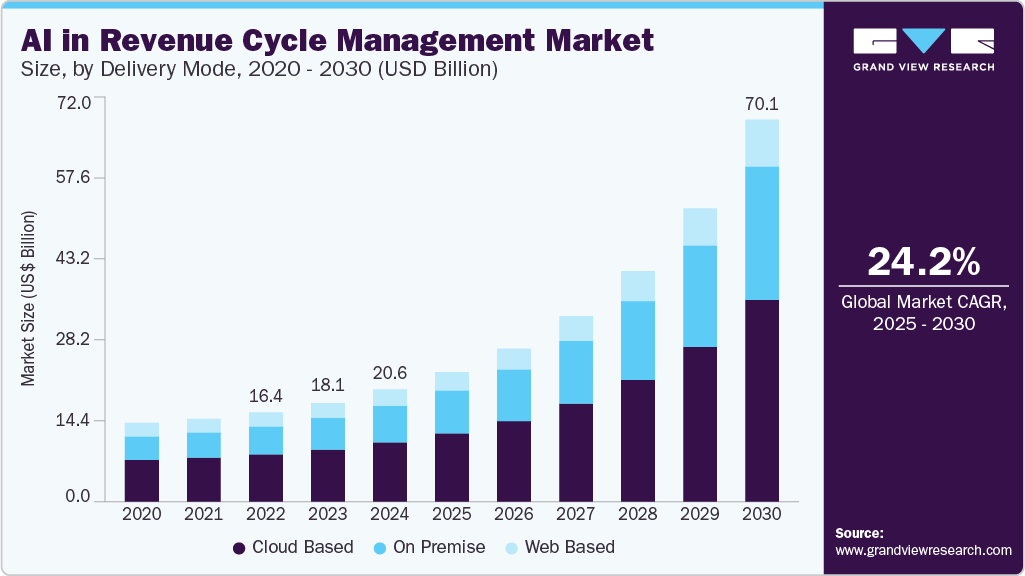
Investors must evaluate the scope of their project to determine the final budget. The following table summarizes the typical investment tiers for modern healthcare billing solutions.
| Platform Tier | Estimated Cost | Core Focus |
| MVP Build | $70,000 – $120,000 | Basic automation and eligibility |
| Mid-Level | $120,000 – $220,000 | AI coding and denial prediction |
| Enterprise | $220,000 – $420,000+ | Full automation and payer rules |
1. AI RCM MVP Cost: $70,000–$120,000
The Minimum Viable Product focuses on the foundational elements of the billing cycle. It aims to solve the most immediate friction points for small practices or initial market testing.
At this level, the software handles basic data entry and tracking without deep machine learning.
- Eligibility checks: Automated verification ensures patients have active coverage before services.
- Claims dashboard: A centralized view allows staff to monitor the status of every submission.
- Basic claim scrubbing: Rules-based engines check for missing fields or simple coding errors.
- Simple denial tracking: The system logs rejected claims for manual follow-up by billers.
- Limited integration: Connectivity is usually restricted to one major EHR or a single clearinghouse.
- Admin features: Basic reporting tools provide snapshots of monthly revenue and pending claims.
2. Mid-Level AI RCM Platform Cost: $120,000–$220,000
Mid-level platforms introduce proactive intelligence to reduce the workload of billing departments. These systems move beyond simple tracking and start predicting outcomes based on historical data.
Therefore, the return on investment becomes more visible through higher clean claim rates.
- AI-assisted coding: Natural Language Processing helps suggest the correct ICD-10 codes from clinical notes.
- Denial prediction: Machine learning models identify claims likely to be rejected before they are sent.
- Work queue automation: The system prioritizes tasks for staff based on the value of the claim.
- Payment tracking: Advanced modules reconcile payments across multiple channels and patient accounts.
- Patient billing: Automated portals send digital invoices and collect payments via secure gateways.
3. Enterprise AI RCM Platform Cost: $220,000–$420,000+
Large healthcare networks require a platform that manages massive data volumes across various locations. This tier includes sophisticated AI models that handle complex payer-specific logic. It is a comprehensive financial ecosystem designed for maximum scale and security.
- Payer-specific rules: The engine adapts to the unique requirements of hundreds of different insurance providers.
- Prior authorization support: AI manages the documentation and submission process for specialty care.
- Revenue forecasting: Predictive analytics provide CFOs with accurate cash flow projections for the coming quarters.
- Advanced compliance: Extensive audit trails and HIPAA-ready infrastructure ensure data remains protected.
- Model monitoring: Continuous updates keep the AI accurate as healthcare regulations and payer behaviors change.
Need a clear cost range for your AI RCM platform? Talk to Intellivon’s healthcare software team and get a scope-based estimate.
Selecting the right tier depends on the specific volume of claims and the complexity of the medical specialties involved. Each level offers a different path toward reducing administrative overhead and capturing lost revenue.
What Is An AI Revenue Cycle Management Platform?
An AI revenue cycle management platform transforms the traditional billing process into a proactive financial system.
It replaces manual data entry with intelligent automation to ensure healthcare providers receive accurate payments for their services.
1. Connects Patient Access, Claims, Payments, And Denials
Modern revenue cycle management is a unified financial workflow rather than a collection of separate features. The platform bridges the gap between the initial patient encounter and the final payment reconciliation.
A truly integrated AI platform ensures that patient insurance data flows seamlessly into the claims engine. This connectivity allows for real-time updates on payment status across the entire organization.
Therefore, teams can manage the full lifecycle of a claim without switching between multiple disconnected software tools.
2. Uses AI To Prevent Revenue Leakage Before It Happens
The primary value of AI in billing is the ability to identify errors before they lead to financial loss. Predictive models analyze historical payer behavior to flag claims that are likely to be rejected. In addition, the system automatically detects missing documentation that might trigger a technical denial.
It matches every claim against a massive library of constantly changing payer rules. High-risk claim alerts notify managers about high-value submissions that require an extra level of manual review. These preventative measures significantly increase the clean claim rate and accelerate the overall speed of the revenue cycle.
3. Gives Revenue Teams A Command Center
An enterprise-grade platform acts as a central infrastructure for all financial operations. It is much more than a simple dashboard for viewing past performance. The command center provides a strategic view of the entire organization and allows for rapid decision-making. Administrators can monitor staff productivity and adjust work queues based on current priorities.
It also offers a deep look into payer performance trends and identifies which insurance companies are delaying payments. This high-level visibility helps leaders maintain a stable cash flow while reducing the administrative burden on their billing teams.
Strategic investment in this technology allows healthcare businesses to focus on growth rather than administrative recovery. A robust platform ensures that every dollar earned is a dollar collected.
Why AI RCM Platform Development Costs More Than Standard Billing Software
AI RCM platforms cost more than standard billing software because they require healthcare integrations, payer logic, predictive models, secure data pipelines, compliance controls, and workflow automation.
1. Healthcare Data Is Fragmented
Healthcare information lives in isolated silos that rarely communicate effectively. Developers must build bridges between disparate systems to create a unified data view.
- Data Sources: The platform must ingest EHR and PMS data alongside payer portals and claims files.
- Reconciliation: Engineers map payment files to patient billing records to ensure accuracy.
- Engineering Effort: Custom API development and extensive data testing drive up the initial investment.
2. Payer Rules Change Often
Insurance companies update plan-specific rules and coding requirements frequently. A static system cannot keep up with these shifts without constant manual updates.
- Dynamic Logic: The engine tracks changing authorization rules and documentation requirements in real time.
- Denial Intelligence: Systems must interpret hundreds of unique denial reasons across various payers.
3. AI Needs Clean
High-quality outcomes depend on the integrity of the underlying data. Industry standards like those from the HFMA emphasize that AI success relies on strict governance and integrated systems.
- Performance Metrics: Platforms must track clean claim rates, cost per claim, and staff productivity.
- Maintenance: Continuous model monitoring prevents AI drift and ensures long-term accuracy.
4. Compliance Cannot Be Added Later
Security must be part of the core architecture from the first day of development. Failing to implement robust controls early creates significant legal risks for the enterprise.
- Strict Controls: Systems require HIPAA-compliant encryption, granular access controls, and immutable audit logs.
- Governance: Formal data governance frameworks manage how sensitive information is stored and shared.
Building a sophisticated AI RCM platform requires specialized expertise to handle these high-stakes requirements. These costs ensure the system remains reliable in a complex financial landscape in the long run.
AI RCM Platform Cost Breakdown By Module
A modular approach allows enterprises to prioritize the most critical financial leaks first. This breakdown helps leaders allocate budgets based on specific operational pain points and automation goals.
The AI RCM platform cost depends on the modules you build, including eligibility verification, coding support, claim scrubbing, denial prediction, payment posting, patient billing, and analytics.
| Module | Estimated Cost (USD) |
| Patient Eligibility Verification | $10,000 – $20,000 |
| AI Charge Capture & Coding | $25,000 – $40,000 |
| Predictive Claim Scrubbing | $30,000 – $50,000 |
| Denial Prevention Engine | $35,000 – $60,000 |
| Payment Posting & Portals | $20,000 – $40,000 |
| Total Estimated Range | $50,000 – $250,000 |
1. Front-End Modules: Eligibility and Authorization
Fixing the revenue cycle starts before the patient even sees a provider. These modules prevent downstream errors by ensuring all administrative data is accurate at the point of entry.
- Verification: Automation checks insurance status in real time to reduce front-end rejections.
- Authorization: Digital workflows manage the complex documentation required by specific payers.
- Impact: Cleaner data at the start leads to faster payments and less manual rework for staff.
2. Mid-Cycle Modules: Coding and Claim Scrubbing
The technical accuracy of a claim determines whether it gets paid or ignored. These tools use intelligence to match medical services with the correct billing codes.
- AI Coding: Systems suggest ICD-10 codes by analyzing clinical notes with high precision.
- Scrubbing: Predictive engines identify missing fields or incorrect modifiers before submission.
- Impact: High clean claim rates reduce the cost per claim and accelerate cash flow.
3. Back-End Modules: Denial Management and Payments
The final stage of the cycle focuses on capturing every dollar owed and improving the patient experience. Automation here reduces the need for large teams of manual collectors.
- Denial Prevention: The platform identifies patterns in rejections to suggest proactive workflow changes.
- Payment Portals: Secure digital interfaces allow patients to pay balances through convenient channels.
- Impact: Modernizing the payment experience increases collection rates and reduces bad debt.
Modular development ensures that each dollar invested targets a specific inefficiency in the billing process. This strategy allows for a scalable rollout that matches the financial growth of the enterprise.
Main Factors That Affect AI RCM Software Development Cost
The total investment for a financial platform depends on technical depth and the complexity of the existing ecosystem. Engineering a system that thinks for itself requires deep medical domain logic.
The main cost factors include platform scope, AI complexity, EHR integrations, payer workflows, claims automation, compliance needs, user roles, data quality, and deployment model.
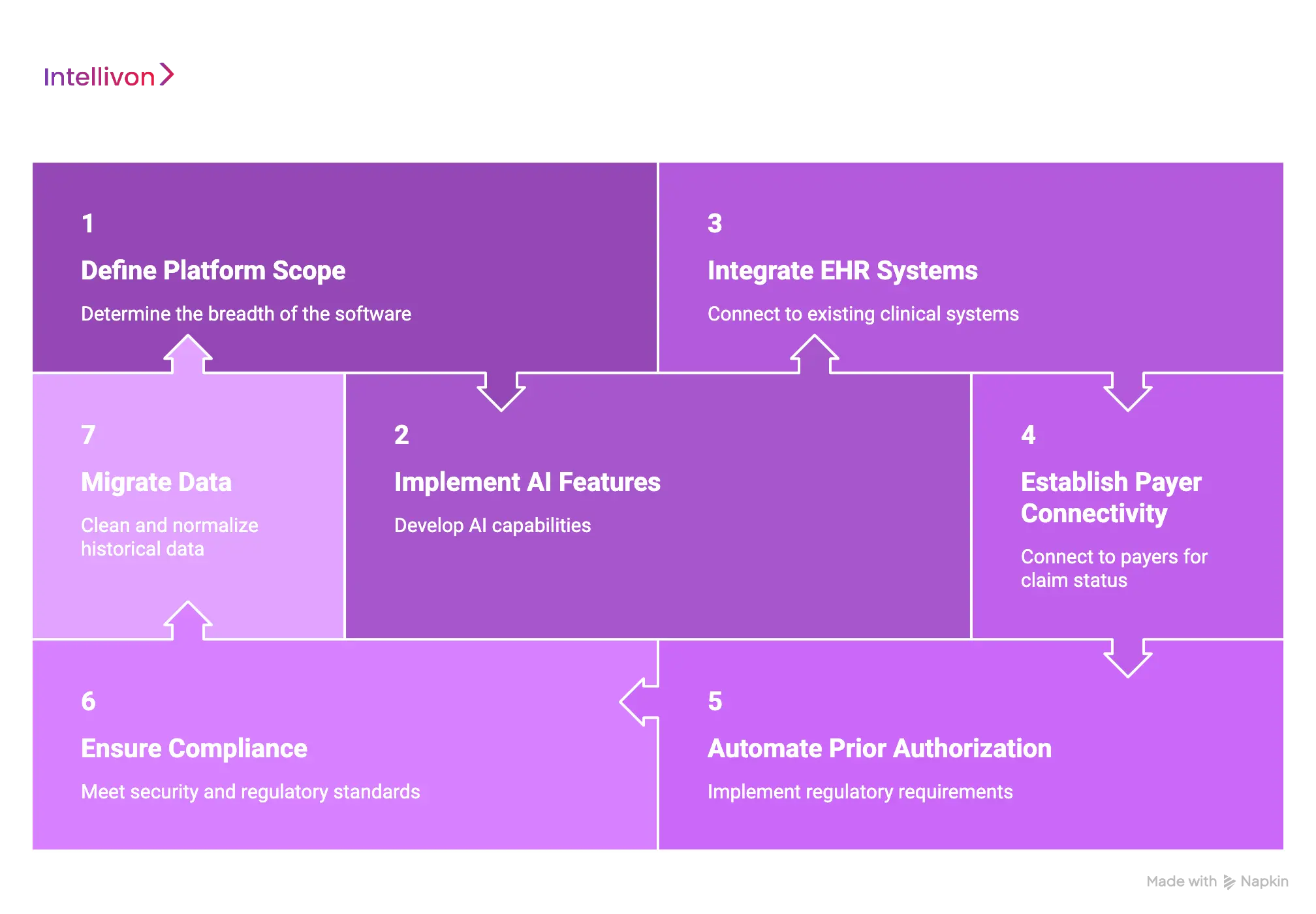
1. Platform Scope
The breadth of the software significantly impacts the final budget. A focused MVP addresses specific leaks while a full enterprise platform manages the entire financial lifecycle.
- Initial Build: Starting with a Minimum Viable Product allows for faster market entry and lower initial costs.
- Scaling Up: Enterprise platforms require multi-location support and complex hierarchy management for large health systems.
- Strategic Choice: Most founders begin with a core module and expand features as they prove the return on investment.
2. AI Feature Complexity
Not all AI carries the same price tag. Simple automation rules are affordable, but predictive modeling requires specialized data science expertise.
- Basic Logic: Rule-based engines for claim scrubbing are relatively straightforward to implement.
- Advanced Models: Predictive denial models and AI-assisted coding require extensive training on massive healthcare datasets.
- Infrastructure: Real-time processing and continuous model retraining add to the ongoing operational expenses.
3. EHR And Practice Management Integration
Connecting to existing clinical systems is one of the most resource-intensive phases of development. Each EHR vendor has unique protocols and data structures that must be synchronized.
- Major Vendors: Integrating with Epic, Cerner, or Athenahealth requires navigating specific API frameworks and certification processes.
- Legacy Systems: Older or custom EHRs often lack modern connectivity and require manual data mapping.
- Technical Burden: High-fidelity integrations ensure that clinical data flows into the billing engine without human intervention.
4. Clearinghouse And Payer Connectivity
The lack of standardization in how payers report claim status remains a major hurdle for developers. According to CAQH, claim status workflows face constant inconsistency because providers must juggle phone calls, portals, and X12 276/277 transactions.
- Manual Burden: Varied integration methods increase the engineering hours needed to build a truly automated tracking system.
- Network Depth: The number of clearinghouses and direct payer connections directly scales the development time.
- Reliability: Robust connectivity ensures the platform receives actionable data rather than generic rejection codes.
5. Prior Authorization Automation
Automating the approval process is now a regulatory priority. CMS has pushed for interoperability and prior authorization changes to reduce the administrative burden on providers.
- Deadlines: New API requirements are primarily due by January 1, 2027, making this a critical feature for new platforms.
- Workflow Integration: Systems must now support real-time coverage discovery and documentation submission within the clinical workflow.
- Compliance Gain: Implementing these standards early ensures the platform meets upcoming federal mandates for electronic exchange.
6. Compliance And Security Requirements
Security cannot be an afterthought in healthcare software. Protecting Protected Health Information (PHI) requires an architecture built on a foundation of trust and strict control.
- Frameworks: Platforms must meet HIPAA standards and be ready for SOC 2 audits from day one.
- Protections: Development includes implementing end-to-end encryption, granular access controls, and immutable audit trails.
- Governance: Formal data management policies ensure that the enterprise remains compliant as it scales its operations.
7. Data Migration And Normalization
Moving historical information into a new AI-driven system is often a messy and expensive process. Old claims data and denial history must be cleaned before they can be used for training.
- Data Cleaning: Normalizing records from different payers and coding eras is essential for accurate predictive modeling.
- Historical Depth: The more years of data migrated, the higher the cost of processing and validation.
- Quality Control: Clean data ensures the AI provides reliable insights rather than amplifying past billing errors.
Understanding these variables allows investors to build a realistic roadmap for their technology. Careful planning around these factors prevents budget overruns and ensures a successful launch.
Hidden Costs Of Building An AI RCM Platform
Hidden AI RCM development costs often include data cleanup, third-party API fees, compliance reviews, security testing, model monitoring, user training, maintenance, and integration changes.
1. Preparing the Foundation: Data and Connectivity
Raw data is rarely ready for AI without significant intervention. Connectivity to the broader healthcare ecosystem also carries recurring financial obligations that builders must factor into their models.
- Data Cleaning: Normalizing years of messy claims history and denial records requires extensive engineering time.
- Third-Party Fees: Many EHR providers and clearinghouses charge monthly fees for API access and data transmission.
- Infrastructure: Hosting sensitive healthcare data requires specialized cloud environments with high-level encryption and redundancy.
2. Ensuring Integrity: Compliance and Security
Maintaining a secure platform is a continuous process rather than a one-time setup. These costs ensure the software remains legal and trusted by the large organizations that use it.
- Security Testing: Regular penetration testing and vulnerability scans are required to maintain a strong defense against breaches.
- Compliance Consulting: Bringing in outside experts for HIPAA or SOC 2 audits ensures the platform meets all federal regulations.
- Audit Trails: Building and storing detailed logs of every data access point consumes significant storage and processing power.
3. Operational Sustainability: Training and Maintenance
The software must evolve alongside the business and the people using it. Investing in the human element and technical upkeep prevents the platform from becoming obsolete or ignored by staff.
- Model Retraining: AI models require periodic updates as payer behaviors shift and new medical codes are introduced.
- User Training: Teaching billing teams to work alongside an AI engine requires structured onboarding and support materials.
- Workflow Redesign: Integrating automation often requires changing how staff handle daily tasks to maximize the efficiency of the new tool.
Addressing these hidden variables early prevents budget surprises and builds confidence with your investment partners. A transparent financial plan ensures the project remains viable from development through daily operation.
MVP Vs Enterprise AI RCM Platform: What Should You Build First?
Choosing the right starting point prevents wasted capital and ensures the technology aligns with your current organizational maturity. Every successful platform begins with a clear understanding of its immediate mission.
An AI RCM MVP should focus on one high-value workflow first, such as denial prediction, eligibility verification, claim scrubbing, or payment tracking, before expanding into full-cycle automation.
1. Build An MVP If You Need Market Validation
A Minimum Viable Product is the most efficient path for startups looking to prove a specific concept. It allows you to test a single hypothesis without the massive overhead of a full financial suite.
- Targeted Focus: You might solve only eligibility errors or claim scrubbing to demonstrate immediate ROI.
- Resource Efficiency: Lower upfront costs mean you can pivot quickly based on early user feedback.
- Strategic Advantage: This path is ideal for SaaS teams looking to secure venture funding or initial pilot customers.
2. Build A Mid-Level Platform If You Already Have Users
Existing billing companies often need to modernize their legacy systems to remain competitive. A mid-level build integrates intelligence into established workflows that already handle real patient data.
- Automation Depth: You move beyond basic rules to implement predictive models for denial management.
- Scale: These platforms handle higher claim volumes across multiple medical specialties effectively.
- Market Fit: This is the best choice for established providers who need to increase their clean claim rates immediately.
3. Build An Enterprise Platform If You Need Operational Control
Large-scale health systems require a robust infrastructure that can manage complex hierarchies and massive data sets. An enterprise build focuses on total visibility and centralized management of the revenue cycle.
- Global Rules: The system manages payer-specific logic across hundreds of different insurance plans.
- Unified View: CFOs gain a single command center to monitor financial health across dozens of locations.
- Ownership: This is built for organizations that want to own their technology stack and eliminate third-party dependencies.
4. Build AI Infrastructure If You Want A Scalable Product
Companies aiming to become the next generation of RCM service providers must focus on the underlying architecture. Building for scale ensures that the platform can support thousands of concurrent users without performance lag.
- Modular Design: Create an ecosystem where new AI models can be plugged in as healthcare regulations change.
- Data Liquidity: Focus on high-speed data pipelines that can normalize information from any EHR source.
- Future Proofing: This approach allows you to sell access to your platform as a white-label solution or a specialized API.
Not sure whether to start with an MVP or a full AI RCM platform? Intellivon helps you define the right build scope before development begins.
The decision rests on your immediate business goals and the specific problems you intend to solve. Starting small often provides the data needed to build a much more effective large-scale system later.
AI Features That Add The Most Value To RCM Platforms
Investing in the right features ensures the platform solves real financial problems rather than just providing data. High-value automation targets the specific stages where revenue is most likely to be lost or delayed.
The most valuable AI RCM features include denial prediction, claim risk scoring, coding assistance, prior authorization intelligence, payment forecasting, appeal drafting, and work queue prioritization.
1. Denial Prediction
Modern platforms analyze historical data to identify claims likely to be rejected before they leave the system. This pre-submission risk assessment allows staff to fix errors while the patient data is still fresh.
- Proactive Analysis: Algorithms compare outgoing claims against millions of past payer responses.
- Risk Scoring: Each claim receives a score indicating the likelihood of a technical or medical necessity denial.
2. AI Claim Scrubbing
Standard scrubbing tools often miss the nuances of changing insurance policies. Intelligent scrubbing uses machine learning to keep up with evolving modifier rules and documentation requirements.
- Rule Matching: The system cross-references claims with specific payer contracts and state regulations.
- Missing Data Alerts: The software flags claims that lack the specific documentation needed for high-value procedures.
3. AI-Assisted Coding
Translating clinical notes into billable codes is a major bottleneck in the revenue cycle. AI can read physician notes and suggest the most accurate ICD-10 or CPT codes for review.
- Efficiency: Automated suggestions reduce the time professional coders spend on routine visits.
- Accuracy: The system identifies potential coding gaps that could lead to undercoding or audits.
4. Prior Authorization Intelligence
Managing approvals is one of the most manual and frustrating tasks in healthcare. AI streamlines this by matching patient procedures against payer-specific authorization requirements automatically.
- Status Tracking: The platform monitors payer portals and updates approval statuses in real time.
- Documentation Support: The system alerts staff exactly which clinical files are needed to secure an approval.
5. Work Queue Prioritization
Not every claim carries the same financial weight or urgency. AI ranks tasks for the billing team based on a combination of dollar value, filing deadlines, and historical payer behavior.
- Strategic Focus: Staff members are automatically directed to the claims with the highest recovery potential.
- Deadline Management: The system ensures that claims nearing their filing limit move to the top of the list.
6. Appeal Letter Drafting
When denials do happen, the speed of the appeal often determines the outcome. Controlled generative AI can draft personalized appeal letters by pulling relevant clinical data and payer language.
- Templates: The AI uses approved legal and clinical templates to ensure consistency and compliance.
- Human Review: Billing specialists review and sign off on drafts before they are sent to the insurance company.
7. Revenue Forecasting
Predictive analytics provides leadership with a clear view of future cash flow. By analyzing current A/R and historical payment speeds, the platform estimates exactly when money will arrive.
- Cash Flow Visibility: CFOs can see expected reimbursements for the next thirty to ninety days.
- Risk Identification: The system flags shifts in payer behavior that might indicate future payment delays or systemic issues.
Selecting these features based on your specific medical specialty ensures the highest return on investment. A well-designed platform turns complex data into a predictable and steady stream of revenue.
AI RCM Platform Architecture and Tech Stack
Modern revenue cycle management requires a layered architecture that balances data fluidity with extreme security. Every layer in this stack serves a specific functional purpose and represents a distinct portion of the development investment.
AI RCM platform architecture includes data ingestion, EHR integration, claims processing, AI models, payer rules, workflow automation, dashboards, compliance controls, and secure cloud infrastructure.
| Architecture Layer | Primary Function | Business Impact |
| Data Ingestion | Connects to EHR and PMS systems | Eliminates manual data entry |
| AI Prediction | Analyzes denial risks and coding | Prevents revenue leakage |
| Rules Engine | Matches claims to payer logic | Ensures high clean claim rates |
| Security Layer | Manages HIPAA and encryption | Protects against legal liability |
1. Data Ingestion and Integration Layer
This layer acts as the entry point for all clinical and administrative information. It must normalize data from various sources to ensure the AI models receive high-quality input.
- Purpose: It bridges the gap between the platform and external systems like Epic or Cerner.
- Tech Stack: Developers use FastAPI and Node.js for high-speed processing. Connectivity relies on HL7 and FHIR standards to maintain healthcare interoperability.
2. AI Prediction and Machine Learning Layer
The prediction layer is the brain of the platform, where complex algorithms identify patterns in claims and denials. This is the most research-intensive part of the development process.
- Purpose: It identifies denial risks and suggests optimal medical codes by analyzing clinical notes.
- Tech Stack: Data scientists utilize TensorFlow, PyTorch, and Scikit-learn. Apache Airflow manages the data pipelines that feed these models.
3. Workflow Orchestration and Rules Engine
This layer translates technical data into actionable tasks for the billing team. It ensures that the most important claims are handled first according to specific payer requirements.
- Purpose: It automates the routing of claims and manages the logic for hundreds of different insurance plans.
- Tech Stack: Python powers the core logic while PostgreSQL or MongoDB stores complex rule sets. React.js or Next.js provides the interface for staff to manage their daily work queues.
4. Security, Compliance, and Monitoring Layer
Healthcare platforms must operate within a fortress of digital protection. This layer ensures that every action is logged and every piece of patient data is encrypted.
- Purpose: It maintains HIPAA compliance and provides the audit trails necessary for enterprise-grade security.
- Tech Stack: Deployment happens on AWS or Azure using Docker and Kubernetes. Security protocols include OAuth 2.0, multi-factor authentication, and end-to-end encryption.
5. Analytics and Reporting Dashboard
The final layer converts raw operational data into strategic insights for leadership. It provides the visibility needed to manage the financial health of the entire organization.
- Purpose: It tracks clean claim rates and provides accurate revenue forecasting for the CFO.
- Tech Stack: Integration with Power BI or Tableau allows for custom visual reporting. High-performance databases ensure that dashboards update in real time.
Building a platform with this level of architectural depth ensures long-term scalability and reliability. A well-chosen tech stack reduces technical debt and allows the system to grow with the enterprise.
Development Timeline For An AI RCM Platform
A structured timeline is essential for aligning technical delivery with financial expectations. Building an intelligent billing system is a multi-phased journey that requires careful coordination between software engineers and healthcare domain experts.
AI RCM platform development usually takes 4–12+ months, depending on product scope, integrations, AI model complexity, data readiness, compliance, and enterprise deployment needs.
| Project Scope | Estimated Timeline | Primary Objective |
| MVP | 4–6 months | Core automation and initial validation |
| Mid-level platform | 6–9 months | Advanced AI and deeper integrations |
| Enterprise platform | 9–12+ months | Full-cycle automation and multi-entity support |
| AI RCM Infrastructure | 12–18+ months | Scalable ecosystem for diverse health networks |
Phase 1: Strategy and Architecture (Months 1–2)
The initial phase focuses on aligning the technology with the existing operational workflows. Rushing this stage often leads to integration failures later in the development cycle.
- Discovery: Teams identify the specific financial leaks and manual bottlenecks that the AI must solve first.
- Workflow Mapping: Specialists document the path of a claim from patient registration to final payment reconciliation.
- Compliance Setup: The foundation for HIPAA and data security is established to ensure the architecture is protected.
Phase 2: Design and Core Infrastructure (Months 3–5)
During this phase, the digital environment is built to handle sensitive healthcare data. Developers focus on creating a user interface that makes complex AI insights easy for billing staff to act upon.
- UI/UX Design: Designers create intuitive dashboards that prioritize high-value tasks and reduce cognitive load.
- Backend Development: Engineers build the secure databases and server logic required to process massive claim volumes.
- Data Ingestion: The initial pipelines for EHR and Practice Management System connectivity are established.
Phase 3: AI Development and System Integration (Months 6–9)
This is the most technical stage, where the intelligence of the platform is actually created. It involves training models on historical data and ensuring the software communicates correctly with payers.
- AI Model Development: Data scientists build and train the predictive engines for denial management and coding assistance.
- Integration Development: The platform is connected to clearinghouses and insurance portals for real-time data exchange.
- Testing: Rigorous quality assurance ensures that the AI provides accurate suggestions without introducing new errors.
Phase 4: Deployment and Continuous Optimization (Months 10+)
The final phase involves moving the platform into a live environment and training the staff. Deployment is treated as a gradual transition rather than a single event to ensure operational stability.
- Enterprise Deployment: The software is rolled out across different departments or locations in controlled stages.
- Staff Training: Billing teams learn to use the AI insights to improve their daily productivity and recovery rates.
- Monitoring: Continuous tracking of model performance and system health ensures the platform remains accurate as payer rules change.
Planning for these phases allows organizations to set realistic milestones and avoid the pitfalls of fragmented development. A clear roadmap ensures that the final product is not just functional but truly transformative for the revenue cycle.
Reduce Development Cost Without Weakening The Product
Smart financial leadership focuses on maximizing impact while minimizing technical waste. You can build a high-performance system by prioritizing the most expensive leaks in your revenue cycle before expanding the software footprint.
You can reduce AI RCM development cost by starting with one high-value workflow, using modular architecture, prioritizing integrations, reusing secure components, and scaling AI gradually.
1. Start with Denial Prediction or Claim Scrubbing
The most efficient way to see an immediate return on investment is to target the points where revenue is most frequently lost. By focusing on these high-impact areas, the platform begins paying for itself almost immediately.
- Preventing Loss: These modules address technical errors and payer mismatches before they turn into unpaid claims.
- Focused Data: Starting here allows you to train your initial AI models on the most critical financial data points.
- Operational Wins: Staff can see the benefits of automation quickly, which builds internal support for the larger project.
2. Avoid Building Every Module in Phase One
Trying to replicate a full enterprise suite in the first release often leads to budget overruns and missed deadlines. Focusing on core functionality ensures that the initial launch is stable and effective.
- Scope Control: Limiting the first phase to essential features keeps the development team focused on quality over quantity.
- Market Testing: An initial version allows you to gather real-world user feedback before committing to the next set of features.
- Capital Preservation: You save significant resources by not building complex modules that your specific workflow may not even require.
3. Use Modular Architecture
A flexible foundation is the key to a long-lasting and cost-effective platform. Designing the system as a collection of independent services prevents the need for expensive rewrites as your needs evolve.
- Scalability: You can add new features or payer connections like building blocks, without disrupting the existing system.
- Easier Maintenance: Troubleshooting a specific module is faster and cheaper than trying to fix a monolithic software structure.
- Future Proofing: This approach allows you to swap out specific technologies as newer AI models or healthcare standards emerge.
4. Prioritize Integrations by Business Value
Not all Electronic Health Records (EHR) or payer portals are created equal in terms of their impact on your bottom line. Focus your engineering resources on the connections that handle the bulk of your financial volume.
- High-Volume First: Connect with the EHRs and insurance companies that represent at least 80% of your current claims.
- Reduced Complexity: Mastering a few key integrations first is more efficient than struggling with dozens of low-volume legacy systems.
- Strategic Growth: You can gradually add specialized or lower-volume integrations once the primary revenue streams are fully automated.
5. Clean Data Before Model Development
AI is only as good as the information it processes. Investing time in organizing your historical claims data early prevents the high cost of retraining inaccurate models later.
- Accuracy: Normalizing data ensures your denial prediction engine identifies real patterns rather than clerical noise.
- Efficiency: Clean data speeds up the training process for your data science team and reduces the trial-and-error phase.
- Integrity: High-quality data pipelines provide a reliable foundation for all future AI-driven insights and reporting.
6. Build with Compliance from Day One
In healthcare, security is a core feature that cannot be added as an afterthought. Integrating strict protections from the start is significantly more affordable than performing a retrospective security overhaul.
- Legal Safety: Implementing HIPAA-compliant encryption and audit trails early protects the enterprise from massive potential fines.
- Trust: Decision-makers are more likely to approve a platform that has security baked into its very architecture.
- Seamless Audits: Having compliance controls in place simplifies future SOC 2 or regulatory reviews as you scale.
7. Use Human-in-the-Loop AI First
Full automation is a long-term goal, but the safest and most cost-effective entry point is collaborative intelligence. This approach allows the AI to learn from experts while ensuring every claim remains accurate.
- Risk Mitigation: Human specialists act as a final check, preventing the AI from making costly automated mistakes during its learning phase.
- Model Training: Every manual correction provides the system with the data it needs to improve its autonomous capabilities.
- Staff Confidence: Employees are more likely to adopt the technology if they feel it supports their work rather than replacing it without oversight.
8. Add Automation Gradually
A phased rollout allows for a smoother transition and better budget management. By increasing the level of autonomy in small steps, you ensure the organization remains stable throughout the digital transformation.
- Continuous Improvement: Each new automation feature can be tested and refined based on the performance of previous phases.
- Budget Alignment: You can fund subsequent automation rounds using the savings captured from the initial modules.
- Operational Stability: Gradually shifting the workload prevents the chaos that often follows a sudden switch to fully automated systems.
Following this disciplined roadmap keeps the project within a manageable financial scope. It allows the enterprise to capture immediate savings that can then fund the next stage of growth.
ROI Of AI Revenue Cycle Management Software
Investing in an AI RCM platform is a critical strategy for revenue protection. The data shows that moving from manual to intelligent billing is a direct path to higher margins and operational stability.
AI RCM software improves ROI by reducing avoidable denials, improving clean claim rates, lowering manual rework, accelerating reimbursements, and giving finance teams better revenue visibility.
1. Fewer Denied Claims and Faster Correction
The 2025 CAQH Index reports that over $20 billion in annual savings remain untapped through the automation of administrative workflows. Initial claim denial rates reached 11.65% this year, yet industry benchmarks confirm that nearly 90% of these rejections are entirely avoidable.
- Predictive Prevention: AI platforms can reduce denial rates by up to 40% by identifying errors before submission.
- Rapid Rework: While manual claims resolution takes 12–18 days, automated systems cut this cycle to just 2–4 days.
- First-Pass Success: AI-enabled organizations consistently achieve 96–98% first-pass acceptance rates, compared to the industry average of 85%.
2. Reduced Manual Follow-Up and Better Productivity
The American Medical Association (AMA) highlights that administrative burdens are a primary driver of physician and staff burnout. Automating repetitive inquiries allows your most expensive human assets to focus on complex cases that require genuine clinical judgment.
- Cost Reduction: Processing a manual claim costs between $15 and $25, while automated adjudication drops that expense by 60–70%.
- Staff Efficiency: Automation reduces the time spent on billing by up to 60%, allowing a leaner team to manage higher claim volumes.
- Accuracy Gains: AI reduces the 12% error rate typical of manual entry down to less than 3%, significantly lowering the need for rework.
3. Lower Cost to Collect and Stronger Cash Flow
Healthcare organizations traditionally spend 2 to 4 cents to collect every dollar of revenue they earn. McKinsey reports that agentic AI and advanced automation can cut this cost-to-collect by 30 to 60%.
- Direct Savings: For a health system with $200 million in revenue, a 1% improvement in collection efficiency adds $2 million directly to the bottom line.
- Faster Reimbursement: Organizations using advanced analytics see an average ROI of 147% within three years as days in A/R drop significantly.
- Revenue Visibility: Predictive forecasting provides CFOs with a clear view of expected payments, reducing the uncertainty that plagues manual revenue cycles.
4. Better Authorization Tracking and Compliance
The complexity of prior authorizations has increased, with 61% of physicians reporting that payer AI is making denials more frequent. Transitioning to electronic authorization, which rose to 40% adoption this year, is essential for staying ahead of payer scrutiny.
- Regulatory Alignment: CMS requirements for API-based interoperability by 2027 make AI infrastructure a non-negotiable compliance investment.
- Error Prevention: AI matches patient data against thousands of constantly changing payer rules to ensure every claim is documentation-ready.
- Audit Readiness: Automated systems maintain immutable logs, ensuring your organization is always prepared for regulatory or payer audits.
AI RCM is an operational cost-control and revenue-protection investment. By leveraging these intelligent systems, enterprises can stop chasing payments and start capturing the full value of the care they provide.
Conclusion
Building an AI revenue cycle management platform is a strategic pivot from reactive billing to proactive financial intelligence. While the initial investment varies based on complexity, the long-term gains in clean claim rates and reduced administrative overhead are undeniable.
By prioritizing high-value modules and scalable architecture, enterprises can secure their cash flow against evolving payer rules. Investing in automation today ensures a leaner, more resilient financial future.
Build AI Revenue Cycle Management Software With Intellivon
A. We Build Payor-Aware AI Workflows
RCM software becomes valuable when it understands how payers behave. A generic billing workflow cannot prevent denials, prioritize risky claims, or guide teams through payer-specific requirements.
Intellivon builds payer-aware AI workflows that help revenue teams catch problems before claims move forward. The system can score claim risk, flag missing documentation, identify denial patterns, and help teams focus on the claims that need attention first.
We develop workflows for:
- Claim risk scoring based on payer, code, and documentation patterns
- Denial prediction before claim submission
- Prior authorization logic for requirement checks and status tracking
- Documentation checks for missing or inconsistent claim details
- Work queue prioritization based on risk, value, and urgency
- Appeal support for denied claims and follow-up actions
As a result, your RCM platform does more than process claims. It helps teams make better revenue decisions earlier in the workflow.
B. We Integrate Your RCM Platform With Healthcare Systems
AI RCM software cannot work in isolation. It needs secure access to clinical, billing, payer, payment, and reporting data. Without strong integrations, teams still end up switching between systems and correcting errors manually.
Intellivon builds RCM platforms that connect with the healthcare systems your teams already use. We design integration flows that keep patient data, claim records, payment updates, denial information, and performance reports moving through one connected platform.
We integrate with:
- EHR systems for patient, encounter, and clinical data
- Practice management systems for billing and scheduling workflows
- Clearinghouses for claims submission and status tracking
- Payer portals for eligibility, authorization, and claim updates
- Payment gateways for patient payments and transaction records
- Reporting tools for finance, operations, and leadership dashboards
This gives your team a clearer view of revenue activity and reduces the manual work caused by disconnected systems.
C. We Make AI RCM Platforms Secure And Scalable
Healthcare revenue platforms handle sensitive patient, billing, insurance, and payment data. That means security, compliance, access control, and audit visibility cannot be treated as later-stage additions.
Intellivon designs AI RCM platforms with a secure architecture from the beginning. We add the controls needed to protect PHI, manage users, track actions, monitor AI outputs, and support enterprise-level deployment.
Our approach includes:
- HIPAA-ready architecture for healthcare data protection
- PHI protection through encryption and secure data handling
- Role-based access for billing, coding, finance, and admin teams
- Audit logs to track claim actions, reviews, and system changes
- Secure cloud deployment for reliable platform performance
- Model monitoring to track AI accuracy, drift, and decision quality
This helps your RCM platform stay reliable as claim volume grows, workflows expand, and more teams depend on the system.
If you are planning to build an AI revenue cycle management platform, contact Intellivon to define your scope, estimate your development cost, and build a system designed for real healthcare revenue workflows.
Common Queries
Q1. How much does it cost to build an AI RCM platform?
A1. The cost to build an AI RCM platform usually ranges from $70,000 to $420,000+, depending on scope, AI modules, EHR integrations, payer workflows, compliance, and reporting needs. A focused MVP costs less, while enterprise systems with denial prediction, prior authorization, coding support, and analytics need higher investment.
Q2. Can AI really reduce claim denials in revenue cycle management?
A2. Yes, AI can reduce claim denials when it checks claims before submission, flags missing documentation, reviews payer rules, predicts denial risk, and prioritizes high-risk claims. However, it works best with clean data, strong human review, and proper integration across billing, coding, EHR, and payer workflows.
Q3. What integrations does an AI RCM platform need?
A3. An AI RCM platform usually needs integrations with EHR systems, practice management software, clearinghouses, payer portals, eligibility verification tools, payment gateways, and reporting systems. These integrations help claims, remittances, denials, patient data, and payment updates move through one connected workflow instead of staying scattered across tools.
Q4. Should we build a full AI RCM platform or start with one module?
A4. Most healthcare companies should start with one high-value module, such as denial prediction, claim scrubbing, eligibility checks, or prior authorization automation. This reduces cost, proves ROI faster, and helps teams test adoption before expanding into full-cycle revenue automation, advanced analytics, payment posting, and enterprise reporting.